Abstract
Background
The positive impact of Roux-en-Y gastric bypass (RYGB) on metabolic syndrome and glycemic control has been proven in obese patients. One anastomosis gastric bypass (OAGB) is a simple, effective and easy to learn procedure. OAGB provides encouraging results for the treatment of diabetes obese patients, but does it have the ability to be an alternative procedure to RYGB in the treatment of these patients? The aim of this study is to evaluate the outcomes of OAGB on diabetic obese patients at the bariatric centre of our university hospital. By extension, we evaluated the possibility of BMI and the preoperative antidiabetic medication usage to be predictive factors for postoperative diabetes resolution.
Methods
This is a retrospective single-centre study of 472 diabetic patients who underwent OAGB from November 2009 to December 2015. All patients were followed-up for at least 1 year, and up to 3 years, where available. Weight, HbA1c, and anti-diabetic medications were recorded at baseline, 3, 6, 12, 24 and 36 months.
Results
A total of 472 patients have been followed-up for 1 year and 361 for 3 years. The mean BMI decreased from 46.8 ± 7.2 to 29.5 ± 2.8 kg/m2 and HbA1c from 9.6 ± 1.3 to 5.7 ± 1.5% at the 12-month follow-up. At the 3-year follow-up, the mean BMI was 32.1 ± 3.3 and HbA1c mean was 5.8 ± 0.9%. Diabetes remission was achieved by 84.1% of patients.
Conclusions
OAGB can be an excellent alternative to RYGB for the treatment of diabetes and obesity. Pre-operative medications may be used to predict postoperative diabetes remission, but not BMI.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Morbid obesity and its associated comorbidities including type 2 diabetes mellitus (T2DM) are increasing at alarming rates [1]. T2DM affects more than 312 million people worldwide and about 80% of the diagnosed cases are obese [2]. The term ‘diabesity’ describes the overlap between T2DM and obesity [3]. The risk of developing T2DM increases progressively with increased body mass index (BMI). In fact, in people with BMI >27 kg/m2, the risk of developing T2DM increases by 20% for every 1 kg/m2 increase in the BMI [4].
Despite the marked advances in the treatment interventions of T2DM, less than 50% of patients achieve the therapeutic goal of a glycated haemoglobin (HbA1c) <7% [5]. Patients with uncontrolled diabetes are at higher risk of developing microvascular and macrovascular complications such as myocardial infarction, ischemic stroke, blindness, neuropathy, and end-stage renal disease [6, 7]. Although approximately 80% of patients diagnosed with diabetes are obese, only 20–30% of them seek metabolic surgery [8, 9].
Metabolic surgery is the most effective treatment for clinically severe obesity (BMI > 35 kg/m2) and its associated comorbidities such as T2DM [10, 11]. Metabolic surgery differs conceptually from bariatric surgery as the latter aims to improve body weight as the primary objective and improvement in comorbidities as the secondary objective. On the other hand, metabolic surgery aims to improve glycaemic control in obese patients with weight loss being a helpful ‘side effect’. Thus metabolic surgery is now considered a new treatment modality for T2DM in patients with BMI <35 kg/m2 [12, 13]. Several randomised trials have previously demonstrated that metabolic surgery is superior to non-surgical interventions for the control of hyperglycaemia in T2DM patients [14, 15].
The postoperative improvement of the metabolic milieu such as remission of diabetes is attributed to weight loss-dependent and independent mechanisms. Gastric bypass results in greater remission rates of diabetes when compared to adjustable gastric banding (AGB) or vertical sleeve gastrectomy (VSG), even if similar postoperative weight loss is achieved [16].
Although Roux-en-Y gastric bypass (RYGB) is accepted as the gold standard procedure of metabolic surgery, it is associated with high complication rates particularly with un-experienced surgeons [2, 17]. One anastomosis gastric bypass (OAGB) is a simple, easy, and reversible procedure with fewer complication rate and equal or even potentially better efficacy for the treatment of obesity and T2DM than RYGB [18,19,20,21]. The short- and long-term follow-up outcomes of the OAGB showed impressive diabetic remission rates even in patients with lower BMI [22, 23]. Therefore, the aim of this study is to evaluate the outcome of OAGB on diabetic obese patients at the bariatric centre of our university hospital. By extension, we evaluate the possibility of BMI and the preoperative antidiabetic medication usage to be predictive factors for postoperative diabetes resolution.
Material and Methods
Between November 2009 and December 2015, a total of 1520 obese patients underwent OAGB in our bariatric unit; 683 of those patients were diabetic. Out of those patients, 472 (349 women) patients were applicable for this study and had at least 1-year follow-up (465 patients were T2DM and 7 patients were T1DM). All patients were preoperatively evaluated by a multidisciplinary and integrated medical team. Pre- and postsurgical management were conducted by the bariatric surgery team. The inclusion criteria were based on the recommendations of the National Institutes of Health Consensus Development Panel, created in 1991 [24]. Patients with Barrett’s oesophagus and severe gastroesophageal reflux disease (GERD) were a contraindication to OAGB and thus shifted to receive an RYGB instead.
Data Collection and Management
Clinical evaluation forms were used for the collection of demographic and clinic data. The data sources included office and hospital charts, interviews with patients, physicians’ reports, follow-up notes and telephone contacts. All data were entred into a computer database that was maintained prospectively.
Preoperative Evaluation
Patients were evaluated by history and physical examination. The surgical details, risks, benefits and consequences of the OAGB procedure and its effect on DM were discussed in details during the initial meeting of the patient with the surgeon, dietician and diabetologist. Laboratory assessments included complete blood count, prothrombin concentration, random blood sugar, liver function test, renal function test, thyroid function, glycated haemoglobin (HbA1c) and serology for viral hepatitis or HIV. Patients with HbA1c >6.5% were referred to the diabetology department for a medical management of DM and to assess any associated secondary complications. These patients were followed-up until a preoperative satisfactory level of HbA1c was achieved. Written informed consents were obtained from all patients before being scheduled for the surgery.
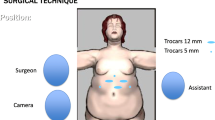
Operative Technique
The five-port technique which was previously described by Rutledge was used [25]. A long and narrow gastric tube calibrated with a 36-French bougie was created, starting by one horizontal gastrointestinal anastomosing (GIA) stapler loaded with cartridges (4.8 mm staples) at the level of the crow’s foot, then three to four vertical 60-mm GIA upward to the angle of His. There was no need for reinforcement of the staple lines with continuous sutures in the majority of patients. Then, antecolic end to side anastomosis between the gastric pouch and jejunum using a posterior 30-mm roticulator endo-GIA stapler and an anterior hand suture at a distance 150–300 cm distal to the ligament of Treitz based on the BMI of the patient was performed. Intraoperative methylene blue test for leak was performed in all patients. In the majority of cases, abdominal drain was inserted and no nasogastric tube was needed.
Postoperative Care
Only water was allowed on the evening of the surgery and patients were informed about the importance of early (2–4 h) postoperative ambulation. Patients had to follow a clear fluid diet for 10 days postoperatively followed by a slow introduction of semi-solid food. By the postoperative week 4, solid food was allowed. At discharge, all patients received detailed dietary instruction sheets and were instructed to take daily multivitamins, supplemental minerals and proton pump inhibitor (PPI) prophylaxis for at least 6 months. Follow-up appointments were scheduled at 2 weeks postoperatively then monthly for the first year, increasing every 3 months thereafter.
Diagnosing Criteria of DM and Definition of Diabetes Remission
The preoperative diagnosis of type 2 diabetes mellitus (T2DM) in the current series was based on the criteria of the American Diabetes Association [26] after adding the HbA1c by the International Expert Committee [26, 27]. The preoperative T1DM defined as the inability to achieve glycaemic control with non-insulin therapies and random C-peptide level <0.6 nmol/l or fasting C-peptide level <0.25 nmol/l [28]. Complete remission of DM was defined as HbA1c <6.0% without anti-diabetic medication for 1 year. Partial remission was defined as HbA1c <6.5% for at least 1 year without anti-diabetes medications. Improved disease was defined as HbA1c <7.0% for at least 1 year. These definitions were based on the ADA criteria for DM remissions [29].
Statistical Analysis
Data are presented as mean ± SD or as percentages when appropriate. The continuous data through the first year follow-up were compared to the baseline data by paired t test and compared to the 3-year follow-up data by unpaired t test after using Levene’s test to assess the equality of variance. Statistical significance was set at p values <0.05. All data were analysed using SPSS version 15.0 for Windows (SPSS Inc., Chicago, IL, USA).
Results
Preoperative demographics and patient characteristics are shown in Table 1. The mean age of the study subjects was 42.5 ± 16.6 years. The mean preoperative weight was 125.8 ± 24.8 kg, BMI was 46.8 ± 7.2 kg/m2 and the preoperative HbA1c was 9.6 ± 1.3% (Table 1).
Regarding the preoperative diabetes medications, 43 (9.1%) patients had a stable HbA1c (around 6.5%) without receiving any treatment, 154 (32.6%) received one oral hypoglycemic drug, 146 (30.9%) received two, 29 (6.1%) received three different types of oral drugs and 100 (21.9%) required insulin to stabilise their HbA1c in the normal range. All patients were followed up for 1 year, but only 361 of them were applicable for 3 years of follow-up.
Complications
All patients underwent laparoscopic OAGB with no mortality and the overall complication rate was 6.8%. Six (1.3%) patients presented with abdominal bleeding requiring blood transfusions. In five of these patients, the bleeding was related to the trocar insertion site, and all cases were managed conservatively. One patient developed gastrointestinal bleeding; this patient was managed by a secondary surgical intervention to control the source of bleeding, which was the short gastric vessel near the His angle. Jejunal perforation occurred in one patient (0.2%), and this was discovered and sutured intraoperatively. A late revision was required in one patient who presented with >100% excess weight loss (EWL). Interactable reflux was presented by five (1.1%) patients, four of them were treated by PPI, but surgical interference in the form of Braun anastomosis (jejunojejunostomy at 80 cm distal to the gastrojejunostomy) was needed for the fifth patient. The most common complication was iron deficiency anaemia, presented by 18 (3.8%) patients. Symptomatic anastomotic ulcers unrelated to the administration of anti-inflammatory drugs also occurred in one patient (0.2%), who was treated with PPI.
Weight Loss
At 3 months postoperative, weight decreased from 125.8 ± 24.8 to 106 ± 14.7 kg, 91 ± 10.9 kg at 6 months, 79.3 ± 9.1 kg at 1 year and 84 ± 9.8 kg in patients who followed up for 3 years. Also, the BMI mean was 40 ± 6.1, 34.7 ± 5.2, 29.5 ± 2.8 and 32.1 ± 3.3 kg/m2 at 3, 6, 12 and 36 months, respectively (Table 2) (Fig. 1).
In the current study, at the 1-year follow-up, weight and BMI decreased on average by 36.9% (p < 0.01). There was a mild elevation of weight and BMI at the 3-year follow-up when compared to the 1-year follow-up data. However, comparing the 3-year follow-up data to the baseline data showed a significant reduction by average 33.3% (p < 0.01) (Fig. 1 and Table 2).
Diabetes Remission
Up to 1 year, a total of 472 patients have been followed-up. Out of those patients, only 361 were followed-up up to 3 years. HbA1c decreased to 5.7 ± 1.5% after 1 year and to 5.8 ± 0.9% after 3 years (Table 2 and Fig. 2). Complete diabetes remission was achieved by 397/472 (84.1%) patients. Thirty-seven (7.8%) patients achieved partial remission, and 33 (7%) patients had moderate improvements (Fig. 3). No improvement was encountered in five patients (Fig. 3). At the 3-year follow-up, diabetes remission was achieved by 328/361 (90.9%) patients (Table 3).
Remission of diabetes achievement at 1-year follow-up in the current series was significantly higher in patients who were receiving oral hypoglycaemic drugs before surgery than in those who were receiving an injection treatment (p < 0.01). Remission was 92.2% (142/154) in patients who were receiving a single oral hypoglycaemic drug preoperatively. In patients treated with a bi-therapy, the remission rate was 95.2% (139/146) and 72.4% (21/29) in patients who were on three oral hypoglycaemic drugs. Diabetic patients who were discovered accidentally during the preoperative assessments showed 100% (43/43) complete diabetic remission. Patients who received preoperative insulin injection to control DM showed 52% (52/100) remission rate (Table 4).
The 472 patients were divided into 3 groups according to BMI: group 1 BMI < 35 kg/m2 (n = 68), group 2 BMI 35–45 kg/m2 (n = 284) and group 3 BMI > 45 kg/m2. The diabetes remission rates were 76.5, 91.5 and 94.2% for patients of groups 1, 2 and 3, respectively. The mean postoperative changes in HbA1c were −3.7 ± 2.1% for group 1, −3.6 ± 1.2% for group 2 and −3.5 ± 1.9% for group 3. No significant difference was detected in comparing the HbA1c changes between groups (p = 0.94) (Fig. 4). Patients of all groups showed a rapid reduction in HbA1c, which was apparent at the 3-month follow-up (Fig. 2). Although there was less prediction of diabetic remission in patients with lower BMI, no significant difference in the percentage of remission between patients with BMI <35 kg/m2(76.5%) vs patients with BMI >35 kg/m2 (92.3%) (p = 0.06).
In the current study, seven patients were presented preoperatively with type 1 DM. Although all hypotheses have reported no beneficial role of metabolic surgeries in type 1 diabetes mellitus (T1DM) [30,31,32]; in the current study, two out of these seven patients achieved diabetic remission at 1-year follow-up. One of them was 32 years old, BMI was 39.7 kg/m2 and his preoperative HbA1c was 11.6% on insulin. Six months after the surgery, his HbA1c was 7.1%, his insulin dosage was decreased and complete remission was noted at 1-year postoperatively when his HbA1c was 5.8%. The HbA1c of the other patient decreased continuously; the values were 10.3, 7.9, and 6%, at preoperative, 6 months, and 1 year after the surgery, respectively.
Discussion
The positive impact of metabolic surgery such as RYGB or biliopancreatic diversion (BPD) on metabolic syndrome and glycaemic control has been reported in obese patients [33, 34]. The mechanism of this glycemic control was thought to be weight loss independent because it occurs immediately even before any weight loss occurs [35,36,37]. T2DM remission after gastric bypass surgery can be a result of several possible mechanisms: increased secretion of glucagon-like peptide 1 (GLP-1) and PYY hormones, decreased ghrelin hormone production and decrease in insulin resistance through weight loss are among the strongest hypotheses [38, 39]. Early exposure to nutrients in the ileum stimulates L-cells to secrete GLP-1, which has anti-diabetogenic and strong insulinotropic effect. During hyperglycaemia, GLP-1 improves insulin sensitivity, decreases glucagon secretion, increases insulin secretion, delays gastric emptying and reduces appetite [40, 41].
Although RYGB is approved as a gold standard treatment for T2DM in obese and non-obese patients, approaching it laparoscopically still remains a challenge and still requires a long learning period with high complication rates particularly when performed by less experienced surgeons [10, 42,43,44,45,46]. Since Rutledge presented the OAGB procedure in the USA in 1997, ten thousands of OAGB have been performed with highly promising results [47]. Lee et al.’s studies demonstrated that OAGB is as effective as RYGB in reducing weight, if not more effective. Also, it is associated with less operative duration, shorter learning curve and fewer major complications [2, 19, 23, 48, 49]. At the presentation of OAGB, it was received with scepticism because of possible complications such as biliary reflux, which is associated with the ‘old Mason’s loop gastric bypass’ [50]. The published data over the last 16 years demonstrated a significantly low incidence of bile reflux being associated with OAGB [51].
A large number of studies reported the beneficial impact of RYGB on diabetes remission. In a study by Cohen et al. 2012, the T2DM resolution was 88% for patients who underwent RYGB at 3 years of follow-up [52]. Similarly, the diabetic remission rate was 93% in patients who underwent RYGB in Navarrete et al.’s study [53]. VSG appears less effective than gastric bypass in glycaemic control but still shows good results in terms of diabetes remission. This is apparent in multiple studies; in a study by Gill et al., diabetes remission was 66.2% [54]. Therefore, in our current series, diabetes remission of 90.9% at 3 years of follow-up (328/361) appears to be an encouraging result.
The overall results of our current study revealed a diabetic remission rate of 84.1%, a decrease in HbA1c mean from 9.6 to 5.7% in the 1-year follow-up, no mortality and acceptable complication rates (overall morbidity rate was 6.8%). These results are complementary to the results of the largest OAGB published studies as shown in Table 5 [2, 55,56,57,58]. Although OAGB had a better glycaemic control than RYGB and VSG, we need to be careful about micronutrient malnutrition such as iron deficiency as a long-term disadvantage. In our study, iron deficiency anaemia was presented by 18 (3.8%) patients, which is comparable to that seen in other OAGB series reports [2, 19, 23], but a little higher than VSG [59] or RYGB series [60].
Some authors postulate that diabetes is a single disease, rather than two distinct entities, type 1 and type 2 diabetes. They argue that the two types of diabetes are distinguished only by the rate of β-cell loss. Proponents of the previous hypothesis claim that the rise in childhood obesity parallels the rise in both types of diabetes in childhood and that the decreasing age of onset of type 1 diabetes in heavier children lends further support to their argument [61,62,63]. On the other hand, there is a significant inconsistency regarding the effect of bariatric surgery on HbA1C in T1DM patients. Most authors have reported a non-significant improvement or even worsening of HbA1C, claiming that poor preoperative glycaemic control may have accounted for the apparent improvement demonstrated by others [31, 64,65,66]. Brethauer et al. and Middelbeek et al. found a significant reduction in HbA1C after surgery [67, 68].
There were two forms of T1DM are identified; type 1A results from a cell-mediated autoimmune attack on β-cells [69, 70], whereas type 1B has no known cause and associated with variable degrees of insulin deficiency between sporadic episodes of ketoacidosis [71, 72]. Pathogenesis of T1DM characterised by continuous damage of β-cells which leads to progressive loss of insulin secretion capacity with, in order, loss of first-phase insulin secretion in response to an intravenous glucose tolerance test, then to clinical diabetes when insulin secretion falls below a critical amount and finally, in most but not all T1DM patients, to a state of absolute insulin deficiency [72, 73].
Although talking about the relationship between OAGB and T1DM remission may initiate a lot of criticism, we had two T1DM patients have achieved remission at 1-year follow-up after surgery. We have no clear explanation, but the previous hypothesis which demonstrated that not all T1DM patients have an absolute absent of insulin secretion may explain the remission in these two patients in our study. Nevertheless, the misdiagnoses of those two cases of T1DM is still highly possible. Moreover, both patients underwent the surgery in 2015 and they were applicable only for the 1-year follow-up; further investigation, and continuation of the follow-up of these patients will be performed. Future prospective and large subjective trials about the impact of bariatric surgery on type 1 DM should be performed.
Preoperative weight, BMI, sex, age, DM duration and hypoglycaemic drugs act as predictive factors for the post-bariatric DM remission [16, 43, 74,75,76]. The complete DM remission is remarkable after OAGB, which is comparable or even superior to RYGB but is still less than BPD [10, 20, 77,78,79]. Maintenance of weight loss over time after OAGB could lead to better long-term DM remission than that obtained with RYGB [10, 75, 80,81,82]. Some studies showed a link between the preoperative BMI and postoperative DM resolution with better remission rates at higher BMI [10, 74]. Although increased remission rates in patients with higher BMI were observed in this study, we could not confirm it as a predictive factor since there was no significant difference in DM remission rates between different BMI groups (76.5% in patients with BMI < 35 kg/m2, 91.5% for 35–45 kg/m2 group and 94.2% in patients with BMI > 45 kg/m2). These results support the results of the previously published studies that demonstrate a link between BMI and DM remission remains controversial [58, 83].
In our study, remission of diabetes at 1-year follow-up was significantly higher in patients that were receiving oral hypoglycaemic drugs before surgery than in those who were receiving an injection treatment (p < 0.01) (Table 4). These results were comparable with the published data reporting that insulin usage is a poor predictor for resolution of DM, and easy preoperative glycaemic control (diet and monotherapy) is associated with high remission rates [23, 43, 75, 76, 84].
The main limitations of our study were the dropout of patients at follow-up assessment and a predictable loss of some data. A significant effort was put in place to reduce the follow-up loss; however, it was proved difficult as many patients were travelling from different cities and overseas.
Conclusion
OAGB is a simple, safe, effective, easy to learn and easy to reverse procedure. It has acceptable complications and mortality rates. Therefore, OAGB has the ability to be an excellent alternative to RYGB in the treatment of diabetic obese patients. BMI could not be used for the prediction of postoperative diabetic remission, but preoperative medication is a good predictive factor. Longer follow-up for diabetic remission is needed. Future prospective and large subjective trials about the impact of bariatric surgery on type 1 DM should be performed.
References
Danaei G, Finucane MM, Lu Y, et al. National, regional, and global trends in fasting plasma glucose and diabetes prevalence since 1980: systematic analysis of health examination surveys and epidemiological studies with 370 country-years and 2.7 million participants. Lancet. 2011;378(9785):31–40.
Lee WJ, Ser KH, Lee YC, et al. Laparoscopic Roux-en-Y vs. mini-gastric bypass for the treatment of morbid obesity: a 10-year experience. Obes Surg. 2012;22(12):1827–34.
Dixon JB. Obesity and diabetes: the impact of bariatric surgery on type-2 diabetes. World J Surg. 2009;33(10):2014–21.
Hartemink N, Boshuizen HC, Nagelkerke NJ, et al. Combining risk estimates from observational studies with different exposure cutpoints: a meta-analysis on body mass index and diabetes type 2. Am J Epidemiol. 2006;163(11):1042–52.
Xu Y, Wang L, He J, et al. Prevalence and control of diabetes in Chinese adults. JAMA. 2013;310(9):948–59.
Stratton IM, Adler AI, Neil HA, et al. Association of glycaemia with macrovascular and microvascular complications of type 2 diabetes (UKPDS 35): prospective observational study. BMJ. 2000;321(7258):405–12.
Yokoyama H, Okudaira M, Otani T, et al. High incidence of diabetic nephropathy in early-onset Japanese NIDDM patients. Risk analysis Diabetes Care. 1998;21(7):1080–5.
Leibson CL, Williamson DF, Melton 3rd LJ, et al. Temporal trends in BMI among adults with diabetes. Diabetes Care. 2001;24(9):1584–9.
Fetner R, McGinty J, Russell C, et al. Incretins, diabetes, and bariatric surgery: a review. Surg Obes Relat Dis. 2005;1(6):589–97. discussion 97-8
Buchwald H, Avidor Y, Braunwald E, et al. Bariatric surgery: a systematic review and meta-analysis. JAMA. 2004;292(14):1724–37.
Sjostrom L, Narbro K, Sjostrom CD, et al. Effects of bariatric surgery on mortality in Swedish obese subjects. N Engl J Med. 2007;357(8):741–52.
Lee WJ, Wang W. Bariatric surgery: Asia-Pacific perspective. Obes Surg. 2005;15(6):751–7.
Dixon JB, Zimmet P, Alberti KG, et al. International diabetes federation taskforce on E, prevention. Bariatric surgery: an IDF statement for obese type 2 diabetes. Diabet Med. 2011;28(6):628–42.
Dixon JB, O’Brien PE, Playfair J, et al. Adjustable gastric banding and conventional therapy for type 2 diabetes: a randomized controlled trial. JAMA. 2008;299(3):316–23.
Schauer PR, Bhatt DL, Kirwan JP, et al. Bariatric surgery versus intensive medical therapy for diabetes—3-year outcomes. N Engl J Med. 2014;370(21):2002–13.
Buchwald H, Estok R, Fahrbach K, et al. Weight and type 2 diabetes after bariatric surgery: systematic review and meta-analysis. Am J Med. 2009;122(3):248–56. e5
Lee WJ, Huang MT, Wang W, et al. Effects of obesity surgery on the metabolic syndrome. Arch Surg. 2004;139(10):1088–92.
Lee WJ, Wang W, Lee YC, et al. Effect of laparoscopic mini-gastric bypass for type 2 diabetes mellitus: comparison of BMI>35 and <35 kg/m2. J Gastrointest Surg. 2008;12(5):945–52.
Lee WJ, Yu PJ, Wang W, et al. Laparoscopic Roux-en-Y versus mini-gastric bypass for the treatment of morbid obesity: a prospective randomized controlled clinical trial. Ann Surg. 2005;242(1):20–8.
Lee WJ, Chong K, Chen CY, et al. Diabetes remission and insulin secretion after gastric bypass in patients with body mass index <35 kg/m2. Obes Surg. 2011;21(7):889–95.
Garcia-Caballero M, Valle M, Martinez-Moreno JM, et al. Resolution of diabetes mellitus and metabolic syndrome in normal weight 24-29 BMI patients with one anastomosis gastric bypass. Nutr Hosp. 2012;27(2):623–31.
Chakhtoura G, Zinzindohoue F, Ghanem Y, et al. Primary results of laparoscopic mini-gastric bypass in a French obesity-surgery specialized university hospital. Obes Surg. 2008;18(9):1130–3.
Wang W, Wei PL, Lee YC, et al. Short-term results of laparoscopic mini-gastric bypass. Obes Surg. 2005;15(5):648–54.
Gastrointestinal surgery for severe obesity: National Institutes of Health consensus development conference statement. Am J Clin Nutr. 1992; 55(2 Suppl):615S–9S.
Rutledge R. The mini-gastric bypass: experience with the first 1,274 cases. Obes Surg. 2001;11(3):276–80.
American Diabetes A. Diagnosis and classification of diabetes mellitus. Diabetes Care. 2008;31(Suppl 1):S55–60.
Kilpatrick ES, Bloomgarden ZT, Zimmet PZ. International expert committee report on the role of the A1C assay in the diagnosis of diabetes: response to the international expert committee. Diabetes Care. 2009;32(12):e159. author reply e60
WHO. Definition and diagnosis of diabetes mellitus and intermediate hyperglycemia, http://www.who.int/diabetes/publications/diagnosis_diabetes2006/en/ 2006.
American Diabetes A. Standards of medical care in diabetes—2012. Diabetes Care. 2012;35(Suppl 1):S11–63.
Sjostrom L, Lindroos AK, Peltonen M, et al. Lifestyle, diabetes, and cardiovascular risk factors 10 years after bariatric surgery. N Engl J Med. 2004;351(26):2683–93.
Chuang J, Zeller MH, Inge T, et al. Bariatric surgery for severe obesity in two adolescents with type 1 diabetes. Pediatrics. 2013;132(4):e1031–4.
Rottenstreich A, Keidar A, Yuval JB, et al. Outcome of bariatric surgery in patients with type 1 diabetes mellitus: our experience and review of the literature. Surg Endosc. 2016;30(12):5428–33.
Scopinaro N, Marinari GM, Camerini GB, et al. Specific effects of biliopancreatic diversion on the major components of metabolic syndrome: a long-term follow-up study. Diabetes Care. 2005;28(10):2406–11.
Tejirian T, Jensen C, Dutson E. Bariatric surgery and type 2 diabetes mellitus: surgically induced remission. J Diabetes Sci Technol. 2008;2(4):685–91.
Mingrone G, DeGaetano A, Greco AV, et al. Reversibility of insulin resistance in obese diabetic patients: role of plasma lipids. Diabetologia. 1997;40(5):599–605.
Pories WJ, Albrecht RJ. Etiology of type II diabetes mellitus: role of the foregut. World J Surg. 2001;25(4):527–31.
Rubino F, Gagner M. Potential of surgery for curing type 2 diabetes mellitus. Ann Surg. 2002;236(5):554–9.
Perley MJ, Kipnis DM. Plasma insulin responses to oral and intravenous glucose: studies in normal and diabetic subjects. J Clin Invest. 1967;46(12):1954–62.
Preitner F, Ibberson M, Franklin I, et al. Gluco-incretins control insulin secretion at multiple levels as revealed in mice lacking GLP-1 and GIP receptors. J Clin Invest. 2004;113(4):635–45.
Gribble FM, Williams L, Simpson AK, et al. A novel glucose-sensing mechanism contributing to glucagon-like peptide-1 secretion from the GLUTag cell line. Diabetes. 2003;52(5):1147–54.
Holst JJ. Glucagon and glucagon-like peptides 1 and 2. Results Probl Cell Differ. 2010;50:121–35.
Schauer P, Ikramuddin S, Hamad G, et al. The learning curve for laparoscopic Roux-en-Y gastric bypass is 100 cases. Surg Endosc. 2003;17(2):212–5.
Arterburn DE, Bogart A, Sherwood NE, et al. A multisite study of long-term remission and relapse of type 2 diabetes mellitus following gastric bypass. Obes Surg. 2013;23(1):93–102.
Abbatini F, Rizzello M, Casella G, et al. Long-term effects of laparoscopic sleeve gastrectomy, gastric bypass, and adjustable gastric banding on type 2 diabetes. Surg Endosc. 2010;24(5):1005–10.
American Diabetes A, Bantle JP, Wylie-Rosett J, et al. Nutrition recommendations and interventions for diabetes: a position statement of the American Diabetes Association. Diabetes Care. 2008;31(Suppl 1):S61–78.
American DA. Executive summary: standards of medical care in diabetes—2011. Diabetes Care. 2011;34(Suppl 1):S4–10.
Mahawar KK, Kumar P, Carr WR, et al. Current status of mini-gastric bypass. J Minim Access Surg. 2016;12(4):305–10.
Carbajo M, Garcia-Caballero M, Toledano M, et al. One-anastomosis gastric bypass by laparoscopy: results of the first 209 patients. Obes Surg. 2005;15(3):398–404.
Rutledge R, Walsh TR. Continued excellent results with the mini-gastric bypass: six-year study in 2,410 patients. Obes Surg. 2005;15(9):1304–8.
Fisher BL, Buchwald H, Clark W, et al. Mini-gastric bypass controversy. Obes Surg. 2001;11(6):773–7.
Mahawar KK, Jennings N, Brown J, et al. “Mini” gastric bypass: systematic review of a controversial procedure. Obes Surg. 2013;23(11):1890–8.
Cohen RV, Pinheiro JC, Schiavon CA, et al. Effects of gastric bypass surgery in patients with type 2 diabetes and only mild obesity. Diabetes Care. 2012;35(7):1420–8.
Navarrete Aulestia S, Leyba J, Navarrete LLS, et al. Roux-en-Y gastric bypass for treatment of patients with DM type 2 and BMI of 30 to 35 kg/m(2). Nutr Hosp. 2012;27(4):1160–5.
Gill RS, Birch DW, Shi X, et al. Sleeve gastrectomy and type 2 diabetes mellitus: a systematic review. Surg Obes Relat Dis. 2010;6(6):707–13.
Musella M, Susa A, Greco F, et al. The laparoscopic mini-gastric bypass: the Italian experience: outcomes from 974 consecutive cases in a multicenter review. Surg Endosc. 2014;28(1):156–63.
Darabi S, Talebpour M, Zeinoddini A, et al. Laparoscopic gastric plication versus mini-gastric bypass surgery in the treatment of morbid obesity: a randomized clinical trial. Surg Obes Relat Dis. 2013;9(6):914–9.
Kular KS, Manchanda N, Rutledge R. A 6-year experience with 1,054 mini-gastric bypasses—first study from Indian subcontinent. Obes Surg. 2014;24(9):1430–5.
Guenzi M, Arman G, Rau C, et al. Remission of type 2 diabetes after omega loop gastric bypass for morbid obesity. Surg Endosc. 2015;29(9):2669–74.
Gagner M, Deitel M, Erickson AL, et al. Survey on laparoscopic sleeve gastrectomy (LSG) at the fourth International Consensus summit on sleeve gastrectomy. Obes Surg. 2013;23(12):2013–7.
Higa KD, Boone KB, Ho T, et al. Laparoscopic Roux-en-Y gastric bypass for morbid obesity: technique and preliminary results of our first 400 patients. Arch Surg. 2000;135(9):1029–33. discussion 33-4
Daneman D. Type 1 diabetes. Lancet (London, England). 2006;367(9513):847–58.
Wilkin TJ. The accelerator hypothesis: weight gain as the missing link between type I and type II diabetes. Diabetologia. 2001;44(7):914–22.
Betts P, Mulligan J, Ward P, et al. Increasing body weight predicts the earlier onset of insulin-dependent diabetes in childhood: testing the ‘accelerator hypothesis’ (2). Diabet Med J Br Diabet Assoc. 2005;22(2):144–51.
Robert M, Belanger P, Hould FS, et al. Should metabolic surgery be offered in morbidly obese patients with type I diabetes? Surg Obes Relat Dis. 2015;11(4):798–805.
Maraka S, Kudva YC, Kellogg TA, et al. Bariatric surgery and diabetes: implications of type 1 versus insulin-requiring type 2. Obesity (Silver Spring). 2015;23(3):552–7.
Lannoo M, Dillemans B, Van Nieuwenhove Y, et al. Bariatric surgery induces weight loss but does not improve glycemic control in patients with type 1 diabetes. Diabetes Care. 2014;37(8):e173–4.
Brethauer SA, Aminian A, Rosenthal RJ, et al. Bariatric surgery improves the metabolic profile of morbidly obese patients with type 1 diabetes. Diabetes Care. 2014;37(3):e51–2.
Middelbeek RJ, James-Todd T, Patti ME, et al. Short-term insulin requirements following gastric bypass surgery in severely obese women with type 1 diabetes. Obes Surg. 2014;24(9):1442–6.
Redondo MJ, Fain PR, Eisenbarth GS. Genetics of type 1A diabetes. Recent Prog Horm Res. 2001;56:69–89.
Lambert AP, Gillespie KM, Thomson G, et al. Absolute risk of childhood-onset type 1 diabetes defined by human leukocyte antigen class II genotype: a population-based study in the United Kingdom. J Clin Endocrinol Metab. 2004;89(8):4037–43.
Abiru N, Kawasaki E, Eguch K. Current knowledge of Japanese type 1 diabetic syndrome. Diabetes Metab Res Rev. 2002;18(5):357–66.
Devendra D, Liu E, Eisenbarth GS. Type 1 diabetes: recent developments. BMJ Clin Res Ed. 2004;328(7442):750–4.
Eisenbarth GS. Type I diabetes mellitus. A chronic autoimmune disease. N Engl J Med. 1986;314(21):1360–8.
Sjostrom CD, Lissner L, Wedel H, et al. Reduction in incidence of diabetes, hypertension and lipid disturbances after intentional weight loss induced by bariatric surgery: the SOS intervention study. Obes Res. 1999;7(5):477–84.
Schauer PR, Burguera B, Ikramuddin S, et al. Effect of laparoscopic Roux-en Y gastric bypass on type 2 diabetes mellitus. Ann Surg. 2003;238(4):467–84. discussion 84-5
Hayes MT, Hunt LA, Foo J, et al. A model for predicting the resolution of type 2 diabetes in severely obese subjects following Roux-en Y gastric bypass surgery. Obes Surg. 2011;21(7):910–6.
Sarson DL, Scopinaro N, Bloom SR. Gut hormone changes after jejunoileal (JIB) or biliopancreatic (BPB) bypass surgery for morbid obesity. Int J Obes. 1981;5(5):471–80.
Sugerman HJ, Wolfe LG, Sica DA, et al. Diabetes and hypertension in severe obesity and effects of gastric bypass-induced weight loss. Ann Surg. 2003;237(6):751–6. discussion 7-8
Zervos EE, Agle SC, Warren AJ, et al. Amelioration of insulin requirement in patients undergoing duodenal bypass for reasons other than obesity implicates foregut factors in the pathophysiology of type II diabetes. J Am Coll Surg. 2010;210(5):564–72. 72-4
Campos GM, Rabl C, Mulligan K, et al. Factors associated with weight loss after gastric bypass. Arch Surg. 2008;143(9):877–83. discussion 84
Carbonell AM, Wolfe LG, Meador JG, et al. Does diabetes affect weight loss after gastric bypass? Surg Obes Relat Dis. 2008;4(3):441–4.
Melton GB, Steele KE, Schweitzer MA, et al. Suboptimal weight loss after gastric bypass surgery: correlation of demographics, comorbidities, and insurance status with outcomes. J Gastrointest Surg. 2008;12(2):250–5.
Kular KS, Manchanda N, Cheema GK. Seven years of mini-gastric bypass in type II diabetes patients with a body mass index <35 kg/m(2). Obes Surg. 2016;26(7):1457–62.
Chikunguwo SM, Wolfe LG, Dodson P, et al. Analysis of factors associated with durable remission of diabetes after Roux-en-Y gastric bypass. Surg Obes Relat Dis. 2010;6(3):254–9.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflicts of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Rights and permissions
About this article
Cite this article
Taha, O., Abdelaal, M., Abozeid, M. et al. Outcomes of One Anastomosis Gastric Bypass in 472 Diabetic Patients. OBES SURG 27, 2802–2810 (2017). https://doi.org/10.1007/s11695-017-2711-9
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11695-017-2711-9