Abstract
Background
Tumor-associated macrophages (TAMs) are known to play important roles in the initiation and progression of human cancers, as well as in angiogenesis. TAMs are considered as main components of the tumor microenvironment. Targeting TAMs may serve as a therapeutic strategy for the treatment of cancer. In this review, the signaling pathways, origin, function, polarization and clinical application of TAMs are discussed. The role of TAMs in tumor initiation, progression, angiogenesis, invasion and metastasis are also emphasized. In addition, a variety of clinical and pre-clinical approaches to target TAMs are discussed.
Conclusions
Clinical therapeutic approaches that show most promise include blocking the extravasation of TAMs along with using TAMs as diagnostic biomarkers for cancer progression. The targeting of TAMs in a variety of clinical settings appears to be a promising strategy for decreasing metastasis formation and for improving patient outcome.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
It has been well-established now that solid tumors are composed of both malignant cells and a number of non-malignant hematopoietic and mesenchymal cells [1,2,3]. Among these non-malignant cells, macrophages play an important role in promoting tumor neovascularization and progression. Macrophages represent a multifunctional component of innate myeloid cells that are released from bone marrow as immature monocyte precursors, circulate in the bloodstream and migrate to different tissues where they differentiate [4]. These cells can engulf invading microbes or cell debris from injured sites, and also release immunomodulatory cytokines that activate the adaptive immune system [5]. The broad degree of heterogeneity of macrophages enables these cells to adapt or alter their phenotype to match the microenvironment in which they reside.
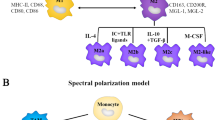
A classification mirroring the Th1/Th2 division of T-lymphocytes has been introduced [6]. The ability of macrophages to adapt to a large variety of biological stimuli by rapidly changing their phenotype and function has resulted in the understanding that a classification of macrophages into M1 versus M2 is a simplification of the in vivo situation [7]. Another classification of macrophages that has been suggested is into pro-inflammatory or classically activated macrophages and alternatively activated macrophages [6, 8]. M1 macrophages are stimulated by Th1 mediators such as interferon-γ (IFN-γ), tumor necrosis factor-alpha (TNF-α) and lipopolysaccharide (LPS) [8]. The main cytokine is IFN-γ. Receptors using Janus kinase Jak1 and Jak2 adaptors can activate signal transducer and activator of transcription 1 (STAT1) and interferon regulatory factors [8]. For the regulation of signaling pathways, IFN-γ and STAT1 recruit toll-like receptors (TLRs), inflammatory factors, tissue-destructive cytokines, anti-inflammatory cytokines and cytokines that activate opposing STATs. These signaling pathways disclose insight into how IFN-γ regulates macrophage activation, inflammation, tissue remodeling, and helper and regulatory T cell differentiation [9]. Some specific genes regulated by IFN-γ include those encoding the cytokine receptors CSF2RB, IL15 receptor alpha (RA), IL2RA and IL6R, cell activation markers (CD36, CD38, CD69, and CD97), as well as a number of cell adhesion molecules (intercellular adhesion molecule 1(ICAM1), integrin alpha L (ITGAL), ITGA4, ITGbeta-7 (B7), mucin 1 (MUC1), and ST6 beta-galactosamide alpha-2,6-sialyl transferase 1 (SIAT1)) [10]. According to the M1/M2 paradigm, IFN-γ is combined with LPS, and the gene expression profile of this mode is different from the LPS or IFN-γ profiles alone [11, 12]. The M1 and M2-associated gene expression and function profiles are listed in Tables 1 and 2.
M1 macrophages secrete pro-inflammatory cytokines such as IL-12 and IL-23, present antigens by their MHC-II complex molecules and enhance the differentiation of naïve CD4+ T-cells into Th1 effector cells and Th17 cells. They also remove intracellular bacteria and viruses [6, 13, 14]. By contrast, M2 activators are classified primarily based on their capacity to antagonize prototypical inflammatory responses and markers. However, as M1 activators, their origin, function, receptors and signaling pathways differ. So far, five main M2 stimuli have been identified: firstly interleukin 4 (IL-4), which is produced by Th2 cells, basophils, eosinophils, or macrophages themselves and is recognized by three different receptor pairs. To form these receptor pairs, IL-4Rα1 can either pair with the common gamma chain (γc), allowing IL-4 binding, or with IL-13Rα1 enabling IL-4 or IL-13 binding. After binding, the receptors can activate JAK1 and JAK3. Activation of JAK leads to STAT6 activation and translocation, after which IL-4 induces macrophage fusion and a decrease in phagocytosis [15]. Interleukin 13 (IL-13) is another stimulator that has a signature similar to IL-4, but they do not completely overlap [16]. Other stimulators of M2 macrophages are glucocorticoids, IL-10 and macrophage colony-stimulating factor (M-CSF). The M-CSF receptor is a tyrosine kinase transmembrane receptor. When M-CSF binds to its receptor, this may lead to several specific modifications, including dimerization, autophosphorylation, activation of extracellular signal-regulated kinases (ERK), activation of phosphatidylinositol 3-kinase, activation of phospholipase C and, eventually, Sp1 transcription factor nuclear localization. Ultimately, M-CSF causes a series of transcriptional responses that comprise transient gene clusters with overrepresentation of cell cycle genes (e.g. cyclins A2, B1, D1 and E1) and downregulation of human leukocyte antigen [17] members and stable gene clusters, including TLR7 and the complement C1QA/B/C subunits. Activated M2 stimulates CD+ Th2 cells and regulatory T cell (Treg) differentiation. M2 cells have also been implicated in homeostatic processes and to be critical in angiogenesis, tissue remodeling, anti-inflammatory processes and wound healing [18, 19]. Several investigators have attempted to classify them into different sub-groups, to better reflect the situation in vivo. Among them, Mantovani and colleagues sub-classified the M2 population into M2a, M2b and M2c, where M2a was stimulated by the representative Th2 cytokines IL-4 and IL-13, M2b by immune complexes along with TLR or the IL-1 receptor antagonist and M2c by glucocorticoids and IL-10 [7].
The classification of macrophages in this way faces two major challenges: the in vitro influences of chosen immune-related ligands on the phenotype of macrophages and in vivo evidence for distinct subsets of macrophages in disease, comparable to polarized B- and T cell responses. The main restrictions of the current view are (i) that it ignores the origin and context of the stimuli, (ii) that the M1 and M2 stimuli do not exist singly in tissues and (iii) that macrophages may not form clearly defined activation subunits nor broaden clonally [20]. Tumor-associated macrophages (TAMs) have been found to play a leading role in the development and progression of tumors, and to enhance the tumor environment to facilitate angiogenesis and metastasis. As a consequence, TAMs have been proposed as potential therapeutic targets for cancer treatment [21]. Here, we review the role of TAMs in tumor initiation, progression, angiogenesis, invasion and metastasis. Different therapeutic approaches targeting TAMs in each of these steps are also discussed.
2 Role of TAMs in tumor initiation and progression
The German pathologist Rudolph Virchow in the nineteenth century suggested a pathophysiological association between inflammation and cancer. Inflammation usually occurs in two stages, acute and chronic. Later on, it has been proposed that inflammation in its chronic stage may trigger cancer initiation. About 90–95% of all neoplasms are connected to tobacco, obesity, smoke, radiation, environmental pollutants and chronic infections, all of which induce a chronic inflammatory state [22]. Macrophages are present in the inflammatory environment including the tumor microenvironment. Macrophages are involved in immune responses to tumors in a polarized manner: classical M1 macrophages produce IL-12 and promote tumor initiation, whereas M2 macrophages produce IL-10 and promote tumor progression. To define the role of macrophages in tumor progression, it is necessary to understand TAM differentiation and their tumor promoting properties. M2-like macrophages encompass the majority of TAMs with a representative M2 marker expression profile, including a mannose receptor, a low MHC class II complex, stabilin-1 and arginase-1 [14]. These markers are involved in tissue remodeling, immune regulation and angiogenic processes within the tumor microenvironment by releasing high levels of IL-10, low levels of IL-12, angiogenic factors such as vascular endothelial growth factor (VEGF), prostaglandin E2 and matrix metalloproteinase-9 (MMP9) [14].
M1-like macrophages promote tumor initiation via chronic inflammation in the tumor microenvironment that is caused by intrinsic and extrinsic signals and leads to proliferation and survival of malignant cells, angiogenesis, suppression of adaptive immunity and reduced responses to hormones and chemotherapeutic agents [23]. The intrinsic pathways include genetic alterations in oncogenes such as RET [24], RAS [25], MYC [26], or in tumor suppressor genes such as the von Hippel-Lindau tumor suppressor (VHL) [27], which contributes to the transcription of pro-inflammatory cytokines and growth factors in the genetically altered tumor cells and induces a tumor-driven inflammatory environment. The extrinsic pathway leads to chronic inflammation that increases the risk of developing cancer at a specific anatomical site, often prostate, colon or pancreas [28]. The extrinsic and intrinsic pathways co-operate in the activation of transcription factors such as NF-кB or STAT3, which promote tumor progression in the microenvironment [29,30,31]. NF-кB is an essential factor for the transcription of pro-inflammatory and angiogenic factors such as IL-12, TNF-α, inducible nitric oxide synthase (iNOS) [32] and cyclooxygenase-2 (COX-2), and is associated with the promotion of carcinogenesis in different tumor types [33]. Activation of STAT3 also allows tumor cells to resist apoptosis, inhibit inflammation, impede dendritic cell maturation, induce growth, and to stimulate migration, invasion and angiogenesis, culminating in an active tumor environment [34]. During early carcinogenesis, all macrophages exhibit a higher degree of similarity to M1, but in later stages the majority of tumors recruit M2-like macrophages to their microenvironment. In hepatocellular carcinoma, for example, macrophages in the early stage of development mostly express high levels of MHC-class II, which has been associated with high concentrations of IL-1β, IL-6, IL-12 and iNOS. In contrast, macrophages in late stages of development mainly express typical M2-associated molecules such as macrophage mannose receptor c1 (MRC1), arginase, IL-10 and TGF-β, and low levels of MHC-class II [35].
Some causative signals that are involved in the M1/M2 switch have been identified. It has been found, for example, that COX-2 innately contributes to changing TAMs from M1 to M2. Inhibition of COX-2 leads to a decreased number of M2 macrophages and causes an increase in IFN-γ level, thereby reducing the progression of intestinal tumors in patients with colon carcinoma [36]. Another regulatory pathway that has been found to be important for TAM differentiation comprises TLR signaling. Some of the extracellular matrix proteins such as versican, hyaluronan fragments or heat shock proteins, which act as ligands for TLR in the tumor environment, have been associated with tumor progression and metastasis [37]. TLR signaling pathways are dependent on both myeloid differentiation primary response gene88 (MyD88) and TIR-domain-containing adapter-inducing interferon-β (TRIF). It has been found that an imperfect activation of MyD88, but an undamaged TRIF-mediated signal transduction, increases the phosphorylation of ERK1/2. Phosphorylation of ERK1/2 leads to increased secretion of IL-10 from TAMs, causing extensive expression of interleukin-1 receptor-associated kinase M (IRAK M). IRAK M is an inhibitor of the MyD88-dependent pathway. Generally, defective TLR-MyD88/TRIF signal pathway regulation in TAMs favors an increased immunosuppressive function of these macrophages [38].
Another condition that affects TAM differentiation during tumor progression is a limited oxygen supply in highly expanding regions of the developing tumor. When macrophages are in a hypoxic condition, the expression of hypoxia-inducible factor-1 (HIF-1) is increased, which is closely associated with NF-кB activation [39]. The Notch signaling pathway is also involved in TAM differentiation. Notch signaling may be activated in M1 macrophages, which leads to enhanced expression of IL-12 that, in turn, limits tumor progression. In addition, the M2 response has been found to be induced by M1 inducers at the expense of M1 when Notch signaling is blocked. Macrophages deficient in canonical Notch signaling have been found to show TAM phenotypes [40, 41]. In addition to transcription factors and innate signaling pathways, chemokines are also involved in M1-M2 transition during tumor progression. CXCL12, also known as stromal cell-derived factor-1 (SDF-1), is one of the chemokines that is highly secreted from monocytes in the tumor microenvironment. This chemokine not only facilitates the attraction and migration of monocytes to the tumor site, but also leads to the differentiation of TAMs into a pro-angiogenic and immunosuppressive phenotype by up-regulating CCL1 and VEGF [41]. CXCL12 also drives TAM aggregation and survival in hypoxic tumor areas [42]. This chemokine may enhance scavenger receptor CD163 expression, thereby shaping monocyte differentiation towards an immunosuppressive and proangiogenic phenotype [41]. CXCL12 expression has been found to be significantly correlated with augmented CD163+ TAMs in tumor stroma (TS) and tumor margin (TM) in gastric cancer patients [43]. Wang et al. reported that the prodrug of the green tea polyphenol (−)-epigallocatechin-3-gallate (Pro-EGCG) may serve as an angiogenesis inhibitor in endometrial cancer. They found that Pro-EGCG decreased tumor angiogenesis in xenograft models through downregulation of CXCL12 in the host stroma, and VEGFA and HIF1α in the tumor cells, as shown by immunohistochemical staining. Down-regulation of CXCL12 in the stromal cells by Pro-EGCG treatment restricted the migration and differentiation of macrophages, thereby inhibiting infiltration of VEGFA-expressing TAMs [44].
As noted above, the presence of TAMs in the tumor environment may result in cancer promoting inflammation, which plays a central role in tumor initiation [22, 45]. Several experimental studies support the role of inflammation in cancer initiation. For instance, chronic obstructive pulmonary disease in human leads to persistent colonization of the bacterium Haemophilus influenza and this colonization has been associated with an increased risk of lung cancer. Concordantly, in a lung cancer mouse model, bronchial inflammation elicited by H. influenzae led to an increase in tumorigenesis [46], but more work needs to be conducted in lung cancer models. Mechanistically, the transcriptional factors NFκB and STAT3 work oppositely [47]. STAT3 is a transcription factor that suppresses inflammation and, therefore, absence of STAT3 in myeloid cells leads to an abundant expression of TNFα and IL-6 via macrophages, which consequently results in chronic colitis and invasive colonic adenocarcinomas [48, 49]. In addition, the inflammatory condition is controlled by NFκB, which is an essential transcription factor that triggers downstream inflammatory signaling pathways and activates TLR, which leads to the expression of inflammatory cytokines such as IL-12 and TNFα, as well as iNOS [47]. Concordantly, it has been found that impeding IκB kinase α (IKKα) in myeloid cells in a mouse model of intestinal cancer diminished inflammation and inhibited tumor progression [50]. Furthermore, macrophages produce both reactive nitrogen and oxygen species. Nitric oxide (NO) can react with peroxidases to produce nitrosoperoxycarbonate, which can lead to progression of inflammation [51]. This effect is due to the fact that the highly reactive components create a mutagenic environment that causes mutations in adjacent epithelial cells [51]. In addition, it has been found that inflammation in the tumor microenvironment may promote genetic instability within developing tumor epithelial cells [23].
The tumor immune microenvironment mainly consist of macrophages, T lymphocytes, natural killer (NK) cells, dendritic cells, neutrophils and myeloid-derived suppressor cells (MDSCs) [52, 53]. TAMs in the tumor microenvironment express both chemokines and cytokines promoting an immunosuppressive tumor microenvironment [54, 55]. Chemokines secreted by TAMs such as CCL5, CCL22 and CCL20 recruit regulatory T (Treg) cells, whereas cytokines such as IL-10 and TGF-β induce Treg cells. In addition, TAMs may suppress the antitumor activity of tumor-infiltrating NK cells and T cells, and via MDSCs, tumor-associated dendritic cells and neutrophils that promote an immunosuppressive tumor microenvironment synergistically [55, 56]. Inhibition of T cell function may result from secretion of specific enzymes by TAMs such as NOS and arginase [57,58,59,60]. In addition, expression by TAMs of ligands such as programmed cell death protein ligand 1 (PD-L1) and B7-H1 for receptors programmed cell death protein (PD-1) and CTLA-4, may lead to the inhibition of cytotoxic functions of T-cells, NKT cells and NK cells [61]. In one study, the role of inhibitory CD163+ monocytes or macrophages, and NK cells in diffuse large B cell lymphoma (DLBCL) and Hodgkin lymphoma [12] have been investigated. It was found that PD-1 expression in CD3−CD56hiCD16-ve NK cells was higher than in CD3−CD56dimCD16+ cells, which spread in blood and tissue more markedly in cHL than in DLBCL patients. In this regard, within diseased lymph nodes TAMs have been found to express high levels of PD-L1/PD-L2. In an in vitro functional model TAM-like monocytes were found to suppress the activation of PD-1hi NK cells, which could be reversed by PD-1 blockade. Importantly, suppression of NK cells can occur indirectly by PD-L1/PD-L2 expressing TAMs [62].
3 Role of TAMs in tumor growth
TAMs may exhibit both tumor growth promoting and inhibiting activities [63, 64]. They may promote tumor growth not only through stimulating angiogenesis, but also through suppressing acquired immune responses. TAMs may act as gatekeepers in tumors, producing various factors for tumor invasion and metastasis (Fig. 1). The role of TAMs in the growth of various cancers, including breast cancer [65, 66], hepatocellular carcinoma (HCC) [67], colorectal cancer [68] and glioblastoma [69, 70] has been well-established. Using a spontaneous genetic model of breast cancer metastasis and orthotopic transplant experiments it has, for example, been shown that SNAIL1, an epidermal to mesenchymal transition inducer [71], regulates the production of GM-CSF, TNFα, IL1α and IL-6, and modulates the polarization of TAMs. This modulation ultimately leads to the growth and metastasis of primary breast tumor cells [72]. ERK5 plays a role in determining macrophage polarity, and it has been found that in ERK5-deficient mice the growth of carcinoma grafts is halted. Targeting ERK5 in macrophages has been found to lead to a transcriptional switch that favors proinflammatory mediators. Further molecular studies have shown that STAT3 activation via phosphorylation of Tyr705 is impaired in ERK5-deleted TAMs. So, impeding STAT3-induced gene expression via blocking ERK5 may serve as a strategy for cancer treatment through reprogramming macrophages towards an antitumor state [73].
4 Role of TAMs in angiogenesis
TAMs play an important role in tumor progression and invasion and act as key players in angiogenesis [74, 75]. In response to hypoxic conditions, TAMs begin to express a number of transcription factors such as HIFs that regulate a range of genes to promote angiogenesis, which in turn increases the invasion of tumor cells. TAMs also secrete angiogenic factors such as VEGF, FGF2, bFGF, PDGF and adrenomedullin [76], YKL-40, thymidine phosphorylase (TP), MMPs and urokinase-type plasminogen activator, all of which play important roles in tumor progression and invasion (Fig. 1) [59, 74, 77]. Badawi et al. examined the relationship between macrophage infiltration and the degree of angiogenesis in human colon carcinoma. They found that the number of infiltrating macrophages was significantly higher in malignant/invasive tumors and that their blood vessels were denser compared to those in benign polyps. Thus, a significant relationship was observed between macrophage infiltration and angiogenesis, invasion and metastasis of colon cancer cells [78]. Additionally, Tie2-expressing monocytes (TEMs), a type of TAMs that are present in both human peripheral blood and tumors, have been found to play an important role in tumor angiogenesis and growth. Studies aimed at examining human and murine endometriosis lesions, pancreatic cancer, ovarian cancer and other cancers have revealed a role for TEMs in angiogenesis [79,80,81,82,83]. In addition, it has been found that elimination of TEMs may lead to inhibition of angiogenesis in various tumor models. Angiopoietin-2 (Ang-2), a ligand for Tie2, is produced by angiogenic tumor vessels and serves as a chemoattractant for TEMs. Hypoxia has been found to enhance Tie2 expression in TEMs and, together with Ang-2, to down-regulate their antitumor capacity [84]. Ang is secreted by endothelial cells. According to Chen et al., there is a close relationship between tumor recurrence and Tie2 over-expression after chemotherapy. This recurrence occurs via re-regeneration of blood vessels within tumors. Hence, removal of Tie2 in myeloid cells may be used to prevent the regeneration of blood vessels and, thereby, tumor recurrence [85].
5 Therapeutic targeting of angiogenesis
Targeting TAM-induced angiogenesis serves as a potential approach for cancer treatment. VEGFA is one of the most important TAM-secreted factors that plays an important role in angiogenesis and tumor metastasis. Inhibition of the VEGF pathway is a commonly used treatment option for controlling tumors. Bevacizumab is a monoclonal antibody directed against VEGF that has been approved by the US Food and Drug Administration (FDA) [78]. It acts through binding to VEGF and, thereby, inhibiting its interaction with the VEGF receptor (VEGFR). The efficacy of bevacizumab has currently been investigated in several cancer types including ovarian, colorectal, breast, renal, non-small cell lung and cervical cancers [86,87,88,89,90,91].
The role of Ang2 as a potential target in patients with naive and bevacizumab-resistant glioblastoma was investigated by Scholz et al. [92]. Ang-2 is an angiogenic growth factor that is not expressed in normal human brain, but its expression is increased in glioblastoma patients who are resistant to bevacizumab. Blocking VEGF in murine models has led to increased expression of Ang2 in endothelial cells, thereby impeding the effect of VEGF (aflibercept). In addition, it was found that application of an anti-human Ang-2 antibody led to reduced vascular permeability, eliminated TAMs and increased the number of intra-tumoral T lymphocytes. As a result, it was found that inhibition of both the VEGF/VEGFR and Ang-2/Tie2 pathways led to the removal of TAMs and suppression of the pro-angiogenic process. Peterson et al. [93] investigated the effect of MEDI3617 (an anti-Ang2-neutralizing antibody) in combination with cediranib (a pan-VEGFR tyrosine kinase inhibitor) in orthotopic glioblastoma Gl261 and U87 models. They concluded that dual inhibition of VEGFR/Ang-2 was superior compared to inhibition of VEGFR alone, and increased the lifespan of the vessels.
YKL-40 is used as biomarker to diagnose tumor angiogenesis in renal cell carcinoma (RCC) and melanoma patients [94, 95]. It has been found that YKL-40 levels in serum and pleural fluid in patients with malignant pleural effusions are increased compared to those in patients with transudative or non-malignant exudative effusions. The importance of this biomarker in the diagnosis of malignant pleural infections has been shown [96]. Also, an increase in serum YKL-40 and IL-6 levels in patients with colorectal cancer has been reported to serve as a useful prognostic biomarker before liver resection [97]. Furthermore, Shao et al. [98] reported that an YKL-40 neutralizing antibody (mAY) and ionizing irradiation (IR) may prevent angiogenesis and tumor growth in glioblastoma patients. Specifically, it was found that mAY blocked mural cell-mediated vascular stability and angiogenesis through interfering with intercellular contact by N-cadherin, while IR only stimulated tumor cells. From their results, they also concluded that dual treatment with IR and bevacizumab in glioblastoma patients was more effective than IR alone, regardless YKL-40 expression. For patients with advanced glioblastoma, the therapeutic combination of mAY, IR and bevacizumab was found to be efficacious [98].
Cytochrome P450 4A (CYP4A) is known to play an important role in tumor angiogenesis and metastatic niche development. CYP4 enzymes can biosynthesize 20-hydroxyeicosatetraenoic acid (20-HETE), which is an important mediator of VEGF-mediated angiogenesis [99]. Blocking CYP4A to inhibit angiogenesis in glioblastoma by the novel flavonoid FLA-16 has, therefore, been examined. It was found that inhibition of FLA-16 by CYP4A in TAMs and endothelial progenitor cells (EPCs) leads to downregulation of TAM- and EPC-derived VEGF and TGF-β via the PI3K/Akt pathway, thereby providing another mechanism for inhibiting angiogenesis and survival of glioma cells [100].
6 Role of TAMs in invasion
As the number of TAMs increases, invasion and metastasis increases [101]. Important stages of metastasis include invasion, intravasation, circulation and extravasation. In order for invasion to occur cancer cells must undergo a process called epithelial-mesenchymal transition [71] [97] [102]. A strong correlation between EMT and the beginning of the invasion phase, including loss of cell-cell binding and cell-basement membrane binding, invasive behavior and resistance to apoptosis has been found to exist [103,104,105,106]. Several studies have addressed the role of TAMs in EMT. Zhang et al. [107], for example, observed a role of TAMs and their relationship with EMT in the progression and invasion of gastric cancer by measuring the level of infiltrated TAMs and the expression of EMT markers. They concluded that TAMs may play an important role in EMT induction and in the promotion of migration and metastasis of gastric cancer cells.
7 Role of TAMs in intravasation
Intravasation is a phase through which tumor cells enter blood vessels to metastasize to distant sites [108]. It has been reported that there is a significant relationship between tumor cells and TAMs and their role in intravasation [64, 109]. This relationship has also been reported in animal models for breast cancer exploring the relationship between peripheral macrophages and the intravasation of tumor cells [110]. Through the secretion of various factors such as (epidermal growth factor) EGF, CCL18, TNF-α, cathepsin and osteonectin, TAMs are able to promote tumor cell intravasation [111]. Specifically, Gorelik et al. [112] revealed a role of macrophages in the intravasation of murine tumor cells and the subsequent development of pulmonary metastatic tumors. In a similar study, Hu et al. [113] revealed a role of TAMs in the progression and invasion of Kazakh esophageal squamous cell carcinoma (ESCC) cells. They showed that an increase in the number of TAMs, using CD163 as a marker, in the tumor stroma significantly correlated with ESCC progression and metastasis. Furthermore, they found that there was a close relationship between a high number of TAMs and an increased expression of VEGF-C, either in the tumor nests or in the tumor stroma, which ultimately led to ESCC invasion and metastasis [113].
A positive interaction between tumor cells and TAMs may lead to secretion of CSF1 by the tumor cells, which stimulates TAMs to secrete EGF. These factors play an important role in the invasion and migration of both cell types into blood vessels [114, 115]. CSF1 is a chemokine that plays an important role in regulating macrophages. A high CSF-1 level has also been found to be associated with poor prognoses in many cancers [116,117,118]. TAM-derived EGF leads to an increase in the invasion and movement of tumor cells by destroying the matrix and, thereby, by accelerating tumor invasion [64, 119]. The interaction between CSF1 and EGF forms a paracrine loop between tumor cells and macrophages, which subsequently has been found to result in the intravasation and migration of breast tumor cells. This observation was first made in vivo by Wyckoff et al. [119]. TNF-α is another important factor known to be involved in tumor intravasation. Wang et al. [120] found for example, using a Zebrafish model, that TNF-α and IL-6 may increase the ability of TAMs to promote tumor metastasis.
8 Therapeutic interventions to prevent intravasation
Targeting CSF1/CSF1R or EGF/EGFR has been found to inhibit the reduction of bone marrow monocyte mobilization. Thus, inhibition of CSF1-CSF1R may serve as a therapeutic tool to prevent tumor intravasation [110, 121, 122]. The effect of inhibition of CSF1R in a mouse glioblastoma model was investigated by Pyonteck et al. [123]. From their results they concluded that inhibition of CSF-1R by BLZ945 led to changes in macrophage accumulation, increased survival and blockage of tumor growth. The CSF1R inhibitor was also found to affect CSF1R expressed at the TAM level. This type of intervention is currently being investigated clinically, as a phase I/II study of BLZ945 alone or in combination with PDR001, in patients with malignant tumors (NCT02829723). Another phase I trial assessing CSF-1R inhibitor LY3022855 in combination with Durvalumab (MEDI4736) or Tremelimumab has been started in patients with advanced solid tumors (NCT02718911).
9 Role of TAMs in circulation
After tumor cells enter the bloodstream, they must survive to migrate throughout the body. These cells are called circulating tumor cells (CTCs). After tumor cells have entered the bloodstream successfully, they are faced with a new survival challenge. TAMs play an important role in the survival of CTCs in peripheral blood [124, 125]. Adams et al. [125] have shown that cancer-associated macrophage-like cells (CAMLs) can bind to CTCs in the peripheral blood. Such binding facilitates the implantation of tumor cells at distant locations. Furthermore, the authors confirmed the presence of TAMs bound to CTCs in peripheral blood of patients with breast, pancreatic and prostate cancer. These results underscore the importance of macrophages in the circulation of cancer patients and their involvement in the development of distant metastases. It was also concluded that evaluation of the fluid phase of solid tumors is important for the detection of metastases. In a similar study, the presence of CALMs in the peripheral blood of 93% of patients with malignant breast cancer was confirmed. In 88% of patients undergoing core biopsies for the diagnosis of invasive carcinoma CAMLs were detected, compared to 26% of patients with benign breast conditions [126]. According to these results, screening for the presence of TAMs regardless of the stage of the disease is warranted [126]. In addition, it has been found that TAMs, by secreting factors such as MMPs and CXCL12, can convert solid tumor cells to CTCs. Therefore, the detection of TAM as a diagnostic biomarker for disease progression may be important.
10 Therapeutic interventions to prevent tumor cell circulation
The use of cabozantinib against circulating monocytes has shown a strong association between monocyte reprograming and therapeutic bone responsivity. As such, this observation may be used for patient selection at early stages of treatment. Based on this notion, a re-evaluation of tyrosine kinase inhibitor-based therapeutic strategies in prostate cancer has been considered for suitable patient populations based on tumor microenvironment responses [127]. In addition, inhibition of M-CSFR by PLX3397 (pexidartinib), a CSF-1R kinase inhibitor, has been found to decrease the number of TAMs and circulating monocytes effectively in mesothelioma mouse models, although the survival outcome was not favorable. The subsequent use of PLX3397 in combination with dendritic cell vaccination was found to augment survival synergistically, to decrease TAMs and to increase CD8+ T cell numbers and functionalities [128]. It has also been shown that legumain, an asparaginyl endopeptidase, is highly expressed on the surface of TAMs. Specifically, legumain activates a doxorubicin-based prodrug, which selectively results in the reduction of angiogenic factors by ablation of TAMs. The use of this prodrug also inhibited CTCs and led to significant inhibition of tumor growth and metastasis formation in murine tumor models [129].
11 Role of TAMs in extravasation
Extravasation is the last stage of tumor cell travel in the blood circulatory system [130]. Through extravasation, tumor cells pass the blood vessel endothelium and invade target tissues [130, 131]. The extravasation of tumor cells occurs through interactions between tumor cells, endothelium and immune cells such as platelets, granulocytes/neutrophils and macrophages [132, 133]. Similar to the intravasation process, macrophages play a prominent role in the extravasation process. CCL2 is a chemokine that is secreted from tumor cells and is absorbed by TAMs. Its role in the extravasation of tumor cells has amply been shown. It has, for example, been shown that tumor-derived CCL2 can facilitate tumor metastasis through TAMs and metastasis-associated macrophages (MAMs) [134, 135]. CCL2 and its receptor CCR2 are expressed by macrophages. CCL2 stimulates the production of CCL3 from MAMs. Kitamura et al. [136] found that CCL3 secreted from MAMs and the CCL3-CCR1 axis may increase breast cancer cell implantation via MAM accumulation. In addition, they found that removal of CCL3 or CCR2 reduced the metastasis of lung cancer cells in humans and breast cancer cells in mice, and that both were associated with decreased MAM accumulation. Also, macrophages are known to produce VEGFs that play an important role in vascular permeability and facilitate the extravasation of tumor cells [137]. Therefore, prevention of extravasation may serve as a tool by which cancer metastasis may be impaired.
12 Therapeutic interventions for extravasation
Inhibition of the CCL2-CCR2 chemokine axis may be used as a mechanism to decrease tumor progression. A phase II study of PF-04136309 in combination with FOLFIRINOX in PDAC patients has indicated that this drug was safe and well tolerated by patients. PF-04136309 inhibits CCR2 activity, which decreases the infiltration of TAMs and prevents the mobilization of inflammatory macrophages into blood vessels (NCT01413022) [138]. Furthermore, inhibition of CCR2 signaling has been found to block tumor cell extravasation [139]. In another study, a protein consisting of a CCL2 mutant fused to human serum albumin (i.e., dnCCL2-HSA chimera) was constructed that prevented the absorption of inflammatory monocytes by binding to endothelial cells, thereby reducing the permeability of lung vessels and, thus, tumor seeding. This reduction in extravasation was supported by a decrease in vascular permeability in lung carcinoma samples [140].
13 Preparation of the metastatic niche
Metastatic niche refers to an environment in a secondary organ that provides the proper environment for the metastasis of a primary tumor. Primary tumor-secreted factors, such as VEGFA, TGF-β, TNF and LOX, have been found to stimulate expression of the S100A8, S100A9 and SAA3 proteins, and to lead to extracellular matrix remodeling at metastatic sites. This remodeling provides a suitable metastatic environment before tumor cells arrive. S100A8 and S100A9 have been reported to play important roles in the establishment of pre-metastatic niches, and blocking of these factors has been found to prevent tumor cell infiltration of pre-metastatic Mac1+ myeloid cells [64, 141, 142]. These TAMs represent one class of the bone marrow-derived cell (BMDC) population that contributes to the formation of metastatic niches through the promotion of tumor cell dissemination, as well as through providing an environment that supports the growth of cancer cells [143]. This was shown by Wang et al. [144], who found that colorectal cancer-derived VEGFA can stimulate TAMs to produce CXCL1 in the primary tumor. This CXCL1 subsequently recruited CXCR2-positive MDSCs and neutrophils in pre-metastatic liver tissue to form a pre-metastatic niche that ultimately promoted liver metastasis. The authors also showed that CXCR2 antagonist could prevent tumor progression and expansion. Similar results from Miyake et al. also showed that TAM- and cancer-associated fibroblast (CAF)-derived CXCL1 may play an important role in adhesion between tumor cells and stromal cells, thereby enhancing human bladder cancer growth [145].
A group of proteases secreted from TAMs, including cathepsin, MMP2, MMP7 and MMP9, has been found to be involved in ECM destruction, the migration of tumor cells and the formation of metastatic niches [63]. Another factor derived from TAMs that is involved in metastasis is CCL18. Through binding to the PITPNM3 receptor, CCL18 has been found to stimulate integrin clustering on the surface of breast cancer cells and to increase their binding to the ECM [63, 146, 147]. In addition, TAM-derived TNF-α, VEGF and TGF-β have been found to induce macrophages to produce S100A8 and serum amyloid A3, factors that recruit tumor cells and macrophages and stimulate the formation of metastatic niches [63]. CYP4A expression by TAMs and its role in the formation of pre-metastatic niches has also been reported. Chen et al. [99] showed that over-expression of CYP4A may play an important role in clinical specimens from patients with invasive breast carcinoma and melanoma. CYP4A was found to induce the production of cytokines derived from M2 macrophages, including VEGF, SDF-1 and TGF-β. These cytokines can activate the migration of VEGFR1+ myeloid cells from bone marrow and fibroblasts, thereby leading to the formation of pre-metastatic niches and the promotion of metastasis [99]. Inhibition of the formation of metastatic niches may be a promising strategy to prevent tumor metastasis [148]. This could potentially be achieved by decreasing the expression of CYP4A and by inhibiting angiogenic factor production. For example, N-(4-butyl-2-methylphenyl)-N′-hydroxyformamidine has been found to inhibit the synthesis of 20-HETE and to decrease the production of pro-angiogenic factors such as VEGF [99]. Therefore, inhibition of the expression of CYP4A in CYP4A positive TAMs may be used as a method to inhibit the formation of metastatic niches and, thus, metastasis [99].
14 Conclusions and perspectives
In this review, the origin, function, polarization and signaling pathways involved in TAMs, and putative clinical applications of TAMs are discussed. The role of TAMs in tumor initiation, progression, angiogenesis, invasion and metastasis, as well as different TAM-targeting therapeutic approaches related to each step were emphasized. In addition, M1 and M2-associated gene expression profiles and their functional consequences were explained.
Since TAMs are known to play critical roles in the development and progression of human cancers, their targeting may be used as a potential therapeutic strategy. Previous and ongoing experimental, preclinical and clinical investigations have indeed shown potential. Clinical applications that appear to show most promise include blocking the extravasation of TAMs and using TAMs as diagnostic biomarkers for cancer progression. The future targeting of TAMs may well turn out to be a promising strategy for decreasing metastasis formation and for improving patient outcome.
References
F. Balkwill, A. Mantovani, Inflammation and cancer: Back to Virchow? Lancet 357, 539–545 (2001)
N. Eiro, L. Gonzalez, A. Martinez-Ordonez, B. Fernandez-Garcia, L.O. Gonzalez, S. Cid, F. Dominguez, R. Perez-Fernandez, F.J. Vizoso, Cancer-associated fibroblasts affect breast cancer cell gene expression, invasion and angiogenesis. Cell Oncol 41, 369–378 (2018)
P. Nilendu, S.C. Sarode, D. Jahagirdar, I. Tandon, S. Patil, G.S. Sarode, J.K. Pal, N.K. Sharma, Mutual concessions and compromises between stromal cells and cancer cells: Driving tumor development and drug resistance. Cell Oncol 41, 353–367 (2018)
S.K. Biswas, P. Allavena, A. Mantovani, Tumor-associated macrophages: Functional diversity, clinical significance, and open questions. Semin Immunopathol 35, 585–600 (2013)
S. Gordon, P.R. Taylor, Monocyte and macrophage heterogeneity. Nat Rev Immunol 5, 953–964 (2005)
C.D. Mills, K. Kincaid, J.M. Alt, M.J. Heilman, A.M. Hill, M-1/M-2 macrophages and the Th1/Th2 paradigm. J Immunol 164, 6166–6173 (2000)
F.O. Martinez, A. Sica, A. Mantovani, M. Locati, Macrophage activation and polarization. Front Biosci 13, 453–461 (2008)
L.A.J. O'Neill, R.J. Kishton, J. Rathmell, A guide to immunometabolism for immunologists. Nat Rev Immunol 16, 553–565 (2016)
X. Hu, L.B. Ivashkiv, Cross-regulation of signaling pathways by interferon-gamma: Implications for immune responses and autoimmune diseases. Immunity 31, 539–550 (2009)
S.J. Waddell, S.J. Popper, K.H. Rubins, M.J. Griffiths, P.O. Brown, M. Levin, D.A. Relman, Dissecting interferon-induced transcriptional programs in human peripheral blood cells. PLoS One 5, e9753 (2010)
F.O. Martinez, S. Gordon, M. Locati, A. Mantovani, Transcriptional profiling of the human monocyte-to-macrophage differentiation and polarization: New molecules and patterns of gene expression. J Immunol 177, 7303–7311 (2006)
G.J. Nau, J.F. Richmond, A. Schlesinger, E.G. Jennings, E.S. Lander, R.A. Young, Human macrophage activation programs induced by bacterial pathogens. Proc Natl Acad Sci U S A 99, 1503–1508 (2002)
A. Mantovani, A. Sica, S. Sozzani, P. Allavena, A. Vecchi, M. Locati, The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol 25, 677–686 (2004)
A. Mantovani, S. Sozzani, M. Locati, P. Allavena, A. Sica, Macrophage polarization: Tumor-associated macrophages as a paradigm for polarized M2 mononuclear phagocytes. Trends Immunol 23, 549–555 (2002)
F.O. Martinez, L. Helming, R. Milde, A. Varin, B.N. Melgert, C. Draijer, B. Thomas, M. Fabbri, A. Crawshaw, L.P. Ho, N.H. Ten Hacken, V. Cobos Jimenez, N.A. Kootstra, J. Hamann, D.R. Greaves, M. Locati, A. Mantovani, S. Gordon, Genetic programs expressed in resting and IL-4 alternatively activated mouse and human macrophages: Similarities and differences. Blood 121, e57–e69 (2013)
C.J. Scotton, F.O. Martinez, M.J. Smelt, M. Sironi, M. Locati, A. Mantovani, S. Sozzani, Transcriptional profiling reveals complex regulation of the monocyte IL-1 beta system by IL-13. J Immunol 174, 834–845 (2005)
F. Davatchi, F. Shahram, C. Chams-Davatchi, H. Shams, A. Nadji, M. Akhlaghi, T. Faezi, Z. Ghodsi, A. Faridar, F. Ashofteh, Behcet’s disease: From east to west. Clin Rheumatol 29, 823–833 (2010)
D.J. Cua, S.A. Stohlman, In vivo effects of T helper cell type 2 cytokines on macrophage antigen-presenting cell induction of T helper subsets. J Immunol 159, 5834–5840 (1997)
N.D. Savage, T. de Boer, K.V. Walburg, S.A. Joosten, K. van Meijgaarden, A. Geluk, T.H. Ottenhoff, Human anti-inflammatory macrophages induce Foxp3+ GITR+ CD25+ regulatory T cells, which suppress via membrane-bound TGFbeta-1. J Immunol 181, 2220–2226 (2008)
F.O. Martinez, S. Gordon, The M1 and M2 paradigm of macrophage activation: Time for reassessment. F1000Prime Rep 6, 13 (2014)
D. Hanahan, R.A. Weinberg, Hallmarks of cancer: The next generation. cell 144, 646–674 (2011)
B.B. Aggarwal, R.V. Vijayalekshmi, B. Sung, Targeting inflammatory pathways for prevention and therapy of cancer: Short-term friend, long-term foe. Clin Cancer Res 15, 425–430 (2009)
F. Colotta, P. Allavena, A. Sica, C. Garlanda, A. Mantovani, Cancer-related inflammation, the seventh hallmark of cancer: Links to genetic instability. Carcinogenesis 30, 1073–1081 (2009)
G. Cassinelli, E. Favini, D. Degl'Innocenti, A. Salvi, G. De Petro, M.A. Pierotti, F. Zunino, M.G. Borrello, C. Lanzi, RET/PTC1-driven neoplastic transformation and Proinvasive phenotype of human Thyrocytes involve met induction and β-catenin nuclear translocation. Neoplasia 11, 10–21 (2009)
A. Sparmann, D. Bar-Sagi, Ras-induced interleukin-8 expression plays a critical role in tumor growth and angiogenesis. Cancer Cell 6, 447–458 (2004)
K. Shchors, E. Shchors, F. Rostker, E.R. Lawlor, L. Brown-Swigart, G.I. Evan, The Myc-dependent angiogenic switch in tumors is mediated by interleukin 1beta. Genes Dev 20, 2527–2538 (2006)
P. Staller, J. Sulitkova, J. Lisztwan, H. Moch, E.J. Oakeley, W. Krek, Chemokine receptor CXCR4 downregulated by von Hippel-Lindau tumour suppressor pVHL. Nature 425, 307–311 (2003)
A. Mantovani, P. Allavena, A. Sica, F. Balkwill, Cancer-related inflammation. Nature 454, 436–444 (2008)
J.F. Bromberg, M.H. Wrzeszczynska, G. Devgan, Y. Zhao, R.G. Pestell, C. Albanese, J.E. Darnell Jr., Stat3 as an oncogene. Cell 98, 295–303 (1999)
A. Saccani, T. Schioppa, C. Porta, S.K. Biswas, M. Nebuloni, L. Vago, B. Bottazzi, M.P. Colombo, A. Mantovani, A. Sica, p50 nuclear factor-kappaB overexpression in tumor-associated macrophages inhibits M1 inflammatory responses and antitumor resistance. Cancer Res 66, 11432–11440 (2006)
T. Wang, G. Niu, M. Kortylewski, L. Burdelya, K. Shain, S. Zhang, R. Bhattacharya, D. Gabrilovich, R. Heller, D. Coppola, W. Dalton, R. Jove, D. Pardoll, H. Yu, Regulation of the innate and adaptive immune responses by Stat-3 signaling in tumor cells. Nat Med 10, 48–54 (2004)
T. Itesako, N. Seki, H. Yoshino, T. Chiyomaru, T. Yamasaki, H. Hidaka, T. Yonezawa, N. Nohata, T. Kinoshita, M. Nakagawa, The microRNA expression signature of bladder cancer by deep sequencing: The functional significance of the miR-195/497 cluster. PLoS One 9, e84311 (2014)
Y. Ben-Neriah, M. Karin, Inflammation meets cancer, with NF-kappaB as the matchmaker. Nat Immunol 12, 715–723 (2011)
M. Kortylewski, M. Kujawski, T. Wang, S. Wei, S. Zhang, S. Pilon-Thomas, G. Niu, H. Kay, J. Mule, W.G. Kerr, R. Jove, D. Pardoll, H. Yu, Inhibiting Stat3 signaling in the hematopoietic system elicits multicomponent antitumor immunity. Nat Med 11, 1314–1321 (2005)
B. Wang, Q. Li, L. Qin, S. Zhao, J. Wang, X. Chen, Transition of tumor-associated macrophages from MHC class II (hi) to MHC class II (low) mediates tumor progression in mice. BMC Immunol 12, 43 (2011)
Y. Nakanishi, M. Nakatsuji, H. Seno, S. Ishizu, R. Akitake-Kawano, K. Kanda, T. Ueo, H. Komekado, M. Kawada, M. Minami, T. Chiba, COX-2 inhibition alters the phenotype of tumor-associated macrophages from M2 to M1 in ApcMin/+ mouse polyps. Carcinogenesis 32, 1333–1339 (2011)
K. Chen, J. Huang, W. Gong, P. Iribarren, N.M. Dunlop, J.M. Wang, Toll-like receptors in inflammation, infection and cancer. Int Immunopharmacol 7, 1271–1285 (2007)
S. Banerjee, K. Halder, A. Bose, P. Bhattacharya, G. Gupta, S. Karmahapatra, S. Das, S. Chaudhuri, S. Bhattacharyya Majumdar, S. Majumdar, TLR signaling-mediated differential histone modification at IL-10 and IL-12 promoter region leads to functional impairments in tumor-associated macrophages. Carcinogenesis 32, 1789–1797 (2011)
J. Rius, M. Guma, C. Schachtrup, K. Akassoglou, A.S. Zinkernagel, V. Nizet, R.S. Johnson, G.G. Haddad, M. Karin, NF-kappaB links innate immunity to the hypoxic response through transcriptional regulation of HIF-1alpha. Nature 453, 807–811 (2008)
Y.C. Wang, F. He, F. Feng, X.W. Liu, G.Y. Dong, H.Y. Qin, X.B. Hu, M.H. Zheng, L. Liang, L. Feng, Y.M. Liang, H. Han, Notch signaling determines the M1 versus M2 polarization of macrophages in antitumor immune responses. Cancer Res 70, 4840–4849 (2010)
L. Sanchez-Martin, A. Estecha, R. Samaniego, S. Sanchez-Ramon, M.A. Vega, P. Sanchez-Mateos, The chemokine CXCL12 regulates monocyte-macrophage differentiation and RUNX3 expression. Blood 117, 88–97 (2011)
S.-C. Wang, J.-H. Hong, C. Hsueh, C.-S. Chiang, Tumor-secreted SDF-1 promotes glioma invasiveness and TAM tropism toward hypoxia in a murine astrocytoma model. Lab Investig 92, 151–162 (2012)
J.Y. Park, J.Y. Sung, J. Lee, Y.K. Park, Y.W. Kim, G.Y. Kim, K.Y. Won, S.J. Lim, Polarized CD163+ tumor-associated macrophages are associated with increased angiogenesis and CXCL12 expression in gastric cancer. Clin Res Hepatol Gastroenterol 40, 357–365 (2016)
J. Wang, G.C.W. Man, T.H. Chan, J. Kwong, C.C. Wang, A prodrug of green tea polyphenol (−)-epigallocatechin-3-gallate (pro-EGCG) serves as a novel angiogenesis inhibitor in endometrial cancer. Cancer Lett 412, 10–20 (2018)
A. Mantovani, A. Sica, Macrophages, innate immunity and cancer: Balance, tolerance, and diversity. Curr Opin Immunol 22, 231–237 (2010)
S.J. Moghaddam, H. Li, S.N. Cho, M.K. Dishop, I.I. Wistuba, L. Ji, J.M. Kurie, B.F. Dickey, F.J. Demayo, Promotion of lung carcinogenesis by chronic obstructive pulmonary disease-like airway inflammation in a K-ras-induced mouse model. Am J Respir Cell Mol Biol 40, 443–453 (2009)
M. Karin, F.R. Greten, NF-kappaB: Linking inflammation and immunity to cancer development and progression. Nat Rev Immunol 5, 749–759 (2005)
L. Deng, J.F. Zhou, R.S. Sellers, J.F. Li, A.V. Nguyen, Y. Wang, A. Orlofsky, Q. Liu, D.A. Hume, J.W. Pollard, L. Augenlicht, E.Y. Lin, A novel mouse model of inflammatory bowel disease links mammalian target of rapamycin-dependent hyperproliferation of colonic epithelium to inflammation-associated tumorigenesis. Am J Pathol 176, 952–967 (2010)
F. Gotsch, R. Romero, L. Friel, J.P. Kusanovic, J. Espinoza, O. Erez, N.G. Than, P. Mittal, S. Edwin, B.H. Yoon, C.J. Kim, S. Mazaki-Tovi, T. Chaiworapongsa, S.S. Hassan, CXCL10/IP-10: A missing link between inflammation and anti-angiogenesis in preeclampsia? J Matern-Fetal Neonatal Med 20, 777–792 (2007)
F.R. Greten, L. Eckmann, T.F. Greten, J.M. Park, Z.W. Li, L.J. Egan, M.F. Kagnoff, M. Karin, IKKbeta links inflammation and tumorigenesis in a mouse model of colitis-associated cancer. Cell 118, 285–296 (2004)
B. Pang, X. Zhou, H. Yu, M. Dong, K. Taghizadeh, J.S. Wishnok, S.R. Tannenbaum, P.C. Dedon, Lipid peroxidation dominates the chemistry of DNA adduct formation in a mouse model of inflammation. Carcinogenesis 28, 1807–1813 (2007)
Q. Guo, J. Li, H. Lin, Effect and molecular mechanisms of traditional Chinese medicine on regulating tumor immunosuppressive microenvironment. Biomed Res Int 12, 2015 (2015)
J. Kim, J.-S. Bae, Tumor-associated macrophages and neutrophils in tumor microenvironment. Mediat Inflamm 2016, 1–11 (2016)
S. Farajzadeh Valilou, M. Keshavarz-Fathi, N. Silvestris, A. Argentiero, N. Rezaei, The role of inflammatory cytokines and tumor associated macrophages (TAMs) in microenvironment of pancreatic cancer. Cytokine Growth Factor Rev 39, 46–61 (2018)
Q. Guo, Z. Jin, Y. Yuan, R. Liu, T. Xu, H. Wei, X. Xu, S. He, S. Chen, Z. Shi, W. Hou, B. Hua, New mechanisms of tumor-associated macrophages on promoting tumor progression: Recent research advances and potential targets for tumor immunotherapy. J Immunol Res 2016, 12 (2016)
M. Lohela, A.J. Casbon, A. Olow, L. Bonham, D. Branstetter, N. Weng, J. Smith, Z. Werb, Intravital imaging reveals distinct responses of depleting dynamic tumor-associated macrophage and dendritic cell subpopulations. Proc Natl Acad Sci U S A 111, E5086–E5095 (2014)
A. Angelis, D. Tordrup, P. Kanavos, Socio-economic burden of rare diseases: A systematic review of cost of illness evidence. Health Policy 119, 964–979 (2015)
K. Van Naarden Braun, D. Christensen, N. Doernberg, L. Schieve, C. Rice, L. Wiggins, D. Schendel, M. Yeargin-Allsopp, Trends in the prevalence of autism Spectrum disorder, cerebral palsy, hearing loss, intellectual disability, and vision impairment, metropolitan Atlanta, 1991–2010. PLoS One 10, 1991-2010 (2015)
T. Lu, R. Ramakrishnan, S. Altiok, J.-I. Youn, P. Cheng, E. Celis, V. Pisarev, S. Sherman, M.B. Sporn, D. Gabrilovich, Tumor-infiltrating myeloid cells induce tumor cell resistance to cytotoxic T cells in mice. J Clin Invest 121, 4015–4029 (2011)
P.C. Rodriguez, D.G. Quiceno, J. Zabaleta, B. Ortiz, A.H. Zea, M.B. Piazuelo, A. Delgado, P. Correa, J. Brayer, E.M. Sotomayor, S. Antonia, J.B. Ochoa, A.C. Ochoa, Arginase I production in the tumor microenvironment by mature myeloid cells inhibits T-cell receptor expression and antigen-specific T-cell responses. Cancer Res 64, 5839–5849 (2004)
A. Kondo, T. Yamashita, H. Tamura, W. Zhao, T. Tsuji, M. Shimizu, E. Shinya, H. Takahashi, K. Tamada, L. Chen, K. Dan, K. Ogata, Interferon-gamma and tumor necrosis factor-alpha induce an immunoinhibitory molecule, B7-H1, via nuclear factor-kappaB activation in blasts in myelodysplastic syndromes. Blood 116, 1124–1131 (2010)
F. Vari, D. Arpon, C. Keane, M.S. Hertzberg, D. Talaulikar, S. Jain, Q. Cui, E. Han, J. Tobin, R. Bird, D. Cross, A. Hernandez, C. Gould, S. Birch, M.K. Gandhi, Immune evasion via PD-1/PD-L1 on NK-cells and monocyte/macrophages is more prominent in Hodgkin lymphoma than DLBCL. Blood 131, 1809–1819 (2018)
L. Yang, Y. Zhang, Tumor-associated macrophages: From basic research to clinical application. J Hematol Oncol 10, 58 (2017)
T. Chanmee, P. Ontong, K. Konno, N. Itano, Tumor-associated macrophages as major players in the tumor microenvironment. Cancers 6, 1670–1690 (2014)
J. Choi, J. Gyamfi, H. Jang, J.S. Koo, The role of tumor-associated macrophage in breast cancer biology. Histol Histopathol 6, 11–916 (2017)
E. Obeid, R. Nanda, Y.-X. Fu, O. Olopade, The role of tumor-associated macrophages in breast cancer progression. Int J Oncol 43, 5–12 (2013)
D. Capece, M. Fischietti, D. Verzella, A. Gaggiano, G. Cicciarelli, A. Tessitore, F. Zazzeroni, E. Alesse, The inflammatory microenvironment in hepatocellular carcinoma: A pivotal role for tumor-associated macrophages. Biomed Res Int 2013, 15–30 (2012)
M. Erreni, A. Mantovani, P. Allavena, Tumor-associated macrophages (TAM) and inflammation in colorectal Cancer. Cancer Microenviron 4, 141–154 (2011)
C. Lapa, T. Linsenmann, K. Lückerath, S. Samnick, K. Herrmann, C. Stoffer, R.-I. Ernestus, A.K. Buck, M. Löhr, C.-M. Monoranu, Tumor-associated macrophages in glioblastoma Multiforme—A suitable target for somatostatin receptor-based imaging and therapy? PLoS One 10, e0122269 (2015)
Z. Chen, X. Feng, C.J. Herting, V.A. Garcia, K. Nie, W.W. Pong, R. Rasmussen, B. Dwivedi, S. Seby, S.A. Wolf, D.H. Gutmann, D. Hambardzumyan, Cellular and molecular identity of tumor-associated macrophages in glioblastoma. Cancer Res 77, 2266–2278 (2017)
R.M. Fawzy, E.A. Said, S.M. Mohamed, N.A. Fouad, E.M. Akl, Serum Interleukin-33 in Behcet's disease: Its relation to disease activity and clinical manifestations. Egypt J Immunol 22, 1 (2015)
A. Brenot, B.L. Knolhoff, D.G. DeNardo, G.D. Longmore, SNAIL1 action in tumor cells influences macrophage polarization and metastasis in breast cancer through altered GM-CSF secretion. Oncogenesis 7, 32 (2018)
E. Giurisato, Q. Xu, S. Lonardi, B. Telfer, I. Russo, A. Pearson, K.G. Finegan, W. Wang, J. Wang, N.S. Gray, W. Vermi, Z. Xia, C. Tournier, Myeloid ERK5 deficiency suppresses tumor growth by blocking protumor macrophage polarization via STAT3 inhibition. Proc Natl Acad Sci U S A 115, E2801–E2e10 (2018)
V. Riabov, A. Gudima, N. Wang, A. Mickley, A. Orekhov, J. Kzhyshkowska, Role of tumor associated macrophages in tumor angiogenesis and lymphangiogenesis. Front Physiol 5, 75 (2014)
C. Medrek, F. Pontén, K. Jirström, K. Leandersson, The presence of tumor associated macrophages in tumor stroma as a prognostic marker for breast cancer patients. BMC Cancer 12, 306 (2012)
A. Ferrer-Admetlla, M. Sikora, H. Laayouni, A. Esteve, F. Roubinet, A. Blancher, F. Calafell, J. Bertranpetit, F. Casals, A natural history of FUT2 polymorphism in humans. Mol Biol Evol 26, 1993–2003 (2009)
A.J. Majmundar, W.J. Wong, M.C. Simon, Hypoxia-inducible factors and the response to hypoxic stress. Mol Cell 40, 294–309 (2010)
M.A. Badawi, D.M. Abouelfadl, S.L. El-Sharkawy, W.E.A. El-Aal, N.F. Abbas, Tumor-associated macrophage (TAM) and angiogenesis in human Colon carcinoma. Maced J Med Sci 3, 209–214 (2015)
C.E. Lewis, M. De Palma, L. Naldini, Tie2-expressing monocytes and tumor angiogenesis: Regulation by hypoxia and angiopoietin-2. Cancer Res 67, 8429–8432 (2007)
A. Capobianco, A. Monno, L. Cottone, M.A. Venneri, D. Biziato, F. Di Puppo, S. Ferrari, M. De Palma, A.A. Manfredi, P. Rovere-Querini, Proangiogenic Tie2(+) macrophages infiltrate human and murine Endometriotic lesions and dictate their growth in a mouse model of the disease. Am J Pathol 179, 2651–2659 (2011)
R. Turrini, A. Pabois, I. Xenarios, G. Coukos, J.-F. Delaloye, M.-A. Doucey, TIE-2 expressing monocytes in human cancers. Oncoimmunology 6, e1303585 (2017)
J. Lee, J. Song, E.S. Kwon, S. Jo, M.K. Kang, Y.J. Kim, Y. Hwang, H. Bae, T.H. Kang, S. Chang, H.J. Cho, S.C. Kim, S. Kim, S.S. Koh, CTHRC1 promotes angiogenesis by recruiting Tie2-expressing monocytes to pancreatic tumors. Exp Mol Med 48, 87 (2016)
X. Wang, Q. Zhu, Y. Lin, L. Wu, X. Wu, K. Wang, Q. He, C. Xu, X. Wan, Crosstalk between TEMs and endothelial cells modulates angiogenesis and metastasis via IGF1-IGF1R signalling in epithelial ovarian cancer. Br J Cancer 12, 297 (2017)
C.E. Lewis, M. De Palma, L. Naldini, Tie2-expressing monocytes and tumor angiogenesis: Regulation by hypoxia and Angiopoietin-2. Cancer Res 67, 8429–8432 (2007)
L. Chen, J. Li, F. Wang, C. Dai, F. Wu, X. Liu, T. Li, R. Glauben, Y. Zhang, G. Nie, Y. He, Z. Qin, Tie2 expression on macrophages is required for blood vessel reconstruction and tumor relapse after chemotherapy. Cancer Res 76, 6828–6838 (2016)
B.I. Rini, Vascular endothelial growth factor-targeted therapy in renal cell carcinoma: Current status and future directions. Clin Cancer Res 13, 1098–1106 (2007)
M. Yousefi, R. Nosrati, A. Salmaninejad, S. Dehghani, A. Shahryari, A. Saberi, Organ-specific metastasis of breast cancer: Molecular and cellular mechanisms underlying lung metastasis. Cell Oncol 41, 123–140 (2018)
L. Manso, F. Moreno, R. Márquez, B. Castelo, A. Arcediano, M. Arroyo, A.I. Ballesteros, I. Calvo, M.J. Echarri, S. Enrech, A. Gómez, R. González del Val, E. López-Miranda, M. Martín-Angulo, N. Martínez-Jañez, C. Olier, P. Zamora, Use of bevacizumab as a first-line treatment for metastatic breast cancer. Curr Oncol 22, e51–e60 (2015)
L. Rossi, M. Verrico, E. Zaccarelli, A. Papa, M. Colonna, M. Strudel, P. Vici, V. Bianco, F. Tomao, Bevacizumab in ovarian cancer: A critical review of phase III studies. Oncotarget 8, 12389–12405 (2017)
M. Yousefi, T. Bahrami, A. Salmaninejad, R. Nosrati, P. Ghaffari, S.H. Ghaffari, Lung cancer-associated brain metastasis: Molecular mechanisms and therapeutic options. Cell Oncol 40, 419–441 (2017)
K.S. Tewari, M.W. Sill, R.T. Penson, H. Huang, L.M. Ramondetta, L.M. Landrum, A. Oaknin, T.J. Reid, M.M. Leitao, H.E. Michael, P.J. DiSaia, L.J. Copeland, W.T. Creasman, F.B. Stehman, M.F. Brady, R.A. Burger, J.T. Thigpen, M.J. Birrer, S.E. Waggoner, D.H. Moore, K.Y. Look, W.J. Koh, B.J. Monk, Bevacizumab for advanced cervical cancer: Final overall survival and adverse event analysis of a randomised, controlled, open-label, phase 3 trial (gynecologic oncology group 240). Lancet 27, 31607–31600 (2017)
A. Scholz, P.N. Harter, S. Cremer, B.H. Yalcin, S. Gurnik, M. Yamaji, M. Di Tacchio, K. Sommer, P. Baumgarten, O. Bahr, J.P. Steinbach, J. Trojan, M. Glas, U. Herrlinger, D. Krex, M. Meinhardt, A. Weyerbrock, M. Timmer, R. Goldbrunner, M. Deckert, C. Braun, J. Schittenhelm, J.T. Frueh, E. Ullrich, M. Mittelbronn, K.H. Plate, Y. Reiss, Endothelial cell-derived angiopoietin-2 is a therapeutic target in treatment-naive and bevacizumab-resistant glioblastoma. EMBO Mol Med 8, 39–57 (2016)
T.E. Peterson, N.D. Kirkpatrick, Y. Huang, C.T. Farrar, K.A. Marijt, J. Kloepper, M. Datta, Z. Amoozgar, G. Seano, K. Jung, W.S. Kamoun, T. Vardam, M. Snuderl, J. Goveia, S. Chatterjee, A. Batista, A. Muzikansky, C.C. Leow, L. Xu, T.T. Batchelor, D.G. Duda, D. Fukumura, R.K. Jain, Dual inhibition of Ang-2 and VEGF receptors normalizes tumor vasculature and prolongs survival in glioblastoma by altering macrophages. Proc Natl Acad Sci U S A 113, 4470–4475 (2016)
K. Erturk, F. Tas, M. Serilmez, E. Bilgin, V. Yasasever, Clinical Signifčcance of Serum Ykl-40 (Chitinase-3-Like-1 protein) as a biomarker in melanoma: An analysis of 112 Turkish patients. ASIAN PAC J CANCER P 18, 1383–1387 (2017)
T. Vaananen, J. Kallio, K. Vuolteenaho, A. Ojala, T. Luukkaala, M. Hamalainen, T. Tammela, P.L. Kellokumpu-Lehtinen, E. Moilanen, High YKL-40 is associated with poor survival in patients with renal cell carcinoma: A novel independent prognostic marker. Scand J Urol 23, 1–6 (2017)
A. Attia, A. Rasmy, A. Amin, M. Alanazi, Evaluation of pleural fluid YKL-40 as a marker of malignant pleural effusion. Egypt J Chest Dis Tuberc 64, 489–495 (2015)
R.V. Ghartavol, R. Mombeiny, A. Salmaninejad, S.M.R. Sorkhabadi, R.F. Majidi, M.R. Jaafari, H. Mirzaei, Tumor-associated macrophages and epithelial–mesenchymal transition in cancer: Nanotechnology comes into view. J Cell Physiol 233, 9223–9236 (2018)
R. Shao, R. Francescone, N. Ngernyuang, B. Bentley, S.L. Taylor, L. Moral, W. Yan, Anti-YKL-40 antibody and ionizing irradiation synergistically inhibit tumor vascularization and malignancy in glioblastom. Carcinogenesis 35, 373–382 (2013)
X.W. Chen, T.J. Yu, J. Zhang, Y. Li, H.L. Chen, G.F. Yang, W. Yu, Y.Z. Liu, X.X. Liu, C.F. Duan, H.L. Tang, M. Qiu, C.L. Wang, H. Zheng, J. Yue, A.M. Guo, J. Yang, CYP4A in tumor-associated macrophages promotes pre-metastatic niche formation and metastasis. Oncogene 36, 5045–5057 (2017)
C. Wang, Y. Li, H. Chen, J. Zhang, T. Qin, C. Duan, X. Chen, Y. Liu, X. Zhou, J. Yang, Inhibition of CYP4A by a novel flavonoid FLA-16 prolongs survival and normalizes tumor vasculature in glioma. Cancer Lett 402, 131–141 (2017)
J.-W. Tjiu, J.-S. Chen, C.-T. Shun, S.-J. Lin, Y.-H. Liao, C.-Y. Chu, T.-F. Tsai, H.-C. Chiu, Y.-S. Dai, H. Inoue, P.-C. Yang, M.-L. Kuo, S.-H. Jee, Tumor-associated macrophage-induced invasion and angiogenesis of human basal cell carcinoma cells by Cyclooxygenase-2 induction. J Invest Dermatol 129, 1016–1025 (2009)
H. Son, A. Moon, Epithelial-mesenchymal transition and cell invasion. Toxicological Res 26, 245–252 (2010)
T. Wu, B. Cheng, L. Fu, Clinical applications of circulating tumor cells in pharmacotherapy: Challenges and perspectives. Mol Pharmacol 92, 232–239 (2017)
S. Lamouille, J. Xu, R. Derynck, Molecular mechanisms of epithelial–mesenchymal transition. Nat Rev Mol Cell Biol 15, 178–196 (2014)
M.A. Huber, N. Kraut, H. Beug, Molecular requirements for epithelial-mesenchymal transition during tumor progression. Curr Opin Cell Biol 17, 548–558 (2005)
H. Fazilaty, M. Gardaneh, T. Bahrami, A. Salmaninejad, B. Behnam, Crosstalk between breast cancer stem cells and metastatic niche: Emerging molecular metastasis pathway? Tumor Biol 34, 2019–2030 (2013)
J. Zhang, Y. Yan, Y. Yang, L. Wang, M. Li, J. Wang, X. Liu, X. Duan, J. Wang, High infiltration of tumor-associated macrophages influences poor prognosis in human gastric Cancer patients, associates with the phenomenon of EMT. Medicine 95, e2636 (2016)
S.P. Chiang, R.M. Cabrera, J.E. Segall, Tumor cell intravasation. Am J Physiol Cell Physiol 311, 1–14 (2016)
A. Dovas, A. Patsialou, A.S. Harney, J. Condeelis, D. Cox, Imaging interactions between macrophages and tumour cells that are involved in metastasis in vivo and in vitro. J Microsc 251, 261–269 (2013)
J.B. Wyckoff, Y. Wang, E.Y. Lin, J.F. Li, S. Goswami, E.R. Stanley, J.E. Segall, J.W. Pollard, J. Condeelis, Direct visualization of macrophage-assisted tumor cell intravasation in mammary tumors. Cancer Res 67, 2649–2656 (2007)
J. Kim, J.S. Bae, Tumor-associated macrophages and neutrophils in tumor microenvironment. Mediat Inflamm 6058147, 1–11 (2016)
E. Gorelik, R.H. Wiltrout, M.J. Brunda, H.T. Holden, R.B. Herberman, Augmentation of metastasis formation by thioglycollate-elicited macrophages. Int J Cancer 29, 575–581 (1982)
J.M. Hu, K. Liu, J.H. Liu, X.L. Jiang, X.L. Wang, L. Yang, Y.Z. Chen, C.X. Liu, S.G. Li, X.B. Cui, H. Zou, L.J. Pang, J. Zhao, Y. Qi, W.H. Liang, X.L. Yuan, F. Li, The increased number of tumor-associated macrophage is associated with overexpression of VEGF-C, plays an important role in Kazakh ESCC invasion and metastasis. Exp Mol Pathol 102, 15–21 (2017)
R.D. Leek, N.C. Hunt, R.J. Landers, C.E. Lewis, J.A. Royds, A.L. Harris, Macrophage infiltration is associated with VEGF and EGFR expression in breast cancer. J Pathol 190, 430–436 (2000)
S. Sousa, J. Määttä, The role of tumour-associated macrophages in bone metastasis. J Bone Oncol 5, 135–138 (2016)
V. Chitu, E.R. Stanley, Colony-stimulating factor-1 in immunity and inflammation. Curr Opin Immunol 18, 39–48 (2006)
R. Noy, J.W. Pollard, Tumor-associated macrophages: From mechanisms to therapy. Immunity 41, 49–61 (2014)
C.H. Ries, S. Hoves, M.A. Cannarile, D. Ruttinger, CSF-1/CSF-1R targeting agents in clinical development for cancer therapy. Curr Opin Pharmacol 23, 45–51 (2015)
J. Wyckoff, W. Wang, E.Y. Lin, Y. Wang, F. Pixley, E.R. Stanley, T. Graf, J.W. Pollard, J. Segall, J. Condeelis, A paracrine loop between tumor cells and macrophages is required for tumor cell migration in mammary tumors. Cancer Res 64, 7022–7029 (2004)
J. Wang, Z. Cao, X.M. Zhang, M. Nakamura, M. Sun, J. Hartman, R.A. Harris, Y. Sun, Y. Cao, Novel mechanism of macrophage-mediated metastasis revealed in a zebrafish model of tumor development. Cancer Res 75, 306–315 (2015)
S. Goswami, E. Sahai, J.B. Wyckoff, M. Cammer, D. Cox, F.J. Pixley, E.R. Stanley, J.E. Segall, J.S. Condeelis, Macrophages promote the invasion of breast carcinoma cells via a Colony-stimulating Factor-1/epidermal growth factor paracrine loop. Cancer Res 65, 5278–5283 (2005)
J.A. Joyce, J.W. Pollard, Microenvironmental regulation of metastasis. Nat Rev Cancer 9, 239–252 (2009)
S.M. Pyonteck, L. Akkari, A.J. Schuhmacher, R.L. Bowman, L. Sevenich, D.F. Quail, O.C. Olson, M.L. Quick, J.T. Huse, V. Teijeiro, M. Setty, C.S. Leslie, Y. Oei, A. Pedraza, J. Zhang, C.W. Brennan, J.C. Sutton, E.C. Holland, D. Daniel, J.A. Joyce, CSF-1R inhibition alters macrophage polarization and blocks glioma progression. Nat Med 19, 1264–1272 (2013)
D. Hambardzumyan, D.H. Gutmann, H. Kettenmann, The role of microglia and macrophages in glioma maintenance and progression. Nat Neurosci 19, 20–27 (2016)
D.L. Adams, S.S. Martin, R.K. Alpaugh, M. Charpentier, S. Tsai, R.C. Bergan, I.M. Ogden, W. Catalona, S. Chumsri, C.M. Tang, M. Cristofanilli, Circulating giant macrophages as a potential biomarker of solid tumors. Proc Natl Acad Sci 111, 3514–3519 (2014)
D.L. Adams, D.K. Adams, R.K. Alpaugh, M. Cristofanilli, S.S. Martin, S. Chumsri, C.M. Tang, J.R. Marks, Circulating Cancer-associated macrophage-like cells differentiate malignant breast Cancer and benign breast conditions. Cancer Epidemiol Biomark Prev 25, 1037–1042 (2016)
M. Tripathi, S. Nandana, S. Billet, K.A. Cavassani, R. Mishra, L.W. Chung, E.M. Posadas, N.A. Bhowmick, Modulation of cabozantinib efficacy by the prostate tumor microenvironment. Oncotarget 8, 87891- 902 (2017)
F. Dammeijer, L.A. Lievense, M.E. Kaijen-Lambers, M. van Nimwegen, K. Bezemer, J.P. Hegmans, T. van Hall, R.W. Hendriks, J.G. Aerts, Depletion of tumor-associated macrophages with a CSF-1R kinase inhibitor enhances antitumor immunity and survival induced by DC immunotherapy. Cancer Immunol Res 5, 535–546 (2017)
Y. Lin, C. Wei, Y. Liu, Y. Qiu, C. Liu, F. Guo, Selective ablation of tumor-associated macrophages suppresses metastasis and angiogenesis. Cancer Sci 104, 1217–1225 (2013)
K. Stoletov, H. Kato, E. Zardouzian, J. Kelber, J. Yang, S. Shattil, R. Klemke, Visualizing extravasation dynamics of metastatic tumor cells. J Cell Sci 123, 2332–2341 (2010)
A.B. Al-Mehdi, K. Tozawa, A.B. Fisher, L. Shientag, A. Lee, R.J. Muschel, Intravascular origin of metastasis from the proliferation of endothelium-attached tumor cells: A new model for metastasis. Nat Med 6, 100–102 (2000)
D. Schumacher, B. Strilic, K.K. Sivaraj, N. Wettschureck, S. Offermanns, Platelet-derived nucleotides promote tumor-cell transendothelial migration and metastasis via P2Y2 receptor. Cancer Cell 24, 130–137 (2013)
T. Kitamura, B.-Z. Qian, J.W. Pollard, Immune cell promotion of metastasis. Nat Rev Immunol 15, 73–86 (2015)
S.Y. Lim, A.E. Yuzhalin, A.N. Gordon-Weeks, R.J. Muschel, Targeting the CCL2-CCR2 signaling axis in cancer metastasis. Oncotarget 7, 28697–28710 (2016)
S.R. Nielsen, M.C. Schmid, Macrophages as key drivers of Cancer progression and metastasis. Mediat Inflamm 9624760, 1–11 (2017)
T. Kitamura, B.-Z. Qian, D. Soong, L. Cassetta, R. Noy, G. Sugano, Y. Kato, J. Li, J.W. Pollard, CCL2-induced chemokine cascade promotes breast cancer metastasis by enhancing retention of metastasis-associated macrophages. J Exp Med 212, 1043–1059 (2015)
S. Weis, J. Cui, L. Barnes, D. Cheresh, Endothelial barrier disruption by VEGF-mediated Src activity potentiates tumor cell extravasation and metastasis. J Cell Biol 167, 223–229 (2004)
T.M. Nywening, A. Wang-Gillam, D.E. Sanford, B.A. Belt, R.Z. Panni, B.M. Cusworth, A.T. Toriola, R.K. Nieman, L.A. Worley, M. Yano, K.J. Fowler, A.C. Lockhart, R. Suresh, B.R. Tan, K.H. Lim, R.C. Fields, S.M. Strasberg, W.G. Hawkins, D.G. DeNardo, S.P. Goedegebuure, D.C. Linehan, Targeting tumour-associated macrophages with CCR2 inhibition in combination with FOLFIRINOX in patients with borderline resectable and locally advanced pancreatic cancer: A single-Centre, open-label, dose-finding, non-randomised, phase 1b trial. Lancet Oncol 17, 651–662 (2016)
B.Z. Qian, J. Li, H. Zhang, T. Kitamura, J. Zhang, L.R. Campion, E.A. Kaiser, L.A. Snyder, J.W. Pollard, CCL2 recruits inflammatory monocytes to facilitate breast-tumour metastasis. Nature 475, 222–225 (2011)
M. Roblek, E. Strutzmann, C. Zankl, T. Adage, M. Heikenwalder, A. Atlic, R. Weis, A. Kungl, L. Borsig, Targeting of CCL2-CCR2-glycosaminoglycan Axis using a CCL2 decoy protein attenuates metastasis through inhibition of tumor cell seeding. Neoplasia 18, 49–59 (2016)
T. Kitamura, B.-Z. Qian, J.W. Pollard, Immune cell promotion of metastasis. Nat Rev Immunol 15, 73–86 (2015)
S. Hiratsuka, A. Watanabe, H. Aburatani, Y. Maru, Tumour-mediated upregulation of chemoattractants and recruitment of myeloid cells predetermines lung metastasis. Nat Cell Biol 8, 1369–1375 (2006)
A. Zoccoli, M. Iuliani, F. Pantano, M. Imperatori, S. Intagliata, B. Vincenzi, P. Marchetti, N. Papapietro, V. Denaro, G. Tonini, D. Santini, Premetastatic niche: Ready for new therapeutic interventions? Expert Opin Ther Targets 16(23), S119–S129 (2012)
D. Wang, H. Sun, J. Wei, B. Cen, R.N. DuBois, CXCL1 is critical for Premetastatic niche formation and metastasis in colorectal Cancer. Cancer Res 77, 3655–3665 (2017)
M. Miyake, S. Hori, Y. Morizawa, Y. Tatsumi, Y. Nakai, S. Anai, K. Torimoto, K. Aoki, N. Tanaka, K. Shimada, N. Konishi, M. Toritsuka, T. Kishimoto, C.J. Rosser, K. Fujimoto, CXCL1-mediated interaction of Cancer cells with tumor-associated macrophages and Cancer-associated fibroblasts promotes tumor progression in human bladder Cancer. Neoplasia 18, 636–646 (2016)
J. Ursini-Siegel, P.M. Siegel, The influence of the pre-metastatic niche on breast cancer metastasis. Cancer Lett 380, 281–288 (2016)
J. Chen, Y. Yao, C. Gong, F. Yu, S. Su, J. Chen, B. Liu, H. Deng, F. Wang, L. Lin, H. Yao, F. Su, K.S. Anderson, Q. Liu, M.E. Ewen, X. Yao, E. Song, CCL18 from tumor-associated macrophages promotes breast Cancer metastasis via PITPNM3. Cancer Cell 19, 814–816 (2011)
H. Peinado, H. Zhang, I.R. Matei, B. Costa-Silva, A. Hoshino, G. Rodrigues, B. Psaila, R.N. Kaplan, J.F. Bromberg, Y. Kang, M.J. Bissell, T.R. Cox, A.J. Giaccia, J.T. Erler, S. Hiratsuka, C.M. Ghajar, D. Lyden, Pre-metastatic niches: Organ-specific homes for metastases. Nat Rev Cancer 17, 302–317 (2017)
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict if interests
None declared.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Salmaninejad, A., Valilou, S.F., Soltani, A. et al. Tumor-associated macrophages: role in cancer development and therapeutic implications. Cell Oncol. 42, 591–608 (2019). https://doi.org/10.1007/s13402-019-00453-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-019-00453-z