Abstract
Background
Various cancers have been found to be associated with heterogeneous and adaptive tumor microenvironments (TMEs) and to be driven by the local TMEs in which they thrive. Cancer heterogeneity plays an important role in tumor cell survival, progression and drug resistance. The diverse cellular components of the TME may include cancer-associated fibroblasts, adipocytes, pericytes, mesenchymal stem cells, endothelial cells, lymphocytes and other immune cells. These components may support tumor development through the secretion of growth factors, evasion from immune checkpoints, metabolic adaptations, modulations of the extracellular matrix, activation of oncogenes and the acquisition of drug resistance. Here, we will address recent advances in our understanding of the molecular mechanisms underlying stromal-tumor cell interactions, with special emphasis on basic and pre-clinical information that may facilitate the design of novel personalized cancer therapies.
Conclusions
This review presents a holistic view on the translational potential of the interplay between stromal cells and cancer cells. This interplay is currently being employed for the development of promising preclinical and clinical biomarkers, and the design of small molecule inhibitors, antibodies and small RNAs for (combinatorial) cancer treatment options. In addition, nano-carriers, tissue scaffolds and 3-D based matrices are being developed to precisely and safely deliver these compounds.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Cancer is the second leading cause of death worldwide [1]. In the past several basic, preclinical and clinical studies have been aimed at the development of novel, and/or the improvement of existing, cancer drugs [2,3,4,5]. The efficacies of these drugs, that are subjected to successive preclinical and clinical trials in various cancer models, face a plethora of hurdles, including the occurrence of tumor heterogeneity. In addition, it has become evident that several of the drugs used may be, or may become, ineffective due to the resurgence of drug resistance [4,5,6,7,8,9,10,11,12,13]. A major factor that promotes cancer development, including accelerated tumor cell proliferation, invasion, metastasis, angiogenesis and drug resistance, is related to tumor microenvironment (TME) heterogeneity [5, 11, 12, 14,15,16,17,18,19]. The TME is defined as a diverse environment that includes stromal cells, extracellular matrix components and secreted extracellular factors [4, 6,7,8, 11, 13, 17]. The cellular components of the TME include cancer-associated fibroblasts, adipocytes, pericytes, mesenchymal stem cells, endothelial cells, lymphocytes and other immune cells. [5, 11, 12, 15,16,17,18,19]. Ample evidence indicates that intercellular communication between cancer cells and stromal cells may be achieved through paracrine signaling. This paracrine signaling is thought to promote tumor development and progression, including invasion, metastasis, angiogenesis, drug resistance and recurrence [3, 6, 20,21,22,23,24,25]. In this review we summarize our current understanding of the paracrine crosstalk between stromal cells and cancer cells and its potential use for the design of novel therapeutic approaches at both preclinical and clinical levels.
2 Heterogeneous tumor landscapes
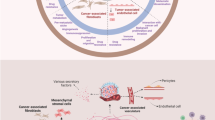
Intra-tumor heterogeneity refers to the occurrence of different cellular and non-cellular factors within a single tumor, whereas inter-tumor heterogeneity refers to the occurrence of different cellular and non-cellular factors within a similar tumor type in different patients [4, 5, 7, 9,10,11]. Several accumulating alterations and synergistic factors emanating from genetic and epigenetic changes are known to contribute to these heterogeneities [3,4,5, 10, 26] (Fig. 1), whereas their TMEs in conjunction with the genetic and epigenetic alterations, contribute to cancer development, progression, metastasis, angiogenesis and drug resistance [20, 23,24,25] (Fig. 2). A significant portion of tumor heterogeneity is attributed to its cellular heterogeneity, and the cellular components within the TME (see above) are known to be structurally, genetically, physiologically, functionally and anatomically distinct [20, 23,24,25]. These cellular components are subject to intensive investigations aimed at establishing their role in tumor development and drug resistance.
Stromal cells within the tumor microenvironment. Stromal components of the tumor microenvironment are depicted, including cancer-associated fibroblasts, adipocytes, pericytes, endothelial cells and mesenchymal stem cells. Additionally, factors that are exchanged between stromal cells and cancer cells to create a pro-cancer environment are depicted
In recent years, accumulating data have also uncovered a role of the cancer microbiome in tumor initiation and progression [27,28,29,30]. Currently, the diversity of microbiomes in local tumor niches is widely appreciated and some microorganisms have even been shown to support tumor development [28, 29]. Conversely, it has been found that some microbiomes may exhibit anti-tumor activities and, as such, increase the efficacy of chemotherapy [30]. So, also local microbiomes may contribute to inter- and intra-tumor heterogeneity. It should also be noted here that intra-tumor heterogeneity and tumor evolution over time may be linked to gradually changing microbiomes within individual tumors.
3 Cancer-associated fibroblasts
It has amply been reported that cancer-associated fibroblasts (CAFs) may play significant roles in cancer progression and metastasis through paracrine signaling [5, 19, 31,32,33,34,35,36,37]. CAFs mostly encompass mesenchyme-derived fibroblasts and myofibroblasts as supporting cells in different tumor types [19, 31, 32]. CAFs may express myofibroblast markers, such as stromal cell-derived factor-1 (SDF-1) and α-smooth muscle actin (α-SMA), as well as transforming growth factor-β1 (TGF-β1) [19, 31, 32]. Overall, it has been found that CAFs may secrete vast amounts of growth factors, chemokines, cytokines and proteases, as well as small regulatory RNAs, to enhance tumor cell proliferation, angiogenesis and invasion [19, 21, 31, 34, 35, 38,39,40,41].
3.1 Factors secreted by CAFs and their roles in tumor development
It has been reported that CAFs may play a role in modulating TMEs in various cancers, including breast cancer, prostate cancer, pancreatic cancer and oral cancer [41,42,43,44,45,46,47,48,49,50,51,52,53,54,55,56,57], and that the pro-cancer capabilities of these CAFs are mediated by paracrine signaling mediators [45,46,47,48,49,50,51,52,53,54,55,56,57]. Hendrayani et al. [44], for example, reported a tumor promoting role for CAF-secreted IL-6 in highly invasive breast carcinomas, indicated by the induction of reduced levels of the tumor suppressor proteins p16INK4A, p21WAF1 and p53. It has also been found that the CAF-secreted chemokines C-X-C motif ligand 14 (CXCL14) and CC chemokine ligand 2 (CCL2) may serve as paracrine signaling molecules to promote breast cancer cell survival. These secreted chemokines have also been found to serve as useful prognostic biomarkers [46, 47]. Others have found that TGF-ß1 levels in gastric cancer cells may be affected by rhomboid 5 homolog 2 (RHBDF2) in CAFs. Additional studies have revealed bidirectional communications between CAFs and cancer cells through the secretion of inflammatory cytokines by cancer cells, such as IL-1A, IL-1B and tumor necrosis factor (TNF), which may control the expression of RHBDF2 in CAFs [45]. Similarly, it has been found that CAFs may secrete CXCL12 and α-SMA and that these factors may enhance the invasive potential of breast cancer cells [55]. Importantly, Orimo et al. [56] found that CAFs can promote various cancer characteristics including growth and angiogenesis via increased secretion of SDF-1 and CXCL12. Cohen et al. [33] reported a new class of chitinase 3 like-1 (Chi3L1) factors that may be secreted by CAFs, thereby revealing a role of cellular crosstalk between CAFs, immune cells and cancer cells to establish favorable local tumor niches. Others have reported that platelet-derived growth factor (PDGF) secreted by CAFs may induce angiogenesis in luminal breast carcinoma and metastasis in colon carcinoma [52, 53]. Neri et al. [54] reported that the process of epithelial-mesenchymal transition (EMT) in cancer cells may result in an elevated secretion of PDGF-BB by CAFs, which is a subunit of the dimeric platelet-derived growth factor. This secreted growth factor plays a role in CAF-mediated cancer invasion. Kramer et al. [49] reported that canonical Wingless-Type 2 (WNT2) signaling may facilitate the communication between CAFs and colorectal cancer cells. Specifically, they found that WNT2 is secreted as a paracrine signaling molecule by CAFs that can induce canonical signaling in wild-type APC/β-catenin colon cancer cells. In another clinical breast cancer cohort study a role for tumor cell-secreted WNT7a in the modulation of TGF-β signaling in CAFs within the TME has been reported [50]. A recent report also indicated that communication between CAFs and pancreatic ductal adenocarcinoma (PDAC) cells may drive their invasive tendency [32, 57]. The authors revealed a role of SerpinB2 in collagen remodeling, and that reduced SerpinB2 levels may create a favorable TME. Subsequent data from a clinical study indicated that direct crosstalk between cancer cells and CAFs may drive tumor progression and extracellular matrix (ECM) remodeling [32]. Taken together, it has become evident that various factors secreted by CAFs may create favorable tumor niches via paracrine signaling. Disruption of the signaling axes created by these factors may pave the way for the design of novel therapeutic options.
3.2 Receptor-mediated CAF signaling within tumor niches
For both intracellular and extracellular signaling within the TME, CAFs and other cells use several types of receptors [50,51,52,53,54,55,56,57,58,59,60,61,62,63]. It has, for example, been reported that endothelial protein C receptor (EPCR) expression by endothelial cells can promote cancer progression and metastasis. These effects may be mediated by the matricellular secreted proteoglycan SPOCK1/testican 1 [58]. Another study has uncovered a role for transforming growth factor-β receptor type-2 (TGFβR2), a receptor of pleiotropic cytokines, in bridging crosstalk between CAFs and breast cancer cells. Additional data indicate that down-regulation of TGFβR2 in CAFs can trigger breast cancer cell growth and survival [59]. Hammer et al. [60] reported that stromal-derived platelet derived growth factor receptor (PDGFR)-α can modulate ECM components within the tumor niche. Another study has reported a role of cell surface marker CD44 expression on CAFs in maintaining stem cell-like properties of cancer cells, and that this marker may induce drug resistance [61]. Additional data suggest that CAFs may play essential roles in drug resistance through EMT mediated by HGF and, by doing so, stimulate anti-apoptotic signaling pathways [62]. Substantial evidence also suggests that PDGFR-ß may play a role in promoting tamoxifen resistance in breast cancer [63] and Corsa et al. [64] noted a role for fibrillar collagen receptor discoidin domain receptor 2 (DDR2) as potential therapeutic target to interrupt paracrine signaling during breast cancer metastasis. Among various factors investigated, clinical findings have suggested that fibroblast growth factor-inducible 14 (Fn14) may impart growth and drug resistance by activating the NF-κB pathway in small-cell lung cancer (SCLC) cells [65]. Another study has reported that IL-6 plays a role in enhancing the expression of the chemokine receptor CXCR7 via the STAT3/NF-κB signaling pathway in CAFs, and that the IL6-CXCR7 axis contributes to drug resistance in esophageal squamous cell carcinoma (ESCC) [10]. Another G protein-coupled estrogen receptor (GPER) has been found to play a role in insulin growth factor 1/insulin growth factor receptor signaling by modulating interactions between tumor cells and CAFs. Targeting the multifaceted interactions between cancer cells and their microenvironmental components through both G protein-coupled receptors (GPCRs) and other receptors may hold promise for the design of future anticancer therapies [65, 66].
3.3 Transcriptional and epigenetic regulation of CAF signaling
Crosstalk between cancer cells and CAFs has been found to be orchestrated by various downstream signaling pathways, including the Janus kinase/signal transducers and activators of transcription (JAK/STAT), mammalian target of rapamycin (mTOR), sonic hedgehog (SHH) and NF-kB pathways [19, 21, 31, 42, 43]. Yeo et al. [67] emphasized that overexpression of Twist Family BHLH Transcription Factor 1 (TWIST1) in CAFs may enhance ESCC development, and they suggested that this transcription factor may serve as a prognostic factor. CAFs may also favor breast tumor development through induction of the p38-signal transducers and activators of transcription 1 (STAT1) signaling axis. Other interesting data revealed a key role of STAT4 in CAF-mediated ovarian cancer development via cancer-secreted Wnt7a signaling [48]. Additionally, downregulation of ATF3, a stress-responsive transcriptional repressor, and its crosstalk with CSL-1, another type of transcriptional repressor, has been observed in CAFs. These two transcriptional repressors can modulate the epigenetic landscape in CAFs and, by doing so, promote cancer progression and metastasis [68].
3.4 Contribution of CAFs to metabolic tumor adaptations
Experimental evidence suggests that energy crosstalk between tumor cells and CAFs may create a favorable metabolic niche [21, 69, 70]. It has, for example, been found that CAFs can recycle tumor-derived lactate to meet cellular energy demands and that, in turn, CAFs may secrete other metabolites required for the lactate pathway, such as pyruvate, to support tumor growth. It has also been found that the majority of CAF-derived glucose is spared for tumor metabolic needs to support invasion and metastasis [70, 71] and that high levels of glycolysis in CAFs and secreted energetic metabolites may drive tumor growth and invasion [19, 21, 31, 70]. Additionally, it has been reported that energy metabolites, such as lactate and ketone, can serve as fuel for oxidative metabolism in cancer cells. Genetic evidence has also indicated that enhanced pyruvate kinase (PKM1 or PKM2) expression in CAFs may support the growth of breast cancer cells [72]. Alterations in lipid metabolism in cancer cells have been found to promote associations of CAFs with cancer cells [19, 21, 70, 73]. CAF exposure may enhance lipid levels in cancer cells and metabolic synergy between CAFs and cancer cells, which may be mediated by fatty acid transporter protein 1 (FATP1) [73].
3.5 Role of small regulatory RNAs in CAF-mediated cancer development
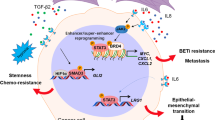
Several reports indicate that microRNAs (miRNAs) may modulate CAFs within the TME [39, 40, 74, 75]. Liu et al. [75] reported, for example, that miRNA-29b may play a role in interactions between cancer cells and CAFs and that miRNA-29b levels may be reduced in CAFs. Others found that downregulation of miRNA-200 in CAFs may play a role in ECM remodeling and, thereby, in promoting tumor cell invasion [74]. Another interesting report has suggested that high levels of initiator methionine tRNA in CAFs may promote tumor growth and angiogenesis [76]. Concise information on molecular signaling and potential therapeutic inhibitors specific for CAFs and the TME is depicted in Fig. 3.
Interactions between CAFs and cancer cells in the tumor niche and potential therapeutic inhibitors. Illustration of the putative role of cancer-associated fibroblasts (CAFs) in driving tumor growth, invasion, metastasis and immunosuppression by releasing cytokines (IL-6, IL-8, TNF), inflammatory factors, MMP(s) and growth factors (FGF, HGF and SDF) to increase proliferation. CAFs may also release signaling molecules, such as Chi3L1 and TGF-β1, which play an essential role in silencing pro-cancer immune cells. Recently reported therapeutic options to target CAF cancer cell communication are depicted
3.6 p53 and PTEN mutations in CAFs and their role in the TME
The tumor suppressor p53 is known to play a pivotal role as transcription factor in preventing tumorigenesis by activating apoptosis and senescence [13, 77, 78]. Another classical tumor suppressor, i.e., phosphatase and tensin homologue (PTEN), has also been found to be involved in the regulation of cellular proliferation [13, 79]. Dysfunction of p53 (due to mutation) has been reported to be associated with various hallmarks of cancer and with adaptations of the TME [77,78,79]. Although p53 mutations in cancer cells and their role in carcinogenesis are well known, p53 alterations and defects in CAFs have only recently gained interest. A recent report highlights, for example, the importance of simultaneous loss of CBF1/Suppressor of Hairless/Lag1 (CSL) and p53 activity in CAFs to support cancer cell expansion in a keratinocyte-derived tumor model [80]. Dauer et al. [81] also suggested that functional deficiency of p53 in human pancreatic cancer cells may promote angiogenesis mediated by CAFs within the TME. These authors found that a novel drug, minnelide, could attenuate CAF activity and, in turn, diminish the progression potential of KRAS/mut p53-deficient pancreatic cancer cells. Another recent study revealed crosstalk between CAFs and tumor epithelial cells derived from KRAS/mut p53-deficient colon cancer cells [82]. Yet another study supported the interplay between p53-mediated activities in cancer cells and CAFs within the tumor niche, including their response to cisplatin treatment [83].
To emphasize the importance of PTEN in the TME, Liao et al. [84] reported on the role of CAFs in enhancing the potential of prostate cancer stem cells in a conditional PTEN deletion prostate cancer mouse model. Additionally, Trimboli et al. [85] found that genetic loss of PTEN in CAFs of mouse mammary glands can enhance the development of mammary epithelial tumors by increasing the activity of Ets2 transcription factors. Recent findings have also indicated that PTEN deficiency in CAFs may play a role in carcinogenesis involving the JAGGED-1 axis within the NOTCH signaling pathway [86]. It was found that this signaling axis may promote the proliferation of mammary epithelial stem cells and, consequently, support tumor progression. Taken together, these data indicate that impairment of p53 and PTEN may mediate responses in CAFs that support a pro-growth and survival TME. As such, they may provide clues to the development of novel therapeutic approaches aimed at restoring the anti-cancer cellular signaling axes mediated by p53 and PTEN.
4 Adipocytes and their crosstalk with cancer cells
Adipocytes represent another component of the TME, and they are known as cancer-associated adipocytes (CAAs) [87,88,89,90,91]. Growing evidence indicates that these CAAs may secrete several key signaling mediators, such as hormones, growth factors, cytokines and adipokines, and that these mediators can establish crosstalk between cancer cells and stromal cells [87,88,89,90]. Recently, CAAs have been associated with the induction of particular cancer characteristics, such as EMT and drug resistance [87,88,89,90,91,92,93]. It has also been reported that adipocyte-derived fibroblasts may secrete fibronectin and collagen I and, by doing so, increase the level of the CAF marker FSP-1 [88]. As an example of the role of CAAs in ECM remodeling, Lee et al. [91] reported that CAAs may be associated with elevated levels of matrix metallopeptidase (MMP)-9 and TWIST1, which may promote breast cancer cell migration and invasion. Huang et al. [92] reported that associations between adipocytes and cancer cells may be driven by β-hydroxybutyrate secreted by primary mammary gland-derived adipocytes (MGDAs). Jia et al. [93] found that adiponectin, a hormone secreted by adipocytes, can induce the migration of breast carcinoma cells. Additional evidence suggests that adipocytes can produce adipokines and energy to support cancer development and metabolic heterogeneity, whereas lipids and other secreted factors, such as endotrophin, may sustain cancer growth and invasion [87, 89]. It has also been reported that within the breast TME, adipocytes may affect gene expression via the regulation of hypoxia and EMT through an increased expression of hypoxia-inducible factor 1-alpha (HIF1α), TGF-β1, lectin-type oxidized LDL receptor 1 (LOX1) [90], forkhead box protein C2 (FOXC2) and TWIST1 [94]. Wang et al. [95] have reported that several components are secreted by adipocytes to induce up-regulation of MMP-2 within the TME and, additionally, it has been found that elevated MMP-2 levels in CAFs may enhance the expression of human epidermal growth factor receptor 2 (HER2) in invasive breast carcinomas [96]. D’Esposito et al. [97] found that insulin-like growth factor-1 (IGF1) released from adipocyte-derived differentiating cells may be involved in the modulation of breast cancer growth and progression. Bochet et al. [98] reported that adipocytes may be involved in modulating breast cancer characteristics to thwart radio-resistance via increasing checkpoint kinase 1 (CHEK1) expression levels. Through an in vitro co-culture study it was found that cytokines, such as IL-6 and monocyte chemotactic protein-1 (MCP-1), may facilitate the crosstalk between adipocytes and breast cancer cells [99,100,101,102]. D’Esposito et al. [100] reported that CC-chemokine ligand 5 (CCL5) secreted by adipocytes may contribute to invasion and metastasis in triple-negative breast cancer cells. It has also been found that trastuzumab-treated HER2 expressing breast cancer cells may acquire drug resistance through crosstalk with adipocytes [101]. In addition to breast cancer, recent work has shown that adipocyte differentiation may result in blocking STAT3 activity, which affects the invasiveness and metastasis of melanoma cells [102]. So, currently several studies have highlighted molecular and cellular aspects of adipocyte-guided TME development. This knowledge may be employed for the design of novel therapeutic options (Fig. 4).
Behavior of adipocytes in the TME and potential therapeutic inhibitors. Schematic illustration of the role of cancer-associated adipocytes (CAAs) in cancer growth and progression. These CAAs release IL-6, which induces pro-survival signaling pathways, such as JAK2/STAT3 signaling, in cancer cells. CAAs also release adipokines, which subsequently stimulate the growth and metastatic ability of tumor cells. In addition, CAAs release growth factors, such as hepatocyte growth factor (HGF), which leads to increased proliferation, invasion and drug resistance. Recently defined therapeutic inhibitors, such as celastrol and miRNA-135a-5p, that can inhibit crosstalk between CAAs and cancer cells, are depicted
5 Pericytes and their modulatory roles
Pericytes are multipotent perivascular cells that have been found to play a role in promoting tumor vasculature development [27, 103, 104]. Within the TME pericytes have also been found to play a role in the transmigration of myeloid-derived suppressor cells, which are immature myeloid cells that exhibit antagonistic effects against the antitumor activities of T cells [27, 103, 104]. Based on their results, Hong et al. [105] suggested the existence of paracrine signaling between pericytes and inflammatory cells, leading to a pro-cancer hypoxic TME in breast cancer. In addition, it has been reported that pericyte-mediated promotion of angiogenesis and vessel maturation in tumors may be mediated by the pericyte surface receptor tyrosine kinase with Ig and EGF homology domains-2 (TIE2) and its downstream targets, including calpain, protein kinase B (PKB) and FOXO3 [106, 107]. Reynolds et al. [108] reported a prominent role of α6β1-integrin in the modulation of PDGFRβ and PKB-mTOR signaling in cancer. This integrin is a major laminin receptor expressed on pericytes. Additional evidence from Hosaka et al. [104] has indicated that pericyte-fibroblast transition can be induced by secreted PDGF-BB, which may subsequently augment cancer invasion and metastasis. In addition to breast tumors, pericytes have been found to contribute to the melanoma TME by promoting EMT and invasion via the secretion of TGF-β1 signaling molecules [106]. In a preclinical study, Sinha et al. [109] observed a potential role of pericytes in the promotion of ovarian cancer in mice, and they suggested that these cells may be used as prognostic markers for the occurrence of relapse. So, emerging data indicate that pericytes within the TME may play a role in tumor progression, angiogenesis and metastasis.
6 Role of mesenchymal stem cells in the TME
One category of adult multipotent stem cells is denoted as mesenchymal stromal cells (MSCs) [12, 110, 111]. These cells are found in various tissues and organs and are thought to give rise to specialized cells to assist wound healing and tissue repair [110, 112,113,114]. Watts et al. [115] found that the recruitment of MSCs in the head and neck squamous cell carcinoma TME is driven by the secretion of PDGF-AA by the tumor cells. To establish the role of secreted factors within the TME, it has been found that the ability of umbilical cord-derived MSCs (UC-MSCs) to orchestrate breast tumor-promoting signaling pathways is driven by IL-6 and IL-8 [116]. McAndrews et al. [113] emphasized the importance of MSCs in the directional migration of invasive breast cancer cells, which was found to be guided by MSC-secreted TGF-β1. Concordantly, also Yu et al. [117] reported the existence of bidirectional paracrine signaling between MSCs and cancer cells and that this signaling may potentially be mediated by secreted TGF-β1 and reduced CXCL12 expression levels. Leyh et al. [111] found that MSCs and CAFs may contribute to resistance against the anti-estrogen drug fulvestrant through the insulin-like growth factor binding protein 5/B-cell leukemia/lymphoma 3 (Bcl-3) pathway in ERα-positive breast carcinomas. In addition to the role of MSCs, it has been found that bone marrow mesenchymal stem/stromal cells (BM-MSCs) derived from acute myeloid leukemia (AML) patients can protect AML cells from genotoxic threats [110, 112]. Specifically, the authors found that AML-derived BM-MSCs can be immunosuppressive and anti-inflammatory, and express low levels of pro-inflammatory cytokines. In summary, these reports indicate that MSCs have the potential to promote cancer development, metastasis and drug resistance. Inhibitors that can prevent paracrine interactions between MSCs and cancer cells may have therapeutic potential.
7 Changing roles of endothelial cells from gatekeepers to tumor promoters
Accumulating evidence indicates that organ-specific endothelial cells may play a role in tissue homeostasis, cancer angiogenesis and metastasis, as well as in metabolic and other pathological adaptations [11, 118,119,120,121]. As an example of functional crosstalk between endothelial cells and cancer cells, Wieland et al. [121] found that NOTCH1 expressed on endothelial cells may facilitate ovarian and melanoma cancer cell progression and metastasis through activation of the intracellular domain of the NOTCH1 receptor. In addition to this NOTCH signaling pathway crosstalk, it has been found that the application of vascular endothelial growth factor (VEGF) inhibiting drugs in glioblastoma multiforme (GBM) may lead to increased expression of angiopoietin-2 in endothelial cells [119]. Others have reported a role of NOTCH3 signaling in promoting juxtacrine interactions between melanoma cells and endothelial cells to create growth-promoting tumor niches [120]. Crosstalk between endothelial cells and cancer cells may also be facilitated by the action of prolactin on endothelial cells, which may promote pro-vascular tumor heterogeneity [122]. Ghiabi et al. [123] additionally found that NOTCH signaling may induce mesenchymal phenotypes in endothelial cells, thereby forming a favorable TME. They also noted that NOTCH and TGF-β1 signaling pathways may play a role in maintaining the mesenchymal phenotype, and that these pathways may serve as therapeutic targets in breast cancer. Recently, it was found that miRNA-103 may play a role in the control over the pro-tumor function of endothelial cells via a reduced secretion of pro-inflammatory cytokines in the TME [124]. Among the various types of stromal cells, endothelial cells have received specific attention regarding their role in tumor angiogenesis and metastasis. Currently, promising drugs and inhibitors are being developed to debilitate the intricacies between endothelial cells and cancer cells.
8 Microenvironment modulation in pre-malignancies
Carcinogenesis is a continuous process in which local microenvironments continually evolve from normal tissue to pre-malignant tissue to cancer tissue. In particular, the changes that occur in the pre-malignant microenvironment may be exploited for cancer prevention. The best experimental models for such efforts are oral potentially malignant disorders (OPMDs) that exhibit significant changes in both cellular and non-cellular components of the microenvironment [125,126,127]. First, it has been found that CAFs are present in abnormally high numbers in OPMDs, and these levels increase as the disease progresses from OPMD to oral squamous cell carcinoma (OSCC) [125, 126]. In addition, it has been found that cases with oral submucous fibrosis, which exhibits the highest malignant transformation rate among all OPMDs, have the highest numbers of (CAF) myofibroblasts. Second, it has been found that MSCs may display an imbalance between regenerative and metabolic self-regulatory functions in OPMD. During malignant progression of oral leukoplakia (OLK), collagen IV (Col IV) expression was found to be decreased and MMP-9 expression was found to be increased in MSCs [127, 128]. In addition, it was found that the Col IV continuity was destroyed and that the number of MMP-9 positive cells increased in the zones adjacent to fragmented basement membranes in epithelial dysplasia and cancer [129, 130]. Therefore, MSC impairment may be critical to the destruction of basement membranes in the mucosa of OPMD and OSCC patients. Third, it has been found that IL-1 and histamine secretion by mast cells may aggravate the progression from OLK to OSCC. In addition, it has been found that the number of MSCs may increase during the development from normal tissue to OLK with high-grade dysplasia, and that this process may be associated with increased angiogenesis [131, 132]. A high expression of FGF-2 and its receptors, FGFR-2 and FGFR-3, in the microenvironment of OPMD has been found to be associated with progression to OSCC [133]. It has also been found that a high expression of the ECM glycoproteins tenascins and MMP-2 may predict the malignant potential of tobacco-associated OLK [134]. Finally, proteomics has revealed that distinct extracellular cues may be derived from distinct cells within the TME [135] and that these extracellular cues (i.e., matrisome) may provide new opportunities to prevent OPMD from acquiring malignant characteristics.
9 Avenues to target pro-tumor stromal cells
As outlined above, communication between stromal cells and cancer cells is implicated in tumor development, invasion, drug resistance and relapse [5,6,7, 10,11,12, 136]. Various reports have suggested that inhibition of CAFs within TMEs may serve as a promising avenue towards cancer therapy [5,6,7, 137,138,139,140,141,142,143,144,145,146,147,148,149,150,151]. Concordantly, several approaches, including the use of nano-carrier delivery systems, synthetic miRNAs, small molecule inhibitors and monoclonal antibodies, are currently being used to combat tumor cells and associated stromal cells [25,26,27,28,29,30,31,32,33,34,35,36,37, 137,138,139]. In addition, scaffold- and 3D-based matrix drug delivery systems are being developed. These drug delivery systems are generated from natural and artificial sources to deliver drugs to target stromal cells and, by doing so, to reprogram the TME [137,138,139]. Also, nano-modification of peptide drugs and their derivatives may serve as an approach to target the TME given the selectivity, efficiency, amphoteric nature and activity of these agents towards several biological processes, such as blood vessel formation and immune reactions. In addition, it has been found that these drugs may easily pass through the plasma membrane and act as signaling molecules in various cellular pathways [138]. Nanoparticle-based therapeutic approaches to disrupt the TME have also been suggested to serve as a suitable option to overcome drug resistance. Given their highly selective nature for targeting particular cellular and non-cellular components within the TME, these agents may represent effective treatment options [139].
Along the same line, cell-cell communication between stromal cells and cancer cells has been found to induce proliferative and survival signaling pathways [23, 25]. In a mammary tumor model, for example, Valenti et al. [140] found that the Wnt/β-catenin and Hedgehog signaling pathways in CAFs may play a role. Others have found that dovitinib can block the PI3K/PKB/mTOR signaling pathway in CAFs [141]. Through a bidirectional response, it has been found that CAFs can affect breast cancer stem cell (BCSC) self-renewal by secreting signaling factors. Based on their results, the authors suggested that the smoothened (Smo) inhibitor vismodegib may impair the expansion of both CAFs and BCSCs [142, 143]. Du et al. [143] found that curcumin can block pro-cancer paracrine signaling between CAFs and cancer cells via disruption of the MAO-A/mTOR/HIF-1α signaling pathway. Another report has described the therapeutic inhibition of CAFs via cathelicidins, which represent a group of endogenous antimicrobial and anti-inflammatory peptides, such as LL-37 in humans and mCRAMP in mice. In a similar report, Li et al. [144] noted a possible role of the aromatase inhibitor letrozole in inhibiting signaling responses by preventing the secretion of cytokines, such as CCL2, CCL5 and CXCL1, from CAFs. Brennen et al. [69] reported on the potential of targeting CAFs with a fibroblast activation protein-activated prodrug, i.e., post-prolyl endopeptidase, to deliver cytotoxic prodrugs to the TME. Through a combinatorial therapy, Fabian et al. [145] found that specific vaccines can block tumor pericyte-associated antigens, such as the NOTCH antagonist delta-like homolog 1 (DLK1) and its homologue DLK2, in a range of vascularized cancers. This group also advocated the use of AMD3100 and imatinib to abolish MSC maturation and migration to treat cancer. A clinical efficacy of the anti-PDGFR agent imatinib has also been reported for luminal breast and colon cancers [52, 53]. A novel flavonoid, FLA-16, has been found to exhibit therapeutic effects on endothelial cells within the glioma TME by reducing the enzymatic activity of cytochrome P450 [146]. Another compound, GDC-0449, which inhibits sonic hedgehog (SHH) signaling, has been found to target CAF-mediated pro-tumor induction in pancreatic cancer cells [147]. More recently, it has been found that GDC-0449 inhibits the activity of NAD(P)H Oxidase-4 (NOX4) and, by doing so, disrupts the pro-tumor effect of CAFs in various tumor types [148]. Gabasa et al. [149] revealed an inhibitory effect of nintedanib, a FDA approved multi-kinase receptor inhibitor, in CAAs within non-small cell lung cancers (NSCLCs) with an adenocarcinoma (ADC) microenvironment. Within CAFs, an inhibitory role of trihydroxyphenolic compounds on the TGF-β1 receptor has been described and this inhibition may be employed for cancer therapy [150].
Another prominent example aimed at targeting pericytes has been reported by Chen et al. [151]. They found that activated fibroblast activation protein α vascular disrupting agents may reduce tumor drug resistance [151]. In addition, it has been found that small molecule inhibitors targeting anti-NOTCH1 or vascular cell adhesion molecule 1 (VECAM1) may hinder NOTCH-controlled metastasis [121]. Another preclinical study reported that the combined use of a CSF1R inhibitor and a CXCR2 antagonist can prevent the recruitment of granulocytes within tumors and that these inhibitors, by doing so, can prevent the activation of pro-cancer CAFs [9]. It has also been noted that SHH ligand secreted by breast cancer stem cells may regulate the function of the CAFs via paracrine signaling, and that an inhibitor of multiple tyrosine kinases may hinder CAF-mediated breast tumor invasion and reduce the expression and secretion of CCL2, CCL5 and VEGF by CAFs. Further evidence suggests that CAFs can modulate the TME via secretion of adrenomedullin (AM). This multifunctional peptide exhibits a modulatory role by binding to calcitonin receptor-like modifying protein-2 and -3 on cancer cells [37]. The authors demonstrated the clinical relevance of this peptide using an anti-AM antibody to inhibit crosstalk between CAFs and breast cancer cells.
10 Genetic ablation of CAFs as therapeutic option
Based on the crucial role of CAFs in the TME, therapeutic approaches aimed at ablating genes contributing to their pro-tumor activities have been developed [152–155]. Zhou et al. [152] noted anti-tumor effects of genetic ablation of β-catenin in melanoma-associated CAFs and that this ablation resulted in disruption of the MAPK/ERK signaling pathway and an arrest of the tumor cells in the S and G2/M phases of the cell cycle. Another approach was aimed at blocking paracrine Hedgehog signaling through genetic ablation of Smo in CAFs in a mouse model of pancreatic acinar-to-ductal metaplasia. It was found that ablation of the Smo gene within CAFs resulted in enhanced secretion of TGF-α, which in turn led to induction of EGFR signaling and promotion of pancreatic acinar-to-ductal metaplasia [153]. In support of genetic ablation approaches, Shukla et al. [154] found that genetic ablation of CLIC4, a key protein in TGF-β signaling, may block the pro-tumor activity of CAFs. An additional report by Martínez-Bosch et al. [155] showed the importance of genetic ablation of the galectin 1 (Gal-1) gene in CAFs in a mouse model of PDAC. They found that Gal-1 ablation hampered both proliferation and angiogenesis via the induction of Hedgehog pathway signaling in PDAC and CAF cells.
Taken together, ample reports have highlighted the importance of targeting stromal cells within the TME using various methods, drugs and inhibitors, ranging from small pharmacological inhibitors to monoclonal antibodies. Based on pre-clinical and clinical evaluations, however, there are still concerns regarding the suitability, precision and efficacy of such approaches. A summary of pre-clinical scopes and consequences pertaining the interplay between cancer-associated stromal cells and cancer cells is depicted in Fig. 5.
Scheme of pre-clinical therapeutic drugs/inhibitors that may disrupt communications between stromal cells and cancer cells. Robust and appreciable paracrine signaling within the TME is known to drive pro-cancer activities of stromal cells, including cancer-associated fibroblasts, cancer-associated adipocytes and mesenchymal stem cells. Different classes of drugs/inhibitors, including small molecule inhibitors antibodies, exosomal miRNAs, genetic ablation approaches and cytokine antagonists, are depicted
11 Conclusions and future prospects
Stromal cells within tumor niches are indispensable for inducing and sustaining cancer characteristics, such as proliferation, invasion, metastasis, angiogenesis and drug resistance. Therefore, translational research is warranted to conceive new and efficacious drugs or combinations of drugs to disrupt the communication between stromal cells and cancer cells. Currently, there is consensus that the recruitment of stromal cells, including CAFs, adipocytes, pericytes and vascular endothelial cells, to the TME may be prevented using combinatorial approaches. Conversely, the already existing pool of tumor-associated stromal cells may be deactivated using multiple-drugs/inhibitors in order to disrupt the pro-tumor niche supported by these stromal cells. Additional factors that may enhance pro-cancer activities of stromal cells may be related to cancer progression and the concomitant evolvement of heterogeneity within existing stromal cell populations. Therefore, efforts are being made to develop suitable stromal cell-specific biomarkers to monitor the transition of the TME from a pro-cancer to an anti-cancer state. Currently, several therapeutic options, including the use of small molecule inhibitors, peptide mimetics, exosomal miRNAs, epigenetic modulators, monoclonal antibodies, natural compounds and genetic ablation are being evaluated at various pre-clinical stages to test their efficacy and potential to disrupt the interplay between stromal cells and cancer cells. These therapeutic options aimed at targeting cancer-associated stromal cells are complemented by the design of nano-carriers, tissue scaffolds and 3-D-based matrices to precisely and safely deliver therapeutic compounds with minimal harm to healthy tissues. Due to these developments, cancer therapeutics centered on modulating stromal cells holds great promise. Also, certain bottlenecks need to be mentioned here, including targeted delivery, reliable efficacy at preclinical and clinical levels and the importance of addressing the issue of intra-tumor heterogeneity adaptation in cancer patients.
References
M. Plummer, C. de Martel, J. Vignat, J. Ferlay, F. Bray, S. Franceschi, Global burden of cancers attributable to infections in 2012: A synthetic analysis. Lancet Glob. Health 4, e609–e616 (2016)
J. Bishop, The molecular genetics of cancer. Science 235, 305–311 (1987)
M.M. Gottesman, Mechanisms of cancer drug resistance. Annu. Rev. Med. 53, 615–627 (2002)
A.A. Alizadeh, V. Aranda, A. Bardelli, C. Blanpain, C. Bock, C. Borowski, C. Caldas, A. Califano, M. Doherty, M. Elsner, M. Esteller, R. Fitzgerald, J.O. Korbel, P. Lichter, C.E. Mason, N. Navin, D. Peer, K. Polyak, C.W.M. Roberts, L. Siu, A. Snyder, H. Stower, C. Swanton, R.G.W. Verhaak, J.C. Zenklusen, J. Zuber, J. Zucman-Rossi, Toward understanding and exploiting tumor heterogeneity. Nat. Med. 21, 846–853 (2015)
J.W. Clark, B.A. Chabner, Limits to precision cancer medicine. N. Engl. J. Med. 376, 95–97 (2017)
L.A. Liotta, E.C. Kohn, The microenvironment of the tumour host interface. Nature 411, 375–379 (2001)
B.S. Wiseman, Stromal effects on mammary gland development and breast cancer. Science 296, 1046–1049 (2002)
J.W. Pollard, Tumour-educated macrophages promote tumour progression and metastasis. Nat. Rev. Cancer 4, 71–78 (2004)
V. Kumar, L. Donthireddy, D. Marvel, T. Condamine, F. Wang, S. Lavilla-Alonso, A. Hashimoto, P. Vonteddu, R. Behera, M.A. Goins, C. Mulligan, B. Nam, N. Hockstein, F. Denstman, S. Shakamuri, D.W. Speicher, A.T. Weeraratna, T. Chao, R.H. Vonderheide, L.R. Languino, P. Ordentlich, Q. Liu, X. Xu, A. Lo, E. Puré, C. Zhang, A. Loboda, M.A. Sepulveda, L.A. Snyder, D.I. Gabrilovich, Cancer-associated fibroblasts neutralize the anti-tumor effect of CSF1 receptor blockade by inducing PMN-MDSC infiltration of tumors. Cancer Cell 32 e655, 654–668 (2017)
Y. Qiao, C. Zhang, A. Li, D. Wang, Z. Luo, Y. Ping, B. Zhou, S. Liu, H. Li, D. Yue, Z. Zhang, X. Chen, Z. Shen, J. Lian, Y. Li, S. Wang, F. Li, L. Huang, L. Wang, B. Zhang, J. Yu, Z. Qin, Y. Zhang, IL6 derived from cancer-associated fibroblasts promotes chemoresistance via CXCR7 in esophageal squamous cell carcinoma. Oncogene 37, 873–883 (2017). https://doi.org/10.1038/onc.2017.387
H.G. Augustin, G.Y. Koh, Organotypic vasculature: From descriptive heterogeneity to functional pathophysiology. Science 357, eaal2379 (2017)
M. Spaw, S. Anant, S.M. Thomas, Stromal contributions to the carcinogenic process. Mol. Carcinog. 56, 1199–1213 (2017)
T. Shibue, R.A. Weinberg, EMT, CSCs, and drug resistance: The mechanistic link and clinical implications. Nat. Rev. Clin. Oncol. 14, 611–629 (2017)
M. Cheng, S. Ho, J.H. Yoo, D.H. Tran, K. Bakirtzi, B. Su, D.H. Tran, Y. Kubota, R. Ichikawa, H.W. Koon, Cathelicidin suppresses colon cancer development by inhibition of cancer associated fibroblasts. Clin. Exp. Gastroenterol. 8, 13–29 (2015)
V. Gkretsi, A. Stylianou, P. Papageorgis, C. Polydorou, T. Stylianopoulos, Remodeling components of the tumor microenvironment to enhance cancer therapy. Front. Oncol. 5, 214 (2015)
D. Jahagirdar, S. Purohit, A. Jain, N.K. Sharma, Export of microRNAs: A bridge between breast carcinoma and their neighboring cells. Front. Oncol. 6, 147 (2016)
M. Najar, H. Fayyad-Kazan, W.H. Faour, B. Badran, F. Journe, L. Lagneaux, Breast cancer cells and bone marrow mesenchymal stromal cells: A regulated modulation of the breast tumor in the context of immune response. Inflamm. Res. 66, 129–139 (2017)
P. Nilendu, A. Kumar, A. Kumar, J.K. Pal, N.K. Sharma, Breast cancer stem cells as last soldiers eluding therapeutic burn: A hard nut to crack. Int. J. Cancer 142, 7–17 (2017)
R. Kalluri, The biology and function of fibroblasts in cancer. Nat. Rev. Cancer 16, 582–598 (2016)
P.J. Morin, in Cancer Drug Resistance, ed. by B.A. Teicher (Humana Press, Totowa, NJ, 2006), pp. 201–210
A. Morandi, E. Giannoni, P. Chiarugi, Nutrient exploitation within the tumor–stroma metabolic crosstalk. Trends Cancer 2, 736–746 (2016)
K. Cyll, E. Ersvær, L. Vlatkovic, M. Pradhan, W. Kildal, M.A. Kjær, A. Kleppe, T.S. Hveem, B. Carlsen, S. Gill, S. Löffeler, E.S. Haug, H. Wæhre, P. Sooriakumaran, H.E. Danielsen, Tumour heterogeneity poses a significant challenge to cancer biomarker research. Br. J. Cancer 117, 367–375 (2017)
M. Majidinia, B. Yousefi, Breast tumor stroma: A driving force in the development of resistance to therapies. Chem. Biol. Drug Des. 89, 309–318 (2017)
N. McGranahan, C. Swanton, Clonal heterogeneity and tumor evolution: Past, present, and the future. Cell 168, 613–628 (2017)
N. Picco, E. Sahai, P.K. Maini, A.R.A. Anderson, Integrating models to quantify environment-mediated drug resistance. Cancer Res. 77, 5409–5418 (2017)
R.F. Schwabe, C. Jobin, The microbiome and cancer. Nat. Rev. Cancer 13, 800–812 (2013)
A.L. Ribeiro, O.K. Okamoto, Combined effects of pericytes in the tumor microenvironment. Stem Cells Int. 868475, 2015 (2015)
C.C. Maley, A. Aktipis, T.A. Graham, A. Sottoriva, A.M. Boddy, Classifying the evolutionary and ecological features of neoplasms. Nat. Rev. Cancer 17, 605–619 (2017)
H. Omar Al-Hassi, O. Ng, M. Brookes, Tumour-associated and non-tumour-associated microbiota in colorectal cancer. Gut 67, 395 (2018)
E. Perez-Chanona, G. Trinchieri, The role of microbiota in cancer therapy. Curr. Opin. Immunol. 39, 75–81 (2016)
Z. Benyahia, N. Dussault, M. Cayol, R. Sigaud, C. Berenguer-Daize, C. Delfino, A. Tounsi, S. Garcia, P.M. Martin, K. Mabrouk, L. Ouafik, Stromal fibroblasts present in breast carcinomas promote tumor growth and angiogenesis through adrenomedullin secretion. Oncotarget 8, 15744–15762 (2017)
L. Bolm, S. Cigolla, U.A. Wittel, U.T. Hopt, T. Keck, D. Rades, P. Bronsert, U.F. Wellner, The role of fibroblasts in pancreatic cancer: Extracellular matrix versus paracrine factors. Transl. Oncol. 10, 578–588 (2017)
N. Cohen, O. Shani, Y. Raz, Y. Sharon, D. Hoffman, L. Abramovitz, N. Erez, Fibroblasts drive an immunosuppressive and growth-promoting microenvironment in breast cancer via secretion of Chitinase 3-like 1. Oncogene 36, 4457–4468 (2017)
N.A. Bhowmick, E.G. Neilson, H.L. Moses, Stromal fibroblasts in cancer initiation and progression. Nature 432, 332–337 (2004)
A. Aboussekhra, Role of cancer-associated fibroblasts in breast cancer development and prognosis. Int. J. Dev. Biol. 55, 841–849 (2011)
U.M. Polanska, A. Orimo, Carcinoma-associated fibroblasts: Non-neoplastic tumour-promoting mesenchymal cells. J. Cell. Physiol. 228, 1651–1657 (2013)
H. Luo, G. Tu, Z. Liu, M. Liu, Cancer-associated fibroblasts: A multifaceted driver of breast cancer progression. Cancer Lett. 361, 155–163 (2015)
A. Orimo, R.A. Weinberg, Stromal fibroblasts in cancer: A novel tumor-promoting cell type. Cell Cycle 5, 1597–1601 (2006)
G.S. Markopoulos, E. Roupakia, M. Tokamani, E. Chavdoula, M. Hatziapostolou, C. Polytarchou, K.B. Marcu, A.G. Papavassiliou, R. Sandaltzopoulos, E. Kolettas, A step-by-step microRNA guide to cancer development and metastasis. Cell. Oncol. 40, 303–339 (2017)
P. Mishra, D. Banerjee, A. Ben-Baruch, Chemokines at the crossroads of tumor-fibroblast interactions that promote malignancy. J. Leukoc. Biol. 89, 31–39 (2011)
K.O. Osuala, M. Sameni, S. Shah, N. Aggarwal, M.L. Simonait, O.E. Franco, Y. Hong, S.W. Hayward, F. Behbod, R.R. Mattingly, B.F. Sloane, Il-6 signaling between ductal carcinoma in situ cells and carcinoma-associated fibroblasts mediates tumor cell growth and migration. BMC Cancer 15, 584 (2015)
Ö. Sağlam, Z.S. Ünal, C. Subaşı, E. Ulukaya, E. Karaöz, IL-6 originated from breast cancer tissue-derived mesenchymal stromal cells may contribute to carcinogenesis. Tumour Biol. 36, 5667–5677 (2015)
D. von Ahrens, T.D. Bhagat, D. Nagrath, A. Maitra, A. Verma, The role of stromal cancer-associated fibroblasts in pancreatic cancer. J. Hematol. Oncol. 10, 76 (2017)
S.-F. Hendrayani, H.H. Al-Khalaf, A. Aboussekhra, The cytokine IL-6 reactivates breast stromal fibroblasts through transcription factor STAT3-dependent up-regulation of the RNA-binding protein AUF1. J. Biol. Chem. 289, 30962–30976 (2014)
T. Ishimoto, K. Miyake, T. Nandi, M. Yashiro, N. Onishi, K.K. Huang, S.J. Lin, R. Kalpana, S.T. Tay, Y. Suzuki, B.C. Cho, D. Kuroda, K. Arima, D. Izumi, M. Iwatsuki, Y. Baba, E. Oki, M. Watanabe, H. Saya, K. Hirakawa, H. Baba, P. Tan, Activation of transforming growth factor beta 1 signaling in gastric cancer-associated fibroblasts increases their motility, via expression of rhomboid 5 homolog 2, and ability to induce invasiveness of gastric cancer cells. Gastroenterology 153, 191-204. e116 (2017), 204.e16
E. Sjöberg, M. Augsten, J. Bergh, K. Jirström, A. Östman, Expression of the chemokine CXCL14 in the tumour stroma is an independent marker of survival in breast cancer. Br. J. Cancer 114, 1117–1124 (2016)
M. Yao, E. Yu, V. Staggs, F. Fan, N. Cheng, Elevated expression of chemokine C-C ligand 2 in stroma is associated with recurrent basal-like breast cancers. Mod. Pathol. 29, 810–823 (2016)
L. Zhao, G. Ji, X. Le, Z. Luo, C. Wang, M. Feng, L. Xu, Y. Zhang, W.B. Lau, B. Lau, Y. Yang, L. Lei, H. Yang, Y. Xuan, Y. Chen, X. Deng, T. Yi, S. Yao, X. Zhao, Y. Wei, S. Zhou, An integrated analysis identifies STAT4 as a key regulator of ovarian cancer metastasis. Oncogene 36, 3384–3396 (2017)
N. Kramer, J. Schmöllerl, C. Unger, H. Nivarthi, A. Rudisch, D. Unterleuthner, M. Scherzer, A. Riedl, M. Artaker, I. Crncec, D. Lenhardt, T. Schwarz, B. Prieler, X. Han, M. Hengstschläger, J. Schüler, R. Eferl, R. Moriggl, W. Sommergruber, H. Dolznig, Autocrine WNT2 signaling in fibroblasts promotes colorectal cancer progression. Oncogene 36, 5460–5472 (2017)
A. Avgustinova, M. Iravani, D. Robertson, A. Fearns, Q. Gao, P. Klingbeil, A.M. Hanby, V. Speirs, E. Sahai, F. Calvo, C.M. Isacke, Tumour cell-derived Wnt7a recruits and activates fibroblasts to promote tumour aggressiveness. Nat. Commun. 7, 10305 (2016)
J.S.K. Chan, M.K. Sng, Z.Q. Teo, H.C. Chong, J.S. Twang, N.S. Tan, Targeting nuclear receptors in cancer-associated fibroblasts as concurrent therapy to inhibit development of chemoresistant tumors. Oncogene 37, 160–173 (2017)
M.P. Pinto, W.W. Dye, B.M. Jacobsen, K.B. Horwitz, Malignant stroma increases luminal breast cancer cell proliferation and angiogenesis through platelet-derived growth factor signaling. BMC Cancer 14, 735 (2014)
Y. Kitadai, T. Sasaki, T. Kuwai, T. Nakamura, C.D. Bucana, S.R. Hamilton, I.J. Fidler, Expression of activated platelet-derived growth factor receptor in stromal cells of human colon carcinomas is associated with metastatic potential. Int. J. Cancer 119, 2567–2574 (2006)
S. Neri, T. Miyashita, H. Hashimoto, Y. Suda, M. Ishibashi, H. Kii, H. Watanabe, T. Kuwata, M. Tsuboi, K. Goto, T. Menju, M. Sonobe, H. Date, A. Ochiai, G. Ishii, Fibroblast-led cancer cell invasion is activated by epithelial–mesenchymal transition through platelet-derived growth factor BB secretion of lung adenocarcinoma. Cancer Lett. 395, 20–30 (2017)
P.S.H. Soon, E. Kim, C.K. Pon, A.J. Gill, K. Moore, A.J. Spillane, D.E. Benn, R.C. Baxter, Breast cancer-associated fibroblasts induce epithelial-to-mesenchymal transition in breast cancer cells. Endocr. Relat. Cancer 20, 1–12 (2013)
A. Orimo, P.B. Gupta, D.C. Sgroi, F. Arenzana-Seisdedos, T. Delaunay, R. Naeem, V.J. Carey, A.L. Richardson, R.A. Weinberg, Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 121, 335–348 (2005)
N.L.E. Harris, C. Vennin, J.R.W. Conway, K.L. Vine, M. Pinese, M.J. Cowley, R.F. Shearer, M.C. Lucas, D. Herrmann, A.H. Allam, M. Pajic, J.P. Morton, A.V. Biankin, M. Ranson, P. Timpson, D.N. Saunders, SerpinB2 regulates stromal remodelling and local invasion in pancreatic cancer. Oncogene 36, 4288–4298 (2017)
N. Perurena, C. Zandueta, S. Martínez-Canarias, H. Moreno, S. Vicent, A.S. Almeida, E. Guruceaga, R.R. Gomis, M. Santisteban, M. Egeblad, EPCR promotes breast cancer progression by altering SPOCK1/testican 1-mediated 3D growth. J. Hematol. Oncol. 10, 23 (2017)
S. Busch, A. Acar, Y. Magnusson, P. Gregersson, L. Ryden, G. Landberg, TGF-beta receptor type-2 expression in cancer-associated fibroblasts regulates breast cancer cell growth and survival and is a prognostic marker in pre-menopausal breast cancer. Oncogene 34, 27–38 (2015)
A.M. Hammer, G.M. Sizemore, V.C. Shukla, A. Avendano, S.T. Sizemore, J.J. Chang, R.D. Kladney, M.C. Cuitiño, K.A. Thies, Q. Verfurth, A. Chakravarti, L.D. Yee, G. Leone, J.W. Song, S.N. Ghadiali, M.C. Ostrowski, Stromal PDGFR-α activation enhances matrix stiffness, impedes mammary ductal development, and accelerates tumor growth. Neoplasia 19, 496–508 (2017)
Y. Kinugasa, T. Matsui, N. Takakura, CD44 expressed on cancer-associated fibroblasts is a functional molecule supporting the stemness and drug resistance of malignant cancer cells in the tumor microenvironment. Stem Cells 32, 145–156 (2014)
B.Y. Owusu, S. Thomas, P. Venukadasula, Z. Han, J.W. Janetka, R.A. Galemmo Jr., L. Klampfer, Targeting the tumor-promoting microenvironment in MET-amplified NSCLC cells with a novel inhibitor of pro-HGF activation. Oncotarget 8, 63014–63025 (2017)
J. Paulsson, L. Rydén, C. Strell, O. Frings, N.P. Tobin, T. Fornander, J. Bergh, G. Landberg, O. Stål, A. Östman, High expression of stromal PDGFRβ is associated with reduced benefit of tamoxifen in breast cancer. J. Pathol. Clin. Res. 3, 38–43 (2016)
C.A.S. Corsa, A. Brenot, W.R. Grither, S. Van Hove, A.J. Loza, K. Zhang, S.M. Ponik, Y. Liu, D.G. DeNardo, K.W. Eliceiri, P.J. Keely, G.D. Longmore, The action of discoidin domain receptor 2 in basal tumor cells and stromal cancer-associated fibroblasts is critical for breast cancer metastasis. Cell Rep. 15, 2510–2523 (2016)
X. Li, W. Zhu, Z. Chen, L. Luo, J. Huang, F. Zhang, M. Li, Y. Guo, L. Guo, Fibroblast growth factor-inducible 14 regulates cell growth and multidrug resistance of small-cell lung cancer through the nuclear factor-κB pathway. Anti-Cancer Drugs 25, 1152–1164 (2014)
E.M. De Francesco, A.H. Sims, M. Maggiolini, F. Sotgia, M.P. Lisanti, R.B. Clarke, GPER mediates the angiocrine actions induced by IGF1 through the HIF-1alpha/VEGF pathway in the breast tumor microenvironment. Breast Cancer Res. 19, 129 (2017)
S.Y. Yeo, S.Y. Ha, K.W. Lee, Y. Cui, Z.T. Yang, Y.H. Xuan, S.H. Kim, Twist1 is highly expressed in cancer-associated fibroblasts of esophageal squamous cell carcinoma with a prognostic significance. Oncotarget 8, 65265–65280 (2017)
D.E. Kim, M.-G. Procopio, S. Ghosh, S.-H. Jo, S. Goruppi, F. Magliozzi, P. Bordignon, V. Neel, P. Angelino, G.P. Dotto, Convergent roles of ATF3 and CSL in chromatin control of cancer-associated fibroblast activation. J. Exp. Med. 214, 2349–2368 (2017)
W.N. Brennen, D.M. Rosen, H. Wang, J.T. Isaacs, S.R. Denmeade, Targeting carcinoma-associated fibroblasts within the tumor stroma with a fibroblast activation protein-activated prodrug. J. Natl. Cancer Inst. 104, 1320–1334 (2012)
U.E. Martinez-Outschoorn, M.P. Lisanti, F. Sotgia, Catabolic cancer-associated fibroblasts transfer energy and biomass to anabolic cancer cells, fueling tumor growth. Semin. Cancer Biol. 25, 47–60 (2014)
B.B. Patel, E. Ackerstaff, I.S. Serganova, J.E. Kerrigan, R.G. Blasberg, J.A. Koutcher, D. Banerjee, Tumor stroma interaction is mediated by monocarboxylate metabolism. Exp. Cell Res. 352, 20–33 (2017)
B. Chiavarina, D. Whitaker-Menezes, U.E. Martinez-Outschoorn, A.K. Witkiewicz, R. Birbe, A. Howell, R.G. Pestell, J. Smith, R. Daniel, F. Sotgia, M.P. Lisanti, Pyruvate kinase expression (PKM1 and PKM2) in cancer-associated fibroblasts drives stromal nutrient production and tumor growth. Cancer Biol. Ther. 12, 1101–1113 (2011)
F. Lopes-Coelho, S. Andre, A. Felix, J. Serpa, Breast cancer metabolic cross-talk: Fibroblasts are hubs and breast cancer cells are gatherers of lipids. Mol. Cell. Endocrinol. 462, 93–106 (2018)
X. Tang, Y. Hou, G. Yang, X. Wang, S. Tang, Y.E. Du, L. Yang, T. Yu, H. Zhang, M. Zhou, S. Wen, L. Xu, M. Liu, Stromal miR-200s contribute to breast cancer cell invasion through CAF activation and ECM remodeling. Cell Death Differ. 23, 132–145 (2016)
Y. Liu, J. Zhang, X. Sun, Q. Su, C. You, Down-regulation of miR-29b in carcinoma associated fibroblasts promotes cell growth and metastasis of breast cancer. Oncotarget 8, 39559–39570 (2017)
C.J. Clarke, T.J. Berg, J. Birch, D. Ennis, L. Mitchell, C. Cloix, A. Campbell, D. Sumpton, C. Nixon, K. Campbell, V.L. Bridgeman, P.B. Vermeulen, S. Foo, E. Kostaras, J.L. Jones, L. Haywood, E. Pulleine, H. Yin, D. Strathdee, O. Sansom, K. Blyth, I. McNeish, S. Zanivan, A.R. Reynolds, J.C. Norman, The initiator methionine tRNA drives secretion of type II collagen from stromal fibroblasts to promote tumor growth and angiogenesis. Curr. Biol. 26, 755–765 (2016)
K.H. Vousden, Lane D.P. p53 in health and disease. Nat. Rev. 8, 275–283 (2007)
A.J. Levine, p53, the cellular gatekeeper for growth and division. Cell 88, 323–331 (1997)
M.S. Song, L. Salmena, P.P. Pandolfi, The functions and regulation of the PTEN tumour suppressor. Nat. Rev. Mol. Cell Biol. 13, 283–296 (2012)
M.G. Procopio, C. Laszlo, D. Al Labban, D.E. Kim, P. Bordignon, S.H. Jo, S. Goruppi, E. Menietti, Combined CSL and p53 downregulation promotes cancer-associated fibroblast activation. Nat. Cell Biol. 17, 1193–1204 (2015)
P. Dauer, X. Zhao, V.K. Gupta, N. Sharma, K. Kesh, P. Gnamlin, Inactivation of Cancer-associated-fibroblasts disrupts oncogenic signaling in pancreatic Cancer cells and promotes its regression. Cancer Res. 78, 1321–1333 (2018)
Y. Hayashi, M. Tsujii, T. Kodama, T. Akasaka, J. Kondo, H. Hikita, T. Inoue, p53 functional deficiency in human colon cancer cells promotes fibroblast-mediated angiogenesis and tumor growth. Carcinogenesis 37, 972–984 (2016)
J.O. Schmid, M. Dong, S. Haubeiss, G. Friedel, S. Bode, A. Grabner, G. Ott, T.E. Mürdter, Cancer cells cue the p53 response of cancer-associated fibroblasts to cisplatin. Cancer Res. 72, 5824–5832 (2012)
C.P. Liao, H. Adisetiyo, M. Liang, P. Roy-Burman, Cancer-associated fibroblasts enhance the gland-forming capability of prostate cancer stem cells. Cancer Res. 70, 7294–7303 (2010)
A.J. Trimboli, C.Z. Cantemir-Stone, F. Li, J.A. Wallace, A. Merchant, N. Creasap, Pten in stromal fibroblasts suppresses mammary epithelial tumors. Nature 461, 1084–1091 (2009)
G.M. Sizemore, H.A.M. Balakrishnan, K.A. Thies, A.J. Trimboli, J.A. Wallace, Stromal PTEN inhibits the expansion of mammary epithelial stem cells through Jagged-1. Oncogene 36, 2297–2308 (2017)
J. Park, P.E. Scherer, Adipocyte-derived endotrophin promotes malignant tumor progression. J. Clin. Invest. 122, 4243–4256 (2012)
L. Bochet, C. Lehuede, S. Dauvillier, Y.Y. Wang, B. Dirat, V. Laurent, C. Dray, R. Guiet, I. Maridonneau-Parini, S. Le Gonidec, B. Couderc, G. Escourrou, P. Valet, C. Muller, Adipocyte-derived fibroblasts promote tumor progression and contribute to the desmoplastic reaction in breast cancer. Cancer Res. 73, 5657–5668 (2013)
K.M. Nieman, I.L. Romero, B. Van Houten, E. Lengyel, Adipose tissue and adipocytes support tumorigenesis and metastasis. Biochim. Biophys. Acta 1831, 1533–1541 (2013)
J. Zhang, L. Zhang, C. Li, C. Yang, L. Li, S. Song, H. Wu, F. Liu, L. Wang, J. Gu, LOX-1 is a poor prognostic indicator and induces epithelial-mesenchymal transition and metastasis in pancreatic cancer patients. Cell. Oncol. 41, 73–84 (2018)
Y. Lee, W.H. Jung, J.S. Koo, Adipocytes can induce epithelial-mesenchymal transition in breast cancer cells. Breast Cancer Res. Treat. 153, 323–335 (2015)
C.-K. Huang, P.-H. Chang, W.-H. Kuo, C.-L. Chen, Y.-M. Jeng, K.-J. Chang, J.-Y. Shew, C.-M. Hu, W.-H. Lee, Adipocytes promote malignant growth of breast tumours with monocarboxylate transporter 2 expression via β-hydroxybutyrate. Nat. Commun. 8, 14706 (2017)
Z. Jia, Y. Liu, S. Cui, Adiponectin induces breast cancer cell migration and growth factor expression. Cell Biochem. Biophys. 70, 1239–1245 (2014)
A. Yao-Borengasser, B. Monzavi-Karbassi, R.A. Hedges, L.J. Rogers, S.A. Kadlubar, T. Kieber-Emmons, Adipocyte hypoxia promotes epithelial-mesenchymal transition-related gene expression and estrogen receptor-negative phenotype in breast cancer cells. Oncol. Rep. 33, 2689–2694 (2015)
C. Wang, C. Gao, K. Meng, H. Qiao, Y. Wang, Human adipocytes stimulate invasion of breast cancer MCF-7 cells by secreting IGFBP-2. PLoS One 10, e0119348 (2015)
X. Catteau, P. Simon, J.-C. NoëL, Stromal expression of matrix metalloproteinase 2 in cancer-associated fibroblasts is strongly related to human epidermal growth factor receptor 2 status in invasive breast carcinoma. Mol. Clin. Oncol. 4, 375–378 (2016)
V. D’Esposito, F. Passaretti, A. Hammarstedt, D. Liguoro, D. Terracciano, G. Molea, L. Canta, C. Miele, U. Smith, F. Beguinot, P. Formisano, Adipocyte-released insulin-like growth factor-1 is regulated by glucose and fatty acids and controls breast cancer cell growth in vitro. Diabetologia 55, 2811–2822 (2012)
L. Bochet, A. Meulle, S. Imbert, B. Salles, P. Valet, C. Muller, Cancer-associated adipocytes promotes breast tumor radioresistance. Biochem. Biophys. Res. Commun. 411, 102–106 (2011)
K. Fujisaki, H. Fujimoto, T. Sangai, T. Nagashima, M. Sakakibara, N. Shiina, M. Kuroda, Y. Aoyagi, M. Miyazaki, Cancer-mediated adipose reversion promotes cancer cell migration via IL-6 and MCP-1. Breast Cancer Res. Treat. 150, 255–263 (2015)
V. D'Esposito, D. Liguoro, M.R. Ambrosio, F. Collina, M. Cantile, R. Spinelli, G.A. Raciti, C. Miele, R. Valentino, P. Campiglia, M. De Laurentiis, M. Di Bonito, G. Botti, R. Franco, F. Beguinot, P. Formisano, Adipose microenvironment promotes triple negative breast cancer cell invasiveness and dissemination by producing CCL5. Oncotarget 7, 24495–24509 (2016)
M.N. Duong, A. Cleret, E.L. Matera, K. Chettab, D. Mathe, S. Valsesia-Wittmann, B. Clemenceau, C. Dumontet, Adipose cells promote resistance of breast cancer cells to trastuzumab-mediated antibody-dependent cellular cytotoxicity. Breast Cancer Res. 17, 57 (2015)
D. Katoh, M. Nishizuka, S. Osada, M. Imagawa, Fad104, a positive regulator of adipocyte differentiation, suppresses invasion and metastasis of melanoma cells by inhibition of STAT3 activity. PLoS One 10, e0117197 (2015)
A.L. Ribeiro, C. Kaid, P.B.G. Silva, B.A. Cortez, O.K. Okamoto, Inhibition of lysyl oxidases impairs migration and angiogenic properties of tumor-associated pericytes. Stem Cells Int. 4972078, 2017 (2017)
K. Hosaka, Y. Yang, T. Seki, C. Fischer, O. Dubey, E. Fredlund, J. Hartman, P. Religa, H. Morikawa, Y. Ishii, M. Sasahara, O. Larsson, G. Cossu, R. Cao, S. Lim, Y. Cao, Pericyte–fibroblast transition promotes tumor growth and metastasis. Proc. Natl. Acad. Sci. U. S. A. 113, E5618–E5627 (2016)
J. Hong, N.P. Tobin, H. Rundqvist, T. Li, M. Lavergne, Y. García-Ibáñez, H. Qin, J. Paulsson, M. Zeitelhofer, M.Z. Adzemovic, I. Nilsson, P. Roswall, J. Hartman, R.S. Johnson, A. Östman, J. Bergh, M. Poljakovic, G. Genové, Role of tumor pericytes in the recruitment of myeloid-derived suppressor cells. J. Natl. Cancer Inst. 107, djv209 (2015)
J.H. Trevino-Villarreal, R. Sepulveda, D.A. Cotanche, R.A. Rogers, Effect of pericytes on epithelial-to-mesenchymal transition in melanoma. J. Clin. Oncol. 30, 84–84 (2012)
M. Teichert, L. Milde, A. Holm, L. Stanicek, N. Gengenbacher, S. Savant, T. Ruckdeschel, Z. Hasanov, K. Srivastava, J. Hu, S. Hertel, A. Bartol, K. Schlereth, H.G. Augustin, Pericyte-expressed Tie2 controls angiogenesis and vessel maturation. Nat. Commun. 8, 16106 (2017)
L.E. Reynolds, G. D'Amico, T. Lechertier, A. Papachristodoulou, J.M. Muñoz-Félix, A. De Arcangelis, M. Baker, B. Serrels, K.M. Hodivala-Dilke, Dual role of pericyte α6β1-integrin in tumour blood vessels. J. Cell Sci. 130, 1583–1595 (2017)
D. Sinha, L. Chong, J. George, H. Schlüter, S. Mönchgesang, S. Mills, J. Li, C. Parish, D. Bowtell, P. Kaur, Pericytes promote malignant ovarian cancer progression in mice and predict poor prognosis in serous ovarian cancer patients. Clin. Cancer Res. 22, 1813–1824 (2015)
A. Chavez-Gonzalez, B. Bakhshinejad, K. Pakravan, M.L. Guzman, S. Babashah, Novel strategies for targeting leukemia stem cells: Sounding the death knell for blood cancer. Cell. Oncol. 40, 1–20 (2017)
B. Leyh, A. Dittmer, T. Lange, J.W. Martens, J. Dittmer, Stromal cells promote anti-estrogen resistance of breast cancer cells through an insulin-like growth factor binding protein 5 (IGFBP5)/B-cell leukemia/lymphoma 3 (Bcl-3) axis. Oncotarget 6, 39307–39328 (2015)
R.D. Guardia, B. Lopez-Millan, J.R. Lavoie, C. Bueno, J. Castaño, M. Gómez-Casares, S. Vives, L. Palomo, M. Juan, J. Delgado, M.L. Blanco, J. Nomdedeu, A. Chaparro, J.L. Fuster, E. Anguita, M. Rosu-Myles, P. Menéndez, Detailed characterization of mesenchymal stem/stromal cells from a large cohort of AML patients demonstrates a definitive link to treatment outcomes. Stem Cell Reports 8, 1573–1586 (2017)
K.M. McAndrews, D.J. McGrail, N. Ravikumar, M.R. Dawson, Mesenchymal stem cells induce directional migration of invasive breast cancer cells through TGF-β. Sci. Rep. 5, 16941 (2015)
H.H. Wang, Y.L. Cui, N.G. Zaorsky, J. Lan, L. Deng, X.L. Zeng, Z.Q. Wu, Z. Tao, W.H. Guo, Q.X. Wang, L.J. Zhao, Z.Y. Yuan, Y. Lu, P. Wang, M.B. Meng, Mesenchymal stem cells generate pericytes to promote tumor recurrence via vasculogenesis after stereotactic body radiation therapy. Cancer Lett. 375, 349–359 (2016)
T.L. Watts, R. Cui, P. Szaniszlo, V.A. Resto, D.W. Powell, I.V. Pinchuk, PDGF-AA mediates mesenchymal stromal cell chemotaxis to the head and neck squamous cell carcinoma tumor microenvironment. J. Transl. Med. 14, 337 (2016)
F. Ma, D. Chen, F. Chen, Y. Chi, Z. Han, X. Feng, X. Li, Z. Han, Human umbilical cord mesenchymal stem cells promote breast cancer metastasis by interleukin-8- and interleukin-6-dependent induction of CD44+/CD24- cells. Cell Transplant. 24, 2585–2599 (2015)
P.F. Yu, Y. Huang, C.L. Xu, L.Y. Lin, Y.Y. Han, W.H. Sun, G.H. Hu, A.B. Rabson, Y. Wang, Y.F. Shi, Downregulation of CXCL12 in mesenchymal stromal cells by TGFβ promotes breast cancer metastasis. Oncogene 36, 840–849 (2017)
A.C. Dudley, Tumor endothelial cells. Cold Spring Harb Perspect Med 2, a006536 (2012)
A. Scholz, P.N. Harter, S. Cremer, B.H. Yalcin, S. Gurnik, M. Yamaji, M. Di Tacchio, K. Sommer, P. Baumgarten, O. Bahr, J.P. Steinbach, J. Trojan, M. Glas, U. Herrlinger, D. Krex, M. Meinhardt, A. Weyerbrock, M. Timmer, R. Goldbrunner, M. Deckert, C. Braun, J. Schittenhelm, J.T. Frueh, E. Ullrich, M. Mittelbronn, K.H. Plate, Y. Reiss, Endothelial cell-derived angiopoietin-2 is a therapeutic target in treatment-naive and bevacizumab-resistant glioblastoma. EMBO Mol. Med. 8, 39–57 (2016)
M.-Y. Hsu, M.H. Yang, C.I. Schnegg, S. Hwang, B. Ryu, R.M. Alani, Notch3 signaling-mediated melanoma–endothelial crosstalk regulates melanoma stem-like cell homeostasis and niche morphogenesis. Lab. Invest. 97, 725–736 (2017)
E. Wieland, J. Rodriguez-Vita, S.S. Liebler, C. Mogler, I. Moll, S.E. Herberich, E. Espinet, E. Herpel, A. Menuchin, J. Chang-Claude, M. Hoffmeister, C. Gebhardt, H. Brenner, A. Trumpp, C.W. Siebel, M. Hecker, J. Utikal, D. Sprinzak, A. Fischer, Endothelial Notch1 activity facilitates metastasis. Cancer Cell 31, 355–367 (2017)
B. Balinisteanu, A.M. Cimpean, E. Melnic, M. Coculescu, R.A. Ceausu, M. Raica, Crosstalk between tumor blood vessels heterogeneity and hormonal profile of pituitary adenomas: Evidence and controversies. Anticancer Res. 34, 5413–5420 (2014)
P. Ghiabi, J. Jiang, J. Pasquier, M. Maleki, N. Abu-Kaoud, N. Halabi, B.S. Guerrouahen, S. Rafii, A. Rafii, Breast cancer cells promote a notch-dependent mesenchymal phenotype in endothelial cells participating to a pro-tumoral niche. J. Transl. Med. 13, 27 (2015)
R. Wilson, C. Espinosa-Diez, N. Kanner, N. Chatterjee, R. Ruhl, C. Hipfinger, S.J. Advani, J. Li, O.F. Khan, A. Franovic, S.M. Weis, S. Kumar, L.M. Coussens, D.G. Anderson, C.C. Chen, D.A. Cheresh, S. Anand, MicroRNA regulation of endothelial TREX1 reprograms the tumour microenvironment. Nat. Commun. 7, 13597 (2016)
K. Gupta, R. Metgud, J. Gupta, Evaluation of stromal myofibroblasts in oral leukoplakia, oral submucous fibrosis, and oral squamous cell carcinoma - an immunohistochemical study. J. Cancer Res. Ther. 11, 893–898 (2015)
M. Chaudhary, A.R. Gadbail, G. Vidhale, M.P. Mankar, S.M. Gondivkar, M. Gawande, S. Patil, Comparison of myofibroblasts expression in oral squamous cell carcinoma, verrucous carcinoma, high risk epithelial dysplasia, low risk epithelial dysplasia and normal oral mucosa. Head Neck Pathol. 6, 305–313 (2012)
M. Mehdipour, M. Shahidi, S. Manifar, S. Jafari, F. Mashhadi Abbas, M. Barati, H. Mortazavi, M. Shirkhoda, A. Farzanegan, Z. Elmi Rankohi, Diagnostic and prognostic relevance of salivary microRNA-21, −125a, −31 and -200a levels in patients with oral lichen planus - a short report. Cell. Oncol. 41, 329–334 (2018)
R. Tamamura, H. Nagatsuka, C.H. Siar, N. Katase, I. Naito, Y. Sado, N. Nagai, Comparative analysis of basal lamina type IV collagen α chains, matrix metalloproteinases-2 and -9 expressions in oral dysplasia and invasive carcinoma. Acta Histochem. 115, 113–119 (2013)
H.-X. Fan, H.-X. Li, D. Chen, Z.-X. Gao, J.-H. Zheng, Changes in the expression of MMP2, MMP9, and ColIV in stromal cells in oral squamous tongue cell carcinoma: Relationships and prognostic implications. J. Exp. Clin. Cancer Res. 31, 90 (2012)
P. Le Bars, P. Piloquet, A. Daniel, B. Giumelli, Immunohistochemical localization of type IV collagen and laminin (alpha1) in denture stomatitis. J. Oral Pathol. Med. 30, 98–103 (2001)
F.B. Galateau-Salle, R.E. Luna, K. Horiba, M.N. Sheppard, T. Hayashi, M.V. Fleming, T.V. Colby, W. Bennett, C.C. Harris, W.G. Stetler-Stevenson, L. Liotta, V.J. Ferrans, W.D. Travis, Matrix metalloproteinases and tissue inhibitors of metalloproteinases in bronchial squamous preinvasive lesions. Hum. Pathol. 31, 296–305 (2000)
M. Sathyakumar, G. Sriram, T.R. Saraswathi, B. Sivapathasundharam, Immunohistochemical evaluation of mast cells and vascular endothelial proliferation in oral precancerous lesion-leukoplakia. J. Oral Maxillofac. Pathol. 16, 343–348 (2012)
S. Ramsridhar, M. Narasimhan, Immunohistochemical evaluation of mast cells in leukoplakia and oral squamous cell carcinoma. J. Clin. Diagn. Res. 10, ZC100–ZC103 (2016)
M. Kinra, K. Ramalingam, A. Sarkar, F. Rehman, K.L. Girish, Comparison of mast cell count and mast cell density in normal mucosa, oral leukoplakia, oral lichen planus, oral submucous fibrosis and oral squamous cell carcinoma–a study on 50cases. JPSI 1, 4–11 (2012)
S. Nayak, M.M. Goel, A. Makker, V. Bhatia, S. Chandra, S. Kumar, S.P. Agarwal, Fibroblast growth factor (FGF-2) and its receptors FGFR-2 and FGFR-3 may be putative biomarkers of malignant transformation of potentially malignant oral lesions into oral squamous cell carcinoma. PLoS One 10, e0138801 (2015)
P.A. Kenny, M.J. Bissell, Tumor reversion: Correction of malignant behavior by microenvironmental cues. Int. J. Cancer 107, 688–695 (2003)
S.P. Kerkar, N.P. Restifo, Cellular constituents of immune escape within the tumor microenvironment. Cancer Res. 72, 3125–3130 (2012)
H. Qin, C. Zhao, Y. Sun, J. Ren, X. Qu, Metallo-supramolecular complexes enantioselectively eradicate cancer stem cells in vivo. J. Am. Chem. Soc. 139, 16201–16209 (2017)
V. Pautu, D. Leonetti, E. Lepeltier, N. Clere, C. Passirani, Nanomedicine as a potent strategy in melanoma tumor microenvironment. Pharmacol. Res. 126, 31–53 (2017)
G. Valenti, H.M. Quinn, G.J.J.E. Heynen, L. Lan, J.D. Holland, R. Vogel, A. Wulf-Goldenberg, W. Birchmeier, Cancer stem cells regulate cancer-associated fibroblasts via activation of hedgehog signaling in mammary gland tumors. Cancer Res. 77, 2134–2147 (2017)
C. Zang, J. Eucker, P. Habbel, C. Neumann, C.-O. Schulz, N. Bangemann, L. Kissner, H. Riess, H. Liu, Targeting multiple tyrosine kinase receptors with Dovitinib blocks invasion and the interaction between tumor cells and cancer-associated fibroblasts in breast cancer. Cell Cycle 14, 1291–1299 (2015)
F. Mpekris, P. Papageorgis, C. Polydorou, C. Voutouri, M. Kalli, A.P. Pirentis, T. Stylianopoulos, Sonic-hedgehog pathway inhibition normalizes desmoplastic tumor microenvironment to improve chemo- and nanotherapy. J. Control. Release 261, 105–112 (2017)
Y. Du, Q. Long, L.I.N. Zhang, Y. Shi, X. Liu, X. Li, B.I.N. Guan, Y. Tian, X. Wang, L.E.I. Li, D. He, Curcumin inhibits cancer-associated fibroblast-driven prostate cancer invasion through MAOA/mTOR/HIF-1α signaling. Int. J. Oncol. 47, 2064–2072 (2015)
K. Li, H. Kang, Y. Wang, T. Hai, G. Rong, H. Sun, Letrozole-induced functional changes in carcinoma-associated fibroblasts and their influence on breast cancer cell biology. Med. Oncol. 33, 64 (2016)
K.P.L. Fabian, N. Chi-Sabins, J.L. Taylor, R. Fecek, A. Weinstein, W.J. Storkus, Therapeutic efficacy of combined vaccination against tumor pericyte-associated antigens DLK1 and DLK2 in mice. Oncoimmunology 6, e1290035 (2017)
C. Wang, Y. Li, H. Chen, J. Zhang, J. Zhang, T. Qin, C. Duan, X. Chen, Y. Liu, X. Zhou, J. Yang, Inhibition of CYP4A by a novel flavonoid FLA-16 prolongs survival and normalizes tumor vasculature in glioma. Cancer Lett. 402, 131–141 (2017)
Q. Zhou, Y. Zhou, X. Liu, Y. Shen, GDC-0449 improves the antitumor activity of nano-doxorubicin in pancreatic cancer in a fibroblast-enriched microenvironment. Sci. Rep. 7, 13379 (2017)
C.J. Hanley, M. Mellone, K. Ford, S.M. Thirdborough, T. Mellows, S.J. Frampton, D.M. Smith, E. Harden, C. Szyndralewiez, M. Bullock, F. Noble, K.A. Moutasim, E.V. King, P. Vijayanand, A.H. Mirnezami, T.J. Underwood, C.H. Ottensmeier, G.J. Thomas, Targeting the myofibroblastic cancer-associated fibroblast phenotype through inhibition of NOX4. J. Natl. Cancer Inst. 110, 109–120 (2018). https://doi.org/10.1093/jnci/djx121
M. Gabasa, R. Ikemori, F. Hilberg, N. Reguart, J. Alcaraz, Nintedanib selectively inhibits the activation and tumour-promoting effects of fibroblasts from lung adenocarcinoma patients. Br. J. Cancer 117, 1128–1138 (2017)
Y. Wei, T.J. Kim, D.H. Peng, D. Duan, D.L. Gibbons, M. Yamauchi, J.R. Jackson, C.J. Le Saux, C. Calhoun, J. Peters, R. Derynck, B.J. Backes, H.A. Chapman, Fibroblast-specific inhibition of TGF-β1 signaling attenuates lung and tumor fibrosis. J. Clin. Invest. 127, 3675–3688 (2017)
M. Chen, X. Lei, C. Shi, M. Huang, X. Li, B. Wu, Z. Li, W. Han, B. Du, J. Hu, Q. Nie, W. Mai, N. Ma, N. Xu, X. Zhang, C. Fan, A. Hong, M. Xia, L. Luo, A. Ma, H. Li, Q. Yu, H. Chen, D. Zhang, W. Ye, Pericyte-targeting prodrug overcomes tumor resistance to vascular disrupting agents. J. Clin. Invest. 127, 3689–3701 (2017)
Acknowledgements
The authors acknowledge financial support from DST-SERB, Government of India, New Delhi, India (SERB/LS-1028/2013) and Dr. D.Y. Patil Vidyapeeth, Pune, India (DPU/05/01/2016).
Funding
This study was funded by DST-SERB, Government of India, New Delhi, India (SERB/LS-1028/2013) and Dr. D.Y. Patil Vidyapeeth, Pune, India (DPU/05/01/2016).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical approval
Ethical approval for this study is not required.
Informed consent
Informed consent for this study is not required.
Rights and permissions
About this article
Cite this article
Nilendu, P., Sarode, S.C., Jahagirdar, D. et al. Mutual concessions and compromises between stromal cells and cancer cells: driving tumor development and drug resistance. Cell Oncol. 41, 353–367 (2018). https://doi.org/10.1007/s13402-018-0388-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13402-018-0388-2