Abstract
Osteoarthritis (OA) is a common form of arthritis in humans. It has long been regarded as a non-inflammatory disease, but a degree of inflammation is now recognized as being a vital inducer of subpopulation of OA. Besides inflammation, the establishment and development of OA are associated with alterations in metabolism and profiles of amino acids (AA), including glutamate- and arginine-family AA as well as their related metabolites (e.g., creatinine, hydroxyproline, γ-aminobutyrate, dimethylarginines and homoarginine). Functional AA (e.g., glutamine, arginine, glutamate, glycine, proline, and tryptophan) have various benefits (i.e., anti-inflammation and anti-oxidation) in treatment of inflammation-associated diseases, including OA. Thus, these AA have potential as immunomodulatory nutrients for patients with inflammation-induced OA.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis (OA) is a common form of arthritis characterized by articular cartilage destruction and osteophyte formation (Berenbaum 2013). It is a painful and disabling disease and reduces life quality of patients. The exact etiology of OA is still unknown, but various risk factors have been reported, including age (Blagojevic et al. 2010), obesity (Koonce and Bravman 2013), metabolic syndrome (Karlson et al. 2003), genetic predisposition (Spector et al. 1996), malalignment (Felson et al. 2013), acute joint injury (Gelber et al. 2000), and reduced sex hormone levels (Arden and Nevitt 2006). At present, there is no drug approved for structural protection of the joint or prolongation of joint life. With the growing understanding about OA, it can be divided into at least four subpopulations: (a) synovium-driven, (b) cartilage-driven, (c) bone-driven, and (d) other idiopathic conditions that remain to be understood (Siebuhr et al. 2015). OA has long been regarded as a non-inflammatory disease, but a degree of inflammation is now recognized as being a vital part of OA pathology (Siebuhr et al. 2015; Goldring and Otero 2011). Elevated levels of inflammatory mediators, such as interleukin (IL)-1β, IL-6, and IL-8, have been detected in both the synovial fluid and the serum from people with OA (Attur et al. 2013; Siebuhr et al. 2015). The inflammation and inflammation-related molecules from other underlying pathologies, such as trauma, metabolic syndrome and age, contribute to the initiation and persistence of OA, and synergize with other risk factors in the pathogenesis of OA (Sellam and Berenbaum 2010; Berenbaum 2013). For example, nuclear factor-κB (NF-κB) pathway is activated in OA disease by proinflammatory cytokines (i.e., tumor necrosis factor-α and IL-1β; Marcu et al. 2010). Once activated, the NF-κB signaling induces expression of various catabolic genes in articular chondrocytes (Marcu et al. 2010), including a disintegrin and matrix metalloproteinase (MMP) with thrombospondin motifs (ADAMTS)-5, inducible nitric oxide (NO) synthase (iNOS) and matrix metalloproteinase-13, which are highly involved in the pathogenesis of OA (Gao et al. 2015; Yang et al. 2014; Xu et al. 2013). Subsequently, inflammation has been regarded as a driver of joint destruction, OA symptoms, and progression of OA in a subpopulation of OA patients (Siebuhr et al. 2015).
Alterations of amino acid profiles in OA
Amino acids (AA) are not only building blocks of peptides and proteins, but are also precursors of low molecular weight substances (e.g., NO, dopamine, serotonin, polyamines, glucosamine, creatine, glutathione, homoarginine, and agmatine) with enormous physiological functions (Hou et al. 2015a; Yang et al. 2015a; Tsikas and Wu 2015; Wu 2013a, 2013b). For example, physiological concentrations of arginine (Jobgen et al. 2009a, b; Wu et al. 2013), glycine (Wang et al. 2013, 2014a, b), glutamine (Haynes et al. 2009; Wang et al. 2015b; Yi et al. 2015; Zhu et al. 2015), glutamate (Jiao et al. 2015; Rezaei et al. 2013a, b), proline (Obayashi et al. 2012, 2015; Wu et al. 2011a), cysteine (Hou et al. 2015b; Wu et al. 2004), and tryptophan (Yao et al. 2011) inhibit oxidative injury in cells. Furthermore, as an inhibitor of iNOS expression, glucosamine (a metabolite of glutamine) has been proposed to alleviate inflammation in OA patients (Meininger et al. 2000). This is analogous to the use of anti-inflammatory proteins (e.g., interferon-tau) to inhibit inflammation-induced cell injury under physiological (e.g., pregnancy) and pathological (e.g., autoimmune disease) conditions (Bazer et al. 2015).
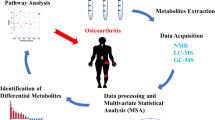
Besides inflammation, alterations in AA metabolism and profiles are also involved in the pathogenesis of OA (Dimitroulas et al. 2015; Mayboroda et al. 2007; Mickiewicz et al. 2015; Wen et al. 2015). In a recent study, Zignego et al. (2015) employed liquid chromatography-mass spectrometry-based metabolomics to understand short-term metabolic responses of human chondrocytes to sub-injurious physiological compression. Based on changes in the concentrations of threonine, homoserine, and allothreonine, these authors suggested that rates of glycine, serine, and threonine metabolism were increased after mechanical loading (Zignego et al. 2015). Results of the analysis of metabolites in synovial fluid by magnetic resonance spectroscopy-based metabolomics indicated that an anterior cruciate ligament reconstruction injury resulted in perturbed pathways for the metabolism of: (a) glycine, serine and threonine; (b) arginine and proline; and (c) alanine, aspartate, and glutamate in patients (Mickiewicz et al. 2015). As such, the profiles of glycine, serine, creatine, choline, hydroxyproline, proline, asparagine, succinate, alanine, and histidine were altered in subjects with injured joints (Mickiewicz et al. 2015). In rabbits with an anterior cruciate ligament reconstruction injury, there are marked changes in plasma levels of AA, particularly alanine, threonine and methionine (Ohnishi et al. 2013). Likewise, there are negative correlations between histological assessments and changes in plasma concentrations of many AA (including arginine, glutamate, citrulline, ornithine and hydroxyproline; Ohnishi et al. 2013). Furthermore, sheep with anterior cruciate ligament transaction exhibited decreases in serum concentrations of tyrosine, valine, isoleucine, and leucine, but increases in serum concentrations of glycine and 3-methylhistidine at week 4 after surgery, compared with the sham control (Maher et al. 2012). The animals also had lower concentrations of serum valine, isoleucine, and leucine, but higher concentrations of serum glutamine, creatine, creatinine and 3-methylhistidine at week 12 after surgery, than those from the sham surgery (Maher et al. 2012). Indeed, the ratio of branched-chain AA to histidine, including the ratios of valine to histidine and leucine or isoleucine to histidine, is potentially a useful biomarker for osteoarthritis (Zhai et al. 2010). With the use of ultra-performance liquid chromatography coupled to mass spectrometry, fourteen significantly altered metabolites were eventually identified in the serum of OA, compared to healthy controls (Zhang et al. 2015). Among them, serum levels of 4-oxoproline, glycine and histidine were decreased, while serum levels of tryptophan were increased in OA, compared to healthy controls (Zhang et al. 2015). The amount of plasma iNOS in the OA group was higher than that in healthy controls (Suantawee et al. 2015). This result indicates changes in arginine metabolism in OA patients, as arginine is the physiological nitrogenous substrate for iNOS (Wu et al. 2009). In support of this view, OA patients have a lower concentration of arginine, a lower ratio of arginine/asymmetric dimethylarginine, and a higher concentration of symmetric dimethylarginine in the plasma, compared to healthy controls (Pascale et al. 2013). Also, concentrations of arginine and asymmetric dimethylarginine in synovial fluid are higher than that in the plasma of OA patients (Pascale et al. 2013). Similarly, altered concentrations of arginine, homoarginine and dimethylarginines in the plasma of OA patients have recently been reported by other researchers (Kayacelebi et al. 2015).
Anti-inflammatory treatments in OA
Anti-inflammatory treatments by targeting inflammatory cytokines, such as IL-1β, IL-23 and TNF-α, are used in inflammation-related diseases such as rheumatoid arthritis, gout, juvenile idiopathic arthritis, and ankylosing spondylitis (Tyring et al. 2006; Whibley and Gaffen 2015; Ren et al. 2013f, 2015; Wang et al. 2015a). The benefits of anti-inflammatory treatment are also observed in OA. Oral administration of naringin attenuates TNF-α-mediated inflammation and catabolism in chondrocytes, alleviates degradation of cartilage matrix, and protects against OA development in surgically induced mouse OA models through inhibition of NF-κB pathways (Zhao et al. 2015). Berberine reduces the induction of IL-1β expression in response to connective tissue growth factor and reverses cartilage damage in an experimental rat model of collagenase-induced OA (Liu et al. 2015). Through its anti-inflammatory property, diosgenin inhibits production of NO and prostaglandin E2, and expression of MMP-3, MMP-13, iNOS, and cyclooxygenase-2 in human OA chondrocytes (Wang et al. 2015a, b). Interestingly, one study has explored an anti-TNF-α therapy in OA by conducting an open-label evaluation of adalimumab over 12 weeks in 20 patients with OA of the knee (Maksymowych et al. 2012). After anti-TNF-α therapy, the authors observed a significant improvement in mean WOMAC pain, stiffness, function, physician and patient global, as well as target joint swelling at 12 weeks (Maksymowych et al. 2012). This result indicates that targeting TNF-α may be of therapeutic benefit in OA. However, anti-inflammatory treatments in OA by other investigations have shown limited effects (Siebuhr et al. 2015; Chevalier et al. 2009; Cohen et al. 2011), possibly due to the lack of preselection of patients with inflammation, ineffective drugs, and suboptimal treatment procedures. Nonetheless, these interesting studies show that anti-inflammatory treatments may be a potentially effective therapy for OA, especially for patients with inflammation-induced OA. Thus, the development of drugs with active anti-inflammatory properties is promising in treating this inflammatory disease.
AA interventions in OA
Nutritional interventions and nutraceutical applications for medical conditions are currently riding the crest of public enthusiasm. Based on the alterations in AA metabolism and AA profile in the pathogenesis of OA, it is potentially attractive to use nutritional interventions with AA to manipulate the pathogenesis of OA. Indeed, nutritional interventions with functional AA are beneficial in various models, such as mice with virus or bacteria infection (Ren et al. 2012b, 2013d), mice with vaccine immunization (Ren et al. 2013g), and mice with inflammatory disease (Ren et al. 2014b). The following sections highlight glutamine, arginine, glutamate, aspartate, and S-adenosylmethionine.
Glutamine
Glutamine is the most prevalent AA in both body fluids and skeletal muscle and is considered as a nutritionally essential AA under specific physiological conditions, such as malnutrition, infection and inflammation (Ren et al. 2012a, 2013c, 2013d, 2013e; Wu et al. 2011b). Glutamine has an anti-inflammatory role in various intestinal inflammatory models through its regulatory function in signaling pathways, including NF-κB, signal transducer and activator of transcription (STAT), mitogen-activated protein kinases, phosphoinositide 3-kinase-protein kinase B, activating protein-1, NOS-NO, peroxisome proliferator-activated receptor-γ (PPAR γ), heat shock factor-1-heat shock proteins (HSP), and glutathione-reactive oxygen species (Ren et al. 2013f). For example, glutamine inhibits NF-κB signaling through three levels. At the NF-κB level, glutamine inhibits NF-κB protein expression and the dimer (p50 and p65) translocation from the cytoplasm to the nucleus and promotes p65 protein degradation through the phosphorylation at serine-536. At the inhibitor of κBs (IκB) level, glutamine reduces its ubiquitination and degradation through the decrease of IκB phosphorylation. At the IκB kinase level, glutamine decreases IκB kinase-α and IκB kinase-β abundance (Ren et al. 2013f). Thus, glutamine has anti-oxidative functions not only in inflammatory diseases of the intestine, but also in other inflammation-associated diseases, such as arthritis and asthma (Ren et al. 2013f). Indeed, in the dextran sulfate sodium-induced colitis model, which is similar to human ulcerative colitis, dietary glutamine supplementation has beneficial effects on clinical and biochemical parameters (i.e., total superoxide dismutase, IL-17 and TNF-α) in colitis model, and these results are associated with colonic NF-κB and phosphoinositide 3-kinase-protein kinase B signaling pathways, suggesting glutamine could be a potential therapy for intestinal inflammatory diseases (Ren et al. 2014b). Glutamine could be also as an adjuvant therapy for OA with its anti-inflammatory function. Notably, glutamine treatment affects expression of HSP70 in articular chondrocytes, abrogates the cytotoxic outcome of sodium nitroprusside dehydrate in chondrocytes, and renders chondrocytes unsusceptible to NO-induced apoptosis (Tonomura et al. 2006). Furthermore, glutamine treatment affects expression of aggrecan and HSP70, and the severity of OA in rat models (Fujita et al. 2012). However, these observed benefits of glutamine in chondrocytes and in animal OA models depend on HSP70 (Fujita et al. 2012; Tonomura et al. 2006). Thus, whether glutamine exerts beneficial roles on OA patients through anti-inflammation merits further investigations.
Arginine
Arginine had long been considered as a nutritionally non-essential AA for adult animals and humans, but has recently been classified as a nutritionally semi-essential AA for young mammals (such as rats, swine, and infants), as well as males and females in certain situations (Wu 2014; Wu et al. 2014a). This is because the rate of arginine utilization in the whole body is greater than the rate of arginine synthesis under certain conditions (e.g., early weaning, lactation, pregnancy, inflammation, burns, injury, infection, heat stress, and cold stress) (Wu et al. 2014a; Wu 2009; Ren et al. 2012b). In humans, pigs, and rats, most of dietary arginine is metabolized via arginase and arginine–glycine amidinotransferase pathways, but the production of NO from arginine by NO synthase plays an important role in immune responses (Wu et al. 2009). It is now known that three isoforms of NOS generate NO from arginine in a cell-specific manner (Wu et al. 2009). The nutritional significance of this metabolic pathway is supported by the observations that dietary supplementation with arginine improves immunity, leading to the killing of pathogens (e.g., bacteria and virus) (Ren et al. 2012b, 2013g, 2014a, 2014b; Li et al. 2007). At molecular and cellular levels, arginine activates both cell- and antibody-mediated immune responses in mice (Ren et al. 2013g, 2014a; Shang et al. 2003), humans (Moriguti et al. 2005), chickens (Munir et al. 2009; Perez-Carbajal et al. 2010), pigs (Chen et al. 2012), and fish (Pohlenz et al. 2012). Interestingly, arginine has various benefits in mice with dextran sulfate sodium-induced colitis, including improvements in clinical parameters of survival, body weight loss, colon weight, and reduction of colonic permeability, number of myeloperoxidase-positive neutrophils, and expression of proinflammatory cytokines and chemokines (Coburn et al. 2012). Indeed, in our previous study, we also found arginine supplementation increased colon length, superoxide dismutase activity, and claudin-1 expression, while alleviating infiltration of neutrophils, expression of IL-17 and TNF-α, and activation of colonic phosphoinositide 3-kinase-protein kinase B and myosin light-chain kinase-myosin light chain-20 pathways (Ren et al. 2014b). These findings suggest that it is fruitful to suppress the pathogenesis of OA by manipulating arginine metabolism. S-Methylisothiourea, an iNOS inhibitor, reduces the release of MMP-13, TNF-α, prostaglandin E2, and nitrite in stimulated rabbit cartilage media, while attenuating the production of nitrite, prostaglandin E2, IL-1β and TNF-α from synovial explants. (Balaganur et al. 2014). These results indicate chondroprotective and anti-inflammatory effects of S-methylisothiourea in OA. N-iminoethyl-l-lysine, an iNOS inhibitor, has a beneficial effect in OA through: (a) preventing lipid peroxidation and reactive oxygen species production via NO-dependent and/or independent mechanisms; (b) attenuating 4-hydroxynonenal (a product of LPO)-induced cell death; and (c) different mediators of cartilage damage (Bentz et al. 2012).
Glutamate and aspartate
Glutamate and aspartate are excitatory AA neurotransmitters in the mammalian central nervous system. Glutamate and aspartate are associated with the production of ATP and other biological active molecules, including glutamine, glutathione, proline, ornithine, and arginine, thereby affecting cell metabolism and signaling, host anti-oxidative ability, immunity under physiological and pathological conditions, and animal growth performance (Rezaei et al. 2013a, 2013b; Wu 2009, 2010). Dietary supplementation with glutamate or aspartate protects hosts from damage caused by stimulators exposure, such as decrease in oxidative stress, alteration of serum AA concentrations, and changes in expression of intestinal AA transporters (Duan et al. 2014, 2015; Wu et al. 2014b, 2014c). Glutamate or aspartate may have vital role in the acute and ongoing progressive processes of soft tissue injuries that impact early OA development because there is a significant increase in levels of glutamate and aspartate in the microdialysates of anterior cruciate ligament transected knee joints in rats, compared to those in the contralateral sham-operated knee (Jean et al. 2005). Additionally, glutamate and aspartate in synovial fluid from patients with synovitis are 54 and 28 times higher, respectively, than those from healthy controls, suggesting that glutamate and aspartate may contribute to the pathogenesis of human arthritic conditions (McNearney et al. 2000). Additionally, γ-aminobutyrate (a product of glutamate decarboxylation) may affect OA progress possibly by blocking the activation-induced calcium signal and inhibiting NF-κB activation (Huang et al. 2015). Further studies have demonstrated the significant associations between glutamate or aspartate and inflammatory mediators, such as TNF-α, regulated on activation normal T cell expressed and secreted (RANTES) protein, and IL-8, in the synovial fluid of patients with active inflammatory arthropathies, such as rheumatoid arthritis, acute gout, and symptomatic OA (McNearney et al. 2004; 2010). Indeed, bone and joints have the components of glutamate signaling, including glutamate receptors, glutamate transporters, and vesicular glutamate transporters (Wen et al. 2015). Thus, glutamate or aspartate can be used as therapeutic targets for OA. Intrathecal administration of ketamine, an uncompetitive N-methyl-d-aspartate receptor channel blocker, reduces the pain and severity of arthritis in antigen-induced arthritis in rats, including reductions in joint swelling and infiltration of inflammatory cells into the joint cavity (Boettger et al. 2010). A Phase II trial of LY545694, an antagonist of ionotropic glutamate receptor 5, in the treatment of knee OA pain has been completed (Martel-Pelletier et al. 2012; Wen et al. 2015), and some benefits have been observed.
Other functional amino acids and metabolites
S-adenosylmethionine (SAM) is the activated form of methionine and is a methyl group donor in protein and DNA methylation reactions (Wu 2013a, b). SAM has been reported to protect synovial cells through promoting glutathione peroxidase production, and blocking the activity and synthesis of enzymes that degrade cartilage (Lieber and Packer 2002; Lopez 2012). SAM may also protect cartilage proteins and proteoglycans in the joint lining. These results suggest an interesting therapeutic potency of SAM in the pathogenesis of OA. Indeed, SAM is effective to treat OA, and the efficacy is equal to, even more effective, and better tolerated than administration of indomethacin or ibuprofen (Glorioso et al. 1985; Vetter 1987). Moreover, the clinical improvements achieved by the 12-week treatment with SAM on 45 patients with knee OA can sustain for a longer period of time than with piroxicam treatment (Maccagno et al. 1987).
In a study to investigate the efficacy of creatine (a product of arginine, glycine and methionine metabolism) supplementation combined with strengthening exercises in OA, the authors found that creatine supplementation can improve physical function, stiffness subscales, lower limb lean mass, and quality of life, while reducing the pain for OA patients (Neves et al. 2011). Thus, creatine administration has potential to be used as adjuvant therapy for OA.
Conclusion and perspectives
The establishment and development of OA are associated with inflammation and alterations in AA metabolism and profiles. Emerging evidence shows that OA patients have lower concentrations of plasma l-valine, l-isoleucine, and l-leucine (Maher et al. 2012; Zhai et al. 2010), but higher concentrations of plasma l-glutamate and l-aspartate (McNearney et al. 2000; Jean et al. 2005), compared to healthy controls. As most AA have numerous biological functions in vivo (Wu 2009, 2010; Chen et al. 2014), they may be considered in nutritional therapy of OA through dietary supplementation. Additionally, results of recent research indicate that some functional AA can have benefits on inhibiting the pathogenesis of OA and alleviating its complications. It is interesting to uncover the regulatory functions of other AA in the initiation, establishment, development and progression of OA, such as proline, threonine, glycine, tryptophan, and methionine. For example, proline has been demonstrated to regulate immune responses in virus or bacteria infected models (Ren et al. 2013a, 2013b). Threonine and methionine are reported to regulate epithelial cell migration and proliferation, cell differentiation, restoration of epithelial barrier functions, and modulation of cell apoptosis, thereby enhancing mucosal healing after intestinal mucosal inflammation (Lan et al. 2015) and modulating autophagic responses of porcine intestinal epithelial cells to enterotoxigenic Escherichia coli infection (Tang et al. 2015). Furthermore, leucine, which can inhibit NO synthesis (Yang et al. 2015b), may also be effective to attenuate the progression of OA. Further research is necessary to provide much-needed data on roles of functional AA in the prevention and treatment of OA.
Abbreviations
- AA:
-
Amino acid(s)
- HSP:
-
Heat shock proteins
- IκB:
-
Inhibitor of κBs
- IL:
-
Interleukin
- iNOS:
-
Inducible nitric oxide synthase
- MMP:
-
Matrix metalloproteinase
- NF-κB:
-
Nuclear factor-κB
- NO:
-
Nitric oxide
- OA:
-
Osteoarthritis
- PPAR γ:
-
Peroxisome proliferator-activated receptor-γ
- SAM:
-
S-Adenosylmethionine
- TNF-α:
-
Tumor necrosis factor-α
References
Arden N, Nevitt MC (2006) Osteoarthritis: epidemiology. Best Pract Res Clin Rheumatol 20:3–25
Attur M, Krasnokutsky-Samuels S, Samuels J et al (2013) Prognostic biomarkers in osteoarthritis. Curr Opin Rheumatol 25:136–144
Balaganur V, Pathak NN, Lingaraju MC et al (2014) Chondroprotective and anti-inflammatory effects of S-methylisothiourea, an inducible nitric oxide synthase inhibitor in cartilage and synovial explants model of osteoarthritis. J Pharm Pharmacol 66:1021–1031
Bazer FW, Ying W, Wang XQ et al (2015) The many faces of interferon tau. Amino Acids 47:449–460
Bentz M, Zaouter C, Shi Q et al (2012) Inhibition of inducible nitric oxide synthase prevents lipid peroxidation in osteoarthritic chondrocytes. J Cell Biochem 113:2256–2267
Berenbaum F (2013) Osteoarthritis as an inflammatory disease (osteoarthritis is not osteoarthrosis!). Osteoarthritis Cartilage 21:16–21
Blagojevic M, Jinks C, Jeffery A et al (2010) Risk factors for onset of osteoarthritis of the knee in older adults: a systematic review and meta-analysis. Osteoarthritis Cartilage 18:24–33
Boettger MK, Weber K, Gajda M et al (2010) Spinally applied ketamine or morphine attenuate peripheral inflammation and hyperalgesia in acute and chronic phases of experimental arthritis. Brain Behav Immun 24:474–485
Chen Y, Chen D, Tian G et al (2012) Dietary arginine supplementation alleviates immune challenge induced by Salmonella enterica serovar Choleraesuis bacterin potentially through the Toll-like receptor 4-myeloid differentiation factor 88 signalling pathway in weaned piglets. Br J Nutr 108:1069–1076
Chen S, Liu S, Zhang F et al (2014) Effects of dietary l-glutamine supplementation on specific and general defense responses in mice immunized with inactivated Pasteurella multocida vaccine. Amino Acids 46:2365–2375
Chevalier X, Goupille P, Beaulieu AD et al (2009) Intraarticular injection of anakinra in osteoarthritis of the knee: a multicenter, randomized, double-blind, placebo-controlled study. Arthritis Rheum 61:344–352
Coburn LA, Gong X, Singh K et al (2012) L-arginine supplementation improves responses to injury and inflammation in dextran sulfate sodium colitis. PLoS One 7:e33546
Cohen SB, Proudman S, Kivitz AJ et al (2011) A randomized, double-blind study of AMG 108 (a fully human monoclonal antibody to IL-1R1) in patients with osteoarthritis of the knee. Arthritis Res Ther 13:R125
Dimitroulas T, Hodson J, Sandoo A et al (2015) Symmetric dimethylarginine (SDMA) serum levels in rheumatoid arthritis: correlations with insulin resistance and disease activity scores. Amino Acids 47:1995–2004
Duan J, Yin J, Wu M et al (2014) Dietary glutamate supplementation ameliorates mycotoxin-induced abnormalities in the intestinal structure and expression of amino acid transporters in young pigs. PLoS One 9:e112357
Duan J, Yin J, Ren W et al (2015) Dietary supplementation with l-glutamate and l-aspartate alleviates oxidative stress in weaned piglets challenged with hydrogen peroxide. Amino Acids. doi:10.1007/s00726-015-2065-3
Felson DT, Niu J, Gross KD et al (2013) Valgus malalignment is a risk factor for lateral knee osteoarthritis incidence and progression: findings from the Multicenter Osteoarthritis Study and the Osteoarthritis Initiative. Arthritis Rheum 65:355–362
Fujita S, Arai Y, Nakagawa S et al (2012) Combined microwave irradiation and intraarticular glutamine administration-induced HSP70 expression therapy prevents cartilage degradation in a rat osteoarthritis model. J Orthop Res 30:401–407
Gao SG, Zeng C, Song Y et al (2015) Effect of osteopontin on the mRNA expression of ADAMTS4 and ADAMTS5 in chondrocytes from patients with knee osteoarthritis. Exp Ther Med 9:1979–1983
Gelber AC, Hochberg MC, Mead LA et al (2000) Joint injury in young adults and risk for subsequent knee and hip osteoarthritis. Ann Intern Med 133:321–328
Glorioso S, Todesco S, Mazzi A et al (1985) Double-blind multicentre study of the activity of S-adenosylmethionine in hip and knee osteoarthritis. Int J Clin Pharmacol Res 5:39–49
Goldring MB, Otero M (2011) Inflammation in osteoarthritis. Curr Opin Rheumatol 23:471–478
Haynes TE, Li P, Li XL et al (2009) l-Glutamine or l-alanyl-l-glutamine prevents oxidant- or endotoxin-induced death of neonatal enterocytes. Amino Acids 37:131–142
Hou YQ, Yin YL, Wu G (2015a) Dietary essentiality of “nutritionally nonessential amino acids” for animals and humans. Exp Biol Med 240:997–1007
Hou YQ, Wang L, Yi D et al (2015b) N-acetylcysteine and intestinal health: a focus on mechanisms of its actions. Front Biosci 20:872–891
Huang S, Mao J, Wei B et al (2015) The anti-spasticity drug baclofen alleviates collagen-induced arthritis and regulates dendritic cells. J Cell Physiol 230:1438–1447
Jean YH, Wen ZH, Chang YC et al (2005) Increased concentrations of neuro-excitatory amino acids in rat anterior cruciate ligament-transected knee joint dialysates: a microdialysis study. J Orthop Res 23:569–575
Jiao N, Wu ZL, Ji Y et al (2015) l-Glutamate enhances barrier and anti-oxidative functions in intestinal porcine epithelial cells. J Nutr 145:2258–2264
Jobgen WJ, Meininger CJ, Jobgen SC et al (2009a) Dietary l-arginine supplementation reduces white-fat gain and enhances skeletal muscle and brown fat masses in diet-induced obese rats. J Nutr 139:230–237
Jobgen WJ, Fu WJ, Gao H et al (2009b) High fat feeding and dietary l-arginine supplementation differentially regulate gene expression in rat white adipose tissue. Amino Acids 37:187–198
Karlson EW, Mandl LA, Aweh GN et al (2003) Total hip replacement due to osteoarthritis: the importance of age, obesity, and other modifiable risk factors. Am J Med 114:93–98
Kayacelebi AA, Willers J, Pham VV et al (2015) Plasma homoarginine, arginine, asymmetric dimethylarginine and total homocysteine interrelationships in rheumatoid arthritis, coronary artery disease and peripheral artery occlusion disease. Amino Acids 47:1885–1891
Koonce RC, Bravman JT (2013) Obesity and osteoarthritis: more than just wear and tear. J Am Acad Orthop Surg 21:161–169
Lan A, Blachier F, Benamouzig R et al (2015) Mucosal healing in inflammatory bowel diseases: is there a place for nutritional supplementation? Inflamm Bowel Dis 21:198–207
Li P, Yin YL, Li D et al (2007) Amino acids and immune function. Br J Nutr 98:237–252
Lieber CS, Packer L (2002) S-Adenosylmethionine: molecular, biological, and clinical aspects—an introduction. Am J Clin Nutr 76:1148S–1150S
Liu SC, Lee HP, Hung CY et al (2015) Berberine attenuates CCN2-induced IL-1beta expression and prevents cartilage degradation in a rat model of osteoarthritis. Toxicol Appl Pharmacol 289:20–29
Lopez HL (2012) Nutritional interventions to prevent and treat osteoarthritis. Part II: focus on micronutrients and supportive nutraceuticals. PM R 4 (5 Suppl):S155–168
Maccagno A, Di Giorgio EE, Caston OL et al (1987) Double-blind controlled clinical trial of oral S-adenosylmethionine versus piroxicam in knee osteoarthritis. Am J Med 83(5A):72–77
Maher AD, Coles C, White J et al (2012) 1H NMR spectroscopy of serum reveals unique metabolic fingerprints associated with subtypes of surgically induced osteoarthritis in sheep. J Proteome Res 11:4261–4268
Maksymowych WP, Russell AS, Chiu P et al (2012) Targeting tumour necrosis factor alleviates signs and symptoms of inflammatory osteoarthritis of the knee. Arthritis Res Ther 14:R206
Marcu KB, Otero M, Olivotto E et al (2010) NF-kappaB signaling: multiple angles to target OA. Curr Drug Targets 11:599–613
Martel-Pelletier J, Wildi LM, Pelletier JP (2012) Future therapeutics for osteoarthritis. Bone 51:297–311
Mayboroda OA, Neusüss C, Pelzing M et al (2007) Amino acid profiling in urine by capillary zone electrophoresis—mass spectrometry. J Chromatogr A 1159:149–153
McNearney T, Speegle D, Lawand N et al (2000) Excitatory amino acid profiles of synovial fluid from patients with arthritis. J Rheumatol 27:739–745
McNearney T, Baethge BA, Cao S et al (2004) Excitatory amino acids, TNF-alpha, and chemokine levels in synovial fluids of patients with active arthropathies. Clin Exp Immunol 137:621–627
McNearney TA, Ma Y, Chen Y et al (2010) A peripheral neuroimmune link: glutamate agonists upregulate NMDA NR1 receptor mRNA and protein, vimentin, TNF-alpha, and RANTES in cultured human synoviocytes. Am J Physiol Regul Integr Comp Physiol 298:R584–598
Meininger CJ, Kelly KA, Li H et al (2000) Glucosamine inhibits inducible nitric oxide synthesis. Biochem Biophys Res Commun 279:234–239
Mickiewicz B, Heard BJ, Chau JK et al (2015) Metabolic profiling of synovial fluid in a unilateral ovine model of anterior cruciate ligament reconstruction of the knee suggests biomarkers for early osteoarthritis. J Orthop Res 33:71–77
Moriguti JC, Ferriolli E, Donadi EA et al (2005) Effects of arginine supplementation on the humoral and innate immune response of older people. Eur J Clin Nutr 59:1362–1366
Munir K, Muneer MA, Masaoud E et al (2009) Dietary arginine stimulates humoral and cell-mediated immunity in chickens vaccinated and challenged against hydropericardium syndrome virus. Poult Sci 88:1629–1638
Neves M Jr, Gualano B, Roschel H et al (2011) Beneficial effect of creatine supplementation in knee osteoarthritis. Med Sci Sports Exerc 43:1538–1543
Obayashi Y, Arisaka H, Yoshida S et al (2012) Proline protects liver from d-galactosamine hepatitis by activating the IL-6/STAT3 survival signaling pathway. Amino Acids 43:2371–2380
Obayashi Y, Arisaka H, Yoshida S et al (2015) The protection mechanism of proline from d-galactosamine hepatitis involves the early activation of ROS-eliminating pathway in the liver. Springerplus 4:199
Ohnishi A, Osaki T, Matahira Y et al (2013) Correlation of plasma amino acid concentrations and chondroprotective effects of glucosamine and fish collagen peptide on the development of osteoarthritis. J Vet Med Sci 75:497–502
Pascale V, Pascale W, Lavanga V et al (2013) l-arginine, asymmetric dimethylarginine, and symmetric dimethylarginine in plasma and synovial fluid of patients with knee osteoarthritis. Med Sci Monit 19:1057–1062
Perez-Carbajal C, Caldwell D, Farnell M et al (2010) Immune response of broiler chickens fed different levels of arginine and vitamin E to a coccidiosis vaccine and Eimeria challenge. Poult Sci 89:1870–1877
Pohlenz C, Buentello A, Criscitiello MF et al (2012) Synergies between vaccination and dietary arginine and glutamine supplementation improve the immune response of channel catfish against Edwardsiella ictaluri. Fish Shellfish Immunol 33:543–551
Ren WK, Liu G, Li TJ et al (2012a) Dietary supplementation with arginine and glutamine confers a positive effect in porcine circovirus-infected pig. J Food Agric Environment 10:485–490
Ren WK, Yin YL, Liu G et al (2012b) Effect of dietary arginine supplementation on reproductive performance of mice with porcine circovirus type 2 infection. Amino Acids 42:2089–2094
Ren W, Wu M, Luo W et al (2013a) Dietary supplementation with proline confers a positive effect in both porcine circovirus-infected pregnant and non-pregnant mice. Br J Nutr 110:1492–1499
Ren W, Zou L, Ruan Z et al (2013b) Dietary l-proline supplementation confers immunostimulatory effects on inactivated Pasteurella multocida vaccine immunized mice. Amino Acids 45:555–561
Ren WK, Li YH, Yu XL et al (2013c) Glutamine modifies immune responses of mice infected with porcine circovirus type 2. Br J Nutr 110:1053–1060
Ren WK, Liu SP, Chen S et al (2013d) Dietary l-glutamine supplementation increases Pasteurella multocida burden and the expression of its major virulence factors in mice. Amino Acids 45:947–955
Ren WK, Luo W, Wu MM et al (2013e) Dietary l-glutamine supplementation improves pregnancy outcome in mice infected with type-2 porcine circovirus. Amino Acids 45:479–488
Ren WK, Yin J, Zhu XP et al (2013f) Glutamine on intestinal inflammation: a mechanistic perspective. Eur J Inflammation 11:315–326
Ren WK, Zou LX, Li NZ et al (2013g) Dietary arginine supplementation enhances immune responses to inactivated Pasteurella multocida vaccination in mice. Br J Nutr 109:867–872
Ren W, Chen S, Yin J et al (2014a) Dietary arginine supplementation of mice alters the microbial population and activates intestinal innate immunity. J Nutr 144:988–995
Ren W, Yin J, Wu M et al (2014b) Serum amino acids profile and the beneficial effects of l-arginine or l-glutamine supplementation in dextran sulfate sodium colitis. PLoS One 9:e88335
Ren W, Yin J, Duan J et al (2015) mTORC1 signaling and IL-17 expression: defining pathways and possible therapeutic targets. Eur J Immunol. doi:10.1002/eji.201545886
Rezaei R, Wang W, Wu Z et al (2013a) Biochemical and physiological bases for utilization of dietary amino acids by young Pigs. J Anim Sci Biotechnol 4:7
Rezaei R, Knabe DA, Tekwe CD et al (2013b) Dietary supplementation with monosodium glutamate is safe and improves growth performance in postweaning pigs. Amino Acids 44:911–923
Sellam J, Berenbaum F (2010) The role of synovitis in pathophysiology and clinical symptoms of osteoarthritis. Nat Rev Rheumatol 6:625–635
Shang HF, Tsai HJ, Chiu WC et al (2003) Effects of dietary arginine supplementation on antibody production and antioxidant enzyme activity in burned mice. Burns 29:43–48
Siebuhr AS, Bay-Jensen AC, Jordan JM et al (2015) Inflammation (or synovitis)-driven osteoarthritis: an opportunity for personalizing prognosis and treatment? Scand J Rheumatol:1–12
Spector TD, Cicuttini F, Baker J et al (1996) Genetic influences on osteoarthritis in women: a twin study. BMJ 312:940–943
Suantawee T, Tantavisut S, Adisakwattana S et al (2015) Upregulation of inducible nitric oxide synthase and nitrotyrosine expression in primary knee osteoarthritis. J Med Assoc Thai 98(Suppl 1):S91–97
Tang Y, Tan B, Xiong X et al (2015) Methionine deficiency reduces autophagy and accelerates death in intestinal epithelial cells infected with enterotoxigenic Escherichia coli. Amino Acids 47:2199–2204
Tonomura H, Takahashi KA, Mazda O et al (2006) Glutamine protects articular chondrocytes from heat stress and NO-induced apoptosis with HSP70 expression. Osteoarthritis Cartilage 14:545–553
Tsikas D, Wu G (2015) Homoarginine, arginine, and relatives: analysis, metabolism, transport, physiology, and pathology. Amino Acids 47:1697–1702
Tyring S, Gottlieb A, Papp K et al (2006) Etanercept and clinical outcomes, fatigue, and depression in psoriasis: double-blind placebo-controlled randomised phase III trial. Lancet 367:29–35
Vetter G (1987) Double-blind comparative clinical trial with S-adenosylmethionine and indomethacin in the treatment of osteoarthritis. Am J Med 83(5A):78–80
Wang WW, Wu ZL, Dai ZL et al (2013) Glycine metabolism in animals and humans: implications for nutrition and health. Amino Acids 45:463–477
Wang WW, Dai ZL, Wu ZL et al (2014a) Glycine is a nutritionally essential amino acid for maximal growth of milk-fed young pigs. Amino Acids 46:2037–2045
Wang WW, Wu ZL, Lin G et al (2014b) Glycine stimulates protein synthesis and inhibits oxidative stress in pig small-intestinal epithelial cells. J Nutr 144:1540–1548
Wang L, Ma T, Zheng Y et al (2015a) Diosgenin inhibits IL-1beta-induced expression of inflammatory mediators in human osteoarthritis chondrocytes. Int J Clin Exp Pathol 8:4830–4836
Wang B, Wu G, Zhou ZG et al (2015b) Glutamine and intestinal barrier function. Amino Acids 47:2143–2154
Wen ZH, Chang YC, Jean YH (2015) Excitatory amino acid glutamate: role in peripheral nociceptive transduction and inflammation in experimental and clinical osteoarthritis. Osteoarthritis Cartilage 23:2009–2016
Whibley N, Gaffen SL (2015) Gut-Busters: IL-17 Ain’t Afraid of No IL-23. Immunity 43:620–622
Wu G (2009) Amino acids: metabolism, functions, and nutrition. Amino Acids 37:1–17
Wu G (2010) Functional amino acids in growth, reproduction, and health. Adv Nutr 1:31–37
Wu G (2013a) Functional amino acids in nutrition and health. Amino Acids 45:407–411
Wu G (2013b) Amino acids: biochemistry and nutrition. CRC Press, Boca Raton
Wu G (2014) Dietary requirements of synthesizable amino acids by animals: a paradigm shift in protein nutrition. J Anim Sci Biotechnol 5:34
Wu G, Fang YZ, Yang S et al (2004) Glutathione metabolism and its implications for health. J Nutr 134:489–492
Wu G, Bazer FW, Davis TA et al (2009) Arginine metabolism and nutrition in growth, health and disease. Amino Acids 37:153–168
Wu G, Bazer FW, Burghardt RC et al (2011a) Proline and hydroxyproline metabolism: implications for animal and human nutrition. Amino Acids 40:1053–1063
Wu G, Bazer FW, Johnson GA et al (2011b) Important roles for l-glutamine in swine nutrition and production. J Anim Sci 89:2017–2030
Wu G, Bazer FW, Satterfield MC et al (2013) Impacts of arginine nutrition on embryonic and fetal development in mammals. Amino Acids 45:241–256
Wu G, Bazer FW, Dai Z et al (2014a) Amino Acid nutrition in animals: protein synthesis and beyond. Annu Rev Anim Biosci 2:387–417
Wu M, Xiao H, Ren W et al (2014b) An NMR-based metabolomic approach to investigate the effects of supplementation with glutamic acid in piglets challenged with deoxynivalenol. PLoS One 9:e113687
Wu M, Xiao H, Ren W et al (2014c) Therapeutic effects of glutamic acid in piglets challenged with deoxynivalenol. PLoS One 9:e100591
Xu M, Zhang L, Zhao L et al (2013) Phosphorylation of osteopontin in osteoarthritis degenerative cartilage and its effect on matrix metalloprotease 13. Rheumatol Int 33:1313–1319
Yang Y, Gao SG, Zhang FJ et al (2014) Effects of osteopontin on the expression of IL-6 and IL-8 inflammatory factors in human knee osteoarthritis chondrocytes. Eur Rev Med Pharmacol Sci 18:3580–3586
Yang Y, Wu ZL, Jia SC et al (2015a) Safety of long-term dietary supplementation with l-arginine in rats. Amino Acids 47:1907–1920
Yang Y, Wu ZL, Meininger CJ et al (2015b) l-Leucine and NO-mediated cardiovascular function. Amino Acids 47:435–447
Yao K, Yin YL, Feng ZM et al (2011) Tryptophan metabolism in animals: important roles in nutrition and health. Front Biosci S3:286–297
Yi D, Hou YQ, Wang L et al (2015) l-Glutamine enhances enterocyte growth via activation of the mTOR signaling pathway independently of AMPK. Amino Acids 47:65–78
Zhai G, Wang-Sattler R, Hart DJ et al (2010) Serum branched-chain amino acid to histidine ratio: a novel metabolomic biomarker of knee osteoarthritis. Ann Rheum Dis 69:1227–1231
Zhang Q, Li H, Zhang Z et al (2015) Serum metabolites as potential biomarkers for diagnosis of knee osteoarthritis. Dis Markers 2015:684794
Zhao Y, Li Z, Wang W et al (2015) Naringin protects against cartilage destruction in osteoarthritis through repression of NF-κB signaling sathway. Inflammation. doi:10.1007/s10753-015-0260-8
Zhu YH, Lin G, Dai ZL et al (2015) l-Glutamine deprivation induces autophagy and alters the mTOR and MAPK signaling pathways in porcine intestinal epithelial cells. Amino Acids 47:2185–2197
Zignego DL, Hilmer JK, June RK (2015) Mechanotransduction in primary human osteoarthritic chondrocytes is mediated by metabolism of energy, lipids, and amino acids. J Biomech 48:4253–4261
Acknowledgments
This work was supported by the National Natural Science Foundation of China (No. 81201420, 81272034, 81402224, 81472130), the Provincial Science Foundation of Hunan (No. 14JJ3032, No. 2015JJ3139), the Development and Reform Commission of Hunan Province ([2013]1199, [2014]658-8), the Science and Technology Office of Hunan Province (2012FJ6001,2013SK2018),the Science and Technology Office of Changsha City (K1203040-31), the Health and Family Planning Commission of Hunan Province (B2014-12), the Administration of Traditional Chinese Medicine of Hunan Province (No.2015115), and Texas A&M AgriLife Research (H-8200).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
There is no potential conflict of interest and no human participants and/or animals are involved in this review.
Conflict of interest
There is no conflicting interest.
Rights and permissions
About this article
Cite this article
Li, Y., Xiao, W., Luo, W. et al. Alterations of amino acid metabolism in osteoarthritis: its implications for nutrition and health. Amino Acids 48, 907–914 (2016). https://doi.org/10.1007/s00726-015-2168-x
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00726-015-2168-x