Abstract
Purpose of Review
In the last decade many studies have suggested an association between the altered gut microbiota and multiple systemic diseases including diabetes. In this review, we will discuss potential pathophysiological mechanisms, the latest findings regarding the mechanisms linking gut dysbiosis and type 2 diabetes (T2D), and the results obtained with experimental modulation of microbiota.
Recent Findings
In T2D, gut dysbiosis contributes to onset and maintenance of insulin resistance. Different strategies that reduce dysbiosis can improve glycemic control.
Summary
Evidence in animals and humans reveals differences between the gut microbial composition in healthy individuals and those with T2D. Changes in the intestinal ecosystem could cause inflammation, alter intestinal permeability, and modulate metabolism of bile acids, short-chain fatty acids and metabolites that act synergistically on metabolic regulation systems contributing to insulin resistance. Interventions that restore equilibrium in the gut appear to have beneficial effects and improve glycemic control. Future research should examine in detail and in larger studies other possible pathophysiological mechanisms to identify specific pathways modulated by microbiota modulation and identify new potential therapeutic targets.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
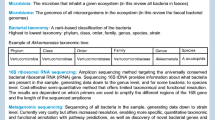
Trillions of microorganisms reside in the human gut in a complex ecosystem which operates as a “hidden organ” [1]. This microbial community and its genome (microbiome) include not only bacteria but also protozoans, viruses, and archaea collectively termed microbiota.
Gut microbiota exerts diverse physiological features such as modulation of immune and inflammatory response; regulation of neuronal signaling; regulation of integrity and mobility of the gut barrier; biosynthesis of vitamins, steroid hormones, and neurotransmitters; and metabolism of branched-chain aromatic amino acids, bile salts, and drugs [2].
In the last decades, improvement of analytical methods allowed researchers to show that alteration of microbiota is associated with many human diseases: gastrointestinal diseases [3], cancer [4], metabolic disease [5, 6], neurodegenerative disorders [7], cardiovascular [8], renal [9], and lung diseases [10]. Although experimental data in mice support the hypothesis of a possible causal role in the etiology of these diseases, human data that favor causality are often insufficient or conflicting.
T2D is thought to arise at the intersection of genetic factors, sedentary lifestyle, poor diet, excessive visceral obesity, and other environmental exposures throughout life [11]. While the precise causes of disease are not completely clear, increasing evidence supports a role for the intestinal microbiota in development of T2DM [12••]; however, the pathophysiological mechanisms that link the microbiota to T2D have not been well elucidated.
In this review, we provide an overview of the most recent findings, with the aim to understand more about pathophysiology and identify new potential therapeutic approaches.
Gut Microbiota: a Dynamic Ecosystem
Analytical Methods
Since it is very difficult to identify intestinal microorganisms through culture-based methods, alternative techniques allow a much more comprehensive mapping of bacteria. For the study of microbial DNA from fecal samples, considered representative of the distal gut microbiota composition, culture-independent methods have benefited from evolution of next-generation sequencing technology, such as 16S ribosomal RNA gene amplicon sequencing and shotgun metagenomics sequencing [13].
The 16S rRNA gene sequencing provides information on the composition of microbial communities. With this method, polymerase chain reaction (PCR) is used to amplify a specific region in the 16S gene; this product is subsequently sequenced. By contrast, shotgun metagenomics sequencing is able to analyze the entire genomic content of a community, by using direct sequencing of microbial RNA without prior amplification. A subsequent taxonomic assignment requires assembly tools and updated databases [14]. In recent years, both methods have improved substantially, with increased throughput and reduced costs. However, specific bioinformatics tools and up-to-date databases continue to evolve. Although each method has its own advantages and limitations, new data suggest that shotgun sequencing provides a higher resolution representation of the microbial composition and allows better characterization of complexity as compared to 16S rRNA amplicon sequencing [15]. Further studies comparing the two methods are required.
Microbial Changes in Humans with T2D
Although the human gut microbiota composition differs in different parts of intestinal tract, six main phyla are dominant: Firmicutes, Bacteroidetes, Actinobacteria, Fusobacteria, Verucomicrobia, and Proteobacteria [16•]. Over 90% of the 1000 prevailing bacterial species belong to the Firmicutes and Bacteroidetes phyla. Recent reports show that interindividual variation in the composition of communities is very high, potentially related to age, diet, illness, genetic and environmental factors, and medication [17••, 18••].
The first study describing a substantial difference in the composition of gut microbiota between individuals with T2D and healthy individuals dates back to 2010 [19]. In this small study from Denmark, the authors analyzed the fecal bacterial composition of 18 men without and with T2D using 16S rRNA amplicon sequencing. T2D was associated with changes in the intestinal microbiota composition (dysbiosis) at a phylum level, with a reduction in the proportion of Firmicutes and a slight increase in Bacteroidetes and Proteobacteria. However, these results were not confirmed in two large metagenome-wide association studies conducted in China and Europe [20, 21]; moderate dysbiosis was observed in T2D but the differential microbial composition varied between two studies. This could be due to ethnic and dietary heterogeneity in the populations studied, differences in antidiabetic drugs or other medications, or disease status, as well as different sequencing techniques used. Nonetheless, both the Chinese and European studies found butyrate-producing bacteria (Roseburia intestinalis and Faecalibacterium prausnitzii) concentrations lower in T2D while certain Lactobacillus species and some opportunistic pathogens, such as Bacteroides caccae, Clostridium hathewayi, Clostridium ramosum, Clostridium symbiosum, and E. coli, were higher in T2D. Increased expression of the microbial genes involved in oxidative stress and the pro-inflammatory state typical of T2D was also observed in the two larger studies, but not the smaller Danish study [22].
Using 16S rRNA-based high-throughput sequencing analysis, Zhang et al. [23] found decreased abundance of Akkermansia muciniphila inindividuals with prediabetes and newly diagnosed T2D suggesting that low concentrations of this bacteria in the gut could be a biomarker for glucose intolerance [24]. A. muciniphila is a mucin-degrading bacterium that colonizes the intestinal mucous layer and constitutes 3–5% of the human intestinal microbial composition. Interestingly, daily treatment with viable A. muciniphila in mice with dietary obesity yielded decreased metabolic endotoxemia, insulin resistance, adipose tissue macrophage infiltration, and improvement in fasting glycemia [25].
Another study of Danish individuals with insulin resistance demonstrated increases in serum levels of branched-chain amino acid (BCAA), potentially linked to both increased production by intestinal microorganisms (Prevotellacopri and Bacteroides vulgatus) and reduced transport within the bacterial cell [26]. This is intriguing, as increased plasma BCAA are associated with a greater future probability of developing insulin resistance and T2D in both children and adults [27, 28]. Thus, these data support the hypothesis that the intestinal microbiota could play a fundamental role in systemic metabolism and insulin resistance.
Stool analysis of 50 individuals with T2D from Japan showed both increased total counts of Lactobacillus, together with a reduction of Clostridium coccoides and Prevotellaas compared with the control group. Intestinal bacteria were also found in the blood in patients with T2D, suggesting a translocation from the intestine to the bloodstream [29].
Recent studies based on the analysis of 16S rRNA gene using next-generation sequencing (Illumina MiSeq) found that Firmicutes/Bacteroidetes ratio in patients with T2D was significantly higher than in controls [11, 30]. These results are in contrast with those obtained in Danish, Chinese, and European studies in which patients with T2D had a lower Firmicutes/Bacteroidetes ratio compared to controls. Egshatyan et al. [30] identified Blautia as the most represented genus; its representation was higher in patients with T2D and prediabetes than in subjects with normal glucose tolerance. It is noteworthy that some Clostridia and Blautia coccoides can stimulate the secretion of TNFα and inflammatory cytokines to a greater extent than LPS [31].
In summary, the results to date suggest that patients with T2D show evidence of gut dysbiosis. Discrepancies between studies are numerous, probably due to various confounding factors such as different study populations, different sequencing techniques used, and differences in dietary intake and medication use. Large studies that take into account these different variables are necessary. A cross-sectional and observational prospective study in patients with T2D is ongoing ( ClinicalTrials.gov ID: NCT03204799).
Bacteria, Metabolities, and Host Interactions
In the last 10 years, low-grade inflammation has been hypothesized to be the link between microbiome and T2D risk, via mechanisms related to bacterial toxins, short-chain fatty acids, bile acids and BCAA metabolism (Fig. 1).
Influence of the gut microbiota in promoting insulin resistance and T2D. TLR-4 Toll-like receptor 4, MyD88 myeloid differentiation protein 88, TAK1 transforming growth factor B-associated kinase 1, GPR43 G-protein-coupled receptor 43, GPR41 G-protein-coupled receptor 41, TMAO trimethylamine N-oxide, FMO3 flavin monooxygenase 3, LPS lipopolysaccharides, NF-kB nuclear factor-kappa B, GLP-2 glucagon-like-peptide 2, IL interleukin, TNF tumor necrosis factor, eNOS endothelial nitric oxide synthase, MCP-1 monocyte chemoattractant protein-1, GLP-1 glucagon-like peptide-1, IRS insulin receptor substrate, ZO-1 zonula occludens-1, PYY intestinal peptide YY, TGR5 G-protein-coupled bile acid receptor 1, FXR farnesoid X receptor, Fgf15 fibroblast growth factor 15, GIP glucose-dependent insulinotropic polypeptide, CB endocannabinoid receptor, eCB endocannabinoid (yellow circles), SCFAs short-chain fatty acids (blue circles), BCAA branched-chain amino acids (green circles)
Low-Grade Inflammation and Bacterial Toxins
Animal and human studies suggested that a high-fat diet (HFD) can change the intestinal ecosystem and increase the circulating levels of proinflammatory mediators. Caniet al. [32] defined “metabolic endotoxemia” as a condition characterized by a two- to threefold increase in circulating lipopolysaccharide (LPS) levels; this may result in low-grade systemic inflammation and contribute to insulin resistance. LPS is a component of the gram-negative bacterial wall which can activate local immune response via high-affinity binding to specific receptors (e.g., Toll-like receptors (TLRs), the NLRP3 inflammasome and NOD like receptors (NLRs)) expressed at high levels on the surface of macrophages and dendritic cells [33]. In blood and tissues, LPS also activates the TLR4/MyD88/NF-κB pathway, triggering an inflammatory response through release of pro-inflammatory molecules TNF-α, IL-1, IL-6, and iNOS. With activation of this inflammatory cascade, activated serine kinases (JNK and IKK) can induce IRS (insulin receptor substrate) serine phosphorylation, which inhibits insulin signaling, resulting in cellular insulin resistance (IR) [34]. In human muscle cell lines TLR4 inhibitors suppressed inflammation and decreased LPS-induced insulin resistance [35].
N-acetyl cysteine (NAC) is a potent antioxidant that exerts anti-inflammatory activity via inhibition of NF-kB, while reducing glucose intolerance and insulin resistance in T2D and inhibiting the growth and adhesion of some pathogens [36]. Zheng et al. recently evaluated the effects of NAC (1 mg/mL, in drinking water) on the microbiota of HFD-fed mice. After 5 months of treatment, NAC improved glucose tolerance and reduced fasting glucose, body weight, and plasma endotoxin levels, while increasing the prevalence of beneficial bacteria such as Akkermansia, Lactobacillus, and Bifidobacterium [37•]. Since systemic levels of NAC were not measured, the precise site of action is uncertain.
Patients with T2D have higher blood levels of LPS (a component of the gram-negative bacterial wall) compared to healthy subjects. This may seem like a paradox, because in the microbiota of patients with T2D, there is a decrease in the percentage of gram-negative and increase in gram-positive Firmicutes. The explanation is that high endotoxemia is directly related to increase of intestinal permeability [38••]. Increases in LPS may even precede the development of T2D; indeed, the CORDIOPREV study [39••] demonstrated that postprandial LPS levels were higher in individuals who developed T2D over a median of 60 months, as compared with those who remained free of T2D during a median follow-up of 60 months.
Intestinal permeability is usually regulated by tight and adherence junction proteins between intestinal epithelial cells, which create a barrier that prevents bacteria, toxins and intestinal lumen products from reaching the circulation. In mice fed a high-fat diet, reduced expression of zonula occludens-1 (ZO-1), occludin, and claudin-1 leads increased translocation of bacteria and LPS into the circulation [40]. A recent paper showed that in mice with streptozotocin-induced diabetes, hyperglycemia could reduce tight and adherence junction integrity via a direct effect on reprogramming of intestinal epithelial cells through GLUT2-dependent mechanism [41••].
Taken together, these data suggest that hyperglycemia could lead to an increase in intestinal permeability, favoring translocation of proinflammatory bacteria and toxins which in turn impairs glucose metabolism.
Short-Chain Fatty Acids
One mechanism potentially mediating the impact of intestinal dysbiosis to regulate systemic metabolism and T2D risk is related to alterations in short-chain fatty acids (SCFAs). SCFA acetate, propionate, and butyrate are the most abundant microbial metabolites derived from fermentation of non-digestible carbohydrates introduced with diet. SCFAs play diverse roles including cell growth and differentiation, promotion of gut epithelial integrity, anti-inflammatory and immunomodulatory functions [42], and regulation of pancreatic β cell proliferation and insulin biosynthesis [43]. SCFAs have also been shown to modulate intestinal inflammation by Treg cells and influence fluid secretion, motility, and duodenal barrier function through mechanisms that may also involve GLP-2 secretion [44]. SCFA principally bind G-protein-coupled receptors 43 and 41 (GPR43/FFA2 and GPR41/FFA3) expressed not only on enteroendocrine and intestinal epithelial cells but also in the islets of Langerhans [45]. In turn, animal data show that GPR41 regulates intestinal gluconeogenesis, food intake and energy expenditure, and stimulate secretion of the intestinal peptide YY. This regulates appetite and energy intake with direct effects on the central nervous system [46]. Similarly, GPR43 stimulates production of glucagon-like peptide-1 (GLP-1), a gut hormone that increases glucose-dependent insulin secretion and inhibits glucagon secretion [47]. SCFAs can also bind GPR119, another receptor expressed in intestinal L-cells and pancreatic β-cells. GPR119 agonists reduce blood glucose by promoting intestinal secretion of GLP-1, improving pancreatic β-cell function and insulin secretion [48]. Thus, activation of G-protein-coupled receptors by SCFAs may have beneficial effects via reducing food intake, improving insulin sensitivity, inhibiting fat accumulation, and reducing systemic inflammation. Decreases in SCFA-producing bacteria may reduce these beneficial effects and promote the development of insulin resistance and T2D.
Nevertheless, there are animal [49] and human studies [50] in which an increased concentration of SCFAs in feces was associated with higher body weight and fat gain (via GPR41 receptor action) and insulin resistance. The role of SCFAs is thus controversial and needs further investigation in this context.
Bile Acid Metabolism
Intestinal bacteria play an important role in the conversion of primary bile acids to secondary bile acids, and can also influence their composition. However, bile acids, in turn, could regulate the composition of the gut microbiota because of their antimicrobial activity [51]. Previous reports found that bile acid composition is different between control and germ-free mice, and probiotic administration changes gut microbiota composition and increases bile acid deconjugation [52]. Secondary bile acids can stimulate GLP-1 secretion through G-protein-coupled bile acid receptor 1 (TGR5), modulate expression of farnesoid X receptor (FXR) and fibroblast growth factor 15 (Fgf15), thus regulating hepatic glucose metabolism and insulin sensitivity [53].
Branched Chain Amino Acids
Gut microorganisms are a potential source of circulating BCAA through both biosynthesis and by modifying nutrient absorption. Although many of the underlying mechanisms have not yet been identified, several authors suggest that microbial amino acid metabolism may play multiple roles in the genesis of insulin resistance [54]. Human studies have demonstrated that both dietary intake of BCAA and high plasma levels of BCAA are associated with an increased risk of T2D [55]. Multiple mechanisms may contribute to elevations in BCAA in this context. Firstly, insulin resistance may cause reduced suppression of proteolysis [56]. Moreover, obesity and proinflammatory states are linked to reductions in BCAA catabolism in peripheral tissues, potentially mediated at least in part by reduced adiponectin secretion [57]; this effect may precede insulin resistance. BCAA may affect insulin, glucagon, GLP-1 and glucose-dependent insulinotropic polypeptide (GIP) secretion [58].
A latest meta-analysis of three genome-wide association studies provides genetic evidence linking IR with elevated circulating BCAAs levels [59]. While these data do not provide conclusive data about cause and effect relationships, it is important to note that experimental reductions in dietary BCAA results in increased energy expenditure and improved insulin sensitivity in rodents [60].
TMAO
Trimethylamine (TMA) is an organic compound synthesized exclusively by gut microbiota from dietary nutrients including phosphatidylcholine, choline, and carnitine. After being absorbed, it is converted in the liver by flavin monooxygenase 3 (FMO3) to form trimethylamine N-oxide (TMAO). Higher TMAO plasma levels are associated with an increased risk of T2D [61] and cardiovascular disease [9]. Overexpression of FMO3 in human hepatoma cell lines elicited a significant increased glucose production and insulin resistance probably through the PPARα and Kruppel-like factor 15 pathways; in mice, its deletion conferred protection against obesity [62]. In the POUNDS Lost trial [63], the author highlight that dietary changes can modify plasma levels of TMAO, choline and L-carnitine, and their reduction is associated with improved insulin sensitivity.
Endocannabinoid System
Another emerging mechanism involved in intestinal permeability, glucose metabolism, and energy homeostasis is alteration in the endocannabinoid (eCB) system. Gut metabolites can activate several pathways via cannabinoid CB1 and CB2 receptors, an important target in the context of inflammation, T2D, and obesity [64]. In rodents, CB1 receptor blockade improves intestinal barrier function while stimulation of CB2 receptors improves insulin resistance [65].
Microbiota Modulation: a New Therapeutic Strategy for Diabetes?
Diet
More than 10 years ago, the results of the CARDIA study highlighted how high-fat diet and lower consumption of dietary fibers are associated with weight gain and insulin resistance while the consumption of dairy products improved glycemic control [66]. Animal-based diets may reduce the levels of Firmicutes that metabolize the plant-derived polysaccharides and produce beneficial SCFAs [67].
Emerging data indicate that dietary interventions can indeed change the composition of the bacterial community. A meta-analysis evaluated the efficacy of dietary interventions, finding modulation of intestinal microbiota in parallel with improved blood glucose control, as measured by HbA1c, while having little or no effect on fasting blood glucose, fasting insulin, insulin resistance, inflammation, and SCFA levels compared to the control group [68••].
In another recent clinical study, high dietary fiber intake improved hemoglobin HbA1c levels and increased GLP-1 production. Shotgun metagenomics and metabolomic analysis showed increase abundance of SCFA-producing bacteria and lower levels of deleterious metabolites such as indole and hydrogen sulfide [69•]. Therefore, diet represents an important factor contributing to the composition of the intestinal microbiome. However, responses to intervention can vary substantially between individuals; for example, abundance of several Firmicutes species at baseline, predicted the responsiveness to intervention in one study [70]. Large RCT will be required to fully test whether dietary modifications aimed at changing the microbiome could represent a new therapeutic target for the prevention and management of T2D.
Probiotics
Probiotics are defined as “live microorganisms that, when administered in proper amounts, may exert health benefits to the host” [71]. While the type and composition of bacteria in various commercial products differ considerably, the most common probiotic products contain Lactobacillus sp., Enterococcus sp., Bifidobacterium sp., and Streptococcus sp. A promising technique could be to use recombinant bacteria to improve glycemic control: recently, a genetically modified strain of Lactococcus lactis was shown to enhance insulin secretion and improve glucose tolerance in mice [72]. The beneficial effects of probiotics on T2D have been extensively demonstrated in animal studies, with reduction of Firmicutes/Bacteroidetes ratio, increased abundance of SCFA-producing bacteria, decreased levels of inflammatory molecules TNFα, IL-1, IL-6; increased levels of GLP-1; and improved insulin resistance [73]. Furthermore, probiotics reduce inflammatory phenotypes, improve β-cell dysfunction, and can have beneficial effects on the intestinal wall, reducing intestinal permeability and preventing translocation of bacterial LPS [74]. Experimental data suggest also a potential immunomodulatory role: B. infantis can induce T regulatory (Treg) cells, stimulate production of CD25+ lymphocytes, stimulate human dendritic cells (DCs), and induce the production of IL-10 [75].
While the limited studies conducted in humans are generally concordant with animal studies (Table 1), there are some exceptions. Ivey et al. did not find any effect of probiotic supplementation for 6 weeks using a capsule containing L. acidophilus La5 and B. animalis subsp. lactis Bb12 on glycemic parameters in overweight subjects [80]. In another RCT, 31 glucose-tolerant patients were enrolled to evaluate the efficacy of L. reuteri SD5865 administered over 4 weeks; increases in GLP-1 and insulin secretion were found, without changes in insulin sensitivity [82]. More recently, Mobini et al. [84] evaluated the effects of Lactobacillus reuteri DSM 17938 over 12 weeks in patients with T2D on insulin therapy: probiotic supplementation improved insulin sensitivity in a subgroup but did not affect overall glycemic control measured by HbA1c.
Several systematic reviews and meta-analyses concluded that probiotics could have beneficial effects on glycemic control in T2D, but effects on HbA1c, anti-inflammatory and anti-oxidative benefit are inconsistent [89,90,91,92,93]. Limitations of the RCT conducted thus far include: heterogeneity of the groups studied (ethnicity, metabolic state, drugs, duration of diabetes), different bacterial strains used, short period of treatment, different methods of analysis, and small sample sizes. Therefore, given the considerable disparities in both the design and findings of the studies, and substantial interindividual variation in response to probiotic integration, future long-term, multi-center RCT utilizing consistent methods will be required to determine their usefulness as prevention or as synergistic approach in T2D treatment. Several trials are ongoing (IRCT201511032321N2; ACTRN12613001378718).
Fecal Transplantation
Fecal microbiota transplant (FMT) consists of administering fecal matter, taken from a healthy donor, via endoscopy or enema. FMT is a technique that has produced good results in the treatment of Clostridium difficile infection when medical therapy is ineffective, and it is a promising treatment for a variety of diseases [94]. Thus far, there has been only one human study evaluating the effects of FMT in patients with metabolic syndrome [95]. In this work, FMT from healthy subjects to adults with metabolic syndrome led to increased butyrate-producing bacteria in the stool of the recipient microbiota and improvement in peripheral insulin sensitivity. This study, while promising, was limited by small sample size and absence of data on glycemic control and inflammation markers. Given the limited data available at present, future studies will be required to fully define the adverse effects of such treatment, including transplantation of potentially pathogenic microorganisms, and to critically evaluate the risk/benefit ratio. Several RCTs are ongoing (ChiCTR1800014569; NCT03127696; NCT01790711; NTR 5141). Ultimately, it is hoped that defining the microbiota mediating beneficial effects will allow administration of cultured bacterial treatments.
Impact of Diabetes Treatments on the Microbiome
Different drugs, including antidiabetic medications, can affect the intestinal microbiota [96].
Metformin, currently the cornerstone of T2D treatment, has long been recognized to improve insulin sensitivity and reduce hepatic glucose production [97]; it also alters the composition of the microbiota: increase abundance of A. muciniphila, Lactobacillus, and Escherichia spp. and decrease abundance of some pathogens [98]. Metformin also promotes the production of SCFAs, regulates bile acid turnover, improves intestinal permeability, reduces endotoxin levels, and stimulates the activity of endocrine cells by enhancing release of GLP-1 and PYY peptides [99].
Incretin-based therapies can also affect the composition of the microbiota in rodents, but results differ across studies. In mice fed a HFD, the GLP1RA liraglutide reduces Bacteroidetes, Proteobacteria, and Actinobacteria and increases Firmicutes abundance. Similar results were obtained in obese rats after treatment with saxagliptin. On the contrary, in HFD-fed mice sitagliptin induces an increase in the relative abundance of Bacteroidetes and Proteobacteria and decrease in Firmicutes [100]. It is not clear whether these discrepancies are due to the model (rat vs. mouse) or to the drug. The effect of DPP-4i on the microbiota could be related to an enhancement of intestinotrophic effect of GLP-2, which improves intestinal mucosal barrier integrity and thus reduces permeability.
SGLT2 inhibitors may also impact the microbiome. In db/db mice, treatment with SGLT2i yields an anti-inflammatory effect and increases SCFA levels in cecum [9]. There are no published data on humans thus far.
Various studies to evaluate changes in the composition of the intestinal microbiota before and after the use of diabetes medications agents are underway (eudract_number: 2015-000199-86; ChiCTR-OPC-17010757; ClinicalTrials.gov ID: NCT02900417; ChiCTR-OPC-17010757).
Bariatric Surgery
Bariatric surgery has proved to be one of the most effective interventions for severe obesity. Moreover, there are several weight loss-independent effects of “metabolic surgery” including beneficial effects on intestinal glucose metabolism, insulin sensitivity, β-cell function, changes in bile acids, and gut microbiota composition [101]. A recent systematic review of 12 animal and 9 clinical studies [102] demonstrated an increase of Bacteroidetes, Fusobacteria, Verrucomicrobia, Proteobacteria, and a decrease of Firmicutes, Clostridiaceae, Clostridiales, Blautia, and Dorea. Three studies showed an increase in abundance of A. muciniphila. The mechanisms responsible for these changes are unknown but may include intestinal remodeling, antibiotic use, and dietary changes.
Conclusion
In recent years, the study of human gut microbiota has led to interesting discoveries that open the frontiers for innovative treatments for many diseases including T2D. Available data suggest that human microbiota plays an important role in the onset and maintenance of insulin resistance in patients with T2D. Given the personal and societal impact of T2D worldwide, large-scale randomized trials will be required to fully assess whether microbiome modulation may be a therapeutic option to improve glycemic control and reduce the risk of complications.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Harsch IA, Konturek PC. The role of gut microbiota in obesity and type 2 and type 1 diabetes mellitus: new insights into “old” diseases. Med Sci (Basel). 2018 ;6(2). https://doi.org/10.3390/medsci6020032.
Lynch SV, Pedersen O. The human intestinal microbiome in health and disease. N Engl J Med. 2016;375(24):2369–79.
Tong M, Li X, Wegener Parfrey L, Roth B, Ippoliti A, Wei B, et al. A modular organization of the human intestinal mucosal microbiota and its association with inflammatory bowel disease. PLoS One. 2013;8:e80702.
Garrett WS. Cancer and the microbiota. Science. 2015;348:80–6.
Musso G, Gambino R, Cassader M. Obesity, diabetes, and gut microbiota: the hygiene hypothesis expanded? Diabetes Care. 2010;33(10):2277–84.
Musso G, Gambino R, Cassader M. Interactions between gut microbiota and host metabolism predisposing to obesity and diabetes. Annu Rev Med. 2011;62:361–80.
Hsiao EY, McBride SW, Hsien S, et al. Microbiota modulate behavioral and physiological abnormalities associated with neurodevelopmental disorders. Cell. 2013;155:1451–63.
Wang Z, Klipfell E, Bennett BJ, Koeth R, Levison BS, DuGar B, et al. Gut flora metabolism of phosphatidylcholine promotes cardiovascular disease. Nature. 2011;472:57–63.
Sircana A, De Michieli F, Parente R, Framarin L, Leone N, Berrutti M, Paschetta E, Bongiovanni D, Musso G. Gut microbiota, hypertension and chronic kidney disease: recent advances. Pharmacol Res. 2018. https://doi.org/10.1016/j.phrs.2018.01.013.
Cui L, Morris A, Huang L, Beck JM, Twigg HL 3rd, von Mutius E, et al. The microbiome and the lung. Ann Am Thorac Soc. 2014;11(Suppl 4):S227–32. https://doi.org/10.1513/AnnalsATS.201402-052PL.
Salamon D, Sroka-Oleksiak A, Kapusta P, Szopa M, Mrozińska S, Ludwig-Słomczyńska AH, et al. Characteristics of the gut microbiota in adult patients with type 1 and 2 diabetes based on the analysis of a fragment of 16S rRNA gene using next-generation sequencing. Pol Arch Intern Med. 2018; https://doi.org/10.20452/pamw.4246.
•• Cani PD, Neyrinck AM, Fava F, et al. Selective increases of bifidobacteria in gut microflora improve high-fat-diet-induced diabetes in mice through a mechanism associated with endotoxaemia. Diabetologia. 2007;50(11):2374–83. The first paper describing a possible link between gut microbiota and type 2 diabetes.
D'Argenio V. Human microbiome acquisition and bioinformatic challenges in metagenomic studies. Int J Mol Sci. 2018;19(2). https://doi.org/10.3390/ijms19020383.
Jovel J, Patterson J, Wang W, Hotte N, O'Keefe S, Mitchel T, et al. Characterization of the gut microbiome using 16S or shotgun metagenomics. Front Microbiol. 2016;7:459. https://doi.org/10.3389/fmicb.2016.00459.
Laudadio I, Fulci V, Palone F, Stronati L, Cucchiara S, Carissimi C. Quantitative assessment of shotgun metagenomics and 16S rDNA amplicon sequencing in the study of human gut microbiome. OMICS. 2018;22(4):248–54. https://doi.org/10.1089/omi.2018.0013.
• Human Microbiome Project Consortium. Structure, function and diversity of the healthy human microbiome. Nature. 2012;486(7402):207–14. https://doi.org/10.1038/nature11234. Report that delineates the range of structural and functional configurations of microbial communities in healthy population.
•• Falony G, Joossens M, Vieira-Silva S, Wang J, Darzi Y, Faust K, et al. Population-level analysis of gut microbiome variation. Science. 2016;352(6285):560–4. https://doi.org/10.1126/science.aad3503. The first two population-based studies published on gut microbiota.
•• Zhernakova A, Kurilshikov A, Bonder MJ, et al. Populationbased metagenomics analysis reveals markers for gut microbiome composition and diversity. Science. 2016;352(6285):565–9. https://doi.org/10.1126/science.aad3369. The first two population-based studies published on gut microbiota.
Larsen N, Vogensen FK, van den Berg FW, Nielsen DS, Andreasen AS, Pedersen BK, et al. Gut microbiota in human adults with type 2 diabetes differs from non-diabetic adults. PLoS One. 2010;5(2):e9085. https://doi.org/10.1371/journal.pone.0009085.
Qin J, Li Y, Cai Z, Li S, Zhu J, Zhang F, et al. A metagenome-wide association study of gut microbiota in type 2 diabetes. Nature. 2012;490(7418):55–60. https://doi.org/10.1038/nature11450.
Karlsson FH, Tremaroli V, Nookaew I, Bergström G, Behre CJ, Fagerberg B, et al. Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature. 2013;498(7452):99–103. https://doi.org/10.1038/nature12198.
Tilg H, Moschen AR. Microbiota and diabetes: an evolving relationship 2014;63(9):1513–21. https://doi.org/10.1136/gutjnl-2014-306928.
Zhang X, Shen D, Fang Z, Jie Z, Qiu X, Zhang C, et al. Human gut microbiota changes reveal the progression of glucose intolerance. PLoS One. 2013;8(8):e71108. https://doi.org/10.1371/journal.pone.0071108.
Yassour M, Lim MY, Yun HS, Tickle TL, Sung J, Song YM, et al. Sub-clinical detection of gut microbial biomarkers of obesity and type 2 diabetes. Genome Med. 2016;8(1):17. https://doi.org/10.1186/s13073-016-0271-6.
Everard A, Belzer C, Geurts L, Ouwerkerk JP, Druart C, Bindels LB, et al. Cross-talk between Akkermansia muciniphila and intestinal epithelium controls diet-induced obesity. Proc Natl Acad Sci U S A. 2013;110(22):9066–71. https://doi.org/10.1073/pnas.1219451110.
Pedersen HK, Gudmundsdottir V, Nielsen HB, Hyotylainen T, Nielsen T, Jensen BA, et al. Human gut microbes impact host serum metabolome and insulin sensitivity. Nature. 2016;535(7612):376–81.
McCormack SE, Shaham O, McCarthy MA, Deik AA, Wang TJ, Gerszten RE, et al. Circulating branched-chain amino acid concentrations are associated with obesity and future insulin resistance in children and adolescents. Pediatr Obes. 2013;8(1):52–61. https://doi.org/10.1111/j.2047-6310.2012.00087.x.
Wang TJ, Larson MG, Vasan RS, Cheng S, Rhee EP, McCabe E, et al. Metabolite profiles and the risk of developing diabetes. Nat Med. 2011;17(4):448–53. https://doi.org/10.1038/nm.2307.
Sato J, Kanazawa A, Ikeda F, Yoshihara T, Goto H, Abe H, et al. Gut dysbiosis and detection of "live gut bacteria" in blood of Japanese patients with type 2 diabetes. Diabetes Care. 2014;37(8):2343–50. https://doi.org/10.2337/dc13-2817.
Egshatyan L, Kashtanova D, Popenko A, Tkacheva O, Tyakht A, Alexeev D, et al. Gut microbiota and diet in patients with different glucose tolerance. Endocr Connect. 2016;5(1):1–9. https://doi.org/10.1530/EC-15-0094.
Tuovinen E, Keto J, Nikkilä J, Mättö J, Lähteenmäki K. Cytokine response of human mononuclear cells induced by intestinal Clostridium species. Anaerobe. 2013;19:70–6. https://doi.org/10.1016/j.anaerobe.2012.11.002.
Cani PD, Amar J, Iglesias MA, Poggi M, Knauf C, Bastelica D, et al. Metabolic endotoxemia initiates obesity and insulin resistance. Diabetes. 2007;56(7):1761–72.
Li X, Watanabe K, Kimura I. Gut microbiota dysbiosis drives and implies novel therapeutic strategies for diabetes mellitus and related metabolic diseases. Front Immunol. 2017;8:1882. https://doi.org/10.3389/fimmu.2017.01882.
Saad MJ, Santos A, Prada PO. Linking gut microbiota and inflammation to obesity and insulin resistance. Physiology (Bethesda). 2016;31(4):283–93. https://doi.org/10.1152/physiol.00041.2015.
Liang H, Hussey SE, Sanchez-Avila A, Tantiwong P, Musi N. Effect of lipopolysaccharide on inflammation and insulin action in human muscle. PLoS One. 2013;8(5):e63983. https://doi.org/10.1371/journal.pone.0063983.
Lasram MM, Dhouib IB, Annabi A, El Fazaa S, Gharbi N. A review on the possible molecular mechanism of action of N-acetylcysteine against insulin resistance and type-2 diabetes development. Clin Biochem. 2015;48(16–17):1200–8. https://doi.org/10.1016/j.clinbiochem.2015.04.017.
• Zheng J, Yuan X, Zhang C, Jia P, Jiao S, Zhao X, et al. N-Acetyl-cysteine alleviates gut dysbiosis and glucose metabolic disorder in high-fat diet-induced mice. J Diabetes. 2018; https://doi.org/10.1111/1753-0407.12795. The first study evaluating the potential effects of NAC on microbiota in T2DM.
•• Horton F, Wright J, Smith L, Hinton PJ, Robertson MD. Increased intestinal permeability to oral chromium (51 Cr)-EDTA in human type 2 diabetes. Diabet Med. 2014;31(5):559–63. https://doi.org/10.1111/dme.12360. The first demonstration that increased intestinal permeability may be a feature of human Type 2 diabetes.
•• Camargo A, Jimenez-Lucena R, Alcala-Diaz JF, Rangel-Zuñiga OA, Garcia-Carpintero S, Lopez-Moreno J, et al. Postprandial endotoxemia may influence the development of type 2 diabetes mellitus: from the CORDIOPREV study. Clin Nutr. 2018; https://doi.org/10.1016/j.clnu.2018.03.016. Recent study that shows high levels of LPS could precede the development of T2DM.
Cani PD, Bibiloni R, Knauf C, Waget A, Neyrinck AM, Delzenne NM, et al. Changes in gut microbiota control metabolic endotoxemia-induced inflammation in high-fat diet-induced obesity and diabetes in mice. Diabetes. 2008;57:1470–81.
•• Thaiss CA, Levy M, Grosheva I, Zheng D, Soffer E, Blacher E, et al. Hyperglycemia drives intestinal barrier dysfunction and risk for enteric infection. Science. 2018;359(6382):1376–83. https://doi.org/10.1126/science.aar3318. This study proposes a new mechanism responsible for increasing intestinal permeability.
Tan J, McKenzie C, Potamitis M, Thorburn AN, Mackay CR, Macia L. The role of short-chain fatty acids in health and disease. Adv Immunol. 2014;121:91–119. https://doi.org/10.1016/B978-0-12-800100-4.00003-9.
Tang C, Ahmed K, Gille A, Lu S, Gröne HJ, Tunaru S, et al. Loss of FFA2 and FFA3 increases insulin secretion and improves glucose tolerance in type 2 diabetes. Nat Med. 2015;21(2):173–7. https://doi.org/10.1038/nm.3779.
Wan Saudi WS, Sjöblom M. Short-chain fatty acids augment rat duodenal mucosal barrier function. Exp Physiol. 2017;102(7):791–803. https://doi.org/10.1113/EP086110.
Priyadarshini M, Navarro G, Layden BT. Gut microbiota: FFAR reaching effects on islets. Endocrinology. 2018;159(6):2495–505. https://doi.org/10.1210/en.2018-00296.
Chambers ES, Viardot A, Psichas A, Morrison DJ, Murphy KG, Zac-Varghese SE, et al. Effects of targeted delivery of propionate to the human colon on appetite regulation, body weight maintenance and adiposity in overweight adults. Gut. 2015;64(11):1744–54. https://doi.org/10.1136/gutjnl-2014-307913.
Grasset E, Puel A, Charpentier J, Collet X, Christensen JE, Tercé F, et al. A specific gut microbiota dysbiosis of type 2 diabetic mice induces GLP-1 resistance through an enteric NO-dependent and gut-brain axis mechanism. Cell Metab. 2017;25(5):1075–1090.e5. https://doi.org/10.1016/j.cmet.2017.04.013.
Mandøe MJ, Hansen KB, Hartmann B, Rehfeld JF, Holst JJ, Hansen HS. The 2-monoacylglycerol moiety of dietary fat appears to be responsible for the fat-induced release of GLP-1 in humans. Am J Clin Nutr. 2015;102(3):548–55. https://doi.org/10.3945/ajcn.115.106799.
Turnbaugh PJ, Ley RE, Mahowald MA, Magrini V, Mardis ER, Gordon JI. An obesity-associated gut microbiome with increased capacity for energy harvest. Nature. 2006;444(7122):1027–31.
Teixeira TF, Grześkowiak Ł, Franceschini SC, Bressan J, Ferreira CL, Peluzio MC. Higher level of faecal SCFA in women correlates with metabolic syndrome risk factors. Br J Nutr. 2013;109(5):914–9. https://doi.org/10.1017/S0007114512002723.
Fiorucci S, Distrutti E. Bile acid-activated receptors, intestinal microbiota, and the treatment of metabolic disorders. Trends Mol Med. 2015;21(11):702–14. https://doi.org/10.1016/j.molmed.2015.09.001.
Yang JY, Kweon MN. The gut microbiota: a key regulator of metabolic diseases. BMB Rep. 2016;49(10):536–41.
Pathak P, Xie C, Nichols RG, Ferrell JM, Boehme S, Krausz KW, et al. Intestine farnesoid X receptor agonist and the gut microbiota activate G-protein bile acid receptor-1 signaling to improve metabolism. Hepatology. 2018; https://doi.org/10.1002/hep.29857.
Neis EP, Dejong CH, Rensen SS. The role of microbial amino acid metabolism in host metabolism. Nutrients. 2015;7(4):2930–46. https://doi.org/10.3390/nu7042930.
Asghari G, Farhadnejad H, Teymoori F, Mirmiran P, Tohidi M, Azizi F. High dietary intake of branched-chain amino acids is associated with an increased risk of insulin resistance in adults. J Diabetes. 2018;10(5):357–64. https://doi.org/10.1111/1753-0407.12639.
Giesbertz P, Daniel H. Branched-chain amino acids as biomarkers in diabetes. Curr Opin Clin Nutr Metab Care. 2016;19(1):48–54. https://doi.org/10.1097/MCO.0000000000000235.
Lian K, Du C, Liu Y, Zhu D, Yan W, Zhang H, et al. Impaired adiponectin signaling contributes to disturbed catabolism of branched-chain amino acids in diabetic mice. Diabetes. 2015;64(1):49–59. https://doi.org/10.2337/db14-0312.
Gojda J, Straková R, Plíhalová A, Tůma P, Potočková J, Polák J, et al. Increased Incretin but not insulin response after oral versus intravenous branched chain amino acids. Ann Nutr Metab. 2017;70(4):293–302. https://doi.org/10.1159/000475604.
Wang Q, Holmes MV, Davey Smith G, Ala-Korpela M. Genetic support for a causal role of insulin resistance on circulating branched-chain amino acids and inflammation. Diabetes Care. 2017;40(12):1779–86. https://doi.org/10.2337/dc17-1642.
Bloomgarden Z. Diabetes and branched-chain amino acids: what is the link? J Diabetes. 2018;10(5):350–2. https://doi.org/10.1111/1753-0407.12645.
Shan Z, Sun T, Huang H, Chen S, Chen L, Luo C, et al. Association between microbiota-dependent metabolite trimethylamine-N-oxide and type 2 diabetes. Am J Clin Nutr. 2017;106(3):888–94. https://doi.org/10.3945/ajcn.117.157107.
Shih DM, Wang Z, Lee R, Meng Y, Che N, Charugundla S, et al. Flavin containing monooxygenase 3 exerts broad effects on glucose and lipid metabolism and atherosclerosis. J Lipid Res. 2015;56(1):22–37. https://doi.org/10.1194/jlr.M051680.
Heianza Y, Sun D, Li X, DiDonato JA, Bray GA, Sacks FM, et al. Gut microbiota metabolites, amino acid metabolites and improvements in insulin sensitivity and glucose metabolism: the POUNDS Lost trial. Gut. 2018; https://doi.org/10.1136/gutjnl-2018-316155.
Richey JM, Woolcott O. Re-visiting the Endocannabinoid system and its therapeutic potential in obesity and associated diseases. Curr Diab Rep. 2017;17(10):99. https://doi.org/10.1007/s11892-017-0924-x.
Cani PD, Plovier H, Van Hul M, Geurts L, Delzenne NM, Druart C, et al. Endocannabinoids—at the crossroads between the gut microbiota and host metabolism. Nat Rev Endocrinol. 2016;12(3):133–43. https://doi.org/10.1038/nrendo.2015.211.
Pereira MA, Kartashov AI, Ebbeling CB, Van Horn L, Slattery ML, Jacobs DR Jr, et al. Fast-food habits, weight gain, and insulin resistance (the CARDIA study): 15-year prospective analysis. Lancet. 2005;365(9453):36–42.
David LA, Maurice CF, Carmody RN, Gootenberg DB, Button JE, Wolfe BE, et al. Diet rapidly and reproducibly alters the human gut microbiome. Nature. 2014;505(7484):559–63. https://doi.org/10.1038/nature12820.
•• Houghton D, Hardy T, Stewart C, Errington L, Day CP, Trenell MI, et al. Systematic review assessing the effectiveness of dietary intervention on gut microbiota in adults with type 2 diabetes. Diabetologia. 2018; https://doi.org/10.1007/s00125-018-4632-0. An up-to-date review on the role of diet in modulating the microbiota and improving diabetes management.
• Zhao L, Zhang F, Ding X, Wu G, Lam YY, Wang X, et al. Gut bacteria selectively promoted by dietary fibers alleviate type 2 diabetes. Science. 2018;359(6380):1151–6. https://doi.org/10.1126/science.aao5774. Later study that confirms diet as additional approach for the management of DM2.
Smith PM, Howitt MR, Panikov N, Michaud M, Gallini CA, Bohlooly-Y M, et al. The microbial metabolites, short-chain fatty acids, regulate colonic Treg cell homeostasis. Science. 2013;341(6145):569–73. https://doi.org/10.1126/science.1241165.
Sanders ME. Probiotics: definition, sources, selection, and uses. Clin Infect Dis. 2008;46:S58–61.
Brunkwall L, Orho-Melander M. The gut microbiome as a target for prevention and treatment of hyperglycaemia in type 2 diabetes: from current human evidence to future possibilities. Diabetologia. 2017;60(6):943–51. https://doi.org/10.1007/s00125-017-4278-3.
Li X, Wang E, Yin B, Fang D, Chen P, Wang G, et al. Effects of Lactobacillus casei CCFM419 on insulin resistance and gut microbiota in type 2 diabetic mice. Benef Microbes. 2017;8(3):421–32. https://doi.org/10.3920/BM2016.0167.
Tian P, Li B, He C, Song W, Hou A, Tian S, et al. Antidiabetic (type 2) effects of Lactobacillus G15 and Q14 in rats through regulation of intestinal permeability and microbiota. Food Funct. 2016;7(9):3789–97.
Daliri EB, Lee BH, Oh DH. Current perspectives on antihypertensive probiotics. Probiotics Antimicrob Proteins. 2017;9(2):91–101.
Andreasen AS, Larsen N, Pedersen-Skovsgaard T, Berg RM, Møller K, Svendsen KD, et al. Effects of Lactobacillus acidophilus NCFM on insulin sensitivity and the systemic inflammatory response in human subjects. Br J Nutr. 2010;104(12):1831–8. https://doi.org/10.1017/S0007114510002874.
Ejtahed HS, Mohtadi-Nia J, Homayouni-Rad A, Niafar M, Asghari-Jafarabadi M, Mofid V. Probiotic yogurt improves antioxidant status in type 2 diabetic patients. Nutrition. 2012;28(5):539–43. https://doi.org/10.1016/j.nut.2011.08.013.
Asemi Z, Zare Z, Shakeri H, Sabihi SS, Esmaillzadeh A. Effect of multispecies probiotic supplements on metabolic profiles, hs-CRP, and oxidative stress in patients with type 2 diabetes. Ann Nutr Metab. 2013;63(1–2):1–9. https://doi.org/10.1159/000349922.
Mazloom Z, Yousefinejad A, Dabbaghmanesh MH. Effect of probiotics on lipid profile, glycemic control, insulin action, oxidative stress, and inflammatory markers in patients with type 2 diabetes: a clinical trial. Iran J Med Sci. 2013;38(1):38–43.
Ivey KL, Hodgson JM, Kerr DA, Lewis JR, Thompson PL, Prince RL. The effects of probiotic bacteria on glycaemic control in overweight men and women: a randomised controlled trial. Eur J Clin Nutr. 2014;68(4):447–52. https://doi.org/10.1038/ejcn.2013.294.
Ostadrahimi A, Taghizadeh A, Mobasseri M, Farrin N, Payahoo L, Beyramalipoor Gheshlaghi Z, et al. Effect of probiotic fermented milk (kefir) on glycemic control and lipid profile in type 2 diabetic patients: a randomized double-blind placebo-controlled clinical trial. Iran J Public Health. 2015;44(2):228–37.
Simon MC, Strassburger K, Nowotny B, Kolb H, Nowotny P, Burkart V, et al. Intake of Lactobacillus reuteri improves incretin and insulin secretion in glucose-tolerant humans: a proof of concept. Diabetes Care. 2015;38(10):1827–34. https://doi.org/10.2337/dc14-2690.
Firouzi S, Majid HA, Ismail A, Kamaruddin NA, Barakatun-Nisak MY. Effect of multi-strain probiotics (multi-strain microbial cell preparation) on glycemic control and other diabetes-related outcomes in people with type 2 diabetes: a randomized controlled trial. Eur J Nutr. 2017;56(4):1535–50. https://doi.org/10.1007/s00394-016-1199-8.
Mobini R, Tremaroli V, Ståhlman M, Karlsson F, Levin M, Ljungberg M, et al. Metabolic effects of lactobacillus reuteri DSM 17938 in people with type 2 diabetes: a randomized controlled trial. Diabetes Obes Metab. 2017;19(4):579–89. https://doi.org/10.1111/dom.12861.
Tonucci LB, Olbrich Dos Santos KM, Licursi de Oliveira L, Rocha Ribeiro SM, Duarte Martino HS. Clinical application of probiotics in type 2 diabetes mellitus: a randomized, double-blind, placebo-controlled study. Clin Nutr. 2017;36(1):85–92. https://doi.org/10.1016/j.clnu.2015.11.011.
Feizollahzadeh S, Ghiasvand R, Rezaei A, Khanahmad H, Sadeghi A, Hariri M. Effect of probiotic soy milk on serum levels of adiponectin, inflammatory mediators, lipid profile, and fasting blood glucose among patients with type II diabetes mellitus. Probiotics Antimicrob Proteins. 2017;9(1):41–7. https://doi.org/10.1007/s12602-016-9233-y.
Khalili L, Alipour B, Asghari Jafar-Abadi M, Faraji I, Hassanalilou T, Mesgari Abbasi M, Vaghef-Mehrabany E, Alizadeh Sani M. The effects of Lactobacillus casei on glycemic response, serum sirtuin1 and fetuin-a levels in patients with type 2 diabetes mellitus: a randomized controlled trial Iran Biomed J. 2018.
Kobyliak N, Falalyeyeva T, Mykhalchyshyn G, Kyriienko D, Komissarenko I. Effect of alive probiotic on insulin resistance in type 2 diabetes patients: randomized clinical trial. Diabetes Metab Syndr. 2018. https://doi.org/10.1016/j.dsx.2018.04.015.
Ruan Y, Sun J, He J, Chen F, Chen R, Chen H. Effect of probiotics on glycemic control: a systematic review and meta-analysis of randomized, controlled trials. PLoS One. 2015;10(7):e0132121. https://doi.org/10.1371/journal.pone.0132121.
Li C, Li X, Han H, Cui H, Peng M, Wang G, et al. Effect of probiotics on metabolic profiles in type 2 diabetes mellitus: a meta-analysis of randomized, controlled trials. Medicine (Baltimore). 2016;95(26):e4088. https://doi.org/10.1097/MD.0000000000004088.
Samah S, Ramasamy K, Lim SM, Neoh CF. Probiotics for the management of type 2 diabetes mellitus: a systematic review and meta-analysis. Diabetes Res Clin Pract. 2016;118:172–82. https://doi.org/10.1016/j.diabres.2016.06.014.
Akbari V, Hendijani F. Effects of probiotic supplementation in patients with type 2 diabetes: systematic review and meta-analysis. Nutr Rev. 2016;74(12):774–84.
Yao K, Zeng L, He Q, Wang W, Lei J, Zou X. Effect of probiotics on glucose and lipid metabolism in type 2 diabetes mellitus: a meta-analysis of 12 randomized controlled trials. Med Sci Monit. 2017;23:3044–53.
de Groot PF, Frissen MN, de Clercq NC, Nieuwdorp M. Fecal microbiota transplantation in metabolic syndrome: history, present and future. Gut Microbes. 2017;8(3):253–67. https://doi.org/10.1080/19490976.2017.1293224.
Vrieze A, Van Nood E, Holleman F, Salojärvi J, Kootte RS, Bartelsman JF, et al. Transfer of intestinal microbiota from lean donors increases insulin sensitivity in individuals with metabolic syndrome. Gastroenterology. 2012;143(4):913–6.e7. https://doi.org/10.1053/j.gastro.2012.06.031.
Devkota S. MICROBIOME. Prescription drugs obscure microbiome analyses. Science. 2016;351(6272):452–3. https://doi.org/10.1126/science.aaf1353.
Rena G, Hardie DG, Pearson ER. The mechanisms of action of metformin. Diabetologia. 2017;60(9):1577–85. https://doi.org/10.1007/s00125-017-4342-z.
Malik F, Mehdi SF, Ali H, Patel P, Basharat A, Kumar A, et al. Is metformin poised for a second career as an antimicrobial? Diabetes Metab Res Rev. 2018;34(4):e2975. https://doi.org/10.1002/dmrr.2975.
Rodriguez J, Hiel S, Delzenne NM. Metformin: old friend, new ways of action-implication of the gut microbiome? Curr Opin Clin Nutr Metab Care. 2018;21(4):294–301. https://doi.org/10.1097/MCO.0000000000000468.
Montandon SA, Jornayvaz FR. Effects of antidiabetic drugs on gut microbiota composition. Genes (Basel). 2017 ;8(10). https://doi.org/10.3390/genes8100250.
Mulla CM, Middelbeek RJW, Patti ME. Mechanisms of weight loss and improved metabolism following bariatric surgery. Ann N Y Acad Sci. 2018;1411(1):53–64. https://doi.org/10.1111/nyas.13409.
Guo Y, Huang ZP, Liu CQ, Qi L, Sheng Y, Zou DJ. Modulation of the gut microbiome: a systematic review of the effect of bariatric surgery. Eur J Endocrinol. 2018;178(1):43–56. https://doi.org/10.1530/EJE-17-0403.
Funding
This manuscript has no funding source, and no author received payments from any pharmaceutical company or other agency to write this article.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Antonio Sircana, Luciana Framarin, Nicola Leone, Mara Berrutti, Francesca Castellino, Renato Parente, Franco De Michieli, Elena Paschetta, and Giovanni Musso declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Pathogenesis of Type 2 Diabetes and Insulin Resistance
Rights and permissions
About this article
Cite this article
Sircana, A., Framarin, L., Leone, N. et al. Altered Gut Microbiota in Type 2 Diabetes: Just a Coincidence?. Curr Diab Rep 18, 98 (2018). https://doi.org/10.1007/s11892-018-1057-6
Published:
DOI: https://doi.org/10.1007/s11892-018-1057-6