Abstract
Probiotic therapies are going to be an effective alternative therapeutic strategy in the treatment and management of diabetes. The mechanism behind the essential effects of probiotic therapies in diabetic patients was not fully understood. The objective of this study was to evaluate the effects of probiotic soy milk containing Lactobacillus planetarum A7 on inflammation, lipid profile, fasting blood glucose, and serum adiponectin among patients with type 2 diabetes mellitus. Forty patients with type 2 diabetes, at the age of 35–68 years old, were assigned to two groups in this randomized, double-blind, controlled clinical trial. The patients in the intervention group consumed 200 ml/day of probiotic soy milk containing L. planetarum A7 and those in control group consumed 200 ml/day of pure soy milk for 8 weeks. Serum TNF-α, C reactive protein, adiponectin, lipid profile, and fasting blood glucose were determined before and after intervention. In intervention group, serum adiponectin in pre- and post-treatment did not show any significant changes (2.52 ± 0.74 vs 2.84 ± 0.61, P = 0.658), as well as changes in serum TNF-α and C reactive protein (172.44 ± 5.7 vs 172.83 ± 7.6, P = 0.278, 4.2 ± 1.4 vs 4.5 ± 1.9, P = 0.765, respectively). Low-density cholesterol and high-density cholesterol changed significantly (P = 0.023, P = 0.017, respectively), but fasting blood glucose did not show any significant changes. The results of this study showed that consumption of probiotic soy milk and soy milk has no effect on serum adiponectin and inflammation, but it can change lipid profile among type 2 diabetic patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Type 2 diabetes (T2D) is a heterogeneous and multifactorial disease that both genetic and environmental factors are involved in its development and pathogenesis [1]. Increased insulin resistance is one of the main pathophysiological features of T2D [2]. It takes place before disease onset and contributes to the development of disease. Hyperglycemia, high free fatty acids and pro-inflammatory cytokines develop insulin resistance. It seems that pro-inflammatory cytokines play a key role in the development of insulin resistance. It is known that elevation of inflammatory cytokines in obesity is responsible for the development of insulin resistance and other obesity related complications [3].
Two key mediators of insulin resistance, adiponectin (Apn) and TNF-α are known to have critical roles in developing obesity complications and T2D [4–6]. An earlier study reported that obesity and T2D cause a decrease in Apn and an increase in TNF-α [7]. Apn is a 30 KD protein which mainly secretes from adipose tissue. It circulates in human blood at levels of 3–30 μg/ml in the forms of trimmer, hexamer, and multimer [4]. New evidence shows Apn plays a preventive role in developing insulin resistance and T2D and can be considered as an improving factor for insulin resistance and cardiovascular diseases [8]. Apn has anti-inflammatory effects and decreases the level of TNF-α [9]. It has also anti-inflammatory effect on monocytes and endothelial cells and attenuates atherogenesis [9].
TNF-α is a pro-inflammatory cytokine produce as a17 KD soluble form (sTNF) by various cell types and weakly by adipose tissue [5]. Inflammation develops insulin resistance through interference and blockade of the insulin signaling pathway [6]. Inflammation increases in obesity and contributes and is related to insulin resistance and development of T2D in obese patients [3]. It seems that TNF-α and Apn antagonize each other, regulate expressing each other, and act antagonistically in modulating insulin action [10]. Decrease of systemic TNF-α and increase of Apn can be an effective therapeutic target for managing T2D and inhibiting insulin resistance in obesity.
Recently, probiotic therapies are going to be a new effective therapeutic strategy in preventing and management of many chronic diseases such as T2D [11, 12]. Probiotics are safe and nonpathogenic live microorganisms that confer health benefits to consumers [13]. They exert health benefits through change in gut micobiota and enhancement of gut immune system [14]. Nowadays, many strains of isolated probiotics and genetically improved strains are developed for therapeutic aims and their applications are under investigation [15]. New evidence has suggested that probiotics can regulate and stimulate innate and adaptive immune system locally and systematically [16, 17].
Consumption of probiotics in T2D was associated with some improvements in clinical symptoms [18, 19]. Recent systematic review and meta-analysis indicated moderate hypoglycemic effect of lactic acid bacteria, but findings on anti-inflammatory effects remain inconsistent [20]. It seems anti-inflammatory effects of lactic acid bacteria may vary from strain to strain. Since lowering inflammation between diabetic patients is a health promoting characteristic there is a need to find new probiotic strains with anti-inflammatory effects. Lactobacillus plantarum A7 has been isolated from fecal flora of healthy infants and may reduce inflammation [21].
Human and animal studies indicated that soy phytoestrogen can improve several parameters related to diabetes risk factor [22–24]. We believe using probiotic and soy milk together can increase probiotic protective effect, because probiotic can increase soy isoflavones absorption [25, 26]. Therefore according to other studies with significant results and no side effects we fortified soy milk with 2 × 107 Lactobacillus plantarum A7 [27].
The aim of this study was to find a probiotic strain with anti-inflammatory effect and revealing molecular mechanisms behind the beneficial effects of this probiotic consumption in T2D.
Materials and Methods
Study Design and Participants
This randomized double-blinded parallel-group controlled clinical trial was carried out in Isfahan, Iran. Subjects were 48 T2D patients aged 35–68 years. All subjects were interviewed; a questionnaire was used to collect data about age and medical history. Subjects who have a history of inflammatory bowel disease, infection, liver disease, rheumatoid arthritis, smoking, alcoholism, recent antibiotic therapy, C reactive protein (CRP) positive and daily intake of multivitamin and mineral were excluded from this study. Subjects were randomly divided in two distinct groups. The study group (n = 24, i.e., 12 males and 12 females) took soy milk containing probiotic and control group (n = 24, i.e., 10 males and 14 females) took soy milk without probiotic for eight weeks. During 8 weeks, intervention subjects took 200 ml soy milk/day and for study group, their milk was supplemented with 2 × 107 CFU of L. plantarum A7. Subjects who intended to change their ordinary dietary habits and consume fermented products during the intervention period were excluded from the study. The study was approved by Ethical Committee of Isfahan University of Medical Sciences, and informed written consent was taken from all participants. The trial has been registered in the Iranian Registry of Clinical Trials, identifier: IRCT: IRCT201405265062N8 available at: http://www.irct.ir.
Intervention and Anthropometric Measurements
Conventional soy milk and probiotic soy milk were produced every 3 days and distributed to the participants. The probiotic soy milks were sampled at the time of distribution and were microbiologically analyzed every 2 weeks. Samples were refrigerated at 4 °C for 3 days, and next analyzing was done on the third day of storage. MRS agar (Sigma-Aldrich) was used for colony counting of Lactobacillus plantarum A7 by pour plate method. Microbiological analyses of the probiotic soymilk showed the average colony counts of Lactobacillus plantarum A7 on day one and day three were the same. Therefore, the bacterial survival rate in soy milk during a 3 days storage period was intact. All subjects entered a 2 week run-in period during which they had to stop taking any probiotic food or probiotic supplements. Their weight, height, waist to hip ratio (WHR), and medication history were recorded before and after the intervention, and information on physical activity (PA) levels and micro and macronutrients intakes were gathered every 2 week by international physical activity questionnaires (IPAQ) and a 24 h diet recall interview, respectively.
Subjects’ weights were recorded by digital scale (Seca, Germany), with an accuracy of 100 g, and standing height was recorded by non-stretchable tape (Seca, Germany), with an accuracy of 0.1 cm. Body mass index (BMI) was got by dividing weight by the square of height. All subjects had to have a stable dietary habit, physical activity, and medication during intervention. Subjects who intended to change their dietary habits, physical activity, or body weight during the intervention period were excluded from the study.
Biochemical Analysis
At beginning and the end of trial, venous blood sample was taken after 12 h overnight fasting. Serum was separated by centrifugation at 3000 rpm for 10 min and stored at −20 °C. All serum samples were analyzed on the same run soon after the end of the study to avoid interassay variations.
A standard human Apn detecting ELISA kit (Mediagnost, Germany) based on sandwich ELISA was used for detection of serum Apn. Concentrations of Apn were calculated in comparison to a standard curve (a serial dilution of Apn standard provided in kit).
Serum TNF-α and CRP was measured using standard ELISA kit for human TNF-α and CRP based on sandwich ELISA (Id Labs™ Inc Biotechnology, Canada).
Serum triglyceride (TG), high-density lipoprotein cholesterol (HDL-C), and low-density cholesterol (LDL-C) were measured using the standard enzymatic–colorimetric method by Bionik Diagnostic Kits (Iran). Fasting blood sugar (FBS) was measured by Glucose kit (GOD, Pars Azmon product, Iran) with enzymatic and Colorimetric method (GOD-PAP).
Statistical Analysis
All data were checked for normal distribution using kolmogrove-Smirnoff test. Data are presented as mean ± S.E. Independent samples t test was used for data on dietary intakes between groups. We used repeated measure analysis of variance (ANOVA) for checking changes in intakes throughout study period. Possible confounding factors in this study were calorie and carbohydrate intake.
For comparison the levels of PA and sex between two groups, Chi-square test was used. Analysis of covariance (ANCOVA) was used for determining any differences between two studied groups in terms of main outcomes after intervention (adjustment was made for baseline values and confounding factors). Paired-sample t tests were used to detect within group differences. Differences were considered significant when P values were less than 0.05. All analysis was performed using the statistical software (SPSS) version 20.0 (SPSS Inc., Chicago, IL).
Results
Base Line Data
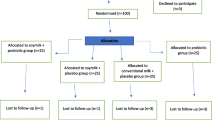
This study was carried out from November 2013 to February 2014, and 48 diabetic patients took part in this study. There were no adverse reactions or symptoms in patients, and they all displayed good compliance. From study group and control group, four participants could not complete this trial and were excluded. Therefore, finally 40 subjects (soy milk, n = 20; probiotic soy milk, n = 20) successfully completed the trial (Fig. 1). There were no statistical significant differences in the baseline characteristics of the patients between the two groups (Table 1).
In terms of BMI and waist to hip ratio (WHR), there was not any significant difference at the beginning of study between two groups, but probiotic soy milk caused a significant within group reduction in BMI and WHR. There was not any significant difference between two groups after adjusting by baseline values, energy, and carbohydrate intake with ANCOVA.
24 h Diet Recall
We observed no significant differences between the two groups in dietary intake at the beginning of study except for carbohydrate (Table 2). The intake of carbohydrate was significantly higher in placebo group (P < 0.001). Dietary intake of nutrients at the beginning and during the study did not show any significant differences in within each group separately, but statistically significant difference was found between the two groups for dietary intakes of energy and carbohydrate throughout the study.
Changes of Inflammatory Mediators
As shown in Table 3, no significant changes were indicated for serum Apn, TNF-α, and CRP levels before and after intervention in both intervention (P = 0.658, 0.973, and 0.765, respectively) and control group (P = 0.278, 0.309, 0.619, respectively).
Between groups comparison did not indicate any significant changes in serum TNF-α, CRP, and Apn in intervention group, in compare with control group, after adjusting with baseline value, calorie, and carbohydrate intake (P = 0.112, 0.269, and 0.317, respectively).
Changes of Lipid Profile, and FBS
Within group comparisons of LDL, and HDL revealed that the probiotic soy milk increased HDL, and decreased LDL (P < 0.05, Table 3), while there was not any significant difference in the placebo group. FBS and TG did show any significant change in neither probiotic soy milk (P = 0.369, 0.814, respectively) nor soy milk group after intervention (P = 0.326, 0.601, respectively). Between groups comparison did not reveal any significant changes in FBS and TG in intervention group, in compare with control group, after adjusting with baseline value, calorie, and carbohydrate intake (P = 0.294 and 0.406, respectively).
Discussion
This study revealed that the consumption of probiotic soy milk, compared to the soy milk, for 8 weeks, among patients with T2D diabetes does not have any effect on serum Apn, inflammatory mediators, and FBS, but it could decrease LDL and increase HDL significantly.
Most of the previous articles results that studied the effect of probiotics on glycemic control in T2D, indicated that probiotics, especially Lactobacillus, can reduce FBS, HbA1c, insulin, and inflammation [28, 29]. The increase of GLUT4 mRNA expression has also been reported [28]. Previous studies among diabetic subjects have shown controversial result especially on inflammation and glycemic index. We hypothesized that effect of probiotics on glycemic control could be through immune-modulatory effects. To capture these interrelations were selected a set of key inflammatory and anti-inflammatory cytokines, including Apn, TNF-α, and CRP.
To the best of our knowledge, this is the first human study to compare the effect of probiotic soy milk and soy milk on anti-inflammatory mediator Apn, and pro-inflammatory mediator TNF-α and CRP among diabetic patients. Probiotics has recently been considered as an effective alternative biological method for chemical agents in managing many chronic diseases [11, 12]. They confer useful effects through many mechanisms related to their effect on local gut environment and systemic effects [14]. However, their mechanisms of action could be different based on type of probiotics and genetic background of hosts.
Apn increases fatty acid beta-oxidation, improves glucose metabolism and decreases gluconeogenesis enzymes at mRNA expression level [4]. It has been repeatedly reported that an increase in serum Apn level was associated with increased insulin sensitivity [4] and β-cells protection from autoimmunity and lipotoxicity injuries [30]. Li and colleagues showed that higher Apn levels were consistently associated with a lower risk of T2D diabetes in prospective studies of diverse populations. Other studies also showed that Apn is a promising target for reducing risk of T2D diabetes and improving health indices in T2D [31]. Experimental studies have been showed that probiotics can increase Apn concentration [32], but there is not any study among patients with T2D or metabolic syndrome for comparison their result with our result. In one study among people with obesity using fermented milk could increase Apn significantly [33], but in our study, we did not find any significant changes in serum Apn after L. plantarum A7 consumption in T2D patients. Circulating Apn concentrations increase during caloric limit in animals and humans, such as patients with anorexia nervosa [4].In the present study, participants did not experience any significant weight fall; therefore, L. plantarum A7 consumption have no effect on serum Apn level.
Changing of serum TNF-α after probiotic consumption was evaluated with other authors, and it was controversial. In the clinical trial by Hatakka et al. [34], probiotic supplementation resulted in no significant change within- or between-group for cytokines such as TNF-α. But in another study by Alipour et al. [35], probiotic supplementation among female with rheumatoid arthritis caused significant decrease in TNF-α concentration. Among diabetic patients using fermented milk for 12 week could decrease TNF-α [36].
In the present study, we did not see any significant change in serum levels of TNF-α after 8 week L. plantarum A7 consumption. The increase in mean TNF-α level in control group after treatment was due to significant increase of TNF-α in two patients (unknown reason without any sign of infection and CRP change) but in others was unchanged, then overall was not significant. The disagreement between studies may be in part because of the different strain and dose of the administered probiotic which consequently resulted in a different immunological pattern.
In our study, probiotic soy milk could not decrease FBS, but it could change lipid profile significantly. Several studies about the effects of different probiotics strains on glycemic status and lipid profile in patients with T2D have yielded inconsistent results. Recent meta-analysis about probiotic effect on FBS believes that consumption of probiotics can decrease FBS borderline statistically significant, but multiple species of probiotics showed a more pronounced reduction [37]. Our result about probiotic effect on lipid profile was similar with Tonucci LB et al. They believe probiotics in T2D can decrease lipid profile significantly [36].
Marta et al. [38] in their study indicated that anti-inflammatory properties of probiotics are strain specific, and it depends on antigens present on the bacterial wall. Therefore, nonsignificant changes in CRP levels in this study may be associated with differences in strain-specific efficacy.
Our limitations in this study were short duration of treatment, the absence of control group that did not take soy milk, and the lack of probiotic measurement before and after treatment in stool. These limitations must be considered while interpreting the results.
Conclusion
Overall, this study revealed the consumption of probiotic soy milk and soy milk for eight weeks did not change serum concentration of Apn, CRP, and TNF-α in patient with T2D. Further studies are needed to better clarify the effects of probiotic soy milk and soy milk on profile of adipokines and cytokines related to metabolic disorders including T2D. It seems that there are long way to probiotics to enter in the management of T2D patients. The isolation of some useful strains and improvement of their properties with genetic engineering tools could expand this new field of biological therapy using probiotics.
References
Stumvoll M, Goldstein BJ, van Haeften TW (2005) Type 2 diabetes: principles of pathogenesis and therapy. Lancet 365:1333–1346
Relimpio F (2003) “The relative contributions of insulin resistance and beta-cell dysfunction to the pathophysiology of Type 2 diabetes”, by Kahn SE. Diabetologia 46:1707
Bastard JP, Maachi M, Lagathu C, Kim MJ, Caron M, Vidal H et al (2006) Recent advances in the relationship between obesity, inflammation, and insulin resistance. Eur Cytokine Netw 17:4–12
Lihn AS, Pedersen SB, Richelsen B (2005) Adiponectin: action, regulation and association to insulin sensitivity. Obes Rev 6:13–21
Moller DE (2000) Potential role of TNF-alpha in the pathogenesis of insulin resistance and type 2 diabetes. Trends Endocrinol Metab 11:212–217
Borst SE (2004) The role of TNF-alpha in insulin resistance. Endocrine 23:177–182
Lin X, Zhang Z, Chen JM, Xu YY, Ye HR, Cui J et al (2015) Role of APN and TNF-alpha in type 2 diabetes mellitus complicated by nonalcoholic fatty liver disease. Genet Mol Res 14:2940–2946
Larter CZ, Farrell GC (2006) Insulin resistance, adiponectin, cytokines in NASH: which is the best target to treat? J Hepatol 44:253–261
Ouchi N, Walsh K (2007) Adiponectin as an anti-inflammatory factor. Clin Chim Acta Int J Clin Chem 380:24–30
Hui JM, Hodge A, Farrell GC, Kench JG, Kriketos A, George J (2004) Beyond insulin resistance in NASH: tNF-alpha or adiponectin? Hepatology 40:46–54
Lye HS, Kuan CY, Ewe JA, Fung WY, Liong MT (2009) The improvement of hypertension by probiotics: effects on cholesterol, diabetes, renin, and phytoestrogens. Int J Mol Sci 10:3755–3775
Panwar H, Rashmi HM, Batish VK, Grover S (2013) Probiotics as potential biotherapeutics in the management of type 2 diabetes—prospects and perspectives. Diabetes Metab Res Rev 29:103–112
Goldin BR (1998) Health benefits of probiotics. Br J Nutr 80(4):S203–S207
Boirivant M, Strober W (2007) The mechanism of action of probiotics. Curr Opin Gastroenterol 23:679–692
Sanders ME (2003) Probiotics: considerations for human health. Nutr Rev 61(3):91–99
Corthesy B, Gaskins HR, Mercenier A (2007) Cross-talk between probiotic bacteria and the host immune system. J Nutr 137:781s–790s
Isolauri E, Sutas Y, Kankaanpaa P, Arvilommi H, Salminen S (2001) Probiotics: effects on immunity. Am J Clin Nutr 73:444s–450s
Hariri M, Salehi R, Feizi A, Mirlohi M, Kamali S, Ghiasvand R (2015) The effect of probiotic soy milk and soy milk on anthropometric measures and blood pressure in patients with type II diabetes mellitus: a randomized double-blind clinical trial. ARYA Atheroscler 11:74–80
Olveira G, Gonzalez-Molero I (2016) An update on probiotics, prebiotics and symbiotics in clinical nutrition. Endocrinol Nutr. doi:10.1016/j.endonu.2016.07.006
Samah S, Ramasamy K, Lim SM, Neoh CF (2016) Probiotics for the management of type 2 diabetes mellitus: a systematic review and meta-analysis. Diabetes Res Clin Pract 118:172–182
Sadeghi-Aliabadi H, Mohammadi F, Fazeli H, Mirlohi M (2014) Effects of Lactobacillus plantarum A7 with probiotic potential on colon cancer and normal cells proliferation in comparison with a commercial strain. Iran J Basic Med Sci 17:815–819
Bahls LD, Venturini D, Scripes Nde A, Lozovoy MA, Simao TN, Simao AN et al (2011) Evaluation of the intake of a low daily amount of soybeans in oxidative stress, lipid and inflammatory profile, and insulin resistance in patients with metabolic syndrome. Arq Bras Endocrinol Metabol 55:399–405
Nordentoft I, Jeppesen PB, Hong J, Abudula R, Hermansen K (2008) Increased insulin sensitivity and changes in the expression profile of key insulin regulatory genes and beta cell transcription factors in diabetic KKAy-mice after feeding with a soy bean protein rich diet high in isoflavone content. J Agric Food Chem 56:4377–4385
Ristic Medic D, Ristic V, Arsic A, Postic M, Ristic G, Blazencic Mladenovic V et al (2006) Effects of soybean D-LeciVita product on serum lipids and fatty acid composition in type 2 diabetic patients with hyperlipidemia. Nutr Metab Cardiovasc Dis NMCD 16:395–404
Zielinska D, Kolozyn-Krajewska D, Goryl A, Motyl I (2014) Predictive modelling of Lactobacillus casei KN291 survival in fermented soy beverage. J Microbiol 52:169–178
Tsangalis D, Wilcox G, Shah NP, Stojanovska L (2005) Bioavailability of isoflavone phytoestrogens in postmenopausal women consuming soya milk fermented with probiotic bifidobacteria. Br J Nutr 93:867–877
Li C, Li X, Han H, Cui H, Peng M, Wang G et al (2016) Effect of probiotics on metabolic profiles in type 2 diabetes mellitus: a meta-analysis of randomized, controlled trials. Medicine 95:e4088
Hsieh FC, Lee CL, Chai CY, Chen WT, Lu YC, Wu CS (2013) Oral administration of Lactobacillus reuteri GMNL-263 improves insulin resistance and ameliorates hepatic steatosis in high fructose-fed rats. Nutr Metab 10:35
Tabuchi M, Ozaki M, Tamura A, Yamada N, Ishida T, Hosoda M et al (2003) Antidiabetic effect of Lactobacillus GG in streptozotocin-induced diabetic rats. Biosci Biotechnol Biochem 67:1421–1424
Lee YH, Magkos F, Mantzoros CS, Kang ES (2011) Effects of leptin and adiponectin on pancreatic beta-cell function. Metab Clin Exp 60:1664–1672
Spranger J, Kroke A, Mohlig M, Bergmann MM, Ristow M, Boeing H et al (2003) Adiponectin and protection against type 2 diabetes mellitus. Lancet 361:226–228
Kim SW, Park KY, Kim B, Kim E, Hyun CK (2013) Lactobacillus rhamnosus GG improves insulin sensitivity and reduces adiposity in high-fat diet-fed mice through enhancement of adiponectin production. Biochem Biophys Res Commun 431:258–263
Kadooka Y, Sato M, Imaizumi K, Ogawa A, Ikuyama K, Akai Y et al (2010) Regulation of abdominal adiposity by probiotics (Lactobacillus gasseri SBT2055) in adults with obese tendencies in a randomized controlled trial. Eur J Clin Nutr 64:636–643
Hatakka K, Martio J, Korpela M, Herranen M, Poussa T, Laasanen T et al (2003) Effects of probiotic therapy on the activity and activation of mild rheumatoid arthritis–a pilot study. Scand J Rheumatol 32:211–215
Alipour B, Homayouni-Rad A, Vaghef-Mehrabany E, Sharif SK, Vaghef-Mehrabany L, Asghari-Jafarabadi M et al (2014) Effects of Lactobacillus casei supplementation on disease activity and inflammatory cytokines in rheumatoid arthritis patients: a randomized double-blind clinical trial. Int J Rheum Dis 17:519–527
Tonucci LB, Olbrich Dos Santos KM, Licursi de Oliveira L, Rocha Ribeiro SM, Duarte Martino HS (2015) Clinical application of probiotics in type 2 diabetes mellitus: a randomized, double-blind, placebo-controlled study. Clin Nutr. doi:10.1016/j.clnu.2015.11.011
Nikbakht E, Khalesi S, Singh I, Williams LT, West NP, Colson N (2016) Effect of probiotics and synbiotics on blood glucose: a systematic review and meta-analysis of controlled trials. Eur J Clin Nutr. doi:10.1007/s00394-016-1300-3
Kasinska MA, Drzewoski J (2015) Effectiveness of probiotics in type 2 diabetes: a meta-analysis. Pol Arch Med Wewn 125:803–813
Acknowledgments
We are grateful to the Isfahan soy milk company that provided soy milk products for the present study, and we express our special thanks to all patients that participate in our study. Funding was provided by Isfahan University of Medical Sciences (Grant No. 393150).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declares that they have no conflict of interest.
Additional information
Reza Ghiasvand and Sadegh Feizollahzadeh are first co-author.
Rights and permissions
About this article
Cite this article
Feizollahzadeh, S., Ghiasvand, R., Rezaei, A. et al. Effect of Probiotic Soy Milk on Serum Levels of Adiponectin, Inflammatory Mediators, Lipid Profile, and Fasting Blood Glucose Among Patients with Type II Diabetes Mellitus. Probiotics & Antimicro. Prot. 9, 41–47 (2017). https://doi.org/10.1007/s12602-016-9233-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12602-016-9233-y