Abstract
Purpose of Review
Limbic-predominant age-related TDP-43 encephalopathy (LATE) is a recently defined neurodegenerative disease characterized by amnestic phenotype and pathological inclusions of TAR DNA-binding protein 43 (TDP-43). LATE is distinct from rarer forms of TDP-43 diseases such as frontotemporal lobar degeneration with TDP-43 but is also a common copathology with Alzheimer’s disease (AD) and cerebrovascular disease and accelerates cognitive decline. LATE contributes to clinicopathologic heterogeneity in neurodegenerative diseases, so it is imperative to distinguish LATE from other etiologies.
Recent Findings
Novel biomarkers for LATE are being developed with magnetic resonance imaging (MRI) and positron emission tomography (PET). When cooccurring with AD, LATE exhibits identifiable patterns of limbic-predominant atrophy on MRI and hypometabolism on 18F-fluorodeoxyglucose PET that are greater than expected relative to levels of local AD pathology. Efforts are being made to develop TDP-43-specific radiotracers, molecularly specific biofluid measures, and genomic predictors of TDP-43. LATE is a highly prevalent neurodegenerative disease distinct from previously characterized cognitive disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Limbic-predominant age-related TDP-43 encephalopathy (LATE) is a common, primary neurodegenerative disease in older adults typified by memory impairment and pathological accumulation of transactivation response (TAR) DNA-binding protein 43 (TDP-43), particularly in the medial temporal lobe (MTL) [1••, 2]. Inclusions of TDP-43 were first discovered in FTLD and ALS [3••, 4••], and later in hippocampal sclerosis and amnestic cognitive impairment not associated with FTLD/ALS [5••]. Compared to other neurodegenerative diseases such as Alzheimer’s disease (AD), Lewy body disease (LBD), and vascular contributions to cognitive impairment and dementia (VCID), LATE was formally defined much more recently in 2019 as a clinical manifestation of older adults who possess LATE neuropathological change (LATE-NC). LATE-NC describes a pattern of TDP-43 inclusions, either with or without hippocampal sclerosis [1••]. LATE is extremely prevalent with ~ 40% of individuals over 80 with LATE-NC across multiple autopsy studies [6•]. Moreover, the contribution of LATE to late-life cognitive impairment is relatively high with some estimates at approximately 20% of the attributable risk vs ~ 40% for AD and 30% for VCID [1••]. While AD is defined by the presence of amyloid-β and neurofibrillary tau [7], AD and LATE are often concomitant disease entities within cognitively impaired older adults. Indeed, estimates across autopsy cohorts suggest that patients with both LATE and AD comprise ~ 55% of patients with AD [6•], with individual study estimates ranging from 25 to 60% [5••, 8, 9, 10].
Hippocampal sclerosis (HS) is the profound loss of pyramidal cells and associated gliosis in the cornu ammonis 1 and subiculum regions of the hippocampus [11•] and a common feature in anywhere from 60 to 95% of cases with LATE [1••]. Given this strong overlap, various biomarkers and genetic risk factors that are associated with HS are also linked to LATE.
Here, we survey the recent literature on LATE and HS focusing on clinical and pathological features as well as emerging biomarkers, such as neuroimaging and biofluid tests.
Clinical Presentation
Older Age
As the name of LATE suggests, LATE is defined by TDP-43 in older adults with limbic neurodegeneration. While frontotemporal lobar degeneration (FTLD) and amyotrophic lateral sclerosis (ALS) have an earlier age of onset and lower prevalence with more advanced age [12, 13], LATE is enriched in older adults [2]. Indeed, > 30% of autopsied brains over the age of 80 have the presence of TDP-43 and/or severe hippocampal atrophy that is pathologically confirmed as HS [11•]. The coincidence of LATE with AD is also thought to increase over the duration and severity of AD [14].
Memory Impairment
Patients with LATE demonstrate episodic memory impairment, often HS [1••, 11•]. Patients with pure LATE often show an amnestic phenotype with fairly indolent progression relative to AD, while patients with mixed LATE + AD have a faster decline in hippocampal volume and cognition, suggesting a potential additive or synergistic relationship between AD and TDP-43 pathologies [9, 15, 16•]. As might be expected, LATE with HS is associated with worse memory and orientation than LATE without HS [1••, 11•, 17•]. In addition to memory loss, LATE-associated clinical features may involve impairment of semantic memory, such as measured with tests of categorical fluency, particularly in the presence of HS [18], though there is also evidence of deficits of working memory as well [19, 20]. Therefore, when compared to patients with pathologically defined AD alone, the current clinical data on LATE suggests a rather prominent and relatively isolated amnestic presentation that is slowly progressive in isolated LATE. Alternatively, LATE with AD is associated with a more rapid progression, exacerbating memory decline and likely contributing to semantic and perhaps other domains.
Additional Clinical Symptomatology
Compared to LATE with AD, pure LATE may have a slightly higher prevalence of frontal lobe-associated behavioral symptoms while pure AD has a higher frequency of agitation symptoms on the Neuropsychiatric Inventory [21•]. Potential symptoms associated with HS and LATE involve decreased personal care [17•] and inappropriate behavior and apathy [22]. Nevertheless, such behavioral symptoms are much more pronounced in frontotemporal dementia (FTD) syndromes [23].
Differential Diagnosis
The clinical syndrome of LATE should be considered in the differential diagnosis of patients with amnestic cognitive impairment, along with AD and VCID [7]. Clinical suspicion for LATE should be raised in patients with memory loss with negative AD markers for amyloid or tau pathology on imaging or biofluid markers, though mixed disease with concomitant AD and LATE pathologies is common (up to 60% of patients with AD) [8]. More severe hippocampal atrophy also may be suggestive of the condition. While there is some overlap in TDP-43 pathology and potential behavioral symptoms between LATE and FTD, FTD is much less prevalent [23] and does not classically have an amnestic phenotype. Furthermore, behavioral symptoms appear to be unlikely primary salient features in LATE. A relatively slowly progressive and isolated amnestic syndrome without progressive involvement of other domains over time is perhaps more suggestive of LATE than AD, particularly in those over 80 years old. Overall, the symptomatology of LATE is clinically similar with AD and should be considered in patients with amnestic cognitive impairment.
Pathology
TDP-43
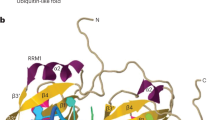
TDP-43 is an RNA-binding protein and encoded by the TARDP gene. Its function includes the regulation of splicing and transcription of mRNA in the cell nucleus [24]. In the context of neurodegeneration and cellular perturbation, TDP-43 is aberrantly phosphorylated and ubiquitinated, which promote the misfolding of TDP-43 [3••, 4••], and mislocalization of TDP-43 to the cytoplasm. TDP-43 also forms ribonucleoprotein complexes within stress granules [25], which may serve as a protective response [26]. Ultimately, the mislocalization of TDP-43 aggregates triggers organelle dysfunction and neurotoxic sequelae [27], impairing dendritic integrity [28] and activating neuroinflammatory microglia [29].
In current guidelines, LATE-NC is staged by propagation pattern from the amygdala to the medial temporal lobe (MTL) and beyond: no TDP-43 cytoplasmic inclusions (stage 0), amygdala-predominant (stage 1), extension to the hippocampus and entorhinal cortex (stage 2), and spreading to the middle frontal gyrus and neocortex (stage 3) [1••]. Stages 1 through 3 are roughly similar in prevalence [30]. Neurodegeneration in LATE has a predilection for anterior and limbic areas, including MTL, temporal pole, and orbitofrontal cortex. There is a relationship between asymmetry of the MTL and HS [1••, 20].
Hippocampal Sclerosis (HS)
Patients with LATE either with or without HS do not differ in terms of amyloid, tau, or Lewy body pathology, as well as clinical history of stroke, cardiovascular disease, or epilepsy. Yet, patients with LATE and HS were more likely to have stage 3 neocortical TDP-43 burden than patients with LATE without HS and had a higher burden of cerebral arteriosclerosis and atherosclerosis [17•], suggesting a link with vascular disease.
Additional TDP-43 Proteinopathies
TDP-43 inclusions were first observed in FTLD and ALS. Frontotemporal lobar degeneration due to TDP-43 (FTLD-TDP) exhibits at least five different pathologic subtypes (A through E), each with different histopathological characteristics, organellar distribution, and regional spreading patterns [31]. About 50% of FTLD cases display TDP-43 pathology [32]. Outside of rare SOD1 or FUS mutations, ~ 97% of sporadic ALS and about 90% of familial ALS cases have TDP-43 aggregates [33, 34]. Despite similarities, LATE and FTLD-TDP are considered distinct entities based on a number of differential features, including epidemiology, disease onset, clinical phenotype, and the neuropathological density of TDP-43 inclusions; simple criteria based on density patterns of neocortical TDP-43 immunoreactivity achieve about 90% sensitivity and specificity between LATE and FTLD-TDP [35]. Perry syndrome is a rare primary TDP-43 disease with rapidly progressive parkinsonism, hypoventilation, depression, and TDP-43 inclusions in substantia nigra and globus pallidus [36]. Overall, TDP-43 pathology is present in many diseases (Table 1).
Genomic Landscape of LATE
Progress in uncovering the genetic architecture of TDP-43 diseases has been steadily mounting. Several genetic risk factors for LATE and/or HS are shared with FTLD and ALS, such as common variants in the progranulin gene GRN [37•]. However, mutations in the gene encoding for TDP-43, TARDBP, may be associated with ALS-TDP, but not dementia with TDP-43 pathology [38]. The APOE4 allele of the apolipoprotein E gene (APOE) is associated with increased risk in a variety of cognitive impairments, including AD [39, 40], VCID [41], and LATE [10, 42, 43•]. Additional risk alleles such as those in RBFOX1 are also associated with TDP-43 pathology [43•]. The gene ABCC9 codes for the potassium channel and sulfonylurea receptor SUR2; genetic risk alleles of ABCC9 are associated with HS [44]. In fact, ABCC9 polymorphisms are preferentially associated with HS over LATE, while polymorphisms in broader neurodegenerative risk genes TMEM106B, GRN, and APOE are associated with both LATE and HS [45]. While LATE and HS are inter-related, these findings suggest that the potential dissociation of LATE and HS is influenced by certain molecular markers.
Pathology and Genetics of TMEM106B
TMEM106B is a regulator of lysosomal degradation deeply implicated in TDP-43 proteinopathies [45, 46]. A common noncoding variant rs1990622 alters TMEM106B expression via local genome topology [47] and is strongly associated with TDP-43 pathology in autopsy cohorts of FTLD-TDP [48••, 49••] and LATE [50•]. Additional TMEM106B polymorphisms are also enriched in late-onset AD [51], which may perhaps represent (i) complicated interplay between distinct proteinopathies and risk alleles, (ii) common mechanisms such as degradation and clearance that link several proteinopathies, and/or (iii) pathological heterogeneity within the cohort for genetic sampling [52]. Interestingly, several studies have shown that TMEM106B fibrils are present in a variety of neurodegenerative diseases, including FTLD-TDP [53, 54, 55], so it is possible that TMEM106B deposits may also be present in LATE. The causal relationship between TMEM106B, TDP-43, and neurodegeneration is still unknown, but recent literature demarcates an emerging role for TMEM106B in several neurological disorders.
Non-TDP-43 Copathologies and Interactions
Deposition and misfolding of distinct proteins may interact, producing potential nonlinear combinatorial effects [56]. Autopsy and preclinical studies show the intermingling of TDP-43 with neurofibrillary tau tangles [57] and perhaps intracellular amyloid-β [58]. Associations have been found between TDP-43 burden and vascular disease markers, including robust relationships with arteriolosclerosis and microvascular damage in the basal ganglia and watershed areas [59, 60, 61], with some correlations between TDP-43 and microinfarcts and cerebral amyloid angiopathy [61]. Moreover, there are regional relationships and overlapping prevalence for α-synuclein and TDP-43 pathologies in LATE [9, 62•, 63] and FTLD-TDP [64, 65]. Compared to LATE + AD, LATE + LBD may harbor more frequent TDP-43 inclusions with differential severity in specific hippocampal subfields and earlier spread to dentate gyrus and brainstem [62•]. Note that other pathologies such as FUS may be mutually exclusive with TDP-43 in FTLD and ALS [66]. Such findings highlight intricate interactions of different pathologies to modulate the templating, misfolding, and spreading of other polypathologies. Cumulatively, the synergy between copathologies, or lack thereof, may typify a model of biochemical pathologies and cellular responses as actions and corresponding reactions and illuminate mixed disease contributors.
Emerging Biomarkers
Structural Imaging
Serial structural imaging with magnetic resonance imaging (MRI) offers an ideal platform to assess atrophy patterns associated with LATE. T1-weighted MRI is preferred for overall structural visualization of the brain while T2-weighted sequences can distinguish features in the MTL. Anterior-predominant neurodegeneration is seen in MTL, amygdala, and frontal structures [1••]. The rate of atrophy may be relatively slow in pure LATE as exemplified by the case in Fig. 1. Conversely, a more rapid decline in cognition and volume of limbic structures may be appreciated in cases of LATE mixed with AD (15; 16•). Distortion of amygdalar volume and shape is seen with TDP-43 inclusions [67]. With ex vivo imaging, TDP-43 severity is correlated to MTL thickness [68•, 69•]. Furthermore, anterior–posterior gradients of postmortem TDP-43 burden appear to manifest as greater atrophy in the anterior hippocampus and anterior cortical MTL structures (such as the entorhinal cortex). Indeed, TDP-43 pathology may be correlated with thinner cortex in the anterior MTL [70•] in comparison to tau burden, which may have a greater association with atrophy of the posterior MTL; the ratio of which may allow for distinguishing AD with or without concomitant TDP-43 pathology [70•, 71]. It has also been noted that atrophy rates in anterior brain regions are higher in FTLD-TDP than in LATE or mixed LATE and AD [72].
Example clinical vignette of a patient with LATE. A 78-year-old woman presents with several years of subjective memory loss and was clinically diagnosed with AD. A At baseline, T1-weighted coronal MRI (top) shows some volume loss in the bilateral hippocampi and medial temporal lobes, with axial FLAIR sequence scan depicting periventricular white matter hyperintensities corresponding to small vessel ischemia. B Ten years after baseline scan, coronal (top) computed tomography (CT) shows mild interval change of limbic structures, with some ventricular dilatation and widening of the lateral fissures compared to prior studies. Small vessel disease is redemonstrated as periventricular hypodensities on axial CT (bottom). C Psychometric testing over about nine years shows slow, minimal decline in Mini-Mental Status Examination (MMSE), Animal fluency, Word List (WL) delayed recall, and Trails B time (natural log-transformed). D At autopsy, immunohistochemistry of the hippocampus with TDP-43 antibody (1D3, images at × 20 and × 50) reveals TDP-43 cytoplasmic inclusions, consistent with a primary neuropathological diagnosis of LATE-NC. Additional staining showed diagnostic evidence of primary age-related tauopathy and Lewy body disease (amygdala-predominant) and did not reflect AD neuropathologic change
Positron Emission Tomography (PET)
Radionuclide imaging with 18F-Fluorodeoxyglucose (18F-FDG) has shown great promise in identifying in vivo spatial patterns that correlate well with postmortem confirmation of LATE [73••]. By assessing the hypometabolism of the MTL and frontal supraorbital ratio (FSO) relative to the metabolic sparing of the inferior temporal gyrus (I), a measure such as the I/MTL/FSO ratio can distinguish LATE with roughly 80% sensitivity and specificity [74•]. A similar regional ratio based on structural MRI had similar sensitivity but poorer specificity. Together, these studies support the notion that hypometabolism and atrophy on 18F-FDG and MRI can provide probabilistic support for a clinical diagnosis of LATE. Importantly, novel radiotracers that bind to TDP-43 are also being explored [75] and the molecular structure of brain-derived TDP-43 has been discovered [76], though it may be several more years until clinical studies for TDP-43 in vivo imaging are available [77]. Overall, currently available 18F-FDG PET imaging markers provide useful probabilistic prediction of LATE-NC.
Comparison of Imaging Biomarkers to Infer LATE Patterns
Without direct and specific imaging tracers for TDP-43 and other non-AD pathologies, we can infer the presence of unobservable copathologies based on their effects on observable AD measures. While tau pathology is tightly linked to neuronal loss and hypometabolism in AD [78, 79], additional entities such as non-AD pathologies and resilience factors may drive the decoupling of tau and neurodegeneration. Hence, comparing the amount of neurodegeneration on MRI or 18F-FDG PET expected based on a measure of AD pathology (such as 18F-Flortaucipir PET) has potential to highlight non-AD copathology such as TDP-43-related patterns of neurodegeneration, as well as spatial patterns associated with resilience due to genetic or environmental factors. In a series of studies, our group has shown that mismatch of neurodegeneration relative to tau pathology can predict the presence of non-AD pathologies, such as limbic-associated atrophy and hypometabolism suggestive of mixed AD with LATE [80•, 81•]. On imaging, patients in this group have elevated I/MTL/FSO ratio (Fig. 2). On longitudinal psychometric assessment, the limbic susceptible group has faster cognitive decline and more severe memory impairment than other groups [81•], all congruent with AD and LATE co-pathology [15, 20].
Limbic PET imaging patterns in susceptible and resilient patients with similar 18F-FDG standardized uptake value ratio (SUVR 0.87 to 0.89) but different tau load (SUVR 1.41 to 1.75) in the inferior temporal gyrus (ITG). 18F-Florbetaben (amyloid), 18F-Flortaucipir (tau), and.18F-FDG PET scans are shown for a A cognitively impaired 84-year-old male with amyloid + /tau + status and AD Assessment Scale-Cognitive (ADAS-Cog) score of 37.0 (higher is worse) and a B cognitively impaired 62-year-old female with A + /T + status and ADAS-Cog of 14.7. The patient in A demonstrates an imaging marker related to LATE seen as the relative sparing of the inferior temporal gyrus (I) relative to medial temporal lobe (MTL) and frontal supraorbital gyrus (FSO), measured by higher I/MTL/FSO than the patient in B. Hence, the patient in A has evidence concerning for both AD and non-AD (TDP-43) pathology potentially contributing to neurodegeneration not accounted for by tau pathology alone (as in “limbic susceptibility”)
Biofluid Measures of TDP-43
Assays reflecting TDP-43 pathology are currently in development. Improvements in immunoassays for TDP-43 and phospho-TDP-43 present in cerebrospinal fluid (CSF) and blood have led to some promise as markers of FTLD-TDP [82, 83•, 84•] and ALS-TDP [84•, 85, 86, 87, 88]. TDP-43 is packaged into neuronal and glial exosomes, which may also be detected in plasma [23, 89]. Hence, work is now underway to detect peripheral markers of TDP-43 in LATE cohorts. Since some studies saw an elevation of blood TDP-43 levels in patients with clinically diagnosed MCI or AD [83•, 90], it is possible that such measures may be detecting some TDP-43 pathology in the context of either LATE or mixed LATE and AD.
Additional Neuronal Markers
An array of neuron-specific markers may be dysregulated by TDP-43 pathology. For instance, calsyntenin-1 and neurexin-2a promote cell adhesion by regulating calcium homeostasis and synaptic cleft interactions, respectively. These proteins show lower expression in cerebrospinal fluid (CSF) of patients with FTLD-TDP and negative correlations with TDP-43 burden [91•]. CSF panels including calsyntenin-1 and neurexin-2a promoted the discrimination of FTLD-TDP from AD and FTLD-Tau with areas under the curve around 0.8 [91•]. As an mRNA-binding protein, TDP-43 enables the splicing of Stathmin-2 (STMN2) mRNA to its proper, full-length form by suppressing a cryptic polyadenylation site [92, 93]. However, in FTLD-TDP and ALS-TDP, TDP-43 loses this capacity and the cryptic site is unmasked, leading to aberrant accumulation of prematurely truncated STMN2 mRNA and reduction in full-length STMN2 mRNA [94, 95, 96]. Future steps for such biomarkers should determine if expression changes can be detected in additional sample sources. Although such biofluid and neural tissue markers are associated with TDP-43 pathology in FTLD-TDP and ALS-TDP, it is currently unclear if they also translate to LATE. Nevertheless, these encouraging findings support candidate neuronal biomarkers as downstream readouts of TDP-43 function and aggregation.
Clinical Management
Due to the recent definition of LATE as a distinct disease entity, the clinical evidence is still unclear whether symptomatic treatments for AD (such as acetylcholinesterase inhibitors or memantine) have beneficial effects on HS or LATE and potential therapies for LATE and HS are currently under investigation [1••]. For example, ABCC9/SUR2 is a potential target given the molecular relationships of ABCC9 in LATE, HS, and arteriolosclerosis. Sulfonylureas inhibit ABCC9/SUR2 and are associated with an increased risk of HS, even when controlling for the presence of diabetes [44]. Thus, ABCC9/SUR2 agonists such as nicorandil (NCT04120766) are currently being studied as possible investigational drugs for HS [97].
New therapeutic targets may emerge with increasing recognition of the diagnosis and pathobiology of LATE. Accordingly, greater insight into the natural history and clinical care of patients with LATE may coincide with a more comprehensive diagnosis and clinical trials for AD and other neurodegenerative disorders, as “precision medicine” paradigms are adopted to tailor the management of individual patients across heterogeneous and overlapping disease spectra.
Conclusion
Overall, LATE is a unique and highly prevalent disease process that can also coincide with and accelerate other neurodegenerative diseases. TDP-43 pathology and HS are linked to amnestic phenotype and slow clinical progression when presenting alone and faster decline when interacting with AD pathology. An assortment of genetic and imaging biomarkers exist that can be used to potentially support a diagnosis of LATE. Moreover, additional biomarkers from radiotracer imaging to biofluid assays of proteins and exosomes are on the horizon. Together, LATE is a common neurocognitive disease entity that should be recognized in the clinical setting.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Nelson PT, Dickson DW, Trojanowski JQ, et al. Limbic-predominant age-related TDP-43 encephalopathy (LATE): consensus working group report. Brain. 2019;142(6):1503–27 (Important paper from a consensus panel that establishes recommendations for diagnosing LATE.).
Besser LM, Teylan MA, Nelson PT. Limbic predominant age-related TDP-43 encephalopathy (LATE): clinical and neuropathological associations. J Neuropathol Exp Neurol. 2020;79(3):305–13.
Neumann M, Sampathu DM, Kwong LK, et al. Ubiquitinated TDP-43 in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Science. 2006;314(5796):130–3 (One of the first studies to discover TDP-43 pathology in neurodegenerative diseases, including FTLD and ALS.).
Arai T, Hasegawa M, Akiyama H, et al. TDP-43 is a component of ubiquitin-positive tau-negative inclusions in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Biochem Biophys Res Commun. 2006;351(3):602–11 (One of the first studies to discover TDP-43 pathology in neurodegenerative diseases, including FTLD and ALS.).
Amador-Ortiz C, Lin W-L, Ahmed Z, et al. TDP-43 immunoreactivity in hippocampal sclerosis and Alzheimer’s disease. Ann Neurol. 2007;61(5):435–45 (First study to find TDP-43 inclusions in hippocampal sclerosis and AD.).
Nelson PT, Brayne C, Flanagan ME, et al. Frequency of LATE neuropathologic change across the spectrum of Alzheimer’s disease neuropathology: combined data from 13 community-based or population-based autopsy cohorts. Acta Neuropathol. 2022;144(1):27–44 (Updated study determining prevalence of LATE in older adults.).
Jack CR, Bennett DA, Blennow K, et al. NIA-AA Research Framework: toward a biological definition of Alzheimer’s disease. Alzheimers Dement. 2018;14:535–62.
Meneses A, Koga S, O’Leary J, Dickson DW, Bu G, Zhao N. TDP-43 Pathology in Alzheimer’s disease. Mol Neurodegen. 2021;16:84.
Thomas DX, Bajaj S, McRae-McKee K, Hadjichrsanthou C, Anderson RM, Collinge J. Association of TDP-43 proteinopathy, cerebral amyloid angiopathy, and Lewy bodies with cognitive impairment in individuals with or without Alzheimer’s disease neuropathology. Sci Rep. 2020;10:14579.
Robinson JL, Lee EB, Xie SX, et al. Neurodegenerative disease concomitant proteinopathies are prevalent, age-related and APOE4-associated. Brain. 2018;141(7):2181–93.
Dickson DW, Davies P, Bevona C, et al. Hippocampal sclerosis: a common pathological feature of dementia in very old (> or =80 years of age) humans. Acta Neuropathol. 1994;88:212–21 (First pathological study to define hippocampal sclerosis, a common neuroanatomical feature in LATE.).
Mehta P, Kaye W, Raymond J, et al. Prevalence of amyotrophic lateral sclerosis — United States, 2015. MMWR Morb Mortal Wkly Rep. 2018;67:1285–9.
Onyike CU, Diehl-Schmid J. The epidemiology of frontotemporal dementia. Int Rev Psychiatry. 2013;25(2):130–7.
Lopez OL, Kofler J, Chang YF, et al. Hippocampal sclerosis, TDP-43, and the duration of the symptoms of dementia of AD patients. Ann Clin Transl Neurol. 2020;7(9):1546–56.
Josephs KA, Dickson DW, Tosakulwong N, et al. Rates of hippocampal atrophy and presence of post-mortem TDP-43 in patients with Alzheimer’s disease: a longitudinal retrospective study. Lancet Neurol. 2017;16(11):917–24.
Kapasi A, Yu L, Boyle PA, Barnes LL, Bennett DA, Schneider JA. Limbic-predominant age-related TDP-43 encephalopathy (LATE), ADNC pathology, and cognitive decline in aging. Neurology. 2020;95(14):e1951–62 (Recent study on the influence of LATE and AD pathologies on cognitive decline rates.).
Gauthreaux KM, Teylan MA, Katsumata Y, et al. Limbic-predominant age-related TDP-43 encephalopathy: medical and pathologic factors associated with comorbid hippocampal sclerosis. Neurology. 2022;98(14):e1422–33 (Important study dissecting the differences in clinical and pathological factors affecting LATE with HS vs. LATE without HS.).
Wilson RS, Yu L, Trojanowski JQ, et al. TDP-43 pathology, cognitive decline, and dementia in old age. JAMA Neurol. 2013;70(11):1418–24.
Josephs KA, Murray ME, Whitwell JL, et al. Staging TDP-43 pathology in Alzheimer’s disease. Acta Neuropathol. 2014;127(3):441–50.
Nag S, Yu L, Boyle PA, Leurgans SE, Bennett DA, Schneider JA. TDP-43 pathology in anterior temporal pole cortex in aging and Alzheimer’s disease. Acta Neuropathol Commun. 2018;6:33.
Liu KY, Reeves S, McAleese KE, Attems J, Francis P, Thomas A, Howard R. Neuropsychiatric symptoms in limbic-predominant age-related TDP-43 encephalopathy and Alzheimer’s disease. Brain. 143(12):3842–3849. Important investigation on neurological and psychiatric symptoms in LATE and AD.
Blass DM, Hatanpaa KJ, Rao V, Steinberg M, Troncoso JC, Rabins PV. Dementia in hippocampal sclerosis resembles frontotemporal dementia more than Alzheimer disease. Neurology. 2004;63(3):492–7.
Jo M, Lee S, Jeon YM, Kim S, Kwon Y, Kim HJ. The role of TDP-43 propagation in neurodegenerative diseases: integrating insights from clinical and experimental studies. Exp Mol Med. 2020;52(10):1652–62.
Cohen TJ, Lee VM-Y, Trojanowski TJ. TDP-43 functions and pathogenic mechanisms implicated in TDP-43 proteinopathies. Trends Mol Med. 2011;17(11):659–667.
Colombrita C, Zennaro E, Fallini C, et al. TDP-43 is recruited to stress granules in conditions of oxidative insult. J Neurochem. 2009;111(4):1051–61.
McGurk L, Gomes E, Guo L, et al. Poly(ADP-ribose) prevents pathological phase separation of TDP-43 by promoting liquid demixing and stress granule localization. Mol Cell. 2018;71(5):703–17.
Barmada SJ, Skibinski G, Korb E, Rao EJ, Wu JY, Finkbeiner S. Cytoplasmic mislocalization of TDP-43 is toxic to neurons and enhanced by a mutation associated with familial amyotrophic lateral sclerosis. J Neurosci. 2010;30(2):639–49.
Herzog JJ, Xu W, Deshpande M, et al. TDP-43 dysfunction restricts dendritic complexity by inhibiting CREB activation and altering gene expression. Proc Natl Acad Sci USA. 2020;117(21):11760–9.
Paolicelli RC, Jawaid A, Henstridge CM, et al. TDP-43 Depletion in microglia promotes amyloid clearance but also induces synapse loss. Neuron. 2017;95:293–308.
James BD, Wilson RS, Boyle PA, Trojanowski JQ, Bennett DA, Schneider JA. TDP-43 stage, mixed pathologies, and clinical Alzheimer’s-type dementia. Brain. 2016;139(11):2983–93.
Porta S, Xu Y, Lehr T, et al. Distinct brain-derived TDP-43 strains from FTLD-TDP subtypes induce diverse morphological TDP-43 aggregates and spreading patterns in vitro and in vivo. Neuropathol Appl Neurobiol. 2021;47(7):1033–49.
Tan RH, Ke YD, Ittner LM, Halliday GM. ALS/FTLD: experimental models and reality. Acta Neuropathol. 2017;133(2):177–96.
de Boer EMJ, Orie VK, Williams T, et al. TDP-43 proteinopathies: a new wave of neurodegenerative diseases. J Neurol Neurosurg Psychiatry. 2021;92:86–95.
Niccoli T, Partridge L, Isaacs AM. Ageing as a risk factor for ALS/FTD. Hum Mol Genet. 2017;26(R2):R105–13.
Robinson JL, Porta S, Garrett FG, et al. Limbic-predominant age-related TDP-43 encephalopathy differs from frontotemporal lobar degeneration. Brain. 2020;143(9):2844–57.
Wider C, Dickson DW, Stoessl AJ, et al. Pallidonigral TDP-43 pathology in Perry syndrome. Parkinsonism Relat Disord. 2009;15(4):281–6.
Dickson DW, Baker M, Rademakers R. Common variant in GRN is a genetic risk factor for hippocampal sclerosis in the elderly. Neurodegenerative Dis. 2010;7:170–4 (One of the first inquiries into genetic risk for hippocampal sclerosis.).
Mackenzie IRA, Rademakers R. The role of TDP-43 in amyotrophic lateral sclerosis and frontotemporal dementia. Curr Opin Neurol. 2008;21(6):693–700.
Strittmatter WJ, Saunders AM, Schmechel D, Pericak-Vance M, Enghild J, Salvesen GS, Roses AD. Apolipoprotein E: high-avidity binding to beta-amyloid and increased frequency of type 4 allele in late-onset familial Alzheimer disease. Proc Natl Acad Sci USA. 1993;90(5):1977–81.
Wolk DA, Dickerson BC. Alzheimer’s disease neuroimaging initiative. Apolipoprotein E (APOE) genotype has dissociable effects on memory and attentional-executive network function in Alzheimer’s disease. Proc Natl Acad Sci USA. 2010;107(22):10256–61.
Duong MT, Nasrallah IM, Wolk DA, Chang CCY, Chang T-Y. Cholesterol, atherosclerosis, and APOE in vascular contributions to cognitive impairment and dementia (VCID): potential mechanisms and therapy. Front Aging Neurosci. 2021;13: 647990.
Yang H-S, Yu L, Whie CC, et al. Evaluation of TDP-43 proteinopathy and hippocampal sclerosis in relation to APOE ε4 haplotype status: a community-based cohort study. Lancet Neurol. 2018;17(9):773–81.
Yang H-S, White CC, Klein H-U, et al. Genetics of gene expression in the aging human brain reveal TDP-43 proteinopathy pathophysiology. Neuron. 2020;107:496–508 (Important study that identified several risk loci of TDP-43 proteinopathies.).
Nelson PT, Estus S, Abner EL, et al. ABCC9 gene polymorphism is associated with hippocampal sclerosis of aging pathology. Acta Neuropathol. 2014;127(6):825–43.
Dugan AJ, Nelson PT, Katsumata Y, et al. Analysis of genes (TMEM106B, GRN, ABCC9, KCNMB2, and APOE) implicated in risk for LATE-NC and hippocampal sclerosis provides pathogenetic insights: a retrospective genetic association study. Acta Neuropathol Comm. 2021;9:152.
Brady OA, Zheng Y, Murphy K, Huang M, Hu F. The frontotemporal lobar degeneration risk factor, TMEM106B, regulates lysosomal morphology and function. Hum Mol Genet. 2013;22(4):685–95.
Gallagher MD, Posavi M, Huang P, et al. A dementia-associated risk variant near TMEM106B alters chromatin architecture and gene expression. Am J Hum Genet. 2017;101(5):643–63.
Van Deerlin VM, Sleiman PMA, Martinez-Lage M, et al. Common variants at 7p21 are associated with frontotemporal lobar degeneration with TDP-43 inclusions. Nat Genet. 2010;42(3):234–9 (First study to map the genetic architecture of TDP-43 disorders.).
van der Zee J, Van Langenhove T, Kleinberger G, et al. TMEM106B is associated with frontotemporal lobar degeneration in a clinically diagnosed patient cohort. Brain. 2011;134(Pt 3):808–15 (First study to map the genetic architecture of TDP-43 disorders.).
Yu L, De Jager PL, Yang J, Trojanowski JQ, Bennett DA, Schneider JA. The TMEM106B locus and TDP-43 pathology in older persons without FTLD. Neurology. 2015;84(9):927–34.
Wightman DP, Jansen IE, Savage JE, et al. A genome-wide association study with 1,126,563 individuals identifies new risk loci for Alzheimer’s disease. Nat Genet. 2021;53:1276–82.
Li Z, Farias FHG, Dube U, et al. The TMEM106B FTLD-protective variant, rs1990621, is also associated with increased neuronal proportion. Acta Neuropathol. 2020;139(1):45–61.
Chang A, Xiang X, Wang J, et al. Homotypic fibrillization of TMEM106B across diverse neurodegenerative diseases. Cell. 2022;185:1–10.
Jiang YX, Cao Q, Sawaya MR, et al. Amyloid fibrils in disease FTLD-TDP are composed of TMEM106B not TDP-43. Nature. 2022;605:304–9.
Schweighauser M, Arseni D, Bacioglu M, et al. Age-dependent formation of TMEM106B amyloid filaments in human brains. Nature. 2022;605:310–4.
Robinson JL, Richardson H, Xie SX, et al. The development and convergence of copathologies in Alzheimer’s disease. Brain. 2021;144(3):953–62.
Latimer CS, Burke BT, Liachko NF, et al. Resistance and resilience to Alzheimer’s disease pathology are associated with reduced cortical pTau and absence of limbic-predominant age-related TDP-43 encephalopathy in a community-based cohort. Acta Neuropathol Commun. 2019;7:91.
Shih Y-H, Tu L-H, Chang T-Y, et al. TDP-43 interacts with amyloid-β, inhibits fibrillization, and worsens pathology in a model of Alzheimer’s disease. Nat Commun. 2020;11:5950.
Katsumata Y, Fardo DW, Kukull WA, Nelson PT. Dichotomous scoring of TDP-43 proteinopathy from specific brain regions in 27 academic research centers: associations with Alzheimer’s disease and cerebrovascular disease pathologies. Acta Neuropathol Comm. 2018;6:142.
Raghavan S, Przybelski SA, Reid RI, et al. White matter damage due to vascular, tau, and TDP-43 pathologies and its relevance to cognition. Acta Neuropathol Comm. 2022;10:16.
Agrawal S, Yu L, Kapasi A, et al. Limbic-predominant age-related TDP-43 encephalopathy neuropathologic change and microvascular pathologies in community-dwelling older persons. Brain Pathol. 2021;31(3): e12939.
Uemura MT, Robinson JL, Cousins KAQ, et al. Distinct characteristics of limbic-predominant age-related TDP-43 encephalopathy in Lewy body disease. Acta Neuropathol. 2022;143(1):15–31 (Recent investigation elucidating the histopathological differences between LATE+LBD and LATE+AD.).
Agrawal S, Yu L, Nag S, et al. The association of Lewy bodies with limbic-predominant age-related TDP-43 encephalopathy neuropathologic changes and their role in cognition and Alzheimer’s dementia in older persons. Acta Neuropathol Commun. 2021;9:156.
Bayram E, Shan G, Cummings JL. Associations between comorbid TDP-43, Lewy body pathology, and neuropsychiatric symptoms in Alzheimer’s disease. J Alzheimers Dis. 2019;69(4):953–61.
Nakashima-Yasuda H, Uryu K, Robinson J, et al. Co-morbidity of TDP-43 proteinopathy in Lewy body related diseases. Acta Neuropathol. 2007;114(3):221–9.
Guo L, Shorter J. Biology and pathobiology of TDP-43 and emergent therapeutic strategies. Cold Spring Harb Perspect Med. 2017;7(9): a024554.
Makkinejad N, Schneider JA, Yu J, et al. Associations of amygdala volume and shape with transactive response DNA-binding protein 43 (TDP-43) pathology in a community cohort of older adults. Neurobiol Aging. 2019;77:104–11.
Ravikumar S, Wisse LEM, Lim S, et al. Ex vivo MRI atlas of the human medial temporal lobe: characterizing neurodegeneration due to tau pathology. Acta Neuropathol Comm. 2021;9:173 (Recent investigation comparing the effects of TDP-43 and tau pathology on MTL thickness on postmortem imaging.).
Wisse LEM, Ravikumar S, Ittyerah R, et al. Downstream effects of polypathology on neurodegeneration of medial temporal lobe subregions. Acta Neuropathol Comm. 2021;9:128 (Recent work to evaluate the contributions of TDP-43, amyloid, tau, and α-synuclein pathology on MTL thickness with ex vivo MRI.).
de Flores R, Wisse LEM, Das SR, et al. Contribution of mixed pathology to medial temporal lobe atrophy in Alzheimer’s disease. Alzheimers Dement. 2020;16(6):843–52 (Important investigation on the effects of TDP-43 and tau pathology on MTL thickness. TDP-43 burden was associated with anterior MTL atrophy.).
de Flores R, Das SR, Xie L, et al. Medial temporal lobe networks in Alzheimer’s disease: structural and molecular vulnerabilities. J Neurosci. 2022;42(10):2131–41.
Buciuc M, Martin PR, Tosakulwong N, et al. TDP-43-associated atrophy in brains with and without frontotemporal lobar degeneration. Neuroimage Clin. 2022;34: 102954.
Botha H, Mantyh WG, Murray ME, et al. FDG-PET in tau-negative amnestic dementia resembles that of autopsy-proven hippocampal sclerosis. Brain. 2018;141(4):1201–17 (First study to show a distinct 18F-FDG PET pattern for pathologically defined LATE.).
Buciuc M, Botha H, Murray ME, et al. Utility of FDG-PET in diagnosis of Alzheimer-related TDP-43 proteinopathy. Neurology. 2020;85:e23–34 (Important study that improves an 18F-FDG PET pattern for LATE and compares this biomarker to structural MRI.).
Tanzey S, Brooks A, Shao X, Scott P. Extraction of enriched phosphorylated TDP43 from ALS tissue for evaluation of new TDP-43 radiotracers. J Nucl Med. 2020;61(S1):1038.
Arseni D, Hasegawa M, Murzin AG, Kametani F, Arai M, Yoshida M, Ryskeldi-Falcon B. Structure of pathological TDP-43 filaments from ALS with FTLD. Nature. 2022;601(7891):139–43.
Tiepolt S, Patt M, Aghakhanyan G, et al. Current radiotracers to image neurodegenerative diseases. EJNMMI Radiopharm Chem. 2019;4:17.
Gómez-Isla T, Hollister R, West H, et al. Neuronal loss correlates with but exceeds neurofibrillary tangles in Alzheimer’s disease. Ann Neurol. 1997;41(1):17–24.
Gómez-Isla T, Frosch MP. Lesions without symptoms: understanding resilience to Alzheimer disease neuropathological changes. Nat Rev Neurol 2022;18(6):323–332
Das SR, Lyu X, Duong MT, et al. Tau-atrophy variability reveals phenotypic heterogeneity in Alzheimer’s disease. Ann Neurol. 2021;90:751–62 (First imaging study to explicitly model the mismatch between tau pathology and neurodegeneration on MRI).
Duong MT, Das SR, Lyu X, et al. Dissociation of tau pathology and neuronal hypometabolism within the ATN framework of Alzheimer’s disease. Nat Commun. 2022;13(1):1495 (First PET study to infer non-AD copathologies such as TDP-43 and α-synuclein imaging patterns based on hypometabolism relative to AD tau accumulation.).
Goossens J, Vanmechelen E, Trojanowski JQ, et al. TDP-43 as a possible biomarker for frontotemporal lobar degeneration: a systematic review of existing antibodies. Acta Neuropathol Comm. 2015;3:15.
Foulds P, McAuley E, Gibbons L, et al. TDP-43 protein in plasma may index TDP-43 brain pathology in Alzheimer’s disease and frontotemporal lobar degeneration. Acta Neuropathol. 2008;116:141–6 (One of the first papers to detect plasma TDP-43 protein in patients with FTLD and AD. The patients with AD and TDP-43 biomarkers may in fact have mixed LATE with AD.).
Steinacker P, Hendrich C, Sperfeld AD, et al. TDP-43 in cerebrospinal fluid of patients with frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Arch Neurol. 2008;65(11):1481–7 (One of the first studies to detect elevated TDP-43 protein in the CSF of patients with TDP-43 pathology.).
Ren Y, Li S, Chen S, et al. TDP-43 and phosphorylated TDP-43 levels in paired plasma and CSF samples in amyotrophic lateral sclerosis. Front Neurol. 2021;12: 663637.
Beyers L, Günther R, Koch JC, et al. TDP-43 as structure-based biomarker in amyotrophic lateral sclerosis. Ann Clin Transl Neurol. 2021;8(1):271–7.
Majumder V, Gregory JM, Barria MA, Green A, Pal S. TDP-43 as a potential biomarker for amyotrophic lateral sclerosis: a systematic review and meta-analysis. BMC Neurol. 2018;18:90.
Kasai T, Tokuda T, Ishigami N, et al. Increased TDP-43 protein in cerebrospinal fluid of patients with amyotrophic lateral sclerosis. Acta Neuropathol. 2009;117(1):55–62.
Zhang N, Gu D, Meng M, Gordon ML. TDP-43 is elevated in plasma neuronal-derived exosomes of patients with Alzheimer’s disease. Front Aging Neurosci. 2020;12:166.
Sun L, Li W, Yue L, Xiao S. Blood TDP-43 combined with demographics information predicts dementia occurrence in community non-dementia elderly. J Alzheimers Dis. 2021;79(1):301–9.
González AC, Irwin DJ, Alcolea D, et al. Multimarker synaptic protein cerebrospinal fluid panels reflect TDP-43 pathology and cognitive performance in a pathological cohort of frontotemporal lobar degeneration. Mol Neurodegen. 2022;17:29 (Essential study identifying CSF markers of TDP-43 pathology in FTLD-TDP compared to FTLD-Tau and AD.).
Mann JR, Gleixner AM, Mauna JC, et al. RNA binding antagonizes neurotoxic phase transitions of TDP-43. Neuron. 2019;102:321–38.
Benarroch E. What is the role of stathmin-2 in axonal biology and degeneration? Neurology. 2021;97:330–3.
Klim JR, Williams LA, Limone F, et al. ALS-implicated protein TDP-43 sustains levels of STMN2, a mediator of motor neuron growth and repair. Nat Neurosci. 2019;22:167–79.
Melamed Z, López-Erauskin J, Baughn MW, et al. Premature polyadenylation-mediated loss of stathmin-2 is a hallmark of TDP-43-dependent neurodegeneration. Nat Neurosci. 2019;22:180–90.
Prudencio M, Humphrey J, Pickles S, et al. Truncated stathmin-2 is a marker of TDP-43 pathology in frontotemporal dementia. J Clin Invest. 2020;130(11): e139741.
Ighodaro ET, Jicha GA, Schmitt FA, et al. Hippocampal sclerosis of aging can be segmental: two cases and review of the literature. J Neuropathol Exp Neurol. 2015;74(7):642–52.
Acknowledgements
The authors thank our lab members for helpful discussions and for study investigators, staff, participants, and families for their support.
Funding
Funding was provided by the Ruth L. Kirschstein National Research Service Award (NIA F30 AG074524, Michael Tran Duong) and the University of Pennsylvania Alzheimer’s Disease Core Center grant (NIA P30 AG072979, David A. Wolk).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
David A. Wolk reports grants from Merck, Biogen, Eli Lilly/Avid and additional fees from GE Healthcare, Functional Neuromodulation and Neuronix, all outside of this work. Michael Tran Duong has no conflicts of interest to report.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Dementia
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Duong, M.T., Wolk, D.A. Limbic-Predominant Age-Related TDP-43 Encephalopathy: LATE-Breaking Updates in Clinicopathologic Features and Biomarkers. Curr Neurol Neurosci Rep 22, 689–698 (2022). https://doi.org/10.1007/s11910-022-01232-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11910-022-01232-4