Abstract
TDP-43 immunoreactivity occurs in 19–57 % of Alzheimer’s disease (AD) cases. Two patterns of TDP-43 deposition in AD have been described involving hippocampus (limbic) or hippocampus and neocortex (diffuse), although focal amygdala involvement has been observed. In 195 AD cases with TDP-43, we investigated regional TDP-43 immunoreactivity with the aim of developing a TDP-43 in AD staging scheme. TDP-43 immunoreactivity was assessed in amygdala, entorhinal cortex, subiculum, hippocampal dentate gyrus, occipitotemporal, inferior temporal and frontal cortices, and basal ganglia. Clinical, neuroimaging, genetic and pathological characteristics were assessed across stages. Five stages were identified: stage I showed scant-sparse TDP-43 in the amygdala only (17 %); stage II showed moderate-frequent amygdala TDP-43 with spread into entorhinal and subiculum (25 %); stage III showed further spread into dentate gyrus and occipitotemporal cortex (31 %); stage IV showed further spread into inferior temporal cortex (20 %); and stage V showed involvement of frontal cortex and basal ganglia (7 %). Cognition and medial temporal volumes differed across all stages and progression across stages correlated with worsening cognition and medial temporal volume loss. Compared to 147 AD patients without TDP-43, only the Boston Naming Test showed abnormalities in stage I. The findings demonstrate that TDP-43 deposition in AD progresses in a stereotypic manner that can be divided into five distinct topographic stages which are supported by correlations with clinical and neuroimaging features. Given these findings, we recommend sequential regional TDP-43 screening in AD beginning with the amygdala.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In 2006, two independent investigators reported that the TAR DNA binding protein of 43 kDa (TDP-43) was accumulated pathologically in the brains of patients with frontotemporal lobar degeneration (FTLD) and with motor neuron disease (MND) [2, 31]. Subsequently, we demonstrated that TDP-43 pathology is also detected in the brains of patients with Alzheimer’s disease (AD) [1]. This finding has been confirmed by many different groups of investigators [3, 4, 9, 14, 15, 18, 20, 22, 33, 37]. When studies that had assessed more than 50 AD patients were reviewed [1, 3, 4, 9, 37] (Table 1), the proportion of AD patients with TDP-43 ranged from 19 to 57 % and a common finding across studies was that the presence of TDP-43 was associated with older age at death.
We have previously demonstrated that the distribution of TDP-43 in AD is variable and can show one of two patterns [1]. In the first pattern, TDP-43 immunoreactivity is limited to the entorhinal cortex and dentate gyrus of the hippocampus with minimal or no involvement of occipitotemporal cortex (OTC) while in the second pattern, immunoreactivity is more widespread and involves OTC and inferior temporal gyri. While we refer to the former as limbic, and the later as diffuse, a subsequent study of an independent series of 29 AD cases found that TDP-43 can deposit in the amygdala without there being additional involvement of the dentate gyrus of the hippocampus or involvement elsewhere [15]. In fact, it is clear that studies which assess the amygdala find a higher proportion of AD patients with TDP-43 immunoreactivity (Table 1). Furthermore, the identification of focal amygdala involvement raises the question of whether there is a sequential progression of TDP-43 deposition in AD that starts in the amygdala.
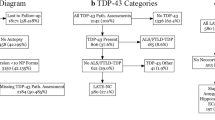
Variability in morphology and distribution of neuronal inclusions in FTLD led to two independent methods to subtype FTLD by ubiquitin [25, 34]. The two classification systems were harmonized [26], although the schemes did not provide a means for classifying TDP-43 that occurs in the setting of AD and other disorders, such as amyotrophic lateral sclerosis (ALS). Three main subtypes were recognized: Type A was characterized by pleomorphic neuronal cytoplasmic inclusions (NCIs), sometimes accompanied by neuronal intranuclear inclusions (NIIs), as well as dystrophic neurites (DNs) that were most numerous in the upper cortical layers; Type B had a predominance of NCIs, as well as cytoplasmic TDP-43 that does not form well-defined inclusions (“pre-inclusions”) with minimal DNs; and Type C had a predominance of DNs, which were often longer and thicker than DNs in Type A and they were found in all cortical layers with minimal NCIs. In neither Type B nor Type C are NIIs common. Unfortunately, in these typing schemes, the characterization was limited to assessing hippocampus and neocortex.
The aim of this study was to develop a staging scheme of TDP-43 progression in AD and to determine whether clinical, neuroimaging and pathological features would support such a scheme. In order to accomplish our aims we assessed clinical, neuroimaging and pathological characteristics, including TDP-43 typing, across a large cohort of 195 AD cases that had TDP-43 immunoreactivity.
Materials and methods
Three hundred and forty-two cases with intermediate-high probability AD according to the National Institute on Aging and the Reagan Institute criteria (NIA-Reagan) [40], and Braak neurofibrillary tangle (NFT) stage of IV–VI [6] were utilized in this study. Of these 342 cases, 195 had TDP-43 immunoreactivity while the remainder did not. All cases had been prospectively recruited and followed in the Mayo Clinic Alzheimer’s Disease Research Center (ADRC) or Alzheimer Patient Registry (ADPR) between 1992 and 2005. For this study, we assessed education, sex, age at onset, age at death, Mini-Mental State Examination (MMSE) [12], Clinical Dementia Rating Scale Sum of Boxes (CDR-SB) [29], the memory subscore of the Dementia Rating Scale (mDRS) [27], the Boston Naming Test (BNT) [21], and apolipoprotein E (APOE) e4 status [8, 17].
Briefly, neuropathological examinations had been performed according to the recommendations of the Consortium to Establish a Registry for AD (CERAD) [28] by one of two board certified neuropathologists (DWD or JEP). Each case was assigned a Braak neurofibrillary tangle (NFT) stage [6] using modified Bielschowsky silver stain, on the basis of the earliest appearance of NFT pathology. The presence of Lewy bodies outside of the amygdala was recorded using alpha-synuclein stain. Hippocampal sclerosis (HpScl) was diagnosed on Hematoxylin and Eosin stained slides as the presence of neuronal loss in the subiculum and/or CA1 regions of the hippocampus out of proportion to the burden of NFTs present in these regions [10].
For TDP-43 analysis, formalin-fixed, paraffin-embedded tissue for each region-of-interest was immunostained for TDP-43 (polyclonal antibody MC2085 that recognizes a peptide sequence in the 25-kDa C-terminal fragment [42]) with a DAKO-Autostainer (DAKO-Cytomaton, Carpinteria, California) and 3,3′-diaminobenzidine as the chromogen. Sections were lightly counterstained with Hematoxylin. For this study, the following regions were reviewed: amygdala, entorhinal cortex, subiculum, dentate gyrus of the hippocampus, OTC, inferior temporal cortex, middle frontal cortex and basal ganglia. For basal ganglia, we assessed the putamen, globus pallidus and caudate. All slides were reviewed simultaneously by two observers (DWD, KAJ) who agreed on the presence of TDP-43 immunoreactivity defined as NCIs, DNs or NIIs in any region (TDP-positive). The severity of TDP-43 deposition in the amygdala was graded on a four-point scale (1 = scant [one to two inclusions only], 2 = sparse, 3 = moderate, 4 = frequent). TDP-43 typing was performed in cases with hippocampal or neocortical TDP-43 immunoreactive inclusions based on the Harmonized criteria [26].
Two-hundred and forty-eight cases had an antemortem volumetric MRI scan performed according to a standardized protocol, as previously detailed [16]. For this study, the MRI scan closest to death was used. Preprocessing steps included correction for gradient non-linearity and intensity non-uniformity [35]. Grey matter volumes of amygdala, hippocampus, entorhinal cortex, OTC, lateral temporal lobe, and lateral frontal lobe were measured using atlas-based parcellation in SPM5 and the automated anatomic labeling (AAL) atlas [36], as previously described [38]. These regions were selected to mirror the regions included in the pathological analysis. Left and right volumes were averaged for each region. Total intracranial volume was calculated as previously described [39], and used to correct for differences in head size.
Demographic and pathological variables were assessed using Chi-square tests for categorical variables and ANOVA for continuous variables. Significance was set at p < 0.05. Post hoc t tests with unequal variances were performed if the ANOVA was significant. Clinical and neuroimaging variables were assessed with ANOVA and logistic regression with age at test and time from disease onset to test included as a covariate. Pair-wise correlations were performed between clinical and neuroimaging continuous variables and the staging scheme. Statistical analyses were performed utilizing JMP (JMP Software, version 9.0.0; SAS Institute Inc., Cary, NC, USA). Results reported as median (inter-quartile range).
Results
TDP-43 in AD staging scheme
Of the 195 TDP-positive cases, three cases were missing some paraffin blocks and were excluded from further analysis. Therefore, staging was performed in 192 cases. Five stages were identified based on the sequential progression of regional TDP-43 deposition in AD (Table 2).
Stage I consisted of 33 cases (17 %) which showed scant to sparse involvement of the amygdala (Fig. 1). None of these 33 cases showed involvement of the entorhinal cortex, subiculum, dentate gyrus of the hippocampus, OTC, inferior temporal cortex or middle frontal cortex. One case, however, had scant TDP-43 immunoreactive inclusions in the amygdala and basal ganglia (Table 2).
Pathological findings from representative cases for each of the five stages. In stage I, scant-sparse TDP-43 immunoreactive inclusions are observed only in the amygdala. In stage II, inclusions are moderate-frequent in the amygdala and extend into entorhinal cortex, but are not identified in dentate, OTC, temporal or frontal cortices. In stage III, inclusions extend into hippocampus and OTC, but are not identified in temporal or frontal cortices. In stage IV, inclusions extend into the inferior temporal cortex. In stage V, TDP-43 immunoreactivity is widespread and affects the frontal cortex or basal ganglia. Bar 30 micron. All images are the same magnification. Arrows point to NCI’s
Stage II consisted of 48 cases (25 %) which showed involvement of both the amygdala and entorhinal cortex or subiculum (Fig. 1). In these cases, TDP-43 deposition in the amygdala was moderate-frequent. Forty-three of the 48 cases had TDP-43 deposition in the entorhinal cortex, of which 29 also had involvement of the subiculum. Five cases in stage II did not show involvement of entorhinal cortex but had TDP-43 immunoreactivity in the amygdala and subiculum (Table 2).
Stage III consisted of 59 cases (31 %). The amygdala was involved in all stage III cases, with entorhinal cortex and subiculum involved in all but two cases (Table 2). All stage III cases showed involvement of the dentate gyrus of the hippocampus or the OTC (Fig. 1). The majority of these 59 cases (n = 51) had involvement of both the dentate gyrus of the hippocampus and the OTC. However, six cases showed involvement of the dentate gyrus of the hippocampus without involvement of the OTC, and two cases showed involvement of the OTC without involvement of the dentate gyrus (Table 2).
Stage IV consisted of 39 cases (20 %). The amygdala, entorhinal cortex, subiculum, OTC and inferior temporal cortex were involved in all cases (Fig. 1). The dentate gyrus of the hippocampus was involved in all cases but one (Table 2).
Stage V consisted of 13 cases (7 %). All but one of the stage V cases showed involvement of amygdala, entorhinal cortex, subiculum, dentate gyrus of the hippocampus, OTC and inferior temporal cortex. All stage V cases showed involvement of the middle frontal cortex or basal ganglia (Fig. 1). Of these 13 cases, 11 showed involvement of both the middle frontal cortex and basal ganglia, while two showed involvement of just the middle frontal cortex. One case did not show involvement of the inferior temporal cortex (Table 2).
Clinical, neuroimaging and pathological differences across stages I–V
Demographic variables did not differ across the five stages, although there were trends for differences in age at onset and disease duration (Table 3). All four clinical measures differed across the five stages, with stage I generally showing the best performance and stage V showing the worst performance (Table 3). On post hoc testing, stage I showed better performance on MMSE, CDR-SB and mDRS compared to the other stages, and better performance on BNT than stage III. Stage II showed better performance on CDR-SB, mDRS and BNT compared to stage IV, and better performance on mDRS compared to stage V. In addition, differences were observed between stages III and IV on BNT, and stages III and V on mDRS. Statistically significant correlations were observed between stages I–V and all four clinical measures (Table 4), showing a decline in performance with increasing stage.
Volumes of the hippocampus, entorhinal cortex and lateral frontal lobe differed across the five stages (Table 3). For the hippocampus, stage I showed significantly larger volumes than all the other stages. Stage I also showed the largest entorhinal cortex volume, with significant differences observed from stages III, IV and V. Stage II showed significantly larger entorhinal volumes than stages III and V. Volumes of the lateral frontal lobe were largest in stage I, which differed significantly from stages II, III and V. However, stage IV showed significantly larger volumes than stages II, III and V. Only the hippocampal and entorhinal cortex volumes, but not lateral frontal lobe volume, showed statistically significant correlations with stage (Table 4), showing that only the hippocampus and entorhinal cortex volumes progressively declined with increasing stage.
The severity of amygdala TDP-43 immunoreactivity increased across the five stages (Table 3), with stages I and II showing lower TDP-43 burdens than stages III, IV and V. The proportion of TDP types A, B and C differed across stages III, IV and V. While the majority of cases in each of these stages showed pathological characteristics consistent with type A, stage III showed the highest proportion of type B cases (36 %) and stage V showed the highest proportion of type C cases (15 %). The presence of HpScl was rare in stages I and II, but was observed in almost half of the stage III cases and more than three quarters of the stage IV and V cases. No differences were observed across stages in Braak stage or the proportion of Lewy bodies.
TDP-43 in AD stages I–V compared to TDP-negative AD
Clinical and neuroimaging features were also compared between each of the five stages and the 147 AD cases that did not have any TDP-43 immunoreactive inclusions (TDP-negative) (Fig. 2). Consistent with the findings above, there was a graded difference in the clinical variables and hippocampal volumes with stage I showing the least differences compared to TDP-negative AD, followed by stage II, stage III and then stage IV. The entorhinal cortex volumes also declined with increasing stage, although the most significant differences from TDP-negative AD were observed at stage III. Clinical performance and hippocampal and entorhinal volumes in stage V were similar to stage IV, although the p values were less striking. The only variable that showed a significant difference between stage I and the TDP-negative AD cases was the BNT. On the contrary, all variables differed between stages II, III, IV and V and the TDP-negative cases, except for the entorhinal cortex in stage II.
Line plots show significant differences between TDP-negative cases and all five stages. Data points represent median values for each variable. *p < 0.05; **p < 0.01; ***p < 0.001. Hippocampal and entorhinal MRI volumes are shown as volume/TIV × 100. MMSE Mini-Mental State Examination, CDR-SB Clinical Dementia Rating Scale Sum of Boxes, mDRS memory subscale of the Dementia Rating Scale, BNT Boston Naming Test
Discussion
In our large cohort of patients, we have identified five distinct stages showing stereotypic progression of TDP-43 deposition in AD. TDP-43 deposition in AD occurs first in the amygdala (stage I), and then progresses to entorhinal cortex and subiculum (stage II), followed by hippocampal dentate gyrus and OTC (stage III), and then to temporal (stage IV) and frontal neocortices and basal ganglia (stage V). The staging scheme was validated by significant correlations with clinical and neuroimaging variables and will be important for future clinical, neuroimaging, pathologic and even genetic analyses in AD.
The staging scheme was developed based on the observation of a systematic progressive regional deposition of TDP-43 in AD. All cases in this study had amygdala involvement, with a large proportion having only amygdala involvement suggesting that deposition occurs first in the amygdala and then progresses elsewhere. Using this concept of regional involvement, the entorhinal cortex and subiculum were the next most commonly involved regions. It was difficult, however, to precisely determine whether the entorhinal cortex was affected before the subiculum, or vice versa, given that we had cases with entorhinal involvement without subiculum involvement and cases with subiculum involvement without entorhinal involvement. Although we observed a greater number of cases with involvement of the entorhinal cortex than the subiculum, another study identified more cases with involvement of the subiculum than entorhinal cortex [3]. We observed further progression involving the dentate gyrus of the hippocampus and OTC. These two regions appeared to be simultaneously involved since the great majority of cases showed involvement of both regions. The next region that was apparently involved was the temporal cortex. There were a large number of cases with involvement of the temporal cortex that did not show involvement of the frontal cortex or basal ganglia. Two similar cases have been previously reported [3]. Of cases that spread into the temporal cortices, we observed that in approximately a third there was additional involvement of the frontal cortex and basal ganglia. In fact, in all but two cases, whenever the frontal cortex was involved the basal ganglia were also involved. This observed pattern of progression from the amygdala through the frontal cortex and basal ganglia accounted for almost 100 % of the cases, with only a few outliers that were missing a preceding region, and one case with amygdala and basal ganglia involvement. The parietal lobe has been assessed in two previous studies, although it is difficult to determine whether parietal involvement follows or precedes frontal involvement [3, 15].
Previous studies have suggested that RNA binding proteins, such as TDP-43, have prion-like properties and hence may propagate from cell-to-cell [5, 23]. The fact that TDP-43 has been shown to have filamentous properties with electron microscopic analysis [24] and the fact that TDP-43 does progress in a stereotypic fashion in AD support this hypothesis. However, it is unclear why the regional progression in AD would differ from the regional progression of TDP-43 in ALS [7] and why progression in both do not follow an established anatomic route.
The staging scheme extends findings from previous studies that reported different patterns of regional TDP-43 involvement in AD. In the original study by Amador-Ortiz et al. [1], two patterns were described; limbic and diffuse. The former was defined by involvement of the dentate gyrus of the hippocampus and entorhinal cortex, with scant involvement of the OTC. The latter was defined by involvement of OTC and inferior temporal cortex. Therefore, stage III corresponds most closely to the limbic group, while stages IV and V correspond most closely to the diffuse group. This fits with the fact that the limbic group has been previously reported to be more common than the diffuse group [1] and the most common stage was indeed stage III. Subsequent studies identified cases with involvement of only the amygdala, but these studies were limited by a small number of cases and hence were not able to adequately assess progression [3, 13, 15, 22]. Similarly, only two cases with amygdala and entorhinal cortex involvement have been previously reported [3].
We identified clinical, neuroimaging and pathological differences that helped to validate the TDP-43 in AD staging scheme by demonstrating that there were differences between all five stages. Firstly, there were significant clinical and/or neuroimaging differences between stage I and the other four stages, between stages II and III, between stages III and IV, and between stages IV and V. It is unlikely that these findings were driven by age at onset since stage III cases were in fact the oldest, and age was included as a covariate in our analyses. Similarly, for disease duration, the stage II cases had longer disease duration compared to stage III cases, yet did not have worse clinical scores. Second, there were significant differences in the frequency of HpScl, with low frequencies observed in stages I and II, and higher frequencies observed in stages III, IV and V. In fact, stages IV and V showed significantly higher frequencies than all the other stages, with all but one of the stage V cases having HpScl. Hippocampal sclerosis has been previously shown to be associated with TDP-43 deposition [1, 9, 11, 18, 22, 30, 32, 37, 41], but in this study we further demonstrate that the association is driven by stages III–V. In addition, there was a difference in amygdala TDP-43 burden between stages I and II, with stage I showing scant-sparse inclusions and stage II cases showing moderate-frequent inclusions. This finding further validates the separation of stage I from stage II. We did not observe a difference in the APOE genotype frequencies across stages, suggesting that TDP-43 progression in AD is unrelated to APOE.
In addition to demonstrating differences between all five stages, we also demonstrate differences between all five stages and a large group of AD subjects that were TDP-43 negative. Furthermore, when compared to the AD patients that did not have TDP-43, we identified a graded worsening of cognitive impairment, including memory loss and naming difficulties, as well as volume loss of the hippocampus and entorhinal cortex, across stages. This decline in clinical and neuroimaging variables also correlated with progression from stage I to V.
It was intriguing that the only variable that showed a significant decline in stage I was the BNT; a test of confrontational naming. While the lack of differences in MMSE, CDR-SB and mDRS can be explained by the absence of entorhinal and hippocampal atrophy in the stage I cases, it is unclear why the BNT showed abnormalities. One possibility may be the sensitivity of the BNT to detect subtle changes in language as compared to the ability of the other cognitive tests to detect subtle changes in other cognitive domains. In fact, in one of our previous studies with a much smaller number of subjects, and hence less power, where we assessed the impact of TDP-43 in AD, only the BNT differed across AD cases with and without TDP-43 [18].
Previously, we and others have applied TDP-43 typing to cases of AD [3, 18, 37], with somewhat conflicting results regarding typing. We initially reported in a small sample of 29 cases that the majority of cases were type B [18], while two other studies reported that the most common type was type A [3, 37]. In this current study, of those with hippocampal or neocortical involvement (stages III–V) in which we are able to apply the typing, type A pathology was indeed the most common, with the highest proportion of type A observed in stage IV. Two cases in stage V and one case in stage III had characteristics of FTLD-TDP type C. Interestingly, one type C case in stage V with a clinical diagnosis of AD had prominent aphasia and anteromedial temporal atrophy on neuroimaging (reminiscent of semantic dementia), as well as pathological burden of TDP-43 similar to the amount observed in FTLD (Fig. 3). Therefore, whenever AD pathology is identified in cases with prominent aphasia and anteromedial temporal atrophy, TDP-43 pathology should be assessed. We were unable to apply the typing scheme to the stage I and II cases since the typing scheme is based on hippocampal and neocortical TDP-43 deposition. However, typing may be possible by utilizing information from one study that assessed TDP-43 morphology in subcortical regions, including amygdala, across the TDP-43 types in frontotemporal lobar degeneration cases [19].
Neuroimaging and pathological findings in a case with AD and TDP-43 type C pathology. Top panel shows three coronal T1-weighted MRI slices highlighting left anteromedial temporal lobe atrophy. Bottom panel shows TDP-43 immunoreactive inclusions consistent with FTLD type C, including long thick DNs in frontal (a) and insula (b) cortices, and Pick body-like NCIs in the putamen (c) and the hippocampal dentate gyrus (d). Bar 30 micron
In conclusion, we have identified five distinct stages of TDP-43 immunoreactivity in AD. Based on these findings, we recommend that pathological screening for TDP-43 deposition in AD begin with assessment of the amygdala. If positive, we then recommend further sequential screening based on the regions that are involved across the stages. Further analysis is now needed to determine the association of additional cortical, subcortical and brainstem regions to these five stages and whether there are biochemical differences between the stages.
References
Amador-Ortiz C, Lin WL, Ahmed Z et al (2007) TDP-43 immunoreactivity in hippocampal sclerosis and Alzheimer’s disease. Ann Neurol 61:435–445
Arai T, Hasegawa M, Akiyama H et al (2006) TDP-43 is a component of ubiquitin-positive tau-negative inclusions in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Biochem Biophys Res Commun 351:602–611
Arai T, Mackenzie IR, Hasegawa M et al (2009) Phosphorylated TDP-43 in Alzheimer’s disease and dementia with Lewy bodies. Acta Neuropathol 117:125–136
Bigio EH, Mishra M, Hatanpaa KJ et al (2010) TDP-43 pathology in primary progressive aphasia and frontotemporal dementia with pathologic Alzheimer disease. Acta Neuropathol 120:43–54. doi:10.1007/s00401-010-0681-2
Bigio EH, Wu JY, Deng HX et al (2013) Inclusions in frontotemporal lobar degeneration with TDP-43 proteinopathy (FTLD-TDP) and amyotrophic lateral sclerosis (ALS), but not FTLD with FUS proteinopathy (FTLD-FUS), have properties of amyloid. Acta Neuropathol 125:463–465. doi:10.1007/s00401-013-1089-6
Braak H, Braak E (1991) Neuropathological stageing of Alzheimer-related changes. Acta Neuropathol 82:239–259
Brettschneider J, Del Tredici K, Toledo JB et al (2013) Stages of pTDP-43 pathology in amyotrophic lateral sclerosis. Ann Neurol 74:20–38. doi:10.1002/ana.23937
Crook R, Hardy J, Duff K (1994) Single-day apolipoprotein E genotyping. J Neurosci Methods 53:125–127
Davidson YS, Raby S, Foulds PG et al (2011) TDP-43 pathological changes in early onset familial and sporadic Alzheimer’s disease, late onset Alzheimer’s disease and Down’s syndrome: association with age, hippocampal sclerosis and clinical phenotype. Acta Neuropathol 122:703–713. doi:10.1007/s00401-011-0879-y
Dickson DW, Davies P, Bevona C et al (1994) Hippocampal sclerosis: a common pathological feature of dementia in very old (>or =80 years of age) humans. Acta Neuropathol 88:212–221
Dickson DW, Baker M, Rademakers R (2010) Common variant in GRN is a genetic risk factor for hippocampal sclerosis in the elderly. Neurodegener Dis 7:170–174. doi:10.1159/000289231
Folstein MF, Folstein SE, McHugh PR (1975) “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 12:189–198
Geser F, Robinson JL, Malunda JA et al (2010) Pathological 43-kDa transactivation response DNA-binding protein in older adults with and without severe mental illness. Arch Neurol 67:1238–1250. doi:10.1001/archneurol.2010.254
Higashi S, Iseki E, Yamamoto R et al (2007) Concurrence of TDP-43, tau and alpha-synuclein pathology in brains of Alzheimer’s disease and dementia with Lewy bodies. Brain Res 1184:284–294. doi:10.1016/j.brainres.2007.09.048
Hu WT, Josephs KA, Knopman DS et al (2008) Temporal lobar predominance of TDP-43 neuronal cytoplasmic inclusions in Alzheimer disease. Acta Neuropathol 116:215–220
Jack CR Jr, Lowe VJ, Senjem ML et al (2008) 11C PiB and structural MRI provide complementary information in imaging of Alzheimer’s disease and amnestic mild cognitive impairment. Brain J Neurol 131:665–680. doi:10.1093/brain/awm336
Josephs KA, Tsuboi Y, Cookson N, Watt H, Dickson DW (2004) Apolipoprotein E epsilon 4 is a determinant for Alzheimer-type pathologic features in tauopathies, synucleinopathies, and frontotemporal degeneration. Arch Neurol 61:1579–1584. doi:10.1001/archneur.61.10.1579
Josephs KA, Whitwell JL, Knopman DS et al (2008) Abnormal TDP-43 immunoreactivity in AD modifies clinicopathologic and radiologic phenotype. Neurology 70:1850–1857
Josephs KA, Stroh A, Dugger B, Dickson DW (2009) Evaluation of subcortical pathology and clinical correlations in FTLD-U subtypes. Acta Neuropathol 118:349–358
Kadokura A, Yamazaki T, Lemere CA, Takatama M, Okamoto K (2009) Regional distribution of TDP-43 inclusions in Alzheimer disease (AD) brains: their relation to AD common pathology. Neuropathol Off J Jpn Soc Neuropathol 29:566–573. doi:10.1111/j.1440-1789.2009.01017.x
Kaplan E, Goodglass H, Weintraub S (1978) The Boston Naming Test. Veterans Administration Medical Center, City
King A, Sweeney F, Bodi I, Troakes C, Maekawa S, Al-Sarraj S (2010) Abnormal TDP-43 expression is identified in the neocortex in cases of dementia pugilistica, but is mainly confined to the limbic system when identified in high and moderate stages of Alzheimer’s disease. Neuropathol Off J Jpn Soc Neuropathol 30:408–419. doi:10.1111/j.1440-1789.2009.01085.x
King OD, Gitler AD, Shorter J (2012) The tip of the iceberg: RNA-binding proteins with prion-like domains in neurodegenerative disease. Brain Res 1462:61–80. doi:10.1016/j.brainres.2012.01.016
Lin WL, Dickson DW (2008) Ultrastructural localization of TDP-43 in filamentous neuronal inclusions in various neurodegenerative diseases. Acta Neuropathol 116:205–213. doi:10.1007/s00401-008-0408-9
Mackenzie IR, Baborie A, Pickering-Brown S et al (2006) Heterogeneity of ubiquitin pathology in frontotemporal lobar degeneration: classification and relation to clinical phenotype. Acta Neuropathol 112:539–549. doi:10.1007/s00401-006-0138-9
Mackenzie IR, Neumann M, Baborie A et al (2011) A harmonized classification system for FTLD-TDP pathology. Acta Neuropathol 122:111–113. doi:10.1007/s00401-011-0845-8
Mattis S (1988) Dementia rating scale. Psychological Assessment Resources, City
Mirra SS, Heyman A, McKeel D et al (1991) The consortium to establish a registry for Alzheimer’s Disease (CERAD). Part II. Standardization of the neuropathologic assessment of Alzheimer’s disease. Neurology 41:479–486
Morris JC (1993) The clinical dementia rating (CDR): current version and scoring rules. Neurology 43:2412–2414
Nelson PT, Schmitt FA, Lin Y et al (2011) Hippocampal sclerosis in advanced age: clinical and pathological features. Brain J Neurol 134:1506–1518. doi:10.1093/brain/awr053
Neumann M, Sampathu DM, Kwong LK et al (2006) Ubiquitinated TDP-43 in frontotemporal lobar degeneration and amyotrophic lateral sclerosis. Science 314:130–133
Pao WC, Dickson DW, Crook JE, Finch NA, Rademakers R, Graff-Radford NR (2011) Hippocampal sclerosis in the elderly: genetic and pathologic findings, some mimicking Alzheimer disease clinically. Alzheimer Dis Assoc Disord 25:364–368. doi:10.1097/WAD.0b013e31820f8f50
Robinson JL, Geser F, Corrada MM et al (2011) Neocortical and hippocampal amyloid-beta and tau measures associate with dementia in the oldest-old. Brain J Neurol 134:3708–3715. doi:10.1093/brain/awr308
Sampathu DM, Neumann M, Kwong LK et al (2006) Pathological heterogeneity of frontotemporal lobar degeneration with ubiquitin-positive inclusions delineated by ubiquitin immunohistochemistry and novel monoclonal antibodies. Am J Pathol 169:1343–1352. doi:10.2353/ajpath.2006.060438
Sled JG, Zijdenbos AP, Evans AC (1998) A nonparametric method for automatic correction of intensity nonuniformity in MRI data. IEEE Trans Med Imaging 17:87–97
Tzourio-Mazoyer N, Landeau B, Papathanassiou D et al (2002) Automated anatomical labeling of activations in SPM using a macroscopic anatomical parcellation of the MNI MRI single-subject brain. NeuroImage 15:273–289
Uryu K, Nakashima-Yasuda H, Forman MS et al (2008) Concomitant TAR-DNA-binding protein 43 pathology is present in Alzheimer disease and corticobasal degeneration but not in other tauopathies. J Neuropathol Exp Neurol 67:555–564
Whitwell JL, Jack CR Jr, Przybelski SA et al (2011) Temporoparietal atrophy: a marker of AD pathology independent of clinical diagnosis. Neurobiol Aging 32:1531–1541
Whitwell JL, Dickson DW, Murray ME et al (2012) Neuroimaging correlates of pathologically defined subtypes of Alzheimer’s disease: a case-control study. Lancet Neurol 11:868–877. doi:10.1016/S1474-4422(12)70200-4
Working Group (1997) Consensus recommendation for the postmortem diagnosis of Alzheimer’s disease. The National Institute on Aging, and Reagan Institute Working Group on Diagnostic Criteria for Neuropathologic Assessment of Alzheimer’s Disease. Neurobiol Aging 18(1):1–2
Yokota O, Davidson Y, Bigio EH et al (2010) Phosphorylated TDP-43 pathology and hippocampal sclerosis in progressive supranuclear palsy. Acta Neuropathol 120:55–66. doi:10.1007/s00401-010-0702-1
Zhang YJ, Xu YF, Cook C et al (2009) Aberrant cleavage of TDP-43 enhances aggregation and cellular toxicity. Proc Natl Acad Sci USA 106:7607–7612. doi:10.1073/pnas.09006881060900688106
Acknowledgments
This study was funded by the US National Institute of Aging (NIA) grants R01-AG037491 (to KAJ), R21-AG038736 (to JLW), P01-AG003949 (to DWD) and P50-AG016574 (to RCP). We wish to thank the families of the patients who donated their brains to science allowing completion of this study. We further wish to thank Kris Johnson, Linda Rousseau, Virginia Phillips and Monica Casey-Castanedes for pathological support.
Conflict of interest
The authors declare that they have no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Josephs, K.A., Murray, M.E., Whitwell, J.L. et al. Staging TDP-43 pathology in Alzheimer’s disease. Acta Neuropathol 127, 441–450 (2014). https://doi.org/10.1007/s00401-013-1211-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-013-1211-9