Abstract
Purpose
To study the association between baseline heart rate and outcome in patients with multiple organ dysfunction (MODS) as well as the course of heart rate over the first 4 days during MODS.
Methods
Prospective observational study in 89 patients with MODS, defined as an APACHE-II score ≥20. Baseline heart rate (HR0) was determined over a 60-minute period at the time of MODS diagnosis. 28-day all-cause mortality was the primary endpoint of the study, a fall of the APACHE-II score by 4 points or more from day 0 to day 4 constituted the secondary endpoint. Hazard ratios for heart rate of 90 beats per minute (bpm) or greater relative to less than 90 bpm were calculated using Cox proportional hazards model and adjusted for confounding variables.
Results
Median baseline heart rate was 83 bpm in survivors and 92 bpm in non-survivors (p = 0.048). 28-day mortality was 32 and 61% in patients with HR0 < 90 bpm and HR0 ≥ 90 bpm, respectively. The adjusted hazard ratio for 28-day mortality was 2.30 (95% confidence interval 1.21–4.36, p = 0.001) for HR0 ≥ 90 bpm relative to HR0 < 90 bpm. No correlation was found between baseline heart rate and the secondary endpoint. From day 0 to day 4, heart rate remained elevated in all patients, as well as in survivors and non-survivors.
Conclusions
A heart rate ≥90 bpm at the time of MODS diagnosis is an independent risk factor for increased 28-day mortality. As in patients with cardiovascular conditions such as coronary heart disease or chronic heart failure, heart rate might constitute a target for heart rate-lowering therapy in the narrow initial treatment window of MODS.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Multiple organ dysfunction (MODS) refers to an acute functional impairment of two or more organs such that homeostasis cannot be maintained without intervention [1]. It carries a high mortality, ranging from 22% (2 failing organs) to 95% (4 or more failing organs) [2], entails tremendous health care costs [3], and is the leading cause of death on intensive care units [4]. Evidence-based therapeutic interventions are scarce and innovations to improve morbidity and mortality are urgently needed [5]. Increased resting heart rate is now universally recognized as an independent risk factor both in the general population and in patients with cardiovascular conditions [6]. Patients with MODS typically present with an elevated heart rate that accompanies a highly impaired autonomic dysfunction with depressed parasympathetic control of the heart [7, 8]. Observational clinical data suggest that betablocker medication results in improved heart rate variability and reduced MODS mortality [9]. In murine sepsis models betablockade reduces concentrations of systemic and myocardial pro-inflammatory cytokines, mitigates septic myocardial dysfunction and improves survival [10, 11]. The aim of the present study was therefore (1) to explore the prognostic significance of heart rate at the time of MODS diagnosis, (2) describe the course of the heart rate over the first 5 days of MODS, and (3) explore the correlation between initial heart rate and illness severity.
Subjects and methods
Study population
A prospective observational study was performed on a tertiary 12-bed medical intensive care unit (ICU). Between January and September 2009 all consecutive patients were screened for inclusion.
Protocol
APACHE-II and SOFA scores were calculated at 10 a.m. every day. MODS was defined as an APACHE-II score ≥20 [12–14]. MODS patients older than 18 years were included in the study if they presented with sinus rhythm. Patients with (a) a cardiac pacemaker, (b) palliative treatment goal, or (c) transferred from other high-dependency units with MODS already under treatment for 8 h or longer were excluded.
A one-channel electrocardiogram (ECG) derived from the routine intensive care monitoring (SC 7000, Siemens AG, Erlangen, Germany) was recorded on a separate personal computer. Recording was commenced on admission and maintained for at least the first five ICU days. The recording software (DMS, Stateline, Nevada, USA) calculated hourly heart rates (HHR) from the arithmetic mean of all R–R intervals over 60-minute periods. Prognostic significance of heart rate at the time of MODS diagnosis was evaluated using baseline heart rate (HR0). HR0 was defined as the HHR calculated for the period between 9 a.m. and 10 a.m. on the day when MODS was first diagnosed. The course of the heart rate during the first five days of MODS was evaluated using the median of HHR for 24-hour periods from days 0 to 4.
As for the APACHE-II score, sedated patients were assigned the best Glasgow Coma Scale rating observed on the ICU over the rating period [12]. Treating physicians were blinded to the output of the heart rate recording software. According to local practice, only norepinephrine and dobutamine were used as catecholamines/vasopressors. All cardiac arrest victims were subjected to mild therapeutic hypothermia. 28-day all-cause mortality was the primary endpoint; a fall of the APACHE-II score by 4 points or more from day 0 to day 4 constituted the secondary endpoint of the study. Intention-to-treat analysis was performed and and with regard to dropouts for the secondary endpoint the last observation carried forward method was used [15].
The study was approved by the ethics committee of the Martin Luther University of Halle/Wittenberg and informed consent was obtained either from the patient, a proxy, or next of kin.
Statistical analysis
A p value <0.05 was considered statistically significant. Categorical variables are presented as percentages and compared between groups using Chi-square test or Fisher’s exact test. Continuous parameters are presented as median with interquartile range (IQR) and compared between unrelated samples using Mann–Whitney test and between related samples using Wilcoxon signed-rank test, respectively. Non-parametric correlation analysis was performed using Spearman’s rho. The risk associated with elevated heart rate was tested by comparing survival in patients with HR0 < 90 beats per minute (bpm) versus HR0 ≥ 90 bpm as well as at the HR0 cut-off which yielded the maximum product (sensitivity × specificity) for the prediction of the primary endpoint in a receiver-operating characteristic. The predefined cut-off at 90 bpm was derived from a dataset of a previous MODS study by our group [8]. Kaplan–Meier analysis with logrank test provided a univariate survival model. Cox regression was used to derive a multivariate survival model, with hazard ratios and 95% confidence intervals (CI). Eleven potential confounding variables were included in the multivariate model based on epidemiological, pathophysiological and clinical reasoning: age, gender, acute myocardial infarction, severe sepsis/septic shock, APACHE-II score, mean arterial pressure, central venous pressure, body temperature, analgosedation, dobutamine administration, and norepinephrine administration. The variables were measured at the time of MODS diagnosis. For continuous variables (age in years, body temperature in °C, APACHE-II score), the hazard ratio was indexed to an increment of one unit. For dichotomous variables, the hazard ratio expressed the hazard associated with the presence of the criterion. The following variables were not considered as covariates for multiple regression because of their close correlation with other parameters (in brackets): invasive ventilation (analgosedation), cardiac arrest (myocardial infarction, body temperature), and procalcitonin (severe sepsis/septic shock). Data analysis was performed using SPSS 16.0 (SPSS Inc., Chicago, IL, USA).
Results
Study population
89 consecutive patients (55 males, 34 females, all Caucasian) were included in the study (Table 1). Severe sepsis/septic shock, acute myocardial infarction, cardiac arrest, decompensated heart failure, and decompensated liver cirrhosis contributed to the aetiology of the MODS in 43, 33, 27, 11, and 6%, respectively (multiple triggers conceptually permitted). Other main initial diagnoses included intoxication, acute pancreatitis, hypothermia, ileus, intracranial haemorrhage, anaphylactic shock, withdrawal syndrome, and thrombotic thrombocytopenic purpura, each of which affected less than 5% of the study population. All-cause 28-day mortality was 43%.
Baseline heart rate and primary endpoint
Median HR0 was 85 bpm (IQR 71–97) in all patients included in the study, 83 bpm (IQR 70–90) in survivors to day 28, and 92 bpm (IQR 76–107) in non-survivors. 28-day mortality was 32% for patients with HR0 < 90 bpm and 61% for patients with HR0 ≥ 90 bpm (p = 0.009). MODS aetiology was inequally distributed between the two pre-specified groups. While myocardial infarction and cardiac arrest were more prevalent as the trigger of MODS in patients with HR0 < 90 bpm, sepsis was more frequent in patients with HR0 ≥ 90 bpm. Median baseline heart rate was generally higher in septic patients as compared with non-septic patients (90 vs. 81 bpm, p = 0.011) and lower in patients post cardiac arrest compared with those without cardiac arrest (88 vs. 78 bpm, p = 0.018).
Figure 1 illustrates the univariate survival model for patients with HR0 < 90 bpm compared with patients with HR0 ≥ 90 bpm.
In the initial Cox model, including age, gender, acute myocardial infarction, severe sepsis/septic shock, APACHE-II score, mean arterial pressure, central venous pressure, body temperature, analgosedation, dobutamine administration, norepinephrine administration, HR0 ≥ 90 bpm was assigned a hazard ratio of 3.00 (95% CI 1.41–6.33, p = 0.004). After stepwise backward regression by likelihood ratio, only mean arterial pressure and HR0 ≥ 90 bpm remained in the survival model. The adjusted hazard ratio for high (≥90 bpm) relative to low (<90 bpm) baseline heart rate was 2.30 (95% CI 1.21–4.36, p = 0.001) with regard to 28-day mortality. The HR0 cut-off with the maximum product (sensitivity × specificity) was 93 bpm. 28-day mortality was 30% for patients with HR0 < 93 bpm and 73% for patients with HR0 ≥ 93 bpm (p < 0.001). In the initial Cox model HR0 ≥ 93 bpm was assigned a hazard ratio of 4.95 (95% CI 2.38–10.27, p < 0.001). After stepwise backward regression, age, mean arterial pressure, and HR0 ≥ 93 bpm remained in the model. The adjusted hazard ratio for high (≥93 bpm) relative to low (<93 bpm) baseline heart rate was 4.86 (95% CI 2.50–9.48, p < 0.001) with regard to 28-day mortality.
Baseline heart rate and secondary endpoint
In patients with a decline in APACHE-II score of 4 points or more from day 0 to day 4, HR0 was 83 (IQR 72–90) while in patients in whom APACHE-II score increased, remained constant or decreased by less than 4 points, HR0 was 86 (IQR 70–104). There was no statistically significant difference between these two groups (p = 0.459). The secondary endpoint was reached in 33 patients (59%) with HR0 < 90 bpm and in 15 patients (61%) with HR0 ≥ 90 bpm (p = 0.218).
Heart rate and illness severity
On day 0, median heart rate over 24 h did neither correlate with APACHE-II nor with SOFA score (Spearman’s rho 0.03, p = 0.80, and 0.16, p = 0.14, respectively). The heart rate was, however, significantly correlated to body temperature (Fig. 2).
Course of heart rate over the first five days of MODS
Figure 3 illustrates the heart rate course in all patients as well as survivors and non-survivors during MODS days 0 to 4. Although the heart rate was generally higher in non-survivors compared with survivors, this difference only reached statistical significance on day 0 (Table 2). Heart rate increased from day 0 to day 2 both in the whole population (84–96 bpm, i.e. +14%, p = 0.023) and in survivors (83–92 bpm, i.e. +11%, p = 0.045) while in non-survivors it was elevated from the outset and did not change significantly from day 0 to day 2 (89–96 bpm, i.e. +8%, p = 0.25). From day 0 to day 4, no significant heart rate change could be demonstrated within either group (all patients 84–89 bpm, p = 0.23; survivors 83–85 bpm, p = 0.35; non-survivors 89–94 bpm, p = 0.51), and the change in heart rate between day 0 to day 4 was not different between survivors and non-survivors (p = 0.88).
Median heart rates over 24 h from day 0 to day 4 with comparison of survivors and non-survivors (28-day mortality). Depicted are medians, 25th and 75th percentile. Only on day 0 the heart rate of non-survivors was significantly higher than that of survivors (see also Table 2)
Discussion
Heart rate as a risk factor
A large body of evidence identifies elevated heart rate as an independent risk factor for early death both in the general population and various groups of patients with cardiovascular conditions [6]. As a rule, after correction for relevant confounders the lower the heart rate the longer the survival. This has been thoroughly studied in patients with chronic heart failure (CHF) and those with coronary artery disease (CAD) [16, 17]. Evidence is accumulating that heart rate reduction should be one of the key treatment goals of medical therapy in these chronically ill patients [18, 19]. In acute illness, heart rate is conventionally regarded as a risk marker, reflecting the severity of the underlying illness.
Heart rate in MODS
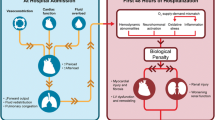
In MODS, heart rate is increased due to multiple factors such as systemic and myocardial inflammation [20], increased sympathetic activity with endogenous catecholamine excess [21, 22], administration of catecholamines, autonomic dysfunction with decreased parasympathetic control of the heart [8, 23], direct effects of toxins such as lipopolysaccharide and cytokines such as thromboxane A2 and prostaglandins on the myocardium [24–26], and a physiologic response to absolute or relative hypovolemia. In healthy subjects with intact cardiac force–frequency relationship (FFR) and frequency-dependent acceleration of relaxation (FDAR) an increase in heart rate results in an increase in cardiac output. It is unclear whether this useful mechanism is actually intact in MODS patients, many of which develop some degree of systolic and diastolic dysfunction [27]. Moreover, severe impairment of FFR and FDAR has been demonstrated at least in a sepsis model [28]. In fact, in severely ill medical ICU patients, correlation between change in heart rate and change in cardiac output is poor [29]. Therefore, to what extent heart rate elevation in MODS is actually capable of contributing to a better cardiac output, and, thus, could be potentially useful to maintain oxygen delivery, is unknown. It can be speculated that some MODS patients exhibit a high heart rate that is elevated beyond physiologically useful compensatory mechanisms thus merely increasing myocardial oxygen demand without any functional benefits, and contributing itself to an unfavourable prognosis [30]. In patients with severe acute heart failure and tachycardia heart rate lowering with ivabradine, a selective sinuatrial node blocking agent has been reported without compromising the systemic perfusion, but resulting in an increase in stroke volume with stable or increasing cardiac output [31–33].
In general higher heart rates aggravate atherosclerosis and endothelial dysfunction, reduce diastolic coronary perfusion time with increased risk of subendocardial ischaemia in patients with compromised coronary flow reserve and lead to a higher incidence of plaque rupture in patients with coronary atherosclerosis [34]. Heart rate reduction improves diastolic perfusion [35], unloads the ventricle [36], and decreases energy expenditure [37]. In patients with coronary artery disease heart rate reduction reduces ischaemia/angina episodes [38, 39] and the incidence of myocardial infarctions [18]. In fact, in critically ill patients with cardiovascular risk factors, too, an elevated heart rate entails a higher rate of major cardiac events [40]. In MODS, sympathoadrenergic overstimulation, endotoxin and pro-inflammatory mediators cause myocardial inflammation, calcium overload, energy depletion, apoptosis and structural changes similar to the pathophysiology of CHF [41]. Thus, the evolving comprehension of increased heart rate as a risk factor rather than a risk marker in CHF could hold true for MODS, too, but has never been investigated prospectively.
Baseline heart rate
In the present study, an elevated heart rate at the time of MODS diagnosis was a strong independent predictor of increased 28-day mortality. After adjusting for potentially confounding parameters, a baseline heart rate of 90 bpm or greater increased the relative risk for all-cause death within 28 days more than twofold. The findings are in accordance with previous studies, showing that a high heart rate in the acutely ill is deleterious. Parker et al. [42] demonstrated that in patients with septic shock admission heart rate >106 bpm as well as a heart rate >95 bpm after 24 h implicate increased mortality. Hjalmarsson et al. [43] found a J-shaped correlation between heart rate on admission and hospital mortality in patients with acute myocardial infarction, with a steep incline of the curve at a heart rate of approximately 90 bpm indicating a doubling of the mortality rate. In large cohorts of patients with acute myocardial infarction admission heart rate >90–100 bpm was associated with about triple the mortality as compared with an admission heart rate <60–70 bpm [44, 45]. The magnitude of excess risk associated with elevated heart rate proposed by this study is in accordance with these previous findings in acutely ill patients, but higher than those reported for chronic cardiovascular conditions. In the BEAUTIFUL trial [46] in patients with CAD and left ventricular ejection fraction of <40%, a heart rate ≥70 bpm had a hazard ratio of 1.34 for cardiovascular death. In the SHIFT trial [47] CHF patients in the highest baseline heart rate group (≥87 bpm) had a 1.86-fold higher risk for all-cause mortality compared with patients with a baseline heart rate of 70 to <72 bpm.
In these patients, sympathoadrenergic activation increases both cardiovascular events and mortality, and blocking sympathoadrenergic effects on heart rate is evolving as a novel treatment goal. Active protection of the heart from catecholamine excess has also been hypothesized to improve survival in the case of septic shock [48].
The independent association of heart rate and mortality in the present study suggests a potential role for heart rate as a therapeutic target also in the initial phase of MODS either at the level of the heart itself or, systemically, by rebalancing the autonomic dysfunction in favour of vagal activity [27, 49]. In normotensive murine sepsis models betablockers attenuate myocardial inflammation, reverse systolic dysfunction, and have shown potential to improve survival [10, 11]. However, betablockers are contraindicated in the majority of MODS patients due to their negative inotropic effect. Ivabradine, a direct sinus node—If channel—blocking agent not impairing inotropy, is currently under investigation in MODS patients in a randomized trial at our institution (“MODI f Y trial”, clinicaltrials.gov identifier NCT01186783) [50]. The results of this study may be of particular interest as endotoxin, an agent not only present in gram-negative sepsis but, due to intestinal bacterial translocation, also in cardiogenic shock, haemorrhagic shock and cardiac arrest, acts directly on the If channel and has been implicated in the pathogenesis of autonomic dysfunction in MODS [25, 27].
In contrast to the striking association between baseline heart rate and 28-day mortality, no relationship could be established between baseline heart rate and development of illness severity over the first four days. A decrease in APACHE-II score of ≥4 points from day 0 to day 4 has recently been suggested as an endpoint for studies into the critically ill as it reflects initial treatment effects more directly than the remote endpoint 28-day mortality [51]. In patients with cardiogenic shock and in patients with severe sepsis or septic shock, such decrease in illness severity score does not only indicate an improvement of the clinical condition but also eventually translates into improved survival [12, 52]. In MODS, however, patients with a low baseline heart rate although having a lower mortality neither show a substantial improvement in illness severity over the first few days nor a lower 7-day mortality (Table 1). Thus, elevated baseline heart rate does not seem to affect the early course of MODS but rather be conceptualized as a general mid- to long-term risk factor.
Correlation between heart rate and other parameters
It has been suggested that in acute illness heart rate may just be a mirror of the severity of the underlying condition [53]. In the current study this hypothesis could not be confirmed. The heart rate on day 0 was not correlated to illness severity expressed as either SOFA or APACHE-II score, although the latter score even contains the heart rate as a component. In critical care heart rate is subject to multiple influences. For example, sicker patients are more likely to be invasively ventilated which may actually reduce heart rate due to analgosedation. In contrast, a positive correlation between heart rate and body temperature was revealed. The temperature is likely to be the main reason for the unequal distribution of MODS aetiologies between the high and the low heart-rate group (Table 1). Maximum body temperature on day 0 was higher in septic patients as compared with non-septic patients (median 37.7 vs. 36.5°C, p = 0.008), and lower in patients post cardiac arrest (who were subjected to mild therapeutic hypothermia) compared with those without cardiac arrest (median 36.0 vs. 37.5°C, p < 0.001). The relationship between temperature and heart rate has been previously accounted for by Leibovici et al. [54] who established the parameter heart rate divided by temperature as “relative tachycardia” in septic patients. In a multivariate analysis in 3,529 patients, a relative tachycardia greater than 2.71 bpm/°C was an independent predictor of 30-day mortality [54].
Course of heart rate
The main findings of the sequential heart rate recording in the present study are that (1) the elevated heart rate which can be demonstrated at the time of MODS diagnosis remains elevated over the first four days, and (2) the course of heart rate between day 0 and day 4 is unable to discriminate between survivors and non-survivors. Persistency of tachycardia over the first few days has already been described in septic shock by Jardin et al. [55]. If elevated heart rate is conceptualized as an expression of autonomic dysfunction with its depressed vagal activity in MODS [27], these findings are in accordance with a report by Flieger [56] who found heart rate variability highly depressed at day 0 in septic MODS with no significant change until day 4.
The reasons for the heart rate increase from day 0 to day 2 in both the whole population and in survivors are not entirely clear. It may be the result of the following factors: (1) The MODS and the underlying pathology, respectively, were still evolving over the first few days and therapeutic measures (e.g. antibiotics) took their time to effect. (2) Clinical improvement was often followed by discontinuation of analgosedation and mechanical ventilation resulting in stress and, hence, an increase in heart rate; this was more often the case in the survivor group.
Limitations
The sample size of the study was small and the study was performed in a single centre only. The findings need confirmation in further trials. In particular, the results might not be transferable to patient populations from surgical or mixed ICUs due to a lower prevalence of patients with pre-existing cardiovascular conditions. Although the authors acknowledge common pathways in the pathophysiology of MODS, it is not assumed that MODS of all aetiologies are uniform. Whether the prognostic relevance of an elevated heart rate applies to MODS of all aetiologies remains to be determined as the present study was not powered to distinguish between causes. It should be noted that patients who died before the first daily APACHE-II score could be calculated were not included in the study. The idea was to identify heart rate as a potential treatment target which is unlikely to apply to such moribund patients.
Conclusions
An elevated heart rate in the early phase of MODS, represented in this study by a heart rate ≥90 bpm at the time of MODS diagnosis, was an independent predictor of increased 28-day mortality. Heart rate might constitute a direct target for therapy in the narrow initial treatment window of MODS.
Abbreviations
- APACHE:
-
Acute physiology and chronic health evaluation
- BEAUTIFUL:
-
Morbidity-mortality evaluation of the If inhibitor ivabradine in patients with coronary disease and left ventricular dysfunction
- bpm:
-
Beats per minute
- CAD:
-
Coronary artery disease
- CHF:
-
Chronic heart failure
- CI:
-
Confidence interval
- ECG:
-
Electrocardiogram
- FDAR:
-
Frequency-dependent acceleration of relaxation
- FFR:
-
Force-frequency relationship
- ICU:
-
Intensive care unit
- IQR:
-
Interquartile range
- HHR:
-
Hourly heart rate
- HR0 :
-
Baseline heart rate
- MODS:
-
Multiple organ dysfunction
- SHIFT:
-
Systolic heart failure treatment with If inhibitor ivabradine trial
- SOFA:
-
Sequential organ failure assessment
References
Bone RC, Balk RA, Cerra FB, Dellinger RP, Fein AM, Knaus WA, Schein RM, Sibbald WJ (1992) Definitions for sepsis and organ failure and guidelines for the use of innovative therapies in sepsis. The ACCP/SCCM Consensus Conference Committee. American College of Chest Physicians/Society of Critical Care Medicine. Chest 101(6):1644–1655
Vincent JL, de Mendonca A, Cantraine F, Moreno R, Takala J, Suter PM, Sprung CL, Colardyn F, Blecher S (1998) Use of the SOFA score to assess the incidence of organ dysfunction/failure in intensive care units: results of a multicenter, prospective study. Working group on “sepsis-related problems” of the European Society of Intensive Care Medicine. Crit Care Med 26(11):1793–1800
Moerer O, Schmid A, Hofmann M, Herklotz A, Reinhart K, Werdan K, Schneider H, Burchardi H (2002) Direct costs of severe sepsis in three German intensive care units based on retrospective electronic patient record analysis of resource use. Intensive Care Med 28(10):1440–1446
Deitch EA (1992) Multiple organ failure. Pathophysiology and potential future therapy. Ann Surg 216(2):117–134
Bone RC (1996) Sir Isaac Newton, sepsis, SIRS, and CARS. Crit Care Med 24(7):1125–1128
Fox K, Borer JS, Camm AJ, Danchin N, Ferrari R, Lopez Sendon JL, Steg PG, Tardif JC, Tavazzi L, Tendera M (2007) Resting heart rate in cardiovascular disease. J Am Coll Cardiol 50(9):823–830
Azimi G, Vincent JL (1986) Ultimate survival from septic shock. Resuscitation 14(4):245–253
Schmidt H, Muller-Werdan U, Hoffmann T, Francis DP, Piepoli MF, Rauchhaus M, Prondzinsky R, Loppnow H, Buerke M, Hoyer D, Werdan K (2005) Autonomic dysfunction predicts mortality in patients with multiple organ dysfunction syndrome of different age groups. Crit Care Med 33(9):1994–2002
Hennen R, Friedrich I, Hoyer D, Nuding S, Rauchhaus M, Schulze M, Schlisske S, Schwesig R, Schlitt A, Buerke M, Muller-Werdan U, Werdan K, Schmidt H (2008) Autonomic dysfunction and beta-adrenergic blockers in multiple organ dysfunction syndrome. Dtsch Med Wochenschr 133(48):2500–2504
Suzuki T, Morisaki H, Serita R, Yamamoto M, Kotake Y, Ishizaka A, Takeda J (2005) Infusion of the beta-adrenergic blocker esmolol attenuates myocardial dysfunction in septic rats. Crit Care Med 33(10):2294–2301
Ackland GL, Yao ST, Rudiger A, Dyson A, Stidwill R, Poputnikov D, Singer M, Gourine AV (2010) Cardioprotection, attenuated systemic inflammation, and survival benefit of beta1-adrenoceptor blockade in severe sepsis in rats. Crit Care Med 38(2):388–394
Werdan K, Pilz G, Bujdoso O, Fraunberger P, Neeser G, Schmieder RE, Viell B, Marget W, Seewald M, Walger P, Stuttmann R, Speichermann N, Peckelsen C, Kurowski V, Osterhues HH, Verner L, Neumann R, Muller-Werdan U (2007) Score-based immunoglobulin G therapy of patients with sepsis: the SBITS study. Crit Care Med 35(12):2693–2701
Schmidt H, Hennen R, Keller A, Russ M, Muller-Werdan U, Werdan K, Buerke M (2006) Association of statin therapy and increased survival in patients with multiple organ dysfunction syndrome. Intensive Care Med 32(8):1248–1251
Schmidt H, Hoyer D, Hennen R, Heinroth K, Rauchhaus M, Prondzinsky R, Hottenrott K, Buerke M, Muller-Werdan U, Werdan K (2008) Autonomic dysfunction predicts both 1- and 2-month mortality in middle-aged patients with multiple organ dysfunction syndrome. Crit Care Med 36(3):967–970
Unnebrink K, Windeler J (2001) Intention-to-treat: methods for dealing with missing values in clinical trials of progressively deteriorating diseases. Stat Med 20(24):3931–3946
McAlister FA, Wiebe N, Ezekowitz JA, Leung AA, Armstrong PW (2009) Meta-analysis: beta-blocker dose, heart rate reduction, and death in patients with heart failure. Ann Intern Med 150(11):784–794
Cucherat M (2007) Quantitative relationship between resting heart rate reduction and magnitude of clinical benefits in post-myocardial infarction: a meta-regression of randomized clinical trials. Eur Heart J 28(24):3012–3019
Fox K, Ford I, Steg PG, Tendera M, Ferrari R (2008) Ivabradine for patients with stable coronary artery disease and left-ventricular systolic dysfunction (BEAUTIFUL): a randomised, double-blind, placebo-controlled trial. Lancet 372(9641):807–816
Swedberg K, Komajda M, Bohm M, Borer JS, Ford I, Dubost-Brama A, Lerebours G, Tavazzi L (2010) Ivabradine and outcomes in chronic heart failure (SHIFT): a randomised placebo-controlled study. Lancet. doi:10.1016/S0140-6736(10)61198-1
Kumar A, Krieger A, Symeoneides S, Parrillo JE (2001) Myocardial dysfunction in septic shock: part II. Role of cytokines and nitric oxide. J Cardiothorac Vasc Anesth 15(4):485–511
Boldt J, Menges T, Kuhn D, Diridis C, Hempelmann G (1995) Alterations in circulating vasoactive substances in the critically ill—a comparison between survivors and non-survivors. Intensive Care Med 21(3):218–225
Benedict CR, Grahame-Smith DG (1978) Plasma noradrenaline and adrenaline concentrations and dopamine-beta-hydroxylase activity in patients with shock due to septicaemia, trauma and haemorrhage. Q J Med 47(185):1–20
Stein PK (2008) Measures of parasympathetic function and risk stratification in critical care. Crit Care Med 36(3):1025–1027
Muller-Werdan U, Schumann H, Loppnow H, Fuchs R, Darmer D, Stadler J, Holtz J, Werdan K (1998) Endotoxin and tumor necrosis factor alpha exert a similar proinflammatory effect in neonatal rat cardiomyocytes, but have different cardiodepressant profiles. J Mol Cell Cardiol 30(5):1027–1036
Zorn-Pauly K, Pelzmann B, Lang P, Machler H, Schmidt H, Ebelt H, Werdan K, Koidl B, Muller-Werdan U (2007) Endotoxin impairs the human pacemaker current If. Shock 28(6):655–661
Takayama K, Yuhki K, Ono K, Fujino T, Hara A, Yamada T, Kuriyama S, Karibe H, Okada Y, Takahata O, Taniguchi T, Iijima T, Iwasaki H, Narumiya S, Ushikubi F (2005) Thromboxane A2 and prostaglandin F2alpha mediate inflammatory tachycardia. Nat Med 11(5):562–566
Werdan K, Schmidt H, Ebelt H, Zorn-Pauly K, Koidl B, Hoke RS, Heinroth K, Muller-Werdan U (2009) Impaired regulation of cardiac function in sepsis, SIRS, and MODS. Can J Physiol Pharmacol 87(4):266–274
Joulin O, Marechaux S, Hassoun S, Montaigne D, Lancel S, Neviere R (2009) Cardiac force-frequency relationship and frequency-dependent acceleration of relaxation are impaired in LPS-treated rats. Crit Care 13(1):R14
Sasse SA, Chen PA, Mahutte CK (1996) Relationship of changes in cardiac output to changes in heart rate in medical ICU patients. Intensive Care Med 22(5):409–414
Muller-Werdan U, Buerke M, Ebelt H, Heinroth KM, Herklotz A, Loppnow H, Russ M, Schlegel F, Schlitt A, Schmidt HB, Soffker G, Werdan K (2006) Septic cardiomyopathy—a not yet discovered cardiomyopathy? Exp Clin Cardiol 11(3):226–236
Link A, Reil JC, Selejan S, Bohm M (2009) Effect of ivabradine in dobutamine induced sinus tachycardia in a case of acute heart failure. Clin Res Cardiol 98(8):513–515
De Ferrari GM, Mazzuero A, Agnesina L, Bertoletti A, Lettino M, Campana C, Schwartz PJ, Tavazzi L (2008) Favourable effects of heart rate reduction with intravenous administration of ivabradine in patients with advanced heart failure. Eur J Heart Fail 10(6):550–555
Vitale D, De Santis V, Guarracino F, Fontana A, Pellegrini F, Tritapepe L (2010) Use of ivabradine in catecholamine-induced tachycardia after high-risk cardiac surgery. Clin Res Cardiol 99(12):853–855
Reil JC, Custodis F, Swedberg K, Komajda M, Borer JS, Ford I, Tavazzi L, Laufs U, Bohm M (2011) Heart rate reduction in cardiovascular disease and therapy. Clin Res Cardiol 100(1):11–19
Colin P, Ghaleh B, Monnet X, Hittinger L, Berdeaux A (2004) Effect of graded heart rate reduction with ivabradine on myocardial oxygen consumption and diastolic time in exercising dogs. J Pharmacol Exp Ther 308(1):236–240
Reil JC, Reil GH, Bohm M (2009) Heart rate reduction by I(f)-channel inhibition and its potential role in heart failure with reduced and preserved ejection fraction. Trends Cardiovasc Med 19(5):152–157
Mulder P, Barbier S, Chagraoui A, Richard V, Henry JP, Lallemand F, Renet S, Lerebours G, Mahlberg-Gaudin F, Thuillez C (2004) Long-term heart rate reduction induced by the selective I(f) current inhibitor ivabradine improves left ventricular function and intrinsic myocardial structure in congestive heart failure. Circulation 109(13):1674–1679
Koester R, Kaehler J, Meinertz T (2011) Ivabradine for the treatment of stable angina pectoris in octogenarians. Clin Res Cardiol 100(2):121–128
Koester R, Kaehler J, Ebelt H, Soeffker G, Werdan K, Meinertz T (2010) Ivabradine in combination with beta-blocker therapy for the treatment of stable angina pectoris in every day clinical practice. Clin Res Cardiol 99(10):665–672
Sander O, Welters ID, Foex P, Sear JW (2005) Impact of prolonged elevated heart rate on incidence of major cardiac events in critically ill patients with a high risk of cardiac complications. Crit Care Med 33(1):81–88 (discussion 241–242)
Dunser MW, Hasibeder WR (2009) Sympathetic overstimulation during critical illness: adverse effects of adrenergic stress. J Intensive Care Med 24(5):293–316
Parker MM, Shelhamer JH, Natanson C, Alling DW, Parrillo JE (1987) Serial cardiovascular variables in survivors and nonsurvivors of human septic shock: heart rate as an early predictor of prognosis. Crit Care Med 15(10):923–929
Hjalmarson A, Gilpin EA, Kjekshus J, Schieman G, Nicod P, Henning H, Ross J Jr (1990) Influence of heart rate on mortality after acute myocardial infarction. Am J Cardiol 65(9):547–553
Disegni E, Goldbourt U, Reicher-Reiss H, Kaplinsky E, Zion M, Boyko V, Behar S (1995) The predictive value of admission heart rate on mortality in patients with acute myocardial infarction. SPRINT Study Group. Secondary Prevention Reinfarction Israeli Nifedipine Trial. J Clin Epidemiol 48(10):1197–1205
Zuanetti G, Mantini L, Hernandez-Bernal F, Barlera S, di Gregorio D, Latini R, Maggioni AP (1998) Relevance of heart rate as a prognostic factor in patients with acute myocardial infarction: insights from the GISSI-2 study. Eur Heart J 19(Suppl F):F19–F26
Fox K, Ford I, Steg PG, Tendera M, Robertson M, Ferrari R (2008) Heart rate as a prognostic risk factor in patients with coronary artery disease and left-ventricular systolic dysfunction (BEAUTIFUL): a subgroup analysis of a randomised controlled trial. Lancet 372(9641):817–821
Bohm M, Swedberg K, Komajda M, Borer JS, Ford I, Dubost-Brama A, Lerebours G, Tavazzi L (2010) Heart rate as a risk factor in chronic heart failure (SHIFT): the association between heart rate and outcomes in a randomised placebo-controlled trial. Lancet 376(9744):886–894
Schmittinger CA, Wurzinger B, Deutinger M, Wohlmuth C, Knotzer H, Torgersen C, Dunser MW, Hasibeder WR (2010) How to protect the heart in septic shock: a hypothesis on the pathophysiology and treatment of septic heart failure. Med Hypotheses 74(3):460–465
Huston JM, Tracey KJ (2011) The pulse of inflammation: heart rate variability, the cholinergic anti-inflammatory pathway and implications for therapy. J Intern Med 269(1):45–53
Nuding S, Ebelt H, Hoke RS, Krummenerl A, Wienke A, Muller-Werdan U, Werdan K (2011) Reducing elevated heart rate in patients with multiple organ dysfunction syndrome by the I (f) (funny channel current) inhibitor ivabradine: MODI (f)Y Trial. Clin Res Cardiol 100(10):915–923
Pilz G, Werdan K (1990) Cardiovascular parameters and scoring systems in the evaluation of response to therapy in sepsis and septic shock. Infection 18(5):253–262
Prondzinsky R, Lemm H, Swyter M, Wegener N, Unverzagt S, Carter JM, Russ M, Schlitt A, Buerke U, Christoph A, Schmidt H, Winkler M, Thiery J, Werdan K, Buerke M (2010) Intra-aortic balloon counterpulsation in patients with acute myocardial infarction complicated by cardiogenic shock: the prospective, randomized IABP SHOCK Trial for attenuation of multiorgan dysfunction syndrome. Crit Care Med 38(1):152–160
Kumar A, Schupp E, Bunnell E, Ali A, Milcarek B, Parrillo JE (2008) Cardiovascular response to dobutamine stress predicts outcome in severe sepsis and septic shock. Crit Care 12(2):R35
Leibovici L, Gafter-Gvili A, Paul M, Almanasreh N, Tacconelli E, Andreassen S, Nielsen AD, Frank U, Cauda R (2007) Relative tachycardia in patients with sepsis: an independent risk factor for mortality. QJM 100(10):629–634
Jardin F, Fourme T, Page B, Loubieres Y, Vieillard-Baron A, Beauchet A, Bourdarias JP (1999) Persistent preload defect in severe sepsis despite fluid loading: a longitudinal echocardiographic study in patients with septic shock. Chest 116(5):1354–1359
Flieger RR (2004) Pathophysiologie-orientiertes, prognose-validiertes und praktikables Monitoring von Patienten mit schwerer Sepsis und septischem Schock. Univ. Diss. Medizinische Fakultät der Martin-Luther-Universität Halle-Wittenberg, Halle/Saale
Acknowledgments
We are indebted to the patients who participated in the study as well as to the staff of our department for the support of our work.
Conflict of interest
K. Werdan is national study coordinator and consultant for Servier, manufacturer of Procoralan® (ivabradine) and has received speaker’s fees, and research grants from Servier. H. Ebelt has received research and travel grants from Servier. R. S. Hoke has received travel grants from Servier.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Hoke, R.S., Müller-Werdan, U., Lautenschläger, C. et al. Heart rate as an independent risk factor in patients with multiple organ dysfunction: a prospective, observational study. Clin Res Cardiol 101, 139–147 (2012). https://doi.org/10.1007/s00392-011-0375-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00392-011-0375-3