Abstract
Purpose
To evaluate the accuracy of integrated positron emission tomography and computed tomography (PET/CT) with iodinated contrast agent and 18F-fluorodeoxyglucose (FDG) in the diagnosis of suspected uterine cancer recurrence and to assess the impact of PET/CT findings on clinical management, compared with PET alone and enhanced CT alone.
Methods
Of 103 women who had undergone treatment for histopathologically proven uterine cervical or endometrial cancer, 90 underwent FDG-PET/contrast-enhanced CT examination for suspected recurrence. PET-alone, CT-alone, and fused PET/CT images were interpreted by two radiologists by consensus for each investigation. Lesion status was determined on the basis of histopathology, radiological imaging and clinical follow-up for longer than 6 months. Differences among the three modalities were tested using the Cochran Q test, followed by multiple comparisons using the McNemar test with Bonferroni adjustment.
Results
Patient-based analysis showed that the sensitivity, specificity, and accuracy of PET alone were 79.5% (35/44), 73.9% (34/46), and 76.7% (69/90), respectively, whereas those of CT alone were 68.2% (30/44), 87.0% (40/46), and 77.8% (70/90), respectively, and those of PET/CT were 90.9% (40/44), 93.5% (43/46), and 92.2% (83/90), respectively. PET/CT findings resulted in a change of management in 38 of the 90 patients (42%) with an additional effect on patient management in 13 patients (14%) diagnosed by CT alone and 14 patients (16%) diagnosed by PET alone.
Conclusion
FDG-PET/contrast-enhanced CT is a more accurate modality for assessing recurrence of uterine cancer, and led to more appropriate subsequent clinical management than that resulting from PET alone or enhanced CT alone.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Despite continuing advances in surgical and nonsurgical therapeutic strategies, cancer recurrence and distant metastasis after initial treatment are often a major problem for women with gynaecological cancer. Early and accurate detection of recurrence in patients with uterine cancer has an important influence on therapy, and selection of appropriate treatment strategies can be expected to have a significant impact on overall survival [1, 2]. Physical examination and measurement of tumour markers have often been used for follow-up. However, benign gynaecological as well as benign and malignant nongynaecological conditions are known to be associated with elevated levels of tumour markers, and furthermore, elevated levels of tumour markers do not provide any information about the location of recurrence [3].
In gynaecological malignancies, conventional morphological imaging modalities, including radiography, computed tomography (CT), and magnetic resonance (MR) imaging, have been widely used for diagnosis of recurrent lesions [4–9]. However, when used alone, these conventional imaging modalities are poor at visualizing small disseminated lesions and lymph node metastases, and for differentiating recurrence from postoperative or postradiation changes [4–8]. Recent advances in CT technology with the availability of multidetector row scanners and multiplanar images offer the potential to improve visualization of small lesions on curved surfaces throughout the whole body [9].
In the late 1990s, positron emission tomography (PET) with 18F-fluorodeoxyglucose (FDG), which exploits the increased utilization of glucose by malignant cells and thereby their high uptake of glucose, has opened a new field in clinical imaging and is widely used for staging, restaging, therapeutic response monitoring, and prognostication in patients with various cancers. PET makes it possible to diagnose cancer recurrence and distant metastasis in the preclinical stage before it becomes evident by conventional imaging modalities. However, PET does not provide anatomical information, and precise localization of any suspicious lesions may be difficult. PET is also impaired by the presence of increased glucose uptake in physiological, nonpathological, and inflammatory states [10, 11]. Recently, an integrated PET/CT system, in which a full-ring detector clinical PET scanner and multidetector row helical CT (MDCT) scanner are combined, has made it possible to acquire both metabolic and anatomical imaging data using a single device in a single diagnostic session, and provides precise anatomical localization of suspicious areas of increased FDG uptake and rules out false-positive PET findings [12, 13].
There have been many reports of PET [14–21] and several reports of PET/CT [22–27] describing their usefulness for the diagnosis of recurrent uterine cancer. Although several authors discussed the diagnostic accuracy of PET/CT [22–27], the quality of the CT component did not fully reach sufficient diagnostic levels in these six studies. No intravenous contrast material was used and the radiation dose was relatively low (40–100 mA) for the CT component in the previous studies. The purpose of the present study was to assess the diagnostic patient- and lesion site-based accuracies of fused images from contrast-enhanced, full-dose CT and PET acquired on a PET/CT scanner and for the follow-up of patients previously treated for uterine cancer, and the impact of the PET/CT findings on patient management, as compared with PET alone and enhanced CT alone.
Materials and methods
Patients
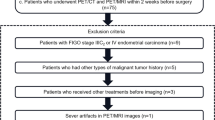
Between July 2006 and October 2007, 103 consecutive patients who had undergone treatment for histopathologically proven uterine cancer underwent PET/CT examinations for suspected recurrence at our institution with the approval of the institutional review board. After exclusion of 13 patients who did not receive intravenous contrast medium due to contraindications such as history of allergic reaction to iodinated contrast media or renal insufficiency, 90 patients comprising 50 patients with cervical cancer and 40 patients with endometrial cancer underwent PET/CT with intravenous contrast medium, and these 90 patients (age range 37–82 years, mean 59 years) comprised the final study population. Informed consent was obtained from each patient after the nature of the procedures had been fully explained. Further details of these patients and their demographic data are presented in Table 1. Recurrence was suspected on the basis of elevated levels of tumour markers (SCC, CEA, CA-125, or CA 19-9; n = 40), physical examination (n = 19), abnormal CT and/or MR imaging findings (n = 15), both elevated tumour marker levels and abnormal CT and/or MR imaging findings (n = 12), and an abnormal Papanicolau (Pap) smear (n = 4).
FDG-PET/CT study
Whole-body imaging was performed using a combined PET/CT scanner (Biograph, Sensation 16 PET/CT system; Siemens, Erlangen, Germany). The CT scan covered a region ranging from the meatus of the ear to the mid-thigh. The technical parameters of the 16-detector row helical CT scanner were a gantry rotation speed of 0.5 s, and a table speed of 24 mm per gantry rotation. The PET component of the combined imaging system had a z-axis of 16.2 cm (per bed position) with an interslice space of 3.75 mm in one bed position, and provided an image from the meatus of the ear to the mid-thigh with six or seven bed positions. The transaxial field of view and pixel size of the PET images reconstructed for fusion were 58.5 cm and 4.57 mm, respectively, with a matrix size of 128×128. To avoid artefacts caused by the urinary tract, patients were asked to drink 1,000 ml of water 1–2 h prior to image acquisition, and to void just before the start of the acquisition. No urinary bladder catheterization was used. After at least 4 h of fasting, patients received an intravenous injection of 4.0 MBq/kg body weight of FDG. The blood glucose levels were checked in all patients before FDG injection and no patients showed a blood glucose level of more than 160 mg/dl.
About 50 min later, an initially unenhanced low-dose CT scan was performed at 140 kV and 40 mA for attenuation correction of the PET image. A whole-body emission PET scan was performed immediately after the low-dose CT scan, with a 3-min acquisition per bed position using a three-dimensional acquisition mode. Attenuation-corrected PET images were reconstructed with an ordered-subset expectation maximization iterative reconstruction algorithm (eight subsets, three iterations). Finally, diagnostic contrast-enhanced full-dose CT was performed for the same axial coverage at 140 kV and 230 mA, with a 2-mm slice thickness. A total volume of 150 ml (maximum) or 2 ml/kg of iodinated contrast material (Iomeprole 300, Eisai, Japan) containing 300 mg of iodine per millilitre was injected intravenously via a power injection at a rate of 2.5 ml/s, and the scan of the neck/thorax, upper/middle abdomen, and lower abdomen/pelvis was started at 45 s, 75 s, and 90 s, respectively, after injection. No oral contrast agent was administered. PET, CT, and fused PET/CT images were generated for review on a computer workstation with a 2-mm slice thickness (AZE Virtual Place version 3.0035).
Image analysis
PET-alone images were retrospectively assessed in consensus by two experienced radiologists (readers A and B with 2 and 9 years of experience in PET, respectively) who had knowledge of neither the other imaging results nor the clinical data. PET images were viewed in coronal, axial, and sagittal sections as is typically performed during clinical interpretation. Focal FDG uptake with an intensity higher than that of surrounding tissues in areas unrelated to physiological or nonpathological processes was defined as recurrence and/or distant metastasis.
Contrast-enhanced full-dose CT-alone images were retrospectively evaluated in consensus by two experienced radiologists (readers C and D with 8 and 20 years of experience in CT, respectively) who had knowledge of neither the other imaging results nor the clinical data. Not only axial CT images were viewed but also coronal and sagittal reconstructions and appropriate windowing was applied. Peritoneal implantation was diagnosed when nodular, plaque-like, or infiltrative soft-tissue lesions with abnormal enhancement were seen in the peritoneal fat or on the peritoneal surface. Lymph nodes (LNs) with a short-axis diameter greater than 1 cm were defined as malignant. Furthermore, the presence of a central unenhancing area suggesting central necrosis was considered a sign of malignancy and the presence of peripheral low attenuation suggesting a fatty hilum within a LN was considered a benign sign, regardless of node size. This method of CT image analysis was based on that used in previous studies [28, 29].
PET/contrast-enhanced CT images were prospectively interpreted in consensus by two experienced radiologists (readers E and F with 3 and 5 years of experience in PET/CT, respectively) who had knowledge of neither the other imaging results nor the clinical data. Attenuation-corrected PET images, contrast-enhanced full-dose CT images and coregistered fused images were displayed together on the monitor. Recurrent or metastatic lesions were diagnosed when abnormal focal FDG uptake observed on the PET images corresponded to an abnormal mass on the CT images. The two readers basically emphasized functional information from PET more than the morphological information from CT in many cases including LN metastasis. However, small pathological lesions such as tiny lung metastases often lack FDG accumulation and tiny lung metastasis was evaluated on the basis of the CT results. When the results of PET and CT were discrepant, two experienced readers carefully determined in consensus which of the two modalities was superior, case by case. LNs with increased glucose uptake were deemed positive for metastatic spread even if their short-axis diameter was less than 1 cm. Conversely, LNs with no detectable tracer uptake were deemed negative for metastatic spread, even if their short-axis diameter was greater than 1 cm. Semiquantitative analysis was not done in this study. This method of PET/CT image analysis was based on that used in previous studies [28–30].
Diagnostic ability was determined on a patient basis and on a ten lesion site basis (retrovesical region, lung, liver, bone, peritoneum, supraclavicular LN, mediastinal and hilar LN, paraaortic LN, pelvic LN, and inguinal LN). The final diagnosis was obtained from the results of histopathological examination after surgery or biopsy (n = 42), or clinical follow-up on the basis of tumour marker levels and contrast-enhanced CT findings (n = 28), and tumour marker levels and PET/contrast-enhanced CT findings (n = 20).
Statistical analysis
We performed patient-based and lesion site-based analyses of the PET/CT results based on the consensus verdict in general, compared with PET alone and CT alone. Sensitivity, specificity and accuracy were calculated using standard statistical formulae, and the 95% confidence interval (95% CI) was determined for each parameter. Differences among the three imaging modalities were tested using the Cochran Q test, followed by multiple comparisons using the McNemar test with Bonferroni adjustment. P values less than 0.05 were considered to indicate statistical significance.
Results
Patient-based analysis
In 44 (48.9%) of the 90 patients, recurrence and/or distant metastasis was confirmed by pathological examination (n = 38) and clinical follow-up study of tumour markers and imaging modality for periods of 2 to 3 months (n = 6). In the other 46 patients (51.1%), no recurrence was confirmed by pathological examination (n = 4) and clinical follow-up for periods of more than 6 months (range 6–20 months, median 14 months; n = 42). PET alone gave a true-positive result in 35 of the 44 patients with recurrence and a true-negative result in 34 of the 46 patients without recurrence. CT alone gave a true-positive result in 30 of the 44 patients with recurrence and a true-negative result in 40 of the 46 patients without recurrence. PET/CT gave a true-positive result in 40 of the 44 patients with recurrence and a true-negative result in 43 of the 46 patients without recurrence (Table 2).
Sensitivity, specificity, and accuracy differed significantly among the three modalities (Cochran Q test: p = 0.0067, p = 0.0009, and p < 0.0001, respectively). Although the difference in sensitivity between CT and PET/CT was significant (McNemar test: p = 0.0078), there were no significant differences in sensitivity between PET and CT (McNemar test: p = 0.33) or between PET and PET/CT (McNemar test: p = 0.05). Although there were significant differences in specificity between PET and PET/CT (McNemar test: p = 0.0054), and between CT and PET/CT (McNemar test: p = 0.029), there was no significant difference in specificity between PET and CT (McNemar test: p = 0.17). Although there were significant differences in accuracy between PET and PET/CT (McNemar test: p = 0.0006) and between CT and PET/CT (McNemar test: p = 0.0009), there was no significant difference in accuracy between PET and CT (McNemar test: p = 0.95). Of 52 patients with elevated levels of tumour markers, the PET/CT findings were positive in 33, and recurrence and/or distant metastasis was confirmed in 31. Of 38 patients without elevated levels of tumour markers, PET/CT findings were positive in 10, and recurrence and/or distant metastasis was confirmed in 9.
Lesion site-based analysis
Ten lesion sites, including the retrovesical region, lung, liver, bone, peritoneum, supraclavicular LN, mediastinal and hilar LN, paraaortic LN, pelvic LN, and inguinal LN, were evaluated in each patient. Therefore, a total of 900 regions of interest were studied in the 90 patients (Table 3). There were 63 sites of lesion recurrence (14 in paraaortic LNs, 10 in the peritoneum, 9 in pelvic LNs, 7 in the lung, 6 in the liver, 5 in the retrovesical regions, 4 in supraclavicular LNs, 4 in mediastinal and hilar LNs, 2 in inguinal LNs, and 2 in bone) and 837 sites of non-recurrent lesions. The lesion site-based sensitivity, specificity, and accuracy of PET alone in terms of overall detection were 71.4% (95% CI 58.3% to 84.5%; 45 of 63 sites), 97.7% (95% CI 96.7% to 98.7%; 818 of 837 sites) and 95.9% (95% CI 94.6% to 97.2%; 863 of 900 sites), respectively. Those of CT alone were 60.3% (95% CI 48.2% to 72.4%; 38 of 63 sites), 99.0% (95% CI 98.4% to 99.7%; 829 of 837 sites), and 96.3% (95% CI 95.1% to 97.6%; 867 of 900 sites), respectively. Finally, those of PET/CT were 90.5% (95% CI 83.3% to 97.7%; 57 of 63 sites), 99.5% (95% CI 99.1% to 100%; 833 of 837 sites) and 98.9% (95% CI 98.2% to 99.6%; 890 of 900 sites), respectively.
Sensitivity, specificity, and accuracy differed significantly among the three modalities (Cochran Q test: p < 0.0001). There were significant differences in sensitivity between PET and CT (McNemar test: p = 0.016), between PET and PET/CT (McNemar test: p = 0.0010), and between CT and PET/CT (McNemar test: p < 0.0002). There were significant differences in specificity between PET and CT (McNemar test: p = 0.032) and between PET and PET/CT (McNemar test: p = 0.0004), but was no significant difference in specificity between CT and PET/CT (McNemar test: p = 0.091). There were significant differences in accuracy between PET and PET/CT (McNemar test: p < 0.0003) and between CT and PET/CT (McNemar test: p < 0.0003), but was no significant difference in accuracy between PET and CT (McNemar test: p = 0.934).
The six lesion sites that were false-negative by PET/CT were two lesions of local recurrence, two lesions of paraaortic LN metastasis measuring 3 mm and 5 mm, one pelvic LN metastasis measuring 4 mm, and one liver metastasis measuring 4 mm. These local recurrences, paraaortic LN metastasis, and pelvic LN metastasis missed by PET/CT increased and were detected on follow-up radiological imaging after 6 months. Liver metastasis missed by PET/CT was detected after 6 months by MRI enhanced with superparamagnetic iron oxide (SPIO). The four lesion sites that were false-positive by PET/CT were two foci of physiological FDG uptake in the intestine that was over-diagnosed as peritoneal dissemination, one degenerative vertebral change that was misinterpreted as bone metastasis, and one case of sarcoidosis that was over-diagnosed as mediastinal and hilar LN metastasis.
The 19 lesion sites that were false-positive by PET alone were three foci of physiological FDG uptake in the intestine that were misinterpreted as peritoneal dissemination, three foci of physiological uptake in the intrapelvic vessels or bowel that were misinterpreted as pelvic LN metastasis, two foci of physiological uptake in the ureter or bowel that were misinterpreted as paraaortic LN metastasis, two foci of nonpathological uptake in the mediastinal and hilar LNs that were misinterpreted as LN metastasis, two degenerative vertebral changes that were misinterpreted as bone metastasis, one vertebral compression fracture that was over-diagnosed as bone metastasis, one case of sarcoidosis that was misinterpreted as mediastinal and hilar LN metastasis, one case of pulmonary tuberculosis that was misinterpreted as lung metastasis, one case of pneumonia that was misinterpreted as lung metastasis, one case of acute cholangitis that was misinterpreted as liver metastasis, one benign thyroid tumour that was misinterpreted as supraclavicular LN metastasis, and one focus of physiological uptake in a neck vessel that was misinterpreted as supraclavicular LN metastasis.
The eight lesion sites that were false-positive by CT alone were two areas of small-bowel thickening due to therapy that were misinterpreted as peritoneal dissemination, one posttherapeutic change that was misinterpreted as local recurrence, one degenerative vertebral change that was misinterpreted as bone metastasis, one liver haemangioma that was misinterpreted as liver metastasis, one parathyroid cyst that was misinterpreted as mediastinal LN metastasis, one case of sarcoidosis that was misinterpreted as mediastinal and hilar LN metastasis, and one reactive inguinal LN swelling that was misinterpreted as LN metastasis.
Effect of PET/CT on patient management
The findings of PET/CT resulted in a change of management in 38 of the 90 patients (42%) which included initiating an unplanned treatment strategy (n = 24), changing the treatment plan (n = 8), and obviating the need for planned treatment (n = 6). Surgery and chemotherapy were undertaken in 17 patients, surgery in 5, and chemoradiotherapy in 2. Chemoradiotherapy was changed to surgery and chemotherapy in four patients, surgery was changed to chemoradiotherapy in three, and surgery was changed to chemotherapy in one. Chemotherapy was cancelled in three patients, surgery was cancelled in two, and radiotherapy was cancelled in one. Improved diagnostic accuracy with PET/CT had an additional effect on patient management in 13 patients (14%) diagnosed by enhanced CT alone and 14 patients (16%) diagnosed by PET alone. Three patients with false-negative PET/CT findings of local recurrence, paraaortic LN metastasis, and pelvic LN metastasis lost proper treatment timing. One patient with a false-negative PET/CT finding of liver metastasis received chemotherapy on the basis of SPIO-enhanced MRI.
Discussion
To our knowledge, this is the first study to have investigated the additional diagnostic value of integrated FDG-PET/contrast-enhanced CT over PET alone and enhanced CT alone for the diagnosis of uterine cancer recurrence. The patient-based sensitivity, specificity, and accuracy of PET were 79.5%, 73.9%, and 76.7%, respectively, those of CT were 68.2%, 87.0%, and 77.8%, respectively, and those of PET/CT were 90.9%, 93.5%, and 92.2%, respectively. Improved diagnostic accuracy with PET/CT had an additional effect on management in 13 patients (14%) diagnosed by CT alone and 14 patients (16%) diagnosed by PET alone. Integrated PET/contrast-enhanced CT is a more accurate modality for assessing uterine cancer recurrence and led to more appropriate therapy than that resulting from enhanced CT alone or PET alone.
Many authors have investigated the usefulness of PET for postoperative or posttherapy surveillance of patients with uterine cervical cancer [14–18] and endometrial cancer [19–21]. They have reported that the sensitivity, specificity, and accuracy of PET for detection of recurrence are 86–94%, 76–99%, and 74–97%, respectively, for cervical cancer and 96–100%, 78–88%, and 90–93%, respectively, for endometrial cancer. Several authors have reported the clinical diagnostic accuracy of integrated PET/CT for posttherapy surveillance of patients with uterine cervical cancer [22, 23, 27] and endometrial cancer [23–26], reporting a sensitivity of 90–93%, a specificity of 81–100% and an accuracy of 87–96%. False-negative cases included local recurrence and paraaortic LN metastasis, and false-positive cases included local recurrence, lung metastasis, bone metastasis, peritoneal dissemination, mediastinal and hilar LN metastasis, axillary LN metastasis, pelvic LN metastasis, and paraaortic LN metastasis. Because these three groups did not evaluate interpretation with PET alone or CT alone, the true diagnostic potential and degree of superiority of inline PET/CT compared with PET alone or CT alone was not clarified. Moreover, no intravenous contrast material was used and the radiation dose was insufficient for the CT component of PET/CT in these six series. Loft et al. [31] evaluated the usefulness of FDG-PET/contrast-enhanced CT in the pretreatment staging of 120 patients with cervical cancer stage IB or more.
In our series, CT alone yielded more false-negative findings than did PET alone (Fig. 1), although the slice thickness of CT was only 2 mm and CT images were evaluated on multiplanar sections, not just axial sections. PET alone yielded more false-positive findings than did CT alone. PET alone was superior for detecting peritoneal dissemination, bone metastasis, and all LN metastases, but not for detecting lung metastasis (Fig. 2) or local recurrence, in comparison with CT alone. PET alone and CT alone showed equal sensitivity in the detection of liver metastasis.
A 56-year-old woman with peritoneal dissemination (true-positive by PET and PET/CT, false-negative by CT). a The PET image shows an area of intense FDG uptake in the right lower abdomen (arrow), suggestive of peritoneal dissemination. b The enhanced CT image shows no abnormal findings. c The PET/contrast-enhanced CT image shows abnormal FDG uptake corresponding to a soft-tissue density mass in the mesentery (arrow), suggesting peritoneal dissemination. Histopathological examination of the surgical specimen revealed peritoneal dissemination
A 67-year-old woman with tiny lung metastases (false-negative by PET and true-positive by CT and PET/CT). a The PET image shows no abnormal FDG uptake in the lung. b The enhanced CT image shows two tiny nodules in the right upper lung (arrows), suggestive of lung metastasis. c The PET/contrast-enhanced CT image does not show abnormal FDG uptake corresponding to the two tiny pulmonary nodules seen in b (arrows), probably due to their small size. A follow-up chest CT scan revealed growth of these lung nodules, and biopsy revealed that they were lung metastases
Although posttherapeutic changes on CT-alone images were misinterpreted as local recurrence and peritoneal dissemination in three cases, these false-positive CT results were ruled out by PET alone and PET/CT as no tracer accumulated in the affected area. Viable tumour tissue can be differentiated from posttherapeutic change on PET and PET/CT images, which allow evaluation of tumour metabolism.
In our series, the performance of PET alone was impaired by the presence of increased uptake due to physiological variation (in the bowel, vessels, and ureter), nonpathological lesions (benign thyroid tumour), or inflammatory states (pulmonary tuberculosis, pneumonia, acute cholangitis). These false-positive PET findings were ruled out by the CT component of PET/CT.
PET/CT detected more malignant lesions than CT alone or PET alone in our series (Fig. 3). The minimum size of lesions detected by PET/CT was 5 mm, and the maximum size of lesions undetected by PET/CT was 5 mm. However, even PET/CT was unable to detect tiny lesions. PET or PET/CT can only detect lesions with a certain volume of malignant cells that is sufficient to produce a change in the observed glucose metabolism, and neither of these modalities can detect micrometastasis [23, 30, 32]. Kitajima et al. [30] demonstrated that the sensitivity for detecting pelvic and paraaortic LN metastatic lesions 4 mm or less by FDG-PET/CT was 17% (4/24), for lesions between 5 and 9 mm was 67% (14/21), and for lesions 10 mm or larger was 93% (14/15). Pannu et al. [32] demonstrated that 50% of peritoneal lesions larger than 1 cm (n = 8) were detectable by PET/CT, and that only 13% of peritoneal lesions no larger than 1 cm (n = 23) were detectable by PET/CT in patients with ovarian cancer recurrence. The spatial resolution of PET scans is insufficient for detection of microscopic lesions. With a spatial resolution of 4–6 mm for currently available PET and PET/CT systems, the detection of microscopic lesions remains challenging. Improving the spatial resolution and sensitivity of PET and PET/CT scanners and developing new, more specific radioactive tracers may help to overcome this limitation in the future.
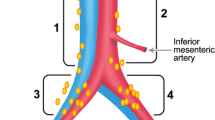
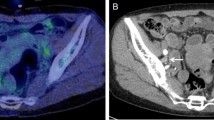
A 50-year-old woman with paraaortic LN metastasis (true-positive by PET/CT, and false-negative by PET and CT). a The PET image shows no abnormal FDG uptake. b The enhanced CT image shows a paraaortic LN measuring 7×7 mm (arrow), which does not rule out LN metastasis on the basis of the size criterion for CT. c The PET/contrast-enhanced CT image shows mild FDG uptake corresponding to a small paraaortic LN (arrow), suggesting the presence of nodal cancer spread. Histopathological examination of the surgical specimen confirmed extensive LN cancer involvement
In our series, the overall node-based sensitivity, specificity, and accuracy of CT for detection of metastasis at all LN sites (inguinal LNs, pelvic LNs, paraaortic LNs, mediastinal and hilar LNs, and supraclavicular LNs) were 57.6% (19 of 33 sites), 99.3% (414 of 417 sites), and 96.2% (433 of 450 sites), respectively, whereas those of PET/CT were 90.9% (30 of 33 sites), 99.8% (416 of 417 sites), and 99.1% (446 of 450 sites), respectively. Because the identification of metastatic LNs by morphological imaging modalities such as CT and MRI is based on measurement of node size, a short-axis diameter exceeding 10 mm or 8 mm being the most accepted criterion for diagnosis of nodal involvement, the sensitivity of CT and MR imaging for diagnosis of metastatic LN is relatively low: the sensitivity rate has been reported to be 27–50% [33, 34]. However, PET is a functional method based on the increased glucose metabolism of cancer cells, regardless of node size, and it seems that PET and PET/CT enable the detection and localization of metastatic LNs that are not enlarged (i.e. smaller than 1 cm). Although PET and PET/CT can sometimes detect metastatic LNs smaller than 1 cm, their sensitivity is insufficient because of their low spatial resolution [30].
The added value of PET/CT in terms of patient clinical management and selection of appropriate treatment strategies relies mainly on its ability to accurately localize sites of recurrent disease anywhere in the body in a single noninvasive procedure. This allows distinction between a local and a disseminated recurrence pattern, thus assisting selection of the optimal therapy: surgical resection with or without radiation versus systemic chemotherapy with or without radiation. Moreover, PET/CT also makes it possible to avoid unnecessary therapy. Our series demonstrated that the findings of PET/CT resulted in a change of management in 38 of our 90 patients (42%). Chung et al. [22] reported a comparative figure of 12 of 52 patients (23%), Park et al. [25] reported a change of management in 14 of 88 patients (22%), and Chung et al. [26] reported a change of management in 7 of 31 patients (23%).
According to the literature reports, the use of CT contrast agents in PET/CT is still controversial [35]. Some argue that CT image data should be used only for attenuation correction of PET, reduction of acquisition time, and localization of hypermetabolic lesions with a low radiation dose (“low-dose CT”) [36], whereas others advocate contrast-enhanced, full-dose, high-resolution CT (“diagnostic CT”) [37–40]. A recent study has demonstrated that there is an increase in standardized uptake value in normal and pathological regions of high concentration when intravenous contrast-enhanced CT is used for attenuation, but this increase is clinically insignificant in the evaluation of patients with cancer, and contrast-enhanced CT could be used for attenuation correction [37]. Because we used unenhanced low-dose CT for attenuation correction in our series to avoid overestimation of PET attenuation factors by contrast medium when contrast-enhanced CT is used for attenuation, the problem of high radiation exposure occurred. Further study in a larger patient population is needed to elucidate the efficacy, radiation exposure, and cost-effectiveness of PET/contrast-enhanced CT.
This study had certain limitations. First, the ideal gold standard for any analysis is histological confirmation of the findings. However, clinical follow-up is a valid way to evaluate diagnostic accuracy and response to therapy, and it would have been unethical to investigate all PET/CT-detected lesions using invasive procedures. Positive findings are easy to confirm, but negative findings only mean that it is not possible to acquire positive findings during the follow-up period, making it uncertain whether the findings are truly negative. Second, no oral contrast materials were used in this series. Adding an oral contrast agent could have helped delineate normal bowel activity better and demonstrate pathological intraabdominal activity (peritoneal implantation). Third, the PET and CT images in our series were acquired as part of a PET/CT study, and so we did not directly compare the diagnostic performance of PET/CT with that of separate CT alone and PET alone.
In conclusion, integrated FDG-PET/contrast-enhanced CT is a more accurate imaging modality than PET alone and enhanced CT alone for assessing recurrence of uterine cancer, and led to changes in the subsequent clinical management in 42% of 90 patients with an additional effect on patient management in 13 patients (14%) diagnosed by CT alone and 14 patients (16%) diagnosed by PET alone.
References
Larson DM, Copeland LJ, Stringer CA, Gershenson DM, Malone Jr JM, Edwards CL. Recurrent cervical carcinoma after radical hysterectomy. Gynecol Oncol 1988;30:381–7.
Irvin WP, Rice LW, Berkowitz RS. Advances in the management of endometrial adenocarcinoma. A review. J Reprod Med 2002;47:173–90.
Lo SS, Khoo US, Cheng DK, Ng TY, Wong LC, Ngan HY. Role of serial markers in the surveillance for recurrence in endometrial cancer. Cancer Detect Prev 1999;23:397–400.
Low RN, Sigeti JS. MR imaging of peritoneal disease: comparison of contrast-enhanced fast multiplanar spoiled gradient-recalled and spin-echo imaging. AJR Am J Roentgenol 1994;163:1131–40.
Sugiyama T, Nishida T, Ushijima K, Sato N, Kataoka A, Imaishi K, et al. Detection of lymph node metastasis in ovarian carcinoma and uterine corpus carcinoma by preoperative computerized tomography or magnetic resonance imaging. J Obstet Gynaecol 1995;21:551–6.
Connor JP, Andrews JI, Anderson B, Buller RE. Computed tomography in endometrial carcinoma. Obstet Gynecol 2000;95:692–6.
Pannu HK, Fishmann EK. Evaluation of cervical cancer by computed tomography: current status. Cancer 2003;98:2039–43.
Jeong YY, Kong HK, Chung TW, Seo JJ, Park JG. Uterine cervical carcinoma after therapy: CT and MR imaging findings. Radiographics 2003;23:968–81.
Pannu HK, Bristow RE, Montz FJ, Fishman EK. Multidetector CT of peritoneal carcinomatosis from ovarian cancer. Radiographics 2003;23:687–701.
Cook GJ, Maisey MN, Fogelman I. Normal variants, artifacts and interpretative pitfalls in PET imaging with 18-fluoro-2-deoxyglucose and carbon-11 methionine. Eur J Nucl Med 1999;26:1363–78.
Kostakoglu L, Agress H Jr, Goldsmith SJ. Clinical role of FDG PET in evaluation of cancer patients. Radiographics 2003;23:315–40.
Beyer T, Townsend DW, Brun T, Kinahan PE, Charron M, Roddy R, et al. A combined PET/CT scanner for clinical oncology. J Nucl Med 2000;41:1369–79.
Bar-Shalom R, Yefremov N, Guralnik L, Gaitini D, Frenkel A, Kuten A, et al. Clinical performance of PET/CT in evaluation of cancer: additional value for diagnostic imaging and patient management. J Nucl Med 2003;44:1200–9.
Ryu SY, Kim MH, Choi SC, Choi CW, Lee KH. Detection of early recurrence with 18F-FDG PET in patients with cervical cancer. J Nucl Med 2003;44:347–52.
Havrilesky LJ, Wong TZ, Secord AA, Berchuck A, Clarke-Pearson DL, Jones EL. The role of PET scanning in the detection of recurrent cervical cancer. Gynecol Oncol 2003;90:186–90.
Lai CH, Huang KG, See LC, Yen TC, Tsai CS, Chang TC, et al. Restaging of recurrent cervical carcinoma with dual-phase [18F]fluoro-2-deoxy-D-glucose positron emission tomography. Cancer 2004;100:544–52.
Chang TC, Law KS, Hong JH, Lai CH, Ng KK, Hsueh S, et al. Positron emission tomography for unexplained elevation of serum squamous cell carcinoma antigen levels during follow-up for patients with cervical malignancies: a phase II study. Cancer 2004;101:164–71.
Yen TC, See LC, Chang TC, Huang KG, Ng KK, Tang SG, et al. Defining the priority of using 18F-FDG PET for recurrent cervical cancer. J Nucl Med 2004;45:1632–9.
Belhocine T, Debarsy C, Hustinx R, Willems-Foidart J. Usefulness of 18F-FDG PET in the post-therapy surveillance of endometrial carcinoma. Eur J Nucl Med Mol Imaging 2002;9:1132–9.
Saga T, Higashi T, Ishimori T, Mamede M, Nakamoto Y, Mukai T, et al. Clinical value of FDG-PET in the follow up of post-operative patients with endometrial cancer. Ann Nucl Med 2003;17:197–203.
Chao A, Chang TC, Ng KK, Hsueh S, Huang HJ, Chou HH, et al. 18F-FDG PET in the management of endometrial cancer. Eur J Nucl Med Mol Imaging 2006;33:36–44.
Chung HH, Jo H, Kang WJ, Kim JW, Park NH, Song YS, et al. Clinical impact of integrated PET/CT on the management of suspected cervical cancer recurrence. Gynecol Oncol 2007;104:529–34.
Sironi S, Picchio M, Landoni C, Galimberti S, Signorelli M, Bettinardi V, et al. Post-therapy surveillance of patients with uterine cancers: value of integrated FDG PET/CT in the detection of recurrence. Eur J Nucl Med Mol Imaging 2007;34:472–9.
Kitajima K, Murakami K, Yamasaki E, Hagiwara S, Fukasawa I, Inaba N, et al. Performance of FDG-PET/CT in the diagnosis of recurrent endometrial cancer. Ann Nucl Med 2008;22:103–9.
Park JY, Kim EN, Kim DY, Suh DS, Kim JH, Kim YM, et al. Clinical impact of positron emission tomography or positron emission tomography/computed tomography in the posttherapy surveillance of endometrial carcinoma: evaluation of 88 patients. Int J Gynecol Cancer 2008; [Epub ahead of print]. doi:10.1111/j.1525-1438.2008.01197.x
Chung HH, Kang WJ, Kim JW, Park NH, Song YS, Chung JK, et al. The clinical impact of [18F]FDG PET/CT for the management of recurrent endometrial cancer: correlation with clinical and histological findings. Eur J Nucl Mol Imaging 2008;35:1081–8.
Kitajima K, Murakami K, Yamasaki E, Domeki Y, Kaji Y, Sugimura K. Performance of FDG-PET/CT for diagnosis of recurrent uterine cervical cancer. Eur Radiol 2008;18:2040–7.
Antoch G, Stattaus J, Nemat AT, Marnitz S, Beyer T, Keuhl H, et al. Non-small cell lung cancer: dual-modality PET/CT in preoperative staging. Radiology 2003;229:526–33.
Antoch G, Saoudi N, Kuehl H, Dahmen G, Mueller SP, Beyer T, et al. Accuracy of whole-body dual-modality fluorine-18-2-fluoro-2-deoxy-D-glucose positron emission tomography and computed tomography (FDG-PET/CT) for tumor staging in solid tumors: comparison with CT and PET. J Clin Oncol 2004;22:4357–68.
Kitajima K, Murakami K, Yamasaki E, Fukasawa I, Inaba N, Kaji Y, et al. Accuracy of FDG PET/CT in detecting pelvic and paraaortic lymph node metastasis in patients with endometrial cancer. AJR Am J Roentgenol 2008;190:1652–8.
Loft A, Berthelsen AK, Roed H, Ottosen C, Lundvall L, Knudsen J, et al. The diagnostic value of PET/CT scanning in patients with cervical cancer: a prospective study. Gynecol Oncol 2007;106:29–34.
Pannu HK, Cohade C, Bristow RE, Fishman EK, Wahl RL. PET-CT detection of abdominal recurrence of ovarian cancer: radiologic-surgical correlation. Abdom Imaging 2004;29:398–403.
Manfredi R, Mirk P, Maresca G, Margariti PA, Testa A, Zannoni GF, et al. Local-regional staging of endometrial carcinoma: role of MR imaging in surgical planning. Radiology 2004;231:372–8.
Rockall AG, Sohaib SA, Haristinghani MG, Babar SA, Singh N, Jeyarajah AR, et al. Diagnostic performance of nanoparticle-enhanced magnetic resonance imaging in the diagnosis of lymph node metastases in patients with endometrial and cervical cancer. J Clin Oncol 2005;23:2813–21.
Coleman ER, Delbeke D, Guiberteau MJ, Conti PS, Royal HD, Weinre JC, et al. Concurrent PET/CT with an integrated imaging system: intersociety dialogue from the joint working group of the American College of Radiology, the Society of Nuclear Medicine, and the Society of Computed Body Tomography and Magnetic Resonance. J Nucl Med 2005;46:1225–39.
Rodriguez-Vigil B, Gomez-Leon N, Pinilla I, Hernandez-Maraver D, Coya J, Martin-Curto L, et al. PET/CT in lymphoma: prospective study of enhanced full-dose PET/CT versus unenhanced low-dose PET/CT. J Nucl Med 2006;7:1643–8.
Mawlawi O, Erasmus JJ, Munden RF, Pan T, Knight A, Macapinlac HA, et al. Quantifying the effect of IV contrast media on integrated PET/CT: clinical evaluation. AJR Am J Roentgenol 2006;186:308–19.
Antoch G, Freudenberg LS, Beyer T, Bockisch A, Debatin JF. To enhance or not to enhance? 18F-FDG and CT contrast agents in dual-modality 18F-FDG PET/CT. J Nucl Med 2004;45:56–65.
Pfannenberg AC, Aschoff P, Brechtel K, Muller M, Bares R, Paulsen F, et al. Low dose non-enhanced CT versus standard dose contrast-enhanced CT in combined PET/CT protocols for staging and therapy planning in non-small cell lung cancer. Eur J Nucl Med Mol Imaging 2007;34:36–44.
Kitajima K, Murakami K, Yamasaki E, Domeki Y, Kaji Y, Fukasawa I, et al. Performance of integrated FDG-PET/contrast-enhanced CT in the diagnosis of recurrent ovarian cancer: comparison with integrated FDG-PET/non-contrast-enhanced CT and enhanced CT. Eur J Nucl Med Mol Imaging 2008;35:1439–48.
Acknowledgments
We thank the gynaecologists, especially Ichio Fukasawa, Noriyuki Inaba for recruiting patients to undergo PET/CT. We also thank Kennichi Kobayashi, Kouichi Asano, Kazufumi Suzuki, and Kaoru Ishida for their excellent technical assistance and generous support.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kitajima, K., Murakami, K., Yamasaki, E. et al. Performance of integrated FDG-PET/contrast-enhanced CT in the diagnosis of recurrent uterine cancer: comparison with PET and enhanced CT. Eur J Nucl Med Mol Imaging 36, 362–372 (2009). https://doi.org/10.1007/s00259-008-0956-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00259-008-0956-1