Abstract
Taxanes including paclitaxel and docetaxel are highly active against many types of cancers. The main obstacle with developing delivery systems of taxanes is their poor water solubility. In this chapter, taxanes were reviewed in terms of their pharmacology, solubility and stability using traditional formulations such as those based on using Cremophor EL and novel nanocarrier-based formulations including liposome, nanoparticle and polymeric micelle delivery systems. Commercially available formulations of paclitaxel such as Taxol, Abraxane and Genexol-PM were highlighted.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
2.1 Plant Origin and Pharmacology of Taxanes
Taxane compounds are anticancer agents derived from a plant source and include paclitaxel and docetaxel (Fig. 2.1). Paclitaxel is isolated from the Pacific yew tree (Taxus brevifolia) [1], whilst the semisynthetic taxane docetaxel is derived from the needles of the European yew (Taxus baccata) [2, 3]. Taxane formulations can treat various types of cancer including ovarian, breast and bladder carcinomas [4] as well as lung cancer and acute leukaemia [2].
Taxanes are classified as anti-microtubule chemotherapeutic compounds that work by interrupting the microtubule function which is important in cell division. They do so by inhibiting mitosis, causing an incomplete formation of the metaphase plate of chromosomes and hence altering the arrangement of the spindle microtubules [5, 6]. Both paclitaxel and docetaxel bind to ß subunit of tubulin (a protein found in microtubules) [7, 8], producing highly stable dysfunctional microtubules [9]. Microtubules are central to cell division forming spindle fibres permitting separation and alignment of chromosomes during mitosis [10]. Paclitaxel inhibits mitosis in the G-phase of the mitotic cycle, whilst docetaxel causes arrest at the S-phase to prevent cell division and produce apoptosis [11]. Docetaxel has been reported to be twice as potent as paclitaxel at inhibiting microtubules [12].
2.2 Conventional Taxane Formulations in Clinical Use
Paclitaxel and docetaxel are highly lipophilic; hence, they are both regarded to be water-insoluble compounds (Table 2.1), making formulation and administration considerably challenging. Paclitaxel is solubilised using a mixture of Cremophor EL (polyethoxylated castor oil) and dehydrated ethanol (50:50 v/v) to provide a drug concentration of 6 mg/mL [13, 14]. Cremophor EL is a non-ionic surfactant that has the ability to form micelles in biological fluids (e.g. plasma) and increase the solubility of paclitaxel. By contrast, docetaxel is slightly more soluble than paclitaxel; therefore polysorbate 80 (Tween 80) and ethanol are used to solubilise it [15, 16]. These paclitaxel and docetaxel formulations are available for clinical use as Taxol® and Taxotere®, respectively, and are administered by intravenous infusion. Before administration of Taxol®, the formulation is diluted with 5–20-fold using NaCl (0.9%) or dextrose (5%) solutions [9].
2.3 Stability of Taxane Formulations
Stability of taxane is extremely important particularly in situations where chemotherapy is prepared for later administration [17]. In these cases, storage conditions may affect the drug dose received. Docetaxel stability can be influenced by the degree of agitation during preparation and by slight temperature fluctuations during storage [18]. By contrast, for paclitaxel, the optimum storage temperature was found to be 2–8 °C [19], suggesting paclitaxel is less affected by changes in storage temperature compared to docetaxel.
The type of vehicle used and the inclusion of other chemotherapeutic drugs may affect the stability of taxanes on storage. Studies have found that when paclitaxel was diluted to 0.3 or 1.2 mg/mL using 5% dextrose or 0.9% NaCl, the drug remained chemically stable for 72 h under conditions of clinical use [20]. However, when doxorubicin 0.2 mg/mL was added to the formulation, samples were stable for only 24 h, whilst by 72 h some samples showed signs of paclitaxel precipitation. However, by day 5, all samples showed precipitation of the drug; this was independent of storage temperature [21]. This might be attributed to the incorporation of doxorubicin which was relatively easier to solubilise, resulting in salting out of paclitaxel. It has also been found that paclitaxel has an optimum stability when the vehicle had a pH range of 3–5 [22]. Drug concentration may also affect storage stability, with higher drug concentrations producing formulations with longer stability [17].
Administration of taxanes via the intravenous route poses many problems in terms of physical stability of the drug. Waugh et al. (1991) studied the stability of various concentrations of paclitaxel using 5% dextrose or 0.9% NaCl as diluent solutions [23]. The solutions were contained within glass bottles, polyolefin containers or PVC infusion bags and stored for 12–24 h. The chemical stability of the drug was unaffected in all cases; however, the solutions in the polyvinyl chloride (PVC) bags showed signs of leaching of the plasticiser di(2-ethylhexyl) phthalate (DEHP) into the formulation. DEHP is a polymer used in PVC to make it more flexible, since without this constituent, PVC would be very brittle at room temperature [24]. Leaching has also occurred during infusion using PVC administration sets. When a similar study was conducted on docetaxel, DEHP also leached during storage in PVC bags. Moreover, after 5 days the drug began to precipitate in the PVC infusion bags, whereas the solution contained within the polyolefin container was physically and chemically stable for 4 weeks [3]. It is worth to note that DEHP has been reported to be carcinogenic and teratogenic. This indicates that using polyethylene-lined infusion bags and administration kits is more appropriate in terms of safety for the patient when administering taxanes.
2.4 Undesirable Toxicities of Taxane Formulations
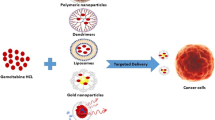
Taxane anticancer compounds may produce adverse effects such as myelosuppression, neuropathy, fatigue, alopecia, nausea and vomiting, with docetaxel also causing nail damage [6]. Moreover, an important limitation of taxane formulations is the toxicity of the excipients used to solubilise the drugs, particularly Cremophor EL and polysorbate 80 [25]. An initial fatal hypersensitivity reactions, nephrotoxicity and hypotension may happen because of using these excipients [16, 26]. Cremophor EL commonly causes serious adverse effects such as severe anaphylactoid hypersensitivity reactions, hyperlipidaemia, abnormal lipoprotein patterns, aggregation of erythrocytes and peripheral neuropathy [27]. Patients are premedicated with corticosteroids and histamine antagonists to reduce the incidence and severity of these hypersensitivity reactions [28]. However, even after premedication, 5–30% of the relevant patients are still affected by mild hypersensitivity reactions [29]. Thus, research has been conducted to provide alternative formulations that may enhance taxane solubility and reduce formulation instability and toxicity. Approaches that have been investigated included the use of nanotechnology, i.e. by involving nanocarrier-based formulations such as liposomes, polymeric micelles, nanoparticles, dendrimers, microemulsions (also called nanoemulsions) and cyclodextrins.
2.5 Formulations Developed to Reduce Instability
A number of strategies have been used to develop taxane formulations that are Cremophor EL-free, aiming to solubilise the drug, minimise adverse effects and improve stability. These strategies include formulating taxanes in the form of albumin nanoparticles, micelles, cyclodextrins and liposomes. A main cause of instability of paclitaxel is the lipophilicity of the drug, which makes it extremely difficult to solubilise in an aqueous solution; therefore new formulations should demonstrate improved drug solubility and show equal or better drug action compared to Cremophor EL-based formulations (e.g. Taxol®).
2.5.1 Liposomes
Liposomes are spherical amphiphilic vesicles comprising lipid bilayers that provide a hydrophobic region permitting interaction with hydrophobic drugs, in order to allow for drug incorporation into the lipid bilayer and enhance its solubility. Liposomal formulations of paclitaxel are well researched in terms of taxane delivery and have shown enhanced drug solubilisation, stability and reduced side effects. Sharma and co-workers researched the effect of liposome-incorporated paclitaxel on toxicity and therapeutic effect in comparison to Taxol® [30]. In comparison to Taxol®, toxicity was markedly reduced using liposomal paclitaxel formulations. Whilst a Taxol® dose of >50 mg/kg in mice (with a human ovarian tumour xenograft) proved fatal, the same dose was well tolerated when administered in liposome formulations. Moreover, liposomal formulations provide a targeted delivery, increasing drug localisation into the tumour tissue due to the enhanced permeability and retention (EPR) effect which may also reduce the toxic effects of the drug on normal cells. Thus, reduced toxicity using liposomes is attributed to the absence of Cremophor EL and promoted targeted delivery to the cancerous cells. Yang and co-workers found that liposomes increased entrapment efficiency and drug solubility to 3.39 mg/mL and exhibited similar antitumour efficacy as compared to paclitaxel in Taxol® [29].
In another study, it has been found that although there was no significant difference in the distribution of the drug, the Cremophor EL-based formulation of paclitaxel is fivefold more toxic to normal tissues when compared to liposomal formulations [31]. Another study showed that when paclitaxel was incorporated into cationic liposomes, it prevented the growth of tumours and decreased the density of blood vessels at the tumour site by limiting the endothelial mitosis, whereas the Cremophor EL formulation elicited an insignificant effect on the growth of tumour and no effect on the blood vessels [32]. Lipusu® (Luye Pharma Group, China) is a recently commercialised liposomal formulation of paclitaxel that has been recommended for the treatment of breast, ovarian and non-small cell lung cancer [33,34,35]. Recently, we have designed liposomes based on a range of lipid compositions, generated using an ethanol-based proliposome technology. Compared to a Taxol-like formulation, the liposomal formulations of paclitaxel showed higher selectivity towards glioma cells when compared to healthy glial cells of the brain [36].
2.5.2 Nanoparticles
Nanoparticles may comprise a novel approach to delivering taxanes, and studies have been carried out using both paclitaxel [37] and docetaxel [38]. Fonseca et al. [39] found that PLGA nanoparticles (biodegradable, biocompatible, stable polymer) prepared using nano-precipitation method entrapped 100% of paclitaxel. Moreover, paclitaxel release from PLGA nanoparticles was initially rapid for the first 24 h after which release was slow and continuous. Furthermore, nanoparticles had a greater cytotoxic effect in comparison to Taxol® [39].
Xu and co-workers [40] used actively targetable nanoparticles (PEG-coated biodegradable polycyanoacrylate nanoparticles conjugated to transferrin) for paclitaxel delivery. Encapsulation efficiency reached as high as 94%, with drug initially released rapidly after which sustained release was achieved (81% of paclitaxel was released over 30 days). The release pattern was similar to that described by Fonseca and co-workers [39], which probably depends on polymer erosion patterns. Moreover, drug clearance from plasma was low in comparison to Taxol®, which can be due to failure by phagocytic system to recognise the nanoparticles, as previously discussed. Additionally, antitumour activity was enhanced and increased the life span of mice to 60 days [40]. Nanoparticles are also capable of providing targeted drug delivery and concentrate in tumour cells greatly compared to Taxol®. This might be due to transferrin conjugated to the nanoparticle as tumour cells have amplified transferrin receptors hence the greater antitumour activity.
Controlled release formulations have also been studied using docetaxel, where a prodrug of the taxane was incorporated into lipid nanoparticles (LNP). Testing of the prodrug on cancer cell lines revealed the drug easily converted to the active form and showed similar activity in vivo to the parent drug. Once loaded into LNPs, it was found that drug half-life was increased, the drug was well tolerated allowing administration of three times higher than the current max dose, and accumulation in the tumour tissue was 50–100 times more than Taxotere [41]. In that study, the development of a weak-base docetaxel derivative that can be loaded into lipid nanoparticles (LNP) was investigated. The LNP functions as a solubilising agent that is similar to polysorbate 80 and Cremophor EL; however, the lipids are less toxic. LNPs in that study were used to avoid the toxicities associated with polysorbate 80. A weak-base docetaxel derivative was efficiently loaded and retained by LNP. The study found that the prodrug that was formulated using polysorbate 80 had acute toxicity (i.e. changes in body weight at a docetaxel equivalent dose of 20 mg/kg). By contrast, the LNP derivative showed no signs of toxicity (no changes in body weight) at a docetaxel dose of 88 mg/kg. The LNP formulation seemed to have advantages over the traditional docetaxel formulation, as the hypersensitivity reactions were not observed.
A widely studied alternative to Taxol® is ABI-007 that is a novel human albumin-stabilised, lyophilised nanoparticle formulation incorporating paclitaxel. It has an average size of 130 nm and is free of Cremophor EL and ethanol [42]. Ibrahim and co-workers [43] conducted a phase I study of ABI-007 on patients who were diagnosed with an advanced solid tumour or had failed the standard therapy. Nineteen patients received doses of ABI-007 which ranged from 135 to 375 mg/m2. Three patients received infusions of ABI-007 over 2–3 h, and hypersensitivity reactions were not observed. Therefore, all the other infusions were administered over 30 min, and even at a faster infusion rate, no hypersensitivity reactions were observed [43]. Though this formulation was reported to be safer in terms of avoiding hypersensitivity reactions, other side effects that were dose dependent were reported, for example, haematological toxicity had occurred as one patient was taken to hospital for febrile neutropenia. Non-haematological toxicities were also reported such as nausea and vomiting, and muscle and joint pain were common. Ocular side effects were also reported such as ‘smoky’ vision and dry eyes. Two patients developed keratopathy where lubricating eye drops and ointments were needed to alleviate this [43]. A phase II trial carried out by Ibrahim and co-workers [44] to investigate the ABI-007 formulation in patients with metastatic breast cancer. Seven patients (11%) in that study discontinued treatment due to adverse effects such as neuropathy. Sixteen patients (25%) required dose reductions for toxicities; toxicities resulting in a dose reduction for two or more patients were uncomplicated neutropenia, sensory neuropathy, febrile neutropenia, myalgia and fatigue. No severe ocular events were reported, and other common taxane-associated toxicities were less severe and less frequent [44]. O’Shaughnessy and co-workers [45] compared the ABI-007 formulation against the standard paclitaxel formulation in patients with metastatic breast cancer. The study involved 454 patients who either received ABI-007260 mg/m2 infused over 30 min once every 3 weeks without premedication or Taxol® 175 mg/m2 administered over 3 h once every 3 weeks with premedication, including dexamethasone and antihistamines. This study confirmed no hypersensitivity reactions in patients received ABI-007, despite the absence of premedication. However, 10% of the patients who received ABI-007 experienced sensory neuropathy compared to 2% who received Taxol®. In order to alleviate sensory neuropathy, ABI-007 was withheld for a number of days. Other toxicities such as neutropenia and flushing were less frequent in patients treated with ABI-007 compared to Taxol® [45]. These clinical trials have led to the development of Abraxane® (ABI-007) which is a relatively recent paclitaxel derivative available in the United States. Abraxane® is used as a second-line treatment in patients with breast cancer if combination therapy fails [46]. Abraxane® has been found to be relatively safe so that the need for the corticosteroid therapy prior to paclitaxel administration was eliminated [47]. Infusion requires only 30 min for Abraxane® compared to 3 h for Taxol® [48]. Abraxane is nowadays referred to as ‘Nab-paclitaxel’. In combination with carboplatin, Nab-paclitaxel is indicated as first-line treatment of non-small cell lung cancer in patients who may not be cured by surgery or radiation therapy [49].
2.5.3 Polymeric Micelles
Genexol-PM is a novel biodegradable Cremophor EL-free polymeric micelle formulation of paclitaxel. A phase I study of Genexol-PM formulation was carried out in patients with advanced malignancies to determine the toxicities of Genexol-PM [50, 51]. Genexol-PM (1 mL) formulation contains 6 mg paclitaxel and 30 mg methoxy polyethylene glycol-poly (d,l-lactide). Nine patients had previously received taxane therapy, six of which showed tumour progression [50]. It was found that acute hypersensitivity was not observed in these patients; however, other toxicities such as neuropathy and myalgia were observed. These toxicities were dose related and the maximum tolerated dose was 390 mg/m2. Phase II trials of Genexol-PM were conducted to evaluate the efficacy and safety of the formulation in combination with cisplatin (antineoplastic drug) in patients with advanced non-small-cell lung cancer [52]. Accordingly, 5.8% of the patients experienced hypersensitivity reactions. Recently, it has been reported that Genexol-PM plus carboplatin as first-line treatment in patients with epithelial ovarian cancer showed high efficacy and low toxicity [51].
2.5.4 Other Formulation Strategies
Many nanocarrier systems can be used for delivery of poorly soluble drugs (e.g. paclitaxel). For example, dendrimers are monodisperse three-dimensional, hyper-branched polymers [53]. The oligomeric-branched structures of dendrimers can be designed to increase their hydrophobicity, aiming to enhance solubility of hydrophobic drugs. It has been found that when ethylene glycol was included within dendrimer formulation, the solubility of paclitaxel markedly enhanced (1.8–2.3 mg/mL) [54]. Moreover, the solubility of hydrophobic compounds was higher, and release rate was faster when G5 dendrimers were used as compared to low-generation dendrimers (e.g. G4 or G3 dendrimers). Lack of biodegradability of many dendrimer formulations (e.g. PAMAM dendrimers) remains an obstacle for the development of clinically applicable paclitaxel formulations.
Cyclodextrins are carrier systems that have shown the ability to enhance the solubility of paclitaxel and decrease its degradation by complexing with the drug in an aqueous solution [22]. Stability of the drug is increased by increasing its solubility as the drug becomes less likely to precipitate on storage. Other methods of enhancing solubility of paclitaxel include emulsion delivery systems [55, 56]. Recently, we have loaded paclitaxel into clinically established parenteral nutrition nanoemulsions and showed that such delivery systems have cytotoxic effect against glioma cell lines [56].
2.6 Conclusions
Paclitaxel, as the most prominent and common taxane, has been traditionally administered in Cremophor EL-based formulations (e.g. Taxol®); this vehicle is reliable for solubilising paclitaxel, but it causes many adverse effects. Several nanocarrier formulations of paclitaxel have shown to be appropriate alternatives to Cremophor EL formulations, owing to their biodegradability and the fewer adverse effects caused by the drug incorporated into these carriers. Many paclitaxel formulations based on nanotechnology are under investigations, and some are in the pipeline of commercialization.
References
Zhang A, Anyarambhatla L, Ma G, Ugwu L, Xuan S, Sardone T, Ahmed T, I. (2004) Development and characterization of a novel Cremophor EL free liposome-based paclitaxel (LEP-ETU) formulation. Eur J Pharm Biopharm 59:177–187
Vaishampayan U, Parchment ER, Bhaskara JR, Maha H (1999) Taxanes: an overview of the pharmacokinetics and pharmacodynamics. Urology 54(6):122–129
Thiesen J, Krämer I (1999) Physico-chemical stability of docetaxel premix solution and docetaxel infusion solutions in PVC bags and polyolefine containers. Pharm World Sci 21(3):137–141
Verweij J, Clavel M, Chevalier B (1994) Paclitaxel and docetaxel: not simply two of a kind. Ann Oncol 5:495–505
Jordan AM, Toso JR, Thrower D, Wilson L (1993) Mechanism of mitotic block and inhibition of cell proliferation by taxol at low concentrations. Proc Natl Acad Sci USA 90:9552–9556
DeVita VT, Lawrence TS, Rosenberg SA, Weinberg RA, DePinho RA (2008) DeVita, Hellman, and Rosenberg’s cancer: principles & practice of oncology, vol 1. Lippincott Williams and Wilkins, Philadelphia, pp 447–450
Schiff PB, Fant J, Horwitz SB (1979) Promotion of microtubule assembly in vitro by taxol. Nature 277:665–667
Rowinsky EK, Cazenave LA, Donehover RC (1990) Taxol: a novel investigational microtubule agent. J. Natl. Cancer Inst. 82:1247–1259
Singla AK, Garg A, Aggarwal D (2002) Paclitaxel and its formulations. Int J Pharm 235:179–192
O’Connell CB, Khodjakov AL (2007) Cooperative mechanisms of mitotic spindle formation. J Cell Sci 120:1717–1722
Crown J, O’Leary M (2000) Taxanes an update. Lancet 355:1176–1178
Kaye S, Piccart JM, Gore M, Huinink BTW, Oosterom VA, Verweij J, Wanders J, Franklin H, Bayssas M (1995) Docetaxel: an active new drug for treatment of advanced epithelial ovarian cancer. J Natl Cancer Inst 87(9):676–681
Engblom P, Pulkkinen OJ, Rantanen V, Hirvonen H, Kulmala J, Grènman R, Grènman S (1999) Effects of paclitaxel with or without cremophor EL on cellular clonogenic survival and apoptosis. Eur J Cancer 35(2):284–288
Nuijen B, Bouma M, Schellens JHM, Beijnen JH (2001) Progress in the development of alternative pharmaceutical formulations of taxanes. Invest New Drugs 19(2):143–153
Immordino ML, Brusa P, Arpicco S, Stella B, Dosio F, Cattel L (2003) Preparation, characterization, cytotoxicity and pharmacokinetics of liposomes containing docetaxel. J Control Release 91:417–429
Engels FK, Mathot RAA, Verweij J (2007) Alternative drug formulations of docetaxel: a review. Anticancer Drugs 18:95–103
Kattige A (2006) Long-term physical and chemical stability of a generic paclitaxel infusion under simulated storage and clinical-use conditions. Eur J Hosp Pharm Sci 12(6):129–134
Eroles AA, Bafalluy IM, Arnaiz JAS (2009) Stability of docetaxel diluted to 0.3 or 0.9 mg/mL with 0.9% sodium chloride injection and stored in polyolefin or glass containers. Am J Health Syst Pharm 66(17):1565–1568
Donyai P, Sewell GJ (2006) Physical and chemical stability of paclitaxel infusions in different container types. J Oncol Pharm Pract 12(4):211–222
Pourro B, Botta C, Solas C, Lacarelle B, Braguer D (2005) Seventy-two-hour stability of Taxol® in 5% dextrose or 0·9% sodium chloride in Viaflo®, Freeflex®, Ecoflac® and Macoflex N® non-PVC bags. J Clin Pharm Ther 30(5):455–458
Trissel LA, Xu QA, Gilbert DL (1998) Compatibility and stability of paclitaxel combined with doxorubicin hydrochloride in infusion solutions. Ann Parmacother 32(10):1013–1016
Dordunoo SK, Burt HM (1996) Solubility and stability of taxol: effects of buffers and cyclodextrins. Int J Pharm 133(1–2):191–201
Waugh WN, Trissel LA, Stella VJ (1991) Stability, compatibility, and plasticizer extraction of taxol (NSC-125973) injection diluted in infusion solutions and stored in various containers. Am J Hosp Pharm 48(7):1520–1524
Murphy SR, Wadey BL (1988) DEHP and toxicity. J Vinyl Technol 10(3):121–124
Dorr RT (1994) Pharmacology and toxicology of Cremophor EL diluent. Ann Pharmacother 28:511–514
Lilley LL, Scott HB (1993) What you need to know about taxol? Am. J. Nurs. 93:46–50
Gelderblom H, Verweij J, Nooter K, Sparreboom A (2001) Cremophor EL: the drawbacks and advantages of vehicle selection for drug formulation. Eur J Cancer 37:1590–1598
Lam YW, Chan CY, Kuhn JG (1997) Pharmacokinetics and pharmacodynamics of the taxanes. J. Oncol. Pharm. Pract 3:76–93
Yang T, Choi MK, Chung SJ, Shim CK, Kim CC (2007) Liposome formulation of paclitaxel with enhanced solubility and stability. Drug Deliv 5:3
Sharma A, Mayhew E, Bolcsak L, Cavanaugh C, Harmon P, Janoff A, Bernacki RJ (1997) Activity of paclitaxel liposome formulations against human ovarian tumor xenografts. Int. J. Cancer 71:103–107
Fetterly GJ, Straubinger RM (2003) Pharmacokinetics of paclitaxel-containing liposomes in rats. Am Assoc Pharm Sci 5(4):90–100
Kunstfeld R, Wickenhauser G, Michaelis U, Teifel M, Umek W, Naujoks K, Wolff K, Petzelbauer P (2003) Paclitaxel encapsulated in cationic liposomes diminishes tumor angiogenesis and melanoma growth in a “humanized” SCID mouse model. J Invest Dermat 120:476–482
Koudelka S, Turánek J (2012) Liposomal paclitaxel formulations. J Control Release 163:322–334
Wang H, Cheng G, Du Y, Ye L, Chen W, Zhang L, Wang T, Tian J, Fu F (2013) Hypersensitivity reaction studies of a polyethoxylated castor oil-free, liposome-based alternative paclitaxel formulation. Mol Med Rep 7:947–952
Bernabeu E, Cagel M, Lagomarsino E, Moretton M, Chiappetta DA (2017) Paclitaxel: what has been done and the challenges remain ahead. Int J Pharm 526:474–495
Najlah M, Jain M, Wan KW, Ahmed W, Albed Alhnan M, Phoenix DA, Taylor KM, Elhissi A (2016) Ethanol-based proliposome delivery systems of paclitaxel for in vitro application against brain cancer cells. J Liposome Res:1–12. https://doi.org/10.1080/08982104.2016.1259628
Musumeci T, Vicari L, Ventura CA, Gulisano M, Pignatello R, Puglisi G (2006) Lyoprotected nanosphere formulations for paclitaxel controlled delivery. J Nanosci Nanotechnol 6:1–8
Ahmad N, Alam MA, Ahmad R, Naqvi AA, Ahmad FJ (2017) Preparation and characterization of surface-modified PLGA-polymeric nanoparticles used to target treatment of intestinal cancer. Artif Cells Nanomed Biotechnol 1-14. doi:https://doi.org/10.1080/21691401.2017.1324466
Fonseca C, Simo’es S, Gaspar R (2002) Paclitaxel-loaded PLGA nanoparticles: preparation, physicochemical characterization and in vitro anti-tumoral activity. J Control Release 83:273–286
Xu Z, Gu W, Huang J, Sui H, Zhou Z, Yang Y, Yan Z, Li Y (2005) In vitro and in vivo evaluation of actively targetable nanoparticles for paclitaxel delivery. Int J Pharm 288:361–368
Zhigaltsev IV, Winters G, Srinivasulu M, Crawford J, Wong M, Amankwa L, Waterhouse D, Masin D, Webb M, Harasym N, Heller L, Bally MB, Ciufolini MA, Cullis PR, Maurer N (2010) Developement of a weak-base docetaxel derivative that can be loaded into lipid nanoparticles. J Control Release 144:332–340
Desai N, Yao Z, Soon-Shiong P, Dykes D (2002) Evidence of enhanced in vivo efficacy at maximum tolerated dose (MTD) of nanoparticle paclitaxel (ABI-007) and taxol in 5 human tumor xenografts of varying sensitivity to paclitaxel. Am Soc Clin Oncol 21:462
Ibrahim NK, Desai N, Legha S, Soon-Shiong P, Richard L, Rivera ET, Esmaeli B, Ring ES, Bedikian A, Hortobagyi NG, Ellerhorst AJ (2002) Phase I and pharmacokinetic study of ABI-007, a cremophor-free protein-stabilized, nanoparticle formulation of paclitaxel. Clin Cancer Res 8:1038–1044
Ibrahim NK, Samuels B, Page R, Doval D, Patel MK, Rao CS, Nair KM, Bhar P, Desai N, Hortobagyi GN (2005) Multicenter phase II trial of ABI-007, an albumin-bound paclitaxel, in women with metastatic breast cancer. J Clin Oncol 23(25):6019–6026
O’Shaughnessy J, Tjulandin S, Davidson N, Shaw H, Desai N, Hawkins MJ (2003) ABI-007 (ABRAXANE™), a nanoparticle albumin-bound (nab) paclitaxel demonstrates superior efficacy vs taxol in MBC: a phase III trial. Proceedings from the 26th annual San Antonio Breast Cancer Symposium, San Antonio, Texas, USA
Green MR, Manikhas GM, Orlov S, Afanasyev B, Makhson AM, Bhar P, Hawkins MJ (2006) Abraxane, a novel cremophor-free, albumin-bound particle form of paclitaxel for the treatment of advanced non-small-cell lung cancer. Ann Oncol 17:1263–1268
Gradishar WJ, Tjulandin S, Davidson N, Shaw H, Desai N, Bhar P, Hawkins M, O’Shaughnessy J (2005) Phase III trial of nanoparticle albumin-bound paclitaxel compared with polyethylated castor oil-based paclitaxel in women with breast cancer. J Clin Oncol 23(31):7794–7803
Garber K (2004) Improved paclitaxel formulation—hints at new chemotherapy approach. J Natl Cancer Inst 96:90–91
Blair HA, Deeks ED (2015) Albumin-bound paclitaxel: a review in non-small cell lung cancer. Drugs 75:2017–2024
Kim T-Y, Kim D-W, Chung J-Y, Shin SG, Kim S-C, Heo SD, Kim KN, Bang Y-J (2004) Phase I and pharmacokinetic study of genexol-pm, a cremophor-free, polymeric micelle-formulated paclitaxel, in patients with advanced malignancies. Clin Cancer Res 10:3708–3716
Lee SW, Kim YM, Cho CH, Kim YT, Kim SM, Hur SY, Kim JH, Kim BG, Kim SC, Ryu HS, Kang SB (2017) An open-label, randomized, parallel, phase II trial to evaluate the efficacy and safety of a cremophor-free polymeric micelle formulation of paclitaxel as first-line treatment for ovarian cancer: a Korean Gynecologic Oncology Group study (KGOG-3021). Cancer Res Treat. In Press Cancer Res Treat. doi: 10.4143/crt.2016.376
Kim D-W, Kim S-Y, Kim H-K, Kim S-W, Shin S-W, Kim SJ, Park K, Lee YM, Heo SD (2007) Multicenter phase II trial of Genexol-PM, a novel Cremophor-free, polymeric micelle formulation of paclitaxel, with cisplatin in patients with advanced non-small-cell lung cancer. European Society for Medical Oncology 18:2009–2014
Najlah M, D’Emanuele A (2006) Crossing cellular barriers using dendrimer nanotechnologies. Curr Opin Pharmacol 6:522–527
Ooya T, Lee J, Park K (2003) Effects of ethylene glycol-based graft, star-shaped, and dendritic polymers on solubilization and controlled release of paclitaxel. J Control Release 93:121–127
Kan P, Chen ZB, Lee CJ, Chu IM (1999) Development of nonionic surfactant/phospholipid o/w emulsion as a paclitaxel delivery system. J Control Release 58:271–278
Najlah M, Kadam A, Wan KW, Ahmed W, Taylor KM, Elhissi AM (2016) Novel paclitaxel formulations solubilized by parenteral nutrition nanoemulsions for application against glioma cell lines. Int J Pharm 506:102–109
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG
About this chapter
Cite this chapter
Elhissi, A., Mahmood, R., Parveen, I., Vali, A., Ahmed, W., Jackson, M.J. (2018). Taxane Formulations: From Plant to Clinic. In: Jackson, M., Ahmed, W. (eds) Micro and Nanomanufacturing Volume II. Springer, Cham. https://doi.org/10.1007/978-3-319-67132-1_2
Download citation
DOI: https://doi.org/10.1007/978-3-319-67132-1_2
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-67130-7
Online ISBN: 978-3-319-67132-1
eBook Packages: EngineeringEngineering (R0)