Abstract
The availability of effective drugs targeting the major risk factors of cardiovascular disease (CVD) has reduced morbidity and mortality. Cumulative relative risk of CVD events can be reduced by 75 % with a combination of aspirin, a β-adrenoceptor antagonist (β-blocker), an HMG-CoA reductase inhibitor (statin), and an angiotensin-converting enzyme inhibitor. The principal pharmacodynamics of these drugs cannot explain the entirety of their cardioprotective action, as other drugs with similar pharmacologic targets have not been associated with favorable clinical effects. This raises the possibility that the cardioprotective drugs have a unique pleiotropic activity that contributes to their clinical efficacy. Recent data suggest that reducing cellular stress such as oxidative, inflammatory, and endoplasmic reticulum stress, might be a common denominator of the drugs with proven efficacy in reducing CVD risk. In this communication, the evidence in favor of this hypothesis is discussed, and ongoing trials with therapeutic agents targeting cellular stresses are reviewed.
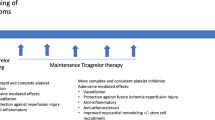
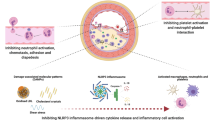
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Cumulative relative risk of cardiovascular events can be reduced by 75 % with a combination of aspirin, a β-adrenoceptor antagonist (β-blocker), an HMG-CoA reductase inhibitor (statin), and an angiotensin-converting enzyme inhibitor. |
These cardioprotective drugs share the pleiotropic effects of reducing cellular stresses such as oxidative, inflammatory, and endoplasmic reticulum stress. |
Selective targeting of oxidative stress has been shown to be ineffective in reducing cardiovascular risk. |
The proof of the hypothesis that reducing cellular stress is a meaningful therapeutic target would hinge on clinical trials with pharmacologic agents that reduce cellular stress without altering the traditional risk factors such as hypertension or dyslipidemia. |
1 Introduction
Over the last 5 decades, there have been remarkable advances in the prevention and treatment of cardiovascular disease (CVD) [1, 2]. Many factors account for this success, including technologic advances in interventional cardiology and coronary care units, early resuscitation and intervention protocols, and effective drugs targeting the major risk factors of CVD such as hypercholesterolemia, hypertension, platelet aggregability, and possibly hyperglycemia. In 2002, Yusuf [3] suggested that the cumulative relative risk of CVD events such as cardiovascular death, myocardial infarction, and stroke could be reduced by 75 % using a combination of aspirin, a β-adrenoceptor antagonist (β-blocker), an HMG-CoA reductase inhibitor (statin), and an angiotensin-converting enzyme (ACE) inhibitor. Among smokers, cessation of smoking for 2 years lowers risk of recurrent myocardial infarction by about one-half, which—along with the four drugs used—increases cumulative risk reduction to 80 %.
Although lowering of blood pressure is the principal driver of reducing cardiovascular events in most people with hypertension, some antihypertensive drug classes have been shown to confer added protection in patients with proteinuria, coronary heart disease, or heart failure [4, 5]. The 2015 American Heart Association/American College of Cardiology/American Society of Hypertension Scientific Statement on Treatment of Hypertension in Patients with Coronary Artery Disease [6] recommended that management should include β-blockers, ACE inhibitors, or angiotensin receptor blockers, and—in people with heart failure—aldosterone antagonists. The statement further concluded that, whereas diuretics and calcium channel blockers can be used for the management of hypertension, the evidence for improved outcomes in hypertension with coronary artery disease (CAD) is very small [6].
The drugs with proven cardioprotective properties are also effective in people with diabetes who are at high risk for CVD. In this population, in addition to statins, β-blockers, and ACE inhibitors, targeting hyperglycemia with metformin can also reduce cardiovascular events [7]. More recently, use of the sodium glucose transporter 2 (SGLT2) inhibitor empagliflozin has been associated with favorable effects [8], whereas other antihyperglycemic agents have had either modestly favorable, marginal, or detrimental effects on CVD [9–13].
The principal pharmacodynamics of these drugs targeting various risk factors of CVD cannot explain the entirety of their cardioprotective action, as many other drugs with similar pharmacologic targets have not been associated with favorable clinical effects. This raises the possibility that these latter drugs either have adverse off-target effects that limit their clinical efficacy in reducing CVD events or that the cardioprotective drugs have unique pleiotropic activity that contributes to their efficacy in reducing major cardiovascular events. Recently available data suggest that reducing cellular stress such as oxidative, inflammatory, and endoplasmic reticulum (ER) stress might be a common denominator of the pleiotropic effects of the drugs with proven efficacy in reducing CVD risk (Table 1) [14–25].
Oxidative and inflammatory processes have been implicated in atherogenesis and in myocardial cell injury especially after ischemia/reperfusion [26]. More recently, ER stress manifesting as abnormal accumulation of misfolded proteins has also been shown to cause cellular apoptosis and is implicated in the progression and rupture of atherosclerotic plaques [27].
In this communication, the cellular stress-reducing properties of drugs known to have reduced cardiovascular mortality in at least subgroups of patients are discussed, and ongoing trials with therapeutic agents targeting cellular stresses are reviewed.
2 Cardioprotective Drugs Targeting Cellular Stress
2.1 Statins
Although hypercholesterolemia and, more specifically, elevated low-density lipoprotein cholesterol (LDL-C) concentration, is an established risk for CVD, and partial ileal bypass-associated reductions in plasma cholesterol levels reduced myocardial infarction and subsequent morbidity [28], only statins have been shown to reduce cardiovascular and all-cause mortality [29–31]. Recently, ezetimibe, a cholesterol-absorption inhibitor, was also shown for the first time to have some cardioprotective effect commensurate with its modest lowering of LDL-C levels [32]. In this trial, patients with an acute coronary syndrome (ACS) within the previous 10 days were randomly assigned to either simvastatin 40 mg plus ezetimibe 10 mg or to simvastatin 40 mg plus placebo. At 1 year, the mean LDL-C level was 53.2 mg/dl (1.4 mmol/l) in the simvastatin-plus-ezetimibe group and 69.9 mg/dl (1.8 mmol/l) in the simvastatin-monotherapy group. At a median of 6 years, the rate of cardiovascular events was modestly but significantly lower in the simvastatin–ezetimibe group [32]. The idea that the benefit of ezetimibe in this trial is mediated solely by the lowering of LDL-C levels has been met with some skepticism because ezetimibe—like statins—has pleiotropic effects, including antioxidant and anti-inflammatory properties [33–36]. Indeed, the levels of high-sensitivity C-reactive protein (hsCRP) were significantly lower in the simvastatin–ezetimibe group than in the simvastatin monotherapy group [36]. The proprotein convertase subtilisin/kexin type 9 (PCSK9) inhibitors may also prove to be clinically effective in reducing cardiovascular events [37, 38], and long-term trials could be helpful in establishing the cholesterol hypothesis. However, it is possible that the favorable effects of statins may exceed their effectiveness in lowering LDL-C. Cell cultures and studies in animals have shown the efficacy of statins in simultaneously reducing oxidative stress and ER stress [14, 15]. These properties have been associated with their ability to optimize the endothelial barrier function and prevent dextrose-induced endothelial cell death [15].
The precise mechanism of protective effects of statins is not known. Statins have been shown to attenuate vascular smooth muscle proliferation by preventing Rho GTPase-induced down-regulation of p27Kip1 [39], and Rho GTPase is instrumental in the regulation of endothelial nitric oxide synthase (eNOS), a key enzyme in modulating vascular function [40]. In spontaneously hypertensive rats, atorvastatin treatment downregulated aortic angiotensin type 1 receptor messenger RNA (mRNA) expression, reduced mRNA expression of the essential NAD(P)H oxidase subunit p22phox, and caused an upregulation of endothelial constitutive NOS (ecNOS) mRNA expression [41]. In cell cultures, mRNA expression of superoxide dismutase isoforms and glutathione peroxidase was not modified by atorvastatin, whereas catalase expression was upregulated [42]. These changes contribute to the antioxidant effects of statins.
2.2 β-Adrenoceptor Antagonists
A host of clinical trials with several β-blockers have shown the capacity of this class of agents to reduce major cardiovascular events in high-risk people with CAD and previous myocardial infarction as well as in those with congestive heart failure (CHF) and low ejection fraction [43, 44]. The efficacy of β-blockers in patients with stable coronary heart disease has been questioned as there are no recent randomized controlled trials demonstrating that β-blockers are cardioprotective in patients who are offered reperfusion interventions and intensive medical therapy with aspirin, statin, ACE inhibitors, and angiotensin receptor blockers [44]. Although β-blockers are effective antihypertensive agents, their enhanced beneficial effects are attributed to their anti-arrhythmogenic activity as well as their effectiveness in reducing myocardial oxygen demand through reducing the heart rate and myocardial contractility. However, many known anti-arrhythmogenic drugs do not reduce cardiovascular mortality [45]. Furthermore, calcium channel blockers, which are effective antihypertensive agents and can reduce the heart rate and myocardial contractility, are not associated with survival advantage, although they can be effective in controlling angina [46, 47]. More recently, ivabradine, an agent that selectively reduces the heart rate without affecting blood pressure or left ventricular systolic function, has been shown to improve outcomes in patients with systolic heart failure [48]. Ivabradine also reduces ischemia in patients with stable angina pectoris but has failed to reduce the incidence of fatal and nonfatal myocardial infarction in a trial in over 19,000 patients with stable CAD [49]. In the latter trial, a disconcerting finding was that ivabradine was associated with a significant increase in the incidence of the primary endpoint among patients with class II or higher angina (7.6 vs. 6.5 % with placebo; p = 0.02) [49, 50].
Overall, clinical trials suggest that the known cardioprotective properties of β-blockers cannot solely be explained by their ability to reduce blood pressure, heart rate, or myocardial contractility. Given this uncertainty, it is possible that the cardioprotective effects of β-blockers could be the results of hitherto underestimated pleiotropic effects as reducers of cellular stresses such as oxidative stress and ER stress [16–19]. The underlying mechanisms of the antioxidant activity of β-blockers are not known. Experiments in vivo and in cell cultures have shown that some β-blockers act as effective scavengers of reactive oxygen species [51, 52].
2.3 Renin Angiotensin Aldosterone System Inhibitors
The renin angiotensin aldosterone system (RAAS) is a hormonal cascade with a pivotal role in maintaining blood pressure and serum electrolyte homeostasis. In addition to these systemic effects, the discovery that the myocardial tissue and endothelial cells have the full complement of the components of RAAS has expanded its physiologic and pathophysiologic effects within these tissues [53]. Activation of this system in people with diabetes has been suspected to play a key pathophysiologic role in premature atherosclerosis, nephropathy, and retinopathy [54–59].
Interrupting RAAS with either ACE inhibitors or angiotensin II (A-II) receptor antagonists (A-II receptor blockers [ARBs]) has been shown to have favorable effects in cardiovascular events and has been the cornerstone of therapy aimed at preventing diabetic nephropathy [58]. Blocking aldosterone receptors with spironolactone or eplerenone has also been effective in reducing major cardiovascular events in patients with CHF [60–62]. The renin inhibitor aliskiren may also be an effective agent in reducing cardiac events in patients with CHF. However, a recent study found that the addition of aliskiren to enalapril led to more adverse events without an increase in benefit, and aliskiren non-inferiority compared with enalapril could not be shown [63].
The vascular-protective effects of RAAS inhibition cannot be explained solely by the changes in blood pressure, as other equally effective antihypertensive agents do not impart the same degree of clinical benefits. A recent study in 253 patients with end-stage renal disease receiving non-heart failure dialysis found that treatment with spironolactone 25 mg once daily for 2 years significantly reduced the primary outcome of a composite of death from cardiocerebrovascular (CCV) events, aborted cardiac arrest, and sudden cardiac death (7.2 vs. 18.0 %; adjusted hazard ratio [HR] 0.42; 95 % confidence interval [CI] 0.26–0.78) [64]. Death from CCV events occurred in 4.0 % of patients in the spironolactone group and in 11.7 % of patients in the control group. The secondary outcome of death from all causes occurred less frequently in the spironolactone group than in the control group (9.6 vs. 19.5 %; adjusted HR 0.52; 95 % CI 0.29–0.94) [64]. The beneficial effect was independent of blood pressure changes or changes in salt or potassium handling in the kidney [64].
A-II receptor signaling has been identified as the mediator of oxidative, inflammatory, and ER stresses in various tissues [20–24]. Interrupting RAAS with ACE or A-II receptor inhibitors or the aldosterone receptor blocker spironolactone has been shown to reduce oxidative stress [20–24]. Spironolactone and ARBs are also effective in reducing ER stress [24]. These pleiotropic effects of diverse inhibitors of RAAS may contribute to the salutary effects of these agents in reducing vascular disease. It is noteworthy that it can be argued that the antioxidative and ER stress-reducing effects of RAAS inhibitors should not be considered pleiotropic effects as the A-II type 1 receptor has a pivotal role in oxidative stress and ER stress [24].
2.4 Antiplatelet Therapy
It is generally accepted that intracoronary artery clot formation is a common terminal event in a large number of people with myocardial infarction. Thus, the effectiveness of antiplatelet agents in reducing major cardiovascular events is supported by strong pharmacologic plausibility and by empiric data from large clinical trials [65–67]. It is intriguing that the two most commonly used antiplatelet agents, namely aspirin and clopidogrel, have significant pleiotropic effects that ameliorate cellular stresses, notably oxidative and inflammatory stresses [68–70]. In one study, the total antioxidant capacity of plasma from people receiving aspirin or clopidogrel was significantly increased [69]. Clopidogrel improves endothelial nitric oxide bioavailability and diminishes biomarkers of oxidant stress and inflammation in patients with symptomatic CAD [70]. It is noteworthy that aspirin at clinically achievable plasma concentrations activates AMP-activated protein kinase (AMPK), a central regulator of cell metabolism [71]. Clopidogrel has also been shown to activate AMPK and the phosphoinositide 3 kinase (PI3 K)-Akt pathway, thereby enhancing vascular protection [72, 73].
2.5 Antihyperglycemic Agents
The role of increased blood glucose concentrations in the pathogenesis of accelerated atherogenesis in diabetes has been challenged because clinical trials have not been able to consistently demonstrate reductions in cardiovascular events associated with improved blood glucose control [10–13]. This failure to demonstrate efficacy has been attributed to a variety of factors, including the peculiarities of patient populations studied, relatively small differentials in blood glucose levels between the intensively treated and standard care groups, off-target effects of the antiglycemic agents used, or lack of sufficient time to observe clinical benefits [13]. However there have been two remarkable exceptions so far. One is the demonstration of cardioprotective effects of metformin in a study of overweight people with diabetes [7] and the other is the recent clinical trial using empagliflozin as an add-on therapy [8].
The main mechanism of action of metformin is believed to be through activation of AMPK. However, metformin has a number of pleiotropic effects that would theoretically contribute to its cardioprotective role [74–76]. These effects include reducing cellular oxidative stress and possibly interfering with advanced glycation end-product accumulation [74–76]. Hyperglycemia and hypertension impair endothelial function in part through oxidative stress-activated poly (adenosine diphosphate [ADP]-ribose) polymerase 1 (PARP1). Metformin and temisartan (an ARB) but not metoprolol reduced PARP1 activity via AMPK activation [77]. In addition, metformin activates the synthesis of Nrf2, which controls the expression of many antioxidant enzymes and blocks the synthesis of the transcription factor nuclear factor (NF)-κB, which controls several molecules involved in the generation of inflammatory responses [74]. Thus, metformin can reduce both oxidative and inflammatory stresses and as such can be designated an antioxidant inflammation modulator (AIM). It is noteworthy that another known AIM molecule is bardoxolone, which in clinical trials failed to show significant reductions in cardiovascular events [78]. It is likely that metformin, through pleiotropic effects, has additional cardioprotective activity.
Pioglitazone is another antiglycemic agent that possesses antioxidative and anti-inflammatory activity that may well contribute to some of the cardioprotective effects observed in a few clinical trials [79–82]. Although peroxisome proliferator-activated receptor (PPAR)-γ activation provides cardioprotection from oxidative stress caused by hydrogen peroxide [79], only pioglitazone but not rosiglitazone has been found to be associated with cardioprotection. However, the US FDA issued a ‘black box warning’ for pioglitazone because of the high risk of developing CHF while using it.
More recently, two additional antiglycemic agents were found to have some cardioprotective effects. In a large randomized study, treatment with empagliflozin, an SGLT2 inhibitor, resulted in a significant reduction in the primary outcome (death from cardiovascular causes, nonfatal myocardial infarction, or nonfatal stroke: 10.5 % in the pooled empagliflozin group vs. 12.1 % in the placebo group; HR in the empagliflozin group, 0.86; p = 0.04 for superiority [8]. In addition, empagliflozin was associated with a slower progression of kidney disease in patients at high cardiovascular risk [83].
Another antiglycemic agent shown to have cardioprotective properties is liraglutide. In a randomized study of patients with type 2 diabetes mellitus and established CVD, liraglutide also demonstrated a significant reduction of the composite endpoint of cardiovascular death, non-fatal myocardial infarction, or non-fatal stroke [84]. The precise mechanisms of the cardioprotective effects of these agents are not known. Multiple factors could have contributed to the cardioprotective effects of empagliflozin, such as changes in arterial stiffness and cardiac oxygen demand, as well as reductions in albuminuria and plasma uric acid concentrations [8].
It is noteworthy that empagliflozin has also been shown to have anti-inflammatory and antioxidative properties [85, 86]. Similarly, the pleotropic effects of liraglutide include reductions in cellular stresses such as inflammatory, oxidative, and ER stresses [87–92]. The glucagon-like peptide (GLP)-1 agonist lixisenatide and three dipeptidyl peptidase (DPP)-4 inhibitors (alogliptin, saxagliptin, and sitagliptin) studied were not associated with a lower rate of cardiovascular events compared with the control of diabetes with other drug classes [93–96]. A number of other trials are in progress [97].
2.6 Hormone-Replacement Therapy
There is considerable debate in the literature as to the cardioprotective effects of estrogen and possibly testosterone. Estrogens reduce ischemic damage during cerebrovascular and coronary artery occlusion [98, 99], and low plasma testosterone levels in men are a predictor of CVD [100, 101]. However, findings from the Women’s Health Initiative suggest that the risk for coronary heart disease was not significantly changed in the conjugated equine estrogens plus medroxyprogesterone acetate trial (HR 1.18; 95 % CI 0.95–1.45) or in the conjugated equine estrogens-alone trial (HR 0.94; 95 % CI 0.78–1.14) [102]. It has been postulated that estrogen may slow early stages of atherosclerosis but may have adverse effects on advanced atherosclerotic lesions [103, 104] This is consistent with the observation that, in women aged <50 years, combination estrogen–progestogen was associated with a reduction in a composite endpoint that included CVD [103]. In addition, preliminary findings from ELITE (Early versus Late Intervention Trial with Estradiol) show that estrogen slows atherosclerosis progression among women in early but not late menopause [104]. However, in ELITE, the primary outcome was surrogate endpoint of carotid artery intima-media thickness (CIMT) and the study population was not large enough to assess cardiovascular events [104].
Estrogens have diverse effects on a host of variables that may change cardiovascular risk. One of the pleiotropic effects of estrogens is their antioxidative and ER stress-reducing effect [105–107]. In endothelial cell cultures, physiologic concentrations of estradiol and testosterone suppress oxidative stress and inhibit dextrose-induced ER stress [107]. The effect of testosterone was attributed to its aromatization to estradiol since non-metabolizable analogs of testosterone such as dehydrotestosterone and 5-methyl testosterone were not effective, and pharmacological inhibition of aromatization prevented testosterone-related reductions in ER stress or superoxide production [108]. Indeed, in a cell-free system, testosterone did not have antioxidant capacity when aromatization was not possible [108].
3 Ongoing Trials Targeting Cellular Stress
Oxidative stress and inflammation play a critical role in the pathogenesis of atherosclerosis [25]. Several drugs with antioxidative and anti-inflammatory properties are being developed for the treatment of atherosclerosis (Table 2) [109–113].
The clinical development of AIMs such as bardoxolone or a synthetic triterpenoid derivative of oleanolic acid, RTA 408, is now being pursued as treatment for premature vascular disease [78, 114]. These novel compounds attenuate the degradation of Nrf2, which promotes the production of important antioxidant enzymes and inhibits pro-inflammatory transcription factors including, NF-κB and STAT3 [109, 110]. However, it is noteworthy that in the BEACON (Bardoxolone Methyl Evaluation in Patients with Chronic Kidney Disease and Type 2 Diabetes Mellitus: the Occurrence of Renal Events) trial, bardoxolone methyl increased risk of heart failure and cardiovascular events [78]. It is possible that this unfavorable effect may have been secondary to drug interactions with ARBs or ACE inhibitors, thereby decreasing their bioavailability and reducing their effectiveness as cardioprotective agents [115].
Another agent with antioxidant and anti-inflammatory properties tested in phase II trials is succinobucol. This compound is a monosuccinic acid ester of probucol, a lipid-lowering agent that has been abandoned in clinical practice because of its adverse effects on cardiac arrhythmias [116, 117]. In the ARISE (Aggressive Reduction in Inflammation Stops Events) trial, 6144 patients with recent ischemia were randomized to receive either succinobucol or placebo and followed for the primary composite endpoint of cardiovascular death, resuscitated cardiac arrest, myocardial infarction, stroke, unstable angina, or revascularization [116]. There were no benefits on this primary endpoint, and serious adverse events were significantly increased in the active treatment arm of the study. Similarly, in a second trial among 232 patients undergoing elective percutaneous coronary interventions (PCIs), succinobucol had no effect on plaque volume or atherosclerotic regression [117]. Given the results of these trials, succinobucol is no longer considered a potential therapeutic agent.
Colchicine is an anti-inflammatory agent commonly used in clinical practice to treat gout or periodic polyserositis. It has also been tested in small clinical trials as a potential cardioprotective agent. In one study, 21 patients with ACS were randomized to receive either oral colchicine or no treatment and compared with nine untreated healthy controls. Colchicine treatment reduced intracellular and secreted levels of interleukin (IL)-1β [118]. In another study of 40 patients with ACS (33 with stable CAD) and ten controls, oral colchicine treatment significantly reduced trans-coronary gradients for IL-1β, IL-18, and IL-6 [119]. The clinical implications of this observation are not yet known.
The anti-IL-1β antibody gevokizumab is in early clinical trials to investigate its ability to reduce the risk of diabetic kidney disease and CVD [120, 121]. Canakinumab is a human monoclonal antibody that selectively neutralizes IL-1β and is currently used for the treatment of a rare group of IL-1β-mediated inflammatory diseases [122, 123]. The outcome of long-term IL-1β inhibition will be evaluated in CANTOS (Canakinumab Anti-inflammatory Thrombosis Outcomes Study). In this study, the rates of major acute cardiovascular events, such as recurrent myocardial infarction, stroke, and cardiovascular death, will be evaluated among 17,000 stable patients with persistent hsCRP elevation after myocardial infarction [123].
Another therapeutic target is arachidonate 5-lipoxygenase (5-LO), a key enzyme in the synthesis of leukotrienes, such as the potent chemoattractant leukotriene B4 (LTB4) and the vascular permeability-enhancing leukotriene E4 (LTE4) [124]. The leukotrienes participate in host defense reactions and pathophysiological conditions such as immediate hypersensitivity and inflammation. Inhibitors of the 5-LO pathway have been tested in small clinical trials [125, 126]. In one of these, 191 patients with ACS were randomly assigned to receive VIA-2291 at doses of 25, 50, or 100 mg or placebo daily for 12 weeks. Levels of whole blood-stimulated leukotriene LTB4 and urine leukotriene LTE4 were reduced; in a subset of 60 compliant patients, coronary computed tomography (CT) examination showed that new coronary plaques were less frequent in the active treatment group [126]. However, another study found that inhibition of 5-LO with VIA-2291 was not associated with significant reductions in vascular inflammation (via fluorodeoxyglucose positron emission tomography [FDG-PET]) or in blood inflammatory markers [126].
Phospholipase A2 inhibitors have been tested for the treatment of atherosclerosis [127]. Darapladib (GlaxoSmithKline) is an inhibitor of lipoprotein-associated phospholipase A2, and varespladib (Anthera) inhibits several forms of the secreted phospholipase A2s [127, 128]. Unexpectedly, in the VISTA-16 trial, treatment with varespladib was associated with an increased incidence of myocardial infarction, cardiovascular mortality, and stroke in patients with ACS despite lower levels of LDL-C and CRP than those receiving placebo [129]. The adverse outcome in the latter study could be the result of lack of specificity of the approach, as prostaglandins are not the only products of arachidonic acid metabolism. Similarly, darapladib did not reduce cardiovascular events in the STABILITY (Stabilization of Atherosclerotic plaque by Initiation of darapladib therapy) and SOLID-TIMI 52 (Stabilization of Plaques Using Darapladib-Thrombolysis in Myocardial Infarction) trials [130, 131]. The precise mechanism behind the increase in the incidence of myocardial infarction has not been elucidated. However, other drugs modulating the prostaglandin metabolites have shown a detrimental effect on the incidence of myocardial infarction [130, 131]. These negative results highlight the complexity of the pathogenesis of the atherosclerotic process. Nevertheless, several anti-inflammatory drugs are still in clinical development, including the p38 mitogen-activated protein kinase (MAPK) inhibitor losmapimod and low-dose methotrexate.
P-selectin belongs to a family of adhesion molecules that are involved in recruitment of leukocytes into atherosclerotic lesions, and inhibition of P-selectin signaling may attenuate inflammatory responses [132, 133]. Two ongoing randomized trials are testing the efficacy and safety of RO4905417 (inclacumab), a novel recombinant monoclonal antibody, against P-selectin. The SELECT-ACS trial is evaluating the efficacy of the drug in reducing procedural damage during PCI, assessed with troponin I levels, and the SELECT-CABG (SELECT-Coronary Artery Bypass Graft) trial tested the efficacy of this compound in preventing saphenous vein graft disease in patients undergoing CABG surgery [132, 133]. The SELECT-ACS trial demonstrated the efficacy of inclacumab in reducing myocardial damage following PCI, whereas the SELECT-CABG trial found that inclacumab had no favorable effects on saphenous vein graft disease progression.
Serp-1 is a secreted glycoprotein of the serpin superfamily, is an inhibitor of tissue and urokinase-type plasminogen activators, and has anti-inflammatory effects [134, 135]. A phase II randomized trial of 48 patients with ACS undergoing a coronary stent procedure and receiving 6 months of treatment with the viral-derived Serp-1 indicated that patients treated with higher doses of Serp-1 experienced fewer major adverse cardiac events than those receiving the lower dose or placebo [134]. Plasminogen activator inhibitor 1 (PAI-1) is the main inhibitor of tissue-type plasminogen activator (tPA) and urokinase plasminogen activator (uPA), and inhibition of PAI-1 activity by small organic molecules is a potential therapeutic strategy to ameliorate atherosclerosis [135].
To date, evidence supporting the use of anti-inflammatory therapies for prevention of CAD is limited to observational studies or small trials with surrogate endpoints.
4 Failure of Selective Targeting of Oxidative Stress
The antioxidative and anti-inflammatory properties of the various cardioprotective drugs cannot fully account for their effectiveness, as large clinical trials with potent antioxidants have failed to show any clinical benefit and some trials have found evidence for increased harm (Table 3) [136–147]. It can be argued that antioxidants used in the clinical trials were not selective enough to target oxidative stress in key cellular compartments. Many factors could explain this paradoxical outcome with antioxidant therapy, including the possibility that antioxidants may aggravate ER stress while reducing oxidative stress [148–150]. It is entirely possible that, given the multiplicity of cellular compartments where stress can occur, an effective strategy is to target the multiple stresses simultaneously rather than selectively. In this regard, the evolution of AIMs seems to be in the right direction.
5 Conclusions
Despite the diversity of pharmacologic profiles of the drugs with proven efficacy in reducing CVD, reducing cellular stress is a shared pleiotropic effect. These drugs have potent antioxidative and anti-inflammatory activity and are often effective in reducing ER stress that is increased in atherosclerotic plaques associated with ACS [27]. It is tempting to speculate that all the known risk factors of CAD promote atherosclerosis through a common pathogenetic mechanism of increased cellular stress (Fig. 1). However, this pathogenesis is extraordinarily complex and much is yet to be learned about the precise underlying mechanisms of cellular stresses. Understanding the nature of the cross talk among these multiple cellular stresses can increase the possibilities of developing new therapeutic agents that can reduce CVD risk. The ultimate proof of the hypothesis that reducing cellular stress is a meaningful therapeutic target would hinge on clinical trials with pharmacologic agents that reduce cellular stress without altering traditional risk factors such as hypertension or dyslipidemia.
References
Gregg EW, Li Y, Wang J, Burrows NR, Ali MK, Rolka D, Williams DE, Geiss L. Changes in diabetes-related complications in the United States, 1990–2010. N Engl J Med. 2014;370:1514–23.
Johnson NB, Hayes LD, Brown K, Hoo EC, Ethier KA, Centers for Disease Control and Prevention (CDC). CDC National Health Report: leading causes of morbidity and mortality and associated behavioral risk and protective factors–United States, 2005–2013. MMWR Surveill Summ. 2014;63(Suppl 4):3–27.
Yusuf S. Two decades of progress in preventing vascular disease. Lancet. 2002;360:2–3.
ALLHAT Officers and Coordinators for the ALLHAT Collaborative Research Group. Major outcomes in high-risk hypertensive patients randomized to angiotensin-converting enzyme inhibitor or calcium channel blocker vs diuretic: the Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial (ALLHAT). JAMA. 2002;288:2981–97.
Law MR, Morris JK, Wald NJ. Use of blood pressure lowering drugs in the prevention of cardiovascular disease: meta-analysis of 147 randomised trials in the context of expectations from prospective epidemiological studies. BMJ. 2009;338:b1665.
Rosendorff C, On behalf of the Writing Committee. Treatment of hypertension in patients with coronary artery disease. A case-based summary of the 2015 AHA/ACC/ASH scientific statement. Am J Med. 2016;129:372–8.
UK Prospective Diabetes Study (UKPDS) Group. Effect of intensive blood-glucose control with metformin on complications in overweight patients with type 2 diabetes (UKPDS 34). Lancet. 1998;352:854–65.
Zinman B, Wanner C, Lachin JM, For the EMPA-REG OUTCOME Investigators, et al. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373:2117–2128.
UK Prospective Diabetes Study (UKPDS) Group. Intensive blood-glucose control with sulphonylureas or insulin compared with conventional treatment and risk of complications in patients with type 2 diabetes (UKPDS 33). Lancet. 1998;352:837–53.
ACCORD Study Group, Gerstein HC, Miller ME, Genuth S, et al. Long-term effects of intensive glucose lowering on cardiovascular outcomes. N Engl J Med. 2011;364:818–28.
Reusch JE, Wang CC. Cardiovascular disease in diabetes: where does glucose fit in? J Clin Endocrinol Metab. 2011;96:2367–76.
Ray KK, Seshasai SR, Wijesuriya S, et al. Effect of intensive control of glucose on cardiovascular outcomes and death in patients with diabetes mellitus: a meta-analysis of randomised controlled trials. Lancet. 2009;373:1765–72.
Hayward RA, Reaven PD, Wiitala WL, et al. Follow-up of glycemic control and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2015;372:2197–206.
Kojanian H, Szafran-Swietlik A, Onstead-Haas LM, Haas MJ, Mooradian AD. Statins prevent dextrose-induced endoplasmic reticulum stress and oxidative stress in endothelial and HepG2 cells. Am J Ther. 2014 [Epub ahead of print].
Haas MJ, Horani MH, Parseghian SA, Mooradian AD. Statins prevent dextrose-induced endothelial barrier dysfunction, possibly through inhibition of superoxide formation. Diabetes. 2006;55:474–9.
Haas MJ, Kurban W, Shah H, Onstead-Haas L, Mooradian AD. Beta blockers suppress dextrose-induced endoplasmic reticulum stress, oxidative stress, and apoptosis in human coronary artery endothelial cells. Am J Ther. 2015 [Epub ahead of print].
Horani MH, Haas MJ, Mooradian AD. Suppression of hyperglycemia-induced superoxide formation and endothelin-1 gene expression by carvedilol. Am J Ther. 2006;13:2–7.
Fahlbusch SA, Tsikas D, Mehls C, et al. Effects of carvedilol on oxidative stress in human endothelial cells and healthy volunteers. Eur J Clin Pharmacol. 2004;60:83–8.
Chan S, Chen MP, Cao JM, Chan GC, Cheung YF. Carvedilol protects against iron-induced microparticle generation and apoptosis of endothelial cells. Acta Haematol. 2014;132:200–10.
Nickenig G, Harrison DG. The AT1-type angiotensin receptor in oxidative stress and atherogenesis, part I: oxidative stress and atherogenesis. Circulation. 2002;105:393–6.
Sowers JR. Hypertension, angiotensin II, and oxidative stress. N Engl J Med. 2002;346:1999–2001.
Nguyen Dinh Cat A, Montezano AC, Burger D, Touyz RM. Angiotensin II, NADPH oxidase, and redox signaling in the vasculature. Antioxid Redox Signal. 2013;19:1110–20.
Zhang H, Schmeisser A, Garlichs CD, et al. Angiotensin II-induced superoxide anion generation in human vascular endothelial cells: role of membrane-bound NADH-/NADPH-oxidases. Cardiovasc Res. 1999;44:215–22.
Haas MJ, Onstead-Haas L, Lee T, Torfah M, Mooradian AD. Angiotensin II receptor one (AT1) mediates dextrose induced endoplasmic reticulum stress and superoxide production in human coronary artery endothelial cells. Int J Cardiol. 2016;220:842–50.
Mooradian AD. Targeting select cellular stress pathways to prevent hyperglycemia-related complications: shifting the paradigm. Drugs. 2016;76:1081–91.
Cominacini L, Mozzini C, Garbin U, et al. Endoplasmic reticulum stress and Nrf2 signaling in cardiovascular diseases. Free Radic Biol Med. 2015;88(Pt B):233–242.
Myoishi M, Hao H, Minamino T, et al. Increased endoplasmic reticulum stress in atherosclerotic plaques associated with acute coronary syndrome. Circulation. 2007;116:1226–33.
Buchwald H, Varco RL, Matts JP, et al. Effect of partial ileal bypass surgery on mortality and morbidity from coronary heart disease in patients with hypercholesterolemia. Report of the Program on the Surgical Control of the Hyperlipidemias (POSCH). N Engl J Med. 1990;323:946–55.
Cholesterol Treatment Trialists’ (CTT) Collaborators. Efficacy of cholesterol-lowering therapy in 18,686 people with diabetes in 14 randomized trials of statins: a meta-analysis. Lancet. 2008;371:117–125.
HPS2-THRIVE Collaborative Group, Landray MJ, Haynes R, Hopewell JC, et al. Effects of extended-release niacin with laropiprant in high-risk patients. N Engl J Med. 2014;371:203–212.
The AIM-HIGH Investigators, Boden WE, Probstfield JL, Anderson T, et al. Niacin in patients with low HDL cholesterol levels receiving intensive statin therapy. N Engl J Med. 2011;365:2255–67.
Cannon CP, Blazing MA, Giugliano RP, et al. Ezetimibe added to statin therapy after acute coronary syndromes. N Engl J Med. 2015;372:2387–97.
Egom EE. Ezetimibe plus a statin after acute coronary syndromes. N Engl J Med. 2015;373:1474.
Yamaoka-Tojo M, Tojo T, Takahira N, Masuda T, Izumi T. Ezetimibe and reactive oxygen species. Curr Vasc Pharmacol. 2011;9:109–20.
Pesaro AE, Serrano CV Jr, Fernandes JL, et al. Pleiotropic effects of ezetimibe/simvastatin vs. high dose simvastatin. Int J Cardiol. 2012;158:400–4.
Kater AL, Batista MC, Ferreira SR. Synergistic effect of simvastatin and ezetimibe on lipid and pro-inflammatory profiles in pre-diabetic subjects. Diabetol Metab Syndr. 2010;2:34.
Blom DJ, Hala T, Bolognese M, et al. A 52-week placebo-controlled trial of evolocumab in hyperlipidemia. N Engl J Med. 2014;370:1809–19.
Robinson JG, Farnier M, Krempf M, et al. Efficacy and safety of alirocumab in reducing lipids and cardiovascular events. N Engl J Med. 2015;372:1489–99.
Laufs U, Marra D, Node K, Liao JK. 3-Hydroxy-3-methylglutaryl-CoA reductase inhibitors attenuate vascular smooth muscle proliferation by preventing Rho GTPase-induced down-regulation of p27Kip1. J Biol Chem. 1999;274:21926–31.
Laufs U, Liao JK. Post-transcriptional regulation of endothelial nitric oxide synthase mRNA stability by Rho GTPase. J Biol Chem. 1998;273:24266–71.
Wassmann S, Laufs U, Bäumer AT, et al. HMG-CoA reductase inhibitors improve endothelial dysfunction in normocholesterolemic hypertension via reduced production of reactive oxygen species. Hypertension. 2001;37:1450–7.
Wassmann S, Laufs U, Müller K, et al. Cellular antioxidant effects of atorvastatin in vitro and in vivo. Arterioscler Thromb Vasc Biol. 2002;22:300–5.
DiNicolantonio JJ, Fares H, Niazi AK, et al. β-Blockers in hypertension, diabetes, heart failure and acute myocardial infarction: a review of the literature. Open Heart. 2015;2(1):e000230.
Winchester DE, Pepine CJ. Usefulness of beta blockade in contemporary management of patients with stable coronary heart disease. Am J Cardiol. 2014;114:1607–12.
Malhotra S, Das MK. Delayed and indirect effects of antiarrhythmic drugs in reducing sudden cardiac death. Future Cardiol. 2011;7:203–17.
Opie LH, Yusuf S, Kübler W. Current status of safety and efficacy of calcium channel blockers in cardiovascular diseases: a critical analysis based on 100 studies. Prog Cardiovasc Dis. 2000;43:171–96.
Godfraind TJ. Calcium channel blockers in cardiovascular pharmacotherapy. Cardiovasc Pharmacol Ther. 2014;19:501–15.
Swedberg K, Komajda M, Böhm M, et al. Ivabradine and outcomes in chronic heart failure (SHIFT): a randomised placebo-controlled study. Lancet. 2010;376:875–85.
Fox K, Ford I, Steg PG, Tardif JC, Tendera M, Ferrari R, SIGNIFY Investigators. Ivabradine in stable coronary artery disease without clinical heart failure. N Engl J Med. 2014;371:1091–9.
Ohman EM, Alexander KP. The challenges with chronic angina. N Engl J Med. 2014;371:1152–3.
Turan B. A comparative summary on antioxidant-like actions of timolol with other antioxidants in diabetic cardiomyopathy. Curr Drug Deliv. 2016;13:418–23.
Obadah M, Al Chekakie AI. Traditional heart failure medications and sudden cardiac death prevention: a review. J Cardiovas Pharmacol Therap. 2012;18:412–26.
Bender SB, Jia G, Sowers JR. Mineralocorticoid receptors: an appealing target to treat coronary microvascular dysfunction in diabetes. Diabetes. 2015;64:3–5.
Garg R, Rao AD, Baimas-George M, et al. Mineralocorticoid receptor blockade improves coronary microvascular function in individuals with type 2 diabetes. Diabetes. 2015;64:236–42.
Reboldi G, Angeli F, Cavallini C, Gentile G, Mancia G, Verdecchia P. Comparison between angiotensin-converting enzyme inhibitors and angiotensin receptor blockers on the risk of myocardial infarction, stroke and death: a meta-analysis. J Hypertens. 2008;26:1282–9.
Dagenais GR, Pogue J, Fox K, Simoons ML, Yusuf S. Angiotensin-converting-enzyme inhibitors in stable vascular disease without left ventricular systolic dysfunction or heart failure: a combined analysis of three trials. Lancet. 2006;368:581–8.
Zheng Z, Chen H, Ke G, et al. Protective effect of perindopril on diabetic retinopathy is associated with decreased vascular endothelial growth factor–to–pigment epithelium–derived factor ratio. Involvement of a mitochondria–reactive oxygen species pathway. Diabetes. 2009;58:954–64.
Lv J, Perkovic V, Foote CV, Craig ME, Craig JC, Strippoli GF. Antihypertensive agents for preventing diabetic kidney disease. Cochrane Database Syst Rev. 2012;12:CD004136.
Dhakarwal P, Agrawal V, Kumar A, Goli KM, Agrawal V. Update on role of direct renin inhibitor in diabetic kidney disease. Ren Fail. 2014;36:963–9.
Parviz Y, Iqbal J, Pitt B, Adlam D, Al-Mohammad A, Zannad F. Emerging cardiovascular indications of mineralocorticoid receptor antagonists. Trends Endocrinol Metab. 2015;26:201–11.
Pitt B, Zannad F, Remme WJ, et al. The effect of spironolactone on morbidity and mortality in patients with severe heart failure. Randomized Aldactone Evaluation Study Investigators. N Engl J Med. 1999;341:709–17.
Pitt B, Remme W, Zannad F, Eplerenone Post-Acute Myocardial Infarction Heart Failure Efficacy and Survival Study Investigators, et al. Eplerenone, a selective aldosterone blocker, in patients with left ventricular dysfunction after myocardial infarction. N Engl J Med. 2003;348:1309–21.
McMurray JJ, Krum H, Abraham WT, et al. Aliskiren, enalapril, or aliskiren and enalapril in heart failure. N Engl J Med. 2016;374:1521–32.
Lin C, Zhang Q, Zhang H, Lin A. Long-term effects of low-dose spironolactone on chronic dialysis patients: a randomized placebo-controlled study. J Clin Hypertens. 2016;18:121–8.
Pilgrim T, Windecker S. Antiplatelet therapy for secondary prevention of coronary artery disease. Heart. 2014;100:1750–6.
Cheng JW. Updates in antiplatelet agents used in cardiovascular diseases. J Cardiovasc Pharmacol Ther. 2013;18:514–24.
Palacio S, Hart RG, Pearce LA, Benavente OR. Effect of addition of clopidogrel to aspirin on mortality: systematic review of randomized trials. Stroke. 2012;43:2157–62.
Schnorbus B, Daiber A, Jurk K, et al. Effects of clopidogrel, prasugrel and ticagrelor on endothelial function, inflammatory and oxidative stress parameters and platelet function in patients undergoing coronary artery stenting for an acute coronary syndrome. A randomised, prospective, controlled study. BMJ Open. 2014;4:e005268.
Gawron-Skarbek A, Chrzczanowicz J, Kostka J, et al. Factors determining the total serum antioxidant capacity in men with coronary heart disease–the powerful effect of treatment with thienopyridines. Nutr Metab Cardiovasc Dis. 2014;24:e21–3.
Heitzer T, Rudolph V, Schwedhelm E, et al. Clopidogrel improves systemic endothelial nitric oxide bioavailability in patients with coronary artery disease: evidence for antioxidant and antiinflammatory effects. Arterioscler Thromb Vasc Biol. 2006;26:1648–52.
Hawley SA, Fullerton MD, Ross FA, et al. The ancient drug salicylate directly activates AMP-activated protein kinase. Science. 2012;336:918–22.
Yang H, Zhao P, Tian S. Clopidogrel protects endothelium by hindering TNFα-induced VCAM-1 expression through CaMKKβ/AMPK/Nrf2 pathway. J Diabetes Res. 2016;2016:9128050.
Hadi NR, Mohammad BI, Ajeena IM, Sahib HH. Antiatherosclerotic potential of clopidogrel: antioxidant and anti-inflammatory approaches. BioMed Res Int. 2013;2013:790263.
Hattori Y, Hattori K, Hayashi T. Pleiotropic benefits of metformin: Macrophage targeting its anti-inflammatory mechanisms. Diabetes. 2015;16:1907–9.
Batandier C, Guigas B, Detaille D, et al. The ROS production induced by a reverse-electron flux at respiratory-chain complex 1 is hampered by metformin. J Bioenerg Biomembr. 2006;38:33–42.
Hirsch HA, Iliopoulos D, Struhl K. Metformin inhibits the inflammatory response associated with cellular transformation and cancer stem cell growth. Proc Natl Acad Sci. 2013;110:972–7.
Shang F, Zhang J, Li Z, et al. Cardiovascular protective effect of metformin and telmisartan: reduction of PARP1 activity via the AMPK-PARP1 cascade. PLoS One. 2016;11(3):e0151845.
de Zeeuw D, Akizawa T, Audhya P, et al. Bardoxolone methyl in type 2 diabetes and stage 4 chronic kidney disease. N Engl J Med. 2013;369:2492–503.
Chen T, Jin X, Crawford BH, et al. Cardioprotection from oxidative stress in the newborn heart by activation of PPARγ is mediated by catalase. Free Radic Biol Med. 2012;53:208–15.
Mizoguchi M, Tahara N, Tahara A, et al. Pioglitazone attenuates atherosclerotic plaque inflammation in patients with impaired glucose tolerance or diabetes a prospective, randomized, comparator-controlled study using serial FDG PET/CT imaging study of carotid artery and ascending aorta. JACC Cardiovasc Imaging. 2011;4:1110–8.
Kernan WN, Viscoli CM, Furie KL, et al. Pioglitazone after Ischemic Stroke or Transient Ischemic Attack. N Engl J Med. 2016;374:1321–31.
PROactive (Prospective Pioglitazone Clinical Trial in Macrovascular Events), Dormandy JA, Charbonnel B, Eckland DJ, et al. Secondary prevention of macrovascular events in patients with type 2 diabetes in the PROactive Study (PROspective pioglitAzone Clinical Trial In macroVascular Events): a randomised controlled trial. Lancet. 2005;366:1279–1289.
Wanner C, Inzucchi SE, Lachin JM, For the EMPA-REG OUTCOME Investigators, et al. Empagliflozin and progression of kidney disease in type 2 diabetes. N Engl J Med. 2016;375:323–334.
Marso SP, Daniels GH, Brown-Frandsen K, et al. Liraglutide and cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2016;375:311–22.
Ojima A, Matsui T, Nishino Y, Nakamura N, Yamagishi S. Empagliflozin, an inhibitor of sodium-glucose cotransporter 2 exerts anti-inflammatory and antifibrotic effects on experimental diabetic nephropathy partly by suppressing AGEs-receptor axis. Horm Metab Res. 2015;47:686–92.
Oelze M, Kröller-Schön S, Welschof P, et al. The sodium-glucose co-transporter 2 inhibitor empagliflozin improves diabetes-induced vascular dysfunction in the streptozotocin diabetes rat model by interfering with oxidative stress and glucotoxicity. PLoS One. 2014;9:e112394.
Inoue T, Inoguchi T, Sonoda N, et al. GLP-1 analog liraglutide protects against cardiac steatosis, oxidative stress and apoptosis in streptozotocin-induced diabetic rats. Atherosclerosis. 2015;240:250–9.
Rizzo M, Abate N, Chandalia M, et al. Liraglutide reduces oxidative stress and restores heme oxygenase-1 and ghrelin levels in patients with type 2 diabetes: a prospective pilot study. J Clin Endocrinol Metab. 2015;100:603–6.
Balestrieri ML, Rizzo MR, Barbieri M, et al. Sirtuin 6 expression and inflammatory activity in diabetic atherosclerotic plaques: effects of incretin treatment. Diabetes. 2015;64:1395–406.
Batchuluun B, Inoguchi T, Sonoda N, et al. Metformin and liraglutide ameliorate high glucose-induced oxidative stress via inhibition of PKC-NAD(P)H oxidase pathway in human aortic endothelial cells. Atherosclerosis. 2014;232:156–64.
Shiraki A, Oyama J, Komoda H, et al. The glucagon-like peptide 1 analog liraglutide reduces TNF-α-induced oxidative stress and inflammation in endothelial cells. Atherosclerosis. 2012;221:375–82.
Shimoda M, Kanda Y, Hamamoto S, et al. The human glucagon-like peptide-1 analogue liraglutide preserves pancreatic beta cells via regulation of cell kinetics and suppression of oxidative and endoplasmic reticulum stress in a mouse model of diabetes. Diabetologia. 2011;54:1098–108.
Pfeffer MA, Claggett B, Diaz R, et al. Lixisenatide in patients with type 2 diabetes and acute coronary syndrome. N Engl J Med. 2015;373:2247–57.
White WB, Cannon CP, Heller SR, et al. Alogliptin after acute coronary syndrome in patients with type 2 diabetes. N Engl J Med. 2013;369:1327–35.
Scirica BM, Bhatt DL, Braunwald E, et al. Saxagliptin and cardiovascular outcomes in patients with type 2 diabetes mellitus. N Engl J Med. 2013;369:1317–26.
Green JB, Bethel MA, Armstrong PW, et al. Effect of sitagliptin on cardiovascular outcomes in type 2 diabetes. N Engl J Med. 2015;373:232–42.
Smith RJ, Goldfine AB, Hiatt WR. Evaluating the cardiovascular safety of new medications for type 2 diabetes: time to reassess? Diabetes Care. 2016;39:738–42.
Elzer JG, Muhammad S, Wintermantel TM, et al. Neuronal estrogen receptor-alpha mediates neuroprotection by 17-beta estradiol. J Cereb Blood Flow Metab. 2010;30:935–42.
Kaunitz AM, Manson JE. Management of menopausal symptoms. Obstet Gynecol. 2015;126:859–76.
Akishita M, Hashimoto M, Ohike Y, et al. Low testosterone level as a predictor of cardiovascular events in Japanese men with coronary risk factors. Atherosclerosis. 2010;210:232–6.
Menke A, Guallar E, Rohrmann S, et al. Sex steroid hormone concentrations and risk of death in US men. Am J Epidemiol. 2010;171:583–92.
Manson JE, Chlebowski RT, Stefanick ML, et al. Menopausal hormone therapy and health outcomes during the intervention and extended poststopping phases of the Women’s Health Initiative randomized trials. JAMA. 2013;310:1353–68.
Schierbeck LL, Rejnmark L, Tofteng CL, et al. Effect of hormone replacement therapy on cardiovascular events in recently postmenopausal women: randomised trial. BMJ. 2012;345:e6409.
Hodis HN, Mack WJ, Henderson VW, For the ELITE Research Group, et al. Vascular effects of early versus late postmenopausal treatment with estradiol. N Engl J Med. 2016;374:1221–1231.
Strehlow K, Rotter S, Wassmann S, et al. Modulation of antioxidant enzyme expression and function by estrogen. Circ Res. 2003;93:170–7.
Song JY, Kim MJ, Jo HH, et al. Antioxidant effect of estrogen on bovine aortic endothelial cells. J Steroid Biochem Mol Biol. 2009;117:74–80.
Haas MJ, Raheja P, Jaimungal S, Sheikh-Ali M, Mooradian AD. Estrogen-dependent inhibition of dextrose-induced endoplasmic reticulum stress and superoxide generation in endothelial cell. Free Radic Biol Med. 2012;52:2161–7.
Mooradian AD. Antioxidant properties of steroids. J Steroid Biochem Mol Biol. 1993;45:509–11.
Duchatelle V, Kritikou EA, Tardif JC. Clinical value of drugs targeting inflammation for the management of coronary artery disease. Can J Cardiol. 2012;28:678–86.
Ridker PM, Lüscher TF. Anti-inflammatory therapies for cardiovascular disease. Eur Heart J. 2014;35:1782–91.
Bäck M, Hansson GK. Anti-inflammatory therapies for atherosclerosis. Nat Rev Cardiol. 2015;12:199–211.
Khan R, Spagnoli V, Tardif JC, L’Allier PL. Novel anti-inflammatory therapies for the treatment of atherosclerosis. Atherosclerosis. 2015;240:497–509.
Adameova A, Xu YJ, Duhamel TA, Tappia PS, Shan L, Dhalla NS. Anti-atherosclerotic molecules targeting oxidative stress and inflammation. Curr Pharm Des. 2009;15:3094–107.
Probst BL, Trevino I, McCauley L, et al. RTA 408, a novel synthetic triterpenoid with broad anticancer and anti-inflammatory activity. PLoS One. 2015;10(4):e0122942.
Chartoumpekis DV, Sykiotis GP. Bardoxolone methyl in type 2 diabetes and advanced chronic kidney disease. N Engl J Med. 2014;370:1767.
Tardif JC, McMurray JJ, Klug E, et al. Effects of succinobucol (AGI-1067) after an acute coronary syndrome: a randomised, double-blind, placebo-controlled trial. Lancet. 2008;371:1761–8.
Tardif JC, Gregoire J, L’Allier PL, et al. Effects of the antioxidant succinobucol (AGI-1067) on human atherosclerosis in a randomized clinical trial. Atherosclerosis. 2008;197:480–6.
Robertson S, Martinez GJ, Payet CA, et al. Colchicine therapy in acute coronary syndrome patients acts on caspase-1 to suppress NLRP3 inflammasome monocyte activation. J Am Heart Assoc. 2015;4:e002128.
Martínez GJ, Robertson S, Barraclough J, et al. Colchicine acutely suppresses local cardiac production of inflammatory cytokines in patients with an acute coronary syndrome. J Am Heart Assoc. 2015;4(8):e002128.
Tousoulis D, Oikonomou E, Economou EK, Crea F, Kaski JC. Inflammatory cytokines in atherosclerosis: current therapeutic approaches. Eur Heart J. 2016;37:1723–32.
Perez-Gomez MV, Sanchez-Niño MD, Sanz AB, et al. Horizon 2020 in diabetic kidney disease: the clinical trial pipeline for add-on therapies on top of renin angiotensin system blockade. J Clin Med. 2015;4:1325–47.
Sager HB, Heidt T, Hulsmans M, et al. Targeting interleukin-1β reduces leukocyte production after acute myocardial infarction. Circulation. 2015;132:1880–90.
Ridker PM, Thuren T, Zalewski A, Libby P. Interleukin-1beta inhibition and the prevention of recurrent cardiovascular events: rationale and design of the Canakinumab Anti-inflammatory Thrombosis Outcomes Study (CANTOS). Am Heart J. 2011;162:597–605.
Samuelsson B, Dahlen SE, Lindgren JA, Rouzer CA, Serhan CN. Leukotrienes and lipoxins: structures, biosynthesis, and biological effects. Science. 1987;237:1171–6.
Tardif JC, L’allier PL, Ibrahim R, et al. Treatment with 5-lipoxygenase inhibitor VIA-releuton) in patients with recent acute coronary syndrome. Circ Cardiovasc Imaging. 2010;3:298–307.
Gaztanaga J, Farkouh M, Rudd JH, et al. A phase 2 randomized, double-blind, placebo-controlled study of the effect of VIA-2291, a 5-lipoxygenase inhibitor, on vascular inflammation in patients after an acute coronary syndrome. Atherosclerosis. 2015;240:53–60.
Suckling KE. Phospholipase A2 inhibitors in the treatment of atherosclerosis: a new approach moves forward in the clinic. Expert Opin Investig Drugs. 2009;18:1425–30.
Ferri N, Ricci C, Corsini A. Pharmacological inhibition of phosholipase A2: Results from phase 3 clinical trials with darapladib and varespladib in patients with cardiovascular disease. Cardiol Pharmacol. 2015;4:137. doi:10.4172/2329-6607.1000137.
Nicholls SJ, Kastelein JJ, Schwartz GG, Bash D, Rosenson RS, et al. Varespladib and cardiovascular events in patients with an acute coronary syndrome: the VISTA-16 randomized clinical trial. JAMA. 2014;311:252–62.
STABILITY Investigators, White HD, Held C, Stewart R, et al. Darapladib for preventing ischemic events in stable coronary heart disease. N Engl J Med. 2014;370:1702–1711.
O’Donoghue ML, Braunwald E, White HD, et al. Effect of darapladib on major coronary events after an acute coronary syndrome: the SOLID-TIMI 52 randomized clinical trial. JAMA. 2014;312:1006–15.
Tardif JC, Tanguay JF, Wright SS, et al. Effects of the P-selectin antagonist inclacumab on myocardial damage after percutaneous coronary intervention for non-ST-segment elevation myocardial infarction: results of the SELECT-ACS trial. J Am Coll Cardiol. 2013;61:2048–55.
Stähli BE, Tardif JC, Carrier M, et al. Effects of P-selectin antagonist inclacumab in patients undergoing coronary artery bypass graft surgery: SELECT-CABG Trial. J Am Coll Cardiol. 2016;67:344–6.
Tardif JC, L’Allier PL, Grégoire J, et al. A randomized controlled, phase 2 trial of the viral serpin Serp-1 in patients with acute coronary syndromes undergoing percutaneous coronary intervention. Circ Cardiovasc Interv. 2010;3:543–8.
Rouch A, Vanucci-Bacqué C, Bedos-Belval F, Baltas M. Small molecules inhibitors of plasminogen activator inhibitor-1 - an overview. Eur J Med Chem. 2015;92:619–36.
Blot WJ, Li JY, Taylor PR, et al. Nutrition intervention trials in Linxian, China: supplementation with specific vitamin/mineral combinations, cancer incidence, and disease specific mortality in the general population. J Natl Cancer Inst. 1993;85:1483–92.
ATBC (Alpha-Tocopherol, Beta Carotene) Cancer Prevention Study Group. The effect of vitamin E and beta carotene on the incidence of lung cancer and other cancers in male smokers. The Alpha Tocopherol, Beta Carotene Cancer Prevention Study Group. N Engl J Med. 1994;330:1029–1035.
Stephens NG, Parsons A, Schofield PM, et al. Randomized, controlled trial of vitamin E in patients with coronary disease: Cambridge Heart Antioxidant Study. Lancet. 1996;347:781–6.
Hennekens CH, Buring JE, Manson JE, et al. Lack of effect of long-term supplementation with beta carotene on the incidence of malignant neoplasms and cardiovascular disease. N Engl J Med. 1996;334:1145–9.
Omenn GS, Goodman GE, Thornquist MD, et al. Risk factors for lung cancer and for intervention effects in CARET: the Beta Carotene and Retinol Efficacy Trial. J Natl Cancer Inst. 1996;88:1550–9.
GISSI-Prevenzione Investigators. Dietary supplements with n-3 poly unsaturated fatty acids and vitamin E after myocardial infarction: results of the GISSI-Prevention Trial. Lancet. 1999;354:447–455.
Yusuf S, Dagenais G, Pogue J, et al. Vitamin E supplementation and cardiovascular events in high-risk patients. The Heart Outcomes Prevention Evaluation Study Investigators. N Engl J Med. 2000;342:154–60.
Collaborative Group of the Primary Prevention Project. Low dose aspirin and vitamin E in people at cardiovascular risk: a randomized trial in general practice. Lancet. 2001;357:89–95.
Heart Protection Study Collaborative Group. MRC/BHF Heart Protection Study of antioxidant vitamin supplementation in 20,536 high-risk individuals: a randomised placebo-controlled trial. Lancet. 2002;360:23–33.
Lee IM, Cook NR, Gaziano JM, et al. Vitamin E in the primary prevention of cardiovascular disease and cancer: the Women’s Health Study: a randomized controlled trial. JAMA. 2005;294:56–65.
Cook NR, Albert CM, Gaziano JM, et al. A randomized factorial trial of vitamins C and E and beta carotene in the secondary prevention of cardiovascular events in women: results from the Women’s Antioxidant Cardiovascular Study. Arch Intern Med. 2007;167:1610–8.
Sesso HD, Buring JE, Christen WG, et al. Vitamins E and C in the prevention of cardiovascular disease in men: the Physicians’ Health Study II randomized controlled trial. JAMA. 2008;300:2123–33.
Sheikh-Ali M, Chehade JM, Mooradian AD. The antioxidant paradox in diabetes mellitus. Am J Ther. 2011;18:266–78.
Mooradian AD, Haas MJ. Glucose-induced endoplasmic reticulum stress is independent of oxidative stress: a mechanistic explanation for the failure of antioxidant therapy in diabetes. Free Radic Biol Med. 2011;50:1140–3.
Mooradian AD, Onstead-Haas L, Haas MJ. Asymmetrical cross-talk between the endoplasmic reticulum stress and oxidative stress caused by dextrose. Life Sci. 2016;144:37–48.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Funding
No sources of funding were used to conduct this study or prepare this review.
Conflict of interest
Arshag D. Mooradian has no conflicts of interests that are directly relevant to the content of this review.
Rights and permissions
About this article
Cite this article
Mooradian, A.D. Therapeutic Targeting of Cellular Stress to Prevent Cardiovascular Disease: A Review of the Evidence. Am J Cardiovasc Drugs 17, 83–95 (2017). https://doi.org/10.1007/s40256-016-0199-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40256-016-0199-7