Abstract
Glioblastoma (GBM) is the most common malignant primary brain tumor, with poor survival despite treatment with surgery, radiotherapy, and chemotherapy with temozolomide. Little progress has been made over the last two decades, and there remain unmet medical needs. Approximately 45% of patients with GBM carry EGFR mutations, and 13% of them possess altered PDGFR genes. Moreover, VEGF/VEGFR mutations are also observed in the patient population. Tyrosine kinase inhibitors (TKIs) are emerging cancer therapy drugs that inhibit signal transduction cascades affecting cell proliferation, migration, and angiogenesis. Indications for small molecule TKIs have been successfully expanded to multiple types of cancer; however, none of the TKIs have been approved for patients with GBM. In this review, we summarize clinical trials of small molecule TKIs in patients with GBM and plausible hypotheses for negative clinical study results. We also discuss the potential TKI candidates that presented significant preclinical outcomes in patients with GBM.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glioblastoma (GBM) is the most common primary malignant brain tumor in adults, despite progress in current treatment approaches, prognosis remains poor. Hereditary factors relevant to GBM are not yet fully understood; receptor tyrosine kinase (RTK) signaling pathway is one of three major pathways involved in GBM. According to a retrospective biospecimen study of the Cancer Genome Atlas, mutations in epidermal growth factor receptor (EGFR)—an RTK—were observed in 45% of the samples (Cancer Genome Atlas Research 2008). Dysregulation of EGFR has also been identified in other types of cancer such as non-small-cell lung cancer, renal cancer, and colon cancer (Yewale et al. 2013). In addition to dysregulation of EGFR, aberrations in platelet-derived growth factor receptor α (PDGFRA) and mutations in vascular endothelial growth factor (VEGF)/VEGF receptor (VEGFR) are also frequently found in patients with GBM. According to the retrospective biospecimen study of the Cancer Genome Atlas, 13% of abnormalities were found in PDGFRA. Furthermore, as GBM is a solid tumor highly dependent on angiogenesis, aberrant tumor vascular network and augmented VEGF expression are observed in patients (Reardon et al. 2008).
As small molecule drugs, tyrosine kinase inhibitors (TKIs) constitute a majority of approved agents for several cancer types. Tyrosine kinase inhibitors work by blocking the receptor signaling, eventually inhibiting cell growth, proliferation, differentiation, and angiogenesis (Arora and Scholar 2005). Figure 1 below shows how a TKI regulates the cell cycle and acts as an inhibitor.
Current treatment of GBM includes surgical resection followed by radiation therapy (RT) and temozolomide (TMZ) administration. The standard of care using TMZ significantly increases the median overall survival for patients with GBM by 2.5 months (median overall survival 12.1 months with RT alone vs. 14.6 months with RT plus TMZ), but the median overall survival remains considerably shorter than that in other types of cancer (Stupp et al. 2005). Tumor recurrence and therapeutic resistance after surgery are the main reasons for poor prognosis. Temozolomide has been a part of standard treatment for patients with newly diagnosed GBM since its first approval in the United States in 1999. However, no other drugs have replaced TMZ for newly diagnosed GBM because most drugs have failed to show efficacy in numerous clinical trials. Therefore, developing new drugs other than TMZ for GBM is crucial considering the limited life expectancy of patients with GBM. Small molecule TKIs are recognized as powerful candidates for treating GBM because they block cell signaling pathways such as EGFR, PDGFR, and VEGF/VEGFR. Moreover, small molecule TKIs are usually more affordable and place less financial burden on patients than biological drugs. Tyrosine kinase inhibitors are also more accessible than biological drugs as most TKIs are available as orally administered drugs, whereas biological drugs are not. The present review discusses small molecule TKIs with expanded indications, clinical trial status of TKIs in patients with GBM, and potential TKI candidates for GBM that have shown remarkable preclinical trial results.
Expanded indications for TKIs
As TK plays various roles in the life cycle of cells, many TKIs are used in multiple types of cancer, and it is common to expand indications for TKIs. Small molecule TKIs with expanded indications are summarized in Table 1.
Imatinib (known as Gleevec®)—called as the “magic bullet”—is one of the most revolutionary drugs; it was first approved as a drug for treating chronic myeloid leukemia by the FDA in 2001. Chronic myeloid leukemia results from a reciprocal translocation between chromosomes 9 and 22 (“Philadelphia chromosome” or “Philadelphia translocation”). This chromosome is unusually short and contains a fusion gene called BCR-ABL. The advent of imatinib—an inhibitor of BCR-ABL—rapidly and dramatically modified the treatment of chronic myeloid leukemia and led to important changes in anti-cancer management.
Gastrointestinal stromal tumors (GISTs) are known as the most common mesenchymal tumors of the gastrointestinal system with an approximate incidence of 10–15 cases per million worldwide (Soreide et al. 2016). Gastrointestinal stromal tumors were considered life threatening owing to their poor response to chemotherapy and RT, until the discovery of activated KIT (CD117) and PDGFRA mutations in 1998 (Mei et al. 2018). Mutations in both receptors lead to dysregulation of downstream intracellular signaling pathways, eventually leading to tumorigenesis. However, structural homology among ABL kinase, KIT, and PDGFRA accelerated the introduction of imatinib in GIST treatment (Mei et al. 2018). Clinical trials in patients with GIST were encouraging, and in 2002, imatinib was approved by the FDA for the treatment of malignant metastatic and/or unresectable GISTs (Dagher et al. 2002). Today, 85–90% of patients with GIST harboring KIT or PDGFRA mutations benefit from imatinib after or before surgery.
Sunitinib (marketed as Sutent®) is an inhibitor of multiple RTKs including VEGFR type 1 and 2 (FLT1 and FLK1/KDR), PDGFR-α and PDGFR-β and the stem cell factor c-KIT receptor. Thus, it is not surprising that sunitinib was the first to be approved as a treatment of renal cell carcinoma, an extremely angiogenesis-dependent cancer (Rizzo and Porta 2017). Furthermore, sunitinib was also approved by the FDA for the treatment of GIST after disease progression or imatinib intolerance. Sunitinib was the first cancer drug to be simultaneously approved for two different indications in 2006.
In 2011, a multinational, randomized, double-blind, placebo-controlled phase III trial of sunitinib showed impressive results in 171 patients with neuroendocrine pancreatic tumors. The median progression-free survival (PFS) values for the sunitinib and placebo arms were 10.2 months and 5.4 months, respectively. Moreover, progression-free survival, overall survival, and objective response rate for sunitinib were also higher than those for the placebo (Raymond et al. 2011). Based on this clinical study, the FDA approved the expanded indications for sunitinib toward progressive neuroendocrine pancreatic cancer that cannot be removed by surgery or that is metastatic.
Unsuccessful clinical study outcomes with tyrosine kinase inhibitors
Owing to the broad availability of TKIs for multiple types of cancer, numerous clinical trials have been conducted for GBM, but no TKI has been approved for GBM until now. Table 2 summarizes negative clinical trials of TKIs for GBM.
Details about the clinical trials presented in Table 2 (except the Imatinib phase II study; CST1571BGR03 and the Gefitinib phase II study; 1839IL/0116) were retrieved from clinicalTrials.gov, a web-based resource that provides researchers with easy access to publicly available information. The website is maintained by the National Library of Medicine at the National Institutes of Health, but it does not contain information about all the clinical studies conducted in the United States because not all studies are required by law to be registered. However, the rate of study registration has increased over time as more policies and laws requiring registration have been enacted and as more sponsors and investigators have voluntarily registered their clinical studies. Information about clinical trials of TKIs was filtered by the disease “Glioblastoma (GBM)” first; then, the results were re-filtered with the recruitment status “completed” or “terminated”.
All drugs in Table 2 are TKIs, but they can be classified into specific categories on the basis of their targets. Imatinib inhibits ABL, BCR-ABL, PDGFRA, and c-KIT (Iqbal and Iqbal 2014). Dasatinib is an inhibitor of multiple targets such as BCR-ABL, c-KIT, PDGFR-β, and ephrin receptor (Lassman et al. 2015). Vandetanib also inhibits multiple targets such as EGFR, VEGFR2, RET(rearranged during transfection)-tyrosine kinase, Protein tyrosine kinase 6, TIE2, EPH kinase receptor, and Src kinase receptor (Jeong et al. 2013; Lee et al. 2015).
Among the TKIs presented in Table 2, erlotinib, gefitinib, and afatinib have received extensive attention as EGFR TKIs because EGFR mutation is the most common type of mutation in patients with GBM. Erlotinib and gefitinib are classified as first-generation EGFR TKIs because they reversibly bind to only EGFR (Erb1), whereas afatinib is regarded as a second-generation TKI because it binds irreversibly to all ErbB family receptors. Clinical trials have been conducted with positive prospects in patients with glioblastoma multiforme because the TKIs showed positive clinical results in non-small cell lung cancer (NSCLC), which is also associated with EGFR mutations; however, all of them only showed limited efficacy in GBM. Recently, third-generation EGFR TKIs such as osimertinib (Tagrisso®), YH5448 (Lazertinib), and AZD3759 have been developed for NSCLC treatment. They have been tested only in preclinical studies for now; they will be discussed later.
Causes of negative clinical trial results are not yet clearly known, but several hypotheses are highly plausible. Drug concentrations in the sub-therapeutic range in the target organ—the brain—is the primary hypothesis. Altered EGFR signaling pathway is another plausible assumption. Another hypothesis is that the extensively heterogeneous cell types in GBM lead to limited efficacy with a single TKI. Lastly, a few TKIs present undesirable adverse effects during the studies. Detailed descriptions ensue.
Why are TKIs ineffective in GBM?
Restricted delivery of targeted agents across the blood brain barrier (BBB) is a critical cause of poor clinical trial results. Tyrosine kinase inhibitors must penetrate the brain; however, the BBB is a substantial obstacle to overcome. Most TKIs such as imatinib (Raymond et al. 2008), dasatinib (Schiff and Sarkaria 2015), vandetanib (Lee et al. 2015), and nintedanib (Muhic et al. 2013) are reported to be suitable substrates for P-glycoproteins, which are highly expressed in the capillary endothelial cells constituting BBB. They are also known to be substrates for breast cancer resistance protein (BCRP). P-glycoproteins and BCRP are both active efflux transporters that block absorption at the apical membrane of the BBB, and they pump drugs out of the cells.
The CYP3A4 enzyme-induced antiepileptic drug (EIAID) regimen frequently used for patients with GBM is reported to result in poor clinical trial outcomes. Drugs such as carbamazepine, phenytoin, and phenobarbital are enzyme-induced anticonvulsants drugs (EIACDs), which are often used for treating epilepsy in patients with GBM (Englot et al. 2016). As these EIACDs are inducers of cytochrome P450 isoenzyme CYP3A4, several TKIs mainly metabolized by CYP3A4 are significantly affected by EIACDs. Imatinib (Reardon et al. 2005), AEE788 (Reardon et al. 2012), gefitinib (Uhm et al. 2011), and lapatinib plus pazopanib (Iwamoto et al. 2010) are negatively affected by co-administration of EIACDs. It is plausible that substantially decreased plasma exposure of TKIs results in reduced plasma drug concentrations in the brain.
Adaptation to altered signaling pathways is another crucial reason for the negative clinical trial outcomes. Tyrosine kinase inhibitors selectively inhibit single or multiple receptor kinase targets; however, GBM cells may compensate by activating numerous TKs. Moreover, treatment with a single agent was not sufficient to completely block the cell signaling (Stommel et al. 2007). According to Muhic et al. (2013), glioma cells rely on other redundant pathways to support angiogenesis, as observed in several previous studies utilizing small molecule dual-VEGFR/PDGFR inhibitors (sunitinib, sorafenib, vatalanib, cediranib, and pazopanib). Thus, in future studies, it would be more effective to use TKIs in combination with agents that target downstream signaling components or reciprocal signaling components.
Unsuccessful clinical trials may also be attributed to the genetic heterogeneity of GBM. Glioblastoma cell growth is less dependent on a single oncogene (Brown et al. 2016); it shows intratumoral heterogeneity at the genetic and cellular level. Amplification of EGFR, MET and PDGFR are common in GBMs and these abnormalities differentially activate within GBM cell subpopulations (Snuderl et al. 2011). Therefore, further research combining appropriate targeted therapies using various TKIs is needed.
A few severe adverse effects were observed in the studies, which were not negligible. In a clinical study with AEE788, 28% of patients discontinued treatment because of adverse effects such as grade 3/4 aspartate aminotransferase or alanine aminotransferase elevation and bilirubin elevation (Reardon et al. 2012). Eventually, this study was prematurely terminated by the sponsor. Clinical research with dovitinib was discontinued in all patients owing to the unacceptable toxicities—including lipid abnormalities, AST/ALT elevation and thrombocytopenia—observed in 33% of participants (Sharma et al. 2019). A trial with erlotinib showed an unacceptably high number of deaths prompting early closure of the study. Four deaths occurred during the study, and three deaths were definitely related to the treatment: two patients developed refractory bone marrow aplasia and one developed pneumocystis carinii pneumonia, as confirmed by bronchoscopy (Peereboom et al. 2010).
Ongoing clinical trials in USA and South Korea
Despite the high clinical trial failure rates of TKIs, considerable effort is directed toward expanding the indications of many other TKIs. Global pharmaceutical companies perform several clinical trials of those TKIs for GBM. Current clinical trials in USA involving small molecule TKIs for GBM are summarized in Table 3. Ongoing clinical trials using TKIs in patients with GBM in South Korea are reviewed in Table 4.
Information about current clinical trials in South Korea is not integrated; therefore, this review was drafted by exploring three separate websites: Korea Clinical trials information center (K-CLIC, https://www.koreaclinicaltrials.org/), Integrated drug safety information system of the Ministry of Food and Drug Safety (https://nedrug.mfds.go.kr/) and Clinical Research Information Service (CRIS, https://cris.nih.go.kr/cris/). Information about clinical trials was first filtered by the keyword “Glioblastoma” or “brain tumor” in the subject, and the information was re-filtered to ensure that the clinical trials included TKIs.
Approximately 23 clinical trials were first screened using the keyword “Glioblastoma” or “Brain tumor”; however, only two clinical trials remained at the end. This is because most of the ongoing clinical trials in South Korea comprise biologicals such as monoclonal antibody and immune cell therapy.
Lenvatinib (known as Lenvima®) was previously mentioned in Table 1 as it expanded indications from differentiated thyroid cancer to advanced renal cell carcinoma and unresectable hepatocellular carcinoma. Lenvatinib acts as a multiple kinase inhibitor against VEGFR1, 2, and 3 as well as FGFR1, 2, 3, and 4 and PDGFR-alpha. Its sponsor Merck Sharp & Dohme Corp. and collaborator Eisai Inc. are currently recruiting worldwide patients with conditions such as GBM, triple negative breast cancer, and ovarian cancer, to determine the safety and efficacy of lenvatinib (Lenvima®) plus pembrolizumab (Keytruda®). The ClinicalTrials.gov identifier number of the trial is NCT03797326, and it is also known as LEAP-005. The estimated enrollment number of patients is 180, and 16 patients will be enrolled in South Korea. The predicted primary completion date of this study is April 11, 2022.
Buparlisib (BKM-120) is an investigational drug and works as a pan-class I phosphoinositide 3-kinase inhibitor. This clinical trial targets patients with recurrent GBM using buparlisib plus carboplatin or lomustine. The estimated enrollment number of patients is 140, and 5 patients will be enrolled in South Korea.
Promising preclinical trials—every dark cloud has a silver lining
Because GBM is a rare disease, there have been more trials to expand the indications of a drug from brain metastases to GBM than trials to test a drug that only targets GBM. According to the Central Brain Tumor Registry of the United States, the incidence rate of GBM is 3.21 per 100,000 people in USA (Ostrom et al. 2018), whereas that in South Korea is 1.26 per 100,000 (Yun et al. 2019). The accurate incidence of brain metastases is unknown because of methodological limitations of population, hospital, and autopsy studies; it is estimated to be approximately 10 per 100,000 (Stelzer 2013), which is considerably higher than the incidence of primary GBM. Lung cancer and breast cancer are the most common sources of brain metastases in men and women, respectively. Approximately 10% of patients with NSCLC have brain metastases at diagnosis, and approximately 25–40% develop brain metastases during the disease (Abdallah and Wong 2018). Moreover, 5–15% of women with breast cancer are estimated to develop brain metastases (Graesslin et al. 2010). Therefore, apart from treating primary GBM, it is also important to treat brain metastases from NSCLC and breast cancer.
Although EGFR TKIs such as erlotinib (Tarceva®), gefitinib (Iressa®) and afatinib (Gilotrif®) are effective in treating NSCLC, all failed to show efficacy in GBM; however, preclinical data of the third-generation EGFR TKIs in brain metastases are promising.
Tyrosine kinase inhibitors that showed positive preclinical results are summarized in Table 5.
Osimertinib, also known as Tagrisso®, is a third-generation EGFR TKI, with sales of $1860 million in 2018. Moreover, it is also anticipated to be AstraZeneca’s largest selling drug in 2019. A preclinical study using EGFR-mutant NSCLC brain metastasis mouse model revealed that osimertinib is highly distributed in severely compromised immunodeficient mouse brain, to a similar extent as in the primary tumor (H1975), showing AUC tissue: plasma ratios of 1.7–2.8. Furthermore, osimertinib was more highly distributed in the mouse brain than gefitinib or afatinib; the brain: plasma Cmax ratio for osimertinib was 3.41, whereas the ratio was only 0.21 and < 0.36 for gefitinib and afatinib, respectively. The unbound brain-to-plasma partition ratio (Kpuu,brain) was 0.39 and 0.02 for osimertinib and gefitinib, respectively, but it could not be determined for afatinib (Ballard et al. 2016).
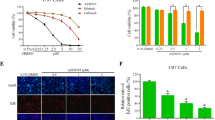
Another preclinical study of osimertinib was conducted in six different GBM cell lines and mice. It showed that osimertinib significantly inhibited the growth of the six GBM cell lines (U87, U251, U118, LN229, T98G, and LN18) in a dose-dependent manner, with IC50 values ranging from 1.25 to 3.00 µM. Notably, its inhibitory activity on GBM cell growth was 10-fold higher than that of either of the first-generation EGFR inhibitors. Moreover, survival of the GBM-bearing mice was significantly prolonged after treatment with osimertinib (Liu et al. 2019).
Lazertinib (YH25448) is also an oral, mutant-selective, irreversible third-generation EGFR TKI, which received enormous attention as Yuhan corporation licensed it out to Janssen in 2018. A preclinical study using EGFR-mutant brain metastasis mouse model reported that YH25448 inhibited intracranial tumor growth more effectively than osimertinib, at 10 and 25 mg/kg once daily during a 49-day treatment period. Although all mice were dead in the vehicle group at 42 days after tumor implantation, lazertinib-treated mice showed significantly longer survival than osimertinib-treated mice. Moreover, in the H1975-luc brain metastasis xenograft model, YH25448 demonstrated excellent BBB penetration. The Kpuu,brain value of YH25448 was 0.29 which is comparable to that of osimertinib, which was previously reported as 0.39. Moreover, YH25448 is not a substrate for BCRP and only a weak substrate for MDR1, suggesting that YH25448 may be less affected by drug efflux transporters (Yun et al. 2019).
AZD3759, another small molecule EGFR TKI, also presents good preclinical trial results with regard to BBB penetration in mice. A study in 2016 evaluating the efficacy of AZD3759 in lung cancer brain metastasis mouse model reported that the Kpuu,brain and Kpuu,CSF for AZD3759 were 0.65 and 0.42, respectively, which were significantly higher than those for erlotinib (Kpuu,brain, 0.13; Kpuu,CSF, 0.14). It has been reported that a Kpuu,brain of > 0.4 is necessary for good CNS penetration in humans. Moreover, the Kpuu,CSF values for AZD3759 in two human patients were 1.1 and 1.4, which strongly suggests that AZD3759 should be similarly effective both intracranially and extracranially (Yang et al. 2016).
Good BBB penetration does not always guarantee efficacy against GBM; however, considering the number of clinical trials that showed limited BBB infiltration (negative result), these preclinical data seem to be extremely promising.
Conclusions
In this review, we discuss small molecule TKIs that could be used for treating patients with GBM. We also outline plausible hypotheses for the negative clinical trial outcomes of many TKIs in patients with GBM. Although none of the TKIs have been approved for GBM treatment, several clinical and preclinical trials are currently ongoing. Tyrosine kinase inhibitors have the potential to treat GBM if they overcome certain limitations such as BBB penetration, adaptation to altered signaling pathways, and heterogeneity of GBM cells. The first small molecule TKI that can be used for GBM treatment has been anticipated since 1999.
References
Abdallah SM, Wong A (2018) Brain metastases in non-small-cell lung cancer: are tyrosine kinase inhibitors and checkpoint inhibitors now viable options? Curr Oncol 25:S103–S114. https://doi.org/10.3747/co.25.3733
Arora A, Scholar EM (2005) Role of tyrosine kinase inhibitors in cancer therapy. J Pharmacol Exp Ther 315:971–979. https://doi.org/10.1124/jpet.105.084145
Ballard P, Yates JW, Yang Z, Kim DW, Yang JC, Cantarini M, Pickup K, Jordan A, Hickey M, Grist M, Box M, Johnstrom P, Varnas K, Malmquist J, Thress KS, Janne PA, Cross D (2016) Preclinical comparison of osimertinib with other EGFR-TKIs in EGFR-mutant NSCLC brain metastases models, and early evidence of clinical brain metastases activity. Clin Cancer Res 22:5130–5140. https://doi.org/10.1158/1078-0432.CCR-16-0399
Brown N, McBain C, Nash S, Hopkins K, Sanghera P, Saran F, Phillips M, Dungey F, Clifton-Hadley L, Wanek K, Krell D, Jeffries S, Khan I, Smith P, Mulholland P (2016) Multi-center randomized phase II study comparing cediranib plus gefitinib with cediranib plus placebo in subjects with recurrent/progressive glioblastoma. PLoS ONE 11:e0156369. https://doi.org/10.1371/journal.pone.0156369
Cancer Genome Atlas Research, N (2008) Comprehensive genomic characterization defines human glioblastoma genes and core pathways. Nature 455:1061–1068. https://doi.org/10.1038/nature07385
Dagher R, Cohen M, Williams G, Rothmann M, Gobburu J, Robbie G, Rahman A, Chen G, Staten A, Griebel D, Pazdur R (2002) Approval summary: imatinib mesylate in the treatment of metastatic and/or unresectable malignant gastrointestinal stromal tumors. Clin Cancer Res 8:3034–3038
Englot DJ, Chang EF, Vecht CJ (2016) Epilepsy and brain tumors. Handb Clin Neurol 134:267–285. https://doi.org/10.1016/B978-0-12-802997-8.00016-5
Franceschi E, Cavallo G, Lonardi S, Magrini E, Tosoni A, Grosso D, Scopece L, Blatt V, Urbini B, Pession A, Tallini G, Crino L, Brandes AA (2007) Gefitinib in patients with progressive high-grade gliomas: a multicentre phase II study by Gruppo Italiano Cooperativo di Neuro-Oncologia (GICNO). Br J Cancer 96:1047–1051. https://doi.org/10.1038/sj.bjc.6603669
Frolov A, Evans IM, Li N, Sidlauskas K, Paliashvili K, Lockwood N, Barrett A, Brandner S, Zachary IC, Frankel P (2016) Imatinib and Nilotinib increase glioblastoma cell invasion via Abl-independent stimulation of p130Cas and FAK signalling. Sci Rep 6:27378. https://doi.org/10.1038/srep27378
Graesslin O, Abdulkarim BS, Coutant C, Huguet F, Gabos Z, Hsu L, Marpeau O, Uzan S, Pusztai L, Strom EA, Hortobagyi GN, Rouzier R, Ibrahim NK (2010) Nomogram to predict subsequent brain metastasis in patients with metastatic breast cancer. J Clin Oncol 28:2032–2037. https://doi.org/10.1200/jco.2009.24.6314
Iqbal N, Iqbal N (2014) Imatinib: a breakthrough of targeted therapy in cancer. Chemother Res Pract 2014:357027. https://doi.org/10.1155/2014/357027
Iwamoto FM, Lamborn KR, Robins HI, Mehta MP, Chang SM, Butowski NA, Deangelis LM, Abrey LE, Zhang WT, Prados MD, Fine HA (2010) Phase II trial of pazopanib (GW786034), an oral multi-targeted angiogenesis inhibitor, for adults with recurrent glioblastoma (North American Brain Tumor Consortium Study 06-02). Neuro Oncol 12:855–861. https://doi.org/10.1093/neuonc/noq025
Jeong W, Doroshow JH, Kummar S (2013) United States Food and Drug Administration approved oral kinase inhibitors for the treatment of malignancies. Curr Probl Cancer 37:110–144. https://doi.org/10.1016/j.currproblcancer.2013.06.001
Kalpathy-Cramer J, Chandra V, Da X, Ou Y, Emblem KE, Muzikansky A, Cai X, Douw L, Evans JG, Dietrich J, Chi AS, Wen PY, Stufflebeam S, Rosen B, Duda DG, Jain RK, Batchelor TT, Gerstner ER (2017) Phase II study of tivozanib, an oral VEGFR inhibitor, in patients with recurrent glioblastoma. J Neurooncol 131:603–610. https://doi.org/10.1007/s11060-016-2332-5
Kim D-W, Yang JC-H, Chen K, Cheng Z, Yin L, Martin PD, Yang Z, Jiang H, Ahn M-J (2015) AZD3759, an EGFR inhibitor with blood brain barrier (BBB) penetration for the treatment of non-small cell lung cancer (NSCLC) with brain metastasis (BM): preclinical evidence and clinical cases. J Clin Oncol 33:8016–8016. https://doi.org/10.1200/jco.2015.33.15_suppl.8016
Lassman AB, Pugh SL, Gilbert MR, Aldape KD, Geinoz S, Beumer JH, Christner SM, Komaki R, DeAngelis LM, Gaur R, Youssef E, Wagner H, Won M, Mehta MP (2015) Phase 2 trial of dasatinib in target-selected patients with recurrent glioblastoma (RTOG 0627). Neuro Oncol 17:992–998. https://doi.org/10.1093/neuonc/nov011
Lee EQ, Kaley TJ, Duda DG, Schiff D, Lassman AB, Wong ET, Mikkelsen T, Purow BW, Muzikansky A, Ancukiewicz M, Huse JT, Ramkissoon S, Drappatz J, Norden AD, Beroukhim R, Weiss SE, Alexander BM, McCluskey CS, Gerard M, Smith KH, Jain RK, Batchelor TT, Ligon KL, Wen PY (2015) A multicenter, phase II, randomized, noncomparative clinical trial of radiation and temozolomide with or without vandetanib in newly diagnosed glioblastoma patients. Clin Cancer Res 21:3610–3618. https://doi.org/10.1158/1078-0432.CCR-14-3220
Liu X, Chen X, Shi L, Shan Q, Cao Q, Yue C, Li H, Li S, Wang J, Gao S, Niu M, Yu R (2019) The third-generation EGFR inhibitor AZD9291 overcomes primary resistance by continuously blocking ERK signaling in glioblastoma. J Exp Clin Cancer Res 38:219. https://doi.org/10.1186/s13046-019-1235-7
Mei L, Du W, Idowu M, von Mehren M, Boikos SA (2018) Advances and challenges on management of gastrointestinal stromal tumors. Front Oncol 8:135. https://doi.org/10.3389/fonc.2018.00135
Muhic A, Poulsen HS, Sorensen M, Grunnet K, Lassen U (2013) Phase II open-label study of nintedanib in patients with recurrent glioblastoma multiforme. J Neurooncol 111:205–212. https://doi.org/10.1007/s11060-012-1009-y
Norden AD, Schiff D, Ahluwalia MS, Lesser GJ, Nayak L, Lee EQ, Rinne ML, Muzikansky A, Dietrich J, Purow B, Doherty LM, LaFrankie DC, Pulverenti JR, Rifenburg JA, Ruland SF, Smith KH, Gaffey SC, McCluskey C, Ligon KL, Reardon DA, Wen PY (2015) Phase II trial of triple tyrosine kinase receptor inhibitor nintedanib in recurrent high-grade gliomas. J Neurooncol 121:297–302. https://doi.org/10.1007/s11060-014-1631-y
Ostrom QT, Gittleman H, Truitt G, Boscia A, Kruchko C, Barnholtz-Sloan JS (2018) CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2011–2015. Neuro Oncol 20:iv1–iv86. https://doi.org/10.1093/neuonc/noy131
Peereboom DM, Shepard DR, Ahluwalia MS, Brewer CJ, Agarwal N, Stevens GH, Suh JH, Toms SA, Vogelbaum MA, Weil RJ, Elson P, Barnett GH (2010) Phase II trial of erlotinib with temozolomide and radiation in patients with newly diagnosed glioblastoma multiforme. J Neurooncol 98:93–99. https://doi.org/10.1007/s11060-009-0067-2
Pollack IF, Jakacki RI, Blaney SM, Hancock ML, Kieran MW, Phillips P, Kun LE, Friedman H, Packer R, Banerjee A, Geyer JR, Goldman S, Poussaint TY, Krasin MJ, Wang Y, Hayes M, Murgo A, Weiner S, Boyett JM (2007) Phase I trial of imatinib in children with newly diagnosed brainstem and recurrent malignant gliomas: a pediatric brain tumor consortium report. Neuro Oncol 9:145–160. https://doi.org/10.1215/15228517-2006-031
Raymond E, Brandes AA, Dittrich C, Fumoleau P, Coudert B, Clement PM, Frenay M, Rampling R, Stupp R, Kros JM, Heinrich MC, Gorlia T, Lacombe D, van den Bent MJ, European Organisation R for and S. Treatment of Cancer Brain Tumor Group (2008) Phase II study of imatinib in patients with recurrent gliomas of various histologies: a European Organisation for Research and Treatment of Cancer Brain Tumor Group Study. J Clin Oncol 26: 4659–4665. https://doi.org/10.1200/JCO.2008.16.9235
Raymond E, Dahan L, Raoul JL, Bang YJ, Borbath I, Lombard-Bohas C, Valle J, Metrakos P, Smith D, Vinik A, Chen JS, Horsch D, Hammel P, Wiedenmann B, Van Cutsem E, Patyna S, Lu DR, Blanckmeister C, Chao R, Ruszniewski P (2011) Sunitinib malate for the treatment of pancreatic neuroendocrine tumors. N Engl J Med 364:501–513. https://doi.org/10.1056/NEJMoa1003825
Razis E, Selviaridis P, Labropoulos S, Norris JL, Zhu MJ, Song DD, Kalebic T, Torrens M, Kalogera-Fountzila A, Karkavelas G, Karanastasi S, Fletcher JA, Fountzilas G (2009) Phase II study of neoadjuvant imatinib in glioblastoma: evaluation of clinical and molecular effects of the treatment. Clin Cancer Res 15:6258–6266. https://doi.org/10.1158/1078-0432.CCR-08-1867
Reardon DA, Wen PY, Desjardins A, Batchelor TT, Vredenburgh JJ (2008) Glioblastoma multiforme: an emerging paradigm of anti-VEGF therapy. Expert Opin Biol Ther 8:541–553. https://doi.org/10.1517/14712598.8.4.541
Reardon DA, Conrad CA, Cloughesy T, Prados MD, Friedman HS, Aldape KD, Mischel P, Xia J, DiLea C, Huang J, Mietlowski W, Dugan M, Chen W, Yung WK (2012) Phase I study of AEE788, a novel multitarget inhibitor of ErbB- and VEGF-receptor-family tyrosine kinases, in recurrent glioblastoma patients. Cancer Chemother Pharmacol 69:1507–1518. https://doi.org/10.1007/s00280-012-1854-6
Reardon DA, Groves MD, Wen PY, Nabors L, Mikkelsen T, Rosenfeld S, Raizer J, Barriuso J, McLendon RE, Suttle AB, Ma B, Curtis CM, Dar MM, de Bono J (2013) A phase I/II trial of pazopanib in combination with lapatinib in adult patients with relapsed malignant glioma. Clin Cancer Res 19:900–908. https://doi.org/10.1158/1078-0432.CCR-12-1707
Reardon DA, Nabors LB, Mason WP, Perry JR, Shapiro W, Kavan P, Mathieu D, Phuphanich S, Cseh A, Fu Y, Cong J, Wind S, Eisenstat DD, B. I. T. Group and C. the Canadian Brain Tumour (2015) Phase I/randomized phase II study of afatinib, an irreversible ErbB family blocker, with or without protracted temozolomide in adults with recurrent glioblastoma. Neuro Oncol 17: 430–439. https://doi.org/10.1093/neuonc/nou160
Reardon DA, Egorin MJ, Quinn JA, Rich JN, Gururangan S, Vredenburgh JJ, Desjardins A, Sathornsumetee S, Provenzale JM, Herndon JE 2nd, Dowell JM, Badruddoja MA, McLendon RE, Lagattuta TF, Kicielinski KP, Dresemann G, Sampson JH, Friedman AH, Salvado AJ, Friedman HS (2005) Phase II study of imatinib mesylate plus hydroxyurea in adults with recurrent glioblastoma multiforme. J Clin Oncol 23:9359–9368. https://doi.org/10.1200/JCO.2005.03.2185
Rizzo M, Porta C (2017) Sunitinib in the treatment of renal cell carcinoma: an update on recent evidence. Ther Adv Urol 9:195–207. https://doi.org/10.1177/1756287217713902
Schiff D, Sarkaria J (2015) Dasatinib in recurrent glioblastoma: failure as a teacher. Neuro Oncol 17:910–911. https://doi.org/10.1093/neuonc/nov086
Sharma M, Schilero C, Peereboom DM, Hobbs BP, Elson P, Stevens GHJ, McCrae K, Nixon AB, Ahluwalia MS (2019) Phase II study of Dovitinib in recurrent glioblastoma. J Neurooncol. https://doi.org/10.1007/s11060-019-03236-6
Snuderl M, Fazlollahi L, Le LP, Nitta M, Zhelyazkova BH, Davidson CJ, Akhavanfard S, Cahill DP, Aldape KD, Betensky RA, Louis DN, Iafrate AJ (2011) Mosaic amplification of multiple receptor tyrosine kinase genes in glioblastoma. Cancer Cell 20:810–817. https://doi.org/10.1016/j.ccr.2011.11.005
Soreide K, Sandvik OM, Soreide JA, Giljaca V, Jureckova A, Bulusu VR (2016) Global epidemiology of gastrointestinal stromal tumours (GIST): A systematic review of population-based cohort studies. Cancer Epidemiol 40:39–46. https://doi.org/10.1016/j.canep.2015.10.031
Stelzer KJ (2013) Epidemiology and prognosis of brain metastases. Surg Neurol Int 4:S192–S202. https://doi.org/10.4103/2152-7806.111296
Stommel JM, Kimmelman AC, Ying H, Nabioullin R, Ponugoti AH, Wiedemeyer R, Stegh AH, Bradner JE, Ligon KL, Brennan C, Chin L, DePinho RA (2007) Coactivation of receptor tyrosine kinases affects the response of tumor cells to targeted therapies. Science 318:287–290. https://doi.org/10.1126/science.1142946
Stupp R, Mason WP, van den Bent MJ, Weller M, Fisher B, Taphoorn MJ, Belanger K, Brandes AA, Marosi C, Bogdahn U, Curschmann J, Janzer RC, Ludwin SK, Gorlia T, Allgeier A, Lacombe D, Cairncross JG, Eisenhauer E, Mirimanoff RO, R European Organisation for, T. Treatment of Cancer Brain, G Radiotherapy and G. National Cancer Institute of Canada Clinical Trials (2005) Radiotherapy plus concomitant and adjuvant temozolomide for glioblastoma. N Engl J Med 352: 987–996. https://doi.org/10.1056/NEJMoa043330
Taylor JW, Dietrich J, Gerstner ER, Norden AD, Rinne ML, Cahill DP, Stemmer-Rachamimov A, Wen PY, Betensky RA, Giorgio DH, Snodgrass K, Randall AE, Batchelor TT, Chi AS (2015) Phase 2 study of bosutinib, a Src inhibitor, in adults with recurrent glioblastoma. J Neurooncol 121:557–563. https://doi.org/10.1007/s11060-014-1667-z
Uhm JH, Ballman KV, Wu W, Giannini C, Krauss JC, Buckner JC, James CD, Scheithauer BW, Behrens RJ, Flynn PJ, Schaefer PL, Dakhill SR, Jaeckle KA (2011) Phase II evaluation of gefitinib in patients with newly diagnosed Grade 4 astrocytoma: Mayo/North Central Cancer Treatment Group Study N0074. Int J Radiat Oncol Biol Phys 80:347–353. https://doi.org/10.1016/j.ijrobp.2010.01.070
Yang Z, Guo Q, Wang Y, Chen K, Zhang L, Cheng Z, Xu Y, Yin X, Bai Y, Rabbie S, Kim DW, Ahn MJ, Yang JC, Zhang X (2016) AZD3759, a BBB-penetrating EGFR inhibitor for the treatment of EGFR mutant NSCLC with CNS metastases. Sci Transl Med 8:368ra172. https://doi.org/10.1126/scitranslmed.aag0976
Yewale C, Baradia D, Vhora I, Patil S, Misra A (2013) Epidermal growth factor receptor targeting in cancer: a review of trends and strategies. Biomaterials 34:8690–8707. https://doi.org/10.1016/j.biomaterials.2013.07.100
Yun J, Hong MH, Kim SY, Park CW, Kim S, Yun MR, Kang HN, Pyo KH, Lee SS, Koh JS, Song HJ, Kim DK, Lee YS, Oh SW, Choi S, Kim HR, Cho BC (2019) YH25448, an irreversible EGFR-TKI with potent intracranial activity in EGFR mutant non-small cell lung cancer. Clin Cancer Res 25:2575–2587. https://doi.org/10.1158/1078-0432.CCR-18-2906
Funding
This research was supported by the Basic Science Research Program and the Pioneer Research Center Program of the National Research Foundation of Korea (NRF) grant funded by the Ministry of Education, Science and Technology (NRF-2017R1A2B4002743 and NRF 2014M3C1A3054153). This research was also supported by the Gachon University research fund of 2019 (GCU-2019-0367).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Kim, G., Ko, Y.T. Small molecule tyrosine kinase inhibitors in glioblastoma. Arch. Pharm. Res. 43, 385–394 (2020). https://doi.org/10.1007/s12272-020-01232-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12272-020-01232-3