Abstract
It is unknown whether sluggish cognitive tempo (SCT) is prospectively associated with depression in adolescence, and possible processes linking SCT to depression remain unexamined. Using a longitudinal study with three timepoints over a two-year period, the current study tested the indirect effects of SCT on depression via peer victimization, specifically physical, relational, and verbal victimization. Participants were 302 adolescents (Mage = 13.17 years; 44.7% female participants; 81.8% White; 52% with ADHD). In the fall of 8th grade, adolescents and parents completed measures of adolescents’ SCT and ADHD symptoms. Adolescents completed a measure of peer victimization in spring of 8th grade and a measure of depressive symptoms in 10th grade. Models examining indirect effects were conducted with and without control of baseline ADHD and/or depressive symptoms. Across analyses, adolescent and parent ratings of SCT symptoms uniquely predicted greater depressive symptoms two years later when controlling for adolescent sex, study site, and either 8th grade depressive or ADHD symptoms. Further, adolescents’ self-reported 8th grade SCT symptoms predicted 10th grade depressive symptoms via verbal victimization when controlling for 8th grade ADHD symptoms, but not in analyses incorporating 8th grade depressive symptoms. Findings underscore the predictive association of SCT on depressive symptoms, the possible role of adverse peer relationships as a mechanism linking SCT to depression, and the importance of considering ADHD and depressive symptoms in research on longitudinal correlates of SCT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sluggish cognitive tempo (SCT) is characterized by excessive daydreaming, mind-wandering, staring or zoning out, drowsiness, and hypoactivity, and is related to, yet separate from, attention-deficit/hyperactivity disorder inattentive (ADHD-IN) symptoms (Barkley, 2014). Although SCT was initially examined within the context of ADHD samples, accumulating evidence suggests that SCT is strongly associated with internalizing psychopathologies, particularly depression (Becker & Willcutt, 2019). However, no study has evaluated the longitudinal association of SCT with depressive symptoms in adolescents, which is important given both symptom domains increase during this developmental period (Kessler et al., 2012; Leopold et al., 2016). Further, studies have yet to examine possible mechanisms explaining the association between SCT and depression symptoms. Given the robust influence of peer victimization on depressive symptoms (Forbes et al., 2019), in addition to evidence indicating that SCT is marked by social impairments (Rondon et al., 2020), the current study utilized a multi-informant design to evaluate peer victimization as a process explaining the longitudinal association of SCT with depressive symptoms across a two-year interval in a sample of adolescents with and without ADHD.
Sluggish Cognitive Tempo and Depression Symptoms
One of the most consistent findings in the SCT literature over the past two decades is the robust association between SCT and internalizing symptoms (Carlson & Mann, 2002; Rondon et al., 2020; Willcutt et al., 2014), with evidence pointing to a unique relation with depressive symptoms. Although factor analytic studies show SCT and depressive symptoms to be distinct (Becker et al., 2015; Burns et al., 2013; Smith et al., 2019), SCT symptoms are associated with greater depressive symptoms in community (Bernad et al., 2014; Lee et al., 2014) and clinical samples (Bauermeister et al., 2012; Carlson & Mann, 2002; McBurnett et al., 2014; Rondon et al., 2020) of school-aged children, above and beyond ADHD symptoms. Although fewer compared to samples of school-aged children, cross-sectional studies in adolescents reveal similar significant associations between SCT and depression symptoms with parent (Becker & Langberg, 2013) and self-report ratings (Becker et al., 2020; Smith & Langberg, 2017).
Despite a number of studies reporting unique associations between SCT and depression across school-aged and adolescent samples, only a handful of studies have assessed this association longitudinally. In a sample of school-aged children, parent-reported SCT symptoms uniquely predicted depressive symptoms across one- and two-year intervals, controlling for ADHD-IN symptoms (Servera et al., 2016). Longitudinal findings using teacher ratings are less consistent, with one study finding SCT symptoms to predict depression, above and beyond ADHD-IN symptoms (Bernad et al., 2016), and another finding ADHD-IN symptoms, but not SCT symptoms, to predict depressive symptoms (Bernad et al., 2014). Two additional studies examined SCT and internalizing symptoms across longer time frames. Specifically, parent ratings of trait SCT (assessed across four periods in early childhood) in early childhood predicted parent-reported adolescent anxiety/depression 10 years later in adolescence, controlling for trait ADHD-IN (Becker et al., 2018). Further, Smith and colleagues (2020) found self-reported SCT symptoms assessed in an interview format in children/adolescents to be associated with self-reported ratings of depressive symptoms 12 years later in adulthood, above and beyond age, sex, race, and family income. However, self-reported SCT was unrelated to subsequent depression when controlling for baseline depressive symptoms (Smith et al., 2020). Finally, Becker and colleagues (2021) examined the bidirectional relationship of SCT and depression in a community sample of school-aged children and found teacher ratings of SCT symptoms to predict increased teacher- and child-reported depressive symptoms, but not vice versa, suggesting that SCT may be a precursor to worsening depressive symptoms.
Although these studies demonstrate that SCT is prospectively related to depressive symptoms, no study has examined whether SCT is longitudinally associated with increased depression in adolescents, above and beyond ADHD symptoms which are known to predict subsequent depression (Meinzer et al., 2021). Nor have studies generally controlled for baseline depression symptoms (for an exception, see Smith et al., 2020). Thus, it is relatively unknown whether adolescents’ own experiences of these symptoms, which is considered important for the assessment of SCT and internalizing psychopathologies (De Los Reyes et al., 2015; Sáez et al., 2019; Smith et al., 2019), are longitudinally associated.
What Might Explain the Link Between SCT and Depression?
Despite an established association between SCT and depression, studies have yet to examine possible mechanisms of this association. Theoretical models of depression propose competency domains, self-perceptions, and information processing as key features in the development and maintenance of symptomatology (Cole et al., 2014). For instance, adverse life events and ongoing negative feedback are theorized to lead to negative self-perceptions which, in turn, increase negative affect, cognitive biases, and social withdrawal (Cole et al., 2014; Sinclair et al., 2012). As adolescence represents a developmental period consisting of increased preoccupation of peer relationships and sensitivities to peer acceptance (Somerville, 2013), one source of negative feedback is peer victimization. Peer victimization is defined as either overt and/or covert relational attacks towards an individual and is often differentiated into physical (e.g., target of physical aggression such as hitting, kicking, or pushing), verbal (e.g., teasing, calling peers names), and relational (e.g., direct attempts to exclude peer from the social group by spreading rumors, gossiping, or not inviting peer to social gatherings) victimization (Card & Hodges, 2008; Sheppard et al., 2019). Physical and verbal victimization are considered overt or direct forms of aggression, whereas relational victimization is defined as indirect attempts to use existing relationships to harm others through social exclusion or gossiping (De Los Reyes & Prinstein, 2004). Evidence clearly documents the negative impact of peer victimization on depressive symptoms both concurrently and longitudinally (Forbes et al., 2019; Stapinski et al., 2015; Sweeting et al., 2006). Although a recent study comprising a large community sample of adolescents found different types of victimization to be similarly associated with depression (Forbes et al., 2020), other studies suggest indirect forms of peer victimization, such as relational and verbal, may be more related than physical victimization to depressive symptoms, due to targeting negative self-perceptions (Prinstein et al., 2001; Sinclair et al., 2012).
Adolescents with elevated SCT may experience greater peer victimization and, in turn, increased depressive symptoms for a number of reasons. Multiple studies demonstrate that SCT symptoms are associated with social withdrawal (Becker et al., 2019a; Marshall et al., 2014; Rondon et al., 2020; Willcutt et al., 2014), lower teacher-reported social skills (Bauermeister et al., 2012; McBurnett et al., 2014), poorer perception of subtle social cues (Mikami et al., 2007), and conflicted shyness (Sáez et al., 2019) in school-aged and adolescent samples. Longitudinal studies also find SCT symptoms to predict poorer teacher-reported peer functioning over a six-month period in school-aged children controlling for ADHD symptoms (Becker, 2014), in addition to parent-reported SCT predicting children’s social impairment one year later (Bernad et al., 2016). Further, SCT symptoms represent a collection of cognitive and behavioral characteristics that likely potentiate risk for peer victimization. Poor social skills and peer relationship difficulties are hallmark risk factors for peer victimization (Hawker & Boulton, 2000; Wolke et al., 2009), and, as mentioned above, studies link elevated SCT symptoms to poorer social competence and impairments in peer relations (see Ferretti et al., 2019, for a review), in addition to impairment in extracurricular activities (Barkley, 2013). Second, when considering the nature of SCT, adolescents who are often staring into space, lost in their own thoughts/mind-wandering, and drowsy/hypoactive may be especially susceptible to being teased and picked on (Card & Hodges, 2008; Karlsson et al., 2014). In line with this possibility, in a recent qualitative study consisting of youth with clinically elevated SCT, one parent directly noted a possible connection between SCT behaviors and peer victimization, stating, “I think because he is zoned out they are able to catch him unaware” (Becker et al., 2022a).
Current Study
The current study investigates whether SCT is longitudinally associated with depression in adolescence, above and beyond ADHD and/or depression symptoms, and to evaluate peer victimization as a process linking SCT to depression. Testing these associations using multiple timepoints in early to mid-adolescence is especially important as this period represents vulnerability for heightened SCT, depression, and peer victimization (Karlsson et al., 2014; Kessler et al., 2012; Leopold et al., 2016). Consistent with research on peer victimization (Card & Hodges, 2008), we tested three types of victimization, specifically physical, verbal, and relational victimization, and used adolescents’ self-report which is considered important for understanding adolescents’ own experiences with peer victimization (Farrell et al., 2016). Finally, given increased emphasis on the multi-informant assessment of SCT (Becker et al., 2020; Sáez et al., 2019), we utilized adolescent and parent ratings of SCT. To ensure a full range of SCT symptoms, we used a sample of adolescents with and without ADHD, as 25–40% of youth with ADHD have clinically elevated SCT (Barkley, 2013; Burns & Becker, 2021; Servera et al., 2018), and adolescents with ADHD also experience higher rates of depression (Becker & Fogleman, 2020) and peer victimization than their peers (Timmermanis & Wiener, 2011). The current study had two primary objectives:
-
1.
First, we examined whether adolescent- and parent-reported SCT symptoms at the first timepoint (T1) would be longitudinally associated with adolescents’ self-reported depressive symptoms at a third timepoint (T3) two years later. Four separate analyses were conducted for the adolescent model (adolescent report of SCT) and parent model (parent report of SCT). Specifically, we conducted analyses without covarying baseline symptoms, controlling for baseline ADHD symptoms, controlling for baseline depression symptoms, and finally controlling for both ADHD and depressive symptoms. Due to the strong correlations among these symptom dimensions (Becker et al., 2016), these analyses allowed us to better understand the unique contribution of SCT on subsequent depressive symptoms when different co-occurring symptoms were included. Given the robust association between SCT and depression concurrently (Becker & Langberg, 2013; Becker et al., 2016, 2020; Smith & Langberg, 2017) and initial prospective evidence (Becker et al., 2018; Bernad et al., 2016; Servera et al., 2016), we anticipated that T1 SCT would predict T3 depressive symptoms for both adolescent and parent report across the various analyses.
-
2.
Second, we tested whether T1 SCT would be indirectly related to T3 self-reported depressive symptoms via adolescent ratings of physical, verbal, or relational victimization collected at the second timepoint (T2), which occurred approximately six months after T1. The same analytic approach in Aim 1 was used, with indirect effects tested with no baseline symptoms, controlling for ADHD symptoms, controlling for depression symptoms, and then controlling for both ADHD and depression symptoms. Peer victimization is strongly associated with elevated depressive symptoms in adolescents (Forbes et al., 2019; Stapinski et al., 2015), with evidence indicating that verbal and relational forms of victimization are most strongly associated with depression compared to physical victimization (Prinstein et al., 2001; Sinclair et al., 2012). Thus, we anticipated that T1 adolescent- and parent-reported SCT would predict T3 depressive symptoms indirectly through T2 verbal and relational victimization.
Methods
Participants
Participants were 302 adolescents (44.7% female participants) with and without ADHD between the ages of 12 and 14 years (M = 13.17, SD = 0.40) at the initial timepoint. Parents identified adolescents’ race/ethnicity as White (81.8%), Multiracial (7.9%), Black (5.3%), and Asian (4.5%), and American Indian/Alaskan (0.3%). Slightly more than half of participants (53%) had a reported family income of $100,000 or higher, 31.2% between $50,000 and $100,000, and 14.5% less than $50,000. Adolescents were recruited from local public schools across two sites in the Southeast and Midwest United States. For purposes of the larger study, recruitment targeted an approximately equal number of adolescents with and without ADHD (n = 162 diagnosed with DSM-5 ADHD; 120 with Predominantly Inattentive Presentation and 42 with Combined Presentation). Further description of the sample and comparisons can be found elsewhere (Becker et al., 2019). Of the 302 participants, 288 completed rating scales at T2 (95.4% retention rate) and 266 completed rating scales at T3 (88% retention rate). Patterns of missingness are discussed in further detail below.
Procedures
This study was approved by the institutional review boards (IRB) at Cincinnati Children's Hospital Medical Center and Virginia Commonwealth University. Adolescents and parents were recruited to participate in a prospective longitudinal study of adolescents with and without ADHD (Becker et al., 2019b). The current study uses data from three timepoints: fall of 8th grade (T1), the spring of 8th grade (T2), and the fall/winter of 10th grade (T3). For recruitment, parents contacted the research staff in response to recruitment materials and were administered a phone screen to determine study eligibility. Inclusion criteria included: a) enrollment in eighth grade, b) Full Scale IQ ≥ 80 on the Weschler Abbreviated Scale of Intelligence, Second Edition (WASI-II) (Wechsler, 2011), and c) meeting criteria for either the ADHD or comparison group as defined below. Exclusion criteria included a) past or current diagnoses per parent-report of autism spectrum disorders, bipolar disorder, or schizophrenia disorder and b) previous diagnosis per parent-report of an organic sleep disorder. Following the screening assessment, families meeting criteria were invited to an in-person study visit to complete rating scales and receive a comprehensive psychological assessment. Parents provided written consent and adolescents provided assent at the first visit.
Diagnostic assessment
Adolescents were evaluated for ADHD at the initial visit in accordance to the Fifth Edition of the Diagnostic and Statistical Manual for Mental Disorders (DSM-5) criteria. The parent version of the Children’s Interview for Psychiatric Syndromes (P-ChIPS) (Weller et al., 1999) was used to determine adolescent eligibility for the ADHD group. Adolescents were required to meet all DSM-5 criteria for either ADHD Combined Presentation or Predominately Inattentive Presentation according to parent-report on the P-ChIPS. Adolescents participated in the comparison group if parents endorsed < 4 symptoms of both inattention and hyperactivity/impulsivity.
Measures
Child Concentration Inventory, Second Edition (CCI-2)
Adolescents’ self-reported SCT symptoms were measured with the CCI-2 (Sáez et al., 2019). The CCI-2 was initially a 16-item measure but recent factor analysis reported poor discriminative validity for three items with ADHD-IN symptoms in adolescents with and without ADHD (Becker et al., 2020). The 13-item CCI-2 is rated on a four-point scale (0 = never, 1 = sometimes, 2 = often, 3 = always), with higher scores reflecting greater SCT symptoms. Previous studies have reported strong internal consistency of scores on the CCI-2 (Becker et al., 2020; Sáez et al., 2019) in addition to moderate correlations with parent- and teacher-reported SCT (Sáez et al., 2019) and is thus considered an optimal measure of youth self-reported SCT (for a review, see, Becker, 2021). Internal consistency on the CCI-2 was α = 0.93.
ADHD Self-Report Scale (ASRS)
Adolescents’ ratings of ADHD symptoms were assessed with the ASRS, which was developed to correspond with the 18 DSM ADHD symptoms (Kessler et al., 2005). Adolescents reported on the 9-item Inattention and 9-item Hyperactive/Impulsive subscale using a four-point scale (0 = never, 3 = very often), with higher scores representing greater ADHD symptoms. A mean score for each subscale was calculated. Past research has documented moderate associations between the ASRS and interview-based assessments of ADHD symptoms (Adler et al., 2012; Sonnby et al., 2015), and discriminative validity from adolescents’ ratings of SCT on the CCI-2 (Becker et al., 2020). Internal consistency for scores on the inattention and hyperactive-impulsive subscale were α = 0.86 and α = 0.84, respectively.
Child and Adolescent Behavior Inventory (CABI)
Parent ratings of adolescents’ SCT symptoms were measured with the 15-item SCT subscale of the CABI (Burns et al., 2015). The CABI SCT items correspond to the items on the full version of the CCI-2 (“my child stares off into space”). Parents were instructed to rate the adolescents’ SCT behaviors over the past month on a 6-point scale (0 = almost never, 5 = almost always). Previous studies report excellent internal consistency of the CABI and interrelations with teacher-reported SCT symptoms on the CABI (Sáez et al., 2019). A recent systematic review found the CABI to be an optimal parent-report measure of SCT (Becker, 2021). Internal consistency in the current study was excellent, α = 0.95.
Vanderbilt ADHD Diagnostic Rating Scale (VADRS)
Parent ratings of adolescents’ ADHD symptoms were measured with the VADRS (Wolraich, 2003; Wolraich et al., 1998). Scores on the VADRS have demonstrated strong internal consistency, factor structure, and concurrent validity with other ADHD assessment instruments (Wolraich, 2003). In the current study, internal consistency on the inattentive and hyperactive-impulsive subscales were α = 0.95 and α = 0.90, respectively.
Problem Behavior Frequency Scales – Revised (PBFS-R)
Adolescents’ self-reported experiences of peer victimization were measured with the PBFS-R (Farrell et al., 2000). The original PBFS includes seven subscales measuring aggression and victimization but, for purposes of the current study, a revised version was used to assess physical victimization (e.g., originally labeled physical aggression, “someone threatened to hit or physically harm you”), relational victimization (e.g., “someone spread a false rumor about you”), and verbal victimization (originally labeled verbal aggression, e.g., “someone teased you to make you mad”). Although the original scale instructs participants to rate the frequency of victimization on a 6-point scale (1 = never, 6 = 20 or more times), this scoring resulted in highly skewed and kurtotic variables (skew > 2.0, kurtosis > 4.0). Due to the non-normal distribution of these subscales, and consistent with previous research (Fogleman et al., 2021), the scoring was changed from a likert to a binary scale (0 = no, 1 = yes) to measure the counts of endorsed victimization across the subscales (skew < 2.00, kurtosis < 4.00 after changing to a binary scale). The PFBS-R has exhibited strong factor structure and concurrent associations with teacher reports of school behavior in a large sample of adolescents (Farrell et al., 2016). In the present study, internal consistency for scores on the physical, relational, and verbal victimization were α = 0.70, 0.70, and 0.72, respectively.
Revised Child Anxiety and Depression Scale (RCADS)
Adolescents’ self-report of depressive symptoms were measured using the 10-item Major Depressive Disorder subscale of the RCADS. Adolescents report on a 4-point scale (0 = never to 3 = always) the extent to which each item is relevant (e.g., “Nothing is much fun anymore”). The Major Depressive Disorder subscale has demonstrated strong internal consistency and convergence with other measures of internalizing symptoms in community and clinical samples (Chorpita et al., 2000, 2005; Fredrick et al., 2019), including in youth evaluated for ADHD (Becker et al., 2019c). In the present study, internal consistency of scores on the RCADS depression subscale was α = 0.89.
Analytic Strategy
Overall, there was a small amount of participant attrition (T2 = 4.6%; T3 = 12%). Little’s MCAR test indicated that data were missing in a pattern consistent with not missing at random (χ2(22) = 52.72, p < 0.001). Participants completing ratings across all three timepoints did not differ from participants who completed ratings at either T1 and/or T2 on sex, race, adolescent-reported ADHD or SCT symptoms (ps > 0.05), though participants completing all timepoint ratings were older, had a higher family income, were more likely to be in the non-ADHD group, and had lower parent-reported ADHD and SCT symptoms (ps < 0.05). Thus, adolescent age and family income were used as auxiliary variables in missing data estimation moving forward. Primary study variables were normally distributed (skew < 2.00, kurtosis < 4.00).
SPSS version 26 was utilized to conduct zero-order correlations among primary study variables. Missing data were handled by using multiple imputation with 40 imputations, with pooled estimates of bivariate correlations presented. Primary analyses were conducted with the Mplus statistical software (version 8.1) using the maximum likelihood estimator. Manifest variables were used given the sample size. All models were just identified (DF = 0). Consistent with prior recommendations on handling non-ignorable missing data, we used Full-Information Maximum Likelihood with adolescent age and family income as auxiliary variables as an approach to reduce the impact of the non-ignorable missing data biased parameter estimates (Graham, 2009; Nicholson et al., 2017). Across these analyses, study site and any T1 demographic characteristic significantly correlated with T3 adolescent self-reported depressive symptoms were included as covariates.
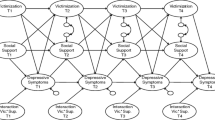
The indirect effect of T1 SCT on T3 depression via T2 peer victimization was evaluated in Mplus v8.1 using path modeling, with the three indirect effects of T2 adolescent-reported peer victimization (i.e., physical, relational, and verbal) estimated simultaneously. Four sets of analyses (e.g., no baseline symptoms covaried, controlling for baseline ADHD symptoms, controlling for baseline depressive symptoms, controlling for both ADHD and depressive symptoms) were conducted for models evaluating adolescents’ self-report and parent-report of SCT. When ADHD symptoms were included as a covariate, within-rater ADHD scores were used (i.e., adolescent-reported ADHD symptoms used in models with adolescent-reported SCT; parent-reported ADHD symptoms used in models with parent-reported SCT). The direct and indirect effects and their 95% confidence intervals (CI) were calculated using 10,000 bias-corrected bootstrapped sampling estimates samples, based on recommendations from prior research on conducting bootstrapped sampling of indirect effects (Mallinckrodt et al., 2006).
Results
Bivariate Associations
Table 1 presents intercorrelations and descriptive statistics for adolescent demographics, T1 parent- and adolescent-reported SCT and ADHD symptoms, T1 depressive symptoms, T2 peer victimization, and T3 depressive symptoms. Study site and adolescent sex (0 = male participant; 1 = female participant) were correlated with higher T3 depressive symptoms (ps < 0.05), and these variables were included as covariates in primary analyses. Adolescent race and family income were unrelated to T3 depressive symptoms. As seen in Table 1, T1 adolescent-reported SCT, depressive, inattentive, and hyperactive-impulsive symptoms were all significantly correlated with T2 peer victimization domains (ps < 0.05), with the exception of a nonsignificant correlation between hyperactive-impulsive symptoms and verbal victimization. T1 parent ratings of adolescents’ SCT symptoms were significantly correlated with T2 verbal victimization, whereas T1 parent ratings for inattentive symptoms were correlated with T2 physical victimization (ps < 0.05). All types of peer victimization were strongly correlated with each other (rs > 0.50). Finally, T1 adolescent- and parent-reported SCT and ADHD symptom dimensions, and T1 depression were significantly associated with T3 depressive symptoms (ps < 0.05), with the exception of T1 parent ratings of hyperactivity-impulsivity being unassociated with T3 depression.
Path Analyses with Adolescent Self-Reported SCT Symptoms
Path analyses were conducted evaluating relations between T1 self-reported SCT, T2 peer victimization, and T3 depressive symptoms. Four separate models were conducted (e.g., no baseline symptoms covaried, baseline self-reported ADHD inattentive and hyperactive/impulsive symptoms only, baseline self-reported depressive symptoms only, both baseline self-reported ADHD and depressive symptoms). Adolescent sex and study site were used as covariates in all analyses. In all analyses, female adolescents reported higher T3 depression than male adolescents (βs = 0.15–0.19, ps ≤ 0.001). In addition, in all analyses T2 verbal victimization was associated with higher T3 depressive symptoms (βs = 0.15–0.23, ps ≤ 0.025), whereas T2 relational and physical victimization were not significantly associated with T3 depression (ps > 0.05).
No Baseline Symptoms Covaried
In the first analyses without control of baseline ADHD or depressive symptoms, T1 adolescent-reported SCT symptoms were uniquely associated with T3 depressive symptoms (β = 0.49, p < 0.001). Further, T1 adolescent-reported SCT was uniquely associated with T2 verbal (β = 0.25, p < 0.001), relational (β = 0.19, p < 0.006), and physical (β = 0.24, p < 0.001) victimization.
Baseline ADHD Symptoms Covaried
When controlling for baseline self-reported ADHD inattentive and hyperactive-impulsive symptoms, T1 adolescent-reported SCT symptoms remained associated with T3 depressive symptoms (β = 0.42, p < 0.001). Conversely, T1 adolescent-reported ADHD inattentive or hyperactive-impulsive symptoms were unrelated to T3 depressive symptoms (ps > 0.05). Further, T1 self-reported SCT remained associated with T2 verbal (β = 0.35, p < 0.001) and physical (β = 0.24, p = 0.007) victimization, but was unrelated to relational victimization.
Baseline Depressive Symptoms Covaried
In analyses controlling for baseline depressive symptoms, T1 adolescent-reported SCT symptoms remained associated with T3 depression symptoms (β = 0.18, p = 0.015). T1 and T3 depressive symptoms were strongly associated (β = 0.43, p < 0.001). In contrast to the two previous analyses, T1 self-reported SCT was no longer associated with T2 peer victimization (p > 0.05) whereas T1 depression was uniquely associated with T2 verbal (β = 0.36, p < 0.001), relational (β = 0.24, p = 0.001), physical (β = 0.25, p = 0.002) victimization.
Baseline ADHD and Depressive Symptoms Covaried
When both baseline self-reported ADHD and depressive symptoms were included in the model, T1 adolescent-reported SCT symptoms were now marginally associated with T3 depressive symptoms (β = 0.16, p = 0.073). T1 self-reported ADHD symptom dimensions remained unrelated to T3 depressive symptoms, and T1 and T3 depressive symptoms were strongly associated (β = 0.42, p < 0.001). Moreover, T1 self-reported SCT remained unassociated with T2 peer victimization (ps > 0.05). T1 depression was uniquely associated with T2 verbal (β = 0.39, p < 0.001), relational (β = 0.26, p = 0.001), physical (β = 0.26, p = 0.002) victimization.
Path Analyses with Parent-Reported SCT Symptoms
The same models were conducted with parent-report of SCT and, when ADHD symptoms were included, parent-reported ADHD symptom dimensions were used. Adolescent sex and study site were covariates in all analyses. Once again, in all analyses T2 verbal victimization was associated with higher T3 depressive symptoms (βs = 0.14–0.25, ps < 0.05), whereas T2 relational and physical victimization were not significantly associated with T3 depression (ps > 0.05).
No Baseline Symptoms Covaried
With neither baseline ADHD nor depression included as covariates, T1 parent-reported SCT symptoms uniquely predicted T3 depressive symptoms (β = 0.29, p < 0.001). T1 parent-reported SCT was also uniquely associated with T2 verbal victimization (β = 0.18, p = 0.035).
Baseline ADHD Symptoms Covaried
When controlling for baseline parent ratings of ADHD inattentive and hyperactive-impulsive symptoms, T1 parent-reported SCT symptoms remained uniquely related to T3 depressive symptoms (β = 0.25, p < 0.001). Neither ADHD inattentive nor hyperactive-impulsive symptoms were associated with T3 depressive symptoms. T1 parent-reported SCT was unrelated to T2 peer victimization in the analyses, with a marginal effect on verbal victimization (β = 0.14, p = 0.075).
Baseline Depressive Symptoms Covaried
In analyses controlling for baseline depressive symptoms, T1 parent-reported SCT remained a significant predictor of T3 depressive symptoms (β = 0.13, p = 0.009). T1 depression was strongly associated with T3 depression ratings (β = 0.52, p < 0.001). T1 parent-reported SCT was unrelated to T2 peer victimization (ps > 0.05). Conversely, T1 depression was uniquely associated with greater verbal, relational, and physical victimization (ps < 0.05).
Baseline ADHD and Depressive Symptoms Covaried
When both baseline ADHD and depressive symptoms were included in the model, T1 parent-reported SCT remained a significant predictor of T3 depressive symptoms (β = 0.17, p = 0.012), whereas neither T1 parent-reported ADHD symptom dimension was significantly associated with T3 depression. T1 depression was associated with all three types of T2 peer victimization (ps < 0.05) and strongly related to T3 depression ratings (β = 0.53, p < 0.001).
Analyses Testing the Indirect Effect of SCT Symptoms Predicting Depression via Peer Victimization
As summarized in Table 2, we tested the indirect effect of T1 self- and parent-reported SCT → T2 physical, relational, and verbal victimization → T3 depression, with and without control for baseline ADHD and/or depressive symptoms. Adolescent sex and study site were used as covariates in all analyses. T1 self-reported SCT was associated with T3 self-reported depression indirectly via verbal victimization in the model when neither baseline ADHD nor baseline depressive symptoms were covaried (ab = 0.05, SE = 0.02, p = 0.02, 95% CI [0.01, 0.10]), and also when controlling for ADHD symptoms (ab = 0.08, SE = 0.03, p = 0.01, 95% CI [0.02, 0.14]). The indirect effects of physical and relational victimization were nonsignificant. In addition, the indirect effect via verbal victimization became nonsignificant in the models controlling for baseline depressive symptoms and both ADHD and depressive symptoms. No indirect effects via victimization were significant in models with parent-reported SCT symptoms.Footnote 1
Discussion
The current study builds on prior studies by testing the longitudinal association of SCT with depressive symptoms in adolescents using both adolescent and parent ratings of SCT and ADHD symptoms, in addition to evaluating peer victimization as a mechanism of this association. Further, we tested the direct effect of SCT on depression two years later across analyses with and without control of baseline symptoms of ADHD and depression to better understand the unique contribution of SCT symptoms. Across analyses, adolescent and parent ratings of SCT symptoms uniquely predicted adolescents’ self-reported depressive symptoms two years later in seven of the eight models conducted (with SCT having a marginal effect in the eighth model). To our knowledge, these findings are the first to show that both parent- and self-reported ratings of SCT predict subsequent depressive symptoms, above and beyond ADHD and depressive symptoms. Regarding the indirect effect, adolescent-report of SCT symptoms was uniquely associated with increased depressive via verbal victimization, above and beyond ADHD symptoms. However, the indirect effect of SCT on depression through verbal victimization became nonsignificant when controlling for baseline depressive symptoms. Taken together, these findings advance the literature by highlighting the robust predictive association of SCT on depressive symptoms over a two-year interval in adolescence and suggest that peer victimization may be one mechanism of this association.
SCT, but not ADHD, Symptoms Predicted Depression Over a Two-Year Interval
A major limitation of the extant longitudinal studies of SCT and depression was the absence of studies assessing SCT with validated self-report rating scales (for an exception using interview methodology, see Smith et al., 2020). Further, the majority of prior longitudinal studies did not test whether SCT predicted change in depressive symptoms, above and beyond baseline depression (Becker et al., 2018; Bernad et al., 2014, 2016; Servera et al., 2016). Findings from the current study extend the literature and replicate prior longitudinal data by showing both adolescent and parent ratings of SCT to uniquely predict adolescents’ self-reported depressive symptoms two years later. These findings remained in analyses without baseline symptoms and when controlling for baseline ADHD symptom dimensions and depression separately or together (with self-reported SCT only marginally associated with subsequent depression when both ADHD dimensions and baseline depression were covaried). To our knowledge, these findings are the first to document significant longitudinal effects of SCT on depression above and beyond ADHD and depressive symptoms (Smith et al., 2020). The cross-informant findings of parent-reported SCT predicting increases in adolescent-reported depression provide particularly compelling evidence for SCT as a possible risk factor for increasing depressive symptoms in adolescence. Conversely, ADHD inattentive or hyperactive-impulsive symptoms were not uniquely prospectively related to depressive symptoms across analyses in either the adolescent or parent models. Additional studies are needed to replicate and confirm these findings, including whether adolescents with co-occurring ADHD and SCT are particularly likely to experience later depression.
Adolescent-Reported SCT Symptoms Predicted Depression via Verbal Victimization, Above and Beyond ADHD Symptoms
Consistent with developmental models on the role of adverse life events and negative feedback on adolescent depression (Cole et al., 2014), we tested peer victimization as a possible mechanism of the prospective relation between SCT and depression. In analyses without controlling for baseline symptoms or when controlling for self-reported ADHD symptom dimensions, adolescent ratings of SCT were prospectively associated with depressive symptoms via verbal victimization. Conversely, the indirect effect of parent-reported SCT on depression via peer victimization was not significant. These findings are the first to provide direct evidence for previous suggestions of peer impairments being a key mechanism explaining the link between SCT and depression (Becker et al., 2021). However, we acknowledge the possibility of shared method variance explaining these relationships and, due to study design, we were unable to test whether SCT predicts residual increase above and beyond baseline peer victimization. Nevertheless, these findings contribute to the ongoing literature documenting unique social impairments among youth with elevated SCT and are the first to provide evidence for SCT predicting peer victimization in adolescence. The interpersonal correlates of SCT, such as social withdrawal (Becker et al., 2019a; Marshall et al., 2014), lower social competence (Becker et al., 2019a; Fredrick et al., 2021), and conflicted shyness (Sáez et al., 2019), may lend youth “susceptible” to being teased, picked on, or physically harmed (Card & Hodges, 2008; Karlsson et al., 2014). When considering symptoms unique to SCT (when controlling for ADHD symptoms) the non-shared symptoms of SCT such excessive internal distractibility (e.g., lost in one’s thoughts, daydreaming) and behavioral symptoms (e.g., apathy, sluggish) may reduce adolescents’ ability to attend and successfully navigate the complexities of peer relationships (Willcutt et al., 2014).
Although we hypothesized parent ratings of SCT would also be associated with peer victimization, this cross-informant hypothesis was not supported. In addition to shared method variance, one possibility for stronger effects between self-reported ratings is that adolescents are potentially reporting on SCT behaviors occurring in the school context in which the frequency and type of peer victimization occurs (which might not be observable to parents) (Fredrick et al., 2021). Prior empirical and theoretical work suggests that ongoing peer victimization impacts the construction and maintenance of one’s self-concept, resulting in negative beliefs of being unacceptable and less socially competent (Sinclair et al., 2012). Thus, adolescents with elevated SCT who experience heightened bullying or teasing may develop negative beliefs of oneself as socially unacceptable, thereby increasing depressive symptoms. Or, peer victimization may reinforce adolescents’ socially withdrawn behaviors and ruminative style of thinking, which may impact depressive symptomatology. These findings for verbal victimization predicting greater depressive symptoms are consistent with a number of prior studies (Prinstein et al., 2001; Sinclair et al., 2012).
Contrary to our expectation, SCT did not predict relational peer victimization. When considering the nature of relational victimization, prior work suggests that these acts are distinct from other types of victimization in that the function is to damage existing social relationships (Xie et al., 2002); thus, relational victimization often occurs between friends or broader peer groups/networks (Casper et al., 2017). Although no study to date has examined the nature of peer interactions (e.g., best friend, number of friends) among adolescents with elevated SCT, given the findings for higher social withdrawal, loneliness, and peer disengagement (Becker et al., 2019a; Rondon et al., 2020; Sáez et al., 2019), it may be that adolescents with elevated SCT behaviors are less likely to encounter relational forms of victimization. These adolescents may not be viewed by their peers as having sufficiently high peer standing to warrant damaging their reputations and relationships via relational victimization (Prinstein & Cillessen, 2003). In contrast, adolescents of lower peer standing may be deemed “easy targets” to being victims of direct verbal and physical victimization, often to get a laugh from other peers (Card & Hodges, 2008).
SCT Symptoms Did Not Predict Depression via Peer Victimization when Baseline Depression Controlled
Findings for the indirect effect differed in models controlling for baseline depressive symptoms. Specifically, when baseline depressive symptoms were covaried (alone or in combination with ADHD symptoms), SCT did not indirectly predict depression via peer victimization. There are several possible explanations for these findings. First, a large body of literature documents the reciprocal association between depressive symptoms and peer victimization in adolescents (Epkins & Heckler, 2011; Forbes et al., 2019; Sweeting et al., 2006). In our sample, bivariate correlations between T1 depression and T2 peer victimization were noticeably larger compared to T1 SCT or ADHD symptoms with T2 peer victimization, likely reducing any ability to detect a unique effect of SCT on later peer victimization. Second, despite numerous studies reporting SCT to be empirically distinct from both ADHD-IN and depression (Becker et al., 2020; Smith et al., 2019), there are some symptoms with overlapping item content. For instance, SCT and ADHD-IN appear to share “attentional” symptoms (e.g., poor sustained attention, forgetfulness), whereas SCT and depression share “behavioral” symptoms (e.g., apathy, fatigue, withdrawal) (Smith et al., 2020). Given the indirect effect reduced in models controlling for depression, but not ADHD symptoms, the behavioral components overlapping with SCT and depression may be uniquely related to subsequent peer victimization. In fact, researchers have suggested that adolescents exhibiting disengagement and isolated behaviors may be at high risk for peer victimization (Card & Hodges, 2008; Karlsson et al., 2014).
Collectively, findings point to the important question of considering associated symptom domains when attempting to tease apart the unique contribution of SCT on peer victimization and depression. The conceptualization of SCT as a discrete psychiatric disorder or transdiagnostic mechanism remains unanswered (Becker et al., 2022b). However, SCT clearly represents a meaningful construct that explains symptoms and impairments in the realm of internalizing psychopathologies (Becker & Willcutt, 2019). According to a Research Domain Criteria (RDoC) perspective, “statistical partialling removes important variance attributable to transdiagnostic mechanisms among disorders (Beauchaine & Hinshaw, 2020, p. 326). Thus, although our findings for the indirect effect of SCT on depression via verbal victimization became nonsignificant when controlling for both ADHD and depressive symptoms, important symptoms (overlapping with depression) attributable to the SCT construct may have been removed. Findings from our study indicate that SCT is a construct that explains increased depressive symptoms (regardless of statistically controlling for psychopathology symptoms) and may represent shared vulnerability for attention difficulties and behavioral disengagement, giving risk for peer victimization and depression. Future research exploring longitudinal outcomes of SCT is encouraged to consider the potential role of ADHD and depressive symptoms given the substantial co-occurrence and shared symptom overlap of these psychopathologies (Smith et al., 2020).
Clinical Implications
Findings point to the unique impact of SCT on depressive symptoms in adolescence and underscore the possible need to assess and intervene on adolescents with elevated SCT symptoms. Although no current evidence-based intervention is available for SCT, recent pilot work recommends consideration of social skills training, mindfulness-based interventions, and cognitive behavioral therapy (Becker et al., 2022a). Additionally, a recent study demonstrated that a positive school climate reduced the effects of peer difficulties on adolescents’ SCT symptoms (Fredrick et al., 2021), aligning with broader recommendations of intervening on the socio-contextual context for mitigating peer victimization (Card & Hodges, 2008). It is also possible that interventions to improve academic functioning (Smith & Langberg, 2020) may have downstream effects for improving peer relationships and/or increasing an adolescent’s sense of competence. Future research examining bullying prevention or school-based interventions more broadly, are strongly encouraged to incorporate measures assessing SCT to identify at-risk adolescents and consider reductions in peer victimization as one avenue to reduce the link between SCT and depression.
Strengths, Limitations, and Future Directions
The current study included many strengths, such as the multi-informant examination of the longitudinal association of SCT with depression in adolescents with and without ADHD and consideration of peer victimization as a process linking SCT to depression. Nevertheless, several limitations are important to note. First, we recognize that links between SCT, peer victimization, and depression may be reciprocal, given evidence pointing to internalizing problems as risk factors for peer victimization (Sweeting et al., 2006). Given a recent study showing SCT as a predictor of depression (but not the reverse) (Becker et al., 2019a), the goal of the current study was to examine peer victimization as a process linking between SCT to depression, though future studies may consider alternative pathways. Further, particularly as the indirect effect of peer victimization became nonsignificant when controlling for baseline depression, future research is needed to examine other potential mechanisms. For instance, other proposed candidate mechanisms may include peer ignoring (Becker et al., 2019a) or excessive mind-wandering (Becker et al., 2020; Fredrick & Becker, 2021; Fredrick et al., 2020). Second, the duration between each timepoint was inconsistent (T1 to T2 was approximately six months; T2 to T3 was approximately 18 months) due to study design and the availability of the primary measures of interest at these timepoints. Future research is encouraged to assess these links spanning multiple periods of adolescence, such as early, mid, and late adolescence would be a rigorous test of mediation (Selig & Preacher, 2009). In addition, it would be advantageous for future studies to measure peer victimization at each timepoint as a test of whether SCT symptoms predicts changes in victimization which in turn predicts changes in depressive symptoms. Third, though self-report of peer victimization is considered an optimal assessment of peer victimization in adolescents (Cornell et al., 2015; Farrell et al., 2016), gathering ratings from teacher or peer-nominations would overcome concerns with shared method variance and contribute to our understanding of the impact of SCT on peer victimization. Similarly, although there is some evidence that adolescents can report on their own ADHD symptoms (Adler et al., 2012; Sonnby et al., 2015), longstanding concerns with adolescents’ self-report remain given weak correlations between adolescent-report with either parent- or teacher-reported ADHD symptoms in adolescents diagnosed with ADHD (Sibley et al., 2012). However, it is important to note that in our sample there were moderate-to-strong correlations between adolescent- and parent-reported ADHD symptoms (Table 1). Fourth, participants who completed ratings across the three timepoints had higher family income, were more likely to be in the non-ADHD group, and had lower parent-reported ADHD and SCT symptoms; thus, future research is encouraged to include adolescents of diverse socioeconomic and racial backgrounds and with more severe ADHD and SCT symptoms. This is especially important as rates of peer victimization and discrimination are pronounced among youth of historically underrepresented and marginalized backgrounds (Cornell et al., 2015).
Conclusion
This study marks an important step in understanding the developmental sequalae of SCT in adolescence. Findings provide the first evidence that self- and parent-reported SCT predicts depressive symptoms over a two-year interval, above and beyond baseline ADHD and depressive symptoms. Further, verbal victimization was a process linking adolescent self-reported SCT to depression above and beyond ADHD symptom dimensions but not when controlling for baseline depressive symptoms. Future research exploring SCT, peer impairments, and depression across longer time frames, in addition to considering shared and non-shared overlap between SCT and co-occurring psychopathologies like ADHD and depression, are necessary to continue advancing our understanding of how SCT contributes to internalizing psychopathologies in adolescence.
Notes
Due to well documented elevations in depressive symptoms among female adolescents (Sinclair et al., 2012), and research showing verbal/relational victimization to be more common and impactful for female adolescents (Prinstein et al., 2001; Sinclair et al., 2012), we explored whether the indirect effect of SCT on subsequent depression via peer victimization was stronger among female than male participants. In moderated mediation models with both adolescent self-reported and parent-reported SCT, no evidence was found for the indirect effect significantly differing between male and female adolescents (all ps > 0.05).
References
Adler, L. A., Shaw, D. M., Spencer, T. J., Newcorn, J. H., Hammerness, P., Sitt, D. J., Minerly, C., Davidow, J. V., & Faraone, S. V. (2012). Preliminary examination of the reliability and concurrent validity of the attention-deficit/hyperactivity disorder self-report scale v1.1 symptom checklist to rate symptoms of attention-deficit/hyperactivity disorder in adolescents. Journal of Child and Adolescent Psychopharmacology, 22(3), 238–244. https://doi.org/10.1089/cap.2011.0062
Barkley, R. A. (2013). Distinguishing sluggish cognitive tempo from ADHD in children and adolescents: Executive functioning, impairment, and comorbidity. Journal of Clinical Child & Adolescent Psychology, 42(2), 161–173. https://doi.org/10.1080/15374416.2012.734259
Barkley, R. A. (2014). Sluggish cognitive tempo (concentration deficit disorder?): Current status, future directions, and a plea to change the name. Journal of Abnormal Child Psychology, 42(1), 117–125. https://doi.org/10.1007/s10802-013-9824-y
Bauermeister, J. J., Barkley, R. A., Bauermeister, J. A., Martínez, J. V., & McBurnett, K. (2012). Validity of the sluggish cognitive tempo, inattention, and hyperactivity symptom dimensions: Neuropsychological and psychosocial correlates. Journal of Abnormal Child Psychology, 40(5), 683–697. https://doi.org/10.1007/s10802-011-9602-7
Beauchaine, T. P., & Hinshaw, S. P. (2020). RDoC and psychopathology among youth: Misplaced assumptions and an agenda for future research. Journal of Clinical Child & Adolescent Psychology, 49(3), 322–340. https://doi.org/10.1080/15374416.2020.1750022
Becker, S. P. (2014). Sluggish cognitive tempo and peer functioning in school-aged children: A six-month longitudinal study. Psychiatry Research, 217(1–2), 72–78.
Becker, S. P. (2021). Systematic review: Assessment of sluggish cognitive tempo over the past decade. Journal of the American Academy of Child & Adolescent Psychiatry, 60(6), 690–709. https://doi.org/10.1016/j.jaac.2020.10.016
Becker, S. P., & Fogleman, N. D. (2020). Psychiatric co-occurrence (comorbidity) in adolescents with ADHD. In Becker S.P. (Ed.), ADHD in adolescents: Development, Assessment, and Treatment (pp. 170–203). New York: Guilford Press.
Becker, S. P., & Langberg, J. M. (2013). Sluggish cognitive tempo among young adolescents with ADHD: Relations to mental health, academic, and social functioning. Journal of Attention Disorders, 17(8), 681–689. https://doi.org/10.1177/1087054711435411
Becker, S. P., & Willcutt, E. G. (2019). Advancing the study of sluggish cognitive tempo via DSM, RDoC, and hierarchical models of psychopathology. European Child & Adolescent Psychiatry, 28(5), 603–613. https://doi.org/10.1007/s00787-018-1136-x
Becker, S. P., Burns, G. L., Leopold, D. R., Olson, R. K., & Willcutt, E. G. (2018). Differential impact of trait sluggish cognitive tempo and ADHD inattention in early childhood on adolescent functioning. Journal of Child Psychology and Psychiatry, 59(10), 1094–1104. https://doi.org/10.1111/jcpp.12946
Becker, S. P., Burns, G. L., Smith, Z. R., & Langberg, J. M. (2020). Sluggish cognitive tempo in adolescents with and without ADHD: Differentiation from adolescent-reported ADHD inattention and unique associations with internalizing domains. Journal of Abnormal Child Psychology, 48(3), 391–406. https://doi.org/10.1007/s10802-019-00603-9
Becker, S. P., Fredrick, J. W., Foster, J. A., Yeaman, K. M., Epstein, J. N., Froehlich, T. E., & Mitchell, J. T. (2022a). “My mom calls it Annaland”: A qualitative study of phenomenology, daily life impacts, and treatment considerations of sluggish cognitive tempo. Journal of Attention Disorders, 26, 915–931. https://doi.org/10.1177/10870547211050946
Becker, S. P., Garner, A. A., Tamm, L., Antonini, T. N., & Epstein, J. N. (2019a). Honing in on the social difficulties associated with sluggish cognitive tempo in children: Withdrawal, peer ignoring, and low engagement. Journal of Clinical Child & Adolescent Psychology, 48(2), 228–237. https://doi.org/10.1080/15374416.2017.1286595
Becker, S. P., Langberg, J. M., Eadeh, H. M., Isaacson, P. A., & Bourchtein, E. (2019b). Sleep and daytime sleepiness in adolescents with and without ADHD: Differences across ratings, daily diary, and actigraphy. Journal of Child Psychology and Psychiatry, 60, 1021–1031. https://doi.org/10.1111/JCPP.13061
Becker, S. P., Leopold, D. R., Burns, G. L., Jarrett, M. A., Langberg, J. M., Marshall, S. A., McBurnett, K., Waschbusch, D. A., & Willcutt, E. G. (2016). The internal, external, and diagnostic validity of sluggish cognitive tempo: A meta-analysis and critical review. Journal of the American Academy of Child & Adolescent Psychiatry, 55(3), 163–178. https://doi.org/10.1016/j.jaac.2015.12.006
Becker, S. P., Luebbe, A. M., & Joyce, A. M. (2015). The Child Concentration Inventory (CCI): Initial validation of a child self-report measure of sluggish cognitive tempo. Psychological Assessment, 27(3), 1037–1052. https://doi.org/10.1037/pas0000083
Becker, S. P., Schindler, D. N., Holdaway, A. S., Tamm, L., Epstein, J. N., & Luebbe, A. M. (2019c). The Revised Child Anxiety and Depression Scales (RCADS): Psychometric evaluation in children evaluated for ADHD. Journal of Psychopathology and Behavioral Assessment, 41(1), 93–106. https://doi.org/10.1007/s10862-018-9702-6
Becker, S. P., Webb, K. L., & Dvorsky, M. R. (2021). Initial examination of the bidirectional associations between sluggish cognitive tempo and internalizing symptoms in children. Journal of Clinical Child & Adolescent Psychology, 50(2), 258–266. https://doi.org/10.1080/15374416.2019.1630836
Becker, S. P., Willcutt, E. G., Leopold, D. R., Fredrick, J. W., Smith, Z. R., Jacobson, L. A., Burns, G. L., Mayes, S. D., Waschbusch, D. A., Froehlich, T. E., McBurnett, K., Servera, M., & Barkley, R. A. (2022b). Report of a work group on sluggish cognitive tempo: Key research directions and a consensus change in terminology to cognitive disengagement hypoactivity syndrome (CDHS). Under review.
Bernad, M., Servera, M., Becker, S. P., & Burns, G. L. (2016). Sluggish cognitive tempo and ADHD Inattention as predictors of externalizing, internalizing, and impairment domains: A 2-year longitudinal study. Journal of Abnormal Child Psychology, 44(4), 771–785. https://doi.org/10.1007/s10802-015-0066-z
Bernad, M., Servera, M., Grases, G., Collado, S., & Burns, G. L. (2014). A cross-sectional and longitudinal investigation of the external correlates of sluggish cognitive tempo and ADHD-inattention symptoms dimensions. Journal of Abnormal Child Psychology, 42(7), 1225–1236. https://doi.org/10.1007/s10802-014-9866-9
Burns, G. L., & Becker, S. P. (2021). Sluggish cognitive tempo and ADHD symptoms in a nationally representative sample of U.S. children: Differentiation using categorical and dimensional approaches. Journal of Clinical Child & Adolescent Psychology, 50(2), 267–280. https://doi.org/10.1080/15374416.2019.1678165
Burns, G. L., Lee, S., Servera, M., McBurnett, K., & Becker, S. P. (2015). Child and Adolescent Behavior Inventory - Parent Version 1.0. Author.
Burns, G. L., Servera, M., Bernad Mdel, M., Carrillo, J. M., & Cardo, E. (2013). Distinctions between sluggish cognitive tempo, ADHD-IN, and depression symptom dimensions in Spanish first-grade children. Journal of Clinical Child and Adolescent Psychology, 42(6), 796–808. https://doi.org/10.1080/15374416.2013.838771
Card, N. A., & Hodges, E. V. (2008). Peer victimization among schoolchildren: Correlations, causes, consequences, and considerations in assessment and intervention. School Psychology Quarterly, 23(4), 451.
Carlson, C. L., & Mann, M. (2002). Sluggish cognitive tempo predicts a different pattern of impairment in the attention deficit hyperactivity disorder, predominantly inattentive type. Journal of Clinical Child and Adolescent Psychology, 31(1), 123–129. https://doi.org/10.1207/S15374424JCCP3101_14
Casper, D. M., Card, N. A., Bauman, S., & Toomey, R. B. (2017). Overt and relational aggression participant role behavior: Measurement and relations with sociometric status and depression. Journal of Research on Adolescence, 27(3), 661–673. https://doi.org/10.1111/jora.12306
Chorpita, B. F., Moffitt, C. E., & Gray, J. (2005). Psychometric properties of the revised child anxiety and depression scale in a clinical sample. Behaviour Research and Therapy, 43(3), 309–322. https://doi.org/10.1016/j.brat.2004.02.004
Chorpita, B. F., Yim, L., Moffitt, C., Umemoto, L. A., & Francis, S. E. (2000). Assessment of symptoms of DSM-IV anxiety and depression in children: A revised child anxiety and depression scale. Behaviour Research and Therapy, 38(8), 835–855. https://doi.org/10.1016/s0005-7967(99)00130-8
Cole, D. A., Dukewich, T. L., Roeder, K., Sinclair, K. R., McMillan, J., Will, E., Bilsky, S. A., Martin, N. C., & Felton, J. W. (2014). Linking peer victimization to the development of depressive self-schemas in children and adolescents. Journal of Abnormal Child Psychology, 42(1), 149–160.
Cornell, D., Shukla, K., & Konold, T. (2015). Peer victimization and authoritative school climate: A multilevel approach. Journal of Educational Psychology, 107(4), 1186.
De Los Reyes, A., Augenstein, T. M., Wang, M., Thomas, S. A., Drabick, D. A., Burgers, D. E., & Rabinowitz, J. (2015). The validity of the multi-informant approach to assessing child and adolescent mental health. Psychological Bulletin, 141(4), 858–900. https://doi.org/10.1037/a0038498
De Los Reyes, A., & Prinstein, M. J. (2004). Applying depression-distortion hypotheses to the assessment of peer victimization in adolescents. Journal of Clinical Child & Adolescent Psychology, 33(2), 325–335. https://doi.org/10.1207/s15374424jccp3302_14
Epkins, C. C., & Heckler, D. R. (2011). Integrating etiological models of social anxiety and depression in youth: Evidence for a cumulative interpersonal risk model. Clinical Child and Family Psychology Review, 14(4), 329–376. https://doi.org/10.1007/s10567-011-0101-8
Farrell, A. D., Kung, E. M., White, K. S., & Valois, R. F. (2000). The structure of self-reported aggression, drug use, and delinquent behaviors during early adolescence. Journal of Clinical Child Psychology, 29(2), 282–292.
Farrell, A. D., Sullivan, T. N., Goncy, E. A., & Le, A.-T.H. (2016). Assessment of adolescents’ victimization, aggression, and problem behaviors: Evaluation of the Problem Behavior Frequency Scale. Psychological Assessment, 28(6), 702–714. https://doi.org/10.1037/pas0000225
Ferretti, N. M., King, S. L., Hilton, D. C., Rondon, A. T., & Jarrett, M. A. (2019). Focus: Attention Science: Social Functioning in Youth with Attention-Deficit/Hyperactivity Disorder and Sluggish Cognitive Tempo. The Yale Journal of Biology and Medicine, 92(1), 29–35.
Fogleman, N. D., McQuade, J. D., Mehari, K. R., & Becker, S. P. (2021). In-person victimization, cyber victimization, and polyvictimization in relation to internalizing symptoms and self-esteem in adolescents with attention-deficit/hyperactivity disorder. Child: Care. Health and Development, 47, 805–815.
Forbes, M. K., Fitzpatrick, S., Magson, N. R., & Rapee, R. M. (2019). Depression, anxiety, and peer victimization: Bidirectional relationships and associated outcomes transitioning from childhood to adolescence. Journal of Youth and Adolescence, 48(4), 692–702. https://doi.org/10.1007/s10964-018-0922-6
Forbes, M. K., Magson, N. R., & Rapee, R. M. (2020). Evidence that different types of peer victimization have equivalent associations with transdiagnostic psychopathology in adolescence. Journal of Youth and Adolescence, 49(3), 590–604.
Fredrick, J. W., & Becker, S. P. (2021). Sluggish cognitive tempo symptoms, but not ADHD or internalizing symptoms, are uniquely related to self-reported mind-wandering in adolescents with ADHD. Journal of Attention Disorders, 25(11), 1605–1611.
Fredrick, J. W., Becker, S. P., & Langberg, J. M. (2021). Low school support exacerbates the association between peer difficulties and sluggish cognitive tempo in adolescents. Journal of Clinical Child & Adolescent Psychology. https://doi.org/10.1080/15374416.2021.1923021 Advance Online Publication.
Fredrick, J. W., Kofler, M. J., Jarrett, M. A., Burns, G. L., Luebbe, A. M., Garner, A. A., Harmon, S. L., & Becker, S. P. (2020). Sluggish cognitive tempo and ADHD symptoms in relation to task-unrelated thought: Examining unique links with mind-wandering and rumination. Journal of Psychiatric Research, 123, 95–101. https://doi.org/10.1016/j.jpsychires.2020.01.016
Fredrick, J. W., Parsons, E. M., Sarfan, L. D., Dreyer-Oren, S., & Luebbe, A. M. (2019). Examining the relation between adolescent social anxiety and positive affect regulation: Self-report vs. observation. Child Psychiatry & Human Development, 50(5), 764–775. https://doi.org/10.1007/s10578-019-00881-w
Graham, J. W. (2009). Missing data analysis: Making it work in the real world. Annual Review of Psychology, 60, 549–576. https://doi.org/10.1146/annurev.psych.58.110405.085530
Hawker, D. S., & Boulton, M. J. (2000). Twenty years’ research on peer victimization and psychosocial maladjustment: A meta-analytic review of cross-sectional studies. The Journal of Child Psychology and Psychiatry and Allied Disciplines, 41(4), 441–455.
Karlsson, E., Stickley, A., Lindblad, F., Schwab-Stone, M., & Ruchkin, V. (2014). Risk and protective factors for peer victimization: A 1-year follow-up study of urban American students. European Child & Adolescent Psychiatry, 23(9), 773–781. https://doi.org/10.1007/s00787-013-0507-6
Kessler, R. C., Adler, L., Ames, M., Demler, O., Faraone, S., Hiripi, E., Howes, M. J., Jin, R., Secnik, K., & Spencer, T. (2005). The World Health Organization Adult ADHD Self-Report Scale (ASRS): A short screening scale for use in the general population. Psychological Medicine, 35(2), 245. https://doi.org/10.1017/S0033291704002892
Kessler, R. C., Avenevoli, S., McLaughlin, K. A., Green, J. G., Lakoma, M. D., Petukhova, M., Pine, D. S., Sampson, N. A., Zaslavsky, A. M., & Merikangas, K. R. (2012). Lifetime co-morbidity of DSM-IV disorders in the US National Comorbidity Survey Replication Adolescent Supplement (NCS-A). Psychological Medicine, 42(09), 1997–2010. https://doi.org/10.1017/s0033291712000025
Lee, S., Burns, G. L., Snell, J., & McBurnett, K. (2014). Validity of the sluggish cognitive tempo symptom dimension in children: Sluggish cognitive tempo and ADHD-inattention as distinct symptom dimensions. Journal of Abnormal Child Psychology, 42(1), 7–19.
Leopold, D. R., Christopher, M. E., Burns, G. L., Becker, S. P., Olson, R. K., & Willcutt, E. G. (2016). Attention-deficit/hyperactivity disorder and sluggish cognitive tempo throughout childhood: Temporal invariance and stability from preschool through ninth grade. Journal of Child Psychology and Psychiatry, 57(9), 1066–1074. https://doi.org/10.1111/jcpp.12505
Mallinckrodt, B., Abraham, W. T., Wei, M., & Russell, D. W. (2006). Advances in testing the statistical significance of mediation effects. Journal of Counseling Psychology, 53(3), 372–378. https://doi.org/10.1037/0022-0167.53.3.372
Marshall, S. A., Evans, S. W., Eiraldi, R. B., Becker, S. P., & Power, T. J. (2014). Social and academic impairment in youth with ADHD, predominately inattentive type and sluggish cognitive tempo. Journal of Abnormal Child Psychology, 42(1), 77–90. https://doi.org/10.1007/s10802-013-9758-4
McBurnett, K., Villodas, M., Burns, G. L., Hinshaw, S. P., Beaulieu, A., & Pfiffner, L. J. (2014). Structure and validity of sluggish cognitive tempo using an expanded item pool in children with attention-deficit/hyperactivity disorder. Journal of Abnormal Child Psychology, 42(1), 37–48. https://doi.org/10.1007/s10802-013-9801-5
Meinzer, M. C., Felton, J. W., Oddo, L. E., Rubin, K. H., & Chronis-Tuscano, A. (2021). Do ADHD symptoms and relationship quality with mothers and best friends across high school predict depressive symptoms for adolescents? Journal of Attention Disorders, 25(12), 1699–1711. https://doi.org/10.1177/1087054720923088
Mikami, A. Y., Huang-Pollock, C. L., Pfiffner, L. J., McBurnett, K., & Hangai, D. (2007). Social skills diferences among attention-deficit/hyperactivity disorder types in a chat room assessment task. Journal of Abnormal Child Psychology, 35(4), 509–521. https://doi.org/10.1007/s10802-007-9108-5
Nicholson, J. S., Deboeck, P. R., & Howard, W. (2017). Attrition in developmental psychology: A review of modern missing data reporting and practices. International Journal of Behavioral Development, 41(1), 143–153.
Prinstein, M. J., Boergers, J., & Vernberg, E. M. (2001). Overt and relational aggression in adolescents: Social-psychological adjustment of aggressors and victims. Journal of Clinical Child & Adolescent Psychology, 30(4), 479–491. https://doi.org/10.1207/s15374424jccp3004_05
Prinstein, M. J., & Cillessen, A. H. (2003). Forms and functions of adolescent peer aggression associated with high levels of peer status. Merrill-Palmer Quarterly (1982-), 49(3), 310–342. https://doi.org/10.1353/mpq.2003.0015
Rondon, A. T., Hilton, D. C., Jarrett, M. A., & Ollendick, T. H. (2020). Sleep, internalizing problems, and social withdrawal: Unique associations in clinic-referred youth with elevated sluggish cognitive tempo symptoms. Journal of Attention Disorders, 24(4), 524–534. https://doi.org/10.1177/1087054718756197
Sáez, B., Servera, M., Burns, G. L., & Becker, S. P. (2019). Advancing the multi-informant assessment of sluggish cognitive tempo: Child self-report in relation to parent and teacher ratings of SCT and impairment. Journal of Abnormal Child Psychology, 47(1), 35–46. https://doi.org/10.1007/s10802-018-0436-4
Selig, J. P., & Preacher, K. J. (2009). Mediation models for longitudinal data in developmental research. Research in Human Development, 6(2–3), 144–164.
Servera, M., Bernad, M. D. M., Carrillo, J. M., Collado, S., & Burns, G. L. (2016). Longitudinal correlates of sluggish cognitive tempo and ADHD-inattention symptom dimensions with Spanish children. Journal of Clinical Child and Adolescent Psychology, 45(5), 632–641. https://doi.org/10.1080/15374416.2015.1004680
Servera, M., Sáez, B., Burns, G. L., & Becker, S. P. (2018). Clinical differentiation of sluggish cognitive tempo and attention-deficit/hyperactivity disorder in children. Journal of Abnormal Psychology, 127(8), 818–829. https://doi.org/10.1037/abn0000375
Sheppard, C. S., Giletta, M., & Prinstein, M. J. (2019). Peer victimization trajectories at the adolescent transition: Associations among chronic victimization, peer-reported status, and adjustment. Journal of Clinical Child & Adolescent Psychology, 48(2), 218–227. https://doi.org/10.1080/15374416.2016.1261713
Sibley, M. H., Pelham, W. E., Molina, B. S. G., Gnagy, E. M., Waschbusch, D. A., Garefino, A. C., Kuriyan, A. B., Babinski, D. E., & Karch, K. M. (2012). Diagnosing ADHD in adolescence. Journal of Consulting and Clinical Psychology, 80(1), 139–150. https://doi.org/10.1037/a0026577
Sinclair, K. R., Cole, D. A., Dukewich, T., Felton, J., Weitlauf, A. S., Maxwell, M. A., Tilghman-Osborne, C., & Jacky, A. (2012). Impact of physical and relational peer victimization on depressive cognitions in children and adolescents. Journal of Clinical Child & Adolescent Psychology, 41(5), 570–583.
Smith, Z. R., & Langberg, J. M. (2017). Predicting academic impairment and internalizing psychopathology using a multidimensional framework of sluggish cognitive tempo with parent- and adolescent reports. European Child & Adolescent Psychiatry, 26(9), 1141–1150. https://doi.org/10.1007/s00787-017-1003-1
Smith, Z. R., Eadeh, H.-M., Breaux, R. P., & Langberg, J. M. (2019). Sleepy, sluggish, worried, or down? The distinction between self-reported sluggish cognitive tempo, daytime sleepiness, and internalizing symptoms in youth with attention-deficit/hyperactivity disorder. Psychological Assessment, 31(3), 365–375.
Smith, Z. R., Zald, D. H., & Lahey, B. B. (2020). Sluggish cognitive tempo and depressive symptoms in children and adolescents predict adulthood psychopathology. Journal of Abnormal Child Psychology, 48(12), 1591–1601. https://doi.org/10.1007/s10802-020-00692-x
Smith, Z. S., & Langberg, J. M. (2020). Do sluggish cognitive tempo symptoms improve with school‐based ADHD interventions? Outcomes and predictors of change. Journal of Child Psychology and Psychiatry, 61(5), 575–583. https://doi.org/10.1111/jcpp.13149
Somerville, L. H. (2013). The teenage brain: Sensitivity to social evaluation. Current Directions in Psychological Science, 22(2), 121–127. https://doi.org/10.1177/0963721413476512
Sonnby, K., Skordas, K., Olofsdotter, S., Vadlin, S., Nilsson, K. W., & Ramklint, M. (2015). Validation of the World Health Organization adult ADHD self-report scale for adolescents. Nordic Journal of Psychiatry, 69(3), 216–223. https://doi.org/10.3109/08039488.2014.968203
Stapinski, L. A., Araya, R., Heron, J., Montgomery, A. A., & Stallard, P. (2015). Peer victimization during adolescence: Concurrent and prospective impact on symptoms of depression and anxiety. Anxiety, Stress, & Coping, 28(1), 105–120. https://doi.org/10.1080/10615806.2014.962023
Sweeting, H., Young, R., West, P., & Der, G. (2006). Peer victimization and depression in early-mid adolescence: A longitudinal study. British Journal of Educational Psychology, 76(3), 577–594. https://doi.org/10.1348/000709905x49890
Timmermanis, V., & Wiener, J. (2011). Social correlates of bullying in adolescents with attention-deficit/hyperactivity disorder. Canadian Journal of School Psychology, 26(4), 301–318. https://doi.org/10.1177/0829573511423212
Wechsler, D. (2011). WASI-II: Wechsler abbreviated scale of intelligence. PsychCorp.
Weller, E., Weller, R., Teare, M., & Fristad, M. (1999). Parent version-children’s interview for psychiatric syndromes (P-ChIPS). American Psychiatric.
Willcutt, E. G., Chhabildas, N., Kinnear, M., Defries, J. C., Olson, R. K., Leopold, D. R., Keenan, J. M., & Pennington, B. F. (2014). The internal and external validity of sluggish cognitive tempo and its relation with DSM–IV ADHD. Journal of Abnormal Child Psychology, 42(1), 21–35. https://doi.org/10.1007/s10802-013-9800-6
Wolke, D., Woods, S., & Samara, M. (2009). Who escapes or remains a victim of bullying in primary school? British Journal of Developmental Psychology, 27(4), 835–851.
Wolraich, M. L. (2003). Psychometric properties of the Vanderbilt ADHD diagnostic parent rating scale in a referred population. Journal of Pediatric Psychology, 28(8), 559–568. https://doi.org/10.1093/jpepsy/jsg046
Wolraich, M. L., Feurer, I. D., Hannah, J. N., Baumgaertel, A., & Pinnock, T. Y. (1998). Obtaining systematic teacher reports of disruptive behavior disorders utilizing DSM-IV. Journal of Abnormal Child Psychology, 26(2), 141–152.
Xie, H., Swift, D. J., Cairns, B. D., & Cairns, R. B. (2002). Aggressive behaviors in social interaction and developmental adaptation: A narrative analysis of interpersonal conflicts during early adolescence. Social Development, 11(2), 205–224. https://doi.org/10.1111/1467-9507.00195
Funding
This research was supported by award number R305A160126 from the Institute of Education Sciences (IES), U.S. Department of Education. The content is solely the responsibility of the authors and does not necessarily represent the official views of the IES.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interests
The authors declare no potential conflicts of interest with respect to the research, authorship, or publication of this article.
Ethical Approval
The study was approved by the Instiutional Review Boards at Cincinnati Children's Hospital Medical Center and Virginia Commonwealth University. The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Informed Consent
Informed consent was obtained from all individual participants in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fredrick, J.W., Langberg, J.M. & Becker, S.P. Longitudinal Association of Sluggish Cognitive Tempo with Depression in Adolescents and the Possible Role of Peer Victimization. Res Child Adolesc Psychopathol 50, 809–822 (2022). https://doi.org/10.1007/s10802-022-00923-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10802-022-00923-3