Abstract
Background
Both obesity and inflammatory bowel disease (IBD) are highly prevalent in Western societies. IBD, including Crohn’s disease (CD) and ulcerative colitis (UC), has been historically associated with cachexia and malnutrition. It is uncertain how obesity, a chronic pro-inflammatory state, may impact the course of IBD.
Aim
The aim of this study was to report the prevalence of obesity in patients with IBD in a metropolitan US population and to assess the impact of obesity on disease phenotypes, treatment, and surgical outcomes in IBD patients.
Methods
We reviewed the medical records of patients identified from the IBD registries of the Dallas Veterans Affairs Medical Center and Parkland Health and Hospital Systems who were seen from January 1, 2000, to December 31, 2012.
Results
Of 581 identified IBD patients, 32.7 % were obese (BMI ≥ 30) and 67.6 % were non-obese (BMI < 30). There were 297 (51.1 %) patients with CD and 284 (48.9 %) patients with UC. The rate of obesity was 30.3 % among CD patients and 35.2 % among UC patients. Overall, obese patients were significantly less likely to receive anti-TNF treatment, undergo surgery, or experience a hospitalization for their IBD than their non-obese counterparts (55.8 vs. 72.1 %, p = .0001).
Conclusion
Obesity is highly prevalent in our IBD patients, paralleling the obesity rates in the US population. Clinical outcomes were significantly different in obese versus non-obese patients with IBD. Despite the plausible mechanisms whereby obesity might exacerbate IBD, we have found that obesity (as defined by BMI) is a marker of a less severe disease course in IBD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Worldwide, the incidence of inflammatory bowel disease (IBD), including Crohn’s disease (CD) and ulcerative colitis (UC), has been rising over the last 50 years. The highest IBD incidence rates are in developed countries, mainly northern Europe, the UK, and North America [1]. Obesity rates also have increased significantly over this same time period in these countries, especially in the USA [2, 3]. While recent data suggest that the prevalence of obesity may be reaching a plateau in this country, 35.5 % of adult American men and 35.8 % of adult American women presently are obese [body mass index (BMI) ≥ 30 kg/m2] [4].
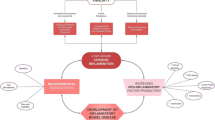
IBD once was associated with weight loss [5] and low body weight [6], but recent studies have documented a growing prevalence of obesity in IBD patients [7–9]. There is reason to suspect that obesity might contribute to gut inflammation in IBD. For example, lymphocytes and macrophages in adipose tissue produce pro-inflammatory cytokines (e.g., IL-6 and TNF) [10, 11] that might promote inflammatory responses in the gut of obese patients. It has also been observed that an increase in zonulin, a marker of increased intestinal permeability, is associated with excess adiposity [12]. The contribution of these putative mechanisms to IBD in obese patients is unclear.
Relatively few studies have investigated the clinical impact of obesity on IBD, with most focused on CD. Adult patients who have CD associated with a high BMI are reported to have a predilection for an anoperineal disease phenotype, an increased risk of hospitalizations [13], and earlier surgery [14] than their thinner counterparts. Similarly, one study in the USA has found that obese children with IBD have an increased need for surgery [7], and a retrospective case–control study has described a positive association between obesity and the development of CD [15]. Conversely, a study of hospitalized children with IBD found no associations between obesity, length of stay, need for surgery, and overall complication rates [16]. Another recent prospective case–control study found that a high BMI in CD is associated with a state of wellness [8]. Unfortunately, studies on the impact of obesity on IBD have been limited by small sample sizes and modest statistical associations, and the findings of these studies often are not reliably replicated.
Better studies are needed to define the impact of obesity on IBD. This might be especially important because IBD therapies (including immunomodulators and biologicals) often are dosed according to weight. The goals of our study were to determine the prevalence of obesity in our large population of adult patients with IBD and to assess the impact of obesity on disease phenotypes and clinical outcomes.
Methods
Study Design and Population
We reviewed the medical records of patients in the IBD databases of the Dallas Veterans Affairs Medical Center (DVAMC) and Parkland Health and Hospital Systems (PHHS) who were seen from January 1, 2000, to December 31, 2012. The Dallas VA IBD database was established in 2008, and the Parkland IBD database was established in 2011. Both databases include all patients with confirmed IBD (as determined by clinical presentation, endoscopic and/or radiological evidence, and pathologic evidence of the disease) seen in the gastroenterology and/or IBD clinics at the Dallas VA or Parkland Hospital, respectively. Data included in these databases have been collected both retrospectively at creation and prospectively since that time. This study was approved by the institutional review board of both the DVAMC and PHHS. Patients were excluded if, on any follow-up visit, a gastroenterology staff physician or an investigator refuted the IBD diagnosis based on clinical history, endoscopy, or histology as documented in the electronic health record. Patients also were excluded if they were <18 years of age or if they had <6 months of follow-up or less than two recorded weights.
Definition of Obese and Non-obese Patients
The average BMI during the period of follow-up was calculated for each patient. Obesity was defined as BMI ≥ 30 kg/m2, overweight as 25–29.9 kg/m2, normal as 18.5–24.9 kg/m2, and underweight as <18.5 kg/m2.
Definitions of Variables and Outcomes
The following data were recorded for all eligible patients: age, sex, race, family history of IBD, tobacco use, Montreal classification [17] (including age of diagnosis, disease location, behavior, and extent), disease duration (determined from time of first diagnosis), IBD medication history, IBD-related surgeries (including colon and intestinal resection, stoma-related surgery, pouch creation or revision, and perianal surgery that involved incision and drainage of abscess, seton placement, examination under anesthesia with stricture dilation, and fistulotomy), time from IBD diagnosis to first IBD-related surgery, IBD-related hospitalizations (including flares or acute disease exacerbation, symptomatic anemia, gastrointestinal bleeding, gastrointestinal infections, complications related to medications, surgeries, poor nutritional state, and iatrogenic interventions), and disease exacerbations or flares. The follow-up period was defined as the time from the first gastroenterology encounter (either in the inpatient or in the outpatient setting) that was electronically documented to the last GI encounter documented within the study dates.
The primary outcome of this study is the development of indicators of moderate-to-severe IBD defined here as the need for anti-TNF therapy, need for an IBD-related surgery, or need for an IBD-related hospitalization at any point in the disease course.
Statistical Analysis
Analyses were performed utilizing SAS for Linux version 9.2 (SAS Institute Inc., Cary, NC, USA) and SPSS 21 for Windows (IBM, New York, New York). Categorical data items were summarized utilizing frequency counts and percentages, while means and standard deviations were calculated for age, age at diagnosis, disease duration, and total surgeries. Pearson Chi-squares were computed for group comparisons of each of the categorical measurements and independent samples t tests or Mann–Whitney U tests for two independent groups for the continuous variables such as age. The three groups categorized by BMI (normal/underweight, overweight, and obese) were compared using Chi-square testing. Multiple logistic regression models using the macro by Bursac et al. [18] were utilized to determine which factors were statistically related to the combined outcome in the two separate diagnosis groups. The SAS algorithm by Bursac et al. automates the variable selection process for multiple logistic regression analysis. Any variable having a significant univariate test at the p value of .25 is selected as a candidate for the multivariate analysis. In the iterative process of variable selection, covariates are removed from the model if they are nonsignificant and not a confounder. Significance is evaluated at the .1 alpha level and confounding as a change in any parameter estimate >15 %. Any that are significant at the .1 level are put in the model, and the model is iteratively reduced as before, but only for the variables that were additionally added.
Ethical Considerations
This study was approved by the institutional review boards of both the Dallas VA Medical Center and the Parkland Health and Hospital System.
Results
Obesity Is Highly Prevalent in Our IBD Patients
We reviewed the medical records of 733 total patients; 152 did not meet entry criteria, all due to not having at least 6 months of follow-up. Among the 581 eligible IBD study patients (307 from the Dallas VA, 274 from Parkland Hospital), 174 (29.9 %) were normal weight, 15 (2.6 %) were underweight, 202 (34.8 %) were overweight, and 190 (32.7 %) were obese. Rather than having an underweight group with numbers too small for meaningful comparisons, the normal weight and underweight patients are combined into a single group for subsequent analyses. Altogether, there were 297 (51.1 %) patients with CD and 284 (48.9 %) patients with UC. Among them, 30.3 % of CD patients and 35.2 % of UC patients were obese (Table 1). Interestingly, the prevalence of obesity in our Dallas metropolitan area IBD patients is comparable to that reported for the general population in Texas (Fig. 1). The majority of the patients were male, reflecting the predominately male VA cohort. There were no statistically significant differences in the racial background or tobacco use between obese, overweight, and normal/underweight IBD patients. However, IBD was diagnosed at an older age in obese patients as compared to underweight/normal patients (41.1 vs. 33.8 years, p < .0001, see Table 1). The overweight patients were significantly more likely to have a family history of IBD than the other groups (p = .046).
Prevalence of obesity in patients with inflammatory bowel disease. 2011 Centers for Disease Control Behavioral Risk Factor Surveillance System (BRFSS) data report 30.4 % (CI 29.1, 31.8) obesity (body mass index, BMI ≥ 30) prevalence in Texas (dashed line). (http://www.cdc.gov/obesity/data/adult.html)
Outcomes of Obese, Overweight, and Normal/Underweight IBD Patients
Compared to normal/underweight patients, overweight and obese patients had significantly less exposure to antibiotics (26 and 30 % for overweight and obese, respectively, vs. 43 % for normal/underweight), steroids (61 and 61 vs. 74 %), and anti-TNF therapy (26 and 25 vs. 43 %). Chi-square analyses revealed that the comparisons of these variables between obese patients and normal/underweight patients were significant (p < .01) as well as between overweight patients and normal/underweight patients (p < .01). However, there were no significant differences between overweight and obese patients in antibiotic use, steroids, and anti-TNF therapy.
Compared to normal/underweight patients, overweight and obese patients had less surgery (41 and 51 vs. 61 %) and were significantly less likely to be hospitalized during the last decade (44 and 42 vs. 66 %; Table 2). Chi-square analyses revealed that the comparison of the likelihood of hospitalization between obese patients and normal/underweight patients was significant (p < .0001) as well as between overweight patients and normal/underweight patients (p < .0001). There was no significant difference between overweight and obese patients in the likelihood of hospitalization (p = .852). The comparison of the likelihood of surgery between obese patients and normal/underweight patients was significant (p = .005), but there was no significant difference in the likelihood of surgery between overweight patients and normal/underweight patients (p = .164), nor between obese and overweight patients (p = .152).
Overall, overweight and obese patients were significantly less likely to receive anti-TNF treatment, undergo surgery, or experience a hospitalization for their IBD than their normal/underweight counterparts (62 and 56 vs. 83 %). Chi-square analyses revealed that the comparison of the likelihood of this composite outcome between obese patients and normal/underweight patients was significant (p < .0001) as well as between overweight patients and normal/underweight patients (p < .0001). There was no significant difference between overweight and obese patients in the likelihood of the composite outcome (p = .185).
For the 297 CD patients (Table 3), there were no significant differences in Montreal age class at the time of diagnosis, CD behavior or location, and upper gastrointestinal and perianal involvement between obese, overweight, and normal/underweight patients with CD. Overweight and obese CD patients had less exposure to steroids, antibiotics, and anti-TNF agents (36 and 38 vs. 60 %) than normal/underweight CD patients. Chi-square analyses revealed that the comparisons of these variables between obese patients and normal/underweight patients were significant (p < .01) as well as between overweight patients and normal/underweight patients (p < .01). However, there were no significant differences between overweight and obese patients in antibiotic use, steroids, and anti-TNF therapy. Moreover, there were fewer obese and overweight CD patients who had at least one surgery (41 and 52 vs. 61 %). The comparison of the likelihood of surgery between obese patients and normal/underweight patients was significant (p = .005), but there was no significant difference in the likelihood of surgery between overweight patients and normal/underweight patients (p = .164), nor between obese and overweight patients (p = .152). For obese and overweight patients, the likelihood of hospitalization was lower compared to normal or underweight CD patients (43 and 54 vs. 72 %). Chi-square analyses revealed that the comparison of the likelihood of hospitalization between obese patients and normal/underweight patients was significant (p = .009) as well as between overweight patients and normal/underweight patients (p < .0001). There was no significant difference between overweight and obese patients in the likelihood of hospitalization (p = .13). Overall, obese or overweight CD patients were less likely to have had either anti-TNF use, surgery, or hospitalization during the last decade (77 and 73 vs. 94 %). Chi-square analyses revealed that the comparison of the likelihood of this composite outcome between obese patients and normal/underweight patients was significant (p < .0001) as well as between overweight patients and normal/underweight patients (p < .0001). There was no significant difference between overweight and obese patients in the likelihood of the composite outcome (p = .585).
For the 284 UC patients (Table 4), there were no significant differences between obese, overweight, and normal/underweight UC patients in disease extent, tobacco use, and medications, including anti-TNF use. The number of patients with colectomy was not significantly different. However, there were significantly fewer obese or overweight UC patients who had at least one hospitalization as compared to normal/underweight UC patients (44 and 31 vs. 58 %). For obese and overweight patients, the likelihood of hospitalization was lower compared to normal or underweight CD patients (43 and 54 vs. 72 %). Chi-square analyses revealed that the comparison of the likelihood of hospitalization between obese patients and normal/underweight patients was significant (p < .0001). There was no significant difference between overweight patients and normal/underweight patients (p = .054), nor between overweight and obese patients in the likelihood of hospitalization (p = .086). Overall, overweight and obese UC patients were less likely to have had anti-TNF use or surgery or experienced hospitalization than obese UC patients (49 and 40 vs. 67 %). Chi-square analyses revealed that the comparison of the likelihood of this composite outcome between obese patients and normal/underweight patients was significant (p < .0001) as well as between overweight patients and normal/underweight patients (p = .014). There was no significant difference between overweight and obese patients in the likelihood of the composite outcome (p = .221).
Predictors of Outcomes in UC and Crohn’s Disease
The predictors of the composite outcome that were tested in patients with Crohn’s disease included age at diagnosis, ethnicity (white, black, and Hispanic), gender, duration of disease, BMI category, family history of IBD, use of tobacco, location of disease (ileal, colonic, or ileocolonic), and presence of disease in perianal or upper GI tract. As shown in Table 5, the final model retained six predictors. Age at diagnosis, having a colonic location of disease, being overweight, and being obese were protective risk factors against experiencing one of the outcomes, after being adjusted for the other predictors in the model. Current tobacco use and having disease in the perianal area were associated with an increased risk of experiencing one of the outcomes, after being adjusted for the other predictors in the model. The Hosmer and Lemeshow goodness-of-fit test was nonsignificant (χ 2(8) = 8.39, p = .40), indicating that the final model is replicable and well calibrated.
The predictors of the composite outcome that were tested in patients with UC included age at diagnosis, ethnicity (white, black, and Hispanic), gender, duration of disease, BMI category, family history of IBD, use of tobacco, and extent of disease (proctitis, extensive, or left-sided). As shown in Table 5, the final model retained seven predictors. Age at diagnosis, ethnic minority status, disease duration, proctitis, left-sided disease, being overweight, and being obese were protective risk factors against experiencing one of the outcomes, after being adjusted for the other predictors in the model. The Hosmer and Lemeshow goodness-of-fit test was nonsignificant (χ 2(8) = 6.83, p = .55), indicating that the final model is replicable and well calibrated.
Discussion
Although IBD once was considered a disorder associated with low body weight [6], we have documented a prevalence of obesity in our current IBD patients that mirrors the high rate of obesity in the general population. Indeed, the majority (68 %) of our 581 IBD patients were either overweight or obese, and only a small minority (2.6 %) were underweight. The frequency of obesity in our IBD patients (32.7 %) is similar to the frequency of obesity in the general population of Texas (30.4 %) reported by the Centers for Disease Control Behavioral Risk Factor Surveillance System in 2011 (Fig. 1).
One of the earliest studies (1974–2000) to describe obesity in IBD patients found that only 3.6 % of 2065 French patients with CD were either overweight or obese (BMI ≥ 25) [13]. In contrast, more recent studies on this issue have found results similar to ours with relatively high rates of obesity in both pediatric [7, 19] and adult IBD patients [8, 20]. The rise in the prevalence of IBD in Western countries has not been as dramatic as the rise in the prevalence of obesity. This suggests that obesity is not contributing to the pathogenesis of IBD and that the increase in the frequency of obesity in IBD patients merely reflects the rising frequency of obesity in the general population. In support of this contention, a recent European epidemiologic study has found no association between high BMI and the development of IBD [21].
Obesity is a pro-inflammatory state that conceivably might contribute to inflammation in IBD [22]. Indeed, the mesenteric fat of patients with CD overexpresses pro-inflammatory substances including C-reactive protein (CRP), TNF [11], and various adipokines [10, 23]. However, relatively few studies have explored the clinical impact of obesity on IBD, with conflicting results [6, 11, 12, 20].
Two frequently cited reports, one from France (1974–2000) and one from the USA (1997–2002), describe a positive association between obesity and the severity of CD [13, 14]. Both of these studies were conducted at a time when biologic therapy for IBD either was not available or was in its infancy. Infliximab was the first biologic therapy to receive approval by the Food and Drug Administration (FDA) for the treatment of CD in 1998, and such anti-TNF therapy is believed to change the natural history of IBD in selected patients [24]. Thus, it is important in clinical IBD studies to include a time period relevant to our current practice in which biologicals are used frequently. The aforementioned clinical studies that predated the widespread use of biologicals found that obese patients (defined as BMI ≥ 25) had more disease activity, more anoperineal disease, older age at diagnosis, and a shorter time to first surgery than non-obese patients [13, 14]. Unlike our study, however, both of those studies were relatively small (including only 110 patients between the two studies), and the alleged increased risk of early surgery (arguably the more important clinical outcome) was the result of a comparison between only 10 patients with BMI ≤ 18.5 and only 48 patients with BMI ≥ 25 [14].
Two studies that investigated the influence of obesity on anti-TNF use (one study just in CD patients and one in both UC and CD patients) found that obese patients required more dose escalations and/or had earlier loss of response to anti-TNF treatment than non-obese patients [25, 26]. In contrast, our study found that obese and overweight IBD patients had significantly less use of anti-TNF therapy than normal or underweight patients. We also found that obese and overweight IBD patients were less likely to have had at least one surgery or hospitalization (41 vs. 52 vs. 61 %, p = .02 and 42 vs. 44 vs. 66 %, p < .0001). This held true on subgroup analysis of CD patients separately for all end points. For UC, only hospitalizations were significantly different (31 vs. 44 vs. 58 %, p = .001). The reason for the disparity between our results and the results of these earlier studies is not clear.
We have found that IBD is more severe in non-obese patients in our cohort. One possible explanation for this phenomenon is that a low BMI promotes IBD activity while a high BMI protects against it. It seems more likely, however, that a low BMI is the result rather than the cause of IBD activity and that obesity is merely a reflection of less aggressive or less severe IBD. Our results are supported by the findings of a recent study from Ireland, which found that obese or overweight patients with CD had an overall less aggressive disease course [8]. Despite the plausible mechanisms for how obesity might exacerbate IBD, our study suggests that obesity is not a risk factor for IBD severity.
Our study has a number of strengths. First, ours is the largest series of obese and overweight patients with IBD reported to date. Moreover, compared to a number of earlier studies, we used stricter criteria for obesity, restricting that diagnosis to patients with a BMI ≥ 30, and considered overweight patients with BMIs between 25 and 29.9 separately. Furthermore, unlike earlier reports, our study includes many obese patients with UC in addition to CD, and ours is the first to describe the influence of obesity on IBD in the era of frequent anti-TNF use.
Our study also has a number of limitations, most notably its retrospective nature. Moreover, BMI itself has limitations and has been reported to have a poor linear relationship with total body fat [27]. Other measures of body fat such as skinfold measurements, waist-to-hip ratio, and waist circumference were not available for our patients. Thus, we do not have a surrogate measurement of mesenteric fat, which might be more important as a contributor to inflammation than subcutaneous fat [23]. To our knowledge, there has been no study investigating the relationship between BMI and visceral fat in UC and CD. One study found the ratio of visceral to subcutaneous fat (as measured by CT imaging) to correlate with complicated CD [28], but this was not correlated with BMI. It has been proposed that there is heterogeneity in the microcirculation in visceral and subcutaneous fat depots resulting in different inflammatory phenotypes [29]. Future studies should explore the relationship of BMI to visceral fat as measured by anthropometric measurements or imaging, or better still, the impact of visceral fat alone in CD and UC.
In summary, we have shown that, in our population of IBD patients in whom obesity is prevalent, there are significant differences in clinical outcomes between obese and non-obese patients with both CD and UC. Despite the plausible mechanisms whereby obesity might exacerbate IBD, we have found that obesity (as defined by BMI) is a marker of a less severe disease course in IBD.
References
Cosnes J, Gower-Rousseau C, Seksik P, Cortot A. Epidemiology and natural history of inflammatory bowel diseases. Gastroenterology. 2011;140:1785–1794.
Ogden CL, Carroll MD, Kit BK, Flegal KM. Prevalence of obesity in the United States, 2009–2010. NCHS Data Brief. 2012;82:1–8.
Flegal KM, Carroll MD, Ogden CL, Curtin LR. Prevalence and trends in obesity among US adults, 1999–2008. JAMA. 2010;303:235–241.
Flegal KM, Carroll MD, Kit BK, Ogden CL. Prevalence of obesity and trends in the distribution of body mass index among US adults, 1999–2010. JAMA. 2012;307:491–497.
Both H, Torp-Pedersen K, Kreiner S, Hendriksen C, Binder V. Clinical appearance at diagnosis of ulcerative colitis and Crohn’s disease in a regional patient group. Scand J Gastroenterol. 1983;18:987–991.
Ferguson A, Sedgwick DM. Juvenile onset inflammatory bowel disease: height and body mass index in adult life. BMJ (Clinical research ed). 1994;308:1259–1263.
Long MD, Crandall WV, Leibowitz IH, et al. Prevalence and epidemiology of overweight and obesity in children with inflammatory bowel disease. Inflamm Bowel Dis. 2011;17:2162–2168.
Nic Suibhne T, Raftery TC, McMahon O, Walsh C, O’Morain C, O’Sullivan M. High prevalence of overweight and obesity in adults with Crohn’s disease: associations with disease and lifestyle factors. J Crohn’s Colitis. 2013;7:e241–e248.
Moran GW, Dubeau MF, Kaplan GG, Panaccione R, Ghosh S. The increasing weight of Crohn’s disease subjects in clinical trials: a hypothesis-generatings time-trend analysis. Inflamm Bowel Dis. 2013;19:2949–2956.
Wozniak SE, Gee LL, Wachtel MS, Frezza EE. Adipose tissue: the new endocrine organ? A review article. Dig Dis Sci. 2009;54:1847–1856.
Hotamisligil GS, Arner P, Caro JF, Atkinson RL, Spiegelman BM. Increased adipose tissue expression of tumor necrosis factor-alpha in human obesity and insulin resistance. J Clin Invest. 1995;95:2409–2415.
Moreno-Navarrete JM, Sabater M, Ortega F, Ricart W, Fernandez-Real JM. Circulating zonulin, a marker of intestinal permeability, is increased in association with obesity-associated insulin resistance. PloS One. 2012;7:e37160.
Blain A, Cattan S, Beaugerie L, Carbonnel F, Gendre JP, Cosnes J. Crohn’s disease clinical course and severity in obese patients. Clin Nutr. 2002;21:51–57.
Hass DJ, Brensinger CM, Lewis JD, Lichtenstein GR. The impact of increased body mass index on the clinical course of Crohn’s disease. Clin Gastroenterol Hepatol. 2006;4:482–488.
Mendall MA, Gunasekera AV, John BJ, Kumar D. Is obesity a risk factor for Crohn’s disease? Dig Dis Sci. 2011;56:837–844.
Zwintscher NP, Horton JD, Steele SR. Obesity has minimal impact on clinical outcomes in children with inflammatory bowel disease. J Pediatr Surg. 2014;49:265–268.
Silverberg MS, Satsangi J, Ahmad T, et al. Toward an integrated clinical, molecular and serological classification of inflammatory bowel disease: report of a working party of the 2005 Montreal world congress of gastroenterology. Can J Gastroenterol = Journal canadien de gastroenterologie. 2005;19:5–36.
Bursac Z, Gauss CH, Williams DK, Hosmer DW. Purposeful selection of variables in logistic regression. Source Code Biol Med. 2008;3:17.
Kugathasan S, Nebel J, Skelton JA, et al. Body mass index in children with newly diagnosed inflammatory bowel disease: observations from two multicenter North American inception cohorts. J Pediatr. 2007;151:523–527.
Steed H, Walsh S, Reynolds N. A brief report of the epidemiology of obesity in the inflammatory bowel disease population of Tayside, Scotland. Obes Facts. 2009;2:370–372.
Chan SS, Luben R, Olsen A, et al. Body mass index and the risk for Crohn’s disease and ulcerative colitis: data from a European Prospective Cohort Study (The IBD in EPIC Study). Am J Gastroenterol. 2013;108:575–582.
Karmiris K, Koutroubakis IE, Kouroumalis EA. The emerging role of adipocytokines as inflammatory mediators in inflammatory bowel disease. Inflamm Bowel Dis. 2005;11:847–855.
Peyrin-Biroulet L, Gonzalez F, Dubuquoy L, et al. Mesenteric fat as a source of C reactive protein and as a target for bacterial translocation in Crohn’s disease. Gut. 2012;61:78–85.
D’Haens GR. Top-down therapy for IBD: rationale and requisite evidence. Nat Rev Gastroenterol Hepatol. 2010;7:86–92.
Harper JW, Sinanan MN, Zisman TL. Increased body mass index is associated with earlier time to loss of response to infliximab in patients with inflammatory bowel disease. Inflamm Bowel Dis. 2013;19:2118–2124.
Bultman E, de Haar C, van Liere-Baron A, et al. Predictors of dose escalation of adalimumab in a prospective cohort of Crohn’s disease patients. Aliment Pharmacol Ther. 2012;35:335–341.
Chrysant SG, Chrysant GS. New insights into the true nature of the obesity paradox and the lower cardiovascular risk. J Am Soc Hypertens JASH. 2013;7:85–94.
Erhayiem B, Dhingsa R, Hawkey CJ, Subramanian V. Ratio of visceral to subcutaneous fat area is a biomarker of complicated Crohn’s disease. Clin Gastroenterol Hepatol. 2011; 9:684–687 e681.
Scalia R. The microcirculation in adipose tissue inflammation. Rev Endocr Metab Disord. 2013;14:69–76.
Acknowledgments
We would like to thank Dr. Stuart J. Spechler for his thoughtful review and helpful suggestions in the preparation of this manuscript.
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Flores, A., Burstein, E., Cipher, D.J. et al. Obesity in Inflammatory Bowel Disease: A Marker of Less Severe Disease. Dig Dis Sci 60, 2436–2445 (2015). https://doi.org/10.1007/s10620-015-3629-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-015-3629-5