Abstract
Purpose
The purpose of this study was to quantify the effect of clinically relevant open-wedge high tibial osteotomies on medial collateral ligament (MCL) strain and the resultant tibiofemoral contact mechanics during knee extension and 30° knee flexion.
Methods
Six human cadaveric knee joints were axially loaded (1 kN) in knee extension and 30° knee flexion. Strains at the anterior and posterior regions of the MCL were determined using strain gauges. Tibiofemoral contact mechanics (contact area, mean and maximum contact pressure) were investigated using pressure-sensitive sensors. Open-wedge osteotomy was performed using biplanar cuts and osteotomy angles of 5° and 10° were maintained using an external fixator. Tests were performed first with intact and then with dissected MCL.
Results
Nonparametric statistical analyses indicated a significant strain increase (p < 0.01) in the anterior and posterior fibres of the MCL with increasing osteotomy angle of up to 8.3% and 6.0%, respectively. Only after releasing the MCL the desired lateralisation of the mechanical axis was achieved, indicating a significant decrease in the maximum contact pressure in knee extension of − 25% (p = 0.028) and 30° knee flexion of − 21% (p = 0.027).
Conclusions
The results of the present biomechanical study suggest, that an open-wedge high tibial osteotomy is most effective in reducing the medial contact pressure when spreading the osteotomy to 10° and concomitantly releasing the MCL. To transfer the results of this biomechanical study to the clinical day-to-day practice, it is necessary to factor in the individual ligamentous laxity of each patient into the treatment options e.g. particularly for patients with distinct knee ligament laxity or medial ligamentary instability, the release of the MCL should be performed with care.
Level of evidence
Controlled laboratory study.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
High tibial osteotomy is an established treatment for osteoarthritis of the medial compartment of the knee [13, 25]. The aim of the procedure is to change the load distribution from the injured medial to the intact lateral compartment of the knee, which has been mainly investigated in vitro by assessing the contact pressure (CP) distribution on the tibial plateau [1, 5]. Clinical publications have shown good long-term results after high tibial osteotomy [6, 10, 17]. The classic procedure is the lateral closed wedge osteotomy. In the last years, medial opening-wedge osteotomy has gained popularity because the adjustment can be performed more accurate, additionally allows correction of the sagittal plane and eliminates the need for fibular osteotomy with the risk of peroneal nerve injury.
Whereas, the lateral closed wedge osteotomy has no or only minor effects on the medial collateral ligament medial opening-wedge high tibial osteotomy (OWHTO) increases strain of the superficial medial collateral ligament (sMCL). This is caused by the fact that the medial opening-wedge osteotomy is typically performed proximal of the distal attachment of the sMCL, therefore, the sMCL is tensioned when performing the osteotomy [14]. There is evidence in the literature that this over tensioning may lead to an undesired re-loading of the medial joint compartment [1, 20]. Therefore, clinically the sMCL is released, on the one hand indicating good results in lateralisation of the mechanical axis but, on the other hand, leading also to knee laxity [27]. This was underlined by biomechanical studies showing that the release of the sMCL must be kept to a minimum to decrease the potential of late valgus instability [20]. By contrast, Agneskirchner et al. [1] have shown, that for effective decompression of the medial compartment a complete release of the distal fibers of the MCL is necessary.
To our knowledge there is no study that analysed to what extent the anterior and posterior parts of the sMCL are tensioned under clinically relevant OWHTO angles of 5° and 10° combined with different knee flexion angles of 0° and 30°. Therefore, the aim of the present study was to investigate the strain of the sMCL after medial opening-wedge osteotomy under different loading conditions. Moreover, the relationship between these strains and the contact mechanics at the medial and lateral tibiofemoral joint could provide clinicians more information regarding partial or total release of the sMCL during OWHTO procedures. Because of the lack of knowledge related to the biomechanics of OWHTO, the following hypotheses were formulated:
-
i.
Increasing OWHTO angle increases the strains at both the anterior and posterior parts of the sMCL under knee extension and 30° knee flexion.
-
ii.
At the clinically relevant OWHTO angles of 5° and 10°, the anterior and posterior sMCL regions are equally strained in knee extension (0°) and the anterior sMCL portion is more strained than the posterior sMCL in knee flexion of 30°.
-
iii.
The loaded CA is not influenced by the OWHTO intervention.
-
iv.
An increased sMCL strain, caused by the intraligamentary approach of the OWHTO, results in unfavourable higher CP and maximum CP (CPmax) at both the medial and lateral joint compartments in knee extension and in 30° knee flexion.
-
v.
Only a release of the sMCL will lead to the desired decrease of the mean CP and CPmax at the medial compartment, and thus to an increase of the mean CP and CPmax at the lateral compartment, resulting in the lateralisation of the mechanical knee axis in knee extension and in 30° knee flexion.
Materials and methods
This experimental cadaveric study investigated the tibiofemoral mean CP and CPmax at six human lateral and medial knee joint compartments and the strains at the anterior (εant) and posterior sMCL (εpost) in knee extension (0°) and 30° knee flexion under a maximum axial joint load of 1000 N. Each knee was investigated with varying the osteotomy angle (0°, 5° and 10°) and the knee flexion (0° and 30°). To account for a potential methodology bias both, the osteotomy angle and the knee flexion states were randomized prior to testing. The knee joints were first tested with intact sMCL and then with dissected sMCL resulting in a total of 12 different test conditions for each knee.
Preparation
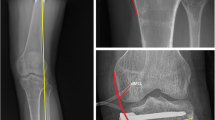
Six left human cadaveric legs (59.5 ± 6.5 years, 4 males) were obtained from an official tissue bank (Southeast Tissue Alliance, Gainesville, FL, USA). The specimens were thawed over 24 h at 4 °C before preparation. Prior to dissection, the joints were examined radiographically to ensure that they were not injured, operated or displayed severe signs of osteoarthritis. Additionally, the X-rays were used to determine the geometrical properties of the lower limb (Table 1) to plan the biplanar OWHTO cuts for each individual knee. Skin, muscles, subcutaneous tissue and the patella were removed, leaving the remaining capsuloligamentous structures intact. To stabilise the lateral collateral ligament, the fibula was cut to a length of 6 cm and fixed to the tibia using a tricortical screw. The bony ends of the tibia and femur were cut to a length of 20 cm from the knee joint gap and potted in polymethyl methacrylate (Technovit® 3040, Heraeus Kulzer GmbH, Wehrheim, Germany). The osteotomy was performed following the biplanar Stäubli method [25], while preserving a 1-cm lateral bony hinge. An external fixator (Modular rod system, Synthes GmbH, Oberdorf, Switzerland) was used in combination with an OWHTO bone spreader (TomoFix bone spreader, Synthes GmbH) to allow full control of the osteotomy angle throughout the procedure. To ensure repeatability of the surgical intervention, only one experienced senior orthopaedic surgeon performed all preparation steps and the same surgeon performed also each surgical modification throughout the biomechanical tests. Throughout the preparation and testing procedure, the specimens were kept moist with saline solution. Tests were performed to investigate the influence of the osteotomy cut itself on contact mechanics (CA, CP, CPmax) and the sMCL strains (εant, εpost), indicating no differences between the intact and osteotomised (0°) knee joint state. Therefore, the osteotomised knee joint state was defined as the initial state for further comparisons.
Measuring devices
Following anterior and posterior windowing of the capsule, the medial and lateral tibial plateau was equipped with a 1-mm thick Teflon sheet, which enhanced the placement of a calibrated thin, flexible pressure sensor in each joint compartment (K-Scan, pressure-mapping sensor 4000, 1500 psi, accuracy < 4%; Tekscan Inc., South Boston, USA). After correct submeniscal placement at the medial and lateral plateau, the Teflon sheet was removed. Subsequently, the sensors were secured using tape and two cortical screws, which were attached at the anterior and posterior proximal tibia (Fig. 1), preventing dislocation of the sensor. Sensor calibration was performed using a previously introduced setup [23] and a customised MATLAB-algorithm allowing a nine-point calibration covering the entire sensor bandwidth. This calibration method has been shown to be more precise for knee joint experiments compared to the manufacturer’s calibration [9]. Equilibration of the sensor maps was performed in accordance to the manufacturer’s guideline. Adequate repeatability (> 80%) of the mean CP and CPmax measurements on the lateral and medial joint compartments were acquired during pretests indicating reliable measurements. The anterior and posterior parts of the sMCL were equipped with two strain gauges (Microminiature LVDT 3; accuracy ± 0.1%; LORD Corp., Williston, USA) by means of barbed pins at the level of the medial knee joint gap to assess the strains at the anterior (εant) and posterior sMCL (εpost) (Fig. 2). During pretests high repeatability (> 85%) of the strain measurements were acquired also indicating reliable measurements. Zero-strain references of both sensors were determined after reaching a previously defined axial knee joint preload of 50 N at either full knee extension (0°) or 30° knee flexion. Synchronised data acquisition of the pressure measurements, sMCL strain measurements and machine data from the materials testing machine was achieved using customised software (LabVIEW, National Instruments, Austin, USA). Further, reliability of the measurements was checked during pretests.
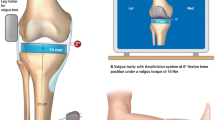
Position of the strain gauges (M-DVRT 3, Lord Corp., USA) at the level of the knee joint gap. The blue sensor measures the anterior (εant) and the green sensor the posterior (εpost) strain of the superficial medial collateral ligament (sMCL). The dark green triangle indicates the 5° osteotomy angle and the light green triangle the 10° osteotomy angle. The dashed line represents the frontal osteotomy at the Tuberositas tibiae. The photograph shows the positioning of the both DVRTs on the sMCL
Test setup
Following preparation, the joints were placed in a material testing machine (Z010, Zwick GmbH, Germany) using a customised setup (Fig. 3), which was described previously [23]. First, the tibial slope was individually adjusted perpendicular to the mechanical loading axis of the material testing machine. The varus–valgus axis, axial rotation and biplanar translation were left unconstrained to allow correct knee alignment. In doing so, the knee was able to optimise its tibiofemoral contact at a preload of 50 N, which was applied via the material testing machine. Subsequently, the varus–valgus axis of the tibia was fixed and the zero-strain references of the anterior and posterior sMCL were registered. In this manner, the tibia was constrained, while the femur was allowed to rotate along its longitudinal axis and translate in the sagittal and frontal planes.
Test protocol
To allow adjustment of the loading setup, control correct positioning and function of the pressure sensor and determine the zero-strain reference of the both sMCL strain gauges, the preload of 50 N was held under force-controlled conditions for 5 min. During this period, the viscoelastic structures of the knee were preconditioned by applying a creep load of 50 N. To account for the viscoelastic behaviour of the remaining knee soft tissues and to ensure measurement repeatability, three loading cycles from 50 to 1000 N were applied at a displacement-controlled loading speed of 4 mm/min. The maximum axial load of 1000 N was chosen to be comparable with the literature [1], which is equivalent to approximately 1.5 times body weight.
Randomisation of the tests were performed for the three osteotomy angles (0°, 5°and 10°) using an external fixator and for the knee flexion angle (0° and 30°), which was adjusted at the femoral jig. The tests were conducted first with intact sMCL. Based on the findings of Agneskircher et al. [1], and to maintain the statistical power of the study, we decided to perform a subsequent complete release of the sMCL. The study and corresponding testing protocol were approved by the local IRB board of the University of Ulm.
Statistical analyses
Based on the results of a similar study [1], a sample-size calculation (G*Power 3.1: α = 0.05, β = 0.2, δ = 30%, SD 25%; n = 5 [7]) was performed to ensure sufficient statistical power of the study. After feedback from the statistical department and because of the eventually observed lower effects, the sample size was increased to n = 6.
Gaussian distribution of the data was tested using Shapiro–Wilk test, resulting in non-normally distributed data. Therefore, non-parametric statistical analyses were performed using a statistical software package (SPSS V24, IBM Corp., Armonk, USA). A p value < 0.05 was considered statistically significant, while p value Bonferroni correction was applied where necessary. The two different knee flexion angles (0° and 30°) were analysed separately. Therefore, the previously formulated hypotheses were statistically evaluated as follows:
-
i.
Influence of the osteotomy angle (0°, 5° and 10°) on the strains at the anterior and posterior parts of the sMCL were investigated using a Friedman-test [two-factor analysis of variance (ANOVA)] followed by a post-hoc test when significant differences were observed.
-
ii.
Comparisons between anterior and posterior sMCL strains at 0°, 5° and 10° OWHTO angles were statistically elaborated using Wilcoxon tests.
-
iii.
Influence of the OWHTO angle (0°, 5°and 10°) on the lateral and medial CA were investigated using a Friedman-test (two-factor ANOVA) followed by a post-hoc test when significant differences were observed. Furthermore, comparisons of the lateral and medial CA before and after sMCL release at three osteotomy angles (0°, 5°and 10°) were statistically investigated using Wilcoxon tests.
-
iv.
Influence of the OWHTO angle (0°, 5° and 10°) on the lateral and medial CP and CPmax were investigated with intact sMCL using a Friedman-test (two-factor ANOVA) followed by a post-hoc test when significant differences were observed.
-
v.
Comparisons of lateral and medial CP and CPmax before and after sMCL release at three osteotomy angles (0°, 5° and 10°) were statistically investigated using Wilcoxon tests.
Results
Influence of the OWHTO angle on the anterior and posterior sMCL strains
Anterior and posterior sMCL strains steadily increased with increasing osteotomy angle in extension (p < 0.008) and flexion (p < 0.015; Fig. 4). Post-hoc testing indicated that increasing the OWHTO angle from 0° to 10° statistically increased both, the anterior sMCL (extension: p = 0.005; flexion: p = 0.005) and the posterior sMCL (extension: p = 0.008; flexion: p = 0.013).
Differences between the anterior and posterior sMCL strains
In knee extension, the strains of the anterior and posterior sMCL were similar. In 30° knee flexion only at an OWHTO angle of 10° the anterior sMCL was 7% significantly higher strained than the posterior sMCL (p = 0.043, Fig. 4).
Influence of the OWHTO and flexion angle on the CA
The tibiofemoral CA ranged between 309 and 466 mm2 at the lateral knee compartment and between 421 and 589 mm2 at the medial compartment (Table 2). With an intact sMCL, lateral CA decreased about 26% (p = 0.028) in knee extension and about 25.9% (p = 0.028) in 30° flexion when comparing the 0° OWHTO state with the 10° OWHTO state.
After sMCL release, the loaded area at the lateral knee compartment was reduced by 31% (p = 0.028) in knee extension and at 0° osteotomy angle (Table 2). At the medial knee compartment, we found a statistically significant reduction of CA for all OWHTO angles in both knee extension (p < 0.046) and 30° knee flexion (p < 0.046), with a maximum reduction of 40% (p = 0.046, knee extension, α = 10°).
Influence of the OWHTO angle on the mean CP and CPmax
At knee extension the lateral mean CP did not change with different osteotomy angles (Table 3), while at 30° knee flexion, the lateral mean CP decreased of 0.22 MPa (63%; p = 0.042) when comparing 0° with 10° osteotomy angle and of 0.19 MPa (54%; p = 0.018) when comparing 5° with 10° osteotomy angle. The medial mean CP was not influenced by OWHTO angle or knee flexion.
Only at 30° knee flexion the lateral CPmax significantly decreased of 22% (p = 0.028, Table 4) when comparing 0° and 5° OWHTO states and of 37% (p = 0.028) when comparing 0° and 10° osteotomy states. The medial CPmax was not influenced by the OWHTO angles.
Influence of sMCL release on lateral and medial CP and CPmax
In knee extension, the release of the sMCL resulted in a decrease in the lateral CP of 0.24 MPa (Table 3; p = 0.028). sMCL release had no effect the lateral CP at 5° OWHTO angle, but lateral CP statistically increased by 0.15 MPa (p = 0.046) at a 10° OWHTO angle. In knee extension, the sMCL release resulted in a significant medial CP decrease of 0.13 MPa (p = 0.028). In 30° knee flexion and 5° osteotomy angle, the lateral CP significantly decreased by 20% (p = 0.043) and at 10° osteotomy angle the medial CP decreased statistically by 17% (p = 0.043).
sMCL release decreased the lateral CPmax by 33% in the knee extension position and 0° osteotomy angle (p = 0.028, Table 4). At a 5° osteotomy state, no statistical differences were observed for the lateral or medial CPmax. In knee extension and 10° OWHTO angle, the lateral CPmax increased by 55%, whereas the medial CPmax was significantly decreased (25%; p = 0.028). At 30° knee flexion medial CPmax was significantly decreased at an OWHTO angle of 0° by 33% (p = 0.028) and at 10° OWHTO angle by 21% (p = 0.027).
Discussion
The most important finding of the present finding was that only after a release of the complete sMCL the desired lateralization of the tibiofemoral load was possible after an OWHTO. In other words, from a biomechanical view it is mandatory to release the sMCL to relief the medial joint compartment after OWHTO.
The study design presented here was appropriate to respond to the previously defined hypotheses: Hypothesis (I) was corroborated. Hypothesis (II) was partially corroborated and hypotheses (III), (IV) and (V) were disproved. With regard to the proposed hypotheses, there were four main findings in this biomechanical study: First, an increase of the osteotomy angle from 0° to 10° led to an increased anterior and posterior sMCL both in knee extension and 30° knee flexion. Second, the affected CA changed with increasing osteotomy angle and after release of the sMCL. Third, the CP decreased tendentially at the medial compartment after sMCL release. Fourth, the medial CPmax was mainly impacted after sMCL dissection at a 10° osteotomy angle, while the lateral CPmax underwent a directional change from a decrease in the native state, being consistent at a 5° OWHTO angle to an increase at the 10° state after sMCL dissection (Fig. 5).
Various clinical studies have confirmed the validity and effectiveness of the OWHTO for the treatment of varus gonarthrosis, reporting good to excellent outcomes [6, 10, 17].
On the other hand, there are only a few biomechanical studies investigating the impact of an OWHTO on the tibiofemoral CP and the strains acting in the MCL. Agneskircher et al. [1] demonstrated an increase of the tibiofemoral CP with increasing strains in the MCL. The authors concluded from their results, that an OWHTO without releasing the MCL might lead to a re-pressurization of the medial tibial plateau, thus preventing the desired lateralisation of the mechanical axis. In the present study, we similarly failed to find a decrease of the medial CP by OWHTO without MCL release, confirming Agneskircher et al.
Regarding MCL strains, there are only a few publications in the literature. Victor et al. [28] investigated the isometry of different knee ligaments during knee flexion. The MCL displayed isometric behaviour between knee extension and a knee flexion of 120°, revealing strains ranging from 0 to 2%. Arms et al. [3] found a mean MCL strain increase of up to 2% when applying a 15 N m external valgus moment at different knee flexion positions. Twenty years later, Gardiner et al. [8] performed a kinematic analysis using cadaveric knees, where they applied an external valgus load of 10 N m and detected a maximum MCL strain at the posterior femoral attachment of up to 7.4%. Furthermore, there is evidence that the long part of the sMCL appears to be the main part of the MCL resisting against valgus moments [22]: Robinson et al. found an increase from 3° to 9° of valgus laxity when dissecting the sMCL. By contrast, a tenotomy of the deep MCL did not result in greater valgus laxity. In conclusion, the authors stated that an undifferentiated MCL dissection might lead to an undesired increase of knee laxity. Our strain measurements showed a significant strain increase of both the anterior and posterior parts of the sMCL of + 3.8% and + 3.7% in knee extension and of + 4.7% and + 4.4% in 30° knee flexion, respectively, when spreading the osteotomy angle to 10°. This increase is less than those reported when applying a valgus moment of 10–15 N m [3, 8]. LaPrade et al. [12] investigated the impact of an OWHTO intervention on the posterolateral stability of the knee joint in a controlled laboratory study. They applied an external rotation moment and measured significantly greater forces at the MCL after a 10° OWHTO compared to the intact joint. The authors concluded that the MCL strain increase resulting after OWHTO might lead to reduced varus translation and an increased external rotation stability, finally leading to a higher knee joint stability, which might be reasonable to treat posterolateral instability. The strains reported in the LaPrade study [12] are in accordance with the findings of the current study.
However, in addition to the described possible improvement in knee joint stability, the proven strain increase of the sMCL after OWHTO might also lead to an undesired increased tibiofemoral joint pressure at the medial compartment. Riegger-Krugh et al. [21] were the first to compare knee joint pressures when applying external varus and valgus loads and combined closing-wedge osteotomy. One of their main findings was, that under an external varus load a 5° closing-wedge osteotomy did not reduce the loads at the medial knee compartment. However, not only did they use Fuji pressure measurement film to assess the tibiofemoral loads, which is known to allow only single pressure measurements, their loading apparatus did not provide six degrees of freedom. Therefore, by not preventing knee joint constraints, they may have loaded the knee in an unphysiological manner. Ogden et al. [18] compared the tibiofemoral load distribution occurring after closing- and open-wedge osteotomy procedures. They released the MCL when performing the OWHTO procedure. Both techniques resulted in a decrease in the medial CP. However, at a 5° angle, the closing-wedge techniques resulted in a significantly better unloading of the medial compartment. Comparisons after 10° osteotomy angle resulted in no difference between both techniques. The results of the present study with an open-wedge procedure indicate that only a release of the sMCL leads to the desired lateralisation of the mechanical axis and, therefore, to the pressure reduction at the medial joint compartment. After 5° and 10° OWHTO and under 1000 N axial load, we observed an increase of the CPmax (and CP) at the medial compartment in single cases of up to 204% (CP 39%) in knee extension and up to 241% (CP 37%) in 30° knee flexion. The CA was also increased after 10° OWHTO by 19% in 30° knee flexion. Only sMCL dissection resulted in the desired reduction of the medial compartment pressure (Tables 3 and 4), indicating a successful shifting of the mechanical axis to the lateral joint compartment. There was also a significant decrease of the medial CA after sMCL release of 40% and 16% in knee extension and 30° flexion, respectively. In contrast to our hypotheses, the measurements at the lateral joint compartment with a 10° OWHTO angle in knee extension (30° knee flexion) registered a 37% (39%) lower CP and a 45% (27%) lower CPmax. These were confirmed by the results of the CA measurements, where when comparing the intact and the 10° OWHTO states the lateral CA was decreased by 21% in knee extension and by 27% in 30° knee flexion. In summary, the results of our biomechanical study suggest that OWHTO is only successful when combined with a release of the sMCL. Without such a release, the outcome is exactly the opposite to the expected result, indicating an increase of the medial tibiofemoral pressure.
Our findings confirm those of Agneskircher et al. [1], who used a similar test setup to investigate the tibiofemoral CP after an OWHTO procedure. Accordingly, they found with intact MCL and under an axial load of 1000 N after OWHTO higher CPs at the medial compared to the lateral compartment. Agneskircher et al. assumed that this pressure increase on the medial compartment is associated with the elevation of the medial aspect of the tibial plateau. Furthermore, they concluded that because of the intraligamentary osteotomy, the tibia becomes more constrained. These assumptions are now confirmed by our investigations, showing an increase in the sMCL strain resulting in an undesired re-loading of the medial compartment of the tibia. The results of Mina et al. [16] also confirmed the suspected influence of the MCL tension on the intraarticular load distribution. The authors performed a high tibial osteotomy 2 cm distal to the Tuberositas tibiae, which is distal to the MCL insertion. In contrast to an intraligamentary bone cut without dissection of the MCL, their results showed a complete unloading of the medial joint compartment at an osteotomy angle of 6°–10° under an axial load of 200 N. Furthermore, at an OWHTO angle of 0°–4°, they detected a homogeneously distributed CP at the lateral and medial joint compartments.
The present study has some limitations, particularly with regard to daily clinical practice. One is the lack of physiological muscle force simulation, which might lead to higher tibiofemoral pressure. Because of the setup used, we assume that the knee was able to perform an adequate self-positioning with little or negligible constraints influencing the results under a pure axial load of 1000 N. This was also improved by maintaining several degrees of freedom during the repeated loading. However, we assume that the general trends both for the sMCL strain and the tibiofemoral CPs would be similar when the axial load would be increased to 2.5 × body weight, as seen during level walking [11]. The use of Tekscan pressure sensors for in vitro human knee joint analyses has been previously reported for the patellofemoral [26] and tibiofemoral joints [1, 5, 27]. The submeniscal placement of the sensors requires windowing of the meniscotibial coronary ligaments. In a study investigating different fixation techniques of meniscal allografts [2], it was shown that this dissection did not affect the tibiofemoral contact. DVRTs have been used in vitro to determine MCL strains [4, 15]. However, limitations were reported because of the restricted local measurement and their sensitivity to interference from surrounding tissue. By locally placing them at the anterior and posterior sMCL, we hoped to gain additional information on the influence of an OWHTO on altered load transmission by tensioning of the sMCL rather than assessing the complex strain distribution in the ligament. The DVRTs were directly anchored on the sMCL, thereby preventing the surrounding soft tissues from falsifying the measurements.
To transfer the results of this biomechanical study to the clinical day-to-day practice, it is necessary to factor in the individual ligamentous laxity of each patient into the treatment options. In particular, for patients suffering from anterior cruciate ligament insufficiency, the MCL is the most important anterior stabiliser of the knee [24]. In the presence of posterolateral instability, LaPrade et al. [12] indicated an OWHTO as a possible surgical treatment to improve the knee joint rotational stability [12, 19]. In both cases, a dissection of the MCL might lead to an increasing valgus instability of the knee and is, therefore, not recommended.
Therefore, prior to a release of the sMCL during OWHTO surgery, the intraligamentary situation of each patient requires assessment [20]. Particularly in patients with distinct knee ligament laxity or medial ligamentary instability, the MCL release should be performed with care.
Conclusions
The results of the present study corroborate the hypothesis of Agneskircher et al. [1], that a OWHTO without sMCL release does not lead to the desired lateralisation of the mechanical axis of the lower limb with the aim of relieving the pressure on the medial tibial plateau. Furthermore, the present study extends the findings to a knee flexion of 30° and adds information about the strains occurring in the sMCL at the clinically relevant OWHTO angles of 5° and 10°. Regarding these strains, we, in particular, investigated the 10° osteotomy state, where the sMCL strains were different in the anterior and posterior parts the more the knee was flexed. However, this is only hypothetical and needs to be further investigated in future studies. In conclusion, the results of the present study implicate that OWHTO is most effective in reducing medial CP when spreading the osteotomy to 10° with concomitant release of the sMCL.
Abbreviations
- CA:
-
Contact area mm2
- CP:
-
Contact pressure MPa
- CPmax :
-
Maximum (peak) contact pressure MPa
- ε ant :
-
Strain at the anterior part of sMCL %
- ε post :
-
Strain at the posterior part of sMCL %
- MCL:
-
Medial collateral ligament
- OWHTO:
-
Open wedge high tibial osteotomy
- sMCL:
-
Superficial medial collateral ligament
References
Agneskirchner JD, Hurschler C, Wrann CD, Lobenhoffer P (2007) The effects of valgus medial opening wedge high tibial osteotomy on articular cartilage pressure of the knee: a biomechanical study. Arthroscopy 23:852–861
Alhalki MM, Howell SM, Hull ML (1999) How three methods for fixing a medial meniscal autograft affect tibial contact mechanics. Am J Sports Med 27:320–328
Arms S, Boyle J, Johnson R, Pope M (1983) Strain measurement in the medial collateral ligament of the human knee: an autopsy study. J Biomech 16:491–496
Bates NA, Nesbitt RJ, Shearn JT, Myer GD, Hewett TE (2017) Knee abduction affects greater magnitude of change in ACL and MCL strains than matched internal tibial rotation in vitro. Clin Orthop Relat Res 475:2385–2396
Bode G, Kloos F, Feucht MJ, Fleischer B, Sudkamp N, Niemeyer P et al (2017) Comparison of the efficiency of an extra-articular absorber system and high tibial osteotomy for unloading the medial knee compartment: an in vitro study. Knee Surg Sports Traumatol Arthrosc 25:3695–3703
DeMeo PJ, Johnson EM, Chiang PP, Flamm AM, Miller MC (2010) Midterm follow-up of opening-wedge high tibial osteotomy. Am J Sports Med 38:2077–2084
Faul F, Erdfelder E, Lang AG, Buchner A (2007) G*Power 3: a flexible statistical power analysis program for the social, behavioral, and biomedical sciences. Behav Res Methods 39:175–191
Gardiner JC, Weiss JA (2003) Subject-specific finite element analysis of the human medial collateral ligament during valgus knee loading. J Orthop Res 21:1098–1106
Kang L, Baer TE, Rudert MJ, Pedersen DR, Brown TD (2010) Traveling-load calibration of grid-array transient contact stress sensors. J Biomech 43:2237–2240
Kolb W, Guhlmann H, Windisch C, Kolb K, Koller H, Grutzner P (2009) Opening-wedge high tibial osteotomy with a locked low-profile plate. J Bone Jt Surg Am 91:2581–2588
Kutzner I, Heinlein B, Graichen F, Bender A, Rohlmann A, Halder A et al (2010) Loading of the knee joint during activities of daily living measured in vivo in five subjects. J Biomech 43:2164–2173
Laprade RF, Engebretsen L, Johansen S, Wentorf FA, Kurtenbach C (2008) The effect of a proximal tibial medial opening wedge osteotomy on posterolateral knee instability: a biomechanical study. Am J Sports Med 36:956–960
Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11:132–138
Madry H, Goebel L, Hoffmann A, Duck K, Gerich T, Seil R et al (2017) Surgical anatomy of medial open-wedge high tibial osteotomy: crucial steps and pitfalls. Knee Surg Sports Traumatol Arthrosc 25:3661–3669
Martineau PA, Fening SD, Miniaci A (2010) Anterior opening wedge high tibial osteotomy: the effect of increasing posterior tibial slope on ligament strain. Can J Surg 53:261–267
Mina C, Garrett WE Jr, Pietrobon R, Glisson R, Higgins L (2008) High tibial osteotomy for unloading osteochondral defects in the medial compartment of the knee. Am J Sports Med 36:949–955
Mondanelli N, Giron F, Losco M, Buzzi R, Aglietti P (2017) Opening wedge high tibial osteotomy using a monoaxial dynamic external fixator. Knee Surg Sports Traumatol Arthrosc 25:306–313
Ogden S, Mukherjee DP, Keating ME, Ogden AL, Albright JA, McCall RE (2009) Changes in load distribution in the knee after opening-wedge or closing-wedge high tibial osteotomy. J Arthroplasty 24:101–109
Pacheco RJ, Ayre CA, Bollen SR (2011) Posterolateral corner injuries of the knee: a serious injury commonly missed. J Bone Jt Surg Br 93:194–197
Pape D, Duchow J, Rupp S, Seil R, Kohn D (2006) Partial release of the superficial medial collateral ligament for open-wedge high tibial osteotomy. A human cadaver study evaluating medial joint opening by stress radiography. Knee Surg Sports Traumatol Arthrosc 14:141–148
Riegger-Krugh C, Gerhart TN, Powers WR, Hayes WC (1998) Tibiofemoral contact pressures in degenerative joint disease. Clin Orthop Relat Res (348): 233–245
Robinson JR, Bull AM, Thomas RR, Amis AA (2006) The role of the medial collateral ligament and posteromedial capsule in controlling knee laxity. Am J Sports Med 34:1815–1823
Seitz AM, Lubomierski A, Friemert B, Ignatius A, Durselen L (2012) Effect of partial meniscectomy at the medial posterior horn on tibiofemoral contact mechanics and meniscal hoop strains in human knees. J Orthop Res 30:934–942
Shelburne KB, Torry MR, Pandy MG (2005) Muscle, ligament, and joint-contact forces at the knee during walking. Med Sci Sports Exerc 37:1948–1956
Staubli AE, De Simoni C, Babst R, Lobenhoffer P (2003) TomoFix: a new LCP-concept for open wedge osteotomy of the medial proximal tibia—early results in 92 cases. Injury 34(Suppl 2):B55–B62
Stoffel K, Willers C, Korshid O, Kuster M (2007) Patellofemoral contact pressure following high tibial osteotomy: a cadaveric study. Knee Surg Sports Traumatol Arthrosc 15:1094–1100
van Egmond N, Hannink G, Janssen D, Vrancken AC, Verdonschot N, van Kampen A (2017) Relaxation of the MCL after an open-wedge high tibial osteotomy results in decreasing contact pressures of the knee over time. Knee Surg Sports Traumatol Arthrosc 25:800–807
Victor J, Wong P, Witvrouw E, Sloten JV, Bellemans J (2009) How isometric are the medial patellofemoral, superficial medial collateral, and lateral collateral ligaments of the knee? Am J Sports Med 37:2028–2036
Funding
No funding was required for this study.
Author information
Authors and Affiliations
Contributions
AMS and MN carried out the in-vitro experiments, and drafted the manuscript. MN prepared all specimen. AMS carried out the statistical analyses. AI participated in the design of the study and helped to interpret the data. LD conceived of the study, and participated in the design and coordination and helped to draft the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
None of the authors declare that they have any conflict of interest related to this work.
Ethical approval
This study was performed with the approval of the institutional review boards of Ulm Universiy.
Rights and permissions
About this article
Cite this article
Seitz, A.M., Nelitz, M., Ignatius, A. et al. Release of the medial collateral ligament is mandatory in medial open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 27, 2917–2926 (2019). https://doi.org/10.1007/s00167-018-5167-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5167-0