Abstract
Purpose
To prospectively assess midterm results in 37 patients (41 knees) who were treated with opening wedge high tibial osteotomy (OW-HTO) with the use of a monoaxial dynamic external fixator (MDEF) for medial knee osteoarthritis.
Methods
Clinical and subjective evaluations were performed using the IKDC and KOOS evaluation forms and the modified Knee Society Clinical Rating System (KSS). Pin tract infections were evaluated according to Checketts–Otterburns classification. Radiographic evaluation included long-standing AP lower limb, standard lateral, Rosenberg and Merchant views.
Results
Thirty-six patients (40 knees) were evaluated at a mean follow-up period of 7 years. Ten patients (25 %) developed a minor pin tract infection. Subjective KOOS and IKDC scores showed statistically significant improvement. Clinical evaluation with IKDC and KSS forms showed no patient with instability or a range-of-motion deficit worst than pre-operatively. At MDEF removal, the mechanical axis was on average 4.5° valgus; anatomical axis 6.8° valgus; the Mikulicz’ line crossed the tibial plateau on average at 64 % of the width of the tibial plateau measured from medial; the posterior slope 5°; the metaphyseal varus 4.3°; and the Insall/Salvati ratio 1.02. At latest follow-up, five patients had a loss of correction of 1°–2° on mechanical axis and one patient had a loss of correction of 3° on mechanical axis and 4 % of mechanical axis on tibial plateau.
Conclusions
The use of a MDEF to perform an OW-HTO showed a good maintenance of correction achieved with satisfactory midterm outcome results in all patients but three who underwent total knee replacement. The only severe post-operative complication was one case of non-union in a heavy smoker.
Level of evidence
Prospective and therapeutic study, Level IV.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
In the young and active adult with mild medial knee osteoarthritis (OA), a high tibial osteotomy (HTO) has been described as a good therapeutic option [1, 2].
Several different techniques have been proposed over the past decades to perform a HTO. Initially, in the early 1960 the deformity correction was achieved using a lateral closing wedge or a dome osteotomy [3]. However, a high rate of complications such as patella baja, tibial slope inversion and lateralization of proximal tibial epiphysis was reported [4–7].
The medial opening wedge HTO (OW-HTO) was first described in 1951 by Debeyre [8] and has become more popular recently in the effort to the decrease post-operative complications [9–11]. Specific instrumentations [12, 13] and fixation devices [14–16] have been introduced. The use of external fixation [13, 17–22] was also advocated to further reduce complications and disadvantages usually associated with the use of internal fixation devices. The use of an external fixator is also advocated in case of large corrections. No bone graft has to be added to fill the gap. The incidence of patella baja is inferior compared with the other types of proximal tibial osteotomies [23]. No additional surgery is needed for hardware removal. Moreover, the most important advantage is that the degree of alignment correction can be set accurately on long-standing anteroposterior (AP) lower limb radiograph at fixed intervals, and in case of overcorrection, the wedge can be closed to the desired amount acting on the fixator. On the other hand, major concerns of this technique are pin tract infection and loss of correction.
Only a few studies investigated the maintenance of lower limb correction after OW-HTO [22, 24]. The purpose of this study was to evaluate the maintenance of limb correction and the outcome results at a longer follow-up of young and active adults with mild medial knee osteoarthritis (OA). The authors hypothesis was that the alignment of the lower limb could be maintained following an OW-HTO performed with the use of a monoaxial dynamic external fixator (MDEF) allowing favourable midterm outcome results with a low rate incidence of complications such as pin tract infection.
Materials and methods
A case series of prospectively collected data are presented. From 1998 to 2007 at First Orthopaedic Clinic, University of Florence, we performed 41 OW-HTO using a MDEF to correct a varus knee deformity in 37 patients. Mean age at surgery was 38 years (SD ±49), there were 25 males (29 knees) and 12 females (male-to-female ratio 2.4), the right knee was involved in 20 cases and the left in 21, dominant knee was involved in 24 cases and non-dominant knee in 17 cases, and mean body mass index (BMI) was 26.7 (SD ±4) kg/m2. Nineteen knees (17 patients) showed a primary medial OA. Seventeen knees (15 patients) underwent a previous arthroscopic medial meniscectomy between 1 and 11 years before. In four patients, a previous tibial fracture had occurred. In one patient, a varus knee deformity was associated with a failed anterior cruciate ligament reconstruction following an untreated associated lateral collateral ligament grade-2 lesion.
Surgical technique
All surgeries were performed under spinal anaesthesia by the senior author (P.A.) with patients in the supine position using a tourniquet. A preliminary arthroscopy was performed in only one patient with a symptomatic lesion of the medial meniscus which was partially resected. Surgery was fluoroscopy assisted in order to check correct pin insertion and guide wire position before the osteotomy.
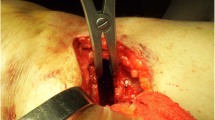
First, the two proximal 6.5-mm pins were inserted from the medial aspect of the proximal tibia parallel to the tibial plateau, on a coronal plane, about 1 cm distal from the joint line. Then the two distal 6.5-mm pins were inserted in the tibial diaphysis using the external fixator arm as a guide and after a preliminary bone drilling. Subsequently, the tibial osteotomy was performed through an anteromedial longitudinal skin incision centred on the pes anserinus. After opening the fascia and lifting the pes’ tendons, two curved retractors were positioned to protect the soft tissues beneath the posterior edge of the tibia and under the patellar tendon, respectively. A Kirschner wire (K-wire) was inserted in an oblique fashion pointing to proximal tibio-fibular joint starting about 5 cm below the joint line. The very distal part of the medial collateral ligament was transected, and the osteotomy was performed at first with an oscillating saw and then with osteotomes up to the lateral cortex. Attention was made to preserve the lateral hinge. The amount of deformity correction was tested with a bone spreader. Finally, the MDEF (ST.A.R. 90, Citieffe, Bologna, Italy in 28 cases and ExFix Orthofix, Verona, Italy in 13 cases) was reassembled on the pins. At the end, osteotomy was left closed and standard wound closure in layers was performed on a suction drain.
Post-operative care
Patients received Cefazolin 2 g IV 30 min before surgery and then 1 g IV every 6 h for 48 h. Pin tract care was performed daily when in the hospital and then every second day at home. Eventual pin tract infections would be evaluated and classified according to Checketts et al. [25] and treated empirically with Ciprofloxacin 500 mg PO every 12 h until clinical resolution. Low-molecular-weight heparin (LMWH) was administered once a day from the first post-operative day up to complete deambulation without crutches at prophylactic dosage.
All the patients were discharged in the second post-operative day. Wedge opening was started 6 days after surgery at a rate of 0.25 mm two times a day. Partial weight bearing was allowed with crutches during the opening phase and then progressed to full weight bearing as tolerated during consolidation phase. Patients were evaluated weekly at our outpatient clinic (Fig. 1). Clinical examination was performed with attention to pin tract aspect, knee range of motion and quadriceps strength. The amount of deformity correction was evaluated using long-standing anteroposterior (AP) lower limb radiograph. A hypercorrection of the deformity was aimed, in order to achieve the mechanical axis of the lower extremity passing through the 64 % of the tibial plateau width measured from medial side [26]. When this goal was achieved, we stopped the distraction and the MDEF was locked. The MDEF was left in place up to a plain radiograph confirmed the healing of the callus, on average twice the time occurred to achieve the desired correction, and was removed in an outpatient setting. Once the MDEF was removed, all the patients were encouraged to gradually return to their usual daily activities. All patients were evaluated again at one, three and six months after MDEF removal and then yearly (Fig. 2).
Serial X-ray controls of the same patient in Fig. 1 at 3, 5, 13 and 26 weeks after surgery, respectively
Subjective evaluation was performed using the knee osteoarthritis outcome score (KOOS) form [27]. Clinical examination was performed using the International Knee Documentation Committee (IKDC) clinical evaluation form [28] and the modified Knee Society Clinical Rating System (KSS) [29].
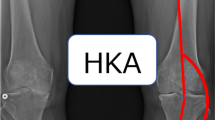
Radiographic evaluation included long-standing AP lower limb, standard lateral, Rosenberg [30] and Merchant [31] views. Anatomical and mechanical axis, the position of weight-bearing line, also known as Mikulicz’ line (centre of the femoral head to the centre of the tibio-talar joint) at the knee, tibial metaphyseal varus angle (MVA), medial proximal tibial angle (MPTA) and lateral distal femoral angle (LDFA) were calculated on long-standing AP view. Tibial slope angle referred to both anterior (Moore–Harvey’s method [32]) and posterior cortices [33, 34] and patellar height using the Insall/Salvati ratio [35] and Caton index [36] were assessed on standard lateral view. Degenerative changes were recorded on long-standing AP and Rosenberg views according to the classification systems of Kellegren and Lawrence’s [37] and Ahlback’s [38]. Patellar position (centred, subluxated or dislocated, and tilted) was evaluated on Merchant view. All radiographic measurements were done by 2 independent observers (N.M. and M.L.) and twice by each of them in a casual fashion, and accepted measures were considered to be the mean values.
No local Bioethical Committee approval for such clinical study was deemed at AOU Careggi, and all patients gave their written informed consent to the procedure and to the follow-ups.
Statistical analysis
Student’s t test was used for continuous data (subjective and radiographic angular measurements), and the Wilcoxon’s signed rank sum test was used for the assessment of the progression of OA. Sample size included 41 knees in 37 patients. Statistical significance was set at p < 0.05. Inter- and intraobserver reproducibility was assessed by intraclass correlation coefficient (ICC) test.
Results
Thirty-six patients (40 knees) were evaluated at a mean follow-up period of 7.2 years (SD ±2). One patient died of unrelated causes 6 months after surgery and was not included in the study. Distraction started 7 days after surgery, final correction was obtained on average after 23.7 days (SD ±46) days, and MDEF was removed after further 47.4 (SD ±15) days. None of the patient mentioned any particular problem in having a MDEF, and all were able to walk without difficulty with one or two crutches.
Two patients (5 %) developed distal a DVTs, so LMWH dosage was adjusted to therapeutic values. At one month, the duplex control showed regression of DVT in both cases. Ten patients (25 %) developed minor pin tract infection, of which six (15 %) were classified as grade I and four (10 %) were classified as grade II. All cases solved with better pin tract care and oral antibiotics.
Only one major complication in this series was recorded: a patient developed a non-union of the wedge-callus. She was a 43-year-old lady with primary mild varus knee OA (mechanical axis 11° varus); her BMI was 21, and surgery and post-operative course were unremarkable. Correction was achieved in 20 days with 3° valgus alignment. MDEF was removed up to 95 days from surgery due to delayed callus ossification. After 3 months, patient was back with medial knee pain and a recurrence of varus deformity. X-rays and MRI showed incomplete ossification of the callus wedge with 2° varus alignment (Fig. 3). At this time, she admitted to be a heavy cigarette smoker, which she denied at first history collection. At revision surger, the osteotomy was stable. The wedge was grafted with autologous bone chips from iliac crest after debriding non-union fibrous tissue at the osteotomy site without correcting the deformity or adding further plate fixation as the patient denied. The osteotomy finally healed in 3 months.
At latest follow-up, all patients but three were satisfied with surgery (92.5 %) (Table 1). No correlation was found between subjective and objective clinical results, BMI, age at surgery, pre-operative deformity and symptoms, and severity of OA.
Radiographic results showed a good maintenance of correction achieved on coronal plane and no significant variation in posterior slope and patellar height (Table 2). A precocious loss of correction (between MDEF removal and the follow-up at one or three months) was identified in four knees. In all of them, the correction loss was less than 3° on mechanical axis. No correlation was found between BMI, age, pre-op deformity, and length of MDEF treatment. At latest follow-up, loss of correction was identified in six knees (15 %) as varus relapse (0°–4°) and as progressed hypercorrection (7° valgus) in one knee (2.5 %). In case of varus, relapse as correlation was found if the corrected mechanical axis was less than 2° valgus (p < 0.05).
We attempted to evaluate proximal tibial MVA, but physeal scar was not always identifiable. It was possible to identify the physeal scar and so to calculate the MVA in only 10 cases; in such small cohort of case, MVA changed from varus 2° to valgus 3°. The MPTA, on the contrary, is always easy and reliable to identify.
A medial OA progression was recorded in four cases (10 %) (Table 3). In four knees (10 %), the medial joint narrowing was evident on standing AP view, while in one case (2.5 %) on the Rosenberg view. A correlation was found between OA progression and the degree of pre-operative OA (p < 0.05). Three patients underwent total knee replacement at 4, 6 and 9 years after the osteotomy without complications.
ICC test was 0.61 or greater in all measurements showing a substantial agreement according to Landis and Koch guidelines [39].
Discussion
The main findings of this investigation are that OW-HTO with MDEF for mild medial knee osteoarthritis showed a good maintenance of correction and only one case of major complication, a non-union in a heavy smoker. The pin tract infection was recorded in about one-fourth of the patients, but it was just superficial and easily resolved with oral antibiotics administration and a better pin tract care.
A high tibial osteotomy still remains the gold standard in the treatment of the mild knee osteoarthritis in a young and active adult population [1, 2, 4, 40]. Lateral closing wedge and dome-shape osteotomies showed a high complication rate and have been shown a progressive decline. OW-HTOs have shown some advantages such as restoration of bone stock, correction of deformity close to its site of origin and absence of a residual metaphyseal deformity, facilitating a subsequent arthroplasty [41, 42]. For the maintenance of the correction, this type of osteotomy can be performed either with the use of an internal fixation device, such a looking plate, or with a MDEF. The major concerns about the use of an external fixation device are the loss of correction after removal of the MDEF and pin tract infection. Immediate loss of correction is not an issue using internal fixation devices, but on the other hand these techniques do not permit to achieve large or complex multiplanar corrections and to perform additional adjustments after surgery (“fine-tuning”), as MDFE does.
Myrnerts [43] and Odenbring et al. [7] achieved satisfactory correction in only 55 % of cases, and Insall [2] described success in 79 % of cases, with internal fixation. More recently, Marti et al. [44] investigating the outcome results of medial OW-HTO with an internal fixation device were able to achieve the desired position of the mechanical axis in only 50 % of the patients. Using a MDEF, Bachhal et al. [24] reported a desired alignment in 84 % of the patients. In our series, four patients (10 %) had a loss of correction of 2°–4° on mechanical axis in the first 3 months after MDEF removal. Early loss of correction can be possible if the callus has not healed, and the proposed time to callus healing twice the time of distraction seems to be a reasonable interval. Nevertheless, we always wait for radiographic appearance of healing with visible ossification. We could not find any correlation between loss of correction, degree of pre-operative deformity, length of MDEF maintenance and age and BMI of the patient. Correlation between loss of correction and patient BMI has been shown at long-term follow-up. Flecher et al. [45], at a mean follow-up of 18 years, found age less than 50 years at surgery, BMI less than 25, post-operative valgus angle of 6° or more and pre-operative Ahlback grade 1 OA to be protective factors of the outcome. Weale et al. [22] found that inadequate correction was caused by premature union of the osteotomy before complete correction and some loss of correction after removal of the fixator, but they did not report about any correlation with possible risk factor and survival of the osteotomy. In the current series, we had no cases of premature union of the osteotomy.
The other major concern about the use of external fixation is infection. If this complication occurs, it can necessitate pin removal before correction and union have been achieved [42] and possibly jeopardize subsequent arthroplasty. Signs of infection develop very frequently using external fixation devices, from 5 to 58 % of patients [2], but up to 96 % of these infections are minor [20]. Magyar et al. [20] recorded pin site infections in 157 out of 308 patients (51 %) operated on of OW-HTO using external fixation for both varus and valgus knee mild OA; of these, 96 % were minor and responded to wound toilet and antibiotic treatment. W-Dahl et al. [46] found no difference between daily and weekly pin site care. Weale et al. [22] registered 28 knees out of 76 (36 %) with signs of minor pin tract infection requiring antimicrobial therapy and one case (1.5 %) of chronic osteomyelitis of proximal tibia 2 years after surgery. Bachhal et al. [24] reported pin tract infection in 23 of 37 patients treated with either pin tract care and oral antibiotics and one sequestrum at the diaphyseal pin site which required curettage. In our series, 25 % of patients developed minor signs of infection (15 % grade I and 10 % grade II) which resolved promptly with better pin tract care and oral antibiotic therapy and none developed major signs or chronic osteomyelitis up to latest follow-up. Furthermore, the three patients, who later underwent TKA, healed without any complication.
At latest follow-up, all patients but three were satisfied with surgery, subjective KOOS and IKDC evaluation showed statistically significant improvement, and clinical evaluation with IKDC and KSS forms showed no patient with swelling, instability or a range-of-motion deficit worst than pre-operatively. These results are in line with similar cases series [1, 4, 23, 24, 44, 47, 48].
Previous studies on HTO have shown satisfactory results [1, 24, 26] but deterioration of subjective, clinical and radiographic results over time. This may be the consequence of degenerative changes in all compartments of the knee with time lapse although it has been suggested that the osteoarthritic process can be arrested by the realignment [1, 49]. In our series, medial progression of OA was found in four patients on standard AP view and in one patient on Rosenberg view.
Only one major complication in this series was recorded: a patient who developed a non-union of the wedge-callus. She was a heavy cigarette smoker, who denied her bad habit at history collection before surgery. The incidence of non-union after a high tibial osteotomy ranges between 3 and 5 % [19, 50]. In most of the cases, this complication is related to a violation of the lateral tibial cortex. In our series, however, this complication was related to the well-known [51, 52, 53] negative effect of cigarette smoking on bone healing.
The main limitation of this study was that the number of patients involved was relatively small and that a control group, maybe with an internal fixation, was lacking.
This study is the first outcome study evaluating the maintenance of limb alignment correction after OW-HTO using a MDEF in young and active adult with mild medial knee osteoarthritis. In our series, we found satisfactory clinical results with a good maintenance of correction in most of the patients. The surgical technique is easy, and the patients well tolerate the MDEF. Complications were few and easy resolvable.
Conclusions
OW-HTOs using a MDEF are a safe and simple procedure, and the results are comparable with other techniques. Outcome is satisfactory in the young and high-demanding patient who does not accept activity restrictions imposed by arthroplasty. The four major advantages of MDEF techniques when performing an OW-HTO are: first, it is possible to correct minimal residual deformity up to exact desired axes on weight-bearing view. Second, due to the hemicallotasis phenomenon, the use of graft is not needed. Third, the external fixator is suggested in case of correction of large deformities. Fourth, no further surgery is requested for hardware removal. On the other hand, the use of MDEF devices requires more patient compliance with need for pin tract care and frequent clinical and radiographic checks on an outpatient basis by the physician.
References
Aglietti P, Rinonapoli E, Stringa G, Taviani A (1983) Tibial osteotomy for the varus osteoarthritic knee. Clin Orthop Relat Res 176:239–251
Insall JN (1993) Osteotomy. In: Insall JN, Windsor RE, Scott WN, Kelly MA, Aglietti P (eds) Surgery of the knee. Churchill Livingstone, New York, pp 635–676
Coventry MB (1965) Osteotomy of the upper portion of the tibia for degenerative arthritis of the knee: a preliminary report. J Bone Joint Surg Am 47-A:984–990
Aglietti P, Buzzi R, Vena LM, Baldini A, Mondaini A (2003) High tibial valgus osteotomy for medial gonarthrosis: a 10- to 21-year study. J Knee Surg 16:21–26
Amendola A, Rorabeck CH, Bourne RB, Apyan PM (1989) Total knee arthoplasty following high tibial osteotomy for osteoarthritis. J Arthroplasty 4(Suppl):S11–S17
Haddad FS, Bentley G (2000) Total knee arthroplasty after high tibial osteotomy: a medium-term review. J Arthroplasty 15:597–603
Odenbring S, Egund N, Knutson K, Lindstrand A, Toksvig-Larsen S (1990) Revision after osteotomy for gonarthrosis: a 10-19-year follow-up of 314 cases. Acta Orthop Scand 61:128–130
Debeyre J (1951) Surgical treatment of arthroses of the knee. Sem Hop 27(61–62):2515–2518
Amendola A, Fowler PJ, Litchfield R, Kirkley S, Clatworthy M (2004) Opening wedge high tibial osteotomy using a novel technique: early results and complications. J Knee Surg 17:164–169
Koshino T, Murase T, Saito T (2003) Medial opening-wedge high tibial osteotomy with use of porous hydroxyapatite to treat medial compartment osteoarthritis of the knee. J Bone Joint Surg Am 85-A:78–85
Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11:132–138
Billings A, Scott DF, Camargo MP, Hofmann AA (2000) High tibial osteotomy with a calibrated osteotomy guide, rigid internal fixation, and early motion. Long-term follow-up. J Bone Joint Surg Am 82:70–79
Ellis RE, Tso CY, Rudan JF, Harrison MM (1999) A surgical planning and guidance system for high tibial osteotomy. Comput Aided Surg 4:264–274
Miniaci A, Ballmer FT, Ballmer PM, Jakob RP (1989) Proximal tibial osteotomy: a new fixation device. Clin Orthop Relat Res 246:250–259
Staubli AE, De Simoni C, Babst R, Lobenhoffer P (2003) TomoFix: a new LCP-concept for open wedge osteotomy of the medial proximal tibia-early results in 92 cases. Injury 34(Suppl 2):B55–B62
Stoffel K, Stachowiak G, Kuster M (2004) Open wedge high tibial osteotomy: biomechanical investigation of the modified Arthrex Osteotomy Plate (Puddu Plate) and the TomoFix Plate. Clin Biomech 19:944–950
Adili A, Bhandari M, Giffin R, Whately C, Kwok DC (2002) Valgus high tibial osteotomy: comparison between an Ilizarov and a coventry wedge technique for the treatment of medial compartment osteoarthritis of the knee. Knee Surg Sports Traumatol Arthrosc 10:169–176
Fowler JL, Gie GA, MacEachern AG (1991) Upper tibial valgus osteotomy using a dynamic external fixator. J Bone Joint Surg Br 73-B:690–691
Magyar G, Toksvig-Larsen S, Lindstrand A (1998) Open wedge tibial osteotomy by callus distraction in gonarthrosis. Operative technique and early results in 36 patients. Acta Orthop Scand 69:147–151
Magyar G, Toksvig-Larsen S, Lindstrand A (1999) Hemicallotasis open-wedge osteotomy for osteoarthritis of the knee: complications in 308 operations. J Bone Joint Surg Br 81-B:449–451
Sen C, Kocaoglu M, Eralp L (2003) The advantages of circular external fixation used in high tibial osteotomy (average 6 years follow-up). Knee Surg Sports Traumatol Arthrosc 11:139–144
Weale AE, Lee AS, MacEachern AG (2001) High tibial osteotomy using a dynamic axial external fixator. Clin Orthop Relat Res 382:154–167
Brouwer RW, Bierma-Zeinstra SM, van Koeveringe AJ, Verhaar JA (2005) Patellar height and the inclination of the tibial plateau after high tibial osteotomy. The open versus the closed-wedge technique. J Bone Joint Surg Br 87:1227–1232
Bachhal V, Sankhala SS, Jindal N, Dhillon MS (2011) High tibial osteotomy with a dynamic axial fixator: precision in achieving alignment. J Bone Joint Surg Br 93(7):897–903
Checketts RG, Otterburn M, MacEachern AG (1993) Pin track infection: definition, incidence and prevention. Int J Orthop Trauma 3:16–19
Dugdale TW, Noyes FR, Styer D (1992) Preoperative planning for high tibial osteotomy. The effect of lateral tibiofemoral separation and tibiofemoral length. Clin Orthop Relat Res 274:248–264
Roos E, Roos G, Lohmander S, Ekdahl C, Beynnon B (1998) Knee injury and Osteoarthritis Outcome Score (KOOS): development of a self-administered outcome measure. J Orthop Sports Phys Ther 2:88–96
Irrgang JJ, Anderson AF, Boland AL, Harner CD, Kurosaka M, Neyret P, Richmond JC, Shelborne KD (2001) Development and validation of the international knee documentation committee subjective knee form. Am J Sports Med 29:600–613
Insall JN, Dorr LD, Scott RD, Scott WN (1989) Rationale of the knee society clinical rating system. Clin Orthop Relat Res 24:13–14
Rosenberg TD, Paulos LE, Parker RD, Coward DB, Scott SM (1988) The forty-five-degree posteroanterior flexion weight-bearing radiograph of the knee. J Bone Joint Surg Am 70-A:1479–1483
Merchant AC, Mercer RL, Jacobsen RH, Cool CR (1974) Roentgenographic analysis of patello-femoral congruence. J Bone Joint Surg Am 56:1391–1396
Moore TM, Harvey JP Jr (1974) Roentgenographic measurement of tibial-plateau depression due to fracture. J Bone Joint Surg Am 56-A:155–160
Brazier J, Migaud H, Gougeon F, Cotten A, Fontaine C, Duquennoy A (1996) Evaluation of methods for radiographic measurement of the tibial slope. A study of 83 healthy knees. Rev Chir Orthop Reparatrice Appar Mot 82:195–200
Genin P, Weill G, Julliard R (1993) The tibial slope: proposal for a measurement method. J Radiol 74:27–33
Insall JN, Salvati E (1971) Patella position in the normal knee joint. Radiology 101(1):101–104
Caton J (1989) Method of measuring the height of the patella. Acta Orthop Belg 55(3):385–386
Kellegren JH, Lawrence JS (1957) Radiological assessment of osteoarthrosis. Ann Rheum Dis 16:494–501
Ahlback S (1968) Osteoarthrosis of the knee. A radiographic investigation. Acta Radiol Supplementum 227:1–72
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics 33(1):159–174
Wright J, Heck D, Hawker G, Dittus R, Freund D, Joyce D, Paul J, Young W, Coyte P (1995) Rates of tibial osteotomies in Canada and the United States. Clin Orthop Relat Res 319:266–275
Kitson J, Weale AE, Lee AS, MacEachern AG (2001) Patellar tendon length following opening wedge high tibial osteotomy using an external fixator with particular reference to later total knee replacement. Injury 32(Suppl 4):140–143
Nakamura E, Mizuta H, Kudo S, Takagi K, Sakamoto K (2001) Open-wedge osteotomy of the proximal tibia with hemicallotasis. J Bone Joint Surg Br 83-B:1111–1115
Myrnerts R (1980) Failure of the correction of varus deformity obtained by high tibial osteotomy. Acta Orthop Scand 51:569–573
Marti CB, Gautier E, Wachtl SW, Jakob RP (2004) Accuracy of frontal and sagittal plane correction in open-wedge high tibial osteotomy. Arthroscopy 20:366–372
Flecher X, Parratte S, Aubianac JM, Argenson JN (2006) A 12-28-Year followup study of closing wedge high tibial osteotomy. Clin Orthop Relat Res 452:91–96
W-Dahl A, Toksvig-Larsen S, Lindstrand A (2003) No difference between daily and weekly pin site care: a randomized study of 50 patients with external fixation. Acta Orthop Scand 74:704–708
Collins B, Getgood A, Alomar AZ, Giffin JR, Willits K, Fowler PJ, Birmingham TB, Litchfield RB (2013) A case series of lateral opening wedge high tibial osteotomy for valgus malalignment. Knee Surg Sports Traumatol Arthrosc 21(1):152–160
Coventry MB (1984) Upper tibial osteotomy. Clin Orthop Relat Res 182:46–52
Coventry MB, Ilstrup DM, Wallrichs SL (1993) Proximal tibial osteotomy: a critical longterm study of eighty-seven cases. J Bone Joint Surg Am 75-A:196–201
Tjörnstrand B, Hagstedt B, Persson BM (1978) Results of surgical treatment for non-union after high tibial osteotomy in osteoarthritis of the knee. J Bone Joint Surg Am 60(7):973–977
Castillo RC, Bosse MJ, MacKenzie EJ, Patterson BM, LEAP Study Group (2005) Impact of smoking on fracture healing and risk of complications in limb-threatening open tibia fractures. J Orthop Trauma 19(3):151–157
Moghaddam A, Weiss S, Wolfl CG, Schmeckenbecher K, Wentzensen A, Grutzner PA, Zimmermann G (2010) Cigarette smoking decreases TGF-b1 serum concentrations after long bone fracture. Inj Int J Care Inj 41:1020–1025
Sloan A, Hussain I, Maqsood M, Eremin O, El-Sheemy M (2010) The effects of smoking on fracture healing. Surgeon 8(2):111–116
Author information
Authors and Affiliations
Corresponding author
Additional information
Paolo Aglietti: Deceased on April 18, 2013.
Rights and permissions
About this article
Cite this article
Mondanelli, N., Giron, F., Losco, M. et al. Opening wedge high tibial osteotomy using a monoaxial dynamic external fixator. Knee Surg Sports Traumatol Arthrosc 25, 306–313 (2017). https://doi.org/10.1007/s00167-015-3564-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-015-3564-1