Abstract
Purpose
To give an overview of the basic knowledge of the functional surgical anatomy of the proximal lower leg and the popliteal region relevant to medial high tibial osteotomy (HTO) as key anatomical structures in spatial relation to the popliteal region and the proximal tibiofibular joint are usually not directly visible and thus escape a direct inspection.
Methods
The surgical anatomy of the human proximal lower leg and its relevance for HTO are illustrated with a special emphasis on the individual steps of the operation involving creation of the osteotomy planes and plate fixation.
Results
The posteriorly located popliteal neurovascular bundle, but also lateral structures such as the peroneal nerve, the head of the fibula and the lateral collateral ligament must be protected from the instruments used for osteotomy. Neither positioning the knee joint in flexion, nor the posterior thin muscle layer of the popliteal muscle offers adequate protection of the popliteal neurovascular bundle when performing the osteotomy. Tactile feedback through a loss-of-resistance when the opposite cortex is perforated is only possible when sawing and drilling is performed in a pounding fashion. Kirschner wires with a proximal thread, therefore, always need to be introduced under fluoroscopic control. Due to anatomy of the tibial head, the tibial slope may increase inadvertently.
Conclusions
Enhanced surgical knowledge of anatomical structures that are at a potential risk during the different steps of osteotomy or plate fixation will help to avoid possible injuries.
Level of evidence
Expert opinion, Level V.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Medial open-wedge high tibial osteotomy (HTO) is an excellent option to treat patients with symptomatic medial tibiofemoral osteoarthritis (OA) and varus malalignment [17]. Biomechanical data suggest that a biplanar osteotomy and the use of a plate fixator are optimal technique [11, 22]. To correctly execute a medial HTO, an extended knowledge of the functional surgical anatomy of the proximal lower leg and the popliteal region is essential [23]. Important structures within these anatomical regions are closely related to the osteotomy planes and are therefore at potential risk at the different surgical steps [10, 31]. Some of these relevant structures may be directly inspected or palpated, and some cannot be directly assessed and are therefore not open for visualization. This pictorial essay describes the functional surgical anatomy of the proximal lower leg and the popliteal region in the context of the individual steps of performing a medial high tibial osteotomy.
Surgically relevant anatomical landmarks of the proximal lower leg and the popliteal region
The tibial tubercle and the insertion of the patellar ligament are important anterior anatomical landmarks. On the lateral side, these include the outer tibiofemoral joint line and the proximal tibiofibular joint, and on the medial side, the inner tibiofemoral joint line and the pes anserinus.
Surgical approach and skin incision
The classical surgical approach to the medial tibial head starts slightly proximal to the insertion of the pes anserinus aiming to the posteromedial corner of the tibial head. It has a length of approximately 6–8 cm. If this approach is used, the infrapatellar branch of the saphenous nerve is rarely injured [17]. Alternatively, a medial approach, as similarly used for knee arthroplasty, aiming from the medial side of the tibial tubercle parapatellar to the inner joint line, may also be employed. Of note, in up to 30 % the infrapatellar branch of the saphenous nerve is injured through this incision, reporting subjective numbness [5], but the same incision may be used, without additional compromization of soft tissues, if knee arthroplasty is needed in the future (Fig. 1). For protection of soft tissues, in case arthroplasty surgery will be needed in future, an already existing median skin incision can be employed for osteotomy.
Medial region of the knee: an oblique approach (light green line) will usually not injure the infrapatellar branch of the saphenous nerve. However, a median parapatellar approach (cyan line) similarly allows displaying the posteromedial corner of the tibial head and might be indicated if further compromising of soft tissues, in case of future knee arthroplasty, should be avoided. P patella, PT patella tendon, TT tibial tuberosity, PA pes anserinus, MFC medial femoral condyle, MTP medial tibial plateau
Surgical anatomy of the medial proximal tibia
The pes anserinus is located approximately 1–2 cm medially and distally of the tibial tubercle. Close to the pes anserinus’ insertion, the tendons of the hamstring muscles are orientated horizontally. The superficial part of the MCL processes vertically and is located adjacent to the tibial bone underneath the sartorius’ fascia. At its front, distally to the K wires, the insertion of the MCL has to be engraved and dissected with a raspatory caudally and distally. The insertion of the MCL proximal to the K wires remains untouched and therefore guarantees the knee’s stability against valgus stress (Fig. 2). The distal fibres of the MCL have to be completely released to prevent unphysiological strains between the medial tibial head and distal femur after completion of an opening medial HTO [1].
Anatomy of the proximal medial tibia. The pes anserinus (PA) is located one thumb width medially and one thumb width distally of the tibial tubercle (TT). The horizontal K wires for the horizontal part of the biplanar osteotomy are introduced at the upper rim of the sartorius tendon. MCL Medial collateral ligament, MTP medial tibial plateau
Functional surgical anatomy relevant to the biplanar osteotomy
Important structures of this step include the tibial tubercle, the insertion of the patella tendon, the patellar tendon and the ventral tibial cortex.
A biplanar osteotomy consists of a horizontal, lateral incomplete transection of two-thirds of the tibial head, while the osteotomy plane proceeds from mediocaudal to superolateral to the proximal tibiofibular joint. It improves, compared to uniplanar osteotomies, the geometrical preconditions for bone healing: The wedge volume for the slower gap healing is reduced, while a larger surface area for expedited contact healing is available [21, 27]. In order to maintain the stability of the osteotomy, outmost care is taken not to fracture the lateral cortex [7, 29].
The coronal plane of the biplanar osteotomy is ascending v-shaped, undercutting the tibial tubercle parallel to the ventral tibial cortex. This plane forms an angle of 110° to the horizontal osteotomy (Fig. 3). Prior to the ascending osteotomy, the anatomical landmarks, especially the insertion of the patella tendon at the tibial tubercle, need to be inspected. With electrosurgery, the course of the bone incision is marked on the periosteum. The ascending retro-tubercle osteotomy starts with a transection of the cortical bone using a narrow saw blade, which at first is orientated orthogonal to the cortical surface. After penetration of the compact bone layer, the oscillating saw is shifted dorsally, thus allowing for an ascending osteotomy parallel to the posterior edge of the proximal tibia (Fig. 4a). After completion of the ascending osteotomy, the narrow saw blade may remain in the osteotomy gap, facilitating the identification of the turning point towards the horizontal osteotomy. This step protects the tubercular segment from the subsequent horizontal osteotomy (Fig. 4b).
a Nomenclature of screw holes, exemplarily shown for the TomoFix Medial High Tibial Plate: the solid part bridges the osteotomy. If the osteotomy gap starts at least 30 mm distal of the medial joint line, the correct osseous segment length of the proximal tibial segment was chosen. Then, drill hole D will not come to lie at the level of the osteotomy. However, if this happens, it is obligatory to use a locking screw, avoiding the creation of a breaking point for implant fatigue. b Locking screws A, B, C fixate the proximal tibial segment and progress convergent aiming to the fibular head. TT tibial tuberosity
Topographical relationship of the horizontal saw cut of the ascending retrotubercular osteotomy to the tibial tuberosity. The patellar ligament was removed for didactic reasons. a Anterior view. b Superior view. ACL anterior cruciate ligament, FH fibular head, LFC lateral femoral condyle, LTP lateral tibial plateau, MFC medial femoral condyle, MTP medial tibial plateau, P patella, PA pes anserinus, PT patella tendon, TG trochlear grove, TT tibial tuberosity
The patellar tendon and the tibial tubercle must be displayed properly by insertion of a retractor dorsocranial its insertion levering the tendon ventrally. Also, a forceps can be used to lift the patella tendon. Thus, a tendon injury caused by the oscillating saw becomes unlikely. The proximal plate design should be narrow to gain enough space for the ascending branch of the biplanar osteotomy (Fig. 3).
Functional surgical anatomy relevant to the insertion of the horizontal Kirschner wires
Key structures of this step include the sartorius tendon, the proximal tibiofibular joint, the opposite cortical tibial bone and potentially the head of the fibula together with the peroneal nerve.
Two 2.5-mm K wires of equal length, containing a tip that has the shape of a three-edged wedge or that is threaded, are placed at an interval of approximately 1 cm superior to the sartorius tendon. The K wires aim towards the upper third of the proximal tibiofibular joint, their tip touching the opposite cortical bone. As the consecutive horizontal osteotomy is performed basally, an intraarticular lateral hinge fracture becomes very unlikely [7, 29]. By measuring the length of the extraosseous portion of the K wire, the depth of the osteotomy incision can be calculated. Based on the triangular shape of the tibia, the saw cut should dorsal be longer than anterior. The K wires should in the sagittal plane be located 1 cm dorsal of the ascending branch of the biplanar osteotomy, making it possible to undercut the tibial tubercle in an ascending angle of 110°.
The intersection of both horizontal K wires should be less than the width of the saw blade, allowing for a sufficient guidance of the saw blade. The anterior K wire should be located 5–10 mm dorsally of the turning point between the horizontal and ascending osteotomy, protecting the tibial tubercle from injury caused by the oscillating saw, thereby preventing an instability of the tibial tubercle and keeping up the function of the extensor mechanisms. When a correct anterior posterior radiographs is performed to confirm the correct placement of the K wires, due to overlaying of the K wires both should appear as one.
The tips of the K wires have a short thread, oppressing the tactile loss-of-resistance feedback while penetrating the opposite cortical bone using a boring machine for the horizontal drills. An untrained surgeon may, after penetration of the contralateral bone, harm with the K wire the anterior tibial loge, the head of the fibula or the peroneal nerve (Fig. 5) [8]. To avoid damage of bony and soft tissue structures lateral of the tibial head, the insertion of the horizontal K wires should be performed under fluoroscopic control.
a Introduction of the horizontal K wires. As the K wires have a short thread, a tactile feedback after penetration of the opposite cortical bone is lacking, putting the anterior tibial loge, the fibular head and the peroneal nerve at a potential risk. b Course of peroneal nerve at level of osteotomy with red arrows highlighting the close relationship to K wires penetrating the lateral corticalis. K Kirschner wires, MFC medial femoral condyle, MTP medial tibial plateau, P patella, PA pes anserinus, PN peroneal nerve, PT patella tendon
Functional surgical anatomy relevant to the horizontal osteotomy of the proximal tibia
Important structures of this step include the posterior tibial cortical bone, the dorsal neurovascular bundle including the tibial nerve and the popliteal vessels and the tibialis posterior and popliteus muscles.
The horizontal osteotomy is issued caudally of the two medially placed K wires (Fig. 6). A saw should always be applied for transection of the medial cortical bone, while completion of the osteotomy can be performed either with the oscillating saw under thorough rinsing [16] or—to avoid heat necrosis—with flat sharp chisels [9]. To protect the soft tissues, a Hohmann retractor should be placed dorsally subperiosteally at the level of the horizontal osteotomy flagging the posterior edge of the tibia (Fig. 6a). Bending the knee to 90° will facilitate a correct and strict mediolateral position of the osteotomy instruments parallel to the posterior corticalis (Fig. 6b). However, flexion of the knee will not significantly shift the neurovascular bundle dorsally [10]. At the level of osteotomy, the tibial nerve and popliteal vessels are, independent from the degree of flexion, located 1–2 cm posterior of the tibial cortex, just separated by the tibialis posterior and popliteus muscles [4, 6, 13, 15, 26]. This thin layer offers no adequate protection for the neurovascular bundle [4, 13]. Also, surgeons need to be aware that in 6 % of all patients, an irregular “high-riding” origin of the anterior tibialis artery is observed which courses anteriorly to the popliteus muscle and highly predisposes to vascular injury during osteotomy [10]. Only the subperiosteal placed Hohmann retractor and the correct orientation of the osteotomy do protect these structures against the osteotomizing instruments. The medially inserted Hohmann retractor should be placed as far laterally as possible, since, at this level, the neurovascular bundle proceeds laterally, too (Fig. 7).
a Illustration of the dorsally placed subperiosteal Hohmann retractor for the protection of soft tissues. b Bending the knee to 90° facilitates a correct and strict mediolateral orientation of the osteotomizing instruments parallel to the posterior corticalis of the tibia (light green line). Cian triangle = schematic and simplified depiction of the geometry of the tibial metaphysis, K Kirschner wires (with red arrows pointing to them), MFC medial femoral condyle, MTP medial tibial plateau, P patella, PA pes anserinus, PT patella tendon, T tibia, TT tibial tuberosity
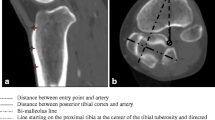
T1-weighted magnetic resonance image. Axial reconstruction of a left knee bent to 70°. Bending the knee will only move the neurovascular bundle a few mm posteriorly, only providing insufficient protection against osteotomizing instruments. T tibia, F fibula, neurovascular bundle = red circle, distance between posterior cortical to neurovascular bundle = D and white line
Executing the osteotomy caudally to the horizontal K wires will prevent driving the osteotomizing instruments into the joint. To avoid heat necrosis, continuous rinsing is required, if a oscillating saw is used. In case sharp chisels are utilized, an anteromedial wiping motion for easing of a stuck chisel has to be omitted. Instead, a parallel forceps should be employed to dislodge the chisel in a strictly medial direction. This will prevent injuries of the neurovascular bundle through a wobbling chisel tip.
Bending the knee to 90° will release the dorsal soft tissues and eases the correct positioning of the osteotomizing instruments. However, a significant dorsal movement of the neurovascular bundle is not detectable angiographically during bending, suggesting that, irrespective of the knees position, these structures are at high risk of injury and therefore need to be particularly protected.
Functional surgical anatomy relevant to the plate fixator
This step is performed along the proximal parts of the medial tibial head. However, the peroneal nerve in relation of the opposite cortical bone may be also compromised.
In order to facilitate the denomination of the screw holes, the nomenclature of the product description of the TomoFix Medial High Tibial Plate(DePuy Synthes, West Chester, PA, USA; http://emea.depuysynthes.com/hcp/trauma/products/qs/tomofix-system) for medial high tibial osteotomy is used here. After completion of the biplanar osteotomy and the exact adjustment of the angle of correction, a bone spreader needs to be inserted dorsally to stabilize the osteotomy result. The bone spreader needs to be placed as far backwards as possible to allow for a parallel opening of the osteotomy while avoiding any increase in tibial slope as an increase in the tibial slope posteriorly maybe caused by anterior positioning of the instruments [27, 28]. Also, an insufficient release of muscles and ligaments on the medial side may increase the slope.
Under fluoroscopic guidance, the TomoFix Medial High Tibial Plate will be positioned subcutaneously at the medial tibial head, in front of the osteotomy spreader, as far posterior as possible providing greater stability [19]. The shaft is oriented parallel to the tibial diaphysis, and its segment without drill holes bridges the osteotomy gap. In screw holes A to C, the proximal locking screws shall be placed 1 cm below the joint line (Fig. 8). After fluoroscopic confirmation of proper plate position, a centring sleeve will be installed in the drill sleeve of screw hole B and the first K wire (2.0 mm, three-edged wedge bit) will be used for temporary fixation of the TomoFix Medial High Tibial Plate. This should be checked as well fluoroscopically to avoid penetration of the thin opposite cortical bone. Tactile feedback as a loss-of-resistance cannot be expected. Therefore, the peroneal nerve is at risk if brusque movements are carried out [8]. Fluoroscopic controls while pushing along the K wires are therefore highly recommended (Fig. 9).
Fluoroscopic images highlighting the individual steps from osteotomy to plate fixation. a Horizontal medial subtotal osteotomy of the tibial head aiming towards the proximal tibiofibular joint. b Careful stepwise opening of the osteotomy gap. The opposite cortex often remains intact if the angle of correction is less than 8°. c Introducing an osteotomy spreader far posteromedial and gradual opening of the osteotomy gap, while taking the tibial slope into account, until the desired angle is reached, resulting in valgization. d After placement of the proximal locking screws, a temporary lag screw should be introduced into the screw hole number 1 for retention and compression of the opposite cortex
Direct relationship of the drill hole (here for screw B) to the peroneal nerve after breaking through the lateral proximal tibial head. For a better illustration, the drill is shown without a drill sleeve. Note that screws A and C aim at the fibula head. Insert: Drill tip penetrating peroneal nerve (with red arrows pointing to them). D drill tip, MFC medial femoral head, P patella, NP peroneal nerve, PT patella tendon, T tibia, TT tibial tuberosity
Next, screw holes A and C are equipped with drill sleeves and are formed in a pounding technique with a twist drill [4.3-mm locking compression plate (LCP) drill bit] until they have advanced laterally to the opposite cortex. The screw length of the three proximal self-tapping locking screws should be long enough to reach the opposite cortex without penetrating it. Drill hole C is, due to its position, at highest risk of causing vascular damage due to overlong screws (Fig. 10).
If the angle of correction accounts more than 8°, a fracture of the opposite cortex is common with a risk of loss of correction [20, 25]. However, not every fracture can be displayed fluoroscopically during surgery. Therefore, for reposition and retention of the opposite cortex, a temporary lag screw should be placed in the dynamic part of the combination hole #1. A 3.2-mm twist drill is used, with a slightly distal drill direction, avoiding any interference with the bicortical locking screw, which, in following steps, will be placed in the locking part of this combination hole. Under fluoroscopic control, the temporary lag screw is stepwise-anchored bicortical, allowing for a reposition and retention of the potentially fractured opposite cortex (Fig. 11). After placement of the three remaining bi- and monocortical locking screws in holes #2 to #4, the temporary lag screw in hole #1 is removed and replaced by a bicortical locking screw.
By brisk blocking of the first and only proximal screw using a torque wrench, there will be a co-rotation of the plate (“propeller effect”) when the locking screw head catches the thread of the locking hole of the TomoFix Medial High Tibial Plate. To avoid plate rotation, all proximal screws should be hand-tighten before a torque wrench is applied. Then, the locking of the proximal screws A to C can be performed using a torque wrench as the plate will then be stabilized against rotation movements.
Selective review of the literature
Complications associated with open-wedge high tibial osteotomies were described in a recent retrospective evaluation of 115 consecutive patients and a literature review [30]. A total of 36 complications were observed in 29 patients, including 2 vascular injuries, 15 minor or major infections, 1 compartment syndrome and 8 patients with an implant irritation, but no deep vein thrombosis (DVT) or implant failure [30]. DVTs were reported by Martin et al. [18] in 4/314 patients. Duivenvorden et al. [8] found 1 compartment syndrome, 4 pseudarthroses and 2 tibial plateau fractures in 112 patients receiving open-wedge HTO, while, due to discomfort, the hardware had to be removed in 79 patients. Pseudo-aneurysms [26], a complete rupture of the popliteal artery [3] or vascular occlusions [24], were also described. Gerich et al. [10] reported on the variation of the origin of the anterior tibial artery with a course between the posterior tibial cortex and the popliteal muscle in 6 % of all patients. Martin et al. [18] reported no vascular complications in 323 procedures (292 patients), but found an increase in tibial slope >10 % in 3/297 patients and hardware failure with loss of correction in 3/303 patients. Undisplaced (64/323) and minimally displaced (18/323) lateral hinge fractures were also observed [18]. Lateral hinge fractures as classified by Takeushi et al. [29] may result in impaired fixation stability and secondary loss of correction resulting also in a relevant number of non-unions [7]. A loss of correction rate between 0 and 17.2 % was described [30]. Asada et al. [2] pointed out that an increase in posterior tibial slope resulted in loss of correction in the frontal plane after medial open-wedge high tibial osteotomy. To achieve the planned tibial slope in HTO is difficult. Lee et al. [14] reported in a case series of 136 patients (170 knees) that in only 12.9 %, an osteotomy parallel to the medial posterior tibial slope in the sagittal plane was achieved. They concluded that because of high rate of the anterior-inclined osteotomy and their correlations with posterior tibial slope, surgeons should make all efforts to perform a parallel osteotomy relative to the medial posterior tibial slope. In a cadaver model, Jacobi et al. [12] observed factors influencing posterior tibial slope and tibial rotation in open-wedge high tibial osteotomy. Significant changes in tibial slope occurred in more than half of the patients, while significant changes in tibial rotation only were visualized in 11.9 %. Advanced postoperative OA, flexion contractures, larger angles of correction or lateral hinge fractures were associated with an increased posterior tibial slope, stressing the importance of a precise intraoperative measurement of the tibial slope.
Discussion
The most important finding of the present study is that a profound knowledge of important anatomical landmarks that are at a potential risk during the different steps of osteotomy or plate fixation is mandatory for a correct technical execution of a HTO. Some of the relevant structures, such as the distal medial collateral ligament (MCL) or the tibial tubercle, may be directly inspected or palpated. However, structures related to the popliteal region or to the proximal tibiofibular joint, like the popliteal neurovascular bundle or the peroneal nerve, cannot be directly assessed and are therefore not open for a direct visualization.
The neurovascular bundle passing dorsally, as well as on the lateral side of the peroneal nerve, fibular head and lateral collateral ligament must be protected against the osteotomizing instruments. This can only be achieved by a meticulous orientation of the instruments and osteotomy, obligatory placement of a Hohmann retractor mediodorsal of the tibial head at the level of osteotomy and by thorough placement of threaded K wires under fluoroscopic control. Neither flexion of the knee, nor the thin muscle layer of the tibialis posterior and popliteus muscles may protect the neurovascular structures from the instruments.
A loss-of-resistance as tactile feedback after transection or drilling through the opposite cortical bone is only possible if a pounding sawing or drilling technique can be applied. However, this tactile feedback is lacking if threaded K wires are utilized, and therefore, fluoroscopic confirmation is warranted here.
Conclusions
High tibial osteotomies are becoming increasingly popular, stressing the clinical relevance of an enhanced surgical knowledge of anatomical structures that are at a potential risk during the different steps of osteotomy or plate fixation. This pictorial essay aims to increase the awareness of such structures at risk to avoid possible injuries.
References
Agneskirchner JD, Hurschler C, Stukenborg-Colsman C, Imhoff AB, Lobenhoffer P (2004) Effect of high tibial flexion osteotomy on cartilage pressure and joint kinematics: a biomechanical study in human cadaveric knees. Winner of the AGA-DonJoy Award 2004. Arch Orthop Trauma Surg 124(9):575–584
Asada S, Akagi M, Mori S, Matsushita T, Hashimoto K, Hamanishi C (2012) Increase in posterior tibial slope would result in correction loss in frontal plane after medial open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 20(3):571–578
Attinger MC, Behrend H, Jost B (2014) Complete rupture of the popliteal artery complicating high tibial osteotomy. J Orthop 11(4):192–196
Bisicchia S, Rosso F, Pizzimenti MA, Rungprai C, Goetz JE, Amendola A (2015) Injury risk to extraosseous knee vasculature during osteotomies: a cadaveric study with CT and dissection analysis. Clin Orthop Relat Res 473(3):1030–1039
Black R, Green C, Sochart D (2013) Postoperative numbness of the knee following total knee arthroplasty. Ann R Coll Surg Engl 95(8):565–568
Darnis A, Villa V, Debette C, Lustig S, Servien E, Neyret P (2014) Vascular injuries during closing-wedge high tibial osteotomy: a cadaveric angiographic study. Orthop Traumatol Surg Res 100(8):891–894
Dexel J, Fritzsche H, Beyer F, Harman MK, Lutzner J (2015) Open-wedge high tibial osteotomy: incidence of lateral cortex fractures and influence of fixation device on osteotomy healing. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3730-5
Duivenvoorden T, van Diggele P, Reijman M, Bos PK, van Egmond J, Bierma-Zeinstra SM, Verhaar JA (2015) Adverse events and survival after closing- and opening-wedge high tibial osteotomy: a comparative study of 412 patients. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3644-2
Fowler PJ, Tan JL, Brown GA (2000) Medial opening wedge high tibial osteotomy: how I do it. Oper Tech Sports Med 8(1):32–38
Gerich T, Lens V, Seil R, Pape D (2014) Open wedge osteotomy of the tibial head Management of vascular complications. Orthopade 43(11):1008–1015
Han JH, Kim HJ, Song JG, Yang JH, Nakamura R, Shah D, Park YJ, Nha KW (2015) Locking plate versus non-locking plate in open-wedge high tibial osteotomy: a meta-analysis. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-015-3850-y
Jacobi M, Villa V, Reischl N, Demey G, Goy D, Neyret P, Gautier E, Magnussen RA (2015) Factors influencing posterior tibial slope and tibial rotation in opening wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 23(9):2762–2768
Kim J, Allaire R, Harner CD (2010) Vascular safety during high tibial osteotomy: a cadaveric angiographic study. Am J Sports Med 38(4):810–815
Lee SY, Lim HC, Bae JH, Kim JG, Yun SH, Yang JH, Yoon JR (2016) Sagittal osteotomy inclination in medial open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc. doi:10.1007/s00167-016-4115-0
Lee YS, Lee BK, Kim WS, Choi JS, Baek JR, Moon CW (2014) Sagittal and coronal plane location of the popliteal artery in the open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 22(11):2629–2634
Lobenhoffer P, Agneskirchner J, Zoch W (2004) Open valgus alignment osteotomy of the proximal tibia with fixation by medial plate fixator. Orthopade 33(2):153–160
Lobenhoffer P, Agneskirchner JD (2003) Improvements in surgical technique of valgus high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 11(3):132–138
Martin R, Birmingham TB, Willits K, Litchfield R, Lebel ME, Giffin JR (2014) Adverse event rates and classifications in medial opening wedge high tibial osteotomy. Am J Sports Med 42(5):1118–1126
Martinez de Albornoz P, Leyes M, Forriol F, Del Buono A, Maffulli N (2014) Opening wedge high tibial osteotomy: plate position and biomechanics of the medial tibial plateau. Knee Surg Sports Traumatol Arthrosc 22(11):2641–2647
Pape D, Adam F, Rupp S, Seil R, Kohn D (2004) Stability, bone healing and loss of correction after valgus realignment of the tibial head. A roentgen stereometry analysis. Orthopade 33(2):208–217
Pape D, Dueck K, Haag M, Lorbach O, Seil R, Madry H (2013) Wedge volume and osteotomy surface depend on surgical technique for high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 21(1):127–133
Pape D, Lorbach O, Schmitz C, Busch LC, Van Giffen N, Seil R, Kohn DM (2010) Effect of a biplanar osteotomy on primary stability following high tibial osteotomy: a biomechanical cadaver study. Knee Surg Sports Traumatol Arthrosc 18(2):204–211
Pape D, van Heerwaarden R, Haag M, Seil R, Madry H (2014) Osteotomy techniques close to the knee. Effect on wedge volume and bony contact surface. Orthopade 43(11):966–975
Schafer R, Mittag F, Wunschel M (2010) Arterial occlusion caused by a non-adsorbable bone graft after open wedge tibial osteotomy. Knee 17(2):174–175
Schroter S, Freude T, Kopp MM, Konstantinidis L, Dobele S, Stockle U, van Heerwaarden R (2015) Smoking and unstable hinge fractures cause delayed gap filling irrespective of early weight bearing after open wedge osteotomy. Arthroscopy 31(2):254–265
Shenoy PM, Oh HK, Choi JY, Yoo SH, Han SB, Yoon JR, Koo JS, Nha KW (2009) Pseudoaneurysm of the popliteal artery complicating medial opening wedge high tibial osteotomy. Orthopedics 32(6):442
Staubli AE, De Simoni C, Babst R, Lobenhoffer P (2003) TomoFix: a new LCP-concept for open wedge osteotomy of the medial proximal tibia—early results in 92 cases. Injury 34(Suppl 2):B55–B62
Staubli AE, Jacob HA (2010) Evolution of open-wedge high-tibial osteotomy: experience with a special angular stable device for internal fixation without interposition material. Int Orthop 34(2):167–172
Takeuchi R, Ishikawa H, Kumagai K, Yamaguchi Y, Chiba N, Akamatsu Y, Saito T (2012) Fractures around the lateral cortical hinge after a medial opening-wedge high tibial osteotomy: a new classification of lateral hinge fracture. Arthroscopy 28(1):85–94
Woodacre T, Ricketts M, Evans JT, Pavlou G, Schranz P, Hockings M, Toms A (2016) Complications associated with opening wedge high tibial osteotomy—a review of the literature and of 15 years of experience. Knee 23(2):276–282
Zaidi SH, Cobb AG, Bentley G (1995) Danger to the popliteal artery in high tibial osteotomy. J Bone Joint Surg Br 77(3):384–386
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare no competing interests. In particular, the authors did not receive and will not receive any benefits or funding from any commercial party related directly or indirectly to the subject of this article.
Rights and permissions
About this article
Cite this article
Madry, H., Goebel, L., Hoffmann, A. et al. Surgical anatomy of medial open-wedge high tibial osteotomy: crucial steps and pitfalls. Knee Surg Sports Traumatol Arthrosc 25, 3661–3669 (2017). https://doi.org/10.1007/s00167-016-4181-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-016-4181-3