Abstract
Neurodegenerative diseases (NDD) are incurable and the most prevalent cognitive and motor disorders of elderly. Mitochondria are essential for a wide range of cellular processes playing a pivotal role in a number of cellular functions like metabolism, intracellular signaling, apoptosis, and immunity. A plethora of evidence indicates the central role of mitochondrial functions in pathogenesis of many aging related NDD. Considering how mitochondria function in neurodegenerative diseases, oxidative stress, and mutations in mtDNA both contribute to aging. Many substantial reports suggested the involvement of numerous contributing factors including, mitochondrial dysfunction, oxidative stress, mitophagy, accumulation of somatic mtDNA mutations, compromised mitochondrial dynamics, and transport within axons in neurodegenerative disorders including Alzheimer’s disease, Parkinson’s disease, Huntington’s disease, and Amyotrophic Lateral Sclerosis. Therapies therefore target fundamental mitochondrial processes such as energy metabolism, free-radical generation, mitochondrial biogenesis, mitochondrial redox state, mitochondrial dynamics, mitochondrial protein synthesis, mitochondrial quality control, and metabolism hold great promise to develop pharmacological based therapies in NDD. By emphasizing the most efficient pharmacological strategies to target dysfunction of mitochondria in the treatment of neurodegenerative diseases, this review serves the scientific community engaged in translational medical science by focusing on the establishment of novel, mitochondria-targeted treatment strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neurodegenerative diseases are diverse group of devastating, and incurable condition, defined by the gradual deterioration and death of cells in the central nervous system. These pathological conditions, such as Alzheimer’s disease (AD), Parkinson’s disease (PD), Huntington disease (HD), and amyotrophic lateral sclerosis (ALS), are distinguished by the gradual loss of neuron cells, impaired motor or cognitive functions, and abnormal accumulation aggregated proteins. An increasing amount of research on NDD shows changes to the brain’s reduction–oxidation (redox) equilibrium as well as bioenergetics deficits (Yap et al. 2009).
The clinical manifestations of neurodegenerative diseases can be widely defined, with pyramidal and extrapyramidal movement abnormalities and cognitive processing impairments is perhaps the most frequent (Amor et al. 2010; Lyman et al. 2014). Few people have homogeneous syndromes, with the majority having a combination of clinical features. Diagnostic precision is crucial because it allows for more accurate prognosis and frequently informs particular care and treatment. But though particular protein accumulates in significant amounts and morphologic vulnerability are closely correlated with neurodegenerative diseases (NDD). Several more underlying principles characterized by a progressive neurological malfunction, such as proteotoxic stress in the ubiquitin and lysosomal systems, reactive oxygen species (ROS), apoptosis, and inflammation, are shared by neurodegenerative diseases (Cenini et al. 2019; Umare et al. 2021).
The cytosolic organelles “mitochondria” is crucial for birth as well as death. Abundant evidence from preclinical and clinical research shows that mitochondria are important in aging, cancer, hyperglycemia, and neurological diseases like Alzheimer’s, Huntington’s, and Parkinson’s disease (Lin and Beal 2006). Mitochondrial malfunction supposed to be a key in the ROS generation, is the fundamental cause of several forms of neurodegenerative illnesses. In neurodegenerative disorders, many evidences suggesting altered mitochondrial architecture and functions, including structure, size, location, and mobility, have appeared recently (Chen et al. 2012; Onyango et al. 2010). Besides looking at neurodegenerative disorders in general, a complete knowledge of mitochondrial activity and their involvement in degeneration might open up new avenues for the management of progressive neurodegenerative diseases. Mitochondria have been identified as critical organelles in the complicated interaction among neurodegeneration since they are both a generator of innate immune signals.
Mitochondrial defensive agents offer a possible novel approach to developing drug compounds that can alter the pathophysiology of neurodegeneration (Moreira et al. 2010). The new finding that mitochondrial dysfunction is at the root of several NDD has given rise to new targeted therapies aimed at preserving/improving mitochondrial function (Missiroli et al. 2020; Umare et al. 2021). Excessive generation of oxygen species by mitochondria, both actively and as a secondary result of all other malfunctions, alteration in energy metabolism, mitochondrial dynamics as well as transport and mutation, are substantial sources of problems in well almost all scenarios in which mitochondrial dysfunction makes a significant contribution to disease. The new revelation that mitochondria seem to be at the crossroads of a cell’s death and life, especially through the engagement of mitochondrial dysfunction in plethora of diseases, has created mitochondria an exciting target for new drugs as well as treatment strategies (Blesa et al. 2015; Picca et al. 2021).
Healthy Mitochondria
Mitochondria are versatile organelles which are already inherited from the mother and form clusters in several cells that keeps the intricate balance of fusion, fission, mitochondrial generation, and mitophagy (Ma et al. 2020). Even though mitochondria are primarily known for producing and storing energy from the oxidation of complex molecules under aerobic conditions via oxygen consumption, their numerous anabolic features are largely neglected (Giorgi et al. 2012; Herst et al. 2017). Cellular energy is primarily produced through oxidative phosphorylation inside mitochondria that are essential organelles for many biological processes such as metabolic activities, lipid biogenesis, calcium homeostasis, and programmed cell death (Guzy and Schumacker 2006). Due to the general significant level of ATP production required to maintain neuronal energy demands, oxidation of glucose is the vital energy source in the central nervous system. Since ATP could not be preserved, the mitochondria should produce large quantities of ATP continuously, takes about 25% of the overall volume of the cell (Mergenthaler et al. 2013).
The fundamental mitochondrial function is to transform the byproducts of glucose, polypeptide, and fat oxidation to carbon dioxide and water by employing the electron transport chain’s (ETC) essential enzymes of complexes I to IV. Ions (H+) are pushed out from matrix to the inter-cristae region during such events, forming a gradient of protons. Through complex V, protons moving back along this gradient start to produce ATP. This process of generating ATP with substrate oxidation in the mitochondria is called as oxidative phosphorylation, and is vital for the health of many body tissues (Hall et al. 2012). Because the onset of metabolic complications is usually characterized by a disturbance in mitochondrial activity, malfunction of above complexes of mitochondria could also display an integral role throughout the development of several chronic illnesses (Giorgi et al. 2012; Upaganlawar et al. 2021).
Mitochondria significantly influence several biochemical cell signaling pathways. It can decode a wide range of extracellular inputs into various intracellular responses, spanning from energy generation to cell mortality. The careful regulation of mitochondrial calcium (Ca2+) balance is critical in several activities involving this organelle. Based on the tissues engaged, numerous pathogenic diseases might emerge when mitochondrial Ca2+ equilibrium is disrupted. Recent research has given insight on the chemical identities of the key proteins that are involved in mitochondrial Ca2+ trafficking (Calì et al. 2012; Erustes et al. 2021; Giorgi et al. 2012; Loncke et al. 2021; Mitochondrial Ca et al. 2022).
In addition to fulfilling the traditional function of providing the cell with energy, mitochondria actively control innate immune responses to sterile insults and infectious agents (Banoth and Cassel 2018; Missiroli et al. 2020). This can happen in two means: firstly, by direct stimulating the production the immune system response, and subsequently, by modifying a reaction. Direct stimulation is frequently associated with mitochondrial injury or dysfunction, although modulation can be found as a consequence of healthy mitochondrial processes and activities (Banoth and Cassel 2018).
Mitochondria perform important part in cell’s apoptotic process activation (Wang and Youle 2009). The stimulation of caspases results in fragmentation and destruction of various cellular components, which is crucial to apoptosis control. Members of Bcl-2 family govern the discharge of proteins from the space between the mitochondrial inner and outer membrane that, once in the cytosol, stimulate caspase proteases which de-stabilize cells and signal effective phagocytosis of cell corpses (Picca et al. 2021; Tsujimoto 1998). Hence, caspase expression must be and is strictly regulated. In humans, mitochondrial pathway has been considered as one of the primary apoptotic routes. It is an important site for the interaction of both antiapoptotic and proapoptotic enzymes which determines cell’s fate. Moreover, it is the source of signals that initiate caspase activation via multiple processes and are stimulated by cytotoxic stress (Fulda and Debatin 2006; Vringer and Tait 2019).
What Goes Wrong in Neurodegenerative Disorders
Abundance of reports supports that significance of mitochondrial affliction in the pathological development of neurodegenerative disorders (Chen et al. 2012; Lin and Beal 2006). Parkinson’s disease (PD), Alzheimer’s disease (AD), Amyotrophic Lateral Sclerosis (ALS), and Huntington’s disease (HD) are some of the most common of these disorders, and they are all delineated by marked neuronal cells loss, impaired cognitive and motor functions, and an abnormal aggregated proteins accumulation [3,30]. The key risk factor for many human illnesses, including NDD, is aging (Akbar et al. 2016; Balaban et al. 2005; Cadenas and Davies 2000; Umare et al. 2021). A plethora of evidence supports impairments in bioenergetics along with brain’s reduction–oxidation (redox) homeostasis alterations with the increasing of the age (Fig. 1). The overall “mitochondrial theory of aging” supports the association of mitochondria in aging and associated disorders like NDD (Cobley et al. 2018; Gandhi and Abramov 2012; Trivedi 2021).
Oxidative Stress
Reactive oxygen species (ROS) production are of biological significance in variety of physiological settings which involves cellular adaptation to hypoxia, immune response, repair processes, synaptic plasticity, differentiation, learning, and memory and cellular survival via mitophagy (Apel and Hirt 2004; Chen et al. 2012). As the brain particularly susceptible to oxidative stress induce injury, overproduction of ROS coupled with reduced antioxidants can aid to neuronal loss in neurodegeneration (Andersen 2004). ROS-induced damage first target mitochondrial structures, which undergo severe oxidative changes (Marde et al. 2022; Umare et al. 2022; Valko et al. 2007). Oxidative stress can alter the mitochondrial function in many different ways including mtDNA mutations, depressing the functions of the respiratory chain, varying mitochondrial membrane permeability; calcium homeostasis disturbances, and damage antioxidant system, altered mitochondrial permeability eventually causing apoptosis.
Nitrogen and reactive oxygen species are primarily produced by mitochondrial monoamine oxidase (MAO) B and complexes I and III, which are found inside the mitochondria. In PD and AD, a region-dependent modulation of MAO has been observed (Tong et al. 2017). Reduced mitochondrial complex I and III activities have been reported in postmortem AD brain (Cardoso et al. 2004). In PD, deficiency of NADH dehydrogenase and mitochondrial complex I in substantia nigra region has been reported (Gatt et al. 2016). As PD has multifactorial origin, environmental toxicants also play important role in pathologic mechanisms, which includes increased ROS in nigral dopaminergic neurons, oxidative phosphorylation inhibition leading to reduce ATP production, alteration in membrane potential and activation of mitochondrial cytochrome C (Agnihotri and Aruoma 2019). HD mainly involves dysfunctional striatum and cortex, and a decrease in activity of mitochondrial complex II has been reported in patients having HD as well as with injection of 3-nitropropionic acid, an animal models for HD implicating the role of striatal mitochondria in HD (Uddin et al. 2020). According to numerous studies disrupted Ca2 + homeostasis in striatal mitochondria was observed in HD mice. Though the involvement of oxidative stress in HD is unclear, the mutant HTT (mHTT) interaction with mitochondria thought to generate ROS mainly through disruption in Ca2 + homeostasis, which triggers the mitochondrial permeability transition pore (mPTP), leading to distorted ATP level and aids the release of cytochrome c, thereby further elevating ROS production (Zheng et al. 2018a). Substantial evidence indicates that an excess ROS production in ALS to be associated with an impaired antioxidant defense attributing mitochondrial dysfunction as important pathological feature associated with neurodegeneration in ALS (Cunha-Oliveira et al. 2020).
Mitochondrial Bioenergetics
In the brain, flexibility of metabolic functions rely on the interplay between mitochondrial oxidative phosphorylation systems (OXPHOS) and glycolytic pathways. The mitochondrial OXPHOS uses amino acids, fatty acids, and glucose as substrates to generate reducing equivalents, which are then converted to ATP. On the other hand, elevated levels of H2O2 are thought to mediate the negative consequences connected to mitochondrial dysfunction in NDD since they have been linked to redox alterations in the mitochondria and macromolecule oxidation throughout aging. Glutathione (GSH) or thioredoxin (Trx)-driven enzymes in the brain mitochondria mostly remove H2O2 and rely on NADPH as the final electron donor. With regard to NDD, including PD, AD, HD, and ALS, there is overwhelming proof that OXPHOS is altered as a result of the accumulation of misfolded proteins brought on by gene mutations or abnormal protein homeostasis (Kawamata and Manfredi 2018; Marde et al. 2021; Wankhede et al. 2022).
Mitochondrial dysfunction due to failure in bioenergetics has been well reported in AD. The positron emission tomography (PET) confirms altered glucose uptake has been linked with the cognitive impairment in AD. Additional, brain atrophy in AD has been associated with impaired mitochondrial transport (Cunnane et al. 2020). Mutation in AD affects mitochondrial Ca2 + signaling and reduces OXPHOS function thereby reducing the further ATP deficit, increased ROS, altered cellular Ca2 + homeostasis and reduced protein synthesis (Dematteis et al. 2020). The PET studies of PD brain reported mitochondrial dysfunction in dopaminergic neurons along with reduced glycolysis and mitochondrial complex I activity (Zambon et al. 2019). Additionally, aberrant pyruvate and glucose metabolism has been reported in AD and PD. The accumulation of mtDNA with subsequent reductions in OXPHOS are thought to responsible for neurodegeneration in AD and PD (Area-Gomez et al. 2019). In HD, the mutant Htt impairs axonal transport in the motor neurons and also affects glucose uptake altering the ATP generation, reduced mitochondrial function and oxidative phosphorylation in HD neurons (Cunnane et al. 2020). Numerus studies reported reduction in glycolysis as well as mitochondrial function, impaired pentose phosphate pathway in ALS. Moreover, impaired mitochondrial energetics and in astrocytes has been linked with ALS (Allen et al. 2019; Delic et al. 2018; Tefera et al. 2019).
Mitochondrial Damage and Mutation
Mitochondrial dysfunction, a causal factor of aging, is characterized by abnormal cellular redox generation and excess mitochondrial DNA accumulation (mtDNA). The strong relation between mtDNA mutation as well as the production of ROS is, however, still debatable. The mtDNA is more prone to oxidative damage as compared to nuclear DNA, thus in weak antioxidant defense it gets easily damaged by excess generation of ROS. Also, the mutant mtDNA accumulation may reduce the ETC capabilities, resulting in lower adenosine triphosphate generation and higher ROS production (Cha et al. 2015; Xia et al. 2009). Oxidative damage to mtDNA in the brain changes with increased age and can result in multiple point mutations. Numerous somatic mtDNA mutations caused by ROS or other processes may aggregate in the nervous system with age and hence have a contribution in aging and NDD, although being uncommon at any one place (Simon et al. 2004).
Mitochondrial genetic malfunction has also been linked to Alzheimer’s disease pathogenesis. Damaged DNA lesions caused by ROS are substantially more common in AD tissues. Degraded mtDNA and associated proteins have also been discovered in the brain of AD patients, and the base excision repair (BER) mechanism has been reported to be faulty (Canugovi et al. 2014; Krishnan et al. 2012). Similarly in AD, tends to be characterized by mitochondrial malfunction. Microscopy of AD brain tissues demonstrates structural abnormalities in mitochondria. These alterations are often linked with the overproduction of ROS, a reduction in ATP levels, and increased release of cytochrome c oxidase along with mtDNA into the cytosol, which together aggravate neurotoxicity (Zheng et al. 2018b; Zorov et al. 2014).
Individuals having high levels of mtDNA mutations frequently exhibit significant neurological dysfunction, also with extent of neurodegeneration varied largely depending on the kind of mutation and the mtDNA mutation burden across the brain. The research for mitochondrial malfunction and mtDNA mutations being involved in PD is arguably greatest. The discovery of family versions of the illness reveals that a variety of genetic alterations are related with mitochondria and have roles in ROS damage (Taylor and Turnbull 2005; Upaganlawar et al. 2021). Numerous factors have been associated with dopaminergic neurons degeneration which includes, excess ROS, mtDNA mutations, and mitochondrial mechanisms malfunction. Furthermore, ETC deficit in dopaminergic neurons causes mitochondrial disruption and a reduction in the delivery of new mitochondria to dopaminergic neuron endings in the striatum (Ciccone et al. 2013). Mitochondrial dysfunction has also been linked with the pathogenesis of Huntington’s disease (HD), with mitochondrial biochemical deficiencies and impaired mitochondrial enzyme activity being observed in HD patients. Huntingtin mHtt or polyQ segments can also cause mitochondrial malfunction. Moreover, investigations have shown that mutated Htt associated ROS targets mtDNA predominantly, which might contribute to mitochondrial change. Also, studies suggested APE1, an BER enzyme is a key target in the preservation of mitochondrial function in HD (Choo et al. 2004; Jimenez-Sanchez et al. 2017; Walker 2007). Also, it has already been postulated that somatic mtDNA mutations might perform a part in the development of a range of distinct neurological illnesses. Elevated concentrations of mutations have been associated with amyotrophic lateral sclerosis, multiple sclerosis, and even neurodevelopmental disorders (Campbell and MacQueen 2006; Simon et al. 2004).
Mitochondrial Quality Control
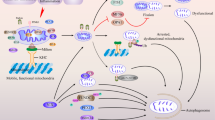
The cell has mitochondrial quality control (MQC) system responsible for overcoming the defects in the mitochondria. It includes processes such as mitochondrial biogenesis, mitochondrial proteostasis mitochondrial dynamics as well as mitophagy (Fig. 2) (Anzell et al. 2017). MQC represents the equilibrium between the rate of biogenesis and degradation (Dominy and Puigserver 2013). The combination of these mechanisms demonstrates mitochondrial quality control, particularly crucial in cellular illnesses ranging from basic mitochondrial hereditary defects to secondary mitochondrial diseases such as neurodegenerative, inflammatory diseases (Chang et al. 2020; Criscuolo et al. 2021; Suliman and Piantadosi 2015). MQC processes play a crucial part in regulating mitochondrial structure and activity. MQC is made up of three primary components: the mitochondrial dynamics, ubiquitin–proteasome system (UPS), and mitophagy. The UPS system has the ability to modulate the levels of proteins associated with mitochondrial dynamics and death receptors. The UPS is broadly active during perkin-dependent mitophagy and plays crucial roles. Mitophagy is heavily influenced by mitochondrial dynamics (Palikaras and Tavernarakis 2012; Suen et al. 2008; Wei et al. 2015). Thus, abnormal MQC can be important mechanism pathogenesis of the origination and progression of neurodegenerative diseases, making it an important therapeutic target (Wang et al. 2021b; Yan et al. 2020).
Mitochondrial quality control (MQC) system. (AMPK) AMP-activated protein kinase, (PGC1α) Peroxisome proliferator-activated receptor–gamma coactivator 1 alpha; (NRF-1/2) nuclear respiratory factor ½; (ERR-α) estrogen-related receptor-alpha; (PPAR-γ) peroxisome proliferator activated receptors; (TFAM) transcription factor A; (mtDNA) mitochondrial DNA, (MPC) mitochondrial pyruvate carrier, (OXPHOS) oxidative phosphorylation system, (Fis1) mitochondrial fission protein 1, dynamin-related protein 1( Drp1), optic atrophy protein 1(OPA1), (MFN2) mitofusin 2, (LC3) microtubule-associated proteins 1A/1B light chain 3. MQC system ensures the mitochondrial homeostasis via biogenesis of mitochondria, its dynamics and mitophagy. Through the appropriate stimuli or AMPK triggers the different transcription factors such as PGC1α and TFAM via PGC1α-ERR-α or PPAR-γ-PGC1α-NRF1/2 pathway. TFAM reaches MTDNA through mitochondrial import machinery and upregulates expression of different genes involved in mitochondrial biogenesis and dynamics. Mitochondrial components are ultimately recycled through a specialized pathway, mitophagy
Impaired Mitochondrial Biogenesis
Cell triggers mitochondrial biogenesis as a result of increased demand and is regulated via several signaling pathways in response to stimulus. The peroxisome proliferator-activated receptor–gamma coactivator 1 alpha (PGC-1α) regulates the mitochondrial biogenesis; along with numerus transcription factors, includes nuclear respiratory factor (NRF-1/2) and peroxisome proliferator activated receptors (PPARs). The activation of NRF-1/2 pathway via PGC-1α stimulates transcription factor A (TFAM) and other proteins expression [31–32]. The activation of PGC-1α is also associated with high energy consumption and uptake. Another protein AMPK, AMP-activated protein kinase deals with mitochondrial biogenesis. Oxidative stress affects activation of AMPK thereby disturbing mitochondrial biogenesis. AMPK activation also stimulates PGC- 1α pathway, thereby improves biogenesis through PGC-1α-NRF-2 pathway (Fig. 2) (Elfawy and Das 2019). Thus, the proteins involved in mitochondrial biogenesis can also act as therapeutic targets for neurodegenerative diseases. Potential role of PPARγ-PGC1α-NRF2 in the initiation and maintenance of mitochondrial biogenesis makes it a potential target and strategies targeting PPARγ-PGC1α-NRF2 signaling plays promising role in developing newer treatment for NDD (Jamwal et al. 2021).
Number of studies reported reduced level of PGC-1 in neurodegenerative conditions like AD, PD, and HD, whereas overexpression of molecule was found to exert neuroprotection in disease models, some conflicting reports also suggested deleterious effect associated with PGC-1 overexpression in dopaminergic neurons (Ciron et al. 2012; Jones et al. 2012). The relative number of mitochondria was found to reduce in HD brains, along with PGC-1 and TFAM (Kim et al. 2010). Furthermore, neurodegenerative lesions in the striatum was seen in PGC-1 null mice model of HD (Lin et al. 2004; Oliveira 2010). In AD patients, the low number of mitochondria along with reduced expression of PGC-1, NRF1, NRF2, and TFAM (Calkins et al. 2011; Hirai et al. 2001; Sheng et al. 2012). Both the levels of PGC-1 and NRF-1 were declined in brain region associated with PD. Additionally, PGC-1 polymorphisms have been associated with PD and HD (Che et al. 2011; Clark et al. 2011; Shin et al. 2011; Weydt et al. 2009). In PD, reduced neurogenesis has been associated with the loss of PARKIN, which directly linked with the downregulation of expression of PGC-1 in basal ganglia (Wang et al. 2021b).
Impaired Mitochondrial Dynamics
Mitochondria are structured in a dynamically changing matrix that undergoes continual fusion and fission in necessary to undertake their activities in the most efficient manner continuously. The processes of fission and fusion of mitochondria are crucial in the formation of new as well as the removal of defective mitochondria. Mitochondria create a densely linked tubular network all across the cell, which encompasses mitochondrial segments constantly breaking away and fusing (Walker et al. 2020; Youle and van der Bliek 2012a, b) (Fig. 2).
The process of fission results in the mitochondrial fragmentation followed by its elimination via mitophagy. (Burman et al. 2017; Frank et al. 2012; Scott and Youle 2010). Several mitochondrial proteins are involved in fission process including mitochondrial fission protein and factor (Fis1 & Mff), GTPase dynamin-related protein 1 (Drp1) and mitochondrial dynamics of 51 kDa protein (MiD51) (Youle and Van Der Bliek 2012a, b; Zhang et al. 2016). Fis1, is an OMM protein which act as receptor for Drp1. Normally Drp1 binds to Fis1 at tetratricopeptide repeat (TPR) present on cytosolic side leads to constriction of mitochondrial outer membrane resembling like ring (Gomes and Scorrano 2008; Panchal and Tiwari 2019; Youle and Van Der Bliek 2012a, b). Oligomerization of Drp1 and subsequent binding with GTP hydrolysis is necessary step in mitochondrial fission. Thus, hyperactivation of Drp1 may lead to mitochondrial fragmentation leading to neuronal death (Feng et al. 2020; Manor et al. 2015). The high rate of fission can hinders the elimination rate of impaired mitochondria; thus, it gets accumulated affecting ETC activity and thereby energy production (Twig et al. 2008). In fusion mitochondria merged to each other in order to preserve mitochondrion for survival and growth during embryonic development (Chen 2011). Different proteins that carry out mitochondrial fusion process are Mitofusin 1, 2 (Mfn1&2), on OMM and Optic Atrophy (Opa1) protein, IMM (Panchal and Tiwari 2019). Numerous studies have stated that altered Mfn2 and Drp1 expression are involved in different NDs pathologies (Fig. 3) (Chen et al. 2003; Gao et al. 2017).
Disrupted mitochondrial fusion and fission have been implicated as major pathogenic components supporting a variety of neurodegenerative diseases pediatric and older people. Because mitochondrial activities are vital, severe mitochondrial fission causes brain malfunction. The buildup of alpha-synuclein and tau in the brains of individuals suffering from neurodegenerative illnesses has also been associated to the impaired mitochondrial fission function. Numerous studies have reported upregulation of fission-related genes such as Drp1 and Fis1, which interact with amyloid-β and tau protein results in fragmentation of mitochondrial in AD (Kandimalla and Reddy 2016).
Increased ROS production one of the target for ROS is regulators of fission proteins thus hampers mitochondrial dynamics in AD (Wang et al. 2008). The Appl gene reported to enhance the fusion process thereby indirectly affecting axonal transport resulting in neuronal loss in AD. Additionally, tau has also been associated with mitochondrial dynamics by interacting with Drp1 (DuBoff et al. 2012; Manczak and Reddy 2012). The mitochondrial dynamics are also controlled by LRRK2 thus its overexpression can lead to increase expression of fission protein resulting in mitochondrial fragmentation (Westermann 2012; Yang et al. 2014). Another ALS gene, TAF15 expression can affect the mitochondrial dynamics, enhancing mitochondrial fragmentation (Altanbyek et al. 2016).
Mitophagy
Mitophagy was initially presented in the research world in 2005 to define a cellular complex process that involves selective sequestering and destruction of old or damaged mitochondria. Under body’s normal settings, mitochondria use mitophagy to supply critical macromolecular components for cells and defend against both neurodegeneration and the buildup of defective mitochondria (Chen and Chan 2009; Palikaras and Tavernarakis 2012; Rodolfo et al. 2018). The aggregation of defective and malfunctioning mitochondria has also been described as an early sign that contributes to various neurodegenerative diseases. Under physiological setting the dysfunctional mitochondria has been selected through fission for fragmentation, then degraded in lysosomes. Mitophagy declines with age which further results in an accumulation of dysfunctional mitochondria (Wang et al. 2019).
Mitochondrial malfunction in these disorders generates bioenergetic shortage, cellular calcium disequilibrium, and excessive ROS production, worsening the effects of Amyloid and tau abnormalities and contributing to synaptic dysfunction, cognitive deficits, and impaired memory (Chakravorty et al. 2019). Reduced function and efficiency of mitochondria in CNS, especially in the hippocampus, are linked to aging process and a variety of neurodegenerative illnesses that impair cognition. Moreover, synaptic and intellectual impairment are heterogeneous, accumulating evidences shows that mitochondria are crucial in all these pathways but also that preserving mitochondrial activity may help to avoid age-related and neuronal changes (Guo et al. 2017).
Defective mitophagy has been found in the neurodegenerative patients, which has been mainly linked with the disease-related genes (Wang et al. 2021a). Several pathways are involved in mitochondria targeted degradation via autophagosome, among which PTEN-induced putative kinase protein 1 (PINK1)/cytosolic E3 ubiquitin ligase PARKIN has been the most explored pathway for mitochondrial homeostasis in neurodegenerative diseases. Similarly, their dysfunction has been involved in the development of various disorders. Previous research has concentrated on the interaction between genes such as PINK1, Parkin, α-synuclein, LRRK2, and DJ-1 with mitophagy. The mitophagy has been directly or indirectly linked with PD, as it controls the calcium imbalance, oxidative stress and cell apoptosis via different mechanism (Wang et al. 2022a, 2021a). PD is frequently caused by mutations in the cytoprotective PINK-Parkin pathway. Furthermore, through collaborating with PINK-Parkin pathway, Drp1 is transported to the OMM, resulting in mitochondrial disruption and thereby increasing mitophagy (Ma et al. 2020; Picca et al. 2021). Also, the Drp1 defect has been associated upstream membrane depolarization and ROS production, thereby impairing mitophagy in PD (Feng et al. 2020). A higher rate of apoptosis has been associated with α-synuclein and its mutant forms, A53T α-synuclein, which suggests its involvement in mitochondrial apoptotic pathway. Another protein parkin is associated with the mitochondria, which prevents cell death by inhibiting cytochrome c release and caspase. Also, patients with parkin mutations shows selective impairment in mitochondrial complex I activity (Federico et al. 2012).
A growing body of evidences shows the involvement of α-synuclein in mitochondrial dynamics and mitophagy. In native form the α-synuclein promotes the fission while inhibits mitochondrial fusion, via interactive with Mfn 1/2 and Opa1. Under the pathological state, aggregation of α-synuclein in mitochondrial reduces activity of complex1 while promotes ROS production and impairs mitophagy (Feng et al. 2021a; Risiglione et al. 2021).
Though involvement of autophagy in HD is poorly understood, the impairment in fission/fusion has been reported in few studies. The Huntington protein Htt has been linked with mitophagy as it link the UNC-51-like kinase-1 (ULK1) and sequestosome 1 (SQSTM1/p62), supporting the mutation in Htt may lead to degeneration (Rui et al. 2015). In ALS, the localization of mSOD1 in the mitochondria activation cytochrome c with subsequent release of caspase and may contribute to apoptotic death (Takeuchi et al. 2016).
Mitochondrial Transport within Axons
Mitochondria have several important functions in adult neurogenesis. Their complicated neuronal movement patterns are distinguished by repeated directional changes. The movement can be anterograde or retrograde between cell body and axon in the direction of microtubules and is mediated by certain proteins which includes, kinesin motor protein, dynein motor protein, mitochondrial Rho GTPase (Miro) and Gamma-aminobutyric acid receptor-interacting factor-1/Trafficking kinesin-binding protein-2 (GRIF-1/TRAK2) (Mishra and Chan 2014). Moving mitochondria can be fixed or stall in places with significant metabolism, then move quickly again in accordance to metabolic responses. For the mitochondrial transport Miro attaches to the motor proteins through GRIF-1/TRAK2, followed by kinesin motor protein and dynein helps in the linking mitochondria and microtubule for the transport. Miro is important part of the axonal transport as it maintenance the mitochondrial motility at physiological Ca2 + concentration. Thus, the onset of neurodegenerative conditions can be due to energy deficiency at synapses because of improper transport between mitochondria and microtubules (Panchal and Tiwari 2019). Impairment in mitochondrial mobility have been associated with numerous major neurological conditions (Sheng and Cai 2012). During persistent neuronal excitability, mitochondria are frequently preserved in presynaptic terminals and postsynaptic dendritic spines(Li et al. 2004). Axonal transport abnormalities were identified as an initial pathogenic characteristic in a number of neurodegenerative disorders. Dynein-mediated alteration and ultimately affecting axonal transport in neurodegenerative diseases is correlated with dynein cytoplasmic 1 heavy chain 1 (DYNC1H1) and dynactin-1 (DCTN1) mutations. In AD, hyperphosphorylated of tau results in its detachment from microtubule resulting in microtubule destabilization and thus impairs axonal transport (Cunha-Oliveira et al. 2020). Amyloid precursor protein (Appl gene) in AD binds with kinesin protein and dynein motor protein which are associated with mitochondrial transport (Lin et al. 2017). Thus its overexpression can affect mitochondrial transport directly by reducing function of kinesin heavy chain (KHC) or indirectly via Tau protein (Wang et al. 2020). Other genes that are associated with the axonal transport include PINK 1 and Parkin. Evidences has revealed that PINK1 and Parkin-mediated phosphorylation of Miro protein arrest the process of axonal transport process (Lin et al. 2017). Additionally, α-synuclein and LRRK2 gene mutaion found to affect the mitochondrial axonal transport by altering microtubule stability (Melo et al. 2018; Sleigh et al. 2019). In HD, mutant Htt overexpression has been also associated with impaired mitochondrial axonal transport and mislocalization (Yang et al. 2021). Axonal transport disease linked to microtubules and neurofilaments is seen in a wide range of neurodegenerative conditions. Mutations in SOD1, one of several genes responsible for ALS, produce neurofilament phosphorylation as well as aggregation and an absence of motor complex formation in early cortical neurons (Guo et al. 2020). Furthermore, mutant TDP-43 expression in ALS impairs the axonal transport (Yang et al. 2021).
Targets for Developing Mitochondrial Medicine
Although some of the underlying processes for the neurodegenerative illnesses are unique to each one and eventually result in the degeneration of a particular subgroup of neurons, they all have similar degenerative characteristics, such as mitochondrial dysfunction(Gao et al. 2017). When mitochondrial homeostasis is negatively affected, pathologies like NDD arise which is a result of secondary mitochondrial dysfunctions (SMD). Defects in mitochondrial energy metabolism, dynamics, biogenesis, quality control etc. are major cause of SMD in NDD. There are only palliative treatments available for NDs right now (Table 1). More research is being done to develop medicines that specifically target mitochondria. There have been extensive efforts made in the creation of pharmacological techniques to reinstate mitochondrial integrity because of the wide range of disorders associated with mitochondrial dysfunction. This section will provide the most promising therapeutic targets (Umare et al. 2021; Upaganlawar et al. 2022).
Targeting Free-Radical Generation
For the normal functioning of the CNS, chemical integrity of brain is utmost important. Due to high oxygen requirement and lipid content, make the brain more prone to oxidative stress. Numerous neurodegenerative disorders like AD, PD, HD, and ALS are the result of biochemical changes due to excessive ROS production. Targeting mitochondrial ROS production is major strategy for the treatment of NDD(Onyango et al. 2010; Umare et al. 2021; Wankhede et al. 2022).
Antioxidants
To counteract the ROS protecting neuron cells and prevents neurodegenerative illnesses, a variety of neuroprotective treatments have been created to date. Specifically, these drugs are antioxidants which exert neuroprotective action by decreasing the oxidative stress and improvement in the overall mitochondrial health. These agents include Olanzapine, Melatonin, Z-LEHDFMK Mitoquinone, Riluzole, Dichloroacetate, Clozapine, N-acetylcysteine, Olesoxime, erythropoietin, vitamin E, Z-FA-MK and Cholest-4-en-3-one, which are extensively studied for their neuroprotective potential (Upaganlawar et al. 2021; Wu et al. 2019). Among these erythropoietin was found to be most promising agent which employ its action by regulating of oxygen balance, glycolysis and mitochondrial dynamics (Aliev et al. 2003; Rey et al. 2021). Several other antioxidants for instance coenzyme Q10, creatine and dimebon, exerts positive action in the AD and PD in preclinical studies, however, some were unsuccessful in the clinical trials (Reddy 2009; Wang et al. 2019).
The small peptide containing-tyrosine (SS-02 and SS-31) are reported as potent antioxidant in preventing oxidative neuronal death (Szeto 2008). These SS peptides act directly on mitochondrial inner membrane. The data from animal studies showed that SS02 and SS-31 readily penetrates the BBB and eliminate free radical in tert butyhydroperoxide (tBHP) mediated ROS generation in cell cultures (Szeto 2006). Evidences also have demonstrated effectiveness of these peptides in PD and ALS (Petri et al. 2006; Xiong et al. 2012).
Targeting Mitochondrial Bioenergetics
The modification of the redox state of mitochondria may serve as an alternate approach for treatment of NDD. There is a mounting body of evidence demonstrated that a diverse mitochondria-mediated signaling cascade is triggered by the mild inhibition of the OXPHOS complexes and enhances various pathways. Complex I inhibition aims to promote healthy aging, postpone the onset of neurodegenerative disease, and provide relief for a number of NDDs, such as AD, HD, PD, and AML. A growing body of evidence supports strong therapeutic potential of nicotinamide riboside, a precursor of NAD + , to prevent cognitive decline, synapse loss, and neuronal death. Additionally, pyruvate improves brain energetics via pyruvate dehydrogenase (Cerutti et al. 2014; Lautrup et al. 2019; Linnane et al. 1992).
OXPHOS Modulators
A number of evidence of mitochondrial alterations specifically, OXPHOS defects have been illustrated which results in neurodegenerative diseases (Kawamata and Manfredi 2018). Some agents act as OXPHOS modulators which employ their function through interacting with components of respiratory chain. Coenzyme Q10, an electron carrier in the ETC with antioxidant properties, extensively used for management of disorders associated with mitochondria. In addition, several neurogenic/neurodegenerative illnesses have been treated using coenzyme Q10 with its equivalents, idebenone and mitoquinone. Idebenone act by transferring of electrons from respiratory complex II to III (Orsucci et al. 2011). It has been investigated in various clinical studies for a range of mitochondria associated illnesses because of its antioxidant characteristics and safety profile(Paudel et al. 2020; Singh et al. 2021). Despite its clinical effectiveness in dealing with the Leber’s hereditary optic neuropathy (LHON), a Complex I disease, it has been less successful in clinical trials for other neurodegenerative diseases. This may be due to lack of neuronal NAD(P)H: quinone oxidoreductase 1 (NQO1) activity which has contributed to the limited efficacy of idebenone in neurodegenerative disease treatment. Reports conferred that carnosic acid–idebenone combination treatment promoted NQO1-dependent complex I bypass activity in neurons, as well as other brain cell types. This may be able to expose the neuroprotective therapeutic potential of idebenone or related quinones (Jaber et al. 2020).
Complex I Inhibitors
Inhibiting complex I partially with various small molecules, being studied in clinical trials has been used as a cutting-edge treatment NDD. In a small number of clinical trials, metformin, berberine, epigallocatechin-3-gallate, and resveratrol were tested for neurodegenerative illnesses (Rotermund et al. 2018; Wankhede et al. 2022). Another molecule that targets complex 1 resveratrol, it binds the mitochondrial complex 1 and shows pro- and antioxidant effects depending on dose (Gueguen et al. 2015). Recent study reported that, in AD partial inhibition of mitochondrial complex I with the small molecule compound CP2 triggers a variety of AMPK pathways that provide neuroprotection (Trushina et al. 2022). On contrary, complex I is also a significant cause for ROS production. Evidences revealed that inhibition of mitochondria complex I is a major cause of PD in drug abusers. Also the administration of rotenone found to mimic clinical features of PD in animals via complex-I inhibition thereby enhancing oxidative stress in nigral-striatal system (Xiong et al. 2012).
Mitochondrial Pyruvate Carrier
The mitochondrial pyruvate carrier (MPC) is another potential mitochondrial target for the treatment of NDD. The high amounts of energy needed for neural transmission are typically produced by oxidative phosphorylation in neurons, but other regions of the brain, comprising the parietal region and prefrontal cortices, were discovered to primarily rely on aerobic glycolysis. Because of this, the MPC in general play a crucial function in neurons. In these cells, pyruvate is mostly produced by glycolysis, while LDH may also convert lactate to pyruvate. The astrocyte-neuron shuttle is the primary source for lactate which is taken up by neurons from astrocytes. (Bélanger et al. 2011). Abundance of reports supports pharmacological MPC inhibition has been explored as a potential target for NDDs (Fig. 4) (Quansah et al. 2018; Zangari et al. 2020).
Possible Pathway in targeting mitochondrial pyruvate carrier to treat NDD. MPC-1, mitochondrial pyruvate carrier; α KG, alpha ketoglutarate; mTOR, mammalian target of rapamycin; ERR-α, estrogen-related receptor alpha; LAP, lapatinib ditosylate. Inhibition of MPC-1 through suppression ERR-α, inhibits mTOR hyperactivity and also shifts the source to glutamate for energy via oxidation which results in reduction of excitotoxicity mediated by glutamate. Inhibition of mTOR directly or indirectly ameliorate the neuroinflammation in NDD
The MSDC-0160 analog of MSDC-0602 K is being studied for treatments of AD and PD. The degeneration of hippocampal neurons in AD rat model has been thought to be ameliorated by blocking the MPC-1, which reduces the activation of the mammalian target of rapamycin (mTOR). In D-galactose/ovariectomized rats, an anti-cancer medication, lapatinib ditosylate (LAP), suppresses MPC-1 via decreasing estrogen-related receptor-alpha (ERR-alpha). According to a study, LAP plays an neuroprotective and anti-inflammatory role in the AD that targets MPC-1. In a phase 2 clinical study, individuals with AD had better cerebral glucose metabolism and less brain damage (Huang et al. 2020; Salomone et al. 2012).
As a single point, MPC is essential for pyruvate entry into the mitochondrial matrix, which in turn affects the energy metabolism that is impaired in PD. Treatment with MSDC-0160 enhanced motor behavior, reduced dopaminergic denervation, and diminished neuroinflammation and mTOR activity in unilateral 6-OHDA mice. Concurrently, MSDC-0160 treatment significantly altered energy metabolism, as seen by an increase in glutamate oxidation, β-oxidation, and ketogenesis to meet energy requirements and preserve energy homeostasis(Mallet et al. 2022). Its neuroprotective and anti-inflammatory characteristics were validated in a pre-clinical investigation using experimental models of PD (Ghosh et al. 2016).
Targeting Mitochondrial Biogenesis
A growing body of evidence supports beneficial effects of drugs targeting PPARγ-PGC1α-NRF2 in NDD. Pioglitazone, an FDA-approved medication, have been demonstrated to enhance biogenesis and mitochondrial function in diabetes individuals (Scarpulla 2011). Positive outcomes from pre-clinical research point to its potential for use in the treatment of neurological disorders linked to mitochondria (Masciopinto et al. 2012). A PPAR activator, thiazolidinediones (TZDs) has shown to improve cognitive impairments in AD via stimulating mitochondrial biogenesis (Cheng et al. 2015; Heneka et al. 2015; Risner et al. 2006; Watson et al. 2005). Analogous results were seen with resveratrol and 5- aminoimidazole-4-carboxamide ribonucleotide (AICAR) through AMPK thereby activating mitochondrial biogenesis (Vingtdeux et al. 2010). Resveratrol also decreases neurodegeneration via activating PGC-1α in AD, PD, HD, and ALS (Blanchet et al. 2008; Ho et al. 2010; Kim et al. 2007; Whitaker et al. 2016). Furthermore, melatonin improved PGC-1α signaling and also restores mitochondrial structure and function in AD (Simmons et al. 2020). In addition, resveratrol increases TFAM expression along with PGC-1α in animal model of PD, demonstrating improved biogenesis (Peng et al. 2016). Treatment with LY344864 improved the expression PGC-1α in different brain regions in PD (Scholpa et al. 2018).
The efficiency of pioglitazone was found in treatment of X-linked adrenoleukodystrophy (X-ALD) which is a neurodegenerative condition marked by mitochondrial and peroxisomal dysfunction, is being studied in a phase 2 clinical trial (Investigators 2015). Rosiglitazone, bezafibrate, and REN001 are additional medications that stimulate the PPAR-PGC-1 axis. Rosiglitazone specifically reduces mitochondrial dysfunction by boosting mitochondrial mass and bezafibrate boosts the ability of mitochondria to produce ATP by boosting mitochondrial proteins. It also found to ameliorate mitochondrial dysfunction in mHtt expressing neurons (Quintanilla et al. 2008). Sirtuin 1 (Sirt1) and AMPK are some potential targets to regulate PGC-1α and reestablish mitochondrial function. For both proteins, a number of activating substances have been discovered, some of which are now undergoing clinical trials for disorders linked to the mitochondria. Sirt1 activity may be controlled pharmacologically via allosteric modulators, also known as Sirt1-activating substances (STACs). Alternately, NAD + precursors often referred to as NAD + boosting molecules (NBMs), targets enzymes that activate NAD + production or prevent its breakdown, can be used to stimulate Sirt1 activation. The use of STACs and NBMs as prospective agents for neurodegenerative disorders associated with mitochondrial malfunction has been suggested by studies using murine models (See Fig. 3). Furthermore, the substantial findings supports the role of SIRT 1 agonists quercetin and resveratrol stimulate the mitochondrial biogenesis by activating sirtuins and AMPK, poses their beneficial effects in NDD (Cerutti et al. 2014; Morató et al. 2015; Valko et al. 2007). Triterpenoids have been shown to promote expression of gene elaborated in mitochondrial biogenesis, thereby activating NrF2 signaling (Tufekci et al. 2011).
Targeting Mitochondrial Dynamics
An important physiological mechanism called mitochondrial dynamics occurs in the appropriate arrangement of positioning of mitochondria in areas with high energy needs by coordinating fission and fusion activities. Neurodegenerative disease development is linked to changes in mitochondrial dynamics. Despite the fact that several genetic, pharmacological, and cellular investigations have suggested that mitochondria play a central role in the development of AD, anomalies in mitochondrial dynamic function are likely to contribute to mitochondrial and neuronal dysfunction (Fig. 4) (Reitz 2012; Smith et al. 1997). Recent research has focused on possible treatments for neurological diseases that target the fission proteins Drp1 and the fusion protein Mfn2. According to two studies, in both APP and tau transgenic models, the prevention of mitochondrial fragmentation by partial Drp1 impairment is adequate to reduce mitochondrial dysfunction resulting in synaptic loss (Kandimalla et al. 2016; Manczak et al. 2016).
Lysine deacetylases (KDAC) inhibitors have been reported to increase histone H3 acetylation and reduce Fis1 expression levels along with Drp1 recruitment without altering other fusion and fission proteins. These results suggest that mitochondrial elongation has been resulted from downregulation of Fis1 (Lee et al. 2012; Zhao et al. 2011).
Another compound quinazolinone which act as a Mdivi-1 inhibitor, found to selective inhibits DRP1 GTPase activity and thus impart neuroprotection and reduces mitochondrial fragmentation in AD and PD (Bordt et al. 2017; Manczak et al. 2019).
Targeting Mitochondrial Quality Control and Metabolism
The cell manages its mitochondria in an order includes both intra-mitochondrial activities like heme, protein replacement and activities like fusion, fission, mitochondrial biogenesis, and mitophagy. The combination of these mechanisms demonstrates MQC, which is particularly crucial in cellular illnesses ranging from basic mitochondrial hereditary defects to secondary mitochondrial diseases such as neurodegenerative, and inflammatory disorders (Cai and Tammineni 2016; Chang et al. 2020; Chen and Chan 2009). These conditions’ genetic and biochemical variability is strikingly comparable to that of several acquired disorders defined by metabolic as well as oxidative stress, exhibiting broad variability. This biologic variation reflects cell-specific and repair mechanisms, complicating reasonable pharmaceutical treatments not only for primary but also secondary mitochondrial diseases. Moreover, novel mitochondrial dynamics and turnover ideas, as well as new mitochondrial illness models, are giving opportunity to create and test MQC-based treatments (Nunnari and Suomalainen 2012; Warda et al. 2013).
Past studies have shown that there is equilibrium among mitochondrial fusion and fission in Alzheimer’s disease, which contributes to disorders pathophysiology. Numerous different investigations have discovered that the production of the Fis1 and the DRP1 are elevated in AD individuals and mutant APP-expressing AD animal models. Interruptions in mitochondrial proteostasis were reported repeatedly in AD. The accumulation of Aβ in AD, directly blocks the import channels, causing mitochondrial protein import to be disrupted and pre-protein maturation to be hampered. These disruptions result in mitochondrial malfunction (Goyal and Chaturvedi 2020). In Parkinson’s disease, irregular mitochondrial dynamics have been documented. It has been demonstrated that alpha-synuclein regulates mitochondrial morphology directly. Recent research has shown the molecular pathways causing alpha-synuclein induced mitochondrial morphological defects. The oligomeric alpha-synuclein attaches to the lipids in the OMM, disrupting membrane curvature and slowing mitochondrial fusion (Gilmozzi et al. 2020; Shaw et al. 2005). The number and form of mitochondria may be influenced by fission and fusion events. Quercetin, a flavonoid chemical derived from onions, and the herbal medicine bupleurum. Its therapeutic effects include increased anti-inflammatory and anti-tumor action. Furthermore, Quercetin has a substantial antioxidant impact on several cell types (Khan et al. 2018; Sandhir and Mehrotra 2013). Quercetin and icariin suppress excess mitosis in mitochondria generated by ROS or cAMP-dependent protein kinase and preserve normal mitochondrial number and quality (Kale et al. 2021; Liu et al. 2020; Tiwari et al. 2021). Resveratrol has the ability to drastically control Drp1 production, enhance mitochondrial lengthening, and boost parkin and PINK1 translocation. Resveratrol also considerably increases LC3-II expression at the same time. Additionally, it protects against oxidative stress produced by hypoxia/reoxygenation injury induced oxidative stress and the mitochondrial apoptotic pathway (Li et al. 2019). Another study reported that GTPase inhibitors such as dynasore regulates the expression of Drp1, ameliorating the motor deficits in PD. The study demonstrated that inhibition of Drp1 prevented excessive mitophagy and mitochondrial fragmentation via regulating the expression of PINK1 and parkin, thereby maintain mitochondrial homeostasis in PD (Feng et al. 2021b).
Other Approaches
Genome Editing and Gene Therapy
Modern genome editing tools are opening up new possibilities for gene therapy for a variety of disorders. Any nucleic acid, for gene addition and deletion like siRNA, cDNA, antisense oligonucleotide, RNA, or DNA editing enzyme, microRNA, can be delivered as a genomic carrier using transgenic methods. This method is used for delivery of cDNA delivery for the nerve growth factor (NGF), human aspartoacylase (ASPA), survival motor neuron (SMN), and AADC, and it has been found to be efficient and well tolerated (Hudry and Vandenberghe 2019). Despite of failure in early clinical trials to provide adequate therapeutic benefits gene therapy is rapidly becoming an important treatment approach for a variety of neurodegenerative conditions like AD, PD, and HD, principally suited for well-established and validated genetic models. Various viral (Adeno associated vectors and lentiviral vectors) REF (Marks et al. 2010; Rafii et al. 2018) and non-viral (Liposomes and nanoparticles) REF (Niu et al. 2017) gene vectors have been studied targeting neurodegenerative disorders. Also being intensively researched and improved delivery methods, such as direct injection or carriers such as liposomes and AAV9. Although, gene therapy using non-viral vectors has not yet been licensed as a treatment for neuronal degeneration, recent developments have created a lot of interest. A plethora of clinical and preclinical studies has been reviewed and describe the current advances of gene therapy for neurodegenerative illness (Chen et al. 2020). Future therapies are focused on editing the genes influencing mitochondrial dynamics. Additionally, overexpression of dynamic and stress controllers gene of mitochondrial, including HSP70, PGC-1, and TFEB, lessens neuronal damage in PD and HD, indicating that the technique may be important approache for various other neurodegenerative disorders (Li et al. 2013; Valdés et al. 2014). An additional cutting-edge method to treat mitochondrial dysfunction is mitochondrial transplantation is proven to be effective in treating neurodegenerative disorders. The delivery of mitochondria has been investigated in many PD models, which restored mitochondrial respiratory function enhanced mitochondrial activity, increased cell viability, and decrease of oxidative stress (Chang et al. 2019).
Caloric Restrictions and Exercise
There are other strategies aimed to enhance mitochondrial function to treat neurodegenerative diseases, it includes caloric restrictions and exercise. The goal of calorie restriction (CR) is to reduce caloric consumption while maintaining adequate nutritional levels and preventing malnutrition. ROS generation is reduced by CR, along with oxidative DNA damage and the aging-related transcriptional alterations. It is believed that sirtuins play a significant part in facilitating the positive role of CR on lifespan. Comparable to CR, overexpression of SIRT1 aids in extending life and lowering illness symptoms associated with neurodegenerative disorders (Cantó and Auwerx 2009; Cunha-Santos et al. 2016). CR stimulates autophagy and suppresses the PI3K/AKT pathway that may enhance atophagy and preserve mitochondria. Furthermore, CR-activate deacetylation of SIRT 3 and inhibition of cyclophilin D, ultimately prevents excitotoxicity. CR increases number of mitochondrial cristae and number of mitochondria (Khraiwesh et al. 2014).
Physical exercise is one of the most promising preventive measures for NDD progression. Exercise increases the biosynthesis, respiration, dynamics, and quality control of mitochondria in skeletal muscle. In neurodegenerative diseases like AD, there are well-established abnormalities in mitochondrial biogenesis and oxidative phosphorylation. Recent reports showed regular, moderate exercise appears to be especially effective at promoting mitochondrial biogenesis (Burtscher et al. 2021; Upaganlawar et al. 2021). Exercise boosts the ability of the mouse hippocampus to repair damaged DNA by activating mitochondrial uncoupling proteins (UCP) to control proliferation and ROS generated from the mitochondria (Andrews et al. 2005). In a animal model of AD and PD, exercise augmented the activity of multiple mitochondrial respiratory chain complexes (Bo et al. 2014; Schmidt et al. 2021). But the beneficial benefits of exercise on AD and PD patients are predominantly mediated by improved mitochondrial activity is yet to confirm (Frederiksen et al. 2018). The future challenge will be finding and analyzing the best exercise treatments for patients with neurodegenerative disorders. These efforts should provide practical therapy alternatives that patients may use at home.
Future Directions
Scientists anticipate that subsequent treatment efforts will consist of a combination of techniques addressing mitochondrial dysfunction from various sites of entry. It is difficult to determine which of the proposed techniques, and which combination, will be the most useful, if any. A positive perspective is that the discipline has unquestionably entered the therapy age. A plausible scenario is that a therapy for mitochondrial dysfunction will take several years from now. Apparent ideas, such as the link connecting mitochondrial malfunction and elevated and damaging ROS production, are far more nuanced than often assumed. Considering the absence of a treatment, it is critical to diagnose mitochondrial diseases since they are a common source of inherent metabolic inefficiencies. As a result, it is critical to raise mitochondrial information among researchers in order to discover novel mitochondrial targeted treatment. As there is the lack of treatment, the diagnosis of a mitochondrial disorder is critical for preventing further mitochondrial malfunction. To ensure safety in translation to humans, it is necessary to have a deeper knowledge of the molecular mechanisms. This includes developing biomarkers that can detect mitochondrial activity and the ability to trigger a healthy stress response. This article will provide a review of several promising developments as well as the numerous hurdles that remain in the search of the successful therapy for mitochondrial disorder.
Conclusion
Significant progress has been achieved in the development of therapeutic approaches in order to restore mitochondrial homeostasis. Mitochondria represent a crucial therapeutic target for a number of prevalent debilitating illnesses. However, there are still a lot of difficulties in developing new drugs for mitochondrial medicine. Additionally, there are a staggering number of pharmaceuticals, both synthetic and natural extracts that target this organelle. However, further development is required to provide novel treatment approaches, such as gene therapy techniques.
Availability of Data and Materials
Not applicable.
Code Availability
Not applicable.
References
Agnihotri A, Aruoma OI (2019) Alzheimer’s disease and Parkinson’s disease: a nutritional toxicology perspective of the impact of oxidative stress, mitochondrial dysfunction, nutrigenomics and environmental chemicals. J Am Coll Nutr 39:16–27. https://doi.org/10.1080/07315724.2019.1683379
Akbar M, Essa MM, Daradkeh G, Abdelmegeed MA, Choi Y, Mahmood L, Song BJ (2016) Mitochondrial dysfunction and cell death in neurodegenerative diseases through nitroxidative stress. Brain Res 1637:34–55. https://doi.org/10.1016/j.brainres.2016.02.016
Aliev G, Seyidova D, Lamb BT, Obrenovich ME, Siedlak SL, Vinters HV, Friedland RP, LaManna JC, Smith MA, Perry G (2003) Mitochondria and vascular lesions as a central target for the development of Alzheimer’s disease and Alzheimer disease-like pathology in transgenic mice. Neurol Res 25:665–674. https://doi.org/10.1179/016164103101201977
Allen SP, Hall B, Woof R, Francis L, Gatto N, Shaw AC, Myszczynska M, Hemingway J, Coldicott I, Willcock A, Job L, Hughes RM, Boschian C, Bayatti N, Heath PR, Bandmann O, Mortiboys H, Ferraiuolo L, Shaw PJ (2019) C9orf72 expansion within astrocytes reduces metabolic flexibility in amyotrophic lateral sclerosis. Brain 142:3771–3790. https://doi.org/10.1093/BRAIN/AWZ302
Altanbyek V, Cha SJ, Kang GU, Im DS, Lee S, Kim HJ, Kim K (2016) Imbalance of mitochondrial dynamics in Drosophila models of amyotrophic lateral sclerosis. Biochem Biophys Res Commun 481:259–264. https://doi.org/10.1016/J.BBRC.2016.10.134
Amor S, Puentes F, Baker D, Van Der Valk P (2010) Inflammation in neurodegenerative diseases. Immunology. Wiley Online Libr 129:154–169. https://doi.org/10.1111/j.1365-2567.2009.03225.x
Andersen JK (2004) Oxidative stress in neurodegeneration: cause or consequence? Nat Med 107(10):S18–S25. https://doi.org/10.1038/nrn1434
Andrews ZB, Diano S, Horvath TL (2005) Mitochondrial uncoupling proteins in the cns: in support of function and survival. Nat Rev Neurosci 611(6):829–840. https://doi.org/10.1038/nrn1767
Anzell AR, Maizy R, Przyklenk K, Sanderson TH (2017) Mitochondrial quality control and disease: insights into ischemia-reperfusion injury. Mol Neurobiol 553(55):2547–2564. https://doi.org/10.1007/S12035-017-0503-9
Apel K, Hirt H (2004) Reactive oxygen species: metabolism, oxidative stress, and signal transduction. Annu Rev Plant Biol. https://doi.org/10.1146/annurev.arplant.55.031903.141701
Area-Gomez E, Guardia-Laguarta C, Schon EA, Przedborski S (2019) Mitochondria, OxPhos, and neurodegeneration: cells are not just running out of gas. J Clin Invest 129:34–45. https://doi.org/10.1172/JCI120848
Balaban RS, Nemoto S, Finkel T (2005) Mitochondria, oxidants, and aging. Cell. https://doi.org/10.1016/j.cell.2005.02.001
Banoth B, Cassel SL (2018) Mitochondria in innate immune signaling. Transl Res 202:52–68. https://doi.org/10.1016/j.trsl.2018.07.014.Mitochondria
Bélanger M, Allaman I, Magistretti PJ (2011) Brain energy metabolism: focus on astrocyte-neuron metabolic cooperation. Cell Metab 14:724–738. https://doi.org/10.1016/j.cmet.2011.08.016
Blanchet J, Longpré F, Bureau G, Morissette M, DiPaolo T, Bronchti G, Martinoli MG (2008) Resveratrol, a red wine polyphenol, protects dopaminergic neurons in MPTP-treated mice. Prog Neuro-Psychopharmacology Biol Psychiatry 32:1243–1250. https://doi.org/10.1016/J.PNPBP.2008.03.024
Blesa J, Trigo-Damas I, Quiroga-Varela A, Jackson-Lewis VR (2015) Oxidative stress and Parkinson’s disease. Front Neuroanat. https://doi.org/10.3389/fnana.2015.00091
Bo H, Kang W, Jiang N, Wang X, Zhang Y, Ji LL (2014) Exercise-induced neuroprotection of hippocampus in APP/PS1 transgenic mice via upregulation of mitochondrial 8-oxoguanine DNA glycosylase. Oxid Med Cell Longev. https://doi.org/10.1155/2014/834502
Bordt EA, Clerc P, Roelofs BA, Saladino AJ, Tretter L, Adam-Vizi V, Cherok E, Khalil A, Yadava N, Ge SX, Francis TC, Kennedy NW, Picton LK, Kumar T, Uppuluri S, Miller AM, Itoh K, Karbowski M, Sesaki H, Hill RB, Polster BM (2017) The putative Drp1 inhibitor mdivi-1 Is a reversible mitochondrial complex I inhibitor that modulates reactive oxygen species. Dev Cell 40:583-594.e6. https://doi.org/10.1016/J.DEVCEL.2017.02.020
Burman JL, Pickles S, Wang C, Sekine S, Vargas JNS, Zhang Z, Youle AM, Nezich CL, Wu X, Hammer JA, Youle RJ (2017) Mitochondrial fission facilitates the selective mitophagy of protein aggregates. J Cell Biol 216:3231–3247. https://doi.org/10.1083/JCB.201612106
Burtscher J, Burtscher M, Millet GP (2021) The central role of mitochondrial fitness on antiviral defenses: an advocacy for physical activity during the COVID-19 pandemic. Redox Biol. 43:101976. https://doi.org/10.1016/J.REDOX.2021.101976
Reitz C (2012) Alzheimer’s disease and the amyloid cascade hypothesis: a critical review. Int J Alzheimers Dis. https://doi.org/10.1155/2012/369808
Cadenas E, Davies KJA (2000) Mitochondrial free radical generation, oxidative stress, and aging. Free Radic Biol Med. https://doi.org/10.1016/S0891-5849(00)00317-8
Cai Q, Tammineni P (2016) Alterations in mitochondrial quality control in alzheimer’s disease. Front Cell Neurosci. https://doi.org/10.3389/fncel.2016.00024
Calì T, Ottolini D, Brini M (2012) Mitochondrial Ca2+ and neurodegeneration. Cell Calcium 52:73–85. https://doi.org/10.1016/J.CECA.2012.04.015
Calkins MJ, Manczak M, Mao P, Shirendeb U, Reddy PH (2011) Impaired mitochondrial biogenesis, defective axonal transport of mitochondria, abnormal mitochondrial dynamics and synaptic degeneration in a mouse model of Alzheimer’s disease. Hum Mol Genet 20:4515–4529. https://doi.org/10.1093/HMG/DDR381
Campbell S, MacQueen G (2006) An update on regional brain volume differences associated with mood disorders. Curr Opin Psychiatry. https://doi.org/10.1097/01.yco.0000194371.47685.f2
Cantó C, Auwerx J (2009) Caloric restriction, SIRT1 and longevity. Trends Endocrinol Metab 20:325–331. https://doi.org/10.1016/J.TEM.2009.03.008
Canugovi C, Shamanna RA, Croteau DL, Bohr VA (2014) Base excision DNA repair levels in mitochondrial lysates of Alzheimer’s disease. Neurobiol Aging 35:1293–1300. https://doi.org/10.1016/j.neurobiolaging.2014.01.004
Cardoso SM, Proença MT, Santos S, Santana I, Oliveira CR (2004) Cytochrome c oxidase is decreased in Alzheimer’s disease platelets. Neurobiol Aging 25:105–110. https://doi.org/10.1016/S0197-4580(03)00033-2
Cenini G, Lloret A, Cascella R (2019) Oxidative stress in neurodegenerative diseases: from a mitochondrial point of view. Oxid Med Cell Longev. https://doi.org/10.1155/2019/2105607
Cerutti R, Pirinen E, Lamperti C, Marchet S, Sauve AA, Li W, Leoni V, Schon EA, Dantzer F, Auwerx J, Viscomi C, Zeviani M (2014) NAD(+)-dependent activation of Sirt1 corrects the phenotype in a mouse model of mitochondrial disease. Cell Metab 19:1042–1049. https://doi.org/10.1016/j.cmet.2014.04.001
Cha MY, Kim DK, Mook-Jung I (2015) The role of mitochondrial DNA mutation on neurodegenerative diseases. Exp Mol Med 47:e150. https://doi.org/10.1038/emm.2014.122
Chakravorty A, Jetto CT, Manjithaya R (2019) Dysfunctional mitochondria and mitophagy as drivers of Alzheimer’s disease pathogenesis. Front Aging Neurosci
Chang CY, Liang MZ, Chen L (2019) Current progress of mitochondrial transplantation that promotes neuronal regeneration. Transl Neurodegener 8:1–12. https://doi.org/10.1186/S40035-019-0158-8/FIGURES/2
Chang X, Zhang W, Zhao Z, Ma C, Zhang T, Meng Q, Yan P, Zhang L, Zhao Y (2020) Regulation of mitochondrial quality control by natural drugs in the treatment of cardiovascular diseases: potential and advantages. Front Cell Dev Biol. 8:616139. https://doi.org/10.3389/fcell.2020.616139
Che HVB, Metzger S, Portal E, Deyle C, Riess O, Nguyen HP (2011) Localization of sequence variations in PGC-1 influence their modifying effect in Huntington disease. Mol Neurodegener 6:1–7. https://doi.org/10.1186/1750-1326-6-1/TABLES/6
Chen C-M (2011) Mitochondrial dysfunction, metabolic deficits, and increased oxidative stress in Huntington’s disease. Chang Gung Med J 34:135–152
Chen H, Chan DC (2009) Mitochondrial dynamics-fusion, fission, movement, and mitophagy-in neurodegenerative diseases. Hum Mol Genet. https://doi.org/10.1093/hmg/ddp326
Chen H, Detmer SA, Ewald AJ, Griffin EE, Fraser SE, Chan DC (2003) Mitofusins Mfn1 and Mfn2 coordinately regulate mitochondrial fusion and are essential for embryonic development. J Cell Biol 160:189–200. https://doi.org/10.1083/JCB.200211046/VIDEO-3
Chen W, Hu Y, Ju D (2020) Gene therapy for neurodegenerative disorders: advances, insights and prospects. Acta Pharm Sin B 10:1347–1359. https://doi.org/10.1016/J.APSB.2020.01.015
Chen X, Guo C, Kong J (2012) Oxidative stress in neurodegenerative diseases. Neural Regen Res 7:376–385. https://doi.org/10.3969/j.issn.1673-5374.2012.05.009
Cheng H, Shang Y, Jiang L, Shi TL, Wang L (2015) The peroxisome proliferators activated receptor-gamma agonists as therapeutics for the treatment of Alzheimer’s disease and mild-to-moderate Alzheimer’s disease: a meta-analysis. Int J Neurosci 126:299–307. https://doi.org/10.3109/00207454.2015.1015722
Choo YS, Johnson GVW, MacDonald M, Detloff PJ, Lesort M (2004) Mutant huntingtin directly increases susceptibility of mitochondria to the calcium-induced permeability transition and cytochrome c release. Hum Mol Genet 13:1407–1420. https://doi.org/10.1093/hmg/ddh162
Ciccone S, Maiani E, Bellusci G, Diederich M, Gonfloni S (2013) Parkinson’s disease: a complex interplay of mitochondrial DNA alterations and oxidative stress. Int J Mol Sci 14:2388–2409. https://doi.org/10.3390/ijms14022388
Ciron C, Lengacher S, Dusonchet J, Aebischer P, Schneider BL (2012) Sustained expression of PGC-1α in the rat nigrostriatal system selectively impairs dopaminergic function. Hum Mol Genet 21:1861–1876. https://doi.org/10.1093/HMG/DDR618
Clark J, Reddy S, Zheng K, Betensky RA, Simon DK (2011) Association of PGC-1alpha polymorphisms with age of onset and risk of Parkinson’s disease. BMC Med Genet 12:1–9. https://doi.org/10.1186/1471-2350-12-69/TABLES/2
Cobley JN, Fiorello ML, Bailey DM (2018) 13 reasons why the brain is susceptible to oxidative stress. Redox Biol 15:490–503. https://doi.org/10.1016/j.redox.2018.01.008
Criscuolo D, Avolio R, Matassa DS, Esposito F (2021) Targeting mitochondrial protein expression as a future approach for cancer therapy. Front. Oncol. 11:797265. https://doi.org/10.3389/fonc.2021.797265
Cunha-Oliveira T, Montezinho L, Mendes C, Firuzi O, Saso L, Oliveira PJ, Silva FSG (2020) Oxidative stress in amyotrophic lateral sclerosis: pathophysiology and opportunities for pharmacological intervention. Oxid Med Cell Longev. https://doi.org/10.1155/2020/5021694
Cunha-Santos J, Duarte-Neves J, Carmona V, Guarente L, De Almeida LP, Cavadas C (2016) Caloric restriction blocks neuropathology and motor deficits in Machado-Joseph disease mouse models through SIRT1 pathway. Nat Commun 71(7):1–14. https://doi.org/10.1038/ncomms11445
Cunnane SC, Trushina E, Morland C, Prigione A, Casadesus G, Andrews ZB, Beal MF, Bergersen LH, Brinton RD, de la Monte S, Eckert A, Harvey J, Jeggo R, Jhamandas JH, Kann O, la Cour CM, Martin WF, Mithieux G, Moreira PI, Murphy MP, Nave KA, Nuriel T, Oliet SHR, Saudou F, Mattson MP, Swerdlow RH, Millan MJ (2020) Brain energy rescue: an emerging therapeutic concept for neurodegenerative disorders of ageing. Nat Rev Drug Discov 199(19):609–633. https://doi.org/10.1038/s41573-020-0072-x
Delic V, Kurien C, Cruz J, Zivkovic S, Barretta J, Thomson A, Hennessey D, Joseph J, Ehrhart J, Willing AE, Bradshaw P, Garbuzova-Davis S (2018) Discrete mitochondrial aberrations in the spinal cord of sporadic ALS patients. J Neurosci Res 96:1353–1366. https://doi.org/10.1002/JNR.24249
Dematteis G, Vydmantaitė G, Ruffinatti FA, Chahin M, Farruggio S, Barberis E, Ferrari E, Marengo E, Distasi C, Morkūnienė R, Genazzani AA, Grilli M, Grossini E, Corazzari M, Manfredi M, Lim D, Jekabsone A, Tapella L (2020) Proteomic analysis links alterations of bioenergetics, mitochondria-ER interactions and proteostasis in hippocampal astrocytes from 3xTg-AD mice. Cell Death Dis 118(11):1–16. https://doi.org/10.1038/s41419-020-02911-1
Dominy JE, Puigserver P (2013) Mitochondrial biogenesis through activation of nuclear signaling proteins. Cold Spring Harb Perspect Biol 5:a015008. https://doi.org/10.1101/CSHPERSPECT.A015008
DuBoff B, Götz J, Feany MB (2012) Tau promotes neurodegeneration via DRP1 mislocalization in vivo. Neuron 75:618–632. https://doi.org/10.1016/J.NEURON.2012.06.026
Elfawy HA, Das B (2019) Crosstalk between mitochondrial dysfunction, oxidative stress, and age related neurodegenerative disease: etiologies and therapeutic strategies. Life Sci 218:165–184. https://doi.org/10.1016/J.LFS.2018.12.029
Erustes AG, D’Eletto M, Guarache GC, Ureshino RP, Bincoletto C, da Silva Pereira GJ, Piacentini M, Smaili SS (2021) Overexpression of α-synuclein inhibits mitochondrial Ca2+ trafficking between the endoplasmic reticulum and mitochondria through MAMs by altering the GRP75–IP3R interaction. J Neurosci Res 99:2932–2947. https://doi.org/10.1002/JNR.24952
Federico A, Cardaioli E, Da Pozzo P, Formichi P, Gallus GN, Radi E (2012) Mitochondria, oxidative stress and neurodegeneration. J Neurol Sci 322:254–262. https://doi.org/10.1016/J.JNS.2012.05.030
Feng ST, Wang ZZ, Yuan YH, Sun HM, Chen NH, Zhang Y (2021a) Update on the association between alpha-synuclein and tau with mitochondrial dysfunction: implications for Parkinson’s disease. Eur J Neurosci 53:2946–2959. https://doi.org/10.1111/EJN.14699
Feng ST, Wang ZZ, Yuan YH, Sun HM, Chen NH, Zhang Y (2019) Mangiferin: a multipotent natural product preventing neurodegeneration in Alzheimer’s and Parkinson’s disease models. Pharmacol Res 146:104336. https://doi.org/10.1016/J.PHRS.2019.104336
Feng ST, Wang ZZ, Yuan YH, Wang X. Le, Guo ZY, Hu JH, Yan X, Chen NH, Zhang Y (2021b) Inhibition of dynamin-related protein 1 ameliorates the mitochondrial ultrastructure via PINK1 and Parkin in the mice model of Parkinson’s disease. Eur J Pharmacol 907. https://doi.org/10.1016/J.EJPHAR.2021.174262
Feng ST, Wang ZZ, Yuan YH, Wang X. Le, Sun HM, Chen NH, Zhang Y (2020) Dynamin-related protein 1: a protein critical for mitochondrial fission, mitophagy, and neuronal death in Parkinson’s disease. Pharmacol Res 151:104553. https://doi.org/10.1016/j.phrs.2019.104553
Frank M, Duvezin-Caubet S, Koob S, Occhipinti A, Jagasia R, Petcherski A, Ruonala MO, Priault M, Salin B, Reichert AS (2012) Mitophagy is triggered by mild oxidative stress in a mitochondrial fission dependent manner. Biochim Biophys Acta - Mol Cell Res 1823:2297–2310. https://doi.org/10.1016/J.BBAMCR.2012.08.007
Frederiksen KS, Gjerum L, Waldemar G, Hasselbalch SG (2018) Effects of physical exercise on Alzheimer’s disease biomarkers: a systematic review of intervention studies. J Alzheimer’s Dis 61:359–372. https://doi.org/10.3233/JAD-170567
Fulda S, Debatin KM (2006) Extrinsic versus intrinsic apoptosis pathways in anticancer chemotherapy. Oncogene 25:4798–4811. https://doi.org/10.1038/sj.onc.1209608
Gan X, Huang S, Wu L, Wang Y, Hu G, Li G, Zhang H, Yu H, Swerdlow RH, Chen JX, Yan SS (2014) Inhibition of ERK-DLP1 signaling and mitochondrial division alleviates mitochondrial dysfunction in Alzheimer’s disease cybrid cell. Biochim Biophys Acta - Mol Basis Dis 1842:220–231. https://doi.org/10.1016/J.BBADIS.2013.11.009
Gandhi S, Abramov AY (2012) Mechanism of oxidative stress in neurodegeneration. Oxid Med Cell Longev. https://doi.org/10.1155/2012/428010
Gao J, Wang L, Liu J, Xie F, Su B, Wang X (2017) Abnormalities of Mitochondrial Dynamics in Neurodegenerative Diseases 6:25
Gatt AP, Duncan OF, Attems J, Francis PT, Ballard CG, Bateman JM (2016) Dementia in Parkinson’s disease is associated with enhanced mitochondrial complex I deficiency. Mov Disord 31:352–359. https://doi.org/10.1002/MDS.26513
Ghosh A, Tyson T, George S, Hildebrandt EN, Steiner JA, Madaj Z, Schulz E, Machiela E, McDonald WG, Escobar Galvis ML, Kordower JH, Van Raamsdonk JM, Colca JR, Brundin P (2016) Mitochondrial pyruvate carrier regulates autophagy, inflammation, and neurodegeneration in experimental models of Parkinson’s disease. Sci Transl Med 8. https://doi.org/10.1126/scitranslmed.aag2210
Gilmozzi V, Gentile G, Castelo Rueda MP, Hicks AA, Pramstaller PP, Zanon A, Lévesque M, Pichler I (2020) Interaction of alpha-synuclein with lipids: mitochondrial cardiolipin as a critical player in the pathogenesis of Parkinson’s disease. Front Neurosci 14:578993. https://doi.org/10.3389/fnins.2020.578993
Giorgi C, Agnoletto C, Bononi A, Bonora M, De Marchi E, Marchi S, Missiroli S, Patergnani S, Poletti F, Rimessi A, Suski JM, Wieckowski MR, Pinton P (2012) Mitochondrial calcium homeostasis as potential target for mitochondrial medicine. Mitochondrion 12:77–85. https://doi.org/10.1016/j.mito.2011.07.004
Gomes LC, Scorrano L (2008) High levels of Fis1, a pro-fission mitochondrial protein, trigger autophagy. Biochim Biophys Acta - Bioenerg 1777:860–866. https://doi.org/10.1016/J.BBABIO.2008.05.442
Goyal S, Chaturvedi RK (2020) Mitochondrial protein import dysfunction in pathogenesis of neurodegenerative diseases. Mol Neurobiol 584(58):1418–1437. https://doi.org/10.1007/S12035-020-02200-0
Gueguen N, Desquiret-Dumas V, Leman G, Chupin S, Baron S, Nivet-Antoine V, Vessières E, Ayer A, Henrion D, Lenaers G, Reynier P, Procaccio V (2015) Resveratrol directly binds to mitochondrial complex i and increases oxidative stress in brain mitochondria of aged mice. PLoS One 10:e0144290. https://doi.org/10.1371/JOURNAL.PONE.0144290
Guo L, Tian J, Du H (2017) Mitochondrial dysfunction and synaptic transmission failure in Alzheimer’s disease. J Alzheimers Dis 57:1071–1086. https://doi.org/10.3233/JAD-160702
Guo W, Stoklund Dittlau K, Van Den Bosch L (2020) Axonal transport defects and neurodegeneration: molecular mechanisms and therapeutic implications. Semin Cell Dev Biol 99:133–150. https://doi.org/10.1016/j.semcdb.2019.07.010
Guzy RD, Schumacker PT (2006) Oxygen sensing by mitochondria at complex III: the paradox of increased reactive oxygen species during hypoxia. Exp Physiol. Blackwell Publishing Ltd, pp. 807–819. https://doi.org/10.1113/expphysiol.2006.033506
Hall CN, Klein-Flügge MC, Howarth C, Attwell D (2012) Oxidative phosphorylation, not glycolysis, powers presynaptic and postsynaptic mechanisms underlying brain information processing. J Neurosci. https://doi.org/10.1523/JNEUROSCI.0026-12.2012
Heneka MT, Fink A, Doblhammer G (2015) Effect of pioglitazone medication on the incidence of dementia. Ann Neurol 78:284–294. https://doi.org/10.1002/ANA.24439
Herst PM, Rowe MR, Carson GM, Berridge MV (2017) Functional mitochondria in health and disease. Front Endocrinol
Hirai K, Aliev G, Nunomura A, Fujioka H, Russell RL, Atwood CS, Johnson AB, Kress Y, Vinters HV, Tabaton M, Shimohama S, Cash AD, Siedlak SL, Harris PLR, Jones PK, Petersen RB, Perry G, Smith MA (2001) Mitochondrial abnormalities in Alzheimer’s disease. J Neurosci 21:3017–3023. https://doi.org/10.1523/JNEUROSCI.21-09-03017.2001
Ho DJ, Calingasan NY, Wille E, Dumont M, Beal MF (2010) Resveratrol protects against peripheral deficits in a mouse model of Huntington’s disease. Exp Neurol 225:74–84. https://doi.org/10.1016/J.EXPNEUROL.2010.05.006
Huang L-K, Chao S-P, Hu C-J (2020) Clinical trials of new drugs for Alzheimer disease. J Biomed Sci 27:18. https://doi.org/10.1186/s12929-019-0609-7
Hudry E, Vandenberghe LH (2019) Therapeutic AAV gene transfer to the nervous system: a clinical reality. Neuron 101:839–862. https://doi.org/10.1016/J.NEURON.2019.02.017
Investigators NET (2015) Pioglitazone in early Parkinson’s disease: a phase 2, multicentre, double-blind, randomised trial. Lancet Neurol 14:795–803. https://doi.org/10.1016/S1474-4422(15)00144-1
Jaber SM, Ge SX, Milstein JL, VanRyzin JW, Waddell J, Polster BM (2020) Idebenone has distinct effects on mitochondrial respiration in cortical astrocytes compared to cortical neurons due to differential NQO1 activity. J Neurosci 40:4609–4619. https://doi.org/10.1523/JNEUROSCI.1632-17.2020
Jamwal S, Blackburn JK, Elsworth JD (2021) PPARγ/PGC1α signaling as a potential therapeutic target for mitochondrial biogenesis in neurodegenerative disorders. Pharmacol Ther 219:107705. https://doi.org/10.1016/j.pharmthera.2020.107705
Jimenez-Sanchez M, Licitra F, Underwood BR, Rubinsztein DC (2017) Huntington’s disease: mechanisms of pathogenesis and therapeutic strategies. Cold Spring Harb Perspect Med 7:a024240. https://doi.org/10.1101/cshperspect.a024240
Jones AWE, Yao Z, Vicencio JM, Karkucinska-Wieckowska A, Szabadkai G (2012) PGC-1 family coactivators and cell fate: roles in cancer, neurodegeneration, cardiovascular disease and retrograde mitochondria–nucleus signalling. Mitochondrion 12:86–99. https://doi.org/10.1016/J.MITO.2011.09.009
Kale MB, Bajaj K, Umare M, Wankhede NL, Taksande BG, Umekar MJ, Upaganlawar A (2021) Exercise and nutraceuticals: eminent approach for diabetic neuropathy. Curr Mol Pharmacol 14. https://doi.org/10.2174/1874467214666210629123010
Kandimalla R, Manczak M, Fry D, Suneetha Y, Sesaki H, Reddy PH (2016) Reduced dynamin-related protein 1 protects against phosphorylated Tau-induced mitochondrial dysfunction and synaptic damage in Alzheimer’s disease. Hum Mol Genet 25:4881–4897. https://doi.org/10.1093/hmg/ddw312
Kandimalla R, Reddy PH (2016) Multiple faces of dynamin-related protein 1 and its role in Alzheimer’s disease pathogenesis. Biochim Biophys Acta - Mol Basis Dis 1862:814–828. https://doi.org/10.1016/J.BBADIS.2015.12.018
Kawamata H, Manfredi G (2018) Correction: proteinopathies and OXPHOS dysfunction in neurodegenerative diseases. J Cell Biol 217:429. https://doi.org/10.1083/JCB.20170917212192017C
Khan A, Ali T, Rehman SU, Khan MS, Alam SI, Ikram M, Muhammad T, Saeed K, Badshah H, Kim MO (2018) Neuroprotective effect of quercetin against the detrimental effects of LPS in the adult mouse brain. Front Pharmacol 9:1383. https://doi.org/10.3389/fphar.2018.01383
Khraiwesh H, López-Domínguez JA, Fernández del Río L, Gutierrez-Casado E, López-Lluch G, Navas P, de Cabo R, Ramsey JJ, Burón MI, Villalba JM, González-Reyes JA (2014) Mitochondrial ultrastructure and markers of dynamics in hepatocytes from aged, calorie restricted mice fed with different dietary fats. Exp Gerontol 56:77–88. https://doi.org/10.1016/J.EXGER.2014.03.023
Kim D, Nguyen MD, Dobbin MM, Fischer A, Sananbenesi F, Rodgers JT, Delalle I, Baur JA, Sui G, Armour SM, Puigserver P, Sinclair DA, Tsai LH (2007) SIRT1 deacetylase protects against neurodegeneration in models for Alzheimer’s disease and amyotrophic lateral sclerosis. EMBO J 26:3169–3179. https://doi.org/10.1038/SJ.EMBOJ.7601758
Kim J, Moody JP, Edgerly CK, Bordiuk OL, Cormier K, Smith K, Flint Beal M, Ferrante RJ (2010) Mitochondrial loss, dysfunction and altered dynamics in Huntington’s disease. Hum Mol Genet 19:3919–3935. https://doi.org/10.1093/HMG/DDQ306
Krishnan KJ, Ratnaike TE, De Gruyter HLM, Jaros E, Turnbull DM (2012) Mitochondrial DNA deletions cause the biochemical defect observed in Alzheimer’s disease. Neurobiol Aging 33:2210–2214. https://doi.org/10.1016/j.neurobiolaging.2011.08.009
Lautrup S, Sinclair DA, Mattson MP, Fang EF (2019) NAD(+) in brain aging and neurodegenerative disorders. Cell Metab 30:630–655. https://doi.org/10.1016/j.cmet.2019.09.001
Lee JS, Yoon YG, Yoo SH, Jeong NY, Jeong SH, Lee SY, Jung DI, Jeong SY, Yoo YH (2012) Histone deacetylase inhibitors induce mitochondrial elongation. J Cell Physiol 227:2856–2869. https://doi.org/10.1002/JCP.23027
Li J, Hart RP, Mallimo EM, Swerdel MR, Kusnecov AW, Herrup K (2013) EZH2-mediated H3K27 trimethylation mediates neurodegeneration in ataxia-telangiectasia. Nat Neurosci 1612(16):1745–1753. https://doi.org/10.1038/nn.3564
Li T, Chen L, Yu Y, Yang B, Li P, Tan X-Q (2019) Resveratrol alleviates hypoxia/reoxygenation injury-induced mitochondrial oxidative stress in cardiomyocytes. Mol Med Rep 19:2774–2780. https://doi.org/10.3892/mmr.2019.9943
Li Z, Okamoto K-I, Hayashi Y, Sheng M (2004) The importance of dendritic mitochondria in the morphogenesis and plasticity of spines and synapses. Cell 119:873–887. https://doi.org/10.1016/j.cell.2004.11.003
Lin J, Wu PH, Tarr PT, Lindenberg KS, St-Pierre J, Zhang CY, Mootha VK, Jäger S, Vianna CR, Reznick RM, Cui L, Manieri M, Donovan MX, Wu Z, Cooper MP, Fan MC, Rohas LM, Zavacki AM, Cinti S, Shulman GI, Lowell BB, Krainc D, Spiegelman BM (2004) Defects in adaptive energy metabolism with CNS-linked hyperactivity in PGC-1α null mice. Cell 119:121–135. https://doi.org/10.1016/J.CELL.2004.09.013
Lin MT, Beal MF (2006) Mitochondrial dysfunction and oxidative stress in neurodegenerative diseases. Nature 443:787–795. https://doi.org/10.1038/nature05292
Lin MY, Cheng XT, Xie Y, Cai Q, Sheng ZH (2017) Removing dysfunctional mitochondria from axons independent of mitophagy under pathophysiological conditions. Autophagy 13:1792–1794. https://doi.org/10.1080/15548627.2017.1356552
Linnane AW, Zhang C, Baumer A, Nagley P (1992) Mitochondrial DNA mutation and the ageing process: bioenergy and pharmacological intervention. Mutat Res Dnaging 275:195–208. https://doi.org/10.1016/0921-8734(92)90023-I
Liu H, You L, Wu J, Zhao M, Guo R, Zhang H, Su R, Mao Q, Deng D, Hao Y (2020) Berberine suppresses influenza virus-triggered NLRP3 inflammasome activation in macrophages by inducing mitophagy and decreasing mitochondrial ROS. J Leukoc Biol 108:253–266. https://doi.org/10.1002/jlb.3ma0320-358rr
Loncke J, Kaasik A, Bezprozvanny I, Parys JB, Kerkhofs M, Bultynck G (2021) Balancing ER-mitochondrial Ca2+ fluxes in health and disease. Trends Cell Biol 31:598–612. https://doi.org/10.1016/J.TCB.2021.02.003
Lyman M, Lloyd DG, Ji X, Vizcaychipi MP, Ma D (2014) Neuroinflammation: the role and consequences. Neurosci Res. https://doi.org/10.1016/j.neures.2013.10.004
Ma K, Chen G, Li W, Kepp O, Zhu Y, Chen Q (2020) Mitophagy, mitochondrial homeostasis, and cell fate. Front Cell Dev Biol 8:467. https://doi.org/10.3389/fcell.2020.00467
Mallet D, Goutaudier R, Barbier EL, Carnicella S, Colca JR, Fauvelle F, Boulet S (2022) Re-routing metabolism by the mitochondrial pyruvate carrier inhibitor MSDC-0160 attenuates neurodegeneration in a rat model of Parkinson’s disease. Mol Neurobiol. https://doi.org/10.1101/2022.01.17.476616
Manczak M, Kandimalla R, Fry D, Sesaki H, Reddy PH (2016) Protective effects of reduced dynamin-related protein 1 against amyloid beta-induced mitochondrial dysfunction and synaptic damage in Alzheimer’s disease. Hum Mol Genet 25:5148–5166. https://doi.org/10.1093/hmg/ddw330
Manczak M, Kandimalla R, Yin X, Hemachandra Reddy P (2019) Mitochondrial division inhibitor 1 reduces dynamin-related protein 1 and mitochondrial fission activity. Hum Mol Genet 28:177–199. https://doi.org/10.1093/HMG/DDY335
Manczak M, Reddy PH (2012) Abnormal interaction between the mitochondrial fission protein Drp1 and hyperphosphorylated tau in Alzheimer’s disease neurons: implications for mitochondrial dysfunction and neuronal damage. Hum Mol Genet 21:2538–2547. https://doi.org/10.1093/HMG/DDS072
Manor U, Bartholomew S, Golani G, Christenson E, Kozlov M, Higgs H, Spudich J, Lippincott-Schwartz J (2015) A mitochondria-anchored isoform of the actin-nucleating spire protein regulates mitochondrial division. Elife 4:1–27. https://doi.org/10.7554/eLife.08828
Marde VS, Atkare UA, Gawali SV, Tiwari PL, Badole SP, Wankhede NL, Taksande BG, Upaganlawar AB, Umekar MJ, Kale MB (2022) Alzheimer’s disease and sleep disorders: insights into the possible disease connections and the potential therapeutic targets. Asian J Psychiatr 68. https://doi.org/10.1016/j.ajp.2021.102961
Marde VS, Tiwari PL, Wankhede NL, Taksande BG, Upaganlawar AB, Umekar MJ, Kale MB (2021) Neurodegenerative Disorders Associated with Genes of Mitochondria 7:1–8. https://doi.org/10.1186/S43094-021-00215-5
Marks WJ, Bartus RT, Siffert J, Davis CS, Lozano A, Boulis N, Vitek J, Stacy M, Turner D, Verhagen L, Bakay R, Watts R, Guthrie B, Jankovic J, Simpson R, Tagliati M, Alterman R, Stern M, Baltuch G, Starr PA, Larson PS, Ostrem JL, Nutt J, Kieburtz K, Kordower JH, Olanow CW (2010) Gene delivery of AAV2-neurturin for Parkinson’s disease: a double-blind, randomised, controlled trial. Lancet Neurol 9:1164–1172. https://doi.org/10.1016/S1474-4422(10)70254-4
Masciopinto F, Di Pietro N, Corona C, Bomba M, Pipino C, Curcio M, Di Castelnuovo A, Ciavardelli D, Silvestri E, Canzoniero LMT, Sekler I, Pandolfi A, Sensi SL (2012) Effects of long-term treatment with pioglitazone on cognition and glucose metabolism of PS1-KI, 3xTg-AD, and wild-type mice. Cell Death Dis 3:e448–e448. https://doi.org/10.1038/cddis.2012.189
Melo TQ, Copray SJCVM, Ferrari MFR (2018) Alpha-synuclein toxicity on protein quality control, mitochondria and endoplasmic reticulum. Neurochem Res 4312(43):2212–2223. https://doi.org/10.1007/S11064-018-2673-X
Mergenthaler P, Lindauer U, Dienel GA, Meisel A (2013) Sugar for the brain: the role of glucose in physiological and pathological brain function. Trends Neurosci 36:587–597. https://doi.org/10.1016/j.tins.2013.07.001
Mishra P, Chan DC (2014) Mitochondrial dynamics and inheritance during cell division, development and disease. Nat Rev Mol Cell Biol 1510(15):634–646. https://doi.org/10.1038/nrm3877
Missiroli S, Genovese I, Perrone M, Vezzani B, Vitto VAM, Giorgi C (2020) The role of mitochondria in inflammation: from cancer to neurodegenerative disorders. J Clin Med 9:740. https://doi.org/10.3390/jcm9030740
Mitochondrial Ca Y, Moccia F, Zhang D, Wang F, Li P, Gao Y (2022) Mitochondrial Ca2+ homeostasis: emerging roles and clinical significance in cardiac remodeling. Int J. Mol Sci 23:3025. https://doi.org/10.3390/IJMS23063025
Morató L, Ruiz M, Boada J, Calingasan NY, Galino J, Guilera C, Jové M, Naudí A, Ferrer I, Pamplona R, Serrano M, Portero-Otín M, Beal MF, Fourcade S, Pujol A (2015) Activation of sirtuin 1 as therapy for the peroxisomal disease adrenoleukodystrophy. Cell Death Differ 22:1742–1753. https://doi.org/10.1038/cdd.2015.20
Moreira PI, Zhu X, Wang X, Lee H-G, Nunomura A, Petersen RB, Perry G, Smith MA (2010) Mitochondria: a therapeutic target in neurodegeneration. Biochim Biophys Acta 1802:212–220. https://doi.org/10.1016/j.bbadis.2009.10.007
Niu S, Zhang LK, Zhang L, Zhuang S, Zhan X, Chen WY, Du S, Yin L, You R, Li CH, Guan YQ (2017) Inhibition by multifunctional magnetic nanoparticles loaded with alpha-synuclein RNAi plasmid in a Parkinson’s disease model. Theranostics 7:344. https://doi.org/10.7150/THNO.16562
Nunnari J, Suomalainen A (2012) Mitochondria: in sickness and in health. Cell. https://doi.org/10.1016/j.cell.2012.02.035
Oliveira JMA (2010) Nature and cause of mitochondrial dysfunction in Huntington’s disease: focusing on huntingtin and the striatum. J Neurochem 114:1–12. https://doi.org/10.1111/J.1471-4159.2010.06741.X
Onyango IG, Lu J, Rodova M, Lezi E, Crafter AB, Swerdlow RH (2010) Regulation of neuron mitochondrial biogenesis and relevance to brain health. Biochim Biophys Acta - Mol Basis Dis. https://doi.org/10.1016/j.bbadis.2009.07.014
Orsucci D, Mancuso M, Ienco EC, LoGerfo A, Siciliano G (2011) Targeting mitochondrial dysfunction and neurodegeneration by means of coenzyme Q10 and its analogues. Curr Med Chem 18:4053–4064. https://doi.org/10.2174/092986711796957257
Palikaras K, Tavernarakis N (2012) Mitophagy in neurodegeneration and aging. Front Genet. https://doi.org/10.3389/fgene.2012.00297
Panchal K, Tiwari AK (2019) Mitochondrial dynamics, a key executioner in neurodegenerative diseases. Mitochondrion 47:151–173. https://doi.org/10.1016/J.MITO.2018.11.002
Paudel YN, Angelopoulou E, Piperi C, Shaikh MF, Othman I (2020) Emerging neuroprotective effect of metformin in Parkinson’s disease: a molecular crosstalk. Pharmacol Res. https://doi.org/10.1016/j.phrs.2019.104593
Peng K, Yang L, Wang J, Ye F, Dan G, Zhao Y, Cai Y, Cui Z, Ao L, Liu J, Zou Z, Sai Y, Cao J (2016) The interaction of mitochondrial biogenesis and fission/fusion mediated by PGC-1α regulates rotenone-induced dopaminergic neurotoxicity. Mol Neurobiol 545(54):3783–3797. https://doi.org/10.1007/S12035-016-9944-9
Petri S, Kiaei M, Damiano M, Hiller A, Wille E, Manfredi G, Calingasan NY, Szeto HH, Beal MF (2006) Cell-permeable peptide antioxidants as a novel therapeutic approach in a mouse model of amyotrophic lateral sclerosis. J Neurochem 98:1141–1148. https://doi.org/10.1111/J.1471-4159.2006.04018.X
Picca A, Calvani R, Coelho-Junior HJ, Marzetti E (2021) Cell death and inflammation: the role of mitochondria in health and disease. Cells 10:537. https://doi.org/10.3390/cells10030537
Quansah E, Peelaerts W, Langston JW, Simon DK, Colca J, Brundin P (2018) Targeting energy metabolism via the mitochondrial pyruvate carrier as a novel approach to attenuate neurodegeneration. Mol Neurodegener 13:28. https://doi.org/10.1186/s13024-018-0260-x
Quintanilla RA, Jin YN, Fuenzalida K, Bronfman M, Johnson GVW (2008) Rosiglitazone treatment prevents mitochondrial dysfunction in mutant huntingtin-expressing cells. J Biol Chem 283:25628–25637. https://doi.org/10.1074/jbc.m804291200
Rafii MS, Tuszynski MH, Thomas RG, Barba D, Brewer JB, Rissman RA, Siffert J, Aisen PS, Mintzer J, Lerner A, Levey A, Burke J, Sano M, Turner S, Zamrini E, Grill J, Marson D (2018) Adeno-associated viral vector (Serotype 2)–nerve growth factor for patients with Alzheimer disease: a randomized clinical trial. JAMA Neurol 75:834–841. https://doi.org/10.1001/JAMANEUROL.2018.0233
Reddy PH (2009) Role of mitochondria in neurodegenerative diseases: mitochondria as a therapeutic target in Alzheimer’s disease. CNS Spectr 14:8–13. https://doi.org/10.1017/S1092852900024901
Rey F, Ottolenghi S, Giallongo T, Balsari A, Martinelli C, Rey R, Allevi R, Giulio AMD, Zuccotti GV, Mazzucchelli S, Foresti R, Samaja M, Carelli S (2021) Mitochondrial Metabolism as target of the neuroprotective role of erythropoietin in Parkinson’s disease. Antioxidants (Basel, Switzerland) 10:121. https://doi.org/10.3390/antiox10010121
Risiglione P, Zinghirino F, Di Rosa MC, Magrì A, Messina A (2021) Alpha-synuclein and mitochondrial dysfunction in parkinson’s disease: the emerging role of vdac. Biomolecules 11. https://doi.org/10.3390/biom11050718
Risner ME, Saunders AM, Altman JFB, Ormandy GC, Craft S, Foley IM, Zvartau-Hind ME, Hosford DA, Roses AD (2006) Efficacy of rosiglitazone in a genetically defined population with mild-to-moderate Alzheimer’s disease. Pharmacogenomics J 64(6):246–254. https://doi.org/10.1038/sj.tpj.6500369
Rodolfo C, Campello S, Cecconi F (2018) Mitophagy in neurodegenerative diseases. Neurochem Int 117:156–166. https://doi.org/10.1016/j.neuint.2017.08.004
Rotermund C, Machetanz G, Fitzgerald JC (2018) The therapeutic potential of metformin in neurodegenerative diseases. Front Endocrinol (Lausanne) 9:400. https://doi.org/10.3389/FENDO.2018.00400/XML/NLM
Rui YN, Xu Z, Patel B, Cuervo AM, Zhang S (2015) HTT/Huntingtin in selective autophagy and Huntington disease: a foe or a friend within? Trends Neurosci 11:858–860. https://doi.org/10.1080/15548627.2015.1039219
Salomone S, Caraci F, Leggio GM, Fedotova J, Drago F (2012) New pharmacological strategies for treatment of Alzheimer’s disease: focus on disease modifying drugs. Br J Clin Pharmacol 73:504–517. https://doi.org/10.1111/j.1365-2125.2011.04134.x
Sandhir R, Mehrotra A (2013) Quercetin supplementation is effective in improving mitochondrial dysfunctions induced by 3-nitropropionic acid: implications in Huntington’s disease. Biochim Biophys Acta - Mol Basis Dis 1832:421–430. https://doi.org/10.1016/j.bbadis.2012.11.018
Scarpulla RC (2011) Metabolic control of mitochondrial biogenesis through the PGC-1 family regulatory network. Biochim Biophys Acta 1813:1269–1278. https://doi.org/10.1016/j.bbamcr.2010.09.019
Schmidt MY, Chamoli M, Lithgow GJ, Andersen JK (2021) Swimming exercise reduces native ⍺-synuclein protein species in a transgenic C. elegans model of Parkinson’s disease. microPublication Biol. https://doi.org/10.17912/MICROPUB.BIOLOGY.000413
Scholpa NE, Lynn MK, Corum D, Boger HA, Schnellmann RG (2018) 5-HT1F receptor-mediated mitochondrial biogenesis for the treatment of Parkinson’s disease. Br J Pharmacol 175:348–358. https://doi.org/10.1111/BPH.14076
Scott I, Youle RJ (2010) Mitochondrial fission and fusion. Essays Biochem 47:85–98. https://doi.org/10.1042/BSE0470085/78199
Shaw RJ, Lamia KA, Vasquez D, Koo SH, Bardeesy N, DePinho RA, Montminy M, Cantley LC (2005) Medicine: the kinase LKB1 mediates glucose homeostasis in liver and therapeutic effects of metformin. Science (80-. ) 310:1642–1646. https://doi.org/10.1126/science.1120781
Sheng B, Wang X, Su B, Lee HG, Casadesus G, Perry G, Zhu X (2012) Impaired mitochondrial biogenesis contributes to mitochondrial dysfunction in Alzheimer’s disease. J Neurochem 120:419–429. https://doi.org/10.1111/J.1471-4159.2011.07581.X
Sheng Z-H, Cai Q (2012) Mitochondrial transport in neurons: impact on synaptic homeostasis and neurodegeneration. Nat Rev Neurosci 13:77–93. https://doi.org/10.1038/nrn3156
Shin JH, Ko HS, Kang H, Lee Y, Lee YI, Pletinkova O, Troconso JC, Dawson VL, Dawson TM (2011) PARIS (ZNF746) Repression of PGC-1α contributes to neurodegeneration in Parkinson’s disease. Cell 144:689–702. https://doi.org/10.1016/J.CELL.2011.02.010
Simmons EC, Scholpa NE, Schnellmann RG (2020) Mitochondrial biogenesis as a therapeutic target for traumatic and neurodegenerative CNS diseases. Exp. Neurol. 329:113309. https://doi.org/10.1016/J.EXPNEUROL.2020.113309
Simon DK, Lin MT, Zheng L, Liu G-J, Ahn CH, Kim LM, Mauck WM, Twu F, Beal MF, Johns DR (2004) Somatic mitochondrial DNA mutations in cortex and substantia nigra in aging and Parkinson’s disease. Neurobiol Aging 25:71–81. https://doi.org/10.1016/S0197-4580(03)00037-X
Singh A, Faccenda D, Campanella M (2021) Pharmacological advances in mitochondrial therapy. EBioMedicine 65:103244. https://doi.org/10.1016/j.ebiom.2021.103244
Sleigh JN, Rossor AM, Fellows AD, Tosolini AP, Schiavo G (2019) Axonal transport and neurological disease. Nat Rev Neurol 1512(15):691–703. https://doi.org/10.1038/s41582-019-0257-2
Smith MA, Harris PLR, Sayre LM, Perry G (1997) Iron accumulation in Alzheimer disease is a source of redox-generated free radicals. Proc Natl Acad Sci USA 94:9866–9868. https://doi.org/10.1073/pnas.94.18.9866
Suen DF, Norris KL, Youle RJ (2008) Mitochondrial dynamics and apoptosis. Genes Dev. https://doi.org/10.1101/gad.1658508
Suliman HB, Piantadosi CA (2015) Mitochondrial quality control as a therapeutic target. Pharmacol Rev 68:20–48. https://doi.org/10.1124/pr.115.011502
Szeto HH (2008) Development of mitochondria-targeted aromatic-cationic peptides for neurodegenerative diseases. Ann N Y Acad Sci 1147:112–121. https://doi.org/10.1196/ANNALS.1427.013
Szeto HH (2006) Cell-permeable, mitochondrial-targeted, peptide antioxidants. AAPS J 82(8):E277–E283. https://doi.org/10.1007/BF02854898
Takeuchi H, Kobayashi Y, Ishigaki S, Doyu M, Sobue G (2016) Mitochondrial localization of mutant superoxide dismutase 1 triggers caspase-dependent cell death in a cellular model of familial amyotrophic lateral sclerosis. J Biol Chem 291:22341. https://doi.org/10.1074/JBC.A116.209356
Taylor RW, Turnbull DM (2005) Mitochondrial DNA mutations in human disease. Nat Rev Genet 6:389–402. https://doi.org/10.1038/nrg1606
Tefera TW, Bartlett K, Tran SS, Hodson MP, Borges K (2019) Impaired pentose phosphate pathway in the spinal cord of the hSOD1G93A mouse model of amyotrophic lateral sclerosis. Mol Neurobiol 568(56):5844–5855. https://doi.org/10.1007/S12035-019-1485-6
Tiwari P, Wankhede N, Badole S, Umare M, Taksande B, Upaganlawar A, Umekar M, Kale M, Umekar M, Upaganlawar A, Umekar M, Kale M (2021) Mitochondrial dysfunction in ageing: involvement of oxidative stress and role of melatonin. researchgate. Net 10:156–172
Tong J, Rathitharan G, Meyer JH, Furukawa Y, Ang L-C, Boileau I, Guttman M, Hornykiewicz O, Kish SJ (2017) Brain monoamine oxidase B and A in human parkinsonian dopamine deficiency disorders. Brain 140:2460–2474. https://doi.org/10.1093/brain/awx172
Trivedi R (2021) Neuropsychiatric disorders: a pharmacovigilance perspective
Trushina E, Trushin S, Hasan MF (2022) Mitochondrial complex I as a therapeutic target for Alzheimer’s disease. Acta Pharm Sin B 12:483–495. https://doi.org/10.1016/J.APSB.2021.11.003
Tsujimoto Y (1998) Role of Bcl-2 family proteins in apoptosis: apoptosomes or mitochondria? Genes Cells 3:697–707. https://doi.org/10.1046/j.1365-2443.1998.00223.x
Tufekci KU, Civi Bayin E, Genc S, Genc K (2011) The Nrf2/ARE pathway: a promising target to counteract mitochondrial dysfunction in Parkinson’s disease. Parkinsons Dis. https://doi.org/10.4061/2011/314082
Twig G, Hyde B, Shirihai OS (2008) Mitochondrial fusion, fission and autophagy as a quality control axis: the bioenergetic view. Biochim Biophys Acta - Bioenerg 1777:1092–1097. https://doi.org/10.1016/J.BBABIO.2008.05.001
Uddin MS, Al Mamun A, Kabir MT, Ahmad J, Jeandet P, Sarwar MS, Ashraf GM, Aleya L (2020) Neuroprotective role of polyphenols against oxidative stress-mediated neurodegeneration. Eur J Pharmacol 886:173412. https://doi.org/10.1016/J.EJPHAR.2020.173412
Umare MD, Wankhede NL, Bajaj KK, Trivedi RV, Taksande BG, Umekar MJ, Mahore JG, Kale MB (2022) Interweaving of reactive oxygen species and major neurological and psychiatric disorders. Ann Pharm Françaises 80:409–425
Umare MD, Wankhede NL, Bajaj KK, Trivedi RV, Taksande BG, Umekar MJ, Mahore JG, Kale MB (2021) Interweaving of reactive oxygen species and major neurological and psychiatric disorders. Ann Pharm Françaises. https://doi.org/10.1016/j.pharma.2021.11.004
Upaganlawar A, Upasani C, Kale MB (2022) Medicinal potential of fenugreek in neuropathy and neuroinflammation associated disorders. Fenugreek 211–229. https://doi.org/10.1201/9781003082767-19
Upaganlawar AB, Wankhede NL, Kale MB, Umare MD, Sehgal A, Singh S, Bhatia S, Al-Harrasi A, Najda A, Nurzyńska-Wierdak R, Bungau S, Behl T (2021) Interweaving epilepsy and neurodegeneration: Vitamin E as a treatment approach. Biomed Pharmacother 143:112146
Valdés P, Mercado G, Vidal RL, Molina C, Parsons G, Court FA, Martinez A, Galleguillos D, Armentano D, Schneider BL, Hetz C (2014) Control of dopaminergic neuron survival by the unfolded protein response transcription factor XBP1. Proc Natl Acad Sci USA 111:6804–6809. https://doi.org/10.1073/PNAS.1321845111/SUPPL_FILE/PNAS.201321845SI.PDF
Valko M, Leibfritz D, Moncol J, Cronin MTD, Mazur M, Telser J (2007) Free radicals and antioxidants in normal physiological functions and human disease. Int J Biochem Cell Biol. https://doi.org/10.1016/j.biocel.2006.07.001
Vingtdeux V, Giliberto L, Zhao H, Chandakkar P, Wu Q, Simon JE, Janle EM, Lobo J, Ferruzzi MG, Davies P, Marambaud P (2010) AMP-activated protein kinase signaling activation by resveratrol modulates amyloid-beta peptide metabolism. J Biol Chem 285:9100–9113. https://doi.org/10.1074/JBC.M109.060061
Vringer E, Tait SWG (2019) Mitochondria and inflammation: Cell death heats up. Front Cell Dev Biol
Walker FO (2007) Huntington’s disease. Lancet 369:218–228. https://doi.org/10.1016/S0140-6736(07)60111-1
Walker OS, Ragos R, Wong MK, Adam M, Cheung A, Raha S (2020) Reactive oxygen species from mitochondria impacts trophoblast fusion and the production of endocrine hormones by syncytiotrophoblasts. PLoS One 15:e0229332. https://doi.org/10.1371/journal.pone.0229332
Wang C, Youle RJ (2009) The role of mitochondria in apoptosis*. Annu Rev Genet 43:95–118. https://doi.org/10.1146/annurev-genet-102108-134850
Wang XL, Feng ST, Wang YT, Yuan YH, Li ZP, Chen NH, Wang ZZ, Zhang Y (2022a) Mitophagy, a form of selective autophagy, plays an essential role in mitochondrial dynamics of Parkinson’s disease. Cell Mol Neurobiol 42:1321–1339. https://doi.org/10.1007/s10571-021-01039-w
Wang X. Le, Feng ST, Wang YT, Zhang NN, Guo ZY, Yan X, Yuan YH, Wang ZZ, Chen NH, Zhang Y (2022b) Mangiferin, a natural glucoxilxanthone, inhibits mitochondrial dynamin-related protein 1 and relieves aberrant mitophagic proteins in mice model of Parkinson’s disease. Phytomedicine 104:154281. https://doi.org/10.1016/J.PHYMED.2022.154281
Wang XL,Feng ST, Wang ZZ, Chen NH, Zhang Y (2021a) Role of mitophagy in mitochondrial quality control: Mechanisms and potential implications for neurodegenerative diseases. Pharmacol Res 165. https://doi.org/10.1016/J.PHRS.2021.105433
Wang XL, Feng ST, Wang ZZ, Yuan YH, Chen NH, Zhang Y (2021b) Parkin, an E3 ubiquitin ligase, plays an essential role in mitochondrial quality control in Parkinson’s disease. Cell Mol Neurobiol 41:1395–1411. https://doi.org/10.1007/S10571-020-00914-2
Wang W, Zhao F, Ma X, Perry G, Zhu X (2020) Mitochondria dysfunction in the pathogenesis of Alzheimer’s disease: recent advances. Mol Neurodegener 151(15):1–22. https://doi.org/10.1186/S13024-020-00376-6
Wang X, Su B, Siedlak SL, Moreira PI, Fujioka H, Wang Y, Casadesus G, Zhu X (2008) Amyloid-β overproduction causes abnormal mitochondrial dynamics via differential modulation of mitochondrial fission/fusion proteins. Proc Natl Acad Sci USA 105:19318–19323. https://doi.org/10.1073/PNAS.0804871105/SUPPL_FILE/0804871105SI.PDF
Wang Y, Xu E, Musich PR, Lin F (2019) Mitochondrial dysfunction in neurodegenerative diseases and the potential countermeasure. CNS Neurosci Ther 25:816–824. https://doi.org/10.1111/cns.13116
Wankhede NL, Kale MB, Upaganlawar AB, Taksande BG, Umekar MJ, Behl T, Abdellatif AAH, Bhaskaran PM, Dachani SR, Sehgal A, Singh S, Sharma N, Makeen HA, Albratty M, Dailah HG, Bhatia S, Al-Harrasi A, Bungau S (2022) Involvement of molecular chaperone in protein-misfolding brain diseases. Biomed Pharmacoth 147:112647
Warda M, Kim HK, Kim N, Ko KS, Rhee BD, Han J (2013) A matter of life, death and diseases: mitochondria from a proteomic perspective. Expert Rev Proteomics. https://doi.org/10.1586/epr.12.69
Watson GS, Cholerton BA, Reger MA, Baker LD, Plymate SR, Asthana S, Fishel MA, Kulstad JJ, Green PS, Cook DG, Kahn SE, Keeling ML, Craft S (2005) Preserved cognition in patients with early Alzheimer disease and amnestic Mild cognitive impairment during treatment with rosiglitazone: a preliminary study. Am J Geriatr Psychiatry 13:950–958. https://doi.org/10.1097/00019442-200511000-00005
Wei H, Liu L, Chen Q (2015) Selective removal of mitochondria via mitophagy: distinct pathways for different mitochondrial stresses. Biochim Biophys Acta - Mol Cell Res. https://doi.org/10.1016/j.bbamcr.2015.03.013
Westermann B (2012) Bioenergetic role of mitochondrial fusion and fission. Biochim Biophys Acta - Bioenerg 1817:1833–1838. https://doi.org/10.1016/J.BBABIO.2012.02.033
Weydt P, Soyal SM, Gellera C, Didonato S, Weidinger C, Oberkofler H, Landwehrmeyer GB, Patsch W (2009) The gene coding for PGC-1α modifies age at onset in Huntington’s Disease. Mol Neurodegener 4:1–6. https://doi.org/10.1186/1750-1326-4-3/TABLES/4
Whitaker RM, Corum D, Beeson CC, Schnellmann RG (2016) Mitochondrial biogenesis as a pharmacological target: a new approach to acute and chronic diseases. Ann Rev Pharmacol Toxicol 56:229–249. https://doi.org/10.1146/annurev-pharmtox-010715-103155
Wu Y, Chen M, Jiang J (2019) Mitochondrial dysfunction in neurodegenerative diseases and drug targets via apoptotic signaling. Mitochondrion 49:35–45. https://doi.org/10.1016/j.mito.2019.07.003
Xia P, An HX, Dang CX, Radpour R, Kohler C, Fokas E, Engenhart-Cabillic R, Holzgreve W, Zhong XY (2009) Decreased mitochondrial DNA content in blood samples of patients with stage I breast cancer. BMC Cancer. https://doi.org/10.1186/1471-2407-9-454
Xiong N, Long X, Xiong J, Jia M, Chen C, Huang J, Ghoorah D, Kong X, Lin Z, Wang T (2012) Mitochondrial complex I inhibitor rotenone-induced toxicity and its potential mechanisms in Parkinson’s disease models. Crit Rev Toxicol 2:613–632. https://doi.org/10.3109/10408444.2012.680431
Yan X, Wang B, Hu Y, Wang S, Zhang X (2020) Abnormal mitochondrial quality control in neurodegenerative diseases. Front Cell Neurosci 14:138. https://doi.org/10.3389/FNCEL.2020.00138/XML/NLM
Yang D, Ying J, Wang X, Zhao T, Yoon S, Fang Y, Zheng Q, Liu X, Yu W, Hua F (2021) Mitochondrial dynamics: a key role in neurodegeneration and a potential target for neurodegenerative disease. Front Neurosci 15:359. https://doi.org/10.3389/FNINS.2021.654785/XML/NLM
Yang S, Xia C, Li S, Du L, Zhang L, Hu Y (2014) Mitochondrial dysfunction driven by the LRRK2-mediated pathway is associated with loss of Purkinje cells and motor coordination deficits in diabetic rat model. Cell Death Dis 55(5):e1217–e1217. https://doi.org/10.1038/cddis.2014.184
Yap LP, Garcia JV, Han D, Cadenas E (2009) The energy–redox axis in aging and age-related neurodegeneration. Adv Drug Deliv Rev 61:1283–1298. https://doi.org/10.1016/J.ADDR.2009.07.015
Youle RJ, van der Bliek AM (2012a) Mitochondrial fission, fusion, and stress. Science 337:1062–1065. https://doi.org/10.1126/science.1219855
Youle RJ, Van Der Bliek AM (2012b) Mitochondrial fission, fusion, and stress. Science (80-. ) 337:1062–1065. https://doi.org/10.1126/SCIENCE.1219855
Zambon F, Cherubini M, Fernandes HJR, Lang C, Ryan BJ, Volpato V, Bengoa-Vergniory N, Vingill S, Attar M, Booth HDE, Haenseler W, Vowles J, Bowden R, Webber C, Cowley SA, Wade-Martins R (2019) Cellular α-synuclein pathology is associated with bioenergetic dysfunction in Parkinson’s iPSC-derived dopamine neurons. Hum Mol Genet 28:2001–2013. https://doi.org/10.1093/HMG/DDZ038
Zangari J, Petrelli F, Maillot B, Martinou J-C (2020) The multifaceted pyruvate metabolism: role of the mitochondrial pyruvate carrier. Biomolecules 10:1068. https://doi.org/10.3390/biom10071068
Zhang Z, Liu L, Wu S, Xing D (2016) Drp1, Mff, Fis1, and MiD51 are coordinated to mediate mitochondrial fission during UV irradiation-induced apoptosis. FASEB J • Res Commun. https://doi.org/10.1096/fj.15-274258
Zhao J, Liu T, Jin S, Wang X, Qu M, Uhlén P, Tomilin N, Shupliakov O, Lendahl U, Nistér M (2011) Human MIEF1 recruits Drp1 to mitochondrial outer membranes and promotes mitochondrial fusion rather than fission. EMBO J 30:2762–2778. https://doi.org/10.1038/EMBOJ.2011.198
Zheng J, Winderickx J, Franssens V, Liu B (2018a) A mitochondria-associated oxidative stress perspective on Huntington’s disease. Front Mol Neurosci 11:329. https://doi.org/10.3389/FNMOL.2018.00329/XML/NLM
Zheng J, Winderickx J, Franssens V, Liu B (2018b) A mitochondria-associated oxidative stress perspective on Huntington’s disease. Front Mol Neurosci
Zorov DB, Juhaszova M, Sollott SJ (2014) Mitochondrial reactive oxygen species (ROS) and ROS-induced ROS release. Physiol Rev 94:909–950. https://doi.org/10.1152/physrev.00026.2013
Author information
Authors and Affiliations
Contributions
SVM, NLW, MBK, and TB: conceived the idea and wrote the article; ABU, BGT, and MJU: figure work; MKA and HGD: literature search; SM and TB: proof read.
Corresponding author
Ethics declarations
Ethics Approval
Not applicable.
Consent for Publication
All the authors have approved the current manuscript for final publication.
Conflicts of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Mangrulkar, S.V., Wankhede, N.L., Kale, M.B. et al. Mitochondrial Dysfunction as a Signaling Target for Therapeutic Intervention in Major Neurodegenerative Disease. Neurotox Res 41, 708–729 (2023). https://doi.org/10.1007/s12640-023-00647-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12640-023-00647-2