Abstract
Regenerative medicine aims to restore, regenerate, or replace tissues or organs affected by disease, trauma, or congenital disabilities. Tissue engineering is one approach used to accomplish these objectives. Tissue engineering is commonly associated with the use of cells placed on tissue scaffolds in developing new living tissue for medicinal purposes, but it is not limited to cell and tissue scaffold applications. It is the procedure of designing tissues in the body in a laboratory and implanting them in patients. Tissue engineering currently plays a minor role in clinical outcomes. People with the disease have extra bladders, tendons, skin grafts, and tiny aorta, as well as an entire bronchial tube transplant, but the therapies are experimental and costly. Regarding this, three-dimensional (3D) and 4D bioprinting methods are beneficial for the production of scaffolds with different shapes, high accuracy, high speed, and control over the size and also porosity. In this chapter, the principal and most popularly used types of 3D bioprinting methods are explained, as well as a summary of bioink compositions in 3D and 4D bioprinting. Eventually, current problems and changing demands are highlighted. Furthermore, the most recent applications in organ and tissue bioprinting are discussed. Lastly, current issues, future requirements, and the potential of bioprinting are reviewed.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
9.1 Introduction
Initially, 3D printing technology was primarily utilized in manufacturing metals and ceramics. With the rapid progress of 3D fabrication, it has wide application in the electronic and optoelectronic military and automotive industry and also, most recently, in biofabrication. The process of organizing cellular and noncellular ingredients in space to imitate the formation, form, and function of human tissue is known as biofabrication. Three-dimensional (3D)-printed materials typically have suitable mechanical performance and resolution. Appropriate biomaterials offer optimization microenvironments for implanted cells, resulting in enhanced viable cells and functionality. The high resolution of the process permits cells/matrix/biomolecules and biomaterials to be accurately distributed to simulate native tissue architecture (Huang et al. 2017; Jana and Lerman 2015). Biomaterials to be used in tissue engineering applications can be fabricated through many traditional methods, such as chemical/gas foaming, solvent casting, emulsion templating, particle/porogen leaching, electrospinning, freeze-drying, phase separation, and also 3D bioprinting. The bulk properties can be managed, while the pore size, shape, topology, and architecture cannot be determined with other techniques except 3D bioprinting. Moreover, 3D bioprinting enables concise and specific placement of biological materials, biochemicals, and living cells by layer-by-layer deposition (Huang et al. 2017; Zhu et al. 2016).
The opportunity for additive manufacturing (AM), also defined as three-dimensional (3D) printing for the production of biomaterials in 3D tissue engineering applications, has increased with rapid innovations in computer-aided design/computer-aided manufacturing (CAD/CAM) systems. In 1986, Charles W. Hull presented 3D printing for the first time. Hull’s stereolithography (SLA) method benefits from ultraviolet (UV) light to cure thin layers of material on top of existing layers, resulting in a 3D pattern. Three-dimensional bioprinting is a multidisciplinary concept with roots in engineering, biology, and also material sciences, which is to manufacture 3D organ structures that protect, reestablish, and/or enhance tissue activity (Seyedmahmoud et al. 2020, 2015; Kruth et al. 1998; Langer and Vacanti 1993; Hull 1986).
The growth of such 3D in vitro applications has gained the interest of medicine. It is mainly based on two requirements: a scarcity of organs (Huang et al. 2008) and a desire for much less costly drug testing concepts (Shafiee and Atala 2016). The popularity of regenerative medicine has risen dramatically in the past years. The number of people on the organ transplant list of the next ones in the United States nearly doubled from 95,000 between 2006 and 2016. The significant increase in the list shows the need for current living donor remedies (Seyedmahmoud et al. 2020; Abouna 2008). Three-dimensional bioprinting methodologies for orthopedic tissue design are illustrated in Fig. 9.1. Moreover, the central concept of 3D bioprinting is depicted in Fig. 9.2.
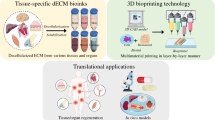
Three-dimensional bioprinting of biomimetic functional tissue constructs and translational applications in orthopedic tissue engineering and regenerative medicine (Chae and Cho 2022)
Schematic diagram showing the three main steps in 3D bioprinting: preprocessing, processing, and postprocessing (Bejoy et al. 2021)
9.2 Prebioprinting
The encompassing objective of this process is to produce a 3D vital point tissue scaffold model, which could be formed using clinical imaging techniques or computer-aided design (CAD). The most widely known imaging technology tools used to obtain data on the anatomical structure of a tissue or organ are magnetic resonance imaging (MRI), X-ray, and computed tomography (CT) (Seyedmahmoud et al. 2020; Murphy and Atala 2014; Mironov et al. 2008).
9.3 3D Bioprinting Technology
Three-dimensional bioprinting is a new form of technology used in tissue engineering and regenerative medicine to create complex tissue structures that mimic organs and tissues. This 3D bioprinting technology involves a layer-by-layer deposition of cell-loaded biomaterials in a predetermined structural architecture to create functional tissues or organs. To create complex structures, this technique integrates biomaterials, living cells, and controlled motor systems. It can produce more advanced structures than some other existing methods, such as electrospinning, emulsion templating, and freeze-drying. Computer-aided design can be used to create complex 3D tissue scaffolds (CAD) (Izbudak 2021; Chen and Shi 2013; Liu et al. 2005). The use of 3D printers enables the fabrication of scaffolds, devices, and also highly complex tissue models. Three-dimensional printers can also be utilized in medical imaging developed through computerized design. Some important features, such as patient-specific design, production on demand, obtaining high structural complexes, low cost, and high efficiency affect the use of 3D printers in the medical field (Yüce Erarslan 2021; Guvendiren et al. 2016; Guillemot et al. 2010).
Three-dimensional bioprinting systems have opened up new valuable applications and are currently progressing as a game-changing technology in the sense of the future of human health, with studies such as artificial organ printing in the healthcare system, the repair of lacking bone parts, and the manufacturing of private implants (Ozbolat 2016; Topuz et al. 2018). Furthermore, 3D bioprinters enable the utilization of direct copies of patient architectural results attained through various scanning systems, such as X-ray CT (Topuz et al. 2018; Hockaday et al. 2012; Inzana et al. 2014) and MR, and they generate biomimetic 3D biological tissue with good precision (Topuz et al. 2018; Yanagawa et al. 2016). Bioprinting is composed of many types (see Fig. 9.3).
The different 3D bioprinting techniques: (a) extrusion-based bioprinting, (b) inkjet-based bioprinting, (c) laser-based bioprinting, and (d) stereolithography (Bejoy et al. 2021)
Advantages of 3D Bioprinting
-
It is faster and mostly more concise than conventional hand-built organ strategies.
-
Organs are rarely to be dismissed concerning transplantation.
-
Organ trafficking has been lowered.
-
Human error is decreased, and scientists will find it less complicated.
-
The final products are not dependent on biomaterials or scaffolding that are not present in native tissues.
-
Without human subjects, the impact of illnesses or drugs may be noted more precisely.
-
Tissue reproducibility is guaranteed through strict control of both composition and shape; minimized changes.
-
Tissue-specific functions can be improved with well-organized and various cell forms (https://sites.google.com/site/gsse2014b2/pros-cons).
Disadvantages of 3D Bioprinting
-
When a printed object fails, liability problems occur.
-
There are several moral considerations.
-
It involves high pricing.
-
A lot of energy is consumed.
-
Some harmful particles are emitted into the atmosphere.
-
There are challenges in regulating cellular media causing the death of cells in a large number of cases.
9.3.1 3D Bioprinting in Tissue Engineering
The traditional technique for developing an engineered-tissue product is associated with the first manufacturing of a unique native tissue design, usually accompanied by the supply of cells and biomolecules. Nevertheless, this strategy can play a part in two major disadvantages: restriction in cell transmission and a decrease in cell growth because of low density at the core zone (Chowdhury et al. 2020; Derakhshanfar et al. 2018). The tissue engineering innovation has influenced the present framework via computer-aided layered manufacturing, also known as 3D bioprinting. In summary, 3D bioprinting is combining the main components identified as “bioink” that serves as a biological template and numerous types of cells with the presence of chemical factors and biologically active compounds to construct a solid and functional in situ 3D living structure (Chowdhury et al. 2020; Guvendiren et al. 2016).
When printing tissue or organs, this bioink generally contains living cells; however, when printing scaffolds, this bioink does not involve living cells. Aside from cells, the bioink is composed of a variety of polymer compositions that the cells are suspended. Polymers serve as the organs’ basic framework, helping to promote cell adhesion, proliferation, and growth (Munaz et al. 2016). They can exist as specific hydrogels or polymers or as a mixture of them. Moreover, bioinks containing bioceramic compounds (tricalcium phosphate and hydroxyapatite) are also used (Mukherjee et al. 2019; Pekkanen et al. 2017; Dávila et al. 2016; Jose et al. 2016). Among the different biomaterials, hydrogels are the most superior materials used as bioinks in 3D bioprinting. The main reason for this is their ability to retain living cells, their changeable chemical structure, their adjustable mechanical and biological degradation properties, and the fact that they can provide good resolution during printing (Izbudak 2021; Topuz et al. 2018). Over the last several decades, three-dimensional (3D) printing (rapid manufacturing or additive manufacturing) technologies have become increasingly popular in a variety of industries (Gu et al. 2018). However, some critical properties must be regarded in these applications (Chan and Leong 2008). First of all, the tissue scaffold to be produced must be biocompatible. The 3D scaffolds should be biodegradable or bioabsorbable, and the tissue must be able to completely substitute the scaffold. The mechanical properties that are suitable for the tissue to be implanted should be present. Moreover, the 3D scaffold should be easily fabricated in a wide range of forms and sizes (Gu et al. 2018).
Bioprinting has mainly three methodologies: imaging, computer-aided design of the tissue to be printed, and printing itself, the formation of bioink through the selection of appropriate materials, the choice of a proper bioprinter based on the product desired, for the manufacturing of scaffolds and/or tissues (Hacıoglu et al. 2018). Numerous techniques for producing 3D scaffolds from synthetic and natural polymers have been developed, such as emulsion templating, freeze-drying, solvent casting, gas foaming, phase separation, electrospinning, and melt molding (Gu et al. 2013; Kim et al. 2016a, b; Ma and Xue 2015; Oh et al. 2003). Fabrication techniques do not allow for effective control of porosity, pore size, scaffold shape, and interconnected pore morphology within the scaffold. Furthermore, the capability to make scaffolds from cells has drawbacks (Gu et al. 2018). Inkjet printing, extrusion-based methods, light-induced (photopolymerization) methods, and particle-fusion-based methods are the four techniques used in 3D bioprinting.
In the past few years, the 3D printing system has progressed quickly in the tissue engineering and regenerative medicine field (Topuz et al. 2018; Cornelissen et al. 2017). At the end of 2022, the global 3D bioprinting market is expected to reach nearly $1.82 billion (Topuz et al. 2018). Considering the future potential of bioprinting and reconstructive surgery and its objectives, it is indisputable that 3D bioprinting technology will emerge in plastic surgery (Jessop et al. 2017). Therefore, current studies will focus on improving novel bio-based materials in the 3D bioprinting sector for tissue engineering, emphasizing printable biomaterials (e.g., bioink) (Topuz et al. 2018).
9.3.2 Bioinks for 3D Bioprinting
The choice of biomaterial suitable for a bioink is a critical step in achieving a promising bioprinting product, as well as other fabrication processes. When polymers are chosen as bioinks, it is essential to know how polymer properties affect printing efficiency and cytocompatibility. These bioinks are anticipated to provide mechanical stability for the printed product due to their use during the process. In this scope, many natural polymers (gelatin, chitosan, cellulose, collagen, etc.) and some synthetic polymers, like polycaprolactone (PCL), polylactic acid (PLA), and poly(lactic acid-co-glycolic acid) (PLGA), are commonly utilized in tissue engineering applications (Hacıoglu et al. 2018).
9.3.2.1 Natural Polymers
9.3.2.1.1 Sodium Alginate
Sodium alginate is a polysaccharide sourced from brown algae. It is extensively used in 3D bioprinting due to its biocompatibility, low cost, and rapid gel formation (Du 2018). According to recent studies, sodium alginate is often blended with other polymers that are easy to mold and have a preferable biological nature, and it is a dominant material in drug and cell transport and cell encapsulation (Ozbolat et al. 2014). Despite all these advantages, alginate has low cell adhesion compared to other natural biomaterials (Yüce Erarslan 2021; Ahn et al. 2012). Furthermore, low-concentration sodium alginate has poor mechanical capacity and yet is helpful in increasing cell viability and proliferation (Du 2018).
9.3.2.1.2 Gelatin
Gelatin is a natural protein that is formed by hydrolyzing collagen. It also has amphoteric properties due to alkaline and acidic amino acid functional groups. It can be obtained through the extraction of other sources (such as bones, skin, or tissues of various animals). (Yüce Erarslan 2021; Chiou et al. 2008). Gelatin has good cell adherence, high biocompatibility, and complete biodegradability properties in vivo conditions without immunogenic, which has increased interest (Du 2018; Kuijpers et al. 2015). Gelatin chains have helical structures at low temperatures, which combine on their own to form a gel-like structure. On the other hand, this physical formation reverts to a random helical structure at high temperatures. Therefore, gelatin is a kind of thermoreversible gel. Some studies indicated that it dissolves when incubated at 37 °C for a long time. To overcome this issue, chemical cross-linking is carried out under UV light in the presence of a photoinitiator by adding unsaturated groups to the main chain of gelatin. The unsaturated groups are usually provided by methacrylic anhydride, and such gelatin derivatives are called methacrylated gelatin “GelMA” (Yüce Erarslan 2021; Sakai et al. 2009). Aldana et al. (2021) designed GelMA-alginate-based biomaterials via 3D bioprinting. In this study, the biomaterials contained sheep-adipose-derived stem cells, and the biomaterials in different blend concentrations were cultivated in vitro for 24 h before being tested for bioactivity in 3D-bioprinted structures (Fig. 9.4).
Fluorescence microscopy images of live (green)/dead (Zhang et al. 2018) cells in (a) G6A5, (b) G6A7, and (c) G8A7 hydrogels at 24 h. (d) Image of printed G8A7 hydrogel construct. (e) Cell viability in gelMA-alginate constructs. Printing of stripe-patterned hydrogels: biaxial mechanical testing (Aldana et al. 2021)
9.3.2.1.3 Silk Fibroin
Fibrinogen is a protein-based polymer formed in a living body, used as a sealant and adhesive in surgery, for cartilage treatment in tissue engineering, and in wound healing applications (Fontes and Marcomini 2020; Skardal et al. 2012; Ahmed et al. 2008). Fibrinogen is required for effective blood coagulation and is utilized as a type of 3D bioink. Fibrin, like other natural polymers, has high biocompatibility, allowing for numerous high affinitie for cell adherence and growth (Tao et al. 2012; Schacht et al. 2015). However, with the fast degradation of fibrin, it is not proper for prolonged culture media to be formed in vivo tests, and low viscosity complicates processability as well (Das et al. 2013). Consequently, several studies have pointed out that fibrin can mix with other natural polymers, such as gelatin, alginate, and collagen (Yu et al. 2020; Schacht et al. 2015).
9.3.2.1.4 Agarose
Agarose is mainly a seaweed-derived marine polysaccharide. Because of its gelation, biocompatibility, and rheological properties, it is widely used in biological applications (Jakus et al. 2016a, b; Fontes and Marcomini 2020). Agarose gelling is caused by the formation of intermolecular hydrogen bonds on cooling, which results in the agglomeration of the helical structure. Although it has excellent biological and mechanical features, its ability to enable cellular proliferation is restricted (Fontes and Marcomini 2020; Hospodiuk et al. 2017). Therefore, the use of agarose alone means that it is inappropriate for the production of cell-loaded biomaterials. Furthermore, it shows a thermo-reversible feature with a sol-gel transition between 32 and 47 °C (Du 2018; Yu et al. 2020; Medina-Esquivel et al. 2008).
9.3.2.1.5 Pullulan
Pullulan is a type of polysaccharide that is typically made from the yeast Aureobasidium pullulans (Saroia et al. 2018). It is generated on the surface of bacteria-infected cells. For the first time, studies on the physicochemical structure of pullulan began to be conducted by Bernier in 1958. It is insoluble in either organic or inorganic solvents, except water. Therefore, pullulan is preferred in food packaging and biomedical applications (Singh and Saini 2008). Additionally, pullulan can be obtained via fermentation, thanks to various types of waste (Saroia et al. 2018; Singh et al. 2009; Thirumavalavan et al. 2009). Studies have been conducted on extracting pullulan and dextran, which help the rapid development of endothelial cells. Pullulan and derived materials with osteo-communication properties were utilized in tissue engineering. The mechanical strength of pullulan was enhanced via the mixing and cross-linking of pullulan and dextran (Saroia et al. 2018; Aschenbrenner et al. 2013).
9.3.2.1.6 Hyaluronic Acid
Hyaluronic acid is a polysaccharide with a high molecular weight, which is one of the main components of the extracellular matrix (ECM) (Yüce Erarslan 2021; Mobaraki et al. 2020; Falcone et al. 2006). It is generally used in surgeries as a skin filler and joint lubricant (Du 2018; Sharif et al. 1995). Cell viability is extremely high in 3D-printed hyaluronic acid hydrogel sealed in cartilage tissue than in collagen hydrogel. Nevertheless, hyaluronic acid has weak mechanical stability that changes with the rate of degradation; it must be modified to allow for the control of the rate of degradation. For this reason, hyaluronic acid is not proper for 3D bioprinting. The obtained 3D hyaluronic acid hydrogel structures have low stability due to the rapid solubility of unmodified hyaluronic acid in water (Pescosolido et al. 2011). Many studies focused on the functional treatment of hyaluronic acid polysaccharide chains with hydrophobic groups and/or by photo-cross-linking methyl acrylate (MA) (Du 2018; Yüce Erarslan 2021).
9.3.2.1.7 Chitosan
Chitosan is a linear amino polysaccharide derived from chitin and its derivatives, consisting of (1–4)-linked d-glucosamine structures and N-acetyl-glucosamine groups that are randomly located (Vega-Cázarez et al. 2018). It cannot be dissolved in aqueous media with a pH greater than neutral due to its semi-crystalline structure. Thanks to its biodegradability, biocompatibility, and antimicrobial structure, it is prevalently preferred in many fields, such as bone, skin, and cartilage regeneration; the formation of sponge scaffolds; and wound dressings. Because chitosan has a slow gelation rate (10 min after injection) and low mechanical strength, just stents with a high viscosity can maintain their form for hours (Du 2018). Chitosan is applied to 3D bioprinting to develop different stents and microflow channels.
9.3.2.1.8 Collagen
Collagen is the most frequently known and utilized protein in tissue engineering due to its triple helix structures with self-aggregating properties via covalent and hydrogen bonds (Saroia et al. 2018). It is the principal protein constituent of ECM in real tissues/organs (Peppas et al. 2006), and collagen sources include rat and pig tendon materials (Yu et al. 2020; Osidak et al. 2019; Diamantides et al. 2019). Collagen offers excellent growth conditions for cell growth, adhesion, and function due to its abundance of integrin-binding areas (Yu et al. 2020). It can make a variety of artificial tissues, including skin, cartilage, heart valves, reconstructed breast, vocal cord, and spinal cord (Saroia et al. 2018; Tangsadthakun et al. 2017; DeLustro et al. 1986; Taylor et al. 2006; Hahn et al. 2006; Slaughter et al. 2009; Cavallo et al. 2015). Collagen can produce various types of gels, sponges, and other materials because of changes in collagen strands and the induction of cross-linking (Saroia et al. 2018). At low temperatures, collagen is in the shape of a pre-gel, and it may be cross-linked thermally at 37 °C. Moreover, it is cross-linked with UV, glutaraldehyde, carbodiimide, and genipin and is vulnerable to collagenase degradation. Despite its advantages, the low viscosity of collagen requires its mixing with other polymers for bioprinting (Yu et al. 2020; Weadock et al. 1995; Harriger et al. 1997; Powell and Boyce 2006; Kim et al. 2016a, b). The suitability of collagen for 3D bioprinting is determined by the concentration of collagen in a solution. Only increased collagen concentrations (higher than 20 mg/mL) in single-component collagen bioinks enable higher printing reliability (Osidak et al. 2020). Figure 9.5 shows collagen-based 3D biomaterials produced for chondral tissue engineering in a study.
A cylindrical CAD model (a) was 3D bioprinted using a chondrocyte-laden type II collagen bioink (b). The scaffolds were cultured for 3 weeks before harvesting to analyze chondrogenic ECM deposition and gene expression (c, d). (Reprinted from Ren et al. (2016) under Creative Commons CC BY license (Chartrain et al. 2022))
Kakarla et al. (2022) designed a hydrogel based on gelatin, alginate, and boron nitride nanotubes via an extrusion 3D bioprinting method. The scaffold model was created in SolidWorks and has dimensions of 10 × 10 × 1 mm, a layer thickness of 0.17 mm (three layers), and a pore size of 0.5 mm (Fig. 9.6).
(a) 3D scaffold designed in SolidWorks and (b) scaffold printing via a 3D bioprinter with the insight of scaffold postprinting (Kakarla et al. 2022)
9.3.2.2 Synthetic Polymers
Synthetic polymers have superior mechanical and chemical properties compared to natural polymers. Nevertheless, synthetic polymers offer few or no cell niches performance. Generally, polycaprolactone (PCL), polylactic acid (PLA), poly(ethylene) glycol (PEG), polyvinyl alcohol (PVA), and polyglycolic acid (PGA) are used in 3D bioprinting. PLA, PGA, and PCL have outstanding biodegradability, biocompatibility, and mechanical properties (Huang et al. 2017; Mota et al. 2015). These polymers were given in detail in this section.
9.3.2.2.1 Polyvinyl Alcohol (PVA)
PVA is a water-soluble synthetic, one that is both biocompatible and biodegradable, and also it is confirmed by the Food and Drug Administration (FDA, USA) (Aslam et al. 2018; Marin et al. 2014). This polymer is usually blended with natural ones (gelatin, alginate, and/or chitosan) due to low cell affinity and has undergone physical modification (Yu et al. 2020).
9.3.2.2.2 Polyethylene Glycol (PEG)
PEG is a convenient polymer for designing 3D scaffolds, owing to its high hydrophilic nature, higher tensile strength than natural-based polymers, and good biocompatibility (Yu et al. 2020; Alcantar et al. 2000). It can be tailored by combining alginate and collagen to meet specific needs (Fontes and Marcomini 2020). Further, to increase the diacrylate (DA) or methacrylate (MA) mechanical properties, it can be modified with other polymers (Yu et al. 2020; Aduba et al. 2019; Cheng and Chen 2017). Many acrylate-based PEG, such as PEG-DA and PEG-MA hydrogels, can be printed on almost all bioprinters, e.g., extrusion-based, laser-based, and droplet-based bioprinting.
9.3.2.2.3 Polycaprolactone (PCL)
PCL is classified into polyesters that are biodegradable, are hydrophobic, and also has semi-crystalline features approved by the FDA (Saroia et al. 2018; Bhavsar and Amiji 2008). The incorporation of bioactive glasses and Ca3(PO4)2-based particles into PCL in bone tissue engineering increases its many properties, especially its mechanical strength (Hajiali et al. 2018). A study showed that PCL has excellent biocompatibility with periosteal cell culture systems and human fibroblasts (Salgado et al. 2012). The mixture of PCL with other polymers or bioactive agents to develop a more appropriate media for protein progression. In many studies, PCL mixed with heparin and curdlan sulfate enhances the response of cultivated tissues and increases the protein ability of the mixture (Saroia et al. 2018). Similarly, various composites, including ceramic particles, such as calcium phosphate (CaP) and hydroxyapatite, were produced for bone regeneration (Huang et al. 2017).
9.3.2.2.4 Polylactic Acid (PLA) and Polyglycolic Acid (PGA)
PLA and PGA are also included in the polyester class, as is PCL. However, PLA and PGA, by themselves or in combination with other bio-based polymers, offer an excellent physiological media for cell growth because their hydrophobic nature can confine cell attachment (Saroia et al. 2018; Bee et al. 2018; Gentile et al. 2014). PLA and PGA are preferred for fabricating artificial vascular grafts, owing to their excellent mechanical strength (Parın and Terzioğlu 2022). Therefore, some modification techniques, such as plasma treatment and/or surface coating, can be applied to printed PLA and PLGA to form 3D cell culture media for the growth of different tissues (Deng et al. 2020).
Bismuth ferrite (BFO)-nanoparticle-loaded PLA scaffolds were fabricated by Bedir et al. (2020). It is clearly seen in Fig. 9.7 that the BFO is agglomerated in the neural tissue scaffolds.
Production of BFO-doped PLA scaffold by a modified 3D printer (a), BFO-doped PLA scaffold (infill 70%) (b), SEM images of BFO-doped PLA scaffold (infill 70%) (c, d) (Bedir et al. 2020)
9.3.3 3D Bioprinting in Tissue Engineering Applications
9.3.3.1 Bone Tissue Engineering
Bone tissue supports the mechanical strength of tissues and organs and movement in the human body. It is essential for homeostasis and blood pH regulation because it acts as a mineral store with a complicated hierarchical structure (Yilmaz et al. 2019; Sowjanya et al. 2013). Bone is comprised mainly of collagen, other proteins, water, and mineral phase. As a result, 3D-printed forms should preferably have similar properties. In this situation, composite materials, such as collagen mixed with various types of bioceramics, are being assertively utilized to enhance 3D-bioprinted structures (Yu et al. 2020; Osidak et al. 2020; Yilmaz et al. 2019).
Biomaterials and tissue-engineered structures have grown in importance over the past few decades. Bone is the second-most commonly implanted tissue in the world, with over four million operations conducted annually to heal damaged tissue using bone grafts. The development of printing processes and the improvement of suitable ink materials are the primary concerns of 3D bioprinting in bone tissue design. To produce new alternatives to conventional bone grafts, different materials have been designed to be used in bioprinting. Hydrogels, ceramics, and also polymers alone cannot completely simulate the properties of bone when used alone. Synthetic and natural polymers are usually mixed with osteogenic components, such as tricalcium phosphate (TCP), hydroxyapatite (HAP), silica, nano calcium phosphates, and bioactive glass particles to enhance bioactivity (Ashammakhi and Kaarela 2017). Furthermore, some growth factors have also been added to the polymer matrix. The major problem in 3D bioprinting is the synchronous incorporation of living cells and biostructural materials. The capability of creating cell-free scaffolds utilizing a variety of 3D-printed materials makes this method desirable for bone tissue engineering applications (Yilmaz et al. 2019). 3D bioprinted tissue structures were produced of by Matrigel TM and alginate-based hydrogels were produced by Fedorovich et al. (2008). In another study, Phillippi et al. (2008) showed the myogenic differentiation of patterned BMP-2 on fibrin-coated lamellar by inkjet bioprinting. The osteogenic and chondrogenic activities of PEGDMA-GelMA bioinks were examined in a study (Gao et al. 2014). The obtained 3D-bioprinted constructs indicated both good cell proliferation (>80%) and an increased degree of differentiation in comparison with pure PGDMA (Ozbolat et al. 2016). The mechanical strength and cell viability of alginate and bone-derivatived methacrylated ECM with hASC cell-loaded mesh structures were investigated by Lee et al. (2020). Furthermore, bioprinted bone-like tissue fabricated from gelatin and alginate hybrid matrix (Zhang et al. 2020). To enhance the mechanical features, photocrosslinkable glycosaminoglycan hyaluronic acid scaffolds were fabricated by (Poldervaart et al. 2014). Skardal et al. (2012) designed bioprinted materials containing fibrous collagen gels with bone marrow mesenchymal stem cells for wound healing, and they analyzed wound closure and epithelial restoration. It demonstrated that the the in vivo bone regeneration impact was studied in a critical-size calvarial defect model of rats (Fig. 9.8).
Construction of a bone defect model and demonstration of the scaffold implant operation process. (a) 5 mm diameter implanted bioprinted scaffolds. (b) 5 mm diameter defective cranial tissue. (c) Isolating surrounding soft tissue to expose the skull and creating a 5 mm diameter defect in rat critical-size calvarial model. (d) Inserting scaffolds into a calvarial defect. (e) and (f) Suturing subcutaneous tissue and skin wounds (Shen et al. 2022)
9.3.3.2 Neural Tissue Engineering
Neural cords have been suggested as a successful neural recovery matrix that supports and helps neuron cells utilize tissue engineering strategies in the therapies of peripheral nerve and spine injuries. Bioprinting is a newer technique for fabricating manageable 3D scaffolds for neural tissues with various cellular categories and complex micro/nanoscopic functions. The main considerations for the layout of nerve guide conduits are ensuring mechanical strength while also optimizing the proximal and distal nerve ends and restricting nerve compression. Extrusion printing is one of the most widely used printing processes in nerve conduit designing because gels can be deposited quickly and easily. Nevertheless, laser-based bioprinting, like stereolithography and inkjet printing, enables higher print resolution, which is important for imitating the anisotropic design of nerve tissue. Because neural cells are comparatively more susceptible to their extracellular environment, the choice of bioink has a substantial influence on neural recovery. Generally, collagen is preferred in nerve regeneration. In collagen hydrogels produced with moderately concentrated collagen solutions, neurite outgrowth is much more noticeable. Furthermore, Hsieh et al. (2015) have bioprinted thermoresponsive polyurethane (PU) (37 °C) hydrogel with adjustable gelling ability and hardness without any cross-linker. In the study, neural stem-cell-loaded bioink has been found to benefit neural injuries. Interestingly, the bioink recovered the function of the damaged nervous system in less than 1 week. Some researchers found that alginate bioinks with the use of cell adhesion factors enhanced cell compatibility. In a study on this, the efficacy of RGD or YIGSR peptide in alginate increased cytocompatibility (Sarker et al. 2019). The scaffolds designed via an extrusion-based 3D bioink method had more cells than pure alginate scaffolds after 9 days in culture media (Sarker et al. 2019; Yilmaz et al. 2019). To assess biocompatibility for in vitro/in vivo tests, gelatin-alginate-based 3D biostructures were created by Wu et al. (2020). More than 90% of Schwann cells lived after 24 h and remained viable for 7 days (Yu et al. 2020). Meanwhile, rat PC-12 cells were investigated by Ngo et al. (2020), who found that by adjusting important characteristics of the bioink design, 3D-printed hydrogels based on hyaluronic acid methacrylate (HAMA) might increase cell survival and aid in peripheral nerve repair (Fig. 9.9).
9.3.3.3 Vascular Tissue Engineering
Artificial blood vessels play a crucial role in linking metabolically demanding organs, allowing nutrients to be delivered while separating waste (Yu et al. 2020). Nutrients and oxygen are easygoing in a 2D cell culture with a cell population thickness of around 20–30 μm (Gu et al. 2018; Colton 1995). Various bioprinting methodologies, including extrusion, droplet, and laser-based bioprinting, have been used to design vascular tissue (Ozbolat et al. 2016). Accordingly, 3D bioprinting methodologies which design objects of the preferred shape utilizing various bioinks and kinds of cells have occurred as intelligent techniques to for designing vessels with small diameters (Gu et al. 2018). Cui and Boland (2009) designed fibrin microchannels via an inkjet-based bioprinting technique. They revealed that when they bioprinted human microvascular endothelial cells (HMVEC) laden with fibrin hydrogel, the cells tailored themselves inside these fibrin networks and reproduced. Consequently, bioprinting both cells and the scaffold at the same time promotes HMVEC proliferation and microvessel generation. Consequently, bioprinting both cells and the scaffold at the same time promotes HMVEC proliferation and microvessel generation was supported by the cells. Human neonatal dermal fibroblasts and human umbilical vein endothelial cells (HUVEC) grew significantly with time, according to the researchers (Gu et al. 2018).
9.3.3.4 Skin Tissue Engineering
Skin is the largest, most complex and outermost organ that acts as a barrier to infections and irritants, antioxidants, environmental factors, and any other externally harmful agents (Askari et al. 2021). In terms of wound size, extent, and depth, researchers have developed a variety of wound dressings or natural-based skin substitutes (Yilmaz et al. 2019; Sheridan 2009). Chronic, nonhealing wounds caused by burns, trauma, or diseases are clinically significant since they place a great deal of pressure on both the patient and the medical system. Biocompatible wound dressings, designed skin grafts, and split-thickness skin grafting from autologous skin are currently used to treat chronic wounds. Though quite efficient, these skin substitutes are generally expensive, have poor adhesiveness, are susceptible to infection, or rely on skin health donation presence. Furthermore, the majority of present clinical practice-utilized skin substitutes are made entirely of dermal fibroblasts and keratinocytes and do not enhance vasculature (Gu et al. 2018; Church et al. 2006).
Consequently, skin damage is a significant issue having in-depth impacts on other tissues (Jean et al. 2011; Metcalfe and Ferguson 2007). During skin damage, autologous grafts sourced from a patient are frequently utilized to prevent immune reactions and regulate skin activity and wound repair. However, autologous grafts do not properly mend skin damage injuries encompassing a big region or having a serious depth (Andreassi et al. 2005). Therefore, there is an urgent need to develop artificial skin replacements employing methodologies for tissue repair. The studies have resulted in complex tissue regeneration that connects with body tissue afterward in vitro regeneration and transplantation (Gu et al. 2018). Bioprinting allows the simultaneous accumulation of multiple kinds of skin cells. Also, 3D bioprinting enables the accurate placement of various types of cells and extremities within a structure (Yilmaz et al. 2019; Ng et al. 2016).
Chronic ulcers can be caused by skin damage, infections, or other genetic or physical conditions. Electrospinning, solvent casting, and freeze-drying are membrane preparation techniques that have long been used for skin graft development. Skin bioprinting is gaining popularity, owing to its intelligent and managed manufacturing qualities, which are difficult to attain with the traditional skin graft manufacturing process (Yilmaz et al. 2019). Droplet-based and laser-based bioprinting techniques are used for skin tissue substitution biofabrication. Bioprinting of skin tissue with a bioprinter with an eight-channel valve, in which a 13-layer tissue is bioprinted using collagen, was performed by Lee et al. (2013). Kim et al. (2019) explored a perfusable and preferable vascularized full-thickness skin equal made up of epidermis, dermis, and hypodermis for enhanced vascularization and effective epidermal progress. The printed HUVECs were found to be covered on the exterior of the vascular stream, forming endothelium that resembled tissue. In another study, Koch et al. (2012) used laser-assisted bioprinting to deposit 20 layers of fibroblasts (mouse NIH-3T3) and 20 layers of keratinocytes (human HaCaT) integrated into collagen gel onto a layer of decellularized dermal matrix to design dermis and epidermis layers, respectively (Yilmaz et al. 2019). Gholami et al. (2017) developed patches for wound healing, which include a 16% alginate solution (w/v) and 4% (w/v) gelatin (Yilmaz et al. 2019). In addition, Michael et al. (2013) used 3D-laser-based bioprinting to generate artificial skin. In this study, fibroblasts and keratinocytes were used to construct the skin substitutes. According to the in vivo test, the bioprinted keratinocytes obtained a multilayered epidermis with initial differentiation and stratum corneum at the end of 11 days in culture media.
Currently, nanoparticles are increasing in popularity in the field of transdermal delivery systems. Surface chemistry and form determine how well they penetrate skin tissue. In this regard, Hou et al. created an easy artificial skin model for the rapid screening of nanoparticles in terms of their transdermal penetration ability with 3D bioprinting methods. Fibroblasts were printed on the structure with collagen hydrogel and silica nanoparticles. The obtained 3D scaffolds were investigated via penetrating ability. As a result, positively charged nanoparticles penetrated deeper (Gu et al. 2018; Cubo et al. 2017). 3D bioink hydrogels consisting of two different layers of catechol-hyaluronic acid (HACA)/alginate and gelatin/horseradish peroxidase (HRP) were produced to mimic the structure of the skin in full thickness (Fig. 9.10).
9.3.3.5 Cartilage Tissue Engineering
Cartilaginous tissue is an avascular and aneural structure with low chondrogenic density and high water content (70%) (Askari et al. 2021; Sophia Fox et al. 2009). It has a functional and heterogeneous texture designed to provide a low-friction, wear-resistant, load-bearing surface for effective joint movement (Askari et al. 2021; You et al. 2017). Even if it is just a few millimeters thick, it prevents friction between the joints and provides excessive load stresses during body activities (Gu et al. 2018; Arkel and Amis 2013). Many researches have been performed try to convey bone marrow stromal cells in alginate hydrogels for extrusion bioprinting bone and cartilage regeneration (Tan et al. 2021; Fedorovich et al. 2008).
Gruene et al. (2010) designed laser-based bioprinting of stem-cell-differentiated chondrocytes, employing a computer-aided fabrication method with the aid of LIFT. The designed material skillfully printed porcine-bone-marrow-derived mesenchymal stem cells (MSCs) with high availability. The cells retained their features and ability to differentiate into osteogenic and chondrogenic bloodlines (Ozbolat et al. 2016). To restore cartilage deficiencies, cartilage tissue has been created through inkjet-based bioprinting. The human chondrocytes integrated into PEGDMA hydrogel was bioprinted an adjusted HP desktop printer (Cui et al. 2012a, b). The mechanical and biochemical composition of the created structures were almost similar to native cartilage (Ozbolat et al. 2016). Sodium alginate has been broadly utilized to create bioprinted cartilage tissue. The hybrid bioprinting of chondrocytes loaded on printed alginate filaments in combination with the bioprinting of chondrocyte spheroids to enhance cell density are demonstrated by Ozbolat et al. (2016) and Ozbolat et al. (2014).
9.3.4 Other Requirements for Effective Scaffold Design
The achievement of the manufactured scaffold is strongly affected by the bioink used and the 3D bioprinting technique (Salah et al. 2020). It also is dependent on other variables to ensure the scaffold’s achievement, which is as described in the following.
9.3.4.1 Pore Size
Porosity, pore size, and interconnected pore morphology represent critical parameters for scaffold production. All three properties allow cellular penetration, vascularization, adequate diffusion of nutrients and oxygen into the cells within the structure, and the new-formed extracellular matrix that ensures cell viability. In particular, pore size is an essential parameter for scaffold efficiency (Bružauskaitė et al. 2016). Actually, the pores must be large enough to allow cells to penetrate and migrate within the scaffold structure but small enough to allow a critical number of cells to connect (Izbudak 2021; Hutmacher 2000). A pore size that ranges from 100 m to more than 300 m is required for bone tissue engineering because it offers a hypoxic situation that improves both osteogenesis and angiogenesis for proper bone growth (Salah et al. 2020; Karageorgiou and Kaplan 2005). The effect of scaffold pore sizes on MSC differentiation by creating a gradient of oxygen required and more in the periphery and hypoxic in the center was studied by Di Luca et al. (2016). All scaffolds used for tissue engineering as a function of the host tissue type must have a specific pore size. In particular, a pore size of 20 μm is required for hepatocyte and fibroblast growth, while a pore size of around 20–150 μm is needed for soft-tissue healing. The researchers also propose a pore size between 200 and 400 μm for bone tissue engineering (Yu et al. 2015). Materials with pore sizes of 250 μm or higher are appropriate for forming blood vessels, as compared to those of smaller size (Yu et al. 2015; Babensee et al. 1998; An et al. 2015; Mukherjee et al. 2018).
A porous structure is required due to the tissue formation, vascularization, and tissue joining after implantation in an ideal tissue scaffold. In this case, the obtained scaffold must have an optimal pore structure for the intercellular nutrient and metabolic transmission to occur without adversely affecting its mechanical properties and stability. The scaffold should have pores that connect to permit cell and nutrient infiltration and waste removal (Bružauskaitė et al. 2016). The size of the pores influences cellular proliferation and attachment along the scaffold to substitute it. Small pore sizes inhibit waste removal and nutrient diffusion, whereas larger pore sizes inhibit intercellular ligand formation, which is required for cellular proliferation (Salah et al. 2020).
9.3.4.2 Surface Area
The surface area is important for cell reinforcement and proliferation. It is clearly regarded that a larger and more available surface area promotes cell and tissue connection in scaffolds. It is critical in the context of tissue or organ function restoration or replacement because a high surface-to-volume ratio allows more cells to be compensated (Mukherjee et al. 2018; Dhandayuthapani et al. 2011; Boyan et al. 1996).
9.3.4.3 Mechanical Properties
Mechanical property is also an important element in polymers as it affects the regeneration potential of hard tissues (Mukherjee et al. 2018; Dhandayuthapani et al. 2011). The structural stability of the resulting 3D shapes is influenced by the mechanical properties of the bioink. Because the scaffold must endure load and stress for new tissues to grow successfully, the rheological properties of polymers, such as maximum strain, elastic modulus, and tensile strength, are critical. Pore connectedness, orientation, form, size, and density are related elements that affect the scaffold’s mechanical behavior and structural stability (Mukherjee et al. 2018).
The shape stability of the resulting 3D structures is influenced by the mechanical properties of the bioink. Natural-based bioinks have poor mechanical properties. To solve this drawback, nanoparticle reinforcement, cross-linking, and hybrid biomultiplies produced by combining synthetic bioinks are commonly used approaches (Yüce Erarslan 2021). The biostability of many scaffolds depends on factors such as strength, elasticity, absorption, and chemical degradation at the material interface (Nair and Laurencin 2007). Besides, the mechanical properties of bioinks are related to their chemical structure and molecular design (Yüce Erarslan 2021).
9.3.4.4 Biodegradability
The biodegradability of a polymer is critical because it enables the degradation of the scaffold after a particular period and substituting itself with new tissues. Separating the polymer’s sensitive hydrolytic or enzymatic bonds promotes polymer biodegradation (Katti et al. 2002; Bružauskaitė et al. 2016; Mukherjee et al. 2018). The biodegradability of polymers is an intrinsic property that is affected by chemical composition, molecular weight, crystalline structure, glass transition temperature (Tg), and the spectrum of wettability (Mukherjee et al. 2018; Ye et al. 1997).
The degradation of 3D structures obtained by printing bioinks during cell culture is necessary for ideal cell differentiation. Although the shape stability of 3D structures is required for printing, controlled degradation of the structure is also vital for tissue regeneration. Microvasculature networks develop alongside tissue to form patient-specific organs through cell differentiation. However, sufficient oxygen and nutrients must be transported between cells, and metabolic waste must be removed from the structure. To successfully manage this process/issue, the cell growth rate and the degradation rate of the 3D structure must be compatible (Yüce Erarslan 2021).
9.3.4.5 Biocompatibility
Biocompatibility refers to the compatibility of a biomaterial with the body (Zhang and Zhang 2015). Biomaterials are substances that do not interfere with the expected changes in the tissues surrounding them, do not cause undesirable reactions in the tissue (inflammation, coagulation, etc.), and do not form. Biocompatibility is categorized into structural and surface compatibility. Surface compatibility refers to a biomaterial’s physical, chemical, and biological suitability to body tissues. On the other hand, structural suitability refers to the material’s optimal compatibility with the mechanical behavior of body tissues (Chen et al. 2016). Synthetic polymers and some natural polymers, which lack cell-binding structures, can inhibit cell adhesion and proliferation. This may cause cell death. To prevent this issue, cell-binding structures can be introduced to the matrix by blending synthetic polymers with natural polymers (Yüce Erarslan 2021).
9.3.4.6 Viscosity
Bioink viscosity has been studied extensively in 3D bioprinting and is one of the essential factors to consider when developing bioprinting methodologies (Tirella et al. 2009). Ceramics, beta-tricalcium phosphate, poly(caprolactone) (PCL), and polylactic acid (PLA) have high viscosity and high concentration, which are used in general in bone tissue engineering (bioprinting) (Theus et al. 2020). Nevertheless, because most thermoplastic materials necessitate an extreme melting temperature and do not encourage viable cell printing, hydrogel-based bioinks have become a favorable option in recent studies. For bone bioinks produced from hydrogels, gelatin methacrylate (GelMA), alginate methacrylate (AlgMA), and hyaluronic acid are utilized and supported by some osteogenic minerals and growth factors (Theus et al. 2020; Huang et al. 2019; Jakus et al. 2016a, b). In extrusion-based bioprinting systems, hydrogel viscosity varies between 30 and 60 × 107 mPa/s, with the concentration of the hydrogel affecting the viscosity level (Iordache 2019). Natural polymer alginate has low viscosity, and therefore, it is not a suitable biomaterial for extrusion-based bioprinters. Its viscosity can be enhanced by blending with materials such as cellulose, gelatin, and PVA (Iordache 2019).
Hydrogels used in inkjet-based bioprinting should be of low viscosity because, then, they can accurately flow through the piping system and nozzle without blockage. Bioink hydrogels must have rheological features that enable viscosity to rise once shear is applied. Viscosity ranges between 3.5 and 12 mPa/s based on the bioink concentration in the inkjet-based bioprinting system (Iordache 2019; Mandrycky et al. 2016). Hydrogel viscosity varies from 1 to 300 mPa/s in laser-based bioprinting. To ensure cell stability and mechanical strength, the hydrogel must be gelation capable (Iordache 2019).
In laser-assisted 3D bioprinting, the viscosity should be 1–300 mPa s. (Hospodiuk et al. 2017). It is critical that the 3D structure be sufficiently cross-linked after printing to strengthen mechanical integrity, owing to low viscosity values. Photosensitive bioinks are used in stereolithographic processes. The main advantage of this printing technique is that it reduces mechanical stresses on more viscous hydrogels containing encapsulated cells while maintaining high cell viability and functionality (Theus et al. 2020; Li et al. 2016a, b).
9.3.5 Types of 3D Bioprinting
3D bioprinting techniques are examined in detail in the following sections.
9.3.5.1 Inkjet 3D Bioprinting
Researchers have started 3D bioprinting by modifying standard 2D inkjet printers to print bioink in successive layers. Inkjet printers operate by collecting ink droplets at specific regions on a substrate. Thermal, piezoelectric, or electromagnetic forces can be used to expel droplets from the reservoir nozzle (Xu et al. 2005). Despite the fact that these forces produce severe regional conditions, the transient nature of the pressure permits the cells to remain viable with low stress. Clogging can occur even when using the best bioink for an inkjet printer (Seyedmahmoud et al. 2020; Ong et al. 2018). Inkjet bioprinting is one of the oldest printing methods. This method, which is based on the noncontact accumulation of biofunctional ink droplets, is divided into thermal, piezoelectric, and mechanical. This technique is generally preferred due to its compatibility with cells and materials, high printing speed, high cell viability, and low cost. High-viscosity materials restrict its application (Akkuş et al. 2020; Hacıoglu et al. 2018; Noh et al. 2017).
Thermal-inkjet-based bioprinters spray the bioink drop by drop from the nozzle by electrically heating the bioink cartridge. In many studies, it has been reported that this local heating has no significant negative effect on the biological molecules in the bioink. On the other hand, inkjet 3D bioprinters with piezoelectric systems have a piezoelectric crystal in the bioprinter card slot to periodically separate the bioink into droplets. When a voltage is applied to this crystal, acoustic waves form, and pressure is applied to the cartridge. The biomarker in the cartridge is sprayed from the nozzle with this pressure (Vurat 2021).
9.3.5.2 Microextrusion 3D Bioprinting
Fused deposition modeling (FDM), also defined as microextrusion-based 3D bioprinting, is an additive manufacturing process that rotates from around the accumulation of a substance in successive layers to form the ideal three-dimensional structure. In comparison to inkjet and laser-assisted bioprinters, microextrusion bioprinters can work with a broader range of viscous bioinks (Seyedmahmoud et al. 2020; Cui et al. 2012a, b; Chang et al. 2011).
The most common and low-cost printing techniques, especially nonbiological ones, are based on the principle of microextrusion. Microextrusion-based systems usually consist of one or more pulley systems that can move along the x, y, and z axes; a temperature-controlled material processing and dispensing system; and a light (UV) source to illuminate the deposition area or activate the photoinitiator (Vurat 2021). Microextrusion bioprinting technology is based on printing ink by mechanical force or pneumatically (with gas or pressure). In addition to being compatible with high-viscosity materials, this method provides the advantage of printing with high cell density. It is low cost and allows easy printing. As the viscosity decreases, the increased pressure negatively affects cell viability (Akkuş et al. 2020; Hacıoglu et al. 2018). Material cross-linking strategies used in extrusion printing are generally classified into three categories: (1) chemical cross-linking, such as sodium alga acid and chitosan; (2) photo-cross-linking, such as GelMA; and (3) physical cross-linking, such as agarose (Du 2018).
9.3.5.3 Laser-Assisted 3D Bioprinting
Laser-assisted bioprinting, simply identified as laser-induced forward transfer, is a droplet-based system (LIFT). Laser-based 3D bioprinters (LTB), based on the principle of laser excitation, were developed primarily for transferring metals. However, peptides have been successfully applied to biological materials, such as deoxyribonucleic acid (DNA) and cells in later times. Although LTB is less common than inkjet or microextrusion-based bioprinting, it is used increasingly for tissue and organ engineering applications. A typical LTB contains a laser-energy-absorbing layer, a pulsed laser beam, and a focusing system (Murphy and Atala 2014). Further, many factors influence the resolution of the structures produced in LTB, including laser fluence (transmitted energy per unit area), the surface tension of the bioink, the air gap between the slide and the substrate, and the viscosity of the biological substance (Yilmaz et al. 2019; Vurat 2021).
In LTB-based 3D bioprinters, the principle of operation entails applying a high-energy pulsed laser to a donor slide coated with the bioink to be printed to ensure the local spraying of small droplets. The laser light is mainly focused on a transparent laser substrate (such as glass or quartz), which is coated with a thin metal layer, such as gold or titanium, that absorbs light energy and promotes bioink transfer. Pressure is created at this step, and a small droplet is pushed toward the lower platform. Cells are printed using a laser beam, which vibrates at controlled speeds in laser-assisted bioprinting (Noh et al. 2017). Unlike inkjet bioprinting, this method can print materials with various viscosities. Since there is no nozzle in this method, there is no possibility of nozzle blockage, which is one of the problems encountered in other techniques (Akkuş et al. 2020). As a result, the viscosity on a broad scale, such as 1 to 300 MPa/s is suitable for printing biomaterials with their values (Vurat 2021; Murphy and Atala 2014). Moreover, the systems can also print bioinks with a cell density of 108 cells/mL at high resolutions and speeds of up to 1.6 mm/s using a laser pulse repetition rate of 5 kHz (Vurat 2021). The disadvantages of this method are that it is quite expensive and the gelling speed must be high for high resolution (Akkuş et al. 2020).
9.3.5.4 Stereolithography (SLA)
To develop 3D shapes from computer-aided design (CAD) data, a stereolithography machine (SLA-250; 3D Systems, Valencia, CA) was developed in the early 1980s. Nowadays, many 3D printers and current bioprinters accept STL files as input. Using the 3D Systems software, this file is first examined and, if necessary, modified. The device utilizes a moving helium-cadmium (HeCd) laser to produce a 250 μm UV light spot on top of the polymer vat. An optical scanning system is applied to manage the movement of this spot. The laser is permitted to finish 8–10 tracks per layer with an intensity of 14–16 mW/cm2 at a wavelength of 365 nm, which allows the polymerization of its solution (Dhariwala et al. 2004; Yilmaz et al. 2019). The system’s main components are a reservoir filled with a photosensitive polymer solution or resin, an x-y-axis controlled laser, and a fabrication stage with z-axis control. In summary, stereolithography is a laser-assisted production that photopolymerizes the surface of a photosensitive polymer bath using an ultraviolet (UV) laser (Yilmaz et al. 2019).
9.4 Transition from 3D Printing to 4D Printing
Four-dimensional bioprinting is a cutting-edge additive processing technique that has the inherent potential of manufacturing de novo living tissue structures that can be designed to alter different mechanical properties (Esworthy et al. 2019). To design a range of biological constructs, including bone, blood vessels, liver, and also heart tissue, many 3D bioprinting techniques are used. But, 3D bioprinting has a key disadvantage in that it just assesses the starting status a printed object and regards it to be artificial and immobile. Natural restoration entails complex 3D structures, microarchitectures, extracellular matrix compositions, and the formation of tissue with specific features obtained due to variations in tissue orientation. The majority of orientational formation is attributed to built-in strategies that reply to inherent stimuli so that 3D bioprinting cannot simulate (Wan et al. 2020; Arslan-Yildiz et al. 2016; Yu et al. 2019; Cui et al. 2016).
The first four-dimensional (4D) printing, capability of multi-material prints with over time, was developed at the Massachusetts Institute of Technology (MIT) in 2014 (Tibbits 2014). The technique has rapidly been practiced in the tissue engineering field, and the theory of time can be incorporated as the fourth dimension within 3D bioprinting technology, which led to the invention of 4D bioprinting. Four-dimensional bioprinting can be utilized to produce numerous 3D designed biologically active structures having the capability of robust orientational changes to adapt to new favored stimulation over time by using stimuli-responsive materials, describing the drawbacks of 3D bioprinting (Wan et al. 2020; Gao et al. 2016; Li et al. 2016a, b). The 4D-printed structures can alter over time in response to different stimuli and adjust to the native niches of fault fields, opening up new ways for tissue engineering, especially bone. To identify existing problems in bone tissue engineering, a sequence of accelerated 4D approaches has been suggested. In bone tissue engineering, shape recovery polymers that respond to different stimuli have been extensively researched as potential injectable hydrogels and appropriate scaffolds (Saravanan et al. 2019; Senatov et al. 2016; Graham et al. 2019; Wan et al. 2020).
The shape-conversion capability of 4D-printed bone tissue structures could satisfy the requirement for individualized bone healing, especially in the context of random bone fractures. The tensile performance of 4D-printed structures can also be regulated via a conditioned cross-linking of stimuli-responsive components (Wan et al. 2020; Suo et al. 2018). In bone tissue engineering, different cells, growth factors, or inorganic nanoparticles (hydroxyapatite and bioactive glass cement, such as calcium phosphate) can serve as support, and a heat-sensitive polysaccharide-based hydrogel that can be injected has been improved. Hydroxypropyl guar-graft-poly (N-vinylcaprolactam), hydroxybutyl chitosan, hydroxypropyl methylcellulose, such that the modified bio-based polymers, have a lower critical solution temperature among optimal room temperature and room temperature and can return into a gel state at skin temperature. Poly(N-isopropylacrylamide) (pNIPAM) (a conventional thermoresponsive material) has been combined with hyaluronic acid and chitosan to construct an injectable hydrogel for bone healing (Wan et al. 2020; Yang et al. 2014; Chen et al. 2013). The mechanical properties of injectable hydrogels were enhanced by the addition of mineral components like nano-hydroxyapatite, bioactive glass, and tricalcium phosphate. Inorganic-organic injectable hydrogels have appropriate rheological and in vivo properties and enhanced alkaline enzymatic activity and calcium formation in osteoblast cells for support (Wan et al. 2020; Azevedo et al. 2014; Dessi et al. 2013). PLA/hydroxyapatite porous scaffolds with increased rates of shape recovery potential could be employed as self-fitting implantable devices to restore minor bone flaws.
Renewable bio-smart scaffolds have positive shape memory effects and shape recovery at body temperature and they have has been prepared by Miao et al. (2014). In the study, PCL and cross-linkers containing predetermined amounts of castor oil were used. Meanwhile, the researchers utilized 3D laser printing to produce a biomaterial temperature-responsive shape-memory scaffold made of epoxidized acrylate materials based on renewable soybean oil. The produced biomaterials showed good mechanical strength, shape-memory effect, and biodegradable properties (Wan et al. 2020). Magneto-responsive polymer structures are polymer networks that have been physically or chemically modified with magnetic nanoparticles (MNP) made of nickel (Ni), cobalt (Co), and iron (Fe), and/or their oxides, as well. Magneto-responsive materials’ possibilities in the biomedical field have been indicated in a variety of specific target pharmaceutical applications, where they provide minimally intrusive, regionally efficient, and controlled treatment activity. In this regard, iron(III)oxide (Fe3O4) nanoparticles involving mesoporous bioactive glass/poly(Ɛ-caprolactone (Fe3O4/MBG/PCL) are examples of 3D-printed polymeric magneto-responsive structures used in tissue engineering applications (Zhang et al. 2014). In addition, PCL/iron-doped hydroxyapatite (PCL/FeHA) nanocomposite scaffolds and iron(III)oxide/poly(ethylene glycol diacrylate) (PEGDA) magneto scaffolds can also be given as examples (Tamay et al. 2019; D’Amora et al. 2017; De Santis et al. 2015).
Polymers of alkaline monomers act as cationic polymers in pH-responsive systems at acidic conditions, while polymers of acidic monomers act as anionic polymers at alkaline conditions. Synthetic pH-responsive polymers that are biocompatible and biodegradable involve poly(histidine) (PHIS), poly(acrylic acid) (PAA), poly(l-glutamic acid) (PGA), and poly(aspartic acid) (PASA), whereas natural pH-responsive polymers involve dextran, hyaluronic acid, alginic acid, chitosan, and gelatin (Tamay et al. 2019; Dutta and Cohn 2017; Kocak et al. 2017). Humidity responsiveness is a natural event with countless examples. Systems made of these substances can convert moisture sorption or desorption into driving forces for mobility. Some humidity-responsive materials that have been investigated include poly(ethylene glycol) diacrylate (PEGDA) cellulose (Mulakkal et al. 2018) and polyurethane copolymers (Tamay et al. 2019). A study with GelMA/alginate-based and poly (dopamine) (PDA)/alginate-based bioinks to create cell-laden scaffolds that change shape in response to near-infrared (NIR) stimuli was performed (Fig. 9.11). The overview of publications related to 3D and 4D between 2008–2019 is shown by years in Fig. 9.12.
Four-dimensional PED-cell-laden bilayered scaffolds, which transformed into saddle-like architecture upon NIR stimulation. The scaffolds were fabricated through cell-laden GelMA/alginate-based and PDA/alginate-based layers, and PDA/alginate instigated a shape morphing effect upon NIR stimulus (Luo et al. 2019). (Adapted with permission) (Arif et al. 2022)
Overview of current publications on 4D bioprinting. (a) The search strategy for viewing current publications on 4D bioprinting on PubMed, MEDLINE, and Web of Science databases (until 30 September 2019). (b) Statistics on the number of publications in recent years (Wan et al. 2020)
9.5 Challenges, Future Directions, and Conclusions
Bioprinting is still in its early stages, but there have been some notable successes in the formation of transplanted conceptual structures for a wide range of tissues. One of the most challenging aspects of 3D bioprinting is developing bioinks that are appropriate for every type of tissue and have adequate physiological, biological, and also mechanical features. The advancement and engineering of novel bioinks or bio-derived material compositions continue to be significant areas of concern and research. Further studies should be performed in developing new matrices and designs to assess and monitor the properties and processes of various bioink materials for this purpose. Bioprinting endeavors toward improved resolution, speed, and biocompatibility. Bioprinting has become popular the variety of suitable materials and methods for material accumulation with higher precision (Seyedmahmoud et al. 2020; Leberfinger et al. 2017). Vascularization is another important limitation in tissue engineering and bioprinting 3D tissues with proper functionalities. The presence of proper vascularization in bioprinted structures is essential for the long-term functionality of 3D-bioprinted tissues. Cells could die of hypoxia and exhibit stagnant growth attributable to waste and contaminant formation if sufficient cellular perfusion is not provided. The ability to effectively build a multiscale perfused vascular network and then promote its vascularization via mechanical or chemical activation is the foundation for biofabricating quite bulky tissues (Gu et al. 2019; Seyedmahmoud et al. 2020). Classical 3D bioprinting systems have mainly been used to develop, engineer 3D bioprinted structures in vitro pre—and implantation of the structure into the body. However, in vitro bioprinting methodologies could confront some logistical problems in terms of clinical applicability, such as the following: (1) 3D bioprinted structures are frequently sensitive, and inner micro-features could be damaged throughout transport from the fabrication condition to the operating condition; (2) extreme sanitized condition is needed; and (3) the bioprinted structure must be modified and trimmed before being implanted. This last problem exists when the configuration of the bioprinted structure differs from the real size of the defect due to the limited resolution ability of the CT and MRI scans used to develop the structure (Seyedmahmoud et al. 2020; Campbell and Weiss 2007; Li et al. 2015). Over the past decades, substantial development has been made in adjusting 3D bioprinting (Osidak et al. 2020). A comprehensive understanding of the effects of system parameters, bioink properties, and cellular structures on printing results offers a significant aid for the creation of new therapeutic bioinks (Ng et al. 2017; Chua et al. 2021). Despite considerable advances, bioprinting has many major challenges, such as the flexibility and function facilitates of printed biomaterials, and the ideal cell sources for innervation, vascularization, and development of printable structures. Materials with cell compatibility and appropriate mechanical properties, such as suitable modifications, the utilization of reinforced biomaterials, and protein-based and other functional group conjugation, must be specifically chosen to enable cell seeding and growth. Decellularized ECM could also be a favorable bioprinting scaffold. Various perspectives on 3D bioprinting have benefits and drawbacks. To resolve the troubles of bioprinting tissues with different properties, bioprinting methods with various mechanisms must be integrated. Moreover, appropriate stem cells, basic or mature cells, must be seriously evaluated in bioprinting to deliver proper functioning of the printable tissue (Huang et al. 2017).
Even though 3D printing has been a hot topic for many years, bioprinting is much more recent, and this field is growing rapidly. The system shows the ability and flexibility to create a variety of living systems with limited or no negative effects. This process is adaptable for the fabrication of both vascular and vascular tissues with 2D and 3D structures for tissue engineering. Nonetheless, in vivo evaluations of the process are now in their early stages, with an incredible deficiency in biological and mechanical characteristics to incorporate between printable structures and native tissue. But nevertheless, owing to its fast accuracy and continuous repeatability, bioprinting has displayed numerous opportunities in pharmaceutical research and clinical trials (Huang et al. 2017). Despite all the difficulties, however, bioprinting has a significant impact on the industry. To overcome all of the obstacles in this strongly interdisciplinary discipline, it is required to hire specialists from diverse areas such as material and biological sciences, computer engineering, and pharmaceutics. The advancement of bioink-based material applications is changed stem cell transplantation, polymer science, and fast manufacturing capabilities (Hacıoglu et al. 2018). As a result, 3D bioprinting provides the potential of manufacturing organs and, eventually, resolves the emergency of organ donor shortfall for transplantation (Huang et al. 2017).
References
Abouna GM (2008) Organ shortage crisis: problems and possible solutions. In: Transplantation proceedings, vol 40, No. 1. Elsevier, pp 34–38
Aduba DC, Margaretta ED, Marnot AEC, Heifferon KV, Surbey WR, Chartrain NA, Whittington AR, Long TE, Williams CB (2019) Vat photopolymerization 3D printing of acid-cleavable PEG-methacrylate networks for biomaterial applications. Mater Today Commun 19:204–211
Ahmed TAE, Dare EV, Hincke M et al (2008) Fibrin: a versatile scaffold for tissue engineering applications. Tissue Eng B Rev 14(2):199–215. https://doi.org/10.1089/ten.teb.2007.0435
Ahn S, Lee H, Bonassar LJ, Kim G (2012) Cells (MC3T3-E1)-laden alginate scaffolds fabricated by a modified solid-freeform fabrication process supplemented with an aerosol spraying. Biomacromolecules 13:2997–3003
Akkuş HG, Günaydin BE, Ustundag CB (2020) DOKU MÜHENDİSLİĞİNDE 3 BOYUTLU BİYO-BASKI İÇİN BİYOFONKSİYONEL MÜREKKEPLER. Int J 3D Print Technol Dig Ind 4(3):285–294
Alcantar NA, Aydil ES, Israelachvili JN (2000) Polyethylene glycol–coated biocompatible surfaces. J Biomed Mater Res 51:343–351
Aldana AA, Valente F, Dilley R, Doyle B (2021) Development of 3D bioprinted GelMA-alginate hydrogels with tunable mechanical properties. Bioprinting 21:e00105
An J, Teoh JEM, Suntornnond R, Chua CK (2015) Design and 3D printing of scaffolds and tissues. Engineering 1(2):261–268
Andreassi A, Bilenchi R, Biagioli M, D’Aniello C (2005) Classification and pathophysiology of skin grafts. Clin Dermatol 23:332–337
Arif ZU, Khalid MY, Ahmed W, Arshad H (2022) A review on four-dimensional bioprinting in pursuit of advanced tissue engineering applications. Bioprinting 2022:e00203
Arkel RV, Amis A (2013) Basics of orthopaedic biomechanics. Orthop Trauma 27(2):67–75
Arslan-Yildiz A, El Assal R, Chen P, Guven S, Inci F, Demirci U (2016) Towards artificial tissue models: past, present, and future of 3D bioprinting. Biofabrication 8(1):014103
Aschenbrenner E et al (2013) Using the polymeric ouzo effect for the preparation of polysaccharide-based nanoparticles. Langmuir 29(28):8845–8855
Ashammakhi N, Kaarela O (2017) Three-dimensional bioprinting can help bone. J Craniofac Surg 00:1
Askari M, Naniz MA, Kouhi M, Saberi A, Zolfagharian A, Bodaghi M (2021) Recent progress in extrusion 3D bioprinting of hydrogel biomaterials for tissue regeneration: a comprehensive review with focus on advanced fabrication techniques. Biomater Sci 9(3):535–573
Aslam M, Kalyar MA, Raza ZA (2018) Polyvinyl alcohol: a review of research status and use of polyvinylalcohol based nanocomposites. Polym Eng Sci 58:2119–2132
Azevedo AS, Sa MJ, Fook MV, Neto PI, Sousa OB, Azevedo SS, Teixeira MW, Costa FS, Araujo AL (2014) Use of chitosan and beta-tricalcium phosphate, alone and in combination, for bone healing in rabbits. J Mater Sci Mater Med 25(2):481–486
Babensee JE, Anderson JM, McIntire LV, Mikos AG (1998) Host response to tissue engineered devices. Adv Drug Deliv Rev 33(1–2):111–139
Bedir T, Ulag S, Ustundag CB, Gunduz O (2020) 3D bioprinting applications in neural tissue engineering for spinal cord injury repair. Mater Sci Eng C 110:110741
Bee S-L, Hamid ZAA, Mariatti M, Yahaya BH, Lim K, Bee S-T, Sin LT (2018) Approaches to improve therapeutic efficacy of biodegradable PLA/PLGA microspheres: a review. Polym Rev 58:495–536
Bejoy AM, Makkithaya KN, Hunakunti BB, Hegde A, Krishnamurthy K, Sarkar A et al (2021) An insight on advances and applications of 3d bioprinting: a review. Bioprinting 24:e00176
Bhavsar MD, Amiji MM (2008) Development of novel biodegradablepolymeric nanoparticles-in-microsphere formulation for local plasmid DNA delivery in the gastrointestinal tract. AAPS PharmSciTech 9(1):288–294
Boyan BD, Hummert TW, Dean DD, Schwartz Z (1996) Role of material surfaces in regulating bone and cartilage cell response. Biomaterials 17(2):137–146
Bružauskaitė I, Bironaitė D, Bagdonas E, Bernotienė E (2016) Scaffolds and cells for tissue regeneration: different scaffold pore sizes-different cell effects. Cytotechnology 68(3):355–369
Campbell PG, Weiss LE (2007) Tissue engineering with the aid of inkjet printers. Expert Opin Biol Ther 7:1123–1127
Cavallo JA et al (2015) Remodeling characteristics and collagen distributions of biologic scaffold materials biopsied from postmastectomy breast reconstruction sites. Ann Plast Surg 75(1):74
Chae S, Cho DW (2022) Biomaterial-based 3D bioprinting strategy for orthopedic tissue engineering. Acta Biomater 156:4–20
Chan BP, Leong KW (2008) Scaffolding in tissue engineering: general approaches and tissue-specific considerations. Eur Spine J 17:S467–S479
Chang CC, Boland ED, Williams SK, Hoying JB (2011) Direct-write bioprinting three-dimensional biohybrid systems for future regenerative therapies. J Biomed Mater Res B Appl Biomater 98:160–170
Chartrain NA, Gilchrist KH, Ho VB, Klarmann GJ (2022) 3D bioprinting for the repair of articular cartilage and osteochondral tissue. Bioprinting 2022:e00239
Chen XL, Shi QN (2013) Research on sol-gel transition process of gelatin. In: Advanced materials research, vol 683. Trans Tech Publications Ltd., pp 474–478
Chen JP, Tsai MJ, Liao HT (2013) Incorporation of biphasic calcium phosphate microparticles in injectable thermoresponsive hydrogel modulates bone cell proliferation and differentiation. Colloids Surf B Biointerfaces 110:120–129
Chen F-M, Liu X, Polym P, ve Author, S. (2016) Advancing biomaterials of human origin for tissue engineering HHS Public Access Author manuscript. Prog Polym Sci 53:86–168. https://doi.org/10.1016/j.progpolymsci.2015.02.004
Cheng YL, Chen F (2017) Preparation and characterization of photocured poly(epsilon-caprolactone)diacrylate/poly(ethylene glycol) diacrylate/chitosan for photopolymerization-type 3D printing tissue engineering scaffold application. Mater Sci Eng C Mater Biol Appl 81:66–73
Chiou BS, AvenaBustillos RJ, Bechtel PJ et al (2008) Cold water fish gelatin films: effects of cross-linking on thermal, mechanical, barrier, and biodegradation properties. Eur Polym J 44:3748–3753
Chowdhury SR, Lokanathan Y, Xian LJ, Busra FM, Yazid MD, Sulaiman N et al (2020) 3D printed bioscaffolds for developing tissue-engineered constructs. In: Design and manufacturing. IntechOpen
Chua CK, Yeong WY, Low HY, Tran T, Tan HW (2021) 3D printing and additive manufacturing of electronics: principles and applications
Church D, Elsayed S, Reid O, Winston B, Lindsay R (2006) Burn wound infections. Clin Microbiol Rev 19(2):403–434
Colton CK (1995) Implantable biohybrid artificial organs. Cell Transplant 4(4):415–436
Cornelissen DJ, Faulkner-Jones A, Shu W (2017) Current developments in 3D bioprinting for tissue engineering. Curr Opin Biomed Eng 2:76–82
Cubo N, Garcia M, Cañizo JF, Velasco D, Jorcano JL (2017) 3D bioprinting of functional human skin: production and in vivo analysis. Biofabrication 9:015006
Cui X, Boland T (2009) Human microvasculature fabrication using thermal inkjet printing technology. Biomaterials 30:6221–6227
Cui X et al (2012a) Direct human cartilage repair using three-dimensional bioprinting technology. Tissue Eng A 18:1304–1312
Cui X, Boland T, D’Lima DD, Lotz MK (2012b) Thermal inkjet printing in tissue engineering and regenerative medicine. Recent Pat Drug Deliv Formul 6:149–155
Cui H, Nowicki M, Fisher JP, Zhang LG (2016) 3D Bioprinting for organ regeneration. Adv Healthc Mater 6(1):1601118
D’Amora U, Russo T, Gloria A, Rivieccio V, D’Antò V, Negri G et al (2017) 3D additive-manufactured nanocomposite magnetic scaffolds: effect of the application mode of a time-dependent magnetic field on hMSCs behavior. Bioact Mater 2:138–145
Das S, Pati F, Chameettachal S, Pahwa S, Ray AR, Dhara S, Ghosh S (2013) Enhanced redifferentiation of chondrocytes on microperiodic silk/gelatin scaffolds: toward tailor-made tissue engineering. Biomacromolecules 14:311–321
Dávila JL, Freitas MS, InforcattiNeto P, Silveira ZC, Silva JVL, d’Ávila MA (2016) Fabrication of PCL/β-TCP scaffolds by 3D mini-screw extrusion printing. J Appl Polym Sci 133(15):43031. 9 pp
De Santis R, D’Amora U, Russo T, Ronca A, Gloria A, Ambrosio L (2015) 3D fibre deposition and stereolithography techniques for the design of multifunctional nanocomposite magnetic scaffolds. J Mater Sci Mater Med 26:250
DeLustro F, Condell RA, Nguyen MA, McPherson JM (1986) A comparative study of the biologic and immunologic response to medical devices derived from dermal collagen. J Biomed Mater Res 20(1):109–120
Deng M, Tan J, Hu C, Hou T, Peng W, Liu J, Yu B, Dai Q, Zhou J, Yang Y et al (2020) Modification of PLGA scaffold by MSC-derived extracellular matrix combats macrophage inflammation to initiate bone regeneration via TGF-beta-induced protein. Adv Healthc Mater 9:e2000353
Derakhshanfar S, Mbeleck R, Xu K, Zhang X, Zhong W, Xing M (2018) 3D bioprinting for biomedical devices and tissue engineering: a review of recent trends and advances. Bioactive Mater 3(2):144–156
Dessi M, Borzacchiello A, Mohamed TH, Abdel-Fattah WI, Ambrosio L (2013) Novel biomimetic thermosensitive beta-tricalcium phosphate/chitosan-based hydrogels for bone tissue engineering. J Biomed Mater Res A 101(10):2984–2993
Dhandayuthapani B, Yoshida Y, Maekawa T, Kumar DS (2011) Polymeric scaffolds in tissue engineering application: a review. Int J Polym Sci 19:290602
Dhariwala B, Hunt E, Boland T (2004) Rapid prototyping of tissue-engineering constructs, using photopolymerizable hydrogels and stereolithography. Tissue Eng 10:1316–1322
Di Luca A, Ostrowska B, Lorenzo-Moldero I, Lepedda A, Swieszkowski W, Van Blitterswijk C, Moroni L (2016) Gradients in pore size enhance the osteogenic differentiation of human mesenchymal stromal cells in three dimensional scaffolds. Sci Rep 6(1):22898
Diamantides N, Dugopolski C, Blahut E, Kennedy S, Bonassar LJ (2019) High density cell seeding affects the rheology and printability of collagen bioinks. Biofabrication 11:045016
Ding YW, Zhang XW, Mi CH, Qi XY, Zhou J, Wei DX (2022) Recent advances in hyaluronic acid-based hydrogels for 3D bioprinting in tissue engineering applications. Smart Mater Med 14(4):839
Du X (2018) 3D bio-printing review. In: IOP conference series: materials science and engineering, vol 301, no 1, p 012023. IOP Publishing
Dutta S, Cohn D (2017) Temperature and pH responsive 3D printed scaffolds. J Mater Chem B 5:9514–9521
Esworthy TJ, Miao S, Lee SJ, Zhou X, Cui H, Zuo YY, Zhang LG (2019) Advanced 4D-bioprinting technologies for brain tissue modeling and study. Int J Smart Nano Mater 10(3):177–204
Falcone SJ, Palmeri D, Berg RA (2006) Biomedical applications of hyaluronic acid. ACS Publications, pp 2006–2014
Fedorovich NE, De Wijn JR, Verbout AJ, Alblas J, Dhert WJ (2008) Three-dimensional fiber deposition of cell-laden, viable, patterned constructs for bone tissue printing. Tissue Eng A 14:127–133
Fontes AB, Marcomini RF (2020) 3D bioprinting: a review of materials, processes and bioink properties. J Eng Exact Sci 6(5):0617–0639
Gao G et al (2014) Bioactive nanoparticles stimulate bone tissue formation in bioprinted three-dimensional scaffold and human mesenchymal stem cells. Biotechnol J 9:1304–1311
Gao B, Yang Q, Zhao X, Jin G, Ma Y, Xu F (2016) 4D bioprinting for biomedical applications. Trends Biotechnol 158(9):746–756
Gentile P, Chiono V, Carmagnola I, Hatton PV (2014) An overview of poly(lactic-co-glycolic) acid (PLGA)-based biomaterials for bone tissue engineering. Int J Mol Sci 15(3):3640–3659
Gholami P, Ahmadi-Pajouh MA, Abolftahi N, Hamarneh G, Kayvanrad M (2017) Segmentation and measurement of chronic wounds for bioprinting. IEEE J Biomed Health Inform 22(4):1269–1277
Graham S, Marina PF, Blencowe A (2019) Thermoresponsive polysaccharides and their thermoreversible physical hydrogel networks. Carbohydr Polym 207:143–159
Gruene M et al (2010) Laser printing of stem cells for biofabrication of scaffold-free autologous grafts. Tissue Eng C Methods 17:79–87
Gu BK, Park SJ, Kim MS, Kang CM, Kim JI, Kim CH (2013) Fabrication of sonicated chitosan nanofiber mat with enlarged porosity for use as hemostatic materials. Carbohy Polym 97:65–73
Gu BK, Choi DJ, Park SJ, Kim YJ, Kim CH (2018) 3D bioprinting technologies for tissue engineering applications. Adv Exp Med Biol 1078:15–28
Gu Z, Fu J, Lin H, He Y (2019) Development of 3D bioprinting: from printing methods to biomedical applications. Asian J Pharm Sci 15(5):529–557
Guillemot F, Souquet S, Lopez M et al (2010) High-throughput laser printing of cells and biomaterials for tissue engineering. Acta Biomater 6(7):2494–2500
Guvendiren M, Molde J, Soares RMD, Kohn J (2016) Designing bio-materials for 3D printing. ACS Biomater Sci Eng 2:1679–1693
Hacıoglu A, Yılmazer H, Ustundag CB (2018) 3D printing for tissue engineering applications. Politeknik Dergisi 21(1):221–227. https://doi.org/10.2339/politeknik.389596
Hahn MS, Teply BA, Stevens MM, Zeitels SM, Langer R (2006) Collagen composite hydrogels for vocal fold lamina propria restoration. Biomaterials 27(7):1104–1109
Hajiali F, Tajbakhsh S, Shojaei A (2018) Fabrication and properties of polycaprolactone composites containing calcium phosphate-based ceramics and bioactive glasses in bone tissue engineering: a review. Polym Rev 58(1):164–207
Harriger MD, Supp AP, Warden GD, Boyce ST (1997) Glutaraldehyde crosslinking of collagen substrates inhibits degradation in skin substitutes grafted to athymic mice. J Biomed Mater Res 35:137–145
Hockaday LA, Kang KH, Colangelo NW, Cheung PYC, Duan B, Malone E, Wu J, Girardi LN, Bonassar LJ, Lipson H, Chu CC, Butcher JT (2012) Rapid 3D printing of anatomically accurate and mechanically heterogeneous aortic valve hydrogel scaffolds. Biofabrication 4(3):005–035
Hospodiuk M, Dey M, Sosnoski D, Ozbolat IT (2017) The bioink: a comprehensive review on bioprintable materials. Biotechnol Adv 35:217–239
Hsieh F-Y et al (2015) 3D bioprinting of neural stem cell-laden thermoresponsive biodegradable polyurethane hydrogel and potential in central nervous system repair. Biomaterials 71:48–57
Huang J, Mao Y, Millis JM (2008) Government policy and organ transplantation in China. Lancet 372(9654):1937–1938
Huang Y, Zhang XF, Gao G, Yonezawa T, Cui X (2017) 3D bioprinting and the current applications in tissue engineering. Biotechnol J 12(8):1600734
Huang YH, Jakus AE, Jordan SW, Dumanian Z, Parker K, Zhao L, Patel PK, Shah RN (2019) Three-dimensionally printed hyperelastic bone scaffolds accelerate bone regeneration in critical-size calvarial bone defects. Plast Reconstr Surg 143:1397–1407
Hull CW (1986) U.S. Patent No. 4,575,330. U.S. Patent and Trademark Office, Washington, DC
Hutmacher DW (2000) Scaffolds in tissue engineering bone and cartilage. In: The biomaterials: Silver Jubilee Compendium, vol 21. https://doi.org/10.1016/B978-008045154-1.50021-6
Inzana J, Olvera D, Fuller SM, Kelly JP, Graeve O, Schwarz EM, Kates SL, Awad H (2014) 3D printing of composite calcium phosphate and collagen scaffolds for bone regeneration. Biomaterials 35(13):4026–4034
Iordache F (2019) Bioprinted scaffolds. In: Materials for biomedical engineering. Elsevier, pp 35–60
Izbudak B (2021) Osteokondral hasarların onarımına yönelik 3B-biyoyazıcı ile çift-tabakalı nanohibrit doku iskelelerinin geliştirilmesi. Master’s Thesis, İstinye Üniversitesi/Sağlık Bilimleri Enstitüsü
Jakus AE, Rutz AL, Shah RN et al (2016a) Advancing the field of 3D biomaterial printing. Biomed Mater (Bristol) 11(1):1–11
Jakus AE, Rutz AL, Jordan SW, Kannan A, Mitchell SM, Yun C, Koube KD, Yoo SC, Whiteley HE, Richter CP et al (2016b) Hyperelastic “bone”: a highly versatile, growth factor-free, osteoregenerative, scalable, and surgically friendly biomaterial. Sci Transl Med 8:358ra127
Jana S, Lerman A (2015) Bioprinting a cardiac valve. Biotechnol Adv 33(8):1503–1521
Jean J, Garcia-Perez ME, Pouliot R (2011) Bioengineered skin: the self-assembly approach. J Tissue Sci Eng S5:001
Jessop ZM, Al-Sabah A, Gardiner MD, Combellack E, Hawkins K, Whitaker IS (2017) 3D bioprinting for reconstructive surgery: principles, applications and challenges. J Plast Reconstr Aesthet Surg 70(9):1155–1170
Jose RR, Rodriguez MJ, Dixon TA, Omenetto F, Kaplan DL (2016) Evolution of bioinks and additive manufacturing technologies for 3D bioprinting. ACS Biomater Sci Eng 2(10):1662–1678
Kakarla AB, Turek I, Kong C, Irving H (2022) Printable gelatin, alginate and boron nitride nanotubes hydrogel-based ink for 3D bioprinting and tissue engineering applications. Mater Des 213:110362
Karageorgiou V, Kaplan D (2005) Porosity of 3D biomaterial scaffolds andosteogenesis. Biomaterials 26(27):5474–5491
Katti DS, Lakshmi S, Langer R, Laurencin CT (2002) Toxicity, biodegradation and elimination of polyanhydrides. Adv Drug Deliv Rev 54(7):933–961
Kim JE, Kim SH, Jung Y (2016a) Current status of three-dimensional printing inks for soft tissue regeneration. Tissue Eng Regen Med 13(6):636–646
Kim YB, Lee H, Kim GH (2016b) Strategy to achieve highly porous/biocompatible macroscale cell blocks, using a collagen/genipin-bioink and an optimal 3D printing process. ACS Appl Mater Interfaces 8:32230–32240
Kim BS, Gao G, Kim JY, Cho D (2019) 3D cell printing of perfusable vascularized human skin equivalent composed of epidermis, dermis, and hypodermis for better structural recapitulation of native skin. Adv Healthc Mater 8:1801019
Kocak G, Tuncer C, Butun V (2017) pH-responsive polymers. Polym Chem 8:144–176
Koch L, Deiwick A, Schlie S, Michael S, Gruene M, Coger V, Zychlinski D, Schambach A, Reimers K, Vogt PM, Chichkov B (2012) Skin tissue generation by laser cell printing. Biotechnol Bioeng 109:1855–1863
Kruth JP, Leu MC, Nakagawa T (1998) Progress in additive manufacturing and rapid prototyping. ClRP Ann 47(2):525–540
Kuijpers AJ, van Wachem PB, van Luyn MJ et al (2015) In vivo compatibility and degradation of crosslinked gelatin gels incorporated in knitted Dacron. J Biomed Mater Res 51(1):136–145
Langer R, Vacanti JP (1993) Tissue engineering. Science 260:920–926
Leberfinger AN, Ravnic DJ, Dhawan A, Ozbolat IT (2017) Concise review: Bioprinting of stem cells for transplantable tissue fabrication. Stem Cells Transl Med 6:1940–1948
Lee V et al (2013) Design and fabrication of human skin by three-dimensional bioprinting. Tissue Eng C Methods 20:473–484
Lee J, Hong J, Kim W, Kim GH (2020) Bone-derived dECM/alginate bioink for fabricating a 3D cell-laden mesh structure for bone tissue engineering. Carbohydr Polym 250:116914
Li Q, Ma L, Gao C (2015) Biomaterials for in situ tissue regeneration: development and perspectives. J Mater Chem B 3:8921–8938
Li H, Liu S, Li L (2016a) Rheological study on 3D printability of alginate hydrogel and effect of graphene oxide. Int J Bioprint 2(2):54–66
Li YC, Zhang YS, Akpek A, Shin SR, Khademhosseini A (2016b) 4D bioprinting: the next-generation technology for biofabrication enabled by stimuli-responsive materials. Biofabrication 9(1):012001
Liu X, Won Y, Ma PX (2005) Surface modification of interconnected porous scaffolds. J Biomed Mater Res A 74(1):84–91
Luo Y, Lin X, Chen B, Wei X (2019) Cell-laden four-dimensional bioprinting using near-infrared-triggered shape-morphing alginate/polydopamine bioinks. Biofabrication 11(4):045019
Ma H, Xue L (2015) Carbon nanotubes reinforced poly(L-lactide) scaffolds fabricated by thermally induced phase separation. Nanotechnology 26:025701
Mandrycky C, Wang Z, Kim K, Kim DH (2016) 3D bioprinting for engineering complex tissues. Biotechnol Adv 34:422–434
Marin E, Rojas J, Ciro Y (2014) A review of polyvinyl alcohol derivatives: promising materials for pharmaceutical and biomedical applications. Afr J Pharm Pharmacol 8:674–684
Medina-Esquivel R, Freile-Pelegrin Y, Quintana-Owen P, Yáñez-Limón JM, Alvarado-Gil JJ (2008) Measurement of the sol–gel transition temperature in agar. Int J Thermophys 29:2036–2045
Metcalfe AD, Ferguson MW (2007) Tissue engineering of replacement skin: the crossroads of biomaterials, wound healing, embryonic development, stem cells and regeneration. J R Soc Interface 4(14):413–437
Miao S, Wang P, Su Z, Zhang S (2014) Vegetable-oil-based polymers as future polymeric biomaterials. Acta Biomater 10(4):1692–1704
Miao S, Zhu W, Castro N, Leng JS, Zhang LG (2016) 4D printing hierarchy scaffolds with highly biocompatible smart polymers for tissue engineering applications. Tissue Eng C 22(10):952–963
Michael S, Sorg H, Peck CT, Koch L, Deiwick A, Chichkov B, Vogt PM, Reimers K (2013) Tissue engineered skin substitutes created by laser-assisted bioprinting form skin-like structures in the dorsal skinfold chamber in mice. PLoS One 8(3):e57741
Mironov V, Kasyanov V, Drake C, Markwald RR (2008) Organ printing: promises and challenges. Regen Med 3:93
Mobaraki M, Ghaffari M, Yazdanpanah A, Luo Y, Mills DK (2020) Bioinks and bioprinting: a focused review. Bioprinting 18:00080
Mota C, Puppi D, Chiellini F, Chiellini E (2015) Additive manufacturing techniques for the production of tissue engineering constructs. J Tissue Eng Regen Med 9:174–190
Mukherjee P, Rani A, Saravanan P (2019) Polymeric materials for 3D bioprinting. In: Ahmad N, Gopinath R, Dutta R (eds) 3D printing technology in nanomedicine, pp 63–81
Mulakkal MC, Trask RS, Ting VP, Seddon AM (2018) Responsive cellulose-hydrogel composite ink for 4D printing. Mater Des 160:108–118
Munaz A, Vadivelu RK, John JS, Barton M, Kamble H, Nguyen NT (2016) Three-dimensional printing of biological matters. J Sci Adv Mater Device 1(1):1–17
Murphy SV, Atala A (2014) 3D bioprinting of tissues and organs. Nat Biotechnol 32(8):773–785
Nair LS, Laurencin CT (2007) Biodegradable polymers as biomaterials. Prog Polym Sci (Oxford) 32(8–9):762–798
Ng WL, Wang S, Yeong WY, Naing MW (2016) Skin bioprinting: impending reality or fantasy. Trends Biotechnol 34:689–699
Ng WL, Lee JM, Yeong WY, Naing MW (2017) Microvalve-based bioprinting–process, bio-inks and applications. Biomater Sci 5(4):632–647
Ngo TB, Spearman BS, Hlavac N, Schmidt CE (2020) Three-dimensional bioprinted hyaluronic acid hydrogel test beds for assessing neural cell responses to competitive growth stimuli. ACS Biomater Sci Eng 6(12):6819–6830
Noh S, Myung N, Park M, Kim S, Zhang SU, Kang HW (2017) 3D bioprinting for tissue engineering. In: Kim BW (ed) Clinical regenerative medicine in urology. Springer, Singapore, pp 105–123
Oh SH, Kang SG, Kim ES, Cho SH, Lee JH (2003) Fabrication and characterization of hydrophilic poly(lactic-co-glycolic acid)/poly(vinyl alcohol) blend cell scaffolds by melt-molding particulate-leaching method. Biomaterials 24:4011–4021
Ong CS, Yesantharao P, Huang CY, Mattson G, Boktor J et al (2018) 3D bioprinting using stem cells. Pediatr Res 83:223–231
Osidak EO, Karalkin PA, Osidak MS, Parfenov VA, Sivogrivov DE, Pereira F, Gryadunova AA, Koudan EV, Khesuani YD, Capital Ka CVA et al (2019) Viscoll collagen solution as a novel bioink for direct 3D bioprinting. J Mater Sci Mater Med 30:31
Osidak EO, Kozhukhov VI, Osidak MS, Domogatsky SP (2020) Collagen as bioink for bioprinting: a comprehensive review. Int J Bioprinting 6(3)
Ozbolat IT (2016) 3D bioprinting: fundamentals, principles and applications. Elsevier, p s.356
Ozbolat IT, Chen H, Yu Y (2014) Development of “Multi-arm Bioprinter” for hybrid biofabrication of tissue engineering constructs. Robot Comput Integr Manuf 30(3):295–304
Ozbolat IT, Peng W, Ozbolat V (2016) Application areas of 3D bioprinting. Drug Discov Today 21(8):1257–1271
Parin FN, Terzioğlu P (2022) Electrospun porous biobased polymer mats for biomedical applications. In: Advanced functional porous materials: from macro to nano scale lengths, pp 539–586
Pekkanen AM, Mondschein RJ, Williams CB, Long TE (2017) 3D printing polymers with supramolecular functionality for biological, applications. Biomacromolecules 18(9):2669–2687
Peppas NA, Hilt JZ, Khademhosseini A, Langer R (2006) Hydrogels in biology and medicine: from molecular principles to bionanotechnology. Adv Mater 18:1345–1360
Pescosolido L, Schuurman W, Malda J, Matricardi P, Alhaique F, Coviello T et al (2011) Hyaluronic acid and dextran-based semi-IPN hydrogels as biomaterials for bioprinting. Biomacromolecules 12:1831–1838
Phillippi JA et al (2008) Microenvironments engineered by inkjet bioprinting spatially direct adult stem cells toward muscle- and bone-like subpopulations. Stem Cells 26:127–134
Poldervaart MT, Gremmels H, van Deventer K, Fledderus JO, Oner FC, Verhaar MC, Dhert WJ, Alblas J (2014) Prolonged presence of VEGF promotes vascularization in 3D bioprinted scaffolds with defined architecture. J Control Release 184:58–66
Powell HM, Boyce ST (2006) EDC cross-linking improves skin substitute strength and stability. Biomaterials 27:5821–5827
Ren X, Wang F, Chen C, Gong X, Yin L, Yang L (2016) Engineering zonal cartilage through bioprinting collagen type II hydrogel constructs with biomimetic chondrocyte density gradient. BMC Musculoskelet Disord 17:1–10
Sakai S, Hirose K, Taguchi K, Ogushi Y (2009) Injectable, in situ enzymatically gellable, gelatin derivative for drug delivery and tissue engineering. Biomaterials 30:3371–3377
Salah M, Tayebi L, Moharamzadeh K, Naini FB (2020) Three-dimensional bio-printing and bone tissue engineering: technical innovations and potential applications in maxillofacial reconstructive surgery. Maxillofac Plastic Reconstr Surg 42(1):1–9
Salgado CL, Sanchez EM, Zavaglia CA, Granja PL (2012) Biocompatibility and biodegradation of polycaprolactone-sebacic acid blended gels. J Biomed Mater Res A 100(1):243–251
Saravanan S, Vimalraj S, Thanikaivelan P, Banudevi S, Manivasagam G (2019) A review on injectable chitosan/beta glycerophosphate hydrogels for bone tissue regeneration. Int J Biol Macromol 121:38–54
Sarker MD, Naghieh S, McInnes AD, Ning L, Schreyer DJ, Chen X (2019) Bio-fabrication of peptide-modified alginate scaffolds: printability, mechanical stability and neurite outgrowth assessments. Bioprinting 14:e00045
Saroia J, Yanen W, Wei Q, Zhang K, Lu T, Zhang B (2018) A review on biocompatibility nature of hydrogels with 3D printing techniques, tissue engineering application and its future prospective. Bio-Design Manufacturing 1:265–279
Schacht K, Jungst T, Schweinlin M, Ewald A, Groll J, Scheibel T (2015) Biofabrication of cell-loaded 3D spidersilk constructs. Angew Chem Int Ed Engl 54:2816–2820
Senatov FS, Niaza KV, Zadorozhnyy MY, Maksimkin AV, Kaloshkin SD, Estrin YZ (2016) Mechanical properties and shape memory effect of 3D-printed PLA-based porous scaffolds. J Mech Behav Biomed Mater 57:139–148
Seyedmahmoud R, Mozetic P, Rainer A, Giannitelli SM, Basoli F, Trombetta M et al (2015) A primer of statistical methods for correlating parameters and properties of electrospun poly(l-lactide) scaffolds for tissue engineering—Part 2: Regression. J Biomed Mater Res A 103(1):103–114
Seyedmahmoud R, Messler MJ, Loboa EG (2020) 3D bioprinting technologies for tissue engineering: a mini review. HSOA J Stem Cells Res Dev Ther 6:046
Shafiee A, Atala A (2016) Printing technologies for medical applications. Trends Mol Med 22(3):254–265
Sharif M, George E, Shepstone L et al (1995) Serum hyaluronic acid level as a predictor of disease progression in osteoarthritis of the knee. Arthrit Rheumatol 38(6):760
Shen M, Wang L, Gao Y, Feng L, Xu C, Li S et al (2022) 3D bioprinting of in situ vascularized tissue engineered bone for repairing large segmental bone defects. Mater Today Bio 16:100382
Sheridan R (2009) Closure of the excised burn wound: autografts, semipermanent skin substitutes, and permanent skin substitutes. Clin Plast Surg 36:643
Singh RS, Saini GK (2008) Pullulan-hyperproducing color variant strain of Aureobasidium pullulans FB-1 newly isolated from phylloplane of Ficus sp. Bioresour Technol 99(9):3896–3899
Singh RS, Singh H, Saini GK (2009) Response surface optimization of the critical medium components for pullulan production by Aureobasidium pullulans FB-1. Appl Biochem Biotechnol 152:42–53
Skardal A, Mack D, Kapetanovic E, Atala A, Jackson JD, Yoo J, Soker S et al (2012) Bioprinted amniotic fluid-derived stem cells accelerate healing of large skin wounds. Stem Cells Transl Med 1:792–802
Slaughter BV, Khurshid SS, Fisher OZ, Khademhosseini A, Peppas NA (2009) Hydrogels in regenerative medicine. Adv Mater 21(32–33):3307–3329
Sophia Fox AJ, Bedi A, Rodeo SA (2009) The basic science of articular cartilage: structure, composition, and function. Sports Health 1:461–468
Sowjanya JA, Singh J, Mohita T, Sarvanan S, Moorthi A, Srinivasan N, Selvamurugan N (2013) Biocomposite scaffolds containing chitosan/alginate/nano-silica for bone tissue engineering. Colloids Surf B Biointerfaces 109:294–300
Suo H, Zhang D, Yin J, Qian J, Wu ZL, Fu J (2018) Interpenetrating polymer network hydrogels composed of chitosan and photocrosslinkable gelatin with enhanced mechanical properties for tissue engineering. Mater Sci Eng C Mater Biol Appl 92:612–620
Tamay DG, Dursun Usal T, Alagoz AS, Yucel D, Hasirci N, Hasirci V (2019) 3D and 4D printing of polymers for tissue engineering applications. Front Bioeng Biotechnol 7:164
Tan B, Gan S, Wang X, Liu W, Li X (2021) Applications of 3D bioprinting in tissue engineering: advantages, deficiencies, improvements, and future perspectives. J Mater Chem B 9(27):5385–5413
Tangsadthakun C, Kanokpanont S, Sanchavanakit N, Banaprasert T, Damrongsakkul S (2017) Properties of collagen/chitosan scaffolds for skin tissue engineering. J Metals Mater Miner 16(1):37–44
Tao H, Kaplan DL, Omenetto FG (2012) Silk materials–a road to sustainable high technology. Adv Mater 24:2824–2837
Taylor PM, Cass AE, Yacoub MH (2006) Extracellular matrix scaffolds for tissue engineering heart valves. Progr Pediatr Cardiol 21(2):219–225
Theus AS, Ning L, Hwang B, Gil C, Chen S, Wombwell A et al (2020) Bioprintability: physiomechanical and biological requirements of materials for 3d bioprinting processes. Polymers 12(10):2262
Thirumavalavan K, Manikkadan T, Dhanasekar R (2009) Pullulan production from coconut by-products by Aureobasidium pullulans. Afr J Biotechnol 8(2):254–258
Tibbits S (2014) 4D printing: multi-material shape change. Archit Des 84(1):116–121
Tirella A, Orsini A, Vozzi G, Ahluwalia A (2009) A phase diagram for microfabrication of geometrically controlled hydrogel scaffolds. Biofabrication 1:045002
Topuz M, Dikici B, Gavgali M, Yilmazer H (2018) A review on the hydrogels used in 3D bio-printing. Int J 3D Print Technol Dig Ind 2(2):68–75
Vega-Cázarez CA, Sánchez-Machado DI, López-Cervantes J (2018) Overview of electrospinned chitosan nanofiber composites for wound dressings. In: Chitin-chitosan-myriad functionalities in science and technology, pp 157–181
Vurat MT (2021) Üç-boyutlu Biyobasım için Yeni Kompozit Biyomürekkep Geliştirilmesi ve Karakterizasyonu. PhD Thesis, Ankara Üniversitesi/Fen Bilimleri Enstitüsü
Wan Z, Zhang P, Liu Y, Lv L, Zhou Y (2020) Four-dimensional bioprinting: current developments and applications in bone tissue engineering. Acta Biomater 101:26–42
Weadock KS, Miller EJ, Bellincampi LD, Zawadsky JP, Dunn MG (1995) Physical crosslinking of collagen fibers: comparison of ultraviolet irradiation and dehydrothermal treatment. J Biomed Mater Res 29:1373–1379
Wu Z, Li Q, Xie S, Shan X, Cai Z (2020) In vitro and in vivo biocompatibility evaluation of a 3D bioprinted gelatin-sodium alginate/rat Schwann-cell scaffold. Mater Sci Eng C Mater Biol Appl 109:110530
Xu T, Jin J, Gregory C, Hickman JJ, Boland T (2005) Inkjet printing of viable mammalian cells. Biomaterials 26:93–99
Yanagawa F, Sugiura S, Kanamori T (2016) Hydrogel microfabrication technology toward three dimensional tissue engineering. Regen Ther 3:45–57
Yang J, van Lith R, Baler K, Hoshi RA, Ameer GA (2014) A thermoresponsive biodegradable polymer with intrinsic antioxidant properties. Biomacromolecules 15(11):3942–3952
Ye WP, Du FS, Jin WH, Yang JY, Xu Y (1997) In vitro degradation of poly(caprolactone), poly(lactide) and their block copolymers: influence of composition, temperature and morphology. React Funct Polym 32(2):161–168
Yilmaz B, Tahmasebifar A, Baran ET (2019) Bioprinting technologies in tissue engineering. Curr Appl Pharm Biotechnol 171:279–319
You F, Eames BF, Chen X (2017) Application of extrusion-based hydrogel bioprinting for cartilage tissue engineering. Int J Mol Sci 18:8–14
Yu X, Tang X, Gohil SV, Laurencin CT (2015) Biomaterials for bone regenerative engineering. Adv Healthc Mater 4(9):1268–1285
Yu C, Ma X, Zhu W, Wang P, Miller KL, Stupin J, Koroleva-Maharajh A, Hairabedian A, Chen S (2019) Scanningless and continuous 3D bioprinting of human tissues with decellularized extracellular matrix. Biomaterials 194:1–13
Yu J, Park SA, Kim WD, Ha T, Xin YZ, Lee J, Lee D (2020) Current advances in 3D bioprinting technology and its applications for tissue engineering. Polymers 12(12):2958
Yüce Erarslan E (2021) Biyolojik Uygulamalarda Kullanılabilecek Polimerik Akıllı Malzemelerin Sentezi ve Karakterizasyonu PhD Thesis, İstanbul Üniversitesi/Lisansüstü Eğitim Enstitüsü
Zhang X, Zhang Y (2015) Tissue engineering applications of three-dimensional bioprinting. Cell Biochem Biophys 72:777–782
Zhang J, Zhao S, Zhu M, Zhu Y, Zhang Y, Liu Z et al (2014) 3D-printedmagnetic Fe3O4/MBG/PCL composite scaffolds with multifunctionality of bone regeneration, local anticancer drug delivery and hyperthermia. J Mater Chem B 2:7583–7595
Zhang J, Allardyce BJ, Rajkhowa R, Zhao Y, Dilley RJ, Redmond SL et al (2018) 3D printing of silk particle-reinforced chitosan hydrogel structures and their properties. ACS Biomater Sci Eng 4(8):3036–3046
Zhang J, Wehrle E, Adamek P, Paul GR, Qin XH, Rubert M, Muller R (2020) Optimization of mechanical stiffness and cell density of 3D bioprinted cell-laden scaffolds improves extracellular matrix mineralization and cellular organization for bone tissue engineering. Acta Biomater 114:307–322
Zhou Y, Fan Y, Chen Z, Yue Z, Wallace G (2021) Catechol functionalized ink system and thrombin-free fibrin gel for fabricating cellular constructs with mechanical support and inner micro channels. Biofabrication 14(1):015004
Zhu W, Ma X, Gou M, Mei D, Zhang K, Chen S (2016) 3D printing of functional biomaterials for tissue engineering. Curr Opin Biotechnol 40:103–112
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2023 The Author(s), under exclusive license to Springer Nature Singapore Pte Ltd.
About this chapter
Cite this chapter
Parın, F.N. (2023). 3D and 4D Bioprinting Technology for Tissue Engineering Applications. In: Sheikh, F.A., Majeed, S., Beigh, M.A. (eds) Interaction of Nanomaterials With Living Cells. Springer, Singapore. https://doi.org/10.1007/978-981-99-2119-5_9
Download citation
DOI: https://doi.org/10.1007/978-981-99-2119-5_9
Published:
Publisher Name: Springer, Singapore
Print ISBN: 978-981-99-2118-8
Online ISBN: 978-981-99-2119-5
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)