Abstract
Magnesium (Mg) alloys have great potential as materials for biodegradable implants and devices because of their excellent mechanical and biological properties; such as the similarity of their mechanical properties to cortical bone and their osteoconductivity. However, Mg alloys degrade rapidly in vivo, which reduces the local pH and can harm cells. Coatings and surface treatments can control the degradation rate of Mg alloys by limiting the diffusion of water and ions to the Mg surface. Coatings can also increase the osteoconductivity of the surface of Mg implants. Polymers and ceramics are frequently used as coating materials, and the processes of their deposition can further tailor the properties of coatings for their intended roles. The controlled degradation and osteoconductivity of Mg implants using coatings will lead to their replacement with natural tissue after they have fulfilled their function; which will avoid foreign body complications and prevent the need for implant removal surgeries.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
- Magnesium
- Coating
- Surface modification
- Degradation
- Biomedical implant
- Degradable metal
- Anodization
- Micro-arc oxidation
- Calcium phosphate
- Polymer
- Dip coating
- Spin coating
- Bioactive factor
1 Introduction
1.1 Magnesium and the Current Orthopedic Materials
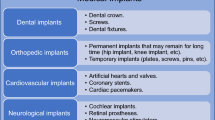
Coated magnesium (Mg) alloys possess many desirable properties that will enable them to supplement the current generation of orthopedic biomaterials. The most common orthopedic implants are generally made from non-degradable alloys such as titanium (Ti), stainless steel, and cobalt-chromium alloys. These alloys have extremely high mechanical strength and fracture toughness, enabling them to withstand the forces that moving bodies exert on them. They are also biocompatible and non-degradable. Orthopedic implants made from these non-degradable alloys have improved the quality of life for millions of patients for decades, and will likely continue to do so for many more years. However, applications that only require implants temporarily may be better served by Mg alloys.
1.2 There Is No Such Thing as Permanent Implants
Non-degradable implants are not permanent. Various phenomena will require their revisions; especially with younger and more active patients. A common challenge with non-degradable implants is encapsulation within fibrous tissue [1]. Encapsulation is the body’s response to foreign objects and impedes osteointegration, which is the formation of a direct bone/implant interface without non-bone tissue in-between. The long term success of orthopedic implants hinges upon their osteointegration [2]. Another challenge is the release of wear debris from biomaterials, which can stimulate immune responses and is a major cause for implant revision [3]. Around 5% of internal fixators become infected [4], which may necessitate removal of those implants [5]. Other reasons for removing implants are pain, swelling, and sub-cutaneous prominence [6]. Non-degradable implants have more opportunities to encounter complications because they reside in the body for long periods of time.
1.3 Why Use Biodegradable Implants?
Certain applications only require implants temporarily. Leaving implants in the body permanently might cause future complications [4], but surgical removal of implants always increases patient morbidity and medical costs [7]. The consequences of surgical removal of implants can include refracture of bone, nerve damage, and infection [6]. Due to these consequences there is still debate among physicians about when non-degradable implants should be surgically removed [7].
Biodegradable implants are a promising alternative that could perform their function for the desired time period, and then be replaced with new healthy tissue as they degrade. The new healthy tissue would no longer need the implant for support after a certain timeframe. This would prevent both the foreign body complications and the need for removal surgery that often accompany non-degradable implants.
Mg is one of the front-runners in the search for new biodegradable materials for implant applications. Much of the research is focused upon orthopedic implants such as screws [8,9,10]. Other diverse implant applications for Mg include: coronary stents [11], securing myocardial grafts [12], uretal stents [13], intestinal anastomosis rings [14], extraluminal tracheal stents [15], microclips for laryngeal microsurgery [16], and nerve guidance conduits [17]. The reasons for the interest in Mg for such diverse applications are its excellent mechanical and biological properties.
1.4 The Advantages of Magnesium
Many of the challenges with the established biomaterials arise because of the differences between their mechanical properties and natural tissue. The most common metallic biomaterials (e.g. Ti) have a much higher elastic modulus than bone, which causes stress shielding [18]. Ceramic biomaterials are brittle, making them vulnerable to breakage [19]. Many polymeric biomaterials have insufficient mechanical properties, limiting the support they provide in load bearing applications [20]. Mg alloys have the advantage of possessing mechanical properties similar to cortical bone [21, 22], which enables Mg to be used for load bearing applications while minimizing stress-shielding. Implants made from Mg alloys slowly lose mass and volume until they are gone from the body without the need for removal surgery (Table 1).
Mg also has many advantageous biological properties . Mg degradation products are non-toxic and rapidly cleared from the body [23]. Mg degradation products can also increase cell proliferation and osteogenic differentiation [24]. Mg is osteoconductive and improves bone growth on implants in vivo [25, 26]. Mg implants can have better osteointegration than Ti implants [27]. Another advantage of Mg implants is that some are not encapsulated [28, 29], although this is not always the case [30]. A Ca rich mineral phase is deposited upon Mg orthopedic implants after implantation [31], which helps increase mineral apposition rates of surrounding bone tissue [9, 32, 33]. Mg inhibits osteolysis induced by wear particles [34]. Mg ion release may prevent some forms of osteoporosis [35]. Mg can protect against bone cancer [36] and nerve damage [37]. Mg degradation can be bacteriocidal due to the increased pH [38, 39]; its bacteriocidal activities can be improved in alloys such as those containing silver (Ag) [40]. These desirable properties make Mg alloys attractive choices for orthopedic implant applications.
1.5 The Challenges of Magnesium
Despite the many advantages of Mg alloys, there are still challenges that must be resolved before the clinical translation of Mg based implants. Most of these challenges are the result of excessively rapid Mg degradation in vivo [10, 41], which causes undesirable physical and chemical changes. Rapid degradation of Mg implants reduces their mechanical properties too early and may lead to a catastrophic mechanical failure. Eroding Mg surfaces are unstable and may limit cell adhesion. Additionally, rapidly degrading surfaces recede from neighboring tissue, creating a gap that can impair tissue ingrowth [42].
Galvanic reactions cause Mg degradation [43,44,45]. Mg is almost always the anode in galvanic couples and forms a Mg hydroxide (Mg(OH)2) passivation layer at the surface of the alloy. The passivation layer acts as a barrier against electrolyte, which limits the rate of further Mg degradation reactions (Fig. 1a). The protection provided by the passivation layer is limited by its inherent porosity, looseness, and vulnerability to aggressive ions [46]. Aggressive ions such as chloride (Cl−) are common in body fluids and can convert the passivation layer into the much more soluble MgCl2, which is then dissolved [47,48,49]. Dissolution of the passivation layer enables further Mg degradation reactions to occur (Fig. 1b). The location where Mg is implanted in the body influences its degradation rate; Mg tends to degrade more quickly in the soft tissue or bone marrow than in cortical bone [2,3,4,5]. This can cause the thread and head of screws to dissolve faster than the shaft [9], and could help explain why degradation rates differ between in vivo and in vitro tests [50,51,52,53].
The dissolution of Mg alloys releases Mg ions, hydrogen gas (H2), and hydroxide ions (OH−) [47]. Mg ions have low toxicity and are rapidly excreted by the kidneys. Diffusion and fluid transport remove H2 from the implant site; but if Mg degradation is too rapid then H2 evolution may exceed the H2 clearance rate. Accumulation of H2 may form subcutaneous gas bubbles [9, 32], create a gap between implant and bone [54], and may also delaminate some coatings from Mg substrates [55]. The most frequently problematic degradation product is OH−, which can significantly increase the pH surrounding a Mg implant. The cytotoxicity exhibited by Mg alloy degradation is often caused by the alkaline pH and not the high Mg ion concentration [23]. Excessively rapid Mg degradation can also cause significant hemolysis (Table 2). Controlling the degradation rate of Mg will resolve many of these challenges.
The degradation rate of implants should be tailored to match the growth rate of bone tissue [56,57,58]. Excessively fast degradation rates can create a gap between implant and bone or lead to insufficient support or premature mechanical failure. Excessively slow degradation rates can lead the body forming an empty bone socket instead of replacing the implant with bone tissue [59, 60]. If the degradation rate and bioactivity are tightly controlled, the biodegradable implants will be replaced with ingrowing natural tissue as they degrade. As time passes, the role of supporting loading forces will be transferred from the implant to the tissue (Fig. 2). The transfer of the mechanical support role has profound implications upon bone remodeling processes, which can lead to healthier bone tissue. If the degradation rate is controlled, Mg screws can be clinically equivalent to Ti screws over the short term [22].
1.6 Coatings Can Address Many Challenges
Coatings and surface modifications can decouple Mg degradation rates from bulk Mg properties. The coated surfaces initially act as barriers protecting the underlying Mg substrates, but coating degradation gradually reduces their effectiveness as barriers. The slow initial Mg degradation can enable implants to retain their mechanical properties for support applications, while the delayed and more rapid degradation minimizes the implants interference with longer term healing processes. Another advantage of coatings is that they may perform multiple functions, such as increasing the bioactivity of implants. Osteoconductive materials, particles, drugs, and growth factors may be incorporated into coatings to improve surface bioactivity. The success or failure of implants is often determined by their initial contact with host cells and tissue. Thus, it is critical to engineer coatings to not just control the bulk substrate degradation rate, but also to improve surface bioactivity.
2 Substrate Preparations
The properties of Mg substrates will obviously affect their degradation, bioactivity, and interactions with coatings. Thus alloy bulk composition is a major means of controlling Mg implants [32]. Substrate bulk structure also plays a role; solid substrates provide more mechanical strength, but porous substrates may have better coating and cell adhesion and the pores can be filled with bioactive materials [61, 62].
The surfaces of metallic substrates must be prepared for coating processes in order to achieve the best results. The surface roughness of substrates affects their degradation [63, 64], coating adhesion strength, cell adhesion, and bone volume/tissue volume ratio (BV/TV) in vivo [65]. Sandblasted Mg surfaces degrade faster than threaded surfaces, which in turn degrade faster than smooth Mg surfaces [66]. An appropriately rough surface provides a larger surface area for binding and can form mechanical interlocks with coatings. Some preparation processes can alter the chemistry of the surface, which may alter the surface’s affinity for the coating. Different surface preparations have varying effects with different coatings [67, 68]. On unclean surfaces, coatings may bond to grease or particulates instead of the surface, which will weaken the coatings adhesion to those surfaces. Surfaces should be clean and have appropriate roughness in order to ensure strong coating adhesion.
3 Structure and Physical Properties of Coatings
The composition and processing routes of coatings determines their structure and physical properties (Fig. 3) [55, 69,70,71,72,73,74,75,76,76]. This in turn determines the barrier mechanisms and effectiveness of coatings (Table 3). Oxide and ceramic coatings are made of impermeable materials, but have cracks and pores that allow the passage of electrolyte. In addition, many oxide and ceramic coatings are susceptible to the same aggressive ions that attack Mg; leading to pitting, undermining, and eventually dissolution of the coating (Fig. 4a). Polymer coatings on the other hand are permeable to electrolyte and aggressive ions, but significantly reduce their diffusion which limits Mg degradation rates (Fig. 4b). It is not desirable to have completely impermeable coatings because then the Mg implants would be non-degradable like Ti. The rate of electrolyte transport through coatings must be tailored so that Mg substrates degrade at a similar rate as tissue growth.
SEM images of coatings deposited by various methods from the literature. HA coatings deposited by (a) sol-gel [70], (b) biomimetic [71], (c) hydrothermal [72], (d) electrophoretic [73], and (e) electrochemical processes [74]. Polymer coatings deposited by (f) dip [75], (g) spin [56], (h) electrospin [76], (i) electrophoretic [77], and (j) electrochemical deposition processes [78]
(a) Surface modifications form dense barriers that prevent electrolyte from reaching the underlying Mg substrate. Electrolyte can still penetrate the surface through cracks and other defects. Many of these surface modifications are slowly undermined by Cl−, reducing their barrier properties over time. (b) Polymer matrices are permeable to electrolyte but significantly reduce the diffusion rates; thus limiting Mg degradation
Thicker coatings tend to slow Mg degradation more effectively than thinner coatings of the same quality, but thicker coatings often have more defects that allow electrolyte and aggressive ions to bypass the coating and directly attack the underlying Mg substrate. It has been observed that moderately thick coatings with fewer defects can provide superior protection when compared to thicker coatings with numerous defects.
Porous coatings generally permit more electrolyte and aggressive ions to reach underlying Mg substrates than solid coatings. However, the pores can promote physical interlocking between multiple layer coatings. Porous surfaces can also improve cell adhesion and integration with tissue if in an appropriate range, but an inappropriate pore size can inhibit bioactivity of surfaces. For example, nanoporous PCL can elicit foreign body response and lower BV/TV than microporous PCL [52].
Delamination is frequently encountered with coatings for Mg substrates due to the unstable Mg surface and H2 evolution. Delamination can lead to rapid Mg degradation and its associated consequences, dislodging or movement of implants, and the departure of fragments from the implant site. Controlling the rate of electrolyte diffusion through coatings will minimize delamination by improving surface stability and limiting H2 evolution. Coating design can be optimized to mitigate delamination as well; thinner coatings [77] and low molecular weight polymers [78] tend to resist delamination more effectively. Maintaining a relatively stable but slowly eroding Mg surface is critical to the function of Mg implants.
4 Surface Modification of Magnesium
Surface modifications transform the surfaces of Mg substrates into substances with increased degradation resistance. This differs from deposition coating processes in that the raw materials for the new surface come from the original Mg substrate. The modified surface is generally much more stable than the Mg substrate and acts as barrier against electrolyte and aggressive ions. Mg surfaces can be modified through numerous methods.
4.1 Chemical Surface Modification
The simplest means of creating protective coatings on Mg substrates is passivation, which is the oxidation of Mg to form a barrier oxide or hydroxide barrier layer. Mg forms passivation layers through chemical reactions in most environments, but alkalinity and heat can create even thicker and more protective barrier layers [72, 79,80,81,82]. The surfaces of alkaline heat treated substrates often have better cell adhesion [79, 82] and implant/tissue interface strength [83] than polished substrates. The parameters of the alkaline baths and the heat treatments control the thickness, structure, and composition of the oxide layer formed [80]. Alkaline baths without heat treatments tend to create loose and porous barrier layers that are susceptible to aggressive ions. Heat treatments can densify the oxide barrier layer so that it resists attacks by aggressive ions and significantly reduces the Mg degradation rate in physiological fluids [79, 80]. Chemical surface modifications significantly reduce Mg degradation rates, but like many other impermeable barriers they are also impaired by the presence of pores and cracks [84].
The chemical composition of the alkaline bath can be used to tailor the chemical composition of the Mg surface. Some alkaline bath compositions can create surface layers that promote more calcium phosphate (CaP) deposition and may therefore improve osteoconductivity [80]. Incorporating silicon (Si) or strontium phosphates into the surface can improve the protectiveness and durability of the passivation layers [83, 85, 86]. Silicates can enhance mineralization activity of osteoblasts [87] and improve the mechanical strength of bone/implant interfaces [83]. Some species of silicates, like akermanite, have better bioactivity than β-tricalcium phosphate (β-TCP) [88]. These properties have attracted much interest in Si as a dopant for coatings. Silicates surfaces may be formed through surface modifications or deposition.
Not all chemical surface modifications occur at alkaline pH; fluoridation [84, 89,90,91] occurs at highly acidic pH. Fluoridation may have additional benefits beyond controlling Mg degradation. The in vivo bioactivity of fluoridated surfaces may be comparable to hydroxyapatite (HA) coatings [61, 89] and superior to collagen coatings [91]. In some cases, and fluoridated surfaces may even have intrinsic anti-bacterial properties [90].
4.2 Anodization
Anodization is an electrochemical process that creates protective amorphous oxide barriers [92,93,94]. Greater potential, current, and anodization time generally increase the thickness of the barrier layer; but too much will create cracks in the surface. The cracks undermine the effectiveness of anodized surfaces as barriers. Certain bath compositions are also more prone to sparking, which increases pore formation in the surface. Additionally, the temperature of the electrolytic bath [92] and the composition of the Mg alloy substrate [93] can influence the properties of the anodized surface. Anodized surfaces are more protective if their degradation products have low solubility and strong adherence to their substrate [94].
4.3 Micro-Arc Oxidation
Micro-arc oxidation (MAO) is a surface modification process related to anodization, but uses higher potentials over shorter times to create ceramic surfaces instead of amorphous oxide surfaces. The ceramic nature of MAO surfaces can provide greater degradation resistance, hardness, crystallinity, and bioactivity than anodized surfaces [95, 96]. The potential during MAO exceeds the breakdown potential of the substrate, creating localized plasma reactions. These plasma reactions can create regions of high heat and pressure that can cause melting, flowing, sintering, annealing, and rapid cooling. The composition of the electrolytic bath can influence the surface composition, surface morphology and roughness, porosity, types of deposits formed during immersion, and the degradation rate [97]. Larger currents for longer times will increase the thickness of MAO surfaces, but may also increase degradation rates due to crack formation [98].
MAO surfaces generally have several layers; a porous outer layer, a compact inner layer, and finally the surface of the substrate [95]. The majority of degradation resistance comes from the compact inner layer [99]. The increased surface roughness of the porous outer layer can improve cell adhesion [100]. However, electrolyte and aggressive ions can enter the pores and cracks to react with Mg [101], causing degradation products to accumulate at the coating/substrate interface and lift the MAO surface off of the Mg substrate [102]. The brittleness of MAO surfaces [103] can exacerbate the damage caused by localized degradation.
5 Deposited Coatings
Deposited coatings are made from materials foreign to the Mg substrates, and may be deposited through numerous methods. Such coatings have a vast range of barrier, mechanical, and biological properties; enabling them to be fine-tuned for specific applications.
5.1 Calcium Phosphate Coatings
Materials derived from CaP are highly osteoconductive because they mimic the mineral content of bone. However, the role of CaP alone is limited in orthopedic applications due to its inherent brittleness. Coatings can take advantage of the superb osteoconductivity of CaP while the underlying Mg substrates provide the mechanical support needed in orthopedic applications.
The phase of CaP that most closely mimics the mineral content of bone and has the greatest osteoconductivity is hydroxyapatite (HA). It is also the slowest dissolving phase, which improves the barrier properties of coatings. Another frequently investigated phase of CaP is β-tricalcium phosphate (β-TCP), which is osteoconductive and known to induce macrophage activity that is beneficial to implant integration [104]. CaP coatings can increase CaP deposition in simulated body fluid (SBF), which suggests improved osteoconductivity [105]. Incorporation of Si into the CaP coating can further increase CaP deposition [106]. Nano-scale HA (nHA) has even better osteoconductivity than microscale HA [107], but may also provide less protection from degradation to underlying Mg substrates [108]. Rod shaped HA crystals may have better bioactivity than flake shaped HA crystals; such as increased cell proliferation and ALP activity [109]. Mesoporous HA structure can ameliorate damage from residual stress, reduce penetration of electrolyte, and reduce Mg corrosion rate [110]. The wide range of properties for CaP can be fine-tuned for specific applications.
CaP coatings can be deposited through numerous methods such as: plasma spray, sol-gel, chemical deposition [69, 70, 111, 112], biomimetic deposition [69, 113], electrophoretic deposition [71], and electrochemical deposition [72, 106] (Fig. 3). There are two general strategies for depositing CaP coatings: (1) synthesizing CaP first and then depositing it onto the substrate; and (2) synthesizing CaP and depositing it onto the substrate simultaneously. The first strategy offers the most control over the properties of CaP, but requires multiple steps. Furthermore, the properties of the CaP that were painstakingly fine-tuned may be altered during the deposition process. High temperature coating processes such as plasma spray can change the phase of CaP [114], alter the crystallinity of CaP [114], or increase the grain size of CaP. Alternatively, low temperature coating processes often create less adherent coatings without subsequent heat treatment [72]. The second strategy for depositing CaP coatings is often simpler, but provides less control over the properties of CaP in the coating.
Many CaP coatings have weak adhesion strength to their substrates. CaP and metallic substrates have very different thermal expansion coefficients, which can damage the coating or coating/substrate interface initially during high temperature coating processes and sintering, or gradually when the implant is exposed to temperature changes and loading cycles in vivo. Both of these challenges are exacerbated by the inherent brittleness of CaP. A potential resolution is the incorporation of CaP into composites with flexible materials, such as polymers.
5.2 Polymer Coatings
5.2.1 Commonly Used Polymer Coatings
Polymers can be divided into two major categories: natural and synthetic. Natural polymers are derived from natural sources while synthetic polymers are manufactured artificially. The advantage of natural polymers is that they often have good bioactivity. The disadvantages of natural polymers are that they have less consistency between different production runs and that they are more likely to carry microbial contamination. Many synthetic polymers are the opposite case. The advantages of synthetic polymers are that they have greater consistency between different production runs and less risk of microbial contamination. A disadvantage of synthetic polymers is that they frequently lack the bioactivity exhibited by some natural polymers.
Examples of natural polymers include chitosan, alginate, collagen, and protein. Chitosan coatings have been investigated for controlling the degradation rate Mg alloys [115,116,117,118,119]. Chitosan is the deacetylated derivative of chitin, which is commercially obtained from crustaceans (i.e., crabs and shrimp). Chitosan is more soluble than chitin, which is important for processing because both polymers thermally degrade before melting [120]. Chitosan has several unique advantages over other polymers: its insolubility above pH 7 may help further protect Mg substrates [117], it can promote bone growth [121], and it has intrinsic antibacterial properties [122,123,124]. Chitosan is degraded enzymatically in vivo [125].
Alginate is a polysaccharide that can be used as a coating material for controlling Mg degradation [126, 127]. An advantage of alginate is that it is commercially produced by bacteria or algae; which enables the production to occur in an industrial setting and may prevent issues associated with harvesting organisms outside of an industrial setting (i.e., risk of microbial contamination and inconsistency between different production runs). Another advantage is that water is a solvent of alginate, which makes it easier to embed coatings with pharmaceuticals. Finally, alginate can protect implants from the immune system, which may be beneficial for some niche applications. A disadvantage of alginate coating materials is their poor cell adhesion [128]. This challenge may be addressed through the covalent attachment of biological recognition sites (i.e., RGD) to alginate polymers [129] or dispersion of bioactive materials such as HA within the alginate matrix [126].
Other natural polymer or protein based coatings used to control Mg degradation include: collagen [91, 130], albumin [131], phytic acid [132,133,134], and other proteins or peptides [135]. Coatings derived from natural proteins can significantly increase bioactivity, especially when the coating proteins are native to the physiological region where the implant is placed. Most proteins carry greater risks of immune responses, although collagen tends to have low antigenicity [136]. Many protein coatings also face more costly mass production, batch to batch variability, and risk of microbial contamination. The immunological and logistical challenges associated with natural polymers can make the readily manufactured and customized synthetic polymers an attractive alternative.
Examples of common synthetic polymers include polyesters such as poly lactic acid (PLA), polyglycolic acid (PGA), and polycaprolactone (PCL). The degradation products of these polyesters are natural metabolites, which improves their biocompatibility and clearance. The polyesters degrade primarily by hydrolysis of their ester bonds by water molecules, though enzyme catalyzed degradation may play a role in vivo.
PLA can be produced as a semicrystalline isomer (PLLA) or an amorphous isomer (PDLA). PLLA is more common in nature [137] and more easily metabolized [138], so it is used more frequently than PDLA. PLLA is one of the most commonly used polymers for orthopedic implants because of its high mechanical strength and low immunogenicity. PLA has an additional methyl group that increases its hydrophobicity and sterically blocks hydrolysis of its ester bonds. These properties enable PLLA coatings to provide significant protection to Mg [78, 139, 140]. However, PLLA is brittle, which limits it use as a load bearing material. It also has limited thermal stability at high temperatures which may complicate the use of some processing routes [137]. Additionally, PLLA also has an excessively long degradation time and low bioactivity, which can lead to poor bone ingrowth at the implant site [59, 60, 141]. The impaired bone ingrowth may be exhibited by empty bone sockets outlining the original implant site after degradation [60, 142, 143].
PGA was investigated as an orthopedic biomaterial in its own right because of its good mechanical properties, but is now mainly used in copolymers. It is insoluble in most organic solvents because of its highly crystalline structure, which limits the compatible processing methods [138]. An increased occurrence of osteolysis from PGA implants has also been observed in some studies [144], while others have shown an inhibition of osteogenesis by PGA [145]. PGA sutures are also more inflammatory than PLA sutures [146].
PLA and PGA are frequently combined in the copolymer poly(lactic-co-glycolic acid) (PLGA) to address their individual challenges. PLGA is one of the most commonly used polymers for implants due to its physical properties, biocompatibility, and it is approved by the FDA for certain applications [147, 148]. PLGA is less brittle than PLLA and is soluble in many organic solvents. The degradation rate [149] and water absorption [150] of PLGA can be tailored by altering the PLA:PGA ratio. PLGA coatings have been used to control Mg degradation [55, 151, 152], but may delaminate due to H2 evolution [55]. PLGA also has mediocre cell adhesion [153, 154], which limits bone growth into the implant site. Finally, both PLA and PGA release acidic degradation products which can lower the pH of the local environment.
PCL is another common polyester coating material for Mg [78, 139, 155,156,157], and one of the earliest biodegradable polymers used for implants in general [158]. PCL coatings can increase the volume of bone growth on Mg substrates [157]. The low melting temperature makes PCL especially easy to process, especially with embedded pharmaceuticals or proteins that are vulnerable to heat or organic solvents. This makes PCL a good choice when drugs or bioactive factors are incorporated into the coating. However, PCL has an excessively long degradation time and mediocre cell adhesion.
Polyester coatings can chemically interact with Mg substrates during degradation ; although the published results are contradictory. Acidic polymer degradation products may attack the Mg substrate while the alkaline Mg degradation products attack the polymers. Additionally, Mg(OH)2 in the passivation layer may catalyze polymer hydrolysis; which has been observed as a positive feedback loop for degradation [73]. Contrarily, it has also been observed that dispersed Mg(OH)2 particles may reduce polymer degradation by stabilizing the pH microclimate and disrupting auto-catalyzation of polymer degradation reactions [159]. These contradictory results may be due to differences in experimental design.
5.2.2 Overview of Polymer Properties
One of the greatest strengths of polymers as a class of coating materials is their versatility (Table 4). Polymers possess a vast range of physical, chemical, and biological properties, although polymers alone often have insufficient mechanical properties for many support applications. Numerous methods exist to deposit polymer coatings including dip [73, 152], spin [55, 160], electrospin [74, 161], electrophoretic [75, 162], and electrochemical [76] deposition processes (Fig. 3). The deposition method controls the structure of the coatings; some methods create solid coatings while others create porous coatings. Finally, a large body of knowledge surrounds polymers, their use as biomaterials, and the means to tailor their properties.
Many of a polymer’s physical properties are inter-related; and so altering one property will also alter others. Molecular weight (Mw) influences the viscosity of solutions/melts, the mechanical properties of the polymer matrix [163], the coating adhesion strength [78], polymer degradation rates [164], and degradation rates of underlying Mg substrates [139]. The Mw decreases during degradation, until it is small enough to allow monomers or short polymer chains to be dissolved. A lower Mw can also lead to more autocatalysis of degradation reactions for some polymers because the number of reactive end groups increases. The glass transition temperature (Tg) determines the temperature at which the polymer becomes rubbery and more susceptible to many physical processes; and is influenced by the Mw. The Tg is often reduced concurrently with Mw during degradation, which can make the coating more vulnerable. Both the Mw and Tg affect the crystallinity of polymers, which influences degradation rates, water permeability [165,166,167], and bioactivity [168]. A more crystalline polymer is generally a more effective barrier to water, but in some cases increased crystallinity is accompanied by crack and void formation that increases water permeability [169]. The interactions between all of the polymer coatings properties must be balanced in order to ensure that Mg implants degrade at the desired rate.
5.2.3 Methods of Depositing Polymer Coatings
Many processes are used to deposit polymer coatings, and each process has its own idiosyncrasies. The coating process used affects the coating structure, and therefore water transport to underlying substrates. Some processes have better compatibility with certain materials and applications than other processes. A thorough understanding of coating materials and processes is necessary for the creation of reliable protective coatings.
Solvents are commonly used for the processing of polymers. The advantage of using solvents to liquefy polymers is that very little heat is needed; which is useful when polymers thermally degrade while melting, for copolymers whose constituents have different melting points, or when viscosity must be controlled. The disadvantages of solvent processing routes are that some polymers have low solubility, the solvents can denature drugs or proteins within the polymer, solvent residues can impair bioactivity, and potential vapor hazards during coating processes.
Different solvents can create polymer matrices with vastly different structures [170]. The choice of solvent impacts the thickness, porosity, and crystallinity of coatings. Solvents with slower evaporation rates can increase the crystallinity of coatings because the polymer chains have more time to form crystals [171]. The size, frequency, and interconnectivity of pores in solvent cast coatings is also heavily influenced by the choice of solvent [170].
Other coating processes liquefy the polymers with high temperatures instead of solvents. Heating polymers above their Tm enables them to be extruded, molded, or dipped onto substrates. Annealing is a process related to melting that can further reduce water absorption by polymer coatings by increasing their crystallinity. During annealing , the coatings are heated above the polymers Tg but below the Tm, causing the polymer chains to align in a more crystalline arrangement. Excessively high annealing temperatures or long annealing times can lead to crack and void formation, undermining the barrier properties of the coating despite the increased crystallinity.
5.2.3.1 Dip Coating
Dip coating is the simplest coating process, wastes very little material, and is able to cover complex geometries. It is applied by dipping substrates into a solution/melt. When the coated substrate is withdrawn from the solution/melt, most of the coating material remains in place, but the pull of gravity can increase inhomogeneity (Fig. 3) [73]. The thickness and structure of dip coatings are influenced by solvent evaporation rate, viscosity, coating material concentration, immersion time, and withdrawal speed from the solution or melt.
5.2.3.2 Spin Coating
Spin coating is another simple coating method with greater homogeneity and control of coating structure than dip coating (Fig. 3) [55]. After the solution/melt is deposited on the substrate, centripetal force removes excess solution/melt to create a uniform coating. The thickness and structure of spin coatings are influenced by the amount of coating material added, solution/melt viscosity, evaporation rate, and substrate roughness. Limitations of spin coating are that it can only be used on flat surfaces and is extremely wasteful of coating materials.
5.2.3.3 Electrospinning
Electrospun coatings have the advantage of exquisite control over the thickness of the coating and the fibers within the coating. The fibrous structure is similar to the structure of the extracellular matrix of some tissues (Fig. 3) [74], which may improve interactions with cells. However; electrospun coatings are extremely porous and may exhibit increased water transport processes [172] with a concomitant increase in Mg degradation, although this is not always the case [130]. Finally, the electrospinning process is more complicated than dip or spin coating.
During electrospinning , a potential is applied to a polymer solution/melt at the tip of a syringe. A strong enough potential will overcome the viscosity and surface tension of the solution/melt, and the polymer will form a fiber that is pulled towards the substrate. The mechanical strength of electrospun fibers may be inversely proportional to fiber diameter because the thicker fibers may contain less organized nanofibers [171]. The fiber structure may be controlled through the operating parameters or solution composition.
Key operating parameters of electrospinning are potential, flow rate, distance, and time. The operating parameters can have significant effects upon fiber morphology and crystallinity [173]. The parameters of the solution/melt are also important; key properties include concentration, viscosity, surface tension, evaporation rate, and conductivity. Some solvents are better suited for the electrospinning process; in general a better solvent will be associated with smooth fiber morphology instead of the “beads on a string” morphology. The latter morphology is observed due to a transition between electrospinning and electrospraying [174]. The choice of solvent also affects the fiber diameter, crystallinity, and presence of holes within the fiber. It is generally more desirable that the solvents have lower viscosity and higher conductivity. Operating conditions can be modified to compensate for solvents that are less suited for electrospinning.
5.2.3.4 Electrodeposition
Electric potential can be used to coat Mg substrates with a variety of materials, and has two general approaches. Electrophoretic deposition is the use of electric potential to transport pre-made coating materials to the substrate and then bind them to that substrate. Electrochemical deposition on the other hand is the use of electric potential to transport coating material precursors to the substrate where they will react to form the final coating material and bind to the substrate. The key parameters of electrodeposition are the potential, current, time, electrolyte, concentration of coating materials in the electrolyte, charge of polymers or particles, and the mobility of the polymers or particles. Electrodeposition can be used to coat Mg with a variety of materials including ceramics [72, 106], polymers [17, 76], ceramic/polymer microspheres [175], and others. However; electrodeposited coatings are often not as homogenous as other methods such as spin coating (Fig. 3) [17, 55], and ensuring homogeneity can be especially difficult for composite coating materials whose constituents have different charges or degrees of mobility under an electric field. Another challenge is that H2 gas evolving during electrodeposition can create void spaces in the coating. These challenges may be addressed by tailoring the operating parameters and electrolyte bath composition.
6 Composite Coatings
Natural bone is a composite material; the unique mechanical and biological properties of bone are enabled by the interplay between the mineral content and the collagenous matrix. No single material possesses the physical and biological properties needed to mimic bone tissue and support injured bones. Thus, composite materials are needed for orthopedic applications.
6.1 Hydroxyapatite Composite Coatings
One of the most frequently investigated composite coatings for orthopedic implants is HA particles dispersed within polymer matrices. The polymer matrix provides a flexible interface between HA and Mg that mitigates the thermal expansion coefficient mismatch. Nano-scale particle size and good dispersion of HA particles throughout the polymer matrix improve both the mechanical strength and the bioactivity of the composite material [176,178,179,180,181,182,182]. Cell adhesion and mechanical strength of PLGA matrices both increase with increasing HA content until they plateau at around 30 wt.% HA. Increasing HA content beyond 30 wt.% in PLGA matrices has only marginal effect upon cell adhesion, but increases brittleness [178, 179]. The incorporation of HA has been shown to significantly improve cell adhesion to chitosan [115], alginate [126], PLA [183, 184], PLGA [185], and PCL [186]. This improvement is not limited to just cell adhesion; improved protein secretion and alkaline phosphatase (ALP) activity are often observed as well [187]. HA composites also improve bone ingrowth at the implant sites in vivo; CaP/PLLA interference screws did not leave behind the empty screw holes [188, 189] in bone tissue that were observed with pure PLLA screws [143, 190].
HA particles have profound effects upon diffusion and uptake of electrolyte in polymer matrices. HA particles increase water uptake by polymer matrices [147], but still tend to improve barrier properties of coatings [55]. Electrolyte diffusion through particle/polymer composites is reduced by the filler effect; which is caused by particles increasing the tortuosity of routes taken by diffusing electrolyte or by particles increasing the local rigidity of the polymer matrix surrounding them [191] (Fig. 5a).
Composite coatings utilize synergy between different materials. (a) Polymer matrix binds HA particles to Mg substrate, provides a flexible interface, and exhibits a filler effect. (b) Polymer inter-layer provides a flexible interface between HA coating and Mg substrate, and acts as an additional barrier. (c) HA outer coating seals defects in inner coating and prevent aggressive ions from reaching ceramic/oxide surface
Alternatively, polymer interlayers can be used to ameliorate the thermal expansion coefficient mismatch between HA and Mg (Fig. 5b). A flexible and elastic interlayer can minimize cracking of the outer HA coating during repeated loading and temperature changes [156]. The combination of coating layers also requires electrolyte to bypass to different barrier mechanisms. Electrolyte must enter through cracks, pores, and voids in the impermeable outer coating. Then the electrolyte must diffuse through the permeable polymer interlayer, but at a significantly reduced diffusion rate that limits Mg degradation reactions.
Polymers are not the only coating matrix that can hold HA particles, MAO surfaces can accomplish this feat as well. HA can be incorporated into MAO surfaces by adding HA particles [98, 192] or HA chemical pre-cursors [193] to the electrolyte during a one-step HA/MAO coating process. This process creates a MAO surface with HA particles dispersed inside it. The HA particles are not always distributed homogeneously throughout the surface, some processes may concentrate the HA particles in the outer region of the coating [98]. Increasing the HA concentration in the electrolyte can increase the HA concentration in the MAO surface [98]. Ultrasonication can increase corrosion resistance and Ca/P ratio of HA/MAO coatings [194]. The high temperatures during the MAO coating process can convert HA to β-TCP [192]. Alternatively, HA/MAO coatings can be created using a two-step coating process. First the MAO surface is created on the Mg substrate, and then HA is deposited onto the MAO surface by sol-gel deposition [105, 195, 196], electrochemical deposition [197,198,199], electrophoretic deposition, or other means. The combination of HA and MAO is beneficial because it can address some of the major challenges of both coating types. The HA can prevent aggressive ions from reaching and attacking the MAO surface, and can seal cracks and pores in the MAO surface (Fig. 5c). Conversely, the porosity of MAO surfaces provides many opportunities for mechanical interlocks with HA coatings, which can significantly increase the often poor adhesion strength of HA coatings. Furthermore, bone-like CaP is often deposited on HA/MAO coatings during immersion [98, 105]. Other materials can be deposited atop MAO surfaces; silicates [200,201,202,203] and polymers are common choices.
6.2 Polymer Coatings and Surface Modifications
Polymers and polymer composites are also used as outer coating layers on top of modified Mg surfaces [204,205,206,207,208,209,210,211,212]. The polymer coatings seal pores and cracks in the underlying modified surfaces [205, 209,210,211], and reduce the diffusion of aggressive ions to that surface. The underlying modified surface is generally an impermeable barrier with the exception of those cracks and pores, and a reduced diffusion of aggressive ions promotes stability of the modified surface. This synergistically improves the barrier properties of the composite coating. Outer polymer coatings can improve the hemocompatibility of modified surfaces [207, 208], but outer coating layers with poor bioactivity may promote encapsulation of the implant [213]. For this reason, the outer coating layer must have both good barrier and biological properties.
7 Incorporation of Bioactive Factors into Coatings
Proteins and other bioactive factors can be attached to the surface of coatings to control interactions with cells and tissue. Attaching heparin to coatings can improve hemocompatibility, increase umbilical vein endothelial cells (HUVEC) proliferation and inhibit human umbilical artery smooth muscle cells (HUASMC) adhesion [212]. Preferential control over which cells adhere to and proliferate on a surface can improve the biological outcome of implants, such as promoting endothelialization of stents.
Coatings can store and release drugs at a controlled rate [215,216,217]. Common examples of these drugs include growth factors to improve healing at the wound site and antibiotics to prevent colonization of the implant. Storing drugs within coatings can resolve three major challenges facing drug use: (1) transporting drugs to the target site, (2) achieving a therapeutic dose at the target site while minimizing the dose outside the target site, and (3) maintaining a constant dose at the target site over time. Polymers, CaP, and other nanoparticles have long been used for controlled storage and release of drugs [218], enabling this technology to be easily translated to coatings.
8 Summary
Coatings have great potential to control Mg degradation and bioactivity because their wide range of physical and biological properties enables them to be tailored to specific functions, and decouple surface properties from bulk properties. A well-controlled Mg degradation rate will prevent many of the challenges associated with rapid degradation (i.e., catastrophic mechanical failure, local alkalization, H2 gas bubbles, swelling) and slow degradation (i.e., empty bone sockets). Ideally, functional natural tissue will replace the biodegradable Mg implants over time. The clinical translation of Mg derived implants will lead to improved patient outcome and lower medical costs by preventing the complications associated with the current generation of non-degradable implants.
References
Jain KK. The handbook of nanomedicine. New York: Springer; 2012.
Mavrogenis AF, Dimitriou R, Parvizi J, Babis GC. Biology of implant osseointegration. J Musculoskelet Neuron. 2009;9(2):61–71.
Jiang Y, Jia T, Wooley PH, Yang SY. Current research in the pathogenesis of aseptic implant loosening associated with particulate wear debris. Acta Orthop Belg. 2013;79(1):1–9.
Darouiche RO. Treatment of infections associated with surgical implants. New Engl J Med. 2004;350(14):1422–9.
Brady R, Calhoun J, Leid J, Shirtliff M. Infections of orthopaedic implants and devices. In: Shirtliff M, Leid J, editors. The role of biofilms in device-related infections. Berlin: Springer; 2009. p. 15–55.
Richards RH, Palmer JD, Clarke NMP. Observations on removal of metal implants. Injury. 1992;23(1):25–8.
Hanson B, van der Werken C, Stengel D. Surgeons’ beliefs and perceptions about removal of orthopaedic implants. BMC Musculoskelet Disord. 2008;9:73.
Helmecke P, Ezechieli M, Becher C, Kohler J, Denkena B. Resorbable interference screws made of magnesium based alloy. Biomed Tech (Berl). 2013. https://doi.org/10.1515/bmt-2013-4074.
Erdmann N, Angrisani N, Reifenrath J, Lucas A, Thorey F, Bormann D, Meyer-Lindenberg A. Biomechanical testing and degradation analysis of MgCa0.8 alloy screws: a comparative in vivo study in rabbits. Acta Biomater. 2011;7(3):1421–8.
Reifenrath J, Angrisani N, Erdmann N, Lucas A, Waizy H, Seitz JM, Bondarenko A, Meyer-Lindenberg A. Degrading magnesium screws ZEK100: biomechanical testing, degradation analysis and soft-tissue biocompatibility in a rabbit model. Biomed Mater. 2013;8(4):045012.
Waksman R, Pakala R, Kuchulakanti PK, Baffour R, Hellinga D, Seabron R, Tio FO, Wittchow E, Hartwig S, Harder C, Rohde R, Heublein B, Andreae A, Waldmann K-H, Haverich A. Safety and efficacy of bioabsorbable magnesium alloy stents in porcine coronary arteries. Catheter Cardiovasc Interv. 2006;68(4):607–17.
Bauer M, Schilling T, Weidling M, Hartung D, Biskup C, Wriggers P, Wacker F, Bach FW, Haverich A, Hassel T. Geometric adaption of biodegradable magnesium alloy scaffolds to stabilise biological myocardial grafts. Part I. J Mater Sci Mater Med. 2014;25(3):909–16.
Lock JY, Wyatt E, Upadhyayula S, Whall A, Nuñez V, Vullev VI, Liu H. Degradation and antibacterial properties of magnesium alloys in artificial urine for potential resorbable ureteral stent applications. J Biomed Mater Res A. 2014;102(3):781–92.
Liu L, Li N, Lei T, Li K, Zhang Y. The in vitro biological properties of Mg-Zn-Sr alloy and superiority for preparation of biodegradable intestinal anastomosis rings. Med Sci Monit. 2014;20:1056–66.
Luffy SA, Chou DT, Waterman J, Wearden PD, Kumta PN, Gilbert TW. Evaluation of magnesium-yttrium alloy as an extraluminal tracheal stent. J Biomed Mater Res A. 2014;102(3):611–20.
Chng CB, Lau DP, Choo JQ, Chui CK. A bioabsorbable microclip for laryngeal microsurgery: design and evaluation. Acta Biomater. 2012;8(7):2835–44.
Sebaa MA, Dhillon S, Liu H. Electrochemical deposition and evaluation of electrically conductive polymer coating on biodegradable magnesium implants for neural applications. J Mater Sci Mater Med. 2013;24(2):307–16.
Yan WY, Berthe J, Wen C. Numerical investigation of the effect of porous titanium femoral prosthesis on bone remodeling. Mater Design. 2011;32(4):1776–82.
Drosos GI, Babourda E, Magnissalis EA, Giatromanolaki A, Kazakos K, Verettas DA. Mechanical characterization of bone graft substitute ceramic cements. Injury. 2012;43(3):266–71.
Sabir MI, Xu XX, Li L. A review on biodegradable polymeric materials for bone tissue engineering applications. J Mater Sci. 2009;44(21):5713–24.
Brar HS, Platt MO, Sarntinoranont M, Martin PI, Manuel MV. Magnesium as a biodegradable and bioabsorbable material for medical implants. JOM. 2009;61(9):31–4.
Windhagen H, Radtke K, Weizbauer A, Diekmann J, Noll Y, Kreimeyer U, Schavan R, Stukenborg-Colsman C, Waizy H. Biodegradable magnesium-based screw clinically equivalent to titanium screw in hallux valgus surgery: short term results of the first prospective, randomized, controlled clinical pilot study. Biomed Eng Online. 2013;12:62.
Zhang Y, Ren L, Li M, Lin X, Zhao HF, Yang K. Preliminary study on cytotoxic effect of biodegradation of magnesium on cancer cells. J Mater Sci Technol. 2012;28(9):769–72.
Li RW, Kirkland NT, Truong J, Wang J, Smith PN, Birbilis N, Nisbet DR. The influence of biodegradable magnesium alloys on the osteogenic differentiation of human mesenchymal stem cells. J Biomed Mater Res A. 2014;102(12):4346–57.
Park J-W, Kim Y-J, Jang J-H, Song H. Osteoblast response to magnesium ion-incorporated nanoporous titanium oxide surfaces. Clin Oral Implants Res. 2010;21(11):1278–87.
Janning C, Willbold E, Vogt C, Nellesen J, Meyer-Lindenberg A, Windhagen H, Thorey F, Witte F. Magnesium hydroxide temporarily enhancing osteoblast activity and decreasing the osteoclast number in peri-implant bone remodelling. Acta Biomater. 2010;6(5):1861–8.
Castellani C, Lindtner RA, Hausbrandt P, Tschegg E, Stanzl-Tschegg SE, Zanoni G, Beck S, Weinberg AM. Bone-implant interface strength and osseointegration: biodegradable magnesium alloy versus standard titanium control. Acta Biomater. 2011;7(1):432–40.
Waizy H, Diekmann J, Weizbauer A, Reifenrath J, Bartsch I, Neubert V, Schavan R, Windhagen H. In vivo study of a biodegradable orthopedic screw (MgYREZr-alloy) in a rabbit model for up to 12 months. J Biomater Appl. 2014;28(5):667–75.
Zhang EL, Xu LP, Yu GN, Pan F, Yang K. In vivo evaluation of biodegradable magnesium alloy bone implant in the first 6 months implantation. J Biomed Mater Res A. 2009;90A(3):882–93.
Witte F, Ulrich H, Rudert M, Willbold E. Biodegradable magnesium scaffolds: Part I: appropriate inflammatory response. J Biomed Mater Res A. 2007;81A(3):748–56.
Xu LP, Yu GN, Zhang E, Pan F, Yang K. In vivo corrosion behavior of Mg-Mn-Zn alloy for bone implant application. J Biomed Mater Res A. 2007;83A(3):703–11.
Witte F, Kaese V, Haferkamp H, Switzer E, Meyer-Lindenberg A, Wirth CJ, Windhagen H. In vivo corrosion of four magnesium alloys and the associated bone response. Biomaterials. 2005;26(17):3557–63.
Witte F, Ulrich H, Palm C, Willbold E. Biodegradable magnesium scaffolds: Part II: peri-implant bone remodeling. J Biomed Mater Res A. 2007;81A(3):757–65.
Zhai Z, Qu X, Li H, Yang K, Wan P, Tan L, Ouyang Z, Liu X, Tian B, Xiao F, Wang W, Jiang C, Tang T, Fan Q, Qin A, Dai K. The effect of metallic magnesium degradation products on osteoclast-induced osteolysis and attenuation of NF-kappaB and NFATc1 signaling. Biomaterials. 2014;35(24):6299–310.
Stendig-Lindberg G, Koeller W, Bauer A, Rob PM. Experimentally induced prolonged magnesium deficiency causes osteoporosis in the rat. Eur J Intern Med. 2004;15(2):97–107.
Nan M, Yangmei C, Bangcheng Y. Magnesium metal—a potential biomaterial with anti-bone cancer properties. J Biomed Mater Res A. 2013;102(8):2644–51.
Saver JL, Kidwell C, Eckstein M, Starkman S, Investigators F-MPT. Prehospital neuroprotective therapy for acute stroke—results of the field administration of stroke therapy-magnesium (FAST-MAG) pilot trial. Stroke. 2004;35(5):E106–8.
Ren L, Lin X, Tan LL, Yang K. Effect of surface coating on antibacterial behavior of magnesium based metals. Mater Lett. 2011;65(23–24):3509–11.
Robinson DA, Griffith RW, Shechtman D, Evans RB, Conzemius MG. In vitro antibacterial properties of magnesium metal against Escherichia coli, Pseudomonas aeruginosa and Staphylococcus aureus. Acta Biomater. 2010;6(5):1869–77.
Tie D, Feyerabend F, Muller WD, Schade R, Liefeith K, Kainer KU, Willumeit R. Antibacterial biodegradable Mg-Ag alloys. Eur Cell Mater. 2013;25:284–98.
Witte F. The history of biodegradable magnesium implants: a review. Acta Biomater. 2010;6(5):1680–92.
Witte F, Reifenrath J, Muller PP, Crostack HA, Nellesen J, Bach FW, Bormann D, Rudert M. Cartilage repair on magnesium scaffolds used as a subchondral bone replacement. Materialwiss Werkst. 2006;37(6):504–8.
Song GL. Recent progress in corrosion and protection of magnesium alloys. Adv Eng Mater. 2005;7(7):563–86.
Lindstrom R, Johansson LG, Thompson GE, Skeldon P, Svensson JE. Corrosion of magnesium in humid air. Corros Sci. 2004;46(5):1141–58.
Mueller WD, de Mele MFL, Nascimento ML, Zeddies M. Degradation of magnesium and its alloys: dependence on the composition of the synthetic biological media. J Biomed Mater Res A. 2009;90A(2):487–95.
Song G, Atrens A. Understanding magnesium corrosion—a framework for improved alloy performance. Adv Eng Mater. 2003;5(12):837–58.
Song G, Atrens A. Recent insights into the mechanism of magnesium corrosion and research suggestions. Adv Eng Mater. 2007;9(3):177–83.
Xin Y, Huo K, Tao H, Tang G, Chu PK. Influence of aggressive ions on the degradation behavior of biomedical magnesium alloy in physiological environment. Acta Biomater. 2008;4(6):2008–15.
Johnson I, Perchy D, Liu H. Interactions between aggressive ions and the surface of a magnesium-yttrium alloy. Conf Proc IEEE Eng Med Biol Soc. 2012;2012:5670–3.
Witte F, Fischer J, Nellesen J, Crostack HA, Kaese V, Pisch A, Beckmann F, Windhagen H. In vitro and in vivo corrosion measurements of magnesium alloys. Biomaterials. 2006;27(7):1013–8.
Mueller WD, Nascimento ML, de Mele MFL. Critical discussion of the results from different corrosion studies of Mg and Mg alloys for biomaterial applications. Acta Biomater. 2010;6(5):1749–55.
Jensen J, Rolfing JH, Svend Le DQ, Kristiansen AA, Nygaard JV, Hokland LB, Bendtsen M, Kassem M, Lysdahl H, Bunger CE. Surface-modified functionalized polycaprolactone scaffolds for bone repair: in vitro and in vivo experiments. J Biomed Mater Res A. 2013;102(9):2993–3003.
Imwinkelried T, Beck S, Iizuka T, Schaller B. Effect of a plasmaelectrolytic coating on the strength retention of in vivo and in vitro degraded magnesium implants. Acta Biomater. 2013;9(10):8643–9.
Zhang S, Zhang X, Zhao C, Li J, Song Y, Xie C, Tao H, Zhang Y, He Y, Jiang Y, Bian Y. Research on an Mg–Zn alloy as a degradable biomaterial. Acta Biomater. 2010;6(2):626–40.
Johnson I, Akari K, Liu H. Nanostructured hydroxyapatite/poly(lactic-co-glycolic acid) composite coating for controlling magnesium degradation in simulated body fluid. Nanotechnology. 2013;24(37):375103.
Degner J, et al. Electrochemical investigations of magnesium in DMEM with biodegradable polycaprolactone coating as corrosion barrier. Applied Surface Science. 2013;282:264–70.
Sung HJ, Meredith C, Johnson C, Galis ZS. The effect of scaffold degradation rate on three-dimensional cell growth and angiogenesis. Biomaterials. 2004;25(26):5735–42.
Dumas JE, Prieto EM, Zienkiewicz KJ, Guda T, Wenke JC, Bible J, Holt GE, Guelcher SA. Balancing the rates of new bone formation and polymer degradation enhances healing of weight-bearing allograft/polyurethane composites in rabbit femoral defects. Tissue Eng A. 2014;20(1–2):115–29.
Walton M, Cotton NJ. Long-term in vivo degradation of poly-L-lactide (PLLA) in bone. J Biomater Appl. 2007;21(4):395–411.
Pihlajamaki H, Bostman O, Tynninen O, Laitinen O. Long-term tissue response to bioabsorbable poly-L-lactide and metallic screws: an experimental study. Bone. 2006;39(4):932–7.
Lalk M, Reifenrath J, Angrisani N, Bondarenko A, Seitz JM, Mueller PP, Meyer-Lindenberg A. Fluoride and calcium-phosphate coated sponges of the magnesium alloy AX30 as bone grafts: a comparative study in rabbits. J Mater Sci Mater Med. 2013;24(2):417–36.
Oosterbeek RN, Seal CK, Staiger MP, Hyland MM. Topologically ordered magnesium-biopolymer hybrid composite structures. J Biomed Mater Res A. 2014;103(1):311–7.
Walter R, Kannan MB, He Y, Sandham A. Effect of surface roughness on the in vitro degradation behaviour of a biodegradable magnesium-based alloy. Appl Surf Sci. 2013;279:343–8.
Walter R, Kannan MB. Influence of surface roughness on the corrosion behaviour of magnesium alloy. Mater Design. 2011;32(4):2350–4.
Suzuki K, Aoki K, Ohya K. Effects of surface roughness of titanium implants on bone remodeling activity of femur in rabbits. Bone. 1997;21(6):507–14.
Von Der Hoh N, Bormann D, Lucas A, Denkena B, Hackenbroich C, Meyer-Lindenberg A. Influence of different surface machining treatments of magnesium-based resorbable implants on the degradation behavior in rabbits. Adv Eng Mater. 2009;11(5):B47–54.
Allen KW, Hatzinikolaou T, Armstrong KB. A comparison of acrylic adhesives for bonding aluminum alloys after using various surface preparation methods. Int J Adhes Adhes. 1984;4(3):133–6.
Molitor P, Barron V, Young T. Surface treatment of titanium for adhesive bonding to polymer composites: a review. Int J Adhes Adhes. 2001;21(2):129–36.
Rojaee R, Fathi M, Raeissi K. Controlling the degradation rate of AZ91 magnesium alloy via sol-gel derived nanostructured hydroxyapatite coating. Mat Sci Eng C Mater. 2013;33(7):3817–25.
Waterman J, et al. Corrosion resistance of biomimetic calcium phosphate coatings on magnesium due to varying pretreatment time. Mater Sci Eng B. 2011;176(20):1756–60.
Tomozawa M, Hiromoto S. Microstructure of hydroxyapatite-and octacalcium phosphate-coatings formed on magnesium by a hydrothermal treatment at various pH values. Acta Materialia. 2011;59(1):355–63.
Rojaee R, Fathi M, Raeissi K. Electrophoretic deposition of nanostructured hydroxyapatite coating on AZ91 magnesium alloy implants with different surface treatments. Appl Surf Sci. 2013;285(Part B):664–73.
Guan R-G, Johnson I, Cui T, Zhao T, Zhao Z-Y, Li X, Liu H. Electrodeposition of hydroxyapatite coating on Mg-4.0Zn-1.0Ca-0.6Zr alloy and in vitro evaluation of degradation, hemolysis, and cytotoxicity. J Biomed Mater Res A. 2012;100A:999–1015.
Conceicao d, Thiago F, et al. Corrosion protection of magnesium AZ31 alloy using poly (ether imide)[PEI] coatings prepared by the dip coating method: Influence of solvent and substrate pre-treatment. Corr Sci. 2011;53(1):338–46.
Abdal-hay A, Barakat NAM, Lim JK. Influence of electrospinning and dip-coating techniques on the degradation and cytocompatibility of Mg-based alloy. Coll Surf A Physicochem Eng Aspects. March 2013;420(5):37–45.
Sun J, Zhu Y, Meng L, Chen P, Shi T, Liu X, Zheng Y. Electrophoretic deposition of colloidal particles on Mg with cytocompatibility, antibacterial performance, and corrosion resistance. Acta Biomaterialia. Volume. 2016;45(1):387–98.
Sebaa M, Nguyen TY, Dhillon S, Garcia S, Liu H. The effects of poly(3, 4-ethylenedioxythiophene) (PEDOT) coating on magnesium degradation and cytocompatibility with human embryonic stem cells for potential neural applications. J Biomed Mater Res A. 2015;103(1):25–37.
Xu LP, Yamamoto A. Characteristics and cytocompatibility of biodegradable polymer film on magnesium by spin coating. Colloid Surface B Biointerfaces. 2012;93:67–74.
Li LC, Gao JC, Wang Y. Evaluation of cyto-toxicity and corrosion behavior of alkali-heat-treated magnesium in simulated body fluid. Surf Coat Technol. 2004;185(1):92–8.
Gu XN, Zheng W, Cheng Y, Zheng YF. A study on alkaline heat treated Mg-Ca alloy for the control of the biocorrosion rate. Acta Biomater. 2009;5(7):2790–9.
Al-Abdullat Y, Tsutsumi S, Nakajima N, Ohta M, Kuwahara H, Ikeuchi K. Surface modification of magnesium by NaHCO(3) and corrosion behavior in Hank’s solution for new biomaterial applications. Mater Trans. 2001;42(8):1777–80.
Lorenz C, Brunner JG, Kollmannsberger P, Jaafar L, Fabry B, Virtanen S. Effect of surface pre-treatments on biocompatibility of magnesium. Acta Biomater. 2009;5(7):2783–9.
Tan L, Wang Q, Lin X, Wan P, Zhang G, Zhang Q, Yang K. Loss of mechanical properties in vivo and bone-implant interface strength of AZ31B magnesium alloy screws with Si-containing coating. Acta Biomater. 2014;10(5):2333–40.
Tsn SN, Park IS, Lee MH. Tailoring the composition of fluoride conversion coatings to achieve better corrosion protection of magnesium for biomedical applications. J Mater Chem B. 2014. https://doi.org/10.1039/c3tb21565b.
Chen XB, Nisbet DR, Li RW, Smith PN, Abbott TB, Easton MA, Zhang DH, Birbilis N. Controlling initial biodegradation of magnesium by a biocompatible strontium phosphate conversion coating. Acta Biomater. 2014;10(3):1463–74.
Ke C, Pohl K, Birbilis N, Chen X-B. Protective strontium phosphate coatings for magnesium biomaterials. Mater Sci Technol. 2014;30(5):521–6.
Kim EJ, Bu SY, Sung MK, Choi MK. Effects of silicon on osteoblast activity and bone mineralization of MC3T3-E1 cells. Biol Trace Elem Res. 2013;152(1):105–12.
Sun H, Wu C, Dai K, Chang J, Tang T. Proliferation and osteoblastic differentiation of human bone marrow-derived stromal cells on akermanite-bioactive ceramics. Biomaterials. 2006;27(33):5651–7.
Sun JE, Wang JB, Jiang HF, Chen MF, Bi YZ, Liu DB. In vivo comparative property study of the bioactivity of coated Mg-3Zn-0.8Zr alloy. Mat Sci Eng C Mater. 2013;33(6):3263–72.
Yan T, Tan L, Zhang B, Yang K. Fluoride conversion coating on biodegradable AZ31B magnesium alloy. J Mater Sci Technol. 2014;30:666–74.
Zhao N, Workman B, Zhu DH. Endothelialization of novel magnesium-rare earth alloys with fluoride and collagen coating. Int J Mol Sci. 2014;15(4):5263–76.
Chai LY, Yu X, Yang ZH, Wang YY, Okido M. Anodizing of magnesium alloy AZ31 in alkaline solutions with silicate under continuous sparking. Corros Sci. 2008;50(12):3274–9.
Xue DC, Yun YH, Schulz MJ, Shanov V. Corrosion protection of biodegradable magnesium implants using anodization. Mat Sci Eng C Mater. 2011;31(2):215–23.
Murakami K, Hino M, Nakai K, Kobayashi S, Saijo A, Kanadani T. Mechanism of corrosion protection of anodized magnesium alloys. Mater Trans. 2008;49(5):1057–64.
Jo JH, Hong JY, Shin KS, Kim HE, Koh YH. Enhancing biocompatibility and corrosion resistance of Mg implants via surface treatments. J Biomater Appl. 2012;27(4):469–76.
Fischerauer SF, Kraus T, Wu X, Tangl S, Sorantin E, Hanzi AC, Loffler JF, Uggowitzer PJ, Weinberg AM. In vivo degradation performance of micro-arc-oxidized magnesium implants: a micro-CT study in rats. Acta Biomater. 2013;9(2):5411–20.
Seyfoori A, Mirdamadi S, Mehrjoo M, Khavandi A. In-vitro assessments of micro arc oxidized ceramic films on AZ31 magnesium implant: degradation and cell-surface response. Prog Nat Sci Mater. 2013;23(4):425–33.
Lin X, Wang X, Tan LL, Wan P, Yu XM, Li Q, Yang K. Effect of preparation parameters on the properties of hydroxyapatite containing micro-arc oxidation coating on biodegradable ZK60 magnesium alloy. Ceram Int. 2014;40(7):10043–51.
Ghasemi A, Raja VS, Blawert C, Dietzel W, Kainer KU. Study of the structure and corrosion behavior of PEO coatings on AM50 maginesium. alloy by electrochemical impedance spectroscopy. Surf Coat Techol. 2008;202(15):3513–8.
Robinson HJ, Markaki AE, Collier CA, Clyne TW. Cell adhesion to plasma electrolytic oxidation (PEO) titania coatings, assessed using a centrifuging technique. J Mech Behav Biomed Mater. 2011;4(8):2103–12.
Sharma AK, Uma Rani R, Giri K. Studies on anodization of magnesium alloy for thermal control applications. Met Finish. 1997;95(3):43–51.
Song GL. Corrosion prevention of magnesium alloys. Amsterdam: Elsevier Science; 2013.
Dey A, Rani RU, Thota HK, Sharma AK, Bandyopadhyay P, Mukhopadhyay AK. Microstructural, corrosion and nanomechanical behaviour of ceramic coatings developed on magnesium AZ31 alloy by micro arc oxidation. Ceram Int. 2013;39(3):3313–20.
Chen Z, Mao X, Tan L, Friis T, Wu C, Crawford R, Xiao Y. Osteoimmunomodulatory properties of magnesium scaffolds coated with beta-tricalcium phosphate. Biomaterials. 2014;35(30):8553–65.
Liu GY, Tang SW, Li DC, Hu J. Self-adjustment of calcium phosphate coating on micro-arc oxidized magnesium and its influence on the corrosion behaviour in simulated body fluids. Corros Sci. 2014;79:206–14.
Qiu X, Wan P, Tan LL, Fan XM, Yang K. Preliminary research on a novel bioactive silicon doped calcium phosphate coating on AZ31 magnesium alloy via electrodeposition. Mat Sci Eng C Mater. 2014;36:65–76.
Ergun C, Liu HN, Halloran JW, Webster TJ. Increased osteoblast adhesion on nanograined hydroxyapatite and tricalcium phosphate containing calcium titanate. J Biomed Mater Res A. 2007;80A(4):990–7.
Sonmez S, Aksakal B, Dikici B. Influence of hydroxyapatite coating thickness and powder particle size on corrosion performance of MA8M magnesium alloy. J Alloys Compd. 2014;596:125–31.
Guan F, Ma S, Shi X, Ma X, Chi L, Liang S, Cui Y, Wang Z, Yao N, Guan S, Yang B. Biocompatibility of nano-hydroxyapatite/Mg-Zn-Ca alloy composite scaffolds to human umbilical cord mesenchymal stem cells from Wharton’s jelly in vitro. Sci China Life Sci. 2014;57(2):181–7.
Ye XY, Cai S, Xu GH, Dou Y, Hu HT, Ye XJ, Zhao H, Sun XH. The influence of mesopores on the corrosion resistance of hydroxyapatite coated AZ31 Mg alloy. J Electrochem Soc. 2014;161(3):C145–50.
Yang JX, Cui FZ, Lee IS, Zhang Y, Yin QS, Xia H, Yang SX. In vivo biocompatibility and degradation behavior of Mg alloy coated by calcium phosphate in a rabbit model. J Biomater Appl. 2012;27(2):153–64.
Shadanbaz S, Walker J, Woodfield TBF, Staiger MP, Dias GJ. Monetite and brushite coated magnesium: in vivo and in vitro models for degradation analysis. J Mater Sci Mater M. 2014;25(1):173–83.
Zhang Y, Zhang G, Wei M. Controlling the biodegradation rate of magnesium using biomimetic apatite coating. J Biomed Mater Res B Appl Biomater. 2009;89((2):408–14.
Wang BC, Chang E, Lee TM, Yang CY. Changes in phases and crystallinity of plasma-sprayed hydroxyapatite coatings under heat-treatment—a quantitative study. J Biomed Mater Res. 1995;29(12):1483–92.
Hahn BD, Park DS, Choi JJ, Ryu JH, Yoon WH, Choi JH, Kim HE, Kim SG. Aerosol deposition of hydroxyapatite-chitosan composite coatings on biodegradable magnesium alloy. Surf Coat Techol. 2011;205(8–9):3112–8.
Bai KF, Zhang Y, Fu ZY, Zhang CL, Cui XZ, Meng EC, Guan SK, Hu JH. Fabrication of chitosan/magnesium phosphate composite coating and the in vitro degradation properties of coated magnesium alloy. Mater Lett. 2012;73:59–61.
Gu XN, Zheng YF, Lan QX, Cheng Y, Zhang ZX, Xi TF, Zhang DY. Surface modification of an Mg-1Ca alloy to slow down its biocorrosion by chitosan. Biomed Mater. 2009;4(4):044109.
Fekry AM, Ghoneim AA, Ameer MA. Electrochemical impedance spectroscopy of chitosan coated magnesium alloys in a synthetic sweat medium. Surf Coat Techol. 2014;238:126–32.
Zhao J, Chen L, Yu K, Chen C, Dai Y, Qiao X, Yan Y. Biodegradation performance of a chitosan coated magnesium-zinc-tricalcium phosphate composite as an implant. Biointerphases. 2014;9(3):031004.
Kumar MNVR. A review of chitin and chitosan applications. React Funct Polym. 2000;46(1):1–27.
Seol YJ, Lee JY, Park YJ, Lee YM, Young-Ku ICR, Lee SJ, Han SB, Chung CP. Chitosan sponges as tissue engineering scaffolds for bone formation. Biotechnol Lett. 2004;26(13):1037–41.
Kong M, Chen XG, Xing K, Park HJ. Antimicrobial properties of chitosan and mode of action: a state of the art review. Int J Food Microbiol. 2010;144(1):51–63.
Benhabiles S, Salah R, Lounici H, Drouiche N, Goosen MFA, Mameri N. Antibacterial activity of chitin, chitosan and its oligomers prepared from shrimp shell waste. Food Hydrocolloid. 2012;29(1):48–56.
Raafat D, von Bargen K, Haas A, Sahl HG. Insights into the mode of action of chitosan as an antibacterial compound. Appl Environ Microbiol. 2008;74(12):3764–73.
Kean T, Thanou M. Biodegradation, biodistribution and toxicity of chitosan. Adv Drug Deliv Rev. 2010;62(1):3–11.
Sangeetha K, Roy A, Singh S, Lee B, Kumta PN. Novel alginate based coatings on Mg alloys. Mater Sci Eng B Adv. 2011;176(20):1703–10.
Kunjukunju S, Roy A, Ramanathan M, Lee B, Candiello JE, Kumta PN. A layer-by-layer approach to natural polymer-derived bioactive coatings on magnesium alloys. Acta Biomater. 2013;9(10):8690–703.
Christensen BE. Alginates as biomaterials in tissue engineering. Carbohydr Chem. 2012;37:227–58.
Rowley JA, Madlambayan G, Mooney DJ. Alginate hydrogels as synthetic extracellular matrix materials. Biomaterials. 1999;20(1):45–53.
Park CH, Pant HR, Kim CS. Effect on corrosion behavior of collagen film/fiber coated Az31 magnesium alloy. Dig J Nanomater Bios. 2013;8(3):1227–34.
Wagener V, Killian MS, Turhan CM, Virtanen S. Albumin coating on magnesium via linker molecules-comparing different coating mechanisms. Colloid Surface B Biointerfaces. 2013;103:586–94.
Liu JR, Guo YN, Huang WD. Phytic acid conversion coatings on magnesium surface treatment with cerium chloride solution. Prot Met Phys Chem+. 2012;48(2):233–7.
Pan FS, Yang X, Zhang DF. Chemical nature of phytic acid conversion coating on AZ61 magnesium alloy. Appl Surf Sci. 2009;255(20):8363–71.
Yang X, Li L, He J, Guo H, Zhang J. In vitro corrosion and bioactivity study of surface phytic acid modified AZ31 magnesium alloy. Mater Sci Appl. 2014;5(2):59–65.
Cui W, Beniash E, Gawalt E, Xu Z, Sfeir C. Biomimetic coating of magnesium alloy for enhanced corrosion resistance and calcium phosphate deposition. Acta Biomater. 2013;9(10):8650–9.
Friess W. Collagen—biomaterial for drug delivery. Eur J Pharm Biopharm. 1998;45(2):113–36.
Lim LT, Auras R, Rubino M. Processing technologies for poly(lactic acid). Prog Polym Sci. 2008;33(8):820–52.
Gunatillake PA, Adhikari R. Biodegradable synthetic polymers for tissue engineering. Eur Cell Mater. 2003;5:1–16. discussion 16
Xu L, Yamamoto A. In vitro degradation of biodegradable polymer-coated magnesium under cell culture condition. Appl Surf Sci. 2012;258(17):6353–8.
Kannan MB, Liyanaarachchi S. Hybrid coating on a magnesium alloy for minimizing the localized degradation for load-bearing biodegradable mini-implant applications. Mater Chem Phys. 2013;142(1):350–4.
Bos RR, Rozema FR, Boering G, Nijenhuis AJ, Pennings AJ, Verwey AB, Nieuwenhuis P, Jansen HW. Degradation of and tissue reaction to biodegradable poly(L-lactide) for use as internal fixation of fractures: a study in rats. Biomaterials. 1991;12(1):32–6.
Barber FA, Dockery WD. Long-term absorption of poly-L-lactic acid interference screws. Arthroscopy. 2006;22(8):820–6.
Stahelin AC, Weiler A, Rufenacht H, Hoffmann R, Geissmann A, Feinstein R. Clinical degradation and biocompatibility of different bioabsorbable interference screws: a report of six cases. Arthroscopy. 1997;13(2):238–44.
Fraser RK, Cole WG. Osteolysis after biodegradable pin fixation of fractures in children. J Bone Joint Surg Br. 1992;74(6):929–30.
Askar I, Gultan S, Erden E, Yormuk E. Effects of polyglycolic acid bioabsorbable membrane and oxidised cellulose on the osteogenesis in bone defects: an experimental study. Acta Chir Plast. 2002;45(4):131–8.
Cutright DE, Beasley JD, Perez B. Histologic comparison of polylactic and polyglycolic acid sutures. Oral Surg Oral Med O. 1971;32(1):165–73.
Huang YX, Ren J, Chen C, Ren TB, Zhou XY. Preparation and properties of poly(lactide-co-glycolide) (PLGA)/nano-hydroxyapatite (NHA) scaffolds by thermally induced phase separation and rabbit MSCs culture on scaffolds. J Biomater Appl. 2008;22(5):409–32.
Smith LJ, Swaim JS, Yao C, Haberstroh KM, Nauman EA, Webster TJ. Increased osteoblast cell density on nanostructured PLGA-coated nanostructured titanium for orthopedic applications. Int J Nanomedicine. 2007;2(3):493–9.
You Y, Lee SW, Youk JH, Min BM, Lee SJ, Park WH. In vitro degradation behaviour of non-porous ultra-fine poly(glycolic acid)/poly(L-lactic acid) fibres and porous ultra-fine poly(glycolic acid) fibres. Polym Degrad Stab. 2005;90(3):441–8.
Lu L, Peter SJ, Lyman MD, Lai HL, Leite SM, Tamada JA, Uyama S, Vacanti JP, Langer R, Mikos AG. In vitro and in vivo degradation of porous poly(DL-lactic-co-glycolic acid) foams. Biomaterials. 2000;21(18):1837–45.
Ostrowski NJ, Lee B, Roy A, Ramanathan M, Kumta PN. Biodegradable poly(lactide-co-glycolide) coatings on magnesium alloys for orthopedic applications. J Mater Sci Mater Med. 2013;24(1):85–96.
Li JN, Cao P, Zhang XN, Zhang SX, He YH. In vitro degradation and cell attachment of a PLGA coated biodegradable Mg-6Zn based alloy. J Mater Sci. 2010;45(22):6038–45.
Lee SJ, Khang G, Lee YM, Lee HB. Interaction of human chondrocytes and NIH/3T3 fibroblasts on chloric acid-treated biodegradable polymer surfaces. J Biomater Sci Polym Ed. 2002;13(2):197–212.
Kanczler JM, Oreffo RO. Osteogenesis and angiogenesis: the potential for engineering bone. Eur Cell Mater. 2008;15:100–14.
Abdal-hay A, Amna T, Lim JK. Biocorrosion and osteoconductivity of PCL/nHAp composite porous film-based coating of magnesium alloy. Solid State Sci. 2013;18:131–40.
Jo JH, Li Y, Kim SM, Kim HE, Koh YH. Hydroxyapatite/poly(epsilon-caprolactone) double coating on magnesium for enhanced corrosion resistance and coating flexibility. J Biomater Appl. 2013;28(4):617–25.
Wong K, Yeung K, Lam J, Chu P, Luk K, Cheung K. Reduction of corrosion behavior of magnesium alloy by PCL surface treatment. In: 55th Annual Meeting of the Orthopaedic Research Society, USA; 2009. p. 22–25.
Woodruff MA, Hutmacher DW. The return of a forgotten polymer-polycaprolactone in the 21st century. Prog Polym Sci. 2010;35(10):1217–56.
Mobedi H, Nekoomanesh M, Orafaei H, Mivehchi H. Studying the degradation of poly(L-lactide) in presence of magnesium hydroxide. Iran Polym J. 2006;15(1):31–9.
Zhu B, Xu Y, Sun J, Yang L, Guo C, Liang J, Cao B. Preparation and characterization of aminated hydroxyethyl cellulose-induced biomimetic hydroxyapatite Coatings on the AZ31 magnesium alloy. Metals. 2017;7(6):214.
Soujanya GK, Hanas T, Chakrapani VY, Sunil BR, Kumar TS. Electrospun nanofibrous polymer coated magnesium alloy for biodegradable implant applications. Procedia Mater Sci. 2014;5:817–23.
Sun J, Zhu Y, Meng L, Wei W, Li Y, Liu X, Zheng Y. Controlled release and corrosion protection by self-assembled colloidal particles electrodeposited onto magnesium alloys. J Mater Chem B. 2015;3(8):1667–76.
Ikada Y, Tsuji H. Biodegradable polyesters for medical and ecological applications. Macromol Rapid Comm. 2000;21(3):117–32.
Park TG. Degradation of poly(lactic-Co-glycolic acid) microspheres—effect of copolymer composition. Biomaterials. 1995;16(15):1123–30.
Shogren R. Water vapor permeability of biodegradable polymers. J Environ Polym Degr. 1997;5(2):91–5.
Bai H, Huang C, Xiu H, Zhang Q, Deng H, Wang K, Chen F, Fu Q. Significantly improving oxygen barrier properties of polylactide via constructing parallel-aligned shish-kebab-like crystals with well-interlocked boundaries. Biomacromolecules. 2014;15(4):1507–14.
Tsuji H, Okino R, Daimon H, Fujie K. Water vapor permeability of poly(lactide)s: effects of molecular characteristics and crystallinity. J Appl Polym Sci. 2006;99(5):2245–52.
Park A, Cima LG. In vitro cell response to differences in poly-L-lactide crystallinity. J Biomed Mater Res. 1996;31(1):117–30.
Loo SCJ, Ooi CP, Wee SHE, Boey YCF. Effect of isothermal annealing on the hydrolytic degradation rate of poly(lactide-co-glycolide) (PLGA). Biomaterials. 2005;26(16):2827–33.
Cao Y, Croll TI, Oconnor AJ, Stevens GW, Cooper-White JJ. Systematic selection of solvents for the fabrication of 3D combined macro- and microporous polymeric scaffolds for soft tissue engineering. J Biomater Sci Polym Ed. 2006;17(4):369–402.
Asran AS, Salama M, Popescu C, Michler GH. Solvent influences the morphology and mechanical properties of electrospun poly(L-lactic acid) scaffold for tissue engineering applications. Macromol Symp. 2010;294(1):153–61.
Shuying G, Zhimei W, Jie R, Chunyan Z. Fabrication and characterization of electrospun poly(L-lactic acid)and poly(L-Lactide-Co-glycolide) mats as wound dressing, bioinformatics and biomedical engineering, ICBBE 2008. In: The 2nd International Conference on, 2008. p. 1514–7.
Ero-Phillips O, Jenkins M, Stamboulis A. Tailoring crystallinity of electrospun plla fibres by control of electrospinning parameters. Polymers. 2012;4(3):1331–48.
Qin XH, Wu DQ. Effect of different solvents on poly(caprolactone) (PCL) electrospun nonwoven membranes. J Therm Anal Calorim. 2012;107(3):1007–13.
Johnson I, Tian Q, Liu H. Nanostructured ceramic and ceramic-polymer composites as dual functional interface for bioresorbable metallic implants. MRS Online Proc Library. 2014;1621:39–45.
Liu HN, Webster TJ. Mechanical properties of dispersed ceramic nanoparticles in polymer composites for orthopedic applications. Int J Nanomedicine. 2010;5:299–313.
Liu HN, Webster TJ. Enhanced biological and mechanical properties of well-dispersed nanophase ceramics in polymer composites: from 2D to 3D printed structures. Mat Sci Eng C Mater. 2011;31(2):77–89.
Wei G, Ma PX. Structure and properties of nano-hydroxyapatite/polymer composite scaffolds for bone tissue engineering. Biomaterials. 2004;25(19):4749–57.
Ebrahimian-Hosseinabadi M, Ashrafizadeh F, Etemadifar M, Venkatraman SS. Evaluating and modeling the mechanical properties of the prepared PLGA/nano-BCP composite scaffolds for bone tissue engineering. J Mater Sci Technol. 2011;27(12):1105–12.
Johnson I, Wang SM, Silken C, Liu H. A systemic study on key parameters affecting nanocomposite coatings on magnesium substrates. Acta Biomater. 2016;36:332–49.
Tian QM, Liu HN. Electrophoretic deposition and characterization of nanocomposites and nanoparticles on magnesium substrates. Nanotechnology. 2015;26(17):175102.
Tian QM, Rivera-Castaneda L, Liu HN. Optimization of of nano-hydroxyapatite/poly(lactic-co-glycolic acid) coatings on magnesium substrates using one-step electrophoretic deposition. Mater Lett. 2017;186:12–6.
Akagi H, Iwata M, Ichinohe T, Amimoto H, Hayashi Y, Kannno N, Ochi H, Fujita Y, Harada Y, Tagawa M, Hara Y. Hydroxyapatite/poly-L-lactide acid screws have better biocompatibility and femoral burr hole closure than does poly-L-lactide acid alone. J Biomater Appl. 2014;28(6):954–62.
Abdal-hay A, Barakat NAM, Lim JK. Hydroxyapatite-doped poly(lactic acid) porous film coating for enhanced bioactivity and corrosion behavior of AZ31 Mg alloy for orthopedic applications. Ceram Int. 2013;39(1):183–95.
Lock J, Nguyen TY, Liu H. Nanophase hydroxyapatite and poly(lactide-co-glycolide) composites promote human mesenchymal stem cell adhesion and osteogenic differentiation in vitro. J Mater Sci Mater Med. 2012;23(10):2543–52.
D’Anto V, Raucci MG, Guarino V, Martina S, Valletta R, Ambrosio L. Behaviour of human mesenchymal stem cells on chemically synthesized HA-PCL scaffolds for hard tissue regeneration. J Tissue Eng Regen Med. 2013;10(2):E147–54.
Ngiam M, Liao SS, Patil AJ, Cheng ZY, Chan CK, Ramakrishna S. The fabrication of nano-hydroxyapatite on PLGA and PLGA/collagen nanofibrous composite scaffolds and their effects in osteoblastic behavior for bone tissue engineering. Bone. 2009;45(1):4–16.
Hasegawa S, Ishii S, Tamura J, Furukawa T, Neo M, Matsusue Y, Shikinami Y, Okuno M, Nakamura T. A 5-7 year in vivo study of high-strength hydroxyapatite/poly(L-lactide) composite rods for the internal fixation of bone fractures. Biomaterials. 2006;27(8):1327–32.
Shikinami Y, Matsusue Y, Nakamura T. The complete process of bioresorption and bone replacement using devices made of forged composites of raw hydroxyapatite particles/poly L-lactide (F-u-HA/PLLA). Biomaterials. 2005;26(27):5542–51.
Barber FA, Dockery WD. Long-term absorption of beta-tricalcium phosphate poly-L-lactic acid interference screws. Arthroscopy. 2008;24(4):441–7.
Kobayashi M, Rharbi Y, Brauge L, Cao L, Winnik MA. Effect of silica as fillers on polymer interdiffusion in poly(butyl methacrylate) latex films. Macromolecules. 2002;35(19):7387–99.
Ma X, Zhu SJ, Wang LG, Ji CX, Ren CX, Guan SK. Synthesis and properties of a bio-composite coating formed on magnesium alloy by one-step method of micro-arc oxidation. J Alloy Compd. 2014;590:247–53.
Pan Y, Chen C, Wang D, Zhao T. Effects of phosphates on microstructure and bioactivity of micro-arc oxidized calcium phosphate coatings on Mg–Zn–Zr magnesium alloy. Colloids Surf B Biointerfaces. 2013;109:1–9.
Qu L, Li M, Liu M, Zhang E, Ma C. Microstructure and corrosion resistance of ultrasonic micro-arc oxidation biocoatings on magnesium alloy. J Adv Ceram. 2013;2(3):227–34.
Liu G, Hu J, Ding Z, Wang C. Bioactive calcium phosphate coating formed on micro-arc oxidized magnesium by chemical deposition. Appl Surf Sci. 2011;257(6):2051–7.
Tang H, Yu D, Luo Y, Wang F. Preparation and characterization of HA microflowers coating on AZ31 magnesium alloy by micro-arc oxidation and a solution treatment. Appl Surf Sci. 2013;264:816–22.
Gao J, Guan S, Chen J, Wang L, Zhu S, Hu J, Ren Z. Fabrication and characterization of rod-like nano-hydroxyapatite on MAO coating supported on Mg–Zn–Ca alloy. Appl Surf Sci. 2011;257(6):2231–7.
Zhao QM, Guo X, Dang XQ, Hao JM, Lai JH, Wang KZ. Preparation and properties of composite MAO/ECD coatings on magnesium alloy. Colloid Surface B Biointerfaces. 2013;102:321–6.
Alabbasi A, Kannan MB, Blawert C. Dual layer inorganic coating on magnesium for delaying the biodegradation for bone fixation implants. Mater Lett. 2014;124:188–91.
Razavi M, Fathi M, Savabi O, Beni BH, Razavi SM, Vashaee D, Tayebi L. Coating of biodegradable magnesium alloy bone implants using nanostructured diopside (CaMgSi2O6). Appl Surf Sci. 2014;288:130–7.
Razavi M, Fathi M, Savabi O, Beni BH, Vashaee D, Tayebi L. Nanostructured merwinite bioceramic coating on Mg alloy deposited by electrophoretic deposition. Ceram Int. 2014;40(7):9473–84.
Razavi M, Fath M, Savabi O, Razavi SM, Beni BH, Vashaee D, Tayebi L. Controlling the degradation rate of bioactive magnesium implants by electrophoretic deposition of akermanite coating. Ceram Int. 2014;40(3):3865–72.
Razavi M, Fathi M, Savabi O, Razavi SM, Heidari F, Manshaei M, Vashaee D, Tayebi L. In vivo study of nanostructured diopside (CaMgSi2O6) coating on magnesium alloy as biodegradable orthopedic implants. Appl Surf Sci. 2014;313:60–6.
Guo MQ, Cao L, Lu P, Liu Y, Xu XH. Anticorrosion and cytocompatibility behavior of MAO/PLLA modified magnesium alloy WE42. J Mater Sci Mater Med. 2011;22(7):1735–40.
Alabbasi A, Mehjabeen A, Kannan MB, Ye Q, Blawert C. Biodegradable polymer for sealing porous PEO layer on pure magnesium: an in vitro degradation study. Appl Surf Sci. 2014;301:463–7.
Ostrowski N, Lee B, Enick N, Carlson B, Kunjukunju S, Roy A, Kumta PN. Corrosion protection and improved cytocompatibility of biodegradable polymeric layer-by-layer coatings on AZ31 magnesium alloys. Acta Biomater. 2013;9(10):8704–13.
Lu P, Cao L, Liu Y, Xu XH, Wu XF. Evaluation of magnesium ions release, biocorrosion, and hemocompatibility of MAO/PLLA-modified magnesium alloy WE42. J Biomed Mater Res B. 2011;96B(1):101–9.
Wei Z, Tian P, Liu X, Zhou B. In vitro degradation, hemolysis, and cytocompatibility of PEO/PLLA composite coating on biodegradable AZ31 alloy. J Biomed Mater Res B Appl Biomater. 2015;103(2):342–54.
Gnedenkov SV, Sinebryukhov SL, Zavidnaya AG, Egorkin VS, Puz’ AV, Mashtalyar DV, Sergienko VI, Yerokhin AL, Matthews A. Composite hydroxyapatite–PTFE coatings on Mg–Mn–Ce alloy for resorbable implant applications via a plasma electrolytic oxidation-based route. J Taiwan Inst Chem Eng. 2014;45:3104–9.
Gnedenkov SV, Sinebryukhov SL, Mashtalyar DV, Egorkin VS, Sidorova MV, Gnedenkov AS. Composite polymer-containing protective coatings on magnesium alloy MA8. Corros Sci. 2014;85(0):52–9.
Li L-H, Sankara Narayanan TSN, Kim YK, Kong Y-M, Park IS, Bae TS, Lee MH. Deposition of microarc oxidation–polycaprolactone duplex coating to improve the corrosion resistance of magnesium for biodegradable implants. Thin Solid Films. 2014;562(0):561–7.
Wei Z, Tian P, Liu X, Zhou B. Hemocompatibility and selective cell fate of polydopamine-assisted heparinized PEO/PLLA composite coating on biodegradable AZ31 alloy. Colloids Surf B Biointerfaces. 2014;121:451–60.
Qi ZR, Zhang Q, Tan LL, Lin X, Yin Y, Wang XL, Yang K, Wang Y. Comparison of degradation behavior and the associated bone response of ZK60 and PLLA in vivo. J Biomed Mater Res A. 2014;102(5):1255–63.
Xu X, Lu P, Guo M, Fang M. Cross-linked gelatin/nanoparticles composite coating on micro-arc oxidation film for corrosion and drug release. Appl Surf Sci. 2010;256(8):2367–71.
Lu P, Fan HN, Liu Y, Cao L, Wu XF, Xu XH. Controllable biodegradability, drug release behavior and hemocompatibility of PTX-eluting magnesium stents. Colloid Surface B Biointerfaces. 2011;83(1):23–8.
Luo XL, Cui XYT. Electrochemical deposition of conducting polymer coatings on magnesium surfaces in ionic liquid. Acta Biomater. 2011;7(1):441–6.
Liu H, Webster TJ. Ceramic/polymer nanocomposites with tunable drug delivery capability at specific disease sites. J Biomed Mater Res A. 2010;93(3):1180–92.
Wong HM, et al. A biodegradable polymer-based coating to control the performance of magnesium alloy orthopaedic implants. Biomaterials. 2010;31(8):2084–96.
Razavi M, et al. Biodegradation, bioactivity and in vivo biocompatibility analysis of plasma electrolytic oxidized (PEO) biodegradable Mg implants. Phys Sci Inter J. 2014;4(5):708.
Lu P, et al. Evaluation of magnesium ions release, biocorrosion, and hemocompatibility of MAO/PLLA‐modified magnesium alloy WE42. J Biomed Mater Res B Appl Biomater. 2011;96(1):101–9.
Tan L -l, et al. Preparation and characterization of Ca-P coating on AZ31 magnesium alloy. Trans Nonferrous Metals Soc China. 2010;20:s648–54.
Wang J, et al. A surface-eroding poly (1, 3-trimethylene carbonate) coating for fully biodegradable magnesium-based stent applications: toward better biofunction, biodegradation and biocompatibility. Acta Biomater. 2013;9(10):8678–89.
Yang X, et al. Enhanced in vitro biocompatibility/bioactivity of biodegradable Mg–Zn–Zr alloy by micro-arc oxidation coating contained Mg2 SiO4. Surf Coat Technol. 2013;233:65–73.
Acknowledgement
The authors thank U.S. National Science Foundation (Award 1512764, 1125801) and National Institutes of Health (Award 1R03AR069373-01) for financial support. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Science Foundation and National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2017 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Johnson, I., Lin, J., Liu, H. (2017). Surface Modification and Coatings for Controlling the Degradation and Bioactivity of Magnesium Alloys for Medical Applications. In: Li, B., Webster, T. (eds) Orthopedic Biomaterials. Springer, Cham. https://doi.org/10.1007/978-3-319-73664-8_13
Download citation
DOI: https://doi.org/10.1007/978-3-319-73664-8_13
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-73663-1
Online ISBN: 978-3-319-73664-8
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)