Abstract
Background
The annually recorded incidence of primary hepatic carcinomas has significantly increased over the past two decades accounting for over 800 thousand of annual deaths caused by hepatocellular carcinoma (HCC) alone globally. Further, secondary liver malignancies are much more widespread compared to primary hepatic carcinomas: almost all solid malignancies are able to metastasise into the liver. The primary tumours most frequently metastasising to the liver are breast followed by colorectal carcinomas. Given the increased incidence of both primary and metastatic liver cancers, a new, revised approach is needed to advance medical care based on predictive diagnostics, innovative screening programmes, targeted preventive measures, and patient stratification for treatment algorithms tailored to individualised patient profile.
Advantages of the approach taken
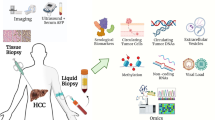
The current pilot study took advantage of systemic alterations characteristic for liver malignancies, utilising liquid biopsy (blood samples) and specific biomarker patterns detected. Key molecular pathways relevant for pathomechanisms of liver cancers have been considered opening a perspective for both—individualised diagnostics and targeted treatment. Systemic alterations have been analysed prior to the therapy application avoiding molecular biological effects potentially diminishing predictive power of the biomarker-panel proposed. Multi-omics at DNA and protein (both expression and activity) levels has been applied. An established biomarker panel is considered as a powerful tool for individualised patient profiling and improved multi-level diagnostics—both predictive and prognostic ones.
Results and conclusions
Biomarker panels have been created for the patient stratification, prediction of a more optimal therapy and prognosis of survival based on the individualised patient profiling. Although there are some limitations of the pilot study performed, the results are encouraging, as it may be possible, through further research along these lines, to find a clinically and cost-effective means of stratifying liver cancer patients for personalised care and therapy. The benefits to the patient and society of accurate treatment stratification cannot be overemphasised.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Heterogeneous population of liver malignancies: epidemiological concerns and operational basis for the paradigm shift in the disease management
Worldwide, primary liver cancer is the sixth most common cancer, with a majority of the cases occurring in developing countries. As compared with other common cancers, such as breast, colorectal, lung, and stomach cancers, the incidence is increasing [1]. The annually recorded incidence of primary hepatic carcinomas has significantly increased over the past two decades accounting for over 800 thousand of annual deaths caused by hepatocellular carcinoma (HCC) alone globally [2]. Specifically modifiable risk factors have been demonstrated to be the major contributors to the development of HCC. In particular, widespread viral hepatic infections (hepatitis B and C) [3] and unhealthy lifestyle specifically linked to the abnormal alcohol consumption, physical inactivity and obesity, individually and/or synergistically, result in chronic inflammatory processes to the liver, fatty liver disease and cirrhosis [4].
Secondary liver malignancies are much more widespread compared to primary hepatic carcinomas: almost all solid malignancies are able to metastasise into the liver [4]. The primary tumours most frequently metastasising to the liver are breast followed by colorectal carcinomas. Further, 27% of the patients with primary lung, colon, or rectum cancers are reported to develop liver metastases [5].
As currently practiced, most healthcare systems are focused on “disease care” and the majority of patients with liver malignancies have advanced disease at the time of diagnosis. As a preferable alternative, it is amongst the goals of predictive, preventive and personalised medicine (PPPM) to provide comprehensive cost-effective care throughout all phases of disease starting with disease prediction before the clinical manifestation as well as providing detection at early stages and prognosis for individualised treatment algorithms. Finally, there is a great need for precise palliative care that is tailored to each patient to achieve satisfactory individual outcomes in a long-term manner.
There is currently a relative lack of reliable predictive and prognostic biomarkers for an advanced PPPM approach that hampers effective implementation of individualised patient profiles and patient stratification essential for tailoring treatment decisions [6]. Although there are tests based on biopsies such as immunohistochemistry for tumour characteristics and chemosensitivities, these tests are invasive, expensive and/or not widely available, applicable and/or affordable. Consequently, the applied approach is usually cost-ineffective, life quality of the affected patients is unsatisfactory and the life-expectance is particularly short.
There are relatively few projects dedicated to the development of specific biomarker-sets for the detection and/or evaluation of liver malignancies. A PubMed search specifically for “predictive biomarker panels” in “advanced liver carcinoma and/or metastasis” and “unresectable liver carcinoma/metastasis” revealed few articles for each item. This actuality provided motivation to use a minimally invasive approach utilising liquid biopsy in order to develop a powerful diagnostic tool for individualised patient profiling and patient stratification essential for tailoring treatment decisions.
Diversity of pathomechanisms and molecular landscape of liver malignancies relevant for predictive and prognostic approaches
Liver malignancies comprise a wide spectrum of cancers ranging from the primary hepatocellular carcinomas (1) to highly heterogeneous group of metastatic diseases which, further, discriminate between metastases spread by the locally situated abdominal primary tumours (e.g. colorectal cancer) (2) and distanced primary tumours such as the breast cancer (3). Consequently, pathomechanisms which underlie individual groups (1–3) of liver malignancies differ dramatically from each other being still poorly understood.
Even more challenging is the detection of a pathology- and stage-specific molecular signature for identifying individual cancer subtypes that would allow the adjustment of optimal treatment modalities and prognosis of individual outcomes. The task requires a comprehensive biomedical approach, since previous studies have demonstrated that an “ideal biomarker” does not exist. Therefore, the most reliable approach requires multi-level diagnostics with application of biomarker panels reflecting pathology/stage-specific alterations at molecular and subcellular levels [7].
Several affected pathways are usually considered for such a panel, to produce a highly sensitive and specific molecular “portrait”. Contextually, patients with hepatic breast cancer metastases demonstrate highly specific profiles of matrix metalloproteinases MMP-2 and MMP-9 after SIRT treatment as compared to other primary and secondary liver tumours [8]. Certainly, tissue remodelling is an essential attribute of aggressive metastatic disease; therefore, metalloproteinases as the key enzymes are strong predictors and prognostic factors in disease monitoring. Further, MMP profiles demonstrated specifically in blood provide strong arguments in favour of systemic processes which underlie liver malignancies [8]. In fact, several groups have recently published research data supporting the relevance of molecular patterns in blood for monitoring the therapy efficacy with sufficient prognostic power for individual outcomes such as lymphocyte-to-monocyte ratio [9], serum procalcitonin levels [10], serum alpha-fetoprotein levels [11, 12], interleukin-8 levels [13], serum fibrinogen levels [14] and serum annexin A3 levels [15].
Biomarker patterns non-invasively detected in blood samples may provide important insights into systemic pathomechanisms of liver malignancies. However, it is important to note that the majority of publications have correlated the overall survival with biomarkers measured after a therapeutic intervention that certainly may have a prognostic value estimating potential survival, however, in no way can be useful for choosing an optimal treatment modality. The focus of the current project is to identify biomarkers which will allow individualised patient profiling that is essential for tailoring treatments.
One of the decisive factors with strong predictive power for individual outcomes is the severity of underlying liver dysfunction that can be characterised as a dysfunction of detoxification pathways. The cause of the detoxification dysfunction differs amongst individual cases. However, the key players are well known, namely the superoxide-dismutase and catalase which are useful biomarkers estimating the systemic detoxification [16,17,18,19].
Particularly, under toxic conditions (deficient detoxification pathways), stress response is pivotal for estimating the efficacy of the DNA repair machinery and even for predicting the systemic capacity to regenerate after highly toxic therapy [20,21,22].
Finally, for estimating metastatic potential of many types of tumours, S100 (calgranulin) has been per evidence successfully implemented in predictive biomarker panels [23,24,25,26,27].
Working hypothesis
Based on the above provided evidence, the following hypotheses have been created:
-
1.
Multi-level diagnostic approach might improve a predictive power of diagnostic tools.
-
2.
Liquid biopsy might be useful source of diagnostic information: systemic alterations reflected in molecular and subcellular blood profiles underlie specific pathomechanisms crucial for predicting individual outcomes, if correlated with overall survival.
-
3.
Biomarker panel should include key-molecules driving tissue remodelling, detoxification, and metastasis potential as well as DNA quality indicators.
-
4.
Contextually, blood multi-omics might create a robust platform for individualised patient profiling.
-
5.
Predictive and prognostic approaches utilising individualised patient profiles can be implemented before therapeutic interventions, to enable an optimal choice of treatment modalities (such as selective internal radiation therapy, SIRT, versus transarterial chemoembolisation, TACE) tailored to the person.
Materials and methods
Recruitment of patients with primary hepatocellular carcinoma and secondary hepatic metastases
This study was designed as a “pilot study” for the identification of a multi-level biomarker screening panel for patients with primary and metastatic liver malignancies who would be undergoing SIRT or TACE. Therefore, a wide range of malignancies of different types were incorporated in the study. The blood tests for the screening panels were performed prior to SIRT or TACE.
A total of 158 patients, treated either by SIRT (126) or TACE (32), were considered for the study (Table 1).
Inclusion criteria:
-
Primary hepatocellular carcinoma
-
Hepatic metastases
-
Treatment by SIRT
-
Treatment by TACE
Exclusion criteria:
-
Pregnancy
-
Acute infections (but not chronic hepatitis)
-
Alcohol abuse
-
Genetic disorders and disorders with premature ageing (Down syndrome, Werner syndrome, Alzheimer’s disease, others)
All the patients were informed about the purposes of the study and consequently have signed their “consent of the patient”. All investigations conformed to the principles outlined in the Declaration of Helsinki and were performed with permission from the responsible Ethics Committee of the Medical Faculty, Rheinische Friedrich-Wilhelms-University of Bonn. Corresponding reference number is 283/10.
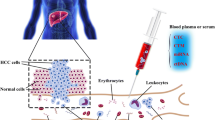
Liquid biopsy: blood samples collection, biobanking and biopreservation
Blood samples (20 ml) anti-coagulated with heparin were collected from the patients prior to any treatment application.
Biobanking: both peripheral leucocytes and blood serum were separated and stored for all follow-up analyses.
Peripheral leucocytes were isolated using Ficoll-Histopaque gradients (Histopaque 1077, Sigma, USA) as described elsewhere [28]. Briefly, blood samples were diluted with equal volumes of physiological buffer solution (PBS, Biochrom AG, Germany). Then, 2 ml of histopaque were placed into 10 ml sterile centrifuge tubes and 5 ml of diluted blood samples were carefully layered onto each histopaque gradient. Gradients were centrifuged at 475 g and 20 °C for 15 min. The leucocytes bands were removed from the interface between plasma and histopaque layers of each tube and collected into one 50 ml tube. The total volume was brought to 50 ml with cold Dulbecco’s Modified Eagle Medium (DMEM, Gibco™, USA). The cell suspension was washed three times with PBS and the total number of cells was determined.
Blood serum (500 μl) was separated by centrifugation from each blood samples not later than within 1 h after individual blood draw.
Biopreservation: Blood serum was frozen and stored at − 80 °C directly after each individual blood sample centrifugation. Separated peripheral leucocytes were finally re-suspended in PBS-DMSO solution, aliquoted into Eppendorf tubes and stored at − 80 °C until molecular profiling has been performed.
Multi-omic analysis
Protein expression analysis by Western blotting
All analyses were performed two times for each sample utilising the standardised procedure described elsewhere [29, 30]. Primary antibody incubation was performed at room temperature using a 1:200 dilution of the specific antibodies to
-
human calgranulin A, a goat polyclonal antibody (C-19) raised against a peptide mapping at the C-teminus of calgranulin A of human origin, sc-8112; Santa Cruz, USA
-
human catalase, a goat polyclonal antibody (S-20) raised against a peptide mapping an internal region of catalase of human origin, sc-34,282, Santa Cruz, USA)
-
human profilin-1, a goat polyclonal antibody (C-15) raised against a peptide mapping at the C-terminus of profilin-1 of human origin, sc-30,522 Santa Cruz, USA
-
human RhoA, a mouse monoclonal antibody (26C4) raised against an epitope corresponding to amino acids 120–150 of RhoA of human origin, sc-418 Santa Cruz, USA
-
human superoxide-dismutase (SOD-2), a goat polyclonal antibody (N-20) raised against a peptide mapping near the N-teminus of SOD-2 of human origin, sc-18503; Santa Cruz, USA
-
human thioredoxin (Trx), a mouse monoclonal antibody (D-4) specific for an epitope mapping between amino acids 1–34 at the N-terminus of Trx of human origin, sc-271281 Santa Cruz, USA
-
and the house-keeping protein - human actin, a goat polyclonal IgG (I-19), epitope mapping at the C-terminus of actin of human origin, recommended for detection of a broad range of actin isoforms of human origin, sc-1616 Santa Cruz, USA
The protein specific signals were measured densitometrically using the Quantity One® imaging system (Bio-Rad, USA).
Analysis of metalloproteinase activity by zymography
For determination of gelatinase activity of MMP-2 and MMP-9 in blood serum “Ready-Gelatin-Gels” (Bio-Rad, USA) were used according to the instructions of the manufacturer. Two microliters from individual serum samples were electrophoresed under non-reducing conditions using Criterion™ Precast Gel System (Bio-Rad, USA). After electrophoresis, each gel was incubated at room temperature in 2% Triton X-100 for 2 × 30 min in order to remove the traces of sodium dodecyl sulphate, and then incubated overnight at 37 °C in buffer (150 mM NaCl, 50 mM Tris-HCl, pH 7.6, containing 5 mM CaCl2 and 0.02% NaN3). Afterwards, a staining with 0.5% Coomassie blue G-250 (Sigma, USA) was performed for each gel. The proteolytic activity of each gelatinase (A and B) was identified as a clear band on a blue background according to the correspondent molecular weight of each gelatinase (A and B that corresponds to the metallproteinase-2 and metallproteinase-9, respectively). Gels were dried between cellophane sheets with a GelAir™ Drying System (Bio-Rad, USA) and then scanned with a yellow filter using Adobe Photoshop (Adobe System, USA) in grey-scale mode. Densitometric analysis of zymographic lysis zones at 66 and 86 kDa for gelatinases A and B, respectively (Fig. 1), was performed using Quantity One® imaging system (Bio-Rad, USA).
Subcellular imaging: comet assay analysis of DNA fragmentation
In order to evaluate DNA quality (DNA damage)‚ the subcellular imaging by Comet Assay™ Trevigen, Inc., Cat. No. 4250-050-K, USA) analysis has been used. The single cell gel electrophoresis assay is based upon the ability of DNA fragments to migrate out of the peripheral leucocytes in the electric field applied, whereas undamaged chromosomal DNA does not migrate into the agarose gel. DNA fragmentation assessment has been performed by evaluation of the DNA “comet” tail shape and specific migration patterns. Peripheral leucocytes have been immobilised in a bed of low-melting point agarose, on a Trevigen CometSlide™. The alkaline electrophoresis is very sensitive and detects small amounts of damage. Therefore, after cell lysis, samples have been treated with alkali to denature the DNA and hydrolyse sites of damage. After electrophoretic separation, staining with a fluorescent DNA intercalating dye (SYBR® GreenI) has been performed. The shape of individual comets has been visualised by epifluorescence microscopy. The evaluation system developed by the authors and published earlier [31] has been applied for the qualification and quantification the DNA fragmentation/damage (Fig. 2).
Comet assay (microscopic subcellular image) analyses four classes of comets: class I indicates intact DNA with a bright head and no tail, while class IV demonstrates an apoptotic DNA fragmentation characterised by (almost) no visible head and a long diffuse tail. Comets with intermediate characteristics but clearly distinguishable patterns are represented by classes II and III distinguishable by the ratio R = T/r, where T represents the comet’s tail length and r is the radius of the comet’s head. The characteristic value of R for class I is 1 and for class IV is infinite, due to the r = 0. Comets with R values ranging between 1 < R > 3 represent class II. D is the diameter of the comet’s “head”
Statistical analysis
Statistical analyses were carried out using the SPSS 22 software package (IBM, Armonk, NY).
Spearman’s rank-order correlation method was used for mutual correlations amongst biomarkers and clinic-pathological characteristics. Survival time was estimated by Kaplan-Meier analyses and compared amongst stratified patient groups using log-rank test.
Multivariate analysis was performed utilising the Cox regression model to test independent significance while adjusting for covariates. Data were presented as hazard ratios (HR) and 95% confidence intervals (95%CI). Overall survival (OS) was defined as the time frame between the diagnosis and death recorded. Reported P values were two sided. P ≤ 0.05 was considered statistically significant.
Results
Structured by corresponding subtitles, the results of the statistical analysis are provided below for the patients stratified by the treatment approach and most promising multi-omic biomarker panel. The results of univariate and multivariate analyses of overall survival for all biomarker measured in the study are summarised in Tables 21 and 22. The results of mutual correlations amongst all biomarkers are provided in Table 23.
Overall survival of patients treated either with SIRT or TACE
OS of patients treated with TACE was more than two times longer compared to the SIRT treatment. The difference is significant in both uni- and multivariate analyses as demonstrated in the Table 2 and Table 3. Figure 3a shows results by the Kaplan-Meier analysis.
Overall survival of patients stratified by the therapy type and individual biomarkers (Kaplan-Meier analysis using log-rank test) as follwing: a stratified by the treatment approach (TACE versus SIRT); b treated with SIRT and stratified by MMP2 activities (middle/high versus low); c treated with TACE and stratified by MMP2 activities (middle/high versus low); d stratified by the level (high versus low) comets class I; e stratified by the level (high versus low) of class III comets; f stratified by the level (high versus low) of class IV comets; g stratified by the level (high versus low) of SOD-2 expression; h stratified by the level (high versus low) of catalase expression; and i stratified by the level (high versus low) of calgranulin A expression; corresponding statistical significance is provided
OS of patients treated with SIRT and stratified by MMP9 activities
No difference has been demonstrated in OS for the SIRT-treated patients demonstrating either low (categories 1 and 2) or middle and high (categories 3, 4 and 5) levels of MMP-9 activity in blood plasma measured prior to the treatment as summarised in Table 4.
OS of patients treated with TACE and stratified by MMP9 activities
In contrast to the SIRT, there is an increase in OS of the TACE-treated patients with low (categories 1 and 2) level of MMP-9 activity in blood plasma measured prior to the treatment as summarised in Table 5.
OS of patients treated with SIRT and stratified by MMP2 activities
OS is significantly increased for the SIRT-treated patients with low (categories 1 and 2) level of MMP-2 activity in blood plasma measured prior to the treatment as summarised in Table 6. Moreover, this patient stratification resulted in a statistically significant difference also by multivariate analysis—Table 7. Figure 3b shows results by the Kaplan-Meier analysis.
OS of patients treated with TACE and stratified by MMP2 activities
In contrast to the SIRT-treated patients stratified by MMP-2 activities (see above), OS is decreased (close to significant) for the TACE-treated patients with low (categories 1 and 2) level of MMP-2 activity in blood plasma measured prior to the treatment as summarised in Table 8. Figure 3c shows results by the Kaplan-Meier analysis.
OS of patients stratified by the class I comets
By the class I comets, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a statistically significant difference for an increased OS of patients with high level of the class I comets compared to the low level (Table 9). Moreover, the multivariate analysis (Table 10) resulted in significant differences for both parameters—class I comets and the type of therapy applied. Figure 3d shows results by the Kaplan-Meier analysis.
OS of patients stratified by the class III comets
By the class III comets, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a statistically significant difference for an increased OS of patients with low level of the class III comets compared to the high level (Table 11). Moreover, the multivariate analysis (Table 12) resulted in significant differences for both parameters—class III comets and the type of therapy applied. Figure 3e shows results by the Kaplan-Meier analysis.
OS of patients stratified by the class IV comets
By the class IV comets, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a statistically significant difference for an increased OS of patients with low level of the class IV comets compared to the high level (Table 13). Moreover, the multivariate analysis (Table 14) resulted in significant differences for both parameters—class IV comets and the type of therapy applied. Figure 3f shows results by the Kaplan-Meier analysis.
OS of patients stratified by the expression level of SOD-2
By the expression level of SOD-2, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a trend for an increased OS of patients with high level of the SOD-2 expression compared to the low level (Table 15). Moreover, the multivariate analysis (Table 16) resulted in significant differences for both parameters—SOD-2 expression and the type of therapy applied. Figure 3g shows results by the Kaplan-Meier analysis.
OS of patients stratified by the expression level of catalase
By the expression level of catalase, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a statistically significant difference for an increased OS of patients with high level of the catalase expression compared to the low level (Table 17). Moreover, the multivariate analysis (Table 18) resulted in significant differences for both parameters—catalase expression and the type of therapy applied. Figure 3h shows results by the Kaplan-Meier analysis.
OS of patients stratified by the expression level of calgranulin A
By the expression level of calgranulin A, patients have been stratified into two groups demonstrating either low or high level compared to the median value. There is a statistically significant difference for an increased OS of patients with low level of calgranulin A expression compared to the high level (Table 19). Moreover, the multivariate analysis (Table 20) resulted in significant differences for both parameters—calgranulin A expression and the type of therapy applied. Figure 3i shows results by the Kaplan-Meier analysis.
Summarising overview
OS of patients in relation to the individual biomarkers (Kaplan-Meier analysis with log-rank test), multivariate analysis of overall survival (OS) of patients in relation to all individual biomarkers measured in the study (Cox proportional hazards regression) and mutual correlations amongst the biomarkers and clinical characteristics (Spearman’s rank-order correlation coefficients) are provided in summarising Tables 21, 22 and 23, respectively.
Discussion
HCC, the most common primary liver malignancy, is characterised by a highly specific geographic distribution varying dramatically amongst world regions. Perhaps an extreme situation is observed in China, where HCC is the most common cancer type and the primary cause of the cancer-related mortality in males under 60 years of age. This is attributed to the widespread of hepatitis B in the country [32]. However, the HCC epidemic has already spread beyond the Eastern Asian predominance into the Western regions, making it especially remarkable in the USA and Western Europe [33]. In the USA, HCC is currently the fastest growing cause of cancer-related death [6]. Noteworthy, HCC related specifically to fatty liver diseases is increasingly prevalent in USA, Europe and other world regions [34]. The global burden of HCC is predicted to grow to 22 million over the next two decades [35].
In addition, almost all solid malignancies have been demonstrated to be capable of metastasising to the liver. The primary tumours most frequently metastasising to the liver are breast cancer followed by colorectal carcinoma [4]. Consequently, specific challenges of secondary liver malignancies to a large extent deals with the breast cancer (BC) epidemic which is recognised as being characteristic for the early twenty-first century accounting for almost two million new cases and a half of million BC-related deaths annually [36]. To this end, new trends demonstrate a persistently increasing incidence of premenopausal breast cancer in young patients diagnosed with particularly aggressive metastatic disease to distant sites with a great prevalence of liver and/or brain metastasis and remarkably short life expectancy such as in the case of triple-negative BC with more than 50% of patients who died within the first 6 months of the metastatic BC diagnosis [37, 38]. A risky status quo has been emphasised, namely that currently applied screening programmes are not skilled to satisfy the needs of young women at high risk [39].
Given the increased incidence of both primary and metastatic liver cancers, a new, revised approach is needed to advance medical care based on innovative screening programmes, predictive diagnostics, targeted preventive measured and patient stratification for treatment algorithms tailored to the person. Altogether, this requires a paradigm shift from reactive to the cost-effective predictive, preventive and personalised medicine (PPPM) as the medicine of the future [40].
Our current project is strongly motivated on the one hand, by the widely recognised epidemics of liver malignancies and, on the other hand, by an evident lack of predictive biomarker panels for advanced/unresectable liver carcinoma and metastasis as stated in the “Introduction”.
Advantages of the approach taken
-
The project takes advantage of the systemic alterations characteristic for liver malignancies, utilising specific biomarker patterns detected in blood samples by a minimally invasive analytical approach.
-
Systemic alterations have been analysed prior to therapy avoiding molecular biological effects which could diminish the predictive power of biomarker panel proposed.
-
The multi-omic biomarker panel has been considered for establishing future multi-level diagnostic (predictive and prognostics) approaches and individualised patient profiling.
-
Key-molecular pathways relevant for pathomechanisms of liver cancers have been included for constructing specific biomarker panels that might open a perspective for both—individualised diagnostics and targeted treatment.
Interpretation of results in the current study: contribution to the innovative approach for the patient stratification, prediction and prognosis in advanced liver malignancies
-
A.
Stratified by the type of therapy (either SIRT or TACE) applied, the overall survival was at significantly higher level in patients treated by TACE. This result should be further validated for patients stratified by the origin of the liver malignancy, namely HCC and liver metastases of different origin as individual groups of comparison.
-
B.
Stratification by key enzymes of the tissue remodelling revealed extremely important results: MMP-9 activity level in blood was irrelevant for OS in SIRT-treated patients, in contrast to TACE-treated patients tending to better survival in case of low activities; MMP-2 activity levels were highly relevant for OS in both SIRT- and TACE-treated patients, however, with opposite effects, namely significantly higher OS with low activities in SIRT but with high activities in TACE. Consequently, synergistically, the MMP-9 and MMP-2 activity patterns in blood might be an excellent predictor for the patient stratification, when deciding between two treatment modalities by equality of other relevant parameters such as tumour size and location. Concretely, in case of low MMP-9 and high MMP-2 activities in blood, an application of TACE is recommended, and independently of MMP-9 levels but low MMP-2 activities, SIRT might be a better choice.
-
C.
Stratification by DNA quality provided an important added prognostic value by three comet classes I (intact DNA), III (strongly damaged), IV (apoptotic). Slightly better OS has been demonstrated for a high (over medical value) level of class I. In contrast, low levels of class III and IV were significantly beneficial for OS.
-
D.
The key enzymes of the detoxification pathway demonstrated similar patterns of a great prognostic value: high (over median value) expression of both SOD-2 and catalase were significantly beneficial for OS.
-
E.
Stratification by calgranulin A (S100 calcium-binding protein A8) as a reliable indicator for an increased metastatic potential was well prognostic for OS demonstrating better survival rates at lower expression levels of the protein. This finding is well in consensus with results published by other groups [41,42,43].
Conclusions and expert recommendations
With this pilot programme, we have shown that for a variety of primary and metastatic liver cancers, liquid biopsy application and multiparametric analysis might be
-
useful for patient stratification,
-
predictive for the treatment approach and
-
prognostic for an individual survival.
Since this was a pilot programme, certain limitations of the study are well recognised by the authors. This includes the fact that only two forms of treatment were enrolled in this study. However, results achieved are encouraging, since it may be possible, through further research along these lines, to elaborate clinically relevant and cost-effective means of stratifying liver cancer patients for more personalised care.
Abbreviations
- HCC:
-
hepatocellular carcinoma
- SIRT:
-
selective internal radiation therapy
- TACE:
-
transarterial chemoembolisation
- OS:
-
overall survival
- MMP:
-
metalloproteinase
- SOD-2:
-
superoxide-dismutase 2
- PPPM:
-
predictive preventive personalised medicine
References
Ananthakrishnan A, Gogineni V, Saeian K. Epidemiology of primary and secondary liver cancers. Semin Interv Radiol. 2006;23:47–63. https://doi.org/10.1055/s-2006-939841.
Global Burden of Disease Cancer Collaboration, Fitzmaurice C, Dicker D, Pain A, Hamavid H, Moradi-Lakeh M, et al. The global burden of cancer 2013. JAMA Oncol. 2015;1:505–27. https://doi.org/10.1001/jamaoncol.2015.0735.
Duarte G, Williams CJ, Vasconcelos P, Nogueira P. Capacity to report on mortality attributable to chronic hepatitis B and C infections by member states: an exercise to monitor progress towards viral hepatitis elimination. J Viral Hepat. 2018;25:878–82. https://doi.org/10.1111/jvh.12882.
Golubnitschaja O, Sridhar KC. Liver metastatic disease: new concepts and biomarker panels to improve individual outcomes. Clin Exp Metastasis. 2016;33:743–55. https://doi.org/10.1007/s10585-016-9816-8.
Ayoub JP, Hess KR, Abbruzzese MC, Lenzi R, Raber MN, Abbruzzese JL. Unknown primary tumors metastatic to liver. J Clin Oncol. 1998;16:2105–12. https://doi.org/10.1200/JCO.1998.16.6.2105.
Mokdad AA, Singal AG, Yopp AC. Advances in local and systemic therapies for hepatocellular cancer. Curr Oncol Rep. 2016;18:9. https://doi.org/10.1007/s11912-015-0494-5.
Grech G, Zhan X, Yoo BC, Bubnov R, Hagan S, Danesi R, et al. EPMA position paper in cancer: current overview and future perspectives. EPMA J. 2015;6:9. https://doi.org/10.1186/s13167-015-0030-6.
Golubnitschaja O, Yeghiazaryan K, Stricker H, Trog D, Schild HH, Berliner L. Patients with hepatic breast cancer metastases demonstrate highly specific profiles of matrix metalloproteinases MMP-2 and MMP-9 after SIRT treatment as compared to other primary and secondary liver tumours. BMC Cancer. 2016;16:357. https://doi.org/10.1186/s12885-016-2382-2.
Hong Y-F, Chen Z-H, Wei L, Ma X-K, Li X, Wen J-Y, et al. Identification of the prognostic value of lymphocyte-to-monocyte ratio in patients with HBV-associated advanced hepatocellular carcinoma. Oncol Lett. 2017;14:2089–96. https://doi.org/10.3892/ol.2017.6420.
Shen H, Zheng S, Chen R, Jin X, Xu X, Jing C, et al. Prognostic significance of serum procalcitonin in patients with unresectable hepatocellular carcinoma treated with transcatheter arterial chemoembolization: a retrospective analysis of 509 cases. Medicine (Baltimore). 2017;96:e7438. https://doi.org/10.1097/MD.0000000000007438.
Ichikawa T, Machida N, Sasaki H, Tenmoku A, Kaneko H, Negishi R, et al. Early prediction of the outcome using tumor markers and mRECIST in unresectable hepatocellular carcinoma patients who underwent transarterial chemoembolization. Oncology. 2016;91:317–30. https://doi.org/10.1159/000448999.
Soydal C, Keskin O, Kucuk ON, Ozkan E, Bilgic S, Idilman R, et al. Prognostic factors for prediction of survival of hepatocellular cancer patients after selective internal radiation therapy. Ann Nucl Med. 2015;29:426–30. https://doi.org/10.1007/s12149-015-0962-x.
Kim SS, Cho HJ, Won JH, Bae JI, Kang DR, Lee J-D, et al. Interleukin-8 level as a prognostic marker in patients with hepatitis B virus-associated hepatocellular carcinoma treated with transarterial chemoembolization. Cytokine. 2015;76:449–57. https://doi.org/10.1016/j.cyto.2015.07.001.
Zhang X, Long Q. Elevated serum plasma fibrinogen is associated with advanced tumor stage and poor survival in hepatocellular carcinoma patients. Medicine (Baltimore). 2017;96:e6694. https://doi.org/10.1097/MD.0000000000006694.
Ma X-L, Jiang M, Zhao Y, Wang B-L, Shen M-N, Zhou Y, et al. Application of serum Annexin A3 in diagnosis, outcome prediction and therapeutic response evaluation for patients with hepatocellular carcinoma. Ann Surg Oncol. 2018;25:1686–94. https://doi.org/10.1245/s10434-018-6402-0.
Margaritelis NV, Veskoukis AS, Paschalis V, Vrabas IS, Dipla K, Zafeiridis A, et al. Blood reflects tissue oxidative stress: a systematic review. Biomarkers 2015;20:97–108. https://doi.org/10.3109/1354750X.2014.1002807.
Coriat R, Nicco C, Chéreau C, Mir O, Alexandre J, Ropert S, et al. Sorafenib-induced hepatocellular carcinoma cell death depends on reactive oxygen species production in vitro and in vivo. Mol Cancer Ther. 2012;11:2284–93. https://doi.org/10.1158/1535-7163.MCT-12-0093.
Marra M, Sordelli IM, Lombardi A, Lamberti M, Tarantino L, Giudice A, et al. Molecular targets and oxidative stress biomarkers in hepatocellular carcinoma: an overview. J Transl Med. 2011;9:171. https://doi.org/10.1186/1479-5876-9-171.
Teppo H-R, Soini Y, Karihtala P. Reactive oxygen species-mediated mechanisms of action of targeted cancer therapy. Oxid Med Cell Longev. 2017;2017:1485283. https://doi.org/10.1155/2017/1485283.
Yang S-F, Chang C-W, Wei R-J, Shiue Y-L, Wang S-N, Yeh Y-T. Involvement of DNA damage response pathways in hepatocellular carcinoma. Biomed Res Int. 2014;2014:153867. https://doi.org/10.1155/2014/153867.
Nishida N, Kudo M. Oxidative stress and epigenetic instability in human hepatocarcinogenesis. Dig Dis. 2013;31:447–53. https://doi.org/10.1159/000355243.
Mansoori AA, Jain SK. Molecular links between alcohol and tobacco induced DNA damage, gene polymorphisms and patho-physiological consequences: a systematic review of hepatic carcinogenesis. Asian Pac J Cancer Prev. 2015;16:4803–12.
Miller P, Kidwell KM, Thomas D, Sabel M, Rae JM, Hayes DF, et al. Elevated S100A8 protein expression in breast cancer cells and breast tumor stroma is prognostic of poor disease outcome. Breast Cancer Res Treat. 2017;166:85–94. https://doi.org/10.1007/s10549-017-4366-6.
Zhong J-M, Li J, Kang A-D, Huang S-Q, Liu W-B, Zhang Y, et al. Protein S100-A8: a potential metastasis-associated protein for breast cancer determined via iTRAQ quantitative proteomic and clinicopathological analysis. Oncol Lett. 2018;15:5285–93. https://doi.org/10.3892/ol.2018.7958.
Moz S, Basso D, Bozzato D, Galozzi P, Navaglia F, Negm OH, et al. SMAD4 loss enables EGF, TGFβ1 and S100A8/A9 induced activation of critical pathways to invasion in human pancreatic adenocarcinoma cells. Oncotarget. 2016;7:69927–44. https://doi.org/10.18632/oncotarget.12068.
De Ponti A, Wiechert L, Schneller D, Pusterla T, Longerich T, Hogg N, et al. A pro-tumorigenic function of S100A8/A9 in carcinogen-induced hepatocellular carcinoma. Cancer Lett. 2015;369:396–404. https://doi.org/10.1016/j.canlet.2015.09.005.
Németh J, Stein I, Haag D, Riehl A, Longerich T, Horwitz E, et al. S100A8 and S100A9 are novel nuclear factor kappa B target genes during malignant progression of murine and human liver carcinogenesis. Hepatology 2009;50(4):1251–62. https://doi.org/10.1002/hep.23099.
Golubnitschaja-Labudova O, Liu R, Decker C, Zhu P, Haefliger IO, Flammer J. Altered gene expression in lymphocytes of patients with normal-tension glaucoma. Curr Eye Res. 2000;21:867–76.
Golubnitschaja O, Filep N, Yeghiazaryan K, Blom HJ, Hofmann-Apitius M, Kuhn W. Multi-omic approach decodes paradoxes of the triple-negative breast cancer: lessons for predictive, preventive and personalised medicine. Amino Acids. 2018;50:383–95. https://doi.org/10.1007/s00726-017-2524-0.
Golubnitschaja O, Yeghiazaryan K, Abraham J-A, Schild HH, Costigliola V, Debald M, et al. Breast cancer risk assessment: a non-invasive multiparametric approach to stratify patients by MMP-9 serum activity and RhoA expression patterns in circulating leucocytes. Amino Acids. 2017;49:273–81. https://doi.org/10.1007/s00726-016-2357-2.
Golubnitschaja O, Moenkemann H, Kim K, Mozaffari MS. DNA damage and expression of checkpoint genes p21(WAF1/CIP1) and 14-3-3 sigma in taurine-deficient cardiomyocytes. Biochem Pharmacol. 2003;66:511–7.
Chen W, Zheng R, Baade PD, Zhang S, Zeng H, Bray F, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016;66:115–32. https://doi.org/10.3322/caac.21338.
Ghouri YA, Mian I, Rowe JH. Review of hepatocellular carcinoma: epidemiology, etiology, and carcinogenesis. J Carcinog. 2017;16:1. https://doi.org/10.4103/jcar.JCar_9_16.
Piñero F, Pages J, Marciano S, Fernández N, Silva J, Anders M, et al. Fatty liver disease, an emerging etiology of hepatocellular carcinoma in Argentina. World J Hepatol. 2018;10:41–50. https://doi.org/10.4254/wjh.v10.i1.41.
Stewart B, Wild C. World Cancer Report 2014 [Internet]. [cited 2018 May 28]. Available from: http://publications.iarc.fr/Non-Series-Publications/World-Cancer-Reports/World-Cancer-Report-2014
Golubnitschaja O, Debald M, Yeghiazaryan K, Kuhn W, Pešta M, Costigliola V, et al. Breast cancer epidemic in the early twenty-first century: evaluation of risk factors, cumulative questionnaires and recommendations for preventive measures. Tumour Biol 2016;37:12941–57. https://doi.org/10.1007/s13277-016-5168-x.
Vaz-Luis I, Lin NU, Keating NL, Barry WT, Winer EP, Freedman RA. Factors associated with early mortality among patients with de novo metastatic breast cancer: a population-based study. Oncologist. 2017;22:386–93. https://doi.org/10.1634/theoncologist.2016-0369.
Polivka J, Kralickova M, Polivka J, Kaiser C, Kuhn W, Golubnitschaja O. Mystery of the brain metastatic disease in breast cancer patients: improved patient stratification, disease prediction and targeted prevention on the horizon? EPMA J. 2017;8:119–27. https://doi.org/10.1007/s13167-017-0087-5.
Golubnitschaja O. Feeling cold and other underestimated symptoms in breast cancer: anecdotes or individual profiles for advanced patient stratification? EPMA J. 2017;8:17–22. https://doi.org/10.1007/s13167-017-0086-6.
Golubnitschaja O, Baban B, Boniolo G, Wang W, Bubnov R, Kapalla M, et al. Medicine in the early twenty-first century: paradigm and anticipation - EPMA position paper 2016. EPMA J. 2016;7:23. https://doi.org/10.1186/s13167-016-0072-4.
Arai K, Takano S, Teratani T, Ito Y, Yamada T, Nozawa R. S100A8 and S100A9 overexpression is associated with poor pathological parameters in invasive ductal carcinoma of the breast. Curr Cancer Drug Targets. 2008;8(4):243–52.
Zha H, Sun H, Li X, Duan L, Li A, Gu Y, et al. S100A8 facilitates the migration of colorectal cancer cells through regulating macrophages in the inflammatory microenvironment. Oncol Rep. 2016;36(1):279–90. https://doi.org/10.3892/or.2016.4790.
Reckenbeil J, Kraus D, Probstmeier R, Allam JP, Novak N, Frentzen M, et al. Cellular distribution and gene expression pattern of Metastasin (S100A4), Calgranulin A (S100A8), and Calgranulin B (S100A9) in oral lesions as markers for molecular pathology. Cancer Investig. 2016;34(6):246–54. https://doi.org/10.1080/07357907.2016.1186172.
Acknowledgements
The authors thank the Department of Radiology, University of Bonn for professional and financial support of the project. The authors are greatly thank the study nurse Mrs. Olga Ramig (Department of Radiology, University of Bonn, Germany) for collecting the patient data and personal supervision of the patients over the entire time of the project.
Funding
The study funding has been performed by the Department of Radiology, University of Bonn, Germany. Kristina Yeghiazaryan has been awarded a research fellowship with the European Association for Predictive, Preventive and Personalised Medicine (EPMA, Brussels, Belgium).
Author information
Authors and Affiliations
Contributions
O. Golubnitschaja created the concept of the project, made the data interpretation and drafted the article. J. Polivka Jr. carried out the statistical evaluation and graphical presentation of the data collected contributing significantly to the final version of the article. K. Yeghiazaryan carried out the molecular biological investigations. L. Berliner contributed to the data interpretation. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare that they have no competing interests.
Ethical approval
All the patients were informed about the purposes of the study and consequently have signed their “consent of the patient”. All investigations conformed to the principles outlined in the Declaration of Helsinki and were performed with permission from the responsible Ethical Committee of the Medical Faculty, Rheinische Friedrich-Wilhelms-University of Bonn. Corresponding reference number is 283/10.
Rights and permissions
About this article
Cite this article
Golubnitschaja, O., Polivka, J., Yeghiazaryan, K. et al. Liquid biopsy and multiparametric analysis in management of liver malignancies: new concepts of the patient stratification and prognostic approach. EPMA Journal 9, 271–285 (2018). https://doi.org/10.1007/s13167-018-0146-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13167-018-0146-6