Abstract
The influence of non-thermal plasma (NTP) treatment on the prevention of antibiotic resistance of microbial biofilms was studied. Staphylococcus epidermidis and Escherichia coli bacteria and a yeast Candida albicans, grown on the surface of Ti-6Al-4V alloy used in the manufacture of prosthetic implants, were employed. Their biofilms were exposed to NTP produced by DC cometary discharge and subsequently treated with antibiotics commonly used for the treatment of infections caused by them: erythromycin (ERY), polymyxin B (PMB), or amphotericin B (AMB), respectively. All biofilms displayed significant reduction of their metabolic activity after NTP exposure, the most sensitive was S. epidermidis. The subsequent action of antibiotics caused significant decrease in the metabolic activity of S. epidermidis and E. coli, but not C. albicans, although the area covered by biofilm decreased in all cases. The combined effect of NTP with antibiotics was thus proved to be a promising strategy in bacterial pathogen treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Plasma is a partially or fully ionized gas, denoted also as the fourth state of matter. In contrast to thermal plasma at temperature of thousands K, the non-thermal plasma (NTP) occurs at nearly ambient temperature and contains low-temperature ions and highly energetic free electrons. NTP may be easily obtained by various electric discharges: some of them are described in Ehlbeck et al. (2011) or Khun et al. (2018). Plasma is widely used in many areas of human activity including biology and medicine; its activity is mediated by reactive particles arising from the surrounding gas, as described by Graves (2012) or Liu et al. (2016). For the more detailed description of plasma physics and applications, the review of Tendero et al. (2006) or the comprehensive book of Metelmann et al. 2018 may be recommended.
Biofilm is a complex microbial consortium adhered to a solid surface and embedded within a semisolid matrix consisting mainly of extracellular polysaccharides. These consortia exhibit many peculiar properties, as the ability of quorum sensing or a distinct phenotype of its components. As a rule, bacteria in biofilm exhibit considerable resistance to antibiotics. Moreover, the matrix protects its content from external influences as biocides and desiccation. Biofilms exhibit not only increased resistance to antibiotics but also to other physical and chemical agents; this phenomenon was described and analyzed in many reports, as, e.g., Costerton (1995), Hornemann et al. (2008), Nadell et al. (2009), Steenackers et al. (2016), and Hall and Mah (2017). Some of the bacteria survive in biofilm in the special life forms of dormant or persistent cells, called also viable but non-culturable (VBNC) cells, allowing bacteria to tolerate environmental stress (Ayrapetyan et al. 2015). Biofilms are very dangerous for human beings because they are often formed on prosthetic implants or catheters, thus causing serious health complications. Biofilm resistance makes conventional processing difficult or impossible; see Hoyle and Costerton (1991), Lewis (2001), or Stewart and Costerton (2001).
Many attempts have been reported to develop and utilize new methods of biofilm destruction and inactivation including plant extracts, plant-derived oils and other natural products, metallic nanoparticles, bacteriophages, or treatments causing the disruption of extracellular polymeric substances. The works of Chung and Toh (2014), Sadekuzzaman et al. (2015), Koo et al. (2017), or Kolouchová et al. (2018) may be useful sources of more detailed information in this area. Some physical methods of biofilm inactivation were proved to be less or completely ineffective; e.g., the exposure to ultrasound caused no reduction of viable Pseudomonas aeruginosa cells even in combination with gentamicin (Carmen et al. 2005). On the other hand, the NTP was used many times for this purpose; Bourke et al. (2017), Puligundla and Mok (2017), Gilmore et al. (2018), or Julák et al. (2018) reviewed numerous attempts in this field. In addition to the 170 original articles summarized in the latter review, the following may be mentioned: Abramzon et al. (2006), Alkawareek et al. (2012, 2014), Pan et al. (2013), Kovalova et al. (2016).
In our previous paper, we attempted to compare the effect of NTP on various P. aeruginosa strains and elucidate the mechanism of observed differences (Paldrychová et al. 2019). We also described its inhibitory effect on microbial biofilms preformed on the surface of Ti-6Al-4V alloy used for the prosthetic implants manufacture (Vaňková et al. 2019): the viability of Escherichia coli, P. aeruginosa, Staphylococcus epidermidis, and Candida albicans biofilms was suppressed significantly and the biofilm re-development from persistent cells surviving in its lower layers was prevented. In this work, we attempted to enhance these effects by combined effect of NTP and antibiotics, using the same methods as in Vaňková et al. (2019).
Materials and methods
Microbiology
Test microorganisms strains were opportunistic microbial pathogens: Gram-positive bacterium Staphylococcus epidermidis DBM 3179, Gram-negative bacterium Escherichia coli DBM 3125, and the yeast Candida albicans DBM 2164, all obtained from the Collection of Microorganisms at University of Chemistry and Technology Prague. S. epidermidis was precultivated in Tryptone Soya Broth medium (TSB) at 37 °C, E. coli in Luria Broth medium (LB) at 37 °C, and C. albicans in Yeast-Peptone-Dextrose medium (YPD) at 30 °C. All microbes were cultivated for 24 h with shaking of 100 rpm. The stock media TSB and LB were purchased from Oxoid (UK), YPD from Carl Roth (Germany). After dissolution, their pH was adjusted to 7 by adding of 10% NaOH or 10% H2SO4 solutions. The grown cultures were stored in 50% glycerol stock at − 70 °C before use.
Biofilm formation
The grown microbial suspensions were diluted in 100 mL of appropriate cultivation medium in Erlenmeyer flasks to absorbance A600 = 0.600 ± 0.005. The circular Ti-6Al-4V alloy chips of 1.5 cm in diameter (obtained from Prospon, Czech Republic) were immersed into the appropriate suspension and incubated for 24 h at 37 °C (in the case of bacteria) or 72 h at 30 °C (in the case of C. albicans), thereby forming a mature biofilm.
Non-thermal plasma exposure
The NTP was produced by the DC cometary discharge described by Scholtz and Julák (2010) and Vaňková et al. (2019); Fig. 1 shows the scheme of this source. It consists of two needle electrodes connected to the 5 kV power supply (UNI-T UT 513A, UNI-TREND, China). The electrodes were arranged at an angle of 30°, their tips were 5 mm apart, and the tip of the positive electrode was shifted 1 mm above the negative one. The insulated metallic grid was inserted between the discharge and the exposed object, improving the inactivation efficiency and size of treated area (Scholtz et al. 2013). The distance of the exposed sample from positive electrode was 30 mm and 10 mm from the insulated grid. The cometary discharge operates in open air at a current of 50–70 μA. Based on our preliminary experiments, the exposure times used for NTP pretreatment before antibiotic addition were chosen to cause circa 50% inhibition of metabolically active biofilm re-development; they were 15 min for S. epidermidis, and 30 min for E. coli and C. albicans.
Antibiotic treatment
Ti-6Al-4V chips covered with biofilm were exposed to NTP and subsequently cultivated in the presence of antibiotic to enhance the prevention of biofilm re-development from persistent cells. The antibiotics were purchased from Sigma-Aldrich (USA) and used at concentrations corresponding to circa 50% inhibition of metabolically active biofilm re-development. These concentrations were 10 mg/L of erythromycin (ERY) used for S. epidermidis, 15 mg/L of polymyxin B (PMB) for E. coli, and 2.5 mg/L of amphotericin B (AMB) for C. albicans. Antibiotics were dissolved in a final volume of 3 mL of appropriate cultivation media. Each chip covered by biofilm was after exposure to NTP separately immersed into sterile polypropylene samplers (height 7 cm, diameter 3 cm, volume 40 mL; P-LAB, Czech Republic) containing antibiotic and cultivated under the same conditions as described above (24 h, 100 rpm, 37 °C or 30 °C). At the end of the cultivation, biofilm was washed three times with phosphate-buffered saline (PBS) and its metabolic activity as well as total biomass was determined.
Metabolic activity of biofilm
Metabolic activity was measured using a method of Traba and Liang (2015) as modified by Vaňková et al. (2019). This measurement is based on the dehydrogenase activity of vital cells which reduces the N′-anilino-N-[(4,5-dimethyl-1,3-thiazol-2-yl)imino]benzenecarboximidamide (MTT) molecule to purple formazan. The washed biofilms on the Ti-6Al-4V chips were immersed into the solution of 227 μL of MTT (1 mg/L, Sigma-Aldrich, USA) and 273 μL of glucose (57.4 mg/L, Penta, Czech Republic) and incubated at 37 °C or 30 °C for 2 h. The formazan crystals formed were consequently dissolved in 500 μL of 40% dimethylformamide in PBS with intensive shaking (230 rpm). A 100-μL aliquot of each sample was then transferred into a 96-well microtiter plate, and the color at 570 nm was measured using the spectrophotometric Sunrise Reader (Tecan, Switzerland). All experiments were performed in triplicate in three independent repetitions (9 measurements in total) and the results are presented as mean values and standard deviations.
Biofilm biomass
The total biofilm biomass was determined using a method described in detail in Vaňková et al. (2019). Briefly, the biofilm cells on the Ti-6Al-4V chips were stained in a polypropylene sampler with 1 mL of crystal violet (0.1%, Carl Roth, Germany) for 20 min statically at room temperature. The cells were then washed three times with the PBS and put into the sampler with 1 mL of 96% ethanol for 10 min, which released the crystal violet dye bound to the biofilm biomass. A 100-μL aliquot was then transferred into a 96-well microtiter plate, and the color was determined spectrophotometrically at 580 nm. All experiments were performed in triplicate in three independent repetitions and the results are presented as mean values and standard deviations.
Statistical analysis
The results obtained in assays for metabolic activity of biofilm cells and total biofilm biomass determination were compared using one-way analysis of variance (ANOVA), and differences were considered statistically significant at the p < 0.05.
Biofilm visualization
The visualization of microbial biofilm in control samples as well as biofilm exposed to the combination of NTP and antibiotic was performed by fluorescent microscopy acc. to Drago et al. (2016). Both agents were used at conditions corresponding to circa 50% inhibition of metabolically active biofilm re-development using each agent alone. Thus, the actual conditions were 15 min of NTP exposure + 10 mg/L of ERY for S. epidermidis; 30 min of NTP exposure + 15 mg/L of PMB for E. coli; and 30 min of NTP exposure + 2.5 mg/L of AMB for C. albicans. After exposure, the biofilm samples on Ti-6Al-4V chips were washed three times with the PBS and their entire surface was then covered by 100 μL of the green fluorescent dye SYTO 13 (0.00002 mg/L, 488/509 nm, Invitrogen, USA) to stain the nucleic acids in whole biofilm structure including the extracellular polymeric matrix. A fluorescent microscope ECLIPSE E400 (Nikon Instruments Europe B.V., Czech Republic) was used to observe and record the appearance of the samples. The area covered by biofilm was only semi-quantitatively estimated.
Results
NTP and antibiotic treatment
The effects of the 15-min NTP exposure, of ERY at 10 mg/L, and their subsequent action (NTP + ERY) on biofilm re-development of S. epidermidis are shown in Fig. 2. As mentioned under “Materials and methods,” the exposure times as well as the concentrations of used antibiotics were chosen to cause circa 50% inhibition of metabolically active biofilm re-development. The results show that the metabolic activity of re-developed biofilm after anti-biofilm agents (NTP and ERY) action alone corresponds to this claim (46% and 47%, respectively), as confirmed by ANOVA analysis (p ˂ 0.05). The combined effect of NTP + ERY (15 min + 10 mg/L) decreased the metabolic activity of S. epidermidis biofilm by 75%. The NTP exposure reduced biofilm biomass by 32%; the exposure to NTP and subsequent ERY treatment led to the overall suppression of biofilm biomass re-development by 79%.
Combined effect of non-thermal plasma (NTP) and erythromycin (ERY) on the S. epidermidis biofilm re-development on the Ti-6Al-4V chips. The empty columns (empty bars, left) represent metabolic activity as assessed by MTT assay, the dark columns (shaded bars, right) express the total biofilm mass. NTP, exposed to non-thermal plasma for 15 min; ERY, exposed to 10 mg/L of erythromycin; NTP + ERY, subsequent action of NTP and ERY. Control, without any treatment. Vertical lines represent the standard deviation of measurements; statistically significant differences against control were calculated using one-way ANOVA (*p < 0.05; ***p < 0.005; ***p < 0.0025)
Figure 3 presents the decrease of metabolic activity of E. coli biofilm to circa 50% when using NTP (30 min) or PMB (15 mg/L) alone (55% and 49%, respectively). However, the total biofilm biomass was reduced to 15% in both cases. Although the exposure of E. coli mature biofilm to NTP with subsequent PMB treatment caused the significant suppression of metabolic activity of re-developed biofilm by 88% (p ˂ 0.05), the total biofilm biomass remained the same (15%).
Combined effect of non-thermal plasma (NTP) and polymyxin B (PMB) on the E. coli biofilm re-development on the Ti-6Al-4V chips. The empty columns (empty bars, left) represent metabolic activity as assessed by MTT assay, the dark columns (shaded bars, right) express the total biofilm mass. NTP, exposed to non-thermal plasma for 30 min; PMB, exposed to 15 mg/L of polymyxin B; NTP + PMB, subsequent action of NTP and PMB. Control, without any treatment. Vertical lines represent the standard deviation of measurements; statistically significant differences against control were calculated using one-way ANOVA (*p < 0.05; ***p < 0.005; ***p < 0.0025)
The lower efficiency of the combination of NTP (30 min) with AMB (2.5 mg/L) toward biofilm re-development was observed in C. albicans (Fig. 4). The metabolic activity of biofilm was decreased by 63% (by 47% when using NTP alone and 59% when using AMB alone) and the content of total biofilm biomass was only slightly reduced (by 54%, NTP; by 52%, AMB; and by 64% after NTP + AMB).
Combined effect of non-thermal plasma (NTP) and amphotericin B (AMB) on the C. albicans biofilm re-development on the Ti-6Al-4V chips. The empty columns (empty bars, left) represent metabolic activity as assessed by MTT assay, the dark columns (shaded bars, right) express the total biofilm mass. NTP, exposed to non-thermal plasma for 30 min; AMB, exposed to 2.5 mg/L of amphotericin B; NTP + AMB, subsequent action of NTP and AMB. Control, without any treatment. Vertical lines represent the standard deviation of measurements; statistically significant differences against control were calculated using one-way ANOVA (*p < 0.05; ***p < 0.005; ***p < 0.0025)
Visualization of mature biofilm
The visualization of the three microbial biofilms (S. epidermidis, E. coli, and C. albicans) using fluorescent microscope showed that the combined action of NTP and antibiotics caused significant decrease in the area of Ti-6Al-4V chips covered by biofilm (Fig. 5). S. epidermidis–untreated biofilm completely covered the surface of the chip, although the coverage by the biofilm cells was discontinuous (Fig. 5a). When treated with the combination of NTP (15 min) and ERY (10 mg/L), only a part of the cells remained adhered to the surface indicating strong additive effect of such combination on the prevention of biofilm re-development of this species (Fig. 5b).
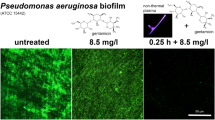
Fluorescent microscopy of biofilms on Ti-6Al-4V and their appearance after combined NTP and antibiotic treatment. Visualized by SYTO 13 staining, the scale bars represent 50 μm. Left column (pictures a, c, and e): controls without treatment. bS. epidermidis biofilm after action of NTP for 15 min, then 10 mg/L of erythromycin. dE. coli biofilm after action of NTP for 30 min, then 15 mg/L of polymyxin B. fC. albicans biofilm after action of NTP for 30 min, then 2.5 mg/L of amphotericin B
Similar trends were observed also in the case of E. coli and C. albicans. The control samples (Figs. 5c, e) showed that the untreated cells formed a very thick complex biofilms in both cases. In the case of E. coli, the treatment of mature biofilm with the combination of NTP (30 min) with PMB (15 mg/L) resulted in the efficient prevention of biofilm re-development and only a small amount of cells remained adhered (Fig. 5d).
The visualization of C. albicans biofilm treated with the combination of NTP (30 min) and AMB (2.5 mg/L) showed a decrease in the area covered by adhered cells and slightly weakened biofilm structure; nevertheless, the biofilm still remained on the chip. This suggests that a longer NTP exposure or a higher concentration of AMB might be needed for the efficient prevention of C. albicans biofilm re-development (Fig. 5f).
Discussion
This paper presents a pilot study of the relationship between anti-biofilm effects of plasma and antibiotics. This relationship includes many variable experimental parameters, of which only a few could be studied in detail here.
The selected exposure times to NTP vary somewhat among exposed species; they were chosen to meet the requirement of the effective combination of NTP and antibiotics. If the exposure times leading to complete reduction of metabolic activity of biofilm cells during its re-development were used, it would not be possible to recognize the additive effect of this combination. The difference between exposure times used for S. epidermidis and the other species tested is caused by their different sensitivity to NTP action. When using 30 min of NTP exposure toward S. epidermidis, the metabolic activity of its biofilm would be almost completely suppressed, as showed in Vaňková et al. (2019).
The sensitivity of S. epidermidis biofilm to NTP, expressed as total biomass, was lower than that of E. coli and C. albicans in this parameter. On the other hand, both its metabolic activity and total biomass decreased significantly after the combined action of NTP and ERY (by 75% and 79%, respectively). E. coli biofilm shows somewhat different picture: its metabolic activity as well as the total biomass were reduced significantly by action of both NTP and PMB alone. The combined action of NTP and PMB did not affect total biomass, but significantly reduced metabolic activity of E. coli biofilm. C. albicans biofilm was remarkably reduced in metabolic activity and total biomass by both NTP and AMB alone; the differences between these two actions and their combination were insignificant.
Although the combined action of NTP and antibiotics caused significant decrease in the covered area by biofilm in all microorganisms, it seems that S. epidermidis biofilm re-development was prevented to a highest degree. However, the differences in the Ti-6Al-4V surface coverage seem to be insignificant between organisms.
The sensitivity of microbes in biofilm to the action of NTP and subsequent antibiotic treatment has been found to be relatively variable for various microbial species. The combined action of NTP and antibiotic was proved useful in the case of S. epidermidis, in lesser extent also in E. coli, but it was negligible in the case of C. albicans. Acc. to Scholtz et al. (2010), planktonic Gram-positive bacteria are generally more sensitive to plasma produced by corona discharge than Gram-negative ones; yeast is much less sensitive. However, when using plasma jet, Gram-negative bacteria were somewhat more sensitive (Daeschlein 2018). Therefore, it appears that the inactivation process takes place by different mechanisms depending on the nature of the source used.
Apart from the mechanism of action of NTP exposure in general, which acts via creation of reactive oxygen or nitrogen species causing oxidative stress to recipient cell, the effect of antibiotics when combined with NTP must be considered. We have to admit that we are unable to explain with certainty the mechanism of ongoing processes, but we presume that the ERY-resistant staphylococcus is damaged by NTP pretreatment and thus becomes sensitive to this antibiotic. ERY stands for common bacteriostatic drug acting via proteosynthesis inhibition (Retsema and Fu 2001; Abu-Gharbieh et al. 2004). Such action is often stopped by efflux pumps expression, which disable ERY uptake by the cells expressing resistance genes. Although ERY would not be able to enter these cells, the NTP exposure possibly disrupts the cell surface, which facilitates ERY uptake. The intake of this drug leads to the inhibition of cell viable processes which slow the cell reaction to its damage and eventually leads to death (Chakraborti et al. 2019). We believe that the combination of NTP and antibiotics is additive in the case of S. epidermidis (ERY), perhaps also in E. coli (PMB), and neutral in C. albicans (AMB). As for PMB and AMB, the proposed explanation of combinatory action of both antibiotics with NTP pretreatment is not seemingly this easy (Zavascki et al. 2007). As both antibiotics act as cell membrane intercalating substances, their mode of action is very similar to those of NTP exposure, which creates radicals from carrier gas (Guo et al. 2015). The NTP pretreatment might probably boost the intercalation of either drug into the membrane, accelerate the cell lysis, and lead to cell death (Chakraborti et al. 2019).
The combined action of NTP and antibiotic was studied here in the consecutive arrangement, i.e., the antibiotic was applied after the direct NTP exposure. The simultaneous action of these agents may be more effective, but it seems to be impossible to perform appropriate experiments due to the degradation of antibiotics by direct NTP action, as described by Sarangapani et al. (2019).
Conclusion
The anti-biofilm activity of NTP was confirmed against biofilms of S. epidermidis, E. coli, and C. albicans. Significant differences between microorganisms were observed: in the case of ERY-resistant S. epidermidis, the preliminary exposure to NTP reduced this resistance. The preliminary action of NTP prior antibiotic treatment was less effective in the case of E. coli and has negligible effect in the case of C. albicans. To generalize these findings, we assume future studies on a broader set of microbial strains.
References
Abramzon N, Joaquin JC, Bray J, Brelles-Mariño G (2006) Biofilm destruction by RF high-pressure cold plasma jet. IEEE Transaction on Plasma Science 34:1304–1309. https://doi.org/10.1109/TPS.2006.877515
Abu-Gharbieh E, Vasina V, Poluzzi E, De Ponti F (2004) Antibacterial macrolides: a drug class with a complex pharmacological profile. Pharmacol Res 50:211–222 https://europepmc.org/article/med/15225662
Alkawareek MY, Algwari QT, Gorman SP, Graham WG, O’Connell D, Brendan F, Gilmore BF (2012) Application of atmospheric pressure nonthermal plasma for the in vitro eradication of bacterial biofilms. FEMS Immunol Med Microbiol 65:381–384. https://doi.org/10.1111/j.1574-695X.2012.00942.x
Alkawareek MY, Gorman SP, Graham WG, Gilmore BF (2014) Eradication of marine biofilms by atmospheric pressure non-thermal plasma: a potential approach to control biofouling? Int Biodeterior Biodegradation 86(2014):14–18. https://doi.org/10.1016/j.ibiod.2013.05.030
Ayrapetyan M, Williams TC, Baxter R, Oliver JD (2015) Viable but nonculturable and persister cells coexist stochastically and are induced by human serum. Infect Immun 83(11):4194–4203. https://doi.org/10.1128/IAI.00404-15 https://www.ncbi.nlm.nih.gov/pubmed/26283335
Bourke P, Ziuzina D, Han L, Cullen PJ, Gilmore BF (2017) Microbiological interactions with cold plasma. J Appl Microbiol 123:308–324. https://doi.org/10.1111/jam.13429
Carmen JC, Roeder BL, Nelson JL, Ogilvie RLR, Robison RA, Schaalje GB, Pitt WG (2005) Treatment of biofilm infections on implants with low-frequency ultrasound and antibiotics. Am J Infect Control 33(5):78–82. https://doi.org/10.1016/jajic.2004.08.002
Chakraborti S, Chakraborti T, Chattopadhyay D, Shaha C (Eds) (2019) Oxidative stress in microbial diseases. Springer, Singapore. https://www.springer.com/gp/book/9789811387623 https://books.google.cz/books?id = Tka5DwAAQBAJ&pg = PA120&lpg = PA120&dq = antibiotic+uptake+boost&source = bl&ots = od1NVpXhEX&sig = ACfU3U3ySSnwMujSpCI8ECj6EqzvVxLkZw&hl = cs&sa = X&ved = 2ahUKEwiXranPxeroAhWITsAKHTVHAU0Q6AEwCHoECAoQAQ#v = onepage&q = antibiotic%20uptake%20boost&f = false
Chung PY, Toh YS (2014) Anti-biofilm agents: recent breakthrough against multi-drug resistant Staphylococcus aureus. Pathogens and Disease 70:231–239. https://doi.org/10.1111/2049-632X.12141
Costerton JW (1995) Overview of microbial biofilms. J Ind Microbiol 15:137–140. https://doi.org/10.1007/BF01569816
Daeschlein G (2018) Antimicrobial activity of plasma. In: Metelmann HR, von Woedtke T, Weltmann KD (eds) Comprehensive clinical plasma medicine. Springer, Cham, pp 113–125. https://springerlink.bibliotecabuap.elogim.com/chapter/10.1007%2F978-3-319-67627-2_6
Drago L, Agrappi S, Bortolin M, Toscano M, Romano CL, De Vecchi E (2016) How to study biofilms after microbial colonization of materials used in orthopaedic implants. Int J Mol Sci 17(3):293. https://doi.org/10.3390/ijms17030293
Ehlbeck J, Schnabel U, Polak MJ, Winter J, von Woedtke T, Brandenburg R, von dem Hagen T, Weltmann KD (2011) Low temperature atmospheric pressure plasma sources for microbial decontamination. Journal of Physics D:Applied Physics 44:013002. https://doi.org/10.1088/0022-3727/44/1/013002
Gilmore BF, Flynn PB, O'Brien S, Hickok N, Freeman T, Bourke P (2018) Cold plasmas for biofilm control: opportunities and challenges. Trends Biotechnol 36(6):627–638. https://doi.org/10.1016/j.tibtech.2018.03.007 https://www.ncbi.nlm.nih.gov/pubmed/29729997
Graves DB (2012) The emerging role of reactive oxygen and nitrogen species in redox biology and some implications for plasma applications to medicine and biology. Journal of Physics D:Applied Physics 45:263001. https://doi.org/10.1088/0022-3727/45/26/263001
Guo J, Huang K, Wang J (2015) Bactericidal effect of various non-thermal plasma agents and the influence of experimental conditions in microbial inactivation: a review. Food Control 50:482–490 https://www.sciencedirect.com/science/article/abs/pii/S0956713514005581
Hall CW, Mah TF (2017) Molecular mechanisms of biofilm-based antibiotic resistance and tolerance in pathogenic bacteria. FEMS Microbiol Rev 41:276–301. https://doi.org/10.1093/femsre/fux010 https://academic.oup.com/femsre/article/41/3/276/3089981
Hornemann JA, Lysova AA, Codd SL, Seymour JD, Busse SC, Stewart PS, Brown JR (2008) Biopolymer and water dynamics in microbial biofilm extracellular polymeric substance. Biomacromolecules 9:2322–2328. https://doi.org/10.1021/bm800269h
Hoyle BD, Costerton JW (1991) Bacterial resistance to antibiotics: the role of biofilms. Prog Drug Res 37:91–105 https://www.ncbi.nlm.nih.gov/pubmed/1763187
Julák J, Scholtz V, Vaňková E (2018) Medically important biofilms and non-thermal plasma. World J Microbiol Biotechnol 34:178. https://doi.org/10.1007/s11274-018-2560-2
Khun J, Scholtz V, Hozák P, Fitl P, Julák J (2018) Various DC driven point-to-plain discharges as non-thermal plasma sources and their bactericidal effects. Plasma Sources Sci Technol 27(6):065002. https://doi.org/10.1088/1361-6595/aabdd0
Kolouchová I, Maťátková O, Paldrychová M, Kodeš Z, Kvasničková E, Sigler K, Čejková A, Šmidrkal J, Demnerová K, Masák J (2018) Resveratrol, pterostilbene, and baicalein: plant-derived anti-biofilm agents. Folia Microbiol 63(3):261. https://doi.org/10.1007/s12223-017-0549-0
Koo H, Allan RN, Howlin RP, Stoodley P, Hall-Stoodley L (2017) Targeting microbial biofilms: current and prospective therapeutic strategies. Nat Rev Microbiol 15:740–755. https://doi.org/10.1038/nrmicro.2017.99
Kovalova Z, Leroy M, Kirkpatrick MJ, Odic E, Machala Z (2016) Corona discharges with water electrospray for Escherichia coli biofilm eradication on a surface. Bioelectrochemistry 112:91–99. https://doi.org/10.1016/j.bioelechem.2016.05.002
Lewis K (2001) Riddle of biofilm resistance. Antimicrob Agents Chemother 45:999–1007. https://doi.org/10.1128/AAC.45.4.999-1007.2001
Liu DX, Liu ZC, Chen C, Yang AJ, Li D, Rong MZ, Chen HL, Kong MG (2016) Aqueous reactive species induced by a surface air discharge: heterogeneous mass transfer and liquid chemistry pathways. Sci Rep 6:23737. https://doi.org/10.1038/srep23737
Metelmann H-R, von Woedtke T, Weltmann K-D (eds) (2018) Comprehensive clinical plasma medicine: cold physical plasma for medical applications. Springer, Cham. ISBN: 978-3-319-67626-5. https://doi.org/10.1007/978-3-319-67627-2
Nadell CD, Xavier JB, Foster KR (2009) The sociobiology of biofilms. FEMS Microbiol Rev 33:206–224 https://www.ncbi.nlm.nih.gov/pubmed/19067751
Paldrychová M, Vaňková E, Scholtz V, Julák J, Sembolová E, Mat’átková O, Masák J (2019) Effect of non-thermal plasma on AHLdependent QS systems and biofilm formation in Pseudomonas aeruginosa: difference between non-hospital and clinical isolates. AIP Adv 9:055117. https://doi.org/10.1063/1.5090451
Pan J, Sun K, Liang Y, Sun P, Yang X, Wang J, Zhang J, Zhu W, Fang J, Becker KH (2013) Cold plasma therapy of a tooth root canal infected with Enterococcus faecalis biofilms in vitro. Cold Plasma Therapy 39:105–110. https://doi.org/10.1016/j.joen.2012.08.017
Puligundla P, Mok C (2017) Potential applications of nonthermal plasmas against biofilm-associated micro-organisms in vitro. J Appl Microbiol 122:1134–1148. https://doi.org/10.1111/jam.13404
Retsema J, Fu WC (2001) Macrolides: structures and microbial targets. Int J Antimicrob Agents 18:3–10 https://europepmc.org/article/med/11574188
Sadekuzzaman M, Yang S, Mizan MFR, Ha SD (2015) Current and recent advanced strategies for combating biofilms. Compr Rev Food Sci Food Saf 14:491–509. https://doi.org/10.1111/1541-4337.12144
Sarangapani C, Ziuzina D, Behan P, Boehm D, Gilmore BF, Cullen PJ, Bourke P (2019) Degradation kinetics of cold plasma-treated antibiotics and their antimicrobial activity. Sci Rep 9:3955. https://doi.org/10.1038/s41598-019-40352-9
Scholtz V, Julák J (2010) Plasma jet-like point-to-point electrical discharge in air and its bactericidal properties. IEEE Transactions on Plasma Science 38:1978–1980. https://doi.org/10.1109/TPS.2010.2051461
Scholtz V, Julák J, Kříha V (2010) The microbicidal effect of low-temperature plasma generated by corona discharge: comparison of various microorganisms on an agar surface or in aqueous suspension. Plasma Process Polym 7:237–243. https://doi.org/10.1002/ppap.200900072
Scholtz V, Kvasničková E, Julák J (2013) Microbial inactivation by electric discharge with metallic grid. Acta Phys Pol A 124:62–65 http://przyrbwn.icm.edu.pl/APP/ABSTR/124/a124-1-12.html
Steenackers HP, Parijs I, Foster KR, Vanderleyden J (2016) Experimental evolution in biofilm populations. FEMS Microbiol Rev 40:373–397. https://doi.org/10.1093/femsre/fuw002
Stewart PS, Costerton JW (2001) Antibiotic resistance of bacteria in biofilms. Lancet 358:135–138 https://www.ncbi.nlm.nih.gov/pubmed/11463434
Tendero C, Tixier C, Tristant P, Desmaison J, Leprince P (2006) Atmospheric pressure plasmas: a review. Spectrochim Acta B 61:2–30. https://doi.org/10.1016/j.sab.2005.10.003
Traba C, Liang JF (2015) The inactivation of Staphylococcus aureus biofilms using low-power argon plasma in a layer-by-layer approach. Biofouling 31(1):39–48. https://doi.org/10.1080/08927014.2014.995643
Vaňková E, Válková M, Kašparová P, Masák J, Scholtz V, Khun J, Julák J (2019) Prevention of biofilm redevelopment on Ti-6Al-4V alloy by cometary discharge with metallic grid. Contributions to Plasma Physics 59:166–172. https://doi.org/10.1002/ctpp.201800044
Zavascki AP, Goldani LZ, Li J, Nation RL (2007) Polymyxin B for treatment of multidrug-resistant pathogens: a critical review. Journal ofAntimicrobial Chemotherapy 60:1206–1215 https://www.ncbi.nlm.nih.gov/pubmed/17878146
Funding
This work was supported by the Charles University research program Progress Q25 and by the Czech Science Foundation (GACR) project 17-15936S.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Julák, J., Vaňková, E., Válková, M. et al. Combination of non-thermal plasma and subsequent antibiotic treatment for biofilm re-development prevention. Folia Microbiol 65, 863–869 (2020). https://doi.org/10.1007/s12223-020-00796-3
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12223-020-00796-3