Abstract
Accumulation of glycine (GLY) is the biochemical hallmark of glycine encephalopathy (GE), an aminoacidopathy characterized by severe neurological dysfunction that may lead to early death. In the present study, we evaluated the effect of a single intracerebroventricular administration of GLY on bioenergetics, redox homeostasis, and histopathology in brain of neonatal rats. Our results demonstrated that GLY decreased the activities of the respiratory chain complex IV and creatine kinase, induced reactive species generation, and diminished glutathione (GSH) levels 1, 5, and 10 days after GLY injection in cerebral cortex of 1-day-old rats. GLY also increased malondialdehyde (MDA) levels 5 days after GLY infusion in this brain region. Furthermore, GLY differentially modulated the activities of superoxide dismutase, catalase, and glutathione peroxidase depending on the period tested after GLY administration. In contrast, bioenergetics and redox parameters were not altered in brain of 5-day-old rats. Regarding the histopathological analysis, GLY increased S100β staining in cerebral cortex and striatum, and GFAP in corpus callosum of 1-day-old rats 5 days after injection. Finally, we verified that melatonin prevented the decrease of complex IV and CK activities and GSH concentrations, and the increase of MDA levels and S100β staining caused by GLY. Based on our findings, it may be presumed that impairment of redox and energy homeostasis and glial reactivity induced by GLY may contribute to the neurological dysfunction observed in GE.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Glycine encephalopathy (GE), also called non-ketotic hyperglycinemia, is an autosomal recessive disease caused by deficient activity of glycine (GLY) cleavage system (GCS), an intramitochondrial enzyme complex composed by four proteins: P-protein (a pyridoxal phosphate-dependent glycine decarboxylase), H-protein (a lipoic acid containing hydrogen-carrier protein), T-protein (tetrahydrofolate-requiring amino methyltransferase), and L-protein (lipoamide dehydrogenase). The prevalence of GE is estimated at 1:60,000 [1, 2], and it has been reported that up to 80 % of the affected patients have a defect in the P-protein. GCS defect results in the accumulation of GLY in all tissues of patients, particularly in the central nervous system (CNS), reaching concentrations as high as 7.3 mM [1, 3].
Most patients with GE present the classical or neonatal form of this disorder, whose symptoms appear in the first days of life and include lethargy, hypotonia, and seizures, frequently leading to coma and early death. Other less frequent forms of GE with late onset are characterized by behavioral problems, cognitive deficit, and developmental delay. Cerebral MRI findings include progressive brain atrophy, hypoplasia of the corpus callosum, and variable degrees of gliosis [4, 5]. Treatment is not effective, but generally consists at decreasing GLY levels and avoiding the effects of GLY at neurotransmitter receptors [6–8].
Although the pathophysiology of brain damage observed in GE is not established, it has been associated to the high tissue levels of GLY. In the CNS, GLY may cause excitotoxicity, since this amino acid is a co-agonist of NMDA glutamate receptor [9–13]. Furthermore, previous in vitro and in vivo studies demonstrated that GLY induces oxidative damage and compromises bioenergetics in brain of young rats [14–16]. It should be noted that GLY has been suggested to exert neurotoxic effects already in utero [7, 17].
Since to the best of our knowledge the in vivo effects of GLY in brain of neonatal rats have not yet been investigated, we evaluated the in vivo influence of GLY intracerebroventricular (ICV) administration (a chemical model of GE) on important parameters of energy metabolism and redox status, namely the activities of the respiratory chain complexes I to IV and of creatine kinase (CK), malondialdehyde (MDA) levels, GSH concentrations, 2′,7′-dichlorofluorescin (DCFH) oxidation, as well as the activities of superoxide dismutase (SOD), catalase (CAT), and glutathione peroxidase (GPx) in cerebral cortex of neonatal rats. We also investigated whether GLY could cause brain damage by performing 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyltetrazolium bromide (MTT) reduction assay and histopathological analysis for gliosis and neuronal death in cerebral cortex, striatum, and corpus callosum. In addition, we evaluated the effects of MEL, a neuroprotective agent, on the alterations exerted by GLY in newborn rat brain.
Material and Methods
Animals and Reagents
We used 1- and 5-day-old Wistar rats obtained from the Central Animal House of the Department of Biochemistry, ICBS, Universidade Federal do Rio Grande do Sul, Porto Alegre, RS, Brazil. The animals were maintained on a 12:12 h light/dark cycle (lights on 07:00–19:00 hours) in air-conditioned constant temperature (22 ± 1 °C) colony room, with free access to water and 20 % (w/w) protein commercial chow (SUPRA, Porto Alegre, RS, Brazil). All reagents used were of analytical grade and purchased from Sigma-Aldrich Co. (St Louis, MO, USA).
The experiments were approved by the local Animal Ethics Commission (Comissão de Ética no Uso de Animais-Universidade Federal do Rio Grande do Sul) under the number 23787, and the National Animal Rights Regulations (Law 11.794/2008). The guidelines of National Institutes of Health Guide for the Care and Use of Laboratory Animals (NIH publication no. 80-23, revised 1996), and Directive 2010/63/EU were followed. All efforts were made to minimize the number of animals used and their suffering.
Glycine and Melatonin Administration
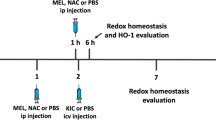
Each littermate of 1- or 5-day-old rats was injected into the fourth ventricle, as previously described [18, 19], with a dose of 0.2 μmol/g of GLY (treated group) or phosphate-buffered saline (PBS; control group). After the injection, the rat pups were returned to their respective dams. The correct position of the needle (size 3 mm) was tested by injecting 1 μL of methylene blue (4 % in saline solution) followed by histological analysis. One-day-old rats were euthanized 1, 5, or 10 days after GLY administration, whereas 5-day-old rats were killed 1 day after GLY injection. In other experiments, 1-day-old rats also received one diary intraperitoneal injection of 20 μmol/g MEL (prepared in dimethyl sulfoxide (DMSO)) during five consecutive days [20]. The first injection of MEL was performed 1 h before the administration of PBS or GLY. All rat pups were injected once a day at 10:00 a.m. to ensure that there were no differences in circadian rhythm between experimental groups. The rats were euthanized 1 h after the last injection of MEL. It was verified that MEL per se did not alter the biochemical parameters evaluated in rat cerebral cortex.
Preparation of Samples
The rats were euthanized by decapitation without anesthesia and had their brain rapidly excised on a Petri dish placed on ice. The cerebral cortex was dissected, weighed, and homogenized in a specific buffer used for each technique. For the determination of the activities of the respiratory chain complexes, the cerebral cortex was homogenized (1:20, w/v) in SET buffer (250 mM sucrose, 2.0 mM ethylenediaminetetraacetic acid (EDTA), and 10 mM Trizma base), pH 7.4. The homogenates were centrifuged at 800×g for 10 min, and the supernatants were kept at −70 °C until being used for enzyme activity determination. For CK activity measurement, the cerebral cortex was homogenized (1:10, w/v) in isosmotic saline solution. For the evaluation of the redox homeostasis parameters, the brain structure was homogenized in 10 volumes (1:10, w/v) of 20 mM sodium phosphate buffer, pH 7.4, containing 140 mM KCl. Homogenates were centrifuged at 750×g for 10 min at 4 °C to discard nuclei and cell debris [21] and the supernatants utilized for the determination of the parameters. Tissue slices (25 mg) were also isolated for DCFH oxidation measurement.
Respiratory Chain Complex Activities
Mitochondrial respiratory chain enzyme activities (complexes I–III, II, II–III, and IV) were measured in the supernatants with a protein concentration varying from 1.5 to 4.0 mg protein/mL. The activity of NADH/cytochrome c oxidoreductase (complexes I–III) was assessed as described by Schapira [22]. The activities of succinate/DCIP-oxidoreductase (complex II) and succinate/cytochrome c oxidoreductase (complex II–III) were determined according to the method of Fischer [23] and that of cytochrome c oxidase (complex IV) according to Rustin [24]. The methods described to measure these activities were slightly modified, as described in details in a previous report [25]. The activities of the respiratory chain complexes were calculated as nanomoles per minute milligram of protein.
Creatine Kinase Activity
The activity of CK was assessed in the supernatants containing 0.4–1.2 μg of protein in a reaction mixture consisting of 60 mM Tris–HCl buffer, pH 7.5, 7 mM phosphocreatine, 9 mM MgSO4, and 0.625 mM lauryl maltoside in a final volume of 100 μL. After 10 min of pre-incubation at 37 °C, the reaction was started by the addition of 0.3 μmol of ADP. The reaction was stopped after 10 min by the addition of 1 μmol of p-hydroxymercuribenzoic acid. The creatine formed was estimated according to the colorimetric method of Hughes [26] with slight modifications as described previously [27]. The color was developed by the addition of 100 μL of 2 % α-naphtol and 100 μL of 0.05 % diacetyl in a final volume of 1 mL and read spectrophotometrically at 540 nm after 20 min. Results were calculated as micromoles creatine per minute per milligram of protein.
Determination of Malondialdehyde Levels
MDA levels were measured according to the method described by Yagi [28] with some modifications. One hundred microliters of cortical supernatants containing 0.3 mg of protein were treated with 200 μL of 10 % trichloroacetic acid and 300 μL of 0.67 % thiobarbituric acid in 7.1 % sodium sulfate and incubated for 2 h in a boiling water bath. The mixture was then cooled on running tap water and the resulting pink-stained pigment was extracted with 400 μL of butanol. Fluorescence of the pigment was read at 515 and 553 nm as excitation and emission wavelengths, respectively. Calibration curve was carried out using 1,1,3,3-tetramethoxypropane and subjected to the same treatment as supernatants. MDA levels were calculated as nanomoles MDA per milligram of protein.
2′,7′-Dichlorofluorescin Oxidation
Reactive species (RS) production was assessed by determining DCFH oxidation [29]. 2′,7′-Dichlorofluorescein diacetate (DCFH-DA) was prepared in 20 mM sodium phosphate buffer, pH 7.4, containing 140 mM KCl, and incubated with tissue slices during 30 min at 37 °C. DCFH-DA is hydrolyzed by intracellular esterases to form non-fluorescent DCFH, which is then rapidly oxidized to form highly fluorescent 2′,7′-dichlorofluorescein (DCF) in the presence of RS. The DCF fluorescence intensity correlates to the amount of RS formed. Fluorescence was measured using excitation and emission wavelengths of 480 and 535 nm, respectively. Calibration curve was performed with standard DCF (0.1–1 μM), and data were calculated as picomoles DCF formed per gram of tissue.
Glutathione Concentrations
GSH concentrations were measured according to Browne and Armstrong [30] with some modifications. One hundred and eighty-five microliters of 100 mM sodium phosphate buffer, pH 8.0, containing 5 mM EDTA, and 15 μL of o-phthaldialdehyde (1 mg/mL) were added to 30 μL of sample (0.3–0.5 mg of protein) previously deproteinized with metaphosphoric acid. This mixture was incubated at room temperature in a dark room for 15 min. Fluorescence was measured using excitation and emission wavelengths of 350 and 420 nm, respectively. Calibration curve was prepared with standard GSH (0.001–1 mM), and the concentrations were calculated as nanomoles GSH per milligram of protein.
Superoxide Dismutase Activity
SOD activity was determined according to Marklund [31]. This assay was based on the capacity of pyrogallol to autooxidize, a process highly dependent on superoxide, which is a substrate for SOD. Thus, the autoxidation of pyragollol is inhibited by SOD, whose activity can be indirectly measured in a spectrophotometer at 420 nm. The reaction medium contained 50 mM Tris buffer/1 mM EDTA, pH 8.2, 80 U/mL CAT, 0.38 mM pyrogallol, and approximately 1 μg of protein. A calibration curve was performed with purified SOD as standard to calculate the activity of SOD in the samples. The results were reported as units per milligram of protein.
Catalase Activity
CAT activity was determined according to Aebi [32] by monitoring the absorbance decrease at 240 nm due to the decomposition of hydrogen peroxide in a reaction medium containing 20 mM hydrogen peroxide, 0.1 % Triton X-100, 10 mM potassium phosphate buffer, pH 7.0, and approximately 1 μg of protein. The specific activity was calculated as units per milligram of protein.
Glutathione Peroxidase Activity
GPx activity was measured according to the method of Wendel [33] by monitoring the disappearance of NADPH at 340 nm in a medium containing 100 mM potassium phosphate buffer/1 mM EDTA, pH 7.7, 2 mM GSH, 0.1 U/mL glutathione reductase, 0.4 mM azide, 0.5 mM tert-butyl-hydroperoxide, 0.1 mM NADPH, and approximately 3 μg of protein. The specific activity was calculated as units per milligram of protein.
MTT Reduction
Cell viability was determined in cerebral cortex slices by measuring the reduction of MTT to a dark violet formazan product [34]. First, cortical slices were washed twice with 500 μL Hank’s balanced salt solution (HBSS) and transferred to a 48-well plate in which each well contained 300 μL HBSS. The reaction was started with the addition of 0.5 mg mL−1 MTT, and after 45 min of incubation at 37 °C, the medium was removed and the slices were dissolved in dimethyl sulfoxide. The rate of MTT reduction was measured spectrophotometrically at a wavelength of 570 nm and a reference wavelength of 630 nm. Results were compared with control samples to which 100 % viability was attributed.
Immunohistochemical Studies
Animals were anesthetized with an intraperitoneal (i.p.) injection of a mixture of ketamine (80 mg/kg) and xylazine (10 mg/kg) until complete unresponsiveness to nociceptive stimuli and then transcardially perfused with 0.9 % saline and 10 % paraformaldehyde (PAF) prepared in 0.1 M phosphate buffer, pH 7.4, to fix the brain. Fixed brains were removed, post-fixed by immersion in PAF during 24 h, and then sectioned on a vibrating microtome to obtain 30–50-μm-thick consecutive coronal series. Immunohistochemistry was performed in cerebral cortex, striatum, and corpus callosum. For each animal and staining procedure, four to eight equivalent sections were immunostained. Free-floating sections were washed with PBS, submitted to antigen retrieval by boiling in 10 mM sodium citrate, pH 6.0, during 10 min, and washed twice for 10 min. The slices were then permeabilized with PBS plus 0.1–0.3 % Triton X-100 (PBST) for 20 min and treated with blocking buffer (PBS + 0.3 % Triton X-100 + 5 % bovine serum albumin) for 60 min. Afterwards, slices were incubated with the antibodies anti-NeuN (Millipore, 1:300), anti-GFAP (Sigma-Aldrich, 1:300), and anti-S100β (Sigma-Aldrich, 1:400). All dilutions were carried out in PBST. After a 4 °C overnight incubation, sections were rinsed in PBS and incubated at room temperature for 120 min with secondary antibodies (1:500) conjugated to fluorescent probes (Molecular Probes). Sections were then washed, mounted in fluoroshield (Sigma), and imaged in a FV300 Olympus confocal microscope provided with 488- and 546-nm lasers. Primary or secondary antibodies were omitted in negative controls [18].
Protein Determination
Protein content was measured by the method of Lowry [35] using bovine serum albumin as standard.
Statistical Analysis
Results are presented as mean ± standard deviation. Assays were performed in triplicate and the mean was used for statistical calculations. Data were analyzed using the Student’s t test for unpaired samples or one-way analysis of variance (ANOVA) followed by the Duncan multiple range test when the F value was significant. Only significant values are shown in the text. Differences between groups were rated significant at P < 0.05. All analyses were carried out in an IBM-compatible PC computer using the Statistical Package for the Social Sciences (SPSS) software.
Results
We first observed that GLY ICV administration at the dose of 0.2 μmol/g into the brain of 1-day-old rats did not cause behavioral alterations. On the other hand, the rats receiving higher doses (0.25 μmol/g and higher) died in less than 2 min after GLY injection.
GLY Administration Decreases Complex IV and CK Activities in Cerebral Cortex of Newborn Rats
We evaluated the effects of GLY injection (0.2 μmol/g) on cellular energy metabolism in cerebral cortex of 1-day-old rats by determining the activities of the respiratory chain complexes and CK. Figure 1 demonstrates that GLY inhibited the activity of complex IV 1 day (t (6) = 2.595; P < 0.05), 5 days (t (8) = 2.33; P < 0.05), or 10 days (t (7) = 3.755; P < 0.01) after its administration (Fig. 1d), whereas the activities of the complexes I–III, II, and II–III were not significantly altered at any period tested (Fig. 1a–c). GLY was also able to inhibit the activity of CK 1 day (t (9) = 3.780; P < 0.01), 5 days (t (8) = 2.765; P < 0.05), or 10 days (t (8) = 2.537; P < 0.05) after its injection (Fig. 2).
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on the activities of the respiratory chain complexes I to IV in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5, or 10 days after GLY injection. The activity of complex II (a) is expressed as nanomoles DCIP reduced per minute per milligram of protein and complexes I–III (b) as nanomoles cytochrome c reduced per minute per milligram of protein. The activities of complexes II–III (c) and IV (d) are expressed, respectively, as nanomoles cytochrome c reduced per minute per milligram of protein and nanomoles cytochrome c oxidized per minute per milligram of protein. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate. *P < 0.05; **P < 0.01, compared with control (Student’s t test for unpaired samples)
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on creatine kinase (CK) activity in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5, or 10 days after GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate and are expressed as micromoles per milligram of protein. *P < 0.05; **P < 0.01, compared with control (Student’s t test for unpaired samples)
GLY Administration Increases Reactive Species Generation and Induces Lipid Peroxidation in Cerebral Cortex of Newborn Rats
The next set of experiments was performed in order to examine whether GLY disturbs redox homeostasis in neonatal rat cerebral cortex. Our results show that GLY significantly increased DCFH oxidation 1 day (t (8) = −2.432; P < 0.05), 5 days (t (8) = −2.483; P < 0.05), or 10 days (t (7) = −4.411; P < 0.01) after its administration (Fig. 3). It was also verified that GLY increased MDA levels in brain of 1-day-old rats at five days after injection (t (9) = −3.547; P < 0.01) (Fig. 4).
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on 2′,7′-dichlorofluorescin oxidation (DCFH) in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5, or 10 days after GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate and expressed as picomoles per gram of tissue. *P < 0.05; **P < 0.01, compared with control (Student’s t test for unpaired samples)
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on malondialdehyde (MDA) levels in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5, or 10 days after GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate and are expressed as nanomoles per milligram of protein. **P < 0.01, compared with control (Student’s t test for unpaired samples)
GLY Administration Decreases GSH Concentrations and Modulates Antioxidant Enzyme Activities in Cerebral Cortex of Newborn Rats
Regarding the antioxidant defenses, GLY decreased GSH concentrations 1 day (t (7) = 2.736; P < 0.05), 5 days (t (9) = 2.297; P < 0.05), or 10 days (t (9) = 3.591; P < 0.01) after its infusion (Fig. 5). GLY also significantly reduced SOD activity at 10 days (t (9) = 4.693; P < 0.01) (Fig. 6a) and CAT activity at 5 days (t (9) = 2.613; P < 0.05) (Fig. 6b) after injection. On the other hand, GPx activity was increased at 1 day (t (8) = −3.132; P < 0.05) but decreased at 5 days (t (8) = 7.153; P < 0.001), and 10 days (t (7) = 2.734; P < 0.05) (Fig. 6c) after GLY infusion.
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on glutathione (GSH) concentrations in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5 or 10 days after GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate and are expressed as nanomoles milligram of protein. *P < 0.05; **P < 0.01, compared with control (Student’s t test for unpaired samples)
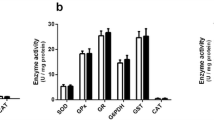
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on the activities of superoxide dismutase (SOD) (a), catalase (CAT) (b), and glutathione peroxidase (GPx) (c) in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 1, 5, or 10 days after the GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals) performed in triplicate and are expressed as units per milligram of protein. *P < 0.05; **P < 0.01; ***P < 0.001, compared with control (Student’s t test for unpaired samples)
GLY Administration Does Not Alter Energy and Redox Homeostasis in Cerebral Cortex of 5-Day-Old Rats
Next, we investigated the effects of GLY on energy and redox homeostasis in older (5-day-old) rats. Table 1 shows that the amino acid did not change the activity of CK, MDA levels, DCFH oxidation, and GSH concentrations 1 or 5 days after GLY injection in cerebral cortex of 5-day-old rats. GLY also did not alter the activities of the respiratory chain complexes, SOD and CAT one day after its injection (Table 1). These data imply that newborn rat brain is more vulnerable to GLY toxic effects.
GLY Administration Increases S100β in Cerebral Cortex and Striatum and GFAP in Corpus Callosum of Newborn Rats
We then evaluated the influence of GLY administration on S100β, GFAP, and NeuN markers in cerebral cortex, striatum, and corpus callosum 5 days after its administration in order to investigate whether GLY could cause brain injury. Figure 7 demonstrates that GLY significantly increased the number of cells stained with S100β in cerebral cortex (t (4) = −3.441; P < 0.05) and striatum (t (4) = −2.937; P < 0.05) 5 days after its administration (Fig. 7). We also found that GLY increased GFAP staining in corpus callosum (t (4) = 0.758; P < 0.05) without significant alterations in cerebral cortex and striatum (Fig. 8). In contrast, NeuN marker was not changed in any brain structure evaluated (data not shown). Aiming to evaluate whether GLY could cause cell death at longer periods after its administration, we examined the effects of GLY on NeuN staining and MTT reduction 15 days after the injection into the cerebral cortex of 1-day-old rats. It can be observed that, even at a longer period after the administration, GLY did not significantly alter MTT reduction (Table 2) and NeuN staining (data not shown).
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on S100β immunofluorescence staining in cerebral cortex, striatum, and corpus callosum of 1-day-old rats. Neonatal rats were euthanized five days after GLY injection. Representative images of S100β immunofluorescence staining in rat cerebral cortex, striatum, and corpus callosum slices. Calibration bar indicates 200 μm (a). Quantification of S100β staining in rat cerebral cortex, striatum, and corpus callosum slices (b). Data are represented as mean ± SD for three independent experiments (animals) and are expressed as percentage of controls. *P < 0.05, compared with control (Student’s t test for unpaired samples)
Effect of intracerebral administration of glycine (GLY; 0.2 μmol g−1) on glial fibrillary acidic protein (GFAP) immunofluorescence staining in cerebral cortex, striatum, and corpus callosum of 1-day-old rats. Representative images of GFAP immunofluorescence staining in rat cerebral cortex, striatum, and corpus callosum slices. Calibration bar indicates 200 μm (a). Quantification of GFAP staining in rat cerebral cortex, striatum, and corpus callosum slices (b). Data are represented as mean ± SD for three independent experiments (animals) and are expressed as percentage of controls. *P < 0.05, compared with control (Student’s t test for unpaired samples)
MEL Treatment Prevents GLY-Induced Neurotoxic Effects in Cerebral Cortex of Newborn Rats
We finally assessed the influence of MEL, a potent free radical scavenger, on the neurotoxicity exerted by GLY administration in cerebral cortex of 1-day-old rats at 5 days after its injection. MEL per se did not alter the parameters of energy and redox homeostasis (Fig. 9). MEL treatment totally prevented GLY-induced inhibition of the activities of complex IV (F (3, 16) = 3.760; P < 0.05) (Fig. 9a) and CK (F (3, 12) = 10.152; P < 0.01) (Fig. 9b). The antioxidant also prevented the decrease of GSH concentrations (F (3, 13) = 3.601; P < 0.05) (Fig. 9c) and the increase of MDA levels (F (3, 13) = 3.722; P < 0.05) (Fig. 9d) caused by GLY. In addition, we found that MEL attenuated GLY-induced increase of S100β staining in cerebral cortex (F (2, 8) = 32.424; P < 0.01) (Fig. 10).
Effect of melatonin (MEL; 20 μmol g−1) on glycine (GLY)-induced decrease of the activities of respiratory chain complex IV (a) and creatine kinase (CK) (b) and of glutathione (GSH) concentrations (c) and increase of MDA levels (d) in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized 5 days after GLY injection. Data are represented as mean ± SD for four to six independent experiments (animals). *P < 0.05; **P < 0.01, compared with control; # P < 0.05; ## P < 0.01, compared with GLY (Duncan multiple range test)
Effect of melatonin (MEL; 20 μmol g−1) on glycine (GLY)-induced increase of S100β immunofluorescence staining in cerebral cortex of 1-day-old rats. Neonatal rats were euthanized five days after GLY injection. Representative images of S100β immunofluorescence staining in rat cerebral cortex slices. Calibration bar indicates 200 μm (a). Quantification of S100β staining in rat cerebral cortex slices (b). Data are represented as mean ± SD for three independent experiments (animals) and are expressed as percentage of controls. *P < 0.05; **P < 0.01, compared with control; # P < 0.05, compared with GLY (Duncan multiple range test)
Discussion
Neonatal GE is a debilitating disorder characterized by severe neurological dysfunction [1, 7]. Although the onset of symptoms usually occurs in the first days of life, there is evidence pointing for brain injury already in utero [5, 7, 36], implying that high levels of GLY may exert damage during the fetal period. Furthermore, treatment for GE is not effective [37] so that the search for new adjuvant therapies is needed to improve patients’ quality of life. In order to clarify these issues, we investigated the effects of GLY administration on energy metabolism, redox homeostasis and histopathology in brain of 1- and 5-day-old rats. The analysis was carried out in rats with these ages because we aimed to mimic the neonatal form of GE, which is characterized by GLY accumulation in the brain of patients in utero and early in life [7, 17].
GLY inhibited the activities of the respiratory chain complex IV and CK in cerebral cortex of newborn rats. Since complex IV plays a major role in the electron transport chain flow and consequently in ATP synthesis and CK is essential for ATP buffering and transfer, it may be presumed that production and transfer of energy are compromised in vivo by GLY in newborn rat brain. This is in accordance with previous findings showing that GLY impairs energy metabolism in brain of young rats [37]. We also verified that the free radical scavenger MEL prevented the GLY-induced decrease of complex IV and CK activities, implying that both enzymes are vulnerable to reactive species generated by GLY [38]. In this context, it was suggested that GLY increases the generation of peroxyl and hydroxyl radicals [14, 39] and that MEL is an efficient scavenger of these free radicals [40–43]. However, we cannot rule out that the protective effects of MEL on the respiratory chain may also be a result of direct interactions that stabilize respiratory chain components in the inner mitochondrial membrane or via the induction of gene expression of complex IV subunits [44–46].
We also observed that GLY increased reactive species generation and induced lipid peroxidation in neonatal brain. These results are in line with previous in vitro and in vivo studies showing that GLY disturbs redox homeostasis in CNS of young rats [14, 16, 39]. Although we did not investigate the reasons by which GLY induced lipid peroxidation 5 days, but not 10 days after GLY administration, it is widely known that after an oxidative insult cells are able to activate signaling pathways that lead to increased expression of antioxidant enzymes in order to reestablish redox homeostasis [47–50]. Treatment with MEL prevented the lipid oxidative damage exerted by GLY, reinforcing that MEL is able to scavenge the reactive species generated by GLY, thus protecting against the GLY-induced pro oxidant insults. It should be noted here that hydroxyl and peroxyl radicals, which were suggested to be generated by GLY in vitro, are thermodynamically capable of initiating lipid peroxidation [38].
In addition, brain antioxidant defenses were also altered by GLY administration. We found that GLY decreased the concentrations of the major brain antioxidant GSH, a marker of non-enzymatic antioxidant capacity of tissues [38]. The decrease of GSH concentrations caused by GLY was fully prevented by MEL, probably due to the scavenging properties of MEL [44, 51]. Furthermore, the fact that MEL is able to maintain a normal GSH homeostasis is possibly related to the prevention exerted by MEL on GLY-induced decrease of CK activity, since this enzyme possesses critical sulfhydryl groups highly vulnerable to oxidative attack [38], which may be protected by GSH.
Regarding the enzymatic antioxidant defenses, we verified that GLY reduced SOD and CAT activities, whereas GPx activity was increased 1 day (short-term effect) and decreased 5 or 10 days (long-term effect) after GLY administration. We cannot at present explain the reasons why the activities of antioxidant enzymes are differentially altered or modulated by GLY. Nevertheless, it is feasible that the short-term increase of GPx activity induced by GLY could be related to an induction of the expression of this antioxidant enzyme at the gene level that might have occurred as a compensatory mechanism in response to increased formation of hydrogen peroxide and/or lipid peroxide [38, 52–54]. On the other hand, the decrease of the activities of SOD and CAT, as well as of GPx at longer periods may be due to inhibition caused by excessive production of reactive species elicited by GLY causing a site-specific amino acid modification in these enzyme structures [53]. Interestingly, investigators studying the effects of metabolites that accumulate in other inborn errors of metabolism also observed differential effects on the activities of antioxidant enzymes [55–58].
Otherwise, GLY did not alter the parameters of energy and redox homeostasis in older rats, indicating that the brain of newborn rats is more vulnerable to GLY neurotoxic effects. In this context, it is known that the neonatal brain is particularly sensitive to free radical attack once it has an immature mitochondrial free radical scavenging system with low levels of enzymatic and non-enzymatic antioxidants [59, 60]. Furthermore, this assumption is in accordance with previous data suggesting that elevation of GLY levels causing brain abnormalities already occurs at prenatal and neonatal stages [17, 61, 62].
Neuropathological findings in patients affected by GE consist of progressive cortical brain atrophy with leukodystrophy of the white matter, abnormalities in corpus callosum, and gliosis [1, 63]. Aiming to evaluate whether GLY could cause brain injury, we assessed the effects of GLY administration on GFAP, S100β, and NeuN immunohistochemical staining, as well as on MTT reduction. GLY increased the number of cells stained with S100β in cerebral cortex and striatum, and with GFAP in corpus callosum, suggesting that this amino acid induces glial reactivity, a condition characterized by proliferation and activation of astrocytes and accompanied by high expression of GFAP and S100β proteins that occurs in response to brain insults [64–67]. Thus, it may be presumed that GLY causes brain damage by inducing glial reactivity. This is in line with data of the literature showing that this process is involved in the pathogenesis of other neurodegenerative disorders, such as Alzheimer’s and Parkinson’s diseases, amyotrophic lateral sclerosis, and multiple sclerosis [60–66]. We also found that MEL attenuated GLY-induced increase of S100β staining in rat cerebral cortex, indicating that reactive species are implicated in GLY-induced glial reactivity. In contrast, we did not find alterations in NeuN staining and MTT reduction, implying that GLY does not induce cell death. It may be speculated that compensatory mechanisms involving cell adaptive responses have occurred in response to GLY oxidative insults, albeit they could not counteract the glial reactivity already in progress. On the other hand, we cannot rule out that higher concentrations of GLY may cause cell death. It should be emphasized here that we were not able to investigate the effects of doses higher than 0.2 μmol/g because the rats died shortly after the administration.
In conclusion, this is the first report showing that GLY, the amino acid accumulating in GE, induces bioenergetic dysfunction, oxidative stress, and glial reactivity in neonatal brain. These findings reinforce the hypothesis that high GLY levels induce neurotoxic effects in utero and/or early in life [7, 17, 68, 69]. It was also shown that MEL exerted beneficial effects against GLY neurotoxicity preventing oxidative stress, bioenergetic dysfunction, and glial reactivity caused by this compound, so that the administration of MEL could be considered as an adjuvant therapy to other pharmacological agents for patients affected by GE.
References
Hamosh A, Johnston MV (2001) Non-ketotic hyperglycinemia. In: Scriver CR, Beaudet A, Sly WS, Valle D (eds) The metabolic and molecular bases of inherited disease, vol Editors, 8th edn. McGraw-Hill, New York, pp 2065–2078
Applegarth DA, Toone JR, Lowry RB (2000) Incidence of inborn errors of metabolism in British Columbia, 1969–1996. Pediatrics 105(1):e10
Heindel W, Kugel H, Roth B (1993) Noninvasive detection of increased glycine content by proton MR spectroscopy in the brains of two infants with nonketotic hyperglycinemia. Am J Neuroradiol 14(3):629–635
Raghavendra S, Ashalatha R, Thomas SV, Kesavadas C (2007) Focal neuronal loss, reversible subcortical focal T2 hypointensity in seizures with a nonketotic hyperglycemic hyperosmolar state. Neuroradiology 49(4):299–305. doi:10.1007/s00234-006-0189-6
Shuman RM, Leech RW, Scott CR (1978) The neuropathology of the nonketotic and ketotic hyperglycinemias: three cases. Neurology 28(2):139–146
Bekiesiniska-Figatowska M, Rokicki D, Walecki J (2001) MRI in nonketotic hyperglycinaemia: case report. Neuroradiology 43(9):792–793
Hennermann JB, Berger JM, Grieben U, Scharer G, Van Hove JL (2012) Prediction of long-term outcome in glycine encephalopathy: a clinical survey. J Inherit Metab Dis 35(2):253–261. doi:10.1007/s10545-011-9398-1
Tsuyusaki Y, Shimbo H, Wada T, Iai M, Tsuji M, Yamashita S, Aida N, Kure S, Osaka H (2012) Paradoxical increase in seizure frequency with valproate in nonketotic hyperglycinemia. Brain Dev 34(1):72–75. doi:10.1016/j.braindev.2011.01.005
Hara H, Sukamoto T, Kogure K (1993) Mechanism and pathogenesis of ischemia-induced neuronal damage. Prog Neurobiol 40(6):645–670. doi:10.1016/0301-0082(93)90009-H
Kure S, Tada K, Narisawa K (1997) Nonketotic hyperglycinemia: biochemical, molecular, and neurological aspects. Jpn J Hum Genet 42(1):13–22. doi:10.1007/BF02766917
Applegarth DA, Toone JR (2001) Nonketotic hyperglycinemia (glycine encephalopathy): laboratory diagnosis. Mol Genet Metab 74(1–2):139–146. doi:10.1006/mgme.2001.3224
Kono Y, Shigetomi E, Inoue K, Kato F (2007) Facilitation of spontaneous glycine release by anoxia potentiates NMDA receptor current in the hypoglossal motor neurons of the rat. Eur J Neurosci 25(6):1748–1756. doi:10.1111/j.1460-9568.2007.05426.x
Katsuki H, Watanabe Y, Fujimoto S, Kume T, Akaike A (2007) Contribution of endogenous glycine and d-serine to excitotoxic and ischemic cell death in rat cerebrocortical slice cultures. Life Sci 81(9):740–749. doi:10.1016/j.lfs.2007.07.001
Leipnitz G, Solano AF, Seminotti B, Amaral AU, Fernandes CG, Beskow AP, Dutra Filho CS, Wajner M (2009) Glycine provokes lipid oxidative damage and reduces the antioxidant defenses in brain cortex of young rats. Cell Mol Neurobiol 29(2):253–261. doi:10.1007/s10571-008-9318-6
Busanello EN, Moura AP, Viegas CM, Zanatta A, da Costa FG, Schuck PF, Wajner M (2010) Neurochemical evidence that glycine induces bioenergetical dysfunction. Neurochem Int 56(8):948–954. doi:10.1016/j.neuint.2010.04.002
Seminotti B, Knebel LA, Fernandes CG, Amaral AU, da Rosa MS, Eichler P, Leipnitz G, Wajner M (2011) Glycine intrastriatal administration induces lipid and protein oxidative damage and alters the enzymatic antioxidant defenses in rat brain. Life Sci 89(7–8):276–281. doi:10.1016/j.lfs.2011.06.013
Pai YJ, Leung KY, Savery D, Hutchin T, Prunty H, Heales S, Brosnan ME, Brosnan JT, Copp AJ, Greene ND (2015) Glycine decarboxylase deficiency causes neural tube defects and features of non-ketotic hyperglycinemia in mice. Nat Commun 6:6388. doi:10.1038/ncomms7388
Olivera-Bravo S, Fernandez A, Sarlabos MN, Rosillo JC, Casanova G, Jimenez M, Barbeito L (2011) Neonatal astrocyte damage is sufficient to trigger progressive striatal degeneration in a rat model of glutaric acidemia-I. PLoS One 6(6):e20831. doi:10.1371/journal.pone.0020831
Olivera-Bravo S, Isasi E, Fernandez A, Rosillo JC, Jimenez M, Casanova G, Sarlabos MN, Barbeito L (2014) White matter injury induced by perinatal exposure to glutaric acid. Neurotox Res 25(4):381–391. doi:10.1007/s12640-013-9445-9
Olivier P, Fontaine RH, Loron G, Van Steenwinckel J, Biran V, Massonneau V, Kaindl A, Dalous J, Charriaut-Marlangue C, Aigrot MS, Pansiot J, Verney C, Gressens P, Baud O (2009) Melatonin promotes oligodendroglial maturation of injured white matter in neonatal rats. PLoS One 4(9):e7128. doi:10.1371/journal.pone.0007128
Evelson P, Travacio M, Repetto M, Escobar J, Llesuy S, Lissi EA (2001) Evaluation of total reactive antioxidant potential (TRAP) of tissue homogenates and their cytosols. Arch Biochem Biophys 388(2):261–266. doi:10.1006/abbi.2001.2292
Schapira AHV, Mann VM, Cooper JM, Dexter D, Daniel SE, Jenner P, Clark JB, Marsden CD (1990) Anatomic and disease specificity of NADH CoQ1 reductase (complex I) deficiency in Parkinson’s disease. J Neurochem 55(6):2142–2145
Fischer JC, Ruitenbeek W, Berden JA, Trijbels JM, Veerkamp JH, Stadhouders AM, Sengers RC, Janssen AJ (1985) Differential investigation of the capacity of succinate oxidation in human skeletal muscle. Clin Chim Acta 153(1):23–36
Rustin P, Chretien D, Bourgeron T, Gerard B, Rotig A, Saudubray JM, Munnich A (1994) Biochemical and molecular investigations in respiratory chain deficiencies. Clin Chim Acta 228(1):35–51
da Silva CG, Ribeiro CAJ, Leipnitz G, Dutra CS, Wyse ATS, Wannmacher CMD, Sarkis JJF, Jakobs C, Wajner M (2002) Inhibition of cytochrome c oxidase activity in rat cerebral cortex and human skeletal muscle by d-2-hydroxyglutaric acid in vitro. Biochim Biophys Acta 1586(1):81–91. doi:10.1016/S09254439(01)00088-6
Hughes BP (1962) A method for estimation of serum creatine kinase and its use in comparing creatine kinase and aldolase activity in normal and pathological sera. Clin Chim Acta 7(5):597–603
da Silva CG, Bueno ARF, Schuck PF, Leipnitz G, Ribeiro CAJ, Rosa RB, Dutra CS, Wyse ATS, Wannmacher CMD, Wajner M (2004) Inhibition of creatine kinase activity from rat cerebral cortex by d-2-hydroxyglutaric acid in vitro. Neurochem Int 44(1):45–52. doi:10.1016/S0197-0186(03)00098-6
Yagi K (1998) Simple procedure for specific assay of lipid hydroperoxides in serum or plasma. Methods Mol Biol 108:107–110. doi:10.1385/0-89603-472-0:107
LeBel CP, Ischiropoulos H, Bondy SC (1992) Evaluation of the probe 2′,7′-dichlorofluorescin as an indicator of reactive oxygen species formation and oxidative stress. Chem Res Toxicol 5(2):227–231
Browne RW, Armstrong D (1998) Reduced glutathione and glutathione disulfide. Methods Mol Biol 108:347–352. doi:10.1385/0-89603-472-0:347
Marklund SL (1985) Product of extracellular-superoxide dismutase catalysis. FEBS Lett 184(2):237–239
Aebi H (1984) Catalase in vitro. Methods Enzymol 105:121–126
Wendel A (1981) Glutathione peroxidase. Methods Enzymol 77:325–333
Mosmann T (1983) Rapid colorimetric assay for cellular growth and survival: application to proliferation and cytotoxicity assays. J Immunol Methods 65(1–2):55–63
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193(1):265–275
Brun A, Borjeson M, Hultberg B, Sjoblad S, Akesson H, Litwin E (1979) Neonatal non-ketotic hyperglycinemia: a clinical, biochemical and neuropathological study including electronmicroscopic findings. Neuropadiatrie 10(2):195–205. doi:10.1055/s-0028-1085325
Korman SH, Wexler ID, Gutman A, Rolland MO, Kanno J, Kure S (2006) Treatment from birth of nonketotic hyperglycinemia due to a novel GLDC mutation. Ann Neurol 59(2):411–415. doi:10.1002/ana.20759
Halliwell B, Gutteridge JMC (2007) Measurement of reactive species. Free radicals in biology and medicine, 4th edn. Oxford University Press, Oxford
Moura AP, Grings M, Marcowich GF, Bumbel AP, Parmeggiani B, de Moura Alvorcem L, Wajner M, Leipnitz G (2014) Evidence that glycine induces lipid peroxidation and decreases glutathione concentrations in rat cerebellum. Mol Cell Biochem 395(1–2):125–134. doi:10.1007/s11010-014-2118-z
Reiter RJ, Tan DX, Rosales-Corral S, Manchester LC (2013) The universal nature, unequal distribution and antioxidant functions of melatonin and its derivatives. Mini Rev Med Chem 13(3):373–384. doi:10.2174/1389557511313030006
Bromme HJ, Morke W, Peschke D, Ebelt H (2000) Scavenging effect of melatonin on hydroxyl radicals generated by alloxan. J Pineal Res 29(4):201–208. doi:10.1034/j.1600-0633.2002.290402.x
Matuszak Z, Reszka K, Chignell CF (1997) Reaction of melatonin and related indoles with hydroxyl radicals: EPR and spin trapping investigations. Free Radic Biol Med 23(3):367–372. doi:10.1016/S0891-5849(96)00614-4
Stasica P, Ulanski P, Rosiak JM (1998) Melatonin as a hydroxyl radical scavenger. J Pineal Res 25(1):65–66
Reyes-Toso CF, Rebagliati IR, Ricci CR, Linares LM, Albornoz LE, Cardinali DP, Zaninovich A (2006) Effect of melatonin treatment on oxygen consumption by rat liver mitochondria. Amino Acids 31(3):299–302. doi:10.1007/s00726-005-0280-z
Garcia JJ, Lopez-Pingarron L, Almeida-Souza P, Tres A, Escudero P, Garcia-Gil FA, Tan DX, Reiter RJ, Ramirez JM, Bernal-Perez M (2014) Protective effects of melatonin in reducing oxidative stress and in preserving the fluidity of biological membranes: a review. J Pineal Res 56(3):225–237. doi:10.1111/jpi.12128
Martin M, Macias M, Escames G, Reiter RJ, Agapito MT, Ortiz GG, Acuna-Castroviejo D (2000) Melatonin-induced increased activity of the respiratory chain complexes I and IV can prevent mitochondrial damage induced by ruthenium red in vivo. J Pineal Res 28(4):242–248. doi:10.1034/j.1600-079X.2000.280407.x
Gan L, Johnson JA (2014) Oxidative damage and the Nrf2-ARE pathway in neurodegenerative diseases. Biochim Biophys Acta 1842(8):1208–1218. doi:10.1016/j.bbadis.2013.12.011
Itoh K, Ishii T, Wakabayashi N, Yamamoto M (1999) Regulatory mechanisms of cellular response to oxidative stress. Free Radic Res 31(4):319–324
Johnson JA, Johnson DA, Kraft AD, Calkins MJ, Jakel RJ, Vargas MR, Chen PC (2008) The Nrf2-ARE pathway: an indicator and modulator of oxidative stress in neurodegeneration. Ann N Y Acad Sci 1147:61–69. doi:10.1196/annals.1427.036
Shih AY, Johnson DA, Wong G, Kraft AD, Jiang L, Erb H, Johnson JA, Murphy TH (2003) Coordinate regulation of glutathione biosynthesis and release by Nrf2-expressing glia potently protects neurons from oxidative stress. J Neurosci 23(8):3394–3406
Limon-Pacheco JH, Gonsebatt ME (2010) The glutathione system and its regulation by neurohormone melatonin in the central nervous system. Cent Nerv Syst Agents Med Chem 10(4):287–297. doi:10.2174/187152410793429683
Kaushik S, Kaur J (2003) Chronic cold exposure affects the antioxidant defense system in various rat tissues. Clin Chim Acta 333(1):69–77. doi:10.1016/S0009-8981(03)00171-2
Singh P, Jain A, Kaur G (2004) Impact of hypoglycemia and diabetes on CNS: correlation of mitochondrial oxidative stress with DNA damage. Mol Cell Biochem 260(1–2):153–159
Jafari M (2007) Dose- and time-dependent effects of sulfur mustard on antioxidant system in liver and brain of rat. Toxicology 231(1):30–39. doi:10.1016/j.tox.2006.11.048
Costa MZ, da Silva TM, Flores NP, Schmitz F, da Silva Scherer EB, Viau CM, Saffi J, Barschak AG, de Souza Wyse AT, Spanevello RM, Stefanello FM (2013) Methionine and methionine sulfoxide alter parameters of oxidative stress in the liver of young rats: in vitro and in vivo studies. Mol Cell Biochem 384(1–2):21–28. doi:10.1007/s11010-013-1777-5
da Rosa MS, Seminotti B, Amaral AU, Fernandes CG, Gasparotto J, Moreira JC, Gelain DP, Wajner M, Leipnitz G (2013) Redox homeostasis is compromised in vivo by the metabolites accumulating in 3-hydroxy-3-methylglutaryl-CoA lyase deficiency in rat cerebral cortex and liver. Free Radic Res 47(12):1066–1075. doi:10.3109/10715762.2013.853876
Sasso S, Dalmedico L, Delwing-Dal Magro D, Wyse AT, Delwing-de Lima D (2014) Effect of N-acetylarginine, a metabolite accumulated in hyperargininemia, on parameters of oxidative stress in rats: protective role of vitamins and l-NAME. Cell Biochem Funct 32(6):511–519. doi:10.1002/cbf.3045
Viegas CM, Zanatta A, Grings M, Hickmann FH, Monteiro WO, Soares LE, Sitta A, Leipnitz G, de Oliveira FH, Wajner M (2014) Disruption of redox homeostasis and brain damage caused in vivo by methylmalonic acid and ammonia in cerebral cortex and striatum of developing rats. Free Radic Res 48(6):659–669. doi:10.3109/10715762.2014.898842
Ferriero DM, Miller SP (2010) Imaging selective vulnerability in the developing nervous system. J Anat 217(4):429–435. doi:10.1111/j.1469-7580.2010.01226.x
Ikonomidou C, Kaindl AM (2011) Neuronal death and oxidative stress in the developing brain. Antioxid Redox Signal 14(8):1535–1550. doi:10.1089/ars.2010.3581
Paupe A, Bidat L, Sonigo P, Lenclen R, Molho M, Ville Y (2002) Prenatal diagnosis of hypoplasia of the corpus callosum in association with non-ketotic hyperglycinemia. Ultrasound Obstet Gynecol 20(6):616–619. doi:10.1046/j.1469-0705.2002.00869
Press GA, Barshop BA, Haas RH, Nyhan WL, Glass RF, Hesselink JR (1989) Abnormalities of the brain in nonketotic hyperglycinemia: MR manifestations. AJNR Am J Neuroradiol 10(2):315–321
del Toro M, Arranz JA, Macaya A, Riudor E, Raspall M, Moreno A, Vazquez E, Ortega A, Matsubara Y, Kure S, Roig M (2006) Progressive vacuolating glycine leukoencephalopathy with pulmonary hypertension. Ann Neurol 60(1):148–152. doi:10.1002/ana.20887
Sorci G, Bianchi R, Riuzzi F, Tubaro C, Arcuri C, Giambanco I, Donato R (2010). S100B protein, a damage-associated molecular pattern protein in the brain and heart, and beyond. Cardiovasc Psychiatry Neurol. doi:10.1155/2010/656481
Cerutti SM, Chadi G (2000) S100 immunoreactivity is increased in reactive astrocytes of the visual pathways following a mechanical lesion of the rat occipital cortex. Cell Biol Int 24(1):35–49. doi:10.1006/cbir.1999.0451
Griffin WS, Sheng JG, Mrak RE (1998) Senescence-accelerated overexpression of S100beta in brain of SAMP6 mice. Neurobiol Aging 19(1):71–76
Celikbilek A, Akyol L, Sabah S, Tanik N, Adam M, Celikbilek M, Korkmaz M, Yilmaz N (2014) S100B as a glial cell marker in diabetic peripheral neuropathy. Neurosci Lett 558:53–57. doi:10.1016/j.neulet.2013.10.067
Avishai-Eliner S, Brunson KL, Sandman CA, Baram TZ (2002) Stressed-out, or in (utero)? Trends Neurosci 25(10):518–524
Rice D, Barone S Jr (2000) Critical periods of vulnerability for the developing nervous system: evidence from humans and animal models. Environ Health Perspect 108(Suppl 3):511–533
Acknowledgments
The authors declare that there is no conflict of interest. This work was supported by grants from Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq), Programa de Apoio a Núcleos de Excelência (PRONEX II), Fundação de Amparo à Pesquisa do Estado do Rio Grande do Sul (FAPERGS), Pró-Reitoria de Pesquisa/Universidade Federal do Rio Grande do Sul (PROPESQ/UFRGS), Financiadora de estudos e projetos (FINEP), Rede Instituto Brasileiro de Neurociência (IBN-Net) no. 01.06.0842-00, and Instituto Nacional de Ciência e Tecnologia em Excitotoxicidade e Neuroproteção (INCT-EN).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Moura, A.P., Parmeggiani, B., Grings, M. et al. Intracerebral Glycine Administration Impairs Energy and Redox Homeostasis and Induces Glial Reactivity in Cerebral Cortex of Newborn Rats. Mol Neurobiol 53, 5864–5875 (2016). https://doi.org/10.1007/s12035-015-9493-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12035-015-9493-7