Abstract
Mesenchymal Stem Cells (MSCs) are a heterogeneous population of fibroblast-like cells which maintain self-renewability and pluripotency to differentiate into mesodermal cell lineages. The use of MSCs in clinical settings began with high enthusiasm and the number of MSC-based clinical trials has been rising ever since. However; the very unique characteristics of MSCs that made them suitable to for therapeutic use, might give rise to unwanted outcomes, including tumor formation and progression. In this paper, we present a model of carcinogenesis initiated by MSCs, which chains together the tissue organization field theory, the stem cell theory, and the inflammation-cancer chain. We believe that some tissue resident stem cells could be leaked cells from bone marrow MSC pool to various injured tissue, which consequently transform and integrate in the host tissue. If the injury persists or chronic inflammation develops, as a consequence of recurring exposure to growth factors, cytokines, etc. the newly formed tissue from MSCs, which still has conserved their mesenchymal and stemness features, go through rapid population expansion, and nullify their tumor suppressor genes, and hence give rise to neoplastic cell (carcinomas, sarcomas, and carcino-sarcomas). Considering the probability of this hypothesis being true, the clinical and therapeutic use of MSCs should be with caution, and the recipients’ long term follow-up seems to be insightful.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Stem cells are clonogenic cells that have two distinctive features: multipotency and self-renewal capacity [1]. The surge of studies on stem cells emerged by the discovery of a subset of bone marrow residing haematopoietic stem cells (HSCs) which give rise to all blood cell types [2]. Later on, studies by Friedenstein and colleagues reported that the bone marrow stroma can generate mesodermal cell lineages following heterotopic transplantation in mice; an observation suggestive of the presence of non-haematopoietic multipotent precursor cells within the bone marrow [3]. These precursors were a subset of fibroblast-like cells that could be easily isolated by their ability to adhere plastic surfaces and were shown to have hallmarks of stemness [4]. As a result, the term “Mesenchymal Stem Cell (MSC)” was assigned and accepted to refer to these newly identified precursor cells [5].
Bone marrow has been considered the main source of MSCs (bmMSCs), for many years. However; these stem cells are present in many other adult and fetal tissues (with few exceptions) [6]. In an attempt to standardize the definition of an “MSC”, the International Society for Cellular Therapy (ISCT) proposed the concept of essential minimal criteria for MSCs in culture [7]. The four minimal defining criteria for MSCs are: 1) adherence to plastic under standard tissue culture conditions, 2) expression of CD105, CD73, CD90, 3) lack of expression of CD45, CD34, CD14/CD11b, CD79/CD19 and HLA-DR surface markers, and 4) differentiation into adipocytes, osteoblasts and chondroblasts in vitro [7, 8].
MSCs: From Bench to Bedside
It didn’t take long for MSCs to become a subject of clinical research as potential therapeutic modalities in medicine, mostly because of their immunoregulatory and tissue regenerative properties [9], as well as simplicity of isolation and expansion [10]. The use of MSCs in clinical settings began with high enthusiasm and the number of MSC-based clinical trials has been rising since 2004 (Fig. 1a), and till now, there has been over 750 registered clinical trials in different phases aimed at evaluating the potential of MSC-based cell therapy worldwide (Fig. 1b). A number of these trials have shown efficacy of these cells in the treatment of conditions like: GvHD, Crohn’s disease, rheumatoid arthritis, ischemic stroke, myocardial infarction, chronic heart failure, type 1/2 diabetes mellitus, spinal cord injury, bone fractures/defects, chondral/osteochondral defects, cirrhosis, amyotrophic lateral sclerosis, and cerebral palsy [11].
a Number of registered clinical trials of MSC-based therapy. b Clinical phases of MSC-based therapy. (https://clinicaltrials.gov/)
However, it is important to note that not all MSC-based clinical trials have met their primary endpoint of efficacy and claims of benefit may be biased by strong commercial interests [12]. The very unique characteristics of MSCs that made them suitable cells to be used in clinical trials, might give rise to complications and unwanted outcomes, including tumor initiation, progression and metastasis.
Until 2007, most published data were in favor of anti-tumor properties of MSCs [13, 14], but a turning point was encountered when Karnoub and colleagues showed that co-injection of humans MSCs with breast cancer cell lines accelerated tumor growth, and metastasis [15]. Their observations led to further studies scrutinizing anti-tumor vs. tumor promoting properties of these cells [16]. From studies published thus far, it is assumable that MSCs might be among the important players in favor of tumor growth and progression.
MSCs’ Role in Cancer Progression
Tumor microenvironment can be considered as a swamp hosting many anti-tumor and tumor promoting factors such as MSCs. The active migration of endogenous and exogenous MSCs to tumor sites has been demonstrated in several models [17,18,19]. Upon arrival to tumor microenvironment, MSCs exhibit tumor promoting characteristics, due to direct and indirect signals they receive in the new milieu. These cells has been shown to increase proliferation, mobility, dormancy [20] and resistance to therapy [21] in neoplastic cells, by transdifferntiation to cancer associated fibroblasts (CAFs) [21,22,23,24], promotion of angiogenesis and lymphangiogenesis [25,26,27,28], stimulation of epithelial-to-mesenchymal transition (EMT) [29,30,31,32], suppressing tumor immune responses [21], induction of stemness in cancer cells [33,34,35,36,37,38] and probably acting as tumor initiating cells [39, 40].
Bearing these in mind, the question of whether the clinical application of MSCs would help cancer development/progression will be raised. There are studies demonstrating that this assumption could be right. For instance, several murine and human studies have shown the donor origin of CAFs in tumors of transplant recipients. In 2008, for the first time, Mishra et al. showed that human bone marrow–derived MSCs become activated and resemble CAFs on prolonged exposure to conditioned medium from MDA-MB231 human breast cancer cells [24]. Further studies by Spaeth [41] and Quante [18] provided additional evidence for transdifferentiation of donor MSCs to CAFs in recipients’ tumors. Interestingly, in 2009, Worthley and colleagues reported Y-chromosome positive CAFs in female patients with gastric cancer and rectal adenoma, with a history of bone marrow transplants from male donors [42].
Tumor promoting functions of transplanted MSCs via angiogenesis has been attributed to their ability to secrete angiogenic factors such as VEGF and TGF-beta [27, 28, 43], transdifferentiation to pericytes [44, 45]/endothelial cells [46], and recruiting endothelial progenitors [47]. Moreover, studies have shown that MSCs increase mobility, migration and consequently metastasis capacity of neoplastic cells [36, 48,49,50,51]. These observations have been linked to the ability of MSCs to induce EMT in neoplastic cells [30, 31, 35]. Furthermore their role in tumor progression by suppressing immune responses has been shown by several studies (submitted review). In the subsequent sections of this paper, we will review and discuss the possible roles of MSCs in induction of stemness in cancer cells, and their role as tumor initiating cells.
MSCs’ Induction of Stemness in Cancer Cells
Cancer stem cells (CSCs) are rare immortal subpopulation of cells within tumors that can both self-renew and give rise to diverse cell types in tumor milieu [52, 53]. Presumably, tumors’ resistance to therapy and recurrence can be attributed to the quiescent nature of these cells [54]. MSCs supply an advantageous tumor microenvironment for the maintenance of CSCs by secreting a variety of cytokines and formation of tumor cell hybrids by entosis or fusion [52, 53, 55,56,57].
Cabarcas and colleagues demonstrated that MSCs can promote cancer stemness through NF-κB pathway and secretion of CXCL12, IL6, and IL8 [58]. Moreover, it has been shown that MSCs promote undifferentiated state in neoplastic cells by producing BMP antagonist, Gremlin-1 [59], BMP2,4 [60], IL-6 [38, 61], CXCL1, CXCL7, CXCL8 [62], CCL5 [63], CXCR2 ligands (CXCL1, 5, 6, 7, 8) [64], activation of the JAK2-STAT3 pathway [65], FOXD1-ALDH1A3 Signaling [66] and through repression of FoxP2 expression [67]. Induction of stemness in cancer cells by MSCs has been shown in ovarian [60, 68], breast [64, 67], gastric [69], colon [62], and brain neoplasms [70].
Interestingly, El-Badawy and colleagues demonstrated that indirect co-culture of cancer cells and MSCs causes MSCs to acquire some properties of CSCs upon exposure to cancer cell-secreted factors and displayed properties of cells with enhanced sphere formation capacity [34]. This observation raises the question that whether MSCs used for therapeutic purposes can give rise to tumor initiating cells.
MSCs as Tumor Initiating Cells
In 2008, Berger and colleagues reported an osteosarcoma of donor origin in a patient who had received allogenic bone marrow transplant for β-thalassemia, 17 years earlier [71]. The isolated neoplastic cells expressed MSC markers at very high levels [71] and hence, one can assume that MSCs transplanted along with hematopetic stem cells had given rise to the osteosarcoma in the recipient. A more direct observation of engrafted MSCs transition to tumor initiating cells was published by Qian et al. [72]. They reported a sarcoma of donor origin (K3 cell line), found on the tail of a female rat after injection with male rat bone bmMSCs [72]. Considering these observations in addition to the capacity of MSC transdifferntiation to different cell lineages, it is presumable that engrafted MSCs may give rise to a variety of neoplasms in the recipient.
Spontaneous Tumoral Transformation of MSCs
Several studies have demonstrated that Mouse MSCs (mMSCs) are predisposed to acquisition of transformation events after long-term in vitro culture favoring clonal selection of transformed cells [73]. These observations prompt the concern that in the human settings, the ex-vivo expansion of human MSCs (hMSCs) before clinical application may also cause spontaneous neoplastic transformation after long-term culture.
MSCs as the Cell of Origin for Sarcomas
Sarcomas are heterogeneous mesenchymal malignancies arising from the bone, cartilage, muscle, peripheral nerves, adipose and fibrous connective tissues [74]. The definite cells of origin for sarcoma subtypes remain unclear [74]; however, there is increasing evidence suggesting that they probably arise from mesenchymal pluripotent stem cells [39, 74].
For instance, a growing body of evidence indicates an MSC origin for Ewing’s sarcoma. About 85% of Ewing’s sarcomas harbor translocations resulting in the fusion of the EWS gene with FLI1 gene [75]. Ectopic EWS-FLI1 expression in mMSCs results in transformation of these cells to Ewing sarcoma-like cells in vivo [76, 77]. Furthermore, the knock-down of EWS-FLI1 expression in Ewing’s Sarcoma results in conversion of the tumor cells to MSCs [78]. By the same token, both spontaneous and induced MSC models for osteosarcoma have been shown [79,80,81,82] and in both osteosarcoma cells and transformed MSCs, aberrations in genes encoding P53 pathway components have been identified; and targeted mutation in p53 of mMSCs causes development of osteosarcoma [81, 83].
Boeuf and colleagues have reported that less differentiated chondrosarcomas have more similarity with MSCs, while more differentiated ones were more similar to chondrocytes [84]. This observation suggests that chondrosarcoma formation could be the result of deregulated MSC differentiation to chondrocyte. In case of synovial sarcomas, which are often characterized by the presence of SS18-SSX1, SS18-SSX2 or SS18-SSX4 chimerical genes [85], it has been shown that silencing of the fusion gene expression in neoplastic cells induces the expression of mesenchymal markers [86]. Additionally, the expression of SYT-SSX1 in hMSCs induces a transcriptional profile very similar to the Synovial sarcoma cells [87].
In mouse models of Liposarcoma, the expression of FUS-CHOP in both bone marrow and adipose-derived mMSCs gave rise to Liposarcoma like tumors [88, 89]. Furthermore; some subtypes of Rhabdomyosarcomas are formed by the expression of either PAX3-FKHR or PAX7-FKHR fusion genes in MSCs, pushing MSC differentiation towards a myogenic lineage while inhibiting terminal differentiation [90].
All these observations suggest that multipotent and long-lived MSCs may act as the tumor initiating cells for some sarcomas upon the expression of specific fusion genes and it is presumable that engrafted MSCs may give rise to a variety of sarcomas in the recipient. On the other hand, and taking into account the cell fate conversions, these engrafted MSCs may give rise to carcinomas and Carcinosarcomas of donor origin in the recipient as well. In general, the changes from one cell type to another are observed during embryonic development, tumor formation/progression and somatic cell reprogramming [91]. In vitro and in vivo studies have shown that MSCs have the capacity to differentiate into all three embryo cell lineages (ectoderm, mesoderm and endoderm) in special media [92].
MSCs as the Cell of Origin for Carcinoma-Sarcomas
Carcinosarcomas (also known as sarcomatoid carcinomas) are biphasic neoplasms composed of malignant epithelial and mesenchymal elements. They can arise in diverse organs, such as the respiratory system [93,94,95], guts [96,97,98,99], gall bladder [100], pancreas [101], spleen [102], peritoneum [103], skin [104, 105], ovary [106], fallopian tubes [107], uterine [108], urinary system [109, 110] and adrenals [111].
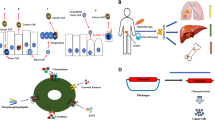
Several hypotheses have been proposed on the basis of carcinosarcomas’ pathology seen in different organs (Fig. 2) [112]. Convergence theory (multiclonal theory) suggests that two independent tumors with separate epithelial and mesenchymal origin have collided (Fig. 2a) [113]. Divergence theory (monoclonal theory) argues that both carcinomatous and sarcomatous components are derived from a single pluripotent stem cell that subsequently diverges along separate epithelial and mesenchymal pathways (Fig. 2b) [114]. Finally; conversion theory proposes that the sarcomatous element of the tumor represents a metaplastic transformation from the epithelial part (EMT) (Fig. 2c) [115]. The reverse mechanism is also supposable and MSCs could be the cells of origin to sarcomatous component and late in tumorigenesis, sarcomatous subclones go through partial MET and result in carcinomatous component formation (Fig. 2DA.
Theories proposed to explain Carcinosarcoma cell of origin; (A) Convergence theory or multiclonal theory suggests that two independent tumors with separate epithelial and mesenchymal origin have collided; (B) Divergence theory or monoclonal theory argues that both carcinomatous and sarcomatous components are derived from a single pluripotent stem cell; (C, D). Conversion theory proposes that a single epithelial or mesenchymal stem cell gives rise to carcinoma or sarcoma, respectively. Subsequently theses neoplasias go through metaplastic transformation and give rise to carcinosarcoma; SC:Stem Cell; EMT: Epithelial to Mesenchymal Transition; MET: Mesenchymal to Epithelial Transition
Monoclonality of Carcinosarcomas is supported by multiple levels of evidence such as: the co-expression of cytokeratins and epithelial membrane antigens in both carcinomatous and sarcomatous components [116], concordance of TP53 and K-ras mutations [117], identical patterns of X chromosome inactivation [118], and similar losses of heterozygosity [119].
MSCs as the Cells of Origin for Carcinomas
The epithelial barrier is exposed to several exogenous insults and the homeostasis of this tissue should be precisely balanced according to cell loss and production. One of the possible cell sources of this homeostasis is considered to be local and bone marrow leaked MSCs [120]. Following an epithelial injury, the MSCs are recruited to this site using the same mechanisms as immune cells [121]. Upon their arrival, MSCs regulate the repair process by differentiation into several kinds of stromal and damaged cell types [122, 123] including myofibroblasts [124], endothelial cell [125], and epithelial cells of the injured tissue.
The presence of MSC derived epithelium in injured ectodermal and endodermal tissues has been demonstrated by several lines of evidence. An interesting observation in regard to hMSC transdifferentiation to keratinocytes was reported by Sivamani and colleagues [126]. They reported that contact co-culture of hMSCs and keratinocytes, caused the hMSCs to adopt epithelial morphology and express keratinocyte markers [126]. Using specific differentiation protocols, several in-vitro models confirmed that acquisition of keratinocyte phenotype is a pretty probable event in epithelial regeneration after injury [127,128,129,130,131]. Interestingly, corneal keratinocyte can also be generated using MSCs [132, 133].
Transdifferentiation of MSCs to alveolar pneumocytes and their role in repair of respiratory epithelium has been studied widely. These cells are well recognized for their ability to differentiate into type II alveolar pneumocytes in damaged lungs, which is critical for re-epithelization in acute lung injury [134, 135].
In gastrointestinal tract, the epithelium needs to be renewed rapidly, in order to conserve its function. Tissue damage, for instance following local irradiation, enhances engraftment of bmMSCs in the epithelial linings of the gut, revealing a close relationship with the course of tissue regeneration [136]. Ferrand and colleagues demonstrated that MSCs fusion with gastrointestinal epithelial cells could be the predominant mechanism by which they acquire epithelial characteristics when in close contact with gastrointestinal epithelium [137]. Furthermore, MSCs transdifferentiation to hepatocytes following liver injury has been reported [138,139,140,141] and endocrine cells of pancreas (beta cells) can also be regenerated using MSCs [142,143,144].
MSCs’ role in repair of urothelial tissue has been demonstrated as well. Ning and colleagues reported that co-culture of hMSCs with urothelial cells, led to development of urothelial features in MSCs [145]. Tian et al. further revealed that MSCs can differentiate into urothelium when cultured in conditioned medium derived from bladder cell culture [146].
Bearing these in mind, it is supposable that in physiologic states, at least some parts of regenerated epithelium are originated from MSCs and the broader (the area) and longer (time duration) the injury, the more MSCs going through transdifferentiation (MET, Mesenchymal to Mesenchymal Transition (MMT), Mesenchymal to endothelial transition (M-endT)).
In 2013, the stem cell misplacement theory (SCMT) was proposed by Wang et al. to explain carcinoma formation and some obscure aspects of this event [147]. They proposed that invasive cancers are the result of misplaced epithelial stem cells which come to the wrong land of connective tissue by accident and give rise to carcinoma in the stroma de novo [147]. Herein we describe an alternative model for carcinoma formation, arising from misplaced MSCs in epithelial tissue, going through defective MET (Fig. 3).
Schematic diagram showing the process of carcinogenesis; (a). The primary insult causes disruptions in the epithelium and its basement membrane; (b, c, d). The injury attracts immune cells along with MSCs by means of chemokines and adhesion molecules; (e, f). MSCs pass through the injured basement membrane, enter the epithelial milieu and transdifferntiate to epithelial tissue (MET); (g, h, i, j); If the insults are repetitive or persistent or chronic inflammation develops (secondary insult), the newly formed epithelium from MSCs, which still has conserved their mesenchymal features, as well as their stemness, go through rapid population expansion, and nullify their tumor suppressor genes, and consequently give rise to carcinoma in situ, invasive carcinoma and metastasis
The primary insult causes disruptions in the epithelium and its basement membrane (for example UV, radiation, etc., Fig. 3a). This injury attracts immune cells along with bmMSCs by means of cytokines/chemokines and adhesion molecules (Fig. 3b,c) [121]. bmMSCs pass through the injured basement membrane, enter the epithelial milieu and transdifferntiate to epithelial tissue (MET), mostly due to direct contact with epithelial cells and encountering their growth media (Fig. 3d,e,f) [126, 145, 146]. At the very beginning these misplaced cells are neither genetically mutated nor transformed neoplastic cells. However, it is supposable that this newly formed epithelial tissue still conserves its mesenchymal and stem cell features. If the insults are repetitive or persistent or chronic inflammation develops (secondary insult), as a consequence of recurring exposure to growth factors, cytokines, etc. the newly formed epithelium from MSCs, which still has conserved their mesenchymal features and stemness, go through rapid population expansion, and nullify their tumor suppressor genes, and consequently give rise to carcinoma cells, presenting EMT/MET markers, and aggressive behavior (Fig. 3G,H,I,J). Our hypothesis chains together other carcinogenesis theories such as the tissue organization field theory, the stem cell theory and the inflammation-cancer chain.
There are multiple lines of molecular and clinical evidence supporting this hypothesis. For instance, both colon and small intestine contain Lgr5+ multipotent stem cells, but cancer of digestive tract occurs preferentially in the colon and rectum, although epithelium turn-over is higher in small intestine [148]. These controversial observations could be explained fairly by the model we proposed. The repetitive injury and inflammatory milieu in colon attracts bmMSCs, which gives rise to colon epithelium and carcinoma consequently due to chronic induction of cytokines and growth factors. The same model can be applied to any carcinoma formation following chronic inflammation, such as Marjolin ulcer, Bladder SCC (following chronic schistozomia infection), hepatocellular carcinoma (HCC) (following chronic hepatitis and cirrhosis), non-small cell lung cancer (following chronic inflammation due to smoking), cervical cancer (following chronic HPV infection), and many other examples. Furthermore, this model easily describes carcinosarcoma formation and its monoclonality.
A more tangible evidence for our model is observed in kidney transplant patients. Squamous Cell Carcinoma (SCC) is a well-known complication in long term kidney transplant recipients [149]. Verneuil and colleagues have reported the presence of donor-derived epithelial cells in skin SCC and actinic keratosis [150]. In an attempt to further clarify the type of donor cell that has homed to these skin lesions, they observed donor-derived stem-cells in basal layers and invasive areas in all skin SCCs, but not in surrounding normal skin. These donor-derived stem-cells expressed the EMT markers, vimentin, snail and slug in SCCs [151]. It is probable that the MSCs engrafted along with the kidney, had been hijacked by injured epithelium and their consequent transdifferentiation to and integration in the epithelium, creates a tissue with higher susceptibility to carcinogens (Fig. 3).
The role of chronic inflammation and the molecules involved in development of carcinomas has been studied extensively. Interestingly, some vague parts of these mechanisms can be enlightened by the model we proposed. For instance, the NF-κB pathway is one of the most fascinating links between inflammation and cancer formation and following its activation EMT regulators Snail and Slug are activated, which leads to downregulation of E-cadherin [152], and supposedly cell separation and cancer progression. However, inhibition of this pathway has been shown to enhance the growth of SCC and HCC [153, 154]. The progression of SCC and HCC following NF-κB pathway inhibition can be explained by our model, considering MSCs going through partial MET and giving rise to these carcinoma cells.
Another observation is in regard to Wnt/β-catenin pathway, which is supposed to play roles in EMT [155]. Vermeulen and colleagues showed that cancer cells with high Wnt pathway activity are observed near stromal myofibroblasts [156]. We can explain this observation by considering MSCs going through both MMT and MET, giving rise to both carcinoma cells and myofibroblasts. In fact, EMT and MET are reversible processes, and observations are a snapshot en route to full EMT/MET and thus could not be representative of a precise epithelial or mesenchymal state [157] and considering the role of MET in carcinoma formation is as fair as EMT based hypotheses.
Conclusion
The high complexity and diversity in cancer development is still unraveled and through previous decades, cancer models have been re-written several times. In this paper, we presented a model of carcinogenesis which chains together the tissue organization field theory, the stem cell theory and the inflammation-cancer chain. In this model we propose that tissue resident stem cells could be leaked cells from bmMSC pool to various injured tissue, which consequently transform and integrate in the host tissue. If the insult persists or chronic inflammation develops, as a consequence of recurring exposure to growth factors, cytokines, etc. the newly formed tissue from MSCs, which still has conserved their mesenchymal features, as well as their stemness, go through rapid population expansion, and nullify their tumor suppressor genes, and hence give rise to neoplastic cell (both carcinoma and sarcoma, as well as carcino-sarcomas). Considering the probability of this hypothesis being true, the clinical and therapeutic use of MSCs should be with caution and careful surveys, and the recipients’ long term follow-up seems to be insightful.
References
Nombela-Arrieta, C., Ritz, J., & Silberstein, L. E. (2011). The elusive nature and function of mesenchymal stem cells. Nature Reviews. Molecular Cell Biology, 12(2), 126–131. https://doi.org/10.1038/nrm3049.
Charbord, P. (2010). Bone marrow mesenchymal stem cells: historical overview and concepts. Human Gene Therapy, 21(9), 1045–1056. https://doi.org/10.1089/hum.2010.115.
Friedenstein, A. J., Piatetzky II, S., & Petrakova, K. V. (1966). Osteogenesis in transplants of bone marrow cells. Journal of Embryology and Experimental Morphology, 16(3), 381–390.
Friedenstein, A. J., Chailakhjan, R. K., & Lalykina, K. S. (1970). The development of fibroblast colonies in monolayer cultures of guinea-pig bone marrow and spleen cells. Cell and Tissue Kinetics, 3(4), 393–403.
Caplan, A. I. (1991). Mesenchymal stem cells. Journal of Orthopaedic Research, 9(5), 641–650. https://doi.org/10.1002/jor.1100090504.
Ullah, I., Subbarao, R. B., & Rho, G. J. (2015). Human mesenchymal stem cells - current trends and future prospective. [Research Support, Non-U.S. Gov't Review]. Bioscience Reports, 35(2). https://doi.org/10.1042/BSR20150025.
Dominici, M., Le Blanc, K., Mueller, I., Slaper-Cortenbach, I., Marini, F., Krause, D., et al. (2006). Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy, 8(4), 315–317. https://doi.org/10.1080/14653240600855905.
Horwitz, E. M., Le Blanc, K., Dominici, M., Mueller, I., Slaper-Cortenbach, I., Marini, F. C., et al. (2005). Clarification of the nomenclature for MSC: The International Society for Cellular Therapy position statement. Cytotherapy, 7(5), 393–395. https://doi.org/10.1080/14653240500319234.
Wang, Y., Chen, X., Cao, W., & Shi, Y. (2014). Plasticity of mesenchymal stem cells in immunomodulation: pathological and therapeutic implications. Nature Immunology, 15(11), 1009–1016. https://doi.org/10.1038/ni.3002.
Meirelles Lda, S., Fontes, A. M., Covas, D. T., & Caplan, A. I. (2009). Mechanisms involved in the therapeutic properties of mesenchymal stem cells. Cytokine & Growth Factor Reviews, 20(5–6), 419–427. https://doi.org/10.1016/j.cytogfr.2009.10.002.
Phinney, D. G., Galipeau, J., Krampera, M., Martin, I., Shi, Y., & Sensebe, L. (2013). MSCs: science and trials. Nature Medicine, 19(7), 812. https://doi.org/10.1038/nm.3220.
Elzaouk, L., Moelling, K., & Pavlovic, J. (2006). Anti-tumor activity of mesenchymal stem cells producing IL-12 in a mouse melanoma model. Experimental Dermatology, 15(11), 865–874. https://doi.org/10.1111/j.1600-0625.2006.00479.x.
Khakoo, A. Y., Pati, S., Anderson, S. A., Reid, W., Elshal, M. F., Rovira, I. I., et al. (2006). Human mesenchymal stem cells exert potent antitumorigenic effects in a model of Kaposi's sarcoma. The Journal of Experimental Medicine, 203(5), 1235–1247. https://doi.org/10.1084/jem.20051921.
Karnoub, A. E., Dash, A. B., Vo, A. P., Sullivan, A., Brooks, M. W., Bell, G. W., et al. (2007). Mesenchymal stem cells within tumour stroma promote breast cancer metastasis. Nature, 449(7162), 557–563. https://doi.org/10.1038/nature06188.
Ridge, S. M., Sullivan, F. J., & Glynn, S. A. (2017). Mesenchymal stem cells: key players in cancer progression. Molecular Cancer, 16(1), 31. https://doi.org/10.1186/s12943-017-0597-8.
Kidd, S., Spaeth, E., Dembinski, J. L., Dietrich, M., Watson, K., Klopp, A., et al. (2009). Direct Evidence of Mesenchymal Stem Cell Tropism for Tumor and Wounding Microenvironments Using In Vivo Bioluminescent Imaging. Stem Cells, 27(10), 2614–2623. https://doi.org/10.1002/stem.187.
Quante, M., Tu, S. P., Tomita, H., Gonda, T., Wang, S. S., Takashi, S., et al. (2011). Bone marrow-derived myofibroblasts contribute to the mesenchymal stem cell niche and promote tumor growth. Cancer Cell, 19(2), 257–272. https://doi.org/10.1016/j.ccr.2011.01.020.
Spaeth, E., Klopp, A., Dembinski, J., Andreeff, M., & Marini, F. (2008). Inflammation and tumor microenvironments: defining the migratory itinerary of mesenchymal stem cells. Gene Therapy, 15(10), 730–738. https://doi.org/10.1038/gt.2008.39.
Bartosh, T. J., Ullah, M., Zeitouni, S., Beaver, J., & Prockop, D. J. (2016). Cancer cells enter dormancy after cannibalizing mesenchymal stem/stromal cells (MSCs). Proceedings of the National Academy of Sciences of the United States of America, 113(42), E6447–E6456. https://doi.org/10.1073/pnas.1612290113.
Shi, Y., Du, L., Lin, L., & Wang, Y. (2017). Tumour-associated mesenchymal stem/stromal cells: emerging therapeutic targets. Nature Reviews. Drug Discovery, 16(1), 35–52. https://doi.org/10.1038/nrd.2016.193.
Ishihara, S., Inman, D. R., Li, W. J., Ponik, S. M., & Keely, P. (2017). Mechano-signal transduction in mesenchymal stem cells induces prosaposin secretion to drive the proliferation of breast cancer cells. Cancer Research. https://doi.org/10.1158/0008-5472.CAN-17-0569.
Barcellos-de-Souza, P., Comito, G., Pons-Segura, C., Taddei, M. L., Gori, V., Becherucci, V., et al. (2016). Mesenchymal stem cells are recruited and activated into carcinoma-associated fibroblasts by prostate cancer microenvironment-derived TGF-1. Stem Cells, 34(10), 2536–2547. https://doi.org/10.1002/stem.2412.
Mishra, P. J., Mishra, P. J., Humeniuk, R., Medina, D. J., Alexe, G., Mesirov, J. P., et al. (2008). Carcinoma-associated fibroblast-like differentiation of human mesenchymal stem cells. Cancer Research, 68(11), 4331–4339. https://doi.org/10.1158/0008-5472.Can-08-0943.
Wang, Y., Liu, J., Jiang, Q., Deng, J., Xu, F., Chen, X., et al. (2017). Human adipose-derived mesenchymal stem cell-secreted CXCL1 and CXCL8 facilitate breast tumor growth by promoting angiogenesis. Stem Cells, 35(9), 2060–2070. https://doi.org/10.1002/stem.2643.
Zhou, X. M., Wang, D., He, H. L., Tang, J., Wu, J., Xu, L., et al. (2017). Bone marrow derived mesenchymal stem cells involve in the lymphangiogenesis of lung cancer and Jinfukang inhibits the involvement in vivo. Journal of Cancer, 8(10), 1786–1794. https://doi.org/10.7150/jca.17859.
Huang, W. H., Chang, M. C., Tsai, K. S., Hung, M. C., Chen, H. L., & Hung, S. C. (2013). Mesenchymal stem cells promote growth and angiogenesis of tumors in mice. Oncogene, 32(37), 4343–4354. https://doi.org/10.1038/onc.2012.458.
Beckermann, B. M., Kallifatidis, G., Groth, A., Frommhold, D., Apel, A., Mattern, J., et al. (2008). VEGF expression by mesenchymal stem cells contributes to angiogenesis in pancreatic carcinoma. British Journal of Cancer, 99(4), 622–631. https://doi.org/10.1038/sj.bjc.6604508.
Chen, K., Liu, Q., Tsang, L. L., Ye, Q., Chan, H. C., Sun, Y., et al. (2017). Human MSCs promotes colorectal cancer epithelial-mesenchymal transition and progression via CCL5/beta-catenin/Slug pathway. Cell Death & Disease, 8(5), e2819. https://doi.org/10.1038/cddis.2017.138.
Takigawa, H., Kitadai, Y., Shinagawa, K., Yuge, R., Higashi, Y., Tanaka, S., et al. (2017). Mesenchymal stem cells induce epithelial to mesenchymal transition in colon cancer cells through direct cell-to-cell contact. Neoplasia, 19(5), 429–438. https://doi.org/10.1016/j.neo.2017.02.010.
Martin, F. T., Dwyer, R. M., Kelly, J., Khan, S., Murphy, J. M., Curran, C., et al. (2010). Potential role of mesenchymal stem cells (MSCs) in the breast tumour microenvironment: stimulation of epithelial to mesenchymal transition (EMT). Breast Cancer Research and Treatment, 124(2), 317–326. https://doi.org/10.1007/s10549-010-0734-1.
So, K. A., Min, K. J., Hong, J. H., & Lee, J. K. (2015). Interleukin-6 expression by interactions between gynecologic cancer cells and human mesenchymal stem cells promotes epithelial-mesenchymal transition. International Journal of Oncology, 47(4), 1451–1459. https://doi.org/10.3892/ijo.2015.3122.
Maffey, A., Storini, C., Diceglie, C., Martelli, C., Sironi, L., Calzarossa, C., et al. (2017). Mesenchymal stem cells from tumor microenvironment favour breast cancer stem cell proliferation, cancerogenic and metastatic potential, via ionotropic purinergic signalling. Scientific Reports, 7(1), 13162. https://doi.org/10.1038/s41598-017-13460-7.
El-Badawy, A., Ghoneim, M. A., Gabr, M. M., Salah, R. A., Mohamed, I. K., Amer, M., et al. (2017). Cancer cell-soluble factors reprogram mesenchymal stromal cells to slow cycling, chemoresistant cells with a more stem-like state. Stem Cell Research & Therapy, 8(1), 254. https://doi.org/10.1186/s13287-017-0709-9.
Jiang, C., Zhang, Q., Shanti, R. M., Shi, S., Chang, T. H., Carrasco, L., et al. (2017). Mesenchymal stromal cell-derived interleukin-6 promotes epithelial-mesenchymal transition and acquisition of epithelial stem-like cell properties in ameloblastoma epithelial cells. Stem Cells, 35(9), 2083–2094. https://doi.org/10.1002/stem.2666.
Cortini, M., Massa, A., Avnet, S., Bonuccelli, G., & Baldini, N. (2016). Tumor-activated mesenchymal stromal cells promote osteosarcoma stemness and migratory potential via IL-6 secretion. PLoS One, 11(11), e0166500. https://doi.org/10.1371/journal.pone.0166500.
Lu, J. H., Wei, H. J., Peng, B. Y., Chou, H. H., Chen, W. H., Liu, H. Y., et al. (2016). Adipose-derived stem cells enhance cancer stem cell property and tumor formation capacity in Lewis lung carcinoma cells through an interleukin-6 paracrine circuit. Stem Cells and Development, 25(23), 1833–1842. https://doi.org/10.1089/scd.2016.0163.
Hossain, A., Gumin, J., Gao, F., Figueroa, J., Shinojima, N., Takezaki, T., et al. (2015). Mesenchymal stem cells isolated from human gliomas increase proliferation and maintain stemness of glioma stem cells through the IL-6/gp130/STAT3 pathway. Stem Cells, 33(8), 2400–2415. https://doi.org/10.1002/stem.2053.
Xiao, W., Mohseny, A. B., Hogendoorn, P. C., & Cleton-Jansen, A. M. (2013). Mesenchymal stem cell transformation and sarcoma genesis. Clinical Sarcoma Research, 3(1), 10. https://doi.org/10.1186/2045-3329-3-10.
Yang, J., Ren, Z., Du, X., Hao, M., & Zhou, W. (2014). The role of mesenchymal stem/progenitor cells in sarcoma: update and dispute. Stem Cell Investigation, 1, 18. https://doi.org/10.3978/j.issn.2306-9759.2014.10.01.
Spaeth, E. L., Dembinski, J. L., Sasser, A. K., Watson, K., Klopp, A., Hall, B., et al. (2009). Mesenchymal stem cell transition to tumor-associated fibroblasts contributes to fibrovascular network expansion and tumor progression. PLoS One, 4(4), e4992. https://doi.org/10.1371/journal.pone.0004992.
Worthley, D. L., Ruszkiewicz, A., Davies, R., Moore, S., Nivison-Smith, I., To, L. B., et al. (2009). Human Gastrointestinal Neoplasia-Associated Myofibroblasts Can Develop from Bone Marrow-Derived Cells Following Allogeneic Stem Cell Transplantation. Stem Cells, 27(6), 1463–1468. https://doi.org/10.1002/stem.63.
Li, G. C., Zhang, H. W., Zhao, Q. C., Sun, L. I., Yang, J. J., Hong, L., et al. (2016). Mesenchymal stem cells promote tumor angiogenesis via the action of transforming growth factor beta1. Oncology Letters, 11(2), 1089–1094. https://doi.org/10.3892/ol.2015.3997.
Bexell, D., Gunnarsson, S., Tormin, A., Darabi, A., Gisselsson, D., Roybon, L., et al. (2009). Bone marrow multipotent mesenchymal stroma cells act as pericyte-like migratory vehicles in experimental gliomas. Molecular Therapy, 17(1), 183–190. https://doi.org/10.1038/mt.2008.229.
Wang, H. H., Cui, Y. L., Zaorsky, N. G., Lan, J., Deng, L., Zeng, X. L., et al. (2016). Mesenchymal stem cells generate pericytes to promote tumor recurrence via vasculogenesis after stereotactic body radiation therapy. Cancer Letters, 375(2), 349–359. https://doi.org/10.1016/j.canlet.2016.02.033.
Sun, B., Zhang, S. W., Ni, C. S., Zhang, D. F., Liu, Y. X., Zhang, W. Z., et al. (2005). Correlation between melanoma angiogenesis and the mesenchymal stem cells and endothelial progenitor cells derived from bone marrow. Stem Cells and Development, 14(3), 292–298. https://doi.org/10.1089/scd.2005.14.292.
Petit, I., Jin, D., & Rafii, S. (2007). The SDF-1-CXCR4 signaling pathway: a molecular hub modulating neo-angiogenesis. Trends in Immunology, 28(7), 299–307. https://doi.org/10.1016/j.it.2007.05.007.
Li, P., Zhou, H., Di, G., Liu, J., Liu, Y., Wang, Z., et al. (2017). Mesenchymal stem cell-conditioned medium promotes MDA-MB-231 cell migration and inhibits A549 cell migration by regulating insulin receptor and human epidermal growth factor receptor 3 phosphorylation. Oncology Letters, 13(3), 1581–1586. https://doi.org/10.3892/ol.2017.5641.
Bie, Q., Zhang, B., Sun, C., Ji, X., Barnie, P. A., Qi, C., et al. (2017). IL-17B activated mesenchymal stem cells enhance proliferation and migration of gastric cancer cells. Oncotarget, 8(12), 18914–18923. https://doi.org/10.18632/oncotarget.14835.
Wu, Y. L., Li, H. Y., Zhao, X. P., Jiao, J. Y., Tang, D. X., Yan, L. J., et al. (2017). Mesenchymal stem cell-derived CCN2 promotes the proliferation, migration and invasion of human tongue squamous cell carcinoma cells. Cancer Science, 108(5), 897–909. https://doi.org/10.1111/cas.13202.
McAndrews, K. M., McGrail, D. J., Ravikumar, N., & Dawson, M. R. (2015). Mesenchymal stem cells induce directional migration of Invasive breast cancer cells through TGF-beta. Scientific Reports, 5, 16941. https://doi.org/10.1038/srep16941.
Melzer, C., von der Ohe, J., Lehnert, H., Ungefroren, H., & Hass, R. (2017). Cancer stem cell niche models and contribution by mesenchymal stroma/stem cells. Molecular Cancer, 16(1), 28. https://doi.org/10.1186/s12943-017-0595-x.
Aponte, P. M., & Caicedo, A. (2017). Stemness in cancer: stem cells, cancer stem cells, and their microenvironment. Stem Cells International, Artn 5619472. https://doi.org/10.1155/2017/5619472.
Visvader, J. E. (2011). Cells of origin in cancer. Nature, 469(7330), 314–322. https://doi.org/10.1038/nature09781.
Plaks, V., Kong, N. W., & Werb, Z. (2015). The Cancer Stem Cell Niche: How Essential Is the Niche in Regulating Stemness of Tumor Cells? Cell Stem Cell, 16(3), 225–238. https://doi.org/10.1016/j.stem.2015.02.015.
Ye, J., Wu, D., Wu, P., Chen, Z. G., & Huang, J. (2014). The cancer stem cell niche: cross talk between cancer stem cells and their microenvironment. Tumor Biology, 35(5), 3945–3951. https://doi.org/10.1007/s13277-013-1561-x.
Sottile, F., Aulicino, F., Theka, I., & Cosma, M. P. (2016). Mesenchymal stem cells generate distinct functional hybrids in vitro via cell fusion or entosis. Scientific Reports, 6, 36863. https://doi.org/10.1038/srep36863.
Cabarcas, S. M., Mathews, L. A., & Farrar, W. L. (2011). The cancer stem cell niche-there goes the neighborhood? International Journal of Cancer, 129(10), 2315–2327. https://doi.org/10.1002/ijc.26312.
Davis, H., Irshad, S., Bansal, M., Rafferty, H., Boitsova, T., Bardella, C., et al. (2015). Aberrant epithelial GREM1 expression initiates colonic tumorigenesis from cells outside the stem cell niche. Nature Medicine, 21(1), 62–70. https://doi.org/10.1038/nm.3750.
McLean, K., Gong, Y., Choi, Y., Deng, N., Yang, K., Bai, S., et al. (2011). Human ovarian carcinoma-associated mesenchymal stem cells regulate cancer stem cells and tumorigenesis via altered BMP production. The Journal of Clinical Investigation, 121(8), 3206–3219. https://doi.org/10.1172/JCI45273.
Ding, D. C., Liu, H. W., & Chu, T. Y. (2016). Interleukin-6 from ovarian mesenchymal stem cells promotes proliferation, sphere and colony formation and tumorigenesis of an ovarian cancer cell line SKOV3. Journal of Cancer, 7(13), 1815–1823. https://doi.org/10.7150/jca.16116.
Li, H. J., Reinhardt, F., Herschman, H. R., & Weinberg, R. A. (2012). Cancer-stimulated mesenchymal stem cells create a carcinoma stem cell niche via prostaglandin E2 signaling. Cancer Discovery, 2(9), 840–855. https://doi.org/10.1158/2159-8290.CD-12-0101.
Luo, J., Ok Lee, S., Liang, L., Huang, C. K., Li, L., Wen, S., et al. (2014). Infiltrating bone marrow mesenchymal stem cells increase prostate cancer stem cell population and metastatic ability via secreting cytokines to suppress androgen receptor signaling. Oncogene, 33(21), 2768–2778. https://doi.org/10.1038/onc.2013.233.
Liu, S., Ginestier, C., Ou, S. J., Clouthier, S. G., Patel, S. H., Monville, F., et al. (2011). Breast cancer stem cells are regulated by mesenchymal stem cells through cytokine networks. Cancer Research, 71(2), 614–624. https://doi.org/10.1158/0008-5472.CAN-10-0538.
Tsai, K. S., Yang, S. H., Lei, Y. P., Tsai, C. C., Chen, H. W., Hsu, C. Y., et al. (2011). Mesenchymal stem cells promote formation of colorectal tumors in mice. Gastroenterology, 141(3), 1046–1056. https://doi.org/10.1053/j.gastro.2011.05.045.
Cheng, P., Wang, J., Waghmare, I., Sartini, S., Coviello, V., Zhang, Z., et al. (2016). FOXD1-ALDH1A3 signaling is a determinant for the self-renewal and tumorigenicity of mesenchymal glioma stem cells. Cancer Research, 76(24), 7219–7230. https://doi.org/10.1158/0008-5472.CAN-15-2860.
Cuiffo, B. G., Campagne, A., Bell, G. W., Lembo, A., Orso, F., Lien, E. C., et al. (2014). MSC-regulated microRNAs converge on the transcription factor FOXP2 and promote breast cancer metastasis. Cell Stem Cell, 15(6), 762–774. https://doi.org/10.1016/j.stem.2014.10.001.
Coffman, L. G., Choi, Y. J., McLean, K., Allen, B. L., di Magliano, M. P., & Buckanovich, R. J. (2016). Human carcinoma-associated mesenchymal stem cells promote ovarian cancer chemotherapy resistance via a BMP4/HH signaling loop. Oncotarget, 7(6), 6916–6932. https://doi.org/10.18632/oncotarget.6870.
Xue, J. G., Zhu, Y., Sun, Z. X., Ji, R. B., Zhang, X., Xu, W. R., et al. (2015). Tumorigenic hybrids between mesenchymal stem cells and gastric cancer cells enhanced cancer proliferation, migration and stemness. BMC Cancer, 15, ARTN 793. https://doi.org/10.1186/s12885-015-1780-1.
Gabashvili, A. N., Baklaushev, V. P., Grinenko, N. F., Mel'nikov, P. A., Cherepanov, S. A., Levinsky, A. B., et al. (2016). Antitumor Activity of Rat Mesenchymal Stem Cells during Direct or Indirect Co-Culturing with C6 Glioma Cells. Bulletin of Experimental Biology and Medicine, 160(4), 519–524. https://doi.org/10.1007/s10517-016-3211-y.
Berger, M., Muraro, M., Fagioli, F., & Ferrari, S. (2008). Osteosarcoma derived from donor stem cells carrying the Norrie's disease gene. The New England Journal of Medicine, 359(23), 2502–2504. https://doi.org/10.1056/NEJMc0807172.
Qian, H., Ding, X., Zhang, J., Mao, F., Sun, Z., Jia, H., et al. (2017). Cancer stemness and metastatic potential of the novel tumor cell line K3: an inner mutated cell of bone marrow-derived mesenchymal stem cells. Oncotarget, 8(24), 39522–39533. https://doi.org/10.18632/oncotarget.17133.
Rodriguez, R., Rubio, R., & Menendez, P. (2012). Modeling sarcomagenesis using multipotent mesenchymal stem cells. Cell Research, 22(1), 62–77. https://doi.org/10.1038/cr.2011.157.
Lye, K. L., Nordin, N., Vidyadaran, S., & Thilakavathy, K. (2016). Mesenchymal stem cells: From stem cells to sarcomas. Cell Biology International, 40(6), 610–618. https://doi.org/10.1002/cbin.10603.
Tu, J., Huo, Z., Gingold, J., Zhao, R., Shen, J., & Lee, D. F. (2017). The Histogenesis of Ewing Sarcoma. Cancer Reports and Reviews, 1(2). https://doi.org/10.15761/CRR.1000111.
Yeny, C. T., Eliazer, S., Xiang, L. L., Richardson, J. A., & Ilaria, R. L. (2005). Expression of the EWS/FLI-1 oncogene in murine primary bone-derived cells results in EWS/FLI-1-dependent, Ewing sarcoma-like tumors. Cancer Research, 65(19), 8698–8705. https://doi.org/10.1158/0008-5472.
Riggi, N., Cironi, L., Provero, P., Suva, M. L., Kaloulis, K., Garcia-Echeverria, C., et al. (2005). Development of Ewing's sarcoma from primary bone marrow-derived mesenchymal progenitor cells. Cancer Research, 65(24), 11459–11468. https://doi.org/10.1158/0008-5472.Can-05-1696.
Tirode, F., Laud-Duval, K., Prieur, A., Delorme, B., Charbord, P., & Delattre, O. (2007). Mesenchymal stem cell features of Ewing tumors. Cancer Cell, 11(5), 421–429. https://doi.org/10.1016/j.ccr.2007.02.027.
Shimizu, T., Ishikawa, T., Sugihara, E., Kuninaka, S., Miyamoto, T., Mabuchi, Y., et al. (2010). c-MYC overexpression with loss of Ink4a/Arf transforms bone marrow stromal cells into osteosarcoma accompanied by loss of adipogenesis. Oncogene, 29(42), 5687–5699. https://doi.org/10.1038/onc.2010.312.
Rodriguez, R., Rubio, R., Masip, M., Catalina, P., Nieto, A., de la Cueva, T., et al. (2009). Loss of p53 induces tumorigenesis in p21-deficient mesenchymal stem cells. Neoplasia, 11(4), 397–U106. https://doi.org/10.1593/neo.81620.
Mohseny, A. B., Szuhai, K., Romeo, S., Buddingh, E. P., Briaire-de Bruijn, I., de Jong, D., et al. (2009). Osteosarcoma originates from mesenchymal stem cells in consequence of aneuploidization and genomic loss of Cdkn2. The Journal of Pathology, 219(3), 294–305. https://doi.org/10.1002/path.2603.
Tolar, J., Nauta, A. J., Osborn, M. J., Mortari, A. P., McElmurry, R. T., Bell, S., et al. (2007). Sarcoma derived from cultured mesenchymal stem cells. Stem Cells, 25(2), 371–379. https://doi.org/10.1634/stemcells.2005-0620.
Lin, P. P., Pandey, M. K., Jin, F., Raymond, A. K., Akiyama, H., & Lozano, G. (2009). Targeted mutation of p53 and Rb in mesenchymal cells of the limb bud produces sarcomas in mice. Carcinogenesis, 30(10), 1789–1795. https://doi.org/10.1093/carcin/bgp180.
Boeuf, S., Kunz, P., Hennig, T., Lehner, B., Hogendoorn, P. C. W., Bovee, J. V. M. G., et al. (2008). A chondrogenic gene expression signature in mesenchymal stem cells is a classifier of conventional central chondrosarcoma. Journal of Pathology, 216(2), 158–166. https://doi.org/10.1002/path.2389.
Jain, S., Xu, R. L., Prieto, V. G., & Lee, P. (2010). Molecular classification of soft tissue sarcomas and its clinical applications. International Journal of Clinical and Experimental Pathology, 3(4), 416–428.
Naka, N., Takenaka, S., Araki, N., Miwa, T., Hashimoto, N., Yoshioka, K., et al. (2010). Synovial sarcoma is a stem cell malignancy. Stem Cells, 28(7), 1119–1131. https://doi.org/10.1002/stem.452.
Cironi, L., Provero, P., Riggi, N., Janiszewska, M., Suva, D., Suva, M. L., et al. (2009). Epigenetic features of human mesenchymal stem cells determine their permissiveness for induction of relevant transcriptional changes by SYT-SSX1. PLoS One, 4(11), ARTN e7904. https://doi.org/10.1371/journal.pone.0007904.
Rodriguez, R., Rubio, R., Gutierrez-Aranda, I., Melen, G. J., Elosua, C., Garcia-Castro, J., et al. (2011). FUS-CHOP fusion protein expression coupled to p53 deficiency induces liposarcoma in mouse but not in human adipose-derived mesenchymal stem/stromal cells. Stem Cells, 29(2), 179–192. https://doi.org/10.1002/stem.571.
Riggi, N., Cironi, L., Provero, P., Suva, M. L., Stehle, J. C., Baumer, K., et al. (2006). Expression of the FUS-CHOP fusion protein in primary mesenchymal progenitor cells gives rise to a model of myxoid liposarcoma. Cancer Research, 66(14), 7016–7023. https://doi.org/10.1158/0008-5472.CAN-05-3979.
Charytonowicz, E., Cordon-Cardo, C., Matushansky, I., & Ziman, M. (2009). Alveolar rhabdomyosarcoma: Is the cell of origin a mesenchymal stem cell? Cancer Letters, 279(2), 126–136. https://doi.org/10.1016/j.canlet.2008.09.039.
Li, X., Pei, D. Q., & Zheng, H. (2014). Transitions between epithelial and mesenchymal states during cell fate conversions. Protein & Cell, 5(8), 580–591. https://doi.org/10.1007/s13238-014-0064-x.
Ullah, I., Subbarao, R. B., & Rho, G. J. (2015). Human mesenchymal stem cells - current trends and future prospective. Bioscience Reports, 35, ARTN e00191. https://doi.org/10.1042/BSR20150025.
Yang, H., Lin, Y., & Liang, Y. (2017). Treatment of Lung Carcinosarcoma and Other Rare Histologic Subtypes of Non-small Cell Lung Cancer. Current Treatment Options in Oncology, 18(9), 54. https://doi.org/10.1007/s11864-017-0494-9.
Jang, S. H., Cho, H. D., Lee, J. H., Lee, H. J., Hong, S. A., Cho, J., et al. (2017). Sarcomatoid carcinoma in the trachea: A case report and literature review. Thoracic Cancer, 8(3), 278–282. https://doi.org/10.1111/1759-7714.12437.
Guan, M., Li, Y., Shi, Z. G., Xie, L. S., & Cao, X. L. (2014). Sarcomatoid carcinoma involving the nasal cavity and paranasal sinus: a rare and highly progressive tumor. International Journal of Clinical and Experimental Pathology, 7(7), 4489–4492.
Tanaka, H., Baba, Y., Matsusaki, S., Isono, Y., Kumazawa, H., Sase, T., et al. (2015). So-called carcinosarcoma of the duodenum with a chondrosarcomatous component. Clinical Journal of Gastroenterology, 8(5), 268–274. https://doi.org/10.1007/s12328-015-0595-6.
Choi, K. W., Lee, W. Y., Hong, S. W., Chang, Y. G., Lee, B., & Lee, H. K. (2013). Carcinosarcoma of the stomach: A case report. Journal of Gastric Cancer, 13(1), 69–72. https://doi.org/10.5230/jgc.2013.13.1.69.
Ambrosini-Spaltro, A., Vaira, V., Braidotti, P., Rovati, M. P., Ferrero, S., & Bosari, S. (2006). Carcinosarcoma of the colon: report of a case with morphological, ultrastructural and molecular analysis. BMC Cancer, 6, 185. https://doi.org/10.1186/1471-2407-6-185.
Feng, D., Fidele, N. B., Agustin, M. M., Jian, G., Bourleyi, S. I., Augustin, L., et al. (2015). Carcinosarcoma of parotid gland (malignant mixed tumor). Annals of Maxillofacial Surgery, 5(2), 240–243. https://doi.org/10.4103/2231-0746.175757.
Gao, S., Huang, L., Dai, S., Chen, D., Dai, R., & Shan, Y. (2015). Carcinosarcoma of the gallbladder: a case report and review of the literature. International Journal of Clinical and Experimental Pathology, 8(6), 7464–7469.
Li, B. Q., Liu, Q. F., Chang, X. Y., Hu, Y., Chen, J., & Guo, J. C. (2017). Pancreatic carcinosarcoma mimics malignant intraductal papillary mucinous neoplasm: A rare case report and literature review. Medicine, 96(23), ARTN e6961. https://doi.org/10.1097/MD.0000000000006961.
Sun, T., Wang, G. F., & Zhang, Y. (2017). Primary splenic carcinosarcoma with local invasion of chest wall: a rare case. Journal of Zhejiang University-Science B, 18(8), 717–722. https://doi.org/10.1631/jzus.B1700262.
Wang, B., Ren, K. W., Yang, Y. C., Wan, D. L., Li, X. J., Zhai, Z. L., et al. (2016). Carcinosarcoma of the lesser omentum a unique case report and literature review. Medicine, 95(14), ARTN e3246. https://doi.org/10.1097/MD.0000000000003246.
Clark, J. J., Bowen, A. R., Bowen, G. M., Hyngstrom, J. R., Hadley, M. L., Duffy, K., et al. (2017). Cutaneous carcinosarcoma: a series of six cases and a review of the literature. Journal of Cutaneous Pathology, 44(1), 34–44. https://doi.org/10.1111/cup.12843.
Harms, P. W., Fullen, D. R., Patel, R. M., Chang, D., Shalin, S. C., Ma, L. L., et al. (2015). Cutaneous basal cell carcinosarcomas: evidence of clonality and recurrent chromosomal losses. Human Pathology, 46(5), 690–697. https://doi.org/10.1016/j.humpath.2015.01.006.
George, E. M., Herzog, T. J., Neugut, A. I., Lu, Y. S., Burke, W. M., Lewin, S. N., et al. (2013). Carcinosarcoma of the ovary: Natural history, patterns of treatment, and outcome. Gynecologic Oncology, 131(1), 42–45. https://doi.org/10.1016/j.ygyno.2013.06.034.
Gupta, R., & Jenison, E. L. (2011). A rare case of carcinosarcoma of the fallopian tube presenting with torsion, rupture and hemoperitoneum. Gynecologic Oncology Case Reports, 2(1), 4–5. https://doi.org/10.1016/j.gynor.2011.11.001.
Singh, R. (2014). Review literature on uterine carcinosarcoma. Journal of Cancer Research and Therapeutics, 10(3), 461–468. https://doi.org/10.4103/0973-1482.138197.
Basibuyuk, I., Topaktas, R., & Elbir, F. (2017). Bladder carcinosarcoma: A case report with review of the literature. Archivio Italiano di Urologia, Andrologia, 89(3), 240–242. https://doi.org/10.4081/aiua.2017.3.240.
Liu, J., & Wu, H. (2011). Carcinosarcoma of female urethra with melanocytic differentiation. International Journal of Clinical and Experimental Pathology, 4(2), 206–209.
Sasaki, K., Desimone, M., Rao, H. R., Huang, G. J., & Seethala, R. R. (2010). Adrenocortical carcinosarcoma: a case report and review of the literature. Diagnostic Pathology, 5, Artn 51. https://doi.org/10.1186/1746-1596-5-51.
Loh, T. L., Tomlinson, J., Chin, R., & Eslick, G. D. (2014). Cutaneous carcinosarcoma with metastasis to the parotid gland. Case Reports in Otolaryngology, 2014, 173235. https://doi.org/10.1155/2014/173235.
Wick, M. R., & Swanson, P. E. (1993). Carcinosarcomas - Current Perspectives and an Historical Review of Nosological Concepts. Seminars in Diagnostic Pathology, 10(2), 118–127.
Bloxham, C. A., Bennett, M. K., & Robinson, M. C. (1990). Bladder carcinosarcomas: three cases with diverse histogenesis. Histopathology, 16(1), 63–67.
Kanthan, R., & Senger, J. L. (2011). Uterine carcinosarcomas (malignant mixed mullerian tumours): a review with special emphasis on the controversies in management. Obstetrics and Gynecology International, 2011, 470795. https://doi.org/10.1155/2011/470795.
Guarino, M., Giordano, F., Pallotti, F., Polizzotti, G., Tricomi, P., & Cristofori, E. (1998). Malignant mixed mullerian tumor of the uterus. Features favoring its origin from a common cell clone and an epithelial-to-mesenchymal transformation mechanism of histogenesis. Tumori, 84(3), 391–397.
Szukala, S. A., Marks, J. R., Burchette, J. L., Elbendary, A. A., & Krigman, H. R. (1999). Co-expression of p53 by epithelial and stromal elements in carcinosarcoma of the female genital tract: an immunohistochemical study of 19 cases. International Journal of Gynecological Cancer, 9(2), 131–136.
Thompson, L., Chang, B., & Barsky, S. H. (1996). Monoclonal origins of malignant mixed tumors (carcinosarcomas). Evidence for a divergent histogenesis. The American Journal of Surgical Pathology, 20(3), 277–285.
Abeln, E. C. A., Smit, V. T. H. B. M., Wessels, J. W., DeLeeuw, W. J. F., Cornelisse, C. J., & Fleuren, G. J. (1997). Molecular genetic evidence for the conversion hypothesis of the origin of malignant mixed Mullerian tumours. Journal of Pathology, 183(4), 424–431.
Xi, J., Yan, X., Zhou, J., Yue, W., & Pei, X. (2013). Mesenchymal stem cells in tissue repairing and regeneration: Progress and future. Burns Trauma, 1(1), 13–20. https://doi.org/10.4103/2321-3868.113330.
Sohni, A., & Verfaillie, C. M. (2013). Mesenchymal stem cells migration homing and tracking. Stem Cells International, 2013, 130763. https://doi.org/10.1155/2013/130763.
Perez, J. R., Ybarra, N., Chagnon, F., Serban, M., Lee, S., Seuntjens, J., et al. (2017). Tracking of Mesenchymal Stem Cells with Fluorescence Endomicroscopy Imaging in Radiotherapy-Induced Lung Injury. Scientific Reports, 7, 40748. https://doi.org/10.1038/srep40748.
Shi, Y., Hu, G., Su, J., Li, W., Chen, Q., Shou, P., et al. (2010). Mesenchymal stem cells: a new strategy for immunosuppression and tissue repair. Cell Research, 20(5), 510–518. https://doi.org/10.1038/cr.2010.44.
Zhang, J., Sun, D. Q., Fu, Q., Cao, Q. W., Zhang, H., & Zhang, K. Q. (2016). Bone mesenchymal stem cells differentiate into myofibroblasts in the tumor microenvironment. Oncology Letters, 12(1), 644–650. https://doi.org/10.3892/ol.2016.4645.
Pankajakshan, D., Kansal, V., & Agrawal, D. K. (2013). In vitro differentiation of bone marrow derived porcine mesenchymal stem cells to endothelial cells. Journal of Tissue Engineering and Regenerative Medicine, 7(11), 911–920. https://doi.org/10.1002/term.1483.
Sivamani, R. K., Schwartz, M. P., Anseth, K. S., & Isseroff, R. R. (2011). Keratinocyte proximity and contact can play a significant role in determining mesenchymal stem cell fate in human tissue. FASEB Journal, 25(1), 122–131. https://doi.org/10.1096/fj.09-148775.
Irfan-Maqsood, M., Matin, M. M., Heirani-Tabasi, A., Bahrami, M., Naderi-Meshkin, H., Mirahmadi, M., et al. (2016). Adipose derived mesenchymal stem cells express keratinocyte lineage markers in a co-culture model. Cellular and Molecular Biology (Noisy-le-Grand, France), 62(5), 44–54.
Li, Z. Z., Han, S. C., Wang, X. Q., Han, F., Zhu, X. X., Zheng, Z., et al. (2015). Rho kinase inhibitor Y-27632 promotes the differentiation of human bone marrow mesenchymal stem cells into keratinocyte-like cells in xeno-free conditioned medium. Stem Cell Research & Therapy, 6, ARTN 17. https://doi.org/10.1186/s13287-015-0008-2.
Chavez-Munoz, C., Nguyen, K. T., Xu, W., Hong, S. J., Mustoe, T. A., & Galiano, R. D. (2013). Transdifferentiation of adipose-derived stem cells into keratinocyte-like cells: engineering a stratified epidermis. PLoS One, 8(12), UNSP e80587. https://doi.org/10.1371/journal.pone.0080587.
Kokubun, K., Pankajakshan, D., Kim, M. J., & Agrawal, D. K. (2016). Differentiation of porcine mesenchymal stem cells into epithelial cells as a potential therapeutic application to facilitate epithelial regeneration. Journal of Tissue Engineering and Regenerative Medicine, 10(2), E73–E83. https://doi.org/10.1002/term.1758.
Ghanavati, Z., Orazizadeh, M., Bayati, V., Abbaspour, M. R., Khorsandi, L., Mansouri, E., et al. (2016). Characterization of A Three-Dimensional Organotypic Co-Culture Skin Model for Epidermal Differentiation of Rat Adipose-Derived Stem Cells. Cell Journal, 18(3), 289–301.
Katikireddy, K. R., Dana, R., & Jurkunas, U. V. (2014). Differentiation Potential of Limbal Fibroblasts and Bone Marrow Mesenchymal Stem Cells to Corneal Epithelial Cells. Stem Cells, 32(3), 717–729. https://doi.org/10.1002/stem.1541.
Yao, L., & Bai, H. Q. (2013). Review: Mesenchymal stem cells and corneal reconstruction. Molecular Vision, 19, 2237–2243.
Li, Y., Shi, X., Yang, L. M., Mou, Y., Li, Y. B., Dang, R. J., et al. (2017). Hypoxia promotes the skewed differentiation of umbilical cord mesenchymal stem cells toward type II alveolar epithelial cells by regulating microRNA-145. Gene, 630, 68–75. https://doi.org/10.1016/j.gene.2017.08.006.
Mendez, J. J., Ghaedi, M., Steinbacher, D., & Niklason, L. E. (2014). Epithelial cell differentiation of human mesenchymal stromal cells in decellularized lung scaffolds. Tissue Engineering. Part A, 20(11–12), 1735–1746. https://doi.org/10.1089/ten.TEA.2013.0647.
Francois, S., Bensidhoum, M., Mouiseddine, M., Mazurier, C., Allenet, B., Semont, A., et al. (2006). Local irradiation not only induces homing of human mesenchymal stem cells at exposed sites but promotes their widespread engraftment to multiple organs: A study of their quantitative distribution after irradiation damage. Stem Cells, 24(4), 1020–1029. https://doi.org/10.1634/stemcells.2005-0260.
Ferrand, J., Noel, D., Lehours, P., Prochazkova-Carlotti, M., Chambonnier, L., Menard, A., et al. (2011). Human bone marrow-derived stem cells acquire epithelial characteristics through fusion with gastrointestinal epithelial cells. PLoS One, 6(5), ARTN e19569. https://doi.org/10.1371/journal.pone.0019569.
Wei, X., Wang, C. Y., Liu, Q. P., Li, J., Li, D., Zhao, F. T., et al. (2008). In vitro hepatic differentiation of mesenchymal stem cells from human fetal bone marrow. Journal of International Medical Research, 36(4), 721–727.
Itaba, N., Matsumi, Y., Okinaka, K., Ashla, A. A., Kono, Y., Osaki, M., et al. (2015). Human mesenchymal stem cell-engineered hepatic cell sheets accelerate liver regeneration in mice. Scientific Reports, 5, 16169. https://doi.org/10.1038/srep16169.
Palakkan, A. A., Drummond, R., Anderson, R. A., Greenhough, S., Tv, K., Hay, D. C., et al. (2015). Polarisation and functional characterisation of hepatocytes derived from human embryonic and mesenchymal stem cells. Biomedical Reports, 3(5), 626–636. https://doi.org/10.3892/br.2015.480.
Hao, N. B., Li, C. Z., Lu, M. H., Tang, B., Wang, S. M., Wu, Y. Y., et al. (2015). SDF-1/CXCR4 axis promotes MSCs to repair liver injury partially through trans-differentiation and fusion with hepatocytes. Stem Cells International, 2015, 960387. https://doi.org/10.1155/2015/960387.
Bhonde, R. R., Sheshadri, P., Sharma, S., & Kumar, A. (2014). Making surrogate beta-cells from mesenchymal stromal cells: perspectives and future endeavors. The International Journal of Biochemistry & Cell Biology, 46, 90–102. https://doi.org/10.1016/j.biocel.2013.11.006.
Ouyang, J. F., Huang, W., Yu, W. W., Xiong, W., Mula, R. V. R., Zou, H. B., et al. (2014). Generation of insulin-producing cells from rat mesenchymal stem cells using an aminopyrrole derivative XW4.4. Chemico-Biological Interactions, 208, 1–7. https://doi.org/10.1016/j.cbi.2013.11.007.
Sun, Y., Chen, L., Hou, X. G., Hou, W. K., Dong, J. J., Sun, L., et al. (2007). Differentiation of bone marrow-derived mesenchymal stem cells from diabetic patients into insulin-producing cells in vitro. Chinese Medical Journal, 120(9), 771–776.
Ning, J. W., Li, C. Y., Li, H. J., & Chang, J. W. (2011). Bone marrow mesenchymal stem cells differentiate into urothelial cells and the implications for reconstructing urinary bladder mucosa. Cytotechnology, 63(5), 531–539. https://doi.org/10.1007/s10616-011-9376-3.
Tian, H., Bharadwaj, S., Liu, Y., Ma, P. X., Atala, A., & Zhang, Y. Y. (2010). Differentiation of Human Bone Marrow Mesenchymal Stem Cells into Bladder Cells: Potential for Urological Tissue Engineering. Tissue Engineering Part A, 16(5), 1769–1779. https://doi.org/10.1089/ten.tea.2009.0625.
Wang, R. A., Li, Z. S., Zhang, H. Z., Zheng, P. J., Li, Q. L., Shi, J. G., et al. (2013). Invasive cancers are not necessarily from preformed in situ tumours an alternative way of carcinogenesis from misplaced stem cells. Journal of Cellular and Molecular Medicine, 17(7), 921–926. https://doi.org/10.1111/jcmm.12078.
Blanpain, C. (2013). Tracing the cellular origin of cancer. Nature Cell Biology, 15(2), 126–134. https://doi.org/10.1038/ncb2657.
Lott, D. G., Manz, R., Koch, C., & Lorenz, R. R. (2010). Aggressive behavior of nonmelanotic skin cancers in solid organ transplant recipients. Transplantation, 90(6), 683–687. https://doi.org/10.1097/TP.0b013e3181ec7228.
Verneuil, L., Varna, M., Leboeuf, C., Plassa, L. F., Elbouchtaoui, M., Loisel-Ferreira, I., et al. (2013). Donor-derived keratinocytes in actinic keratosis and squamous cell carcinoma in patients with kidney transplant. The Journal of Investigative Dermatology, 133(4), 1108–1111. https://doi.org/10.1038/jid.2012.422.
Verneuil, L., Leboeuf, C., Bousquet, G., Brugiere, C., Elbouchtaoui, M., Plassa, L. F., et al. (2015). Donor-derived stem-cells and epithelial mesenchymal transition in squamous cell carcinoma in transplant recipients. Oncotarget, 6(39), 41497–41507. https://doi.org/10.18632/oncotarget.6359.
Korkaya, H., Kim, G. I., Davis, A., Malik, F., Henry, N. L., Ithimakin, S., et al. (2012). Activation of an IL6 inflammatory loop mediates trastuzumab resistance in HER2+ breast cancer by expanding the cancer stem cell population. Molecular Cell, 47(4), 570–584. https://doi.org/10.1016/j.molcel.2012.06.014.
Liu, M., Sakamaki, T., Casimiro, M. C., Willmarth, N. E., Quong, A. A., Ju, X., et al. (2010). The canonical NF-kappaB pathway governs mammary tumorigenesis in transgenic mice and tumor stem cell expansion. Cancer Research, 70(24), 10464–10473. https://doi.org/10.1158/0008-5472.CAN-10-0732.
Shigdar, S., Li, Y., Bhattacharya, S., O'Connor, M., Pu, C., Lin, J., et al. (2014). Inflammation and cancer stem cells. Cancer Letters, 345(2), 271–278. https://doi.org/10.1016/j.canlet.2013.07.031.
Nwabo Kamdje, A. H., Takam Kamga, P., Tagne Simo, R., Vecchio, L., Seke Etet, P. F., Muller, J. M., et al. (2017). Developmental pathways associated with cancer metastasis: Notch, Wnt, and Hedgehog. Cancer Biology & Medicine, 14(2), 109–120. https://doi.org/10.20892/j.issn.2095-3941.2016.0032.
Vermeulen, L., Melo, F. D. S. E., van der Heijden, M., Cameron, K., de Jong, J. H., Borovski, T., et al. (2010). Wnt activity defines colon cancer stem cells and is regulated by the microenvironment. Nature Cell Biology, 12(5), 468–U121. https://doi.org/10.1038/ncb2048.
Lee, J. M., Dedhar, S., Kalluri, R., & Thompson, E. W. (2006). The epithelial-mesenchymal transition: new insights in signaling, development, and disease. The Journal of Cell Biology, 172(7), 973–981. https://doi.org/10.1083/jcb.200601018.
Acknowledgements
This work was supported by Shiraz Institute for Cancer Research, Shiraz University of Medical Sciences. The Hypothesis was proposed and designed by AG. SA prepared the first draft of the Manuscript. The manuscript was critically reviewed by both AG and SA.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interests
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Ghaderi, A., Abtahi, S. Mesenchymal Stem Cells: Miraculous Healers or Dormant Killers?. Stem Cell Rev and Rep 14, 722–733 (2018). https://doi.org/10.1007/s12015-018-9824-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12015-018-9824-y