Abstract
Research on mesenchymal stromal cells (MSCs) has moved at a rapid pace that has been driven by unexpected discoveries about the biology of the cells and their beneficial effects in multiple models for human diseases. There are currently at least three paradigms as to how the MSCs can repair tissues: (I) by engrafting and serving as a niche for stem/progenitor cells; (II) by engrafting and differentiating to repair damaged tissues; and (III) by temporarily engrafting in injured tissues, engaging in extensive “cross-talk” triggered by signals from the injured tissues, and producing factors that both limit injury to the tissues by multiple effects such as modulating excessive inflammatory and immune responses and enhance repair by providing a niche that stimulates the propagation and differentiation of tissue-endogenous stem/progenitor cells. In the background of research to support each of the paradigms is a series of controversies that have not been resolved in spite of the efforts of the thousands of dedicated scientists who have made major contributions to the field. We will review here just a few of these controversies with conclusions that reflect some of our own biases.
Where there is good science, there is always trouble. (Anonymous)
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
These keywords were added by machine and not by the authors. This process is experimental and the keywords may be updated as the learning algorithm improves.
Introduction: The Three Paradigms of MSCs
The cells that are the topic of this chapter have generated a tangled history of changing hypotheses and paradigms. The cells were first identified over 50 years ago in the early experiments on bone marrow: They were spindle-shaped cells that adhered to tissue culture surfaces and were clearly not destined to be hematopoietic. From the outset, the cells were investigated on the basis of two hypotheses or paradigms, in the sense of scientific paradigms as originally defined by the philosopher Thomas Kuhn [1].
Some observers were impressed with the similarity of the cells to cells that formed the stroma of the marrow. This impression prompted the important use of the cells as feeder layers for the culture of hematopoietic cells [2, 3]. In effect, these observers developed the paradigm that the cells provided a niche for hematopoietic stem cells (Paradigm I in Fig. 2.1). Other observers discovered that the cells were readily differentiated into osteoblast-like mineralizing cells, into chondrocytes, and into adipocytes both in culture and in capsules implanted in vivo [5, 6]. They therefore pursued the paradigm that cells were similar to embryonic stem cells and might be used therapeutically to replace many injured tissues by engrafting and differentiating (Paradigm II in Fig. 2.1). Research based on both paradigms advanced in an irregular, stop-and-go manner as the experimental methods improved. The research also took an irregular course because the cells were at an intersection of the rapidly developing fields of stem cells and of tissue regeneration and repair. As the concepts in these fields evolved, there were major changes in the underlying hypotheses for research on MSCs.
Paradigm I: MSCs as Niche for Hematopoietic Stem Cells
The paradigm that the confluent cultures of MSCs could serve as effective feeder layers or niches for the culture of hematopoietic stem cells has proven to be a major breakthrough in the study of bone marrow and the field of bone marrow transplantation [2, 3]. Direct demonstration of a niche function of MSCs was provided by the observation that islands of hematopoiesis were formed within human MSC-seeded ceramic cubes that were implanted under the skin of immunodeficient mice [7]. Also, the niche function of MSCs was indirectly supported by clinical trials in which the cells were shown to hasten the recovery of the hematopoietic system after bone marrow transplants [8]. The paradigm was further supported by recent studies in mice that identified MSCs as nestin+ cells that were part of the neuroendocrine system for mobilization of hematopoietic system [9]. Some of the most direct support for a niche function came from the observation that human MSCs implanted into the hippocampus of mice stimulated the proliferation on endogenous neural stem cells and also their migration and differentiation [10]. The niche function of MSCs may well explain many of the therapeutic benefits that have been reported in multiple animal models for human diseases and a few of the patients in whom therapeutic benefits have been observed in the over 140 of clinical trials with MSCs and related cells that have been registered (clinicaltrials.gov).
Paradigm II: MSCs Repair by Engrafting and Differentiating
The paradigm that MSCs might repair multiple tissues by engrafting and differentiating resonated widely among physicians and scientists interested in new therapies for human diseases [11, 12]. The paradigm reawakened an idea attributed to the classical pathologist Cohnheim who as early as 1867 [13] made observations suggesting that some of the cells involved in tissue repair came from the general circulation and, in the light of further information, from the bone marrow. The paradigm was supported by observations that systemically infused MSCs appeared to be recovered in multiple tissues [14] and that the cells, under some circumstances, differentiated to cells originating from all three germ layers [15–19]. Many of the early experiments were handicapped by inadequate techniques for isolating and characterizing the cells and the lack of markers for the cells that were not readily lost during differentiation or transferred to other cells. Also, all the potential assay artifacts had not yet been recognized such as artifacts from overlapping cells in microscopic sections labeled with antibodies. As these problems were resolved, reports from multiple laboratories established that MSCs could engraft and differentiate in multiple tissues but the process was robust only in limited circumstances such as in rapidly developing tissues of embryonic mice [16] or chick embryos [20], and with local injection into damaged tissue such as fractured bones [21] or injured cartilage [22, 23]. At the same time, there were convincing reports that MSCs or some related cells from bone marrow engrafted in severely injured tissues in patients such as those undergoing organ rejection following transplants of lung [24]. Also, MSCs or some related cells from bone marrow can generate some of the cells found in epithelial cancers [25]. Therefore, the paradigm appears to have limited applicability, but it is not fully excluded as a therapeutic strategy.
Paradigm III: Repair by Transient Cross-Talk and Niche Functions
As MSCs were explored in many laboratories around the world, several unexpected observations emerged: (a) They frequently repaired tissues even though they were detected in the tissues only transiently, and (b) the cells engaged in extensive communication or “cross-talk” with other cells and tissues [26] that dramatically altered the genes they expressed, including those for secreted factors [27, 28]. The observations have provided the new paradigm that is a partial synthesis of the first two paradigms: The cells temporarily engraft in injured tissues, they engage in extensive “cross-talk” triggered by signals from the injured tissues, and, as a result, they are activated to express genes that (a) limit injury to the tissues by modulating excessive inflammatory and immune responses and (b) enhance repair by providing a niche that stimulates the propagation and differentiation of tissue-endogenous stem/progenitor cells.
The three paradigms are summarized in Fig. 2.1.
Schematic summarizing three evolving paradigms for the repair of tissues by MSCs. The morphology of a small number of adherent cells from bone marrow suggested the paradigm that the cells served as a niche for hematopoietic cells (Paradigm I). The ready differentiation of the cells in culture suggested that the cells could repair tissues by engrafting and differentiating (Paradigm II). Clinical trials using the cells to improve bone marrow transplants unexpectedly demonstrated that they improved graft-versus-host diseases in a few patients and thereby drew attention to their immunomodulatory properties. Functional improvement without significant engraftment in animal models and a few patients suggested that MSCs enhanced repair by transiently forming microenvironments or “quasi-niches” (Paradigm III) (Reproduced with permission from Prockop et al. [4])
In the background of research to support each of these paradigms is a series of controversies that have not been resolved in spite of the efforts of the thousands of dedicated scientists who have made major contributions to the field. We will review some of these controversies and provide conclusions that reflect some of our own biases.
Controversy I: What Are the Criteria for Identifying MSCs?
The commonly employed criteria for defining MSCs are that the cells are (a) highly clonogenic; (b) readily differentiate in culture to osteoblasts, adipocytes, and chondrocytes; and (c) lack epitopes for hematopoietic cells and express several epitopes that are shared with other non-hematopoietic cells such as CD73, CD90, and CD105 [29]. Unfortunately, each of the criteria is difficult to apply quantitatively. In addition, many reports have not employed them with rigor.
The criterion of clonogenicity lacks rigor as commonly applied. As originally emphasized by Friedenstein [6, 30], the clonogenicity of MSCs is striking. In the case of human MSCs, if the nucleated cells from bone marrow are first plated at high density, incubated for 7–9 days, and the adherent cells then replated at low density, 10% or more of the cells will give rise to single-cell-derived colonies (defined as colony-forming units or CFUs) in about 2 weeks. With some preparations, from 80 to 90% of the cells are CFUs [31, 32]. However, the CFUs decrease dramatically if the same preparations are plated at a high density or are allowed to expand to confluence [32]. Moreover, there are large differences in the clonogenicity seen with cultures prepared from bone marrow aspirates from different normal donors and even between aspirates drawn from the right and left iliac crests of the same normal donor in the same session [33]. The criterion is further confused by observations with MSCs from rodent bone marrow. Cultures of mouse MSCs are particularly confounding. Nucleated cells from mouse bone marrow that adhere to tissue culture plastic are heavily contaminated by hematopoietic cells. The hematopoietic cells can be removed by immunoselection [34] or by repeated passage as adherent cells [35]. However, mouse MSCs are similar to mouse fibroblasts [36] in that they initially grow slowly until a few cells emerge from a “crisis” in the cultures, become transformed, and then are potentially tumorigenic [37]. Moreover, there are differences among MSCs from different strains of mice and some difference in the media required for optimal yields [35]. With rat bone marrow, plating of nucleated cells from bone marrow of some but not all strains gives rise to MSCs that are relatively free of hematopoietic cells [38]. The MSCs from young rats of strains that provide good yields of MSCs grow rapidly when first plated and are highly clonogenic. However, CFU assays on rat MSCs need to be a carried out carefully by plating single cells in separate wells in microtiter plates because of the tendency of the cells from one colony to detach and generate new colonies [38].
The criterion of differentiation has also been applied loosely. In the case of MSCs from human bone marrow, preparations isolated with the same protocol vary in the extent of differentiation into osteoblast-like mineralizing cells, adipocytes, and chondrocytes [33, 39]. In fact, one surprising observation is that if cells from single-cell-derived colonies are replated at clonal densities, they give rise to new single-cell-derived colonies that vary in their potential to differentiate into mineralizing cells and adipocytes (Fig. 2.2). The colonies also vary in size and morphology (Fig. 2.3).
Variation within and between human donors in osteoblast and adipocyte differentiation capacity of MSC colonies from CFU assays at passage 2. R and L indicate samples from right and left iliac crests of same donor taken at the same time. One to eight large colonies from the same plate were assayed (Reproduced with permission and modified from Digirolamo et al. [39])
Changes in clonogenicity, colony size, and morphology within and among donors upon subcloning. Passage 1 MSCs were plated at 2 cells/cm2 and grown for 10–12 days. Cells (passage 2) were then isolated from either the inner dense region (IN) or outer region (OUT) of the colonies and replated and cultured as above. This passaging continued until the cells no longer generated colonies with distinct IN and OUT regions. Representative colonies of donor 240 (P3) stained with crystal violet, measured, and classified as either type I or type II. (a) Type I colonies were at least 4 mm in size with a dense IN (upper panel). Type II colonies were either less than 4 mm with a dense IN or larger in size but loose (lower panel). Distribution of type I and type II colonies derived from cells isolated from the IN and OUT regions during subcloning for donor (b) 5,064; (c) 240; and (d) 7,012. The fraction of type II colonies increased with passage number for all 3 donors. However, the passage number at which type II colonies predominated varied among the donors. Error bars: standard deviations; n = 3. Scale bar: 1 mm. Abbreviations: CFU-F colony-forming units fibroblast, IN inner region of colony, OUT outer region of colony, P passage (Reproduced with permission and modified from Ylostalo et al. [40])
Usually, differentiation is assayed by incubating cultures in a medium conducive to mineralization and stained with Alizarin red S or incubating in medium conducive to adipogenesis and stained with Oil red O. The extent of differentiation is then evaluated qualitatively by microscopy, and the evaluation of the same samples by different observers can vary. Far more reliable data for mineralization and adipogenesis can be obtained with extraction of the dyes for quantitative colorimetric assays [41]. Unfortunately, quantitative assays have rarely been employed. Alternatively, quantitative RT-PCR assays for gene expression are very helpful. Chondrogenic differentiation requires culturing the cells as a micropellet and incubating for 2–3 weeks in a serum-free chondrogenic medium. The pellets are then fixed, sectioned, and stained with either toluidine blue to detect the proteoglycans or Safranin O to detect glycosaminoglycans. Again, the evaluation is qualitative and varies with different preparations and with expansion of the same preparations. Also, the recombinant cytokines used with the serum-free medium (TGF-β3 and BMP-2) are expensive, and the assay is not frequently repeated. The quantitative RT-PCR assays for cartilage-specific mRNAs are very helpful.
The criterion of epitopes is also problematic. There is consensus that human MSCs from bone marrow should be negative for epitopes found on hematopoietic cells. The expression of epitopes found on non-hematopoietic cells is more useful, but again, some of these can be variable among different preparations, different laboratories, different species, and different passage numbers of the same preparations [42].
How will this controversy be resolved? One approach is for reviewers to encourage authors to apply the existing criteria more rigorously. Another is to make available reference banks of MSCs that investigators can use as standards for comparison. In support of this suggestion, we obtained an NIH grant to prepare and distribute standardized preparations of MSCs to other investigators (http://medicine.tamhsc.edu/irm/msc-distribution.html). We have provided the cells to over 350 laboratories. A more permanent solution will probably be to develop rapid and more reproducible in vivo assays for either the differentiation of MSCs or therapeutic benefits in one or more disease models.
Controversy II: Can MSCs Differentiate into Non-mesenchymal Cells
Early observations with MSCs generated this controversy because they suggested that MSCs were capable of differentiation into neural cells and fibroblasts (see Fig. 2.4 and Pereira et al. [43], Azizi et al. [44], Kopen et al. [16]).
Immunohistochemical localization of BrdUrd-labeled mouse MSCs in transplanted into mouse forebrain. Hematoxylin/eosin (a)- or anti-BrdUrd (b)-stained serial sections of striatum and lateral ventricle, ipsilateral to the injection site at bregma. (c) High-power magnification of BrdUrd-labeled cells in the external capsule. Photomicrograph is from same section as (b) but shows a more lateral field. (d) MSC-derived astrocyte in the molecular layer of the hippocampus double labeled with anti-BrdUrd and anti-GFAP (black). Arrows, BrdUrd-labeled nuclei; arrow-heads, nuclei negative for BrdUrd labeling (a and b – ×40; c – ×400; d – ×1,000) St: Striatum; CC: corpus callosum; EC: external capsule (Reproduced with permission from Kopen et al. [16])
The observations generated controversy in part because the accepted dogma at the time was that cells could not differentiate across germ lines. Also, the accepted dogma at the time was that stem cells differentiated in a defined sequence of progenitor cells referred to as hierarchical differentiation [45]. The controversy became heated at several different levels, particularly at the political level when it was suggested that research on human embryonic stem cells was unnecessary because of the differentiation potential of “adult stem cells” such as MSCs. The controversy also became heated because the early experiments on differentiation of MSCs were limited by available techniques and the generation of artifacts that had not been previously recognized: Cell labeling reagents such as dyes, and even genetic markers, were unexpectedly transferred across membranes from one cell to another; many antibodies were used without fully defined specificities; overlapping cells in immunocytochemistry of tissues at a time when 3D resolution of microscopic imaging was not available; and artifacts introduced by rare cell fusion events. The controversy has become less heated as the assays, and, therefore, the data generated have improved. For example, in our own laboratory, we were able to use time-lapse microscopy and a series of RNA and protein assays to demonstrate that MSCs cocultured with heat-shocked primary epithelial cells differentiated into epithelial cells both with and without cell fusion, at least under those experimental conditions (Fig. 2.5) [18].
Phase-contrast and fluorescence microscopy of small airway epithelial cells (SAECs), bronchial epithelial cells (BEC), and lentiviral GFP+ hMSCs in culture and coculture. Epithelial cells were heat shocked (47 °C, 30 min), and 1–2 h later, GFP+ hMSCs were added to the cultures. (a) Monolayer of SAECs in SAEC serum-free medium. (b) GFP+ hMSCs in 20% FBS MSC medium (FITC overlay on phase). (c, d) GFP+ hMSCs cultured in serum-free SAEC medium. (e, f) Coculture with heat-shocked BEC at 2 week. The differentiated GFP+ cell has an epithelial morphology and has repaired the monolayer formed by the epithelium. The cell is binucleated (yellow arrow), as is a GFP-negative BEC above it (arrowhead). (g–l) Time-lapse images of cocultures of GFP+ hMSCs and heat-shocked SAECs after incubation for 12–120 h. (g, h) GFP+ cell between SAECs undergoing morphological changes (arrow). (i, j) Differentiated GFP+ cell has an epithelial morphology, has repaired the monolayer formed by the SAECs, and has a single nucleus (arrow). Adjacent SAEC is binucleated (arrowhead). (k, l) Differentiated GFP+ cell has three nuclei (yellow arrow). (e, f, k, and l) The outermost cytoplasmic edges of the GFP+ cells are artificially enhanced (Magnification: (a–d) ×10; (e, f) ×40; (g–j) ×20; (k, l) ×40) (Reproduced with permission and modified from Spees [18])
Also, the controversy has become less heated with parallel developments that challenged several dogmas in the field. One of these developments was the discovery of induced pluripotent stem cells that demonstrated the ease with which the genome of cells can be reprogrammed by the introduction of four genes expressed in embryonic cells [46]. The generation of the induced pluripotent cells emphasized the plasticity of the genome, a conclusion demonstrated earlier by experiments in which nuclei of somatic cells were transferred to enucleated embryonic cells [47]. Another development was the recognition that the concept of “hierarchical differentiation” of hematopoietic stem cells had overlooked the important contribution of “niches” in directing differentiation of stem cells [45]. The critical importance of niches in the hematopoietic system was a rediscovery of the role of niches in simpler systems such as ovogenesis in drosophila [48]. Still another development was the extensive observations on epithelial-mesenchymal transition in cancer and other conditions. Among the most remarkable recent publications is the report by Olsen and colleagues [49] that two lines of cultured human endothelial cells can be efficiently transformed in culture to cells with characteristics similar to MSCs by the simple addition of BMP4 or TGFβ2 to the medium.
It is probably too early to conclude that there is a consensus on the differentiation potential of MSCs. However, there are currently 543 entries in PubMed under “mesenchymal stem cells neural differentiation.” A quick scan of the entries indicates that a few challenge the possibility of neural differentiation but several offer extensive data on the functional characteristic of the differentiated cells (see Zeng et al. [50], Delcroix et al. [51], Zhang et al. [52]). These publications continue to appear at a time when both the investigators and reviewers have had an adequate opportunity to recognize the artifacts and criticisms encountered previously. Therefore, they deserve serious attention.
Where does this leave the field? Certainly, there is a consensus that the experimental conditions for differentiation of MSCs are not highly reproducible. Also, the molecular events that drive differentiation such as Wnt and Notch signaling have been touched on by some recent reports [53, 54] but not explored in detail. At the end of the day, it seems clear that carefully prepared MSCs have a potential to differentiate that lies somewhere between mature somatic cells such as skin fibroblasts and ESCs and induced pluripotent cells. The differences from ESCs and iPS cells are probably quantitative ones that hinge on the rigor of the experimental conditions that are required to reprogram the genome.
Controversy III: Are MSCs Pericytes?
Several groups have claimed that a rare population of perivascular CD45−/CD146+ pericytes are the progenitors of MSCs capable of generating the hematopoietic microenvironment [7, 55, 56]. The results demonstrated striking similarities between pericytes and bone marrow-derived MSCs. There are, however, some differences that have not been explained to date. One difference is that most pericytes expand slowly in culture. Another is that most pericytes are contractile cells. Still another is that pericytes from different vessels show considerable heterogeneity. In addition, more recently, Mendez-Ferrer and colleagues identified a rare subset of perivascular nestin-positive cells that had essentially all the properties of MSCs, that spatially associated with the hematopoietic stem cells (HSCs), and that were an essential component of the HSC niche [9]. Although not directly compared, the nestin-positive MSCs did not appear to be pericytes.
How do we resolve these apparently contradictory observations? Clearly, the observations themselves were carefully made and cannot be challenged. The resolution is perhaps to accept that pericytes and MSCs could be members of a large family of cells with many properties in common. Most importantly, they have a remarkable plasticity that approaches transmogrification: changing from one phenotype to another when presented with different niches or microenvironments in vivo and in vitro. We have learned to accept the multiple phenotypes of T lymphocytes and the M1/M2 phenotypes of macrophages. The concept seems more difficult to accept for MSCs.
Controversy IV: Can MSCs Rescue Injured Cells by Transfer of Mitochondria?
Several years ago, we made the unexpected observation that MSCs can rescue cells with nonfunctional mitochondria by the transfer of mitochondria [57]. The observation had broad implications for the therapeutic potentials of MSCs because failure of mitochondria is a common event in many diseases, particularly with ischemia and reperfusion of tissues. The mitochondria are damaged by the ischemia and then fail to provide adequate electrons to reduce oxygen when the tissue is reperfused. The result is an increase in reactive oxygen species (ROS) that rapidly damage cells. Paradoxically, low levels of ROS trigger inflammation and high levels cause apoptosis. The transfer of mitochondria we observed therefore could provide a rationale for the use of MSCs as therapy for stroke, myocardial infarction, and other diseases. All the observations we made, however, were in tissue culture, and we were unable to devise an adequate experiment to prove transfer in vivo. This problem has recently been addressed with an ingenious series of observations on relatively benign genital tumors of dogs that were transmitted as allografts over many generations during coition [58]. Sequencing of two informative regions in mitochondria in 37 samples of the tumors in dogs from four continents indicated extensive capture of host mitochondrial DNA in most of the samples. The results do not conclusively establish that functional mitochondria were transferred, but they do establish the transfer of mitochondrial DNA.
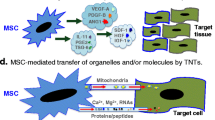
A recent study by Islam et al. [59] is the first demonstration of in vivo mitochondrial transfer from MSCs to LPS-injured mouse lung alveolar epithelial cells leading to promotion of tissue repair and increased survival of the mice. Intravital fluorescence microscopy of ex vivo perfused LPS-damaged lungs was employed to directly observe the interaction of MSCs expressing a fluorescent tag with the lung epithelial cells. The MSCs were administered intratracheally into the lungs and imaged up to 24 h. The MSCs attached to the alveolar cells, and the MSC mitochondria were observed to be transferred in microvesicles and nanotubes to the damaged cells and accompanied by an increase in ATP in the alveolar cells. What are the consequences of transfer of mitochondria by MSCs? One is that some of the beneficial effects of MSCs observed in animal models of human diseases may be explainable by transfer of mitochondria. Another possibility is that if the mitochondria or mitochondrial DNA are transferred in vesicles, the vesicles may also contain microRNAs or even mRNAs that could explain the differentiation of MSCs observed in some cocultures with other cells [18].
Controversy V: Do Intravenously Infused MSCs Escape Entrapment in the Lung?
Early observations with MSCs demonstrated marked improvements in injuries to organ such as the heart, brain, and kidney after intravenous administration of the cells. MSCs were detected in the tissues with assays for markers such as cell-labeling dyes, and marker genes such as GFP. However, subsequent observations demonstrated that many of the experiments were subject to previously unsuspected artifacts. Also, some of the experiments, particularly those with mouse MSCs, were probably confounded by the presence of hematopoietic cells and the tendency of the cells to spontaneously transform. In addition, most of the data were based on manual counting of labeled cells in sections without resort to the quantitative deconvolution and 3D microscopic algorithms now available. To address these problems, we elected to resort to an unconventional approach: infusion of well-characterized human MSCs into either wild-type or immunodeficient mice [10, 27, 28]. The strategy made it possible to use endogenous markers in the MSCs that could be assayed quantitatively for human DNA by real-time PCR assays and for genes expressed by the human cells by RT-PCR assays. The assays themselves required careful attention because of two variables: the efficiency of extraction of DNA and RNA from different tissues and the efficiency of polymerization of nucleic acid by PCR because of variations in the contaminants in extracts of DNAs and RNAs from different tissues. To overcome these problems, Lee et al. [28] developed separate standard curves for each tissue by adding varying numbers of human MSCs to naïve tissues before extraction of the nucleic acids. They also normalized the value of each assay to the total DNA or RNA in the sample by quantitative PCRs with species-specific primers for both mouse and human GAPDH. The results confirmed previous reports based on qualitative imaging techniques that most intravenously infused MSCs are immediately trapped in the lung, probably during the first pass [28, 60, 61]. The results obtained with the assays indicated that after IV infusion of human MSCs, 99% (±1.07 SD) of the cells were cleared from the circulation within 5 min and that most of the cells were trapped in the lung. The cells disappeared from the lungs with a half-life of about 24 h but did not appear in any significant numbers in other tissues that were assayed: A total of 0.04% of the infused Alu sequences (equivalent to about 4,000 cells) were recovered in six tissues after 48 h and 0.01% after 96 h.
The conclusions from these experiments and the prior observations [28, 60, 61] have not been universally accepted in subsequent publications. One criticism was that the human MSCs employed are larger and perhaps more adherent than mouse MSCs and therefore more likely to be trapped in the lungs. However, one of the earlier experiments that provided qualitative data on extensive trapping in lungs used rat MSCs [60], and one used mouse MSCs [61]. Another criticism was that the immune system of the immunodeficient mice (NOD/scid) used in the experiments [28] may have destroyed the human MSCs in the lung before they had a chance to recirculate to other tissues. As discussed below, the use of human MSCs raises concerns but offers distinct advantages, and the concerns can probably be addressed by validating the observations with additional carefully controlled experiments.
At the same time, it seems apparent that the data obtained with quantitative PCR and RT-PCR established that about 90% of human MSCs infused intravenously into mice are trapped in the lungs and very few reach more distal organs, even after selective injury to the organs. Mice appear to have unusually small capillaries, and human MSCs are larger than those from mice. Therefore, larger numbers may escape entrapment in the lung if autologous MSCs are infused in other animals. Also, the number of human MSCs trapped in the lung decreased by 25% when human MSCs were cultured as hanging drops to form spheroids and then are dissociated before being infused intravenously into mice apparently because the MSCs become compacted in spheroids and are about one-quarter the volume of MSCs cultured as monolayers [62]. However, we will not know the extent to which intravenously infused MSCs escape entrapment in the lungs in species other than mice until more quantitative experiments are performed.
At the same time, the impression that most MSCs administered IV are trapped in the lung has prompted great interest in soluble factors released by MSCs that might explain their beneficial effects. For example, in different models of inflammation, the beneficial effects of MSCs were traced to the cells being activated to express the anti-inflammatory protein TSG-6 (Fig. 2.6) [28], prostaglandin E2 [63], the interleukin 1 receptor antagonist [64], or soluble TNF receptor 1 [65]. Still, other factors produced by MSCs including nitric oxide, indoleamine 2,3-dioxygenase, and CCL2 were reported to explain the immunomodulatory effects of MSCs (below).
Effects of human MSCs and recombinant TSG-6 in NOD/scid mice with myocardial infarcts (MI). (a) Schematic illustrating the progressive damage to the myocardium following MI. The ischemia triggers invasion by inflammatory cells. The inflammatory cells and the matrix metalloproteinases they release accentuate damage to the myocardium. TSG-6 synthesized by MSCs or recombinant TSG-6 limits the injury and thereby enhances repair (Reproduced with permission and modified from Prockop et al. [4]). (b) Protective/reparative properties of MSCs and TSG-6 in MI. Three weeks after permanent ligation of the anterior descending coronary artery in mice, each heart was cut from the apex through the base into sequential 5-um sections and stained with Masson trichrome. Every 20th section is shown. Cells (2 × 106) were delivered intravenously (IV) 1 h after MI. Symbols: MI only; MI + hMSCs, hMSCs; MI + scr siRNA, hMSCs transduced with scrambled siRNA; MI + TSG-6 siRNA, hMSCs transduced with TSG-6 siRNA; MI + rhTSG-6, 30 ug recombinant TSG-6 protein infused IV 1 h and again 24 h after MI (Reproduced with permission and modified from Lee et al. [28])
Controversy VI: Is It Valid to Experiment with Human MSCs in Rodent Models?
The use of xenogeneic cells in animals has long been an anathema in biology. However, the difficulties inherent in isolating and expanding mouse MSCs tempted us and others to test human cells in rodents. We were encouraged by the evidence that MSCs are at least partially immune privileged and the apparently successful use of unmatched MSCs from universal donors in patients [66]. Further, we were encouraged by our observations that human MSCs disappeared with about the same half-life whether injected into the hippocampi of wild-type or immunodeficient mice [27]. A number of reports have now established therapeutic benefits from systemic administration of human MSCs in immunodeficient mice with streptozotocin-induced diabetes and with myocardial infarction. Therapeutic benefits were also observed with administration of human MSCs to wild-type rodents that were models for transient global ischemia [27], retinal degeneration [67], peritonitis [68], and meniscal injury (Masafumi Horie, Hosoon Choi, Ryang-Hwa Lee, R.L.R., Joni Ylostalo, Takeshi Muneta, Ichiro Sekiya, and D.J.P., Osteoarthritis and Cartilage, in press). We also note that a number of other investigators have recently used human MSCs from bone marrow in rodent models [69–72]. The use of human MSCs in animal models offers the tremendous advantage of using species-specific markers to follow the cells, including the ability to examine the cross-talk between the human MSCs and endogenous cells and the dramatic changes which result in both cell populations.
Nonetheless, many investigators are still concerned about crossing species barriers in such experiments. The best resolution of this controversy is to define clearly the goals of such experiments. The human MSCs are used in rodents or other species to first establish a therapeutic benefit and then define the mechanisms by which the human cells exert their effects. The strategy provides a powerful tool for following the cross-talk between the MSCs and injured tissues. Autologous or syngeneic MSCs might be more effective in many of the experiments, but the tools for analyzing their effects are much more limited. The happiest resolution of the controversy is probably the one that occurred in observing the effects of human MSCs in a mouse model for myocardial infarction: The beneficial effects were traced to TSG-6, and then the recombinant protein was shown to reproduce most of the beneficial effects of the human MSCs (Fig. 2.5) [28]. Also, most of the beneficial effects of administration of MSCs were lost when the TSG-6 gene was knocked down with an siRNA.
Controversy VII: Can “Universal Donors” of MSCs Be Used in Patients?
The initial efforts to develop clinical therapies generated a dilemma: Would autologous MSCs be required? The question had immediate financial consequences. The autologous MSCs were about twice as expensive (well over $10,000/preparation by our estimates). Quality control was difficult because if freshly prepared MSCs were used, the tests for efficacy of the cells and microbial agents possibly acquired during preparation of the cells could not be completed before the cells were administered. If the samples were frozen before use, the extensive tests required for each autologous preparation were expensive. Also, fresh autologous MSCs were impractical for therapy of acute diseases such as myocardial infarction and stroke. So the most common “business model” for the several biotech companies was to prepare large lots of extensively expanded MSCs from a single donor. We and others persisted with the development of protocols to use autologous MSCs in patients. We pursued this course because we were concerned about (a) administering cells that might elicit immune reactions, and (b) the extensive expansion or highly confluent cultures necessary to produce a large bank of MSCs would eliminate the early progenitor cells that were enriched in early passage low-density cultures. We developed a protocol to prepare autologous MSCs for therapy of patients with spinal cord injuries on the basis of data from experiments in rats indicating that there was a window for therapy of about 1 week following an acute injury to the spine [73, 74]. Sekiya and colleagues in Tokyo [75] developed a similar protocol preparing autologous MSCs generated from a biopsy of synovial tissue to treat acute injuries to knee cartilage. They launched a phase I/II clinical trial now nearing completion.
In the interim, newly launched biotech companies and academic centers have carried out extensive clinical trials with large banks of MSCs from universal donors. In some of the trials, patients have received repeated infusions of large numbers of MSCs from large banks. To date, no major adverse reactions have been reported. Therefore, the use of universal donors for clinical applications is now supported by a considerable body of data, and our commitment to autologous MSCs is a minority position. However, we are convinced that autologous MSCs may be superior for some applications such as the repair of knee cartilage by local application of the cells as is being done by Koga et al. [75].
Controversy VIII: How Do MSCs Modulate Immune Responses?
Important immunomodulatory effects of MSCs were first discovered in clinical trials to improve bone marrow transplants with MSCs: In a proportion of patients, the MSCs improved the manifestations of graft-versus-host disease (GVHD) [66]. The observations were supported by reports that MSCs inhibited the mixed lymphocyte reaction. These observations in turn prompted experiments that demonstrated IV infusions of MSCs reduced neurological deficits in the experimental autoimmune encephalitis (EAE) model for multiple sclerosis [76]. Extensive efforts have been made to explain the immunomodulatory effects of MSCs, but the field remains controversial, and several different scenarios have been advanced by leaders in the field (Fig. 2.7) (For more complete reviews, see Uccelli et al. [79], Bernardo et al. [80]).
Four putative scenarios by which MSCs modulate immune reactions. (a) Stimulation of MSCs by interferon (IFNγ) and other proinflammatory cytokines causes MSCs to produce either nitrous oxide (NO) or indoleamine 2,3-dioxygenase (IDO) and thus suppress T cells. (b) MSCs inhibit activation of CD4+ T cells by secretion of CCL2 that is cleaved into an antagonistic fragment by matrix metalloproteinase-9 (MMP-9), also secreted by MSCs [77]. (c) MSCs enhance T regulatory (Treg) cells. Direct contact with CD4+ T cells induces MSCs to secrete transforming growth factor (TGF)-β1 and prostaglandin E2 which in turn induce expression of the Treg markers FoxP3 and CD25 by the CD4+ T cells [78]. (d) MSCs act on natural killer (NK) cells, dendritic cells (D), T cells, T helper cells, and B cells to modulate immune responses [79]
Shi and associates [81] observed that murine MSCs were activated by IFNγ together with any one of three other proinflammatory cytokines (TNFα, IL-1α, or IL-1β) to become immunomodulatory. The activated MSCs expressed several cytokines and inducible nitric oxide synthase (iNOS). The chemokines attracted T cells to the MSCs, and the NO suppressed the T cells. The same authors [81] subsequently found that human and monkey MSCs did not synthesize NO, but the MSCs suppressed T cells by secreting indoleamine 2,3-dioxygenase (IDO) that depleted tryptophan in the medium or generated toxic concentrations of kynurenine and other suppressive metabolites [81].
Galipeau and associates [77] found that the MSCs inhibited activation of the T cells by secreting both CCL2 (monocyte chemotactic protein-1 or MCP-1) and MMP-9 in the murine EAE model for multiple sclerosis. MMP-9 then cleaved the CCL2 into an immune-suppressive derivative. In support of their proposal, they found that conditioned medium from MSCs inhibited activation of CD4+ T cells from mice in which EAE was induced but not T cells from CCL2−/− EAE mice. François et al. also observed that MSCs can produce opposite effects: They can stimulate immune and inflammatory responses. They observed that MSCs cross-presented exogenous antigen and induced an effective CD8+ T cell immune response [77].
Mahon and associates [78] observed that MSCs enhanced the generation of T regulatory cells. They reported that allogeneic MSC induced expression in CD4+ T cells of two markers of T regulatory cells: Forkhead box P3 (FoxP3) and CD25. They proposed a sequential process in which a first step required direct contact between MSCs and CD4+ T cells followed by secretion of TGF-β1 and prostaglandin E2 by the MSCs to drive differentiation of T cells to T regulatory cells.
Uccelli et al. [79] suggested more pleiotropic effects of MSCs. They suggested that MSCs (a) decreased proliferation, cytotoxicity, and cytokine production by NK cells; (b) impaired maturation and antigen presentation by dendritic cells; (c) decreased proliferation of T cells and impaired T helper cells; and (d) decreased proliferation and antibody production by B cells.
Which of these proposals best accounts for the immunomodulatory effects of MSCs? There is no consensus at the moment and a number of questions remain unanswered. How many of the observations are confounded by the differences between the murine and human immune systems? How many of the differences result from the difficulty of obtaining well-characterized and genetically stable mouse MSCs? How many of these carefully executed and interpreted experiments reflect immune mechanisms that are dramatic in culture but may of secondary importance in vivo? Or are MSCs in fact pleiotropic and does their response depend on the microenvironment of in vivo injury which cannot at this time be completely mimicked in culture? We all await definitive answers to these and many related questions.
Controversy IX: Do Human MSCs Cause Tumors?
The efforts to use human MSCs in clinical trials hit a major roadblock with the appearance of three reports that human MSCs escaped from senescence and generated malignant cells as the MSCs were expanded in culture [82–84]. The reports were surprising since MSCs were regularly observed to become senescent after 35 or so population doublings in culture, and emergence from senescence was not observed in numerous laboratories that had studied the cells for over a decade (see Bernardo et al. [85], Pittenger et al. [86], Digirolamo et al. [39]). In fact, data from two laboratories indicated that human MSCs emerged from senescence at a frequency of much less than 10−9 [87, 88]. The discrepancies were resolved by subsequent reports by two of three laboratories [89, 90] that the transformation of human MSCs they initially observed was explained by contamination of their cultures by a small number of malignant cells. Therefore, scientists working with MSCs had rediscovered the danger of cross-contamination of cell cultures by malignant cells, a danger recognized many decades ago but one that still plagues cancer research [91].
It is clear that the danger of generating tumors in patients with any cell therapy must be weighed carefully. DNA replication is not a perfect process, and every cell division poses some risk of activating an oncogene or inactivating a suppressor gene. What years of experience have taught us is that cells vary widely in the stability of their genomes as they are expanded. Mouse fibroblasts and mouse MSCs are at one end of the spectrum in that they regularly pass through crisis and escape senescence in culture after a few passages [36]. As emphasized by a recent report [92], immortal cells such as embryonic stem cells and induced pluripotent cells consistently demonstrate genomic instability and develop numerous mutations as they are expanded. Also they are consistently tumorigenic when administered to mice. Human MSCs occupy the other end of the spectrum in terms of the probability of becoming tumorigenic with expansion. They have been consistently observed to pass into senescence as they are expanded in culture. The test of senescence in cultures remains the best indication that a culture does not contain any cells that have undergone genomic changes that make them immortal in culture and therefore prone to be tumorigenic and carcinogenic in vivo. In contrast, the test of tumorigenicity in mice, labeled the “most ridiculous assay on the planet,” [93] is of limited value because many human cancers will not form tumors in mice. Also, the steadily improving technologies of genomic sequencing and analysis are likely to remain of limited value. There is no strategy that even in theory can detect the presence of few carcinogenic cells in large preparations unless every cell in the preparation is sampled. However, the danger of tumor formation in cell therapies with MSCs must be considered simply as a low probability, not an absolute guarantee, and the low probability must be weighed carefully in the risk/benefit evaluation for treating any patient.
Conclusions
Controversy I: What are the criteria for identifying MSCs? The existing criteria of clonogenicity and differentiation potential in culture should be applied more rigorously than they have in many publications in the past. Comparisons with standardized preparations prepared by other laboratories are probably useful. It seems unlikely that a single epitope marker for MSCs will be found given the extensive efforts that have already been made to define such a marker and the remarkable ability of the cells to change in culture and in different microenvironments in vivo. However, we are all awaiting an assay that will accurately define the therapeutic potentials of the cells in vivo and that will reflect the remarkable ability of the cells to respond to different microenvironments.
Controversy II: Can MSCs differentiate into non-mesenchymal cells? This controversy has largely been put to bed with the recent observations that reemphasize previous observations that demonstrated the plasticity of the mammalian genome. The differences from ESCs and iPS cells are probably quantitative ones that hinge on the rigor of the experimental conditions that are required to reprogram the genome.
Controversy III: Are MSCs pericytes? MSCs may not cleanly fit the classical criteria of pericytes that are defined primarily as contractile cells whose properties differ in different vascular settings. However, MSCs have striking similarities to cells closely associated with blood vessels and therefore probably belong in the same family of cells.
Controversy IV: Can MSCs rescue injured cells by transfer of mitochondria? Recent observations on transfer of mitochondria from MSCs to damaged alveolar epithelial cells strongly support the earlier suggestion that MSCs can transfer mitochondria to rescue ischemic cells. Also, recent observations indicate they can transfer microRNAs that change the properties of target cells.
Controversy V: Do intravenously infused MSCs escape entrapment in the lung? Our own assays by quantitative PCR and RT-PCR established that about 90% of human MSCs infused intravenously into mice are trapped in the lung and very few reach more distal organs, even after selective injury to the organs. Entrapment of autologous MSCs is probably somewhat less in other animals with larger capillaries, but we will not know the extent to which intravenously infused MSCs escape entrapment in the lung until more quantitative experiments are performed in species other than mice.
Controversy VI: Is it valid to experiment with human MSCs in rodent models? Administration of human MSCs to mouse models for a number of diseases has produced therapeutic benefits that are similar to those obtained by administration of isogeneic MSCs apparently because the cells are at least partially immune privileged. However, both isogeneic and xenogeneic MSCs are degraded, and only a few recovered from most tissues after a week or so. The use of human MSCs provides a wealth of specific assays to follow cross-talk between the MSCs and the host cells, but it is obviously important to extensively verify the observations.
Controversy VII: Can “universal donors” of MSCs be used in patients? No adverse reactions attributable to MSCs have been reported in clinical trials in which cells with large preparations from universal donors were infused into large numbers of patients. Some of the patients received repeated infusions of the cells. However, the results have not excluded the possibility that autologous MSCs may be more efficacious and safer under some circumstances such as local injections of the cells to repair tissues by engraftment and differentiation.
Controversy VIII: How do MSCs modulate immune responses? This controversy cannot be resolved without further evidence, primarily from experiments in vivo, for the four explanations currently proposed (Fig. 2.7) and others that are likely to be generated in the near future.
Controversy IX: Do human MSCs cause tumors? The probability of human MSCs causing tumors is not zero, but it is extremely low. However, there is convincing evidence that MSCs can enhance tumor growth under some circumstances.
References
Kuhn T (1996) The structure of scientific revolutions. University of Chicago Press, Chicago
Dexter TM (1981) Self-renewing haemopoietic progenitor cells and the factors controlling proliferation and differentiation. Ciba Found Symp 84:22–37, Review. PubMed PMID: 7023872
Eaves CJ, Cashman JD, Sutherland HJ, Otsuka T, Humphries RK, Hogge DE, Lansdorp PL, Eaves AC (1991) Molecular analysis of primitive hematopoietic cell proliferation control mechanisms. Ann N Y Acad Sci 628:298–306, Review. PubMed PMID: 1712556
Prockop DJ, Kota DJ, Bazhanov N, Reger RL (2010) Evolving paradigms for repair of tissues by adult stem/progenitor cells (MSCs). J Cell Mol Med 14(9):2190–2199. doi:10.1111/j.1582-4934.2010.01151.x.Review
Friedenstein AJ, Piatetzky-Shapiro II, Petrakova KV (1966) Osteogenesis in transplants of bone marrow cells. J Embryol Exp Morphol 16(3):381–390
Owen M, Friedenstein AJ (1988) Stromal stem cells: marrow-derived osteogenic precursors. Ciba Found Symp 136:42–60, Review. PubMed PMID: 3068016
Sacchetti B, Funari A, Michienzi S, Di Cesare S, Piersanti S, Saggio I, Tagliafico E, Robey PG, Riminucci M, Bianco P (2007) Self-renewing osteoprogenitors in bone marrow sinusoids can organize a hematopoietic microenvironment. Cell 131(2):324–336, Erratum in: Cell. 2008 133(5):928. PubMed PMID: 17956733
Koç ON, Gerson SL, Cooper BW, Dyhouse SM, Haynesworth SE, Caplan AI, Lazarus HM (2000) Rapid hematopoietic recovery after coinfusion of autologous-blood stem cells and culture-expanded marrow mesenchymal stem cells in advanced breast cancer patients receiving high-dose chemotherapy. J Clin Oncol 18(2):307–316
Méndez-Ferrer S, Michurina TV, Ferraro F, Mazloom AR, Macarthur BD, Lira SA, Scadden DT, Ma’ayan A, Enikolopov GN, Frenette PS (2010) Mesenchymal and haematopoietic stem cells form a unique bone marrow niche. Nature 466(7308):829–834, PubMed PMID: 20703299
Munoz JR, Stoutenger BR, Robinson AP, Spees JL, Prockop DJ (2005) Human stem/progenitor cells from bone marrow promote neurogenesis of endogenous neural stem cells in the hippocampus of mice. Proc Natl Acad Sci USA 102(50):18171–18176, Epub 2005 Dec 5. Erratum in: Proc Natl Acad Sci U S A. 2006 Feb 7;103(6):2000–2. PubMed PMID: 16330757; PubMed Central PMCID: PMC1312406
Caplan AI (1995) Osteogenesis imperfecta, rehabilitation medicine, fundamental research and mesenchymal stem cells. Connect Tissue Res 31(4):S9–S14, Review. PubMed PMID: 15612374
Prockop DJ (1997) Marrow stromal cells as stem cells for nonhematopoietic tissues. Science 276(5309):71–74, Review. PubMed PMID: 9082988
Cohnheim J (1867) Über entzündung und Eiterung. Arch Path Anat Physiol Klin Med 40:1
Pereira RF, Halford KW, O’Hara MD, Leeper DB, Sokolov BP, Pollard MD, Bagasra O, Prockop DJ (1995) Cultured adherent cells from marrow can serve as long-lasting precursor cells for bone, cartilage, and lung in irradiated mice. Proc Natl Acad Sci USA 92(11):4857–4861
Tatard VM, D’Ippolito G, Diabira S, Valeyev A, Hackman J, McCarthy M, Bouckenooghe T, Menei P, Montero-Menei CN, Schiller PC (2007) Neurotrophin-directed differentiation of human adult marrow stromal cells to dopaminergic-like neurons. Bone 40(2):360–373
Kopen GC, Prockop DJ, Phinney DG (1999) Marrow stromal cells migrate throughout forebrain and cerebellum, and they differentiate into astrocytes after injection into neonatal mouse brains. Proc Natl Acad Sci USA 96(19):10711–10716
Wang G, Bunnell BA, Painter RG, Quiniones BC, Tom S, Lanson NA Jr, Spees JL, Bertucci D, Peister A, Weiss DJ, Valentine VG, Prockop DJ, Kolls JK (2005) Adult stem cells from bone marrow stroma differentiate into airway epithelial cells: potential therapy for cystic fibrosis. Proc Natl Acad Sci USA 102(1):186–191
Spees JL, Olson SD, Ylostalo J, Lynch PJ, Smith J, Perry A, Peister A, Wang MY, Prockop DJ (2003) Differentiation, cell fusion, and nuclear fusion during ex vivo repair of epithelium by human adult stem cells from bone marrow stroma. Proc Natl Acad Sci USA 100(5):2397–2402
Xu H, Miki K, Ishibashi S, Sun L, Endo S, Sekiya I, Muneta T, Inazawa J, Dezawa M, Mizusawa H (2010) Transplantation of neuronal cells induced from human mesenchymal stem cells improves neurological functions after stroke without cell fusion. J Neurosci Res 88(16):3598–3609. doi:10.1002/jnr.22501
Pochampally RR, Neville BT, Schwarz EJ, Li MM, Prockop DJ (2004) Rat adult stem cells (marrow stromal cells) engraft and differentiate in chick embryos without evidence of cell fusion. Proc Natl Acad Sci USA 101(25):9282–9285
Kallai I, van Lenthe GH, Ruffoni D, Zilberman Y, Muller R, Pelled G, Gazit D (2010) Quantitative, structural, and image-based mechanical analysis of nonunion fracture repaired by genetically engineered mesenchymal stem cells. J Biomech 43(12):2315–2320
Chen FH, Rousche KT, Tuan RS (2006) Technology insight: adult stem cells in cartilage regeneration and tissue engineering. Nat Clin Pract Rheumatol 2(7):373–382, Review. PubMed PMID: 16932723
Koga H, Engebretsen L, Brinchmann JE, Muneta T, Sekiya I (2009) Mesenchymal stem cell-based therapy for cartilage repair: a review. Knee Surg Sports Traumatol Arthrosc 17(11):1289–1297, Review. PubMed PMID: 19333576
Kleeberger W, Versmold A, Rothämel T, Glӧckner S, Bredt M, Haverich A, Kreipe H (2003) Increased chimerism of bronchial and alveolar epithelium in human lung allografts undergoing chronic injury. Am J Pathol 62(5):1487–1494
Houghton J, Stoicov C, Nomura S, Rogers AB, Carlson J, Li H, Cai X, Fox JG, Goldenring JR, Wang TC (2004) Gastric cancer originating from bone marrow-derived cells. Science 306(5701):1568–1571
Gunn WG, Conley A, Deininger L, Olson SD, Prockop DJ, Gregory CA (2006) A crosstalk between myeloma cells and marrow stromal cells stimulates production of DKK1 and interleukin-6: a potential role in the development of lytic bone disease and tumor progression in multiple myeloma. Stem Cells 24(4):986–991
Ohtaki H, Ylostalo JH, Foraker JE, Robinson AP, Reger RL, Shioda S, Prockop DJ (2008) Stem/progenitor cells from bone marrow decrease neuronal death in global ischemia by modulation of inflammatory/immune responses. Proc Natl Acad Sci USA 105(38):14638–14643
Lee RH, Pulin AA, Seo MJ, Kota DJ, Ylostalo J, Larson BL, Semprun-Prieto L, Delafontaine P, Prockop DJ (2009) Intravenous hMSCs improve myocardial infarction in mice because cells embolized in lung are activated to secrete the anti-inflammatory protein TSG-6. Cell Stem Cell 5(1):54–63
Dominici M, Le Blanc K, Mueller I, Slaper-Cortenbach I, Marini F, Krause D, Deans R, Keating A, Prockop DJ, Horwitz E (2006) Minimal criteria for defining multipotent mesenchymal stromal cells. The International Society for Cellular Therapy position statement. Cytotherapy 8(4):315–317, PubMed PMID: 16923606
Friedenstein AJ, Gorskaja JF, Kulagina NN (1976) Fibroblast precursors in normal and irradiated mouse hematopoietic organs. Exp Hematol 4(5):267–274
Smith JR, Pochampally R, Perry A, Hsu SC, Prockop DJ (2004) Isolation of a highly clonogenic and multipotential subfraction of adult stem cells from bone marrow stroma. Stem Cells 22(5):823–831
Lee RH, Seo MJ, Pulin AA, Gregory CA, Ylostalo J, Prockop DJ (2009) The CD34-like protein PODXL and alpha6-integrin (CD49f) identify early progenitor MSCs with increased clonogenicity and migration to infarcted heart in mice. Blood 113(4):816–826, Epub 2008 Sep 25. PubMed PMID: 18818395; PubMed Central PMCID: PMC2630267
Phinney DG, Kopen G, Righter W, Webster S, Tremain N, Prockop DJ (1999) Donor variation in the growth properties and osteogenic potential of human marrow stromal cells. J Cell Biochem 75(3):424–436
Baddoo M, Hill K, Wilkinson R, Gaupp D, Hughes C, Kopen GC, Phinney DG (2003) Characterization of mesenchymal stem cells isolated from murine bone marrow by negative selection. J Cell Biochem 89(6):1235–1249
Peister A, Mellad JA, Larson BL, Hall BM, Gibson LF, Prockop DJ (2004) Adult stem cells from bone marrow (MSCs) isolated from different strains of inbred mice vary in surface epitopes, rates of proliferation, and differentiation potential. Blood 103(5):1662–1668, Epub 2003 Oct 30. PubMed PMID: 14592819
Rubin H (2001) Multistage carcinogenesis in cell culture. Dev Biol (Basel) 106:61–66, discussion 67, 143–60. PubMed PMID: 11761268
Tolar J, Nauta AJ, Osborn MJ, Panoskaltsis Mortari A, McElmurry RT, Bell S, Xia L, Zhou N, Riddle M, Schroeder TM, Westendorf JJ, McIvor RS, Hogendoorn PC, Szuhai K, Oseth L, Hirsch B, Yant SR, Kay MA, Peister A, Prockop DJ, Fibbe WE, Blazar BR (2007) Sarcoma derived from cultured mesenchymal stem cells. Stem Cells 25(2):371–379, Epub 2006 Oct 12. PubMed PMID: 17038675
Javazon EH, Colter DC, Schwarz EJ, Prockop DJ (2001) Rat marrow stromal cells are more sensitive to plating density and expand more rapidly from single-cell-derived colonies than human marrow stromal cells. Stem Cells 19(3):219–225
Digirolamo CM, Stokes D, Colter D, Class R, Prockop DJ (1999) Propagation and senescence of human marrow stromal cells in culture: a simple colony-forming assay identifies samples with the greatest potential to propagate and differentiate. Br J Haematol 107(2):275–281
Ylöstalo J, Bazhanov N, Prockop DJ (2008) Reversible commitment to differentiation by human multipotent stromal cells in single-cell-derived colonies. Exp Hematol 36(10):1390–1402, Epub 2008 Jul 10. PubMed PMID: 18619725; PubMed Central PMCID: PMC2628773
Krause U, Seckinger A, Gregory CA (2011) Assays of osteogenic differentiation by cultured human mesenchymal stem cells. Methods Mol Biol 698:215–230
Semon JA, Nagy LH, Llamas CB, Tucker HA, Lee RH, Prockop DJ (2010) Integrin expression and integrin-mediated adhesion in vitro of human multipotent stromal cells (MSCs) to endothelial cells from various blood vessels. Cell Tissue Res 341(1):147–158, Epub 2010 Jun 20. PubMed PMID: 20563599
Pereira RF, O’Hara MD, Laptev AV, Halford KW, Pollard MD, Class R, Simon D, Livezey K, Prockop DJ (1998) Marrow stromal cells as a source of progenitor cells for nonhematopoietic tissues in transgenic mice with a phenotype of osteogenesis imperfecta. Proc Natl Acad Sci USA 95(3):1142–1147, PubMed PMID: 9448299; PubMed Central PMCID: PMC18700
Azizi SA, Stokes D, Augelli BJ, DiGirolamo C, Prockop DJ (1998) Engraftment and migration of human bone marrow stromal cells implanted in the brains of albino rats – similarities to astrocyte grafts. Proc Natl Acad Sci USA 95(7):3908–3913, PubMed PMID: 9520466; PubMed Central PMCID: PMC19936
Orkin SH, Zon LI (2008) Hematopoiesis: an evolving paradigm for stem cell biology. Cell 132(4):631–644, PubMed PMID: 18295580; PubMed Central PMCID: PMC2628169
Takahashi K, Yamanaka S (2006) Induction of pluripotent stem cells from mouse embryonic and adult fibroblast cultures by defined factors. Cell 126(4):663–676, Epub 2006 Aug 10. PubMed PMID: 16904174
Gurdon JB, Uehlinger V (1966) “Fertile” intestine nuclei. Nature 210(5042):1240–1241
Fuller MT, Spradling AC (2007) Male and female Drosophila germline stem cells: two versions of immortality. Science 316(5823):402–404, Review. PubMed PMID: 17446390
Medici D, Shore EM, Lounev VY, Kaplan FS, Kalluri R, Olsen BR (2011) Conversion of vascular endothelial cells into multipotent stem-like cells. Nat Med 17(4):514
Zeng R, Wang LW, Hu ZB, Guo WT, Wei JS, Lin H, Sun X, Chen LX, Yang LJ (2011) Differentiation of human bone marrow mesenchymal stem cells into neuron-like cells in vitro. Spine (Phila Pa 1976) 36(13):997–1005, Epub 2011 Jan 25. PubMed PMID: 21270716
Delcroix GJ, Curtis KM, Schiller PC, Montero-Menei CN (2010) EGF and bFGF pre-treatment enhances neural specification and the response to neuronal commitment of MIAMI cells. Differentiation 80(4–5):213–227, Epub 2010 Sep 1. PubMed PMID: 20813449
Zhang L, Seitz LC, Abramczyk AM, Liu L, Chan C (2011) CAMP initiates early phase neuron-like morphology changes and late phase neural differentiation in mesenchymal stem cells. Cell Mol Life Sci 68(5):863–876, Epub 2010 Aug 20. PubMed PMID: 20725762; PubMed Central PMCID: PMC3030935
Kurpinski K, Lam H, Chu J, Wang A, Kim A, Tsay E, Agrawal S, Schaffer DV, Li S (2010) Transforming growth factor-beta and notch signaling mediate stem cell differentiation into smooth muscle cells. Stem Cells 28(4):734–742
Robinson AP, Foraker JE, Ylostalo J, Prockop DJ (2011) Human stem/progenitor cells from bone marrow enhance glial differentiation of rat neural stem cells: a role for transforming growth factor β and Notch signaling. Stem Cells Dev 20(2):289–300, Epub 2010 Sep 14. PubMed PMID: 20575640
Crisan M, Corselli M, Chen CW, Peault B (2011) Multilineage stem cells in the adult: a perivascular legacy? Organogenesis 7(2):101–104, Epub 2011 Apr 1. PubMed PMID: 21593599
Bianco P, Robey PG, Saggio I, Riminucci M (2010) “Mesenchymal” stem cells in human bone marrow (skeletal stem cells): a critical discussion of their nature, identity, and significance in incurable skeletal disease. Hum Gene Ther 21(9):1057–1066
Spees JL, Olson SD, Whitney MJ, Prockop DJ (2006) Mitochondrial transfer between cells can rescue aerobic respiration. Proc Natl Acad Sci USA 103(5):1283–1288, Epub 2006 Jan 23. PubMed PMID: 16432190; PubMed Central PMCID: PMC1345715
Rebbeck CA, Leroi AM, Burt A (2011) Mitochondrial capture by a transmissible cancer. Science 331(6015):303
Islam MN, Das SR, Emin MT, Wei M, Sun L, Westphalen K, Rowlands DJ, Quadri SK, Bhattacharya S, Bhattacharya J (2012) Mitochondrial transfer from bone-marrow-derived stromal cells to pulmonary alveoli protects against acute lung injury. Nat Med 18(5):759–765. doi:10.1038/nm.2736
Gao J, Dennis JE, Muzic RF, Lundberg M, Caplan AI (2001) The dynamic in vivo distribution of bone marrow-derived mesenchymal stem cells after infusion. Cells Tissues Organs 169(1):12–20
Schrepfer S, Deuse T, Reichenspurner H, Fischbein MP, Robbins RC, Pelletier MP (2007) Stem cell transplantation: the lung barrier. Transplant Proc 39(2):573–576
Bartosh TJ, Ylöstalo JH, Mohammadipoor A, Bazhanov N, Coble K, Claypool K, Lee RH, Choi H, Prockop DJ (2010) Aggregation of human mesenchymal stromal cells (MSCs) into 3D spheroids enhances their antiinflammatory properties. Proc Natl Acad Sci USA 107(31):13724–13729, Epub 2010 Jul 19. PubMed PMID: 20643923; PubMed Central PMCID: PMC2922230
Nemeth K, Leelahavanichkul A, Yuen PS, Mayer B, Parmelee A, Doi K, Robey PG, Leelahavanichkul K, Koller BH, Brown JM, Hu X, Jelinek I, Star RA, Mezey E (2009) Bone marrow stromal cells attenuate sepsis via prostaglandin E(2)-dependent reprogramming of host macrophages to increase their interleukin-10 production. Nat Med 15:42–49, Epub 2008 Nov 21. Erratum in: Nat Med. 2009 Apr;15(4):462. PubMed PMID: 19098906; PubMed Central PMCID: PMC2706487
Ortiz LA, Dutreil M, Fattman C, Pandey AC, Torres G, Go K, Phinney DG (2007) Interleukin 1 receptor antagonist mediates the antiinflammatory and antifibrotic effect of mesenchymal stem cells during lung injury. Proc Natl Acad Sci USA 104:11002–11007, Epub 2007 Jun 14. PubMed PMID: 17569781; PubMed Central PMCID: PMC1891813
Yagi H, Soto-Gutierrez A, Navarro-Alvarez N, Nahmias Y, Goldwasser Y, Kitagawa Y, Tilles AW, Tompkins RG, Parekkadan B, Yarmush ML (2010) Reactive bone marrow stromal cells attenuate systemic inflammation via sTNFR1. Mol Ther 18(10):1857–1864, Epub 2010 Jul 27. PubMed PMID: 20664529; PubMed Central PMCID: PMC2951565
Le Blanc K, Rasmusson I, Sundberg B, Götherström C, Hassan M, Uzunel M, Ringdén O (2004) Treatment of severe acute graft-versus-host disease with third party haploidentical mesenchymal stem cells. Lancet 363(9419):1439–1441
Lu B, Wang S, Girman S, McGill T, Ragaglia V, Lund R (2010) Human adult bone marrow-derived somatic cells rescue vision in a rodent model of retinal degeneration. Exp Eye Res 91(3):449–455, Epub 2010 Jul 13. PubMed PMID: 20603115
Choi H, Lee RH, Bazhanov N, Oh JY, Prockop DJ (2011) Anti-inflammatory protein TSG-6 secreted by activated MSCs attenuates zymosan-induced mouse peritonitis by decreasing TLR2/NF-{kappa}B signaling in resident macrophages. Blood 118(2):330–338, Epub 2011 May 6. PubMed PMID: 21551236
Garbayo E, Raval AP, Curtis KM, Della-Morte D, Gomez LA, D’Ippolito G, Reiner T, Perez-Stable C, Howard GA, Perez-Pinzon MA, Montero-Menei CN, Schiller PC (2011) Neuroprotective properties of marrow-isolated adult multilineage-inducible cells in rat hippocampus following global cerebral ischemia are enhanced when complexed to biomimetic microcarriers. J Neurochem 119(5):972–988, Apr 15. doi: 10.1111/j.1471-4159.2011.07272.x. Epub 2011 May 13. PubMed PMID: 21496021
Costa-Pinto AR, Correlo VM, Sol PC, Bhattacharya M, Srouji S, Livne E, Reis RL, Neves NM (2012) Chitosan-poly(butylene succinate) scaffolds and human bone marrow stromal cells induce bone repair in a mouse calvaria model. J Tissue Eng Regen Med 6(1):21–28. doi:10.1002/term.391.Epub2011Feb10
Wu H, Lu W, Mahato RI (2011) Mesenchymal stem cells as a gene delivery vehicle for successful islet transplantation. Pharm Res 28(9):2098–2109, Epub 2011 Apr 16. PubMed PMID: 21499838; PubMed Central PMCID: PMC3152657
Sheikh AM, Nagai A, Wakabayashi K, Narantuya D, Kobayashi S, Yamaguchi S, Kim SU (2011) Mesenchymal stem cell transplantation modulates neuroinflammation in focal cerebral ischemia: contribution of fractalkine and IL-5. Neurobiol Dis 41(3):717–724, Epub 2010 Dec 17. PubMed PMID: 21168500
Abrams MB, Dominguez C, Pernold K, Reger R, Wiesenfeld-Hallin Z, Olson L, Prockop D (2009) Multipotent mesenchymal stromal cells attenuate chronic inflammation and injury-induced sensitivity to mechanical stimuli in experimental spinal cord injury. Restor Neurol Neurosci 27(4):307–321
Hofstetter CP, Schwarz EJ, Hess D, Widenfalk J, El Manira A, Prockop DJ, Olson L (2002) Marrow stromal cells form guiding strands in the injured spinal cord and promote recovery. Proc Natl Acad Sci USA 99(4):2199–2204, PubMed PMID: 11854516; PubMed Central PMCID: PMC122342
Koga H, Shimaya M, Muneta T, Nimura A, Morito T, Hayashi M, Suzuki S, Ju YJ, Mochizuki T, Sekiya I (2008) Local adherent technique for transplanting mesenchymal stem cells as a potential treatment of cartilage defect. Arthritis Res Ther 10(4):R84, Epub 2008 Jul 29. PubMed PMID: 18664254; PubMed Central PMCID: PMC2575632
Rafei M, Campeau PM, Aguilar-Mahecha A, Buchanan M, Williams P, Birman E, Yuan S, Young YK, Boivin MN, Forner K, Basik M, Galipeau J (2009) Mesenchymal stromal cells ameliorate experimental autoimmune encephalomyelitis by inhibiting CD4 Th17 T cells in a CC chemokine ligand 2-dependent manner. J Immunol 182(10):5994–6002
François M, Romieu-Mourez R, Stock-Martineau S, Boivin MN, Bramson JL, Galipeau J (2009) Mesenchymal stromal cells cross-present soluble exogenous antigens as part of their antigen-presenting cell properties. Blood 114(13):2632–2638, Epub 2009 Aug 4. PubMed PMID: 19654411
English K, Ryan JM, Tobin L, Murphy MJ, Barry FP, Mahon BP (2009) Cell contact, prostaglandin E(2) and transforming growth factor beta 1 play non-redundant roles in human mesenchymal stem cell induction of CD4+CD25(high) forkhead box P3+ regulatory T cells. Clin Exp Immunol 156(1):149–160, Epub 2009 Feb 3. PubMed PMID: 19210524; PubMed Central PMCID: PMC2673753
Uccelli A, Moretta L, Pistoia V (2008) Mesenchymal stem cells in health and disease. Nat Rev Immunol 8(9):726–736, Review. PubMed PMID: 19172693
Bernardo ME, Locatelli F, Fibbe WE (2009) Mesenchymal stromal cells. Ann N Y Acad Sci 1176:101–117, Review. PubMed PMID: 19796238
Ren G, Su J, Zhang L, Zhao X, Ling W, L’huillie A, Zhang J, Lu Y, Roberts AI, Ji W, Zhang H, Rabson AB, Shi Y (2009) Species variation in the mechanisms of mesenchymal stem cell-mediated immunosuppression. Stem Cells 27(8):1954–1962
Rubio D, Garcia-Castro J, Martín MC, de la Fuente R, Cigudosa JC, Lloyd AC, Bernad A (2005) Spontaneous human adult stem cell transformation. Cancer Res 65(8):3035–3039, PubMed PMID: 15833829
Wang Y, Huso DL, Harrington J, Kellner J, Jeong DK, Turney J, McNiece IK (2005) Outgrowth of a transformed cell population derived from normal human BM mesenchymal stem cell culture. Cytotherapy 7(6):509–519
Røsland GV, Svendsen A, Torsvik A, Sobala E, McCormack E, Immervoll H, Mysliwietz J, Tonn JC, Goldbrunner R, Lønning PE, Bjerkvig R, Schichor C (2009) Long-term cultures of bone marrow-derived human mesenchymal stem cells frequently undergo spontaneous malignant transformation. Cancer Res 69(13):5331–5339, Epub 2009 Jun 9. PubMed PMID: 19509230
Bernardo ME, Zaffaroni N, Novara F, Cometa AM, Avanzini MA, Moretta A, Montagna D, Maccario R, Villa R, Daidone MG, Zuffardi O, Locatelli F (2007) Human bone marrow derived mesenchymal stem cells do not undergo transformation after long-term in vitro culture and do not exhibit telomere maintenance mechanisms. Cancer Res 67(19):9142–9149
Pittenger MF, Mackay AM, Beck SC, Jaiswal RK, Douglas R, Mosca JD, Moorman MA, Simonetti DW, Craig S, Marshak DR (1999) Multilineage potential of adult human mesenchymal stem cells. Science 284(5411):143–147
Izadpanah R, Kaushal D, Kriedt C, Tsien F, Patel B, Dufour J, Bunnell BA (2008) Long-term in vitro expansion alters the biology of adult mesenchymal stem cells. Cancer Res 68(11):4229–4238, PubMed PMID: 18519682; PubMed Central PMCID: PMC2713721
Larson BL, Ylostalo J, Lee RH, Gregory C, Prockop DJ (2010) Sox 11 is expressed in early progenitor human multipotent stromal cells (hMSCs) and decreases with extensive expansion of the cells. Tissue Eng Part A 16(11):3385–3394, Epub 2010 Jul 13. PubMed PMID: 20626275; PubMed Central PMCID: PMC2965191
Garcia S, Bernad A, Martín MC, Cigudosa JC, Garcia-Castro J, de la Fuente R (2010) Pitfalls in spontaneous in vitro transformation of human mesenchymal stem cells. Exp Cell Res 316(9):1648–1650, Epub 2010 Feb 18. PubMed PMID: 20171963
Torsvik A, Røsland GV, Svendsen A, Molven A, Immervoll H, McCormack E, Lønning PE, Primon M, Sobala E, Tonn JC, Goldbrunner R, Schichor C, Mysliwietz J, Lah TT, Motaln H, Knappskog S, Bjerkvig R (2010) Spontaneous malignant transformation of human mesenchymal stem cells reflects cross-contamination: putting the research field on track – letter. Cancer Res 70(15):6393–6396, Epub 2010 Jul 14. PubMed PMID: 20631079
Lacroix M (2008) Persistent use of “false” cell lines. Int J Cancer 122(1):1–4, Review. PubMed PMID: 17960586
Laurent LC, Ulitsky I, Slavin I, Tran H, Schork A, Morey R, Lynch C, Harness JV, Lee S, Barrero MJ, Ku S, Martynova M, Semechkin R, Galat V, Gottesfeld J, Izpisua Belmonte JC, Murry C, Keirstead HS, Park HS, Schmidt U, Laslett AL, Muller FJ, Nievergelt CM, Shamir R, Loring JF (2011) Dynamic changes in the copy number of pluripotency and cell proliferation genes in human ESCs and iPSCs during reprogramming and time in culture. Cell Stem Cell 8(1):106–118, PubMed PMID: 21211785; PubMed Central PMCID: PMC3043464
Dolgin E (2010) Putting stem cells to the test. Nat Med 16(12):1354–1357
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2013 Springer Science+Business Media New York
About this chapter
Cite this chapter
Prockop, D.J., Reger, R.L. (2013). MSCs: Changing Hypotheses, Paradigms, and Controversies on Mechanisms of Action in Repairing Tissues. In: Hematti, P., Keating, A. (eds) Mesenchymal Stromal Cells. Stem Cell Biology and Regenerative Medicine. Humana Press, New York, NY. https://doi.org/10.1007/978-1-4614-5711-4_2
Download citation
DOI: https://doi.org/10.1007/978-1-4614-5711-4_2
Published:
Publisher Name: Humana Press, New York, NY
Print ISBN: 978-1-4614-5710-7
Online ISBN: 978-1-4614-5711-4
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)