Abstract
Background
Colectomies performed according to complete mesocolic excision (CME) principles have demonstrated an improvement in the quality of surgical specimen and a potential improvement of long-term results. Laparoscopic CME right hemicolectomy is considered a demanding procedure and adopted in few centers from the West. The main purpose of this paper is to present a video showing our technique for laparoscopic CME right hemicolectomy and to analyze our short-term results to prove its safety.
Methods
Data from 38 patients operated on at the Division of General and Hepatobiliary Surgery, University of Verona Hospital Trust, between September 2014 and February 2017, were included in the study.
Results
In the present series, 37% of patients were ≥75 years old, 32% of patients were ASA class 3, 46% of patients had ≥2 comorbidities, 30% of patients had BMI >28 and 17% of patients had ≥2 previous abdominal surgeries. Despite these unfavorable clinic characteristics, no mortality was observed, Clavien-Dindo ≥3 complications occurred in 13.1% and redo surgery in 5.3%. Good quality specimens were obtained with a mean (SD) length of 34.5±7.5 cm, a proximal margin of 16.8±9.2 cm and a distal margin of 14.3±6.4 cm. The mean (SD) number of harvested lymph nodes was 24.3 (8.3).
Conclusions
When implemented in a Western center, laparoscopic CME right hemicolectomy is feasible and safe and allows obtaining good quality specimens.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Open and laparoscopic resections for colorectal cancer (CRC) have proved to have comparable long-term results on several randomized controlled trials. However, laparoscopic approach offers better short-term outcomes in terms of intra-operative blood loss, post-operative pain control, return to bowel function, resumption of oral diet, and shorter length of hospital stay.1,2,3,4,5,6,7,8 Several authors have questioned the superiority of the laparoscopic approach in right-sided colon cancer (CC) with regard to both clinical outcomes and technical difficulties due to vascular anatomical variations.9,10,11
Another debated topic is the utility of the complete mesocolic excision (CME) with central vascular ligation (CVL) as proposed by Hohenberger et al.12,13,14,15 A recent study demonstrated that the implementation of CME with CVL in open CC surgery improves locoregional disease control and yields better overall survival in stage III tumors.16
The CME concept is based on two main principles: (1) carrying out the surgical dissection along embryological planes and maintaining the embryological envelope around the mesocolon to allow clear circumferential margins and (2) dividing supplying arteries at their origin after wide colonic mobilization and dissection along the main feeding vessels.12,13,17,18 Such principles result in a wide bowel resection and a complete mesocolic excision and allow a high yield of lymph node retrieval.13,16,17,18
Hohenberger’s surgical principles are maintained in the Japanese experience with D3 lymphadenectomy, in which the extent of bowel resection is however more limited.19,20,21,22
Several studies have demonstrated the feasibility of laparoscopic CME for right-sided CC23,24,25,26,27,28; however, very few of them come from Western centers.23,24,28
The aims of this paper are to present our surgical technique for laparoscopic complete mesocolic excision with D3 lymphadenectomy for right-sided colon cancer and to report our short-term results in order to confirm the feasibility and safeness of this demanding procedure in a Western series.
Methods
Patients Under Study
This single-center retrospective study analyzes the data from 38 consecutive laparoscopic CME colectomies with D3 lymphadenectomy for right-sided colon cancer performed at the Division of General and Hepatobiliary Surgery, University of Verona Hospital Trust, between September 2014 and February 2017. The data reported in the text supplement the video which demonstrates the standardization of the surgical technique.
Surgical Technique
The CME procedure reproduced the technique described by Choi and colleagues.29,30 All the procedures were performed by a single surgeon (C.P.).
The patient is placed on the operative table in the supine position with 20° Trendelenburg and slight left side tilt. The operating surgeon and the camera driver stand to the left of the patient while the assistant stands to the right. A 12-mm camera port is placed below the umbilicus, and four additional 5-mm ports, one in each quadrant of the abdomen, complete the port placement. The upper and lower right trocars are used as main working ports, while the left trocars are used for main tractions. Upon upward positioning of the small bowel, the ileocolic mesentery is retracted upward and cephalad; then, the peritoneum is incised at the basis of the ileocolic mesentery. Thus, the terminal ileum, cecum, and ascending colon are fully mobilized in a lateral to medial and caudal to cephalad fashion. The mobilization is carried out until the complete exposure of the duodenum and pancreatic head together with the root of superior mesenteric vessels and the origin of middle colic vessels is achieved. The right ureter is identified during this maneuver.
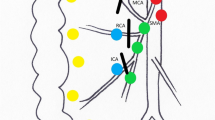
Following this step, downward tension of the ileocolic and upward tension on the middle colic pedicles allow dissection along the anterior aspect of the superior mesenteric vessels. Lymphadenectomy is carried out along the left border of the superior mesenteric vein. For tumor involving the cecum, the ascending colon, and the hepatic flexure, the dissection includes the origin of the middle colic artery and vein, preserving the left branch of middle colic vessels while, for transverse colon tumors, the middle colic vessels are divided at their origin. The procedure is completed by taking down the hepatic flexure and dividing the transverse mesocolon and distal ileum mesenteries. The specimen is extracted by extending the camera port when an extracorporeal anastomosis is performed or through a suprapubic transverse incision when an intracorporeal anastomosis is carried out.
Post-operative Measurements and Data Analysis
All demographic, clinic-pathologic, and outcome data were prospectively collected and stored in a PC dataset by a member of the surgical team. Any deviation from the normal post-operative course was regarded as a complication. Post-operative morbidity and mortality accounted for all adverse events occurring in-hospital or within 30 days after surgery. Complications were graded according to the Clavien-Dindo classification.31
Pathology specimens were analyzed in accord with the 7th Edition of the American Joint Committee on Cancer (AJCC) and the Union International Contre Le Cancer (UICC) criteria. Tumor size, length of specimens, and surgical resection margins were obtained from formalin-fixed specimens.
Continuous data were presented as means (standard deviation) or medians (range). Categorical data were presented as frequencies.
Results
Patient demographics and clinical characteristics are reported in Table 1. Notably, in this series, 44.7% of patients were 75 years or older, 34.2% were classified as ASA 3, 55.3% had at least two associated comorbidities, 36.8% had a BMI higher than 28, and 18.4% received at least two previous abdominal surgeries.
Operative data and post-operative short-term results are presented in Tables 2 and 3. The mean (SD) time of surgery was 207 (58) min. Intraoperative complications occurred in 7.9% of patients, while conversion to open surgery was required in less than 3% of the cases. Estimated blood loss was minimal [median (range), 30 mL (20–140)].
No post-operative deaths occurred during the study period, although 44.5% of patients experienced one or more complications. Complications were classified as Clavien-Dindo grades 1 and 2 in the majority of cases (70.6%), while a Clavien-Dindo grade 3 complication was observed in 5 patients. Among these, 2 patients required redo surgery (Clavien-Dindo grade 3b): one patient for anastomotic leakage and one patient for mechanical bowel obstruction. Histopathological examination results are reported in Table 4. The mean (SD) length of the specimen was 34.5 ± 7.5 cm with proximal and distal margins of 16.8 ± 9.2 cm and 14.3 ± 6.4 cm, respectively. The mean (SD) number of harvested lymph nodes was 24.3 (8.3), and the percentage of patients with an adequate number of analyzed nodes (≥ 12 lymph nodes) was 97.4%. Regarding pTNM staging, 68.4% of the patients had a pT3–T4 tumor and 39.5% showed a pN+ tumor.
None of the patients had microscopic longitudinal or circumferential positive resection margins.
Discussion
A highly debated issue in CC surgery regards the added value of complete mesocolic excision with central vascular ligation (CME with CVL).13,14,18,21 Colectomies performed according to CME principles have demonstrated an improvement in the quality of surgical specimen (margins clearance, numbers of retrieved nodes) with a potential improvement of long-term results.16,32,33
Although laparoscopic surgery is now accepted as the standard treatment for resection of right-sided CC, laparoscopic CME right hemicolectomy is considered a demanding procedure. Firstly popularized by Hohenberger et al.,12 it is currently performed routinely in few Western centers and more frequently in the Far East.18,21,25,34,35,36 We have recently highlighted the differences between Hohenberger’s right hemicolectomy with CME and CVL and Japanese CME with D3 lymphadenectomy.22 In the Japanese CME right hemicolectomy, no Kocher maneuver is performed, lymphadenectomy is limited to the anterior aspect of the SMV, and the extent of bowel resection is guided by supplying arteries (i.e., ileocolic, right colic, and middle colic considering the right and left branches).19,20 When the feeding artery is in close proximity to the tumor, a 10-cm margin is required. When this lies within 10 cm of the tumor, a 5-cm margin is thought to be sufficient.19 Hohenberger’s CME and Japanese CME are therefore similar in cecal and ascending CC, but they differ in hepatic flexure and transverse colon malignancies, whereby the extent of colonic resection is significantly larger in Hohenberger’s procedure.22
Our CME procedure follows the principles described by the Japanese authors. The adequacy of this approach is demonstrated by the high rate of potentially curative (R0) resections with the absence of involved longitudinal and circumferential margins and an adequate number of harvested lymph nodes. These results compare favorably with other studies on standard right hemicolectomy from Europe and the USA1,2,3,4,5,6,7,8, 14,37,38,39,40 and are equivalent to studies on the CME right hemicolectomy from the Western14,23,24,40,41 and Eastern countries.25,28,34,35,42,43
Laparoscopic CME right hemicolectomy is regarded as a complex procedure which presents several technical difficulties.44 The development of robotic surgery may have helped to overcome some of those difficulties. Nonetheless, even though robotic rectal surgery has been extensively analyzed,45 only few studies comparing laparoscopic versus robotic right colectomy have been published.46 Such studies, although able to prove that robotic CME right hemicolectomy is safe and feasible, have failed to demonstrate an advantage of the robotic over the laparoscopic approach.29,47
With regard to patient selection, considering comorbidities, age, and BMI, it is important to notice that our patient population is more similar to the one reported in Western studies than the one that might be reported in Eastern ones.18,23,28,47 This aspect may explain why the number of centers adopting laparoscopic CME right hemicolectomy in Europe and North America is still scant. In our experience, 45% of patients were older than 75 years of age; 37% had a BMI higher than 28, 55% had two or more comorbidities; 35% were as ASA class 3 and 18% had two or more previous abdominal surgeries. Nevertheless, post-operative mortality was nil, and post-operative complication rate was comparable to that of previous reports, although a slightly higher rate of prolonged post-operative ileus was observed (data not shown, 13.8%).15,16,18
Instead of the retrospective nature and the limited sample size, this study represents one of the very few Western experiences demonstrating the safety and feasibility of CME colectomy performed laparoscopically. Due to the short follow-up, no definite conclusions can be drawn with regard to long-term survival and disease-free outcomes.
References
Fleshman J, Sargent DJ, Green E, et al. Laparoscopic colectomy for cancer is not inferior to open surgery based on 5-year data from the COST Study Group trial. Ann Surg. 2007;246(4):655–662; discussion 662–654.
Bagshaw PF, Allardyce RA, Frampton CM, et al. Long-term outcomes of the australasian randomized clinical trial comparing laparoscopic and conventional open surgical treatments for colon cancer: the Australasian Laparoscopic Colon Cancer Study trial. Ann Surg. 2012;256(6):915–919.
Bonjer HJ, Deijen CL, Abis GA, et al. A randomized trial of laparoscopic versus open surgery for rectal cancer. New Engl J Med. 2015;372(14):1324–1332.
Buunen M, Veldkamp R, Hop WC, et al. Survival after laparoscopic surgery versus open surgery for colon cancer: long-term outcome of a randomised clinical trial. Lancet Oncol. 2009;10(1):44–52.
Green BL, Marshall HC, Collinson F, et al. Long-term follow-up of the Medical Research Council CLASICC trial of conventional versus laparoscopically assisted resection in colorectal cancer. Br J Surg. 2013;100(1):75–82.
Martel G, Crawford A, Barkun JS, Boushey RP, Ramsay CR, Fergusson DA. Expert opinion on laparoscopic surgery for colorectal cancer parallels evidence from a cumulative meta-analysis of randomized controlled trials. PloS One. 2012;7(4):e35292.
Pedrazzani C, Moro M, Ghezzi G, Ruzzenente A, Delaini G, Guglielmi A. What should we intend for minimally invasive treatment of colorectal cancer? Surg Oncol. 2014;23(3):147–154.
van der Pas MH, Haglind E, Cuesta MA, et al. Laparoscopic versus open surgery for rectal cancer (COLOR II): short-term outcomes of a randomised, phase 3 trial. Lancet Oncol. 2013;14(3):210–218.
Rondelli F, Trastulli S, Avenia N, et al. Is laparoscopic right colectomy more effective than open resection? A meta-analysis of randomized and nonrandomized studies. Colorectal Dis. Aug 2012;14(8):e447–469.
Alsabilah J, Kim WR, Kim NK. Vascular Structures of the Right Colon: Incidence and Variations with Their Clinical Implications. Scand J Surg. 2017;106(2):107–115.
Jamali FR, Soweid AM, Dimassi H, Bailey C, Leroy J, Marescaux J. Evaluating the degree of difficulty of laparoscopic colorectal surgery. Arch Surg. 2008;143(8):762–767; discussion 768.
Hohenberger W, Weber K, Matzel K, Papadopoulos T, Merkel S. Standardized surgery for colonic cancer: complete mesocolic excision and central ligation--technical notes and outcome. Colorectal Dis. 2009;11(4):354–364; discussion 364–355.
Gouvas N, Agalianos C, Papaparaskeva K, Perrakis A, Hohenberger W, Xynos E. Surgery along the embryological planes for colon cancer: a systematic review of complete mesocolic excision. Int J Colorectal Dis. 2016;31(9):1577–1594.
Athanasiou CD, Markides GA, Kotb A, Jia X, Gonsalves S, Miskovic D. Open compared with laparoscopic complete mesocolic excision with central lymphadenectomy for colon cancer: a systematic review and meta-analysis. Colorectal Dis. 2016;18(7):O224–235.
Olofsson F, Buchwald P, Elmstahl S, Syk I. No benefit of extended mesenteric resection with central vascular ligation in right-sided colon cancer. Colorectal Dis. 2016;18(8):773–778.
Merkel S, Weber K, Matzel KE, Agaimy A, Gohl J, Hohenberger W. Prognosis of patients with colonic carcinoma before, during and after implementation of complete mesocolic excision. Br J Surg. 2016;103(9):1220–1229.
West NP, Hohenberger W, Weber K, Perrakis A, Finan PJ, Quirke P. Complete mesocolic excision with central vascular ligation produces an oncologically superior specimen compared with standard surgery for carcinoma of the colon. J Clin Oncol. 2010;28(2):272–278.
Kim NK, Kim YW, Han YD, et al. Complete mesocolic excision and central vascular ligation for colon cancer: Principle, anatomy, surgical technique, and outcomes. Surg Oncol. 2016;25(3):252–262.
Japanese Society for Cancer of the Colon and Rectum (JSCCR) (2010). Japanese classification of colorectal carcinoma, 2nd edn. Kanehara & Co., Ltd., Tokyo
West NP, Kobayashi H, Takahashi K, et al. Understanding optimal colonic cancer surgery: comparison of Japanese D3 resection and European complete mesocolic excision with central vascular ligation. J Clin Oncol. 2012;30(15):1763–1769.
Ishiguro M, Higashi T, Watanabe T, Sugihara K. Changes in colorectal cancer care in japan before and after guideline publication: a nationwide survey about D3 lymph node dissection and adjuvant chemotherapy. J Am Coll Surg. 2014;218(5):969–977.e961.
Pedrazzani C, Lauka L, Sforza S, et al. Management of nodal disease from colon cancer in the laparoscopic era. Int J Colorectal Dis. 2015;30(3):303–314.
Adamina M, Manwaring ML, Park KJ, Delaney CP. Laparoscopic complete mesocolic excision for right colon cancer. Surg Endosc. 2012;26(10):2976–2980.
Gouvas N, Pechlivanides G, Zervakis N, Kafousi M, Xynos E. Complete mesocolic excision in colon cancer surgery: a comparison between open and laparoscopic approach. Colorectal Dis. 2012;14(11):1357–1364.
Kang J, Kim IK, Kang SI, Sohn SK, Lee KY. Laparoscopic right hemicolectomy with complete mesocolic excision. Surg Endosc. 2014;28(9):2747–2751.
Huang JL, Wei HB, Fang JF, et al. Comparison of laparoscopic versus open complete mesocolic excision for right colon cancer. Int J Surg. 2015;23(Pt A):12–17.
Kim IY, Kim BR, Choi EH, Kim YW. Short-term and oncologic outcomes of laparoscopic and open complete mesocolic excision and central ligation. Int J Surg. 2016;27:151–157.
Melich G, Jeong DH, Hur H, et al. Laparoscopic right hemicolectomy with complete mesocolic excision provides acceptable perioperative outcomes but is lengthy--analysis of learning curves for a novice minimally invasive surgeon. Can J Surg. 2014;57(5):331–336.
Park JS, Choi GS, Park SY, Kim HJ, Ryuk JP. Randomized clinical trial of robot-assisted versus standard laparoscopic right colectomy. Br J Surg. 2012;99(9):1219–1226.
Park IJ, Choi GS, Kang BM, Lim KH, Jun SH. Lymph node metastasis patterns in right-sided colon cancers: is segmental resection of these tumors oncologically safe?. Ann Surg Oncol. 2009;16(6):1501–1506.
Dindo D, Demartines N, Clavien PA. Classification of surgical complications: a new proposal with evaluation in a cohort of 6336 patients and results of a survey. Ann Surg. 2004;240(2):205–213.
Storli KE, Sondenaa K, Furnes B, et al. Short term results of complete (D3) vs. standard (D2) mesenteric excision in colon cancer shows improved outcome of complete mesenteric excision in patients with TNM stages I-II. Tech Coloproctol. 2014;18(6):557–564.
Kotake K, Mizuguchi T, Moritani K, et al. Impact of D3 lymph node dissection on survival for patients with T3 and T4 colon cancer. Int J Colorectal Dis. 2014;29(7):847–852.
Xie D, Yu C, Gao C, Osaiweran H, Hu J, Gong J. An Optimal Approach for Laparoscopic D3 Lymphadenectomy Plus Complete Mesocolic Excision (D3+CME) for Right-Sided Colon Cancer. Ann Surg Oncol. 2017;24(5):1312–1313.
Matsuda T, Iwasaki T, Sumi Y, et al. Laparoscopic complete mesocolic excision for right-sided colon cancer using a cranial approach: anatomical and embryological consideration. Int J Colorectal Dis. 2017;32(1):139–141.
Bokey L, Chapuis PH, Chan C, et al. Long-term results following an anatomically based surgical technique for resection of colon cancer: a comparison with results from complete mesocolic excision. Colorectal Dis. 2016;18(7):676–683.
Hanna NN, Onukwugha E, Choti MA, et al. Comparative analysis of various prognostic nodal factors, adjuvant chemotherapy and survival among stage III colon cancer patients over 65 years: an analysis using surveillance, epidemiology and end results (SEER)-Medicare data. Colorectal Dis. 2012;14(1):48–55.
Benz S, Barlag H, Gerken M, Furst A, Klinkhammer-Schalke M. Laparoscopic surgery in patients with colon cancer: a population-based analysis. Surg Endosc. 2017;31(6):2586–2595.
Stormark K, Soreide K, Soreide JA, et al. Nationwide implementation of laparoscopic surgery for colon cancer: short-term outcomes and long-term survival in a population-based cohort. Surg Endosc. 2016;30(11):4853–4864.
Storli KE, Sondenaa K, Furnes B, Eide GE. Outcome after introduction of complete mesocolic excision for colon cancer is similar for open and laparoscopic surgical treatments. Dig Surg. 2013;30(4–6):317–327.
Siani LM, Lucchi A, Berti P, Garulli G. Laparoscopic complete mesocolic excision with central vascular ligation in 600 right total mesocolectomies: Safety, prognostic factors and oncologic outcome. Am J Surg. 16 2016.
Liang JT, Lai HS, Lee PH. Laparoscopic medial-to-lateral approach for the curative resection of right-sided colon cancer. Ann Surg Oncol. 2007;14(6):1878–1879.
Zou L, Xiong W, Mo D, et al. Laparoscopic Radical Extended Right Hemicolectomy Using a Caudal-to-Cranial Approach. Ann Surg Oncol. 2016;23(8):2562–2563.
Fabozzi M, Cirillo P, Corcione F. Surgical approach to right colon cancer: From open technique to robot. State of art. World J Gastroint Surg. 27 2016;8(8):564–573.
Hui VW, Guillem JG. Minimal access surgery for rectal cancer: an update. Nat Rev Gastroenterol Hepatol. 2014;11(3):158–165.
Petrucciani N, Sirimarco D, Nigri GR, et al. Robotic right colectomy: A worthwhile procedure? Results of a meta-analysis of trials comparing robotic versus laparoscopic right colectomy. J Minim Access Surg. 2015;11(1):22–28.
Spinoglio G, Marano A, Bianchi PP, et al. Robotic Right Colectomy with Modified Complete Mesocolic Excision: Long-Term Oncologic Outcomes. Ann Surg Oncol. 2016;23(Suppl 5):684–691.
Acknowledgements
Dr. Corrado Pedrazzani and Prof. Alfredo Guglielmi thank Prof. Gyu Seog Choi for the great help in demonstrating and teaching them his technique.
Author information
Authors and Affiliations
Contributions
Conception and design: C. Pedrazzani and A. Guglielmi
Acquisition of data: E. Lazzarini, G. Turri, C. Conti, and V. Tombolan
Analysis and interpretation of data: C. Pedrazzani, E. Lazzarini, E. Fernandes, and F. Nifosì
Drafting the manuscript: E. Lazzarini, G. Turri, E. Fernandes, C. Conti, and V. Tombolan
Revising the manuscript: C. Pedrazzani, F. Nifosì, and A. Guglielmi
Final approval and agreement to be accountable for all aspects of the manuscript: C. Pedrazzani, E. Lazzarini, G. Turri, E. Fernandes, C. Conti, V. Tombolan, F. Nifosì, and A. Guglielmi
Corresponding author
Ethics declarations
Informed consent was obtained from all the patients and the study was approved by the local Ethics Committee.
Conflict of Interest
The authors declare that they have no conflict of interest.
Electronic Supplementary Material
ESM 1
(WMV 305097 kb)
Rights and permissions
About this article
Cite this article
Pedrazzani, C., Lazzarini, E., Turri, G. et al. Laparoscopic Complete Mesocolic Excision for Right-Sided Colon Cancer: Analysis of Feasibility and Safety from a Single Western Center. J Gastrointest Surg 23, 402–407 (2019). https://doi.org/10.1007/s11605-018-4040-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-018-4040-2