Abstract
One of the primary deficits in Parkinson’s disease (PD) is the loss of dopaminergic neurons in the substantia nigra pars compacta which leads to striatal dopaminergic deficits that underlie the motor symptoms associated with the disease. A plethora of animal models have been developed over the years to uncover the molecular alterations that lead to PD development. These models have provided valuable information on neurotransmitter pathways and mechanisms involved. One such a system is the nicotinic cholinergic system. Numerous studies show that nigrostriatal damage affects nicotinic receptor-mediated dopaminergic signaling; therefore therapeutic modulation of the nicotinic cholinergic system may offer a novel approach to manage PD. In fact, there is evidence showing that nicotinic receptor drugs may be useful as neuroprotective agents to prevent Parkinson’s disease progression. Additional preclinical studies also show that nicotinic receptor drugs may be beneficial for the treatment of L-dopa induced dyskinesias. Here, we review preclinical findings supporting the idea that nicotinic receptors are valuable therapeutic targets for PD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Parkinson’s Disease Overview
Parkinson’s disease (PD) is the second most common neurodegenerative disorder among the population over 65 years of age worldwide (Bertram and Tanzi 2005). The main neuronal deficit in PD consists of a loss of dopaminergic neurons in the substantia nigra pars compacta (SNc) that leads to striatal dopamine (DA) deficiency. This dopaminergic loss is linked to motor deficits like akinesia, rigidity, resting tremor and postural instability (Di Monte et al. 2000; Meissner et al. 2011; Obeso et al. 2004, 2010; Schapira and Jenner 2011; Wichmann et al. 2011; Wullner et al. 1994). In addition, there are non-motor symptoms such as cognitive deficits (e.g., mild to severe memory impairment), emotional changes (e.g., depression, apathy and anxiety), sleep perturbations (e.g., insomnia, hypersomnia, rapid eye movement sleep behavior disorder, sleep apnea), autonomic dysfunction (e.g., bladder disturbances, orthostatic hypotension, sweating), sensory symptoms (e.g., pain, visual and olfactory deficits, paresthesia) and gastrointestinal symptoms (e.g., constipation, nausea, dysphagia) that are associated with the degeneration of the dopaminergic and other neurotransmitter systems (Barone 2010; Bastide et al. 2015; Bohnen and Albin 2011; Huot et al. 2013; Schaeffer et al. 2014). Current treatment options focus on using dopamine replacement therapy to increase dopamine transmission and counterbalance the motor deficits caused by the degeneration of dopaminergic neurons. However, this strategy leads to various side effects such as motor fluctuations and the development of abnormal involuntary movements or L-dopa induced dyskinesias (LIDs). Given the limited available treatments for this increasingly prevalent disease, research continues to focus on uncovering the molecular defects in PD with the aim to develop novel targeted therapeutics.
Ninety percent of PD cases are of sporadic nature, with risk factors such as age, drug abuse, and gene-environment interactions known to contribute to this form of PD (Blesa and Przedborski 2014; Hirsch et al. 2013; Terzioglu and Galter 2008; Valadas et al. 2015). The remaining 10 % of PD cases are familial forms linked to genetic mutations (Blesa and Przedborski 2014; Hirsch et al. 2013; Terzioglu and Galter 2008; Valadas et al. 2015). Interestingly, genome wide association studies have now shown that some of the genes associated to familial forms of PD may also be risk factors for sporadic forms of the disease (Lesage and Brice 2009). These findings together with the strong resemblance between familial and sporadic PD cases suggest that the affected pathways may be similar or overlapping. For many decades, the pathological focus of PD research had been on the neurodegeneration of the nigrostriatal dopaminergic pathway which most likely underlies the motor symptoms of the disease. However, PD is a heterogeneous disease that affects multiple neurotransmitter systems and various brain circuits that contribute to the motor and non-motor symptoms experienced by patients (Barone 2010; Bastide et al. 2015; Huot et al. 2013). In fact, a role for the serotonergic, noradrenergic, glutamatergic, GABAergic, and cholinergic systems has been identified over the last decade. The focus of this review will be on the nicotinic cholinergic system as it is well known to interact and modulate multiple neurotransmitter systems in the basal ganglia.
Role of the Nicotinic Cholinergic System in Parkinson’s Disease
Normal function of the basal ganglia is dependent on the equilibrium reached between the midbrain dopaminergic and striatal cholinergic systems (Lim et al. 2014). Cholinergic interneurons comprise 1–2 % of striatal neurons and they constitute the main source of acetylcholine in this brain region (Bohnen and Albin 2011; Lenz and Lobo 2013; Zhou et al. 2001). Multiple studies have shown that acetylcholine regulates striatal DA release via an interaction at various nicotinic receptors (nAChRs) (Exley and Cragg 2008; Perez et al. 2010; Quik and Wonnacott 2011; Rice and Cragg 2004; Zhang and Sulzer 2004; Zhou et al. 2001). These receptors are pentameric ligand-gated ion channels of which there are multiple subtypes comprised of either α subunits or a combination of α and β subunits (Albuquerque et al. 2009; Millar and Gotti 2009; Quik and Wonnacott 2011). Extensive studies have shown that the main nAChRs functionally active in the nigrostriatal pathway are the β2* nAChRs which include the α6β2* and α4β2* receptor subtypes (the asterisks indicate the possible presence of other nAChR subunits in the receptor complex), with a minor population of the α7 nAChR subtype (Champtiaux et al. 2003; Quik and Wonnacott 2011). α6β2* nAChRs are highly localized to dopaminergic neurons and terminals while α4β2* nAChRs are abundantly expressed in DA neurons and terminals, GABAergic interneurons and medium spiny neurons as well as afferents. By contrast, nigrostriatal α7 nAChRs are thought to be primarily expressed on glutamatergic terminals. Additionally, α4β2* and α7 nAChRs are widely expressed in other neuronal circuits and connections of the basal ganglia such as the cortex and thalamic regions where they regulate GABA and glutamate transmission, respectively, to ultimately influence nigrostriatal dopaminergic transmission. Given this ability of nAChRs to regulate basal ganglia function and motor control, preclinical studies using available animal models have been carried out to elucidate the role of these receptors on diseases such as PD.
Thus far, the two most commonly used animal models to study the involvement of the nicotinic cholinergic system in PD are the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) and 6-hydroxydopamine (6-OHDA) rodent and primate models (Table 1). Both of these models are typically used to simulate the robust degeneration of the nigrostriatal pathway and subsequent motor deficits that occur in PD. MPTP is widely used in mice and primates via various treatment regimens or administration methods that can lead to acute nigrostriatal lesions or relatively gradual dopaminergic losses. In mice and primates, MPTP intoxication leads to a greater DA loss in the dorsal regions than the ventral regions of the striatum similar to that observed in the human condition. In addition, although there is a lack of Lewy body (LB) pathology in this model, studies investigating α-synuclein expression after MPTP exposure show intraneuronal inclusions reminiscent of LBs in monkeys (Forno et al. 1986; Kowall et al. 2000) but not in mice (Alvarez-Fischer et al. 2008; Shimoji et al. 2005). Behaviorally, MPTP-treated monkeys show features analogous to those observed with PD that are lacking in mice. Yet, motor alterations in mice may be detected using a battery of tests (Fleming and Chesselet 2006; Taylor et al. 2010). A number of non-motor symptoms such as cognitive impairments and sleep disturbances have also been reported in primates but not mice (Fox and Brotchie 2010; Johnston and Fox 2015; Porras et al. 2012).
6-OHDA is a selective catecholaminergic neurotoxin that is used to generate DAergic nigrostriatal lesions in rats and mice (Ungerstedt 1968). It is typically administered as a unilateral injection into the SNc, medial forebrain bundle or striatum as it does not cross the brain–blood barrier. Similar to the MPTP model, injection of 6-OHDA selectively and rapidly degenerates SNc DA neurons and striatal DA terminals (Faull and Laverty 1969; Javoy et al. 1976; Przedborski et al. 1995; Sarre et al. 2004; Ungerstedt 1968). Behavioral assessments of motor impairments in the unilateral 6-OHDA model have been done using drug-induced rotation tests (amphetamines or DA agonist) (Dunnett and Lelos 2010). However, such assays may not be that reliable for preclinical drug testing and drug-free motor tests have now been developed (Schallert et al. 2000). With respect to the non-motor aspects of PD, studies have now shown that the rodent 6-OHDA models also present with cognitive, psychiatric and gastro-intestinal deficits relevant to PD (Campos et al. 2013; Carvalho et al. 2013; Darvas et al. 2014; De Leonibus et al. 2007; Tieu 2011).
In the remainder of this review, we will discuss studies using MPTP-treated mice or primates as well as 6-OHDA-lesioned mice or rats to determine how the nicotinic cholinergic system is affected with nigrostriatal damage and how nAChR targeted drugs may be promising therapeutics for PD management.
Alterations in nAChR-Mediated Function Contribute to Changes in Dopaminergic Transmission in PD Models
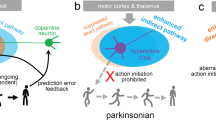
Under normal physiological conditions, activation of nAChRs promotes striatal DA release as these receptors are strategically expressed on DA neurons and terminals as well as GABAergic and glutamatergic neurons and terminals within the basal ganglia circuitry (Quik and Wonnacott 2011; Quik et al. 2015). Nigrostriatal damage alters nAChR expression and their contribution to the release process (Fig. 1). Receptor studies show decreases in α4β2* and α6β2* nAChRs in MPTP- and 6-OHDA-lesioned animals, with nigrostriatal damage having a greater effect on the α6β2* nAChR subtype (Bordia et al. 2007; Perez et al. 2010; Quik et al. 2003). Further studies using striatal synaptosomal preparations and tissue slices from lesioned animals also revealed a decline in DA release mediated via these receptor subtypes (McCallum et al. 2006; Perez et al. 2008, 2010; Quik et al. 2006a; Quik and Wonnacott 2011). In contrast, although no alterations in α7 receptor expression or its mediation of striatal DA release have been found thus far, the dense expression of this receptor subtype in neuronal circuits that regulate striatal function suggests their involvement in PD (Quik et al. 2015).
Schematic of the changes in striatal nAChR expression observed with nigrostriatal damage. Under physiological conditions, α6β2* nAChRs are highly localized to dopaminergic terminals while α4β2* nAChRs are abundantly expressed in DA neurons and terminals, GABAergic interneurons and medium spiny neurons as well as afferents. Striatal α7 nAChRs are thought to be primarily expressed on glutamatergic terminals and further influence nigrostriatal dopaminergic transmission. Nigrostriatal damage leads to a selective loss of dopaminergic terminals and a consequent decrease in striatal dopamine release. This dopaminergic loss is associated with parallel decreases in α6β2* nAChR expression and its influence on DA release. Albeit to a much lesser extent, α4β2* nAChR expression and function is also significantly decreased with nigrostriatal damage. Thus, declines in α6β2* and α4β2* nAChR-mediated dopamine release contribute to the overall dampening in striatal dopaminergic tone observed with DA neuron degeneration. In contrast, although there is enhanced glutamatergic tone after nigrostriatal damage, striatal α7 nAChR expression and function has not been reported to be affected
Additionally, work using cyclic voltammetry in striatal slices has shown that the control exerted by α4β2* and α6β2* nAChRs on DA release is dependent on DA neuron firing frequency (Exley and Cragg 2008; Perez et al. 2010; Perez and Quik 2011; Rice and Cragg 2004; Zhang and Sulzer 2004; Zhou et al. 2001). Interestingly, studies in 6-OHDA lesioned rodents show a dysregulation of DA release after nigrostriatal damage such that release is less sensitive to DA neuron activity (Jennings et al. 2015; Perez et al. 2010). Importantly, these impairments in DA release appear to be exacerbated by a loss of nAChR activation suggesting that nAChR drugs may ameliorate the dopaminergic imbalance observed in PD and may thus be useful therapeutic targets.
Protective Effect of nAChR Drugs Against Neuronal Damage In Vitro and In Vivo
A main focus of PD research has been on identifying molecular targets that could help develop novel drugs that not only treat PD symptoms but also potentially reverse or halt its progression (Kalia et al. 2015). The initial rationale for testing the ability of nAChR drugs as PD therapies emerged from epidemiological studies showing an inverse relationship between smoking and PD incidence (Hernan et al. 2001; Morens et al. 1995; Posadas et al. 2013; Quik 2004; Quik et al. 2014; Tanner 2010). These reports showed that the decrease in Parkinson’s disease incidence correlated with the number of cigarettes consumed and years of smoking (Elbaz and Moisan 2008; Noyce et al. 2012; Searles Nielsen et al. 2012; Tanner 2010; Wirdefeldt et al. 2011). Remarkably, this reduced risk was lost with smoking cessation (Noyce et al. 2012). In addition, other forms of tobacco use also decreased the incidence of Parkinson’s disease (Ritz et al. 2007). Importantly, the inverse correlation between Parkinson’s disease and tobacco use was not due to a selective mortality (Elbaz and Moisan 2008; Noyce et al. 2012; Searles Nielsen et al. 2012; Tanner 2010; Wirdefeldt et al. 2011). These collected findings together with the known ability of nAChRs to regulate nigrostriatal dopaminergic function led researchers to explore nicotine’s potential as a neuroprotective agent.
In vitro and in vivo studies with selective nAChR subtype drugs as well as genetically modified mice, rats and primates have now shown that nicotine protects against neuronal damage induced by 6-OHDA, MPTP, rotenone, paraquat, methamphetamine, glutamate, and β-amyloid via an interaction at β2* and α7 nAChRs (Akaike et al. 1994; Bordia et al. 2015b; Cormier et al. 2003; Huang et al. 2009; Khwaja et al. 2007; Quik et al. 2006a, 2007b; Riveles et al. 2008; Ryan et al. 2001; Serriere et al. 2015; Shimohama et al. 1996; Takeuchi et al. 2009; Vieira-Brock et al. 2015) (Table 2). Activation of these nAChR subtypes activates the ERK/MAPK, PI3K/AKT and JAK2/STAT3 pathways (Quik and Wonnacott 2011; Shimohama 2009). This activation can occur via calcium dependent and independent mechanisms that lead to decreased transcription of pro-inflammatory cytokines such as NF-kB and enhanced activity of cell survival proteins (Bcl-2, Bcl-x) that obstruct the neurodegenerative process. Thus, it is now well accepted that not only nicotine but also subtype specific nAChR drugs protect against neurotoxic insults. However, studies in rodents and primates have now shown that although nicotine can protect against ongoing neuronal damage, it cannot restore neuronal integrity/function once damaged has occurred (Huang et al. 2009). Therefore, nAChR drugs could be of most value when given during the early stages of the disease to slow down its progression. In fact, a phase 2 clinical trial (NCT01560754) is currently underway to assess the disease-modifying potential of nicotine in early PD patients. This is important as being able to slow down the progression of the disease could significantly improve a patient’s prognosis.
Effect of nAChR Drugs on the Motor Deficits Related to PD
In addition to the potential of nAChR drugs to protect against nigrostriatal damage, it was important to establish whether they could also be beneficial to treat the motor symptoms associated with PD. Preclinical studies show that treatment with nicotine or other nAChR drugs improves motor deficits in parkinsonian mice, rats and monkeys in some studies (Kucinski et al. 2013; Meshul et al. 2002) but not others (Bordia et al. 2008; Huang et al. 2011b; Quik et al. 2007a; Zhang et al. 2013, 2014a). Similar inconsistencies have been reported in clinical trials which tested the acute or immediate effect of nicotine or a nAChR agonist on Parkinson’s disease motor function. Open label trials have reported an improvement in parkinsonism with smoking, intravenous nicotine infusions, the nicotine patch and the nicotine gum (Hanagasi et al. 2007; Ishikawa and Miyatake 1993; Kelton et al. 2000; Mitsuoka et al. 2002; Villafane et al. 2007), with the exception of one trial (Lemay et al. 2004). By contrast, the opposite trend has been observed in double-blinded studies in which only one study has reported a positive effect of nicotine on motor deficits (Clemens et al. 1995; Ebersbach et al. 1999; Fagerstrom et al. 1994; Parkinson Study 2006; Vieregge et al. 2001). Thus, it is still unclear whether nicotinic drugs could be of benefit for the treatment of PD motor symptoms.
nAChR Drugs for the Treatment of the Non-Motor Symptoms of PD
The non-motor symptoms associated with PD likely result from neurodegeneration of multiple neuronal systems that lead to neurotransmitter deficits extending beyond the declines in nigrostriatal DA. Alterations in cholinergic neurotransmission with PD are thought to be a contributing factor to non-motor symptoms such as cognitive impairment including dementia, depression and/or apathy, sleep abnormalities, and olfactory deficiencies (Barone 2010; Bohnen and Albin 2011; Muller and Bohnen 2013; Posadas et al. 2013). As nAChRs are widely expressed in brain regions involved in these physiological processes, nicotine and/or other nAChR drugs may be useful to treat some of the non-motor symptoms associated with PD (Albuquerque et al. 2009; Dineley et al. 2015; Hurst et al. 2013; Quik et al. 2014).
Preclinical and clinical studies have shown that nicotine and nAChR drugs improve cognitive performance in a variety of disease conditions such as Alzheimer’s disease and neuropsychiatric disorders (Bitner et al. 2010; Cincotta et al. 2008; Geerts 2012; Hambsch et al. 2014; Jubelt et al. 2008; Lombardo and Maskos 2015; Wallace et al. 2011; Wallace and Porter 2011). In preclinical Alzheimer’s disease models, nicotinic drugs have improved cognition in a delay matching to sample task in monkeys, social recognition in rats and two-trial inhibitory avoidance in mice (Bitner et al. 2010). In addition, these drugs have restored impaired pre-pulse inhibition, working memory, episodic memory and social recognition in rodent models of schizophrenia (Hambsch et al. 2014; Jubelt et al. 2008). Positive effects with nAChR drugs have also been observed in humans. The general nicotinic agonist varenicline improved performance in the Digital Symbol Substitution Test, the Wisconsin Card Substitution Test as well as the Cognition Performance Test hit reaction time and Stroop Interference in patients with Schizophrenia (Shim et al. 2012). In addition, varenicline also improved performance in a stop signal task assessing lapses in attention in treatment-seeking smokers (Rhodes et al. 2012). Similarly, the β2* selective nAChR agonist TC-1734 improved age-associated memory impairment in a randomized placebo-controlled double-blinded study using a Cognitive Drug Research computerized test battery and a Subject Global Impression Scale of Cognition (SCI-Cog) test (Dunbar et al. 2011).
Of relevance to PD, preclinical studies in MPTP-treated primates have shown that nicotine and nAChR agonists are able to alleviate cognitive deficits in executive function, visuospatial function and attention (Bohnen et al. 2012, 2013; Decamp and Schneider 2009). Clinical studies also showed that nicotine can improve semantic processing in PD patients under general and strategy-based priming procedures (Holmes et al. 2011a, b). Thus, the therapeutic effects of nAChR drugs may extend beyond their use to prevent PD progression.
Role for the Cholinergic System in the Management of LIDs
An additional motor complication commonly observed in PD patients arises from the use of the DA precursor L-dopa, which is the main therapeutic agent used to treat the motor deficits associated with the disease. L-dopa has been used as a therapy for PD since the early 1960’s as it enhances synaptic DA transmission to alleviate the dopaminergic deficit that arises with nigrostriatal damage. Although it still remains the most effective treatment for the motor symptoms of PD, long-term L-dopa use is complicated by the development of fluctuations in motor response (Quinn et al. 1982; Quinn 1998). This side effect includes unpredictable changes in mobility, a decrease in the duration of L-dopa action and LIDs (Bastide et al. 2015; Heumann et al. 2014; Huot et al. 2013). LIDs are abnormal involuntary movements that develop in the majority of patients within the first decade of treatment and can be very debilitating (Ahlskog and Muenter 2001; Huot et al. 2013; Schaeffer et al. 2014). To date, amantadine and deep brain stimulation are the only two approved therapies for the management of LIDs (Brotchie 2010; Heumann et al. 2014; Merola et al. 2014; Rizzone et al. 2014; Schaeffer et al. 2014; Tambasco et al. 2012). Although effective, both of these approaches have their associated complications that limit their usefulness. Thus, there is still a need to develop novel and efficient anti-dyskinetic tools. To achieve this, preclinical studies in rodent and primate models of LIDs have been widely used to broaden our understanding of the pathophysiology related to LIDs, identify promising molecular targets, and facilitate preclinical testing of novel therapeutics.
The most commonly used animal model to study LIDs was developed by Cenci and coworkers (Cenci and Lundblad 2007; Lundblad et al. 2002, 2005). Initial work showed that prolonged administration of L-dopa to 6-OHDA-lesioned rodents leads to abnormal involuntary movements (AIMs) that resemble human LIDs in their topographical distribution and time course. These AIMs consists of twisting movements of the neck and trunk toward the side contralateral to the lesion (axial AIMs), purposeless jaw movements with or without contralateral tongue protrusion (oral AIMs) and purposeless tapping or movement of the forelimb contralateral to the lesion side (forelimb AIMs) (Bastide et al. 2015; Breger et al. 2013; Cenci and Lundblad 2007; Cenci et al. 2002; Francardo et al. 2011; Lundblad et al. 2002, 2005; Winkler et al. 2002). Enhanced circular locomotion with a contralateral side bias (locomotive AIMs) is also observed with L-dopa administration. However, the clinical relevance of this latter AIM subtype is limited by the fact that numerous other drugs that do not lead to LIDs also enhance contralateral rotations in unilaterally-lesioned rodents (Lundblad et al. 2002). In general, the severity of AIMs is rated based on the proportion of time during which these behaviors are observed. It is also useful to include an amplitude score for each AIM category to enable comparison between animals with a wide range of DA denervation (Cenci and Lundblad 2007; Winkler et al. 2002).
Chronic L-dopa treatment to MPTP-treated primates results in dyskinetic movements that are remarkably analogous to those observed in humans. Rating scales to evaluate LIDs severity in primates include the abnormal involuntary movement scale (AIMS), the dyskinesia disability scale for MTPT-treated primates, the monkey quality of ON-time rating, the global non-human primate dyskinesia rating scale, the quantitative dyskinesia scale and the St. Kitts biomedical primate dyskinesia scale (Boraud et al. 2001; Boyce et al. 1990; Gomez-Mancilla and Bedard 1993; Henry et al. 1999; Johnston et al. 2010; Johnston and Fox 2015; Pearce et al. 1995; Petzinger et al. 2001; Potts et al. 2015; Tan et al. 2002). These scales take into account choreic and dystonic movements of the limbs, trunk or neck as well as repetitive purposeless movements not observed in the absence of L-dopa. The clinical relevance of these scales has been recently reviewed and revised by Fox and colleges in an attempt to establish a standardized rating scale with clinical applicability that can be used for translational basic research (Fox et al. 2012).
In general, rodent and primate models have been instrumental to our understanding of the mechanisms and neural circuits involved in LIDs as well as for testing of numerous therapeutic drug candidates (for review see (Bastide et al. 2015). We will focus on preclinical studies highlighting the ability of nAChR drugs to decrease LIDs in rodent and primate models.
Non Selective nAChR Drugs Decrease LIDs in Animal Models
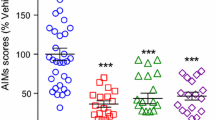
Alterations in the nicotinic cholinergic system have also been implicated in the pathological events leading to LIDs (Bastide et al. 2015; Huot et al. 2013; Schaeffer et al. 2014). The first evidence for this came from studies showing that nicotine decreased LIDs by ~50 % in a small cohort of MPTP-treated primates (Quik et al. 2007a). Additional studies in mice, rats and primates have since shown that route of administration and treatment regimen (pre- vs post-treatment) do not affect nicotine’s antidyskinetic effect (Bordia et al. 2008; Huang et al. 2011b; Quik et al. 2013c, d) (Table 3). Experiments with the non-specific nAChR agonist varenicline as well as with the general nAChR blocker mecamylamine have yielded similar results (Bordia et al. 2010; Huang et al. 2011a) (Table 3). Thus, it appears that nAChR agonists may exert their antidyskinetic effect via a receptor desensitization block as agonists and antagonists yield similar results. Altogether, these observations indicate that nicotinic drugs not only interfere with LIDs development but also reduce existing LIDs. In fact, a small phase I/II clinical trial with nicotine by Neuraltus Inc. has demonstrated the potential of nicotinic drugs to reduce dyskinesias in PD patients with LIDs (http://www.prnewswire.com/news-releases/).
β2* and α7 nAChR-Selective Drugs Decrease LIDs in Animal Models
As non-selective nAChR drugs interact with multiple nAChR subtypes in the peripheral and central nervous system, basic research in the last few years has focused on identifying the specific nAChRs involved in their antidyskinetic effect. Studies in 6-OHDA-lesioned genetically modified mice have shown that nicotine reduces LIDs via β2* and α7 nAChRs. Specifically, it appears that β2* nAChRs are required for the appearance of LIDs as well as for the antidyskinetic effect of nicotine, with the relevant receptors being the α4β2* and α6β2* nAChR subtypes (Bordia et al. 2015a; Huang et al. 2011b; Quik et al. 2012). By contrast, studies with α7 nAChR null mice show that these receptors partly suppress the occurrence of LIDs and are also involved in the mechanism of action through which nicotine decreases LIDs (Quik et al. 2013b). Altogether, these findings suggested that nAChR subtype selective drugs may be beneficial therapeutic agents for LIDs management.
Initial studies to determine the usefulness of nAChR drugs focused on β2* nAChRs as these are the main subtype expressed in the nigrostriatal pathway. β2* nAChR agonists such as A-85380, sazetidine, TC-2696, TI-10165, TC-8831, TC-10600, ABT-089 and ABT-894 decreased LIDs incidence by 20–60 % in dyskinetic rats and primates (Bordia et al. 2013; Huang et al. 2011a; Johnston et al. 2013; Quik et al. 2013a, 2014, 2015; Zhang et al. 2013, 2014a) (Table 3). These drugs decreased LIDs in L-dopa naïve as well as L-dopa primed animals without worsening parkinsonism. Importantly, no tolerance developed with any of the doses tested. Thus, drugs targeting the β2* nAChR subtype alone appear to be a good therapeutic approach to decrease LIDs.
Nicotine also appears to exert its antidyskinetic effect via α7 nAChRs. Although this receptor subtype is not densely expressed in the basal ganglia, it is widely expressed on other neuronal circuits that regulate basal ganglia function (Quik et al. 2015). Therefore, studies were carried out in monkeys to test the ability of the α7 nAChR agonists AQW051, ABT-107 and ABT-126 to modulate LIDs expression (Di Paolo et al. 2014; Zhang et al. 2015a; Zhang et al. 2014b, 2015b). Interestingly, ABT-107 and ABT-126 decreased LIDs to the same extent as β2* nAChR agonists (Table 3). In addition, co-administration of α7 and β2* nAChR agonists did not increase the extent by which either type of drug alone decrease LIDs suggesting they exert their therapeutic effect through a common mechanism of action.
Altogether, preclinical evidence indicates that β2* and α7 nAChR agonists are similarly effective to alleviate LIDs. Thus, both classes of drugs may be promising antidyskinetic agents to test in the clinical setting.
Summary
PD is a complex disease with a multi-factorial etiology. Although none of the currently available preclinical models fully reproduce the human condition, they have provided a wealth of information regarding the molecular and cellular mechanism contributing to the disease. Preclinical studies on the complex interaction between various neurotransmitter systems in PD have identified nAChRs as plausible targets to not only delay disease progression but to alleviate the motor and non-motor symptoms (e.g., cognitive impairment, depression, anxiety) observed in PD. Thus, it may be of value to test nAChR drugs in clinical trials as therapies for PD management.
References
Abin-Carriquiry, J. A., McGregor-Armas, R., Costa, G., Urbanavicius, J., & Dajas, F. (2002). Presynaptic involvement in the nicotine prevention of the dopamine loss provoked by 6-OHDA administration in the substantia nigra. Neurotoxicity Research, 4(2), 133–139.
Ahlskog, J. E., & Muenter, M. D. (2001). Frequency of levodopa-related dyskinesias and motor fluctuations as estimated from the cumulative literature. Movement Disorders, 16(3), 448–458.
Akaike, A., Tamura, Y., Yokota, T., Shimohama, S., & Kimura, J. (1994). Nicotine-induced protection of cultured cortical neurons against N-methyl-D-aspartate receptor-mediated glutamate cytotoxicity. Brain Research, 644(2), 181–187.
Albuquerque, E. X., Pereira, E. F., Alkondon, M., & Rogers, S. W. (2009). Mammalian nicotinic acetylcholine receptors: from structure to function. Physiological Reviews, 89(1), 73–120.
Alvarez-Fischer, D., Guerreiro, S., Hunot, S., Saurini, F., Marien, M., Sokoloff, P., Hirsch, E. C., Hartmann, A., & Michel, P. P. (2008). Modelling Parkinson-like neurodegeneration via osmotic minipump delivery of MPTP and probenecid. Journal of Neurochemistry, 107(3), 701–711.
Barone, P. (2010). Neurotransmission in Parkinson’s disease: beyond dopamine. European Journal of Neurology, 17(3), 364–376.
Bastide, M. F., Meissner, W. G., Picconi, B., Fasano, S., Fernagut, P. O., Feyder, M., Francardo, V., Alcacer, C., Ding, Y., Brambilla, R., Fisone, G., Jon Stoessl, A., Bourdenx, M., Engeln, M., Navailles, S., De Deurwaerdere, P., Ko, W. K., Simola, N., Morelli, M., Groc, L., Rodriguez, M. C., Gurevich, E. V., Quik, M., Morari, M., Mellone, M., Gardoni, F., Tronci, E., Guehl, D., Tison, F., Crossman, A. R., Kang, U. J., Steece-Collier, K., Fox, S., Carta, M., Angela Cenci, M., & Bezard, E. (2015). Pathophysiology of L-dopa-induced motor and non-motor complications in Parkinson’s disease. Progress in Neurobiology, 132, 96–168.
Bertram, L., & Tanzi, R. E. (2005). The genetic epidemiology of neurodegenerative disease. Journal of Clinical Investigation, 115(6), 1449–1457.
Bitner, R. S., Bunnelle, W. H., Decker, M. W., Drescher, K. U., Kohlhaas, K. L., Markosyan, S., Marsh, K. C., Nikkel, A. L., Browman, K., Radek, R., Anderson, D. J., Buccafusco, J., & Gopalakrishnan, M. (2010). In vivo pharmacological characterization of a novel selective alpha7 neuronal nicotinic acetylcholine receptor agonist ABT-107: preclinical considerations in Alzheimer’s disease. Journal of Pharmacol and Experimental Therapeutics, 334(3), 875–886.
Blesa, J., & Przedborski, S. (2014). Parkinson’s disease: animal models and dopaminergic cell vulnerability. Frontiers in Neuroanatomy, 8, 155.
Bohnen, N. I., & Albin, R. L. (2011). The cholinergic system and Parkinson disease. Behavioural Brain Research, 221(2), 564–573.
Bohnen, N. I., Muller, M. L., Kotagal, V., Koeppe, R. A., Kilbourn, M. R., Gilman, S., Albin, R. L., & Frey, K. A. (2012). Heterogeneity of cholinergic denervation in Parkinson’s disease without dementia. Journal of Cerebral Blood Flow and Metabolism, 32(8), 1609–1617.
Bohnen, N. I., Frey, K. A., Studenski, S., Kotagal, V., Koeppe, R. A., Scott, P. J., Albin, R. L., & Muller, M. L. (2013). Gait speed in Parkinson disease correlates with cholinergic degeneration. Neurology, 81(18), 1611–1616.
Boraud, T., Bezard, E., Bioulac, B., & Gross, C. E. (2001). Dopamine agonist-induced dyskinesias are correlated to both firing pattern and frequency alterations of pallidal neurones in the MPTP-treated monkey. Brain, 124(Pt 3), 546–557.
Bordia T, Decker MW and Quik M Unpublished observation.
Bordia, T., Grady, S. R., McIntosh, J. M., & Quik, M. (2007). Nigrostriatal damage preferentially decreases a subpopulation of alpha6beta2* nAChRs in mouse, monkey, and Parkinson’s disease striatum. Molecular Pharmacology, 72(1), 52–61.
Bordia, T., Campos, C., Huang, L., & Quik, M. (2008). Continuous and intermittent nicotine treatment reduces L-3,4-dihydroxyphenylalanine (L-DOPA)-induced dyskinesias in a rat model of Parkinson’s disease. Journal of Pharmacol and Experimental Therapeutics, 327(1), 239–247.
Bordia, T., Campos, C., McIntosh, J. M., & Quik, M. (2010). Nicotinic receptor-mediated reduction in L-DOPA-induced dyskinesias may occur via desensitization. Journal of Pharmacol and Experimental Therapeutics, 333(3), 929–938.
Bordia, T., McIntosh, J. M., & Quik, M. (2013). The nicotine-mediated decline in l-dopa-induced dyskinesias is associated with a decrease in striatal dopamine release. Journal of Neurochemistry, 125(2), 291–302.
Bordia, T., McGregor, M., McIntosh, J. M., Drenan, R. M., & Quik, M. (2015a). Evidence for a role for alpha6(*) nAChRs in l-dopa-induced dyskinesias using Parkinsonian alpha6(*) nAChR gain-of-function mice. Neuroscience, 295, 187–197.
Bordia, T., McGregor, M., Papke, R. L., Decker, M. W., McIntosh, J. M., & Quik, M. (2015b). The alpha7 nicotinic receptor agonist ABT-107 protects against nigrostriatal damage in rats with unilateral 6-hydroxydopamine lesions. Experimental Neurology, 263, 277–284.
Boyce, S., Rupniak, N. M., Steventon, M. J., & Iversen, S. D. (1990). Characterisation of dyskinesias induced by L-dopa in MPTP-treated squirrel monkeys. Psychopharmacology, 102(1), 21–27.
Breger, L. S., Dunnett, S. B., & Lane, E. L. (2013). Comparison of rating scales used to evaluate L-DOPA-induced dyskinesia in the 6-OHDA lesioned rat. Neurobiology of Disease, 50, 142–150.
Brotchie, J. (2010). Antidyskinetic actions of amantadine in Parkinson’s disease: are benefits maintained in the long term? Expert Review of Neurotherapeutics, 10(6), 871–873.
Campos, F. L., Carvalho, M. M., Cristovao, A. C., Je, G., Baltazar, G., Salgado, A. J., Kim, Y. S., & Sousa, N. (2013). Rodent models of Parkinson’s disease: beyond the motor symptomatology. Frontiers in Behavioral Neuroscience, 7, 175.
Carvalho, M. M., Campos, F. L., Coimbra, B., Pego, J. M., Rodrigues, C., Lima, R., Rodrigues, A. J., Sousa, N., & Salgado, A. J. (2013). Behavioral characterization of the 6-hydroxidopamine model of Parkinson’s disease and pharmacological rescuing of non-motor deficits. Molecular Neurodegeneration, 8, 14.
Cenci, M.A. & Lundblad, M. (2007). Ratings of L-DOPA-induced dyskinesia in the unilateral 6-OHDA lesion model of Parkinson’s disease in rats and mice. Current Protocols in Neuroscience Chapter 9: Unit 9 25.
Cenci, M. A., Whishaw, I. Q., & Schallert, T. (2002). Animal models of neurological deficits: how relevant is the rat? Nature Reviews Neuroscience, 3(7), 574–579.
Champtiaux, N., Gotti, C., Cordero-Erausquin, M., David, D. J., Przybylski, C., Lena, C., Clementi, F., Moretti, M., Rossi, F. M., Le Novere, N., McIntosh, J. M., Gardier, A. M., & Changeux, J. P. (2003). Subunit composition of functional nicotinic receptors in dopaminergic neurons investigated with knock-out mice. Journal of Neuroscience, 23(21), 7820–7829.
Cincotta, S. L., Yorek, M. S., Moschak, T. M., Lewis, S. R., & Rodefer, J. S. (2008). Selective nicotinic acetylcholine receptor agonists: potential therapies for neuropsychiatric disorders with cognitive dysfunction. Current Opinion in Investigational Drugs, 9(1), 47–56.
Clemens, P., Baron, J. A., Coffey, D., & Reeves, A. (1995). The short-term effect of nicotine chewing gum in patients with Parkinson’s disease. Psychopharmacology, 117(2), 253–256.
Cormier, A., Morin, C., Zini, R., Tillement, J. P., & Lagrue, G. (2003). Nicotine protects rat brain mitochondria against experimental injuries. Neuropharmacology, 44(5), 642–652.
Costa, G., Abin-Carriquiry, J. A., & Dajas, F. (2001). Nicotine prevents striatal dopamine loss produced by 6-hydroxydopamine lesion in the substantia nigra. Brain Research, 888(2), 336–342.
Darvas, M., Henschen, C. W., & Palmiter, R. D. (2014). Contributions of signaling by dopamine neurons in dorsal striatum to cognitive behaviors corresponding to those observed in Parkinson’s disease. Neurobiology of Disease, 65, 112–123.
De Leonibus, E., Pascucci, T., Lopez, S., Oliverio, A., Amalric, M., & Mele, A. (2007). Spatial deficits in a mouse model of Parkinson disease. Psychopharmacology, 194(4), 517–525.
Decamp, E., & Schneider, J. S. (2009). Interaction between nicotinic and dopaminergic therapies on cognition in a chronic Parkinson model. Brain Research, 1262, 109–114.
Di Monte, D. A., McCormack, A., Petzinger, G., Janson, A. M., Quik, M., & Langston, W. J. (2000). Relationship among nigrostriatal denervation, parkinsonism, and dyskinesias in the MPTP primate model. Movement Disorders, 15(3), 459–466.
Di Paolo, T., Gregoire, L., Feuerbach, D., Elbast, W., Weiss, M., & Gomez-Mancilla, B. (2014). AQW051, a novel and selective nicotinic acetylcholine receptor alpha7 partial agonist, reduces l-Dopa-induced dyskinesias and extends the duration of l-Dopa effects in parkinsonian monkeys. Parkinsonism & Related Disorders, 20(11), 1119–1123.
Dineley, K. T., Pandya, A. A., & Yakel, J. L. (2015). Nicotinic ACh receptors as therapeutic targets in CNS disorders. Trends in Pharmacological Sciences, 36(2), 96–108.
Dunbar, G. C., Kuchibhatla, R. V., Lee, G., & Group T-ACS. (2011). A randomized double-blind study comparing 25 and 50 mg TC-1734 (AZD3480) with placebo, in older subjects with age-associated memory impairment. Journal of Psychopharmacology, 25(8), 1020–1029.
Dunnett, S. B., & Lelos, M. (2010). Behavioral analysis of motor and non-motor symptoms in rodent models of Parkinson’s disease. Progress in Brain Research, 184, 35–51.
Ebersbach, G., Stock, M., Muller, J., Wenning, G., Wissel, J., & Poewe, W. (1999). Worsening of motor performance in patients with Parkinson’s disease following transdermal nicotine administration. Movement Disorders, 14(6), 1011–1013.
Elbaz, A., & Moisan, F. (2008). Update in the epidemiology of Parkinson’s disease. Current Opinion in Neurology, 21(4), 454–460.
Exley, R., & Cragg, S. J. (2008). Presynaptic nicotinic receptors: a dynamic and diverse cholinergic filter of striatal dopamine neurotransmission. British Journal of Pharmacology, 153(Suppl 1), S283–S297.
Fagerstrom, K. O., Pomerleau, O., Giordani, B., & Stelson, F. (1994). Nicotine may relieve symptoms of Parkinson’s disease. Psychopharmacology, 116(1), 117–119.
Faull, R. L., & Laverty, R. (1969). Changes in dopamine levels in the corpus striatum following lesions in the substantia nigra. Experimental Neurology, 23(3), 332–340.
Fleming, S. M., & Chesselet, M. F. (2006). Behavioral phenotypes and pharmacology in genetic mouse models of Parkinsonism. Behavioral Pharmacology, 17(5–6), 383–391.
Forno, L. S., Langston, J. W., DeLanney, L. E., Irwin, I., & Ricaurte, G. A. (1986). Locus ceruleus lesions and eosinophilic inclusions in MPTP-treated monkeys. Annals of Neurology, 20(4), 449–455.
Fox, S. H., & Brotchie, J. M. (2010). The MPTP-lesioned non-human primate models of Parkinson’s disease. Past, present, and future. Progress in Brain Research, 184, 133–157.
Fox, S. H., Johnston, T. H., Li, Q., Brotchie, J., & Bezard, E. (2012). A critique of available scales and presentation of the Non-Human Primate Dyskinesia Rating Scale. Movement Disorders, 27(11), 1373–1378.
Francardo, V., Recchia, A., Popovic, N., Andersson, D., Nissbrandt, H., & Cenci, M. A. (2011). Impact of the lesion procedure on the profiles of motor impairment and molecular responsiveness to L-DOPA in the 6-hydroxydopamine mouse model of Parkinson’s disease. Neurobiology of Disease, 42(3), 327–340.
Gao, Z. G., Cui, W. Y., Zhang, H. T., & Liu, C. G. (1998). Effects of nicotine on 1-methyl-4-phenyl-1,2,5,6-tetrahydropyridine-induced depression of striatal dopamine content and spontaneous locomotor activity in C57 black mice. Pharmacological Research, 38(2), 101–106.
Geerts, H. (2012). alpha7 Nicotinic receptor modulators for cognitive deficits in schizophrenia and Alzheimer’s disease. Expert Opinion on Investigational Drugs, 21(1), 59–65.
Gomez-Mancilla, B., & Bedard, P. J. (1993). Effect of nondopaminergic drugs on L-dopa-induced dyskinesias in MPTP-treated monkeys. Clinical Neuropharmacology, 16(5), 418–427.
Hambsch, B., Keyworth, H., Lind, J., Otte, D. M., Racz, I., Kitchen, I., Bailey, A., & Zimmer, A. (2014). Chronic nicotine improves short-term memory selectively in a G72 mouse model of schizophrenia. British Journal of Pharmacology, 171(7), 1758–1771.
Hanagasi, H. A., Lees, A., Johnson, J. O., Singleton, A., & Emre, M. (2007). Smoking-responsive juvenile-onset Parkinsonism. Movement Disorders, 22(1), 115–119.
Henry, B., Fox, S. H., Peggs, D., Crossman, A. R., & Brotchie, J. M. (1999). The alpha2-adrenergic receptor antagonist idazoxan reduces dyskinesia and enhances anti-parkinsonian actions of L-dopa in the MPTP-lesioned primate model of Parkinson’s disease. Movement Disorders, 14(5), 744–753.
Hernan, M. A., Zhang, S. M., Rueda-deCastro, A. M., Colditz, G. A., Speizer, F. E., & Ascherio, A. (2001). Cigarette smoking and the incidence of Parkinson’s disease in two prospective studies. Annals of Neurology, 50(6), 780–786.
Heumann, R., Moratalla, R., Herrero, M. T., Chakrabarty, K., Drucker-Colin, R., Garcia-Montes, J. R., Simola, N., & Morelli, M. (2014). Dyskinesia in Parkinson’s disease: mechanisms and current non-pharmacological interventions. Journal of Neurochemistry, 130(4), 472–489.
Hirsch, E. C., Jenner, P., & Przedborski, S. (2013). Pathogenesis of Parkinson’s disease. Movement Disorders, 28(1), 24–30.
Holmes, A. D., Copland, D. A., Silburn, P. A., & Chenery, H. J. (2011a). Acute nicotine enhances strategy-based semantic processing in Parkinson’s disease. International Journal of Neuropsychopharmacology, 14(7), 877–885.
Holmes, A. D., Copland, D. A., Silburn, P. A., & Chenery, H. J. (2011b). Nicotine effects on general semantic priming in Parkinson’s disease. Experimental and Clinical Psychopharmacology, 19(3), 215–223.
Huang, L. Z., Parameswaran, N., Bordia, T., Michael McIntosh, J., & Quik, M. (2009). Nicotine is neuroprotective when administered before but not after nigrostriatal damage in rats and monkeys. Journal of Neurochemistry, 109(3), 826–837.
Huang, L. Z., Campos, C., Ly, J., Ivy Carroll, F., & Quik, M. (2011a). Nicotinic receptor agonists decrease L-dopa-induced dyskinesias most effectively in partially lesioned parkinsonian rats. Neuropharmacology, 60(6), 861–868.
Huang, L. Z., Grady, S. R., & Quik, M. (2011b). Nicotine reduces L-DOPA-induced dyskinesias by acting at beta2* nicotinic receptors. Journal of Pharmacol and Experimental Therapeutics, 338(3), 932–941.
Huot, P., Johnston, T. H., Koprich, J. B., Fox, S. H., & Brotchie, J. M. (2013). The pharmacology of L-DOPA-induced dyskinesia in Parkinson’s disease. Pharmacological Reviews, 65(1), 171–222.
Hurst, R., Rollema, H., & Bertrand, D. (2013). Nicotinic acetylcholine receptors: from basic science to therapeutics. Pharmacology and Therapeutics, 137(1), 22–54.
Ishikawa, A., & Miyatake, T. (1993). Effects of smoking in patients with early-onset Parkinson’s disease. Journal of Neurological Sciences, 117(1–2), 28–32.
Janson, A. M., Meana, J. J., Goiny, M., & Herrera-Marschitz, M. (1991). Chronic nicotine treatment counteracts the decrease in extracellular neostriatal dopamine induced by a unilateral transection at the mesodiencephalic junction in rats: a microdialysis study. Neuroscience Letters, 134(1), 88–92.
Janson, A. M., Fuxe, K., & Goldstein, M. (1992). Differential effects of acute and chronic nicotine treatment on MPTP-(1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine) induced degeneration of nigrostriatal dopamine neurons in the black mouse. The Clinical Investigator, 70(3–4), 232–238.
Javoy, F., Sotelo, C., Herbet, A., & Agid, Y. (1976). Specificity of dopaminergic neuronal degeneration induced by intracerebral injection of 6-hydroxydopamine in the nigrostriatal dopamine system. Brain Research, 102(2), 201–215.
Jennings, K. A., Platt, N. J., & Cragg, S. J. (2015). The impact of a parkinsonian lesion on dynamic striatal dopamine transmission depends on nicotinic receptor activation. Neurobiology of Disease, 82, 262–268.
Johnston, T. M., & Fox, S. H. (2015). Symptomatic Models of Parkinson’s Disease and L-DOPA-Induced Dyskinesia in Non-human Primates. Current Topics in Behavioral Neurosciences, 22, 221–235.
Johnston, T. H., Fox, S. H., Piggott, M. J., Savola, J. M., & Brotchie, J. M. (2010). The alpha(2) adrenergic antagonist fipamezole improves quality of levodopa action in Parkinsonian primates. Movement Disorders, 25(13), 2084–2093.
Johnston, T. H., Huot, P., Fox, S. H., Koprich, J. B., Szeliga, K. T., James, J. W., Graef, J. D., Letchworth, S. R., Jordan, K. G., Hill, M. P., & Brotchie, J. M. (2013). TC-8831, a nicotinic acetylcholine receptor agonist, reduces L-DOPA-induced dyskinesia in the MPTP macaque. Neuropharmacology, 73, 337–347.
Jubelt, L. E., Barr, R. S., Goff, D. C., Logvinenko, T., Weiss, A. P., & Evins, A. E. (2008). Effects of transdermal nicotine on episodic memory in non-smokers with and without schizophrenia. Psychopharmacology, 199(1), 89–98.
Kalia, L. V., Kalia, S. K., & Lang, A. E. (2015). Disease-modifying strategies for Parkinson’s disease. Movement Disorders, 30(11), 1442–1450.
Kelton, M. C., Kahn, H. J., Conrath, C. L., & Newhouse, P. A. (2000). The effects of nicotine on Parkinson’s disease. Brain and Cognition, 43(1–3), 274–282.
Khwaja, M., McCormack, A., McIntosh, J. M., Di Monte, D. A., & Quik, M. (2007). Nicotine partially protects against paraquat-induced nigrostriatal damage in mice; link to alpha6beta2* nAChRs. Journal of Neurochemistry, 100(1), 180–190.
Kowall, N. W., Hantraye, P., Brouillet, E., Beal, M. F., McKee, A. C., & Ferrante, R. J. (2000). MPTP induces alpha-synuclein aggregation in the substantia nigra of baboons. Neuroreport, 11(1), 211–213.
Kucinski, A., Wersinger, S., Stachowiak, E. K., Corso, T. D., Parry, M. J., Zhang, J., Jordan, K., Letchworth, S., Bencherif, M., & Stachowiak, M. K. (2013). Neuronal nicotinic receptor agonists ameliorate spontaneous motor asymmetries and motor discoordination in a unilateral mouse model of Parkinson’s disease. Pharmacology, Biochemistry and Behavior, 111, 1–10.
Lemay, S., Chouinard, S., Blanchet, P., Masson, H., Soland, V., Beuter, A., & Bedard, M. A. (2004). Lack of efficacy of a nicotine transdermal treatment on motor and cognitive deficits in Parkinson’s disease. Progress in Neuropsychopharmacology and Biological Psychiatry, 28(1), 31–39.
Lenz, J. D., & Lobo, M. K. (2013). Optogenetic insights into striatal function and behavior. Behavioural Brain Research, 255, 44–54.
Lesage, S., & Brice, A. (2009). Parkinson’s disease: from monogenic forms to genetic susceptibility factors. Human Molecular Genetics, 18(R1), R48–R59.
Lim, S. A., Kang, U. J., & McGehee, D. S. (2014). Striatal cholinergic interneuron regulation and circuit effects. Frontiers in Synaptic Neuroscience, 6, 22.
Lombardo, S., & Maskos, U. (2015). Role of the nicotinic acetylcholine receptor in Alzheimer’s disease pathology and treatment. Neuropharmacology, 96(Pt B), 255–262.
Lundblad, M., Andersson, M., Winkler, C., Kirik, D., Wierup, N., & Cenci, M. A. (2002). Pharmacological validation of behavioural measures of akinesia and dyskinesia in a rat model of Parkinson’s disease. European Journal of Neuroscience, 15(1), 120–132.
Lundblad, M., Usiello, A., Carta, M., Hakansson, K., Fisone, G., & Cenci, M. A. (2005). Pharmacological validation of a mouse model of l-DOPA-induced dyskinesia. Experimental Neurology, 194(1), 66–75.
McCallum, S. E., Parameswaran, N., Perez, X. A., Bao, S., McIntosh, J. M., Grady, S. R., & Quik, M. (2006). Compensation in pre-synaptic dopaminergic function following nigrostriatal damage in primates. Journal of Neurochemistry, 96(4), 960–972.
Meissner, W. G., Frasier, M., Gasser, T., Goetz, C. G., Lozano, A., Piccini, P., Obeso, J. A., Rascol, O., Schapira, A., Voon, V., Weiner, D. M., Tison, F., & Bezard, E. (2011). Priorities in Parkinson’s disease research. Nature Reviews Drug Discovery, 10(5), 377–393.
Merola, A., Rizzi, L., Zibetti, M., Artusi, C. A., Montanaro, E., Angrisano, S., Lanotte, M., Rizzone, M. G., & Lopiano, L. (2014). Medical therapy and subthalamic deep brain stimulation in advanced Parkinson’s disease: a different long-term outcome? Journal of Neurology, Neurosurgery and Psychiatry, 85(5), 552–559.
Meshul, C. K., Kamel, D., Moore, C., Kay, T. S., & Krentz, L. (2002). Nicotine alters striatal glutamate function and decreases the apomorphine-induced contralateral rotations in 6-OHDA-lesioned rats. Experimental Neurology, 175(1), 257–274.
Millar, N. S., & Gotti, C. (2009). Diversity of vertebrate nicotinic acetylcholine receptors. Neuropharmacology, 56(1), 237–246.
Mitsuoka, T., Kaseda, Y., Yamashita, H., Kohriyama, T., Kawakami, H., Nakamura, S., & Yamamura, Y. (2002). Effects of nicotine chewing gum on UPDRS score and P300 in early-onset parkinsonism. Hiroshima Journal of Medical Sciences, 51(1), 33–39.
Morens, D. M., Grandinetti, A., Reed, D., White, L. R., & Ross, G. W. (1995). Cigarette smoking and protection from Parkinson’s disease: false association or etiologic clue? Neurology, 45(6), 1041–1051.
Muller, M. L., & Bohnen, N. I. (2013). Cholinergic dysfunction in Parkinson’s disease. Current Neurology and Neuroscience Reports, 13(9), 377.
Noyce, A. J., Bestwick, J. P., Silveira-Moriyama, L., Hawkes, C. H., Giovannoni, G., Lees, A. J., & Schrag, A. (2012). Meta-analysis of early nonmotor features and risk factors for Parkinson disease. Annals of Neurology, 72(6), 893–901.
Obeso, J. A., Rodriguez-Oroz, M., Marin, C., Alonso, F., Zamarbide, I., Lanciego, J. L., & Rodriguez-Diaz, M. (2004). The origin of motor fluctuations in Parkinson’s disease: importance of dopaminergic innervation and basal ganglia circuits. Neurology, 62(1 Suppl 1), S17–S30.
Obeso, J. A., Rodriguez-Oroz, M. C., Goetz, C. G., Marin, C., Kordower, J. H., Rodriguez, M., Hirsch, E. C., Farrer, M., Schapira, A. H., & Halliday, G. (2010). Missing pieces in the Parkinson’s disease puzzle. Nature Medicine, 16(6), 653–661.
Parain, K., Hapdey, C., Rousselet, E., Marchand, V., Dumery, B., & Hirsch, E. C. (2003). Cigarette smoke and nicotine protect dopaminergic neurons against the 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine Parkinsonian toxin. Brain Research, 984(1–2), 224–232.
Parkinson Study G. (2006). Randomized placebo-controlled study of the nicotinic agonist SIB-1508Y in Parkinson disease. Neurology, 66(3), 408–410.
Pearce, R. K., Jackson, M., Smith, L., Jenner, P., & Marsden, C. D. (1995). Chronic L-DOPA administration induces dyskinesias in the 1-methyl-4- phenyl-1,2,3,6-tetrahydropyridine-treated common marmoset (Callithrix Jacchus). Movement Disorders, 10(6), 731–740.
Perez, X. A., & Quik, M. (2011). Focus on alpha4beta2* and alpha6beta2* nAChRs for Parkinson’s Disease Therapeutics. Molecular and Cellular Pharmacology, 3(1), 1–6.
Perez, X. A., Parameswaran, N., Huang, L. Z., O’Leary, K. T., & Quik, M. (2008). Pre-synaptic dopaminergic compensation after moderate nigrostriatal damage in non-human primates. Journal of Neurochemistry, 105(5), 1861–1872.
Perez, X. A., Bordia, T., McIntosh, J. M., & Quik, M. (2010). alpha6ss2* and alpha4ss2* nicotinic receptors both regulate dopamine signaling with increased nigrostriatal damage: relevance to Parkinson’s disease. Molecular Pharmacology, 78(5), 971–980.
Petzinger, G. M., Quik, M., Ivashina, E., Jakowec, M. W., Jakubiak, M., Di Monte, D., & Langston, J. W. (2001). Reliability and validity of a new global dyskinesia rating scale in the MPTP-lesioned non-human primate. Movement Disorders, 16(2), 202–207.
Porras, G., Li, Q., & Bezard, E. (2012). Modeling Parkinson’s disease in primates: The MPTP model. Cold Spring Harbor Perspectives in Medicine, 2(3), a009308.
Posadas, I., Lopez-Hernandez, B., & Cena, V. (2013). Nicotinic receptors in neurodegeneration. Current Neuropharmacology, 11(3), 298–314.
Potts, L. F., Uthayathas, S., Greven, A. C., Dyavarshetty, B., Mouradian, M. M., & Papa, S. M. (2015). A new quantitative rating scale for dyskinesia in nonhuman primates. Behavioral Pharmacology, 26(1–2), 109–116.
Przedborski, S., Levivier, M., Jiang, H., Ferreira, M., Jackson-Lewis, V., Donaldson, D., & Togasaki, D. M. (1995). Dose-dependent lesions of the dopaminergic nigrostriatal pathway induced by intrastriatal injection of 6-hydroxydopamine. Neuroscience, 67(3), 631–647.
Quik, M. (2004). Smoking, nicotine and Parkinson’s disease. Trends in Neurosciences, 27(9), 561–568.
Quik, M., & Wonnacott, S. (2011). alpha6beta2* and alpha4beta2* nicotinic acetylcholine receptors as drug targets for Parkinson’s disease. Pharmacological Reviews, 63(4), 938–966.
Quik, M., Sum, J. D., Whiteaker, P., McCallum, S. E., Marks, M. J., Musachio, J., McIntosh, J. M., Collins, A. C., & Grady, S. R. (2003). Differential declines in striatal nicotinic receptor subtype function after nigrostriatal damage in mice. Molecular Pharmacology, 63(5), 1169–1179.
Quik, M., Chen, L., Parameswaran, N., Xie, X., Langston, J. W., & McCallum, S. E. (2006a). Chronic oral nicotine normalizes dopaminergic function and synaptic plasticity in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-lesioned primates. Journal of Neuroscience, 26(17), 4681–4689.
Quik, M., Parameswaran, N., McCallum, S. E., Bordia, T., Bao, S., McCormack, A., Kim, A., Tyndale, R. F., Langston, J. W., & Di Monte, D. A. (2006b). Chronic oral nicotine treatment protects against striatal degeneration in MPTP-treated primates. Journal of Neurochemistry, 98(6), 1866–1875.
Quik, M., Cox, H., Parameswaran, N., O’Leary, K., Langston, J. W., & Di Monte, D. (2007a). Nicotine reduces levodopa-induced dyskinesias in lesioned monkeys. Annals of Neurology, 62(6), 588–596.
Quik, M., O’Neill, M., & Perez, X. A. (2007b). Nicotine neuroprotection against nigrostriatal damage: importance of the animal model. Trends in Pharmacological Sciences, 28(5), 229–235.
Quik, M., Campos, C., Parameswaran, N., Langston, J. W., McIntosh, J. M., & Yeluashvili, M. (2010). Chronic nicotine treatment increases nAChRs and microglial expression in monkey substantia nigra after nigrostriatal damage. Journal of Molecular Neuroscience, 40(1–2), 105–113.
Quik, M., Park, K. M., Hrachova, M., Mallela, A., Huang, L. Z., McIntosh, J. M., & Grady, S. R. (2012). Role for alpha6 nicotinic receptors in l-dopa-induced dyskinesias in parkinsonian mice. Neuropharmacology, 63(3), 450–459.
Quik, M., Campos, C., Bordia, T., Strachan, J. P., Zhang, J., McIntosh, J. M., Letchworth, S., & Jordan, K. (2013a). alpha4beta2 Nicotinic receptors play a role in the nAChR-mediated decline in L-dopa-induced dyskinesias in parkinsonian rats. Neuropharmacology, 71, 191–203.
Quik, M., Campos, C., & Grady, S. R. (2013b). Multiple CNS nicotinic receptors mediate L-dopa-induced dyskinesias: studies with parkinsonian nicotinic receptor knockout mice. Biochemical Pharmacology, 86(8), 1153–1162.
Quik, M., Mallela, A., Chin, M., McIntosh, J. M., Perez, X. A., & Bordia, T. (2013c). Nicotine-mediated improvement in L-dopa-induced dyskinesias in MPTP-lesioned monkeys is dependent on dopamine nerve terminal function. Neurobiology of Disease, 50, 30–41.
Quik, M., Mallela, A., Ly, J., & Zhang, D. (2013d). Nicotine reduces established levodopa-induced dyskinesias in a monkey model of Parkinson’s disease. Movement Disorders, 28(10), 1398–1406.
Quik, M., Zhang, D., Perez, X. A., & Bordia, T. (2014). Role for the nicotinic cholinergic system in movement disorders; therapeutic implications. Pharmacology and Therapeutics, 144(1), 50–59.
Quik, M., Zhang, D., McGregor, M., & Bordia, T. (2015). Alpha7 nicotinic receptors as therapeutic targets for Parkinson’s disease. Biochemical Pharmacology, 97(4), 399–407.
Quinn, N. P. (1998). Classification of fluctuations in patients with Parkinson’s disease. Neurology, 51(2 Suppl 2), S25–S29.
Quinn, N., Marsden, C. D., & Parkes, J. D. (1982). Complicated response fluctuations in Parkinson’s disease: response to intravenous infusion of levodopa. Lancet, 2(8295), 412–415.
Rhodes, J. D., Hawk, L. W., Jr., Ashare, R. L., Schlienz, N. J., & Mahoney, M. C. (2012). The effects of varenicline on attention and inhibitory control among treatment-seeking smokers. Psychopharmacology, 223(2), 131–138.
Rice, M. E., & Cragg, S. J. (2004). Nicotine amplifies reward-related dopamine signals in striatum. Nature Neuroscience, 7(6), 583–584.
Ritz, B., Ascherio, A., Checkoway, H., Marder, K. S., Nelson, L. M., Rocca, W. A., Ross, G. W., Strickland, D., Van Den Eeden, S. K., & Gorell, J. (2007). Pooled analysis of tobacco use and risk of Parkinson disease. Archives of Neurology, 64(7), 990–997.
Riveles, K., Huang, L. Z., & Quik, M. (2008). Cigarette smoke, nicotine and cotinine protect against 6-hydroxydopamine-induced toxicity in SH-SY5Y cells. Neurotoxicology, 29(3), 421–427.
Rizzone, M. G., Fasano, A., Daniele, A., Zibetti, M., Merola, A., Rizzi, L., Piano, C., Piccininni, C., Romito, L. M., Lopiano, L., & Albanese, A. (2014). Long-term outcome of subthalamic nucleus DBS in Parkinson’s disease: from the advanced phase towards the late stage of the disease? Parkinsonism & Related Disorders, 20(4), 376–381.
Ryan, R. E., Ross, S. A., Drago, J., & Loiacono, R. E. (2001). Dose-related neuroprotective effects of chronic nicotine in 6-hydroxydopamine treated rats, and loss of neuroprotection in alpha4 nicotinic receptor subunit knockout mice. British Journal of Pharmacology, 132(8), 1650–1656.
Sarre, S., Yuan, H., Jonkers, N., Van Hemelrijck, A., Ebinger, G., & Michotte, Y. (2004). In vivo characterization of somatodendritic dopamine release in the substantia nigra of 6-hydroxydopamine-lesioned rats. Journal of Neurochemistry, 90(1), 29–39.
Schaeffer, E., Pilotto, A., & Berg, D. (2014). Pharmacological strategies for the management of levodopa-induced dyskinesia in patients with Parkinson’s disease. CNS Drugs, 28(12), 1155–1184.
Schallert, T., Fleming, S. M., Leasure, J. L., Tillerson, J. L., & Bland, S. T. (2000). CNS plasticity and assessment of forelimb sensorimotor outcome in unilateral rat models of stroke, cortical ablation, parkinsonism and spinal cord injury. Neuropharmacology, 39(5), 777–787.
Schapira, A. H., & Jenner, P. (2011). Etiology and pathogenesis of Parkinson’s disease. Movement Disorders, 26(6), 1049–1055.
Searles Nielsen, S., Gallagher, L. G., Lundin, J. I., Longstreth, W. T., Jr., Smith-Weller, T., Franklin, G. M., Swanson, P. D., & Checkoway, H. (2012). Environmental tobacco smoke and Parkinson’s disease. Movement Disorders, 27(2), 293–296.
Serriere, S., Domene, A., Vercouillie, J., Mothes, C., Bodard, S., Rodrigues, N., Guilloteau, D., Routier, S., Page, G., & Chalon, S. (2015). Assessment of the Protection of Dopaminergic Neurons by an alpha7 Nicotinic Receptor Agonist, PHA 543613 Using [(18)F]LBT-999 in a Parkinson’s Disease Rat Model. Frontiers in Medicine, 2, 61.
Shim, J. C., Jung, D. U., Jung, S. S., Seo, Y. S., Cho, D. M., Lee, J. H., Lee, S. W., Kong, B. G., Kang, J. W., Oh, M. K., Kim, S. D., McMahon, R. P., & Kelly, D. L. (2012). Adjunctive varenicline treatment with antipsychotic medications for cognitive impairments in people with schizophrenia: a randomized double-blind placebo-controlled trial. Neuropsychopharmacology, 37(3), 660–668.
Shimohama, S. (2009). Nicotinic receptor-mediated neuroprotection in neurodegenerative disease models. Biological and Pharmaceutical Bulletin, 32(3), 332–336.
Shimohama, S., Akaike, A., & Kimura, J. (1996). Nicotine-induced protection against glutamate cytotoxicity. Nicotinic cholinergic receptor-mediated inhibition of nitric oxide formation. Annals of the New York Academy of Sciences, 777, 356–361.
Shimoji, M., Zhang, L., Mandir, A. S., Dawson, V. L., & Dawson, T. M. (2005). Absence of inclusion body formation in the MPTP mouse model of Parkinson’s disease. Brain Research. Molecular Brain Research, 134(1), 103–108.
Soto-Otero, R., Mendez-Alvarez, E., Hermida-Ameijeiras, A., Lopez-Real, A. M., & Labandeira-Garcia, J. L. (2002). Effects of (−)-nicotine and (−)-cotinine on 6-hydroxydopamine-induced oxidative stress and neurotoxicity: relevance for Parkinson’s disease. Biochemical Pharmacology, 64(1), 125–135.
Stuckenholz, V., Bacher, M., Balzer-Geldsetzer, M., Alvarez-Fischer, D., Oertel, W. H., Dodel, R. C., & Noelker, C. (2013). The alpha7 nAChR agonist PNU-282987 reduces inflammation and MPTP-induced nigral dopaminergic cell loss in mice. Journal of Parkinson’s Disease, 3(2), 161–172.
Suzuki, S., Kawamata, J., Matsushita, T., Matsumura, A., Hisahara, S., Takata, K., Kitamura, Y., Kem, W., & Shimohama, S. (2013). 3-[(2,4-Dimethoxy)benzylidene]-anabaseine dihydrochloride protects against 6-hydroxydopamine-induced parkinsonian neurodegeneration through alpha7 nicotinic acetylcholine receptor stimulation in rats. Journal of Neuroscience Research, 91(3), 462–471.
Takeuchi, H., Yanagida, T., Inden, M., Takata, K., Kitamura, Y., Yamakawa, K., Sawada, H., Izumi, Y., Yamamoto, N., Kihara, T., Uemura, K., Inoue, H., Taniguchi, T., Akaike, A., Takahashi, R., & Shimohama, S. (2009). Nicotinic receptor stimulation protects nigral dopaminergic neurons in rotenone-induced Parkinson’s disease models. Journal of Neuroscience Research, 87(2), 576–585.
Tambasco, N., Simoni, S., Marsili, E., Sacchini, E., Murasecco, D., Cardaioli, G., Rossi, A., & Calabresi, P. (2012). Clinical aspects and management of levodopa-induced dyskinesia. Journal of Parkinson’s Disease, 2012, 745947.
Tan, L. C., Protell, P. H., Langston, J. W., & Togasaki, D. M. (2002). The hyperkinetic abnormal movements scale: a tool for measuring levodopa-induced abnormal movements in squirrel monkeys. Movement Disorders, 17(5), 902–909.
Tanner, C. M. (2010). Advances in environmental epidemiology. Movement Disorders, 25(Suppl 1), S58–S62.
Taylor, T. N., Greene, J. G., & Miller, G. W. (2010). Behavioral phenotyping of mouse models of Parkinson’s disease. Behavioural Brain Research, 211(1), 1–10.
Terzioglu, M., & Galter, D. (2008). Parkinson’s disease: genetic versus toxin-induced rodent models. FEBS Journal, 275(7), 1384–1391.
Tieu, K. (2011). A guide to neurotoxic animal models of Parkinson’s disease. Cold Spring Harbor Perspectives in Medicine, 1(1), a009316.
Ungerstedt, U. (1968). 6-Hydroxy-dopamine induced degeneration of central monoamine neurons. European Journal of Pharmacology, 5(1), 107–110.
Valadas, J. S., Vos, M., & Verstreken, P. (2015). Therapeutic strategies in Parkinson’s disease: what we have learned from animal models. Annals of the New York Academy of Sciences, 1338, 16–37.
Vieira-Brock, P.L., McFadden, L.M., Nielsen, S.M., Ellis, J.D., Walters, E.T., Stout, K.A., McIntosh, J.M., Wilkins, D.G., Hanson, G.R., Fleckenstein, A.E. (2015) Chronic Nicotine Exposure Attenuates Methamphetamine-Induced Dopaminergic Deficits. Journal of Pharmacology and Experimental Therapeutics.
Vieregge, A., Sieberer, M., Jacobs, H., Hagenah, J. M., & Vieregge, P. (2001). Transdermal nicotine in PD: a randomized, double-blind, placebo-controlled study. Neurology, 57(6), 1032–1035.
Villafane, G., Cesaro, P., Rialland, A., Baloul, S., Azimi, S., Bourdet, C., Le Houezec, J., Macquin-Mavier, I., & Maison, P. (2007). Chronic high dose transdermal nicotine in Parkinson’s disease: an open trial. European Journal of Neurology, 14(12), 1313–1316.
Wallace, T. L., & Porter, R. H. (2011). Targeting the nicotinic alpha7 acetylcholine receptor to enhance cognition in disease. Biochemical Pharmacology, 82(8), 891–903.
Wallace, T. L., Callahan, P. M., Tehim, A., Bertrand, D., Tombaugh, G., Wang, S., Xie, W., Rowe, W. B., Ong, V., Graham, E., Terry, A. V., Jr., Rodefer, J. S., Herbert, B., Murray, M., Porter, R., Santarelli, L., & Lowe, D. A. (2011). RG3487, a novel nicotinic alpha7 receptor partial agonist, improves cognition and sensorimotor gating in rodents. Journal of Pharmacol and Experimental Therapeutics, 336(1), 242–253.
Wichmann, T., DeLong, M. R., Guridi, J., & Obeso, J. A. (2011). Milestones in research on the pathophysiology of Parkinson’s disease. Movement Disorders, 26(6), 1032–1041.
Winkler, C., Kirik, D., Bjorklund, A., & Cenci, M. A. (2002). L-DOPA-induced dyskinesia in the intrastriatal 6-hydroxydopamine model of parkinson’s disease: relation to motor and cellular parameters of nigrostriatal function. Neurobiology of Disease, 10(2), 165–186.
Wirdefeldt, K., Adami, H. O., Cole, P., Trichopoulos, D., & Mandel, J. (2011). Epidemiology and etiology of Parkinson’s disease: a review of the evidence. European Journal of Epidemiology, 26(Suppl 1), S1–S58.
Wullner, U., Pakzaban, P., Brownell, A. L., Hantraye, P., Burns, L., Shoup, T., Elmaleh, D., Petto, A. J., Spealman, R. D., Brownell, G. L., et al. (1994). Dopamine terminal loss and onset of motor symptoms in MPTP-treated monkeys: a positron emission tomography study with 11C-CFT. Experimental Neurology, 126(2), 305–309.
Zhang, H., & Sulzer, D. (2004). Frequency-dependent modulation of dopamine release by nicotine. Nature Neuroscience, 7(6), 581–582.
Zhang, D., Mallela, A., Sohn, D., Carroll, F. I., Bencherif, M., Letchworth, S., & Quik, M. (2013). Nicotinic receptor agonists reduce L-DOPA-induced dyskinesias in a monkey model of Parkinson’s disease. Journal of Pharmacol and Experimental Therapeutics, 347(1), 225–234.
Zhang, D., Bordia, T., McGregor, M., McIntosh, J. M., Decker, M. W., & Quik, M. (2014a). ABT-089 and ABT-894 reduce levodopa-induced dyskinesias in a monkey model of Parkinson’s disease. Movement Disorders, 29(4), 508–517.
Zhang, D., McGregor, M., Decker, M. W., & Quik, M. (2014b). The alpha7 nicotinic receptor agonist ABT-107 decreases L-Dopa-induced dyskinesias in parkinsonian monkeys. Journal of Pharmacol and Experimental Therapeutics, 351(1), 25–32.
Zhang, D., McGregor, M., Bordia, T., Perez, X.A., Decker, M.W., Quik, M. (2015a). The alpha7 nicotinic receptor agonist ABT-126 decreases l-Dopa-induced dyskinesias in MPTP-lesioned monkeys, in Society for neuroscience, Chicago, IL.
Zhang, D., McGregor, M., Bordia, T., Perez, X.A., McIntosh, J.M., Decker, M.W., Quik, M. (2015b). α7 nicotinic receptor agonists decrease levodopa-induced dyskinesias in monkeys with moderate and severe nigrostriatal damage. Movement disorders In Press.
Zhou, F. M., Liang, Y., & Dani, J. A. (2001). Endogenous nicotinic cholinergic activity regulates dopamine release in the striatum. Nature Neuroscience, 4(12), 1224–1229.
Acknowledgments
The author would like to thank Dr. Maryka Quik and Dr. Tanuja Bordia for helpful discussion and reading of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Perez, X.A. Preclinical Evidence for a Role of the Nicotinic Cholinergic System in Parkinson’s Disease. Neuropsychol Rev 25, 371–383 (2015). https://doi.org/10.1007/s11065-015-9303-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11065-015-9303-z