Abstract
The mammalian multicopper ferroxidases (MCFs) ceruloplasmin (CP), hephaestin (HEPH) and zyklopen (ZP) comprise a family of conserved enzymes that are essential for body iron homeostasis. Each of these enzymes contains six biosynthetically incorporated copper atoms which act as intermediate electron acceptors, and the oxidation of iron is associated with the four electron reduction of dioxygen to generate two water molecules. CP occurs in both a secreted and GPI-linked (membrane-bound) form, while HEPH and ZP each contain a single C-terminal transmembrane domain. These enzymes function to ensure the efficient oxidation of iron so that it can be effectively released from tissues via the iron export protein ferroportin and subsequently bound to the iron carrier protein transferrin in the blood. CP is particularly important in facilitating iron release from the liver and central nervous system, HEPH is the major MCF in the small intestine and is critical for dietary iron absorption, and ZP is important for normal hair development. CP and HEPH (and possibly ZP) function in multiple tissues. These proteins also play other (non-iron-related) physiological roles, but many of these are ill-defined. In addition to disrupting iron homeostasis, MCF dysfunction perturbs neurological and immune function, alters cancer susceptibility, and causes hair loss, but, despite their importance, how MCFs co-ordinately maintain body iron homeostasis and perform other functions remains incompletely understood.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The MCFs are representatives of the large and diverse blue copper protein family (Rydén and Hunt 1993; Nakamura and Go 2005). The blue copper proteins vary greatly in size and complexity, and contain up to 9 copper atoms. Their functions are also broad, and include proteins involved in iron homeostasis (CP, HEPH, ZP), electron transfer (plastocyanin), blood clotting (coagulation factors V and VIII), ascorbate metabolism (ascorbate oxidase), oxidation of polyphenols (laccase), and oxidative phosphorylation (cytochrome c oxidase subunit II). The relatively complex mammalian members of this family evolved from an ancestral single-domain, cupredoxin-fold protein, and the MCFs are the only known members of the blue copper protein family in mammals that contain multiple copper atoms (Nakamura and Go 2005).
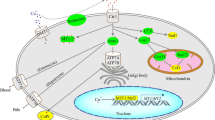
CP is the most studied MCF and is the major ferroxidase in the blood (Hellman and Gitlin 2002). It was first identified in 1948 by Holmberg and Laurell as an abundant plasma protein with a distinctive sky blue color, and was subsequently shown to be synthesized and secreted, mainly by hepatocytes (Hellman and Gitlin 2002). Other cell types, including astrocytes and neurons in the brain, Sertoli cells in the testes and cells in the retina, lung and pancreas can also synthesize CP. While most CP is secreted into the extracellular fluids, alternative splicing of the CP transcript leads to production of a GPI-linked form of the protein which tethers it to the plasma membrane (Fig. 1). GPI-CP is expressed in astrocytes (Patel and David 1997; Jeong and David 2003), Sertoli cells, hepatocytes, macrophages and retinal epithelial cells (Mostad and Prohaska 2011; Marques et al. 2012).
Nature of the mammalian MCFs. A Recombinant mouse HEPH (without its transmembrane domain), generated as described by Deshpande et al. (2017), showing the intense blue color typical of the MCFs and related blue copper proteins. B General structure of the four forms of mammalian MCFs. From left to right: secreted CP; GPI-CP; and the two MCFs with single transmembrane domains, ZP and HEPH. The ribbon diagrams of each protein were generated using AlphaFold (https://alphafold.ebi.ac.uk/entry/Q9BQS7) (Jumper et al. 2021). Created with BioRender.com. (Color figure online)
HEPH is a protein critical for intestinal iron absorption and was cloned by identifying the gene mutated in the sex-linked anemic (sla) mouse (Vulpe et al. 1999). Unlike the secreted form of CP, HEPH is tethered to membranes by a single C-terminal transmembrane domain (Fig. 1). HEPH is strongly expressed in the small intestine, and at low to moderate levels in multiple other tissues, most notably the CNS (Vulpe et al. 1999; Hudson et al. 2009; Jiang et al. 2015).
ZP is the least studied MCF. It was identified relatively recently as a possible placental iron oxidase (Chen et al. 2010), although this now seems unlikely as placental iron transfer is not impeded in mice in which the gene encoding ZP (Hephl1) is knocked out, at least under standard (unstressed) physiological conditions (Helman et al. 2021). The only confirmed role for ZP at present is a contribution to normal hair development (Eragene et al. 2019; Sharma et al. 2019; Kuca et al. 2021). Like HEPH, ZP contains a single C-terminal transmembrane domain. ZP is most strongly expressed in the placenta, mammary gland, kidney, brain and testis (Chen et al. 2010).
The MCFs are very similar structurally (Fig. 1). At the amino acid level, HEPH and ZP show 50% and 46% identity to CP respectively, while HEPH and ZP are 49% identical (Vulpe et al. 1999; Chen et al. 2010). The residues involved in copper binding and disulfide bond formation (the latter suggesting similar folding of the proteins) are highly conserved between the three proteins. In addition, both HEPH and ZP contain a single C-terminal transmembrane domain of 86 amino acids, although the sequences of these domains are only 23% conserved at the protein level (Chen et al. 2010).
Most of our current knowledge about the structure of the mammalian MCFs comes from the detailed characterization of CP (Zaitsev et al. 1999). It is a large protein consisting of 1046 amino acids that are arranged in three major homology units, each of which appears to have arisen from internal duplication of an ancient cupredoxin fold, to give a six-domain protein (Ortel et al. 1984; Nakamura and Go 2005). An X-ray crystallographic structure of CP is available (Zaitseva et al. 1996; Bento et al. 2007), and this confirmed the domain organization of the protein predicted by earlier sequence analysis (Ortel et al. 1984). The six domains are each made up of a plastocyanin-like fold and beta-barrel strands organized similar to those found in the cupredoxin family of metalloreductases (Bento et al. 2007). A key feature of CP’s structure, and one that underlies its biological activity, is the presence of three types of copper-containing sites, each of which has distinct spectroscopic properties resulting from their specific coordination environments. Three of the six copper atoms in CP are distributed between three type I copper sites, in domains 2, 4, and 6, and the remaining three copper atoms are in a distinctive type II/type III trinuclear cluster at the interface of domains 1 and 6. Molecular modelling of HEPH and ZP reveals predicted structures that closely align with the known structure of CP (Syed et al. 2002; Chen et al. 2010).
Both CP and HEPH have been shown to possess a high affinity ferrous iron binding site near the type I copper atom in domain 6, and ZP is predicted to possess a similar site (Lindley et al. 1997; Brown et al. 2002; Vashchenko and MacGillivray 2012). Additional iron-binding sites have also been demonstrated in CP (a second site in domain 4) and HEPH (additional sites in domains 2 and 4), but they are of lower affinity (Lindley et al. 1997; Vashchenko and MacGillivray 2012; Zaitsev and Lindley 2019). Following binding, ferrous iron predicted to deliver an electron to the nearest type I copper site. This is associated with the transfer of the oxidized iron to an adjacent ferric iron holding site. Electrons are subsequently transferred through the protein to the type I copper site in domain 6, and then to the closely associated type II/type III trinuclear cluster where molecular oxygen binds. The Type II/Type III site can then sequentially transfer a total of four electrons, originally donated from different ferrous iron atoms, to dioxygen to form water (Lindley et al. 1997; Vashchenko and MacGillivray 2012). The MCFs can also oxidize a range of substrates in addition to iron, and, in CP, many of these bind at sites different from the iron binding sites (Bielli and Calabrese 2002).
Some of the residues important for ferroxidase and amine oxidase activity in CP have been identified by site directed mutagenesis, (Brown et al. 2002) and most, but not all of these are conserved in HEPH and ZP (Chen et al. 2010). CP interestingly has a non-typical, permanently-reduced type I copper site in domain 2 that is believed to be non-functional, while all three type I copper sites are predicted to be functional in HEPH and ZP (Chen et al. 2010). In CP, the copper atoms in two of the three type I sites are coordinated in a trigonal pyramid arrangement, with three ligands (a cysteine and two histidines) arranged in a plane, and the fourth, a methionine, at the apex of the pyramid. In the third (non-functional) type I site, however, the apical methionine has been replaced by a leucine residue. In contrast, in both HEPH and ZP, the third type I site shows the ‘typical’ coordination arrangement with an apical methionine.
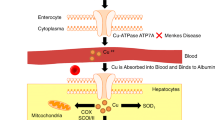
Not only is copper required for the ferroxidase activity of CP and the other MCFs, it is also structurally important and the apo-proteins (lacking copper) are inherently unstable (Gitlin et al. 1992; Reeves and Demars 2005; Chen et al. 2006). The half-life of apo-CP is approximately five hours whereas the holo-protein has a half-life of over five days (Hellman and Gitlin 2002). Although the precise details of the mechanisms responsible for the metalation of CP are not known, the necessary copper is transported into the trans-Golgi network by ATPase copper-transporting Beta (ATP7B) where the metal is inserted into the nascent protein (Sato and Gitlin 1991; Hellman et al. 2002; Lutsenko et al. 2007). In cases of ATP7B deficiency (Wilson Disease), this process is less efficient and much of the CP that is produced lacks both copper and oxidase activity (Członkowska et al. 2018). Consequently, measurements of serum ferroxidase activity are a useful diagnostic tool for Wilson Disease and for assessing moderate to severe copper deficiency (Sánchez-Monteagudo et al. 2021). It is likely that the biosynthetic pathways for HEPH and ZP are similar to that of CP, but these processes have yet to be studied in detail. There is certainly very strong evidence that the biological activities of HEPH and ZP are also copper-dependent (Chen et al. 2006; Chen et al. 2010).
The role of the MCFs in iron homeostasis
In 1966, Frieden and Osaki demonstrated that plasma CP had the ability to oxidize ferrous iron (Osaki et al. 1966) and subsequently showed that the protein was important for mobilizing iron from the liver (Osaki et al. 1971). These pioneering studies, along with an important series of experiments in pigs showing that copper deficiency was associated with anemia (Lee et al. 1968; Roeser et al. 1970), highlighted what is now known to be a very close physiological relationship between copper and iron (Gulec and Collins 2014).
Understanding how the MCFs function requires a basic understanding of iron homeostasis. Despite being essential, iron is also toxic when present in excess as it can catalyze the formation of reactive oxygen species. To meet cellular iron requirements while preventing iron accumulating to toxic levels, cellular and body iron concentrations must be kept within defined limits. To achieve this, both dietary iron absorption and internal iron trafficking are tightly regulated (Anderson and Frazer 2017). Most iron within the body is used for the production of hemoglobin in red blood cells. At the end of their functional life, senescent red cells are phagocytosed by macrophages, which can store iron or return it to the circulation, a process referred to as iron recycling. In addition, iron in excess of immediate metabolic needs may be stored within tissues, particularly in the liver, but it can be readily mobilized in times of metabolic need. Dietary iron absorption, internal iron recycling and mobilization of stored iron are all critically dependent on MCFs. This requirement is best illustrated by situations in which MCF dysfunction occurs. In the rare genetic disease aceruloplasminemia, CP is either absent or expressed at very low levels (Marchi et al. 2019). This condition is typified by extensive iron deposition in many tissues, illustrating the key role that CP plays in iron mobilization. Subsequent studies with Cp knockout mice, and analogous work with mouse models of HEPH deficiency, have supported and extended these early findings (Harris et al. 1999; Fuqua et al. 2014; Fuqua et al. 2018).
Iron is exported from cells as Fe2+ via the unique iron export protein ferroportin (FPN), however, Fe2+ must be oxidized before it can bind to transferrin, the major plasma iron transport protein (Anderson and Vulpe 2009). The MCFs likely facilitate this process, but how they contribute to cellular iron efflux is incompletely understood. The membrane-bound MCFs HEPH and GPI-CP have been demonstrated to interact physically with FPN (Jeong and David 2003; Yeh et al. 2009, 2011; Dlouhy et al. 2019), but there is not yet any convincing data that the soluble form of CP behaves similarly (Musci et al. 2014). FPN has been shown to co-localize with GPI-CP in astrocytes (Jeong and David 2003) and with HEPH in enterocytes (Yeh et al. 2009; Fuqua et al. 2018). It has been suggested that MCFs are able to oxidize Fe2+ that has been transported by FPN and that this oxidation is important for the release of the iron from the transporter (De Domenico et al. 2007). If iron is not released from FPN, the transporter is ubiquitinated, internalized and degraded, which suggests that the MCF is important in maintaining FPN stability. Although, this is an attractive hypothesis, the data have not yet been independently verified, and this work was mentioned in a scientific misconduct investigation (McCormack 2013). Nevertheless, there is some support for this concept. For example, brain microvascular endothelial cells express both HEPH and soluble CP, and when the levels of these proteins are depleted by copper chelation, FPN levels are also reduced (McCarthy and Kosman 2013). Similarly, knockdown of HEPH in neurons reduces FPN levels and iron export (Ji et al. 2018). Interestingly, however, loss of HEPH in the small intestine is not associated with any overt decline in FPN expression (Fuqua et al. 2018), suggesting that the MCFs may only stabilize FPN in some tissues. There is also some evidence that GPI-CP is able to interfere with the binding of hepcidin to FPN (Kono et al. 2010). Hepcidin is a liver-derived peptide hormone that is considered the master regulator of systemic iron homeostasis, and it acts by binding to FPN and removing it from the cell surface, consequently blocking iron export. This interaction could be a second mechanism by which MCFs facilitate iron efflux, and is consistent with a close physical association between FPN and the MCF, but it requires further investigation.
Essentially all of the (ferrous) iron that is exported from cells via FPN and oxidized by an MCF is bound by transferrin (TF) in the plasma, and this protein can then deliver iron to the various sites in the body where it is required (Anderson and Vulpe 2009). TF binds ferric iron (Fe3+), thus oxidation of Fe2+ by MCFs could not only facilitate the release of iron from FPN (as discussed above), but also permit binding of Fe3+ to TF. Although Fe2+ will auto-oxidize in the plasma, this process is considered too slow for the trafficking of iron under physiological conditions (Osaki et al. 1966). While some studies have found evidence for a physical association between CP and TF (Ha-Duong et al. 2010), others have found no evidence that either CP or HEPH can stably interact with TF (Hudson et al. 2008). A strong interaction between CP and lactoferrin (LF), a close relative of TF, has been identified (Zakharova et al. 2000; Ha-Duong et al. 2010), although the physiological relevance of this interaction has yet to be established.
In addition to its well-described role in cellular iron efflux, CP has been shown to stimulate the uptake of iron by some mammalian cells in culture using a TF-independent pathway (Mukhopadhyay et al. 1998; Attieh et al. 1999). In this case, it is proposed that non-transferrin-bound iron (NTBI) is reduced by a ferrireductase and that the resulting ferrous iron is oxidized by CP to make it available for a trivalent cation-specific transporter (Attieh et al. 1999). However, the identity of this uptake pathway remains unknown, and further work is required to determine its physiological relevance in vivo.
Other physiological roles of MCFs
Although their role in oxidizing iron is clear, MCFs have broader roles and can utilize a range of other substrates. Some of these are summarized in Table 1. The non-ferroxidase activities of the MCFs have only been extensively studied in the case of CP. In addition to iron, CP can oxidize a range of organic amines, including biogenic amines (such as catecholamines, serotonin and dopamine), low-density lipoprotein (LDL), and nitric oxide (NO) (Bielli and Calabrese 2002; Vashchenko and MacGillivray 2013). HEPH and ZP can also oxidize amines (e.g. para-phenylene diamine) (Vulpe et al. 1999; Chen et al. 2010; Deshpande et al. 2017), so it is quite possible that they also have a broad spectrum of catalytic actions. Studies with CP and recombinant HEPH have demonstrated that they share the ability to oxidise some amines, but not others (Vashchenko et al. 2011), so there are likely to be some differences in the range of activities that individual MCFs participate in.
The physiological significance of many of these non-iron-related activities has never been clearly defined. For example, in humans with aceruloplasminemia and Cp knockout mice, the dominant phenotypes are either directly or indirectly related to tissue iron accumulation (Harris et al. 1999; Ayton et al. 2013; Marchi et al. 2019), but this does not exclude more subtle effects on other aspects of body physiology. It has been estimated that no more than 5–10% of the CP in plasma is sufficient to perform all its iron-related functions (Roeser et al. 1970; Osaki et al. 1971), so is the excess simply ‘reserve’ iron oxidizing capacity, or does the protein perform other functions? Furthermore, HEPH is expressed at high levels throughout the small intestine and colon, even though dietary iron absorption occurs mainly in the duodenum (Frazer et al. 2001). Its function in the regions of the gut that absorb little iron is unknown. There is also considerable evidence that CP can act as an antioxidant (Goldstein 1983; Song et al. 2010; Bakhautdin et al. 2013; Vasilyev 2019), and HEPH and ZP may play similar roles, but this function of the MCFs has never been investigated systematically. Interestingly, CP can also act as a pro-oxidant, causing damage to macromolecules such as LDL (Mukhopadhyay and Fox 1998; Fox et al. 2000), and thus may act as a risk factor for the development of atherosclerotic disease.
Although the main physiological roles of the MCFs most likely relate to iron homeostasis, they also are relevant to the biology of other metals. For example, CP possesses cuprous oxidase activity (Mukhopadhyay et al. 1997; Stoj and Kosman 2003) and may play a role in copper distribution in some circumstance (such as copper transport to the fetus and neonate) (Lee et al. 1993; Chu et al. 2012; Kenawi et al. 2019). Indeed, CP-bound copper represents the largest pool of copper in the circulation, and it has been suggested that it may provide an important pathway for delivering copper to a range of tissues (Linder 2016). Nevertheless, there is no evidence for altered copper homeostasis in aceruloplasminemia (Meyer et al. 2001). Studies with CP-deficient rodents have also shown that CP plays a role in the body distribution of manganese (Jursa and Smith 2009; Kenawi et al. 2019). Whether HEPH or ZP also contribute to the homeostasis of metals other than iron has yet to be determined.
In addition to its enzymatic roles, CP has been shown to bind to a range of other proteins, thereby affecting their activity (Vasilyev 2019). These include myeloperoxidase (MPO), matrix metalloproteinases 2 and 12, eosinophil peroxidase, 5-lipoxygenase and coagulation factor FIIa. CP binding to other iron-associated proteins such as ferritin (Van Eden and Aust 2000) and lactoferrin (Zakharova et al. 2000; Pulina et al. 2002) has also been reported. The binding of iron by LF is facilitated by CP, and it has been suggested that this is one mechanism by which the host might protect itself against the respiratory burst that occurs when neutrophils infiltrate a site of inflammation or infection (Sokolov et al. 2005). Neutrophils are a rich source of LF, and secreted LF has the capacity to bind a considerable amount of iron at the site of inflammation, particularly in the presence of CP. Another potential anti-inflammatory function of CP is its ability to bind to MPO and inhibit the production of hypochlorous acid (Sokolov et al. 2007; Chapman et al. 2013).
Regulation of the MCFs
Given their important role in cellular iron efflux, it is not surprising that the expression of MCFs is increased under iron deficient conditions (Vulpe et al. 1999; Hellman and Gitlin 2002; Chen et al. 2010; Ranganathan et al. 2011). This response is likely an adaptation to support hemoglobin production in developing red cells when iron supply is limiting. The mechanisms responsible for this regulation have not been defined. The expression of many of the central proteins in iron homeostasis is regulated post-transcriptionally (either translationally or via mRNA stability) by the binding of iron regulatory proteins (IRPs) to iron regulatory elements (IREs) in target transcripts (Zhang et al. 2014), but none of the mRNAs encoding MCFs appears to contain an IRE. Thus, alternative transcriptional or post-transcriptional mechanisms must be involved. CP, at least, can be regulated by a combination of transcriptional and translational mechanisms by factors such as hypoxia (Chepelev and Willmore 2011; Linder 2016), proinflammatory cytokines (Gitlin 1988; Sampath et al. 2003; Conley et al. 2005; Mazumder et al. 2006; Persichini et al. 2010; Linder 2016; Tisato et al. 2018) and oxidative stress (Das et al. 2007; Tapryal et al. 2009; Tisato et al. 2018). The other MCFs have not been extensively investigated, however, HEPH has been shown to be regulated by transcriptional and epigenetic mechanisms. In the small intestine and colon, the HEPH gene is a prominent target of the transcription factor CDX2 (Hinoi et al. 2005), which plays a major role in intestinal development and cancer. In addition, CDX2 itself was found to be regulated by iron, providing a transcriptional loop for the regulation of HEPH in the absorptive epithelium of the gut (Hinoi et al. 2005). The transcription of HEPH is also regulated by the H3K9 methyltransferase G9a (Wang et al. 2017), which represses HEPH expression, resulting in cellular iron accumulation and enhanced growth of breast cancer cells. Other epigenetic modes of regulation of the MCFs are likely to be uncovered upon further investigation.
Changes in the subcellular localization of membrane proteins represent another mode of regulation which is particularly useful as a rapid response mechanism. Several studies have demonstrated that HEPH will re-localize from an intracellular supra-nuclear compartment to the basolateral membrane (or a compartment in close proximity to the basolateral membrane) of polarized epithelial cells in response to iron treatment (Yeh et al. 2009; Lee et al. 2012). This likely represents an adaptation to reduce the risk of intracellular iron increasing to toxic levels by stimulating expression of components of the iron export pathway. This effect has also been observed in non-polarized cells (Dlouhy et al. 2019).
Genetics and the pathology of MCF loss or dysfunction
Loss of MCF function leads to increased cellular iron accumulation and its associated pathological consequences (Hellman and Gitlin 2002; Musci et al. 2014; Linder 2016). The best characterised MCF disturbance in humans is aceruloplasminemia, in which iron accumulates in multiple tissues, particularly the liver, CNS and pancreas (Kono 2013; Piperno and Alessio 2018; Marchi et al. 2019). Liver injury, neurodegenerative disease, diabetes and retinal degeneration are common complications. Reduced CP expression has also been implicated in atherosclerosis (Ji et al. 2015), while increased expression has been noted in various cancers (Gangoda et al. 2017; Matsuoka et al. 2018; Dai et al. 2020; Zhang et al. 2021b). Fewer data are available on HEPH or ZP deficiency. Polymorphisms in HEPH have been associated with migraine (Maher et al. 2012; Albury et al. 2017), and reduced HEPH expression has been noted in atherosclerotic plaques (Ji et al. 2015) and is linked to the iron deficiency associated with a high-fat diet (Albury et al. 2017). Increased HEPH (and CP) levels have also been found in the placenta from a GRACILE syndrome fetus (Kotarsky et al. 2010). A patient carrying a missense mutation in HEPHL1, the gene which encodes ZP, had notable hair defects, including pili torti (flattened, twisted hair) as well as behavioural abnormalities (Sharma et al. 2019). A missense mutation in HEPHL1 has also been identified in patients with Parkinson’s disease (Al Yemni et al. 2019).
Rodent strains with disturbed MCF function have proven particularly important in revealing some of the physiological roles of these proteins. No natural or induced mouse mutants of CP have been identified, but the phenotype of engineered CP knockout mice has been well studied and it largely, but not entirely, parallels the clinical presentation of aceruloplasminemia in humans (Harris et al. 1999; Kenawi et al. 2019). CP null mice accumulate iron in the liver, spleen, brain and retina, and show progressive neurodegeneration. These mice are also more susceptible to oxidative stress, as demonstrated by their enhanced disease severity index in a murine model of inflammatory bowel disease (Bakhautdin et al. 2013). A CP knockout rat has also been generated (Kenawi et al. 2019), and its phenotype is similar to the mouse model and human aceruloplasminemia. In these animals, as in human patients, hepatic and splenic macrophages were not iron loaded. Why this is the case has not yet been resolved. It may suggest that MCFs other than CP are important for macrophage iron release, or that release can occur via an MCF-independent mechanism. Alternatively, the relative paucity of iron in the absence of functional CP may reflect systemic processes, including a preferential redistribution of iron (perhaps as NTBI) to parenchmyal cells such as hepatocytes (Kenawi et al. 2019).
The sex-linked anemia (sla) mouse was first identified in an X-ray induced mutagenesis screen as a strain with a profound anemia (Grewal 1962), and it was the subsequent molecular analysis of these animals that led to the identification of HEPH as the defective gene (Vulpe et al. 1999). The sla mutation is a large in-frame deletion that leads to the loss of 194 amino acids, yet surprisingly, the protein retains some ferroxidase activity. Well before HEPH was identified, extensive physiological characterization of sla mice was carried out, and these studies demonstrated that the animals had reduced iron absorption due to impaired iron efflux from duodenal enterocytes (Pinkerton and Bannerman 1967; Manis 1971). Such observations are completely consistent with HEPH playing a role in increasing the efficiency of FPN-mediated iron export from intestinal epithelial cells. Despite this, when sla mice were placed on an iron deficient diet, their absorption increased to the same level as a wild-type mouse placed on the same diet (Sorbie et al. 1974; Thomson and Valberg 1975), suggesting that the need for HEPH can be overcome when the drive to absorb iron is particularly high. The early studies also showed that the anemia in sla mice was greatest in young animals and largely resolved with age as growth slowed and iron demands decreased. Despite the large deletion in HEPH in sla mice, the fact that the truncated protein (a) only retains 25% of the ferroxidase activity of the wild-type protein and (b) is not appropriately trafficked to the basolateral region of enterocytes, means that its effective function is very limited (Chen et al. 2004; Kuo et al. 2004). Consequently, the phenotypes of whole body HEPH knockout mice and sla mice are very similar, but not identical (Fuqua et al. 2014).
After the gene encoding ZP was identified, HephL1 knockout mice were generated and they showed a surprisingly mild phenotype (Sharma et al. 2019) (i.e. they were overtly normal and were not anemic). ZP had been identified as a protein that may be involved in placental iron transport, but the knockout mice bred normally and knockout animals were not underrepresented in the litters. Interestingly, however, the placentas were 26% larger in these mice (Helman et al. 2021). The only clear physical abnormality displayed by ZP knockout mice was unusually wavy whiskers, and this finding is consistent with the abnormal hair phenotype of the patient carrying HEPHL1 mutations mentioned above. Supporting this observation is the recent identification of HEPHL1 as the gene affected in the Curly Whiskers mouse (Eragene et al. 2019), and demonstration that a mutation in HEPHL1 is responsible for the hair abnormalities in Belted Galloway Cattle (Kuca et al. 2021). While the available data suggest that ZP plays an important role in hair development, whether this role reflects altered iron homeostasis or some other function of ZP has yet to be determined. Whether ZP plays roles in other tissues has not yet been determined.
More recently, mice with disrupted expression of both HEPH and CP have been generated and analysis of their phenotype has clearly shown that both of these MCFs play roles in multiple tissues. Such studies were first carried out by examining the progeny of crosses of Cp knockout and sla mice (Hahn et al. 2004), and more recently by generating animals in which each of these genes has been deleted (Fuqua et al. 2018). These studies have shown that the phenotype arising in the mice when both MCFs are disrupted is more severe than that observed in either of the single mutants. Double knockout mice were severely anemic and had defects in intestinal iron absorption, but they also loaded iron in a broad range of tissues, including the heart, kidney, pancreas, retina and adrenal gland. In these extra-intestinal tissues, little or no iron loading was observed in either single knockout, indicating that the MCFs work together to facilitate iron release from these tissues. Interestingly, even mice lacking both ferroxidases were still able to absorb orally administered iron, but that iron was distributed in an unusual pattern, with particularly high retention in the liver (Fuqua et al. 2018). It is possible that in these mice, the limited ferroxidase activity meant that iron loading onto transferrin was inefficient, and consequently that the level of NTBI was unusually high. NTBI is very efficiently taken up by the liver (Craven et al. 1987). Although there is no report in the literature describing the consequences of the combined deletion of ZP and CP, or ZP and HEPH, our unpublished studies have shown that the progeny of both crosses are viable.
Since an adequate iron supply is required to support cancer cell growth, there are numerous links between the expression of various proteins of iron homeostasis, including the MCFs, and tumor progression (Chen et al. 2019a). Much of the interest in this area in recent years has focused on HEPH. Reduced HEPH protein levels have been associated with more advanced disease in mesothelioma (Crovella et al. 2016), breast cancer (Wang et al. 2017) and colorectal cancer (Brookes et al. 2006), and high HEPH expression has been linked to improved prognosis in lung cancer (Zacchi et al. 2021) and renal clear cell carcinoma (Chen et al. 2019a). In breast cancer, both lower HEPH (Wang et al. 2017) and lower FPN (Pinnix et al. 2010) expression are associated with iron accumulation and more aggressive tumours. Together, these data indicate that reduced iron export favours tumour growth. The recent demonstration that Euchromatic histone-lysine N-methyltransferase 2 (EHMT2) can repress HEPH transcription (Wang et al. 2017) in breast cancer cells makes it a potential therapeutic target for modulating HEPH expression in tumours. Indeed, EHMT2 is frequently elevated in breast cancer (Wang et al. 2017). Reduced HEPH expression has also been linked to enhanced resistance of colon cancer cells to the chemotherapeutic drug methotrexate (Zhang et al. 2021a). In this case, the mechanism involves a regulatory pathway whereby the microRNA miR-24-3p released from cancer-associated fibroblasts acts on colon cancer cells to reduce the activity of the transcription factor CDX2, a major (positive) regulator of the HEPH gene. Although reduced HEPH levels show a clear link to a more severe tumor phenotype, studies with CP have shown the opposite relationship, with increased CP expression being associated with poorer prognosis (Gangoda et al. 2017; Matsuoka et al. 2018; Zhang et al. 2021b). Much of this increase may reflect the fact that CP is an acute phase protein, but some studies have indicated that CP itself can drive cellular changes that promote tumorigenesis (Dai et al. 2020; Zhang et al. 2021b). Understanding how the cellular iron export machinery contributes to tumor progression and exploring the MCFs as therapeutic targets are areas that warrant further investigation.
The need for multiple ferroxidases: tissue and organ-specific roles of the MCFs
As CP is secreted into the plasma, it might be expected that it could be involved in iron mobilization from most cells, but, surprisingly, it only appears to perform this role efficiently for some tissues. In other tissues, either other MCFs are more important, or MCFs work together to coordinate iron efflux. As noted above, the characterization of rare human diseases where MCF function is disturbed and a range of MCF knockout/mutant mouse strains has demonstrated that CP is particularly important for facilitating iron efflux from the liver, and certain cell types in the brain and pancreas (Hellman and Gitlin 2002; Jeong and David 2003; Linder 2016), whereas HEPH is the major MCF functioning in the small intestine (Fuqua et al. 2014). However, more recent studies with mice lacking both CP and HEPH have indicated a more complex picture, with both MCFs contributing to iron efflux from multiple peripheral tissues (Fuqua et al. 2018). Tissue-specific knockouts of particular proteins in mice can be a powerful tool for assessing their function in individual tissues, but very few tissue-specific MCF knockout mice have been generated to date (e.g. HEPH deletion in the intestine (Fuqua et al. 2014) and retina (Wolkow et al. 2012)).
The MCFs clearly function in multiple tissues, but do so with varying efficiencies and in varying combinations. This may reflect factors such as accessibility to circulating CP, varying MCF expression levels, differential subcellular distribution (particularly for membrane-bound MCFs), or even differences in their catalytic profile. A few remarks on the contributions of the MCFs to iron homeostasis in selected tissues are provided below and an overview is provided in Fig. 2.
Relative contributions of CP, HEPH and ZP to iron export from selected tissues. We now know that the MCFs contribute to iron export from multiple tissues, and often from specific cell types within those tissues. For example, in the brain, the MCFs are important for intra-organ iron trafficking. In this diagram, CP, HEPH and ZP are represented by blue, green and yellow balls respectively. For each tissue, the size of the ball represents the relative contribution of that MCF to iron transport from (or within) that tissue. For example, CP appears to be largely, if not solely, responsible for enhancing iron efflux from the liver, whereas in the duodenum, HEPH provides the majority of the ferroxidase activity, with CP contributing, albeit less efficiently, in some circumstances. In a number of tissues, both CP and HEPH appear to contribute significantly. The contributions of ZP to body iron homeostasis have yet to be firmly established, but its role in hair development is well supported. It is presumed a ferroxidase is required for efficient iron transport by the placenta to the fetus, but the identity of that ferroxidase remains uncertain, and is represented here by a grey ball. (Color figure online)
Liver
The liver is quantitatively the major iron storage organ in the body, so it is critically important that iron is efficiently mobilized from the liver when required (Anderson and Frazer 2005). CP is clearly the major MCF involved in liver iron mobilization, as hepatic iron levels increase substantially when CP is missing or dysfunctional (Harris et al. 1999; Piperno and Alessio 2018; Kenawi et al. 2019; Marchi et al. 2019). Loss of HEPH either globally or specifically in the small intestine leads to a reduction in dietary iron absorption, and consequently hepatic iron levels are low (Fuqua et al. 2014). If HEPH played a significant role in hepatic iron release, liver iron levels might be expected to increase, or at least not decrease, but this is not the case. The low expression of HEPH in the liver is consistent with it playing a limited role in this organ (Vulpe et al. 1999; Frazer et al. 2001; Hudson et al. 2009). Nevertheless, studies with CP/HEPH double knockout mice have suggested that lack of HEPH in the intestine may influence the kinetics of iron flux through the liver (Fuqua et al. 2018), and this requires further investigation.
Small intestine
The best characterized role of HEPH is its contribution to dietary iron absorption, as it is required at the basolateral membrane of enterocytes to facilitate the efficient export of iron into the portal circulation (Fuqua et al. 2014; Fuqua et al. 2018; Doguer et al. 2017). Early studies with sla mice demonstrated this phenotype, even though at the time HEPH had not been identified. Heph knockout mice show a similar phenotype to sla animals, but loss of HEPH does not completely block iron absorption and the anemia observed in intestine-specific HEPH knockouts is relatively mild (Fuqua et al. 2014). Indeed, the anemia in these mice is milder than that of whole body HEPH knockout mice, indicating that HEPH makes contributions to iron supply to the plasma from tissues other than the gut. The fact that dietary iron absorption can continue even in the absence of HEPH indicates that either another iron oxidase performs this function or that ferroxidase activity is not essential for iron export from enterocytes. Under normal physiological conditions, CP appears to make little contribution to dietary iron absorption, but when body iron demands are particularly high, such as following hemolysis, CP can help to mobilize iron from enterocytes (Cherukuri et al. 2005). The apparent lower efficiency of CP in facilitating dietary iron absorption may indicate that the precise subcellular location of the ferroxidase activity is important. Although HEPH is generally considered to act on the basolateral membrane and some localization studies support this contention (Han and Kim 2007), other data suggest HEPH could be located in an intracellular compartment very close to the membrane, rather than on the basolateral membrane itself (Kuo et al. 2004). Intriguingly, a ferroxidase activity that cannot be attributed to CP or HEPH has been detected in rodent enterocytes (Ranganathan et al. 2012), but its identity is not yet known. It has also been demonstrated that HEPH appears to be important for iron absorption under normal physiological conditions, but is not limiting when dietary iron absorption is stimulated by iron deficiency or following haemolytic anemia (Doguer et al. 2017), a finding consistent with early studies using sla mice (Sorbie et al. 1974) and supporting the suggestion that other ferroxidase activities are present.
Central nervous system
The important role the MCFs, and particularly CP, play in the CNS has been extensively documented (Piperno and Alessio 2018). Progressive neurodegeneration and retinopathy are characteristic features of aceruloplasminemia and reflect iron deposition in these tissues associated with loss of CP activity (Kono 2013; Marchi et al. 2019). Thus, CP can be considered a neuroprotective molecule. It is the GPI-linked form of CP in astrocytes that appears to be particularly important in brain iron metabolism, as it facilitates the export of iron from astrocytes, which makes this iron available for other types of cells in the brain (Jeong and David 2006; Marchi et al. 2019). When CP is missing or defective, not only is this iron supply disrupted, but iron can accumulate within astrocytes to cytotoxic levels and this in turn may exacerbate the neurodegeneration (Kono 2013). HEPH has also been shown to play a significant role in maintaining iron homeostasis in the brain, and mice lacking both functional CP and HEPH show greater iron accumulation in multiple brain regions than either of the individual mutant strains (Zhao et al. 2015; Zheng et al. 2018b). The double knockout animals also showed significant learning and memory defects (Zheng et al. 2018b). Interestingly, while CP is predominantly expressed in astrocytes, HEPH is most strongly expressed in oligodendrocytes. Loss of CP function in astrocytes or HEPH function in oligodendrocytes leads to iron accumulation in each of these cell types and concomitant oxidative stress (Chen et al. 2019b). Loss of HEPH leads to iron accumulation in oligodendrocytes in the gray matter, but not in the white matter, with a compensatory increase in CP expression in the white matter cells explaining the difference (Schulz et al. 2011). The retina is another component of the CNS where MCFs play important roles. Retinal pigment epithelial (RPE) cells express both CP and HEPH, and mutation or loss of these proteins is associated with iron accumulation in these cells and retinal degeneration (Hahn et al. 2004; Hadziahmetovic et al. 2008; Wolkow et al. 2012). These ferroxidases play a very limited role in photoreceptor cells, but since global MCF knockout mice show more severe retinal damage than mice lacking the CP and HEPH only in the RPE, these MCFs must be contributing to retinal iron homeostasis via their roles in some other cell type(s) (Wolkow et al. 2012).
Pancreas
The pancreas is an organ that is particularly prone to iron loading (Kimita and Petrov 2020), so ensuring it has an efficient mechanism for divesting itself of iron is critical for its normal function. Diabetes is a common feature of aceruloplasminemia (Piperno and Alessio 2018), but interestingly, there is no overt iron loading in the endocrine pancreas in this condition (Kato et al. 1997), suggesting the effects on the endocrine cells are secondary to iron loading in other cell types. In mice, loss of either CP or HEPH alone appears to have little effect on iron levels in the pancreas, but when both genes are ablated together, significant iron loading is observed in this organ (Chen et al. 2018; Fuqua et al. 2018). Most of this iron loading is observed in the exocrine pancreas (i.e. the acinar cells) rather than in the Islets (i.e. the endocrine pancreas). This iron loading causes oxidative damage and enhanced production of plasma lipase and trypsin, which are typically elevated when the exocrine pancreas is damaged, but there were no significant changes in insulin levels (Chen et al. 2018). These studies clearly show the important protective role the MCFs play in the pancreas.
Placenta
Given the importance of MCFs in iron export from other tissues (Vashchenko and MacGillivray 2013), it is likely that a placental ferroxidase is required for efficient transfer of iron from the mother to the fetus, particularly in the final weeks of pregnancy. Although newborn sla mice, which essentially lack functional HEPH, are anemic and have reduced total body iron (Bannerman et al. 1973), radioactive iron transport studies did not indicate a defect in placental iron transfer (Kingston et al. 1978). Fetal CP has also been suggested to facilitate the export of iron from the placenta based on studies in BeWo cells (Danzeisen et al. 2000, 2002), but studies with CP knockout mice argue against CP playing a major role in iron delivery to the fetus (Harris et al. 1999). When ZP was identified, it was initially considered to be a putative placental MCF based on its high expression in the placenta at embryonic day 18 and its major contribution to the ferroxidase activity of BeWo cells (Chen et al. 2010). However, highest expression was observed in the implantation chamber at embryonic day 7, before the definitive placenta has formed. A recent study has shown that when ZP was knocked out in the labyrinth, the nutrient transporting layer of the placenta, there was no change in hemoglobin or total fetal iron content compared with littermate controls (Helman et al. 2021). Dissection of late-gestation placentas to separate the various layers revealed that expression of Hephl1, the gene encoding ZP, is high in the maternal decidua, but undetectable in the labyrinth, making it unlikely to play a role in iron export to the fetus (Helman et al. 2021). Furthermore, no iron phenotype was found under normal conditions when ZP was knocked out in the maternal decidua, but the placentas were 26% heavier, suggesting that ZP may play a role in placental development (Helman et al. 2021). Thus, it appears that no one MCF plays a dominant role in placental iron transport, but the studies conducted to date do not exclude a combined role of multiple ferroxidases.
Hair
An association between iron deficiency and hair loss has been recognized for some time, but the mechanisms involved are poorly understood (Trost et al. 2006; Almohanna et al. 2019). The MCFs may play an important role in hair development as disruption of either HEPH or ZP has been associated with an abnormal hair phenotype. The importance of ZP for maintaining normal hair growth was noted above. A patient carrying a mutation in HEPHL1, as well as Zp−/− and Zpcw/cw mice, all exhibit loss of ferroxidase activity and develop similar hair abnormities, with reduced lysyl oxidase activity in fibroblasts (Eragene et al. 2019; Sharma et al. 2019). A recent genome-wide association study in Belted Galloway cattle with hypotrichosis demonstrated the alopecia phenotype is caused by a mutant variant in HEPHL1 (Kuca et al. 2021). Together, these studies suggest that the skin-expressed ZP may play an important role in facilitating hair growth and preventing hair disorders. HEPH may also play a role in normal hair development. Pre-weaning pups born to or nursed by Heph knockout dams developed truncal hair loss (the “mask” phenotype) and systemic iron deficiency (Wolkow et al. 2012; Zhou 2020). Transcriptomic studies have indicated that the WNT/β-catenin signaling pathway, the key regulatory pathway for hair growth and hair follicle development, was downregulated in the affected skin (Zhou 2020). Preliminary data suggest that decreased expression and activity of stearoyl coenzyme A desaturase, an iron-containing enzyme essential for WNT palmitoylation (Stoffel et al. 2017), may provide the link between disturbed iron homeostasis and hair loss in the Heph deficient mice (Zhou 2020). In addition, single nucleotide polymorphisms in the HEPH gene have been associated with male pattern baldness in humans (Hagenaars et al. 2017), however, whether the association reflects HEPH itself or the nearby androgen receptor gene has yet to be established.
Other tissues
Loss of either CP or HEPH in mice does not lead to overt iron accumulation in the heart, kidney or in adipose tissue, but when both of these MCFs are deleted, iron loading is observed (Qian et al. 2007; Jiang et al. 2016b; Fuqua et al. 2018). This finding suggests that the combined actions of these two ferroxidases are important in maintaining iron homeostasis in these tissues. In the kidney, loss of CP and HEPH leads to iron loading in both the medulla and cortex, and is associated with proteinuria and elevated urinary iron, consistent with renal damage (Jiang et al. 2016a). Some histological changes, particularly in the medulla, were also observed. In the heart, the iron loading in CP/HEPH double knockout mice was particularly apparent in cardiac myocytes (Fuqua et al. 2018). The iron loading that is observed in Cp−/−/Heph−/− adipocytes was associated with decreased leptin and adiponectin mRNA expression (Zheng et al. 2018a). Fasting glucose levels were significantly increased in the double knockout mice, and both glucose and insulin tolerance were impaired. This finding is of clinical interest given the recent observation that adipocyte iron levels regulate intestinal lipid absorption (Zhang et al. 2021c), and raises the possibility that pharmacologically increasing MCF levels could prove beneficial by limiting lipid intake.
Future areas of research
Although CP has been studied for many decades, and HEPH and ZP have been investigated for more than 20 and 10 years respectively, there are still many aspects of their biology that are incompletely understood. The following list highlights some of the areas where further investigation is warranted.
-
(1)
Although we have some valuable clues as to how the MCFs function in conjunction with FPN to facilitate efficient iron export, the precise details of this process remain unclear, and it is possible that MCF/FPN interactions will vary depending on the tissue and the MCF involved. Some key questions include: Do the membrane-tethered MCFs act in the same way as soluble CP? Is the oxidation of recently transported ferrous iron necessary for its release from FPN? What is the link between MCF action and FPN stability?
-
(2)
Understanding the structure of the MCFs individually, and when complexed with FPN (and potentially other proteins) will be extremely helpful in elucidating the mechanisms of MCF action.
-
(3)
The nature of the interactions of the MCFs with transferrin has yet to be defined.
-
(4)
How the three MCFs work together to co-ordinately regulate body iron homeostasis is incompletely understood. Studies with single and multiple MCF knockout in specific tissues are beginning to answer these questions, but more extensive investigations are required.
-
(5)
Why MCF ferroxidase activity is apparently in gross excess in the plasma and some other tissues needs to be resolved.
-
(6)
Are there ferroxidases other than CP, HEPH and ZP that play important roles in body iron trafficking?
-
(7)
Does ZP have physiological roles in addition to its described function in hair development?
-
(8)
Which MCFs contribute to iron recycling through macrophages and what are the relative contributions of cell-specific and systemic mechanisms?
-
(9)
The cell biology of the MCFs, particularly the membrane bound forms, is not well understood and warrants further investigation. This is particularly important as changes in the subcellular localization of these proteins appears to be a significant mode of regulation, at least in response to altered iron availability.
-
(10)
It is known that each of the MCFs is able to oxidize substrates in addition to Fe2+, but how broad this spectrum of substrates is (particularly for HEPH and ZP) has not been determined and the physiological relevance of many of these ‘non-iron’ activities has yet to be defined.
-
(11)
Why does the loss of ferroxidase activity in CP or HEPH knockout mice not lead to a phenotype as severe as might be expected, either in terms of tissue iron loading or the anemia that develops (Prohaska 2011)? While redundancy between the MCFs might explain this observation to some extent, other factors may also be involved.
-
(12)
How does lack of HEPH contribute to anemia beyond its role in intestinal iron absorption? For example, why are Hephint/intCp−/− mice (with knockout of HEPH only in the intestine) not more anemic than Cp knockout mice, while Heph−/−/Cp−/− mice (with global deletion of both HEPH and CP) have a much more severe anemia?
-
(13)
The demonstration that only specific cells in various tissues of Heph/Cp double knockout mice retain iron (Fuqua et al. 2018) suggests a mosaic expression of the MCFs. Understanding MCF function at the single-cell resolution is thus essential to fully understand their biology.
-
(14)
Do the MCFs have sex-specific roles and/or are there quantitative differences in their impact between the sexes? We have some understanding of their role in female specific tissues, but historically, most experimental studies have been carried out in males only, or in mixed sex groups.
-
(15)
What roles do the MCFs play in the pathogenesis of various diseases? Do they generally play a role as antioxidants as appears to be the case with CP? Understanding their role in CNS disorders is particularly significant. Given the association of iron accumulation in specific regions of the brain with multiple neurodegenerative disorders, including both Alzheimer’s disease and Parkinson’s disease, understanding the roles of the MCFs may provide important insight into the pathophysiology of these disorders.
-
(16)
Perhaps the most exciting future direction of MCF research is the exploration of whether modulating MCF function could provide a therapeutic avenue for human diseases. Either blocking or enhancing MCF expression could have application in different situations, and altering MCF functions could be relevant to either iron-related pathologies or to some of their non-iron roles. As an example, there is growing evidence that reduced HEPH expression plays a role in the progression of multiple cancers, so increasing its activity has therapeutic potential.
Concluding remarks
Investigation of the mammalian MCFs over the past several decades has increased our collective understanding of the complex process of iron homeostasis. More recent work has demonstrated new, potentially important functions for these proteins, but additional experimentation is required to make definitive conclusions about possible other physiological roles. Collectively, these advances have led to postulates regarding MCF function and development of chronic diseases in humans, which has logically led to speculation that therapeutic targeting of these proteins could be a fruitful area for future research.
References
Al Yemni E et al (2019) Integrated analysis of whole exome sequencing and copy number evaluation in Parkinson’s disease. Sci Rep 9:1–9
Albury CL, Stuart S, Haupt LM, Griffiths LR (2017) Ion channelopathies and migraine pathogenesis. Mol Genet Genomics 292:729–739. https://doi.org/10.1007/s00438-017-1317-1
Almohanna HM, Ahmed AA, Tsatalis JP, Tosti A (2019) The role of vitamins and minerals in hair loss: a review. Dermatol Ther 9:51–70
Anderson GJ, Frazer DM (2005) Hepatic iron metabolism. Semin Liver Dis 25:420–432. https://doi.org/10.1055/s-2005-923314
Anderson GJ, Frazer DM (2017) Current understanding of iron homeostasis. Am J Clin Nutr 106:1559S-1566S. https://doi.org/10.3945/ajcn.117.155804
Anderson GJ, Vulpe CD (2009) Mammalian iron transport. Cell Mol Life Sci 66:3241–3261. https://doi.org/10.1007/s00018-009-0051-1
Attieh ZK, Mukhopadhyay CK, Seshadri V, Tripoulas NA, Fox PL (1999) Ceruloplasmin ferroxidase activity stimulates cellular iron uptake by a trivalent cation-specific transport mechanism. J Biol Chem 274:1116–1123. https://doi.org/10.1074/jbc.274.2.1116
Ayton S, Lei P, Duce JA, Wong BX, Sedjahtera A, Adlard PA, Bush AI, Finkelstein DI (2013) Ceruloplasmin dysfunction and therapeutic potential for Parkinson disease. Ann Neurol 73:554–559. https://doi.org/10.1002/ana.23817
Bakhautdin B, Febbraio M, Goksoy E, de la Motte CA, Gulen MF, Childers EP, Hazen SL, Li X, Fox PL (2013) Protective role of macrophage-derived ceruloplasmin in inflammatory bowel disease. Gut 62:209–219. https://doi.org/10.1136/gutjnl-2011-300694
Bannerman RM, Bannerman CE, Kingston PJ (1973) Hereditary iron deficiency: X-linked anaemia (sla) in newborn and suckling mice. Br J Haematol 25:280
Bento I, Peixoto C, Zaitsev VN, Lindley PF (2007) Ceruloplasmin revisited: structural and functional roles of various metal cation-binding sites. Acta Crystallogr D 63:240–248. https://doi.org/10.1107/s090744490604947x
Bielli P, Calabrese L (2002) Structure to function relationships in ceruloplasmin: a “moonlighting” protein. Cell Mol Life Sci 59:1413–1427. https://doi.org/10.1007/s00018-002-8519-2
Brookes MJ et al (2006) Modulation of iron transport proteins in human colorectal carcinogenesis. Gut 55:1449–1460. https://doi.org/10.1136/gut.2006.094060
Brown MA, Stenberg LM, Mauk AG (2002) Identification of catalytically important amino acids in human ceruloplasmin by site-directed mutagenesis. FEBS Lett 520:8–12. https://doi.org/10.1016/s0014-5793(02)02652-2
Cha MK, Kim IH (1999) Ceruloplasmin has a distinct active site for the catalyzing glutathione-dependent reduction of alkyl hydroperoxide. Biochem 38:12104–12110. https://doi.org/10.1021/bi990444b
Chapman AL et al (2013) Ceruloplasmin is an endogenous inhibitor of myeloperoxidase. J Biol Chem 288:6465–6477. https://doi.org/10.1074/jbc.M112.418970
Chen H et al (2004) Hephaestin is a ferroxidase that maintains partial activity in sex-linked anemia mice. Blood 103:3933–3939. https://doi.org/10.1182/blood-2003-09-3139
Chen H, Huang G, Su T, Gao H, Attieh ZK, McKie AT, Anderson GJ, Vulpe CD (2006) Decreased hephaestin activity in the intestine of copper-deficient mice causes systemic iron deficiency. J Nutr 136:1236–1241
Chen H et al (2010) Identification of zyklopen, a new member of the vertebrate multicopper ferroxidase family, and characterization in rodents and human cells. J Nutr 140:1728–1735. https://doi.org/10.3945/jn.109.117531
Chen M, Zheng J, Liu G, Xu E, Wang J, Fuqua BK, Vulpe CD, Anderson GJ, Chen H (2018) Ceruloplasmin and hephaestin jointly protect the exocrine pancreas against oxidative damage by facilitating iron efflux. Redox Biol 17:432–439. https://doi.org/10.1016/j.redox.2018.05.013
Chen Y, Fan Z, Yang Y, Gu C (2019a) Iron metabolism and its contribution to cancer. Int J Oncol 54:1143–1154
Chen Z et al (2019b) Multi-copper ferroxidase deficiency leads to iron accumulation and oxidative damage in astrocytes and oligodendrocytes. Sci Rep 9:9437. https://doi.org/10.1038/s41598-019-46019-9
Chepelev NL, Willmore WG (2011) Regulation of iron pathways in response to hypoxia. Free Radic Biol Med 50:645–666. https://doi.org/10.1016/j.freeradbiomed.2010.12.023
Cherukuri S, Potla R, Sarkar J, Nurko S, Harris ZL, Fox PL (2005) Unexpected role of ceruloplasmin in intestinal iron absorption. Cell Metab 2:309–319. https://doi.org/10.1016/j.cmet.2005.10.003
Chu YL, Sauble EN, Cabrera A, Roth A, Ackland ML, Mercer JF, Linder MC (2012) Lack of ceruloplasmin expression alters aspects of copper transport to the fetus and newborn, as determined in mice. Biometals 25:373–382. https://doi.org/10.1007/s10534-011-9509-3
Conley L, Geurs TL, Levin LA (2005) Transcriptional regulation of ceruloplasmin by an IL-6 response element pathway. Brain Res Mol Brain Res 139:235–241. https://doi.org/10.1016/j.molbrainres.2005.05.027
Craven CM, Alexander J, Eldridge M, Kushner JP, Bernstein S, Kaplan J (1987) Tissue distribution and clearance kinetics of non-transferrin-bound iron in the hypotransferrinemic mouse: a rodent model for hemochromatosis. Proc Natl Acad Sci USA 84:3457–3461
Crovella S et al (2016) Iron signature in asbestos-induced malignant pleural mesothelioma: a population-based autopsy study. J Toxicol Environ Health A 79:129–141. https://doi.org/10.1080/15287394.2015.1123452
Członkowska A, Litwin T, Dusek P, Ferenci P, Lutsenko S, Medici V, Rybakowski JK, Weiss KH, Schilsky ML (2018) Wilson disease. Nat Rev Dis Primers 4:21. https://doi.org/10.1038/s41572-018-0018-3
Dai L, Niu J, Feng Y (2020) Knockdown of long non-coding RNA LINC00176 suppresses ovarian cancer progression by BCL3-mediated down-regulation of ceruloplasmin. J Cell Mol Med 24:202–213. https://doi.org/10.1111/jcmm.14701
Danzeisen R, Ponnambalam S, Lea RG, Page K, Gambling L, McArdle HJ (2000) The effect of ceruloplasmin on iron release from placental (BeWo) cells; evidence for an endogenous Cu oxidase. Placenta 21:805–812. https://doi.org/10.1053/plac.2000.0582
Danzeisen R, Fosset C, Chariana Z, Page K, David S, McArdle HJ (2002) Placental ceruloplasmin homolog is regulated by iron and copper and is implicated in iron metabolism. Am J Physiol Cell Physiol 282:C472-478. https://doi.org/10.1152/ajpcell.00019.2001
Das D, Tapryal N, Goswami SK, Fox PL, Mukhopadhyay CK (2007) Regulation of ceruloplasmin in human hepatic cells by redox active copper: identification of a novel AP-1 site in the ceruloplasmin gene. Biochem J 402:135–141. https://doi.org/10.1042/bj20060963
De Domenico I, Ward DM, di Patti MC, Jeong SY, David S, Musci G, Kaplan J (2007) Ferroxidase activity is required for the stability of cell surface ferroportin in cells expressing GPI-ceruloplasmin. EMBO J 26:2823–2831. https://doi.org/10.1038/sj.emboj.7601735
Deshpande CN, Xin V, Lu Y, Savage T, Anderson GJ, Jormakka M (2017) Large scale expression and purification of secreted mouse hephaestin. PLoS ONE 12:e0184366. https://doi.org/10.1371/journal.pone.0184366
Dlouhy AC, Bailey DK, Steimle BL, Parker HV, Kosman DJ (2019) Fluorescence resonance energy transfer links membrane ferroportin, hephaestin but not ferroportin, amyloid precursor protein complex with iron efflux. J Biol Chem 294:4202–4214. https://doi.org/10.1074/jbc.RA118.005142
Doguer C, Ha J-H, Gulec S, Vulpe CD, Anderson GJ, Collins JF (2017) Intestinal hephaestin potentiates iron absorption in weanling, adult, and pregnant mice under physiological conditions. Blood Adv 1:1335–1346. https://doi.org/10.1182/bloodadvances.2017008359
Eragene S, Stewart JJ, Samuel-Constanzo JI, Tan T, Esgdaille NZ, Bigiarelli KJ, DaCosta VD, Jimenez H, King TR (2019) The mouse curly whiskers (cw) mutations are recessive alleles of hephaestin-like 1 (Hephl1). Mol Genet Metab Rep 20:100478. https://doi.org/10.1016/j.ymgmr.2019.100478
Fox PL, Mazumder B, Ehrenwald E, Mukhopadhyay CK (2000) Ceruloplasmin and cardiovascular disease. Free Radic Biol Med 28:1735–1744. https://doi.org/10.1016/s0891-5849(00)00231-8
Frazer DM, Vulpe CD, McKie AT, Wilkins SJ, Trinder D, Cleghorn GJ, Anderson GJ (2001) Cloning and gastrointestinal expression of rat hephaestin: relationship to other iron transport proteins. Am J Physiol Gastrointest Liver Physiol 281:G931-939. https://doi.org/10.1152/ajpgi.2001.281.4.G931
Fuqua BK et al (2014) The multicopper ferroxidase hephaestin enhances intestinal iron absorption in mice. PLoS ONE 9:e98792. https://doi.org/10.1371/journal.pone.0098792
Fuqua BK et al (2018) Severe iron metabolism defects in mice with double knockout of the multicopper ferroxidases hephaestin and ceruloplasmin. Cell Mol Gastroenterol Hepatol 6:405–427. https://doi.org/10.1016/j.jcmgh.2018.06.006
Gangoda L, Liem M, Ang CS, Keerthikumar S, Adda CG, Parker BS, Mathivanan S (2017) Proteomic profiling of exosomes secreted by breast cancer cells with varying metastatic potential. Proteomics. https://doi.org/10.1002/pmic.201600370
Gitlin JD (1988) Transcriptional regulation of ceruloplasmin gene expression during inflammation. J Biol Chem 263:6281–6287
Gitlin JD, Schroeder JJ, Lee-Ambrose LM, Cousins RJ (1992) Mechanisms of caeruloplasmin biosynthesis in normal and copper-deficient rats. Biochem J 282(Pt 3):835–839. https://doi.org/10.1042/bj2820835
Goldstein IC, Charo IF (1983) Ceruloplasmin: an acute phase reactant and antioxidant. In: Pick E (ed) Lymphokines 8, vol 8. Academic Press, London
Grewal MS (1962) A sex-linked anaemia in the mouse. Genet Res 3:238–247. https://doi.org/10.1017/S0016672300035023
Gulec S, Collins JF (2014) Silencing the Menkes copper-transporting ATPase (Atp7a) gene in rat intestinal epithelial (IEC-6) cells increases iron flux via transcriptional induction of ferroportin 1 (Fpn1). J Nutr 144:12–19. https://doi.org/10.3945/jn.113.183160
Ha-Duong NT, Eid C, Hemadi M, El Hage Chahine JM (2010) In vitro interaction between ceruloplasmin and human serum transferrin. Biochem 49:10261–10263. https://doi.org/10.1021/bi1014503
Hadziahmetovic M et al (2008) Ceruloplasmin/hephaestin knockout mice model morphologic and molecular features of AMD. Invest Ophthalmol vis Sci 49:2728–2736. https://doi.org/10.1167/iovs.07-1472
Hagenaars SP et al (2017) Genetic prediction of male pattern baldness. PLoS Genet 13:e1006594
Hahn P, Qian Y, Dentchev T, Chen L, Beard J, Harris ZL, Dunaief JL (2004) Disruption of ceruloplasmin and hephaestin in mice causes retinal iron overload and retinal degeneration with features of age-related macular degeneration. Proc Natl Acad Sci USA 101:13850–13855. https://doi.org/10.1073/pnas.0405146101
Han O, Kim EY (2007) Colocalization of ferroportin-1 with hephaestin on the basolateral membrane of human intestinal absorptive cells. J Cell Biochem 101:1000–1010. https://doi.org/10.1002/jcb.21392
Harris ZL, Durley AP, Man TK, Gitlin JD (1999) Targeted gene disruption reveals an essential role for ceruloplasmin in cellular iron efflux. Proc Natl Acad Sci USA 96:10812–10817. https://doi.org/10.1073/pnas.96.19.10812
Hellman NE, Gitlin JD (2002) Ceruloplasmin metabolism and function. Annu Rev Nutr 22:439–458. https://doi.org/10.1146/annurev.nutr.22.012502.114457
Hellman NE, Kono S, Mancini GM, Hoogeboom AJ, De Jong GJ, Gitlin JD (2002) Mechanisms of copper incorporation into human ceruloplasmin. J Biol Chem 277:46632–46638. https://doi.org/10.1074/jbc.M206246200
Helman SL et al (2021) The placental ferroxidase zyklopen is not essential for iron transport to the fetus in mice. J Nutr 151:2541–2550. https://doi.org/10.1093/jn/nxab174
Hinoi T, Gesina G, Akyol A, Kuick R, Hanash S, Giordano TJ, Gruber SB, Fearon ER (2005) CDX2-regulated expression of iron transport protein hephaestin in intestinal and colonic epithelium. Gastroenterology 128:946–961
Hudson DM, Krisinger MJ, Griffiths TA, Macgillivray RT (2008) Neither human hephaestin nor ceruloplasmin forms a stable complex with transferrin. J Cell Biochem 103:1849–1855. https://doi.org/10.1002/jcb.21566
Hudson DM, Curtis SB, Smith VC, Griffiths TA, Wong AY, Scudamore CH, Buchan AM, Macgillivray RT (2009) Human hephaestin expression is not limited to enterocytes of the GI tract but is also found in the antrum, the enteric nervous system and pancreatic {beta}-cells. Am J Physiol Gastrointest Liver Physiol. https://doi.org/10.1152/ajpgi.00453.2009
Jeong SY, David S (2003) Glycosylphosphatidylinositol-anchored ceruloplasmin is required for iron efflux from cells in the central nervous system. J Biol Chem 278:27144–27148. https://doi.org/10.1074/jbc.M301988200
Jeong SY, David S (2006) Age-related changes in iron homeostasis and cell death in the cerebellum of ceruloplasmin-deficient mice. J Neurosci 26:9810–9819. https://doi.org/10.1523/JNEUROSCI.2922-06.2006
Ji J, Zhou Y, Hao S, Wang Q, Li K, Qiao T (2015) Low expression of ferroxidases is implicated in the iron retention in human atherosclerotic plaques. Biochem Biophys Res Commun 464:1134–1138. https://doi.org/10.1016/j.bbrc.2015.07.091
Ji C, Steimle BL, Bailey DK, Kosman DJ (2018) The ferroxidase hephaestin but not amyloid precursor protein is required for ferroportin-supported iron efflux in primary hippocampal neurons. Cell Mol Neurobiol 38:941–954. https://doi.org/10.1007/s10571-017-0568-z
Jiang R et al (2015) Hephaestin and ceruloplasmin play distinct but interrelated roles in iron homeostasis in mouse brain. J Nutr 145:1003–1009. https://doi.org/10.3945/jn.114.207316
Jiang B et al (2016a) Hephaestin and ceruloplasmin facilitate iron metabolism in the mouse kidney. Sci Rep 6:1–11
Jiang X, Gao M, Chen Y, Liu J, Qi S, Ma J, Zhang Z, Xu Y (2016b) EPO-dependent induction of erythroferrone drives hepcidin suppression and systematic iron absorption under phenylhydrazine-induced hemolytic anemia. Blood Cells Mol Dis 58:45–51. https://doi.org/10.1016/j.bcmd.2016.02.005
Jumper J et al (2021) Highly accurate protein structure prediction with AlphaFold. Nature 596:583–589
Jursa T, Smith DR (2009) Ceruloplasmin alters the tissue disposition and neurotoxicity of manganese, but not its loading onto transferrin. Toxicol Sci 107:182–193. https://doi.org/10.1093/toxsci/kfn231
Kato T, Daimon M, Kawanami T, Ikezawa Y, Sasaki H, Maeda K (1997) Islet changes in hereditary ceruloplasmin deficiency. Hum Pathol 28:499–502
Kenawi M et al (2019) Ceruloplasmin deficiency does not induce macrophagic iron overload: lessons from a new rat model of hereditary aceruloplasminemia. FASEB J 33:13492–13502. https://doi.org/10.1096/fj.201901106R
Kimita W, Petrov MS (2020) Iron metabolism and the exocrine pancreas. Clin Chim Acta 511:167–176
Kingston PJ, Bannerman CE, Bannerman RM (1978) Iron deficiency anaemia in newborn sla mice: a genetic defect of placental iron transport. Br J Haematol 40:265–276. https://doi.org/10.1111/j.1365-2141.1978.tb03663.x
Kono S (2013) Aceruloplasminemia: an update. Int Rev Neurobiol 110:125–151
Kono S, Yoshida K, Tomosugi N, Terada T, Hamaya Y, Kanaoka S, Miyajima H (2010) Biological effects of mutant ceruloplasmin on hepcidin-mediated internalization of ferroportin. Biochim Biophys Acta 1802:968–975. https://doi.org/10.1016/j.bbadis.2010.07.011
Kotarsky H, Karikoski R, Mörgelin M, Marjavaara S, Bergman P, Zhang D-L, Smet J, Van Coster R, Fellman V (2010) Characterization of complex III deficiency and liver dysfunction in GRACILE syndrome caused by a BCS1L mutation. Mitochondrion 10:497–509
Kuca T, Marron BM, Jacinto JGP, Paris JM, Gerspach C, Beever JE, Drögemüller C (2021) A nonsense variant in hephaestin like 1 (HEPHL1) is responsible for congenital hypotrichosis in Belted galloway cattle. Genes 12:643
Kuo YM, Su T, Chen H, Attieh Z, Syed BA, McKie AT, Anderson GJ, Gitschier J, Vulpe CD (2004) Mislocalisation of hephaestin, a multicopper ferroxidase involved in basolateral intestinal iron transport, in the sex linked anaemia mouse. Gut 53:201–206
Lee GR, Nacht S, Lukens JN, Cartwright GE (1968) Iron metabolism in copper-deficient swine. J Clin Invest 47:2058–2069. https://doi.org/10.1172/JCI105891
Lee SH, Lancey R, Montaser A, Madani N, Linder MC (1993) Ceruloplasmin and copper transport during the latter part of gestation in the rat. Proc Soc Exp Biol Med 203:428–439. https://doi.org/10.3181/00379727-203-43619
Lee SM, Attieh ZK, Son HS, Chen H, Bacouri-Haidar M, Vulpe CD (2012) Iron repletion relocalizes hephaestin to a proximal basolateral compartment in polarized MDCK and Caco2 cells. Biochem Biophys Res Commun 421:449–455. https://doi.org/10.1016/j.bbrc.2012.04.008
Linder MC (2016) Ceruloplasmin and other copper binding components of blood plasma and their functions: an update. Metallomics 8:887–905. https://doi.org/10.1039/c6mt00103c
Lindley PF, Card G, Zaitseva I, Zaitsev V, Reinhammar B, Selin-Lindgren E, Yoshida K (1997) An X-ray structural study of human ceruloplasmin in relation to ferroxidase activity. J Biol Inorg 2:454–463
Lutsenko S, LeShane ES, Shinde U (2007) Biochemical basis of regulation of human copper-transporting ATPases. Arch Biochem Biophys 463:134–148. https://doi.org/10.1016/j.abb.2007.04.013
Maher BH et al (2012) An X chromosome association scan of the Norfolk Island genetic isolate provides evidence for a novel migraine susceptibility locus at Xq12. PLoS ONE 7:e37903
Manis J (1971) Intestinal iron-transport defect in the mouse with sex-linked anemia. Am J Physiol 220:135–139
Marchi G, Busti F, Lira Zidanes A, Castagna A, Girelli D (2019) Aceruloplasminemia: a severe neurodegenerative disorder deserving an early diagnosis. Front Neurosci 13:325
Marques L, Auriac A, Willemetz A, Banha J, Silva B, Canonne-Hergaux F, Costa L (2012) Immune cells and hepatocytes express glycosylphosphatidylinositol-anchored ceruloplasmin at their cell surface. Blood Cells Mol Dis 48:110–120. https://doi.org/10.1016/j.bcmd.2011.11.005
Matsuoka R, Shiba-Ishii A, Nakano N, Togayachi A, Sakashita S, Sato Y, Minami Y, Noguchi M (2018) Heterotopic production of ceruloplasmin by lung adenocarcinoma is significantly correlated with prognosis. Lung Cancer 118:97–104. https://doi.org/10.1016/j.lungcan.2018.01.012
Mazumder B, Sampath P, Fox PL (2006) Translational control of ceruloplasmin gene expression: beyond the IRE. Biol Res 39:59–66. https://doi.org/10.4067/s0716-97602006000100007
McCarthy RC, Kosman DJ (2013) Ferroportin and exocytoplasmic ferroxidase activity are required for brain microvascular endothelial cell iron efflux. J Biol Chem 288:17932–17940. https://doi.org/10.1074/jbc.M113.455428
McCormack W, Dorsky R, Wright S, Rainier J, Davis D, Skliar M (2013) Consolidated hearing committee report: complaint—research misconduct. (University of Utah).
Meyer LA, Durley AP, Prohaska JR, Harris ZL (2001) Copper transport and metabolism are normal in aceruloplasminemic mice. J Biol Chem 276:36857–36861. https://doi.org/10.1074/jbc.M105361200
Mostad EJ, Prohaska JR (2011) Glycosylphosphatidylinositol-linked ceruloplasmin is expressed in multiple rodent organs and is lower following dietary copper deficiency. Exp Biol Med 236:298–308. https://doi.org/10.1258/ebm.2010.010256
Mukhopadhyay CK, Fox PL (1998) Ceruloplasmin copper induces oxidant damage by a redox process utilizing cell-derived superoxide as reductant. Biochem 37:14222–14229. https://doi.org/10.1021/bi981137t
Mukhopadhyay CK, Mazumder B, Lindley PF, Fox PL (1997) Identification of the prooxidant site of human ceruloplasmin: a model for oxidative damage by copper bound to protein surfaces. Proc Natl Acad Sci USA 94:11546–11551. https://doi.org/10.1073/pnas.94.21.11546
Mukhopadhyay CK, Attieh ZK, Fox PL (1998) Role of ceruloplasmin in cellular iron uptake. Science 279:714–717. https://doi.org/10.1126/science.279.5351.714
Musci G, Polticelli F, Bonaccorsi di Patti MC (2014) Ceruloplasmin-ferroportin system of iron traffic in vertebrates. World J Biol Chem 5:204–215. https://doi.org/10.4331/wjbc.v5.i2.204
Nakamura K, Go N (2005) Function and molecular evolution of multicopper blue proteins. Cell Mol Life Sci 62:2050–2066. https://doi.org/10.1007/s00018-004-5076-x
Ortel TL, Takahashi N, Putnam FW (1984) Structural model of human ceruloplasmin based on internal triplication, hydrophilic/hydrophobic character, and secondary structure of domains. Proc Natl Acad Sci USA 81:4761–4765. https://doi.org/10.1073/pnas.81.15.4761
Osaki S, Johnson DA, Frieden E (1966) The possible significance of the ferrous oxidase activity of ceruloplasmin in normal human serum. J Biol Chem 241:2746–2751
Osaki S, Johnson DA, Frieden E (1971) The mobilization of iron from the perfused mammalian liver by a serum copper enzyme, ferroxidase I. J Biol Chem 246:3018–3023. https://doi.org/10.1016/S0021-9258(18)62284-7
Park Y, Suzuki K, Taniguchi N, Gutteridge JM (1999) Glutathione peroxidase-like activity of caeruloplasmin as an important lung antioxidant. FEBS Lett 458:133–136
Patel BN, David S (1997) A novel glycosylphosphatidylinositol-anchored form of ceruloplasmin is expressed by mammalian astrocytes. J Biol Chem 272:20185–20190
Persichini T, Maio N, di Patti MC, Rizzo G, Toscano S, Colasanti M, Musci G (2010) Interleukin-1beta induces ceruloplasmin and ferroportin-1 gene expression via MAP kinases and C/EBPbeta, AP-1, and NF-kappaB activation. Neurosci Lett 484:133–138. https://doi.org/10.1016/j.neulet.2010.08.034
Pinkerton PH, Bannerman RM (1967) Hereditary defect in iron absorption in mice. Nature 216:482–483
Pinnix ZK et al (2010) Ferroportin and iron regulation in breast cancer progression and prognosis. Sci Transl Med 2:43ra56. https://doi.org/10.1126/scisignal.3001127
Piperno A, Alessio M (2018) Aceruloplasminemia: waiting for an efficient therapy. Front Neurosci 12:903. https://doi.org/10.3389/fnins.2018.00903
Prohaska JR (2011) Impact of copper limitation on expression and function of multicopper oxidases (ferroxidases). Adv Nutr 2:89–95. https://doi.org/10.3945/an.110.000208
Pulina MO, Zakharova ET, Sokolov AV, Shavlovski MM, Bass MG, Solovyov KV, Kokryakov VN, Vasilyev VB (2002) Studies of the ceruloplasmin-lactoferrin complex. Biochem Cell Biol 80:35–39
Qian ZM et al (2007) Expression of ferroportin1, hephaestin and ceruloplasmin in rat heart. Biochim Biophys Acta 1772:527–532. https://doi.org/10.1016/j.bbadis.2007.02.006
Ranganathan PN, Lu Y, Jiang L, Kim C, Collins JF (2011) Serum ceruloplasmin protein expression and activity increases in iron-deficient rats and is further enhanced by higher dietary copper intake. Blood 118:3146–3153. https://doi.org/10.1182/blood-2011-05-352112
Ranganathan PN, Lu Y, Fuqua BK, Collins JF (2012) Discovery of a cytosolic/soluble ferroxidase in rodent enterocytes. Proc Natl Acad Sci USA 109:3564. https://doi.org/10.1073/pnas.1120833109
Reeves PG, Demars LC (2005) Repletion of copper-deficient rats with dietary copper restores duodenal hephaestin protein and iron absorption. Exp Biol Med 230:320–325
Roeser HP, Lee GR, Nacht S, Cartwright GE (1970) The role of ceruloplasmin in iron metabolism. J Clin Invest 49:2408–2417. https://doi.org/10.1172/jci106460
Rydén LG, Hunt LT (1993) Evolution of protein complexity: the blue copper-containing oxidases and related proteins. J Mol Evol 36:41–66. https://doi.org/10.1007/bf02407305
Sampath P, Mazumder B, Seshadri V, Fox PL (2003) Transcript-selective translational silencing by gamma interferon is directed by a novel structural element in the ceruloplasmin mRNA 3′ untranslated region. Mol Cell Biol 23:1509–1519
Sánchez-Monteagudo A, Ripollés E, Berenguer M, Espinós C (2021) Wilson’s disease: facing the challenge of diagnosing a rare disease. Biomedicines 9:1100
Sato M, Gitlin J (1991) Mechanisms of copper incorporation during the biosynthesis of human ceruloplasmin. J Biol Chem 266:5128–5134
Schulz K, Vulpe CD, Harris LZ, David S (2011) Iron efflux from oligodendrocytes is differentially regulated in gray and white matter. J Neurosci 31:13301–13311
Sharma P et al (2019) Biallelic HEPHL1 variants impair ferroxidase activity and cause an abnormal hair phenotype. PLoS Genet 15:e1008143. https://doi.org/10.1371/journal.pgen.1008143
Shiva S et al (2006) Ceruloplasmin is a NO oxidase and nitrite synthase that determines endocrine NO homeostasis. Nat Chem Biol 2:486–493
Sokolov A, Pulina M, Zakharova E, Shavlovski M, Vasilyev V (2005) Effect of lactoferrin on the ferroxidase activity of ceruloplasmin. Biochem 70:1015–1019
Sokolov A et al (2007) Interaction of ceruloplasmin, lactoferrin, and myeloperoxidase. Biochem 72:409–415
Song N, Wang J, Jiang H, Xie J (2010) Ferroportin1 and hephaestin overexpression attenuate iron-induced oxidative stress in MES23. 5 dopaminergic cells. J Cell Biochem 110:1063–1072
Sorbie J, Hamilton DL, Valberg LS (1974) Effect of various factors on iron absorption in mice with X-linked anaemia. Br J Haematol 27:559–569
Stoffel W, Schmidt-Soltau I, Jenke B, Binczek E, Hammels I (2017) Hair growth cycle is arrested in SCD1 deficiency by impaired Wnt3a-palmitoleoylation and retrieved by the artificial lipid barrier. J Invest Dermatol 137:1424–1433
Stoj C, Kosman DJ (2003) Cuprous oxidase activity of yeast Fet3p and human ceruloplasmin: implication for function. FEBS Lett 554:422–426. https://doi.org/10.1016/s0014-5793(03)01218-3
Syed BA, Beaumont NJ, Patel A, Naylor CE, Bayele HK, Joannou CL, Rowe PS, Evans RW, Srai SK (2002) Analysis of the human hephaestin gene and protein: comparative modelling of the N-terminus ecto-domain based upon ceruloplasmin. Protein Eng 15:205–214
Tapryal N, Mukhopadhyay C, Das D, Fox PL, Mukhopadhyay CK (2009) Reactive oxygen species regulate ceruloplasmin by a novel mRNA decay mechanism involving its 3’-untranslated region: implications in neurodegenerative diseases. J Biol Chem 284:1873–1883. https://doi.org/10.1074/jbc.M804079200
Thomson AB, Valberg LS (1975) Integrity of the iron transport process in mice with X-linked anaemia. Scand J Haematol 14:347–354
Tisato V et al (2018) TRAIL and ceruloplasmin inverse correlation as a representative crosstalk between inflammation and oxidative stress. Mediators Inflamm 2018:1
Trost LB, Bergfeld WF, Calogeras E (2006) The diagnosis and treatment of iron deficiency and its potential relationship to hair loss. J Am Acad Dermatol 54:824–844
Van Eden ME, Aust SD (2000) Intact human ceruloplasmin is required for the incorporation of iron into human ferritin. Arch Biochem Biophys 381:119–126. https://doi.org/10.1006/abbi.2000.1952
Vashchenko G, MacGillivray RT (2012) Functional role of the putative iron ligands in the ferroxidase activity of recombinant human hephaestin. J Biol Inorg 17:1187–1195
Vashchenko G, MacGillivray RT (2013) Multi-copper oxidases and human iron metabolism. Nutrients 5:2289–2313. https://doi.org/10.3390/nu5072289
Vashchenko G, Bleackley MR, Griffiths TA, MacGillivray RT (2011) Oxidation of organic and biogenic amines by recombinant human hephaestin expressed in Pichia pastoris. Arch Biochem Biophys 514:50–56
Vasil’ev V, Kachurin A, Soroka N (1988) Dismutation of superoxide radicals by ceruloplasmin–details of the mechanism. Biokhimiia 53:2051–2058
Vasilyev VB (2019) Looking for a partner: ceruloplasmin in protein-protein interactions. Biometals 32:195–210. https://doi.org/10.1007/s10534-019-00189-1
Vulpe CD, Kuo YM, Murphy TL, Cowley L, Askwith C, Libina N, Gitschier J, Anderson GJ (1999) Hephaestin, a ceruloplasmin homologue implicated in intestinal iron transport, is defective in the sla mouse. Nat Genet 21:195–199. https://doi.org/10.1038/5979
Wang Y-f, Zhang J, Su Y, Shen Y-y, Jiang D-x, Hou Y-y, Geng M-y, Ding J, Chen Y (2017) G9a regulates breast cancer growth by modulating iron homeostasis through the repression of ferroxidase hephaestin. Nat Commun 8:274. https://doi.org/10.1038/s41467-017-00350-9
Wolkow N, Song D, Song Y, Chu S, Hadziahmetovic M, Lee JC, Iacovelli J, Grieco S, Dunaief JL (2012) Ferroxidase hephaestin’s cell-autonomous role in the retinal pigment epithelium. Am J Pathol 180:1614–1624
Yeh KY, Yeh M, Mims L, Glass J (2009) Iron feeding induces ferroportin 1 and hephaestin migration and interaction in rat duodenal epithelium. Am J Physiol Gastrointest Liver Physiol 296:G55-65. https://doi.org/10.1152/ajpgi.90298.2008
Yeh KY, Yeh M, Glass J (2011) Interactions between ferroportin and hephaestin in rat enterocytes are reduced after iron ingestion. J Gastroenterol 141:292–299. https://doi.org/10.1053/j.gastro.2011.03.059
Young SN, Curzon G (1972) A method for obtaining linear reciprocal plots with caeruloplasmin and its application in a study of the kinetic parameters of caeruloplasmin substrates. Biochem J 129:273–283
Zacchi P, Belmonte B, Mangogna A, Morello G, Scola L, Martorana A, Borelli V (2021) The ferroxidase hephaestin in lung cancer: pathological significance and prognostic value. Front Oncol 11:638856–638856. https://doi.org/10.3389/fonc.2021.638856
Zaitsev V, Lindley P (2019) Structural comparison of two mammalian multicopper oxidases, hephaestin and ceruloplasmin. Acta Cryst 75:e137
Zaitsev VN, Zaitseva I, Papiz M, Lindley PF (1999) An X-ray crystallographic study of the binding sites of the azide inhibitor and organic substrates to ceruloplasmin, a multi-copper oxidase in the plasma. J Biol Inorg Chem 4:579–587. https://doi.org/10.1007/s007750050380
Zaitseva I, Zaitsev V, Card G, Moshkov K, Bax B, Ralph A, Lindley P (1996) The X-ray structure of human serum ceruloplasmin at 3.1 Å: nature of the copper centres. J Biol Inorg 1:15–23. https://doi.org/10.1007/s007750050018
Zakharova ET et al (2000) Interaction of lactoferrin with ceruloplasmin. Arch Biochem Biophys 374:222–228
Zhang D-L, Ghosh MC, Rouault TA (2014) The physiological functions of iron regulatory proteins in iron homeostasis-an update. Front Pharmacol 5:124
Zhang HW et al (2021a) Cancer-associated fibroblast-derived exosomal microRNA-24-3p enhances colon cancer cell resistance to MTX by down-regulating CDX2/HEPH axis. J Cell Mol Med 25:3699–3713
Zhang Y, Chen Z, Chen JG, Chen XF, Gu DH, Liu ZM, Gao YD, Zheng B (2021b) Ceruloplasmin overexpression is associated with oncogenic pathways and poorer survival rates in clear-cell renal cell carcinoma. FEBS Open Bio 11:2988
Zhang Z et al (2021c) Adipocyte iron levels impinge on a fat-gut crosstalk to regulate intestinal lipid absorption and mediate protection from obesity. Cell Metab 33:1624-1639.e1629. https://doi.org/10.1016/j.cmet.2021.06.001
Zhao L et al (2015) Cp/Heph mutant mice have iron-induced neurodegeneration diminished by deferiprone. J Neurochem 135:958–974. https://doi.org/10.1111/jnc.13292
Zheng J, Chen M, Liu G, Xu E, Chen H (2018a) Ablation of hephaestin and ceruloplasmin results in iron accumulation in adipocytes and type 2 diabetes. FEBS Lett 592:394–401. https://doi.org/10.1002/1873-3468.12978
Zheng J, Jiang R, Chen M, Maimaitiming Z, Wang J, Anderson GJ, Vulpe CD, Dunaief JL, Chen H (2018b) Multi-copper ferroxidase–deficient mice have increased brain iron concentrations and learning and memory deficits. J Nutr 148:643–649
Zhou J (2020) Associations between the Wnt signaling pathway and iron-deficient milk of Hephaestin knockout mouse dams underlies hair loss in pups. Ph.D Doctoral dissertation, University of Florida, Gainsville, FL, USA
Acknowledgements
SLH is supported by a University of Queensland postgraduate scholarship. Writing of this review was supported by grants R01 DK074867 from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK), R01 DK109717 from NIDDK and the Office of Dietary Supplements (to JFC). The authors thank Madeleine Flynn for her assistance in preparing Figure 2.
Author information
Authors and Affiliations
Corresponding author
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Helman, S.L., Zhou, J., Fuqua, B.K. et al. The biology of mammalian multi-copper ferroxidases. Biometals 36, 263–281 (2023). https://doi.org/10.1007/s10534-022-00370-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10534-022-00370-z