Abstract
Purpose
The aim of this study was to quantify the stabilizing effect of the passive structures in thoracic spinal motion segments by stepwise resections. These data can be used to calibrate finite element models of the thoracic spine, which are needed to explore novel surgical treatments of spinal deformities, fractures, and tumours.
Method
Six human thoracic spinal motion segments from three segmental levels (T2–T3, T6–T7, and T10–T11) were loaded with pure moments of 1 and 2.5 Nm in flexion/extension, lateral bending, and axial rotation. After each loading step, the ligaments, facet capsules, and the nucleus pulposus were stepwise resected from posterior to anterior direction, while the segmental relative motions were measured using an optical motion tracking system.
Results
Significant increases (p < 0.05) in the range of motion were detected after resecting the anterior spinal structures depending on loading magnitude, motion direction, and segmental level. The highest relative increases in the range of motion were observed after nucleotomy in all motion directions. The vertebral arch mostly stabilized the thoracic spinal motion segments in flexion and extension, while the facet joint capsules mainly affected the segmental stability in axial rotation. Coupled motions were not observed.
Conclusions
The anulus fibrosus defines the motion characteristics qualitatively, while the ligaments and the presence of the nucleus pulposus restrict the mobility of a thoracic spinal motion segment solely in a quantitative manner. The posterior ligaments do not predominantly serve for primary stability but for the prevention of hyperflexion.
Graphic abstract
These slides can be retrieved under Electronic Supplementary Material.

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
For a comprehensive understanding of spinal biomechanics in healthy and pathological conditions, finite element models of the entire vertebral column are required. In the past, the lumbar spine has been extensively studied within clinical, experimental, and numerical studies because of its primary role in various pathologies. With regard to sagittal imbalances and spinal deformities, such as scoliosis or hyperkyphosis, as well as vertebral fractures and tumours, however, it is essential to include the thoracic spine in numerical models to evaluate surgical treatments including instrumentation of multiple levels.
In order to provide reliable and physiologically realistic results, finite element models are required to be calibrated with data obtained from in vitro experiments with defined boundary conditions. Ideally, the calibration process of these models is performed by adapting the material properties of each component to those obtained experimentally to include the material properties of each anatomical structure. In a previous in silico study of Schmidt et al. [1], this calibration method was applied to a model of the lumbar functional spinal unit L4–L5, starting from the anulus fibrosus, stepwise adding each anatomical structure, and fitting the material properties to the biomechanical properties of lumbar motion segments using a special algorithm. For this purpose, eight human L4–L5 spinal motion segments were tested in the in vitro study of Heuer et al. [2] by stepwise resecting every anatomical structure in reverse order and determining the ranges of motion in all motion planes. Previous in vitro studies focused on the role of the posterior structures or specific ligaments [3,4,5,6], while others evaluated the effect of the rib cage on the spinal kinematics and stability [4, 7,8,9]. For the accurate calibration of finite element models, however, ideally all structures of the functional spinal unit have to be taken into account.
The purposes of this in vitro study therefore were to perform a biomechanical stepwise reduction test of thoracic functional spinal units from three different segmental levels (upper, middle, and lower thoracic spine) in order to understand the biomechanical effect of each anatomical structure on spinal stability. The obtained data set can be used for the calibration of finite element models of the thoracic spine.
Methods
Specimen selection and preparation
Six fresh-frozen human thoracic spinal motion segments of the levels T2–T3, T6–T7, and T10–T11, respectively, were harvested from nine human donor spines. The donors had an average age of 58 years, ranging from 50 to 65 years (Table 1). During preparation, all soft tissues were carefully removed. Each specimen was visually and manually checked for signs of severe intervertebral disc degeneration and ligamentous injuries. The upper and lower vertebrae were half embedded in PMMA (polymethylmethacrylate, Technovit 3040, Heraeus Kulzer, Wehrheim, Germany), ensuring horizontal alignment of the intervertebral disc as well as coaxiality and parallelism of the cylindrical embeddings. In order to improve the fixation between vertebrae and embedding, screws were drilled into the vertebral body prior to potting.
The samples were stored at − 20 °C and thawed at 5 °C 12 h before preparation and testing. Before mechanical testing, flanges were fixed on the cranial and caudal surface of the PMMA embeddings. The specimens were constantly moistened with 0.9% saline solution, while the preparation and testing time was kept below 8 h in total to avoid specimen disintegration [10, 11].
Experimental protocol
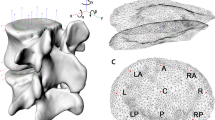
Prior to flexibility testing, an axial compressive preload of 300 N was applied to each specimen for 15 min to simulate water content loss of the intervertebral disc in daily life [12]. Flexibility testing started on intact motion segments (hereafter referred to as INTACT), followed by stepwise resection of anatomical structures (Fig. 1) with subsequent flexibility tests according to the study protocol of Heuer et al. [2]. In the first resection step, the supraspinous ligament was cut (w/o SSL) using a disposable scalpel (#11, Aesculap AG, Tuttlingen, Germany), followed by the resections of the interspinous ligament (w/o ISL), the flaval ligament (w/o FL), and the facet joint capsules (w/o FC). In the fifth resection step, the vertebral arch (w/o VA) was removed by carefully cutting the respective bony portions without damaging the posterior longitudinal ligament using an oscillating saw (OR-SY-518.01, Synthes GmbH, Zuchwil, Switzerland). Subsequently, the posterior longitudinal ligament (w/o PLL) was resected. In the seventh step, the anterior longitudinal ligament was removed by carefully detaching it from the intervertebral disc and subsequent cutting (w/o ALL). In the last resection step, the nucleus pulposus was removed (w/o NUC) on the left side of the intervertebral disc using a scalpel and a standard rongeur (Ulrich medical GmbH, Ulm, Germany).
Resection steps in the present in vitro study: 0 Intact condition (INTACT), 1 without supraspinous ligament (w/o SSL), 2 without interspinous ligament (w/o ISL), 3 without flaval ligament (w/o FL), 4 without facet joint capsules (w/o FC), 5 without vertebral arch (w/o VA), 6 without posterior longitudinal ligament (w/o PLL), 7 without anterior longitudinal ligament (w/o ALL), 8 without nucleus pulposus (w/o NUC)
Flexibility testing and motion analysis
For biomechanical testing, the specimens were loaded with pure moments of ± 1 Nm and ± 2.5 Nm using a well-established spine tester (Fig. 2), which consists of three independent stepper motors generating the displacement and a 6 degree-of-freedom load cell measuring the applied moment in the respective motion plane, allowing almost unconstrained movement around all three rotational axes due to balancing weights [13]. Flexibility testing was performed quasi-statically and displacement-controlled with a constant rate of 1°/s in flexion/extension, lateral bending, and axial rotation. For each flexibility test, 3.5 loading cycles were applied, of which the last cycle was used for data evaluation, whereas the first two loading cycles served to minimize viscoelastic effects of the specimen [10].
Triggered by the start and stop signals of the stepper motors, contact-free motion analysis of the relative motions was performed using the optical tracking system Vicon MX13 (Vicon Motion Systems Ltd., Oxford, UK) consisting of six cameras. For this, three reflective markers per vertebra were fixed to the PMMA embeddings in order to measure the in-plane and out-of-plane motions (Fig. 2). This methodology was already used in previous in vitro studies investigating thoracic spinal stability with and without the rib cage [9, 16, 18].
Data evaluation and statistics
The ranges of motion (ROM) and the neutral zones (NZ) were evaluated using a MATLAB script (MathWorks Inc., Natick, USA). Data processing was conducted using Microsoft Excel (Microsoft Corp., Redmond, USA), while statistical analysis was performed using the statistics software SPSS (IBM Corp., Armonk, USA). First, a Shapiro–Wilk test was carried out to verify the non-normal distribution of the cumulated data of the single groups, followed by a general nonparametric test for more than two conditions (Friedman test) to prove the significant trend. If the p value was below 0.05, a Wilcoxon signed-rank test was performed to identify the statistically significant differences between the anatomical resection steps. In case of p-values below 0.05, differences were considered to be statistically significant. It was hypothesized that all resection steps destabilize the thoracic spinal motion segment.
Ethics
The use of human specimens for this in vitro study was approved by the ethical committee board of the University of Ulm, Germany (No. 302/14). The specimens were acquired from an accredited and ethically approved body donation program (Anatomy Gifts Registry, Hanover, Maryland, USA).
Results
The range of motion of the three segmental levels generally increased after each resection step, while the amount of increase depended on the segmental level and the resected structure (Figs. 3, 4, 5).
For the segmental level T2–T3, a significant effect of the resection of the vertebral arch was examined in all six motion directions (Fig. 3). The resection of the posterior longitudinal ligament increased in flexion and extension, while the resection of the facet joint capsules significantly increased the range of motion in axial rotation. One of the six specimens (No. 4, BMD 84 mgHA/cm3) sustained an anterior vertebral body fracture proximal to the endplate during extension movement, resulting in an immediate failure of the sample.
The motion segment T6–T7 exhibited a significant effect of the posterior longitudinal ligament on the range of motion in all six motion directions (Fig. 4). A significant increase in the range of motion was also found after resection of the facet joint capsules in lateral bending and axial rotation. In flexion and extension, the resections of the flaval ligament and the vertebral arch each led to significant increases in the range of motion, while the resection of the supraspinal ligament had only a significant effect on the range of motion in extension. In one of the six specimens (No. 7, BMD 43 mgHA/cm3), a posterior vertebral body fracture proximal to the endplate was created during flexion movement, leading to an immediate failure.
At the segmental level T10–T11, a significant effect of the nucleotomy on the range of motion was detected in all six motion directions (Fig. 5). Resections of the vertebral arch resulted in a significant increase in the range of motion in axial rotation, while resections of the anterior and posterior longitudinal ligaments significantly increased the range of motion in flexion and extension. Additionally, the resection of the supraspinal ligament led to a significant increase in the range of motion in extension.
The range of motion in the intact condition was generally higher in lateral bending (4.7°/5.3°/3.8°) and axial rotation (4.9°/5.1°/4.2°) than in flexion/extension (3.9°/3.0°/2.7°). After resecting all structures up to the anulus fibrosus, the highest relative increases in the range of motion were found in flexion/extension (+ 184%, + 151%, + 150%), while the relative increases in the ranges of motion in axial rotation (+ 120%, + 75%, + 55%) and lateral bending (+ 76%, + 69%, + 35%) were distinctly lower. In flexion/extension, the resection of the vertebral arch had the biggest effect on the increase in the range of motion (+ 43%, + 25%, + 28%), followed by the resection of the posterior longitudinal ligament (+ 19%, + 13%, + 30%). In lateral bending and axial rotation, the nucleotomy caused the biggest increase in the range of motion (+ 34%, + 20%, + 11% and + 24%, + 17%, + 20%). Coupled motions were not detected, with the exception of a small trend towards a contralateral secondary axial rotation during primary lateral bending in the motion segment T2–T3 after resection of the longitudinal ligaments and nucleotomy.
All results including range of motion and neutral zone values, coupled motions, and comparisons with the data of Heuer et al. [2] are available in the supplementary material file within the electronical version of this publication.
Discussion
In the present study, the effects of stepwise, cumulative defects on the stability of three thoracic segmental levels under different loading magnitudes were investigated. The purposes of the study were to understand the roles of the single anatomical structures in stabilizing the thoracic spine and to provide essential data for the calibration of finite element models of the thoracic spine. Therefore, the resection sequence of the present study was selected to be comparable to the findings of Heuer et al. [2] in order to calibrate numerical models of the thoracic spine in the same way as lumbar spinal models [1].
The results showed that the range of motion increases after every resection step in all three primary motion directions, while there are no distinct changes in the three-dimensional motion characteristics. Since the anulus fibrosus represented the last remaining structure, it seems to define the motion qualitatively, while the ligaments and the nucleus pulposus restrict the mobility of a motion segment solely in a quantitative manner. The highest relative increase in the range of motion was generally observed after nucleotomy in all motion directions, indicating that the presence of the nucleus pulposus is the most important factor in the stabilization of thoracic spinal motion segments by pretensioning of the anulus fibrosus fibres, leading to an increased stiffness of the intervertebral disc.
For the first three resection steps, generally a low effect on the range of motion was found. Therefore, it can be assumed that the posterior ligaments do not predominantly serve for primary stability but for the prevention of hyperflexion due to their distal positions and consequently their long lever arms. Furthermore, it can be derived from the results that the vertebral arch mostly stabilizes the thoracic spinal motion segment in flexion and extension movement, while the facet joint capsules mainly provide stability against axial rotation movement.
Comparing the results with the literature, the range of motion values was within the data range of previous in vitro studies on thoracic spinal motion segments applying pure moments ranging from 1.5 to 8 Nm [14], but distinctly lower than in the study of Wilke et al. [15] using pure moments of 7.5 Nm. Studies which tested the thoracic spine polysegmentally including the rib cage detected lower range of motion values, indicating additional stabilizing effects of the rib cage [7,8,9, 16]. Further results of previous studies also imply that there are possible effects of the specimen length [17], compressive follower load due to bodyweight [18], as well as intervertebral disc degeneration and narrowing discs [19]. In the in vitro study of Wollowick et al., anterior structure release generated more axial rotation than posterior osteotomy [20], indicating, in accordance with the results of the present study, that the posterior structures do not primarily stabilize the thoracic spinal motion segment. In the present study, particularly the posterior ligaments were shown to have a limited effect on segmental stability, which does, however, not apply for the whole ligamentous apparatus, since it can be expected that every ligament fulfils a certain stabilizing function due to its specific morphology, stiffness, and location [3, 21]. In the literature, it is assumed that the anterior longitudinal ligament especially limits extension motions due to its higher cross-sectional area compared to other ligaments, which decreases in inferior direction, whereas the posterior longitudinal ligament is considered to limit flexion motions, particularly in the midthoracic region, where it exhibits its highest strength [21]. It is known that these two ligaments are generally thicker in the thoracic spine than in the other sections [3], partially explaining their higher stabilizing effect compared with the other ligaments in the present study. Furthermore, it can be assumed that the anatomical structures of a thoracic functional spinal unit do not affect its coupled motion characteristics, since there were no distinct secondary motions observed in the present study, indicating a dominant role of the thoracic kyphosis in generating coupled motions [18].
The present study entails some limitations regarding study design and testing methods which should be taken into account when calibrating numerical models. First, the order of resection could have affected the relative differences between the single resection steps. Furthermore, an effect of left-sided nucleotomy on the motion behaviour could not be detected. Another limitation of the present study is that the loading protocol could have influenced the results of the present study. Since the spine is loaded by compressive forces in upright position, an additional axial preload would have been appropriate to simulate more physiological loading, especially with regard to load transmission by the facet joints. In the present study, however, additional preloading was not performed due to further limitations in experimental testing: first, the results of the present study should be comparable with the study of Heuer et al., who did not use axial preloading [2], second, axial preloads were expected to lead to major artefacts in the resulting load–displacement curves, potentially making the results hardly comparable, and third, axial preloads were assumed to facilitate early specimen failure during the process of stepwise resection of the single structures. In spinal in vitro testing, it is recommended to load thoracic spinal motion segments with pure moments of 5 Nm. In the present in vitro study, however, the application of higher moments than 2.5 Nm was not feasible because the structures became too weak due to the resection of stabilizing structures. As a result, two specimens could not be fully included in the data evaluation because of vertebral body fractures, potentially inhibiting significant effects of the nucleotomy in the upper and midthoracic segmental levels. Finally, rib cage structures were not included in the experimental protocol, although showing distinct stabilizing effects [7,8,9]. However, these effects should be considered when calibrating numerical models of the thoracic spine.
Conclusions
The range of motion of thoracic spinal motion segments is lower than in the lumbar spine, while the ligamentous structures exhibit similar stabilizing properties. In the thoracic spine, the anulus fibrosus determines the qualitative motion characteristics, whereas the ligaments and the nucleus pulposus are quantitative motion limiters. Coupled motions are not caused by the anatomical structures of the thoracic functional spinal unit, but most probably by the thoracic kyphosis. The data produced in this study can be used for the calibration of numerical models of the thoracic spine. Using these models, novel surgical treatments of spinal deformities, fractures, and tumours can be developed and optimized.
References
Schmidt H, Heuer F, Drumm J, Klezl Z, Claes L, Wilke HJ (2007) Application of a calibration method provides more realistic results for a finite element model of a lumbar spinal segment. Clin Biomech 22(4):377–384
Heuer F, Schmidt H, Klezl Z, Claes L, Wilke HJ (2007) Stepwise reduction of functional spinal structures increase range of motion and change lordosis angle. J Biomech 40(2):271–280
Panjabi MM, Hausfeld JN, White AA (1981) A biomechanical study of the ligamentous stability of the thoracic spine in man. Acta Orthop Scand 52(3):315–326
Oda I, Abumi K, Cunningham BW, Kaneda K, McAfee PC (2002) An in vitro human cadaveric study investigating the biomechanical properties of the thoracic spine. Spine 27(3):E64–E70
Anderson AL, McIff TE, Asher MA, Burton DC, Glattes RC (2009) The effect of posterior thoracic spine anatomical structures on motion segment flexion stiffness. Spine 34(5):441–446
White AA 3rd, Hirsch C (1971) The significance of the vertebral posterior elements in the mechanics of the thoracic spine. Clin Orthop Relat Res 81:2–14
Watkins R 4th, Watkins R 3rd, Williams L, Ahlbrand S, Garcia R, Karamanian A, Sharp L, Vo C, Hedman T (2005) Stability provided by the sternum and rib cage in the thoracic spine. Spine 30(11):1283–1286
Brasiliense LB, Lazaro BC, Reyes PM, Dogan S, Theodore N, Crawford NR (2011) Biomechanical contribution of the rib cage to thoracic stability. Spine 36(26):E1686–E1693
Liebsch C, Graf N, Appelt K, Wilke HJ (2017) The rib cage stabilizes the human thoracic spine: An in vitro study using stepwise reduction of rib cage structures. PLOS One 12(6):e0178733
Wilke HJ, Wenger K, Claes L (1998) Testing criteria for spinal implants: recommendations for the standardization of in vitro stability testing of spinal implants. Eur Spine J 7(2):148–154
Wilke HJ, Jungkunz B, Wenger K, Claes LE (1998) Spinal segment range of motion as a function of in vitro test conditions: effects of exposure period, accumulated cycles, angular-deformation rate, and moisture condition. Anat Rec 251(1):15–19
Adams MA, Dolan P, Hutton WC (1988) The lumbar spine in backward bending. Spine 13(9):1019–1026
Wilke HJ, Claes L, Schmitt H, Wolf S (1994) A universal spine tester for in vitro experiments with muscle force simulation. Eur Spine J 3(2):91–97
Borkowski SL, Tamrazian E, Bowen RE, Scaduto AA, Ebramzadeh E, Sangiorgio SN (2016) Challenging the conventional standard for thoracic spine range of motion: a systematic review. JBJS Rev 4(4):e51–e511
Wilke HJ, Herkommer A, Werner K, Liebsch C (2017) In vitro analysis of the segmental flexibility of the thoracic spine. PLOS One 12(5):e0177823
Liebsch C, Graf N, Wilke HJ (2017) EUROSPINE, 2016 FULL PAPER AWARD: wire cerclage can restore the stability of the thoracic spine after median sternotomy: an in vitro study with entire rib cage specimens. Eur Spine J 26(5):1401–1407
Kettler A, Wilke HJ, Haid C, Claes L (2000) Effects of specimen length on the monosegmental motion behavior of the lumbar spine. Spine 25(5):543–550
Liebsch C, Graf N, Wilke HJ (2018) The effect of follower load on the intersegmental coupled motion characteristics of the human thoracic spine: an in vitro study using entire rib cage specimens. J Biomech 78:36–44
Healy AT, Mageswaran P, Lubelski D, Rosenbaum BP, Matheus V, Benzel EC, Mroz TE (2015) Thoracic range of motion, stability, and correlation to imaging-determined degeneration. J Neurosurg Spine 23(2):170–177
Wollowick AL, Farrelly EE, Meyers K, Grossman S, Amaral TD, Wright T, Sarwahi V (2013) Anterior release generates more thoracic rotation than posterior osteotomy: a biomechanical study of human cadaver spines. Spine 38(18):1540–1545
Myklebust JB, Pintar F, Yoganandan N, Cusick JF, Maiman D, Myers TJ, Sances A Jr (1988) Tensile strength of spinal ligaments. Spine 13(5):526–531
Acknowledgements
This study was funded by the German Research Foundation (DFG, Projects WI 1352/20-2 and WI 1352/23-1). The authors also gratefully acknowledge David Volkheimer for their assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors of this study declare that they have no conflict of interest to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Wilke, HJ., Grundler, S., Ottardi, C. et al. In vitro analysis of thoracic spinal motion segment flexibility during stepwise reduction of all functional structures. Eur Spine J 29, 179–185 (2020). https://doi.org/10.1007/s00586-019-06196-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00586-019-06196-7