Abstract
The ε4 allele of the apolipoprotein E gene (APOE4) is associated with cognitive decline during aging, is the greatest genetic risk factor for Alzheimer’s disease and has links to other neurodegenerative conditions that affect cognition. Increasing evidence indicates that APOE genotypes differentially modulate the function of the cerebrovasculature (CV), with apoE and its receptors expressed by different cell types at the CV interface (astrocytes, pericytes, smooth muscle cells, brain endothelial cells). However, research on the role of apoE in CV dysfunction has not advanced as quickly as other apoE-modulated pathways. This review will assess what aspects of the CV are modulated by APOE genotypes during aging and under disease states, discuss potential mechanisms, and summarize the therapeutic significance of the topic. We propose that APOE4 induces CV dysfunction through direct signaling at the CV, and indirectly via modulation of peripheral and central pathways. Further, that APOE4 predisposes the CV to damage by, and exacerbates the effects of, additional risk factors (such as sex, hypertension, and diabetes). ApoE4-induced detrimental CV changes include reduced cerebral blood flow (CBF), modified neuron-CBF coupling, increased blood–brain barrier leakiness, cerebral amyloid angiopathy, hemorrhages and disrupted transport of nutrients and toxins. The apoE4-induced detrimental changes may be linked to pericyte migration/activation, astrocyte activation, smooth muscle cell damage, basement membrane degradation and alterations in brain endothelial cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
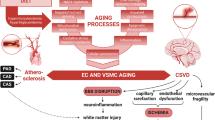
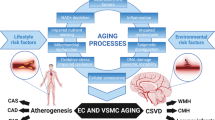
Introduction to apolipoprotein E and the cerebrovasculature (CV) (Fig. 1)
APOE4 is the greatest genetic risk factor for Alzheimer’s disease (AD), is associated with cognitive changes during aging and increases risk for other disorders, e.g., Lewy body disease, compared to APOE3. Thus, there is a critical need to dissect pathways modulated by APOE. There are three polymorphic alleles of the human APOE gene, ε2, ε3 and ε4, which encode three isoforms of apolipoprotein E (apoE, 299 amino acids, 34 kDa, reviewed extensively in [58, 67]). Human apoE isoforms differ at residues 112 or 158: apoE2 contains Cys112, Cys158; apoE3 contains Cys112, Arg158; and apoE4 contains Arg112, Arg158. Mouse apoE is structurally and functionally distinct from human apoE and is not the focus of this review. ApoE plays a key role in a number of biological processes in the periphery and the central nervous system (CNS). In the periphery, apoE is important for cholesterol metabolism and APOE4 is associated with hyperlipidemia, hypercholesterolaemia, atherosclerosis and coronary heart disease. In the CNS, apoE modulates multiple mechanistic pathways that collectively affect cognition including cholesterol/lipid homeostasis, synaptic function, glucose metabolism, neurogenesis, mitochondrial function, tau phosphorylation, neuronal atrophy, neuroinflammation, and the metabolism and aggregation of amyloid-β (Aβ). Peripheral apoE is produced by the liver and macrophages but peripheral apoE-containing lipoproteins do not cross the CV, thus apoE is also produced locally within the brain. ApoE is produced by glia (astrocytes and microglia), pericytes, smooth muscle cells, and to a much lesser extent in neurons under certain stress conditions, and potentially brain endothelial cells (BECs). The major apoE receptors are part of the low-density lipoprotein receptor (LDLR) family, which are expressed throughout the CNS. Astrocytes, microglia, neurons and BEC express LDLR, LDLR-related protein 1 (LRP1), very LDL receptor (VLDLR) and LRP8/ApoE receptor 2 (ApoER2) [58]. LDLR and LRP1 are endocytic receptors and the main apoE metabolic receptors, while VLDLR and ApoER2 are primarily signaling receptors. ApoE also binds to heparan sulfate proteoglycans, which facilitate receptor-independent and receptor-dependent apoE uptake. Therefore, APOE-modulated effects on peripheral and CNS pathways, as well as direct apoE signaling in the cells (astrocytes, pericytes, BECs) of the neurovascular unit (NVU), may collectively induce CV dysfunction and cognitive decline. However, research on the role of apoE in CV dysfunction has not advanced as quickly as other apoE-modulated mechanistic pathways. This review will assess the role of APOE in CV dysfunction in aging and neurodegenerative disorders, discuss potential mechanisms and summarize the therapeutic significance of the topic.
Aging/disease-independent effects (Supplementary Table 1a)
APOE modulates cognitive function during aging
As this article is focused on whether APOE modulates CV function and impacts cognition, an important consideration is the effect of APOE on cognitive function in aging. In young adults, evidence supports that APOE4 imparts behavioral advantages in tasks that require a wider spatial and temporal attentional field [97]. In middle-aged adults there is no clear consensus on whether APOE4 modulates cognitive ability (40–55 years, reviewed in [101]). In older adults (>55 years), APOE4 is associated with cognitive deficits in logical memory, recognition memory and processing speed as well as delayed recall and subjective memory complaints [20, 33, 57, 62, 72]. Proposed hypotheses for APOE-modulated cognition during aging include: APOE4 modulated pathways induce neuronal dysfunction independent of AD; older individuals with APOE4-induced cognitive impairment are in the prodromal AD stage, and antagonistic pleiotropy, i.e., APOE4 exerts beneficial effects early in life, neutral-to-no differences at a mid-age and detrimental effects at old age.
APOE4 synergistically interacts with vascular risk factors to impact cognition
APOE4 could affect cognition later in life through increasing the risk of developing and exacerbating damage caused by cardiovascular risk factors [9]. For example, in APOE4 but not APOE3 carriers, cardiovascular risk factors including hypercholesterolemia, prior cigarette use, diabetes mellitus and hypertension result in longitudinal preclinical memory decline (auditory verbal memory) (mean age 60, 5.6 years follow-up) [21]. Further, the interaction among APOE4, systolic blood pressure and neuropsychological performance was demonstrated in the Framingham Offspring Cohort (mean age 61 years) [141]. APOE4 also potentiates cognitive decline in the absence of pathological hypertension but with increased blood pressure. Normotensive APOE4 carriers with higher systolic blood pressure present with smaller prefrontal volume, slower processing speed and decreased verbal recognition [13]. Although some data conflict [32, 89], overall evidence supports that APOE4 interacts with peripheral cardiovascular risk factors to impact cognition and these factors share common downstream pathogenic properties: atherosclerosis, stroke and BEC dysfunction.
APOE4 disrupts cerebral blood flow
There is an intimate bi-directional association between CBF and neuronal metabolism. CBF ensures sufficient oxygen and nutrient supply, and neurons can secrete factors that influence CBF. APOE modulates CBF when assessed using PET or arterial spin labeling (ASL) MRI. In a small cohort of young college students, APOE4 carriers exhibited lower resting CBF in the left and right inferior temporal gyri and higher CBF in the left insula, right supramarginal gyrus and the inferior occipital gyrus compared to non-carriers [102]. In middle age and older adults (52–81 years) APOE4 is associated with higher CBF as a function of longer sedentary time [148]. These data are consistent with the finding that CBF is elevated for APOE4 carriers in the medial temporal lobes and left parahippocampal and fusiform gyri, the latter of which is positively correlated with verbal memory [133]. Therefore, younger middle-aged adults could display compensatory mechanisms in brain regions at risk for AD, but the data are also compatible with antagonistic pleiotropy. Indeed, CBF is lower in older (50–78 years) compared to younger (20–35 years) APOE4 carriers [36]. Further, with APOE4 there is higher baseline CBF followed by greater CBF decline with age in frontal parietal and temporal cortices in longitudinal analysis (mean age 69.2, interval length 7.8) [121]. In vivo data support the idea that APOE modulates CBF during aging. In APOE4-targeted replacement mice (APOE4-TR mice), which express human apoE4 under the control of the mouse endogenous apoE promoter, there is a reduction in cortical CBF compared to wild type, but not compared to apoE-knockout mice at 18 months of age. Although compared to wild-type mice the changes in functional connectivity were apparent at 12 months in APOE4-TR mice, reduced post-synaptic density levels occurred with perfusion deficits at 18 months [143].
A number of groups have performed fMRI with no clear consensus on the effects of APOE genotype on CBF as assessed by imaging (reviewed in [123]). Evidence for a role of APOE in CBF and CV dysfunction is derived from analysis of blood oxygenation level-dependent functional MRI (BOLD-fMRI). In BOLD-fMRI a signal represents a transient increase in CBF during neural activity, which in turn is dependent on a combination of neuronal activity, neuronal vascular coupling, CBF and general CV function. Young APOE4 carriers (~25 years) display a higher task-related BOLD signal; however, they also demonstrate the lowest CV reactivity when assessed using a CO2 inhalation challenge [114]. It is tempting to speculate that a disrupted CV may underlie the BOLD signal changes in young adults. Middle-aged (50–65) APOE4 carriers exhibit higher resting CBF when assessed by ASL and decreased BOLD and perfusion responses [37]. Collectively, the higher CBF with APOE4 in younger and middle-aged adults may be related to antagonistic pleiotropy or functional compensation due to CV damage and lead to CBF and cognitive impairments in older APOE4 carriers.
APOE2 and APOE4 increase cerebral amyloid angiopathy (CAA)
CAA is the deposition of proteins, including Aβ (particularly Aβ40), in the leptomeningeal medium and small arteries, cortical arterioles and capillaries and is frequently observed with aging. CAA can induce inflammation, fibrinoid necrosis, microaneurysm, microbleeds, transient ischemic attack, hemorrhages and white matter damage. APOE4 is associated with the increased risk of CAA [22, 41] in the occipital lobe [79], neocortex [85] and meninges and correlates with neurofibrillary tangles [85]. Further, APOE4 enhances the amount of Aβ per vessel [4], which may cause CAA-induced hemorrhage. APOE2 carriers are also overrepresented in patients with CAA-related hemorrhage [26, 41, 74–76, 79, 80], and indices of intracerebral hemorrhage severity including hematoma size, functional outcome and mortality are greater in APOE2 carriers [90]. As APOE2 does not influence the severity of CAA, APOE2 is likely a risk factor for hemorrhage of vessels with CAA. ApoE2 binds with lower affinity to LDLR compared to apoE3 and apoE4 in the periphery [131] leading to hyperlipoproteinemia, which could damage the CV and contribute to CAA.
APOE4 induces BBB/blood–CSF barrier dysfunction
Compelling but limited data support that APOE4 induces CV leakiness in humans. In a seminal study, a higher cerebrospinal fluid/plasma albumin quotient (QAlb) was demonstrated in cognitively normal older APOE3/4 carriers (66–85 years) compared to younger APOE3/4 carriers and both younger and older non-APOE4 carriers [47]. In the Rotterdam study, APOE4 was associated with microbleeds regardless of age (mean age 60.3) [86]. APOE4 also modulates the function of the CV as vasoreactivity is lower in younger APOE4 carriers [114] and in older adults [45]. Furthermore, in older adults, APOE4-induced cognitive deficits are amplified by hypertension and with low CO2 vasoreactivity [45]. White matter hyperintensities (WMH) are regarded as indications of CV dysfunction and are associated with changes in white matter integrity. Reports conflict on whether APOE4 increases or decreases the occurrence of WMH or white matter damage in aging [1, 69, 70, 130]. One factor that may underlie these discrepancies is the interaction between APOE and vascular risk factors. Indeed, vascular risk factor-induced deficits in white matter microstructure integrity are exacerbated in APOE4 carriers [128].
Data from APOE-TR mice support APOE4-induced CV dysfunction. Compared to APOE3-TR mice, in APOE4-TR mice CV permeability to dextran is higher at 6 months [12] and permeability to diazepam [2] is greater at 4 and 12 months. However, a recent study failed to find any differences in CV permeability to exogenously administered IgG in 2–3-month-old APOE4-TR or APOE-KO mice compared to wild type [15]. Further, no differences in dextran (3 and 10 kDa) CV permeability were observed between APOE-KO and wild-type mice, but a comparison for the human APOE genotypes was not performed. Global CV leakiness may be mediated by alterations in the BBB. Reduced microvascular length, DNA fragmentation in pericytes and BEC, diminished microvascular coverage by pericytes, reduced CV vascularization and a thinner basement membrane (including lower levels of collagen IV and laminin) are all observed in APOE4-TR mice compared to APOE3-TR mice [2, 12, 48]. Further, despite no changes in glucose transporter expression, 12-month-old APOE4-TR mice exhibit a lower glucose transport into the brain, as well as increased levels of the receptor for advanced glycation end products [2].
Alzheimer’s disease (AD) (Supplementary Table 1b; Fig. 2)
APOE4 increases AD risk
AD, the most common form of dementia, is a rapidly growing worldwide problem facing society and modern science. Subtypes of AD include early-onset/familial AD (FAD, 5 % of all AD cases) and late-onset AD (LOAD, 95 % of all AD cases). The major pathological hallmarks of AD include extracellular plaques of the Aβ peptide and intraneuronal neurofibrillary tangles comprised of hyperphosphorylated tau. Other broad changes in AD include synaptic and neuronal degeneration, lower hippocampal and cortical volume, reduced glucose metabolism, neuroinflammation, impaired insulin signaling, higher soluble Aβ levels and CV dysfunction. Evidence for APOE4-induced AD risk is unequivocal. APOE4 is the greatest genetic risk for LOAD, increasing risk up to 12-fold compared to APOE3, whereas APOE2 reduces risk [58]. APOE4 is also associated with a lower age of AD onset and an increased risk of progression from mild cognitive impairment (MCI) to AD. Mechanistically, APOE4 has been linked to virtually every AD-relevant pathogenic process including Aβ levels, altered Aβ-signaling both directly through Aβ binding and indirectly, and Aβ-independent pathways. There is now little doubt if APOE4 impacts upon the CV and its function in all stages of AD.
CV deficits with APOE4 and Aβ in EFAD mice. CD31 (green) and Aβ (red, using the MOAB-2 antibody) staining in 8-month-old male mice that express APOE4 and overexpress human Aβ (EFAD mice described in [139]). a ×10 magnification, scale bar 100 μm (b–e) ×63 magnification, scale bar 20 μm
APOE4 synergistically interacts with vascular risk factors to increase AD risk
APOE4 is not only associated with an increased risk for AD and cardiovascular disease, but the evidence suggests APOE4 and vascular risk factors combine synergistically to exacerbate cognitive decline in AD [43, 55, 73]. For example, neuropathological hallmarks of AD (neurofibrillary tangles, neuritic plaques and CAA) are increased in patients with diabetes who are APOE4 carriers when compared with non-carriers [43]. The combination of hyperglycemia, hyperinsulinemia and insulin resistance observed in type 2 diabetes plus APOE4 exacerbate the development of AD pathology [73].
APOE4 disrupts cerebral blood flow in AD
APOE4 exerts a pronounced effect on CBF in MCI and AD when assessed by ASL-MRI, or single-photon emission computer tomography (SPECT). A number of groups have demonstrated higher CBF in MCI patients with APOE4. CBF is higher in the medial temporal lobes, parahippocampal gyrus, cingulate gyrus, posterior cingulate gyrus and lingual gyrus of patients who are APOE4 positive and have MCI [10, 60, 134]. The effect of APOE4 on CBF in MCI is brain region specific. In the left parahippocampal/fusiform gyrus, CBF is higher with APOE4 in non-demented controls and lower in APOE4 MCI patients, whereas the opposite pattern is observed in frontal regions [134]. The higher CBF in MCI patients who are APOE4 positive may be indicative of compensatory mechanisms in response to stress, or of an ongoing pathogenic response acting on the vasculature (e.g., inflammation, neuronal activity). Although CBF is elevated in posterior brain regions with one risk factor such as APOE4 or MCI, the presence of both results in decreased CBF and a greater likelihood of conversion to dementia [134]. Thus, in the presence of multiple risk factors declining posterior hippocampal function may result in higher CBF to other brain regions as a compensatory mechanism. In AD, APOE4 is associated with cerebral hypoperfusion, including the occipital lobes, middle temporal gyrus, inferior frontal gyrus, anterior cingulate gyrus, claustrum, insula and caudate [51, 65, 66], as well as a greater spread of CBF reductions from the parietotemporal to the frontal area [99]. However, there are also reports of increased CBF asymmetry in APOE4 non-carriers [125], no APOE4-dependent effects in AD patients [96], and a counter argument that APOE4 promotes neuronal dysfunction rather than CV changes. However, the data are most consistent with disrupted CBF with APOE4 in AD.
APOE4 increases capillary CAA in AD
CAA in cortical and leptomeningeal arteries/arterioles of AD patients follows the order; APOE4/4 > APOE3/4 > APOE3/3 [6, 25, 35, 87, 92, 93, 104], and APOE4 increases CAA in the occipital lobes [122]. For example, in one study the prevalence of severe CAA from highest to lowest in AD was 73.4 % for APOE4/4 carriers, 46 % in APOE3/4 carriers and 24.2 % in APOE3/3 carriers [92]. Further, CAA in APOE4 AD patients is more severe [87] and associated with a longer onset period of cognitive decline to death, lower diffuse plaque score, cortical microinfarcts, leukoencephalopathy, enlarged perivascular spaces in the white matter, subcortical and lobar and intracerebral hemorrhages, thrombosis and fibrinogen deposition [6, 25, 35, 54, 87, 92, 93, 104]. APOE4 also leads to substantial CAA compared to APOE3 and also a higher Aβ40/42 ratio in mice that express FAD mutations (FAD-Tg mice) [38]. However, a few studies have reported a lack of association between APOE4 and CAA in AD [83, 112], no link for APOE4 modulated CAA and hemorrhage [25], that CAA in general rather than APOE4 is important for dementia [117] and an association between CAA and lower cognition proximal to death in non-APOE4 carriers [16]. Thus, there is confusion of whether CAA in APOE4 AD patients is a major contributor to overall dementia. One question that remains is how the APOE genotypes correlate with the types of vessels affected by CAA in AD. A body of data supports that the CAA in APOE4 carriers affects cortical capillaries [3, 120, 140]. For example, Thal et al. [120] observed an odds ratio of 4.751 for capillary CAA in APOE4 AD patients. CAA is also linked to amyloid-related imaging abnormalities (ARIA) after passive and active immunization strategies targeting Aβ in AD [98]. ARIA is characterized by vasogenic edema and cortical hemorrhages, is more common in APOE4-AD patients after immunization with antibodies for Aβ and has been linked to CAA [98, 136]. The higher levels of CAA with APOE4 may reflect detrimental changes in the CV with immunization that include splitting of vessel wall, and/or the removal of Aβ from the vessel wall [98]. In contrast to APOE4, there is a negative association of CAA for APOE2 [35]. The evidence that APOE2 increases CAA and ICH in aging, but not in AD, is potentially due to the protection afforded by APOE2 for AD risk through effects on other AD-relevant pathways, e.g., apoE lipidation and inflammation.
APOE4 induces BBB dysfunction in AD
Initial evidence that APOE modulates the BBB (capillaries) in AD was observed by Salloway et al. [100], who demonstrated a thinning of the basement membrane in APOE4/4 compared to APOE3/3 AD patients. When assessed using quantification of agrin (basement membrane protein) staining, the capillary basement membrane area was smaller in APOE4/4 AD patients compared to APOE3/3 AD patients in the prefrontal cortex [100] and APOE3/4 AD patients trended (non-significant) to lay between APOE3/3 and APOE4/4 AD patients. Basement membrane disruptions may be an indication that the BBB is degenerating with APOE4 leading to increased leakiness. Indeed, levels of the plasma protein prothrombin in the prefrontal cortex are higher in APOE4/4 AD patients than APOE3/3 AD patients (significance at the 10 % level) [146]. Further, IgG and fibrin extravasation surrounding microvessels follows the order APOE4AD > APOE3AD > controls in the frontal cortex [47]. In contrast, no APOE genotype-specific effects were observed on the QAlb in AD patients, although there was evidence for a protective effect of APOE3 on BBB leakiness in Creutzfeldt-Jacob disease [59]. There is evidence that APOE modulates microbleeds in AD. In AD, microbleeds are associated with male sex, higher blood pressure, lower CSF Aβ42 and APOE4 [14]. In contrast to the male bias in humans, microbleeds are higher in female mice that express APOE4 and Aβ compared to male mice [18]. Perhaps there are other stressors synergistically interacting with APOE4 in males with higher microbleeds. APOE4 is associated with increased WMH in the parietal lobe compared to non-carriers [17], however, data conflict on whether APOE4 increases WMH risk in AD [17, 49, 61, 78]. Potential confounding factors are that APOE4 and vascular risk factors interact to induce WMH, and that WMH are brain region specific. Our preliminary data also demonstrate that there are CV deficits in mice that express APOE4 and overexpress Aβ (E4FAD mice described in [139] Fig. 2). In 8-month-old male E4FAD mice we have observed characteristics of CV dysfunction including vessels surrounding extracellular Aβ (Fig. 2b), CAA (Fig. 2c, d), the absence of vessels in areas of high Aβ, and vessel degeneration (Fig. 2e). Additional data that apoE modulates the CV include the negative association of APOE-positive capillaries and extracellular Aβ plaques, the positive correlation of APOE and expression of angiogenesis/vasoactive mediators (VEGF, eNOS) in AD brain capillaries [88], and the link between apoE levels and CV leakiness in AD patients with small vessel disease [124]. Collectively these data support that APOE4 increases CV leakiness in AD patients compared to APOE3.
APOE-modulated CV dysfunction in other neurodegenerative conditions
Data suggest that rather than representing a risk factor, APOE4 exacerbates the progression, is inferior or hinders repair mechanisms in vascular dementia (VaD), multiple sclerosis (MS), stroke and traumatic brain injury (TBI), compared to APOE3. For example, APOE4 is linked to greater cognitive impairment in VaD, higher disease progression/severity in MS [107], a detrimental progression or outcome after intracerebral hemorrhage, subarachnoid hemorrhage, stroke [42] and after TBI [28]. Although the CV is important for these conditions, surprisingly the role of APOE-modulated CV dysfunction has not been dissected. Cleaved apoE is considered toxic, but this is also evidence of an ongoing apoE-dependent process. In VaD, cleaved amino-terminal fragments of apoE were identified within blood vessels in an APOE genotype-dependent manner: APOE4/4 > APOE3/4 > APOE3/3 [94]. For MS, in APOE knockout mice subjected to experimental autoimmune encephalitis, a murine model of MS, there are lower levels of proteins in the tight junctions and higher levels of matrix metalloproteinases, suggesting a role for APOE in the progression of disease, but the exact role is still unclear [44, 144]. In TBI, possession of APOE4 promotes CAA, possibly by disruption of the vascular clearance mechanisms for Aβ [145]. Together, these results suggest that it is important to determine whether apoE4 has a detrimental or inferior effect upon cellular and tissue repair mechanisms in the CNS, compared to the other apoE isoforms.
Potential mechanistic pathways underlying APOE-modulated CV dysfunction (Supplementary Table 1; Fig. 3)
Genetic, environmental, physiological and lifestyle risk factors will collectively induce changes in a multitude of biological pathways that determine whether an individual will experience impaired cognition with aging, or begins to progress towards a neurodegenerative disease. Further, the overlapping nature for many of the pathways can result in comorbidities. Accumulating evidence supports that APOE4 modulates a multitude of mechanistic pathways which can affect cognition. However, APOE4, like diabetes, hypertension and aging is a risk factor not a cause. It would be naïve to propose that for every individual, a single risk factor or pathway is the cause of cognitive impairments, especially in the context of chronic conditions, e.g., Aβ causes AD. Similarly, CV deficits are not disease specific and, therefore, are unlikely to be relevant to primary causation. However, multiple risk factor-modulated pathways acting in temporal-specific manner will impact cognition. Within this complexity, we propose that APOE4 induces CV dysfunction through direct signaling at the NVU, and indirectly via modulation of peripheral and central pathways, contributing to cognitive decline in aging and neurodegenerative disorders. Further, that APOE4 predisposes the CV to damage by, and exacerbates the effects of, additional risk factors (e.g., sex, hypertension, diabetes).
Pathways of APOE-modulated neurovascular dysfunction. APOE4 imparts negative effects on a multitude of peripheral and CNS pathways that may contribute to cerebrovascular dysfunction and lead to cognitive impairment. Brain endothelial cells may act as the primary effector interface for these pathways
ApoE4 can directly induce detrimental signaling at the NVU
The question of how the apoE isoforms differentially modulate a diverse range of biological processes to affect cognition is a major focus of a number of groups. ApoE produced by the periphery can signal to BEC and cells of the NVU express apoE and the apoE receptors. The structure and receptor binding properties of apoE could exert a strong influence on the CV. Overall, apoE isoform-specific differences are thought to affect the folding, including the receptor binding domain (N terminus) and the lipid binding domain (C terminus), and stability of apoE (reviewed in [58]). In the CNS differences between the apoE isoforms will affect the structure of lipoproteins, and the majority, if not all, of the apoE in the interstitial fluid of the brain is present as a lipoprotein. One proposed hypothesis is that structural differences among the apoE isoforms in the brain results in lower apoE4 lipidation, lower apoE4-containing lipoprotein stability, the production of toxic apoE4 fragments and lower apoE4 levels, which in turn causes impaired apoE4 cellular recycling and altered receptor activity (reviewed in [116]). Specific for the CV, apoE modulates astrocyte–pericyte–BEC interactions [12, 23, 127, 135]. ApoE4 but not apoE3 (from astrocytes) signaling to LRP1 in pericytes is impaired, resulting in higher activation of the cyclophilin A (cypA)-NFkB-matrix metalloproteinase 9 (MMP9) pathway in pericytes [12, 47]. The higher MMP9 levels with APOE4 leads to CV dysfunction by basement membrane degradation and impaired BEC function. Lipidated apoE is also produced by pericytes in vitro [23] and apoE knockdown in isolated human pericytes accelerates pericyte mobility, which is suppressed by supplementing apoE3, but not apoE4 into the media. Importantly, apoE isoform-dependent modulation of pericyte mobility is mediated by a pathway involving LRP1 and RhoA. Often overlooked is the potential that apoE from the CNS activates apoE receptors in BECs to modulate CV function. Indeed, astrocyte-derived apoE signals via LRP1 on BECs in vitro, an effect greater with apoE3 than apoE4, resulting in lower occludin phosphorylation with apoE4 [81]. Further to agonist activity, the accumulation of toxic apoE4 fragments inside of BEC as observed in VaD could induce CV dysfunction. Therefore, apoE4 receptor signaling cascades may be blunted compared to apoE3 in astrocytes, pericytes and BECs resulting in a disrupted CV.
APOE-modulated neuroinflammation contributes to BBB dysfunction
As reviewed extensively elsewhere [115], APOE4 is increasingly recognized as modulating glial-mediated neuroinflammation in aging and AD. APOE4 is associated with a detrimental response to Aβ-independent neuroinflammation (such as LPS or as occurs in aging) and Aβ-induced inflammation. However, the complexity of chronic neuroinflammation, including multiple detrimental and beneficial effects occurring in a temporal and cell-specific manner, has resulted in conflicting functional data for virtually every inflammatory mediator. Potentially, APOE4 induces a detrimental neuroinflammatory phenotype characterized by higher pro-inflammatory and lower anti-inflammatory cytokines [115]. Importantly, many mediators described as inflammatory exert a strong influence of the CV, including BEC function (e.g., TNFα), angiogenesis (e.g., VEGF, EGF) and the basement membrane (MMPs, TIMPs). In addition, an overlooked topic is how BEC themselves produce inflammatory mediators in response to stress. Mechanistically, the effects on glial inflammation may be mediated in part by direct apoE signaling as described above. Thus, apoE through its effects on soluble mediator release from inflammatory cells within the brain may cause and also prime the CV to damage in response to a subsequent hit from the periphery.
Aβ clearance is slower with APOE4 at the CV
Aβ, in insoluble or soluble form, is considered a key mediator of AD progression and can induce direct (BEC) and indirect (via pathways such as inflammation) CV dysfunction. Therefore, APOE could directly modulate Aβ signaling to affect the CV. For example, Aβ-induced detrimental signaling in glia and BEC may be amplified in the presence of apoE4. In addition, Aβ clearance rates are slower with apoE4 at the BBB [7, 30] and via perivascular drainage [24, 48]. Higher levels of Aβ with APOE4 will result in amplified detrimental pathways in the CNS to cause CV dysfunction. After Aβ42 injections in vivo, Aβ clearance into the plasma follows the pattern APOE3 > APOE4 > APOE-KO/wt [8]. At the BBB, when Aβ binds apoE2 or apoE3 (apoE/Aβ complex) clearance is mediated via LRP1 and LDLR, whereas Aβ-bound apoE4 is cleared at a significantly slower rate via VLDLR [30]. ApoE and Aβ also co-localize in the perivascular elimination pathways of AD transgenic mice as well as in control and AD patients [95]. Importantly, after ICV injections of Aβ into APOE-TR mice, Aβ40 aggregates in the perivascular drainage pathway with APOE4 but not APOE3 [48], evidence that perivascular elimination is slower with APOE4. Further, following Aβ immunotherapy plaque-associated apoE is reduced and CV wall-associated apoE increased [98]. This immunotherapy-mediated translocation of apoE from plaques to the CV mirrors the changes in Aβ and is consistent with a proposed role for apoE as an important transporter of Aβ in the brain. Mechanistically, apoE could affect Aβ clearance through direct binding as an apoE/Aβ complex and an important functional distinction is whether the apoE/Aβ complex is part of a plaque, present in the basement membrane or soluble in the ISF. ApoE when part of a plaque or as part of an initial seed for oAβ may drive Aβ pathology and inflammation and also transport Aβ to the CV, apoE-Aβ interactions at the basement membrane are likely involved in perivascular drainage, and soluble apoE/Aβ complex may prevent oAβ formation and promote Aβ clearance (contrasting in vitro data exist [8]).
APOE4 could prime the CV to damage by increasing the risk of developing and potentiating peripheral stress
A recurrent theme is the potentiation of cognitive decline with APOE4 and peripheral vascular risk factors in aging and AD. APOE4 can increase the risk of developing cardiovascular disease contributing to CV dysfunction, e.g., hypertension increases the risk of BBB disturbances and atherosclerosis. Mechanistically, the N and C terminus of apoE4 interact to a greater extent than apoE3, which directs apoE4 to very low density lipoproteins and increases the incidence of atherosclerosis. The apoE4-induced alterations in lipid metabolism can also modulate CV function. There are higher serum cholesterol, phospholipid and triglyceride levels in APOE4 carriers. Lipolysis products from lipoproteins rich in triglycerides, specifically triacylglycerol-rich lipoproteins (TGRL), alter the structure of apoE4, but not apoE3 [118]. These conformational changes influence the way in which apoE4 binds to BECs [5], which in turn may disrupt BBB permeability, allowing for influx of damaging TGRL lipolysis products. Further, many of the peripheral risk factors have a strong inflammatory component, which will directly affect BEC at the CV. One potential mechanism is that CV active inflammatory mediators in the periphery are modulated by APOE, analogous to neuroinflammation. For example, healthy volunteers injected with lipopolysaccharide exhibit hyperthermia and increases in plasma levels of pro-inflammatory markers (TNFα, IL-6) that are higher in APOE3/4 carriers compared to APOE3/3 carriers [39].
Therapeutic significance (Fig. 4)
Directly targeting apoE or the apoE receptors
Directly targeting the structural and functional deficits of apoE4 may ameliorate detrimental changes that cause CV dysfunction (reviewed in [67]. These strategies may also become relevant for apoE3 in certain conditions. If apoE4 is considered detrimental (toxic gain of function) then lowering apoE4 levels using genetic or antibody-based approaches is optimal. If apoE4 is less functional (loss of positive function) increasing apoE4 lipidation by promoting the activity or levels (e.g., via nuclear receptor agonists) of the primary lipid efflux transporter in the CNS, the ATP-binding cassette transporter A1, or correcting the structure of apoE4 becomes the focus. Both approaches show promise in vivo for AD-relevant pathways. Importantly, nuclear receptor agonists may target BBB dysfunction in AD [149], and are protective against CV dysfunction caused by viral infections [53]. However, both strategies have drawbacks including toxicity and lack of specificity for nuclear receptor agonists, or the necessity of accessing apoE before becoming part of a lipoprotein for structural correctors. The development of more advanced genetic strategies could also lead to overexpression of APOE2 in APOE4 carriers [52]. Directly targeting the LDLR family is an alternative way to circumvent a loss of positive function for apoE4 signaling at the neurovascular unit. ApoE mimetic peptides, which are based on the receptor binding region of apoE, reduce edema after focal brain ischemia and lower CV dysfunction after TBI in vivo [19, 63].
Targeting inflammation at the NVU and the basement membrane
Targeting either the signaling pathways or the soluble mediators produced by APOE-modulated activated glia (astrocytes and microglia) and pericytes may ameliorate CV dysfunction, or prevent the risk with a subsequent additional hit. For signaling in glia and astrocytes, antagonists/inhibitors of TLR4, p38a, cyclooxygenase 2 (COX2) and nuclear receptor agonists suppress pro-inflammatory cytokines and increase anti-inflammatory cytokines in various in vivo and in vitro models of neurodegenerative conditions. For pericytes, targeting the LRP1-rhoA or cypA-NFkB-MMP9 pathway may prove efficacious. In terms of mediators, likely targets include TNFα, and nitric oxide, a vasoactive mediator proposed as a target for CAA-induced CNS damage. Additional targets include raising levels of tissue inhibitors for metalloproteinases to prevent basement membrane disruption, or targeting soluble mediators that induce changes in angiogenesis and BEC function. Surprisingly, BEC pathways are frequently overlooked as a direct for APOE4-induced CV dysfunction, e.g., reactive oxygen species, COX, mitogen active protein kinase and angiogenic signaling. The main advantage of targeting BECs directly is that therapeutics do not have to cross the BBB into the brain to be active.
Targeting peripheral pathways
Therapeutic or lifestyle interventions for the peripheral factors that synergistically combine with APOE4 to cause CV dysfunction may provide a great benefit for neurodegenerative disorders. For example anti-hypertensive drugs, particularly angiotensin receptor blockers, have shown promise in AD but the effects of these drugs correlated with APOE genotype are unknown. For hypercholesterolemia statins have been tested in clinical trials for the treatment in AD with disappointing results. The biological mechanisms behind why hypercholesterolemia increases AD risk are still unclear, but elevated cholesterol levels can disrupt the integrity of the BBB. Thus, it is proposed that BBB penetrant lipophilic statins disrupt cholesterol synthesis in the brain resulting in detrimental effects on cognition whereas less-BBB penetrant hydrophilic statins may be promising [27]. Targeting peripheral inflammation can be achieved using the same approaches as for neuroinflammation and include nonsteroidal anti-inflammatory drugs (NSAIDs); however, results from the clinic are not as promising as observed in epidemiological studies. Potentially, therapeutics that target hypertension, hypercholesterolemia and peripheral inflammation will prove efficacious for cognitive decline in APOE4 carriers with CV dysfunction. There is growing evidence supporting the adoption of lifestyle changes to improve cognition, which partially act through modulating the CV. ApoE is also necessary for the prevention of age-induced CV dysfunction by exercise in vivo [111]. With professional guidance and assistance most individuals, particularly APOE4 carriers, would be able to curtail damaging habits that put them at risk of cognitive damage caused by CV dysfunction.
Conclusion
ApoE4 exerts a strong influence of CV dysfunction, an effect exacerbated by additional risk factors. Identifying APOE-modulated CV-specific mechanistic pathways via basic and preclinical therapeutic research may ultimately lead to prevention and treatment options to improve cognition in aging and neurodegenerative disorders.
Abbreviations
- Aβ:
-
Amyloid-β
- AD:
-
Alzheimer’s disease
- apoE:
-
Apolipoprotein E
- APOE-TR:
-
APOE-targeted replacement mice
- ASL:
-
Arterial spin labeling
- BBB:
-
Blood–brain barrier
- BEC:
-
Brain endothelial cells
- CAA:
-
Cerebral amyloid angiopathy
- CBF:
-
Cerebral blood flow
- CSF:
-
Cerebrospinal spinal fluid
- CNS:
-
Central nervous system
- CV:
-
Cerebrovasculature
- cypA:
-
Cyclophilin A
- FAD:
-
Familial AD
- ISF:
-
Interstitial fluid
- KO:
-
Knockout
- LDLR:
-
Low-density lipoprotein receptor
- LRP1:
-
Low-density lipoprotein receptor-related protein 1
- MCI:
-
Mild cognitive impairment
- MMP:
-
Matrix metalloproteinase
- MS:
-
Multiple sclerosis
- NVU:
-
Neurovascular unit
- oAβ:
-
Oligomeric Aβ
- TJ:
-
Tight junction
- TNFα:
-
Tumor necrosis factor α
- VaD:
-
Vascular dementia
- VLDLR:
-
Very LDL receptor
- WMH:
-
White matter hyperintensities
References
Adluru N, Destiche DJ, Lu SY, Doran ST, Birdsill AC, Melah KE, Okonkwo OC, Alexander AL, Dowling NM, Johnson SC et al (2014) White matter microstructure in late middle-age: effects of apolipoprotein E4 and parental family history of Alzheimer’s disease. Neuroimage Clin 4:730–742
Alata W, Ye Y, St-Amour I, Vandal M, Calon F (2015) Human apolipoprotein E varepsilon4 expression impairs cerebral vascularization and blood-brain barrier function in mice. J Cereb Blood Flow Metab 35:86–94
Allen N, Robinson AC, Snowden J, Davidson YS, Mann DM (2014) Patterns of cerebral amyloid angiopathy define histopathological phenotypes in Alzheimer’s disease. Neuropathol Appl Neurobiol 40:136–148
Alonzo NC, Hyman BT, Rebeck GW, Greenberg SM (1998) Progression of cerebral amyloid angiopathy: accumulation of amyloid-beta40 in affected vessels. J Neuropathol Exp Neurol 57:353–359
Altman R, Rutledge JC (2010) The vascular contribution to Alzheimer’s disease. Clin Sci (Lond) 119:407–421
Attems J, Jellinger KA, Lintner F (2005) Alzheimer’s disease pathology influences severity and topographical distribution of cerebral amyloid angiopathy. Acta Neuropathol 110:222–231
Bachmeier C, Beaulieu-Abdelahad D, Crawford F, Mullan M, Paris D (2012) Stimulation of the retinoid X receptor facilitates beta-amyloid clearance across the blood-brain barrier. J Mol Neurosci 49:270–276
Bachmeier C, Paris D, Beaulieu-Abdelahad D, Mouzon B, Mullan M, Crawford F (2013) A multifaceted role for apoE in the clearance of beta-amyloid across the blood-brain barrier. Neurodegener Dis 11:13–21
Bangen KJ, Beiser A, Delano-Wood L, Nation DA, Lamar M, Libon DJ, Bondi MW, Seshadri S, Wolf PA, Au R (2013) APOE genotype modifies the relationship between midlife vascular risk factors and later cognitive decline. J Stroke Cerebrovasc Dis 22:1361–1369
Bangen KJ, Restom K, Liu TT, Wierenga CE, Jak AJ, Salmon DP, Bondi MW (2012) Assessment of Alzheimer’s disease risk with functional magnetic resonance imaging: an arterial spin labeling study. J Alzheimers Dis 31(Suppl 3):S59–S74
Barber R, Gholkar A, Scheltens P, Ballard C, McKeith IG, Morris CM, O’Brien JT (1999) Apolipoprotein E epsilon4 allele, temporal lobe atrophy, and white matter lesions in late-life dementias. Arch Neurol 56:961–965
Bell RD, Winkler EA, Singh I, Sagare AP, Deane R, Wu Z, Holtzman DM, Betsholtz C, Armulik A, Sallstrom J et al (2012) Apolipoprotein E controls cerebrovascular integrity via cyclophilin A. Nature 485:512–516
Bender AR, Raz N (2012) Age-related differences in memory and executive functions in healthy APOE varepsilon4 carriers: the contribution of individual differences in prefrontal volumes and systolic blood pressure. Neuropsychologia 50:704–714
Benedictus MR, Goos JD, Binnewijzend MA, Muller M, Barkhof F, Scheltens P, Prins ND, van der Flier WM (2013) Specific risk factors for microbleeds and white matter hyperintensities in Alzheimer’s disease. Neurobiol Aging 34:2488–2494
Bien-Ly N, Boswell CA, Jeet S, Beach TG, Hoyte K, Luk W, Shihadeh V, Ulufatu S, Foreman O, Lu Y et al (2015) Lack of Widespread BBB Disruption in Alzheimer’s Disease Models: focus on Therapeutic Antibodies. Neuron 88:289–297
Brenowitz WD, Nelson PT, Besser LM, Heller KB, Kukull WA (2015) Cerebral amyloid angiopathy and its co-occurrence with Alzheimer’s disease and other cerebrovascular neuropathologic changes. Neurobiol Aging 36:2702–2708
Brickman AM, Schupf N, Manly JJ, Stern Y, Luchsinger JA, Provenzano FA, Narkhede A, Razlighi Q, Collins-Praino L, Artero S et al (2014) APOE epsilon4 and risk for Alzheimer’s disease: do regionally distributed white matter hyperintensities play a role? Alzheimers Dement 10:619–629
Cacciottolo M, Christensen A, Moser A, Liu J, Pike CJ, Smith C, LaDu MJ, Sullivan PM, Morgan TE, Dolzhenko E et al (2016) The APOE4 allele shows opposite sex bias in microbleeds and Alzheimer’s disease of humans and mice. Neurobiol Aging 37:47–57
Cao F, Jiang Y, Wu Y, Zhong J, Liu J, Qin X, Chen L, Vitek MP, Li F, Xu L et al (2016) Apolipoprotein E-mimetic COG1410 reduces acute vasogenic edema following traumatic brain injury. J Neurotrauma 33:175–182
Caselli RJ, Dueck AC, Locke DE, Hoffman-Snyder CR, Woodruff BK, Rapcsak SZ, Reiman EM (2011) Longitudinal modeling of frontal cognition in APOE epsilon4 homozygotes, heterozygotes, and noncarriers. Neurology 76:1383–1388
Caselli RJ, Dueck AC, Locke DE, Sabbagh MN, Ahern GL, Rapcsak SZ, Baxter LC, Yaari R, Woodruff BK, Hoffman-Snyder C et al (2011) Cerebrovascular risk factors and preclinical memory decline in healthy APOE ε4 homozygotes. Neurology 76:1078–1084
Caselli RJ, Walker D, Sue L, Sabbagh M, Beach T (2010) Amyloid load in nondemented brains correlates with APOE e4. Neurosci Lett 473:168–171
Casey CS, Atagi Y, Yamazaki Y, Shinohara M, Tachibana M, Fu Y, Bu G, Kanekiyo T (2015) Apolipoprotein E inhibits cerebrovascular pericyte mobility through a RhoA-mediated pathway. J Biol Chem 290:14208–14217
Castellano JM, Kim J, Stewart FR, Jiang H, DeMattos RB, Patterson BW, Fagan AM, Morris JC, Mawuenyega KG, Cruchaga C et al (2011) Human apoE isoforms differentially regulate brain amyloid-beta peptide clearance. Sci Transl Med 3:89ra57
Chalmers K, Wilcock GK, Love S (2003) APOE epsilon 4 influences the pathological phenotype of Alzheimer’s disease by favouring cerebrovascular over parenchymal accumulation of A beta protein. Neuropathol Appl Neurobiol 29:231–238
Charidimou A, Martinez-Ramirez S, Shoamanesh A, Oliveira-Filho J, Frosch M, Vashkevich A, Ayres A, Rosand J, Gurol ME, Greenberg SM et al (2015) Cerebral amyloid angiopathy with and without hemorrhage: evidence for different disease phenotypes. Neurology 84:1206–1212
Chen X, Hui L, Geiger JD (2014) Role of endolysosomes and cholesterol in the pathogenesis of Alzheimer’s disease: insights into why statins might not provide clinical benefit. Austin J Pharmacol Ther 2(6):1035
Crawford FC, Vanderploeg RD, Freeman MJ, Singh S, Waisman M, Michaels L, Abdullah L, Warden D, Lipsky R, Salazar A et al (2002) APOE genotype influences acquisition and recall following traumatic brain injury. Neurology 58:1115–1118
de Leeuw FE, Richard F, de Groot JC, van Duijn CM, Hofman A, Van Gijn J, Breteler MM (2004) Interaction between hypertension, apoE, and cerebral white matter lesions. Stroke 35:1057–1060
Deane R, Sagare A, Hamm K, Parisi M, Lane S, Finn MB, Holtzman DM, Zlokovic BV (2008) apoE isoform-specific disruption of amyloid beta peptide clearance from mouse brain. J Clin Invest 118:4002–4013
DeCarli C, Reed T, Miller BL, Wolf PA, Swan GE, Carmelli D (1999) Impact of apolipoprotein E epsilon4 and vascular disease on brain morphology in men from the NHLBI twin study. Stroke 30:1548–1553
den Heijer T, van der Lijn F, Ikram A, Koudstaal PJ, van der Lugt A, Krestin GP, Vrooman HA, Hofman A, Niessen WJ, Breteler MM (2012) Vascular risk factors, apolipoprotein E, and hippocampal decline on magnetic resonance imaging over a 10-year follow-up. Alzheimers Dement 8:417–425
Dik MG, Jonker C, Comijs HC, Bouter LM, Twisk JW, van Kamp GJ, Deeg DJ (2001) Memory complaints and APOE-epsilon4 accelerate cognitive decline in cognitively normal elderly. Neurology 57:2217–2222
Doody RS, Azher SN, Haykal HA, Dunn JK, Liao T, Schneider L (2000) Does APO epsilon4 correlate with MRI changes in Alzheimer’s disease? J Neurol Neurosurg Psychiatry 69:668–671
Esiri M, Chance S, Joachim C, Warden D, Smallwood A, Sloan C, Christie S, Wilcock G, Smith AD (2015) Cerebral amyloid angiopathy, subcortical white matter disease and dementia: literature review and study in OPTIMA. Brain Pathol 25:51–62
Filippini N, Ebmeier KP, MacIntosh BJ, Trachtenberg AJ, Frisoni GB, Wilcock GK, Beckmann CF, Smith SM, Matthews PM, Mackay CE (2011) Differential effects of the APOE genotype on brain function across the lifespan. Neuroimage 54:602–610
Fleisher AS, Podraza KM, Bangen KJ, Taylor C, Sherzai A, Sidhar K, Liu TT, Dale AM, Buxton RB (2009) Cerebral perfusion and oxygenation differences in Alzheimer’s disease risk. Neurobiol Aging 30:1737–1748
Fryer JD, Simmons K, Parsadanian M, Bales KR, Paul SM, Sullivan PM, Holtzman DM (2005) Human apolipoprotein E4 alters the amyloid-beta 40:42 ratio and promotes the formation of cerebral amyloid angiopathy in an amyloid precursor protein transgenic model. J Neurosci 25:2803–2810
Gale SC, Gao L, Mikacenic C, Coyle SM, Rafaels N, Murray Dudenkov T, Madenspacher JH, Draper DW, Ge W, Aloor JJ et al (2014) APOepsilon4 is associated with enhanced in vivo innate immune responses in human subjects. J Allergy Clin Immunol 134:127–134
Greenberg SM, Rebeck GW, Vonsattel JP, Gomez-Isla T, Hyman BT (1995) Apolipoprotein E epsilon 4 and cerebral hemorrhage associated with amyloid angiopathy. Ann Neurol 38:254–259
Greenberg SM, Vonsattel JP, Segal AZ, Chiu RI, Clatworthy AE, Liao A, Hyman BT, Rebeck GW (1998) Association of apolipoprotein E epsilon2 and vasculopathy in cerebral amyloid angiopathy. Neurology 50:961–965
Gromadzka G, Baranska-Gieruszczak M, Sarzynska-Dlugosz I, Ciesielska A, Czlonkowska A (2007) The APOE polymorphism and 1-year outcome in ischemic stroke: genotype-gender interaction. Acta Neurol Scand 116:392–398
Haan MN, Shemanski L, Jagust WJ, Manolio TA, Kuller L (1999) The role of APOE epsilon4 in modulating effects of other risk factors for cognitive decline in elderly persons. JAMA 282:40–46
Hafezi-Moghadam A, Thomas KL, Wagner DD (2007) ApoE deficiency leads to a progressive age-dependent blood-brain barrier leakage. Am J Physiol Cell Physiol 292:C1256–C1262
Hajjar I, Sorond F, Lipsitz LA (2015) Apolipoprotein E, carbon dioxide vasoreactivity, and cognition in older adults: effect of hypertension. J Am Geriatr Soc 63:276–281
Halliday MR, Pomara N, Sagare AP, Mack WJ, Frangione B, Zlokovic BV (2013) Relationship between cyclophilin a levels and matrix metalloproteinase 9 activity in cerebrospinal fluid of cognitively normal apolipoprotein e4 carriers and blood-brain barrier breakdown. JAMA Neurol 70:1198–1200
Halliday MR, Rege SV, Ma Q, Zhao Z, Miller CA, Winkler EA, Zlokovic BV (2015) Accelerated pericyte degeneration and blood-brain barrier breakdown in apolipoprotein E4 carriers with Alzheimer’s disease. J Cereb Blood Flow Metab 36:216–227
Hawkes CA, Sullivan PM, Hands S, Weller RO, Nicoll JA, Carare RO (2012) Disruption of arterial perivascular drainage of amyloid-beta from the brains of mice expressing the human APOE epsilon4 allele. PLoS One 7:e41636
Hirono N, Yasuda M, Tanimukai S, Kitagaki H, Mori E (2000) Effect of the apolipoprotein E epsilon4 allele on white matter hyperintensities in dementia. Stroke 31:1263–1268
Hogh P, Garde E, Mortensen EL, Jorgensen OS, Krabbe K, Waldemar G (2007) The apolipoprotein E epsilon4-allele and antihypertensive treatment are associated with increased risk of cerebral MRI white matter hyperintensities. Acta Neurol Scand 115:248–253
Hogh P, Knudsen GM, Kjaer KH, Jorgensen OS, Paulson OB, Waldemar G (2001) Single photon emission computed tomography and apolipoprotein E in Alzheimer’s disease: impact of the epsilon4 allele on regional cerebral blood flow. J Geriatr Psychiatry Neurol 14:42–51
Hu J, Liu CC, Chen XF, Zhang YW, Xu H, Bu G (2015) Opposing effects of viral mediated brain expression of apolipoprotein E2 (apoE2) and apoE4 on apoE lipidation and Abeta metabolism in apoE4-targeted replacement mice. Mol Neurodegener 10:6
Huang W, Chen L, Zhang B, Park M, Toborek M (2014) PPAR agonist-mediated protection against HIV Tat-induced cerebrovascular toxicity is enhanced in MMP-9-deficient mice. J Cereb Blood Flow Metab 34:646–653
Hultman K, Strickland S, Norris EH (2013) The APOE varepsilon4/varepsilon4 genotype potentiates vascular fibrin(ogen) deposition in amyloid-laden vessels in the brains of Alzheimer’s disease patients. J Cereb Blood Flow Metab 33:1251–1258
Irie F, Fitzpatrick AL, Lopez OL, Kuller LH, Peila R, Newman AB, Launer LJ (2008) Enhanced risk for Alzheimer disease in persons with type 2 diabetes and APOE epsilon4: the cardiovascular health study cognition study. Arch Neurol 65:89–93
Itoh Y, Yamada M (1997) Cerebral amyloid angiopathy in the elderly: the clinicopathological features, pathogenesis, and risk factors. J Med Dent Sci 44:11–19
Jochemsen HM, Muller M, van der Graaf Y, Geerlings MI (2012) APOE epsilon4 differentially influences change in memory performance depending on age. The SMART-MR study. Neurobiol Aging 33(832):e815–e822
Kanekiyo T, Xu H, Bu G (2014) ApoE and Abeta in Alzheimer’s disease: accidental encounters or partners? Neuron 81:740–754
Karch A, Manthey H, Ponto C, Hermann P, Heinemann U, Schmidt C, Zerr I (2013) Investigating the association of ApoE genotypes with blood-brain barrier dysfunction measured by cerebrospinal fluid-serum albumin ratio in a cohort of patients with different types of dementia. PLoS One 8:e84405
Kim SM, Kim MJ, Rhee HY, Ryu CW, Kim EJ, Petersen ET, Jahng GH (2013) Regional cerebral perfusion in patients with Alzheimer’s disease and mild cognitive impairment: effect of APOE epsilon4 allele. Neuroradiology 55:25–34
Kljajevic V, Meyer P, Holzmann C, Dyrba M, Kasper E, Bokde AL, Fellgiebel A, Meindl T, Hampel H, Teipel S et al (2014) The epsilon4 genotype of apolipoprotein E and white matter integrity in Alzheimer’s disease. Alzheimers Dement 10:401–404
Krell-Roesch J, Woodruff BK, Acosta JI, Locke DE, Hentz JG, Stonnington CM, Stokin GB, Nagle C, Michel BF, Sambuchi N et al (2015) APOE epsilon4 genotype and the risk for subjective cognitive impairment in elderly persons. J Neuropsychiatry Clin Neurosci 27:322–325
Laskowitz DT, Lei B, Dawson HN, Wang H, Bellows ST, Christensen DJ, Vitek MP, James ML (2012) The apoE-mimetic peptide, COG1410, improves functional recovery in a murine model of intracerebral hemorrhage. Neurocrit Care 16:316–326
Lee YM, Ha JK, Park JM, Lee BD, Moon E, Chung YI, Kim JH, Kim HJ, Mun CW, Kim TH et al (2015) Impact of apolipoprotein E4 polymorphism on the gray matter volume and the white matter integrity in subjective memory impairment without white matter hyperintensities: voxel-based morphometry and tract-based spatial statistics study under 3-Tesla MRI. J Neuroimaging 26:144–149
Lehtovirta M, Kuikka J, Helisalmi S, Hartikainen P, Mannermaa A, Ryynanen M, Riekkinen P, Soininen H (1998) Longitudinal SPECT study in Alzheimer’s disease: relation to apolipoprotein E polymorphism. J Neurol Neurosurg Psychiatry 64:742–746
Lehtovirta M, Soininen H, Laakso MP, Partanen K, Helisalmi S, Mannermaa A, Ryynanen M, Kuikka J, Hartikainen P, Riekkinen PJ Sr (1996) SPECT and MRI analysis in Alzheimer’s disease: relation to apolipoprotein E epsilon 4 allele. J Neurol Neurosurg Psychiatry 60:644–649
Liu CC, Kanekiyo T, Xu H, Bu G (2013) Apolipoprotein E and Alzheimer disease: risk, mechanisms and therapy. Nat Rev Neurol 9:106–118
Love S, Nicoll JA, Hughes A, Wilcock GK (2003) APOE and cerebral amyloid angiopathy in the elderly. NeuroReport 14:1535–1536
Lyall DM, Harris SE, Bastin ME, Munoz Maniega S, Murray C, Lutz MW, Saunders AM, Roses AD, Valdes Hernandez Mdel C, Royle NA et al (2014) Alzheimer’s disease susceptibility genes APOE and TOMM40, and brain white matter integrity in the Lothian Birth Cohort 1936. Neurobiol Aging 35(1513):e1525–e1533
Lyall DM, Munoz Maniega S, Harris SE, Bastin ME, Murray C, Lutz MW, Saunders AM, Roses AD, Valdes Hernandez MD, Royle NA et al (2015) APOE/TOMM40 genetic loci, white matter hyperintensities, and cerebral microbleeds. Int J Stroke 10:1297–1300
Makela M, Paetau A, Polvikoski T, Myllykangas L, Tanskanen M (2015) Capillary amyloid-beta protein deposition in a population-based study (vantaa 85+). J Alzheimers Dis 49:149–157
Marioni RE, Campbell A, Scotland G, Hayward C, Porteous DJ, Deary IJ (2015) Differential effects of the APOE e4 allele on different domains of cognitive ability across the life-course. Eur J Hum Genet. doi:10.1038/ejhg.2015.210
Matsuzaki T, Sasaki K, Tanizaki Y, Hata J, Fujimi K, Matsui Y, Sekita A, Suzuki SO, Kanba S, Kiyohara Y et al (2010) Insulin resistance is associated with the pathology of Alzheimer disease: the Hisayama study. Neurology 75:764–770
McCarron MO, Nicoll JA (2000) Apolipoprotein E genotype and cerebral amyloid angiopathy-related hemorrhage. Ann N Y Acad Sci 903:176–179
McCarron MO, Nicoll JA (1998) High frequency of apolipoprotein E epsilon 2 allele is specific for patients with cerebral amyloid angiopathy-related haemorrhage. Neurosci Lett 247:45–48
McCarron MO, Nicoll JA, Stewart J, Cole GM, Yang F, Ironside JW, Mann DM, Love S, Graham DI (2000) Amyloid beta-protein length and cerebral amyloid angiopathy-related haemorrhage. NeuroReport 11:937–940
McCarron MO, Nicoll JA, Stewart J, Ironside JW, Mann DM, Love S, Graham DI, Dewar D (1999) The apolipoprotein E epsilon2 allele and the pathological features in cerebral amyloid angiopathy-related hemorrhage. J Neuropathol Exp Neurol 58:711–718
Morgen K, Schneider M, Frolich L, Tost H, Plichta MM, Kolsch H, Rakebrandt F, Rienhoff O, Jessen F, Peters O et al (2015) Apolipoprotein E-dependent load of white matter hyperintensities in Alzheimer’s disease: a voxel-based lesion mapping study. Alzheimers Res Ther 7:27
Nelson PT, Pious NM, Jicha GA, Wilcock DM, Fardo DW, Estus S, Rebeck GW (2013) APOE-epsilon2 and APOE-epsilon4 correlate with increased amyloid accumulation in cerebral vasculature. J Neuropathol Exp Neurol 72:708–715
Nicoll JA, Burnett C, Love S, Graham DI, Dewar D, Ironside JW, Stewart J, Vinters HV (1997) High frequency of apolipoprotein E epsilon 2 allele in hemorrhage due to cerebral amyloid angiopathy. Ann Neurol 41:716–721
Nishitsuji K, Hosono T, Nakamura T, Bu G, Michikawa M (2011) Apolipoprotein E regulates the integrity of tight junctions in an isoform-dependent manner in an in vitro blood-brain barrier model. J Biol Chem 286:17536–17542
Nyberg L, Salami A (2014) The APOE epsilon4 allele in relation to brain white-matter microstructure in adulthood and aging. Scand J Psychol 55:263–267
Olichney JM, Hansen LA, Hofstetter CR, Lee JH, Katzman R, Thal LJ (2000) Association between severe cerebral amyloid angiopathy and cerebrovascular lesions in Alzheimer disease is not a spurious one attributable to apolipoprotein E4. Arch Neurol 57:869–874
Paternoster L, Chen W, Sudlow CL (2009) Genetic determinants of white matter hyperintensities on brain scans: a systematic assessment of 19 candidate gene polymorphisms in 46 studies in 19,000 subjects. Stroke 40:2020–2026
Pfeifer LA, White LR, Ross GW, Petrovitch H, Launer LJ (2002) Cerebral amyloid angiopathy and cognitive function: the HAAS autopsy study. Neurology 58:1629–1634
Poels MM, Vernooij MW, Ikram MA, Hofman A, Krestin GP, van der Lugt A, Breteler MM (2010) Prevalence and risk factors of cerebral microbleeds: an update of the Rotterdam scan study. Stroke 41:S103–S106
Premkumar DR, Cohen DL, Hedera P, Friedland RP, Kalaria RN (1996) Apolipoprotein E-epsilon4 alleles in cerebral amyloid angiopathy and cerebrovascular pathology associated with Alzheimer’s disease. Am J Pathol 148:2083–2095
Provias J, Jeynes B (2011) Correlation analysis of capillary APOE, VEGF and eNOS expression in Alzheimer brains. Curr Alzheimer Res 8:197–202
Qiu C, Winblad B, Fratiglioni L (2006) Cerebrovascular disease, APOE epsilon4 allele and cognitive decline in a cognitively normal population. Neurol Res 28:650–656
Rannikmae K, Kalaria RN, Greenberg SM, Chui HC, Schmitt FA, Samarasekera N, Al-Shahi Salman R, Sudlow CL (2014) APOE associations with severe CAA-associated vasculopathic changes: collaborative meta-analysis. J Neurol Neurosurg Psychiatry 85:300–305
Raz N, Yang Y, Dahle CL, Land S (2012) Volume of white matter hyperintensities in healthy adults: contribution of age, vascular risk factors, and inflammation-related genetic variants. Biochim Biophys Acta 1822:361–369
Ringman JM, Sachs MC, Zhou Y, Monsell SE, Saver JL, Vinters HV (2014) Clinical predictors of severe cerebral amyloid angiopathy and influence of APOE genotype in persons with pathologically verified Alzheimer disease. JAMA Neurol 71:878–883
Roher AE, Kuo YM, Esh C, Knebel C, Weiss N, Kalback W, Luehrs DC, Childress JL, Beach TG, Weller RO et al (2003) Cortical and leptomeningeal cerebrovascular amyloid and white matter pathology in Alzheimer’s disease. Mol Med 9:112–122
Rohn TT, Day RJ, Sheffield CB, Rajic AJ, Poon WW (2014) Apolipoprotein E pathology in vascular dementia. Int J Clin Exp Pathol 7:938–947
Rolyan H, Feike AC, Upadhaya AR, Waha A, Van Dooren T, Haass C, Birkenmeier G, Pietrzik CU, Van Leuven F, Thal DR (2011) Amyloid-beta protein modulates the perivascular clearance of neuronal apolipoprotein E in mouse models of Alzheimer’s disease. J Neural Transm 118:699–712
Rosengarten B, Paulsen S, Burr O, Kaps M (2010) Effect of ApoE epsilon4 allele on visual evoked potentials and resultant flow coupling in patients with Alzheimer. J Geriatr Psychiatry Neurol 23:165–170
Rusted JM, Evans SL, King SL, Dowell N, Tabet N, Tofts PS (2013) APOE e4 polymorphism in young adults is associated with improved attention and indexed by distinct neural signatures. Neuroimage 65:364–373
Sakai K, Boche D, Carare R, Johnston D, Holmes C, Love S, Nicoll JA (2014) Abeta immunotherapy for Alzheimer’s disease: effects on apoE and cerebral vasculopathy. Acta Neuropathol 128:777–789
Sakamoto S, Matsuda H, Asada T, Ohnishi T, Nakano S, Kanetaka H, Takasaki M (2003) Apolipoprotein E genotype and early Alzheimer’s disease: a longitudinal SPECT study. J Neuroimaging 13:113–123
Salloway S, Gur T, Berzin T, Tavares R, Zipser B, Correia S, Hovanesian V, Fallon J, Kuo-Leblanc V, Glass D et al (2002) Effect of APOE genotype on microvascular basement membrane in Alzheimer’s disease. J Neurol Sci 203–204:183–187
Salvato G (2015) Does apolipoprotein E genotype influence cognition in middle-aged individuals? Curr Opin Neurol 28:612–617
Scarmeas N, Habeck CG, Stern Y, Anderson KE (2003) APOE genotype and cerebral blood flow in healthy young individuals. JAMA 290:1581–1582
Schilling S, DeStefano AL, Sachdev PS, Choi SH, Mather KA, DeCarli CD, Wen W, Hogh P, Raz N, Au R et al (2013) APOE genotype and MRI markers of cerebrovascular disease: systematic review and meta-analysis. Neurology 81:292–300
Schmechel DE, Saunders AM, Strittmatter WJ, Crain BJ, Hulette CM, Joo SH, Pericak-Vance MA, Goldgaber D, Roses AD (1993) Increased amyloid beta-peptide deposition in cerebral cortex as a consequence of apolipoprotein E genotype in late-onset Alzheimer disease. Proc Natl Acad Sci USA 90:9649–9653
Schmidt H, Schmidt R, Fazekas F, Semmler J, Kapeller P, Reinhart B, Kostner GM (1996) Apolipoprotein E e4 allele in the normal elderly: neuropsychologic and brain MRI correlates. Clin Genet 50:293–299
Serrano-Pozo A, Qian J, Monsell SE, Betensky RA, Hyman BT (2015) APOEepsilon2 is associated with milder clinical and pathological Alzheimer disease. Ann Neurol 77:917–929
Shi J, Tu JL, Gale SD, Baxter L, Vollmer TL, Campagnolo DI, Tyry TM, Zhuang Y, Kuniyoshi SM (2011) APOE epsilon4 is associated with exacerbation of cognitive decline in patients with multiple sclerosis. Cogn Behav Neurol 24:128–133
Shu N, Li X, Ma C, Zhang J, Chen K, Liang Y, Chen Y, Zhang Z (2015) Effects of APOE promoter polymorphism on the topological organization of brain structural connectome in nondemented elderly. Hum Brain Mapp 36:4847–4858
Skoog I, Hesse C, Aevarsson O, Landahl S, Wahlstrom J, Fredman P, Blennow K (1998) A population study of apoE genotype at the age of 85: relation to dementia, cerebrovascular disease, and mortality. J Neurol Neurosurg Psychiatry 64:37–43
Son SJ, Lee KS, Lee Y, Baek JH, Choi SH, Na DL, Seo SW, Oh BH, Hong CH (2012) Association between white matter hyperintensity severity and cognitive impairment according to the presence of the apolipoprotein E (APOE) epsilon4 allele in the elderly: retrospective analysis of data from the CREDOS study. J Clin Psychiatry 73:1555–1562
Soto I, Graham LC, Richter HJ, Simeone SN, Radell JE, Grabowska W, Funkhouser WK, Howell MC, Howell GR (2015) APOE stabilization by exercise prevents aging neurovascular dysfunction and complement induction. PLoS Biol 13:e1002279
Stopa EG, Butala P, Salloway S, Johanson CE, Gonzalez L, Tavares R, Hovanesian V, Hulette CM, Vitek MP, Cohen RA (2008) Cerebral cortical arteriolar angiopathy, vascular beta-amyloid, smooth muscle actin, Braak stage, and APOE genotype. Stroke 39:814–821
Sun ZW, Zhu YX, Liu HY, Liu J, Zhu XQ, Zhou JN, Liu RY (2007) Decreased cerebral blood flow velocity in apolipoprotein E epsilon4 allele carriers with mild cognitive impairment. Eur J Neurol 14:150–155
Suri S, Mackay CE, Kelly ME, Germuska M, Tunbridge EM, Frisoni GB, Matthews PM, Ebmeier KP, Bulte DP, Filippini N (2015) Reduced cerebrovascular reactivity in young adults carrying the APOE epsilon4 allele. Alzheimers Dement 11(648–657):e641
Tai LM, Ghura S, Koster KP, Liakaite V, Maienschein-Cline M, Kanabar P, Collins N, Ben-Aissa M, Lei AZ, Bahroos N et al (2015) APOE-modulated Abeta-induced neuroinflammation in Alzheimer’s disease: current landscape, novel data and future perspective. J Neurochem 133:465–488
Tai LM, Mehra S, Shete V, Estus S, Rebeck GW, Bu G, Ladu MJ (2014) Soluble apoE/Abeta complex: mechanism and therapeutic target for APOE4-induced AD risk. Mol Neurodegener 9:2
Tanskanen M, Lindsberg PJ, Tienari PJ, Polvikoski T, Sulkava R, Verkkoniemi A, Rastas S, Paetau A, Kiuru-Enari S (2005) Cerebral amyloid angiopathy in a 95 + cohort: complement activation and apolipoprotein E (ApoE) genotype. Neuropathol Appl Neurobiol 31:589–599
Tetali SD, Budamagunta MS, Voss JC, Rutledge JC (2006) C-terminal interactions of apolipoprotein E4 respond to the postprandial state. J Lipid Res 47:1358–1365
Thal DR, Ghebremedhin E, Rub U, Yamaguchi H, Tredici KD, Braak H (2002) Two types of sporadic cerebral amyloid angiopathy. J Neuropathol Exp Neurol 61:282–293
Thal DR, Papassotiropoulos A, Saido TC, Griffin WS, Mrak RE, Kolsch H, Del Tredici K, Attems J, Ghebremedhin E (2010) Capillary cerebral amyloid angiopathy identifies a distinct APOE epsilon4-associated subtype of sporadic Alzheimer’s disease. Acta Neuropathol 120:169–183
Thambisetty M, Beason-Held L, An Y, Kraut MA, Resnick SM (2010) APOE epsilon4 genotype and longitudinal changes in cerebral blood flow in normal aging. Arch Neurol 67:93–98
Tian J, Shi J, Bailey K, Lendon CL, Pickering-Brown SM, Mann DM (2004) Association between apolipoprotein E e4 allele and arteriosclerosis, cerebral amyloid angiopathy, and cerebral white matter damage in Alzheimer’s disease. J Neurol Neurosurg Psychiatry 75:696–699
Trachtenberg AJ, Filippini N, Mackay CE (2012) The effects of APOE-epsilon4 on the BOLD response. Neurobiol Aging 33:323–334
Utter S, Tamboli IY, Walter J, Upadhaya AR, Birkenmeier G, Pietrzik CU, Ghebremedhin E, Thal DR (2008) Cerebral small vessel disease-induced apolipoprotein E leakage is associated with Alzheimer disease and the accumulation of amyloid beta-protein in perivascular astrocytes. J Neuropathol Exp Neurol 67:842–856
van Dyck CH, Gelernter J, MacAvoy MG, Avery RA, Criden M, Okereke O, Varma P, Seibyl JP, Hoffer PB (1998) Absence of an apolipoprotein E epsilon4 allele is associated with increased parietal regional cerebral blood flow asymmetry in Alzheimer disease. Arch Neurol 55:1460–1466
Vandal M, Alata W, Tremblay C, Rioux-Perreault C, Salem N Jr, Calon F, Plourde M (2014) Reduction in DHA transport to the brain of mice expressing human APOE4 compared to APOE2. J Neurochem 129:516–526
Verbeek MM, Van Nostrand WE, Otte-Holler I, Wesseling P, De Waal RM (2000) Amyloid-beta-induced degeneration of human brain pericytes is dependent on the apolipoprotein E genotype. Ann N Y Acad Sci 903:187–199
Wang R, Fratiglioni L, Laukka EJ, Lovden M, Kalpouzos G, Keller L, Graff C, Salami A, Backman L, Qiu C (2015) Effects of vascular risk factors and APOE epsilon4 on white matter integrity and cognitive decline. Neurology 84:1128–1135
Wang R, Fratiglioni L, Laveskog A, Kalpouzos G, Ehrenkrona CH, Zhang Y, Bronge L, Wahlund LO, Backman L, Qiu C (2014) Do cardiovascular risk factors explain the link between white matter hyperintensities and brain volumes in old age? A population-based study. Eur J Neurol 21:1076–1082
Watfa G, Marteau JB, Rossignol P, Kearney-Schwartz A, Fay R, Bracard S, Felblinger J, Boivin JM, Lacolley P, Visvikis-Siest S et al (2010) Association study of gene polymorphisms involved in vascular alterations in elderly hypertensives with subjective memory complaints. Dement Geriatr Cogn Disord 30:440–448
Weisgraber KH, Innerarity TL, Mahley RW (1982) Abnormal lipoprotein receptor-binding activity of the human E apoprotein due to cysteine-arginine interchange at a single site. J Biol Chem 257:2518–2521
Westlye LT, Reinvang I, Rootwelt H, Espeseth T (2012) Effects of APOE on brain white matter microstructure in healthy adults. Neurology 79:1961–1969
Wierenga CE, Clark LR, Dev SI, Shin DD, Jurick SM, Rissman RA, Liu TT, Bondi MW (2013) Interaction of age and APOE genotype on cerebral blood flow at rest. J Alzheimers Dis 34:921–935
Wierenga CE, Dev SI, Shin DD, Clark LR, Bangen KJ, Jak AJ, Rissman RA, Liu TT, Salmon DP, Bondi MW (2012) Effect of mild cognitive impairment and APOE genotype on resting cerebral blood flow and its association with cognition. J Cereb Blood Flow Metab 32:1589–1599
Wilhelmus MM, Otte-Holler I, Davis J, Van Nostrand WE, de Waal RM, Verbeek MM (2005) Apolipoprotein E genotype regulates amyloid-beta cytotoxicity. J Neurosci 25:3621–3627
Wisniewski T, Goni F (2014) Immunotherapy for Alzheimer’s disease. Biochem Pharmacol 88:499–507
Yasuno F, Tanimukai S, Sasaki M, Ikejima C, Yamashita F, Kodama C, Hidaka S, Mizukami K, Asada T (2012) Effect of plasma lipids, hypertension and APOE genotype on cognitive decline. Neurobiol Aging 33:2633–2640
Yoon B, Shim YS, Cheong HK, Kim YD, Lee KO, Hong YJ, Oh YS, Na HR, Kim BC, Choi SH et al (2013) Interaction of white matter hyperintensities (WMHs) and apolipoprotein E (APOE) genotypes on cognition in patients with amnestic mild cognitive impairment (aMCI). Arch Gerontol Geriatr 57:292–297
Youmans KL, Tai LM, Nwabuisi-Heath E, Jungbauer L, Kanekiyo T, Gan M, Kim J, Eimer WA, Estus S, Rebeck GW et al (2012) APOE4-specific changes in abeta accumulation in a new transgenic mouse model of Alzheimer disease. J Biol Chem 287:41774–41786
Yu L, Boyle PA, Nag S, Leurgans S, Buchman AS, Wilson RS, Arvanitakis Z, Farfel JM, De Jager PL, Bennett DA et al (2015) APOE and cerebral amyloid angiopathy in community-dwelling older persons. Neurobiol Aging 36:2946–2953
Zade D, Beiser A, McGlinchey R, Au R, Seshadri S, Palumbo C, Wolf PA, Decarli C, Milberg W (2010) Interactive effects of apolipoprotein E type 4 genotype and cerebrovascular risk on neuropsychological performance and structural brain changes. J Stroke Cerebrovasc Dis 19:261–268
Zarow C, Zaias B, Lyness SA, Chui H (1999) Cerebral amyloid angiopathy in Alzheimer disease is associated with apolipoprotein E4 and cortical neuron loss. Alzheimer Dis Assoc Disord 13:1–8
Zerbi V, Wiesmann M, Emmerzaal TL, Jansen D, Van Beek M, Mutsaers MP, Beckmann CF, Heerschap A, Kiliaan AJ (2014) Resting-state functional connectivity changes in aging apoE4 and apoE-KO mice. J Neurosci 34:13963–13975
Zheng M, Wei J, Tang Y, Yang C, Wei Y, Yin X, Liu Q (2014) ApoE-deficient promotes blood-brain barrier disruption in experimental autoimmune encephalomyelitis via alteration of MMP-9. J Mol Neurosci 54:282–290
Zhou W, Xu D, Peng X, Zhang Q, Jia J, Crutcher KA (2008) Meta-analysis of APOE4 allele and outcome after traumatic brain injury. J Neurotrauma 25:279–290
Zipser BD, Johanson CE, Gonzalez L, Berzin TM, Tavares R, Hulette CM, Vitek MP, Hovanesian V, Stopa EG (2007) Microvascular injury and blood-brain barrier leakage in Alzheimer’s disease. Neurobiol Aging 28:977–986
Zito G, Polimanti R, Panetta V, Ventriglia M, Salustri C, Siotto MC, Moffa F, Altamura C, Vernieri F, Lupoi D et al (2013) Antioxidant status and APOE genotype as susceptibility factors for neurodegeneration in Alzheimer’s disease and vascular dementia. Rejuvenation Res 16:51–56
Zlatar ZZ, Wierenga CE, Bangen KJ, Liu TT, Jak AJ (2014) Increased hippocampal blood flow in sedentary older adults at genetic risk for Alzheimer’s disease. J Alzheimers Dis 41:809–817
Zolezzi JM, Inestrosa NC (2013) Peroxisome proliferator-activated receptors and Alzheimer’s disease: hitting the blood-brain barrier. Mol Neurobiol 48:438–451
Acknowledgments
L. M. T. is supported by UIC start-up funds. G. B. is supported by National Institutes of Health Grants RF1AG051504, R01AG027924, R01AG035355, R01AG046205, P01AG030128, P01NS074969, and P50AG016574, and grants from the Alzheimer’s Association and Cure Alzheimer’s Fund. The authors would also like to acknowledge Dr. Scott Brady (UIC) for critical scientific discussions on the topic.
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Tai, L.M., Thomas, R., Marottoli, F.M. et al. The role of APOE in cerebrovascular dysfunction. Acta Neuropathol 131, 709–723 (2016). https://doi.org/10.1007/s00401-016-1547-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00401-016-1547-z