Abstract
Purpose
The purpose of this study is to develop a comprehensive complications profile for quadriceps tendon-autograft anterior cruciate ligament reconstruction (QT ACL-R).
Methods
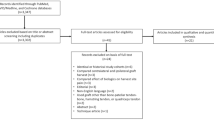
A traditional and grey literature search was conducted in accordance with PRISMA and R-AMSTAR guidelines. PubMed, EMBASE, MEDLINE, CINAHL, Cochrane, Web of Science, and many grey literature sources were searched from inception to May 29, 2022. All studies were searched and screened in duplicate with included studies being of all levels of evidence, reporting complications, and with patients of all ages undergoing primary ACL reconstruction with quadriceps tendon autograft in the last 15 years. Studies were excluded if they had cadaveric or animal subjects or were reviews. Risk of bias assessment was conducted using MINORS criteria for non-randomised studies and Cochrane’s RoB 2.0 for randomised studies. Data were summarised with weighted event rates generated under a random-effects model.
Results
A total of 55 studies (5315 reconstructions) were included: 32 used quadriceps tendon with bone block (B-QT), 19 used all-soft tissue quadriceps tendon (S-QT), and four did not report the QT graft subtype used. Included patients had an age range of 6.2–58 years and an average reported follow-up time of 28.1 months (range, 6–90 months) for non-randomised studies and 34.3 months (range, 0.233–120 months) for randomised studies. Pooled incidence rates for clinically relevant major complications included contralateral ACL injury at 6.0%, postoperative meniscal issues at 5.4%, cyclops lesions at 4.8%, graft failure at 4.1%, patellar fracture at 2.2%, hardware removal at 1.7%, infection at 1.5%, and donor-site quadriceps tendon rupture at 0.7%. Pooled incidence rates for clinically relevant minor complications included anterior knee pain at 9.7%, kneeling pain at 9.5%, sensation deficits at 4.4%, loss of extension at 4.2%, donor-site tendinopathy at 3.9%, cosmetic issues at 1.8%, and hematoma at 1.5%.
Conclusions
QT ACL-R resembles other graft types in its rates and types of postoperative complications. In this exploratory systematic review, no complications of QT ACL-R were found to be disproportionately represented in the literature. This graft type should remain an option with comparable complication rates to other graft choices.
Level of evidence
Level IV.
Registration
This study was preregistered under PROSPERO with preregistration code CRD42022302078.



Similar content being viewed by others
Change history
30 November 2022
A Correction to this paper has been published: https://doi.org/10.1007/s00167-022-07217-7
Abbreviations
- ACL:
-
Anterior cruciate ligament
- ACL-R:
-
Anterior cruciate ligament reconstruction
- B-QT:
-
Bone–quadriceps tendon
- BPTB:
-
Bone–patellar tendon–bone
- CD:
-
Clavien–Dindo
- HT:
-
Hamstrings tendon
- IKDC:
-
International Knee Documentation Committee
- KOOS:
-
Knee Injury and Osteoarthritis Outcome Score
- MINORS:
-
Methodological Index for Non-Randomised Studies
- NR:
-
Not reported
- PCL:
-
Posterior cruciate ligament
- PRISMA:
-
Preferred Reporting Items for Systematic Reviews and Meta-Analyses
- PROMs:
-
Patient-reported outcome measures
- QT:
-
Quadriceps tendon
- R-AMSTAR:
-
Revised Assessment of Multiple Systematic Reviews
- S-QT:
-
All-soft tissue quadriceps tendon
References
Akoto R, Albers M, Balke M, Bouillon B, Hoeher J (2019) ACL reconstruction with quadriceps tendon graft and press-fit fixation versus quadruple hamstring graft and interference screw fixation - a matched pair analysis after one year follow up. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-019-2499-y
Akoto R, Hoeher J (2012) Anterior cruciate ligament (ACL) reconstruction with quadriceps tendon autograft and press-fit fixation using an anteromedial portal technique. BMC Musculoskelet Disord. https://doi.org/10.1186/1471-2474-13-161
Aslam MA, Avasthi S, Aggarwal P, Singh S, Kumar V, Mahapatra S (2021) Clinical outcomes of anterior cruciate ligament reconstruction using quadriceps tendon autograft versus hamstring tendons autograft: a retrospective analysis. Cureus. https://doi.org/10.7759/cureus.18760
Barié A, Koepf M, Jaber A, Moradi B, Schmitt H, Huber J, Streich NA (2018) Long-term follow-up after anterior cruciate ligament reconstruction using a press-fit quadriceps tendon-patellar bone autograft. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-018-2271-8
Barié A, Sprinckstub T, Huber J, Jaber A (2020) Quadriceps tendon vs. patellar tendon autograft for ACL reconstruction using a hardware-free press-fit fixation technique: comparable stability, function and return-to-sport level but less donor site morbidity in athletes after 10 years. Arch Orthop Trauma Surg 140:1465–1474
Cancienne JM, Browning R, Werner BC (2020) Patient-related risk factors for contralateral anterior cruciate ligament (ACL) tear after ACL reconstruction: an analysis of 3707 primary ACL reconstructions. HSS J 16:226–229
Cavaignac E, Coulin B, Tscholl P, Fatmy NNM, Duthon V, Menetrey J (2017) Is quadriceps tendon autograft a better choice than hamstring autograft for anterior cruciate ligament reconstruction? a comparative study with a mean follow-up of 3.6 years. Am J Sports Med 45:1326–1332
Chivot M, Pioger C, Cognault J, Sharma A, Pailhe R, Cavaignac E, Ollivier M, Jacquet C (2020) Every layer of quadriceps tendon’s central and medial portion offers similar tensile properties than Hamstrings or Ilio-tibial band grafts. J Exp Orthop. https://doi.org/10.1186/s40634-020-00261-7
Clavien PA, Barkun J, de Oliveira ML, Vauthey JN, Dindo D, Schulick RD, de Santibañes E, Pekolj J, Slankamenac K, Bassi C, Graf R, Vonlanthen R, Padbury R, Cameron JL, Makuuchi M (2009) The Clavien-Dindo classification of surgical complications: five-year experience. Ann Surg 250:187–196
Csapo R, Runer A, Hoser C, Fink C (2021) Contralateral ACL tears strongly contribute to high rates of secondary ACL injuries in professional ski racers. Knee Surg Sports Traumatol Arthrosc 29:1805–1812
Dai W, Leng X, Wang J, Cheng J, Hu X, Ao Y (2021) Quadriceps tendon autograft versus bone-patellar tendon-bone and hamstring tendon autografts for anterior cruciate ligament reconstruction: a systematic review and meta-analysis. Am J Sports Med. https://doi.org/10.1177/03635465211030259
Fu FH, Rabuck SJ, West RV, Tashman S, Irrgang JJ (2019) Patellar fractures after the harvest of a quadriceps tendon autograft with a bone block: a case series. Orthop J Sports Med. https://doi.org/10.1177/2325967119829051
Gagliardi AG, Carry PM, Albright JC, Daoud AK, Parikh HB (2018) Internal brace ACL repair is associated with high failure rate in the first two years post-surgery. Orthop J Sports Med. https://doi.org/10.1177/2325967118S00068
Gagliardi AG, Carry PM, Parikh HB, Albright JC (2020) Outcomes of quadriceps tendon with patellar bone block anterior cruciate ligament reconstruction in adolescent patients with a minimum 2 year follow-up. Am J Sports Med 48:93–98
Gagliardi AG, Carry PM, Parikh HB, Traver JL, Howell DR, Albright JC (2019) ACL repair with suture ligament augmentation is associated with a high failure rate among adolescent patients. Am J Sports Med 47:560–566
Galan H, Escalante M, Della Vedova F, Slullitel D (2020) All inside full thickness quadriceps tendon ACL reconstruction: Long term follow up results. J Exp Orthop. https://doi.org/10.1186/s40634-020-00226-w
Gobbi A, Karnatzikos G, Chaurasia S, Abhishek M, Bulgherhoni E, Lane J (2016) Postoperative infection after anterior cruciate ligament reconstruction. Sports Health 8:187–189
Goto K, Duthon VB, Menetrey J (2022) Anterior cruciate ligament reconstruction using quadriceps tendon autograft is a viable option for small-statured female patients. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-021-06845-9
Greif DN, Shallop BJ, Allegra PR, Cade WH 2nd, Minesinger KE, Luxenburg D, Kaplan LD, Baraga MG (2021) A comparison of 2 year ACL reconstruction clinical outcomes using all-soft tissue quadriceps tendon autograft with femoral/tibial cortical suspensory fixation versus tibial interference screw fixation. Arthroscopy. https://doi.org/10.1016/j.arthro.2021.06.024
Hadjicostas PT, Soucacos PN, Berger I, Koleganova N, Paessler HH (2007) Comparative analysis of the morphologic structure of quadriceps and patellar tendon: a descriptive laboratory study. Arthroscopy 23:744–750
Higgins LD, Taylor MK, Park D, Ghodadra N, Marchant M, Pietrobon R, Cook C, International Knee Documentation Committee (2007) Reliability and validity of the International knee documentation committee (ikdc) subjective knee form. Joint Bone Spine 74:594–599
Hogan DW, Burch MB, Rund JM, Geeslin DW, Ma R, Gray AF, Chu CR, Ray TE, Pullen WM, Sherman SL (2021) No difference in complication rates or patient-reported outcomes between bone-patella tendon–bone and quadriceps tendon autograft for anterior cruciate ligament reconstruction. Arthrosc Sports Med Rehabil. https://doi.org/10.1016/j.asmr.2021.10.019
Horstmann H, Petri M, Tegtbur U, Felmet G, Krettek C, Jagodzinski M (2021) Quadriceps and hamstring tendon autografts in ACL reconstruction yield comparably good results in a prospective, randomized controlled trial. Arch Orthop Trauma Surg. https://doi.org/10.1007/s00402-021-03862-8
Horteur C, Cavalie G, Gaulin B, Bacry MC, Morin V, Cavaignac E, Pailhe R (2020) Saphenous nerve injury after anterior cruciate ligament reconstruction: reduced numbness area after ligamentoplasty using quadriceps tendon compared with hamstring tendon. Knee 27:1151–1157
Hunnicutt JL, Xerogeanes JW, Tsai L-C, Sprague PA, Newsome M, Slone HS, Lyle MA (2021) Terminal knee extension deficit and female sex predict poorer quadriceps strength following ACL reconstruction using all-soft tissue quadriceps tendon autografts. Knee Surg Sports Traumatol Arthrosc 29:3085–3095
Inderhaug E, Strand T, Solheim E (2015) The impact of sensory deficits after harvesting hamstrings autograft for ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 23:1060–1064
Iriuchishima T, Ryu K, Okano T, Suruga M, Aizawa S, Fu FH (2017) The evaluation of muscle recovery after anatomical single-bundle ACL reconstruction using a quadriceps autograft. Knee Surg Sports Traumatol Arthrosc 25:1449–1453
Irrgang J, Tashman S, Patterson C, Musahl V, West R, Oostdyk A, Galvin B, Poploski K, Fu F (2021) Anatomic single vs. double-bundle ACL reconstruction: a randomized clinical trial-Part 1: clinical outcomes. Knee Surg Sports Traumatol Arthrosc 29:2665–2675
Jacquet C, Pioger C, Khakha R, Argenson J-N, Ollivier M, Seil R, Parratte S, Steltzlen C, Pujol N (2021) Incidence and risk factors for residual high-grade pivot shift after ACL reconstruction with or without a lateral extra-articular tenodesis. Orthop J Sports Med. https://doi.org/10.1177/23259671211003590
Johnson KP, Turk RD, Bastrom TP, Boutelle KE, Pennock AT, Chambers HG, Edmonds EW (2019) Transphyseal anterior cruciate ligament reconstruction in the skeletally immature: quadriceps tendon autograft versus hamstring tendon autograft. Orthop J Sports Med. https://doi.org/10.1177/2325967119872450
Johnston PT, Feller JA, McClelland JA, Webster KE (2021) Strength deficits and flexion range of motion following primary anterior cruciate ligament reconstruction differ between quadriceps and hamstring autografts. J ISAKOS 6:88–93
Kambhampati SBS, Gollamudi S, Shanmugasundaram S, Josyula VVS (2020) Cyclops lesions of the knee: a narrative review of the literature. Orthop J Sports Med. https://doi.org/10.1177/2325967120945671
Karpinski K, Haener M, Bierke S, Diermeier T, Petersen W (2021) Comparing knee laxity after anatomic anterior cruciate ligament reconstruction using quadriceps tendon versus semitendinosus tendon graft. Orthop J Sports Med. https://doi.org/10.1177/23259671211014849
Kawata M, Sasabuchi Y, Taketomi S, Inui H, Matsui H, Fushimi K, Yasunaga H, Tanaka S (2018) Atopic dermatitis is a novel demographic risk factor for surgical site infection after anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:3699–3705
Kim BH, Kim JI, Lee O, Lee KW, Lee MC, Han HS (2018) Preservation of remnant with poor synovial coverage has no beneficial effect over remnant sacrifice in anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 26:2345–2352
Kim S-J, Jo S-B, Kim T-W, Chang J-H, Choi H-S, Oh K-S (2009) A modified arthroscopic anterior cruciate ligament double-bundle reconstruction technique with autogenous quadriceps tendon graft: remnant-preserving technique. Arch Orthop Trauma Surg 129:403–407
Kohl S, Stutz C, Decker S, Ziebarth K, Slongo T, Ahmad SS, Kohlhof H, Eggli S, Zumstein M, Evangelopoulos DS (2014) Mid-term results of transphyseal anterior cruciate, ligament reconstruction in children and adolescents. Knee 21:80–85
Korol E, Johnston K, Waser N, Sifakis F, Jafri HS, Lo M, Kyaw MH (2013) A systematic review of risk factors associated with surgical site infections among surgical patients. PLoS ONE 8:e83743
Kwak Y-H, Lee S, Lee MC, Han H-S (2018) Anterior cruciate ligament reconstruction with quadriceps tendon-patellar bone allograft: matched case control study. BMC Musculoskelet Disord. https://doi.org/10.1186/s12891-018-1959-0
Lazarides AL, Alentorn-Geli E, Vinson EN, Hash TW, Samuelsson K, Toth AP, Moorman CT, Garrett WE, Taylor DC (2018) Advanced patellar tendinopathy is associated with increased rates of bone-patellar tendon–bone autograft failure at early follow-up after anterior cruciate ligament reconstruction. Orthop J Sports Med. https://doi.org/10.1177/2325967118807710
Lee JK, Lee S, Lee MC (2016) Outcomes of anatomic anterior cruciate ligament reconstruction: bone-quadriceps tendon graft versus double-bundle hamstring tendon graft. Am J Sports Med 44:2323–2329
Lee JK, Lee S, Seong SC, Lee MC (2014) Anatomic single-bundle ACL reconstruction is possible with use of the modified transtibial technique: a comparison with the anteromedial transportal technique. J Bone Joint Surg 96:664–672
Lee MC, Lee JK, Lee S, Kim TW, Park SJ, Im SH, Seong SC (2013) Single bundle anterior cruciate ligament reconstruction using quadriceps tendon-bone autograft: mid to long term follow-up. Arthroscopy 29:e144
Lind M, Nielsen T, Soerensen O, Mygind-Klavsen B, Faunø P (2020) Quadriceps tendon grafts does not cause patients to have inferior subjective outcome after anterior cruciate ligament (ACL) reconstruction than do hamstring grafts: a 2 year prospective randomised controlled trial. Br J Sports Med 54:183–187
Lind M, Strauss MJ, Nielsen T, Engebretsen L (2021) Low surgical routine increases revision rates after quadriceps tendon autograft for anterior cruciate ligament reconstruction: results from the danish knee ligament reconstruction registry. Knee Surg Sports Traumatol Arthrosc 29:1880–1886
Lund B, Nielsen T, Faunø P, Christiansen S, Lind M (2014) Is quadriceps tendon a better graft choice than patellar tendon? a prospective randomized study. Arthroscopy 30:593–598
Lyman S, Lee Y-Y, Franklin PD, Li W, Cross MB, Padgett DE (2016) Validation of the KOOS, JR: a short-form knee arthroplasty outcomes survey. Clin Orthop 474:1461–1471
Magnussen RA, Verlage M, Flanigan DC, Kaeding CC, Spindler KP (2015) Patient-reported outcomes and their predictors at minimum 10 years after anterior cruciate ligament reconstruction: a systematic review of prospectively collected data. Orthop J Sports Med. https://doi.org/10.1177/2325967115573706
Malinowski K, Ebisz M, LaPrade RF, Mostowy M (2021) Platelet-rich plasma in anterior cruciate ligament quadriceps tendon bone reconstruction-impact of PRP administration on pain, range of motion restoration, knee stability, tibial tunnel widening and functional results. Appl Sci 11(9):3993
Malliaras P, Cook J, Purdam C, Rio E (2015) Patellar tendinopathy: clinical diagnosis, load management, and advice for challenging case presentations. J Orthop Sports Phys Ther 45:887–898
Marom N, Kapadia M, Nguyen JT, Ammerman B, Boyle C, Wolfe I, Halvorsen KC, Miller AO, Henry MW, Brause BD, Hannafin JA, Marx RG, Ranawat AS (2022) Factors associated with an intra-articular infection after anterior cruciate ligament reconstruction: a large single-institution cohort study. Am J Sports Med 50:1229–1236
Martin-Alguacil J, Arroyo-Morales M, Martín-Gomez J, Monje-Cabrera I, Abellán-Guillén J, Esparza-Ros F, Lozano M, Cantarero-Villanueva I (2018) Strength recovery after anterior cruciate ligament reconstruction with quadriceps tendon versus hamstring tendon autografts in soccer players: a randomized controlled trial. Knee 25:704–714
Mouarbes D, Dagneaux L, Olivier M, Lavoue V, Peque E, Berard E, Cavaignac E (2020) Lower donor-site morbidity using QT autografts for ACL reconstruction. Knee Surg Sports Traumatol Arthrosc 28:2558–2566
Mutsuzaki H, Kinugasa T, Sakane M (2019) Safety and feasibility of using calcium phosphate hybridization method for quadriceps tendon-bone graft in anterior cruciate ligament reconstruction. J Orthop 16:422–425
Nekolaichuk E (2022) Research guides: Searching the Literature: A Guide to Comprehensive Searching in the Health Sciences: Grey Literature. https://guides.library.utoronto.ca/c.php?g=577919&p=4123572. Accessed 5 Mar 2022
Noailles T, Chalopin A, Boissard M, Lopes R, Bouguennec N, Hardy A (2019) Incidence and risk factors for cyclops syndrome after anterior cruciate ligament reconstruction: A systematic literature review. Orthop Traumatol Surg Res 105:1401–1405
Noyes FR (2009) The function of the human anterior cruciate ligament and analysis of single- and double-bundle graft reconstructions. Sports Health 1:66–75
Ouweleen AJ, Hall TB, Finlayson CJ, Patel NM (2021) Predictors of arthrofibrosis after pediatric anterior cruciate ligament reconstruction: what is the impact of quadriceps autograft? J Pediatr Orthop 41:395–399
Pache S, Del Castillo J, Moatshe G, LaPrade RF (2020) Anterior cruciate ligament reconstruction failure and revision surgery: current concepts. J ISAKOS 5:351–358
Page MJ, McKenzie JE, Bossuyt PM, Boutron I, Hoffmann TC, Mulrow CD, Shamseer L, Tetzlaff JM, Akl EA, Brennan SE, Chou R, Glanville J, Grimshaw JM, Hróbjartsson A, Lalu MM, Li T, Loder EW, Mayo-Wilson E, McDonald S, McGuinness LA, Stewart LA, Thomas J, Tricco AC, Welch VA, Whiting P, Moher D (2021) The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. Brit Med J 372:n71
Pailhe R, Cavaignac E, Murgier J, Laffosse J-M, Swider P (2015) Biomechanical study of ACL reconstruction grafts. J Orthop Res 33:1188–1196
Pandey V, Madi S, Joseph A, Acharya K (2015) Late quadriceps tendon rupture at the donor site following cruciate ligament reconstruction using central quadriceps tendon graft. Brit Med J Case Rep. https://doi.org/10.1136/bcr-2015-212621
Parikh HB, Gagliardi AG, Howell DR, Albright JC, Mandler TN (2020) Femoral nerve catheters and limb strength asymmetry at 6 months after primary anterior cruciate ligament reconstruction in pediatric patients. Pediatr Anesth 30:1109–1115
Perez JR, Emerson CP, Barrera CM, Greif DN, Cade WH II, Kaplan LD, Baraga MG (2019) Patient-reported knee outcome scores with soft tissue quadriceps tendon autograft are similar to bone-patellar tendon-bone autograft at minimum 2 year follow-up: a retrospective single-center cohort study in primary anterior cruciate ligament reconstruction surgery. Orthop J Sports Med. https://doi.org/10.1177/2325967119890063
Poehling-Monaghan KL, Salem H, Ross KE, Secrist E, Ciccotti MC, Tjoumakaris F, Ciccotti MG, Freedman KB (2017) Long-Term outcomes in anterior cruciate ligament reconstruction: a systematic review of patellar tendon versus hamstring autografts. Orthop J Sports Med. https://doi.org/10.1177/2325967117709735
Premkumar A, Samady H, Slone H, Hash R, Karas S, Xerogeanes J (2016) Liposomal bupivacaine for pain control after anterior cruciate ligament reconstruction: a prospective, double-blinded, randomized, positive-controlled trial. Am J Sports Med 44:1680–1686
Runer A, Csapo R, Hepperger C, Herbort M, Hoser C, Fink C (2020) Anterior cruciate ligament reconstructions with quadriceps tendon autograft result in lower graft rupture rates but similar patient-reported outcomes as compared with hamstring tendon autograft: a comparison of 875 patients. Am J Sports Med 48:2195–2204
Runer A, Suter A, Roberti di Sarsina T, Hepperger C, Gföller P, Hoser C, Csapo R, Fink C (2021) Quadriceps Tendon- Vs. Hamstring Tendon Autograft In Primary Anterior Cruciate Ligament Reconstruction: A Matched-Pairs Study With A Mean Follow-Up Of 6.5 Years. Paper presented at the German congress of orthopaedics and traumatology, German Medical Society, Berlin, 26–29.
Runer A, Wierer G, Herbst E, Hepperger C, Herbort M, Gfoeller P, Hoser C, Fink C (2018) There is no difference between quadriceps- and hamstring tendon autografts in primary anterior cruciate ligament reconstruction: a 2 year patient-reported outcome study. Knee Surg Sports Traumatol Arthrosc 26:605–614
Saper M, Wong C, Strauss N (2021) Adolescent patients exhibit significant improvements in strength and functional performance from 6 to 9 months after ACL reconstruction with quadriceps autograft. Arthrosc Sports Med Rehabil 3:e837–e843
Schmucker M, Haraszuk J, Holmich P, Barfod KW (2021) Graft failure, revision ACLR, and reoperation rates after ACLR with quadriceps tendon versus hamstring tendon autografts: a registry study with review of 475 patients. Am J Sports Med 49:2136–2143
Schulz AP, Lange V, Gille J, Voigt C, Frohlich S, Stuhr M, Jurgens C (2013) Anterior cruciate ligament reconstruction using bone plug-free quadriceps tendon autograft: intermediate-term clinical outcome after 24–36 months. J Sports Med 4:243–249
Sevimli R, Gormeli G, Polat H, Kilinc O, Turkmen E, Aslanturk O (2020) Comparison of medium-term revision rates after autograft and allograft anterior cruciate ligament reconstruction. Ann Ital Chir 91:410–416
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J, Moher D, Tugwell P, Welch V, Kristjansson E, Henry DA (2017) AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. Brit Med J. https://doi.org/10.1136/bmj.j4008
Slim K, Nini E, Forestier D, Kwiatkowski F, Panis Y, Chipponi J (2003) Methodological index for non-randomized studies (MINORS): development and validation of a new instrument. ANZ J Surg 73(9):712–716
Slone HS, Xerogeanes JW (2014) Anterior cruciate ligament reconstruction with quadriceps tendon autograft: a minimally invasive harvest technique. J Bone Joint Surg Essent Surg Tech 4:e16–e16
Sofu H, Sahin V, Gursu S, Yildirim T, Issin A, Ordueri M (2013) Use of quadriceps tendon versus hamstring tendon autograft for arthroscopic anterior cruciate ligament reconstruction: a comparative analysis of clinical results. Eklem Hastalik Cerrahisi 24:139–143
Sonnery-Cottet B, Lavoie F, Ogassawara R, Kasmaoui H, Scussiato RG, Kidder JF, Chambat P (2010) Clinical and operative characteristics of cyclops syndrome after double-bundle anterior cruciate ligament reconstruction. Arthroscopy 26:1483–1488
Stucken C, Garras DN, Shaner JL, Cohen SB (2013) Infections in anterior cruciate ligament reconstruction. Sports Health 5:553–557
Swärd P, Kostogiannis I, Roos H (2010) Risk factors for a contralateral anterior cruciate ligament injury. Knee Surg Sports Traumatol Arthrosc 18:277–291
Adrian T, Dan Viorel N, Sergiu C (2019) Outcomes after ACL reconstruction with free quadriceps tendon autograft versus hamstring tendons autograft. A retrospective study with a minimal follow-up 2 years. ACTA Orthop Traumatol Turc 53:180–183
Vaughn NH, Dunleavy ML, Jackson T, Hennrikus W (2022) The outcomes of quadriceps tendon autograft for anterior cruciate ligament reconstruction in adolescent athletes: a retrospective case series. Eur J Orthop Surg Traumatol. https://doi.org/10.1007/s00590-021-03032-x
von Essen C, Sarakatsianos V, Cristiani R, Stalman A (2022) Suture tape reinforcement of hamstring tendon graft reduces postoperative knee laxity after primary ACL reconstruction. J Exp Orthop. https://doi.org/10.1186/s40634-022-00454-2
Wilder JH, Patel AH, Ross BJ, Weldy JM, Wang H, Sherman WF (2022) Fracture risk with patella resurfacing during total knee arthroplasty after anterior cruciate ligament reconstruction using bone-patella-bone autograft: a biomechanical analysis. Arthroplasty Today 13:142–148
Funding
None.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
See conflict of interest forms submitted.
Ethical approval
Not required.
Informed consent
Not required
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
The original online version of this article was revised: The affiliation of the author Yuichi Hoshino corrected and figures 1–3 are ordered correctly.
Supplementary Information
Below is the link to the electronic supplementary material.
167_2022_7175_MOESM1_ESM.docx
Supplementary figure 4 Pooled incidence analysis for contralateral ACL injury. Note that figures 4–18 are available as online supplements. Supplementary figure 5 Pooled incidence analysis for postoperative meniscal issues. Supplementary figure 6 Pooled incidence analysis for cyclops lesion. Supplementary figure 7 Pooled incidence analysis for graft failure. Supplementary figure 8 Pooled incidence analysis for patellar fracture. Supplementary figure 9 Pooled incidence analysis for hardware removal. Supplementary figure 10 Pooled incidence analysis for infection. Supplementary figure 11 Pooled incidence analysis for donorsite quadriceps tendon rupture. Supplementary figure 12 Pooled incidence analysis for anterior knee pain. Supplementary figure 13 Pooled incidence analysis for kneeling pain. Supplementary figure 14 Pooled incidence analysis for sensation deficits. Supplementary figure 15 Pooled incidence analysis for loss of extension. Supplementary figure 16 Pooled incidence analysis for donor-site tendinopathy. Supplementary figure 17 Pooled incidence analysis for cosmetic issue. Supplementary figure 18 Pooled incidence analysis for hematoma (DOCX 902 kb)
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Singh, H., Glassman, I., Sheean, A. et al. Less than 1% risk of donor-site quadriceps tendon rupture post-ACL reconstruction with quadriceps tendon autograft: a systematic review. Knee Surg Sports Traumatol Arthrosc 31, 572–585 (2023). https://doi.org/10.1007/s00167-022-07175-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-022-07175-0