Abstract
Introduction
Comparable data of functional outcomes of anterior cruciate ligament reconstruction using either hamstring- or quadriceps tendon grafts is controversial. This prospective, randomized controlled trial aims to provide data comparing both grafts regarding the functional outcome.
Materials and methods
A two centre trial involving symptomatic patients 18 years of age or older with an anterior cruciate ligament tear was conducted. We randomly assigned 27 patients to quadruple hamstring tendon reconstruction and 24 to quadriceps tendon reconstruction. The patients were evaluated preoperatively, at 3, 6, 12 and 24 months post-surgery. The primary outcome parameter was the side-to-side knee laxity measured with an arthrometer. Secondary outcomes included results in the International Knee Documentation Committee (IKDC) and Lysholm Scores and isokinetic testing of strength in knee extension and flexion.
Results
Forty-four patients (86%) completed the 2-year follow-up. There was significantly improved knee stability at all time intervals with no difference between the two study groups. The manual side-to-side displacement improved by 4.7 ± 3.0 mm in patients with hamstring tendon reconstruction and 5.5 ± 2.9 mm in patients with quadriceps tendon reconstruction. In addition, muscle strength and outcome scores (IKDC and Lysholm Score) did not show any differences between the hamstring tendon group and the quadriceps tendon group. Patients in the hamstring tendon group returned to their pre-injury activity level after 95.2 ± 45.5 days while patients in the quadriceps tendon group needed 82.1 ± 45.6 days.
Conclusion
Quadriceps and hamstring tendon autografts yield comparably good results in primary anterior cruciate ligament reconstruction.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Injury of the anterior cruciate ligaments (ACL) represent the highest burden for sports related disability [24, 33]. ACL reconstruction is recommended for both chronic instabilities and athletes that wish to return early to pivoting sports and fail conservative treatment attempts. There are four major types of graft, which are commonly used for ACL reconstruction: Patellar, hamstring and quadriceps tendon autografts and allografts.
However, due to partially restricted clinical results as well as the legal situation in some countries the use of allografts is limited. The focus stays on autografts with a graft choice between patellar-, hamstring- and quadriceps tendon depending on patients factors and surgeons preferences as well as surgeons experiences [6, 20].
Hamstring tendons are the most commonly used graft in ACL reconstruction, which is due to the good biomechanical characteristics, the clinical outcomes and a reliable harvesting of the graft.
Quadriceps tendon grafts show excellent biomechanical qualities as well. Furthermore, the donor site morbidity is low and its use preserves the hamstring tendons as an ACL agonist [3, 29].
There are some cohort studies that compared knee stability and functional outcome scores of quadriceps- and hamstring tendon autograft, showing similar knee stability and functional outcome scores [7, 21, 29, 32].
To our knowledge only one randomized controlled trial comparing quadriceps- and hamstring tendon autograft has been published [38]. This study revealed similar clinical results and postoperative pain for both groups.
Therefore, high-level data comparing outcomes of quadriceps and hamstring tendon grafts for ACL reconstruction is sparse [35].
The goal of our study was to conduct a randomized, controlled two centre trial involving adults with an acute or chronic tear of the ACL to determine whether reconstruction with a hamstring tendon graft is superior to surgery using quadriceps tendon graft. We hypothesized that quadriceps tendon grafts would provide equal knee stability and comparable clinical results for the Lysholm and IKDC Score with respect to hamstring tendon grafts after 24 months of follow up.
Methods
Demographic data
We conducted a two centre randomized controlled trial involving patients 18 years of age or older with a symptomatic anterior cruciate ligament tear. One blinded surgeon who was not participating during the surgical procedure investigated the patients. The knee incisions were covered by adhesive dressings before follow up. Randomization and reporting were done according to Consort requirements [23]. All eligible subjects were randomly assigned by computer generated random numbers in permuted blocks of 6 to undergo ACL reconstruction with either a hamstring tendon or quadriceps tendon graft. An investigator who was not involved in the randomization procedure prepared all sequentially numbered, opaque, sealed envelopes containing the assigned interventions to ensure that the sequence was concealed. We randomly assigned 27 patients to hamstring tendon reconstruction (H) and 24 to quadriceps tendon reconstruction (Q). Seven patients were lost to follow up. Graft rupture and other complications were recorded but kept for final analysis. See Fig. 1 Consort flow chart. Patients were recruited from December 2010 until June 2013. Details of the demographic data are shown in Table 1.
The local ethics committee approved the study, and informed consent was obtained from all participants. Inclusion as well as exclusion criteria are shown in Table 2.
Surgical technique
Two senior knee surgeons, both with more than 10 years of experience in ACL reconstruction, performed all surgeries in two independent surgical centres.
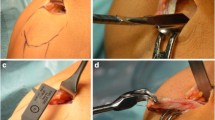
Both surgeons used implant-free press-fit fixation techniques in a standardized fashion as described previously [10, 12, 13, 26]. Briefly, harvest of hamstring and quadriceps tendon was performed in a standard technique. Hamstring tendons were prepared as 4-strand grafts. A cortical-cancellous bone cylinder was sutured into the graft at the tibial end of the graft as a counter bearing [11]. The quadriceps tendon was harvested with a patellar bone block. The femoral tunnel was reamed in the size of the graft using the anteromedial portal technique. The tibial tunnel was similarly reamed using the size of the graft using a standard tibial aiming device. The femoral as well as the tibial tunnel was reamed with a hollow reamer. The cortico-cancellous bone plug, which was harvested before, was applied into the femoral tunnel to fix the graft in a press-fit technique [11]. A standard fluoroscopic lateral X-ray according to Bernard et al. [4] controlled all tunnel positions with a beath pin in centre A.
In both groups, a rehabilitation program with 3 weeks of partial weight bearing, immediate full range of motion and no hinge orthosis was used for all participants [7, 29]. COX-2 inhibitors were administered until pain levels were below a visual analogue scale (VAS) of 4 and then discontinued. Low molecular weight heparin was administered as the standard thromboprophylaxis over the time of partial weight bearing.
Outcome measures
Patients were evaluated preoperatively and at 3, 6, 12 and 24 months after surgery. An independent examiner assessed all patients. At each visit, subjects completed the International Knee Documentation Committee (IKDC) evaluation form [28] and the Lysholm Score [5]. Side-to-side knee laxity was measured on manual maximum testing. Two arthrometers were used (KT-1000 arthrometer (MEDmetric Corp, San Diego, California) in centre A; Articometer (ARTICO Sportklinik, Germany) [19] in centre B). While the construction principle of the two arthrometers is similar, the only difference is that the Articometer measured digitally and the KT1000 measured in a mechanical setup. Strength measurement for extension and flexion in the knee was tested at each visit. Subjects were placed with hip flexed at 80°.
To determine the maximum strength using isokinetic testing, the most common method measuring extension and flexion strength of the lower limb was used [17, 18]. The setup included measurement of the point of rotation and lever arm. Knee strength was assessed using isokinetic parameters at angular velocities of 60°/sec (5 repetitions) with 3 sets and a one-minute break in between the sets. The peak torque value was determined. The testing was performed on a CON-TREX Multi-Joint System (CMV AG, Dübendorf Switzerland) [18]. The results were adjusted with the lever arm of the force and the body weight of the patients. The outcome is presented in Newton per kilogram body weight and compared to the strength of the healthy limb.
Statistical analysis
For the determination of sample size, n-query Advisor 7.0 for Windows (Statcon, Witzenhausen, Germany) was used. The following parameters were chosen for the assessment of sample size: 2-side test, significance level of 0.05, difference in maximum manual knee laxity, difference in Lysholm score and difference in IKDC score of greater than 20% between the groups. For all of these parameters a sample size of 25 per group was sufficient to obtain a power of > 80% [16]. No interim analysis was performed. All reported P values are two-sided.
Baseline characteristics were analyzed by descriptive statistics. All mean values are reported with standard deviations. Analysis of binary and categorical variables between two groups was tested with the two-tailed Fishers exact test and the χ2-test. The 2 groups were compared using a 2-tailed Student’s t test for normal distribution. The Mann–Whitney U test was used as a nonparametric test. A two-sided P value of 0.05 was considered to indicate statistical significance. All reported P values are two-sided and were not adjusted for multiple comparisons. Statistical comparisons were made with the use of SPSS software (SPSS, Chicago, Illinois), version 24.
Results
There was significantly improved knee stability, IKDC Score, Lysholm Score and pivot shift measurement at two-year follow-up. No significant difference was observed between the hamstring and quadriceps tendon group at any time. No significant difference between the two study groups was detected for return to work or sport. Complete data are shown in Table 3.
Strength for knee flexion and extension
The data of knee extension strength are shown in Fig. 2. No significant difference between group H and Q was noted.
Extension Maximum Strength (injured–healthy knee extension) in Newton per kg bodyweight (mean ± SD, significance is marked with *) measured with isokinetic testing of the hamstring- and quadriceps tendon group (No. at data point represents the number of patients from preoperatively to two years of follow up)
The data of knee flexion strength are shown in Fig. 3. Similar to knee extension strength, no significant difference between the groups was observed.
Flexion Maximum Strength (injured – healthy knee flexion) in Newton per kg bodyweight (mean ± SD, significance is marked with *) measured with isokinetic testing of the hamstring- and quadriceps tendon group (No. at data point represents the number of patients from preoperatively to two years of follow up)
Adverse events
Clinical records were reviewed for all study visits. Anaesthesia and surgery records were retrieved for all surgical procedures, including the initial study treatment. There were six complications overall. In the hamstring tendon group, there was one graft retear, which was treated with revision ACL reconstruction with quadriceps tendon and one residual anteromedial knee instability, which was treated with reconstruction of the medial collateral knee ligament and revision of the ACL graft. In the quadriceps tendon group, there was one early infection, which was treated transplant retaining with antibiotics and arthroscopic lavage and three ACL graft retears, which were treated with ACL graft revision (two revision reconstructions with hamstring tendon graft and one healing response). The data of the two study groups did not differ significantly for retear rates or overall complications.
Discussion
The most important finding of this study was that quadriceps tendon grafts yield comparably good results to hamstring tendon grafts in primary autograft ACL reconstruction at 2-year follow-up. No significant difference was found for IKDC- or Lysholm Score, anterior–posterior instability or Pivot shift.
There is no significant difference between quadriceps and hamstrings tendon graft fixation in a cadaveric study [9]. Ultimate failure loads for quadriceps and hamstring tendon grafts have been reported between 2352 and 4090 N.[25, 40]. Clinical data comparing quadriceps and hamstring tendon grafts are sparse. To the best of our knowledge, there is no randomized controlled trial comparing quadriceps tendon graft with hamstring tendon graft in primary ACL reconstruction with a follow up of two years. Nevertheless, there is a number of cohort studies which, compare quadriceps tendon and hamstring tendon reconstruction [7, 21, 29]. Besides the lower level of evidence, several differences of study design of these trials have to be taken into account. Contrary to our study, these former studies lack in strength testing and the presentation of side-to-side stability measured with arthrometer [29] or reporting about retears in their cohort [21]. A recently published randomized controlled trial, which compares quadriceps tendon autograft with hamstring tendon autograft reports similar clinical results and post-operative pain levels compared to our study [38]. However, this study has a sample size of only 28 analysed patients and only a 12-month follow-up [38]. In addition, no information on complications, strength and stability is provided.
Our study showed no significant difference between the two groups either, which is consistent with former studies. Different level I or II studies did not detect any difference in clinical performance no matter what treatment protocol was used [14, 28, 38, 41, 41, 42]. Our study showed that both surgical techniques result in a firm ACL reconstruction without a significant elongation of the graft during the observed time interval of 24 months. This was tested in centre A with the KT-1000 arthrometer, which is a commonly used instrument to measure the anterior–posterior laxity of the knee [1] and the Articometer [19] in centre B. Likewise the postoperative reduction of instability, measured by the antero–posterior translation, has previously been shown [21]. Biomechanical studies assume that there is a significant lengthening of the graft in the first couple of thousands cycles with medium load [31]. Similar to our trial, previous clinical studies detected no difference regarding side-to-side stability between the two graft types [7, 29]. Postoperative strength of extension of the injured knee is starting with a deficit, which is almost compensated towards the end of the 2-year follow-up time. In accordance with a previous study no extension strength deficit was found for quadriceps tendon grafts [7]. The greater postoperative weakness of knee extension in the injured limb compared to the healthy limb has been described previously [37]. Surprisingly, preoperative data in our study showed higher extension strength in the hamstring tendon group than in the quadriceps tendon group. Although previous data showed that relevant preoperative strength deficits lead to persisting reduction in strength for up to two years of follow up [8], our data did not confirm this finding. The postoperative strength rehabilitation developed similarly between the quadriceps and hamstring tendon group. An explanation for that result might either be measurement errors or, which is more likely, a randomization bias. The development of the flexion strength of the injured lower limb compared to the healthy limb did not differ significantly between the hamstring tendon group and the quadriceps tendon group. The postoperative strength showed a peak at the 1-year mark and dropped slightly, but not significantly, afterwards. These results are similar to previous trials [7, 21]. Consistently to the results by Lee et al., our data showed a slight but not significant weakness of the hamstring tendon group compared to the quadriceps tendon group in flexion strength recovery [21].
In cases of additional medial knee joint instability, it is desirable to preserve the hamstring tendons contributing to medial joint stability. Furthermore, some hamstring tendons might have previously been used for other reconstruction surgeries or might be too small in diameter to obtain a sufficient ACL graft. In these cases, the quadriceps tendon offers a promising alternative, providing sufficient graft thickness and avoiding weakening of medial joint stability [29].
There was a non-significant tendency towards more graft ruptures in centre B (three full thickness retears and one partial retear), compared with one graft elongation in a patient with recurrent anteromedial instability in centre A, leading up to an overall graft retear rate of 9.8%. The graft ruptures were divided into two hamstrings tendon ruptures and three quadriceps tendon ruptures. A possible reason might be the faster rehabilitation and earlier return to sport in centre B. The graft ruptures had all been adequate traumata with insufficient muscular performance, which are typical for young athletes returning back to competition too early. The overall rate of graft ruptures in our study seems to be slightly higher than in most previous studies [15, 27, 30]. However, a similar graft rupture rate of 9.4% has been reported previously [2].
Several limitations apply to this study. First, the relatively low number of patients failed to accomplish the determined sample size. Nevertheless, a high follow-up rate of 86% could be obtained. Second, randomization lead to three mismatches. The male/female ratio, the height of the patients and age differed significantly between the two groups. Owing to randomization, we had no control of the male/female ratio. It has been shown that the male/female ratio [38] as well as age of the patients [2] might have an impact on the outcome in ACL reconstruction. The graft size differed between the two groups, which might have been a result of the male/female mismatch as well. Retrospectively, the inclusion criteria for age could have been more strict. Furthermore, 5-strand or 6 strand hamstring autografts could have been used when undersized diameter grafts were harvested [22]. Compared to male patients, female patients reported significantly less extensor muscle strength and less improvement 1 year after ACL reconstruction [18], which could have had an impact on our strength results. Similarly, the significant difference of mean age between the two groups could as well have biased results [36, 39]. The height should not have an impact on the overall outcome, particularly as the BMI did not differ significantly [34].
Future randomized studies with an even-handed male/female ratio as well as balanced age groups should be conducted. Sufficient sample sizes and homogeneous surgical techniques are desirable to determine the optimal graft choice in primary ACL reconstruction.
Conclusion
This prospective randomized controlled trial comparing quadriceps and hamstring tendon autografts in bone plug technique ACL reconstruction showed comparably good results in the Lysholm- and IKDC Score, anterior knee stability, strength for knee extension and flexion as well as return to work and sport at a follow-up of 24 months.
Abbreviations
- ACL:
-
Anterior cruciate ligament
- BMI:
-
Body mass index
- Centre A:
-
Trauma Department, Hannover Medical School (MHH), Carl-Neuberg-Str. 1, 30625 Hannover, Germany
- Centre B:
-
ARTICO Sportklinik, Hirschbergstrasse 25, 78045 Villingen-Schwenningen, Germany
- Group H:
-
Group of patients operated with hamstring tendon graft
- Group Q:
-
Group of patients operated with quadriceps tendon graft
- IKDC:
-
International Knee Documentation Committee Score
- Kg:
-
Kilogram
- MRI Scan:
-
Magnetic resonance imaging
- SD:
-
Standard deviation
References
Anderson AF, Lipscomb AB (1989) Preoperative instrumented testing of anterior and posterior knee laxity. Am J Sports Med 17:387–392
Barber FA, Cowden CH 3rd, Sanders EJ (2014) Revision rates after anterior cruciate ligament reconstruction using bone-patellar tendon-bone allograft or autograft in a population 25 years old and younger. Arthroscopy 30:483–491
Barie A, Sprinckstub T, Huber J, Jaber A (2020) Quadriceps tendon vs. patellar tendon autograft for ACL reconstruction using a hardware-free press-fit fixation technique: comparable stability, function and return-to-sport level but less donor site morbidity in athletes after 10 years. Arch Orthop Trauma Surg 140:1465–1474
Bernard M, Hertel P, Hornung H, Cierpinski T (1997) Femoral insertion of the ACL Radiographic quadrant method. Am J Knee Surg 10:14–21 (discussion 21–2)
Briggs KK, Lysholm J, Tegner Y, Rodkey WG, Kocher MS, Steadman JR (2009) The reliability, validity, and responsiveness of the Lysholm score and Tegner activity scale for anterior cruciate ligament injuries of the knee: 25 years later. Am J Sports Med 37:890–897
Budny J, Fox J, Rauh M, Fineberg M (2017) Emerging Trends in Anterior Cruciate Ligament Reconstruction. J Knee Surg 30:63–69
Cavaignac E, Coulin B, Tscholl P, Nik Mohd Fatmy N, Duthon V, Menetrey J (2017) Is quadriceps tendon autograft a better choice than hamstring autograft for anterior cruciate ligament reconstruction? A comparative study with a mean follow-up of 3.6 years. Am J Sports Med 45:1326–1332
Eitzen I, Holm I, Risberg MA (2009) Preoperative quadriceps strength is a significant predictor of knee function two years after anterior cruciate ligament reconstruction. Br J Sports Med 43:371–376
Ettinger M, Werner-Lebeda T, Calliess T, Omar M, Becher C, Ezechieli M, Klintschar M, Petri M (2016) Femoral interference screw fixation of hamstring and quadriceps tendons for ACL reconstruction. Knee Surg Sports Traumatol Arthrosc
Felmet G (2017) Press-Fit ACL Reconstruction, in Controversies in the Technical Aspects of ACL Reconstruction: An Evidence-Based Medicine Approach. ISAKOS: Springer S.Z. Norimasa Nakamura, Robert G. Marx, Volker Musahl:247–261
Felmet G (2012) Anatomic Double Bundle single tunnel Foreign Material Free ACL-Reconstruction - a technical note. Muscles Ligaments Tendons J 1:148–152
Felmet G (2010) Implant-free anterior cruciate ligament reconstruction with diamond instruments. A biological and anatomic method for every ligament transplantation. Unfallchirurg 113:621–628
Felmet G (2010) Implant-free press-fit fixation for bone–patellar tendon-bone ACL reconstruction: 10-year results. Arch Orthop Trauma Surg 130:985–992
Frobell RB, Roos EM, Roos HP, Ranstam J, Lohmander LS (2010) A randomized trial of treatment for acute anterior cruciate ligament tears. N Engl J Med 363:331–342
Gupta R, Sood M, Malhotra A, Masih GD, Kapoor A, Raghav M, Dhillon M (2017) Low re-rupture rate with BPTB autograft and semitendinosus gracilis autograft with preserved insertions in ACL reconstruction surgery in sports persons. Knee Surg Sports Traumatol Arthrosc
Jagodzinski M, Geiges B, von Falck C, Knobloch K, Haasper C, Brand J, Hankemeier S, Krettek C, Meller R (2010) Biodegradable screw versus a press-fit bone plug fixation for hamstring anterior cruciate ligament reconstruction: a prospective randomized study. Am J Sports Med 38:501–508
Kannus P (1992) Normality, variability and predictability of work, power and torque acceleration energy with respect to peak torque in isokinetic muscle testing. Int J Sports Med 13:249–256
Kim do K, Park WH, (2015) Sex differences in knee strength deficit 1 year after anterior cruciate ligament reconstruction. J Phys Ther Sci 27:3847–3849
Krauter A, Rohnstock L, Moeller K, Zhao Z, Felmet G (2012) Instrumented Arthrometry of the anterior cruciate ligament. A comparison, Biomed Tech (Berl)
Kurz A, Evaniew N, Yeung M, Samuelsson K, Peterson D, Ayeni OR (2017) Credibility and quality of meta-analyses addressing graft choice in anterior cruciate ligament reconstruction: a systematic review. Knee Surg Sports Traumatol Arthrosc 25:538–551
Lee JK, Lee S, Lee MC (2016) Outcomes of anatomic anterior cruciate ligament reconstruction: bone-quadriceps tendon graft versus double-bundle hamstring tendon graft. Am J Sports Med 44:2323–2329
Mariscalco MW, Flanigan DC, Mitchell J, Pedroza AD, Jones MH, Andrish JT, Parker RD, Kaeding CC, Magnussen RA (2013) The influence of hamstring autograft size on patient-reported outcomes and risk of revision after anterior cruciate ligament reconstruction: a Multicenter Orthopaedic Outcomes Network (MOON) Cohort Study. Arthroscopy 29:1948–1953
Moher D, Jones A, Lepage L, CONSORT Group (Consolidated Standards for Reporting of Trials) (2001) Use of the CONSORT statement and quality of reports of randomized trials: a comparative before-and-after evaluation. JAMA 285:1992–1995
Morvan A, Bouguennec N, Graveleau N (2020) ACL injuries before 15 years of age: could the young become an athlete? Arch Orthop Trauma Surg 140:1055–1063
Noyes FR, Butler DL, Grood ES, Zernicke RF, Hefzy MS (1984) Biomechanical analysis of human ligament grafts used in knee-ligament repairs and reconstructions. J Bone Joint Surg Am 66:344–352
Paessler HH, Mastrokalos DS (2003) Anterior cruciate ligament reconstruction using semitendinosus and gracilis tendons, bone patellar tendon, or quadriceps tendon-graft with press-fit fixation without hardware. A new and innovative procedure. Orthop Clin North Am 34:49–64
Persson A, Fjeldsgaard K, Gjertsen JE, Kjellsen AB, Engebretsen L, Hole RM, Fevang JM (2014) Increased risk of revision with hamstring tendon grafts compared with patellar tendon grafts after anterior cruciate ligament reconstruction: a study of 12,643 patients from the Norwegian Cruciate Ligament Registry, 2004–2012. Am J Sports Med 42:285–291
Pinczewski LA, Lyman J, Salmon LJ, Russell VJ, Roe J, Linklater J (2007) A 10-year comparison of anterior cruciate ligament reconstructions with hamstring tendon and patellar tendon autograft: a controlled, prospective trial. Am J Sports Med 35:564–574
Runer A, Wierer G, Herbst E, Hepperger C, Herbort M, Gfoller P, Hoser C, Fink C (2018) There is no difference between quadriceps- and hamstring tendon autografts in primary anterior cruciate ligament reconstruction: a 2-year patient-reported outcome study. Knee Surg Sports Traumatol Arthrosc 26:605–614
Salmon L, Russell V, Musgrove T, Pinczewski L, Refshauge K (2005) Incidence and risk factors for graft rupture and contralateral rupture after anterior cruciate ligament reconstruction. Arthroscopy 21:948–957
Simonian PT, Levine RE, Wright TM, Wickiewicz TL, Warren RF (2000) Response of hamstring and patellar tendon grafts for anterior cruciate ligament reconstruction during cyclic tensile loading. Am J Knee Surg 13:8–12
Sofu H, Sahin V, Gursu S, Yildirim T, Issin A, Ordueri M (2013) Use of quadriceps tendon versus hamstring tendon autograft for arthroscopic anterior cruciate ligament reconstruction: a comparative analysis of clinical results. Eklem Hastalik Cerrahisi 24:139–143
Spindler KP, Wright RW (2008) Clinical practice. Anterior cruciate ligament tear. N Engl J Med 359:2135–2142
Stropnik D, Sajovic M, Kacin A, Pavlic-Zaloznik S, Drobnic M (2020) Early clinical and neuromuscular properties in patients with normal or sub-normal subjective knee function after anterior cruciate ligament reconstruction. Arch Orthop Trauma Surg 140:1231–1239
Svantesson E, Hamrin Senorski E, Webster KE, Karlsson J, Diermeier T, Rothrauff BB, Meredith SJ, Rauer T, Irrgang JJ, Spindler KP, Ma CB, Musahl V (2020) Clinical outcomes after anterior cruciate ligament injury: panther symposium ACL injury clinical outcomes consensus group. Knee Surg Sports Traumatol Arthrosc 28:2415–2434
Tay KS, Tan AHC (2018) Clinical outcomes, return to sports, and patient satisfaction after anterior cruciate ligament reconstruction in young and middle-aged patients in an asian population-a 2-year follow-up study. Arthroscopy
Thomas AC, Villwock M, Wojtys EM, Palmieri-Smith RM (2013) Lower extremity muscle strength after anterior cruciate ligament injury and reconstruction. J Athl Train 48:610–620
Vilchez-Cavazos F, Davila-Martinez A, Garza-Castro S, Simental-Mendia M, Garay-Mendoza D, Tamez-Mata Y, Pena-Martinez V, Acosta-Olivo C (2020) Anterior cruciate ligament injuries treated with quadriceps tendon autograft versus hamstring autograft: a randomized controlled trial. Cir Cir 88:76–81
Webster KE, Feller JA (2017) Younger patients and men achieve higher outcome scores than older patients and women after anterior cruciate ligament reconstruction. Clin Orthop Relat Res 475:2472–2480
West RV, Harner CD (2005) Graft selection in anterior cruciate ligament reconstruction. J Am Acad Orthop Surg 13:197–207
Xie X, Liu X, Chen Z, Yu Y, Peng S, Li Q (2015) A meta-analysis of bone-patellar tendon-bone autograft versus four-strand hamstring tendon autograft for anterior cruciate ligament reconstruction. Knee 22:100–110
Yunes M, Richmond JC, Engels EA, Pinczewski LA (2001) Patellar versus hamstring tendons in anterior cruciate ligament reconstruction: a meta-analysis. Arthroscopy 17:248–257
Acknowledgements
We thank Bernhard Vaske, Michael Schwarze and Jessica Westphal for their support.
Funding
Open Access funding enabled and organized by Projekt DEAL. The Richard and Annemarie Wolf-Foundation as funder of the study had no role in data collection, storage or analysis; in the writing of the manuscript; or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Contributions
HH wrote the manuscript with support from UT, GF, MP and MJ. In addition, he contributed to the data collection and analysis. MP had impact on the design of the study. In addition, he wrote and contributed to the final manuscript. UT wrote the manuscript. He had significant impact on the figures and graphs. GF. had impact on the design of the study. He collected the data at centre B. In addition, he wrote and contributed to the final manuscript. CK had impact on the design of the study. In addition, he wrote and contributed to the final manuscript. MJ wrote the manuscript and was in charge of the overall direction of the project. In addition, he wrote and contributed to the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no relevant financial or non-financial interests to disclose.
Consent to participate
Informed consent was obtained from all individual participants included in the study.
Ethical approval
Approval was obtained from the Ethics Committee of Hannover Medical School, Germany (Nr. 5456). The procedures used in this study adhere to the tenets of the Declaration of Helsinki.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Horstmann, H., Petri, M., Tegtbur, U. et al. Quadriceps and hamstring tendon autografts in ACL reconstruction yield comparably good results in a prospective, randomized controlled trial. Arch Orthop Trauma Surg 142, 281–289 (2022). https://doi.org/10.1007/s00402-021-03862-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00402-021-03862-8