Abstract
Purpose
The mechanical axis of the lower limb has shown to vary between different weight-bearing conditions and change after total knee arthroplasty (TKA). The purpose of this study was to investigate the correlation between mechanical axis alignment in standing long-leg radiographs and limb loading after TKA.
Methods
Mechanical axis of the lower limb and limb loading have been prospectively evaluated in 115 patients 10 days and 3 months after TKA. By the moment of standing long-leg radiography for analysis of the mechanical leg axis, two digital scales separately captured the load of each limb.
Results
Mechanical axis changed from an initial − 1° ± 2° valgus alignment to a varus axis of + 1° ± 2° (p < 0.01). This change in alignment was associated with an increase of limb loading from 89.9 ± 10.7 to 93.0 ± 7.0% (p < 0.01). The mechanical axis strongly correlated with relative limb loading at the first and second measurements (r = 0.804, p < 0.001, respectively, r = 0.562, p < 0.001). A significant change in the rate of outliers was registered within the observation period. These alterations and distinctions were much more pronounced in patients with postoperative incomplete extension (n = 15).
Conclusions
The postoperative mechanical axis correlates with limb loading. A clinical relevant change in frontal alignment of the lower limb is associated with increased limb loading after TKA. The actual mechanical axis can only be assessed at physiological limb loading in long-leg radiographs with complete extension at full weight bearing.
Level of evidence
Diagnostic study, Level II.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The frontal alignment of the lower limb determines the load distribution of the knee [7]. Mechanical leg axis is thought to be important in the evolution of osteoarthritis [41]. A neutral mechanical axis with an acceptable range of 3° in axis deviation is considered as optimal alignment, and supposed to influence function and survival rates after TKA [2, 8, 30, 31, 47]. The axis alignment of the lower limb can be reliably measured in standing long-leg radiographs [5, 9, 37]. Different factors affecting the accuracy of the mechanical axis measured in long-leg radiographs have been identified including position of the leg with rotation or knee flexion [17, 21, 26, 28, 38]. Correct radiographic technique is, therefore, essential for the measurement.
Mechanical axis alignment has been supposed to be affected by different weight-bearing conditions. A significant difference of the mechanical axis between weight-bearing and non-weight-bearing radiographs has been reported [13, 14, 35, 36, 39]. A clinical relevant change of the radiological mechanical axis within the first 3 months after TKA was assumed to depend on limb loading [53]. The underlying mechanism for the change in mechanical axis alignment has not yet been determined. Muscle activation and forces have shown to be reduced after TKA and non-physiological weight bearing may have an effect on the measurement of the mechanical axis [35, 49, 50, 52]. Limb loading could influence the mechanical axis alignment of the lower limb measured in standing long-leg radiographs.
The purpose of this study was to investigate the mechanical axis in relation to limb loading after TKA. A correlation between weight-bearing radiography and loading of the lower limb was hypothesised. The underlying mechanism of the variation of the mechanical axis alignment between different weight-bearing conditions and the change of after TKA would be revealed. A significant different distribution of outliers would indicate the clinical relevance of the findings.
Materials and methods
This study prospectively investigated a consecutive series of 115 TKAs in 115 patients with primary osteoarthritis (Table 1). Exclusion criteria were a preoperative extension deficit > 20°, a valgus or varus malalignment > 15° and previous surgery of the affected joint (Fig. 1). Between December 2014 and September 2015, 115 TKAs (Journey Bicruciate Substituting Knees, Smith & Nephew, Memphis, TN, USA) without retropatellar replacement were implanted with patient-specific instrumentation (Visionaire®, Smith & Nephew, Memphis, TN) via a medial parapatellar approach under general anaesthesia [37]. The preoperative planning consisted of a neutral mechanical axis. Planning of the implant position was done in the MRI’s frontal plane and perpendicular to the mechanical femoral and tibial axes [53]. Rotation of the femoral component was adjusted by the gap-balancing method around the transepicondylar axis [15]. Posterior tibial slope was set to 3° [15].
All included 115 patients were available at the follow-up at 10 days (range 7 to 12 postoperative day) and 3 months postoperative (Fig. 1). Demographic data (sex, age, weight, height), date of surgery and follow-up were recorded for each patient.
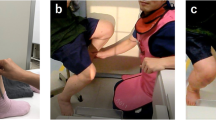
Mechanical axis of the lower limb was determined by performing a standardised long-leg radiograph (Centricity Enterprise Web 3.0; GE Healthcare Pty Ltd, Piscataway, NJ, USA) as previously described [2, 53]. Anterior–posterior, long-leg radiographs with the radiographic beam centred to the joint line were taken with the patients standing with feet at shoulder width, equally distributed weight bearing and patella pointing straight forward at maximum knee extension [53]. The digitally processed radiographs were obtained in one exposure with a tube-to-plate distance of 2 m on an imaging plate measuring 354 × 1245 mm, at 80–90 kV and 63–100 mA depending on body mass index [5, 9, 53]. Radiographs were only accepted for further analysis if the requirements were fully implemented: central patellar tracking, coverage of the fibular head by the tibia (2/3; 1/3), position of the ankle, neutral rotation of the leg with correct visualisation and projection of the trochanter minor [13, 19, 38].
Mechanical axis was analysed as previously described [13, 34, 39, 53]. A varus axis was indexed in the case of positive angles and a valgus axis in the case of negative angles. Limb loading of each leg was assessed using two scales while performing the long-leg radiograph in accordance with a previously described method [16]. Each scale was securely mounted to the ground at the same level and calibrated by using known weights. The patient was asked to distribute the weight as evenly as possible between the two legs while looking directly ahead and stably standing still. Absolute limb loading was read off and documented in kilograms (kg), and relative limb loading was calculated relative to the equal contributed body weight. Patients were not able to see the display of the scales.
At each follow-up and radiograph, range of motion was measured using a goniometer [11, 23]. The 115 patients were differentiated into two groups: patients with complete postoperative extension to neutral position after TKA (n = 100) and patients with incomplete extension with a deficit of extension ranging from 5 to 15% (n = 15) at the time of the first postoperative radiograph (Table 1).
Pain level was assessed with a standardised Numerical Rating Scale (NRS) ranging from 0 to 10. All patients received standardised, multimodal, postoperative treatment regarding pain therapy, thromboembolic prophylaxis and physiotherapeutic regime. Full weight bearing and passive and active mobilisation were performed for all patients starting at the first postoperative day. The competent ethics committee gave approval for the study (AS 17 (bB)/2015) and an informed consent was obtained from all patients.
Statistical analysis
Parameters are presented by means, standard deviations and ranges. For statistical analysis, we used the Wilcoxon test for paired samples, the Mann–Whitney U test for non-paired samples and Pearson’s test for correlation analysis. All radiographs were assessed by the two authors (HH, RZ). The mean correlation coefficient of interobserver reliability of all measurements was 0.966 (range: 0.955–0.974), whereas the mean correlation coefficient of intraobserver reliability was 0.959 (range: 0.946–0.969). A post hoc analysis revealed a power of > 0.8 for n = 100 patients with a two-tailed alpha < 0.05 for all evaluated parameters. Statistical analysis was performed using SPSS software with a level of significance set at p < 0.05 (SPSS version 21; SPSS Inc, Chicago, IL, USA).
Results
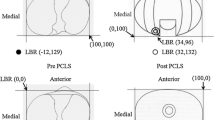
Patients with complete extension (n = 100) presented with a mechanical axis of − 1° ± 2° at the 10th day after the TKA (Fig. 2; Table 2). After 3 postoperative months, mechanical axis changed to a varus alignment of + 1° ± 2° (p < 0.001; Figs. 2, 3; Table 2). At the first measurement, 16 of the 100 patients had a valgus alignment of more than − 3°. Two of them continued to demonstrate an increased valgus alignment up to − 4° after 3 months and two others were found to have an increased varus alignment of 4° after 3 months compared to the neutral axis assessed before.
The change in alignment was accompanied by an increase of limb loading (p < 0.01). Patients assessed with a relative limb loading of at least 90% at the first measurement showed an increase of the mechanical axis from 0° ± 1° to 1.0° ± 1° (n = 72). This difference was significantly larger (p < 0.001) in patients with an initial loading below 90% as initially calculated with − 3° ± 0° and 0° ± 2° in the second radiograph (n = 28).
Mechanical axis was strongly correlated with relative limb loading at the first (r = 0.804, p < 0.001; Fig. 4) and second measurement (r = 0.562, p < 0.001). Mechanical axis also correlated with a minor manifestation with absolute limb loading at both measurements (r = 0.581, p < 0.001, respectively, r = 0.27, p < 0.01).
Pain levels measured by NRS decreased during the postoperative observation time (p < 0.001). There was no significant correlation between pain levels, BMI or body weight with the mechanical axis or relative limb loading.
In the 15 patients with incomplete extension, the initial axis was assessed with a valgus of − 3 ± 1 (range − 5° valgus to − 1° valgus) and showed a change to a valgus axis of − 1 ± 2 (range − 4° valgus to 2° varus) at the second measurement (p < 0.001). Relative limb loading increased from 66.3 ± 6.7 to 87.3% ± 11.3% (p < 0.001) and absolute limb loading from 31 ± 4 to 41 ± 8 kg (p < 0.001) during the observation period. Pain levels simultaneously decreased from 4 ± 1 to 1 ± 1 (p < 0.01). The mechanical axis in both radiographs differed between patients with complete extension compared to those with incomplete extension (p < 0.001 and p < 0.01, respectively, Fig. 5). Absolute and relative loading showed a subgroup specific difference at the first measurement (p < 0.001, each). Significant differences were found between these two groups for body weight (p < 0.01)—not for BMI—and pain levels at both assessments (p < 0.01 and p < 0.05, respectively).
Discussion
The most important finding of the present study was the correlation beween mechanical axis of the leg and limb loading after TKA, which was observed for the first time. Weight-bearing radiography strongly correlated with limb loading and the mechanical axis of the lower limb was dependent on limb loading.
The findings reflect the influence of individual physiological limb loading on mechanical axis alignment with its adaption on weight bearing and rebalancing within the first months after TKA. These processes may include adaptive alterations of soft tissue with ligaments, capsule of the knee joint and muscular interactions, which even may exist with an intraoperative gap-balancing method or kinematic alignment [4, 10, 15, 24, 25, 42, 48]. It has been previously demonstrated that the mechanical axis was comparably affected by different weight-bearing conditions before and after high tibial osteotomy and TKA [6, 35, 39, 40, 45, 51].
The second main finding of this study is that limb loading immediately after TKA is often reduced, even though direct postoperative full weight bearing would be technically possible [3]. Pain levels simultaneously decreased within the observation time, which indicates a likely pain-related component of reduced postoperative limb loading despite potent analgesia.
The results of alignment analysis agree with those of a different study with a distinct study cohort [53]. In the actual study, 14% of patients would falsely be considered as malaligned in the first measurement. Outliers could only be verified in 4% after 3 months, indeed. The shift in the rate of outliers within the first 3 months after TKA indicates the clinical relevance of the findings. Immediate postoperative standing long-leg radiographs are not able to assess the actual mechanical axis alignment, when limb loading is reduced.
Patients with incomplete extension showed a significant different axis alignment, limb loading and more distinct changes compared to patients with complete extension, which highlights the impact of limb loading. Body weight seems to influence the function after TKA, as the subgroup analysis (see Table 1) and previous studies revealed [12]. This information is limited by the small number of patients with postoperative incomplete extension.
The follow-up of the actual study was limited to 3 months due to no further observed changes in mechanical axis between 3 and 12 postoperative months in a previous study [53]. Changes over a longer time period could exist and depend on different loading scenarios, especially at high body weight. Subsequent studies could investigate the effects of different loading scenarios on function and survival time after TKA [43]. Static weight bearing, which was analysed in the actual and previous studies, may not reflect the conditions of physiologic dynamic loading during walking, which could even be more important for a functional analysis [33, 48].
The accuracy of the evaluation is warranted and limited by the precision of the method [5, 9, 20]. Standing long-leg radiographs have been shown to reliably detect differences of few degrees in several studies investigating the accuracy of mechanical axis alignment [18, 32, 35, 37]. Differences and changes of mechanical axis alignment to the extent evaluated in the actual study are statistically significant and clinically relevant [1, 2, 7, 8, 27, 37, 38]. However, the effect of a minor increase in weight bearing may be enhanced by further loading depending interactions [3, 29, 49]. Additional weight-bearing independent factors may even exist and influence the measurement of mechanical axis alignment [22, 44].Even if computed tomography has a higher accuracy in determination of axis alignment, standing long-leg radiographs represent the only routine radiographic technique under weight-bearing condition [46].
Exact limb loading was measured with a digital device, which did not change the standardised procedure of long-leg radiography. Patients were not able to visualise the weight by themselves, so any influences of the limb loading assessment on the radiography may be considered as excluded.
Conclusions
Mechanical alignment of the leg correlates with limb loading. Only at physiological loading with full weight bearing and complete knee extension, long-leg radiographs reflect the true mechanical axis of the lower limb.
Abbreviations
- BMI:
-
Body mass index
- TKA:
-
Total knee arthroplasty
- NRS:
-
Numerical rating scale
References
Abane L, Anract P, Boisgard S, Descamps S, Courpied JP, Hamadouche M (2015) A comparison of patient-specific and conventional instrumentation for total knee arthroplasty: a multicentre randomised controlled trial. Bone Joint J 97-B:56–63
Abdel MP, Oussedik S, Parratte S, Lustig S, Haddad FS (2014) Coronal alignment in total knee replacement: historical review, contemporary analysis, and future direction. Bone Joint J 96-B:857–862
Alnahdi AH, Zeni JA, Snyder-Mackler L (2016) Quadriceps strength asymmetry predicts loading asymmetry during sit-to-stand task in patients with unilateral total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 24:2587–2594
Amis AA (2013) Biomechanics of high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 21:197–205
Babazadeh S, Dowsey MM, Bingham RJ, Ek ET, Stoney JD, Choong PF (2013) The long leg radiograph is a reliable method of assessing alignment when compared to computer-assisted navigation and computer tomography. Knee 20:242–249
Bae DK, Lee JW, Cho SJ, Song SJ (2017) Comparison of mechanical axis and dynamic range assessed with weight bearing radiographs and navigation system in closed wedge high tibial osteotomy. Knee Surg Relat Res 29:225–231
Becker R, Kopf S, Karlsson J (2013) Loading conditions of the knee: what does it mean? Knee Surg Sports Traumatol Arthrosc 21:2659–2660
Bellemans J, Colyn W, Vandenneucker H, Victor J (2012) The Chitranjan Ranawat award: is neutral mechanical alignment normal for all patients? The concept of constitutional varus. Clin Orthop Relat Res 470:45–53
Bowman A, Shunmugam M, Watts AR, Bramwell DC, Wilson C, Krishnan J (2016) Inter-observer and intra-observer reliability of mechanical axis alignment before and after total knee arthroplasty using long leg radiographs. Knee 23:203–208
Calliess T, Bauer K, Stukenborg-Colsman C, Windhagen H, Budde S, Ettinger M (2017) PSI kinematic versus non-PSI mechanical alignment in total knee arthroplasty: a prospective, randomized study. Knee Surg Sports Traumatol Arthrosc 25:1743–1748
Edwards JZ, Greene KA, Davis RS, Kovacik MW, Noe DA, Askew MJ (2004) Measuring flexion in knee arthroplasty patients. J Arthroplasty 19:369–372
Fuchs MC, Janssen RP (2015) Clinical evaluation of 292 Genesis II posterior stabilized high-flexion total knee arthroplasty: range of motion and predictors. Eur J Orthop Surg Traumatol 25:161–166
Gbejuade HO, White P, Hassaballa M, Porteous AJ, Robinson JR, Murray JR (2013) Do long leg supine CT scanograms correlate with weight-bearing full-length radiographs to measure lower limb coronal alignment? Knee 21:549–552
Holme TJ, Henckel J, Hartshorn K, Cobb JP, Hart AJ (2015) Computed tomography scanogram compared to long leg radiograph for determining axial knee alignment. Acta Orthop 86:440–443
Hommel H, Perka C (2015) Gap-balancing technique combined with patient-specific instrumentation in TKA. Arch Orthop Trauma Surg 135:1603–1608
Hopkins S, Smith C, Toms A, Brown M, Welsman J, Knapp K (2013) Evaluation of a dual-scales method to measure weight-bearing through the legs, and effects of weight-bearing inequalities on hip bone mineral density and leg lean tissue mass. J Rehabil Med 45:206–210
Jamali AA, Meehan JP, Moroski NM, Anderson MJ, Lamba R, Parise C (2017) Do small changes in rotation affect measurements of lower extremity limb alignment? J Orthop Surg Res 12:77
Jiang J, Kang X, Lin Q, Teng Y, An L, Ma J et al (2015) Accuracy of patient-specific instrumentation compared with conventional instrumentation in total knee arthroplasty. Orthopedics 38:e305–e313
Kannan A, Hawdon G, McMahon SJ (2012) Effect of flexion and rotation on measures of coronal alignment after TKA. J Knee Surg 25:407–410
Khare R, Jaramaz B (2017) Accuracy of leg alignment measurements from antero-posterior radiographs. Biomed Tech (Berl) 62:315–320
Kim AD, Scott RD (2016) Can the visibility of both prosthetic posterior femoral condyles on a postoperative radiograph assure that limb rotation is appropriate to allow accurate measurement of the anatomic knee axis? J Arthroplasty 31:2593–2596
Kutzner I, Bender A, Dymke J, Duda G, von Roth P, Bergmann G (2017) Mediolateral force distribution at the knee joint shifts across activities and is driven by tibiofemoral alignment. Bone Joint J 99-B:779–787
Lavernia C, D’Apuzzo M, Rossi MD, Lee D (2008) Accuracy of knee range of motion assessment after total knee arthroplasty. J Arthroplasty 23:85–91
Lee DH, Park SC, Park HJ, Han SB (2016) Effect of soft tissue laxity of the knee joint on limb alignment correction in open-wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 24:3704–3712
Lee YS, Howell SM, Won YY, Lee OS, Lee SH, Vahedi H et al (2017) Kinematic alignment is a possible alternative to mechanical alignment in total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 25:3467–3479
Lee YS, Lee BK, Lee SH, Park HG, Jun DS, Moon DH (2013) Effect of foot rotation on the mechanical axis and correlation between knee and whole leg radiographs. Knee Surg Sports Traumatol Arthrosc 21:2542–2547
Lombardi AV, Berend KR, Adams JB (2014) Why knee replacements fail in 2013: patient, surgeon, or implant? Bone Joint J 96-B:101–104
Lonner JH, Laird MT, Stuchin SA (1996) Effect of rotation and knee flexion on radiographic alignment in total knee arthroplasties. Clin Orthop Relat Res 331:102–106
Loyd BJ, Jennings JM, Falvey JR, Kim RH, Dennis DA, Stevens-Lapsley JE (2017) Magnitude of deformity correction may influence recovery of quadriceps strength after total knee arthroplasty. J Arthroplasty 32:2730–2737
Manjunath KS, Gopalakrishna KG, Vineeth G (2015) Evaluation of alignment in total knee arthroplasty: a prospective study. Eur J Orthop Surg Traumatol 25:895–903
Matsuda S, Kawahara S, Okazaki K, Tashiro Y, Iwamoto Y (2013) Postoperative alignment and ROM affect patient satisfaction after TKA. Clin Orthop Relat Res 471:127–133
Maus U, Marques CJ, Scheunemann D, Lampe F, Lazovic D, Hommel H et al (2017) No improvement in reducing outliers in coronal axis alignment with patient-specific instrumentation. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4741-1
Miller EJ, Pagnano MW, Kaufman KR (2014) Tibiofemoral alignment in posterior stabilized total knee arthroplasty: static alignment does not predict dynamic tibial plateau loading. J Orthop Res 32:1068–1074
Paley D, Pfeil J (2000) Principles of deformity correction around the knee. Orthopade 29:18–38
Paternostre F, Schwab PE, Thienpont E (2014) The difference between weight-bearing and non-weight-bearing alignment in patient-specific instrumentation planning. Knee Surg Sports Traumatol Arthrosc 22:674–679
Petterwood J, Dowsey MM, Rodda D, Choong PF (2014) The immediate post-operative radiograph is an unreliable measure of coronal plane alignment in total knee replacement. Front Surg 1:35
Pfitzner T, Abdel MP, von Roth P, Perka C, Hommel H (2014) Small improvements in mechanical axis alignment achieved with MRI versus CT-based patient-specific instruments in TKA: a randomized clinical trial. Clin Orthop Relat Res 472:2913–2922
Radtke K, Becher C, Noll Y, Ostermeier S (2010) Effect of limb rotation on radiographic alignment in total knee arthroplasties. Arch Orthop Trauma Surg 130:451–457
Schoenmakers DAL, Feczko PZ, Boonen B, Schotanus MGM, Kort NP, Emans PJ (2017) Measurement of lower limb alignment: there are within-person differences between weight-bearing and non-weight-bearing measurement modalities. Knee Surg Sports Traumatol Arthrosc 25:3569–3575
Schroter S, Ateschrang A, Lowe W, Nakayama H, Stockle U, Ihle C (2017) Early full weight-bearing versus 6-week partial weight-bearing after open wedge high tibial osteotomy leads to earlier improvement of the clinical results: a prospective, randomised evaluation. Knee Surg Sports Traumatol Arthrosc 25:325–332
Sharma L, Song J, Felson DT, Cahue S, Shamiyeh E, Dunlop DD (2001) The role of knee alignment in disease progression and functional decline in knee osteoarthritis. JAMA 286:188–195
Shelton TJ, Nedopil AJ, Howell SM, Hull ML (2017) Do varus or valgus outliers have higher forces in the medial or lateral compartments than those which are in-range after a kinematically aligned total knee arthroplasty? limb and joint line alignment after kinematically aligned total knee arthroplasty. Bone Joint J 99-B:1319–1328
Shimada N, Deie M, Hirata K, Hiate Y, Orita N, Iwaki D et al (2016) Courses of change in knee adduction moment and lateral thrust differ up to 1 year after TKA. Knee Surg Sports Traumatol Arthrosc 24:2506–2511
Silva M, Shepherd EF, Jackson WO, Pratt JA, McClung CD, Schmalzried TP (2003) Knee strength after total knee arthroplasty. J Arthroplasty 18:605–611
Sim JA, Kwak JH, Yang SH, Choi ES, Lee BK (2010) Effect of weight-bearing on the alignment after open wedge high tibial osteotomy. Knee Surg Sports Traumatol Arthrosc 18:874–878
Slevin O, Hirschmann A, Schiapparelli FF, Amsler F, Huegli RW, Hirschmann MT (2017) Neutral alignment leads to higher knee society scores after total knee arthroplasty in preoperatively non-varus patients: a prospective clinical study using 3D-CT. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-017-4744-y
Slevin O, Schmid FA, Schiapparelli FF, Rasch H, Amsler F, Hirschmann MT (2017) Coronal femoral TKA position significantly influences in vivo patellar loading in unresurfaced patellae after primary total knee arthroplasty. Knee Surg Sports Traumatol Arthrosc 25:3605–3610
Specogna AV, Birmingham TB, Hunt MA, Jones IC, Jenkyn TR, Fowler PJ et al (2007) Radiographic measures of knee alignment in patients with varus gonarthrosis: effect of weightbearing status and associations with dynamic joint load. Am J Sports Med 35:65–70
Stevens-Lapsley JE, Balter JE, Kohrt WM, Eckhoff DG (2010) Quadriceps and hamstrings muscle dysfunction after total knee arthroplasty. Clin Orthop Relat Res 468:2460–2468
Thomas AC, Judd DL, Davidson BS, Eckhoff DG, Stevens-Lapsley JE (2014) Quadriceps/hamstrings co-activation increases early after total knee arthroplasty. Knee 21:1115–1119
Wang JH, Shin JM, Kim HH, Kang SH, Lee BH (2017) Discrepancy of alignment in different weight bearing conditions before and after high tibial osteotomy. Int Orthop 41:85–92
Yaffe MA, Koo SS, Stulberg SD (2008) Radiographic and navigation measurements of TKA limb alignment do not correlate. Clin Orthop Relat Res 466:2736–2744
Zahn RK, Fussi J, von Roth P, Perka CF, Hommel H (2016) postoperative increased loading leads to an alteration in the radiological mechanical axis after total knee arthroplasty. J Arthroplasty 31:1803–1807
Funding
No funding hase been received for this study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest.
Ethical approval
This study was approved by the competent ethical committee (AS 17 (bB)/2015).
Informed consent
A written informed consent was obtained from all patients.
Rights and permissions
About this article
Cite this article
Zahn, R.K., Renner, L., Perka, C. et al. Weight-bearing radiography depends on limb loading. Knee Surg Sports Traumatol Arthrosc 27, 1470–1476 (2019). https://doi.org/10.1007/s00167-018-5056-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00167-018-5056-6