Abstract
Maple syrup urine disease (MSUD) is an inherited aminoacidopathy resulting from dysfunction of the branched-chain keto acid dehydrogenase complex, leading to accumulation of the branched-chain amino acids (BCAA) leucine, isoleucine and valine as well as their corresponding transaminated branched-chain α-ketoacids. This disorder is clinically characterized by ketoacidosis, seizures, coma, psychomotor delay and mental retardation whose pathophysiology is not completely understood. Recent studies have shown that oxidative stress may be involved in neuropathology of MSUD. However, the effect of accumulating α-ketoacids in MSUD on neurotrophic factors has not been investigated. Thus, the objective of the present study was to evaluate the effects of acute intracerebroventricular administration of α-ketoisocaproic acid (KIC) on brain-derived neurotrophic factor (BDNF) and nerve growth factor (NGF) levels in the brains of young male rats. Ours results showed that intracerebroventricular administration of KIC decreased BDNF levels in hippocampus, striatum and cerebral cortex, without induce a detectable change in pro-BDNF levels. Moreover, NGF levels in the hippocampus were reduced after intracerebroventricular administration of KIC. In conclusion, these data suggest that the effects of KIC on demyelination and memory processes may be mediated by reduced trophic support of BDNF and NGF. Moreover, lower levels of BDNF and NGF are consistent with the hypothesis that a deficit in this neurotrophic factor may contribute to the structural and functional alterations of brain underlying the psychopathology of MSUD, supporting the hypothesis of a neurodegenerative process in MSUD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Maple syrup urine disease (MSUD) or branched-chain ketoaciduria is an autosomal recessive metabolic disorder caused by a deficiency of the branched-chain α-keto acid dehydrogenase complex (BCKAD) activity, with a world frequency estimated in approximately 1 in 185,000 newborns (Chuang et al. 2008). The metabolic defect leads to accumulation of the branched-chain amino acids leucine, isoleucine and valine, as well as their corresponding transaminated branched-chain α-keto acids α-ketoisocaproic (KIC), α-ketoisovaleric (KIV) and α-keto-β-methylvaleric (KMV) acids in tissue and body fluids (Chuang and Shih 2001). The major clinical features presented by MSUD patients include convulsions, ketoacidosis, apnea, hypoglycemia, coma, ataxia, psychomotor delay, and mental retardation (Chuang and Shih 2001; Schonberger et al. 2004). Neuropathologic findings characteristic of the disease are cerebral edema, atrophy of the cerebral hemispheres, spongy degeneration of the white matter, and delayed myelination (Chuang and Shih 2001; Jan et al. 2003; Klee et al. 2013; Treacy et al. 1992).
Although the mechanisms of brain damage in MSUD are still unclear, it appears that leucine and KIC are considered to be the main neurotoxic metabolites since increased plasma concentrations of these metabolites are associated with the appearance of neurological symptoms (Chuang and Shih 2001; Snyderman et al. 1964) and can reach concentrations as high as 5.0 mM in untreated patients (Zielke et al. 1996). In addition, it has been postulated that metabolites accumulation in MSUD causes brain energy deficit (Amaral et al. 2010; Howell and Lee 1963; Ribeiro et al. 2008; Sgaravatti et al. 2003), oxidative stress (Barschak et al. 2008; Barschak et al. 2009; Bridi et al. 2005; Mescka et al. 2011; Mescka et al. 2013; Scaini et al. 2012b), neuronal apoptosis (Jouvet et al. 2000a; Jouvet et al. 2000b), and increases acetylcholinesterase activity in brain (Scaini et al. 2012a). Furthermore, these metabolites are also reported to cause impairment of myelin development (Taketomi et al. 1983; Treacy et al. 1992; Tribble and Shapira 1983), reduced brain uptake of essential amino acids and subsequently disturbed neurotransmission (Araujo et al. 2001; Tavares et al. 2000; Wajner et al. 2000; Wajner and Vargas 1999; Zielke et al. 2002).
Brain-derived neurotrophic factor (BDNF) and nerve growth factor (NGF) are members of the neurotrophin (NT) gene family, which play critical roles on growth, differentiation, maintenance, and synaptic plasticity in neuronal systems (Bibel and Barde 2000; Huang and Reichardt 2001). NGF serves as a neurotrophic factor for basal forebrain cholinergic neurons (Gnahn et al. 1983; Gu et al. 2009; Klein et al. 2000; Mendell et al. 2001; Nagahara et al. 2009; Sofroniew et al. 2001), while BDNF is associated with a broader spectrum of functions, promoting the functioning and survival of dopaminergic, GABAergic, noradrenergic, and serotonergic neurons (Lee et al. 2001; Lu et al. 2008; Murer et al. 2001; Soule et al. 2006; Tyler et al. 2002). Two different types of receptors expressed by responsive cells regulate the biological activity of NGF and BDNF: the specific Trk family of tyrosine protein kinases (NGF/TrkA and BDNF/TrkB) and p75 receptor that is a member of the tumor necrosis factor receptor superfamily (Lim et al. 2003; Lu et al. 2005; Meakin and Shooter 1992; Yoshii and Constantine-Paton 2010). Dysregulation of the levels of neurotrophins or their receptors, or alterations in neurotrophin function or trafficking, can damage neurons, leading to gradual neuronal degeneration (Mufson et al. 2003). Moreover, studies have shown a link between lower BDNF and NGF concentrations and neuronal and cognitive dysfunction (Belrose et al. 2014; Gelfo et al. 2011; Gu et al. 2009; Peng et al. 2004; Peng et al. 2005).
Accumulating evidence suggests BDNF and NGF as candidate molecules involved in the pathophysiology of MSUD. Scaini et al. (2013b) suggested that decreased NGF levels in hippocampus may play a role in cognitive dysfunction observed in MSUD. A recent study showed an increase in BDNF levels after chronic administration of H-BCAA, suggesting that the increase of BDNF levels had a correlation with the cognitive impairment (Scaini et al. 2013a). Moreover, it has been also shown that acute administration of H-BCAA causes an increase in the levels of pro-BDNF and a decrease tPA levels in brain of rats, suggesting that BCAA may play a role in BDNF post-translational processing (Scaini et al. 2015). However, the effect of the accumulating organic acids in MSUD on neurotrophic factors has not been so far investigated. Therefore, in order to determine the specific participation of KIC in neurotrophins levels in MSUD, the objective of the present study was to evaluate the effects of acute intracerebroventricular administration of KIC on BDNF and NGF levels in the brain of young male rats.
Materials and methods
Animals
Male Wistar rats at 30 days old (weighing 60–80 g) were obtained from the Central Animal House of the Universidade do Extremo Sul Catarinense. All rats were caged in groups of 5 with free access to food and water and were maintained on a 12-h light/dark cycle (lights on 7:00 am) at a temperature of 23 ± 1 °C. All experimental procedures were carried out in accordance with the National Institutes of Health Guide for the Care and Use of Laboratory Animals and the Brazilian Society for Neuroscience and Behavior recommendations for animal care, with the approval of the Ethics Committee of the Universidade do Extremo Sul Catarinense (protocol number 05/2014).
α-ketoisocaproic acid administration
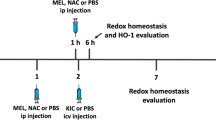
Rats were anesthetized with an intraperitoneal (i.p.) injection of a mixture of ketamine (80 mg/kg) and xylazine (10 mg/kg) and thereafter placed on a stereotaxic apparatus. One small hole was drilled in the skull for microinjection, and 2 μL of a 0.8 μmol KIC solution dissolved in freshly prepared artificial CSF (aCSF) (147 mM NaCl; 2.9 mM KCl; 1.6 mM MgCl2; 1.7 mM CaCl2 and 2.2 mM dextrose) or ACFs (controls) at the same volume and concentration, was slowly injected bilaterally over 4 min into the lateral ventricle via needle connected by a polyethylene tube to a 10 μL Hamilton syringe (de Castro et al. 2004). The needle was left in place for another 1 min before being softly removed. The pH of each solution was previously adjusted to 7.4 with 0.1 N NaOH or 0.1 N HCl. The coordinates for injections were as follows: 0.6 mm posterior to bregma, 1.0 mm lateral to midline and 3.2 mm ventral from dura (Paxinos and Watson 1986). The rats were killed by decapitation without anesthesia 60 min after the intracerebroventricular administration of KIC or ACFs. The brain was rapidly excised on a Petri dish placed on an ice plate and the hippocampus, striatum and cerebral cortex were dissected.
BDNF and NGF protein levels
BDNF and NGF levels in the brain tissues [homogenized in phosphate buffer solution with a protease inhibitor cocktail (Sigma-Aldrich, St. Louis, MO, USA)] were determined using a sandwich-ELISA assay with monoclonal antibodies specific for BDNF or NGF (Millipore, USA & Canada). Briefly, microtiter plates (96-well flat-bottom) were coated for 24 h with the samples (diluted 1:2 in sample diluent) and a standard curve (ranging from 7.8 to 500 pg/ml of BDNF or 15.6 to 1000 pg/ml of NGF). The plates were then washed four times with the sample diluent. After washing, a monoclonal anti-BDNF or anti-NGF rabbit antibody (diluted 1:1000) was added to each well and incubated for 3 h at room temperature. After washing again, a peroxidase-conjugated anti-rabbit antibody (diluted 1:1000) was added to each well and incubated at room temperature for 1 h. After the addition of the streptavidin-enzyme, substrate and stop solution, the amount of BDNF and NGF were determined by measuring the absorbance at 450 nm. The total protein was measured by Lowry et al. (1951) utilizing bovine serum albumin as a standard.
Immunoblotting
To perform the immunoblot experiments, the samples were first homogenized in Laemmli-sample buffer (62.5 mM Tris–HCl, pH 6.8, 1 % (w/v) SDS, 10 % (v/v) glycerol). Equal amounts of protein (30 μg/well) were fractionated by SDS-PAGE and electro-blotted onto nitrocellulose membranes. The protein loading and electro-blotting efficiency were verified with Ponceau S staining. The membranes were blocked in Tween-Tris-buffered saline (TTBS: 100 mM Tris-HCl, pH 7.5, containing 0.9 % NaCl and 0.1 % Tween-20) containing 5 % albumin. The membranes were incubated overnight at 4 °C with an antibody against pro-BDNF (Abcam - ab72440). The primary antibody was then removed, and the membranes were washed 4 times for 15 min. After washing, an anti-rabbit and anti-goat IgG peroxidase-linked secondary antibody was incubated with the membranes for 1 h (1:10,000 dilution) and the membranes were washed again. Finally, the immunoreactivity was detected using an enhanced chemiluminescence ECL Plus kit. After exposure, the membranes were stripped and incubated with a mouse monoclonal antibody to β-actin (Sigma - A2228) in the presence of 5 % milk. An anti-mouse IgG peroxidase-linked secondary antibody was incubated with the membranes for 1 h (1:10,000 dilution), and the membranes were washed again. The immunoreactivity was detected using an enhanced chemiluminescence ECL Plus kit. Densitometry was performed using the Image J v.1.34 software. SeeBlue ® Plus2 Prestained Standard (Invitrogen) was used as a molecular weight marker to make sure that the correct bands were analyzed for pro-BDNF and β-actin.
Statistical analysis
Results are presented as mean ± standard deviation. All assays were performed in duplicate, and mean was used for statistical analysis. Tests for determination of normality and equal variances were performed to examine whether our data qualified for parametric statistical tests. The data were normally distributed (Shapiro–Wilks, p > 0.05) with equal variances among samples (equal variances test, p > 0.05). Thus, Student’s t test was used for the comparison of two means, and differences between the groups were considered to be significant at p < 0.05. All analyses were carried out on an IBM-compatible PC computer using the Statistical Package for the Social Sciences software (Armonk, New York, USA).
Results
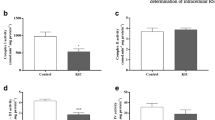
We first investigated whether a single intracerebroventricular administration of KIC could induce changes in BDNF levels in hippocampus, striatum and cerebral cortex of young rats. We verified that the intracerebroventricular administration of KIC decreased the BDNF levels in hippocampus, striatum and cerebral cortex, when compared to the control group (Fig. 1). The assay does not allow us to distinguish between pro-BDNF and mature BDNF, as they are equally recognized by the antibody used in the ELISA. Due to the potential contrasting effects of pro-BDNF and mature BDNF, we felt that it was important to measure the level of the precursor protein in the brain. Immunoblot analysis detected a specific pro-BDNF signal (ab72440 antibody; Abcam) in the 28 kDa range. Intracerebroventricular administration of KIC showed a trend towards a slight reduction in the protein levels of pro-BDNF in the hippocampus and cerebral cortex; however it did not reach significance (Fig. 2).
The effect of acute administration of intracerebroventricular administration of α-ketoisocaproic acid (KIC) on brain-derived neurotrophic factor (BDNF) levels in the hippocampus, striatum and cerebral cortex of 30-day-old rats. Data are expressed as the mean ± standard deviation for five to six animals per group. *p < 0.05 compared to the control group (Student’s t test)
The effect of acute administration of intracerebroventricular administration of α-ketoisocaproic acid (KIC) on pro-brain-derived neurotrophic factor (pro-BDNF) levels in the hippocampus, striatum and cerebral cortex of 30-day-old rats. Figure shows representative immunoblot bands in the shown groups. The ratio of the immunoblot integrated optical density (IOD) of the protein of interest to β-actin was used for statistical analysis. Data are expressed as the mean ± standard deviation for five to six animals per group
We also analyzed the effects of intracerebroventricular administration of KIC on NGF levels in the hippocampus, striatum and cerebral cortex. ELISA measurements demonstrated that NGF levels in the hippocampus were reduced after intracerebroventricular administration of KIC. On the other hand, no differences in NGF levels were observed in striatum or cerebral cortex when compared to the control group (Fig. 3).
The effect of acute administration of intracerebroventricular administration of α-ketoisocaproic acid (KIC) on nerve growth factor (NGF) levels in the hippocampus, striatum and cerebral cortex of 30-day-old rats. Data are expressed as the mean ± standard deviation for five to six animals per group. *p < 0.05 compared to the control group (Student’s t test)
Discussion
Neurological sequelae are frequent in untreated patients affected by MSUD, but the mechanisms underlying the neurotoxicity in this disease are yet not well established. However, it is well known that KIC and its precursor leucine, which achieve 5.0 mM concentrations in tissues of MSUD patients, are the most toxic metabolites in this disease (Chuang and Shih 2001; Snyderman et al. 1964). We have previously demonstrated that the acute administration of BCAAs in young rats increased pro-BDNF, total-BDNF and tPA levels in striatum and decrease NGF levels in hippocampus. In the present report, we investigated the effects of the KIC, at concentrations similar to those found in MSUD patients on pro-BDNF, total-BDNF and NGF levels in hippocampus, striatum and cerebral cortex of young rats. Our present results showed that KIC provokes the most significant effects on BDNF levels in brain, since intracerebroventricular administration of KIC decrease BDNF levels in all analyzed structures, and decreased the NGF levels only in hippocampus.
Although the exact mechanism through which KIC decreases the BDNF and NGF levels are still unknown, evidence from the literature shows that oxidative stress causes selective alterations in signalling cascades activated by BDNF and NGF, through several mechanisms, including p38 MAPK phosphorylation, decreased CREB phosphorylation or increased NF-kB DNA-binding activity (Haddad and Land 2002; Iwata et al. 1997; Zou and Crews 2006). Moreover, Jean et al. (2008) have demonstrated that glutamate, through the metabotropic glutamate receptors, also supports the production and release of BDNF from cultured basal forebrain astrocytes (Jean et al. 2008). Studies also showed that glutamate increases BDNF release in hippocampal neurons and in glial cells, such as Schwann cells and Muller cells (Canossa et al. 2001; Taylor et al. 2003; Verderio et al. 2006). Notably, oxidative stress and a decrease in glutamate levels have been implicated in the pathophysiology of MSUD, thus these findings may be closely related to the decrease in BDNF and NGF levels elicited by KIC in brain, observed in the present study.
Neurotrophins have several important effects in developing neurons, such as controlling neurite outgrowth, differentiation and cell survival, as well as synaptic plasticity and function (Huang and Reichardt 2001). Moreover, neurotrophins have been implicated in influencing the dynamic and complex signals that occur between neurons and glial cells that regulate myelination (Cellerino et al. 1997; Chan et al. 2004; Du et al. 2006; Vondran et al. 2010; Walsh et al. 1999; Xiao et al. 2010). Furthermore, studies demonstrate the importance of the reciprocal synergistic relationship between NGF and BDNF and acknowledge their potential implications in myelin formation and repair (Canossa et al. 1997; Michael et al. 1997; Reichardt 2006). Additionally, NGF and BDNF also play key roles in the fine-tuning of learning and memory performances (Mu et al. 1999; Rantamaki et al. 2013). Studies have shown that BDNF and NGF mRNA and protein are decreased in post-mortem brain tissue from subjects with AD, and these reduction correlates with the degree of cognitive impairment (Garzon et al. 2002; Gelfo et al. 2011; Hock et al. 2000; Mufson et al. 2003; Peng et al. 2005).
It has been reported that BCAA can cause demyelination and impair memory performance (de Castro et al. 2004; Glaser et al. 2010; Scaini et al. 2012c; Taketomi et al. 1983; Treacy et al. 1992; Tribble and Shapira 1983; Vasques et al. 2005; Walsh and Scott 2010). Taking together these findings and the present results, we suggest that the effects of KIC on demyelination and memory processes may be mediated by reduced trophic support of BDNF and NGF. Moreover, lower levels of BDNF and NGF are consistent with the hypothesis that a deficit in this neurotrophic factor may contribute to the structural and functional alterations of brain underlying the psychopathology of MSUD, supporting the hypothesis of a neurodegenerative process in MSUD.
References
Amaral AU, Leipnitz G, Fernandes CG, Seminotti B, Schuck PF, Wajner M (2010) Alpha-ketoisocaproic acid and leucine provoke mitochondrial bioenergetic dysfunction in rat brain. Brain Res 1324:75–84. doi:10.1016/j.brainres.2010.02.018
Araujo P et al. (2001) Reduction of large neutral amino acid levels in plasma and brain of hyperleucinemic rats. Neurochem Int 38:529–537
Barschak AG, Sitta A, Deon M, Barden AT, Dutra-Filho CS, Wajner M, Vargas CR (2008) Oxidative stress in plasma from maple syrup urine disease patients during treatment. Metab Brain Dis 23:71–80. doi:10.1007/s11011-007-9077-y
Barschak AG et al. (2009) Amino acids levels and lipid peroxidation in maple syrup urine disease patients. Clin Biochem 42:462–466. doi:10.1016/j.clinbiochem.2008.12.005
Belrose JC, Masoudi R, Michalski B, Fahnestock M (2014) Increased pro-nerve growth factor and decreased brain-derived neurotrophic factor in non-Alzheimer's disease tauopathies. Neurobiol Aging 35:926–933. doi:10.1016/j.neurobiolaging.2013.08.029
Bibel M, Barde YA (2000) Neurotrophins: key regulators of cell fate and cell shape in the vertebrate nervous system. Genes Dev 14:2919–2937
Bridi R, Braun CA, Zorzi GK, Wannmacher CM, Wajner M, Lissi EG, Dutra-Filho CS (2005) alpha-keto acids accumulating in maple syrup urine disease stimulate lipid peroxidation and reduce antioxidant defences in cerebral cortex from young rats. Metab Brain Dis 20:155–167
Canossa M, Griesbeck O, Berninger B, Campana G, Kolbeck R, Thoenen H (1997) Neurotrophin release by neurotrophins: implications for activity-dependent neuronal plasticity. Proc Natl Acad Sci U S A 94:13279–13286
Canossa M, Gartner A, Campana G, Inagaki N, Thoenen H (2001) Regulated secretion of neurotrophins by metabotropic glutamate group I (mGluRI) and Trk receptor activation is mediated via phospholipase C signalling pathways. The EMBO journal 20:1640–1650. doi:10.1093/emboj/20.7.1640
Cellerino A, Carroll P, Thoenen H, Barde YA (1997) Reduced size of retinal ganglion cell axons and hypomyelination in mice lacking brain-derived neurotrophic factor. Mol Cell Neurosci 9:397–408. doi:10.1006/mcne.1997.0641
Chan JR et al. (2004) NGF controls axonal receptivity to myelination by Schwann cells or oligodendrocytes. Neuron 43:183–191. doi:10.1016/j.neuron.2004.06.024
Chuang DT, Shih VE (2001) Maple syrup urine disease (branched-chain ketoaciduria). In: Scriver CR, Beaudet AL, Sly WS, Valle D (eds) The metabolic and molecular bases of inherited disease. McGraw-Hill, New York, pp. 1971–2005
Chuang DT, Wynn M, Shih VE (2008) Maple syrup urine disease (branched-chain ketoaciduria). In: Scriver CR, Beaudet AL, Sly WL, Valle D (eds) The metabolic and molecular bases of inherited disease. McGraw-Hill, New York, pp. 1971–2005
de Castro VV, de Boer MA, Diligenti F, Brinco F, Mallmann F, Mello CF, Wajner M (2004) Intrahippocampal administration of the alpha-keto acids accumulating in maple syrup urine disease provokes learning deficits in rats. Pharmacol Biochem Behav 77:183–190
Du Y, Fischer TZ, Clinton-Luke P, Lercher LD, Dreyfus CF (2006) Distinct effects of p75 in mediating actions of neurotrophins on basal forebrain oligodendrocytes. Mol Cell Neurosci 31:366–375. doi:10.1016/j.mcn.2005.11.001
Garzon D, Yu G, Fahnestock M (2002) A new brain-derived neurotrophic factor transcript and decrease in brain-derived neurotrophic factor transcripts 1, 2 and 3 in Alzheimer's disease parietal cortex. J Neurochem 82:1058–1064
Gelfo F, Tirassa P, De Bartolo P, Caltagirone C, Petrosini L, Angelucci F (2011) Brain and serum levels of nerve growth factor in a rat model of Alzheimer's disease. J Alzheimer's disease : JAD 25:213–217. doi:10.3233/JAD-2011-110047
Glaser V et al. (2010) The intra-hippocampal leucine administration impairs memory consolidation and LTP generation in rats. Cell Mol Neurobiol 30:1067–1075. doi:10.1007/s10571-010-9538-4
Gnahn H, Hefti F, Heumann R, Schwab ME, Thoenen H (1983) NGF-mediated increase of choline acetyltransferase (ChAT) in the neonatal rat forebrain: evidence for a physiological role of NGF in the brain? Brain Res 285:45–52
Gu H, Long D, Song C, Li X (2009) Recombinant human NGF-loaded microspheres promote survival of basal forebrain cholinergic neurons and improve memory impairments of spatial learning in the rat model of Alzheimer's disease with fimbria-fornix lesion. Neurosci Lett 453:204–209. doi:10.1016/j.neulet.2009.02.027
Haddad JJ, Land SC (2002) Redox/ROS regulation of lipopolysaccharide-induced mitogen-activated protein kinase (MAPK) activation and MAPK-mediated TNF-alpha biosynthesis. Br J Pharmacol 135:520–536. doi:10.1038/sj.bjp.0704467
Hock C, Heese K, Hulette C, Rosenberg C, Otten U (2000) Region-specific neurotrophin imbalances in Alzheimer disease: decreased levels of brain-derived neurotrophic factor and increased levels of nerve growth factor in hippocampus and cortical areas. Arch Neurol 57:846–851
Howell RK, Lee M (1963) Influence of alpha-ketoacids on the respiration of brain in vitro. Proc Soc Exp Biol Med 113:660–663
Huang EJ, Reichardt LF (2001) Neurotrophins: roles in neuronal development and function. Annu Rev Neurosci 24:677–736. doi:10.1146/annurev.neuro.24.1.677
Iwata E, Asanuma M, Nishibayashi S, Kondo Y, Ogawa N (1997) Different effects of oxidative stress on activation of transcription factors in primary cultured rat neuronal and glial cells Brain research. Mol Brain Res 50:213–220
Jan W, Zimmerman RA, Wang ZJ, Berry GT, Kaplan PB, Kaye EM (2003) MR diffusion imaging and MR spectroscopy of maple syrup urine disease during acute metabolic decompensation. Neuroradiology 45:393–399. doi:10.1007/s00234-003-0955-7
Jean YY, Lercher LD, Dreyfus CF (2008) Glutamate elicits release of BDNF from basal forebrain astrocytes in a process dependent on metabotropic receptors and the PLC pathway. Neuron Glia Biol 4:35–42. doi:10.1017/S1740925X09000052
Jouvet P, Kozma M, Mehmet H (2000a) Primary human fibroblasts from a maple syrup urine disease patient undergo apoptosis following exposure to physiological concentrations of branched chain amino acids. Ann N Y Acad Sci 926:116–121
Jouvet P et al. (2000b) Branched chain amino acids induce apoptosis in neural cells without mitochondrial membrane depolarization or cytochrome c release: implications for neurological impairment associated with maple syrup urine disease. Mol Biol Cell 11:1919–1932
Klee D et al. (2013) Structural white matter changes in adolescents and young adults with maple syrup urine disease. J Inherit Metab Dis 36:945–953. doi:10.1007/s10545-012-9582-y
Klein RL, Hirko AC, Meyers CA, Grimes JR, Muzyczka N, Meyer EM (2000) NGF gene transfer to intrinsic basal forebrain neurons increases cholinergic cell size and protects from age-related, spatial memory deficits in middle-aged rats. Brain Res 875:144–151
Lee R, Kermani P, Teng KK, Hempstead BL (2001) Regulation of cell survival by secreted proneurotrophins. Science 294:1945–1948. doi:10.1126/science.1065057
Lim KC, Lim ST, Federoff HJ (2003) Neurotrophin secretory pathways and synaptic plasticity. Neurobiol Aging 24:1135–1145
Lowry OH, Rosebrough NJ, Farr AL, Randall RJ (1951) Protein measurement with the Folin phenol reagent. J Biol Chem 193:265–275
Lu B, Pang PT, Woo NH (2005) The yin and yang of neurotrophin action. Nat Rev Neurosci 6:603–614. doi:10.1038/nrn1726
Lu Y, Christian K, Lu B (2008) BDNF: a key regulator for protein synthesis-dependent LTP and long-term memory? Neurobiol Learn Mem 89:312–323. doi:10.1016/j.nlm.2007.08.018
Meakin SO, Shooter EM (1992) The nerve growth factor family of receptors. Trends Neurosci 15:323–331
Mendell LM, Munson JB, Arvanian VL (2001) Neurotrophins and synaptic plasticity in the mammalian spinal cord. J Physiol 533:91–97
Mescka C et al. (2011) In vivo neuroprotective effect of L-carnitine against oxidative stress in maple syrup urine disease. Metab Brain Dis 26:21–28. doi:10.1007/s11011-011-9238-x
Mescka CP et al. (2013) Protein and lipid damage in maple syrup urine disease patients: l-carnitine effect. Int J Dev Neurosci 31:21–24. doi:10.1016/j.ijdevneu.2012.10.109
Michael GJ, Averill S, Nitkunan A, Rattray M, Bennett DL, Yan Q, Priestley JV (1997) Nerve growth factor treatment increases brain-derived neurotrophic factor selectively in TrkA-expressing dorsal root ganglion cells and in their central terminations within the spinal cord. J Neurosci Off J Soc Neurosci 17:8476–8490
Mu JS, Li WP, Yao ZB, Zhou XF (1999) Deprivation of endogenous brain-derived neurotrophic factor results in impairment of spatial learning and memory in adult rats. Brain Res 835:259–265
Mufson EJ et al. (2003) Preservation of brain nerve growth factor in mild cognitive impairment and Alzheimer disease. Arch Neurol 60:1143–1148. doi:10.1001/archneur.60.8.1143
Murer MG, Yan Q, Raisman-Vozari R (2001) Brain-derived neurotrophic factor in the control human brain, and in Alzheimer's disease and Parkinson's disease. Prog Neurobiol 63:71–124
Nagahara AH et al. (2009) Long-term reversal of cholinergic neuronal decline in aged non-human primates by lentiviral NGF gene delivery. Exp Neurol 215:153–159. doi:10.1016/j.expneurol.2008.10.004
Paxinos G, Watson C (1986) The Rat Brain in Stereotaxic Coordinates vol 2. Academic Press, San Diego
Peng S, Wuu J, Mufson EJ, Fahnestock M (2004) Increased proNGF levels in subjects with mild cognitive impairment and mild Alzheimer disease. J Neuropathol Exp Neurol 63:641–649
Peng S, Wuu J, Mufson EJ, Fahnestock M (2005) Precursor form of brain-derived neurotrophic factor and mature brain-derived neurotrophic factor are decreased in the pre-clinical stages of Alzheimer's disease. J Neurochem 93:1412–1421. doi:10.1111/j.1471-4159.2005.03135.x
Rantamaki T et al. (2013) The impact of Bdnf gene deficiency to the memory impairment and brain pathology of APPswe/PS1dE9 mouse model of Alzheimer's disease. PLoS One 8:e68722. doi:10.1371/journal.pone.0068722
Reichardt LF (2006) Neurotrophin-regulated signalling pathways. Philos Trans R Soc Lond Ser B Biol Sci 361:1545–1564. doi:10.1098/rstb.2006.1894
Ribeiro CA et al. (2008) Inhibition of brain energy metabolism by the branched-chain amino acids accumulating in maple syrup urine disease. Neurochem Res 33:114–124. doi:10.1007/s11064-007-9423-9
Scaini G et al. (2012a) Evaluation of acetylcholinesterase in an animal model of maple syrup urine disease. Mol Neurobiol 45:279–286. doi:10.1007/s12035-012-8243-3
Scaini G et al. (2012b) DNA damage in an animal model of maple syrup urine disease. Mol Genet Metab 106:169–174. doi:10.1016/j.ymgme.2012.04.009
Scaini G et al. (2012c) Antioxidant administration prevents memory impairment in an animal model of maple syrup urine disease. Behav Brain Res 231:92–96. doi:10.1016/j.bbr.2012.03.004
Scaini G et al. (2013a) Chronic administration of branched-chain amino acids impairs spatial memory and increases brain-derived neurotrophic factor in a rat model. J Inherit Metab Dis 36:721–730. doi:10.1007/s10545-012-9549-z
Scaini G et al. (2013b) Acute and chronic administration of the branched-chain amino acids decreases nerve growth factor in rat hippocampus. Mol Neurobiol 48:581–589. doi:10.1007/s12035-013-8447-1
Scaini G et al. (2015) Acute Administration of Branched-Chain Amino Acids Increases the Pro-BDNF/Total-BDNF Ratio in the Rat Brain. Neurochem Res 40:885–893. doi:10.1007/s11064-015-1541-1
Schonberger S, Schweiger B, Schwahn B, Schwarz M, Wendel U (2004) Dysmyelination in the brain of adolescents and young adults with maple syrup urine disease. Mol Genet Metab 82:69–75. doi:10.1016/j.ymgme.2004.01.016
Sgaravatti AM et al. (2003) Inhibition of brain energy metabolism by the alpha-keto acids accumulating in maple syrup urine disease. Biochim Biophys Acta 1639:232–238
Snyderman SE, Norton PM, Roitman E, Holt LE, Jr. (1964) Maple Syrup Urine Disease, with Particular Reference to Dietotherapy. Pediatrics 34:454–472
Sofroniew MV, Howe CL, Mobley WC (2001) Nerve growth factor signaling, neuroprotection, and neural repair. Annu Rev Neurosci 24:1217–1281. doi:10.1146/annurev.neuro.24.1.1217
Soule J, Messaoudi E, Bramham CR (2006) Brain-derived neurotrophic factor and control of synaptic consolidation in the adult brain. Biochem Soc Trans 34:600–604. doi:10.1042/BST0340600
Taketomi T, Kunishita T, Hara A, Mizushima S (1983) Abnormal protein and lipid compositions of the cerebral myelin of a patient with maple syrup urine disease. Jpn J Exp Med 53:109–116
Tavares RG, Santos CE, Tasca CI, Wajner M, Souza DO, Dutra-Filho CS (2000) Inhibition of glutamate uptake into synaptic vesicles of rat brain by the metabolites accumulating in maple syrup urine disease. J Neurol Sci 181:44–49
Taylor S, Srinivasan B, Wordinger RJ, Roque RS (2003) Glutamate stimulates neurotrophin expression in cultured Muller cells. Brain Res Mol Brain Res 111:189–197
Treacy E, Clow CL, Reade TR, Chitayat D, Mamer OA, Scriver CR (1992) Maple syrup urine disease: interrelations between branched-chain amino-, oxo- and hydroxyacids; implications for treatment; associations with CNS dysmyelination. J Inherit Metab Dis 15:121–135
Tribble D, Shapira R (1983) Myelin proteins: degradation in rat brain initiated by metabolites causative of maple syrup urine disease. Biochem Biophys Res Commun 114:440–446
Tyler WJ, Perrett SP, Pozzo-Miller LD (2002) The role of neurotrophins in neurotransmitter release. Neuroscientist 8:524–531
Vasques VC, Brinco F, Wajner M (2005) Intrahippocampal administration of the branched-chain alpha-hydroxy acids accumulating in maple syrup urine disease compromises rat performance in aversive and non-aversive behavioral tasks. J Neurol Sci 232:11–21. doi:10.1016/j.jns.2004.12.015
Verderio C, Bianco F, Blanchard MP, Bergami M, Canossa M, Scarfone E, Matteoli M (2006) Cross talk between vestibular neurons and Schwann cells mediates BDNF release and neuronal regeneration. Brain Cell Biol 35:187–201. doi:10.1007/s11068-007-9011-6
Vondran MW, Clinton-Luke P, Honeywell JZ, Dreyfus CF (2010) BDNF+/− mice exhibit deficits in oligodendrocyte lineage cells of the basal forebrain. Glia 58:848–856. doi:10.1002/glia.20969
Wajner M, Vargas CR (1999) Reduction of plasma concentrations of large neutral amino acids in patients with maple syrup urine disease during crises. Arch Dis Child 80:579
Wajner M, Coelho DM, Barschak AG, Araujo PR, Pires RF, Lulhier FL, Vargas CR (2000) Reduction of large neutral amino acid concentrations in plasma and CSF of patients with maple syrup urine disease during crises. J Inherit Metab Dis 23:505–512
Walsh KS, Scott MN (2010) Neurocognitive profile in a case of maple syrup urine disease. Clin Neuropsychol 24:689–700. doi:10.1080/13854040903527279
Walsh GS, Krol KM, Crutcher KA, Kawaja MD (1999) Enhanced neurotrophin-induced axon growth in myelinated portions of the CNS in mice lacking the p75 neurotrophin receptor. The J Neurosci Official J Soc Neurosci 19:4155–4168
Xiao J, Wong AW, Willingham MM, van den Buuse M, Kilpatrick TJ, Murray SS (2010) Brain-derived neurotrophic factor promotes central nervous system myelination via a direct effect upon oligodendrocytes. Neurosignals 18:186–202. doi:10.1159/000323170
Yoshii A, Constantine-Paton M (2010) Postsynaptic BDNF-TrkB signaling in synapse maturation, plasticity, and disease. Dev Neurobiol 70:304–322. doi:10.1002/dneu.20765
Zielke HR, Huang Y, Tildon JT, Zielke CL, Baab PJ (1996) Elevation of amino acids in the interstitial space of the rat brain following infusion of large neutral amino and keto acids by microdialysis: alpha-ketoisocaproate infusion. Dev Neurosci 18:420–425
Zielke HR, Zielke CL, Baab PJ, Collins RM (2002) Large neutral amino acids auto exchange when infused by microdialysis into the rat brain: implication for maple syrup urine disease and phenylketonuria. Neurochem Int 40:347–354
Zou J, Crews F (2006) CREB and NF-kappaB transcription factors regulate sensitivity to excitotoxic and oxidative stress induced neuronal cell death. Cell Mol Neurobiol 26:385–405. doi:10.1007/s10571-006-9045-9
Acknowledgments
Laboratory of Bioenergetics (Brazil) is one of the centers of the National Institute for Molecular Medicine (INCT-MM) and one of the members of the Center of Excellence in Applied Neurosciences of Santa Catarina (NENASC). This research was supported by grants from Universidade do Extremo Sul Catarinense (UNESC), Coordenação de Aperfeiçoamento de Pessoal de Nível Superior (CAPES) and Conselho Nacional de Desenvolvimento Científico e Tecnológico (CNPq).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Wisniewski, M.S.W., Carvalho-Silva, M., Gomes, L.M. et al. Intracerebroventricular administration of α-ketoisocaproic acid decreases brain-derived neurotrophic factor and nerve growth factor levels in brain of young rats. Metab Brain Dis 31, 377–383 (2016). https://doi.org/10.1007/s11011-015-9768-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11011-015-9768-8