Abstract
Microglia are the brain resident phagocytes that act as the primary form of the immune defense in the central nervous system. These cells originate from primitive macrophages that arise from the yolk sac. Advances in imaging and single-cell RNA-seq technologies provided new insights into the complexity of microglia biology.
Microglia play an essential role in the brain development and maintenance of brain homeostasis. They are also crucial in injury repair in the central nervous system. The tumor microenvironment is complex and includes neoplastic cells as well as varieties of host and infiltrating immune cells. Microglia are part of the glioma microenvironment and play a critical part in initiating and maintaining tumor growth and spread. Microglia can also act as effector cells in treatments against gliomas. In this chapter, we summarize the current knowledge of how and where microglia are generated. We also discuss their functions during brain development, injury repair, and homeostasis. Moreover, we discuss the role of microglia in the tumor microenvironment of gliomas and highlight their therapeutic implications.
Access provided by Autonomous University of Puebla. Download chapter PDF
Similar content being viewed by others
Keywords
- Microglia
- Brain tumor
- Glioma
- High-grade glioma
- Glioblastoma
- Gliomagenesis
- Macrophage
- Development
- Pericyte
- M1
- M2
- Microenvironment extracellular matrix
- Immune therapy
- CD47
11.1 Introduction
Gliomas are a heterogeneous group of tumors (WHO Grade I–IV), including astrocytoma, oligodendroglioma, and ependymoma [40]. They represent the most common brain tumor in adults, making up 30% of all Central Nervous System (CNS) neoplasms and more than 80% of malignant CNS tumors [24]. The most common glioma in adults is Glioblastoma Multiforme (GBM), which is a highly aggressive tumor with a dismal prognosis. The current standard-of-care for adults with malignant glioma is maximal surgical resection, followed by radiation and occasionally chemotherapy. With few available therapy options and little improvement in survival over the past several decades, this disease is in dire need of a new treatment paradigm.
In recent years, immunotherapy in the treatment of CNS neoplasms has become a subject of great interest. The CNS is home to microglia, a resident intracerebral phagocyte critically involved in brain development, homeostasis, and response to injury and disease. Our understanding of the origin, function, and phenotype of microglia has dramatically advanced in the past three decades. Because of these advances, it is now possible to study microglia in the context of brain tumor pathophysiology. In this chapter, we will provide a brief introduction to the origin and functions of microglia and subsequently discuss the role of microglia within the brain tumor microenvironment. Finally, we will examine the therapeutic potential of microglia as a target or effector cell in the treatment of glioma.
11.2 Embryological Origin, Development, and Function of Microglia
11.2.1 Origin and Development
The exact origin of microglia has remained a subject of debate since their discovery in 1919 by del Río Hortega. Microglia were initially thought to derive from the neuroectoderm, along with neurons and other resident CNS cells that make up the brain parenchyma. When microglia were found to express distinctive macrophage antigens on their surface, an extracerebral hematopoietic origin was suggested [56]. In the 1990s, researchers posited that microglial progenitors arise from the mesodermal tissue in the yolk sac and migrate into the brain rudiment in rodents and humans [2, 3]. In 2010, Ginhoux et al. provided conclusive evidence that these “microglial progenitors” are, in fact, primitive macrophages [23].
By E9.5, around the start of angiogenesis, these primitive macrophages surround the developing neuroepithelium and begin migrating into the neuroectoderm by E10.5. At this stage, immature, amoeboid microglia begin populating the cerebral cortex and white matter before migrating into the telencephalon [49]. These amoeboid microglia are highly active and proliferative, expressing Ki67 and Runx1, a transcription factor involved in myeloid lineage differentiation [67]. Mature, ramified microglia can be observed throughout the fetal brain parenchyma by E28, earlier than any other glial cell [51].
Though the origin of microglia from a singular source is widely accepted, the heterogeneity of microglia has led to further investigation into their ontogeny. It has been suggested that a Hoxb8+ subset of microglia are derived from the bone marrow of adult mice or during a “second wave” of hematopoiesis during development [14].
11.2.2 Function of Microglia Within the Developing Fetal and Postnatal Brain
The development and organization of the cerebral cortex during prenatal development is dependent upon the proper balance between proliferation and inhibition of growth: too many neural precursor cells and resulting cortical neurons can have devastating effects. Microglia serve a vital role in this balance by regulating the number of precursor cells within the neural proliferative zones through phagocytosis. Importantly, evidence suggests that microglia not only phagocytose abnormal or apoptotic cells, but also viable precursor cells [16].
Microglia also play a critical role in normal postnatal brain development. Microglia are actively involved in the formation of neuronal circuitry, primarily through pruning of extraneous presynaptic material [71]. During a specific window of time in which synaptic creation and elimination are peaking, the complement cascade proteins C1q and C3b are expressed on the surface of developing synapses. As the only known CNS-resident cell with a receptor for activated C3 (C3b), microglia are the most likely phagocytes responding to opsonized C3b [64].
During the third postnatal week (P21), microglia numbers begin to decline gradually and reach a population steady state by postnatal week six [52]. Using a multicolor “Microfetti” fate-mapping mouse model, Tay et al. concluded that every mature microglial cell is plastic and can divide to give rise to a clone [66]. Thus, the population of microglia within the developed brain is self-sustaining and maintained by a precise balance of apoptosis and proliferation in the absence of injury or disease.
11.3 Characterization of Microglia
11.3.1 Homeostasis
In addition to the controversy surrounding the ontogeny of microglia, the phenotypic characterization of microglia has been a source of debate and conjecture. In order to study their unique physiological role, it is necessary to distinguish microglia from other antigen-presenting or CNS-resident cells. Early studies of microglia within the glioma microenvironment relied on surface proteins, such as CD45, to eliminate non-immune cells and CD11b to further isolate dendritic cells. Other early studies relied on CD45low expression and cell morphology to distinguish microglia from other cells. However, these two characteristics are subject to change with disease and injury. Further, it is known that microglia within the tumor microenvironment (TME) can upregulate CD45, further complicating its use in this context [6].
The first functional surface protein with reported expression on the surface of mature microglia was the fractalkine CX3CR1, which is necessary for neuron–microglia crosstalk [30]. Jung et al. subsequently established a transgenic mouse model for the study of microglia in which CX3CR1 was replaced with a reporter GFP gene [35]. The specificity of CX3CR1 expression in microglia was confirmed in a gene expression profile analysis across various phagocyte populations [21]. TMEM119 is another promising microglia-specific surface marker. TMEM119 may be particularly useful in studying microglia throughout development, as its expression is evident from early development through maturation [7]. A third microglia-specific surface marker, P2RY12, was identified through RNAseq and proteomics [11]. The presence of both TMEM119 and P2RY12 has been confirmed in other transcriptomic profiling studies [78].
Recent advances in single-cell RNA-sequencing has allowed for regional and temporal transcriptional-level characterization of microglia across both the human and mouse brain [44]. This technology has generated a tremendously comprehensive profile of microglial regional heterogeneity in both healthy and diseased human brain. In the healthy, homeostatic brain, TMEM119, P2RY13, CX3CR1, SLC2A5, and P2RY12 are the most enriched genes. The expression of these “core” genes changes in the setting of demyelination and neurodegeneration. Additional genes are often enriched depending on disease state , which may establish a disease-specific genetic signature.
11.3.2 Polarization
Peripheral blood-derived macrophages are often characterized by their state of polarization. M1macrophages are considered “pro-inflammatory,” while M2macrophages are considered anti-inflammatory and are involved in tissue healing [48]. This dichotomy may be an oversimplification of actual macrophage activity in vivo, which likely exists as a complex spectrum. However, this M1/M2 nomenclature is widely utilized to describe macrophage behavior [75].
The existence of a similar polarization state or activity spectrum in microglia in vivo is controversial [60]. Based upon this a priori definition of activated macrophage classification, multiple studies have similarly attempted to categorize microglia into this dichotomous relationship. However, in-depth transcriptomic analyses of microglia have failed to prove this relationship in vivo [72]. Such investigations have revealed that microglia are incredibly diverse . This conclusion should come as no surprise given their complex range of functions within an ever-changing microenvironment across the lifespan.
11.4 Function of Microglia
11.4.1 Homeostasis
In 2005, two landmark studies provided conclusive proof of active microglia within the homeostatic adult brain [17, 53]. Thanks to technological advances in microscopy allowing for intravital imaging, interactions between microglia and other CNS-resident cells within their native environment could be visualized for the first time. This imaging modality revealed highly active “resting” microglia, perpetually surveying their environment by extending their long processes. Microglia can detect minute changes within their microenvironment due to the presence of diverse signaling receptors for both endogenous and exogenous insults. After a threat is detected, microglia react through phagocytosis or production of inflammatory and trophic factors [19]. This response, while necessary for the protection of the CNS , can also lead to aberrant effects.
The adult brain has two sites of continued neurogenesis: the subgranular zone (SGZ) of the dentate nucleus found in the hippocampus and in the olfactory bulb. Within the SGZ, the majority of quiescent neural progenitor cells (NPCs) that become activated die as neuroblasts before becoming immature neurons. Apoptotic cells and debris are phagocytosed by unchallenged microglia within this niche. In this setting, microglia do not need to be “activated,” as has been reported in other conditions. These microglia maintain their high phagocytic efficiency in the presence of inflammatory conditions and in spite of decreased neurogenesis due to age [63].
11.4.2 Injury
An in-depth discussion of microglia’s role in diseases outside of brain tumors is beyond the scope of this chapter; however, the inclusion of some background information is warranted. In the setting of brain tumors, injury occurs during tumor growth and radiation therapy-induced inflammation. Both processes elicit changes within the brain that promote activation and chemotaxis of microglia.
Microglia are primarily directed to sites of injury to the blood-brain barrier (BBB) by stimulation of P2Y G-protein coupled receptors. Upon P2Y receptor stimulation by extracellular ATP, ADP, or UTP, microglia rapidly converge at the site of injury and begin proliferating [17]. In addition to stimulating the motility of microglia , ATP can induce microglial production of IL1β, TNF-α, and plasminogen [31]. Clopidogrel was administered in a mouse model to inhibit P2YR12. As a result, chemotaxis of microglia to sites of BBB injury and subsequent closure of the defect were greatly impaired [39].
Neuroinflammation is a significant complication resulting from radiation therapy for glioma [26]. In response to irradiation, it has been reported that microglia begin secreting cytotoxic and proinflammatory factors, including IL-6, TNF-α, and PGE2 [33]. PGE2 release by microglia has been suggested to significantly contribute to inflammation and reactive gliosis following irradiation. Irradiation-induced changes to the BBB further attract microglia, which bolster the proinflammatory milieu. While this inflammation can be pharmacologically mitigated by the use of COX-2 inhibitors, potentially positive neuroprotective functions of microglia are also stifled.
11.5 Microglia Within the Tumor Microenvironment
In 1925, Wilder Penfield published the first description of microglia in the context of glioma. Penfield, who studied the development and behavior of microglia under del Rio-Hortega, suggested that microglia within the TME play a significant role in extracellular matrix (ECM) remodeling and the destruction of by-products from this process [55]. It was not until much later that this ECM-remodeling role of microglia was suggested to be pro-tumorigenic and not merely a reaction to tissue injury. In 2002, Bettinger et al. published a study in which Boyden chambers were used to study the effect of microglia on glioma cell migration in vitro [8]. They found that in the presence of microglia or microglia-conditioned media, glioma cells exhibited up to a threefold increase in motility (Fig. 11.1).
The complex interplay between brain-resident microglia and tumor cells is highlighted by this very simplified schematic. Brain microglia and infiltrating peripheral macrophages are reprogrammed or re-educated to produce growth factors that increase glioma cell proliferation, attenuate glioma cell apoptosis, and promote tumor cell migration. Chemokines produced by glioma cells actively recruit resident microglia from the brain, as well as macrophages from the blood, through binding to their cognate receptors. In addition, glioma cells either intrinsically produce proteins that increase cytokine release and induce extensive ECM remodeling or can co-opt glioma-associated microglia to do the same. Extensive remodeling of the ECM is not restricted to physical alteration of the tissue microenvironment but also induce immune suppression by blocking the infiltration of T cells and inducing apoptosis of Fas-L-expressing T cells
11.5.1 Immune-Suppression and Evasion
Increased prostaglandin synthases and upstream enzyme cyclooxygenase-2 (COX-2) have been reported in a variety of malignancies, including glioma [47]. COX-2 is an inducible enzyme involved in the conversion of arachidonic acid to prostaglandins (PGE1 and PGE2). COX-2 upregulation in gliomas is associated with more aggressive tumors and a worse prognosis [62]. PGE2 blocks the activation of T cells by inhibiting T cell–dendritic cell interactions [73]. Glioma cells are known to release PGE2. However, when glioma-released soluble factors are present, microglia may release a more significant quantity of PGE2 [50]. In addition to inhibition of T-cell activation, PGE2 production is associated with TNF downregulation, which is a potential mechanism of decreased TRAIL-mediated apoptosis in glioma cells [29].
Fas-Fas ligand (FasL) may also play a role in the microglia-induced immunosuppressive environment of gliomas [5]. Some level of FasL expression is seen in neurons, astrocytes, and microglia in homeostatic and pathological conditions, perhaps as a protective mechanism against inflammation. Upregulation of FasL on the surface of tumor-associated microglia leads to apoptosis of FasL-expressing T cells. Supporting this hypothesis, when FasL expression was inhibited in a murine model of glioma, leukocyte infiltration into tumors increased up to threefold.
In addition to its involvement in ECM remodeling, discussed below, TLR2 plays a role in glioma immune evasion. In a murine model of glioma, TLR2 was reported to cause downregulation of MHC Class II expression on microglia [59]. This decreases the antigen-presenting capabilities of microglia, limiting the role of CD4+ T cells in antitumor immunity.
11.5.2 ECM Remodeling
Microglia secrete a variety of factors to increase their motility, which is necessary to their role as resident surveyors of the CNS. In the setting of glioma, this increase in motility comes at a cost. Glioma cells exploit ECM remodeling, which is necessary to allow microglia to survey their environment and migrate toward threats.
TGF-β1, which is necessary for microglial development and activation, also promotes glioma invasiveness and progression. In a syngeneic mouse glioma model, high levels of TGF-β1 production by TAMs caused an increase in MMP-9 production by CD133+ glioma “stem-like cells” (GSLCs). This paracrine stimulation via the TGFBR2 pathway is thought to be the direct cause of glioma invasiveness into surrounding parenchyma [76]. Another modulator of MMP-9, STI1 (stress inducible protein 1), is also upregulated in the TME and its increase is associated with disease progression [13].
Another proinflammatory cytokine, IL-6, has been implicated as a protumorigenic signal in the TME of gliomas. IL-6 secretion by microglia/TAMs is induced by interaction with CD133+ GSLCs and acts as a mitogen for GSLCs [18]. The exact pathway by which this occurs is the subject of debate, with in vitro evidence suggesting TLR4 or CCR2 as the key mediator of this pathway [18, 77].
TLR2 has also been implicated as a mediator of microglia–glioma interactions [68]. TLR2 stimulation ex vivo leads to MT1-MMP upregulation in microglia, presumably leading to remodeling of the ECM and further invasion of glioma cells in vivo. The importance of TLR2 in glioma pathobiology was further confirmed in a TLR2-KO mouse model in which TLR2-KO mice showed smaller tumors and better survival than those in WT mice. A vicious cycle of TLR–glioma interactions has been posited in which microglia expressing TLR2 are stimulated by glioma-released factors (e.g. HMGB1, HSPs, hyaluronan) and microglia increase ECM remodeling by TLR2-induced MT1-MMP upregulation. This ECM remodeling further amplifies TLR2 signaling, thereby advancing glioma invasion and expansion [68]. When the MT1-MMP pathway is inhibited in vivo, glioma cell growth and invasion are attenuated [43]. This MT1-MMP upregulation in mouse microglia was not observed in human microglia; instead, MT3-MMP serves an analogous role in the human glioma microenvironment [54].
11.5.3 Microglia and Pericytes
Pericytes are multifunctional cells that wrap around endothelial cells lining the microvasculature of tumors, as well as normal capillaries and venules. These cells serve a multitude of essential blood vessel functions, including regulation of flow, clearance of cellular debris via phagocytosis, and help in the maturation and stabilization of the endothelial cells. Pericytes interact with blood vessel-associated cells via paracrine signaling and direct cell-to-cell membrane interactions . Pericytes play an essential role in maintaining the blood–brain barrier (BBB) during homeostasis and disease, and have unique functions within the CNS [4].
Pericytes have recently been classified into two subtypes [9]. Both subtypes (Type-1 and Type-2) express the classical pericyte markers CD146/PDGFRβ/NG2, but only Type-2 express Nestin. Using a syngeneic model, Birbrair et al. found that only Type-2 pericytes participate in normal and tumor angiogenesis both in vivo and in vitro [10]. Additionally, cerebral host pericytes are actively recruited to the tumor site and participate in vascular formation in a murine syngeneic orthotopic model of glioma [65].
Depending upon disease states (e.g., tumor progression or radiation-induced injury) pericytes can alter the activation state of microglia. In the setting of neuroinflammation, pericytes are stimulated by TNF-α and release proinflammatory factors, causing upregulation of iNOS and IL-1β in microglia [46]. Microglia in this setting are phagocytic and likely to be actively involved in tissue remodeling, which may also contribute to tumor invasion. Conversely, microglia can influence pericytes to promote tumor growth. Wallman et al. recently demonstrated that M2-polarized microglia induced high expression of PDGFRβ expression in glioma cells and stimulated their migratory capacity [70]. They proposed that microglia–glioma cell-to-cell contact regulates PDGFRβ transcription, affecting the known transcription factors promoting PDGFRβ transcription. The microglial PDGFRβ expression results in a feed-forward cycle of tissue remodeling, PDGF release, and chemotaxis of angiogenic pericytes and migratory glioma cells. In a mouse model of PDGFβ-driven high-grade glioma, the vast majority of tumor pericytes were found in close association with microglia rather than in conjugation with perfused vessels [70]. Thus, microglia act to actively recruit pericytes to the tumor microvasculature.
Interestingly, glioblastoma-associated pericytes have also been observed to express signals associated with immune suppression, such as IL-10 and TGF-β [61]. These signals are associated with inactive microglia, thus reducing their ability to act as phagocytes. Recent evidence suggests that targeting pericytes in glioma improves response to therapy, either by increasing drug permeability or by decreasing immune suppression [25]. Another study used an Ang-2/VEGF bi-specific antibody to target tumor angiogenesis in GBM. The authors observed increased survival and reprogramming of microglia and macrophages to an antitumor phenotype [36]. Collectively, these results suggest that reversing the immune-suppressive environment supported by pericytes is a promising treatment strategy.
11.5.4 Microglia–Glioma Crosstalk
Glioma cells are thought to secrete a variety of factors that attract microglia/macrophages to the tumor site, among other downstream effects. One such factor released by glioma cells is CSF-1 (M-CSF), a ligand of CSF-1R [37]. Glioma cells constitutively release CSF-1, which attracts TAMs to the tumor site and enhances TAM–glioma crosstalk. CSF-1R is also necessary for maintenance of the steady-state microglia population in adult mice [20]. In a preclinical murine model, inhibition of CSF-1R with the small molecule PLX3397 stopped glioma cells from invading the surrounding parenchyma, perhaps due to inhibition of microglia activation and proliferation [15].
The WNT/β-catenin pathway is important for gliomagenesis, and its expression correlates with disease progression [58]. Microglia express a variety of WNT receptors, including multiple FZDs and LRP6 [28]. Expression of WNT3a by glioma cells is thought to increase glioma–microglia interactions. Matias et al. have demonstrated that WNT3a stimulation of microglia induces their expression of ARG-1 and STI1 and pushes them toward an “M2-like” phenotype [45].
CXCL16, released by glioma cells, polarizes microglia and TAMs toward an “anti-inflammatory” phenotype in vitro. The importance of the CXCL16/CXCR6 axis for tumor growth was confirmed in a syngeneic mouse model. GL261, a mouse glioma cell line, expresses both CXCL16 and CXCR6, with the highest expression on CD133+ cells. When GL261 tumor cells with a knockdown of CXCR6 were engrafted in WT mice, a lower tumor volume was observed compared to mice engrafted with parental GL261 cells. Additionally, stimulation of tumors with CXCL16 causes increased proliferation and invasion into surrounding parenchyma [38].
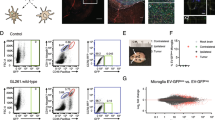
Within the tumor microenvironment, microglia readily take up extracellular vesicles (EVs) released by glioma cells. These extracellular vesicles contain proteins, lipids, and nucleic acids, which, upon uptake into microglia, can serve as intercellular messengers [41]. Recent evidence suggests that microRNA (miRNA) contained in these vesicles may affect tumor-associated microglial transcription. Specifically, miR-21 is thought to downregulate Btg2, which is involved in the regulation of cell proliferation [1]. Btg2 downregulation by miR-21 leads to increased microglia proliferation, which in turn increases glioma invasiveness.
11.6 Therapeutic Implications
11.6.1 Microglia as a Therapeutic Target
The preclinical success of CSFR-1 inhibitor, PLX3397, set the stage for a clinical trial for the treatment of recurrent GBM. Although the treatment was well tolerated and effectively crossed the BBB, no clinical response was seen (NCT01349036) [12]. In another Phase II trial (NCT01790503), PLX3397 was combined with temozolomide and radiation for the treatment of primary GBM. The complete results of this study have not been published, but the available preliminary results do not suggest this treatment approach was effective.
Microglia suppression by minocycline was effective in reducing glioma growth and progression in preclinical murine models of glioma [43]. Minocycline may block expression of MT1-MMP, slowing ECM remodeling by microglia. However, this success was not replicated when minocycline was used as an adjuvant treatment in human clinical trials (NCT01580969, NCT02272270, and NCT02770378) [27]. This lack of translation is likely due to the involvement of MT3-MMP expression, rather than MT1-MMP, in human gliomas, which was discussed earlier in this chapter.
THIK-1, a constitutively active K+ channel on the surface of microglia, has recently been reported to regulate microglial motility, surveillance, and IL-1β release [42]. IL-1β is known to be necessary for glioma angiogenesis and invasion [69]. Pharmacological inhibition of THIK-1 as a therapy in the treatment of glioma has been suggested [57]. Assessment of the efficacy of THIK-1 inhibition as a treatment strategy against glioma has thus far been limited by a lack of drugs targeting THIK-1 and the need for a better understanding of this pathway.
11.6.2 Microglia as an Effector Cell
One common mechanism of tumor cell immune evasion is the upregulation of CD47, which, upon binding to SIRPα on the phagocyte’s surface, acts as an antiphagocytic “don’t eat me” signal [34]. This protective mechanism has been successfully abrogated in multiple in vivo studies by the treatment of tumors with an anti-CD47 mAb [22, 32, 74]. Until recently, peripheral CCR2+macrophages were the only known effector cell of this treatment. Using a transgenic mouse model constitutively expressing RFP+ CCR2+ peripheral macrophages and GFP+ CX3CR1+ microglia, Hutter et al. showed for the first time that microglia are also potent mediators of the anti-CD47 response against an adult GBM xenograft [32]. Perhaps the most striking finding of this study was the strength of phagocytic response to anti-CD47 treatment even in mice with absent CCR2+peripheral macrophages. With a lower inflammatory signature than activated peripheral macrophages, microglia have promising therapeutic potential in the treatment of glioma.
11.7 Conclusion and Future Directions
Despite recent advances in understanding the ontogeny and physiology of microglia, many questions remain. By necessity, microglia promote ECM remodeling, a function that has been implicated as pro-tumorigenic. However, efforts to target this process to reduce tumor invasion have been unsuccessful in clinical trials, perhaps due to inter-species differences or heterogeneity of microglia. A recent in vivo study has shown microglia to be a promising effector cell in checkpoint inhibitor therapy against GBM [32]. Future studies should aim to further characterize these microglia in order to fully exploit this potential.
References
Abels ER, Maas SLN, Nieland L, Wei Z, Cheah PS, Tai E, Kolsteeg CJ, Dusoswa SA, Ting DT, Hickman S, El Khoury J, Krichevsky AM, Broekman MLD, Breakefield XO (2019) Glioblastoma-associated microglia reprogramming is mediated by functional transfer of extracellular miR-21. Cell Rep 28(12):3105–3119. e3107. https://doi.org/10.1016/j.celrep.2019.08.036
Alliot F, Godin I, Pessac B (1999) Microglia derive from progenitors, originating from the yolk sac, and which proliferate in the brain. Dev Brain Res 117(2):145–152. https://doi.org/10.1016/S0165-3806(99)00113-3
Alliot F, Lecain E, Grima B, Pessac B (1991) Microglial progenitors with a high proliferative potential in the embryonic and adult mouse brain. Proc Natl Acad Sci U S A 88(4):1541–1545. https://doi.org/10.1073/pnas.88.4.1541
Armulik A, Genove G, Mae M, Nisancioglu MH, Wallgard E, Niaudet C, He L, Norlin J, Lindblom P, Strittmatter K, Johansson BR, Betsholtz C (2010) Pericytes regulate the blood-brain barrier. Nature 468(7323):557–561. https://doi.org/10.1038/nature09522
Badie B, Schartner J, Prabakaran S, Paul J, Vorpahl J (2001) Expression of Fas ligand by microglia: possible role in glioma immune evasion. J Neuroimmunol 120(1–2):19–24. https://doi.org/10.1016/s0165-5728(01)00361-7
Badie B, Schartner JM (2000) Flow cytometric characterization of tumor-associated macrophages in experimental gliomas. Neurosurgery 46(4):957–961; discussion 961–952. https://doi.org/10.1097/00006123-200004000-00035
Bennett ML, Bennett FC, Liddelow SA, Ajami B, Zamanian JL, Fernhoff NB, Mulinyawe SB, Bohlen CJ, Adil A, Tucker A, Weissman IL, Chang EF, Li G, Grant GA, Hayden Gephart MG, Barres BA (2016) New tools for studying microglia in the mouse and human CNS. Proc Natl Acad Sci U S A 113(12):E1738–E1746. https://doi.org/10.1073/pnas.1525528113
Bettinger I, Thanos S, Paulus W (2002) Microglia promote glioma migration. Acta Neuropathol 103(4):351–355. https://doi.org/10.1007/s00401-001-0472-x
Birbrair A, Zhang T, Wang ZM, Messi ML, Enikolopov GN, Mintz A, Delbono O (2013) Skeletal muscle pericyte subtypes differ in their differentiation potential. Stem Cell Res 10(1):67–84. https://doi.org/10.1016/j.scr.2012.09.003
Birbrair A, Zhang T, Wang ZM, Messi ML, Olson JD, Mintz A, Delbono O (2014) Type-2 pericytes participate in normal and tumoral angiogenesis. Am J Physiol Cell Physiol 307(1):C25–C38. https://doi.org/10.1152/ajpcell.00084.2014
Butovsky O, Jedrychowski MP, Moore CS, Cialic R, Lanser AJ, Gabriely G, Koeglsperger T, Dake B, Wu PM, Doykan CE, Fanek Z, Liu L, Chen Z, Rothstein JD, Ransohoff RM, Gygi SP, Antel JP, Weiner HL (2014) Identification of a unique TGF-beta-dependent molecular and functional signature in microglia. Nat Neurosci 17(1):131–143. https://doi.org/10.1038/nn.3599
Butowski N, Colman H, De Groot JF, Omuro AM, Nayak L, Wen PY, Cloughesy TF, Marimuthu A, Haidar S, Perry A, Huse J, Phillips J, West BL, Nolop KB, Hsu HH, Ligon KL, Molinaro AM, Prados M (2016) Orally administered colony stimulating factor 1 receptor inhibitor PLX3397 in recurrent glioblastoma: an Ivy Foundation Early Phase Clinical Trials Consortium phase II study. Neuro-Oncology 18(4):557–564. https://doi.org/10.1093/neuonc/nov245
Carvalho da Fonseca AC, Wang H, Fan H, Chen X, Zhang I, Zhang L, Lima FR, Badie B (2014) Increased expression of stress inducible protein 1 in glioma-associated microglia/macrophages. J Neuroimmunol 274(1–2):71–77. https://doi.org/10.1016/j.jneuroim.2014.06.021
Chen SK, Tvrdik P, Peden E, Cho S, Wu S, Spangrude G, Capecchi MR (2010) Hematopoietic origin of pathological grooming in Hoxb8 mutant mice. Cell 141(5):775–785. https://doi.org/10.1016/j.cell.2010.03.055
Coniglio SJ, Eugenin E, Dobrenis K, Stanley ER, West BL, Symons MH, Segall JE (2012) Microglial stimulation of glioblastoma invasion involves epidermal growth factor receptor (EGFR) and colony stimulating factor 1 receptor (CSF-1R) signaling. Mol Med 18:519–527. https://doi.org/10.2119/molmed.2011.00217
Cunningham CL, Martinez-Cerdeno V, Noctor SC (2013) Microglia regulate the number of neural precursor cells in the developing cerebral cortex. J Neurosci 33(10):4216–4233. https://doi.org/10.1523/JNEUROSCI.3441-12.2013
Davalos D, Grutzendler J, Yang G, Kim JV, Zuo Y, Jung S, Littman DR, Dustin ML, Gan WB (2005) ATP mediates rapid microglial response to local brain injury in vivo. Nat Neurosci 8(6):752–758. https://doi.org/10.1038/nn1472
Dzaye O, Hu F, Derkow K, Haage V, Euskirchen P, Harms C, Lehnardt S, Synowitz M, Wolf SA, Kettenmann H (2016) Glioma stem cells but not bulk glioma cells upregulate IL-6 secretion in microglia/brain macrophages via toll-like receptor 4 signaling. J Neuropathol Exp Neurol 75(5):429–440. https://doi.org/10.1093/jnen/nlw016
ElAli A, Rivest S (2016) Microglia ontology and signaling. Front Cell Dev Biol 4:72. https://doi.org/10.3389/fcell.2016.00072
Elmore MR, Najafi AR, Koike MA, Dagher NN, Spangenberg EE, Rice RA, Kitazawa M, Matusow B, Nguyen H, West BL, Green KN (2014) Colony-stimulating factor 1 receptor signaling is necessary for microglia viability, unmasking a microglia progenitor cell in the adult brain. Neuron 82(2):380–397. https://doi.org/10.1016/j.neuron.2014.02.040
Gautier EL, Shay T, Miller J, Greter M, Jakubzick C, Ivanov S, Helft J, Chow A, Elpek KG, Gordonov S, Mazloom AR, Ma’ayan A, Chua WJ, Hansen TH, Turley SJ, Merad M, Randolph GJ, Immunological Genome C (2012) Gene-expression profiles and transcriptional regulatory pathways that underlie the identity and diversity of mouse tissue macrophages. Nat Immunol 13(11):1118–1128. https://doi.org/10.1038/ni.2419
Gholamin SM, Mitra SS, Feroze A, Liu J, Kahn S, Zhang M, Esparza R (2017) Disrupting the CD47-SIRPa anti-phagocytic axis by a humanized anti-CD47 antibody is an efficacious treatment for malignant pediatric brain tumors. Sci Transl Med 9(381):eaaf2968
Ginhoux F, Greter M, Leboeuf M, Nandi S, See P, Gokhan S, Mehler MF, Conway SJ, Ng LG, Stanley ER, Samokhvalov IM, Merad M (2010) Fate mapping analysis reveals that adult microglia derive from primitive macrophages. Science 330(6005):841–845. https://doi.org/10.1126/science.1194637
Goodenberger ML, Jenkins RB (2012) Genetics of adult glioma. Cancer Genet 205(12):613–621. https://doi.org/10.1016/j.cancergen.2012.10.009
Guerra DAP, Paiva AE, Sena IFG, Azevedo PO, Silva WN, Mintz A, Birbrair A (2018) Targeting glioblastoma-derived pericytes improves chemotherapeutic outcome. Angiogenesis 21(4):667–675. https://doi.org/10.1007/s10456-018-9621-x
Gupta K, Burns TC (2018) Radiation-induced alterations in the recurrent glioblastoma microenvironment: therapeutic implications. Front Oncol 8:503. https://doi.org/10.3389/fonc.2018.00503
Gutmann DH, Kettenmann H (2019) Microglia/brain macrophages as central drivers of brain tumor pathobiology. Neuron 104(3):442–449. https://doi.org/10.1016/j.neuron.2019.08.028
Halleskog C, Mulder J, Dahlstrom J, Mackie K, Hortobagyi T, Tanila H, Kumar Puli L, Farber K, Harkany T, Schulte G (2011) WNT signaling in activated microglia is proinflammatory. Glia 59(1):119–131. https://doi.org/10.1002/glia.21081
Hao CB, Beguinot F, Condorelli G, Alessandra Trencia EG, Van Meir V, Yong W, Parney IF, Roa WH, Petruk KC (2001) Induction and intracellular regulation of tumor necrosis factor-related apoptosisinducing ligand (TRAIL) mediated Apotosis in human malignant glioma cells. Cancer Res 61(3):1162–1170
Harrison JK, Jiang Y, Chen SZ, Xia YY, Maciejewski D, McNamara RK, Streit WJ, Salafranca MN, Adhikari S, Thompson DA, Botti P, Bacon KB, Feng LL (1998) Role for neuronally derived fractalkine in mediating interactions between neurons and CX3CR1-expressing microglia. Proc Natl Acad Sci U S A 95(18):10896–10901. https://doi.org/10.1073/pnas.95.18.10896
Honda S (2001) Extracellular ATP or ADP induce chemotaxis of cultured microglia through Gi/o-coupled P2Y receptors. The Journal of Neuroscience 21(6):1975–1982
Hutter G, Theruvath J, Graef CM, Zhang M, Schoen MK, Manz EM, Bennett ML, Olson A, Azad TD, Sinha R, Chan C, Assad Kahn S, Gholamin S, Wilson C, Grant G, He J, Weissman IL, Mitra SS, Cheshier SH (2019) Microglia are effector cells of CD47-SIRPalpha antiphagocytic axis disruption against glioblastoma. Proc Natl Acad Sci U S A 116(3):997–1006. https://doi.org/10.1073/pnas.1721434116
Hwang SY, Jung JS, Kim TH, Lim SJ, Oh ES, Kim JY, Ji KA, Joe EH, Cho KH, Han IO (2006) Ionizing radiation induces astrocyte gliosis through microglia activation. Neurobiol Dis 21(3):457–467. https://doi.org/10.1016/j.nbd.2005.08.006
Jaiswal S, Jamieson CH, Pang WW, Park CY, Chao MP, Majeti R, Traver D, van Rooijen N, Weissman IL (2009) CD47 is upregulated on circulating hematopoietic stem cells and leukemia cells to avoid phagocytosis. Cell 138(2):271–285. https://doi.org/10.1016/j.cell.2009.05.046
Jung SA, Aliberti J, Graemmel P, Sunshine M, Kreutzberg G, Sher A, Littman D (2000) Analysis of fractalkine receptor CX3CR1 function by targeted deletion and green fluorescent protein reporter gene insertion. Mol Cell Biol 20(11):4106–4114
Kloepper J, Riedemann L, Amoozgar Z, Seano G, Susek K, Yu V, Dalvie N, Amelung RL, Datta M, Song JW, Askoxylakis V, Taylor JW, Lu-Emerson C, Batista A, Kirkpatrick ND, Jung K, Snuderl M, Muzikansky A, Stubenrauch KG, Krieter O, Wakimoto H, Xu L, Munn LL, Duda DG, Fukumura D, Batchelor TT, Jain RK (2016) Ang-2/VEGF bispecific antibody reprograms macrophages and resident microglia to anti-tumor phenotype and prolongs glioblastoma survival. Proc Natl Acad Sci U S A 113(16):4476–4481. https://doi.org/10.1073/pnas.1525360113
Komohara Y, Ohnishi K, Kuratsu J, Takeya M (2008) Possible involvement of the M2 anti-inflammatory macrophage phenotype in growth of human gliomas. J Pathol 216(1):15–24. https://doi.org/10.1002/path.2370
Lepore F, D’Alessandro G, Antonangeli F, Santoro A, Esposito V, Limatola C, Trettel F (2018) CXCL16/CXCR6 axis drives microglia/macrophages phenotype in physiological conditions and plays a crucial role in glioma. Front Immunol 9:2750. https://doi.org/10.3389/fimmu.2018.02750
Lou N, Takano T, Pei Y, Xavier AL, Goldman SA, Nedergaard M (2016) Purinergic receptor P2RY12-dependent microglial closure of the injured blood-brain barrier. Proc Natl Acad Sci U S A 113(4):1074–1079. https://doi.org/10.1073/pnas.1520398113
Louis DN, Ohgaki H, Wiestler OD, Cavenee WK, Burger PC, Jouvet A, Scheithauer BW, Kleihues P (2007) The 2007 WHO classification of tumours of the central nervous system. Acta Neuropathol 114(2):97–109. https://doi.org/10.1007/s00401-007-0243-4
Maas SLN, Breakefield XO, Weaver AM (2017) Extracellular vesicles: unique intercellular delivery vehicles. Trends Cell Biol 27(3):172–188. https://doi.org/10.1016/j.tcb.2016.11.003
Madry C, Kyrargyri V, Arancibia-Carcamo IL, Jolivet R, Kohsaka S, Bryan RM, Attwell D (2018) Microglial ramification, surveillance, and interleukin-1beta release are regulated by the two-pore domain K(+) channel THIK-1. Neuron 97(2):299–312. e296. https://doi.org/10.1016/j.neuron.2017.12.002
Markovic DS, Vinnakota K, van Rooijen N, Kiwit J, Synowitz M, Glass R, Kettenmann H (2011) Minocycline reduces glioma expansion and invasion by attenuating microglial MT1-MMP expression. Brain Behav Immun 25(4):624–628. https://doi.org/10.1016/j.bbi.2011.01.015
Masuda T, Sankowski R, Staszewski O, Bottcher C, Amann L, Sagar SC, Nessler S, Kunz P, van Loo G, Coenen VA, Reinacher PC, Michel A, Sure U, Gold R, Grun D, Priller J, Stadelmann C, Prinz M (2019) Spatial and temporal heterogeneity of mouse and human microglia at single-cell resolution. Nature 566(7744):388–392. https://doi.org/10.1038/s41586-019-0924-x
Matias D, Dubois LG, Pontes B, Rosario L, Ferrer VP, Balca-Silva J, Fonseca ACC, Macharia LW, Romao L, TCLS ES, Chimelli L, Filho PN, Lopes MC, Abreu JG, Lima FRS, Moura-Neto V (2019) GBM-derived Wnt3a induces M2-like phenotype in microglial cells through Wnt/beta-catenin signaling. Mol Neurobiol 56(2):1517–1530. https://doi.org/10.1007/s12035-018-1150-5
Matsumoto J, Takata F, Machida T, Takahashi H, Soejima Y, Funakoshi M, Futagami K, Yamauchi A, Dohgu S, Kataoka Y (2014) Tumor necrosis factor-alpha-stimulated brain pericytes possess a unique cytokine and chemokine release profile and enhance microglial activation. Neurosci Lett 578:133–138. https://doi.org/10.1016/j.neulet.2014.06.052
Mattila S, Tuominen H, Koivukangas J, Stenback F (2009) The terminal prostaglandin synthases mPGES-1, mPGES-2, and cPGES are all overexpressed in human gliomas. Neuropathology 29(2):156–165. https://doi.org/10.1111/j.1440-1789.2008.00963.x
Mills CD, Kincaid K, Alt JM, Heilman MJ, Hill AM (2000) M-1/M-2 macrophages and the Th1/Th2 paradigm. J Immunol 164(12):6166–6173. https://doi.org/10.4049/jimmunol.164.12.6166
Monier A, Adle-Biassette H, Delezoide AL, Evrard P, Gressens P, Verney C (2007) Entry and distribution of microglial cells in human embryonic and fetal cerebral cortex. J Neuropathol Exp Neurol 66(5):372–382. https://doi.org/10.1097/nen.0b013e3180517b46
Nakano Y, Kuroda E, Kito T, Uematsu S, Akira S, Yokota A, Nishizawa S, Yamashita U (2008) Induction of prostaglandin E2 synthesis and microsomal prostaglandin E synthase-1 expression in murine microglia by glioma-derived soluble factors. Laboratory investigation. J Neurosurg 108(2):311–319. https://doi.org/10.3171/JNS/2008/108/2/0311
Nayak D, Roth TL, McGavern DB (2014) Microglia development and function. Annu Rev Immunol 32:367–402. https://doi.org/10.1146/annurev-immunol-032713-120240
Nikodemova M, Kimyon RS, De I, Small AL, Collier LS, Watters JJ (2015) Microglial numbers attain adult levels after undergoing a rapid decrease in cell number in the third postnatal week. J Neuroimmunol 278:280–288. https://doi.org/10.1016/j.jneuroim.2014.11.018
Nimmerjahn A, Kirchhoff F, Helmchen F (2005) Resting microglial cells are highly dynamic surveillants of brain parenchyma in vivo. Science 308(5726):1314–1318. https://doi.org/10.1126/science.1110647
Okada M, Saio M, Kito Y, Ohe N, Yano H, Yoshimura S, Iwama T, Takami T (2009) Tumor-associated macrophage/microglia infiltration in human gliomas is correlated with MCP-3, but not MCP-1. Int J Oncol 34(6):1621–1627. https://doi.org/10.3892/ijo_00000292
Penfield W (1925) Microglia and the process of phagocytosis in gliomas. Am J Pathol 1(1):77–90. 15
Prinz M, Jung S, Priller J (2019) Microglia biology: one century of evolving concepts. Cell 179(2):292–311. https://doi.org/10.1016/j.cell.2019.08.053
Prionisti I, Buhler LH, Walker PR, Jolivet RB (2019) Harnessing microglia and macrophages for the treatment of glioblastoma. Front Pharmacol 10:506. https://doi.org/10.3389/fphar.2019.00506
Pu P, Zhang Z, Kang C, Jiang R, Jia Z, Wang G, Jiang H (2009) Downregulation of Wnt2 and beta-catenin by siRNA suppresses malignant glioma cell growth. Cancer Gene Ther 16(4):351–361. https://doi.org/10.1038/cgt.2008.78
Qian J, Luo F, Yang J, Liu J, Liu R, Wang L, Wang C, Deng Y, Lu Z, Wang Y, Lu M, Wang JY, Chu Y (2018) TLR2 promotes glioma immune evasion by downregulating MHC class II molecules in microglia. Cancer Immunol Res 6(10):1220–1233. https://doi.org/10.1158/2326-6066.CIR-18-0020
Ransohoff RM (2016) A polarizing question: do M1 and M2 microglia exist? Nat Neurosci 19(8):987–991. https://doi.org/10.1038/nn.4338
Sena IFG, Paiva AE, Prazeres P, Azevedo PO, Lousado L, Bhutia SK, Salmina AB, Mintz A, Birbrair A (2018) Glioblastoma-activated pericytes support tumor growth via immunosuppression. Cancer Med 7(4):1232–1239. https://doi.org/10.1002/cam4.1375
Shono T, Tofilon PJ, Bruner JM, Owolabi O, Lang FF (2001) Cyclooxygenase-2 expression in human gliomas: prognostic significance and molecular correlations. Cancer Res 61(11):4375–4381
Sierra A, Encinas JM, Deudero JJ, Chancey JH, Enikolopov G, Overstreet-Wadiche LS, Tsirka SE, Maletic-Savatic M (2010) Microglia shape adult hippocampal neurogenesis through apoptosis-coupled phagocytosis. Cell Stem Cell 7(4):483–495. https://doi.org/10.1016/j.stem.2010.08.014
Stevens B, Allen NJ, Vazquez LE, Howell GR, Christopherson KS, Nouri N, Micheva KD, Mehalow AK, Huberman AD, Stafford B, Sher A, Litke AM, Lambris JD, Smith SJ, John SW, Barres BA (2007) The classical complement cascade mediates CNS synapse elimination. Cell 131(6):1164–1178. https://doi.org/10.1016/j.cell.2007.10.036
Svensson A, Ozen I, Genove G, Paul G, Bengzon J (2015) Endogenous brain pericytes are widely activated and contribute to mouse glioma microvasculature. PLoS One 10(4):e0123553. https://doi.org/10.1371/journal.pone.0123553
Tay TL, Mai D, Dautzenberg J, Fernandez-Klett F, Lin G, Sagar DM, Drougard A, Stempfl T, Ardura-Fabregat A, Staszewski O, Margineanu A, Sporbert A, Steinmetz LM, Pospisilik JA, Jung S, Priller J, Grun D, Ronneberger O, Prinz M (2017) A new fate mapping system reveals context-dependent random or clonal expansion of microglia. Nat Neurosci 20(6):793–803. https://doi.org/10.1038/nn.4547
Tay TL, Savage JC, Hui CW, Bisht K, Tremblay ME (2017) Microglia across the lifespan: from origin to function in brain development, plasticity and cognition. J Physiol 595(6):1929–1945. https://doi.org/10.1113/JP272134
Vinnakota K, Hu F, Ku MC, Georgieva PB, Szulzewsky F, Pohlmann A, Waiczies S, Waiczies H, Niendorf T, Lehnardt S, Hanisch UK, Synowitz M, Markovic D, Wolf SA, Glass R, Kettenmann H (2013) Toll-like receptor 2 mediates microglia/brain macrophage MT1-MMP expression and glioma expansion. Neuro-Oncology 15(11):1457–1468. https://doi.org/10.1093/neuonc/not115
Voronov E, Shouval DS, Krelin Y, Cagnano E, Benharroch D, Iwakura Y, Dinarello CA, Apte RN (2003) IL-1 is required for tumor invasiveness and angiogenesis. Proc Natl Acad Sci U S A 100(5):2645–2650. https://doi.org/10.1073/pnas.0437939100
Wallmann T, Zhang XM, Wallerius M, Bolin S, Joly AL, Sobocki C, Leiss L, Jiang Y, Bergh J, Holland EC, Enger PO, Andersson J, Swartling FJ, Miletic H, Uhrbom L, Harris RA, Rolny C (2018) Microglia induce PDGFRB expression in glioma cells to enhance their migratory capacity. iScience 9:71–83. https://doi.org/10.1016/j.isci.2018.10.011
Weinhard L, di Bartolomei G, Bolasco G, Machado P, Schieber NL, Neniskyte U, Exiga M, Vadisiute A, Raggioli A, Schertel A, Schwab Y, Gross CT (2018) Microglia remodel synapses by presynaptic trogocytosis and spine head filopodia induction. Nat Commun 9(1):1228. https://doi.org/10.1038/s41467-018-03566-5
Wes PD, Holtman IR, Boddeke EW, Moller T, Eggen BJ (2016) Next generation transcriptomics and genomics elucidate biological complexity of microglia in health and disease. Glia 64(2):197–213. https://doi.org/10.1002/glia.22866
Wiemer AJ, Hegde S, Gumperz JE, Huttenlocher A (2011) A live imaging cell motility screen identifies prostaglandin E2 as a T cell stop signal antagonist. J Immunol 187(7):3663–3670. https://doi.org/10.4049/jimmunol.1100103
Willingham SB, Volkmer JP, Gentles AJ, Sahoo D, Dalerba P, Mitra SS, Wang J, Contreras-Trujillo H, Martin R, Cohen JD, Lovelace P, Scheeren FA, Chao MP, Weiskopf K, Tang C, Volkmer AK, Naik TJ, Storm TA, Mosley AR, Edris B, Schmid SM, Sun CK, Chua MS, Murillo O, Rajendran P, Cha AC, Chin RK, Kim D, Adorno M, Raveh T, Tseng D, Jaiswal S, Enger PO, Steinberg GK, Li G, So SK, Majeti R, Harsh GR, van de Rijn M, Teng NN, Sunwoo JB, Alizadeh AA, Clarke MF, Weissman IL (2012) The CD47-signal regulatory protein alpha (SIRPa) interaction is a therapeutic target for human solid tumors. Proc Natl Acad Sci U S A 109(17):6662–6667. https://doi.org/10.1073/pnas.1121623109
Xue J, Schmidt SV, Sander J, Draffehn A, Krebs W, Quester I, De Nardo D, Gohel TD, Emde M, Schmidleithner L, Ganesan H, Nino-Castro A, Mallmann MR, Labzin L, Theis H, Kraut M, Beyer M, Latz E, Freeman TC, Ulas T, Schultze JL (2014) Transcriptome-based network analysis reveals a spectrum model of human macrophage activation. Immunity 40(2):274–288. https://doi.org/10.1016/j.immuni.2014.01.006
Ye XZ, Xu SL, Xin YH, Yu SC, Ping YF, Chen L, Xiao HL, Wang B, Yi L, Wang QL, Jiang XF, Yang L, Zhang P, Qian C, Cui YH, Zhang X, Bian XW (2012) Tumor-associated microglia/macrophages enhance the invasion of glioma stem-like cells via TGF-beta1 signaling pathway. J Immunol 189(1):444–453. https://doi.org/10.4049/jimmunol.1103248
Zhang J, Sarkar S, Cua R, Zhou Y, Hader W, Yong VW (2012) A dialog between glioma and microglia that promotes tumor invasiveness through the CCL2/CCR2/interleukin-6 axis. Carcinogenesis 33(2):312–319. https://doi.org/10.1093/carcin/bgr289
Zhang Y, Chen K, Sloan SA, Bennett ML, Scholze AR, O’Keeffe S, Phatnani HP, Guarnieri P, Caneda C, Ruderisch N, Deng S, Liddelow SA, Zhang C, Daneman R, Maniatis T, Barres BA, Wu JQ (2014) An RNA-sequencing transcriptome and splicing database of glia, neurons, and vascular cells of the cerebral cortex. J Neurosci 34(36):11929–11947. https://doi.org/10.1523/JNEUROSCI.1860-14.2014
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2020 The Editor(s) (if applicable) and The Author(s), under exclusive license to Springer Nature Switzerland AG
About this chapter
Cite this chapter
Cole, A.P. et al. (2020). Microglia in the Brain Tumor Microenvironment. In: Birbrair, A. (eds) Tumor Microenvironment. Advances in Experimental Medicine and Biology, vol 1273. Springer, Cham. https://doi.org/10.1007/978-3-030-49270-0_11
Download citation
DOI: https://doi.org/10.1007/978-3-030-49270-0_11
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-030-49269-4
Online ISBN: 978-3-030-49270-0
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)