Abstract
The cell culture techniques are in the base of any biology-based science. The standard techniques are commonly static platforms as Petri dishes, tissue culture well plates, T-flasks, or well plates designed for spheroids formation. These systems faced a paradigm change from 2D to 3D over the current decade driven by the tissue engineering (TE) field. However, 3D static culture approaches usually suffer from several issues as poor homogenization of the formed tissues and development of a necrotic center which limits the size of in vitro tissues to hundreds of micrometers. Furthermore, for complex tissues as osteochondral (OC), more than recovering a 3D environment, an interface needs to be replicated. Although 3D cell culture is already the reality adopted by a newborn market, a technological revolution on cell culture devices needs a further step from static to dynamic already considering 3D interfaces with dramatic importance for broad fields such as biomedical, TE, and drug development. In this book chapter, we revised the existing approaches for dynamic 3D cell culture, focusing on bioreactors and microfluidic systems, and the future directions and challenges to be faced were discussed. Basic principles, advantages, and challenges of each technology were described. The reported systems for OC 3D TE were focused herein.
Access provided by CONRICYT-eBooks. Download chapter PDF
Similar content being viewed by others
Keywords
1 Introduction
Tissue engineering (TE) technologies are based on the biological triad of cells, signaling molecular pathways and ECM. Although TE leads a transition from 2D to 3D cell culture techniques in order to achieve more physiologically relevant tissue substitutes and models, culture techniques are still limited. Typically, current 3D cell culture techniques do not yet allow meeting the multicellular complexity of tissues, do not offer fine control over gradients, and require medium exchange at discrete time points instead of in a continuous manner because they rely on static environments [1]. Additionally, bioreactors and microfluidic devices, as a dynamic stimulus element, may be used as an alternative to or in conjunction with molecular growth factors for the signaling part of the TE triad. A TE bioreactor can be defined as a device to perform maturation of cell-material constructs under a controlled environment, using or not mechanical means to direct biological processes . This generally means that bioreactors are used not only to flow cell culture medium but also to stimulate cells and induce them to produce ECM [2]. Microfluidic devices, as an alternative, were born from the combination of bioreactor principles and microfabrication techniques to reduce either time or costs of cell culture process and diagnostic systems.
The available culture systems , including bioreactors, allow monocultures in 3D scaffolds but are not adapted for co-cultures, which currently is a big challenge of the field [3]. The classic case of the OC interface, which consists of a hyaline cartilage layer and an integrated subchondral bone, is a good example of an interface requiring for more complex scaffold design and a dual environment when cultured in vitro. Interfaced bone-cartilage in vitro models keep being predominantly limited to cell co-culture systems in which bone and cartilage cells are both exposed to the same medium, perhaps a very distant condition from the in vivo environment [4]. Regarding this, when co-culturing stem cells in 3D scaffolds, researchers either need to use costly pre-differentiation operations before cell seeding and keep its phenotype over cell culture or, as a more challenging alternative, simultaneously modulate differentiation down to distinct lineages in a unified culture environment [5]. So, using conventional bioreactor systems based on one single culture chamber, supplementing the culture media with lineage-specific signaling molecules for directed differentiation of stem cells is invalid for biphasic constructs . This limitation has been addressed by using custom made dual-chamber culture systems to spatially direct delivery preventing dominance of one phenotype over the other throughout the construct [5, 6].
Microfluidics , as an alternative to bioreactors at the microscale , allows spatial control over fluids in micrometer-sized channels and has become a valuable tool to further increase the physiological relevance of 3D cell culture by enabling controlled co-cultures, perfusion, and spatial control of signaling gradients [7, 8].
Over the next sections of this chapter, we discuss the current bioreactor and microfluidic systems, the current issues and advantages of using a dynamic cell culture instead of a static one, and the features to be considered when designing the devices for dynamic 3D cell culture approaches. The reported bioreactor and microfluidic studies for OC tissue regeneration and in vitro modeling are overviewed and discussed.
2 Dynamic Systems Designs
Bioreactor and microfluidic systems are cell culture environments confined in a reservoir with a shape of a vessel, flask, or even channels , connected to inlets and outlets for continuous flowing of nutrients through the cell culture. A bioreactor can be described as a dynamic device or system for culturing cells or tissues in suspension, 2D or 3D, under controlled biochemical or mechanical conditions. Microfluidic technique was created as an option for the perfusion of cell cultures, since the compartmentalized nature of microfluidic devices interconnected by microchannels allows perfusing media adjacent to or through a population of cells or 3D tissue-like construct .
In general, bioreactors and microfluidic systems are designed to perform at least one of the following five functions:
-
1.
To achieve uniform cell distribution
-
2.
To keep constant and optimized concentration of gasses and nutrients
-
3.
To perform mass transport to the tissue
-
4.
To increase tissue maturation by applying physical stimuli
-
5.
To provide information about the formation of 3D tissue by attaching sensors and designing transparent chambers [9]
A bioreactor or microfluidic device incorporating a flow pump to continuously circulate culture medium is the minimum criteria to define as dynamic a cell culture technique. The pump or motor must be small enough to fit into an incubator and also be usable at 37°C and in a humid environment. The forces needed for cellular stimulation are very small, so it is important to ensure that the pump/motor has the capability to apply small forces accurately. Tissue culture is a continuous, non-steady-state process in which the cultivation and tissue-specific parameters change with time. Furthermore, the scaffold and chamber shapes are of significant importance for controlling the nutrition flow pattern [10].
2.1 Mass Transport : Diffusion and Convection
Static culture systems rely primarily on diffusion, and to a lesser extent natural convection, for transport of oxygen to cells. The depth of media in the static conditions limits the supply of oxygen from the gas phase, which is not a big issue when culturing a monolayer of cells [11]. However, in a 3D cell culture approach, improving local perfusion of thick tissue constructs remains a significant challenge for 3D-based devices. Static culture of cell-seeded 3D scaffolds typically results into localized tissue growth in the construct periphery because of lack on mass transport of fresh nutrients through the tissue [12]. Mass transport through the scaffolds can be improved using perfusion methodologies by housing the construct within a flow-through column [13, 14] or by suspending cell spheroids or constructs within rotary culture devices or spinner flasks, generating a dynamic culture [15, 16].
The important role of mass transport in a cell culture device is to keep cell metabolism within a physiological range by providing metabolic substrates and removing toxic degradation products. Understanding how device geometry is related to convective or diffusive transport limitations is therefore a key element of the bioreactor and microfluidic systems design.
The rate of diffusion is proportional to the metabolite concentration gradient, being the constant of proportionality and the diffusion coefficient:
The Stokes-Einstein equation relates the radius of the diffusing particle and temperature to the diffusion coefficient, where k is Boltzmann’s constant, T is temperature, and R is the particle radius. The volume of a sphere is proportional to the cube of its radius, V = 4/3πr 3, so the diffusion coefficient is approximately inversely related to the cube root of molecular weight.
The mass flux is also related to the gradient that can be generated at the interface between cells and medium, according to Fick’s first law of diffusion:
Fick’s equation relates the diffusive flux “J” to the concentration when assuming a steady state (if a system is in a steady state, then the recently observed behavior of the system will continue into the future). The diffusion flux dimension is amount of substance per unit area per unit time, so it is expressed in mol m−2 s−1 and quantifies the amount of substance that will flow through a unit area during a time interval. D is the diffusion coefficient, and its dimension is area per unit time, so standard units would be m2/s. φ is the concentration in ideal mixtures, of which the dimension is amount of substance per unit volume as mol/m3. x is the position, the dimension of which is length; it might thus be expressed in the unit m.
2.2 Flow Conditions for Dynamic Cell Cultures
Diffusion is the only driving force to move nutrients and waste in a static culture system. As the size of the scaffold increases, diffusion of nutrients and waste removal to and from the interior of the construct becomes more difficult, leading to necrosis at the core of the scaffold [16]. Defects requiring TE solutions are typically many millimeters in size for which, in static cell culture systems, it can be quite difficult to enable sufficient fresh medium circulation through the engineering construct [11]. Scaffolds in such a size range are easily fabricated. However, problems arise when culturing cells on these scaffolds. The main challenge in preparing constructs larger than few millimeters is to obtain a homogeneous distribution of cells, and hence new tissue, throughout the whole 3D scaffold volume [17]. This problem is increased by the static culture conditions, which result in scaffolds with few cells in the center of the construct. It has been shown that despite uniform cell seeding, over cell culture period, more cells distribute predominantly on the periphery of the constructs [18]. The main reasons for this distribution in scaffolds at millimeter scale or more are cell sedimentation, necrosis, as a consequence of the previous ones, and cell chemotaxis. For instance, mineralized bone matrix reaches a maximum penetration depth of 240 μm when stromal osteoblasts are cultures onto poly(dl-lactic-co-glycolic acid) scaffolds, which is far thinner than an ideal bone graft needed for the clinic [19].
Perfusion flow performed by bioreactors and microfluidic devices provides several benefits such as stable nutrient supply, waste metabolites washed away, and control of oxygen tension distribution. Furthermore, perfusion is one of the key stimuli in vasculature, as it provides shear stress, which affects the cellular morphology and gene expression [20, 21]. So, constant nutrition, oxygen flow supply and metabolic product elimination must be performed when culturing cells up to higher density which is one of the most important tasks to achieve physiologically meaningful functions for TE and sufficient cell number for in vitro construct development [22].
While the first generation of bioreactors for culturing cells was designed simply to pump nutrient through the assembling tissue followed by waste removal [17], the next wave of bioreactors was designed for maturing tissues such as blood vessels [23], cartilage [12], or cardiac muscle [24], subjecting the emerging tissue to mechanical compression, shear stresses, and even culture medium pulsatile flow. Such stresses lead to improved mechanical properties of engineered tissues such as cartilage [25].
2.3 Flow Shear Stress and Related Stimuli
Flow-derived shear stress provides a physiologically relevant mechanical stimulation that significantly promotes specific protein expression and elicits paracrine effects by increasing the probability of randomly happen secretion and protein-protein and cell-cell contact [26]. These events are particularly relevant when culturing complex tissues as interfaces requiring co-cultures. Given the central role of several protein pathways in specific disorders, these stimuli represent a significant dynamic, for example, for an in vitro model of a disorder condition as OA.
Mechanical cues are also crucial for tissue specification and maturation, which can be transduced by the bioreactor chamber design [10] or microfluidic channel geometry, as suggested by a study of the effect of shear stress on mature osteoblasts. Kou et al. [27] developed a device capable of applying four different magnitudes of shear stress in parallel channels on one chip. The intracellular calcium intensity peak was proportional to intensity of shear stress, while response time was independent of shear stress for values larger than 0.03 Pa.
While flow rate can be used to modulate media exchange [28], pore size, interconnectivity, and anisotropy can influence different rates of media exchange and shear stress on cells distributed within the construct [29]. Mechanobiological aspects, such as active stretch and tension, are another functional feature that can be added using microfabrication techniques. Although interesting, it has received minor attention in combination with 3D cell culture. Regarding this challenge, sophisticated devices for 3D cell culture are one of the main needs for the current regenerative medicine and TE evolution [30].
3 Bioreactor Designs
3.1 Bioreactor General Principles
Bioreactors arise as a proposed solution when addressing the reported issues afore. Although the requirements for bioreactor design are application specific, there are a few general principles which have to be considered when developing a bioreactor. Biocompatible and bioinert materials must be selected to fabricate a bioreactor. Although stainless steel can be used if it is treated avoiding chromium ions leaching out into the culture medium, most metals are eliminated by this permit. Furthermore, a bioreactor operates at 37°C in a humid atmosphere, so selected materials cannot change drastically under these conditions, which avoids the use of some plastics. If a material changes volume under this humid condition, it can trigger medium leakage, which can be a problem in any design involving fluids. In most cases, fluid seals are necessary, and a good design should be considered to minimize the number of junctions needing for seals. Gharravi et al. designed a tissue chamber made of stainless steel presenting multiple pores and two inlets and outlets for the media and the gases (O2 and CO2) to replicate the perfusion process and oxygen tension in the body. The inside geometry of the central part of culture chamber was designed to mimic ball and socket of the temporomandibular joint for cartilage TE with round shape and as a tissue sized at a large dimension. Alginate was selected for the chondrocytes encapsulation in a sheet configuration [31].
A bioreactor has to operate under aseptic conditions to prevent any contamination of microorganisms. To guarantee the aseptic environment, bioreactor parts can be either sterilized by autoclaving or disinfected by submersion in alcohol or under a sterilizing gas (e.g., ethylene oxide), limiting the range of materials considered for a bioreactor fabrication. Autoclave runs cycles of a severe protocol performing high temperature and pressure, restricting even more the number of materials that can be selected for the bioreactor manufacturing. Alternatively, some non-stabilizable disposable bioreactor parts may be used and replaced after each use. Considering transparent materials for the culture chambers is advantageous for monitoring the construct during culture. For instance, Powers et al. have presented a bioreactor that enables both morphogenesis of 3D constructs under flow perfusion while allowing in situ observation by light microscopy, which is an important feature to take into account when designing a cell culture device [32].
Sensors should be incorporated into the design if parameters such as pH, nutrient (e.g., glucose) concentration, or oxygen levels are to be monitored. However, at the moment, it is not easy to measure all of these variables in “real time,” and the existing microsensors are too expensive. Therefore, there is a requirement to develop sensors for “real-time” measurement or alternatively to remove samples for as close as possible a “real-time” analysis. Dissolved oxygen and culture medium pH have been monitored with fluorescent sensors developed to study the metabolic state of cells in culture without removing or damaging cells during cultivation [33].
As a market approach perspective, a prototype bioreactor has to be designed thinking about the scale-up opportunity. This means designing a device that is easy to enlarge without changing its characteristics or projecting a simple and user-friendly device easy to multiply in number. Moreover, thinking about an industrial application, a high-throughput system is the ideal strategy so that numerous scaffolds can be cultured at one time, which currently is not considered in most of the bioreactor systems reported. A bidirectional perfusion bioreactor was developed enabling implementing perfusion flow and flow direction which can be varied along the culturing period. For large-scale applications, the most important feature that this system comprises is its compact and user-friendly design made of autoclavable materials and enabling to culture up to 20 samples simultaneously [34].
A bioreactor can also be designed not to expand cells in number but to obtain de novo tissue with biomechanical properties comparable to the native one, by applying various mechanical or electromagnetic stimuli. Suckosky et al. [35] performed a characterization of the flow field within a spinner flask system working under optimized conditions to produce cartilage. The simulation and experimental collected data have shown that subjecting a scaffold to a dynamic flow provided a uniform cell distribution throughout the 3D construct resulting in a homogenous matrix deposition, whereas Altman et al. [36] have reported that directional strain applied on silicone-based constructs promoted cell differentiation into a ligament-like phenotype instead of bone or cartilage lineages. Electric [37] and magnetic [38] stimuli have also been used experimentally with encouraging results on stimulation of 3D muscle maturation and osteogenesis, respectively.
The new generation of bioreactors should also be able to support the culture of two or more cell types simultaneously, relevant for the regeneration of interfaced tissues. This currently involves first maintaining the different cell types under different static culture conditions to obtain the desired phenotypes and then at appropriate time, switching to a common cultivation protocol in one bioreactor. The formed tissue either presents a lose interface or fused phenotype. The appropriate design should consider chamber compartments (named dual chambers) interfaced by 3D scaffolds [39, 40]. This way the cell adhesion, proliferation, and differentiation phases can be promoted in a whole construct immersed in different environments over all culture time.
3.2 Bioreactor Types
The basic principle applied at the first generation of bioreactors for TE was the agitation-based approach. According to this approach, a cell suspension is placed into a container while keeping the suspension in motion. Gentle stirring is used to provide motion to cells. Due to this, cells do not adhere to the walls and form cell-to-cell interactions. Based on this principle, several bioreactor designs were created, which are summarized in Fig. 18.1.
3.2.1 Spinner Flask Bioreactors
Spinner flasks consist of a container and a stirring element to continuously stir the cell suspension (Fig. 18.1B). These flasks are traditionally used to form cell spheroids but can also be applied to constructs attached to needles from the top cover. The size of the cell spheroids or constructs depends on the volume of the container. Culture medium agitation is performed using a magnetic stir bar placed at the bottom of the flask [41] promoting the nutrients diffusion and removal of waste products keeping the cells fed with fresh culture medium [42].
The main issues associated to the spinner flask bioreactors are related to the shear force of the stirring bar, requiring a larger amount of culture medium and resulting in inconsistency of size of the formed cell spheroids [43]. However, constructs cultured in spinner flasks have a higher cell seeding density and more uniform distribution of cells when compared to a static culture model [44].
The spinner flask bioreactor has been tested to promote osteogenesis. Sikavitsas et al. [45] compared steady flask, spinner flask, and rotating vessel (described below) systems by culturing rat mesenchymal stem cells (MSCs) in 3D scaffolds for a period of 21 days. The author observed that the highest alkaline phosphatase activity and osteocalcin secretion were obtained using the spinner flask system. Moreover, constructs cultured in the agitated systems had higher proliferation rate and calcium content than the steady flask system.
3.2.2 Rotating Cell Culture Bioreactors
The rotating bioreactor spins the whole container instead of using a stirrer bar/rod as in the case of the spinner flask bioreactor (Fig. 18.1C). The culture chamber is initially rotated at low speed which is increased when cells start forming large aggregates to maintain the spheroids in suspension. This concept was developed at NASA to simulate microgravity conditions. The systems design consists of two concentric cylindrical containers, within which lies an annular space containing the scaffold [46]. The outside wall rotates, and to obtain a microgravity condition, the gravitational forces must balance the centrifugal forces, subjecting the scaffold to dynamic laminar flow [47]. The main advantage of this system is the reduced shear force applied [48]. Using this approach, Marlovits et al. [49] suspended differentiated chondrocytes in a rotating wall vessel. After 90 days of cultivation under microgravity, cartilage-like neotissue was formed, encapsulated by fibrous tissue that closely resembled the perichondrium, without the use of any scaffolding material.
Saini et al. [50] have also shown the potential of this technique in cartilage TE, but, using porous polylactic acid scaffolds, seeded dynamically in the bioreactor using bovine chondrocytes. Four weeks after cell seeding, constructs from condition seeded at the highest cell densities contained up to 15 M cells, 2 mg glycosaminoglycan, and 3.5 mg collagen per construct and exhibited morphology similar to that of native cartilage. Overall the rotating wall vessel bioreactor has been shown to optimize nutrient transport and promote cartilage growth and differentiation [51].
While this system is simple, allowing easy handling and large-scale and long-term production of spheroids, there is large variability in the size of the spheroids as observed in the spinner flask bioreactors [52].
3.2.3 Flow Perfusion Bioreactors
Flow perfusion bioreactors utilize a pump to percolate medium continuously through the scaffold’s interconnected pores (Fig. 18.1D). A molecular weight cutoff membrane isolates the chamber inlet and outlet avoiding cells from leaving the container. The enhanced nutrient transfer has been shown to result in improved mass transfer [41], contributing for a homogeneous cell distribution and high seeding efficiency throughout the thickness of the scaffold [53]. Furthermore, the fluid shear forces resulting from flow perfusion have been shown to enhance the expression of the osteoblastic phenotype [54]. Gomes et al. [55] cultured bone marrow MSCs under static and perfusion conditions. A superficial layer of cells was formed when the constructs were cultured statically, while a homogeneous cell distribution filled the scaffolds in the perfusion bioreactor. Although the proliferation rate and alkaline phosphatase activity patterns were similar for both conditions, the constructs cultured under perfused conditions showed a significant increase in calcium deposition.
Goldstein et al. [16] compared the three systems described above: rotating wall vessel, spinner flask, and flow perfusion. Osteoblastic cells were seeded onto PLGA foams and cultured for 2 weeks. Although cell seeding efficiencies and osteocalcin content were similar for the three systems, the spinner flask produced the least uniform cell distribution throughout the foams and the rotating wall vessel system resulted in the lowest levels of alkaline phosphatase activity. Consequently, the flow perfusion system appears to be the most attractive culturing system for bone constructs among those three bioreactors. Moreover, rotary perfusion bioreactor system has the main advantage of eliminating the internal transport limitations of the spinner flask and the rotating wall vessel [41].
3.2.4 Compression Bioreactors
Compression bioreactors are designed to exert controllable mechanical forces under physiological environment to reproduce, in vitro, the in vivo mechanical stimuli (Fig. 18.1E). Hydrodynamic shear, hydrostatic pressure, mechanical compression, tension, and friction are some of the mechanical forces applied by this class of bioreactors. One of the main applications of these systems is in cartilage engineering [56]. Correia et al. [57] tested the effect of either a pulsatile or a steady hydrostatic pressure to human adipose-derived stem cells (ASCs) encapsulated in gellan gum hydrogel constructs over a period of 3 weeks. The authors observed that pulsatile hydrostatic pressure regimen led to greater chondrogenic differentiation and matrix deposition, as evidenced by gene expression of aggrecan, collagen type II, and sox-9, metachromatic staining of cartilage extracellular matrix, and immunolocalization of collagens.
Cochis et al. [58] used a bioreactor to mechanically stimulate a hydrogel laden with bone marrow MSCs by simultaneously applying compression and shear forces days using a ceramic hip ball over 21 days. The mechanically stimulated MSCs successfully expressed chondrogenic genes, and the GAG quantification confirmed the higher differentiation of MSCs under compression stimulus. Histological analysis showed the retention of the cells within the polyurethane scaffold pores and the presence of a surrounding matrix of collagen and proteoglycan.
The compression bioreactors have as main advantage the ability to apply very specific and accurate mechanical stimuli which are not possible to promote with any other culture system. On the other side, the specificity of this approach makes these systems not so interesting for large-scale or high-throughput applications.
3.2.5 In Vivo Bioreactors
The in vivo bioreactor is a regenerative medicine concept where the bone is grown in vivo (Fig. 18.1F). This bioengineering approach relies on the conductive properties of the implanted scaffold to recruit MSCs from neighboring tissue and takes advantage of the physiological environment to supply the necessary growth factors and nutrients to the construct. Several studies have been made to take advantage from in vivo bioreactors to generate vascularized bone tissue [59, 60].
In the design of an in vivo bioreactor, Holt et al. [59] used a scaffold composed of coralline cylinders supplemented with BMP-2. To recruit MSCs from the blood circulation into the bioreactor by BMP-2, a vascular pedicle channel was incorporated into the scaffold. This closed system isolated by silicone ensured that bone formation would depend on the scaffold and the invading cells. The designed in vivo bioreactor implanted in male rats was harvested after 6 weeks. New bone formation was observed at 11.3% with neovascular ingrowth. In a different approach, Stevens et al. [60] manipulated an artificial space to perform as a bioreactor between the tibia and the periosteum, a layer rich in MSCs, and taking advantage from the body’s healing mechanism to leverage neo-bone formation. The authors incorporated alginate gel in New Zealand white rabbits. Bone tissue was formed and showed biomechanical similarities to the native bone. Furthermore, the authors observed enhanced cartilage formation within the bioreactor when angiogenesis was inhibited promoting a more hypoxic environment.
4 Microfluidics Designs
Microfluidic devices experienced a fast evolution starting in the 1990s [61] and nowadays contribute with versatile platforms in fields as molecular analysis, laboratory diagnostics, biodefense, and consumer electronics [62]. Applications of microfluidic systems based on cell and tissue culture have been also emerging, and TE is taking advantage from micro- and nanofabrication techniques for the development of sophisticated features on tissue modeling and drug testing as platforms for high-throughput screening [22]. First at two dimensions, but during last 10 years, the third dimension of cell culture has been also revolutionized by the integration of microfluidics. When several integrated chambers culture cells mimicking more than one tissue or organ in a single device, the approach became known as organ-on-a-chip [8].
4.1 Microfluidic Systems General Principles
Microfluidic systems typically consist of devices with channel geometries having characteristic length scaled from tens to hundreds of microns [63]. When microfluidics are designed for cell culture, it might encompass from millions to single cells providing a level of flexibility beyond that possible in conventional well plates or even with bioreactors [64, 65]. Structural features in microfluidic devices may be designed to provide spatial control over cell behavior, and interactions between cell populations may be controlled through the use of channels, membranes, and other features incorporated into these systems [66, 67].
Fabrication is typically done by photolithography by applying a standard technique as Radio Corporation of America (RCA) cleaning, thin film deposition, wet hydrofluoric etching, access hole forming, or chip bonding (Fig. 18.4) [61]. Soft lithography and other processing techniques have enabled rapid, simple fabrication of microfluidic devices from a broad range of substrate materials including thermoplastics and thermoset polymers, typically produced in optically transparent formats that may be rigid or elastomeric [68]. Some significant features which make this technology distinguishable are:
-
1.
Microscale resolution and flow conditions match with the cellular structure dimensions and traffic present in the human organism.
-
2.
Spatial control over chemical gradients can mimic the dynamic 3D network existing in vivo.
-
3.
Reduced costs as it requires samples in nanoliter volumes.
-
4.
Design of microfluidic devices is compatible with substrates permeable to oxygen enabling cell culture in 3D.
-
5.
Microfluidics can handle several processes at one time such as culture, replenishment of medium , cell detachment, and subsequent detection. Furthermore, fabrication can use transparent materials allowing microscopic imaging.
4.2 Microfluidic Types of Devices
Different types of microfluidic systems have been used to establish and support 3D culture and have been categorized based on the substrates used to fabricate the microdevices, namely, glass-/silicon-based, polymer-based, and paper-based platforms [22].
4.2.1 Glass-/Silicon-Based Platforms
Glass-based systems can be reusable and applied for long-term studies because of its stable surface with reproducible and reliable electroosmotic flow. The main advantage of this systems is the enhanced optical properties which are advantageous in high-resolution microscopy [69]. Glass-based channels are impermeable to oxygen, which has been repeatedly utilized to create hypoxic conditions [70]. Khan et al. designed a microfluidic platform able to create gradients of oxygen tension. A glass coating on the inner microfluidic channel prevented multi-directional diffusion of oxygen across Polydimethylsiloxane (PDMS) enabling and keeping the gradient resolution and stability which is monitored by incorporation of sensors [71]. Silicon-based systems, on the contrary, have the disadvantage of being expensive and demand complicated fabrication procedures.
4.2.2 Polymer-Based Platforms
Various polymers such as PDMS, polycarbonate, polystyrene, and polymethyl methacrylate (PMMA) have been used as biocompatible substrates for microdevices [22]. Among these polymers, PDMS is the most predominant because it is permeable to oxygen and cost-effective [61]. Microchannels are formed by contacting the PDMS structure with a substrate, and these channels deliver the fluid to restricted areas on the substrate. The microchannels can selectively deliver the materials for cell adhesion or cell suspension to desired areas of a substrate [72, 73].
Natural origin polymers such as agarose, fibrin, and collagens have also been used for 3D cell culture on microfluidic applications [74].
4.2.3 Paper-Based Platforms
Paper-based microfluidic systems were born as a relatively simple and cost-effective approach. Moreover, these systems are flexible and can be designed in varied architectures, as demonstrated by Martinez et al. by creating several 3D microfluidic devices fabricated in layered paper and tape [75]. 3D cell culture was recently demonstrated by Derda et al. for the first time on a paper-based microfluidic platform [76]. The authors used chromatographic papers to pattern hydrophobic barriers by wax printing. Cell suspensions were then impregnated on the papers. To mimic the 3D architecture, multiple papers sheets were stacked over each other. These papers can later be detached for layer-by-layer molecular analysis.
4.3 Microfluidic Potential for 3D Cell Culture
One of the main advantages of microfluidic approaches is the spatial fine control over fluids at micrometer scale, which can be explored to increase the physiological significance of 3D tissue models . Early examples demonstrate spatial patterning of adhesion molecules [77] and hydrogels [78, 79], which are still used in microfluidic 3D cell culture. Today, the most important drivers for the use of microfluidic techniques in 3D cell culture are:
-
(i)
The integration of perfusion/flow
-
(ii)
The ability of co-culturing cells in a spatially controlled manner
-
(iii)
Generation of and control over (signaling) gradients [1]
Spatial control is essential for the increasing need for more complex tissues in vitro modeling, since our body presents several interfaced tissues and barriers. These are, for example, determinant for testing drug efficacy as drug molecules either have to cross barriers or be effective to treat a tissue without affecting the adjacent one. Microfluidic fabrication allows patterning surfaces for cells and extracellular microenvironment stratified (co-)cultures with basal-apical access, controlling gradient formation and medium perfusion. In classical culture techniques, the spatial control is usually achieved by a membrane to support surface-attached cell growth dividing the culture well in two independent compartments [80]. The recent trend in microfluidic systems is to use hydrogels interfaced by two channels offering a physiologically more relevant environment. By using laminar flow, two or more streams are joined into a single channel flowing parallel to each other without any turbulent mixing, allowing the only mixing by diffusion across the interface. This ability to sustain parallel streams of different solutions in a single microchannel has been applied to pattern cells and their environments [81, 82]. This method can also be used to study subcellular processes by positioning a single cell interfacing two adjacent streams [83]. Furthermore, by patterning a hydrogel between two fluids, stable and predictable linear gradients are formed, which can be controlled by the channel geometry and applied flow rates [84]. To integrate this type of assays into the high-throughput drug-screening pipeline, Trietsch et al. [85] created a microfluidic platform based on a 96-well titer plate format enabling a double flow perfusion to generate a gradient over an hydrogel. Perfusion flow was maintained by passive leveling between two reservoirs, thereby eliminating the need for external pumps. This allows high-throughput migration assays and gradient formation in combination with stratified co-cultures.
An interesting technology to study chondrocytes was introduced by Neve et al. [86]. The developed technique integrates micron-resolution particle image velocimetry with dual optical tweezers that allow for the capture and maintenance of a single chondrocyte in a flow field that can be measured in real time.
From the microfluidic devices was born the organ-on-a-chip concept, which is based on a microfluidic cell culture device created with microchip manufacturing methods that contains continuously perfused chambers inhabited by living cells arranged to simulate tissue- and organ-level physiology. By recapitulating the multicellular architectures, tissue-tissue interfaces, physicochemical microenvironments, and vascular perfusion of the body, these devices could produce levels of tissue and organ functionality not possible with conventional static 2D or 3D culture systems. This concept was born for the creation of tools to enable in vitro analysis of biochemical and metabolic paracrine activities in between different tissues and can have a huge impact in the future after maturation and optimization of the concept (Fig. 18.2).
Microfluidic devices designed over several substrates and for broad applications. (A) Crossed microfluidic channels creating interfaces in layered paper-tape-based device. (Adapted with permission from [75] Copyright © 2008 National Academy of Sciences). (B) Microfluidic concept of parallel channels separated by laminar flow from multiple input that are optically clear on each face, chemically inert, reusable, and inexpensive and can be fabricated on the benchtop in approximately 1 h. (Adapted with permission from [87] Copyright © 2009 Courson, Rock). (C) Microfluidic device compartmentalized for 3D cell aggregates analysis at high-throughput scale. (Adapted with permission from [88] Copyright © 2017, Rights Managed by Nature Publishing Group). (D) Perfusable vascular network interfacing two microchannels creating an organ-on-a-chip system. (Adapted with permission from [89] Copyright © 2015, Royal Society of Chemistry)
In addition to the physiological relevance , microfluidic systems can potentially improve reproducibility, cost-effectiveness, and implementation at larger scales for diagnostics and drug screening. For example, the reduced dimensions offer advantages such as reduced consumption of expensive cell material, hydrogels, and screening reagents. Well-defined heights of microfluidic channels improve imaging quality and speed. Precise metering of liquids with microfluidic techniques enables better quantification of assays. However, moving to a microfluidic reality implies changing several exclusive factors to microfluidic from macroscopic cell culture, such as different culture surfaces, reduced media volumes, and vastly different rates of, and methods for, medium exchange. These unique features slowdown the acceptance and adaptation of the current state-of-the-art of cell culture techniques to the dynamic microscale. Furthermore, even though there are reports about 3D cell culture in microfluidic devices, a further push is needed to consolidate this interesting concept for more complex 3D tissues as interfaces and co-culture-based studies.
5 Bioreactors vs Microfluidics in OC Tissue Modeling
Over the last decades, strategies to investigate bone-cartilage interactions in vitro were mostly limited to cell co-culture well plates in which bone and cartilage cells are both exposed to the same medium [4], arguably a very distant condition from the in vivo environment . Alternatively, co-cultures imply the use of transwells avoiding direct cell contact which is also crucial, for example, for interfaced tissues. Using TE techniques, two construct pieces can be independently cultured under chondrogenic and osteogenic medium and joined together after tissue maturation, resulting in an interrupted interface.
Traditional bioreactors have not been frequently explored in the development of skeletal tissues interfaces but either applied to bone or cartilage tissue development [90]. When applied to the interfaced OC junction, explants were usually used. Understanding the mechanical properties of the articular surface is the main focus of interest, because the OC junction and the subchondral bone are known to confer significant protective mechanical properties to the overlying cartilage [91]. Specifically, the subchondral bone reduces impact-induced fissuring, chondrocyte cell death, and matrix degradation, all of which are hallmarks of pre-osteoarthritis [92]. Studies of chronic joint disorders have revealed the influence of subchondral bone changes in the etiology of osteoarthritis, but these changes have not been effectively reproduced in vitro [93, 94].
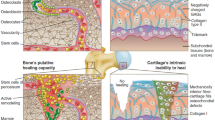
Biological characterization of the OC tissue present in any joint of the human body already revealed the existing and key communication between chondrocytes and osteoblasts across the junction. This interface is characterized by a transition of collagen type I to type II and also of collagen fibers orientation. Moreover, several gradients, such as cellularity, cell size, proteoglycans, and collagen content, characterize the OC tissue interface (Fig. 18.3). However, understanding OC phenotype and related disorders through specific communications require an in vitro culture system that supports native or engineered osseous and chondral components of an OC unit.
Subchondral bone and articular cartilage interface make the OC tissue which is characterized by specific collagen orientation and several content gradients. (A) Histological H&E section of healthy human OC tissue. (B) Representation of the organization of collagen and cells. (C) Scheme of collagen orientation. (D) Scheme of cellular distribution. (E) Representation of gradients and collagen orientation
Bioreactors and microfluidic systems, as mentioned in previous sections, are capable of creating gradients which are of great interest to OC tissue in vitro development. While conventional in vitro culture systems such as static cultures, spinner flasks, rotating wall vessels, and flow perfusion fail to provide physiological conditions capable of reproducing physiological interfaces, the use of in vivo models can give the wrong impression of translation readiness. Indeed, most of the cases fail when translated to clinical trials, mainly because of genotypic and morphological differences . Regarding this, in vitro models, able of mimicking 3D interfaces by using gradient or bilayer scaffolds in general and OC tissue in particular, based on human cells are still urgently needed. Since the traditional culturing systems are not specifically adapted for engineering 3D interfaced tissues, new technologies have been emerging over the last 5 years targeting this gap [5, 40, 95].
Recent developments in the bioreactor field, as the creation of systems adapted for the maturation of interfaces and able to spatially control gradients, will open up new possibilities to foster interfaced TE as it is the case of the OC tissue unit. We described a new bioreactor concept [39, 40], which was designed for the maturation of interfaces by using multi-compartmentalized chambers interconnected by 3D structures (Fig. 18.4). This concept not only allows the co-culture of multiple cell types under different environments but is also designed to avoid cell sedimentation and to improve culture medium exchange in and out of the tissue constructs by rotational movements and flow perfusion (Fig. 18.4A and B). Moreover, this bioreactor concept allows the connection by flowing medium between several multi-chambers, adapting the concept of organ-on-a-chip microfluidics to the bioreactors reality (Fig. 18.4C).
Bioreactor systems adapted for organ-on-a-chip and high-throughput concepts. (A) Dynamic platform for 3D cell culture homogenization and increased diffusion by rotational movements. (B) The dynamic platform performs inversion of the cell culture chambers avoiding heterogeneous cell distribution in 3D scaffolds. (C) Dual-chambers from bioreactor are adaptable to 6-well culture plate as a concept for 3D interfaced in vitro tissues. (D) Transition from bioreactors to microfluidics concepts as a high-throughput device for 3D interfaced tissues. (Adapted with permission from ([97], http://pubs.acs.org/doi/abs/10.1021%2Fmp500136b) Copyright © 2014 American Chemical Society)
Concurrently, some dual-chamber bioreactors were tested for OC TE. Chang et al. [96] cultured a gelatin-infused shinbone block to generate OC constructs in a dual-chambered bioreactor for the production of hyaline cartilage within the gelatin portion of the scaffold while the bony portion was acellular. Mahmoudifar and Doran [97] used a similar dual-chambered bioreactor for the maturation of two sutured polyglycolic acid meshes seeded with ASCs. After 2 weeks of culture, both layers were cellularized, but showed statistically undifferentiated GAG content. The main differences in comparison to our system are related to specific dynamic features. While these two reported dual-chambers are under flow perfusion, our bioreactor allows rotational movements to improve medium diffusion and vertical turning movements to increase cell homogenization though the 3D structures.
OC in vitro models based on microfluidic devices were recently reported. Goldman and Babino [98] created a microfluidic dual-chamber device for the control over the osteo- and chondrogenic phenotypes. Bovine MSC were encapsulated in agarose, casted against micromolds of a serpentine network, and stacked to produce tissue constructs containing two independent microfluidic channel networks. Constructs receiving differentiation media showed differential chondrogenic and osteogenic gene expression, which was confirmed at the protein level as collagens I, II, and X. The control group under basal culture medium corroborated the results by showing homogeneous expression of the same biomarkers measured in lower concentrations at both the mRNA and protein level.
Shi et al. [99] compared a strategy based on a gradient generated by a microfluidic device with a conventional approach where two pieces of ASCs-laden hydrogel were cultured under osteogenic and chondrogenic conditions and joined together. The microfluidic system allowed generating a gradient of differentiation mimicking the OC interface. Although the dynamic cell differentiation methods using the microfluidic device consumed more cell culture media than the static method, the microfluidic system continuously supplied new nutrition and transported the wastes produced by cell metabolism out of the device generating a nontoxic environment. In addition, the flowing media could be collected and reused because much of the nutrients in the flowing media are not consumed during the continuous flow of culture media.
Lately, a technological approach using a high-throughput platform was designed, and osteoarthritic condition was already assessed to validate the system (Fig. 18.4D). Lin et al. [100] developed the platform adapted for interfaced OC tissue in a well plate format. This approach represents a transition design in between bioreactors and microfluidics. The system consists in a single bioreactor formed by the inserts and lid in the context of a 24-well plate. The device was designed to accommodate the biphasic nature of an OC plug by creating two separate compartments for the “chondral” and “osseous” microenvironments. The two microenvironments are independently controlled and the medium flow through each row of wells. The authors have shown that MSC-based chondral and osseous tissues respond to IL-1β in a manner that the changes in one tissue compartment are communicated to the other along the OC axis.
While bioreactors are now seeing its concept turned to the field of tissue modeling, microfluidic systems have been tested more often for this goal. However, the main difference of both concepts is that bioreactors were firstly developed for tissue production to be used as grafts for implantation and are now useful platforms for in vitro tissue modeling, while microfluidic devices can only be used for this last purpose as a drug testing or diagnostic tool.
6 Future Directions and Conclusions
The combination of culture systems as bioreactors and microfluidics with 3D cell culture has triggered alternatives reporting great potential to provide efficient methods for biomedical applications, TE, and drug screening. However, increased complexity associated with access to cultivated cells in 3D constructs and further sampling for assays is a combination of problematic challenges to be solved. The current systems allow the creation of gradients and the spatial arrangement of cells enabled mainly by microfluidics, but overall lack control of dynamics and spatial presentation of various signals over 3D constructs, which requires meticulous attention.
There is also a strong need of cost-effective and easy-to-use systems. High-throughput systems have been reported to solve these needs, but still require optimization when applied for 3D interfaced tissues as OC. Although organ-on-a-chip has drawn attention for integrated studies of tissue interplay, the integration of microenvironments in a single device still needs further developments. Furthermore, the transition from 2D to 3D adds one more dimension not only in terms of shape and structure but also in terms of data acquisition.
The integration of materials engineering, nanofabrication, and biology already opened up new roots guiding us to the current scenario. However, bringing new tools from bioinformatics, systems biology, and sensors for real-time monitoring may help in overcoming the remaining challenges. In the near future, the development of automated, high-throughput, reproducible, cost-effective, and easy-to-use 3D cell culture systems is expected. Advances of microfluidics and bioreactors cell culturing technologies will trigger a new coming era of developments and discoveries not only about OC-related disorders and therapeutics but in the field of TE and drug discovery in general.
References
van Duinen V, Trietsch SJ, Joore J, Vulto P, Hankemeier T (2015) Microfluidic 3D cell culture: from tools to tissue models. Curr Opin Biotechnol [Internet] 35(Supplement C):118–126. Available from: http://www.sciencedirect.com/science/article/pii/S0958166915000713
Griffith LG, Swartz MA (2006) Capturing complex 3D tissue physiology in vitro. Nat Rev Mol Cell Biol 7(3):211–224
Martin I, Miot S, Barbero A, Jakob M, Wendt D (2007) Osteochondral tissue engineering. J Biomech [Internet] 40(4):750–765. Available from: http://www.sciencedirect.com/science/article/pii/S0021929006000960
Lories RJ, Luyten FP (2011) The bone-cartilage unit in osteoarthritis. Nat Rev Rheumatol 7(1):43–49
Goldman SM, Barabino GA (2016) Spatial engineering of osteochondral tissue constructs through Microfluidically directed differentiation of Mesenchymal stem cells. Biores Open Access [Internet] 5(1):109–117. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4854211/
Liu X, Jiang H (2013) Preparation of an osteochondral composite with mesenchymal stem cells as the single-cell source in a double-chamber bioreactor. Biotechnol Lett [Internet] 35(10):1645–1653. Available from: https://doi.org/10.1007/s10529-013-1248-9
Khademhosseini A, Langer R, Borenstein J, Vacanti JP (2006) Microscale technologies for tissue engineering and biology. Proc Natl Acad Sci U S A [Internet]. 103(8):2480–2487. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC1413775/
Bhatia SN, Ingber DE (2014) Microfluidic organs-on-chips. Nat Biotech [Internet] 32(8):760–772. Available from: https://doi.org/10.1038/nbt.2989
Barron V, Lyons E, Stenson-Cox C, McHugh PE, Pandit A (2003) Bioreactors for cardiovascular cell and tissue growth: a review. Ann Biomed Eng [Internet] 31(9):1017–1030. Available from: https://doi.org/10.1114/1.1603260
Costa PF, Vaquette C, Baldwin J, Chhaya M, Gomes ME, Reis RL et al (2014) Biofabrication of customized bone grafts by combination of additive manufacturing and bioreactor knowhow. Biofabrication [Internet] 6(3):35006. Available from: http://stacks.iop.org/1758-5090/6/i=3/a=035006
Antoni D, Burckel H, Josset E, Noel G (2015) Three-dimensional cell culture: a breakthrough in vivo. Rahaman MN, editor. Int J Mol Sci [Internet] 16(3):5517–5527. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4394490/
Grayson WL, Bhumiratana S, Cannizzaro C, Chao PH, Lennon DP, Caplan AI et al (2008) Effects of initial seeding density and fluid perfusion rate on formation of tissue-engineered bone. Tissue Eng Part A [Internet] 14(11):1809–1820. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2773295/
Kleinhans C, Mohan RR, Vacun G, Schwarz T, Haller B, Sun Y et al (2015) A perfusion bioreactor system efficiently generates cell-loaded bone substitute materials for addressing critical size bone defects. Biotechnol J 10(11):1727–1738
Gardel LS, Serra LA, Reis RL, Gomes ME (2013) Use of perfusion bioreactors and large animal models for long bone tissue engineering. Tissue Eng Part B Rev [Internet] 20(2):126–146. Available from: https://doi.org/10.1089/ten.teb.2013.0010
Massai D, Isu G, Madeddu D, Cerino G, Falco A, Frati C et al (2016) A versatile bioreactor for dynamic suspension cell culture. Application to the culture of cancer cell spheroids. Pesce M, editor. PLoS One [Internet] 11(5):e0154610. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4856383/
Goldstein AS, Juarez TM, Helmke CD, Gustin MC, Mikos AG (2001) Effect of convection on osteoblastic cell growth and function in biodegradable polymer foam scaffolds. Biomaterials [Internet] 22(11):1279–1288. Available from: http://www.sciencedirect.com/science/article/pii/S0142961200002805
Andersson H, van den Berg A (2004) Microfabrication and microfluidics for tissue engineering: state of the art and future opportunities. Lab Chip [Internet] 4(2):98–103. Available from: https://doi.org/10.1039/B314469K
Cartmell SH, Porter BD, Garcia AJ, Guldberg RE (2003) Effects of medium perfusion rate on cell-seeded three-dimensional bone constructs in vitro. Tissue Eng 9(6):1197–1203
Ishaug SL, Crane GM, Miller MJ, Yasko AW, Yaszemski MJ, Mikos AG (1997) Bone formation by three-dimensional stromal osteoblast culture in biodegradable polymer scaffolds. J Biomed Mater Res 36(1):17–28
Polacheck WJ, German AE, Mammoto A, Ingber DE, Kamm RD (2014) Mechanotransduction of fluid stresses governs 3D cell migration. Proc Natl Acad Sci [Internet] 111(7):2447–2452. Available from: http://www.pnas.org/content/111/7/2447.abstract
Tarbell JM, Shi Z-D, Dunn J, Jo H (2014) Fluid mechanics, arterial disease, and gene expression. Annu Rev Fluid Mech [Internet] 46:591–614. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4211638/
Li X (James), Valadez AV, Zuo P, Nie Z (2012) Microfluidic 3D cell culture: potential application for tissue-based bioassays. Bioanalysis [Internet] 4(12):1509–1525. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3909686/
Song L, Zhou Q, Duan P, Guo P, Li D, Xu Y et al (2012) Successful development of small diameter tissue-engineering vascular vessels by our novel integrally designed pulsatile perfusion-based bioreactor. PLoS One [Internet] 7(8):e42569. Available from: https://doi.org/10.1371/journal.pone.0042569
Wang B, Wang G, To F, Butler JR, Claude A, McLaughlin RM et al (2013) Myocardial scaffold-based cardiac tissue engineering: application of coordinated mechanical and electrical stimulations. Langmuir [Internet] 29(35):11109–11117. Available from: https://doi.org/10.1021/la401702w
Grodzinsky AJ, Levenston ME, Jin M, Frank EH (2000) Cartilage tissue remodeling in response to mechanical forces. Annu Rev Biomed Eng [Internet] 2(1):691–713. Available from: https://doi.org/10.1146/annurev.bioeng.2.1.691
Santoro M, Lamhamedi-Cherradi S-E, Menegaz BA, Ludwig JA, Mikos AG (2015) Flow perfusion effects on three-dimensional culture and drug sensitivity of Ewing sarcoma. Proc Natl Acad Sci U S A [Internet] 112(33):10304–10309. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4547215/
Kou S, Pan L, van Noort D, Meng G, Wu X, Sun H et al (2011) A multishear microfluidic device for quantitative analysis of calcium dynamics in osteoblasts. Biochem Biophys Res Commun [Internet] 408(2):350–355. Available from: http://www.sciencedirect.com/science/article/pii/S0006291X11006188
Porter B, Zauel R, Stockman H, Guldberg R, Fyhrie D (2005) 3-D computational modeling of media flow through scaffolds in a perfusion bioreactor. J Biomech [Internet] 38(3):543–549. Available from: http://www.sciencedirect.com/science/article/pii/S0021929004001964
Godara P, McFarland CD, Nordon RE (2008) Design of bioreactors for mesenchymal stem cell tissue engineering. J Chem Technol Biotechnol [Internet] 83(4):408–420. Available from: https://doi.org/10.1002/jctb.1918
Mao AS, Mooney DJ (2015) Regenerative medicine: current therapies and future directions. Proc Natl Acad Sci U S A [Internet] 112(47):14452–14459. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4664309/
Gharravi AM, Orazizadeh M, Ansari-Asl K, Banoni S, Izadi S, Hashemitabar M (2012) Design and fabrication of anatomical bioreactor systems containing alginate scaffolds for cartilage tissue engineering. Avicenna J Med Biotechnol [Internet] 4(2):65–74. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3558208/
Powers MJ, Domansky K, Kaazempur-Mofrad MR, Kalezi A, Capitano A, Upadhyaya A et al (2002) A microfabricated array bioreactor for perfused 3D liver culture. Biotechnol Bioeng 78(3):257–269
Naciri M, Kuystermans D, Al-Rubeai M (2008) Monitoring pH and dissolved oxygen in mammalian cell culture using optical sensors. Cytotechnology [Internet] 57(3):245–250. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2570003/
da Costa PF, Martins AMP, Gomes MME, das Neves NJMA, dos Reis RLG (2011) Multichamber bioreactor with bidirectional perfusion integrated in a culture system for tissue engineering strategies [Internet]. Google Patents. Available from: https://www.google.ch/patents/EP2151491A3?cl=en
Sucosky P, Osorio DF, Brown JB, Neitzel GP (2004) Fluid mechanics of a spinner-flask bioreactor. Biotechnol Bioeng [Internet] 85(1):34–46. Available from: https://doi.org/10.1002/bit.10788
Altman GH, Horan RL, Martin I, Farhadi J, Stark PRH, Volloch V et al (2002) Cell differentiation by mechanical stress. FASEB J [Internet] 16(2):270–272. Available from: http://www.fasebj.org/content/early/2002/02/02/fj.01-0656fje.short
van der DWJ S, van ACC S, Boonen KJM, Langelaan MLP, Bouten CVC, Baaijens FPT (2013) Engineering skeletal muscle tissues from murine myoblast progenitor cells and application of electrical stimulation. J Vis Exp 73:e4267
Tsimbouri PM, Childs PG, Pemberton GD, Yang J, Jayawarna V, Orapiriyakul W et al (2017) Stimulation of 3D osteogenesis by mesenchymal stem cells using a nanovibrational bioreactor. Nat Biomed Eng [Internet] 1(9):758–770. Available from: https://doi.org/10.1038/s41551-017-0127-4
Canadas RF, Marques AP, Oliveira JM, Reis RL (2014) Rotational dual chamber bioreactor: methods and uses thereof [Internet]. WO2014141136 A1. Available from: http://www.google.com/patents/WO2014141136A1?cl=en
Canadas RF, Oliveira JM, Marques AP, Reis RL (2016) Multi-chambers bioreactor, methods and uses [Internet]. Association for the Advancement of Tissue Engineering and Cell Based Technologies and Therapies - A4Tec; WO 2016042533 A1. Available from: https://www.google.com/patents/WO2016042533A1?cl=en
Bancroft GN, Sikavitsas VI, Mikos AG (2003) Technical note: design of a flow perfusion bioreactor system for bone tissue-engineering applications. Tissue Eng [Internet] 9(3):549–554. Available from: http://www.liebertonline.com/doi/abs/10.1089/107632703322066723
Kim JB (2005) Three-dimensional tissue culture models in cancer biology. Semin Cancer Biol [Internet] 15(5):365–377. Available from: http://www.sciencedirect.com/science/article/pii/S1044579X05000301
Rodday B, Hirschhaeuser F, Walenta S, Mueller-Klieser W (2011) Semiautomatic growth analysis of multicellular tumor spheroids. J Biomol Screen [Internet] 16(9):1119–1124. Available from: https://doi.org/10.1177/1087057111419501
Vunjak-Novakovic G, Obradovic B, Martin I, Bursac PM, Langer R, Freed LE (1998) Dynamic cell seeding of polymer scaffolds for cartilage tissue engineering. Biotechnol Prog [Internet] 14(2):193–202. Available from: https://doi.org/10.1021/bp970120j
Sikavitsas VI, Bancroft GN, Mikos AG (2002) Formation of three-dimensional cell/polymer constructs for bone tissue engineering in a spinner flask and a rotating wall vessel bioreactor. J Biomed Mater Res [Internet] 62(1):136–148. Available from: http://doi.wiley.com/10.1002/jbm.10150
Vunjak-Novakovic G, Searby N, De Luis J, Freed LE (2002) Microgravity studies of cells and tissues. Ann N Y Acad Sci [Internet] 974(1):504–517. Available from: https://doi.org/10.1111/j.1749-6632.2002.tb05927.x
Vunjak-Novakovic G, Martin I, Obradovic B, Treppo S, Grodzinsky AJ, Langer R et al (1999) Bioreactor cultivation conditions modulate the composition and mechanical properties of tissue-engineered cartilage. J Orthop Res [Internet] 17(1):130–138. Available from: http://doi.wiley.com/10.1002/jor.1100170119
Goodwin TJ, Prewett TL, Wolf DA, Spaulding GF (1993) Reduced shear stress: a major component in the ability of mammalian tissues to form three-dimensional assemblies in simulated microgravity. J Cell Biochem [Internet] 51(3):301–311. Available from: https://doi.org/10.1002/jcb.240510309
Marlovits S, Tichy B, Truppe M, Gruber D, Vecsei V (2003) Chondrogenesis of aged human articular cartilage in a scaffold-free bioreactor. Tissue Eng 9(6):1215–1226
Saini S, Wick TM (2003) Concentric cylinder bioreactor for production of tissue engineered cartilage: effect of seeding density and hydrodynamic loading on construct development. Biotechnol Prog [Internet] 19(2):510–521. Available from: http://doi.wiley.com/10.1021/bp0256519
Williams KA, Saini S, Wick TM (2002) Computational fluid dynamics modeling of steady-state momentum and mass transport in a bioreactor for cartilage tissue engineering. Biotechnol Prog [Internet] 18(5):951–963. Available from: https://doi.org/10.1021/bp020087n
Barrila J, Radtke AL, Crabbé A, Sarker SF, Herbst-Kralovetz MM, Ott CM et al (2010) Organotypic 3D cell culture models: using the rotating wall vessel to study host–pathogen interactions. Nat Rev Micro [Internet] 8(11):791–801. Available from: https://doi.org/10.1038/nrmicro2423
Wendt D, Marsano A, Jakob M, Heberer M, Martin I (2003) Oscillating perfusion of cell suspensions through three-dimensional scaffolds enhances cell seeding efficiency and uniformity. Biotechnol Bioeng [Internet] 84(2):205–214. Available from: https://doi.org/10.1002/bit.10759
Sikavitsas VI, Bancroft GN, Holtorf HL, Jansen JA, Mikos AG (2003) Mineralized matrix deposition by marrow stromal osteoblasts in 3D perfusion culture increases with increasing fluid shear forces. Proc Natl Acad Sci U S A [Internet] 100(25):14683–14688. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC299759/
Gomes ME, Sikavitsas VI, Behravesh E, Reis RL, Mikos AG (2003) Effect of flow perfusion on the osteogenic differentiation of bone marrow stromal cells cultured on starch-based three-dimensional scaffolds. J Biomed Mater Res Part A [Internet] 67A(1):87–95. Available from: https://doi.org/10.1002/jbm.a.10075
Shahin K, Doran PM (2015) Shear and compression bioreactor for cartilage synthesis BT – cartilage tissue engineering: methods and protocols. In: Doran PM, editor. New York, NY: Springer New York. Methods Mol Biol 1340:221–233. Available from: https://doi.org/10.1007/978-1-4939-2938-2_16
Correia C, Pereira AL, Duarte ARC, Frias AM, Pedro AJ, Oliveira JT et al (2012) Dynamic culturing of cartilage tissue: the significance of hydrostatic pressure. Tissue Eng Part A [Internet] 18(19–20):1979–1991. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3463283/
Cochis A, Grad S, Stoddart MJ, Farè S, Altomare L, Azzimonti B et al (2017) Bioreactor mechanically guided 3D mesenchymal stem cell chondrogenesis using a biocompatible novel thermo-reversible methylcellulose-based hydrogel. Sci Rep [Internet] 7:45018. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC5362895/
Holt GE, Halpern JL, Dovan TT, Hamming D, Schwartz HS (2005) Evolution of an in vivo bioreactor. J Orthop Res [Internet] 23(4):916–923. Available from: https://doi.org/10.1016/j.orthres.2004.10.005
Stevens MM, Marini RP, Schaefer D, Aronson J, Langer R, Shastri VP (2005) In vivo engineering of organs: the bone bioreactor. Proc Natl Acad Sci U S A [Internet] 102(32):11450–11455. Available from: http://www.pnas.org/content/102/32/11450.abstract
Gupta N, Liu JR, Patel B, Solomon DE, Vaidya B, Gupta V (2016) Microfluidics-based 3D cell culture models: utility in novel drug discovery and delivery research. Bioeng Transl Med [Internet] 1(1):63–81. Available from: https://doi.org/10.1002/btm2.10013
Inamdar NK, Borenstein JT (2011) Microfluidic cell culture models for tissue engineering. Curr Opin Biotechnol [Internet] 22(5):681–689. Available from: http://www.sciencedirect.com/science/article/pii/S0958166911006161
Novotný J, Foret F (2017) Fluid manipulation on the micro-scale: basics of fluid behavior in microfluidics. J Sep Sci [Internet] 40(1):383–394. Available from: https://doi.org/10.1002/jssc.201600905
Gu H, Duits MHG, Mugele F (2011) Droplets formation and merging in two-phase flow microfluidics. Int J Mol Sci [Internet] 12(4):2572–2597. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3127135/
Lin L, Chu Y-S, Thiery JP, Lim CT, Rodriguez I (2013) Microfluidic cell trap array for controlled positioning of single cells on adhesive micropatterns. Lab Chip [Internet] 13(4):714–721. Available from: https://doi.org/10.1039/C2LC41070B
Geng T, Bredeweg EL, Szymanski CJ, Liu B, Baker SE, Orr G et al (2015) Compartmentalized microchannel array for high-throughput analysis of single cell polarized growth and dynamics. Sci Rep [Internet] 5:16111. Available from: https://doi.org/10.1038/srep16111
Horayama M, Shinha K, Kabayama K, Fujii T, Kimura H (2016) Spatial chemical stimulation control in microenvironment by microfluidic probe integrated device for cell-based assay. PLoS One [Internet] 11(12):e0168158. Available from: https://doi.org/10.1371/journal.pone.0168158
Jivani RR, Lakhtaria GJ, Patadiya DD, Patel LD, Jivani NP, Jhala BP (2016) Biomedical microelectromechanical systems (BioMEMS): revolution in drug delivery and analytical techniques. Saudi Pharm J [Internet] 24(1):1–20. Available from: http://www.sciencedirect.com/science/article/pii/S131901641300114X
Lin J-L, Wang S-S, Wu M-H, Oh-Yang C-C (2011) Development of an integrated microfluidic perfusion cell culture system for real-time microscopic observation of biological cells. Sensors 11(9):8395–8411
Mauleon G, Fall CP, Eddington DT (2012) Precise spatial and temporal control of oxygen within in vitro brain slices via microfluidic gas channels. PLoS One [Internet] 7(8):e43309. Available from: https://doi.org/10.1371/journal.pone.0043309
Khan DH, Roberts SA, Cressman JR, Agrawal N (2017) Rapid generation and detection of biomimetic oxygen concentration gradients in vitro. Sci Rep [Internet] 7(1):13487. Available from: https://doi.org/10.1038/s41598-017-13886-z
Folch A, Ayon A, Hurtado O, Schmidt MA, Toner M (1999) Molding of deep polydimethylsiloxane microstructures for microfluidics and biological applications. J Biomech Eng [Internet] 121(1):28–34. Available from: https://doi.org/10.1115/1.2798038
Folch A, Toner M (1998) Cellular micropatterns on biocompatible materials. Biotechnol Prog 14(3):388–392
Ling Y, Rubin J, Deng Y, Huang C, Demirci U, Karp JM et al (2007) A cell-laden microfluidic hydrogel. Lab Chip [Internet] 7(6):756–762. Available from: https://doi.org/10.1039/B615486G
Martinez AW, Phillips ST, Whitesides GM (2008) Three-dimensional microfluidic devices fabricated in layered paper and tape. Proc Natl Acad Sci [Internet] 105(50):19606–19611. Available from: http://www.pnas.org/content/105/50/19606.abstract
Derda R, Laromaine A, Mammoto A, Tang SKY, Mammoto T, Ingber DE et al (2009) Paper-supported 3D cell culture for tissue-based bioassays. Proc Natl Acad Sci [Internet] 106(44):18457–18462. Available from: http://www.pnas.org/content/106/44/18457.abstract
Chen CS, Mrksich M, Huang S, Whitesides GM, Ingber DE (1997) Geometric control of cell life and death. Science [Internet] 276(5317):1425–1428. Available from: http://science.sciencemag.org/content/276/5317/1425.abstract
Koh W-G, Pishko MV (2006) Fabrication of cell-containing hydrogel microstructures inside microfluidic devices that can be used as cell-based biosensors. Anal Bioanal Chem [Internet] 385(8):1389–1397. Available from: https://doi.org/10.1007/s00216-006-0571-6
Tan W, Desai TA (2005) Microscale multilayer cocultures for biomimetic blood vessels. J Biomed Mater Res Part A [Internet] 72A(2):146–160. Available from: https://doi.org/10.1002/jbm.a.30182
Boyden S (1962) The chemotactic effect of mixtures of antibody and antigen on polymorphonuclear leucocytes. J Exp Med [Internet] 115(3):453–466. Available from: http://jem.rupress.org/content/115/3/453.abstract
Chung S, Sudo R, Mack PJ, Wan C-R, Vickerman V, Kamm RD (2009) Cell migration into scaffolds under co-culture conditions in a microfluidic platform. Lab Chip [Internet] 9(2):269–275. Available from: https://doi.org/10.1039/B807585A
Kuo C-T, Liu H-K, Huang G-S, Chang C-H, Chen C-L, Chen K-C et al (2014) A spatiotemporally defined in vitro microenvironment for controllable signal delivery and drug screening. Analyst [Internet] 139(19):4846–4854. Available from: https://doi.org/10.1039/C4AN00936C
Takayama S, Ostuni E, LeDuc P, Naruse K, Ingber DE, Whitesides GM (2001) Laminar flows: subcellular positioning of small molecules. Nature [Internet] 411(6841):1016. Available from: https://doi.org/10.1038/35082637
Baker BM, Trappmann B, Stapleton SC, Toro E, Chen CS (2013) Microfluidics embedded within extracellular matrix to define vascular architectures and pattern diffusive gradients. Lab Chip [Internet] 13(16):3246–3252. Available from: https://doi.org/10.1039/C3LC50493J
Trietsch SJ, Israels GD, Joore J, Hankemeier T, Vulto P (2013) Microfluidic titer plate for stratified 3D cell culture. Lab Chip [Internet] 13(18):3548–3554. Available from: https://doi.org/10.1039/C3LC50210D
Nève N, Kohles SS, Winn SR, Tretheway DC (2010) Manipulation of suspended single cells by microfluidics and optical tweezers. Cell Mol Bioeng [Internet] 3(3):213–228. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2932633/
Courson DS, Rock RS (2009) Fast benchtop fabrication of laminar flow chambers for advanced microscopy techniques. PLoS One [Internet] 4(8):e6479. Available from: https://doi.org/10.1371/journal.pone.0006479
Sart S, Tomasi RF-X, Amselem G, Baroud CN (2017) Multiscale cytometry and regulation of 3D cell cultures on a chip. Nat Commun [Internet] 8(1):469. Available from: https://doi.org/10.1038/s41467-017-00475-x
Wang X, Phan DTT, George SC, Hughes CCW, Lee AP (2016) Engineering anastomosis between living capillary networks and endothelial cell-lined microfluidic channels. Lab Chip [Internet] 16(2):282–290. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4869859/
Responte DJ, Lee JK, Hu JC, Athanasiou KA (2012) Biomechanics-driven chondrogenesis: from embryo to adult. FASEB J [Internet] 26(9):3614–3624. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3425829/
Alexander PG, Song Y, Taboas JM, Chen FH, Melvin GM, Manner PA et al (2013) Development of a spring-loaded impact device to deliver injurious mechanical impacts to the articular cartilage surface. Cartilage [Internet] 4(1):52–62. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4297114/
Buckwalter JA (2002) Articular cartilage injuries. Clin Orthop Relat Res (402):21–37
Repo RU, Finlay JB (1977) Survival of articular cartilage after controlled impact. J Bone Joint Surg Am 59(8):1068–1076
Haut RC, Ide TM, De Camp CE (1995) Mechanical responses of the rabbit patello-femoral joint to blunt impact. J Biomech Eng [Internet] 117(4):402–408. Available from: https://doi.org/10.1115/1.2794199
Kuiper NJ, Wang QG, Cartmell SH (2014) A perfusion co-culture bioreactor for osteochondral tissue engineered plugs. J Biomater Tissue Eng [Internet] 4(2):162–171. Available from: https://doi.org/10.1166/jbt.2014.1145
Chang C-H, Lin F-H, Lin C-C, Chou C-H, Liu H-C (2004) Cartilage tissue engineering on the surface of a novel gelatin–calcium-phosphate biphasic scaffold in a double-chamber bioreactor. J Biomed Mater Res Part B Appl Biomater [Internet] 71B(2):313–321. Available from: https://doi.org/10.1002/jbm.b.30090
Mahmoudifar N, Doran PM (2013) Osteogenic differentiation and osteochondral tissue engineering using human adipose-derived stem cells. Biotechnol Prog [Internet] 29(1):176–185. Available from: https://doi.org/10.1002/btpr.1663
Goldman SM, Barabino GA (2017) Cultivation of agarose-based microfluidic hydrogel promotes the development of large, full-thickness, tissue-engineered articular cartilage constructs. J Tissue Eng Regen Med [Internet] 11(2):572–581. Available from: https://doi.org/10.1002/term.1954
Shi X, Zhou J, Zhao Y, Li L, Wu H (2013) Gradient-regulated hydrogel for interface tissue engineering: steering simultaneous osteo/chondrogenesis of stem cells on a chip. Adv Healthc Mater [Internet] 2(6):846–853. Available from: https://doi.org/10.1002/adhm.201200333
Lin H, Lozito TP, Alexander PG, Gottardi R, Tuan RS (2014) Stem cell-based microphysiological osteochondral system to model tissue response to interleukin-1β. Mol Pharm [Internet] 11(7):2203–2212. Available from: http://www.ncbi.nlm.nih.gov/pmc/articles/PMC4086740/
Acknowledgments
This work is a result of the project FROnTHERA (NORTE-01-0145- FEDER-000023), supported by Norte Portugal Regional Operational Programme (NORTE 2020), under the Portugal 2020 Partnership Agreement, through the European Regional Development Fund (ERDF). Thanks are also due to the Portuguese Foundation for Science and Technology (FCT) for the project PEst-C/SAU/LA0026/201 and for the distinction attributed to J.M. Oliveira under the Investigator FCT program (IF/00423/2012 and IF/01285/2015). The authors also thank FCT for the Ph.D. scholarship provided to R. F. Canadas (SFRH/BD/92565/2013).
Author information
Authors and Affiliations
Corresponding author
Editor information
Editors and Affiliations
Rights and permissions
Copyright information
© 2018 Springer International Publishing AG, part of Springer Nature
About this chapter
Cite this chapter
Canadas, R.F., Marques, A.P., Reis, R.L., Oliveira, J.M. (2018). Bioreactors and Microfluidics for Osteochondral Interface Maturation. In: Oliveira, J., Pina, S., Reis, R., San Roman, J. (eds) Osteochondral Tissue Engineering. Advances in Experimental Medicine and Biology, vol 1059. Springer, Cham. https://doi.org/10.1007/978-3-319-76735-2_18
Download citation
DOI: https://doi.org/10.1007/978-3-319-76735-2_18
Published:
Publisher Name: Springer, Cham
Print ISBN: 978-3-319-76734-5
Online ISBN: 978-3-319-76735-2
eBook Packages: Biomedical and Life SciencesBiomedical and Life Sciences (R0)