Abstract
Cerebral microdialysis can be used to detect mitochondrial dysfunction, a potential target of neuroprotective treatment. Cyclosporin A (CsA) is a mitochondrial stabiliser that in a recent clinical stroke trial showed protective potential in patients with successful recanalisation. To investigate specific metabolic effects of CsA during reperfusion, and hypothesising that microdialysis values can be used as a proxy outcome measure, we assessed the temporal patterns of cerebral energy substrates related to oxidative metabolism in a model of transient focal ischaemia. Transient ischaemia was induced by intracerebral microinjection of endothelin-1 (150 pmol/15 µL) through stereotaxically implanted guide cannulas in awake, freely moving rats. This was immediately followed by an intravenous injection of CsA (NeuroSTAT; 15 mg/kg) or placebo solution during continuous microdialysis monitoring. After reperfusion, the lactate/pyruvate ratio (LPR) was significantly lower in the CsA group vs placebo (n = 17, 60.6 ± 24.3%, p = 0.013). Total and striatal infarct volumes (mm3) were reduced in the treatment group (n = 31, 61.8 ± 6.0 vs 80.6 ± 6.7, p = 0.047 and 29.9 ± 3.5 vs 41.5 ± 3.9, p = 0.033). CsA treatment thus ameliorated cerebral reperfusion metabolism and infarct size. Cerebral microdialysis may be useful in evaluating putative neuroprotectants in ischaemic stroke.
Similar content being viewed by others
Introduction
For several decades it has been recognised that mitochondrial dysfunction, characterised by impaired oxidative metabolism in spite of ample oxygen and substrate delivery, occurs after transient cerebral ischaemia1,2. Cerebral mitochondrial dysfunction can be identified and distinguished from cerebral ischaemia by analysing the patterns of energy metabolites obtained by microdialysis under experimental or clinical conditions3,4,5,6. Microdialysis is currently the only effective means of continuously monitoring cerebral metabolism in neurocritical patients, and it is used to detect secondary injury and to optimise treatment7.
A neuroprotective effect of the immunosuppressing drug cyclosporin A (CsA) in experimental transient cerebral ischaemia was first described by Shiga et al.8. The extent of this effect varies between studies9,10,11,12,13,14,15,16,17, however, and the results under clinical conditions have been equivocal. In a recent prospective randomised clinical study of 127 patients, no significant decrease of 30-day infarct volume was found when comparing CsA to placebo in ischaemic stroke patients eligible for thrombolysis18,19. However, the infarct volume was significantly reduced in the subset of patients who had successful recanalisation after proximal cerebral artery occlusion. These results imply that a positive treatment effect of CsA may be dependent on reperfusion and subsequent mitochondrial dysfunction rather than ischaemia per se.
In the current study, standard clinical cerebral microdialysis was used in combination with the previously described endothelin-1 (ET-1) model of focal transient ischaemia20,21,22. Contrary to the standard model of middle cerebral artery occlusion (MCAO), this design allows continuous monitoring in awake, freely moving rats, and effectively avoids the potential confounding effects of anaesthetics23.
The aim of the study was to (1) assess the temporal patterns of cerebral energy metabolites associated with mitochondrial dysfunction in the ET-1 rat model of transient focal ischaemia, (2) investigate whether intravenous cyclosporin A improved cerebral oxidative metabolism after reperfusion, and (3) investigate if such an effect correlated with 24-hour infarct volumes.
Methods and Materials
Animals and experimental model
The experiments were conducted from October 2016 to March 2017 at the animal facility of the Institute of Molecular Medicine, University of Southern Denmark, Odense. All experiments were performed in accordance with the Danish Animal Experiment Inspectorate under the Ministry of Food and Agriculture (licence no. 2012-DY-2934- 00008). The study was designed as a reiterated three-day procedure (Fig. 1) with two test animals per trial (treatment and vehicle). Male Sprague Dawley rats (Taconic Biosciences A/S Ejby, Denmark) weighing on average 262 g (range 198–344) and with mean age 7.5 weeks (range 6–9) were individually housed with cage enrichment in a 12-hour light/dark cycle with free access to food and water. This article is written in accordance with the ARRIVE guidelines.
Experiment timeline. Schematic timeline of the 3-day experiment reiterated with two animals per trial. On Day 1, 34 adult Sprague Dawley rats were stereotaxically implanted with two cerebral guides in the left hemisphere and a femoral vein access. On Day 2, the awake and freely moving rats were equipped with microinjection and microdialysis probes and attached to a balanced swivel. Continuous cerebral microdialysis was commenced, and dialysates were analysed every 15 min. When baseline values had stabilised, focal transient ischaemia was induced through intracerebral ET-1 microinjection followed by a randomised i.v. dose of CsA (15 mg/kg NeuroSTAT) or placebo solution. Microdialysis was continued for 5 hours, and after 24 hours rats were sacrificed for histological infarct volume estimation. CsA = cyclosporin A, ET-1 = endothelin-1.
On Day 1, the rats were anaesthetised with a subcutaneous injection of 3 ml/kg Hypnorm/Dormicum (Hypnorm: 0.315 mg/mL fentanyl and 10 mg/mL fluanisone, Janssen Pharmaceuticals, Beerse, Belgium; Dormicum: 5 mg/mL midazolam, Hoffmann-La Roche, Basel, Switzerland) and maintained with a supplemental dose of 1 ml/kg every 40 minutes. Lidocaine (20 mg/ml, Farmaplus AS, Oslo, Norway) was used as a local anaesthetic. Under the microscope (Leica WILD M680), rats were implanted with a heparinised femoral vein catheter (Micro-renatane MRE-033, Braintree/AgnTho’s, Stockholm, Sweden) tunnelled subcutaneously to a cranial midline incision. Using a stereotaxic frame (KOPF instruments, Tujunga, US), two 4 mm microdialysis guides (Brainlink, Groningen, Netherlands) were implanted in the left cerebral hemisphere; one adjacent to the proximal MCA in the piriform cortex (for ET-1 injection), and one in the ipsilateral striatum (for microdialysis). The stereotaxic coordinates relative to bregma, with the nose bar at −3.9 mm (according to the atlas of Paxinos and Watson, 1986), were:
Guide cannula for ET-1 injection: A + 0.9 mm; L 5.2 mm; V −4.6 mm
Guide cannula for microdialysis probe: A + 0.5 mm; L 2.5 mm; V −3.2 mm
The fused silica tubing of a microdialysis probe, from which the membrane was removed, was used as ET-1 probe. After insertion of the injection probe, the tip ended 3.0 mm below the guide cannula, 7.6 mm ventral to bregma.
The guides were fixed to the skull by a glass ionomer luting cement (GC Fuji plus capsule, GC corporation, Tokyo, Japan) with a slotted screw for head block tethering (Instech labs Inc., Plymouth Meeting, PA, USA) to connect the tubing to a dual channel microdialysis swivel (AgnTho’s AB, Stockholm, Sweden) and the tunnelled femoral vein catheter. Body temperature was controlled throughout surgery with a thermostatically regulated heating pad at 37.5 °C (Bosch CTKI3, München, Germany). Postoperative analgesia was achieved through a slow release oral formulation of 0.4 mg/kg buprenorphine (Temgesic 0.2 mg sublingual tab., RB Pharmaceuticals, Slough, UK). 5 ml NaCl was injected subcutaneously to secure post-operative rehydration.
Experimental Design and Drug Administration
On Day 2, the microdialysis probe (50 kDa, 3 mm membrane, BrainLink, Groningen, the Netherlands) and the ET-1 injection probe, connected with FEP-tubing (1.2 mL/10 cm AgnTho’s AB, Stockholm, Sweden), were inserted and connected to the swivel and monitoring equipment under short-acting isoflurane (Baxter A/S, Allerød, Denmark) anaesthesia. A 100 µL Hamilton syringe containing ET-1 diluted in sterile Ringer’s solution (147 mM NaCl, 4 mM KCl, 1.1 mM CaCl2, 1.0 mM MgCl2) was connected to the tubing of the ET cannula for manual microinfusion of ET-1. The dialysis probe was perfused with sterile Ringer’s solution using a syringe pump (22 Harvard Apparatus, Inc., Holliston, USA) at a flow rate of 1.0 µL/min. The microdialysis outlet was connected to a sample fraction collector (CMA 142, Stockholm, Sweden) programmed to shift vial every 15 minutes. All connections were made using the aforementioned FEP-tubing and 0.38 mm IDEX silicon. The samples were analysed continuously for glucose, pyruvate and lactate using an ISCUSflex analyser (MDialysis, Stockholm, Sweden) set to sensitivity intervals relevant to the measured concentrations (low linearity).
When a stable baseline was achieved (approx. 3 hours), focal transient ischaemia was induced using a reiterated regimen of intracerebral ET-1 injections of 6 + 3 + 3 + 3 µl (10 pmol/µl, dissolved in sterile Ringer’s solution, stored in 50 µl aliquots at −20 °C; Sigma-Aldrich Denmark A/S, Copenhagen) with 5 min intervals to produce a mean 30 min period of vascular constriction detected by a minimum glucose drop of 50% in concomitant ipsilateral microdialysis. (The optimal dosing regimen was established in pilot studies, where doses previously used by Gramsbergen et al.21 were modified to minimise permanent occlusion while maximising sufficient ischaemia time). Immediately after ET-1 injection, a randomised blinded intravenous administration of CsA or vehicle (15 mg/kg, 0.5 mg/ml NeuroSTAT and NeuroSTAT-placebo solution, NeuroVive, Lund, Sweden) was commenced at the infusion rate of 0.1 ml/min (maximal tolerated effective single dose – see section 3.3). The microdialysis sampling was continued for at least 5 hours after the insult.
On Day 3 (24 hours after transient ischaemia), the rats were euthanised using barbiturate injection (pentobarbital 200 mg/ml with lidocaine hydrochloride 20 mg/ml, Glostrup Apotek, Denmark) and then decapitated. The brains were rapidly removed and frozen using high pressure CO2 and stored in −80 °C until cryostat sectioning, Nissl staining (toluidine blue) and histopathological examination.
Randomisation and blinding
The experiment was conducted in series using two rats per trial. All surgical and non-surgical procedures were identical until randomisation to treatment or placebo. Randomisation and blinding of treatment versus placebo were performed using unlabelled vials with content unknown to the investigator (numbered 1 and 2). The animals were numbered with a tail marking and paired with treatment number. Unblinding was performed at the end of the experimental procedures. The infarct volume was estimated by investigators blinded to the treatment group assignment.
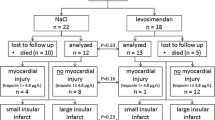
Altogether, 34 animals were randomised. One animal died after randomisation, and transient ischaemia was not achieved in two animals as evaluated by continuous real-time analysis of cerebral microdialysates of glucose concentrations in the affected cerebral volume (all three randomised to placebo group). Accordingly, infarct volume was evaluated in 17 CsA animals and 14 placebo animals. Due to technical problems with microdialysis perfusion flow rendering further analyses impossible (12 rats), as well as exclusion of animals displaying permanent MCA occlusion as defined by incomplete normalisation of cerebral glucose in real-time continuous cerebral microdialysis (2 rats), the complete biochemical analysis was performed in 10 CsA animals and 7 placebo animals.
Infarct volumetry
The whole rat forebrain was sectioned coronally into 30 μm slices in three parallel series (Leica CM 3050S cryostat) that were then placed on microscope slides. Two series were kept for reference, and one series was used for infarct volume (IFV) estimation and stained with toluidine blue24. Correct placement of probes was confirmed. Infarct volume was estimated using the Computer Assisted Stereological Test (CAST) Grid System (Olympus, Denmark) and the Cavalieri principle for volume estimation as described by Lambertsen et al.25 (standardised from 3.12 mm anterior and 3.12 mm posterior to the anterior commissure).
Statistics
All results are reported as mean ± SEM unless otherwise stated. Metabolite concentrations were visualised in timeline graphs. Means were calculated with values clustered at 15 min intervals. Lactate/pyruvate ratios (LPR) computed separately for specimens were normalised to baseline (i.e. changes of LPR are expressed as mean percentage of baseline values) in ICUpilot (v 2.0, MDialysis software, Sweden). Outliers were not cleared except in cases of documented instrumental failure and unintended permanent MCA occlusion. For statistical comparison of LPR (normally distributed in QQ-plot), a mixed effects linear regression model for repeated measurements was used with time and group as random effect and individual specimen as fixed effect. When an overall treatment effect was found, post hoc linear combinations of estimators were used to generate P values at the selected time interval, and regression diagnostics confirmed normally distributed residuals. Infarct volumes were analysed with regard to striatal and total (striatal + cortical) infarction and grouped according to treatment. Student’s t-test was used to analyse difference in means after confirming normal distribution using the QQ-plot technique. A P value below 0.05 was considered significant. Sample size estimation for comparing metabolite concentrations was based on variance from a pilot study (n = 10, SD 3.8), with a power of 80% and significance level at 5% and giving 7–8 rats per group based on a minimum treatment effect of 20% (STATA v 14.1, StataCorp., US).
Results
Table 1 presents the original mean baseline concentrations of the energy metabolites glucose, lactate, pyruvate and the lactate/pyruvate ratio along with their mean percentage change after reperfusion compared to the normalised baseline.
Figure 2 illustrates the ET-1 induced changes of glucose, lactate, pyruvate and LPR in the rat striatum for treatment and placebo groups. Immediately after ET-1 injection (Fig. 2, 1 hour time point), a nearly identical, marked decrease in glucose level was seen, confirming the reliability of the lesioning technique. The subsequent increase in glucose after approximately 30 min, indicating return of blood flow, was similar in both groups.
Temporal patterns of microdialysis metabolite concentrations – treatment vs placebo. Timeline graphs with normalised baselines showing the dynamic changes of brain interstitial mean (±SEM) concentrations of main intermediate metabolites of the redox-state in CsA (n = 10) and placebo (n = 7) specimens. At 1 hour, transient cerebral ischaemia was induced through intracerebral microinjection of ET-1. (A) Glucose levels showed similar patterns of transient ischaemia/reperfusion in both groups. (B) Lactate levels were very similar in the two groups, with low variance and a tendency to lower post-ischaemic values in the treatment group. (C) Pyruvate levels with the characteristic dip and overshoot pattern of this model, with CsA-treated animals showing slightly higher values. (D) The primary outcome variable LPR showed a significant point difference of 60.6 ± 24.3% at 3–5 hours (p = 0.013, mixed effect regression analysis). CsA = cyclosporin A, ET-1 = endothelin-1, LPR = lactate/pyruvate ratio.
Lactate levels increased markedly in both groups shortly after induction of ischaemia. The subsequent decrease of lactate toward baseline and the simultaneous increase in pyruvate concentration was more pronounced in the CsA treated animals. As a result, LPR decreased more in the CsA group, almost reaching normal baseline level (Fig. 2D). The mean 60.6 ± 24.3% point difference in LPR between the two groups (CsA 126.2 ± 24.3% vs controls 186.8 ± 18.4%) in the 3–5 hours after induction of ischaemia was significant (p = 0.013).
As shown in Fig. 3, the decreases in the total and striatal 24-hour infarct volumes (mm3) were statistically significant in the 17 animals treated with CsA compared to the 14 placebo animals (total volume: 61.8 ± 6.0 vs 80.6 ± 6.7, p = 0.047 and striatal volume: 29.9 ± 3.5 vs 41.5 ± 3.9, p = 0.033).
24-hour total and striatal infarct volumes – treatment vs placebo. Scatterplot with mean (±SEM) infarct volumes (mm3 in CsA (n = 17) and placebo (n = 14) groups. The two left columns show total infarct volume, the two right columns show the striatal infarct volumes alone. The infarct volume difference is significant for both total volume (61.8 ± 6.0 vs 80.6 ± 6.7, p = 0.047) and striatal volume (29.9 ± 3.5 vs 41.5 ± 3.9, p = 0.033).
In each specimen, the stereotaxic placement of the microdialysis probe and the ET-1 cannula was confirmed in the histologic sections with the intended 0.4 mm AP offset (Fig. 4, see method section for coordinates).
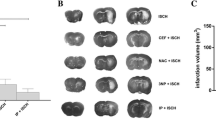
Representative micrographs of toluidine-stained rat brain sections – microdialysis and endothelin-1 probe placement. Representative toluidine blue-stained 30 µm rat brain sections with visible striatal and cortical infarcts and 5 mm scale bars. Arrows indicate the location of the microdialysis probe canal in the centre striatum (A) and the endothelin-1 probe canal in the piriform cortex (B).
Discussion
Relating to the treatment of acute cerebrovascular disease, this study links the potential neuroprotectant CsA26 to the proxy outcome measure of a widely used neurocritical monitoring method. It describes the effect of CsA treatment on oxidative metabolism and mitochondrial function in the ET-1 ischaemia-reperfusion model.
The results of this study are of direct clinical relevance, as the microdialysis technique used is identical to clinical routine, the treatment regimen is translationally sound and the model is unaffected by potential neuroprotective properties of anaesthetics.
The ET-1 model as ischaemia-reperfusion model
Under clinical conditions, infarct size has been shown to decrease in stroke patients treated with CsA only after successful recanalisation18,19. Hence, an animal model with in vivo testing of the neuroprotective properties of CsA should possess both ischaemia and reperfusion properties.
In the present model, we achieved a transient constriction of the proximal middle cerebral artery through stereotaxic application of ET-1, as previously described20,21,22. Contrary to the widespread standard MCAO model, the ET-1 model allows the rats to be awake and freely moving and avoids the potential confounding effects of anaesthetics. Combined with cerebral microdialysis, this enables continuous monitoring of cerebral energy metabolism during interventions under translational conditions.
CsA as a neuroprotective agent
The neuroprotective effect of CsA, a drug otherwise used for immunosuppression purposes, is believed to be exerted through inhibition of the cyclophilin D-mediated activation of the mitochondrial permeability transition pore (mPTP). The mPTP is activated under various pathophysiological conditions such as trauma, infection and cerebral ischaemia, inducing mitochondrial dysfunction and cell death27,28,29.
Previous experimental and clinical studies of CsA have utilised the Sandimmune formulation. This drug is known to be associated with severe anaphylactic complications, probably since CsA is administered in the polyoxyethylated castor oil base Cremophor EL30,31. The present study was conducted with a lipid-free emulsion (CicloMulsion) of CsA (NeuroSTAT) with fewer adverse reactions32.
Dosing, timing and route of administration
There is an overlap of reported optimal treatment effect on one side and toxicity on the other, concerning dose, time-window and route of administration in CsA treatment for neuroprotective purposes33. The intravenous route of administration is translationally preferable, and the optimal dose ranges from 10 mg/kg to 18.75 mg/kg, with reported side-effects at the higher dose34. For single dose i.v. administration, 15 mg/kg, 0.5 mg/ml CsA was thus chosen as a tolerable and efficient dose in the present study. The timing aspect is also important, with positive results occurring in pre-ischaemia treatment regimens and up to 6–24 hour post-insult35,36. Pre-reperfusion treatment, as opposed to treatment prior to the ischaemic event itself, is clinically plausible in patients selected for thrombolysis and thrombectomy as well as in patients with the stroke subtype subarachnoid haemorrhage with a high risk of delayed cerebral ischaemia.
The biochemical pattern during ischaemia-reperfusion and CsA treatment
In the present study, the levels of interstitial glucose decreased with reduced cerebral blood flow and then increased to above baseline during reperfusion. This pattern is compatible with cerebral ischaemia-reperfusion37.
The LPR increased five-fold during ischaemia. Although both treatment and placebo groups subsequently slowly returned toward baseline, the LPR level of the CsA group decreased significantly faster after reperfusion (Fig. 2D).
LPR reflects the cytoplasmic redox state, and compromised energy metabolism will cause an immediate increase in LPR38. Different biochemical patterns of LPR have been observed under various pathological metabolic conditions:
-
1.
Cerebral ischaemia. Decreased blood flow yields a pattern characterised by an elevated LPR with simultaneous reduced tissue levels of glucose and pyruvate21,39,40.
-
2.
Excessive cerebral energy utilisation. When energy demands exceed the mitochondrial capacity for oxidative metabolism e.g. during generalised epileptic seizures, the biochemical pattern is characterised by increased LPR, increased pyruvate and decreased cerebral glucose concentration41,42.
-
3.
Hypoxia. In pronounced arterial hypoxia, LPR and tissue pyruvate increase and – as cerebral blood flow is increased – so does the tissue concentration of glucose43.
-
4.
Mitochondrial dysfunction. In experimentally induced mitochondrial dysfunction, the metabolic pattern is characterised by a large increase in tissue lactate concentration together with a normal or moderately increased pyruvate level3,4,44,45. Similar patterns have been described in clinical situations with supposed mitochondrial dysfunction e.g. post-ischaemic recirculation and bacterial meningitis5,6,46.
As we did not observe seizures or hypoxic hypoxia, the LPR changes we observed in both groups are interpreted as transient ischaemia with subsequent mitochondrial dysfunction. This is supported by previous studies documenting mitochondrial dysfunction cerebral ischaemia-reperfusion injury1,2. The fact that LPR after reperfusion is significantly lower in animals treated with CsA (NeuroSTAT 15 mg/kg i.v.) suggests mitochondrial stabilisation. The ameliorating effect of CsA on energy metabolism is further supported by the reduction in 24-hour infarct volumes.
Limitations
Although our animals treated with CsA showed a marked (albeit smaller) striatal infarct upon histologic examination, the biochemical results nearly normalised after reperfusion. A similar finding has been described in patients with malignant cerebral infarct treated with hemicraniectomy5. To further explore this aspect of post-ischaemia metabolism, perfusion fluid labelling coupled with metabolomic analysis may be useful47.
The short duration from lesion and treatment to sacrifice (24 hours) may have reduced infarct size differences48, but it was sufficient for the study aim and in agreement with refinement guidelines of animal study ethics.
CsA only passes the intact blood-brain barrier in small amounts, and disruption of the blood-brain barrier is crucial to treatment efficacy49. This problem, bypassed in the current study by the intracerebral double guide insertion inherent to the model, may be one of the remaining obstacles in efficient clinical treatment strategies.
Conclusions
This study found that CsA (NeuroSTAT) reduced infarct volumes in the ET-1 rat model of focal transient cerebral ischaemia. This correlated with improved oxidative metabolism, as shown by decreased post-ischaemic LPR on intracerebral microdialysis. The results suggest that CsA may be neuroprotective in selected cerebrovascular patient groups and that the ET-I rat model may be useful in pre-clinical trials of putative neuroprotective substances. Further, routine cerebral microdialysis should be considered in clinical trials of neuroprotective treatment in cerebrovascular disease, in addition to evaluations of the short- and long-term outcome.
Data Availability
The datasets generated and analysed during the current study are available from the corresponding author on reasonable request.
References
Rehncrona, S., Mela, L. & Siesjö, B. K. Recovery of brain mitochondrial function in the rat after complete and incomplete cerebral ischemia. Stroke 10, 437–446 (1979).
Nordström, C. H., Rehncrona, S. & Siesjö, B. K. Restitution of cerebral energy state, as well as of glycolytic metabolites, citric acid cycle intermediates and associated amino acids after 30 minutes of complete ischemia in rats anaesthetized with nitrous oxide or phenobarbital. J. Neurochem. 30, 479–486 (1978).
Nielsen, T. H. et al. Cerebral energy metabolism during induced mitochondrial dysfunction. Acta Anaesthesiol. Scand. 57, 229–235 (2013).
Nielsen, T. H., Olsen, N. V., Toft, P. & Nordström, C. H. Cerebral energy metabolism during mitochondrial dysfunction induced by cyanide in piglets. Acta Anaesthesiol. Scand. 57, 793–801 (2013).
Nielsen, T. H. et al. Bedside diagnosis of mitochondrial dysfunction after malignant middle cerebral artery infarction. Neurocrit. Care 21, 35–42 (2014).
Jacobsen, A., Nielsen, T. H., Nilsson, O., Schalén, W. & Nordström, C. H. Bedside diagnosis of mitochondrial dysfunction in aneurysmal subarachnoid hemorrhage. Acta Neurol. Scand. 130, 156–163 (2014).
Nordström, C.-H., Koskinen, L.-O. & Olivecrona, M. Aspects on the physiological and biochemical foundations of neurocritical care. Front. Neurol. 8 (2017).
Shiga, Y., Onodera, H., Matsuo, Y. & Kogure, K. Cyclosporin A protects against ischemia-reperfusion injury in the brain. Brain Res. 595, 145–148 (1992).
Kuroda, S., Janelidze, S. & Siesjö, B. K. The immunosuppressants cyclosporin A and FK506 equally ameliorate brain damage due to 30-min middle cerebral artery occlusion in hyperglycemic rats. Brain Res. 835, 148–153 (1999).
Matsumoto, S., Friberg, H., Ferrand-Drake, M. & Wieloch, T. Blockade of the mitochondrial permeability transition pore diminishes infarct size in the rat after transient middle cerebral artery occlusion. J. Cereb. Blood Flow Metab. 19, 736–741 (1999).
Yoshimoto, T. & Siesjö, B. K. Posttreatment with the immunosuppressant cyclosporin A in transient focal ischemia. Brain Res. 839, 283–291 (1999).
Matsumoto, S., Isshiki, A., Watanabe, Y. & Wieloch, T. Restricted clinical efficacy of cyclosporin A on rat transient middle cerebral artery occlusion. Life Sci. 72, 591–600 (2002).
Yu, G., Hess, D. C. & Borlongan, C. V. Combined cyclosporine-A and methylprednisolone treatment exerts partial and transient neuroprotection against ischemic stroke. Brain Res. 1018, 32–37 (2004).
Borlongan, C. V. et al. Acute functional effects of cyclosporine-A and methylprednisolone treatment in adult rats exposed to transient ischemic stroke. Life Sci. 76, 1503–1512 (2005).
Muramatsu, Y. et al. Neuroprotective efficacy of FR901459, a novel derivative of cyclosporin A, in in vitro mitochondrial damage and in vivo transient cerebral ischemia models. Brain Res. 1149, 181–190 (2007).
Leger, P.-L. et al. Evaluation of cyclosporine A in a stroke model in the immature rat brain. Exp. Neurol. 230, 58–66 (2011).
Cho, T.-H. et al. Pre-and post-treatment with cyclosporine A in a rat model of transient focal cerebral ischaemia with multimodal MRI screening. Int. J. Stroke 8, 669–674 (2013).
Nighoghossian, N. et al. Cyclosporine in acute ischemic stroke. Neurology 84, 2216–2223 (2015).
Ong, E. et al. Effect of cyclosporine on lesion growth and infarct size within the White and gray Matter. Front. Neurol. 8 (2017).
Van Hemelrijck, A. et al. Effect of resuscitative mild hypothermia on glutamate and dopamine release, apoptosis and ischaemic brain damage in the endothelin-1 rat model for focal cerebral ischaemia. J. Neurochem. 87, 66–75 (2003).
Gramsbergen, J. B., Skjøth-Rasmussen, J., Rasmussen, C. & Lambertsen, K. L. On-line monitoring of striatum glucose and lactate in the endothelin-1 rat model of transient focal cerebral ischemia using microdialysis and flow-injection analysis with biosensors. J. Neurosci. Methods 140, 93–101 (2004).
Sharkey, J. Perivascular microapplication of endothelin-1: a new model of focal cerebral ischaemia in the rat. J. Cereb. Blood Flow Metab. 13, 865–871 (1993).
Chen, F., Duan, G., Wu, Z., Zuo, Z. & Li, H. Comparison of the cerebroprotective effect of inhalation anaesthesia and total intravenous anaesthesia in patients undergoing cardiac surgery with cardiopulmonary bypass: a systematic review and meta-analysis. BMJ Open 7, 014629, https://doi.org/10.1136/bmjopen-2016-014629 (2017).
Popp, A., Jaenisch, N., Witte, O. W. & Frahm, C. Identification of ischemic regions in a rat model of stroke. Plos One 4 (2009).
Lambertsen, K. L., Gregersen, R. & Finsen, B. Microglial-macrophage synthesis of tumor necrosis factor after focal cerebral ischemia in mice is strain dependent. J. Cereb. Blood Flow Metab. Off. J. Int. Soc. Cereb. Blood Flow Metab. 22, 785–797 (2002).
Nighoghossian, N., Ovize, M., Mewton, N., Ong, E. & Cho, T.-H. Cyclosporine A, a potential therapy of ischemic reperfusion Injury. A common history for heart and brain. Cerebrovasc. Dis. 42, 309–318 (2016).
Crompton, M. The mitochondrial permeability transition pore and its role in cell death. Biochem. J. 341, 233–249 (1999).
Hansson, M. J. et al. Brain-derived respiring mitochondria exhibit homogeneous, complete and cyclosporin-sensitive permeability transition. J. Neurochem. 89, 715–729 (2004).
Hansson, M. J. et al. Calcium-induced generation of reactive oxygen species in brain mitochondria is mediated by permeability transition. Free Radic. Biol. Med. 45, 284–294 (2008).
Kahan, B., Wideman, C., Flechner, S. & Van Buren, C. Anaphylactic reaction to intravenous cyclosporin. The Lancet 323, 52 (1984).
Friedman, L. S., Dienstag, J. L., Nelson, P. W., Russell, P. S. & Cosimi, A. B. Anaphylactic reaction and cardiopulmonary arrest following intravenous cyclosporine. Am. J. Med. 78, 343–345 (1985).
Ehinger, K. H. J., Hansson, M. J., Sjövall, F. & Elmér, E. Bioequivalence and tolerability assessment of a novel intravenous ciclosporin lipid emulsion compared to branded ciclosporin in Cremophor EL. Clin. Drug Investig. 33, 25–34 (2013).
Serkova, N. J., Christians, U. & Benet, L. Z. Biochemical mechanisms of cyclosporine neurotoxicity. Mol. Interv. 4, 97 (2004).
Lulic, D., Burns, J., Bae, E. C., van Loveren, H. & Borlongan, C. V. A review of laboratory and clinical data supporting the safety and efficacy of cyclosporin A in traumatic brain injury. Neurosurgery 68, 1172–1186 (2011).
Sullivan, P. G. et al. Dose-response curve and optimal dosing regimen of cyclosporin A after traumatic brain injury in rats. Neuroscience 101, 289–295 (2000).
Sullivan, P. G., Sebastian, A. H. & Hall, E. D. Therapeutic window analysis of the neuroprotective effects of cyclosporine A after traumatic brain injury. J. Neurotrauma 28, 311–318 (2011).
Valtysson, J., Persson, L. & Hillered, L. Extracellular ischaemia markers in repeated global ischaemia and secondary hypoxaemia monitored by microdialysis in rat brain. Acta Neurochir. (Wien) 140, 387–395 (1998).
Siesjö BK. Brain energy metabolism. (Chichester) (John Wiley, 1978).
Amer-Wåhlin, I. et al. Fetal cerebral energy metabolism and electrocardiogram during experimental umbilical cord occlusion and resuscitation. J. Matern.-Fetal Neonatal Med. 23, 158–166 (2010).
Persson, L. & Hillered, L. Chemical monitoring of neurosurgical intensive care patients using intracerebral microdialysis. J. Neurosurg. 76, 72–80 (1992).
Blennow, G., Brierley, J. B., Meldrum, B. S. & Siesjö, B. K. Epileptic brain damage: the role of systemic factors that modify cerebral energy metabolism. Brain J. Neurol. 101, 687–700 (1978).
Folbergrová, J., Ingvar, M. & Siesjö, B. K. Metabolic changes in cerebral cortex, hippocampus, and cerebellum during sustained bicuculline-induced seizures. J. Neurochem. 37, 1228–1238 (1981).
Norberg, K. & Siesjö, B. K. Cerebral metabolism in hypoxic hypoxia. I. Pattern of activation of glycolysis: a re-evaluation. Brain Res. 86, 31–44 (1975).
MacMillan, V. H. Cerebral energy metabolism in cyanide encephalopathy. J. Cereb. Blood Flow Metab. 9, 156–162 (1989).
Munk, M., Poulsen, F. R., Larsen, L., Nordström, C. H. & Nielsen, T. H. Cerebral metabolic changes related to oxidative metabolism in a model of bacterial meningitis induced by lipopolysaccharide. Neurocrit. Care 3, 0509–9, https://doi.org/10.1007/s12028-018-0509-9 (2018).
Poulsen, F. R. et al. Bedside evaluation of cerebral energy metabolism in severe community-acquired bacterial meningitis. Neurocrit. Care 22, 221–228 (2015).
Jalloh, I. et al. Focally perfused succinate potentiates brain metabolism in head injury patients. J. Cereb. Blood Flow Metab. 1, 16672665, https://doi.org/10.1177/0271678X16672665 (2016).
McBride, D. W. et al. Changes in brain swelling and infarction volume over four days after hypoxia ischemia in neonatal rats. Acta Neurochir. Suppl. 121, 111–114 (2016).
Uchino, H. et al. Amelioration by cyclosporin A of brain damage in transient forebrain ischemia in the rat. Brain Res. 812, 216–226 (1998).
Acknowledgements
The authors thank technician Ulla Munk for laboratory services and technical personnel of the animal facility for help with animal maintenance. We thank Bettina Hjelm Clausen and the Bente Finsen Group for help in using the computerised microscope, and Arnon Møldrup Knudsen and the Bjarne Winther group for the use of the digital pathology slide scanner. We thank Claire Gudex for language editing. We thank Kasper Stokbro Nielsen, Andreas Jensen and Jonas Schöley for statistical consults and NeuroVive AB for providing the CsA and placebo formulations for this study. Faculty scholarship from the Department of Clinical Research, University of Southern Denmark [AF], Odense University Hospitals PhD scholarship [AF], Fonden for lægevidenskabens fremme [AF, grant number 12–260] and Karen S Jensens legat [AF, grant number 40-A1922].
Author information
Authors and Affiliations
Contributions
A.F., T.H.N., J.B.G. and C.H.N. conceived and designed the experiments. A.F., J.B.G., T.H.N. and K.H.N. participated in data acquisition. A.F., T.H.N., C.H.N., J.B.G. and F.R.P. analysed and interpreted the data. A.F. drafted the manuscript, and all authors helped with critical revision. F.R.P. and J.B.G. supervised the project. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing Interests
CHN is a member of the advisory board of NeuroVive AB, who provided the tested CsA and placebo formulations. AF, THN, JBG, KHN and FRP declare no potential conflicts of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in a credit line to the material. If material is not included in the article’s Creative Commons license and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Forsse, A., Nielsen, T.H., Nygaard, K.H. et al. Cyclosporin A ameliorates cerebral oxidative metabolism and infarct size in the endothelin-1 rat model of transient cerebral ischaemia. Sci Rep 9, 3702 (2019). https://doi.org/10.1038/s41598-019-40245-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1038/s41598-019-40245-x
- Springer Nature Limited
This article is cited by
-
Imeglimin Is Neuroprotective Against Ischemic Brain Injury in Rats—a Study Evaluating Neuroinflammation and Mitochondrial Functions
Molecular Neurobiology (2022)
-
Preclinical studies of mesenchymal stem cells transplantation in amyotrophic lateral sclerosis: a systemic review and metaanalysis
Neurological Sciences (2021)
-
A Prospective Observational Feasibility Study of Jugular Bulb Microdialysis in Subarachnoid Hemorrhage
Neurocritical Care (2020)
-
Cyclosporine therapy in cytokine storm due to coronavirus disease 2019 (COVID-19)
Rheumatology International (2020)