Abstract
High salt intake induces hypertension and enhances stroke onset. However, whether an increase in brain sodium exposure itself is harmful and has poor prognosis remains unknown. Therefore, we employed hypertensive rats that underwent intracerebroventricular (ICV) infusion of sodium for 28 days and evaluated stroke onset and related cytotoxic brain injuries. Forty-seven spontaneously hypertensive stroke-prone (SHRSP) and 39 normotensive rats (Wistar Kyoto rats [WKY]) underwent persistent ICV infusion of the following four solutions: artificial cerebrospinal fluid, 0.9%, 2.7%, and 9% saline for 28 days. We evaluated stroke onset and all-cause mortality between SHRSP and WKY at each ICV sodium concentration as the primary endpoints. Our secondary objective was to explore histological brain injuries associated with SHRSP induced by high sodium ICV. The results indicated that ICV infusion of 2.7% and 9% sodium showed a significant increase in stroke onset, decrease in body weight, and increase rate of brain water content in SHRSP compared to WKY. Increased blood pressure was not observed for ICV infusion of high sodium, while serum sodium concentration was significantly increased in SHRSP compared to WKY. Histological evaluations revealed that higher sodium infusion significantly increased the number of activated microglia, superoxide, neuronal cell loss, and microbleeds compared to WKY and SHRSP with 0.9% sodium. We conclude that persistent exposure to high sodium in the brain is one of the risk factors for stroke onset upregulating cerebral microbleeds and oxidative stress in hypertensive rats.

Similar content being viewed by others
Introduction
High salt intake is strongly associated with hypertension, which is a risk factor for stroke onset. However, recent studies have reported that salt intake causes direct brain toxicity independent of hypertension [1,2,3]. Currently, salt intake itself affects the development of dementia without causing an increase in blood pressure. For example, salt intake produces interleukin-17 in the small intestine, which circulates throughout the body, causing cerebrovascular endothelial cell damage and dysfunction, leading to cognitive dysfunction [2, 4]. However, whether brain sodium exposure induces brain damage, including stroke onset, remains unknown.
In addition to elevated blood pressure, high salt intake can also enhance sympathetic nerve activity. Although sodium cannot pass through the blood–brain barrier (BBB), the subfornical organ and organum vasculosum of the lamina terminalis, which have structurally fragile BBB, detect elevated blood sodium level and plasma osmolarity and transmit this information to the ventral lateral area of the rostral medulla via the paraventricular nucleus of the hypothalamus, thus activating sympathetic nerve activity and causing brain toxicity [5, 6]. We previously demonstrated that renal denervation, which has been introduced to reduce blood pressure by way of sympathetic outflow [7, 8], reduced high-salt diet-induced stroke onset in hypertensive rats, which was correlated with a reduction in brain oxidative stress and microglial activation [9]. Other studies have reported that intraventricular infusion of hypertonic saline induces hypertension, activates microglia, desensitizes baroreceptor reflexes, and affects the inflammatory response [10,11,12]. Although sympathetic nerve activation and brain oxidative stress may be key targets for salt-induced stroke onset, whether direct brain sodium exposure is correlated with stroke onset remains unclear.
In the present study, we aimed to test the hypothesis that persistent brain exposure to high sodium levels enhances stroke onset in hypertensive rats. To test this hypothesis, we employed hypertensive and normotensive rats, continuously administered multiple doses of sodium intracerebroventricularly, and evaluated stroke onset and the related brain injuries between the rats.
Materials and methods
Animals and experimental protocol
All experiments were approved by the Institutional Animal Care and Use Committee of Kurume University and performed in accordance with the National Institute of Health Guide for the Care and Use of Laboratory Animals. Eleven-week-old male spontaneously hypertensive stroke-prone rats/Izm (SHRSP, n = 47) weighting 238–269 g and age-matched male Wistar Kyoto rats/Izm (WKY, n = 39) weighting 279–348 g were assigned to the following groups: (1) intracerebroventricular (ICV) infusion with commercially available artificial cerebrospinal fluid (CSF) (ARTCEREB; Otsuka Pharmaceutical Factory, Tokushima, Japan) to SHRSP (SHRSP-CSF, n = 10), (2) ICV infusion with 0.9% saline to SHRSP (SHRSP-0.9%, n = 13), (3) ICV infusion with 2.7% saline to SHRSP (SHRSP-2.7%, n = 10), (4) ICV infusion with 9% saline to SHRSP (SHRSP-9%, n = 10), (5) ICV infusion with 0.9% saline to WKY (WKY-0.9%, n = 13, control group), (6) ICV infusion with 2.7% saline to WKY (WKY-2.7%, n = 11), and (7) ICV infusion with 9% saline to WKY (WKY-9%, n = 11). In addition, in preconditioned animals without ICV saline both SHRSP (n = 4) and WKY (n = 4) were included. Those animals were purchased from Japan SLC, Inc., Shizuoka, Japan keeping the strains officially sustained by the Disease Model Cooperative Research Association, Kyoto, Japan. All animals were fed a 0.3% sodium diet from 11 to 15 weeks of age. Experiment 1 was performed to compare the rate of stroke onset between CSF and 0.9% saline in SHRSP. The next experiments were performed to explore the dose-dependent effects of sodium on stroke onset in hypertensive rats compared with normotensive rats. We monitored the rate of stroke onset and all-cause mortality as the primary endpoints in all experiments, and our secondary objective was to explore histological brain injuries of SHRSP, including activated microglia, superoxide, neuronal cell loss, and microbleeds, compared to WKY with 0.9% saline as a control. Detailed protocols are shown in Supplementary Fig. 1.
Surgery
Implantation of an infusion cannula into the cerebral ventricles and an osmotic pump was performed according to our previous method [13, 14]. Briefly, the rats were anesthetized with 2% isoflurane through a face mask, and stainless steel cannulas (ALZET Brain Infusion Kit 1, Durect Co., Cuperito, CA, USA) using osmotic minipumps (Model 2004, Durect Co.) were inserted into the right cerebral ventricle at 1.0 mm posterior and 2.0 mm lateral from the bregma through the subcutaneous pockets on their backs. The solutions were continuously administered at a rate of 6 µL/day for 4 weeks. After the surgery, the operative lesion was disinfected with iodine, and meloxicam (1 mg/kg) was administered subcutaneously for appropriate analgesia [15].
Monitoring of stroke-related neurological symptoms and death
Stroke-related neurological symptoms were assessed every day through 4 weeks from the start of ICV infusion and scored as follows: 6, normal; 5, slight decrease/increase in motor activity; 4, evident decrease/increase in motor activity; 3, paralysis of hind limbs or involuntary movement; 2, slight movement; 1, unable to stand; and 0, death [16]. The score was measured as a symptom test, and stroke onset was defined as a score ≤4. All mortalities were also assessed daily.
Measurement of body weight and blood pressure
The weight of the rats was monitored weekly, and their systolic blood pressure was measured before the start of ICV infusion and 2 weeks after infusion using a tail sphygmomanometer (MK-2000ST, Muromachi Kikai Co., Ltd., Tokyo, Japan) [17].
Measurement of rotarod test and beam walking test
To assess motor function, coordination, and activity, we performed rotarod and beam walking tests according to our previous method [15, 16, 18].
In the rotarod test, the rats were placed on a horizontal drum (MK-630B, Muromachi Kikai) and walked at a speed of four rotations per minute (RPM) for a maximum of 60 s as a training session. The animals were then subjected to a trial on the accelerating spindle (4–40 RPM) for 5 min, and the latency to fall off the cylinder was recorded. The mean times for the three test trials were assigned to each animal.
In the beam walking test, the rats were placed on a beam (100 cm in length, 2.5 cm in width, and 20 cm in height), and their performance was evaluated as follows: 0 or 1 point for rats that hung/stood off the beam without walking, 2 points for animals that walked but fell down from the beam within 1 min, and 3 or 4 points for animals that could walk less than or at least 20 cm on the beam for 1 min. The trial was performed thrice for each rat, and the mean scores were used for each animal.
Measurement of the brain water content
At the end of the experiment, blood samples from the left ventricle were taken from each animal, euthanized under deep anesthesia with an overdose of isoflurane, and their brains were quickly resected. The brains were cut at the point of the bregma, and the caudal side was kept in 4% paraformaldehyde solution, embedded in paraffin, and cut into 5-µm section (K.I. Stainer Inc., Kumamoto, Japan). The serum sodium concentration was measured at SRL, Inc. (Tokyo, Japan).
According to the evaluation of brain water content (BWC), the brains, including the left hemisphere of the rostral side, cerebellum, and brain stem, were separated and weighed (wet weight) and subsequently incubated in an oven at 105 °C for 72 h and weighed again (dry weight) [15]. The following formula was used to calculate the percentage of BWC: ([wet weight – dry weight]/wet weight) × 100 and the increase rate was calculated as: (the value at the endpoint/the value at the baseline) × 100.
Histology
Ionized calcium binding adaptor molecule-1 staining
To assess the number of microglia, brain sections were immunostained with anti-ionized calcium binding adaptor molecule-1 (Iba-1; 1:2000; Fujifilm Wako Pure Chemical Corporation, Osaka, Japan), as previously described [19]. The number of positive cells was counted using images taken from three fields of the left somatosensory cortex at ×200 magnification. The number of resting microglia (resting and ramified microglia) and activated microglia (reactive and phagocytic microglia) was counted separately based on their morphological appearance [20] and expressed as cells/mm2. Additionally, we quantified microglial morphology using skeleton analysis, as previously described [21,22,23].
Dihydroethidium staining
To detect superoxide levels in the cortex, we employed dihydroethidium (DHE; Sigma-Aldrich St. Louis, MO, USA) because we previously confirmed that the fluorescence was derived from superoxide [24]. Brain sections were incubated with DHE for 30 min, as previously described with slight modification [19, 25]. Superoxide levels were detected by density of DHE fluorescence dye using Lumina Vision version 2.2.0 analysis software (Mitani Corporation, Tokyo, Japan) and quantified using images taken from three fields of the left somatosensory cortex at ×200 magnification. The mean values in the SHRSP groups were divided by those in the WKY-0.9% group in the same trial.
Nissl staining
Nissl staining was performed to evaluate the number of surviving neurons in the cortex. The number of positive cells was counted using images taken from three fields of the left somatosensory cortex at ×200 magnification. The mean number of cells was expressed as cells/mm2.
Prussian blue staining (iron staining)
To detect hemosiderin deposits, Prussian blue staining was performed according to the manufacturer’s instructions (Muto Pure Chemicals Co., Ltd., Tokyo, Japan). Briefly, the sections were washed twice with distilled water and incubated with Prussian blue staining solution at room temperature for 30 min. The staining solution was prepared by blending 75 mL of a 2% potassium ferrocyanide solution (Muto Pure Chemicals Co., Ltd., Tokyo, Japan) and 1% hydrochloric acid in equal volumes. The sections were then rinsed twice in distilled water for 5 min and incubated in a cologne echolate solution (Muto Pure Chemicals Co., Ltd., Tokyo, Japan) for 5 min. Microbleeds in the ipsilateral hemisphere of each animal were counted at ×400 magnification, and the number was compared between the groups.
Statistical analyses
We performed all measurements in a blinded manner. Statistical analyses were performed using GraphPad Prism (version 9) for Windows (GraphPad Software Inc., San Diego, CA, USA) and Ekuseru-Tokei 2019 statistical software (Social Survey Research Information Co., Ltd., Tokyo, Japan). All data are presented as the median ± interquartile. The incidence of stroke onset and mortality was analyzed using a standard Kaplan–Meier curve with a log-rank test and χ2 analysis. Statistical significance was determined using the Mann–Whitney U-test between the two groups. Since the main purpose of the secondary endpoints was to compare the phenotype between the control (WKY-0.9% or SHRSP-0.9) and other SHRSP groups, statistical significance was tested using the Kruskal–Wallis test, followed by Shirley–Williams’ multiple comparison test. Differences were considered statistically significant at p < 0.05 in all tests.
Results
To avoid confounding factors, such as direct traumatic brain injuries by stainless steel cannulas, we excluded rats that showed injury-related symptoms within 7 days after the start of both experiments (WKY-0.9%, 2; SHRSP-CSF, 0; SHRSP-0.9%, 2; SHRSP-2.7%, 0; SHRSP-9%, 0; WKY-2.7%, 0; WKY-9%, 0).
Experiment 1
No significant difference in the rate of stroke onset was observed between the SHRSP-CSF (20%, 2 of 10 rats) and SHRSP-0.9% (27.3%, 3 of 11 rats) groups (data not shown). Therefore, we evaluated experiment 2 using 0.9% saline as the solvent.
Experiment 2
Effect of mortality and incidence of stroke
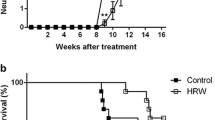
The incidence rate of stroke onset in SHRSP-2.7% (5 of 10 rats, 50%) and SHRSP-9% (7 of 10 rats, 70%) was significantly higher than that in WKY-2.7 % (0 of 11 rats, 0%) and WKY-9% (1 of 11 rats, 9.1%) respectively, while there were no changes between WKY-0.9% (2 of 11 rats, 18.2%) and SHRSP-0.9% (3 of 11 rats, 27.3%) (Fig. 1a). The mortality rate did not differ among the six groups (1 of 11 rats, 0.9%-WKY group; 0 of 11 rats, 2.7%-WKY group; 1 of 11 rats, 9%-WKY group; 2 of 11 rats, SHRSP-0.9% group; 0 of 10 rats, SHRSP-2.7% group, 1 of 10 rats; SHRSP-9% group) (Fig. 1b). The score of the symptom test at 3 weeks in the SHRSP-2.7% (4.5 [2.8–6], n = 10) and SHRSP-9% group (3.5 [2.5–6.0], n = 10) was significantly lower than that in the WKY-2.7% group (6.0 [6.0–6.0], n = 11) and WKY-9% group (6.0 [6.0–6.0], n = 11) respectively, while there was no changes between WKY-0.9% (6.0 [6.0–6.0], n = 11) and SHRSP-0.9% (6.0 [2.0–6.0], n = 11) (Fig. 1c).
Effect of systolic blood pressure and weight
No significant increase in blood pressure was observed between WKY and SHRSP groups with any ICV sodium concentration (Fig. 2a and Supplementary Fig. 2a). SHRSP demonstrated lower body weight than WKY before the start of experiment 2 (Supplementary Fig. 2b). The increase of body weight through 4 weeks in the SHRSP-2.7% (–5.7 [–48.6 to 39.9] g, n = 10) and 9%-SHRSP (–23.0 [–38.1 to 22.1] g, n = 9) groups was significantly lower compared with that in the WKY-2.7% (60.8 [40.7–66.8] g, n = 11) and WKY-9% (59.4 [50.3–72.4] g, n = 10) groups respectively, while there were no changes between WKY-0.9% (39.9 [33.3–50.9], n = 11) and SHRSP-0.9% (13.2 [–19.5 to 41.7], n = 11) (Fig. 2b).
Effect of neurological functions
There were no significant between-group differences in rotarod, while beam walking tests in SHRSP-2.7% (50.8 [0–68.8] s) group was lower than those in WKY-2.7% (56.7 [49.7–58.7] s) group (Fig. 3a, b).
Effect of serum sodium concentration
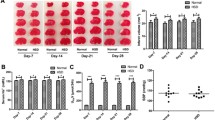
In comparison with the baseline sodium concentration of WKY (139.0 [139.0–139.0], n = 4) mEq/L and SHRSP (139.5 [138.3–140], n = 4) mEq/L, the values of sodium concentration were 140.0 [139.0–141.0] mEq/L in WKY-0.9% (n = 9), 144.0 [143.5–145.5] mEq/L in SHRSP-0.9% (n = 9), 138.0 [136.0–139.0] mEq/L in WKY-2.7% (n = 11), 142.0 [141.0–145.0] mEq/L in SHRSP-2.7% (n = 9), 136.5 [134.5–138.0] mEq/L in WKY-9% (n = 11), and 143.0 [139.5–144.5] mEq/L in SHRSP-9% (n = 9). The values in all groups were within normal range regardless of sodium concentration, but those in SHRSP were increased over 28 days and significantly higher than those in WKY in each ICV sodium concentration (Fig. 3c).
Effect of brain edema
Compared to the WKY groups, the BWCs of the SHRSP groups were significantly higher at the both baseline and endpoint (Table 1). However, the increase rate of SHRSP-2.7% and SHRSP-9% were significantly higher than that of WKY at each ICV sodium concentration.
Histological examination
Because no significant changes were observed in primary endpoints among WKY groups, we further used only WKY-0.9% as a control in the secondary endpoint. The number of total and resting microglia was not significantly different among the group, whereas the number of activated microglia was significantly higher in the SHRSP-9% group (87.6 [50.7–375.8] cells, n = 9) than in the WKY-0.9% group (35.7 [8.6–42.1] cells, n = 10) (Fig. 4a). We then evaluated skeleton analysis by quantifying the number of microglial process endpoints and length per cell to confirm the significant microglial activation, for which characteristics should be reduction of the endpoints and length [20]. The number of microglia process endpoints and length were significantly lower in the SHRSP-9% group (13.6 [11.4–15.9] and 9.7 [7.7–11.9], respectively) than those in WKY-0.9% group (19.4 [16.2–34.8] and 14.6 [13.3–25.9], respectively) (Supplementary Fig. 3). Brain superoxide levels detected by DHE staining was significantly higher in the SHRSP-2.7% group (133.4 [104.7–184.8] %, n = 10) and SHRSP-9% (157.7 [95.5–222.0] %, n = 9) compared to the 0.9%-WKY group (92.8 [83.5–113.7] %, n = 10) (Fig. 4b). The number of surviving neuronal cells detected by Nissl staining in SHRSP-9% (622.5 [283.6–819.7] cells, n = 9) were less than WKY-0.9% group (854.3 [747.6–1056.6] cells, n = 10) (Fig. 5a). Cerebral microbleeds (CMBs) detected by Prussian blue staining were significantly higher in the SHRSP-2.7% (4.5 [2.8–6.3], n = 10) and SHRSP-9% (7.0 [5.5–8.5], n = 9) groups than in the WKY-0.9% group (1.0 [0.8–2.3], n = 10) (Fig. 5b). In addition, higher sodium infusion significantly increased the number of activated microglia, superoxide, neuronal cell loss, and microbleeds compared to the SHRSP-0.9% group (Figs. 4 and 5 and Supplementary Fig. 3).
The number of total, resting, and activated microglia (a) and superoxide detected by dihydroethidium (b) in the left somatosensory cortex in experiment 2. SHRSP spontaneously hypertensive stroke-prone rat, WKY Wistar Kyoto rat. *p < 0.05 vs. WKY-0.9% and #p < 0.05 vs. SHRSP-0.9%. Bar indicates 200 µm
The number of surviving neuron detective by Nissl staining (a) in the left somatosensory cortex and number of microbleeds in the left hemisphere (b) in experiment 2. SHRSP spontaneously hypertensive stroke-prone rat, WKY Wistar Kyoto rat. *p < 0.05 vs. WKY-0.9% and #p < 0.05 vs. SHRSP-0.9%. Bar indicates 200 µm. Arrows indicate Prussian blue-positive microbleeds
Discussion
Our previous studies revealed that oral feeding of a high-sodium diet for 28 days significantly induced stroke onset in hypertensive rats, which was hypothesized to be due to the elevation of blood pressure and sympathetic activity [9, 13, 16]. These results encouraged us to explore whether persistent brain exposure to high sodium levels enhanced stroke onset. Therefore, we used hypertensive and normotensive rats and evaluated the effects of persistent brain exposure to multiple doses of sodium on stroke onset and related brain injuries. In comparison with normotensive animals, persistent ICV infusion with high sodium in hypertensive rats induced stroke onset and worsened morbidity, representing symptom score and poor weight gain, independently increased blood pressure. Additionally, the hypertensive animals exhibited brain edema and increased activated microglia, superoxide, neuronal cell loss, and microbleeds. Based on these findings, we suggest that continuous exposure of the brain to high sodium levels is a risk factor for stroke onset and related brain injuries in rats with a hypertensive background.
In experiment 2, our primary endpoint was significant, which represented a significant difference in the stroke onset and symptom test between SHRSP and WKY in 2.7 and 9% ICV sodium concentration, whereas there were no changes in the mortality rate in any group. As histological deteriorations were upregulated in the 2.7% and 9% SHRSP groups compared to the 0.9% WKY-0.9% and/or SHRSP-0.9% groups, we suspected that those brain injuries were associated with the phenotype of primary endpoint. Additionally, the values of serum sodium concentration were increased over 28 days in SHRSP only. Although we thought that the phenomena partially affected the stroke onset, the animals’ primary and secondary endpoints mainly represented the effects of exposure to higher sodium in the cerebral ventricle and the surrounding organs, rather than that in blood, given that the values of serum sodium concentration in SHRSP were increased regardless of ICV sodium concentration and also within normal range. Andersson et al. reported that the subfornical organ and organum vasculosum of the lamina terminalis in the anterior wall of the third ventricle were the sites of sodium sensing [26] and another study revealed that long-term ICV administration of hypertonic sodium solution induced sympathetic activation and blood pressure elevation through sodium channels in the organum vasculosum of the lamina terminalis [27]. Although we did not evaluate the parameters of sympathetic nerve activation nor showed significant increase of blood pressure by ICV infusion with high sodium, ICV infusion with high sodium might enhance deteriorative effects in SHRSP easily rather than WKY. Further research is needed to elucidate the mechanism of how ICV infusion with high sodium increases stroke onset in rats with hypertensive background by evaluating sympathetic nerve activation, etc.
Hypertensive rats showed increased serum sodium concentration which may not reflect dehydrate status, as no body weight reduction was observed in SHRSP. As blood sodium concentration levels at baseline were similar between WKY and SHRSP, we believe that the responses to ICV infusion with sodium differed between WKY and SHRSP, although we did not clarify why serum sodium concentration was significantly increased in only SHRSP. Contrastingly, BWC in SHRSP was significantly increased in comparison with WKY at both baseline and endpoint, while the increase rate of SHRSP-2.7% and SHRSP-9% were significantly higher than that of WKY at each ICV sodium concentration. The findings were consistent with the data observed at stroke onset, suggesting that ICV infusion with sodium induced significant brain edema which was associated with stroke onset. Although we did not clarify the mechanism further, we suspect that brain injuries by ICV infusion with sodium induced clinical and subclinical vasogenic edema by partially upregulating oxidative stress and microbleeds in hypertensive rats.
According to our secondary endpoint, the study showed upregulating CMBs and superoxide in the hypertensive rats with 2.7% and 9% sodium in comparison with WKY-0.9% and SHRSP-0.9%. The CMBs are thought to be correlated with the rupture of small arteries, arterioles, and/or capillaries and occurred by disruption of basement membrane [28]. As high sodium intake increased vascular superoxide level [29], we speculate that circulating sodium in CSF along with perivascular space upregulated cerebrovascular superoxide and disrupted basement membrane, resulting development of CMBs. On the other hand, microglia are resident innate immune cells. Resting microglia are activated by multiple pathological events, such as cerebral ischemia, transform into amoeba with large cell bodies, and play significant roles in oxidative stress and inflammatory responses [30]. Therefore, we suspect that ICV infusion with high sodium also activated microglia and participated in production of oxidative stress, resulting in CMBs induction and neuronal cell loss. However, it cannot be excluded that the activated microglia and increased oxidative stress were secondary to CMB induction and neuronal cell loss.
This study has limitations that must be acknowledged. First, we did not measure the sodium concentration in either urine or CSF. Second, stroke onset was observed in a few animals in the WKY-0.9% group, which we considered the control group. WKY feeding with a normal sodium diet did not represent stroke onset over 28 days, while stroke onset was observed in a few animals in the WKY-0.9% group in this study. We think the discrepancy might come from an unfavorable effect of the long-term ICV infusion procedure. However, persistent brain exposure to high sodium represented significant stroke onset, even when the confounding factors were taken into consideration.
Conclusions
In this study, we demonstrated that persistent brain exposure to high sodium levels increased stroke onset and morbidity, such as stroke-related symptoms and poor weight gain, in hypertensive rats. In addition, ICV infusion with high sodium upregulated CMBs and oxidative stress in hypertensive rats.
Data availability
The data that support the findings of this study are available from the corresponding author upon reasonable request.
References
Adams JM, Bardgett ME, Stocker SD. Ventral lamina terminalis mediates enhanced cardiovascular responses of rostral ventrolateral medulla neurons during increased dietary salt. Hypertension. 2009;54:308–14.
Farquhar WB, Edwards DG, Jurkovitz CT, Weintraub WS. Dietary sodium and health: more than just blood pressure. J Am Coll Cardiol. 2015;65:1042–50.
Stocker SD, Madden CJ, Sved AF. Excess dietary salt intake alters the excitability of central sympathetic networks. Physiol Behav. 2010;100:519–24.
Faraco G, Brea D, Garcia-Bonilla L, Wang G, Racchumi G, Chang H, et al. Dietary salt promotes neurovascular and cognitive dysfunction through a gut-initiated TH17 response. Nat Neurosci. 2018;21:240–9.
Chen QH, Toney GM. AT(1)-receptor blockade in the hypothalamic PVN reduces central hyperosmolality-induced renal sympathoexcitation. Am J Physiol Regul Integr Comp Physiol. 2001;281:R1844–53.
Toney GM, Chen QH, Cato MJ, Stocker SD. Central osmotic regulation of sympathetic nerve activity. Acta Physiol Scand. 2003;177:43–55.
Esler MD, Krum H, Sobotka PA, Schlaich MP, Schmieder RE, Böhm M. Renal sympathetic denervation in patients with treatment-resistant hypertension (The Symplicity HTN-2 Trial): a randomised controlled trial. Lancet. 2010;376:1903–9.
Hering D, Lambert EA, Marusic P, Walton AS, Krum H, Lambert GW, et al. Substantial reduction in single sympathetic nerve firing after renal denervation in patients with resistant hypertension. Hypertension. 2013;61:457–64.
Nakagawa T, Hasegawa Y, Uekawa K, Ma M, Katayama T, Sueta D, et al. Renal denervation prevents stroke and brain injury via attenuation of oxidative stress in hypertensive rats. J Am Heart Assoc. 2013;2:e000375.
Colonna M, Butovsky O. Microglia function in the central nervous system during health and neurodegeneration. Annu Rev Immunol. 2017;35:441–68.
Smykiewicz P, Segiet A, Keag M, Żera T. Proinflammatory cytokines and ageing of the cardiovascular-renal system. Mech Ageing Dev. 2018;175:35–45.
Subha M, Pal P, Pal GK, Habeebullah S, Adithan C, Sridhar MG. Decreased baroreflex sensitivity is linked to sympathovagal imbalance, low-grade inflammation, and oxidative stress in pregnancy-induced hypertension. Clin Exp Hypertens. 2016;38:666–72.
Hasegawa Y, Takemoto Y, Hayashi K, Kameno K, Kim-Mitsuyama S. The endogenous and exogenous brain-derived neurotrophic factor plays pivotal roles in the pathogenesis of stroke onset in high salt-loaded hypertensive rats. Exp Gerontol. 2021;147:111286.
Takane K, Hasegawa Y, Lin B, Koibuchi N, Cao C, Yokoo T, et al. Detrimental effects of centrally administered angiotensin II are enhanced in a mouse model of alzheimer disease independently of blood pressure. J Am Heart Assoc. 2017;6:e004897.
Takemoto Y, Hasegawa Y, Hayashi K, Cao C, Hamasaki T, Kawano T, et al. The stabilization of central sympathetic nerve activation by renal denervation prevents cerebral vasospasm after subarachnoid hemorrhage in rats. Transl Stroke Res. 2020;11:528–40.
Hasegawa Y, Nakagawa T, Uekawa K, Ma M, Lin B, Kusaka H, et al. Therapy with the combination of amlodipine and irbesartan has persistent preventative effects on stroke onset associated with BDNF preservation on cerebral vessels in hypertensive rats. Transl Stroke Res. 2016;7:79–87.
Kubota Y, Umegaki K, Kagota S, Tanaka N, Nakamura K, Kunitomo M, et al. Evaluation of blood pressure measured by tail-cuff methods (without heating) in spontaneously hypertensive rats. Biol Pharm Bull. 2006;29:1756–8.
Hayashi K, Hasegawa Y, Takemoto Y, Cao C, Takeya H, Komohara Y, et al. Continuous intracerebroventricular injection of Porphyromonas gingivalis lipopolysaccharide induces systemic organ dysfunction in a mouse model of Alzheimer’s disease. Exp Gerontol. 2019;120:1–5.
Ma M, Hasegawa Y, Koibuchi N, Toyama K, Uekawa K, Nakagawa T, et al. DPP-4 inhibition with linagliptin ameliorates cognitive impairment and brain atrophy induced by transient cerebral ischemia in type 2 diabetic mice. Cardiovasc Diabetol. 2015;14:54.
Smolek T, Cubinkova V, Brezovakova V, Valachova B, Szalay P, Zilka N, et al. Genetic background influences the propagation of tau pathology in transgenic rodent models of tauopathy. Front Aging Neurosci. 2019;11:343.
Morrison HW, Filosa JA. A quantitative spatiotemporal analysis of microglia morphology during ischemic stroke and reperfusion. J Neuroinflammation. 2013;10:4.
Young K, Morrison H. Quantifying microglia morphology from photomicrographs of immunohistochemistry prepared tissue using ImageJ. J Vis Exp. 2018:57648. https://doi.org/10.3791/57648.
Morrison H, Young K, Qureshi M, Rowe RK, Lifshitz J. Quantitative microglia analyses reveal diverse morphologic responses in the rat cortex after diffuse brain injury. Sci Rep. 2017;7:13211.
Lin B, Hasegawa Y, Takane K, Koibuchi N, Cao C, Kim-Mitsuyama S. High-fat-diet intake enhances cerebral amyloid angiopathy and cognitive impairment in a mouse model of Alzheimer’s disease, independently of metabolic disorders. J Am Heart Assoc. 2016;5:e003154.
Kim-Mitsuyama S, Yamamoto E, Tanaka T, Zhan Y, Izumi Y, Izumiya Y, et al. Critical role of angiotensin II in excess salt-induced brain oxidative stress of stroke-prone spontaneously hypertensive rats. Stroke. 2005;36:1083–8.
Andersson B. Thirst–and brain control of water balance. Am Sci. 1971;59:408–15.
Nomura K, Hiyama TY, Sakuta H, Matsuda T, Lin CH, Kobayashi K, et al. Na(+)] increases in body fluids sensed by central Na(x) induce sympathetically mediated blood pressure elevations via H(+)-dependent activation of ASIC1a. Neuron. 2019;101:60–75.e66.
Ungvari Z, Tarantini S, Kirkpatrick AC, Csiszar A, Prodan CI. Cerebral microhemorrhages: mechanisms, consequences, and prevention. Am J Physiol Heart Circ Physiol. 2017;312:H1128–43.
Koibuchi N, Hasegawa Y, Katayama T, Toyama K, Uekawa K, Sueta D, et al. DPP-4 inhibitor linagliptin ameliorates cardiovascular injury in salt-sensitive hypertensive rats independently of blood glucose and blood pressure. Cardiovasc Diabetol. 2014;13:157.
Li QQ, Li JY, Zhou M, Qin ZH, Sheng R. Targeting neuroinflammation to treat cerebral ischemia – the role of TIGAR/NADPH axis. Neurochem Int. 2021;148:105081.
Acknowledgements
We would like to thank Editage (www.editage.com) for English language editing.
Funding
This work was supported by research grants from The Salt Science Research Foundation (2034), JSPS KAKENHI (21K09193), and IUHW Research Grants.
Author information
Authors and Affiliations
Contributions
SK and YH contributed to study conception and design. SK, KF, ST, KK, and HU performed the experiments. YH performed the statistical analysis. MM helped with the interpretations. SK wrote the first draft of the manuscript. YH revised the manuscript. All authors reviewed and approved the manuscript.
Corresponding author
Ethics declarations
Ethics approval and consent to participate
All procedures performed in studies involving animals were conducted in accordance with the ethical standards of the institution or practice at which the studies conducted.
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kajiwara, S., Hasegawa, Y., Fujimori, K. et al. Persistent brain exposure to high sodium induces stroke onset by upregulation of cerebral microbleeds and oxidative stress in hypertensive rats. Hypertens Res 47, 78–87 (2024). https://doi.org/10.1038/s41440-023-01447-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41440-023-01447-z
- Springer Nature Singapore Pte Ltd.
Keywords
This article is cited by
-
Dietary salt promotes cognitive impairment through repression of SIRT3/PINK1-mediated mitophagy and fission
Molecular and Cellular Biochemistry (2024)
-
Brain sodium exposure: inducing stroke onset independent of blood pressure elevation in stroke-prone spontaneously hypertensive rats
Hypertension Research (2023)