Abstract
Among cancer immunotherapies, granulocyte–macrophage colony-stimulating factor (GM-CSF) gene-transduced tumor cell vaccine (GVAX) therapies appear promising and have been shown to be safe and effective in multiple clinical trials. However, the antitumor efficacies of GVAX therapy alone are in some cases limited. Here we showed that GVAX therapy targeting cancer stem cells (CSCs) substantially suppressed tumor development in syngeneic immunocompetent mice recapitulating normal immune systems. CSCs were isolated as side population (SP) cells from 4T1 murine breast carcinoma cell line and transduced with GM-CSF gene delivered by non-transmissible Sendai virus (4T1-SP/GM). Impaired tumorigenicity of subcutaneously injected 4T1-SP/GM depended on CD8+ T cells in concert with CD4+ T cells and natural killer cells. Mice therapeutically vaccinated with irradiated 4T1-SP/GM cells had markedly suppressed tumor development of subcutaneously transplanted 4T1-SP cells compared with those treated with irradiated cells of non-transduced 4T1-SP cells or non-SP (4T1-NSP/GM) cells. Tumor suppression was accompanied by the robust accumulation of mature dendritic cells at vaccination sites and T-helper type 1-skewed systemic cellular immunity. Our results suggested that CSC cell-based GVAX immunotherapy might be clinically useful for inducing potent tumor-specific antitumor immunity.
Similar content being viewed by others
Introduction
Cancer immunotherapy comprises diverse treatment modalities, which incorporate the specificities of both adaptive and innate immunity. Such therapies include the use of cancer cell vaccines, adoptive T-cell transfer of ex vivo-activated T cells and natural killer (NK) cells, and use with an adjuvant to costimulate immune cells.1 Among them, granulocyte–macrophage colony-stimulating factor (GM-CSF)-secreting cancer cell vaccines (GVAXs), which are genetically modified to produce GM-CSF protein and then irradiated (ir) to prevent further cell division, have been shown to induce successful antitumor immune responses in preclinical animal models.2, 3, 4, 5 Using whole cancer cells, GVAX induces immune responses against both unidentified and known tumor-associated antigens. Multiple clinical trial therapy in patients with solid and hematological cancers have demonstrated the feasibility, safety and objective immunological antitumor effects of GVAXs.6, 7, 8, 9 However, the antitumor efficacies of GVAX therapy alone are limited, probably because of several reasons, including the induction of myeloid-derived suppressor cell-mediated immune evasion by GM-CSF, which results in the reduced activity of cytotoxic T lymphocytes.10, 11
Cancer stem cells (CSCs), which constitute a small fraction of malignant tumors, are considered to establish an immunosuppressive tumor microenvironment that enables them to escape from host immune surveillance.12 We hypothesized that the introduction of a new cancer treatment targeting CSCs might provide a new opportunity to achieve a clinically beneficial outcome of GM-CSF. This urged us to investigate to what extent and how CSCs in tumors are susceptible to the GM-CSF-driven antitumor immunological responses remain ambiguous.
Most CSC-related studies have used human CSCs, which could only be xenogenetically transplanted into immunosuppressed mice; this is inadequate to assess the true immunogenicity of CSCs. In this study, we used syngeneic immunocompetent mice recapitulating normal immune systems and side population (SP) cells isolated from 4T1 murine breast carcinoma (4T1-SP) cells as putative CSCs. To develop CSC-based GVAX therapy toward more efficacious immunotherapeutic modalities for patients with advanced cancer, we explored whether mouse CSCs are susceptible to in vivo GM-CSF-driven antitumor immunity. The present animal models using enriched mouse SP cells and syngeneic immunocompetent mice will allow a deeper understanding of the interplay between CSC-like cells and host immune responses. Our study underscores the significance of using GM-CSF as a potent immunostimulatory adjuvant in SP cell-based immunotherapies that might improve antitumor effects in the clinical setting.
Materials and methods
Mice and cell culture
Female BALB/c mice aged 6–8 weeks (Charles River Laboratories Japan, Yokohama, Japan) were used for the in vivo experiments. All animal experiments were carried out under the Guidelines for Animal Experiments of Kyushu University and Law 105 Notification 6 of the Japanese Government. The mouse breast cancer cell line 4T1 was obtained from the American Type Culture Collection and maintained in RPMI-1640 supplemented with 10% fetal bovine serum (Sigma, St Louis, MO, USA) and 1% antibiotic–antimycotic mixed stock solution (Nacalai Tesque, Kyoto, Japan).
Fluorescence-activated cell sorting and SP analysis
Cell suspensions were labeled with Hoechst 33342 dye (Sigma) using the methods described by Goodell et al.13 with some modifications. Briefly, the cells were resuspended at 1 × 106 cells per ml in prewarmed RPMI-1640 supplemented with 2% fetal bovine serum and 10 mmol l−1 HEPES buffer. Hoechst 33342 dye was added to the cell suspensions at a final concentration of 5 μg ml−1 in the presence or absence of verapamil hydrochloride (150 μM; Sigma) and incubated at 37 °C for 1 h with intermittent shaking. To detect viable cells, propidium iodide (Nacalai Tesque) was added to the cells at a final concentration of 1 μg ml−1. Analyses and sorting were performed on either an Epics ALTRA (Beckman Coulter, Fullerton, CA, USA) or FACSAria II (Becton Dickinson, San Diego, CA, USA) flow cytometer. Flow cytometric data were analyzed by FlowJo software (Tree Star, Ashland, OR, USA).
Sendai virus-mediated gene transduction
For in vitro assays, 4T1-SP and 4T1-non-SP (NSP) cells were plated and treated with 100 μl serum-free solutions of non-transmissible Sendai viruses (SeV/dF/green fluorescent protein (GFP) or SeV/dF/GM) at predefined multiplicities of infection (MOIs). For in vivo assays, shortly after cell sorting, the cells were infected with 100 μl virus solution in suspension. After incubation for 1.5 h at 37 °C with intermittent shaking, the cells were washed two times with phosphate-buffered saline.
In vivo depletion assay
CD4+ or CD8+ T cells were depleted in BALB/c mice by intraperitoneally injecting each mouse with 50 μg anti-CD4 or anti-CD8 antibodies, or rat IgG 5, 4 and 3 days before and 3 days after tumor cell injection. Fluorescence-activated cell sorting analysis demonstrated that the respective treatments resulted in ~95% depletion of CD4+ or CD8+ T-cell populations in lymph nodes (data not shown). For NK cell depletion, mice were intraperitoneally injected with rabbit anti-asialo GM1 anti-serum (freeze-dried anti-serum diluted at 1:20 in phosphate-buffered saline; Wako, Osaka, Japan) 1 and 7 days before and every 7 days after tumor cell injection. 4T1-SP/GM cells were then subcutaneously injected into the right flank of mice. The tumor volume was calculated by the following formula: tumor (mm3)=(length) × (width)2 × 0.4. Animals were killed when the tumor diameter exceeded 1.5 cm.
In vivo therapeutic studies
On the day of tumor challenge, 1 × 104 sorted 4T1-SP cells were subcutaneously injected into the lower right flank of mice. On days 2 and 9 after tumor challenge, 2 × 104 tumor cells resuspended in 100 μl phosphate-buffered saline were subcutaneously injected into the upper right flank of mice. The tumor volume was measured once every other day.
Fluorescence-activated cell sorting analysis of the tumor vaccination site
Eighteen hours after the first vaccination, mice subcutaneously injected with ir.4T1-SP/GFP or ir.4T1-SP/GM cells were killed, and samples from the tumor vaccination sites (TVSs) were collected from each mouse. Mechanical homogenization was applied to prepare a single-cell suspension of the harvested TVS. To analyze the maturation level of dendritic cells (DCs) at the TVS, after blocking with anti-CD16/32 antibody, the cell suspensions were stained with anti-mouse CD80-phycoerythrin, CD11c-peridin chlorophyll protein/cyanine 5.5 (PerCP/cy5.5) and CD86-phycoerythrin/cyanine 7 (PE/cy7) antibodies. Analysis was carried out using FACSVerse.
Enzyme-linked immunospot assay
Antigen-specific responses were evaluated by a mouse immunospot kit (IFN-γ ELISPOT Kit; BD Pharmingen, Franklin Lakes, NJ, USA). Red blood cell-depleted splenocytes (1 × 105 cells) obtained from the spleens of mice vaccinated with ir.4T1-SP/GFP or ir.4T1-SP/GM cells were collected and incubated for 48 h at 37 °C with 5% CO2 in the presence or absence of ir.4T1-SP, ir.4T1-NSP or ir.CT26 cells at splenocyte:irradiated tumor cell ratios of 20:1 and 5:1 in a total volume of 200 μl. Phorbol 12-myristate 13-acetate (50 ng ml−1; Sigma) and ionomycin (1 μg ml−1) were added to cells as a positive control. ELISPOT plates were developed according to the manufacturer’s instructions. Color spots were counted using an automated ELISPOT analyzer (Cellular Technology, Cleveland, OH, USA).
Microarray analysis
cRNA was amplified, labeled using an Agilent Low-Input QuickAmp Labeling Kit (Agilent Technologies, Santa Clara, CA, USA) and then hybridized to a SurePrint G3 Mouse GE 8 × 60 K Microarray (Agilent Technologies) according to the manufacturer’s instructions. The hybridized microarray slides were scanned by an Agilent scanner, and the signals of all probes were calculated using the Feature Extraction Software (Agilent Technologies). Our data have been uploaded to the Gene Expression Omnibus database (accession number GSE53444). Transcripts with a fold change of >1.5 (upregulated in 4T1-SP cells) and a Z-score of >2 were considered to be significantly differentially expressed in each cell population. Microarray data analysis was supported by Cell Innovator (Fukuoka, Japan).
Real-time PCR analysis
RNA samples were isolated by RNeasy Kit (Qiagen, Hilden, Germany) and converted to cDNA by using RiverTra Ace qPCR RT Kit (Toyobo, Osaka, Japan) under the manufacturer' s guidance. Quantitative PCR was performed with Power SYBR PCR Master Mix (Thermo Fisher) in StepOne Plus System (Thermo Fisher). We especially focused on several important oncogenesis-related genes. PCR primers used were as follows: GAPDH F, 5′-AGGTCGGTGTGAACGGATTTG-3′ and GAPDH R, 5′-GGGGTCGTTGATGGCAACA-3′; Ccbp2 F, 5′-CCGGTCGTCTACAGCCTGA-3′ and Ccbp2 R, 5′-CATCGTCCGTCTTCGAGGT-3′; Ror1 F, 5′-TCCAAGAACCTCGGAGAATCT-3′ and Ror1 R, 5′-GAAGTAACCAGTGTCTGTGGTG-3′; Abcg2 F, 5′-GAACTCCAGAGCCGTTAGGAC-3′ and Abcg2 R, 5′-CAGAATAGCATTAAGGCCAGGTT-3′.
Statistical analysis
Statistical analyses were performed with the GraphPad Prism 5.0d software package (GraphPad Software, La Jolla, CA, USA). Statistical analysis among groups was performed using the two-tailed unpaired Student’s t-test, one-way analysis of variance, followed by Tukey’s multiple comparison test, or nonparametric Mann–Whitney U-test. P<0.05 was considered statistically significant.
Results
Mouse breast cancer 4T1-SP cell sub-population displays diverse CSC-related phenotypes
Because SP cells exhibit properties of both normal stem cells and CSCs,14, 15 we used the SP fraction as putative CSCs and the NSP fraction as non-CSCs, and isolated these distinct cell sub-populations from 4T1 cells. A characteristic SP fraction prestained with Hoechst 33342 dye was identified, which was defined by low fluorescence staining with both Hoechst 33342 blue and red filters. The SP fraction was abolished by adding verapamil, an inhibitor of ATP-binding cassette transporters including ABCG2. The SP fraction of 4T1 cells, 1–2% sub-population of the entire cell population (Figure 1a), was successfully isolated with >90% purity and >95% viability. 4T1-SP cells and the NSP fraction (4T1-NSP) were cultured for 2 days and then cell viability was evaluated. The number of propidium iodide-positive dead cells was not significantly different in the two distinctive cellular fractions (Figure 1b). To examine whether 4T1-SP cells possess the properties of CSCs, we firstly compared the clonogenic capacities of 4T1-SP and 4T1-NSP cells. 4T1-SP cells formed four times more colonies than 4T1-NSP cells did, indicating the higher clonogenic capacity of 4T1-SP cells (Figures 1c and d). The stem cell maker expression of stem cell antigen-1 (Sca-1) has been shown to enhance tumorigenicity, implicating its role as CSCs marker;16 we comparatively analyzed Sca-1 expression between 4T1-SP and 4T1-NSP cells. The Sca-1 expression level in 4T1-SP cells was significantly higher compared with that in 4T1-NSP cells (Figure 1e). Because CSCs exhibit higher chemoresistance,17, 18 we evaluated the chemoresistances of 4T1-SP and 4T1-NSP cells by anticancer agent docetaxel (DTX) exposure. 4T1-SP cells displayed significantly higher dose-dependent chemoresistance than 4T1-NSP cells did against DTX (Figure 1f). To evaluate tumorigenicity of 4T1-SP and 4T1-NSP cells, these cells ranging from 5 × 103 to 2 × 104 cells were subcutaneously injected into mice. As few as 5 × 103 of injected 4T1-SP cells developed significantly larger tumors than those of 4T1-NSP cells (P<0.05) (Figure 1g). All mice injected with 5 × 103 4T1-SP cells formed tumors, whereas only 16.7% of mice subcutaneously injected with 5 × 103 4T1-NSP cells formed tumors (Table 1). Collectively, these data demonstrated that 4T1-SP cells possessed several characteristic properties of CSCs both in vitro and in vivo, as reported earlier.15
Identification and characterization of SP cells using the Hoechst dye efflux assay. (a) 4T1 cells were stained with Hoechst 33342 dye in the presence (left) or absence (right) of verapamil. The SP fraction, which disappeared in the presence of verapamil, was gated and is shown as a percentage of the total viable cell population. (b) The frequency of dead cells was quantified by flow cytometry after culturing 4T1-SP and 4T1-NSP cells. Error bars represent the s.d. of the combined data from two independent experiments with similar results. (c and d) Comparison of the colony-forming abilities of 4T1-SP and 4T1-NSP cells. The colonies were fixed and stained with crystal violet and then photographed (c). The number of colonies derived from 4T1-SP and 4T1-NSP cells was counted in triplicate (d). Error bars represent the s.d. of two independent experiments (****P<0.0001). (e) Comparison of the expression levels of Sca-1 in 4T1-SP and 4T1-NSP cells by flow cytometry. Error bars represent the s.d. of the combined data from two independent experiments with similar results (***P<0.001). (f) 4T1-SP and 4T1-NSP cells were treated with 10–100 nM DTX. MTS assays were then performed to measure cell viability in response to DTX treatment (*P<0.05). (g) Tumorigenic potential of 4T1-SP cells. Subcutaneous tumor growth of 4T1-SP and 4T1-NSP cells (5 × 103 cells per mouse) in the right flank of mice was measured. The mean values and s.e.m. of tumor growth are depicted (*P<0.05 and **P<0.01). Representative data from two independent experiments with similar results are shown. DTX, docetaxel; MTS, 3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl-2H-tetrazolium bromide; NSP, non-SP; SP, side population.
Gene transduction mediated by SeV/dF infection does not affect 4T1 cell properties
We used SeV/dF as the gene transduction vector because the SeV receptors, sialic acid residues on cell surface glycoproteins (asialoglycoproteins), are expressed ubiquitously on most mammary cells and are safe and highly effective in gene transduction in panels of mouse and human cancer cells.19 To evaluate the gene transduction efficiency, 4T1-SP cells were infected with SeV/dF/GFP in vitro (4T1-SP/GFP cells). Substantial numbers of GFP+ 4T1-SP cells were detected at MOIs of 1–200, with peak expression at an MOI of 50 (Supplementary Figures S1a and b). Sufficient and comparable amounts of mouse GM-CSF and GFP proteins were produced from 4T1-SP and 4T1-NSP cells 72 h after infection with SeV/dF/GM (4T1-SP/GM and 4T1-NSP/GM, respectively) in a virus dose-dependent manner (Figure 2a and Supplementary Figures S1c and d). To exclude the possibility that the exogenous expression of GFP or GM-CSF gene by SeV affected 4T1-SP proliferation, growth curves of 4T1-SP, 4T1-SP/GFP or 4T1-SP/GM cells were evaluated. SeV/dF/GFP and SeV/dF/GM infection, even at the highest MOI of 100, showed negligible effects on the proliferation of 4T1-SP cells (Figure 2b).
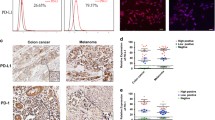
Transduction efficacy of the mGM-CSF gene and functional characterization of 4T1-SP cells as CSCs. (a) Cell culture supernatants from 4T1-SP cells infected with SeV/dF/GM at several MOIs were collected to measure the mGM-CSF concentration by ELISA. (b) 4T1-SP, 4T1-SP/GFP and 4T1-SP/GM cells were plated in 96-well plates at 1 × 103 cells per well. At each time point (days 1, 2, 3 and 4), MTS assays were performed to analyze the effect of SeV/dF/GFP or SeV/dF/GM infection on cell proliferation rates. Error bars represent the s.d. of triplicate experiments. (c–e) Expression levels of p-STAT3, VEGF and PD-L1 were quantified among 4T1-SP, 4T1-SP/GM, 4T1-NSP and 4T1-NSP/GM cells (MOI=100). Each cell lysate obtained was subjected to western blotting assay for p-STAT3 on Tyr705 detection. The cell lysate from MDA-MB-468, a human breast cancer cell line, was used as a positive control (PC) (c). After 72 h of culture, culture supernatants were harvested, and the expression levels of VEGF were measured (d). Error bars represent the s.d. of triplicate experiments (**P<0.01). 4T1-SP (black bar) and 4T1-NSP (white bar) cells were infected with SeV/dF/GM and cultured for 48 h. The expression level of PD-L1 was then quantified by flow cytometry (e). Error bars represent the s.d. of triplicate experiments (*P<0.05 and **P<0.01). CSC, cancer stem cell; ELISA, enzyme-linked immunosorbent assay; GFP, green fluorescent protein; mGM-CSF, mouse granulocyte–macrophage colony-stimulating factor; MOI, multiplicity of infection; MTS, (3-(4,5-dimethylthiazol-2-yl)-2,5-diphenyl-2H-tetrazolium bromide; NSP, non-SP; p-STAT, phosphorylated-signal transducer and activator of transcription 3; SP, side population; VEGF, vascular endothelial growth factor.
We then confirmed that immunosuppressive molecules expressed on 4T1 cells was not influenced by gene transduction by SeV/dF/GM. Signal transducer and activator of transcription 3 (STAT3) activation has been shown to result in the resistance of tumor cells to chemotherapeutic drugs and the expression level of vascular endothelial growth factor (VEGF) resulting in tumor angiogenesis.20, 21, 22 We measured the level of phosphorylated (p)-STAT3 in whole-tumor lysates derived from 4T1-SP and 4T1-NSP cells, as well as the production levels of VEGF in culture supernatants. Although 4T1-SP cells expressed higher levels of p-STAT3 and VEGF than 4T1-NSP cells did (P<0.01), no significant difference was found in p-STAT3 and VEGF levels between SeV/dF/GM-transduced group and -non-transduced group (Figures 2c and d). We then evaluated the expression level of the coinhibitory molecule PD-L1, which is well known to relate to aggressive characteristics of human malignancies with poor clinical prognosis.23 There was no significant difference in PD-L1 expression between SeV/dF/GM-transduced group and -non-transduced group, although isolated 4T1-SP cells expressed a significantly higher level of PD-L1 than 4T1-NSP cells (P<0.001) (Figure 2e).
GM-CSF gene-transduced 4T1-SP cell-based therapeutic vaccination significantly suppresses the tumor growth of subcutaneously transplanted 4T1-SP cells
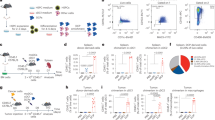
We next investigated the tumorigenicity of 4T1-SP/GM cells after the subcutaneous injection into immunocompetent mice. Remarkably, mice inoculated with 4T1-SP/GM cells voided the tumor development compared with those inoculated with 4T1-SP and 4T1-SP/GFP cells (Figure 3a), illustrating that genetic modification with GM-CSF on 4T1-SP cells conferred a significant impairment of their tumorigenicity. Furthermore, mice injected with 4T1-SP/GM cells survived longer than control mice did (Figure 3b). These data encouraged us to examine which immune cell sub-populations were directly involved in the GM-CSF-triggered loss of tumorigenicity, thus we depleted CD4+ T, CD8+ T or NK cells from mice. The tumor rejection observed in mice injected with 4T1-SP/GM cells was markedly abrogated in mice lacking CD8+ T, CD4+ T and NK cells (Figure 3c), indicating that both innate and adaptive immune cells contributed to the induction of SP cell-specific antitumor immunity.
Impaired tumorigenicity of subcutaneously injected 4T1-SP/GM cells and therapeutic antitumor effects of ir.4T1-SP/GM and ir.p4T1-SP/GM cell-based vaccines. (a and b) A total of 1 × 104 4T1-SP, 4T1-SP/GFP or 4T1-SP/GM cells were subcutaneously inoculated into BALB/c mice. (a) Tumor growth curves are shown as the means±s.e.m. (*P<0.05, **P<0.01 and ***P<0.001). (b) Kaplan–Meier survival curves are shown. Representative data from five independent experiments with similar results are shown. (c) BALB/c mice received intraperitoneal injections of indicated neutralization antibodies. Error bars represent the s.e.m. of the combined data from two independent experiments (**P<0.01). (d and e) Therapeutic tumor vaccination in mice subcutaneously transplanted with 4T1-SP cells. Each group received the indicated cellular vaccinations on days 2 and 9 after the tumor challenge. Tumor volumes of pre-established 4T1-SP cells are shown as the means±s.e.m. (*P<0.05) (d). Comparison of the therapeutic effects of ir.4T1-SP/GM and ir.4T1-NSP/GM cells (e). Error bars represent the s.e.m. of the combined data from three independent experiments with similar results. GFP, green fluorescent protein; GM, granulocyte–macrophage; NSP, non-SP; SP, side population.
We next hypothesized that therapeutic ir.4T1-SP/GM cell vaccination might induce superior antitumor immunity against pre-established 4T1-SP cell-derived tumors. We confirmed that ~10 ng of GM-CSF was produced by 1 × 106 4T1-SP/GM cells 8 h after SeV/dF/GM infection (Supplementary Figure S2), indicating that ir.4T1-SP/GM cells produced a sufficient amount of GM-CSF at the TVS. At days 2 and 9 after tumor challenge, ir.4T1-SP, ir.4T1-SP/GFP or ir.4T1-SP/GM vaccine cells were subcutaneously injected into mice. At 18 days after the tumor challenge, growth of 4T1-SP cell-derived tumors was significantly more suppressed in mice treated with ir.4T1-SP/GM cells than with ir.4T1-SP or ir.4T1-SP/GFP cells (P<0.05) (Figure 3d). We also confirmed that mice treated with ir.4T1-SP/GM cells showed prolonged survival compared with control mice without any severe adverse events (data not shown). In the same therapeutic vaccination, mice treated with ir.4T1-SP/GM cells showed a remarkably decreased number of metastatic lung nodules compared with control mice (Supplementary Figures S3a and b). We also demonstrated that ir.4T1-SP/GM cells were more effective than ir.4T1-NSP/GM cells to suppress tumor growth (Figure 3e).
To investigate the possible application of this method to primary tumors, we prepared putative primary 4T1-SP cells by freshly isolating cells from established tumors in 4T1-SP cell-transplanted immunocompetent mice (Supplementary Figure S4a). We genetically modified primary 4T1-SP cells by SeV/dF/GFP or SeV/dF/GM infection and irradiated them as described above (designated as ir.p4T1-SP/GFP and ir.p4T1-SP/GM cells). Mice injected with ir.p4T1-SP/GM cells markedly suppressed the tumor formation by challenge with 4T1-SP cells compared with control mice (Supplementary Figure S4b).
Mice treated with ir.4T1-SP/GM cells exhibit abundant mature DCs at the TVS and systemic antigen-specific T-helper type 1 responses
DCs harvested from mice vaccinated with ir.4T1-SP/GM cells expressed significantly higher levels of the costimulatory molecules CD80 and CD86 compared with control mice (P<0.01) (Figures 4a and b). Furthermore, to analyze whether antigen-specific T-helper type 1 cellular immune responses were induced in the therapeutic vaccination model, we quantified the number of IFN-γ-secreting splenocytes from mice vaccinated with ir.4T1-SP/GFP or ir.4T1-SP/GM cells after restimulation with ir.4T1-SP, ir.4T1-NSP or ir.CT26 cells as an irrelevant control. When cocultured in the presence of ir.4T1-SP and ir.4T1-NSP cells, but not ir.CT26 cells, the number of IFN-γ-producing splenocytes from mice vaccinated with ir.4T1-SP/GM cells was significantly higher compared with that of the controls (P<0.01) (Figure 4e and Supplementary Figure S5).
In vivo immunological assays during 4T1-SP cell-based therapeutic vaccinations. (a and b) Assessment of DC maturation at the TVS of mice treated with ir.4T1-SP/GFP or ir.4T1-SP/GM cells. Cell suspensions prepared from the TVS of indicated mouse groups were subjected to FACS analysis. Values represent the mean±s.e.m. of the frequencies (left panel) and mean fluorescence intensities (right panel) of CD80+ (a) and CD86+ (b) cells relative to the total CD11c+ cell population at the TVS. (c) Bar graphs representing the means±s.e.m. of the frequencies and CD80+CD86+ cells relative to the total CD11c+ cells. (d) Representative contour plots depicting CD80 and CD86 expression gated on CD11c+ cells. Representative data from two independent experiments with similar results are shown (**P<0.01 and ***P<0.001). (e) ELISPOT assay to quantify the number of IFN-γ-secreting splenocytes. At 10 days after the second 4T1-SP cell-based vaccination, splenocytes harvested from 4T1-SP tumor-bearing untreated mice or mice treated with the ir.4T1-SP/GFP or ir.4T1-SP/GM cells were cocultured with the indicated stimulator cells. Results are expressed as the mean number of spots±s.e.m. of triplicate determinations per 105 splenocytes (**P<0.01 and ***P<0.001). DC, dendritic cell; FACS, fluorescence-activated cell sorting; GM, granulocyte–macrophage; IFN, interferon; ir, irradiated; TVS, tumor vaccination site.
Genes related to metastasis, chemoresistance and invasion are more highly upregulated in 4T1-SP cells than in 4T1-NSP cells
Higher antitumor effect of 4T1-SP cells than 4T1-NSP cells promoted us to perform cDNA microarray analysis. Six hundred ninety-five genes were upregulated in 4T1-SP cells. Among them, we focused on the genes that had been previously reported as cancer-related genes, and their expression was restricted to either the plasma membrane or cytoplasm (Table 2). These genes included the genes categorized into subgroups based on their malignancy-related phenotypes such as prognostic markers in cancer patients, chemo- or radioresistance, metastasis and cellular proliferation (Figures 5a and b).
Heat map representing fold change patterns of the most highly differentially expressed genes in 4T1-SP cells. (a) A heat map was generated to compare fold-change patterns of the most highly differentially expressed genes in 4T1-SP cells, the likely cancer stem-like fraction and 4T1-NSP cells. The 10 most highly expressed genes were categorized into subgroups based on unfavorable cancerous phenotypes such as poor prognosis, metastasis, resistance to conventional therapies and cellular proliferation. Right panel (red): upregulated genes; left panel (green): downregulated genes. (b) Real-time PCR analysis to validate the result of microarray analysis. We especially focused on oncogenesis-related genes, and expression levels of the indicated genes in 4T1-SP cells compared with those in 4T1-NSP cells were calculated by relative quantification using the ddCt method with GAPDH as endogenous control. GAPDH, glyceraldehyde 3-phosphate dehydrogenase; NSP, non-SP; SP, side population.
Discussion
Breast cancer is the leading cause of death in women because of recurrence or metastasis after standard therapies, including surgery, chemotherapy and radiotherapy. The prognosis of patients with metastatic breast cancer remains poor, with a 5-year survival rate of 23.3%.24 Breast CSCs are a relatively rare sub-population of tumor cells that are resistant to conventional therapies and responsible for relapse or metastasis.25, 26, 27 Therefore, novel treatment approaches to specifically target breast CSCs are expected to induce long-term clinical benefits for patients with advanced breast cancer. To date, most of the studies investigating the CSC compartment isolated from human tumors or tumor cell lines have explored their high tumorigenic potential by transplantation into immune-compromised mice.28 However, in these mouse models, the xenografts may not fully recapitulate the activities of bona fide CSCs in human cancers29 as they lack adaptive immune responses, leading to failure of comprehensive immunological assessment.30 Therefore, to evaluate precisely the immunogenicity of CSCs in syngeneic immunocompetent hosts, we used purified mouse breast cancer 4T1-SP cells possessing diverse characteristics of CSCs as tumor antigen sources to fully prime adaptive immunity. We confirmed that 4T1-SP cells exhibited stem cell properties and immunoregulatory characteristics, as evidenced by their increased capacity to form colonies and high expression of Sca-1, p-STAT3, VEGF and PD-L1, which were not affected by genetic manipulation via SeV/dF/GM infection. One possible reason for the negligible influence by SeV/dF/GM transduction might be the fact that 4T1-SP cells did not express the GM-CSF receptor protein, thereby evading the paracrine effects of GM-CSF produced by the gene-transduced cells.
Despite the characteristics of 4T1-SP cells, such as low susceptibility to the cytotoxic effects of DTX, high tumorigenicity in mice and immunosuppressive phenotypes, 4T1-SP/GM cells strikingly lost their tumorigenicity in immunocompetent mice and induced strong immunostimulatory activities. As expected, CD8+ T cells (cytotoxic T lymphocytes) in mice injected with 4T1-SP/GM cells had a predominant role in exerting substantial antitumor immunity, supporting our previous findings that cytotoxic T lymphocytes act as the main effectors in GM-CSF-driven in vivo antitumor immunity, together with CD4+ T cells.2, 31 Importantly, we demonstrated that therapeutic vaccines comprised an irradiated GM-CSF-producing breast SP cell-enriched sub-population as the antigen source, conferring greater antitumor immunity than control vaccines of ir.4T1-NSP/GM cells did. These results suggest that CSC-associated antigens derived from SP cells appear to be more effective to induce therapeutic antitumor effects than unsorted cancer cells or surgically removed autologous tumor cells. The ELISPOT assay showed that CSC-associated antigen-specific T-helper type 1 cellular immunity was induced in ir.4T1-SP/GM cell-treated mice whose splenocytes produced a significantly higher IFN-γ. Furthermore, substantial therapeutic antitumor effects of vaccinations using GM-CSF-transduced primary 4T1-SP cells were observed. Notably, vaccination with ir.4T1-SP/GM cells efficiently inhibited lung metastasis. Collectively, SP cell-based GVAX therapy may provoke potent CSC-associated antigen-specific immune responses as an effective modality to improve the overall survival of patients with breast cancer by suppressing relapse and metastasis.
Only a few studies have reported that DC vaccine therapies using CSCs as antigen sources confer effective protective or therapeutic antitumor immunity in mouse or rat models.32, 33 Here we showed for the first time that a therapeutic strategy using GM-CSF-driven SP cell-based vaccines markedly suppressed tumor development by the challenge with isolated breast cancer SP cells through both enhanced innate and adaptive immunity. Our immunological findings suggested that DCs, which link the innate and adaptive arms of the immune system, were more mature at the TVS stimulated by vaccinations with ir.4T1-SP/GM cells than the control. However, further investigation is required to assess whether these mature DCs at the TVS effectively phagocytose CSC-associated antigens.
Because GM-CSF production from the 4T1-SP/GM cells was 1531 ng/1 × 106 cells per 72 h at an MOI of 10, probably equivalent to over 40 ng/1 × 106 cells per 48 h required for GVAX therapy to provoke in vivo antitumor immunity,34 it is conceivable that we detected substantial antitumor effects by ir.4T1-SP/GM cells. However, the antitumor effects need to be improved by modifying SP cell-based GVAX therapies with respect to administration route, frequency of administration, amount of mGM-CSF produced from cells and combinatorial use with other cytokines.35, 36, 37
Although we demonstrated that SP cell-based cell vaccines were effective in controlling tumor growth, it is very difficult to prepare sufficient number of SP cells as antigen sources from surgically removed tumor tissue because of the small SP cell fraction in primary tumors.38 Accordingly, the development of a new method to expand or amplify SP cells in vitro will be required to translate our findings to the clinical setting.
To ascertain potential CSC-associated antigens responsible for the superior antitumor effects of 4T1-SP cell-based vaccines compared with those of 4T1-NSP cell-based vaccines, cDNA microarray analysis was conducted to compare the gene expression profiles between 4T1-SP and 4T1-NSP cells. We selected the top 10 cancer-related genes predominantly expressed and localized in either the plasma membrane or cytoplasm of 4T1-SP cells as candidates for CSC-associated antigens, including Abcg2, well known as Hoechst 33342 efflux transporter.39 Among them, Ror1 (receptor tyrosine kinase-like orphan receptor), Ube2c (ubiquitin-conjugating enzyme E2C) and Galr1 (galanin receptor 1) have been shown to correlate with unfavorable cancerous characteristics such as metastasis,40, 41 poor prognosis42, 43 and chemoresistance44 in various human solid cancers, including breast cancer. Other candidate genes were Pbk (PDZ-binding kinase), which has recently been characterized as a novel cancer/testis antigen with oncogenic activity in breast cancer,45 and Nek2 (NIMA-related kinase 2), whose expression has been shown to be associated with disease recurrence in patients with breast cancers.46, 47 These findings underscore the possibility that these candidate genes might be promising antigenic targets for future immunotherapy to eradicate breast CSCs. Sca-1-specific T cells, for example, prominently expressed in 4T1-SP cells could be one of the putative CSC-associated antigen-specific T cells and might partially contribute to the observed antitumor effects by ir.4T1-SP/GM cell-driven vaccinations. However, further studies are warranted to validate the most critical gene responsible for breast CSC-directed antitumor immunity.
In conclusion, 4T1-SP cells with CSC phenotype elicited susceptibility to GM-CSF-driven antitumor responses in both in vivo tumorigenicity and therapeutic vaccination assays. Our animal models using enriched mouse SP cells and syngeneic immunocompetent mice will allow a deeper understanding of the mutual interplay between CSC-like cells and host immune responses, and enable us to develop a novel cancer immunotherapy exploiting GM-CSF gene-transduced cancer SP cells for improving the overall survival of cancer patients.
Accession codes
References
Mellman I, Coukos G, Dranoff G . Cancer immunotherapy comes of age. Nature 2011; 480: 480–489.
Dranoff G, Jaffee E, Lazenby A, Golumbek P, Levitsky H, Brose K et al. Vaccination with irradiated tumor cells engineered to secrete murine granulocyte–macrophage colony-stimulating factor stimulates potent, specific, and long-lasting anti-tumor immunity. Proc Natl Acad Sci USA 1993; 90: 3539–3543.
Armstrong CA, Botella R, Galloway TH, Murray N, Kramp JM, Song IS et al. Antitumor effects of granulocyte–macrophage colony-stimulating factor production by melanoma cells. Cancer Res 1996; 56: 2191–2198.
Sanda MG, Ayyagari SR, Jaffee EM, Epstein JI, Clift SL, Cohen LK et al. Demonstration of a rational strategy for human prostate cancer gene therapy. J Urol 1994; 151: 622–628.
Dunussi-Joannopoulos K, Dranoff G, Weinstein HJ, Ferrara JL, Bierer BE, Croop JM . Gene immunotherapy in murine acute myeloid leukemia: granulocyte–macrophage colony-stimulating factor tumor cell vaccines elicit more potent antitumor immunity compared with B7 family and other cytokine vaccines. Blood 1998; 91: 222–230.
Berns AJ, Clift S, Cohen LK, Donehower RC, Dranoff G, Hauda KM et al. Phase I study of non-replicating autologous tumor cell injections using cells prepared with or without GM-CSF gene transduction in patients with metastatic renal cell carcinoma. Hum Gene Ther 1995; 6: 347–368.
Ellem KA, O'Rourke MG, Johnson GR, Parry G, Misko IS, Schmidt CW et al. A case report: immune responses and clinical course of the first human use of granulocyte/macrophage-colony-stimulating-factor-transduced autologous melanoma cells for immunotherapy. Cancer Immunol Immunother 1997; 44: 10–20.
Nemunaitis J, Sterman D, Jablons D, Smith JW II, Fox B, Maples P et al. Granulocyte–macrophage colony-stimulating factor gene-modified autologous tumor vaccines in non-small-cell lung cancer. J Natl Cancer Inst 2004; 96: 326–331.
Simons JW, Mikhak B, Chang JF, DeMarzo AM, Carducci MA, Lim M et al. Induction of immunity to prostate cancer antigens: results of a clinical trial of vaccination with irradiated autologous prostate tumor cells engineered to secrete granulocyte–macrophage colony-stimulating factor using ex vivo gene transfer. Cancer Res 1999; 59: 5160–5168.
Serafini P, Carbley R, Noonan KA, Tan G, Bronte V, Borrello I . High-dose granulocyte–macrophage colony-stimulating factor-producing vaccines impair the immune response through the recruitment of myeloid suppressor cells. Cancer Res 2004; 64: 6337–6343.
Morales JK, Kmieciak M, Knutson KL, Bear HD, Manjili MH . GM-CSF is one of the main breast tumor-derived soluble factors involved in the differentiation of CD11b-Gr1− bone marrow progenitor cells into myeloid-derived suppressor cells. Breast Cancer Res Treat 2010; 123: 39–49.
Wei J, Barr J, Kong LY, Wang Y, Wu A, Sharma AK et al. Glioma-associated cancer-initiating cells induce immunosuppression. Clin Cancer Res 2010; 16: 461–473.
Goodell MA, Brose K, Paradis G, Conner AS, Mulligan RC . Isolation and functional properties of murine hematopoietic stem cells that are replicating in vivo. J Exp Med 1996; 183: 1797–1806.
Goodell MA, Jackson KA, Majka SM, Mi T, Wang H, Pocius J et al. Stem cell plasticity in muscle and bone marrow. Ann NY Acad Sci 2001; 938: 208–218; discussion 218–220.
Kruger JA, Kaplan CD, Luo Y, Zhou H, Markowitz D, Xiang R et al. Characterization of stem cell-like cancer cells in immune-competent mice. Blood 2006; 108: 3906–3912.
Upadhyay G, Yin Y, Yuan H, Li X, Derynck R, Glazer RI . Stem cell antigen-1 enhances tumorigenicity by disruption of growth differentiation factor-10 (GDF10)-dependent TGF-beta signaling. Proc Natl Acad Sci USA 2011; 108: 7820–7825.
Dean M, Fojo T, Bates S . Tumour stem cells and drug resistance. Nat Rev Cancer 2005; 5: 275–284.
Gangopadhyay S, Nandy A, Hor P, Mukhopadhyay A . Breast cancer stem cells: a novel therapeutic target. Clin Breast Cancer 2013; 13: 7–15.
Inoue H, Iga M, Nabeta H, Yokoo T, Suehiro Y, Okano S et al. Non-transmissible Sendai virus encoding granulocyte macrophage colony-stimulating factor is a novel and potent vector system for producing autologous tumor vaccines. Cancer Sci 2008; 99: 2315–2326.
Boehm AL, Sen M, Seethala R, Gooding WE, Freilino M, Wong SM et al. Combined targeting of epidermal growth factor receptor, signal transducer and activator of transcription-3, and Bcl-X(L) enhances antitumor effects in squamous cell carcinoma of the head and neck. Mol Pharmacol 2008; 73: 1632–1642.
Real PJ, Sierra A, De Juan A, Segovia JC, Lopez-Vega JM, Fernandez-Luna JL . Resistance to chemotherapy via Stat3-dependent overexpression of Bcl-2 in metastatic breast cancer cells. Oncogene 2002; 21: 7611–7618.
Niu G, Wright KL, Huang M, Song L, Haura E, Turkson J et al. Constitutive Stat3 activity up-regulates VEGF expression and tumor angiogenesis. Oncogene 2002; 21: 2000–2008.
Ito K, Ralph SJ . Inhibiting galectin-1 reduces murine lung metastasis with increased CD4(+) and CD8 (+) T cells and reduced cancer cell adherence. Clin Exp Metastasis 2012; 29: 763–778.
Siegel R, DeSantis C, Virgo K, Stein K, Mariotto A, Smith T et al. Cancer treatment and survivorship statistics, 2012. CA Cancer J Clin 2012; 62: 220–241.
Al-Hajj M, Wicha MS, Benito-Hernandez A, Morrison SJ, Clarke MF . Prospective identification of tumorigenic breast cancer cells. Proc Natl Acad Sci USA 2003; 100: 3983–3988.
Ponti D, Costa A, Zaffaroni N, Pratesi G, Petrangolini G, Coradini D et al. Isolation and in vitro propagation of tumorigenic breast cancer cells with stem/progenitor cell properties. Cancer Res 2005; 65: 5506–5511.
Fillmore CM, Kuperwasser C . Human breast cancer cell lines contain stem-like cells that self-renew, give rise to phenotypically diverse progeny and survive chemotherapy. Breast Cancer Res 2008; 10: R25.
Patrawala L, Calhoun T, Schneider-Broussard R, Zhou J, Claypool K, Tang DG . Side population is enriched in tumorigenic, stem-like cancer cells, whereas ABCG2+ and ABCG2− cancer cells are similarly tumorigenic. Cancer Res 2005; 65: 6207–6219.
Kuperwasser C, Chavarria T, Wu M, Magrane G, Gray JW, Carey L et al. Reconstruction of functionally normal and malignant human breast tissues in mice. Proc Natl Acad Sci USA 2004; 101: 4966–4971.
Wiseman BS, Werb Z . Stromal effects on mammary gland development and breast cancer. Science 2002; 296: 1046–1049.
Yokota Y, Inoue H, Matsumura Y, Nabeta H, Narusawa M, Watanabe A et al. Absence of LTB4/BLT1 axis facilitates generation of mouse GM-CSF-induced long-lasting antitumor immunologic memory by enhancing innate and adaptive immune systems. Blood 2012; 120: 3444–3454.
Ning N, Pan Q, Zheng F, Teitz-Tennenbaum S, Egenti M, Yet J et al. Cancer stem cell vaccination confers significant antitumor immunity. Cancer Res 2012; 72: 1853–1864.
Xu Q, Liu G, Yuan X, Xu M, Wang H, Ji J et al. Antigen-specific T-cell response from dendritic cell vaccination using cancer stem-like cell-associated antigens. Stem Cells 2009; 27: 1734–1740.
Hege KM, Jooss K, Pardoll D . GM-CSF gene-modifed cancer cell immunotherapies: of mice and men. Int Rev Immunol 2006; 25: 321–352.
Prell RA, Li B, Lin JM, VanRoey M, Jooss K . Administration of IFN-alpha enhances the efficacy of a granulocyte–macrophage colony stimulating factor-secreting tumor cell vaccine. Cancer Res 2005; 65: 2449–2456.
Inoue H, Iga M, Xin M, Asahi S, Nakamura T, Kurita R et al. TARC and RANTES enhance antitumor immunity induced by the GM-CSF-transduced tumor vaccine in a mouse tumor model. Cancer Immunol Immunother 2008; 57: 1399–1411.
Aruga A, Tanigawa K, Aruga E, Yu H, Chang AE . Enhanced adjuvant effect of granulocyte–macrophage colony-stimulating factor plus interleukin-12 compared with either alone in vaccine-induced tumor immunity. Cancer Gene Ther 1999; 6: 89–95.
Tirino V, Desiderio V, Paino F, De Rosa A, Papaccio F, La Noce M et al. Cancer stem cells in solid tumors: an overview and new approaches for their isolation and characterization. FASEB J 2013; 27: 13–24.
Scharenberg CW, Harkey MA, Torok-Storb B . The ABCG2 transporter is an efficient Hoechst 33342 efflux pump and is preferentially expressed by immature human hematopoietic progenitors. Blood 99: 507–512 2002.
Cui B, Zhang S, Chen L, Yu J, Widhopf GF II, Fecteau JF et al. Targeting ROR1 inhibits epithelial–mesenchymal transition and metastasis. Cancer Res 2013; 73: 3649–3660.
Klemm F, Bleckmann A, Siam L, Chuang HN, Rietkotter E, Behme D et al. Beta-catenin-independent WNT signaling in basal-like breast cancer and brain metastasis. Carcinogenesis 2011; 32: 434–442.
Psyrri A, Kalogeras KT, Kronenwett R, Wirtz RM, Batistatou A, Bournakis E et al. Prognostic significance of UBE2C mRNA expression in high-risk early breast cancer. A Hellenic Cooperative Oncology Group (HeCOG) Study. Ann Oncol 2012; 23: 1422–1427.
Parris TZ, Kovacs A, Aziz L, Hajizadeh S, Nemes S, Semaan M et al. Additive effect of the AZGP1, PIP, S100A8, and UBE2C molecular biomarkers improves outcome prediction in breast carcinoma. Int J Cancer 2013; 134: 1617–1629.
Stevenson L, Allen WL, Turkington R, Jithesh PV, Proutski I, Stewart G et al. Identification of galanin and its receptor GalR1 as novel determinants of resistance to chemotherapy and potential biomarkers in colorectal cancer. Clin Cancer Res 2012; 18: 5412–5426.
Park JH, Lin ML, Nishidate T, Nakamura Y, Katagiri T . PDZ-binding kinase/T-LAK cell-originated protein kinase, a putative cancer/testis antigen with an oncogenic activity in breast cancer. Cancer Res 2006; 66: 9186–9195.
Tsunoda N, Kokuryo T, Oda K, Senga T, Yokoyama Y, Nagino M et al. Nek2 as a novel molecular target for the treatment of breast carcinoma. Cancer Sci 2009; 100: 111–116.
Cappello P, Blaser H, Gorrini C, Lin DC, Elia AJ, Wakeham A et al. Role of Nek2 on centrosome duplication and aneuploidy in breast cancer cells. Oncogene 2014; 33: 2375–2384.
Acknowledgements
We thank Dr Kaori Yasuda and Dr Atsushi Doi (Cell Innovator) for their technical support in the microarray gene expression analysis. We also thank Michiko Ushijima, Haruka Yamato and the members of Dr Kenzaburo Tani’s laboratory for providing constructive criticism and technical assistance.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
KT receives research funding from SBI Pharmaceutical and Shinnihonseiyaku to develop novel cancer therapies. The terms of this arrangement have been reviewed and approved by the University of Tokyo in accordance with its conflict of interest policies. The other authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on Cancer Gene Therapy website
Supplementary information
Rights and permissions
About this article
Cite this article
Sakamoto, C., Kohara, H., Inoue, H. et al. Therapeutic vaccination based on side population cells transduced by the granulocyte–macrophage colony-stimulating factor gene elicits potent antitumor immunity. Cancer Gene Ther 24, 165–174 (2017). https://doi.org/10.1038/cgt.2016.80
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/cgt.2016.80
- Springer Nature America, Inc.