Abstract
Introduction
Transduction of the granulocyte-macrophage colony stimulating factor (GM-CSF) gene into mouse tumor cells abrogates their tumorigenicity in vivo. Our previous report demonstrated that gene transduction of GM-CSF with either TARC or RANTES chemokines suppressed in vivo tumor formation. In this paper, we examined whether the addition of either recombinant TARC or RANTES proteins to irradiated GM-CSF-transduced tumor vaccine cells enhanced antitumor immunity against established mouse tumor models to examine its future clinical application.
Materials and methods
Three million irradiated WEHI3B cells retrovirally transduced with murine GM-CSF cDNA in combination with either recombinant TARC or RANTES were subcutaneously inoculated into syngeneic WEHI3B-preestablished BALB/c mice.
Results
Vaccinations were well tolerated. Mice treated with GM-CSF-transduced cells and the chemokines demonstrated significantly longer survival than mice treated with GM-CSF-transduced cells alone. Splenocytes harvested from mice treated with the former vaccines produced higher levels of IL-4, IL-6, IFN-γ, and TNF-α, suggesting enhanced innate and adaptive immunity. Immunohistochemical analysis of tumor sections after vaccination revealed a more significant contribution of CD4+ and CD8+ T cells to tumor repression in the combined vaccine groups than controls.
Conclusions
TARC and RANTES enhance the immunological antitumor effect induced by GM-CSF in mouse WEHI3B tumor models and may be clinically useful.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Granulocyte-macrophage colony stimulating factor (GM-CSF) matures and differentiates dendritic cells (DCs) into functional antigen-presenting cells (APCs), and enhances their capacity to present tumor-associated antigens, effectively inducing an activation of tumor-specific cytotoxic T lymphocytes (CTLs) and augmenting antitumor immunity in mouse tumor models [11, 14, 17, 22, 26, 28, 34, 45]. Therefore, GM-CSF has been postulated to be one of the most potent immunostimulatory cytokine in the initial tumor immune response [7, 41]. However, the detailed molecular mechanism by which GM-CSF induces antitumor immunity is still unknown. In the past decade, clinical trials have shown that autologous GM-CSF-transduced tumor vaccines are feasible, safe, and effective therapies in melanoma [8, 40], renal cell carcinoma (RCC) [38, 44], prostate cancer [19, 39], and non-small cell lung cancer [12, 35]. Our previous clinical studies showed that GM-CSF-transduced tumor vaccines activated acquired immunity, indicated by skewed repertoires of the T cell receptor Vβ chain variables at tumors sites and delayed-type hypersensitivity at vaccination sites with eosinophil infiltation [44]. In spite of these positive immunological findings, the clinical benefits of this therapy alone are insufficient, and additional techniques are required to enhance GM-CSF gene therapy.
We previously analyzed gene expression profiles on temporarily transplanted tumor masses in vivo by serial analysis of gene expression (SAGE) to identify key molecules involved in this antitumor effect [29]. Our results revealed different gene expression levels between the parental and GM-CSF-transduced tumors and identified several molecules involved in the immune response. Among 20 candidate genes, we focused on the chemokine genes of TARC (thymus and activation-regulated chemokine, CCL17) and RANTES (regulated on activation, normal T-cell expressed and secreted, CCL5) [25], which were highly expressed in GM-CSF-transduced tumors. TARC is produced mainly by DCs and specifically chemoattracts Th2 T cells and DCs by binding to the CCR4 surface receptor expressed on Th2 T cells and DCs [16, 36]. RANTES is a CCL5 CC chemokine that is generated by various blood cells including DCs, and binds to the CCR1, CCR3, and CCR5 receptors. As CCR5 is expressed on Th1 cells as well as on macrophages, NK cells and immature DC, RANTES is categorized as both a Th1 cell recruitment mediator and a Th2 cell mediator by activating eosinophils and basophils through CCR3 [9, 20]. Our previous report demonstrated that co-transduction of GM-CSF and TARC/RANTES genes into tumor cells cooperatively inhibited tumor formation in vivo [29]. In this study, we examined whether the therapeutic antitumor effects of irradiated GM-CSF-transduced WEHI3B cells were enhanced by either TARC or RANTES in mouse WEHI3B tumor models to examine its future clinical application.
Materials and methods
Mice
Six- to seven-week-old female BALB/c immunocompetent mice and BALB/c severe combined immunodeficiency (SCID) mice were purchased from CLEA Japan, Inc. (Tokyo, Japan). Experiments were started with mice 7–8 weeks of age. All animal experiments were approved and performed according to the Guidelines of the Animal Ethics Committees of Kyushu University, Fukuoka, Japan. All animal experiments were performed at least twice to confirm results.
Tumor cells
WEHI3B cells, a murine myelomonocytic leukemia cell line obtained from Dr. D. Metcalf (University of Melbourne), were cultured in 5% CO2 at 37°C in RPMI 1640 medium (Gibco BRL, NY, US) supplemented with 10% heat-inactivated fetal bovine serum and antibiotics/antimycotics (Gibco BRL). RENCA cells, derived from a spontaneous renal cell carcinoma in a syngeneic BALB/c mouse, were kindly provided by Dr. Miyuki Azuma (Tokyo Medical and Dental University).
Establishment of GM-CSF-producing WEHI3B cells
Recombinant GM-CSF-transduced WEHI3B cell clones were established as previously described. Briefly, the cCRIP-MFG murine GM-CSF retrovirus producing cell line kindly provided by Richard Mulligan [7] was used to produce recombinant retroviruses; isolated retroviral supernatants were then co-cultivated with WEHI3B cells for 5 days. A single clone, producing high levels of GM-CSF (144 ng/24 h/106 cells), as measured by ELISA (BD Pharmingen, NJ, US), was obtained by limiting dilution and designated as WEHI3B/GM-CSF (W/GM).
Preparation of tumor vaccine cells and quantification of their cytokine production before and after irradiation
Using an established mouse skin cDNA library, we PCR amplified the chemokine cDNAs using specific primers for murine TARC and RANTES as previously described. These cDNAs were subcloned into the pCR4Blunt TOPO sequencing plasmid (Invitrogen, CA, US) to confirm cloning of the full-length cDNA sequences by nucleotide sequencing. These chemokine cDNAs were then subcloned into a retroviral vector (pMXneo). The recombinant pMXneo vectors were transduced using Lipofectamine (Invitrogen) into the Phoenix A retroviral packaging line, kindly provided by Dr. Toshio Kitamura (The University of Tokyo). Retroviral supernatants (viral solution) were harvested after 2 days of culture. W/GM cells (1 × 106) were then suspended and incubated in 1 ml of viral solution at 37°C for 1 h. After centrifugation, W/GM cells were cultured for two additional days in fresh medium. The medium was replaced with selective medium containing G418 (400 μg/ml) for an additional 7 days. Chemokine-transduced clones were selected by limiting dilution in selective medium. Cells producing high levels of chemokines were screened by ELISA (R&D systems, MN, US). Clonal W/GM cells containing TARC and RANTES were designated, respectively, as W/GM + T and W/GM + R.
Cloned cells W/GM, W/GM + T and W/GM + R were irradiated at 50 Gy using 137Cs source gamma cell 40 (Atomic Energy of Canada Limited, Ontario, Canada). These irradiated cells were then incubated for 24 h, suspended in 300 μl HBSS (Hank’s Buffer Salt Solution; Gibco BRL, NY, US) to 1 × 107 cells/ml, and inoculated subcutaneously (s.c.) into the left flank of mice as a tumor vaccine. The murine GM-CSF, TARC, and RANTES production levels in vitro were measured using the ELISA kits described above.
Tumor vaccination and tumor rechallenge
On the day of tumor challenge, 1 × 105 WEHI3B cells preliminarily cultured in vitro for 1–2 weeks were washed twice in PBS and injected s.c. into the right flank of immunocompetent BALB/c mice (n = 7 or 8/group), and the tumor volume was measured twice a week until the end of this experiment. As a treatment, 3 × 106 WEHI3B tumor vaccine cells resuspended in 300 μl HBSS, were injected subcutaneously into the left flank 3 days after tumor challenge then every 4 days for four treatments. The treatment groups included HBSS only, irradiated WEHI3B cells (irW), irradiated W/GM-CSF cells (irW/GM), irradiated W/GM + T cells (irW/GM + T), or irradiated W/GM + R cells (irW/GM + R). In the TARC and RANTES dose escalation study, 20, 60 and 200 ng of recombinant murine TARC (rmTARC) (R&D Systems, MN, US) or 50, 75, 100 and 150 ng of recombinant murine RANTES (rmRANTES) (R&D Systems, MN, US) mixed with 3 × 106 irW/GM cells, irW/GM cells alone, or 100 μl of HBSS were injected s.c. into the left flank of mice on days 3, 6, 9 and 12 after inoculation of 1 × 105 WEHI3B cells into the right flank of BALB/c mice. The products of perpendicular tumor diameters were calculated, plotted, and shown as the mean values and SEM (Bars). Survival was also monitored in WEHI3B-bearing mice and analyzed by a Kaplan–Meier curve. Two bisecting diameters of each tumor were measured with calipers. The tumor volume was calculated using the formula V = 0.4ab 2 with “a” as the larger diameter and “b” as the smaller diameter. Changes in tumor growth were monitored twice a week. Mice that responded and completely rejected the tumor with therapy were rechallenged on day 60 with an s.c. injection of 1 × 105 WEHI3B cells into the right flank and monitored in the same fashion. Mice with tumor burdens greater than 2,000 mm3 were killed and excluded from data for ethical reasons. The serum concentrations of murine TARC and RANTES were measured by ELISA as described above.
CTL assay
Splenocytes were prepared from euthanized tumor-bearing mice 8 days after the fourth tumor vaccinations (s.c. injection in the left flank of 3.0 × 106 irW, irW/GM, irW/GM + rmTARC 200 ng or irW/GM + rmRANTES 75 ng cells), and were depleted of erythrocytes with ammonium chloride. For CTL induction, splenocytes devoid of erythrocytes (4 × 106 cells/well) were co-cultured with mitomycin C-treated WEHI3B cells at a ratio of 10:1 in 1 ml of T cell culture medium (RPMI 1640 medium supplemented with 10% heat-inactivated FBS, antibiotics, and 50 μM 2-ME) in 24-well plates at 37°C in 5%CO2. Two days later, 30 U of recombinant human IL-2 (PeproTech EC, London, U.K.) was added to each well in 500 μl fresh culture medium. Splenocytes including CTLs were harvested on day 6 and used as effector cells in a standard 5 h 51Cr release assay to examine the antitumor cytolytic activity [37]. Briefly, WEHI3B cells as a target tumor and RENCA cells as a nonspecific target (1 × 106 cells) were labeled with 100 μCi of Na2 51CrO4 (PerkinElmer, Boston, MA, US) in 200 μl of RPMI 1640 supplemented with 10% heat-inactivated FBS for 90 min at 37°C. After three washes with PBS, the labeled target cells (1 × 104 cells/well) were incubated with the effector cells for 5 h at 37°C in 96-well round bottomed microtiter plates in 200 μl of T cell medium at the indicated E:T ratios. The plates were then centrifuged at 500 rpm for 5 min, and the radioactivity of the supernatants was measured with a(γ counter, Auto Well Gamma System (ALOKA, Tokyo, Japan). The maximum release and spontaneous release were determined from samples incubated with 1% Triton X-100 or medium alone, respectively. Cytolytic activity was calculated using the following formula: percentage of specific 51Cr release = (experimental release − spontaneous release) × 100/(maximum release − spontaneous release). Assays were performed in triplicate. The spontaneous release in all assays was <20% of the maximum release.
Mouse IFN-γ and IL-4 ELISPOT
In the course of tumor vaccination as described above, splenocytes from WEHI3B-bearing mice at 5 days after the fourth tumor vaccinations (s.c. injection in the left flank of HBSS, 3 × 106 irW/GM, irW/GM + rmTARC 200 ng or irW/GM + rmRANTES 75 ng cells) were tested for secretion of mouse IFN-γ and IL-4 using an ELISPOT assay kit (Cytokine ELISPOT Set, BD Pharmingen, NJ, US). ImmunoSpot™ ELISPOT 96-well plates were coated with 5 μl/ml of purified anti-mouse IFN-γ or anti-mouse IL-4 monoclonal antibody and incubated overnight at 4°C. Wells were washed with PBS containing 0.05% Tween 20 and incubated for 2 h with blocking buffer (RPMI 1640 with 10% FBS) at room temperature. RBC depleted splenocytes (1 × 105) were incubated in the presence or absence of irradiated WEHI3B cells at the indicated splenocyte:WEHI3B cell ratios (100:1, 50:1) in a total volume of 200 μl at 37°C with 5% CO2 for 20 h. As a positive control, PMA (Phorbol 12-myristate 13-acetate 20 ng/ml; Sigma, St Louis, MO, US), known as mitogen for T cell stimulation, was added to the indicated wells. After the plates were washed, the wells were incubated with 2 μl/ml of biotinylated anti-mouse IFN-γ or anti-mouse IL-4 monoclonal antibody for 2 h at room temperature. Then the plates were washed extensively and streptavidin-HRP solution was added for 1 h at room temperature. After washing the plates twice, Final Substrate Solution (AEC Substrate mixed with AEC Chromogen, BD Pharmingen, NJ, US) was added and spot development was monitored for about 5 min at room temperature. After drying, color spots indicating IFN-γ or IL-4-secreting cells were counted manually under a dissecting microscope and expressed as the mean number of spots+SD of quadruplicated determinations.
CBA and ELISA assay to quantitate mouse IL-2, IL-4, IL-5, IL-6, TNF-α, and IFN-γ production by splenocytes
In a similar fashion to ELISPOT, RBC depleted splenocytes (5 × 106) harvested from mice after the fourth vaccination were incubated in the presence or absence of irradiated WEHI3B cells at a 10:1 ratio in a total volume of 1.0 ml at 37°C for 20 h, and then culture supernatants were collected. The concentrations of mouse IL-2, IL-4, IL-5, TNF-α and IFN-γ in the supernatants were measured by the BD Mouse Th1/Th2 Cytokine CBA (Cytometric Bead Array) Kit (BD Pharmingen, NJ, US) according to the manufacturer’s protocol. The concentration of IL-6 was measured using a mouse IL-6 immunoassay kit (R&D Systems, MN, US) following the manufacturer’s instructions.
NK cell depletion in vivo
NK cells were depleted from BALB/c SCID mice by peritoneal injection of 200 μl rabbit anti-asialo GM1 anti-serum (freeze-dried anti-serum diluted 1:20 in PBS; Wako, Osaka, Japan), at 1 day before, and 7 and 14 days after tumor inoculation. As with the therapeutic protocol for immunocompetent BALB/c, indicated tumor vaccines were injected subcutaneously into the left flank a total of four times, once on every fourth day, starting 3 days after the tumor challenge (ten mice per group). Tumor growth and survival rates were assessed. Our previous results following the same experimental conditions confirmed NK cells elimination by the absence of splenocyte cytotoxic activity against YAC-1 cells (ATCC) in a standard 51Cr release assay [30].
Immunohistochemistry
Five days after the fourth tumor vaccinations (s.c. injection in the left flank of 3 × 106 irW, irW/GM, irW/GM + rmTARC 200 ng or irW/GM + rmRANTES 75 ng cells), implanted tumor tissues (n = 4/group) were snap frozen by overlaying with OCT compound (Sakura Fine Technical Co., Tokyo, Japan) and stored at −80°C until analysis. Serial cryostat (8 μm) frozen sections were adhered to Superfrost glass slides (Matsunami, Osaka, Japan), fixed in acetone at room temperature for 10 min, air-dried, and rinsed in distilled water to remove embedding medium. Staining was conducted following standard procedures. Briefly, sections were sequentially incubated overnight at 4°C with appropriately diluted primary antibodies, mouse CD4(GK1.5), CD8(53-6.7), CD11c(N418) (DCs), FoxP3(FJK-16s) (Tregs), CD45R/B220(RA3-6B2) (B cells), F4/80(BM8) (macrophages), and Ly-6G/Gr-1(RB6-8C5) (granulocytes) (all from eBioscience, San Diego, CA, USA) following the manufacturer’s instructions, followed by a 1-h incubation with biotinylated anti-rat or anti-hamster secondary Abs (eBioscience). After a 30-min incubation with streptavidin-peroxidase (Dako Japan Co. Ltd., Kyoto, Japan), Ag–Ab reactions were developed using 3, 3′-diaminobenzidine (Nakalai tesque, Kyoto, Japan) as a substrate. Slides were washed three times with PBS between each incubation step. Slides were counterstained with Mayer’s hematoxylin and dehydrated in sequentially degraded alcohol and xylene prior to mounting. All incubations were conducted in a humidified chamber. Photographs were taken with a Zeiss Axioskop 2 plus microscope (Zeiss, NY, US). The stained cells were counted microscopically at 100× magnification in 10–30 high-power fields. Results are presented as the means ± SD.
Flow cytometric analysis of helper T cells (Th1/Th2 balance) in the tumor and spleen
Five days after the fourth tumor vaccination (s.c. injection in the left flank of 3 × 106 irW, irW/GM, irW/GM + rmTARC 200 ng, or irW/GM + rmRANTES 75 ng), single cell suspensions of primary tumor and splenocytes were obtained from vaccinated mice (n = 3/group). Splenocytes and tumor cells were homogenized by mincing and filtered through a 70 μm cell strainer (BD Labware, NJ, US). The homogenized tumor was then digested with collagenase IV (GIBCO) in RPMI 1640 for 90 min at 37°C with continuous stirring. The splenocytes and tumor infiltrating cells (TILs) were then isolated from tumor cells/erythrocytes by centrifuging the cell suspension on a Lympholyte M gradient (CEDARLANE, Ontario, Canada) following the manufacturer’s protocol. The resulting single cell suspensions were washed twice with 1% FBS in PBS and stained for flow cytometry. Splenocytes and TILs were stimulated with PMA (40 ng/ml) (Sigma) and ionomycin (1 μg/ml) (Sigma) for 5 h. Two hours before harvesting, the cells were treated with brefeldin A (50 μg/ml, eBioscience) to retain cytoplasmic cytokines. After washing twice in a fluorescent antibody buffer (FAB) consisting of 0.1% bovine serum albumin and 0.02% sodium azide in 0.01 M PBS (pH 7.2), cells were pretreated with FcR (CD16/32) block followed by an APC-conjugated anti-CD4 mAb for 30 min. Subsequently, cells were fixed with 2% paraformaldehyde and then stained intracellularly with FITC-conjugated IFN-γ and PE-conjugated IL-4 mAb in permeabilization buffer (eBioscience) for 1 h at room temperature. All mAbs were purchased from eBioscience. Stained cells were washed three times in FAB and analyzed by multiparameter flow cytometry using a Becton Dickinson FACS Calibur (San Jose, CA). Dead cells were excluded by the FSC/SCC profiles. Surface marker profiles were analyzed using CELLQUEST Software (Becton Dickinson) and the percentages of positive cells were determined.
Statistical analysis
Except for the animal survival data, statistical analyses were performed using Student’s t tests. The P values were obtained from two-tailed tests of statistical significance. A Kaplan–Meier curve was used to analyze survival rates, and the statistical relevance was determined using a log-rank comparison. A probability value was considered significant when P < 0.05.
Results
In vivo antitumor effect of irradiated WEHI3B cells producing GM-CSF plus either murine TARC or murine RANTES
We previously reported that mice inoculated s.c. with non-irradiated WEHI3B cells transduced with GM-CSF plus TARC or RANTES exhibited a significantly better survival rate than mice injected with GM-CSF-transduced WEHI3B cells [29]. In this study, the hypothesis whether irW/GM + T or irW/GM + R provided additional antitumor immunity compared to irW/GM was examined. Prior to vaccination, the production of murine GM-CSF, TARC and RANTES from WEHI3B, W/GM, W/GM + T and W/GM + R cells before and 24 h after irradiation was compared to evaluate the influence of irradiation on the production of transduced cytokine genes. There were no striking differences in cytokine production before and after irradiation (Table 1). A total of 1 × 105 of parental WEHI3B cells were injected subcutaneously into the right flank of immunocompetent BALB/c mice. On day 3, 3 × 106 each of irW, irW/GM, irW/GM + T and irW/GM + R were injected s.c. into the left flank of mice every 4 days for four treatments and monitored periodically for 60 days (Fig. 1). At day 27, posttumor inoculation irW/GM significantly inhibited tumor growth compared to irW (P < 0.05). irW/GM + T and irW/GM + R induced a slightly better, although not statistically significant, antitumor effect compared with those induced by irW/GM. Interestingly, the irW/GM + T group had significantly better survival than irW/GM alone (P < 0.05). On day 60 postinoculation, some mice in each therapeutic group had completely rejected tumor formation. In the irW/GM + T group, five of the seven mice rejected the tumor development and showed a longer survival compared with that of both the irW/GM and irW/GM + R groups. Furthermore, when rechallenged with 1 × 105 parental WEHI3B cells s.c. into the right flank, three of the fiive irW/GM + T-treated mice that rejected the original WEHI3B tumor, also rejected the second WEHI3B challenge. In contrast, mice treated with either irW/GM or irW/GM + R rejecting the primary tumor challenge died within 25 days after the rechallenge of WEHI3B cells (Table 2).
Therapeutic antitumor effects of irW/GM, irW/GM + T, or irW/GM + R cells on preestablished tumors. A total of 1 × 105 WEHI3B cells were inoculated s.c. into the right flank of BALB/c mice on day 0. Next, 3 × 106 irW, irW/GM, irW/GM + T, or irW/GM + R cells or 100 μl of HBSS were injected s.c. into the left flank of mice on days 3, 6, 9 and 12. The products of perpendicular tumor diameters were calculated and plotted. The mean products and SEM (bars) are depicted (a). Kaplan–Meier analyses of WEHI3B-bearing mice are shown (b) (*P < 0.05). Data are representative of two independent experiments, with similar results
Both recombinant murine TARC and RANTES enhanced the antitumor effects of irW/GM in mice with established tumors
We then conducted a dose escalation test of rmTARC or rmRANTES mixed with irW/GM cells against pre-established tumors to determine the appropriate dose of TARC or RANTES to enhance the antitumor effect of irW/GM. Three days after the injection of 1 × 106 WEHI3B cells, 3 × 106 irW/GM cells containing either rmTARC (20, 60, 200 ng/mouse) or rmRANTES (50, 75, 100, 150 ng/mouse) were s.c. inoculated into the left flank every 4 days for four treatments, and tumor growth and survival rate were monitored. On day 26, mice treated with irW/GM + rmTARC suppressed WEHI3B growth in an rmTARC dose dependent manner, with a significant additional antitumor effect compared to irW/GM vaccinated mice (P < 0.05) (Fig. 2a). Mice vaccinated with irW/GM + rmTARC at 60 ng and especially 200 ng rmTARC had significantly prolonged survival compared to control mice vaccinated with or without irW/GM, all of which died within 37 days (P < 0.05) (Fig. 2c). Furthermore, 1, 2 and 4 mice vaccinated, respectively, with irW/GM + rmTARC 20, 60 and 200 ng completely rejected tumor formation (Table 3). On day 26, the mice vaccinated with irW/GM + rmRANTES 75 ng suppressed WEHI3B growth most significantly among the rmRANTES treated mice, and three mice completely eradicated their tumors. In contrast, none of the eight mice treated with HBSS or irW/GM rejected tumor challenge. Mice vaccinated with irW/GM + rmRANTES 50, 75, and 100 ng, had significantly prolonged survival compared with control mice vaccinated with or without irW/GM (P < 0.05) (Fig. 2d). Interestingly, a rmRANTES dose of 75 ng per mouse was the optimal dose that promoted antitumor immunity. Moreover, four of eight and three of seven mice vaccinated with irW/GM + rmTARC 200 ng and irW/GM + rmRANTES 75 ng, respectively, were rechallenged as described above, and two of four, and two of three respective mice with rejected tumors survived for more than 60 additional days without tumors (Table 3). The serum concentrations of murine TARC 4 h (2,338.55 ± 168.01 pg/ml) and murine RANTES 2 h (713.99 ± 118.04 pg/ml) after s.c. tumor vaccination with irW/GM + rmTARC 200 ng and irW/GM + rmRANTES 75 ng, respectively, were measured by ELISA. During the vaccinations, mice were well tolerated without any major adverse events.
Therapeutic antitumor effects of irW/GM, irW/GM + rmTARC (20, 60, 200 ng) or irW/GM + rmRANTES (50, 75, 100, 150 ng) cells on pre-established tumors. A total of 1 × 105 WEHI3B cells were implanted s.c. into the right flank of BALB/c mice on day 0. Next, irW/GM, irW/GM + rmTARC (20, 60, 200 ng), irW/GM + rmRANTES (50, 75, 100, 150 ng) cells or 100 μl of HBSS were injected s.c. into the left flank of mice on days 3, 6, 9 and 12. The products of perpendicular tumor diameters were calculated and plotted. The mean products and SEM (bars) are depicted (a, b). Kaplan–Meier analyses of WEHI3B-bearing mice are shown (c, d) (*P < 0.05). Data are representative of two independent experiments, with similar results
Splenocytes from mice vaccinated with irW/GM in combination with either rmTARC or rmRANTES had enhanced antitumor cytotoxicity in vitro
To investigate the mechanism underlying the enhanced specific antitumor immunity by TARC and RANTES, we examined the cytotoxic activity of splenocytes from vaccinated mice against WEHI3B cells in vitro. Murine renal carcinoma (RENCA) cells were used as negative control target cells. Splenocytes of mice vaccinated with irW/GM in combination with rmTARC 200 ng or rmRANTES 75 ng demonstrated more than 20% cytotoxicity against WEHI3B cells at 100:1, 50:1, or 25:1 E/T ratios, showing higher cytolytic activity compared to splenocytes from mice vaccinated with irW/GM alone. In contrast, splenocytes from mice vaccinated with irW/GM with or without rmTARC or rmRANTES exhibited no or lower cytotoxicity against RENCA cells at the indicated E/T ratios. Splenocytes from mice vaccinated with irW demonstrated minimal ability to lyse both WEHI3B cells and RENCA cells at each effector/target ratio tested (Fig. 3).
CTL activity of tumor-bearing mice that received different tumor vaccinations described above. Eight days after the fourth tumor vaccination, splenocytes were harvested from vaccinated mice and used as CTL effector cells in a 51Cr release assay as described in “Materials and methods”. 51Cr labeled WEHI3B cells were used as target cells (a) and RENCA cells were used as nonspecific target cells (b). Cytolytic activity against WEHI3B cells was higher in mice vaccinated with irW/GM plus rmTARC 200 ng or rmRANTES 75 ng compared with mice vaccinated with irW/GM alone (a), whereas no cytolytic effect was observed when RENCA cells were used as target cells (b). The values represent the mean ± SEM (standard error of the mean) of percentage cytotoxicity from four independent experiments
ELISPOT assay and in vitro cytokine production profile of splenocytes from mice vaccinated with irW/GM cells in combination with either rmTARC or rmRANTES
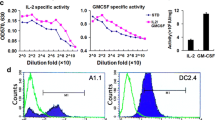
As RANTES and TARC are presumed to recruit or activate Th1 and Th2 T cells in a pathway dependent on the respective CCR4 and CCR5 receptors, we harvested splenocytes from mice receiving HBSS, irW/GM cells with or without rmTARC 200 ng or rmRANTES 75 ng and performed in vitro IFN-γ and IL-4 ELISPOT assays. In the presence of irradiated WEHI3B cells, the numbers of spot-forming IFN-γ or IL-4 secreting splenocytes from tumor-bearing mice treated with irW/GM + rmTARC or rmRANTES were significantly higher than those from mice treated with HBSS or irW/GM (P < 0.05) (Fig. 4a, b).
a, b Induction of WEHI3B tumor-specific splenocytes after s.c. injection of irW/GM in combination with either rmTARC 200 ng or rmRANTES 75 ng was evaluated by mouse IFN-γ (a) and IL-4 (b) ELISPOT assays. A total of 1 × 105 splenocytes from tumor-bearing mice vaccinated with the indicated transfected cells were incubated in 200 μl RPMI 1640 with 10% FBS in ImmunoSpot™ 96-well plates coated with anti-IFN-γ or anti-IL-4 mAb. After a 20 h co-incubation with stimulator cells (RENCA cells were used as negative control) at the indicated ratios, the plates were washed and bound cytokines were visualized by incubating with biotinylated anti-IFN-γ or anti-IL-4 mAb, followed by streptavidin-HRP or premixed peroxidase substrate AEC. Results are expressed as the mean number of spot-forming cells + SD of quadruplicate determinations per 106 splenocytes. (c–h) In vitro cytokine secretion of splenocytes from mice treated with the tumor vaccines described above. Splenocytes were harvested from mice 5 days after the last tumor vaccine and then cultured with or without irradiated WEHI3B stimulator cells. Twenty hours after a mixed lymphocytes/tumor culture was started, the concentrations of mouse TNF-α (c), IFN-γ (d), IL-2 (e), IL-4 (f), IL-5 (g) in the culture supernatants were measured. The concentration of IL-6 (h) was measured using a mouse IL-6 immunoassay ELISA kit. *P < 0.05 when compared with the indicated group
Next, we determined the in vitro cytokine production profiles of mice treated with irW/GM cells in combination with either rmTARC 200 ng or rmRANTES 75 ng Irradiated WEHI3B cells were used as stimulator cells. After 20 h of co-culture, the supernatants were collected and IL-2, IL-4, IL-5, IL-6, IFN-γ and TNF-α levels were measured by CBA or ELISA assay. As seen in the ELISPOT assay, IFN-γ and IL-4 production were significantly higher in the mice treated with irW/GM + rmTARC or irW/GM + rmRANTES than irW/GM (P < 0.05) (Fig. 4d, f). Additionally, a significantly higher production of TNF-α and IL-6 was observed in the mice treated with irW/GM + rmTARC or irW/GM + rmRANTES (P < 0.05) (Fig. 4c, h). The production of IL-4 and IL-6 was significantly higher in the mice treated with irW/GM + rmRANTES 75 ng than irW/GM + rmTARC 200 ng (P < 0.05) (Fig. 4f, h). IL-2 and IL-5 levels were already elevated in the mice treated with irW/GM with or without chemokines and further activation was not induced when splenocytes were co-cultured with restimulator cells (Fig. 4e, g).
In vivo antitumor efficacy of irW/GM cells in combination with either rmTARC or rmRANTES in tumor implanted SCID mice
To determine if the additional effects of rmTARC or rmRANTES in combination with GM-CSF in syngeneic immunocompetent mice were mediated by adaptive immunity, we performed in vivo studies using syngeneic BALB/c SCID mice. Three days after subcutaneous injection of 1 × 105 of WEHI3B into the right flank of SCID mice, 3 × 106 each of irW, irW/GM, irW/GM + rmTARC 200 ng, or irW/GM + rmRANTES 75 ng were subcutaneously injected into the left flank of mice every 4 days for four treatments. Interestingly, only mice treated with irW/GM + rmRANTES 75 ng had significantly retarded tumor growth and revealed better survival than mice treated with irW, irW/GM or irW/GM + rmTARC 200 ng (P < 0.05) (Fig. 5a, b). However, all treated mice succumbed to death within 26 days. As SCID mice retain innate immune systems including NK cells and mononuclear cells, we treated SCID mice with intraperitoneal injections of anti-asialo GM1 anti-serum to abrogate NK cell function and to investigate the contribution of NK cells to the tumor suppression by irW/GM + rmRANTES. The NK-depleted mice treated with irW/GM + rmRANTES had faster tumor growth than controls and SCID mice treated with irW/GM + rmRANTES (P < 0.05) (Fig. 5c, d).
a, b A total of 1 × 105 WEHI3B cells were s.c. injected into the right flank of syngeneic BALB/c SCID mice. Three days later, 3 × 106 each of irW, irW/GM, irW/GM + rmTARC 200 ng, or irW/GM + rmRANTES 75 ng were s.c. injected into the left flank every 4 days for four treatments (n = 10/group). Mice treated with irW/GM + rmRANTES 75 ng had significantly suppressed tumor growth (a) and prolonged survival (b). (c, d) NK cells depletion assay. BALB/c SCID mice received peritoneal injections of rabbit anti-asialo GM1 anti-serum, at 1 day before, and 7 and 14 days after tumor inoculation (n = 8/group). In NK-depleted mice, the additional antitumor effects including prolonged survival by rmRANTES disappeared. Significant differences are denoted with asterisks (*P < 0.05)
Immunohistochemical findings of tumor infiltrating cells in tumor masses during tumor vaccination
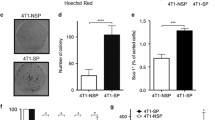
During the course of the tumor vaccination studies, we killed four mice with retarded tumor growth in each vaccination group. The distribution of leukocyte subtypes in the tumor infiltrating cells was analyzed by immunohistochemical (IHC) staining. IHC analysis revealed a significantly greater number of infiltrating CD8+ T cells and CD11+ cells in mice vaccinated with irW/GM than irW (P < 0.05). The number of CD4+ T cells and CD8+ T cells was significantly increased in mice treated with irW/GM + rmTARC 200 ng and irW/GM + rmRANTES 75 ng compared with irW/GM alone (P < 0.05). The number of CD11c+ cells and CD45R/B220+ cells was also significantly increased in mice treated with irW/GM + rmTARC 200 ng than irW/GM (P < 0.05). On the other hand, the number of Ly-6G/Gr-1+ cells was significantly increased, while that of FoxP3+ cells was significantly decreased in mice treated with irW/GM + rmRANTES 75 ng than irW/GM (P < 0.05). F4/80+ cell (macrophage) infiltration also increased in the vaccinated groups, but was not statistically different compared with irW (Fig. 6a).
a Immunophenotypic analysis of tumor-infiltrating cells (TIL) in tumor nodules. Mice were injected s.c. with 1 × 105 non-irradiated WEHI3B cells and treated with the indicated tumor vaccine cells as described in “Materials and methods”. Excised tumors were subjected to immunohistological evaluation. To determine the proportions of CD4+, CD8+, CD11c+, FoxP3+, CD45R+, F4/80+ or Ly-6G+ cells, stained cells were counted microscopically at ×100 in 10–30 HPF. Results are presented as the means ± SEM. Significant differences are denoted with asterisks (*P < 0.05). b, c Th1/Th2 cell cytokine secretion profiles in the tumor (b) and spleen (c) of mice that received therapeutic tumor vaccination. Tumor-bearing mice (n = 3/experiment) were treated with the indicated tumor vaccine cells and killed as described in the immunophenotypic analysis. Single cell suspensions from the primary tumor and spleen were obtained and cultured with PMA and ionomycin for 5 h in the presence of brefeldin A. Cells were harvested and labeled with APC-conjugated anti-CD4 followed by FITC anti-IFN-γ and PE-conjugated anti-IL-4. Gates were set on CD4+ T cell populations, and intracellular cytokine staining profiles within these populations were assessed by multicolor flow cytometry. Numbers indicate the percentages of specified TILs secreting intracellular IFN-γ (Th1) and IL-4 (Th2). Data are averages of two independent experiments with similar results
Cytokine secretion profiles of CD4+ T Cells in the tumor and spleen during tumor vaccination
To examine the effect of chemokines (TARC and RANTES) on GM-CSF based tumor vaccination, we next assessed the profiles of cytokines secreted by CD4+ TIL subpopulations from the sites of primary tumor growth and the spleen on the same day as the IHC analysis. Th1 (IFN-γ) and Th2 (IL-4) cell cytokine profiles (recruitment/accumulation of Th1/Th2 in TILs) were analyzed at the single cell level by intracellular staining and flow cytometry, and the percentages of Th1 and Th2 cells in the tumor (TILs) and spleen were calculated. In mice that were treated with irW/GM cells, there were slightly greater numbers of Th2 cells in the TILs, and rmTARC further enhanced the proportion of Th2 cells. In contrast, the addition of rmRANTES shifted the balance to predominantly Th1 cells. In the spleen, the Th1/Th2 balance in the three groups was similar to that observed in the TILs, but was even more enhanced (Fig. 6b, c).
Discussion
This study, along with our previous studies [29], shows that co-administration of the chemokines TARC or RANTES with irW/GM has additional antitumor effects and is considered to be useful possible applications to enhance the antitumor effects of GM-CSF-transduced tumor vaccines. Our results of in vitro CTL, ELISPOT and ELISA assays using splenocytes harvested from mice immunized with irW/GM mixed with TARC or RANTES suggested that the antigen-specific adaptive immunity induced by GM-CSF secreting vaccine cells was mediated by the production of cytokines, including IFN-γ, IL-4, TNF-α, and IL-6. In addition, our results of immunohistochemical analysis supported these findings by demonstrating a significant increase in CD4+ and CD8+ T cell infiltration in tumors of mice treated with both irW/GM + rmTARC and irW/GM + rmRANTES compared with those treated with irW/GM alone.
GM-CSF released from genetically engineered tumor cells enhances tumor antigen presentation by leading to the local accumulation of DCs, the most important APC, in and around the vaccination site. TARC, RANTES or other chemokines and cytokines are thought to act synergistically with GM-CSF to recruit immature DCs to vaccination sites where they uptake tumor antigens. These mediators also present a “danger signal” that activates antitumor immunity by recruiting Th1 and Th2 cells to the vaccination site and draining lymph nodes, contributing to the interaction of effector T cells with tumor cells [13, 31, 43]. Indeed, TARC and RANTES are proinflammatory cytokines involved in the chemoattraction of a number of different effector cell types. Activation of innate and acquired immunity by a combination of cytokines and chemokines would help enhance antitumor immune responses in vivo. This hypothesis is supported by our in vivo NK depletion studies demonstrating that the antitumor effects of rmRANTES with irW/GM were induced by T cells and partially by NK cells. Interestingly, our observations suggested that an optimal amount of RANTES might augment NK cell cytolytic activity on malignant cells [33]. Actually CCR5, one of the RANTES receptors, is expressed on macrophages, NK cells, DCs, and activated Th1 cells [24]. After binding to CCR5, RANTES potently chemoattracts monocytes/macrophages, NK cells, and CTLs, resulting in tumor lysis through the release of granule enzymes [23, 27]. Similar combination effects were also observed in an antivirus vaccine study. Sumida et al. [42] demonstrated that coadministration of the chemokine macrophage inflammatory protein-1 (MIP-1α) expression plasmid DNA vaccine with DC-specific growth factor fms-like tyrosine kinase3 ligand resulted in the recruitment, expansion, and activation of large numbers of DCs at the inoculation site and induced remarkable cellular and humoral antiviral immunity. Furthermore, our results on the Th1/Th2 balance in the tumor and spleen demonstrated that RANTES shifted the dominant Th2 balance induced by GM-CSF based tumor vaccination to a Th1 dominant condition through local and systemic Th1 cell accumulation. These results suggested that rmRANTES augmented not only Th1 cellular immunity against WEHI3B cells but also NK cell activation.
Results of our in vitro immunological cytokine assays using splenocytes harvested from mice immunized with irW/GM mixed with rmTARC or rmRANTES also suggested that the antigen-specific adaptive immunity induced by GM-CSF secreting cells was potentiated through the production of IFN-γ, IL-2, IL-4, IL-5, IL-6, and TNF-α. Elevated IL-4 and IL-5 produced from splenocytes treated with irW/GM + rmTARC suggested that additional rmTARC might enhance systemic Th2 dominant responses through the activation of eosinophils, which are putatively involved in GM-CSF antitumor responses [3, 4, 40]. Indeed, our analysis of the Th1/Th2 balance supported the hypothesis. Since the combination of GM-CSF with IL-4 was efficient in generating DCs from hematopoietic precursors in vitro [2], localized production of GM-CSF and IL-4 induced by either rmTARC or rmRANTES may potentiate the antitumor effects induced by GM-CSF alone in vivo [10]. Miller et al. [26] reported that GM-CSF-recruited DCs expressed higher levels of both TNF-α and IL-6 than controls, resulting in potent T cell and NK cell activation. Furthermore, TNF-α enhanced the capacity of bone marrow-derived DCs to generate antitumor effects and CTL responses [1].
IL-6 enhanced an autologous tumor cell vaccine that secreted GM-CSF in a mouse RCC therapeutic model [21]. A recent report showed that IL-6 is essential to overcome immune suppression mediated by CD4+CD25+ regulatory T cells (Tregs) [32] and to induce hematopoiesis and acute phase inflammation [15, 32], partially by blocking signaling that facilitates Tregs expansion [5]. Accordingly, our results suggest that both TARC and RANTES in combination with GM-CSF may interfere with the suppressive effects of Tregs, by enhancing IL-6 secretion and creating a microenvironment that does not support tumor growth. However, it is still possible that TARC attracts CCR4+ Treg cells [18]. Our immunohistochemical analysis showing less FoxP3+ positive cells in tumors from mice treated with both irW/GM + rmTARC and irW/GM + rmRANTES further suggests that IL-6 is necessary to suppress Tregs expansion.
We have demonstrated the vaccine efficacy of GM-CSF-transduced tumor cells (auto-GVAX) in preclinical and clinical settings. Particularly, two of four patients had long-term survival greater 5 years with low dose IL-2 and one patient survived more than 8 years in PS0. The combination of auto-GVAX with other immune therapies is thought to potentiate the tumor specific immunity of auto-GVAX. The combination of GVAX with a neutralizing antibody to cytotoxic T lymphocyte antigen-4 (CTLA-4) is one of the strong candidates [6]. In this study, we demonstrated that TARC and RANTES enhanced antitumor immunity induced by GM-CSF, most likely by augmenting dominant Th2 and Th1 T cell immune responses, respectively, in mouse WEHI3B tumor models. These results also suggest that these chemokines have a clinical application in tumor vaccination. Namely, GVAX vaccination with the addition of either recombinant RANTES and/or TARC expression vectors is a promising second-generation GVAX gene therapy candidate. This latter novel gene therapy is currently under investigation using several viral vectors. In this regimen, GVAX may effectively enhance immune recognition of tumor antigens via DC activation and subsequent migration of activated T cells into the tumor tissue, leading to tumor eradication. Further preclinical investigations using different malignant cells types are required to prove this hypothesis.
Abbreviations
- GM-CSF:
-
Granulocyte-macrophage colony stimulating factor
- TARC:
-
Thymus and activation-regulated chemokine
- RANTES:
-
Regulated on activation, normal T-cell expressed and secreted
- APCs:
-
Antigen-presenting cells
References
Brunner C, Seiderer J, Schlamp A, Bidlingmaier M, Eigler A, Haimerl W, Lehr HA, Krieg AM, Hartmann G, Endres S (2000) Enhanced dendritic cell maturation by TNF-alpha or cytidine-phosphate-guanosine DNA drives T cell activation in vitro and therapeutic anti-tumor immune responses in vivo. J Immunol 165:6278
Caux C, Dezutter-Dambuyant C, Schmitt D, Banchereau J (1992) GM-CSF and TNF-alpha cooperate in the generation of dendritic Langerhans cells. Nature 360:258
Chu Y, Xia M, Lin Y, Li A, Wang Y, Liu R, Xiong S (2006) Th2-dominated antitumor immunity induced by DNA immunization with the genes coding for a basal core peptide PDTRP and GM-CSF. Cancer Gene Ther 13:510
Costello R, O’Callaghan T, Sebahoun G (2005) [Eosinophils and antitumour response]. Rev Med Interne 26:479
Doganci A, Eigenbrod T, Krug N, De Sanctis GT, Hausding M, Erpenbeck VJ, Haddad el B, Lehr HA, Schmitt E, Bopp T, Kallen KJ, Herz U, Schmitt S, Luft C, Hecht O, Hohlfeld JM, Ito H, Nishimoto N, Yoshizaki K, Kishimoto T, Rose-John S, Renz H, Neurath MF, Galle PR, Finotto S (2005) The IL-6R alpha chain controls lung CD4+CD25+ Treg development and function during allergic airway inflammation in vivo. J Clin Invest 115:313
Dranoff G (2005) CTLA-4 blockade: unveiling immune regulation. J Clin Oncol 23:662
Dranoff G, Jaffee E, Lazenby A, Golumbek P, Levitsky H, Brose K, Jackson V, Hamada H, Pardoll D, Mulligan RC (1993) Vaccination with irradiated tumor cells engineered to secrete murine granulocyte-macrophage colony-stimulating factor stimulates potent, specific, and long-lasting anti-tumor immunity. Proc Natl Acad Sci USA 90:3539
Ellem KA, O’Rourke MG, Johnson GR, Parry G, Misko IS, Schmidt CW, Parsons PG, Burrows SR, Cross S, Fell A, Li CL, Bell JR, Dubois PJ, Moss DJ, Good MF, Kelso A, Cohen LK, Dranoff G, Mulligan RC (1997) A case report: immune responses and clinical course of the first human use of granulocyte/macrophage-colony-stimulating-factor-transduced autologous melanoma cells for immunotherapy. Cancer Immunol Immunother 44:10
Elsner J, Escher SE, Forssmann U (2004) Chemokine receptor antagonists: a novel therapeutic approach in allergic diseases. Allergy 59:1243
Fujii S, Hamada H, Fujimoto K, Shimomura T, Kawakita M (1999) Activated dendritic cells from bone marrow cells of mice receiving cytokine-expressing tumor cells are associated with the enhanced survival of mice bearing syngeneic tumors. Blood 93:4328
Granucci F, Girolomoni G, Lutz MB, Ricciardi-Castagnoli P (1995) Recombinant GM-CSF induces cytokine production in mouse dendritic cell clones. Adv Exp Med Biol 378:31
Hege KM, Carbone DP (2003) Lung cancer vaccines and gene therapy. Lung Cancer 41(Suppl 1):S103
Hege KM, Jooss K, Pardoll D (2006) GM-CSF gene-modifed cancer cell immunotherapies: of mice and men. Int Rev Immunol 25:321
Heufler C, Koch F, Schuler G (1988) Granulocyte/macrophage colony-stimulating factor and interleukin 1 mediate the maturation of murine epidermal Langerhans cells into potent immunostimulatory dendritic cells. J Exp Med 167:700
Hirano T (1998) Interleukin 6 and its receptor: ten years later. Int Rev Immunol 16:249
Imai T, Nagira M, Takagi S, Kakizaki M, Nishimura M, Wang J, Gray PW, Matsushima K, Yoshie O (1999) Selective recruitment of CCR4-bearing Th2 cells toward antigen-presenting cells by the CC chemokines thymus and activation-regulated chemokine and macrophage-derived chemokine. Int Immunol 11:81
Inaba K, Inaba M, Romani N, Aya H, Deguchi M, Ikehara S, Muramatsu S, Steinman RM (1992) Generation of large numbers of dendritic cells from mouse bone marrow cultures supplemented with granulocyte/macrophage colony-stimulating factor. J Exp Med 176:1693
Ishida T, Ueda R (2006) CCR4 as a novel molecular target for immunotherapy of cancer. Cancer Sci 97:1139
Jaffee EM, Hruban RH, Biedrzycki B, Laheru D, Schepers K, Sauter PR, Goemann M, Coleman J, Grochow L, Donehower RC, Lillemoe KD, O’Reilly S, Abrams RA, Pardoll DM, Cameron JL, Yeo CJ (2001) Novel allogeneic granulocyte-macrophage colony-stimulating factor-secreting tumor vaccine for pancreatic cancer: a phase I trial of safety and immune activation. J Clin Oncol 19:145
Kato Y, Pawankar R, Kimura Y, Kawana S (2006) Increased expression of RANTES, CCR3 and CCR5 in the lesional skin of patients with atopic eczema. Int Arch Allergy Immunol 139:245
Kinoshita Y, Kono T, Yasumoto R, Kishimoto T, Wang CY, Haas GP, Nishisaka N (2001) Antitumor effect on murine renal cell carcinoma by autologous tumor vaccines genetically modified with granulocyte-macrophage colony-stimulating factor and interleukin-6 cells. J Immunother 24:205
Levitsky HI, Montgomery J, Ahmadzadeh M, Staveley-O’Carroll K, Guarnieri F, Longo DL, Kwak LW (1996) Immunization with granulocyte-macrophage colony-stimulating factor-transduced, but not B7-1-transduced, lymphoma cells primes idiotype-specific T cells and generates potent systemic antitumor immunity. J Immunol 156:3858
Loetscher P, Seitz M, Clark-Lewis I, Baggiolini M, Moser B (1996) Activation of NK cells by CC chemokines. Chemotaxis, Ca2+ mobilization, and enzyme release. J Immunol 156:322
Loetscher P, Uguccioni M, Bordoli L, Baggiolini M, Moser B, Chizzolini C, Dayer JM (1998) CCR5 is characteristic of Th1 lymphocytes. Nature 391:344
Mantovani A, Sica A, Sozzani S, Allavena P, Vecchi A, Locati M (2004) The chemokine system in diverse forms of macrophage activation and polarization. Trends Immunol 25:677
Miller G, Pillarisetty VG, Shah AB, Lahrs S, Xing Z, DeMatteo RP (2002) Endogenous granulocyte-macrophage colony-stimulating factor overexpression in vivo results in the long-term recruitment of a distinct dendritic cell population with enhanced immunostimulatory function. J Immunol 169:2875
Murphy PM (2002) International Union of Pharmacology. XXX. Update on chemokine receptor nomenclature. Pharmacol Rev 54:227
Nagai E, Ogawa T, Kielian T, Ikubo A, Suzuki T (1998) Irradiated tumor cells adenovirally engineered to secrete granulocyte/macrophage-colony-stimulating factor establish antitumor immunity and eliminate pre-existing tumors in syngeneic mice. Cancer Immunol Immunother 47:72
Nakazaki Y, Hase H, Inoue H, Beppu Y, Meng XK, Sakaguchi G, Kurita R, Asano S, Nakamura Y, Tani K (2006) Serial analysis of gene expression in progressing and regressing mouse tumors implicates the involvement of RANTES and TARC in antitumor immune responses. Mol Ther 14:599
Nakazaki Y, Tani K, Lin ZT, Sumimoto H, Hibino H, Tanabe T, Wu MS, Izawa K, Hase H, Takahashi S, Tojo A, Azuma M, Hamada H, Mori S, Asano S (1998) Vaccine effect of granulocyte-macrophage colony-stimulating factor or CD80 gene-transduced murine hematopoietic tumor cells and their cooperative enhancement of antitumor immunity. Gene Ther 5:1355
Pardoll D (2003) Does the immune system see tumors as foreign or self? Annu Rev Immunol 21:807
Pasare C, Medzhitov R (2003) Toll pathway-dependent blockade of CD4+CD25+ T cell-mediated suppression by dendritic cells. Science 299:1033
Robertson MJ, Ritz J (1990) Biology and clinical relevance of human natural killer cells. Blood 76:2421
Romani N, Kampgen E, Koch F, Heufler C, Schuler G (1990) Dendritic cell production of cytokines and responses to cytokines. Int Rev Immunol 6:151
Salgia R, Lynch T, Skarin A, Lucca J, Lynch C, Jung K, Hodi FS, Jaklitsch M, Mentzer S, Swanson S, Lukanich J, Bueno R, Wain J, Mathisen D, Wright C, Fidias P, Donahue D, Clift S, Hardy S, Neuberg D, Mulligan R, Webb I, Sugarbaker D, Mihm M, Dranoff G (2003) Vaccination with irradiated autologous tumor cells engineered to secrete granulocyte-macrophage colony-stimulating factor augments antitumor immunity in some patients with metastatic non-small-cell lung carcinoma. J Clin Oncol 21:624
Schaniel C, Sallusto F, Ruedl C, Sideras P, Melchers F, Rolink AG (1999) Three chemokines with potential functions in T lymphocyte-independent and -dependent B lymphocyte stimulation. Eur J Immunol 29:2934
Shibata S, Okano S, Yonemitsu Y, Onimaru M, Sata S, Nagata-Takeshita H, Inoue M, Zhu T, Hasegawa M, Moroi Y, Furue M, Sueishi K (2006) Induction of efficient antitumor immunity using dendritic cells activated by recombinant Sendai virus and its modulation by exogenous IFN-beta gene. J Immunol 177:3564
Simons JW, Jaffee EM, Weber CE, Levitsky HI, Nelson WG, Carducci MA, Lazenby AJ, Cohen LK, Finn CC, Clift SM, Hauda KM, Beck LA, Leiferman KM, Owens AH Jr, Piantadosi S, Dranoff G, Mulligan RC, Pardoll DM, Marshall FF (1997) Bioactivity of autologous irradiated renal cell carcinoma vaccines generated by ex vivo granulocyte-macrophage colony-stimulating factor gene transfer. Cancer Res 57:1537
Simons JW, Mikhak B, Chang JF, DeMarzo AM, Carducci MA, Lim M, Weber CE, Baccala AA, Goemann MA, Clift SM, Ando DG, Levitsky HI, Cohen LK, Sanda MG, Mulligan RC, Partin AW, Carter HB, Piantadosi S, Marshall FF, Nelson WG (1999) Induction of immunity to prostate cancer antigens: results of a clinical trial of vaccination with irradiated autologous prostate tumor cells engineered to secrete granulocyte-macrophage colony-stimulating factor using ex vivo gene transfer. Cancer Res 59:5160
Soiffer R, Lynch T, Mihm M, Jung K, Rhuda C, Schmollinger JC, Hodi FS, Liebster L, Lam P, Mentzer S, Singer S, Tanabe KK, Cosimi AB, Duda R, Sober A, Bhan A, Daley J, Neuberg D, Parry G, Rokovich J, Richards L, Drayer J, Berns A, Clift S, Cohen LK, Mulligan RC, Dranoff G (1998) Vaccination with irradiated autologous melanoma cells engineered to secrete human granulocyte-macrophage colony-stimulating factor generates potent antitumor immunity in patients with metastatic melanoma. Proc Natl Acad Sci USA 95:13141
Steinman RM, Witmer-Pack M, Inaba K (1993) Dendritic cells: antigen presentation, accessory function and clinical relevance. Adv Exp Med Biol 329:1
Sumida SM, McKay PF, Truitt DM, Kishko MG, Arthur JC, Seaman MS, Jackson SS, Gorgone DA, Lifton MA, Letvin NL, Barouch DH (2004) Recruitment and expansion of dendritic cells in vivo potentiate the immunogenicity of plasmid DNA vaccines. J Clin Invest 114:1334
Tan JK, O’Neill HC (2005) Maturation requirements for dendritic cells in T cell stimulation leading to tolerance versus immunity. J Leukoc Biol 78:319
Tani K, Azuma M, Nakazaki Y, Oyaizu N, Hase H, Ohata J, Takahashi K, OiwaMonna M, Hanazawa K, Wakumoto Y, Kawai K, Noguchi M, Soda Y, Kunisaki R, Watari K, Takahashi S, Machida U, Satoh N, Tojo A, Maekawa T, Eriguchi M, Tomikawa S, Tahara H, Inoue Y, Yoshikawa H, Yamada Y, Iwamoto A, Hamada H, Yamashita N, Okumura K, Kakizoe T, Akaza H, Fujime M, Clift S, Ando D, Mulligan R, Asano S (2004) Phase I study of autologous tumor vaccines transduced with the GM-CSF gene in four patients with stage IV renal cell cancer in Japan: clinical and immunological findings. Mol Ther 10:799
Witmer-Pack MD, Olivier W, Valinsky J, Schuler G, Steinman RM (1987) Granulocyte/macrophage colony-stimulating factor is essential for the viability and function of cultured murine epidermal Langerhans cells. J Exp Med 166:1484
Acknowledgments
We thank Dr. Shinji Okano and Dr. Yoshikazu Yonemitsu, Kyushu University, for their helpful advices. We also thank Ms. Michiyo Okada for excellent technical assistance. This work was supported by grants from the Ministry of Health, Labor, and Welfare and the Ministry of Education, Culture, Sports, Science and Technology, Japan.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Inoue, H., Iga, M., Xin, M. et al. TARC and RANTES enhance antitumor immunity induced by the GM-CSF-transduced tumor vaccine in a mouse tumor model. Cancer Immunol Immunother 57, 1399–1411 (2008). https://doi.org/10.1007/s00262-008-0476-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s00262-008-0476-7