Abstract
Medical implant from different materials such as metals, ceramics, polymers and composites have gained a lot of research attraction due to wide applications in medical industry for treatment, surgical operations and preparing artificial body parts. In this work, we highlight a comprehensive review of medical implant mechanism, various types of implant materials, factors affecting the performance of implant and different characterization techniques. This review provides an overall summary of the state-of-the-art progress on various interesting and promising material-based medical implant. Finally, few new prospects are explained from the established theoretical and experimental results for real-life applications. This study is expected to promote extended interest of scientists and engineers in recent trend of modern biomaterials based medical implant.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
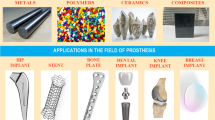
As the life span of people in different part of the world increases, the number of age-related diseases is also increasing concurrently. Apparently, there is an urgent need to look beyond the existing medical treatments, medical implants, and prostheses to make the lives of people much more comfortable. Millions of patients have implanted medical devices in their bodies which help the bodies and in turn the person to function normally. These implanted medical devices involve surgical process for their inclusion into the human body ecosystem. The term medical implant refers to an artificial structure or part that is used to replace a fraction of the whole biological structure of the human body. Today, such medical implants can find their applications in orthopedics, cardiovascular stents, pacemakers, defibrillators, neural prosthesis, dentistry or drug delivery system that can enable a normal functionality of several human body parts [1,2,3]. However, an important step in tissue engineering (medical implant manufacturing) is the selection of an appropriate biomaterial. The efficient biomaterial has to possess certain essential properties such as biocompatibility [4], bio-inertness [5], biofunctionality [6], and most importantly, the material must not cause inflammation or toxicity to the receptor [7].
The first metal alloy developed specifically to work with human tissues was “vanadium steel” in the early 1900s. Actually, the earliest successful implant was bone plates which were used to stabilize bone fractures and speed up the healing and recovery process for a patient. However, these early metal medical implants did not provide sufficient strength and were prone to corrosion. Later on, the stainless steel was introduced as a medical implant material which provided a far better corrosion resistance. Consequently, stainless steel immediately attracted the interest of majority of the medical fraternity working in this field. It created a great momentum and such metal implants experienced significant efforts towards their development and also in the deployment on several clinical use-cases [8]. Currently, different implant materials such as metals and alloys (e.g., Ti, Co, Ta, Nb, Zr, Mg and Fe based) [9, 10], ceramics (bioinert, bioglass and bioresorbable) [11, 12], carbon nanostructured implants [13], polymers, including polymer meshes and their composites [14,15,16,17] are used extensively in medicine. Further, composite material (e.g., zirconia-alumina and carbon fiber-reinforced polymer) [18, 19] is gaining importance as it is formed by combining two or more materials to create a new and superior material. These implant materials are used because of their high biological compatibility, variation of physical as well as mechanical properties, resistance to corrosion and other characteristics. Despite the variety, these materials do not provide solutions to all problems because of the limited strength characteristics, integrative properties, complexity of fixation, and biointegration properties. In particular, the high elastic modulus of metal implants is one of the reasons for bone resorption.
Through this review article, we aim to provide useful insights on various implant materials that are increasingly being developed for next-generation medical treatment in order to improve the life standard and life expectancy of people. This review is an attempt to explore the role of dielectric studies (dielectric constant, dielectric loss, and AC conductivity) on implant material as most of the reviews focused only on mechanical properties. Hence, this is the clear research gap exists till today and this review intends to give a complete overview from classification of implant and surface modification to few new interesting prospects from the established theoretical and experimental results for real-life applications.
2 Implant Based on Area of Application
Based on location where the medical implant has to be inducted in the human body, the implants can be classified as: cardiovascular implants, orthopedic implants, and implants for other use [3]. For instance, cardiovascular diseases include a wide range of conditions affecting both the heart and blood vessels. According to WHO, cardiovascular diseases continue to exist one of the prime cause of death all over the world, especially in developed countries. Annually, more than 17.9 million lives are lost due to such diseases [20]. Therefore, cardiovascular implants can contribute greatly in improving quality of human life as well as in reducing the overall cost of treating heart disease [21]. Lately, polymer-coated, and polymer-based cardiovascular implants such as shape memory polymers are being used extensively in modern medicine [22, 23]. Furthermore, with the changing demographics toward an aging society, they will gain even more importance. In addition, we have the orthopedic implants that capture the maximum of the implantable device market segment in terms of value. In India, approximately, 20 million bone fractures report annually [24]. Such market dominance also reflects the increasing prevalence of the sports and exercise injuries that is seen because of lifestyle changes and degenerative musculoskeletal disorders [25]. Apart from the cardiovascular and orthopedic implants, there are a bunch of implants that can be categorized together as other implants. For instance, evolution of cochlear implant technology helped to enhance hearing and speech abilities in a cost-effective way for children [26]. Moreover, development of perimodiolar electrodes, implantable microphones, and rechargeable batteries promise fully implanted devices for such applications in the coming future. Likewise, such implantable devices can also serve as a solution in treating vitreoretinal diseases by enabling intraocular sustained drug release [27]. Various subcategories under these classes are shown in Table 1.
3 Classification of Implant Based on Material
Generally, the material used for making implants and devices are divided into three categories such as metals, ceramics, and polymers. Furthermore, the metallic materials can be classified as either alloys or pure metals; ceramics can be categorized as glasses, glass-ceramics and carbons; and lastly the polymers can be divided into elastomers, thermosets, thermoplastics, and textiles. In addition, composite materials can also be treated as implant material efficiently. [3, 28].
3.1 Metals
Implants used in load-bearing applications are mostly prepared by metal, such as stainless steel, titanium, cobalt-based alloys, and titanium-based alloys. Such load-bearing medical implants can be simple structures such as wires and screws used for fixation of fracture plates to total joint prostheses (artificial joints) for the knees, shoulders, hips, and ankle. In addition, metallic implants are used as dental materials and maxillofacial cardiovascular surgeries [29]. Materials with mechanical properties closer to human bone can be generally used as long-lasting medical implants [30]. Porous material promotes cell growth and also provides stability [31]. Presently, with the rapid progress in field of medical implant, Ti and its alloys are commonly used as orthopedic implant in applications such as repair of joint, femoral fracture and skeleton structure fixation [32, 33]. Ti and Ti alloys are used because of two reasons. First, the elastic modulus of Ti and Ti alloys is almost same as that of the natural human bones, and second, Ti forms a naturally occurring oxide on its surface [34]. Callioglu et al. [35] reported that elastic modulus of Ti alloys are low compared to stainless steels [36] and CoCrMo alloys [37]. High elastic modulus of alloys can cause stress shielding effect which may not be suitable for hard tissue replacement [38]. In addition, density of Ti alloys [39] is almost half the density of stainless steel and CoCr alloys. Ti shows excellent biocompatibility, high strength, and good corrosion resistance. Light weight Ti is treated as a strong alloy [40], offers flexibility and can be coupled with other elements, such as Ag, Al, Ar, Cu, Fe, Va, and Zn to generate other alloy forms. For example, most commonly used alloy for medical implant is \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) [41].
Apart from Ti, magnesium and its alloys are used as implant materials since the first half of twentieth century [42]. \(\hbox {Mg}^{2+}\) and its alloys are mostly used in trauma surgery and orthopedics as they are non-toxic in nature inside the human body [43]. These alloys offers an inherent property by which they degrade safely in vivo after the healing process is completed. However, surface activation of magnesium alloys is still sought because the medical implants must be durable enough to allow for bone regrowth [44]. However, Kuhlmann et al. [45] reported that \(\hbox {Mg}^{2+}\) alloys corrode rapidly and form subcutaneous gas bubbles, thus limiting their use as implant material. Further, cobalt–chromium–molybdenum alloy (CoCrMo) is commonly used in total hip replacements [46]. CoCrMo has emerged as an alternative to Ti alloys as it offers better corrosion resistance and higher strength [47], although Hart et al. [48] found the existence of \(\hbox {Cr}^{3+}\) ions around the tissue surrounding CoCrMo implants. Cobalt in metallic form is also found around the implant, which can cause significant health consequences in patients. Kop et al. [49] also reported corrosion in CoCrMo neck–stem junction.
However, implant materials with advanced features such as improved tribological properties and low-level costs are required today to meet the growing demand. Additive manufacturing (AM) is one of the techniques to meet these requirements. AM technology allows manufacturing of complex geometric shapes by placing layer upon layer [50, 51]. It is a computer-controlled process that creates three-dimensional objects. Tekdir et al. [52] placed \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) layers on 316L stainless steel using laser powder bed fusion (LPBF) technique, which is one of the metal additive manufacturing methods. It has been reported that AM technology results in formation of a bimetallic implant material which is cost effective and have superior properties such as higher wear resistance.
3.2 Ceramics
Ceramic materials are formed when clay and their mixture with mineral additives, metal oxides and other inorganic compounds undergo the process of sintering. Ceramic materials are generally used to repair rigid connective tissues in the body like bones. It is proved that the bone itself can be seen as a combination of organic and ceramic phases, where the ceramic phase is mostly calcium hydroxyapatite(HA) with a value of 1.67 for Ca/P ratio. In addition to the rigid connectivity of tissues, ceramics implants find their use as restorative materials for dentistry implants, such as crowns, cements, and dentures [53]. Bioceramic materials are mainly classified as—bioinert, bioactive and bioresorbable, according to response of the body to implant material.
In the second half of the twentieth century, ceramics started gaining importance in the field of medical implant as it offers better biocompatibility compared to metals [54]. Bioceramics have mainly evolved through three stages. In the beginning of 1960s, first-generation bioceramics (e.g., alumina, zirconia) were designed with the objective of bio-inertness in which interaction of implant material with the surrounding tissue is as low as possible [55, 56]. In the manufacturing of prostheses components, alumina is used even today as it provides wear resistance and inertness [57]. Nowadays, zirconia implants is used as a substitute to Ti in implant dentistry because of its white color, high biocompatibility, low thermal conductivity and modulus of elasticity, and low bacterial attraction [58,59,60]. Wilmowsky et al. [61] mentioned that surface and microstructure modifications of zirconia improve healing of bone and thus can replace Ti implants. However, in the presence of moisture or hydrogen, zirconia losses its favorable properties such as its strength. This is known as low-temperature degradation [62]. The transformation rate is minimized due to reduction in grain size and/or increase in the concentration of stabilizing oxides [63]. In addition, zirconia fracture strength resistance is reduced during its cyclic loading [64]. Tang et al. [65] prepared zirconia-alumina composite using AM technology for dental implants. High toughness of zirconia is combined with with hardness, wear, and chemical resistance of alumina to overcome the drawbacks of zirconia.
In 1980s, second-generation bioceramics (e.g., calcium phosphates, bioactive glasses and glass-ceramics) were developed in which there is favorable interaction between implant material and surrounding tissue resulting in strong mechanical bond. These are called bioactive ceramics. They are mostly used as bone cements or in coating of implant material [66,67,68,69]. But due to brittle nature of bioceramics, it was felt that bioceramics alone could not meet the requirements of an implant material. This led to the development of third-generation bioceramics at the end of the twentieth century. These types of bioceramics focused on regeneration of tissues rather than replacement of tissues [70,71,72]. Second-generation bioceramics with porosity induced in it are studied for this purpose [73, 74]. Further, new types of advanced bioceramics, such as organic–inorganic hybrids [75, 76], silica mesoporous materials [77, 78], so-called star-gels [79] or mesoporous ordered glasses [80, 81] are also studied. However, ceramic materials have poor fracture toughness which in turn limit their use for load-bearing applications [82].
3.3 Polymers
Both the above-presented classes of metals and ceramics practically lack in terms of versatility. This has attracted a lot of interest to look for the medical implants prepared from polymeric materials. Such polymeric implants due to their versatility can find their applications in wide varieties medical implant use-cases, such as facial prostheses, tracheal tubes, parts of liver and kidney, heart components and even for dentures as well as artificial joints for hip and knee [83, 84]. Polymers which are used as medical implants include poly(tetrauoroethylene), polyamides (nylons), polysulfones, polyvinylchloride, polyesters, silicone, hydrogels, acrylic, chitosan, and collagen [3]. At present, polyaryletherketones (PAEKs) is among the most promising polymers. Polyetheretherketones (PEEK), a semi-crystalline polymer and poly(aryletherketone etherketoneketone) (PEKEKK), which offers high wear resistance are two most widely used PAEK polymers [2, 3]. Lately, conductive polymers such as polyaniline, polythiophene, polypyrrole and their composites are also gaining importance as they improve biocompatibility and mechanical properties [85]. As composite, conductive polymers also improve corrosion resistance of metallic implants [86]. Fonseca et al. [87] reported the use of bioabsorbable polymers (e.g., PLA, PGLA, and PCL) in cancer treatment. Basak [88] utilizes shape memory polymers such as polyethylene to manufacture medical devices.
3.4 Composites
They consist of both organic and inorganic constituents to imitate natural bone tissue. The organic part of implant material provides flexibility and improves its biocompatibility, whereas load-bearing strength and stiffness are executed by inorganic part. In composites, the organic matrix may be composed of natural polymers (e.g., chitosan, collagen) or synthetic polymers (e.g., polylactic acid (PLA), polycaprolactone (PCL)), whereas the inorganic part may be made of metal alloys and ceramics, such as hydroxyapatite (HA) [3, 89]. Desired mechanical properties such as strength, stiffness, toughness, and fatigue resistance can be obtained through development of composite material. Li et al. [90] fabricated carbon-reinforced PEEK material for orthopedic application. An important advantage offered by composites compared to traditional materials is its ability to design anisotropic properties as strengthening mechanism strongly depends upon the geometry of the reinforcement [3]. We summarize each of above-mentioned categories of implants Table 2.
4 Surface Modification of Implant Material
When a medical implant is placed in the human body, different molecular interactions take place at the material surface. The types of interactions are affected by the surface properties of the implant material such as surface chemistry, wettability and surface roughness. At the same time, the environment inside the human body is physically and chemically different from ambient conditions which can lead to failure of implant material [91,92,93]. The major factors which can lead to implant failure are electrochemical degradation, in the form of corrosion, or mechanical degradation, in form of fatigue and wear. These damage mechanisms are explained as follows.
-
1.
Corrosion: It is a natural process which results in gradual degradation of material through chemical or electrochemical reaction. Implant material faces severe corrosive environment inside the human body which includes blood, water, sodium, chlorine, proteins, plasma, and amino acids along with mucin in the case of saliva. The equilibrium of the corrosion reactions around the implant is disturbed by these biological molecules [94, 95]. Corrosion is also affected by changes in the pH values. Diseases, accidents, infections and other factors cause the pH value to change from 3 to 9 as opposed to 7, which is normal pH of human body [96]. Furthermore, the internal partial pressure of oxygen is about one quarter of atmospheric oxygen pressure. Hence, lower oxygen level increases the rate of corrosion as formation of protective passive oxide films on the surface of implant material slows down [97].
-
2.
Fatigue: Fatigue refers to changes in properties when implant material is subjected to cyclic load [97]. It normally occurs at sites where stress concentrates. Imperfections in the form of impurities, holes and pits are bound to be in material as no material is perfect in the real world. So, when implant material is exposed to external loading, stress concentrates at these sites of imperfection leading to permanent defects in form of dislocations and microcracks. These defects cannot be removed even when unloading takes place and finally implant material suffers from catastrophic failure [98, 99]. Bone plates and orthopedics implants such as artificial hip joints are likely to suffer from fatigue [100].
-
3.
Wear: Wear is one of the most common reasons for the failure of metal components. The problem of wear results in implant loosening as friction at joint replacement releases non-compatible metallic ions [101, 102]. In addition, mechanical loading results in corrosion fatigue which further accelerates wear processes. It lead to increase in particle levels over a period of time. These particles are ingested by immune system macrophages, which enhances their destruction. The dying macrophages release metabolites and enzymes resulting in harsh acidic environment in the region around implant material, which further result in erosion of the bone and implant [103, 104].
Thus, high fatigue strength, excellent corrosion and wear resistances are some of the important properties which determine the life span of implant material inside human body [97]. Currently, the most common practice of achieving improvement of implant properties is surface modification. The goal of surface modification is to generate specific chemical and physical surrounding which provide favorable cellular response to implant material. Surface modification of implants is done in order to reduce the problems caused by electrochemical and mechanical degradation. It helps in improving integration of implant with the surrounding tissue. It also decreases bacterial adhesion and inflammatory response. Surface modification affect surface energy, adhesion, biocompatibility, chemical inertness, etc. However, textured surfaces in some cases are counterproductive to the functioning of the device such as articulating surfaces or cardiovascular devices [105]. This review paper puts forward latest findings as shown in Fig. 1 regarding additive and subtractive surface modifications technique in order to improve bone tissue regeneration. One of the most commonly used additive modification method is coating [106].
Different techniques of surface modifications [106]
4.1 Coatings
Coating can improve the surface modification of implant because implants inside a living organism may have to face high degrees of complications. Therefore, it is desired that the implant material must be non-reactive in nature both chemically and physically with the human body and its tissues. Moreover, it has been reported that the infection is one of the major causes of failure of prosthetic implants, so controlling infection inside the human body is a challenge after implantation. As such, functional coatings can be used to alter the substrate’s surface attributes such as adhesion, wet ability, corrosion resistance, and wear resistance. Generally, coatings are used on porous metal surfaces for fixation of orthopedic prostheses which include biological and bioactive fixation [107, 108]. A simple mechanism depicting formation of biofilm on medical implant to protect from infection is illustrated in Fig. 2.
Mechanism showing formation of biofilm to protect the implant from infection [37]
Moreover, the coating method can be classified as—physical vapor deposition and chemical vapor deposition.
4.1.1 Physical Vapor Deposition
Substrate surface is deposited with thin film in physical vapor deposition (PVD) method. Film material in vaporized form is condensed and thereafter it is deposited on the target surface. Moreover, coating method is carried out in physical processes such as high-temperature, vacuum, evaporation followed by condensation. Some of the common coatings used with the help of PVD are zirconium nitride, titanium nitride, chromium nitride, and titanium aluminum nitride. PVD coatings ensure excellent purity of the films because of the high-vacuum condition used by evaporation coatings. PVD coatings are sometimes harder and offer better resistant to corrosion and abrasion. It is also environment friendly than other existing conventional processes of coating, such as electroplating and painting [107,108,109]. Polymers such as polyethylene and polyvinylidene fluoride (PVDF) are used in PVD method [110, 111]. Some of the PVD coating processes applied in medical implant formation are described as follows.
In plasma-spray process, coating is usually formed by spraying a molten or heat softening material onto a substrate. The powdered material is injected into a very high-temperature plasma flame, which heats up the material quickly and accelerates in to high speed. This hot material forms coating on substrate surface when cooled [112]. HA-coated metallic implants using plasma-spray method is widely used in orthopedic and dentistry fields since it is reliable, cost effective and protects the implant material surface from corrosion and wear [113]. It has been reported that composition, coating density and crystallinity of coating can be modified by changing process parameters such as spraying distance and particle size [114]. Sun et al. [115] coated HA using plasma-spray method and conclude structural and phase changes with variation in melting of particle, cooling rate and recrystallization. Singh et al. [116] coated HA and 10 wt % \(80\hbox {Al}_{2}\hbox {O}_{3}-\hbox {20TiO}_{2}\) reinforced HA using plasma-spray method on \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) substrate and reported that implant properties enhanced when coated with reinforced HA compared to pure HA. Further, corrosion properties of nickel–chromium and chromium oxide is enhanced when plasma-spray method is used [117, 118]. However, defects such as cracks, unmolten particles and uneven thickness lead to poor adhesion strength in plasma-spray method [119].
Pulsed laser deposition (PLD) is a thin-film deposition method via a high-powered pulsed laser beam. Here, a high-power and focused laser beam strikes accurately on a material which is target for deposition inside a vacuum chamber. This material forms thin film on a substrate when deposited in vaporized form. This process can be performed in ultra-high vacuum or in the presence of a background gas such as oxygen, which is commonly used for oxide deposition to completely saturate the deposited film with oxygen [120]. Moreover, an argon atmosphere can also be preferred. Biofunctionality of implant materials is improved by the laser through surface modification [121]. PLD method is used to deposit high-quality hydroxyapatite thin film [122]. Crystallinity, morphology and phase of films deposited by pulsed laser technique depends on parameters such as wavelength of laser, duration of pulse and energy density [123]. Pelin et al. [124] deposited HA films using PLD on titanium and \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) substrates. They reported that with increase in deposition temperature, surface roughness is improved. Kuppuswamy et al. [125] deposited HA films on polyimide substrates successfully using PLD technique. Nasar [126] evaluated pulsed laser deposition of HA on \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) for dental applications. But, coating thickness is difficult to control in this technique [127].
In radio-frequency magnetron sputtering electromagnets, permanent magnets or both are used to create magnetic field, so that electrons can be trapped [128]. Sputtering deposit thin films by discharging of material from a source to a substrate. As a result, the ion with very high energy comes out in straight line from the target and impact on the substrate with very high energy [109, 129]. Biocompatible ceramic coating on implant material is deposited using this method [130]. This technique has excellent control over coating composition, improves adhesion strength and requires low substrate temperature. Xu et al. [131] used radio-frequency magnetron sputtering to deposit HA coating on \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) substrate and reported biocompatibility of HA with the surrounding tissue. Further, zirconium nitride-reinforced HA enhances the bone strength of the coating. This composite coating is prepared with the help of radio-frequency magnetron sputtering [132]. Socol et al. [133] reported that polymethylmethacrylate (PMMA) substrate is used as cranio-spinal implant material. They deposited HA film using sputtering technique on PMMA substrate and observed compatibility with surrounding bone cells.
4.1.2 Chemical Vapor Deposition
Chemical vapor deposition (CVD) is a chemical process used to produce high-purity, high-performance solid material. Semiconductor industry and composite material frequently used CVD method for thin film production [109]. In CVD, substrates are exposed to one or more volatile precursors that react or decompose on the surface of substrate to form the desired deposit. CVD is highly useful for depositing thin layers of uniform thickness in complex geometries [134, 135]. CVD methods can be categorized as dip coating and spin coating.
In dip coating, the substrate is sequentially immersed in a solution and removed at a constant rate. This gives a layer of the non-volatile species above the drying line. Dip coating is one of the most ideal method for preparing thin layers in chemical solutions [136]. It is an inexpensive, waste-free process that scales easily and provides excellent thickness control. For this reason, it is gaining more and more importance for developing medical implant not only in research laboratories, but also in industrial processes. Dip coating is best suited to impregnate porosity, to prepare nanocomposites, and to do nano-casting [137]. Ritwik et al. [138] synthesized thin film of HA with intermediate layer of shellac. Dip coating is used to deposit film on \(\hbox {Ti}_{6}\hbox {Al}_{4}\hbox {V}\) substrate and it was reported that the obtained adhesion strength is suitable for the orthopedic application. However, formation of cracks may occur on substrate surface as this method requires high sintering [139].
In spin coating, the substrate rotates around an axis that should be perpendicular to the coverage area. The spin on process has been developed for microelectronics so-called spin on glasses and rotationally symmetric substrates such as optical lenses or lenses for the eye. Moreover, the final thickness of a spin-coated layer will depend on the processing and material parameters such as angular velocity, viscosity and solvent evaporation rate [140]. Different coating techniques that we discussed above have minimal control over coating thickness and are also expensive. However, spin coating is an inexpensive process and shows compatible properties [141]. Spin coating technique is most commonly used for substrates having flat surface. However, it is examined that it can be beneficial for structure having 3D circular shapes such as dental screws and rods [142]. Soule et al. [143] deposited coating of glass on stainless steel 316L using spin coating. They reported enhanced bioactivity, improved antibacterial properties. In addition, it promotes regeneration of tissues around implant materials. Simple comparison between different coating method is depicted in Table 3.
4.2 Nanotechnology-Derived Surface Modification
However, emergence of nanotechnology led to the development of new techniques and methods of surface modification. Nanotechnology refers to materials in which one of their dimension is less than 100 nanometer [144]. It has been reported that osteoconductive and osteointegration properties of nano-modified implant material is improved as it offers large surface area to volume ratio [145]. As compared to conventional materials, nanocrystalline structure is harder, smoother and acts as good binder. Since nano materials have excellent wear resistance, it also reduces the problem of implant loosening [146]. This approach increases the implant material mechanical strength by imitating the composition of bone. Nanoparticles of hydroxyapatite, calcium triphosphate, bioactive glass, synthetic polymers and biodegradable polymers have been manufactured into three-dimensional porus scaffolds for tissue regeneration and bone repair [146,147,148]. Arumugam et al. [149] reported that more successful orthopedic implant materials can be developed by doping carbon nanotubes (CNTs) in small amount in polymer or ceramic matrices. High flexibility, high tensile strength and low density of CNTs make them an attractive material in field of nanotechnology. However, nanomaterial also possesses some threat and harmful effects as they can cause inflammatory response by depositing in the respiratory tract. As they are small in size, they can be transported easily in various parts of the body including heart and brain. The physical and chemical properties of nanoparticles including its shape, size and surface chemistry are also known to increase inflammation and tissue damage [146].
XRD pattern. (a) HA doped with Ga. (b) Pure HA [151]
5 Characterization Techniques of Implant Material
During the last few years, development of implant material has gained momentum. In order to be used over a long period of time, quality and reproducibility of implant materials are essential. Further, characterization of physical property, chemical property and dielectric studies are necessary for increased acceptance and use of implant materials. These characterization techniques including dielectric studies are discussed briefly as follows.
5.1 X-Ray Diffraction (XRD)
X-ray diffraction (XRD) analysis is a method employed in the field of materials science subject to characterize the implant material crystallographic structure. For XRD analysis, target implant material is irradiated via incident X-rays and then measurement is performed on the basis of the intensities and scattering angles of the X-rays that are leaving the material [150]. It is based on Bragg’s law:
where d denotes the interplanar spacing of the crystal, \(\theta\) is angle of incidence, n is an integer which represent the order of reflection, and \(\lambda\) is wavelength of the incident X-rays. Nayak et al. [151] observed the crystallographic structure of gallium-doped hydroxyapatite and pure hydroxyapatite with help of XRD pattern as illustrated in Fig. 3.
5.2 Scanning Electron Microscope (SEM)
The surface morphology, particle size and chemical compositional analysis of implant material at different magnification were examined with scanning electron microscope [152]. SEM images of pure hydroxyapatite and strontium-doped hydroxyapatite [152, 153] are displayed in Fig. 4.
SEM image. (a) Pure HA. (b) Sr-doped HA [153]
5.3 Vector Network Analyzer (VNA)
A VNA is a versatile device which reflects the electrical characteristics of any medical implant. It is normally used to measure transmission parameters, reflection parameters, impedance parameters, scattering parameters, dielectric constant, dielectric loss, conductivity and loss tangent [154].
5.3.1 Dielectric Permittivity/Dielectric Constant (\(\epsilon ^{\prime }\))
Variation of dielectric constant with frequency is significantly observed for different medical implant materials in Fig. 5. Dispersive region is observed in dielectric constant variation graph. The nature of dielectric constant exclusively dependent on implant material property [1, 151] and frequency band used.
5.3.2 Dielectric Loss (\(\epsilon ^{\prime \prime }\))
Variation of dielectric loss or imaginary component of high-frequency complex permittivity with frequency is very important because it clearly signifies the lossy behavior [153, 155] of implant material which is shown in Fig. 6.
5.3.3 AC Conductivity (\(\sigma _{ac}\))
AC conductivity variation with frequency indicates the conducting nature and loss factor associated with implant material [151, 155] as shown in Fig. 7.
6 Current Useful Implant Materials
6.1 Hydroxyapatite (HA)
Biocompatibility is one of the most important property of a biomaterial used in medical implant. Due to injury when bone is lost, that lost bone can be filled by natural bone. But that natural bone may not be biocompatible with the surrounding tissue and can cause possible infection. HA, \(\hbox {Ca}_{10}(\hbox {PO}_{4})_{6}(\hbox {OH})_{2}\) can be used as an alternative to natural bone as its composition is similar to bone. Bioactivity and osteoconductive properties of HA made them suitable for bone regeneration and in improving osteointegration of implant. Thus, HA is ideal candidate for bone tissue engineering scaffolds [156]. However, HA will not be able to integrate with bone and confine within fibrous tissue if the gap between HA and bone is wide [157]. In addition, it is not suitable for major load bearing areas as it is brittle and have poor mechanical properties [1]. Therefore, HA is doped with various ions such as \(\hbox {Zn}^{2+}\), \(\hbox {Sr}^{2+}\), \(\hbox {Ce}^{3+}\), \(\hbox {Bi}^{3+}\), and \(\hbox {Y}^{3+}\) in order to improve its properties. \(\hbox {Ca}^{2+}\) ions in the HA structure is substituted by these ions, thus affecting the crystallinity, lattice parameters and morphology of HA. Hence, through these ionic substitution, characteristic properties of HA can be controlled as crystal structure and composition of HA is directly linked with its properties [158].
Bioactivity and osteointegration of HA improves both in vitro and in vivo under the influence of electrical polarization. It has been reported that a surface with net charge (positive or negative) is more hydrophilic, further easing interfacial processes and protein adsorption as compared to neutral surface [157, 159]. It is also shown that bone growth is faster on negative charge surface [160]. It may be due to adsorption of \(\hbox {Ca}^{2+}\) ions. At the bone implant interface, surface charge also shows to increase early-stage bone mineralization [160]. Thus, surface charge modification provides a new direction in order to improve biological properties and performance of bone scaffold materials as shown in Fig. 8.
Diagram showing the interaction between polarized charge and the material. (a) On neutral material. (b) On negative material. (c) On positive material [159]
Direct current excitation can also accelerate bone healing process. Electroactive materials with high dielectric permittivity under the influence of external electric field results in formation of significant surface charge. High-dielectric permittivity makes material strongly polarized and thus shorten the bone regeneration time [1, 161]. The change in properties of HA doped with various ions was investigated by several researchers [162].
6.2 HA Doped with Different Materials
Yttrium (Y) use in medical applications include treatment of hepatocellular carcinoma [163, 164]. It has been reported that HA doped with Y using hydrothermal method not only helps in accelerating the bone growth but also restricts the oral bacterial growth [165]. Kaygili et al. [155] studied different doped HA samples with 0, 2 and 4 wt % of Y. Since \(\hbox {Y}^{3+}\) ions are smaller than \(\hbox {Ca}^{2+}\) ions, incorporation of Y cause size reduction. It was observed that change in Y content affect crystallinity degree and lattice parameters of the sample. Volume of unit cell decreases gradually as Y is added to the sample [166]. Electrical properties such as dielectric constant (\(\epsilon ^{\prime }\)), dielectric loss (\(\epsilon ^{\prime \prime }\)) and AC conductivity (\(\sigma _{ac}\)) also vary with Y content as well as with frequency [167]. The dielectric loss (\(\epsilon ^{\prime \prime }\)) decreases gradually as content of Y is increased. The AC conductivity (\(\sigma _{ac}\)) increases linearly as frequency is increased but decreases with increasing content of Y. Composite showed insulator behavior as measured resistance values were in range of 1011–1012 \(\Omega\). However, addition of Y did not show any improvement in antimicrobial properties [168].
Bismuth (Bi) containing nanoparticles have recently gained a lot of research attraction in biomedical applications, because of their excellent properties, which include high stability, high surface area and strong diamagnetism [169]. Al-Hazmi [170] prepared \(\hbox {Ca}_{\mathrm{(10-x)}}\hbox {Bi}_{\mathrm{x}}(\hbox {PO}_{4})_{6}(\hbox {OH})_{2}\) ceramics using sol–gel technique and study the effect of Bi on dielectric and ferroelectric properties of composite. HA samples were doped with 0.1, 0.2, 0.3, 0.4 and 0.5 wt % of Bi. FTIR spectra showed that OH is substituted with Bi as Bi content increases [171]. Scanning electron microscopy (SEM) images indicate that the particle size of \(\hbox {Ca}_{\mathrm{(10-x)}}\hbox {Bi}_{\mathrm{x}}(\hbox {PO}_{4})_{6}(\hbox {OH})_{2}\) ceramics lies in nano-region and are randomly distributed. X-ray diffraction (XRD) technique further shows blending of Bi into HA. Bi dopant causes dielectric constant of the ceramics initially to increase and then as Bi content increases, dielectric constant decreases significantly. The reason behind this change in dielectric constant is electrical polarization in the ceramics [172]. AC conductivity shows linear behavior with frequency. It is also reported that due to introduction of Bi dopant, ferroelectric properties of the composite decreases. Further, Ahmed et al. [173] studied the antibacterial properties of Bi and reported that the antibacterial property enhanced when Bi is added with HA.
Strontium (Sr) is mainly found in human bone. It helps in treatment of osteoporosis, bone growth and development [174]. Reem et al. [153] used hydrothermal method to synthesize HA-doped Sr. Sr is added in different concentration, i.e., 0, 0.03, 0.06, 0.12, 0.24 and 0.48 in HA. It was reported that crystallinity value reduces since \(\hbox {Ca}^{2+}\) ions are being substituted by \(\hbox {Sr}^{2+}\). XRD pattern of Sr–HA composite shows similar peaks with reduced intensity compared to pure HA [175]. Dielectric constant (\(\epsilon ^{\prime }\)) at lower frequency do not show much change while it increases with increase in frequency at higher frequency. In addition, dielectric constant increases as concentration of Sr increases in sample, mainly due to ionic polarization [176]. AC conductivity increases with increase in frequency [177].
Bowen et al. [178] synthesized \(\hbox {HA-BaTiO}_{3}\) composite with \(\hbox {BaTiO}_{3}\) (BT) composition varying from 0% to 100% by volume using pressure less sintering method. Effect of \(\hbox {BaTiO}_{3}\) on electrical properties of the composite were studied and reported that with decreasing \(\hbox {BaTiO}_{3}\) concentration, magnitude of dielectric constant as well as degree of dispersion decreases [179]. AC conductivity increases as concentration of \(\hbox {BaTiO}_{3}\) increases since \(\hbox {BaTiO}_{3}\) has higher permittivity compared to HA. For higher frequency, AC conductivity increases almost linearly, while at low frequency, there is no dependence between them [180]. Dang et al. [1] prepared three-phase bio-electroactive nanocomposite and used PVDF with \(\hbox {HA}-\hbox {BaTiO}_{3}\) composite material. \(\hbox {BaTiO}_{3}\) nanoparticles which provide high dielectric permittivity and excellent bioactivity of HA nanoparticles is doped with PVDF to form three-phase bio-electroactive nanocomposites based ferroelectric polymer matrix. It is proved that three-phase (BT-HA)/PVDF nanocomposites exhibits higher dielectric permittivity which results in formation of surface charges due to an applied electrical field. Surface charge reduces bone regeneration time [1]. Three-phase (BT-HA)/PVDF nanocomposites can also be used as bio-dielectric materials since it has low dielectric loss [181]. However, molecular movement of PVDF is inhibited as volume fraction of BT increases because it would result in smaller areas of bulk PVDF phase which in turn result in relatively lower degree of crystallization of PVDF in three-phase nanocomposite.
Gallium (Ga) is used in treatment of osteoporosis and hypercalcemia [182]. It is an important component of composite implant material and shows antibacterial as well as antimicrobial properties when used with phosphate-based glasses (PBGs) [183]. It also helps in controlling drug delivery related issues [184]. HA doped with Ga bioceramics find application in bone formation and growth. Crystalline size increases as \(\hbox {Ga}^{3+}\) ion substitute \(\hbox {Ca}^{2+}\) ion in HA [185]. Nayak et al. [151] reported that Ga-doped HA-based bioceramics forms negative surface charge and HA–Ga experiences lower dielectric loss compared to pure HA establishes the efficiency of HA–Ga as a dielectric material. Further, high electrical polarization in HA–Ga bioceramics results in high value of dielectric constant. However, AC conductivity of HA–Ga is not changed significantly compared to pure HA.
Iron (Fe) is an essential part of human body and present in small amount in bones and teeth. Biomedical properties of HA enhance with addition of small amount of iron as it promote bone growth and had no toxic effect on the osteoblast cells [186]. Kaygili et al. [187] doped hydroxyapatite (HA) with Fe in different concentrations using sol–gel process and their properties were investigated. Crystalline size of the samples decreases gradually as Fe content increases thus affecting crystallinity degree, lattice parameters, unit cell volume and the phase composition [188]. As concentration of Fe increases, the dielectric permittivity of the HA increases for all frequency values. The value of AC conductivity increases as frequency increases and it was also reported that HA doped with Fe showed insulator behavior [189].
Chromium (Cr) improves the ability of insulin to convert glucose thus help cells in human body to gain energy and maintain blood sugar level. Ibrahim et al. [190] doped hydroxyapatite with 0.5, 1.0, 2.0, and 3.0 wt % of chromium using wet precipitation method and studied dielectric properties. It has been reported that chromium improves biocommunication as it causes electrical conductivity to increase [191]. At low frequency, dielectric permittivity increases with increase in wt % of Cr. However, dielectric permittivity at higher frequency remains almost same for pure and doped ones [192]. Thus, HA bioconductivity and electrical properties improves with addition of Cr.
6.3 Piezoelectric-Based Biomaterials
Piezoelectric materials are smart materials as these materials convert the applied mechanical pressure into electrical signals which is called as direct piezoelectric effect. Since piezoelectric effect is a reversible process, these materials also convert electrical signals into mechanical signals [193]. There are two basic requirement for any material to show piezoelectricity. First, crystal lattice structure of the material and second, there should be lack of a center of symmetry [194]. Piezoelectric materials find application in tissue engineering such as in tissue repair and regeneration and they do not require any external power source to generate electrical signal as they are active transducer [195, 196]. Piezoelectric material produces electrical signal which can promote tissue formation by definite pathways and produce suitable bioelectrical signals like natural extracellular matrix (ECM), which is observed during remodeling phenomenon in bone and cartilage [197]. Tissues such as bone, cartilage, and tendon show direct piezoelectricity [198]. Collagen, one of the main constituent in bone and cartilage also shows piezoelectric property [199]. Piezoelectric materials can be used alone as well as a composite with other suitable material. It can either be polymers or ceramics.
6.3.1 Piezoelectric Polymers
Polymers are light in weight and are mechanically as well as electrically tough as compared to organic and inorganic materials. They are flexible and show excellent compatibility with other biomaterials [200]. Polymers possess piezoelectric property must have permanent dipole, the ability to sustain alignment and undergo large strains when mechanical stress is applied [201]. Some interesting piezoelectric polymer widely used as implant material are as follows:
Chitosan is biocompatible, biodegradable and non-toxic. It can be processed and manufactured in various forms such as fibers and films and thus have the ability to mould into the shape of the required tissue. As chitosan is polycationic in nature, it promotes bone growth [201, 202]. It is also used in regenerative medicine. Petrov et al. [203] synthesized chitosan–hydroxyapatite composite material and studied electrical properties. It has been reported that dielectric permittivity increases with increase in frequency. Mechanical properties such as tensile modulus and strength is improved when CNT is added in small amount in chitosan as CNT have excellent mechanical properties [204]. However, chitosan degrades at higher temperature.
Piezoelectric coefficient of poly(3-hydroxybutyrate-co-3-hydroxyvalerate) (PHBV) is similar to human bone and is biocompatible as well as biodegradable [205]. It has been reported that composite material of PHBV/PCL/HA accelerate bone regeneration as PCL enhances surface roughness and hydrophilicity while HA improves bioactivity [206]. Wu et al. [207] fabricated a composite mixture of PHBV/Bioglass which can be used to prepare better engineered cartilage as compared to pure PHBV. But it has been reported that enzymatic degradation mechanism can degrade PHBV and thus failed to form strong interaction with the surrounding tissue [208].
Polyvinylidene fluoride (PVDF) has high flexibility and its non-toxic nature finds application in tissue engineering [209]. P(VDF-TrFE), which is a copolymer of vinylidene fluoride (VDF) and trifluoroethylene (TrFE) have positive effect on cell adhesion and cell growth. When mixed with natural polymers such as starch or cellulose, it finds application in tissue repair and regeneration as scaffold structure [210, 211]. The composite of PVDF-TrFE and barium titanate piezoelectric promotes bone regeneration [212]. However, PVDF is not suitable for biological environment as it tends to degrade in extreme alkaline medium [213]. Non-biodegradable nature of PVDF limits its use in tissue engineering [214].
Poly-l-lactic acid (PLLA) is biocompatible and biodegradable polymer. High value of piezoelectric coefficient and excellent mechanical properties of PLLA finds application in orthopedics such as screws and pins. Since it is degradable, it has been reported for rapid bone regeneration [215]. Chorsi et al. [216] have reported that due to piezoelectric polarization, PLLA promote bone growth. Prabhakaran et al. [217] fabricated composite material of PLLA/collagen and HA and reported improved bone growth compared to PLLA. Further, PLLA/chitosan composite material is used in tissue engineering as chitosan material significantly neutralizes acidity caused by PLLA degradation [218].
6.3.2 Natural Polymers
Natural polymers have gained a lot of research attraction recently compared to synthetic polymers because of their biocompatible and biodegradable behavior. They consist of highly organized structure and provide biological signaling, thus promote cell adhesion and remodeling [219]. Low toxicity and degradable nature of natural polymer further helps them to find application in tissue engineering [220]. However, inadequate physical properties and loss of biological properties during formulations restrict their use in the field of medical implant [221]. Some significant natural polymers are listed as follows.
Cellulose offers excellent biocompatibility and high tensile strength. It has excellent mechanical properties despite high water content. It finds application in bone and cartilage tissue engineering as it promote cell adhesion [222]. However, small pore size of cellulose limits the cell infiltration which can be improved by addition of paraffin microspheres as it results in better pore connectivity and also increases the pore size [223]. Daugela et al. [224] prepared cellulose/HA scaffolds which promote bone formation as highly interconnected porus structure is formed. Eftekhari et al. [225] fabricated a composite material consisting of cellulose/PLLA/HA in which reinforcing agents are homogenously dispersed in PLLA matrix, thus improving mechanical strength of composite material.
Collagen is biocompatible, hydrophilic and has good cell binding properties. It is also used in bone healing and provides structural and mechanical support [226]. It can be treated as a composite material with hydroxyapatite and thus promotes cell growth. However, due to high ionic forces of hydroxyapatite there is slight decrease in piezoelectricity of collagen–HA composite [227]. Yilmaz et al. [228] studied HA/graphene oxide/collagen composite mixture and reported increase in mechanical strength. It has also been reported that penetration of tissue increases with increase in pore size. But rapid degradation and low mechanical stiffness of collagen limits its application in tissue engineering.
Chitin is a natural polysaccharide exhibiting biocompatible and hydrophilic nature. It promotes cell adhesion. Chitin as a composite material with other suitable biomaterial find application in bone and cartilage regeneration [220]. Chang et al. [229] reported that mechanical properties and biocompatibility improved when HA was incorporated with chitin hydrogel network. Chakravarty et al. [230] fabricated a composite mixture of chitin, polylactic acid and hydroxyapatite and found that it acts as excellent material for bone regeneration. However, it is not suitable for hard tissue application as it fails to maintain predefined shape and suffers from poor mechanical properties [231].
6.3.3 Piezoceramics
Piezoceramics such as boron nitride, zinc oxide, and potassium sodium niobate have very high piezoelectric coefficient. Ciofani et al. [232] reported that piezoelectric property of boron nitride nanotube is superior compared to piezoelectric polymers. In addition, it provides excellent mechanical properties and suitable for orthopedic applications as it increases the adhesion of osteoblast cells [233]. Tayel et al. [234] evaluated the antibacterial property of ZnO nanoparticles and reported that it enhances the antibacterial property of implant material. Ito et al. [235] reported that composite mixture of HA–ZnO enhances bone growth. It has also been reported that the doping of ZnO in composites can increase their flexural strength, decrease the shear bond strength, and decrease the compressive strength [236]. However, piezoceramic material suffers from toxicity, which has limited their use in tissue engineering [237]. Mechanical properties (young modulus (Y) and tensile strength (\(\sigma\))) and electrical properties (dielectric constant (\(\epsilon ^{\prime }\)) and AC conductivity (\(\sigma _{ac}\))) of some of the engineering materials which are used as implant material are shown in Table 4.
7 Potential Materials for Future Studies
As hydroxyapatite chemical structure and composition is similar to bone, most of the research regarding biomedical implant revolves around it. It can also be used as a composite material. But, hydroxyapatite suffers from basic problem such as it is not suitable for load-bearing application due to poor mechanical properties. It also suffers from high dissolution in a physiological environment, thus affecting long-term stability which can cause implant failure [265, 266]. Forsterite (\(\hbox {Mg}_{2}\hbox {SiO}_{4}\)), which has an orthorhombic-dipyramidal crystal structure can be used as an alternative to hydroxyapatite since it provides good adhesion strength and osteointegration [267, 268]. Forsterite crystal structure [269] is shown in Fig. 9.
Forsterite crystal structure [269]
Previous studies showed that magnesium keeps bone strong and is one of the essential components in the human body. It helps in maintaining blood glucose level and also assist in production of protein [270]. Silicon also plays an important role in bone development and maintenance. It has also been reported that silicon is mainly found in areas where new bone formation takes place [271]. Forsterite attracted a lot of interest due to better biocompatibility and good mechanical properties compared to HA [272]. Kichi et al. [273] prepared polycaprolactone/gelatin/forsterite nanocomposite. The Non-toxic and biodegradable properties of polycaprolactone allow them to show resistivity in bio fluids and it is also suitable for load-bearing applications. The hydrophobic nature results in reduced corrosion rate of implant materials [274, 275]. Gelatin, a natural polymer is obtained from hydrolysis of collagen, which in turn is extracted from skin and bone of animals. Moreover, Gelatin can be used as a composite material as it contains functional groups such as COOH which can form crosslinking with other biomaterial. It also makes the material more stable with good mechanical properties when mixed with other polymers [276]. It has been reported that as percentage of polycaprolactone in the coating increases, the corrosion resistance increases. In addition, cell growth of nanocomposite structure increases by decreasing the amount of gelatin [277]. Jeffery et al. [278] synthesized manganese oxide-doped forsterite powder. It has been reported that the hardness and fracture toughness increases up to certain temperature and then it starts decreasing. Naga et al. [279] studied the effect of forsterite addition in hydroxyapatite and concluded that in order to improve the physical and mechanical properties of the produced composite, maximum 20% of forsterite can be added.
Steatite can be used as another alternative to hydroxyapatite. Steatite (\(\hbox {MgSiO}_{3}\)) is a magnesium silicate composite material. It offers good electrical properties and high mechanical strength [280]. Due to its good biocompatibility, it is used as a implant material in artificial bone. Further, it can also be used as dental implant due to high hardness and bending strength [281].
8 Conclusions
In this review paper, we discussed about the role played by implant materials in improving the life standard and life expectancy of people. Implants can be classified based on material and area of application. Different coating technique was discussed in detail, and it was shown that surface modification of biomaterials through coating improves corrosion and other (mechanical, electrical, biological) properties of implant materials. This review attempts to show that HA properties can be improved by dopant ions such as \(\hbox {Zn}^{2+}\), \(\hbox {Sr}^{2+}\), and \(\hbox {Y}^{3+}\) and consequently bone regeneration time was reduced under the influence of electrical polarization and negative surface charge. Information is also provided on forsterite, steatite which could be used as an appropriate alternative to HA because of their better mechanical properties. However, electrical properties of forsterite and how it affect bone regeneration are yet to be studied in detail.
Availability of Data and Materials
Data sharing not applicable to this article as no datasets were generated or analyzed during the current study.
References
Dang, Z. M., Tian, C. Y., Zha, J. W., Yao, S. H., Xia, Y. J., Li, J. Y., Shi, C. Y., & Bai, J. (2009). Potential bioelectroactive bone regeneration polymer nanocomposites with high dielectric permittivity. Advanced Engineering Materials, 11(10), 144–147.
Basova, T. V., Vikulova, E. S., Dorovskikh, S. I., Hassan, A., & Morozova, N. B. (2021). The use of noble metal coatings and nanoparticles for the modification of medical implant materials. Materials & Design, 204, 109672.
Ratner, B. D., Hoffman, A. S., Schoen, F. J., & Lemons, J. E. (2004). Biomaterials science: an introduction to materials in medicine. California: San Diego.
Crawford, L., Wyatt, M., Bryers, J., & Ratner, B. (2021). Biocompatibility evolves: phenomenology to toxicology to regeneration. Advanced Healthcare Materials, 10(11), 2002153.
Sharkeev, Y., Eroshenko, A., Legostaeva, E., Kovalevskaya, Z., Belyavskaya, O., Khimich, M., Epple, M., Prymak, O., Sokolova, V., Zhu, Q., & Sun, Z. (2022). Development of Ultrafine-Grained and Nanostructured Bioinert Alloys Based on Titanium, Zirconium and Niobium and Their Microstructure. Mechanical and Biological Properties. Metals, 12(7), 1136.
Riester, O., Borgolte, M., Csuk, R., & Deigner, H. P. (2020). Challenges in bone tissue regeneration: stem cell therapy, biofunctionality and antimicrobial properties of novel materials and its evolution. International Journal of Molecular Sciences, 22(1), 192.
Prakasam, M., Locs, J., Salma-Ancane, K., Loca, D., Largeteau, A., & Berzina-Cimdina, L. (2017). Biodegradable materials and metallic implants-a review. Journal of functional biomaterials, 8(4), 44.
Walley, K. C., Bajraliu, M., Gonzalez, T., Nazarian, A., & Goulet, J. A. (2016). The chronicle of a stainless steel orthopaedic implant. The Orthopaedic Journal at Harvard Medical School, 17, 68–74.
Hanawa, T. (2019). Titanium-tissue interface reaction and its control with surface treatment. Frontiers in bioengineering and biotechnology, 7, 170.
Hryniewicz, T., & Rokicki, R. (2018). Modification of nitinol biomaterial for medical applications. World Scientific News, 96, 35–58.
Kirilova, I. A., Sadovoi, M. A., & Podorozhnaya, V. T. (2013). Ceramic and bone-ceramic implants: promising directions. Khirurgiya Pozvonochnnika, 4, 52–62.
Andreiotelli, M., Wenz, H. J., & Kohal, R. J. (2009). Are ceramic implants a viable alternative to titanium implants? a systematic literature review. Clinical Oral Implants Research, 20, 32–47.
Lawton, K., Le, H., Tredwin, C., & Handy, R. D. (2019). Carbon nanotube reinforced hydroxyapatite nanocomposites as bone implants: Nanostructure, mechanical strength and biocompatibility. International Journal of Nanomedicine, 14, 7947.
Nazerali, R., Rogers, J., Canter, R., Hinchcliff, K. M., & Stevenson, T. R. (2015). The use of polypropylene mesh in chest wall reconstruction; a novel approach. Journal of Plastic, Reconstructive & Aesthetic Surgery, 68(2), 275–276.
Mahabir, R. C., & Butler, C. E. (2011). Stabilization of the chest wall: autologous and alloplastic reconstructions. In Seminars in Plastic Surgery, 25(01), 034–042.
Scholz, M. S., Blanchfield, J. P., Bloom, L. D., Coburn, B. H., Elkington, M., Fuller, J. D., Gilbert, M. E., Muflahi, S. A., Pernice, M. F., Rae, S. I., & Trevarthen, J. A. (2011). The use of composite materials in modern orthopaedic medicine and prosthetic devices: A review. Composites Science and Technology, 71(16), 1791–1803.
Li, C. S., Vannabouathong, C., Sprague, S., & Bhandari, M. (2015). The use of carbon-fiber-reinforced (CFR) PEEK material in orthopedic implants: a systematic review. Clinical Medicine Insights: Arthritis and Musculoskeletal Disorders, 8, 20354.
Magnani, G., Fabbri, P., Leoni, E., Salernitano, E., & Mazzanti, F. (2021). New perspectives on zirconia composites as biomaterials. Journal of Composites Science, 5(9), 244.
Petersen, R. (2016). Carbon fiber biocompatibility for implants. Fibers, 4(1), 1.
Gerasimenko, A. Y., Kurilova, U. E., Savelyev, M. S., Murashko, D. T., & Glukhova, O. E. (2021). Laser fabrication of composite layers from biopolymers with branched 3D networks of single-walled carbon nanotubes for cardiovascular implants. Composite Structures, 260, 113517.
Tang, Z. B., Niu, J. L., Huang, H., Zhang, H., Pei, J., Ou, J. M., & Yuan, G. Y. (2017). Potential biodegradable Zn-Cu binary alloys developed for cardiovascular implant applications. Journal of the Mechanical Behavior of Biomedical Materials, 72, 182–191.
Jung, F., Wischke, C., & Lendlein, A. (2010). Degradable, multifunctional cardiovascular implants: challenges and hurdles. MRS Bulletin, 35(8), 607–613.
Holman, H., Kavarana, M. N., & Rajab, T. K. (2021). Smart materials in cardiovascular implants: shape memory alloys and shape memory polymers. Artificial Organs, 45(5), 454–463.
Godbole, N., Yadav, S., Ramachandran, M., & Belemkar, S. (2016). A review on surface treatment of stainless steel orthopedic implants. International Journal of Pharmaceutical Sciences and Research, 36(1), 190–4.
Wawrzynski, J., Gil, J. A., Goodman, A. D., & Waryasz, G. R. (2017). Hypersensitivity to orthopedic implants: a review of the literature. Rheumatology and Therapy, 4(1), 45–56.
Zeng, F. G., Rebscher, S., Harrison, W., Sun, X., & Feng, H. (2008). Cochlear implants: system design, integration, and evaluation. IEEE Reviews in Biomedical Engineering, 1, 115–142.
Gan, R. Z., Dai, C., Wang, X., Nakmali, D., & Wood, M. W. (2010). A totally implantable hearing system-design and function characterization in 3D computational model and temporal bones. Hearing Research, 263(1–2), 138–144.
Rajak, D. K., Pagar, D. D., Kumar, R., & Pruncu, C. I. (2019). Recent progress of reinforcement materials: a comprehensive overview of composite materials. Journal of Materials Research and Technology, 8(6), 6354–6374.
Mercuri, L. G., Miloro, M., Skipor, A. K., Bijukumar, D., Sukotjo, C., & Mathew, M. T. (2018). Serum metal levels in maxillofacial reconstructive surgery patients: a pilot study. Journal of Oral and Maxillofacial Surgery, 76(10), 2074–2080.
Huang, Q. W., Wang, L. P., & Wang, J. Y. (2014). Mechanical properties of artificial materials for bone repair. Journal of Shanghai Jiaotong University (Science), 19(6), 675–680.
Abbasi, N., Hamlet, S., Love, R. M., & Nguyen, N. T. (2020). Porous scaffolds for bone regeneration. Journal of Science: Advanced Materials and Devices, 5(1), 1–9.
Gode, C., Attarilar, S., Eghbali, B., & Ebrahimi, M. (2015). Electrochemical behavior of equal channel angular pressed titanium for biomedical application. In AIP Conference Proceedings, 1653(1), 020041.
Liang, S. X., Feng, X. J., Yin, L. X., Liu, X. Y., Ma, M. Z., & Liu, R. P. (2016). Development of a new \(\beta\) Ti alloy with low modulus and favorable plasticity for implant material. Materials Science and Engineering: C, 61, 338–343.
Zeller, A., Musyanovych, A., Kappl, M., Ethirajan, A., Dass, M., Markova, D., Klapper, M., & Landfester, K. (2010). Nanostructured coatings by adhesion of phosphonated polystyrene particles onto titanium surface for implant material applications. ACS Applied Materials & Interfaces, 2(8), 2421–2428.
Callioglu, S., & Acar, P. (2020). Design of \(\beta\)-Titanium microstructures for implant materials. Materials Science and Engineering: C, 110, 110715.
Mohammed, M. T., Khan, Z. A., & Siddiquee, A. N. (2014). Beta titanium alloys: the lowest elastic modulus for biomedical applications: a review. International Journal of Research in Chemical, Metallurgical and Civil Engineering, 8(8), 726.
Niinomi, M. (2002). Recent metallic materials for biomedical applications. Metallurgical and Materials Transactions A, 33(3), 477–486.
Liang, S. (2020). Review of the design of titanium alloys with low elastic modulus as implant materials. Advanced Engineering Materials, 22(11), 2000555.
Chen, Q., & Thouas, G. A. (2015). Metallic implant biomaterials. Materials Science and Engineering: R: Reports, 87, 1–57.
Anene, F. A., Aiza Jaafar, C. N., Zainol, I., Azmah Hanim, M. A., & Suraya, M. T. (2021). Biomedical materials: A review of titanium based alloys. Proceedings of the Institution of Mechanical Engineers, Part C: Journal of Mechanical Engineering Science, 235(19), 3792–3805.
Renganathan, G., Tanneru, N., & Madurai, S. L. (2018). Orthopedical and biomedical applications of titanium and zirconium metals (pp. 211–241). Fundamental Biomaterials: Metals.
Song, G. L. (2007). Control of degradation of biocompatible magnesium in a pseudo-physiological environment by a ceramic like anodized coating. Advanced Materials Research, 29, 95–98.
Zhou, H., Liang, B., Jiang, H., Deng, Z., & Yu, K. (2021). Magnesium-based biomaterials as emerging agents for bone repair and regeneration: from mechanism to application. Journal of Magnesium and Alloys, 9(3), 779–804.
Song, G., & Song, S. (2007). A possible biodegradable magnesium implant material. Advanced Engineering Materials, 9(4), 298–302.
Kuhlmann, J., Bartsch, I., Willbold, E., Schuchardt, S., Holz, O., Hort, N., Höche, D., Heineman, W. R., & Witte, F. (2013). Fast escape of hydrogen from gas cavities around corroding magnesium implants. Acta Biomaterialia, 9(10), 8714–8721.
Milošev, I. (2012). CoCrMo alloy for biomedical applications. Biomedical Applications, 2, 1–72.
Huynh, V., Ngo, N. K., & Golden, T. D. (2019). Surface activation and pretreatments for biocompatible metals and alloys used in biomedical applications. International Journal of Biomaterials, 2, 2.
Hart, A. J., Quinn, P. D., Sampson, B., Sandison, A., Atkinson, K. D., Skinner, J. A., Powell, J. J., & Mosselmans, J. F. W. (2010). The chemical form of metallic debris in tissues surrounding metal-on-metal hips with unexplained failure. Acta Biomaterialia, 6(11), 4439–4446.
Kop, A. M., & Swarts, E. (2009). Corrosion of a hip stem with a modular neck taper junction: a retrieval study of 16 cases. The Journal of Arthroplasty, 24(7), 1019–1023.
Tekdir, H., & Yetim, A. F. (2021). Additive manufacturing of multiple layered materials (Ti6Al4V/316L) and improving their tribological properties with glow discharge surface modification. Vacuum, 184, 109893.
Turalioglu, K., Taftali, M., Tekdir, H., Comakli, O., Yazici, M., Yetim, T., & Yetim, A. F. (2021). The tribological and corrosion properties of anodized Ti6Al4V/316L bimetallic structures manufactured by additive manufacturing. Surface and Coatings Technology, 405, 126635.
Tekdir, H., Yetim, T., & Yetim, A. F. (2021). Corrosion properties of ceramic-based TiO2 films on plasma oxidized Ti6Al4V/316L layered implant structured manufactured by selective laser melting. Journal of Bionic Engineering, 18(4), 944–957.
Vallet-Regi, M. (2001). Ceramics for medical applications. Journal of the Chemical Society, Dalton Transactions, 2, 97–108.
McEntire, B. J., Bal, B. S., Rahaman, M. N., Chevalier, J., & Pezzotti, G. (2015). Ceramics and ceramic coatings in orthopaedics. Journal of the European Ceramic Society, 35(16), 4327–4369.
Gallusi, G., Campanella, V., Montemurro, E., Di Taranto, V., & Libonati, A. (2020). Antibacterial activity of first and latest generation bioceramic sealers on the elimination of enterococcus faecalis: An in vitro study. Journal of Biological Regulators and Homeostatic Agents, 34, 73–79.
Kumar, P., Dehiya, B. S., & Sindhu, A. (2018). Bioceramics for hard tissue engineering applications: A review. International Journal of Applied Engineering Research, 13(5), 2744–2752.
Khanna, R., Ong, J. L., Oral, E., & Narayan, R. J. (2017). Progress in wear resistant materials for total hip arthroplasty. Coatings, 7(7), 99.
Huang, J., & Best, S. M. (2022). Ceramic biomaterials for tissue engineering. Tissue Engineering Using Ceramics and Polymers, 2, 3–40.
Chai, J., Chu, F., Chow, T. W., & Liang, B. M. (2007). Chemical solubility and flexural strength of zirconia-based ceramics. International Journal of Prosthodontics, 20, 6.
Grech, J., & Antunes, E. (2019). Zirconia in dental prosthetics: A literature review. Journal of Materials Research and Technology, 8(5), 4956–4964.
von Wilmowsky, C., Moest, T., Nkenke, E., Stelzle, F., & Schlegel, K. A. (2014). Implants in bone: Part I. A current overview about tissue response, surface modifications and future perspectives. Oral and Maxillofacial Surgery, 18(3), 243–257.
Monzavi, M., Noumbissi, S., & Nowzari, H. (2017). The Impact of in vitro accelerated aging, approximating 30 and 60 years in vivo, on commercially available zirconia dental implants. Clinical Implant Dentistry and Related Research, 19(2), 245–252.
Chevalier, J., Gremillard, L., & Deville, S. (2007). Low-temperature degradation of zirconia and implications for biomedical implants. Annual Review of Materials Research, 37, 1–32.
Benzaid, R., Chevalier, J., Saâdaoui, M., Fantozzi, G., Nawa, M., Diaz, L. A., & Torrecillas, R. (2008). Fracture toughness, strength and slow crack growth in a ceria stabilized zirconia-alumina nanocomposite for medical applications. Biomaterials, 29(27), 3636–3641.
Tang, D., Lim, H. B., Lee, K. J., Lee, C. H., & Cho, W. S. (2012). Evaluation of mechanical reliability of zirconia-toughened alumina composites for dental implants. Ceramics International, 38(3), 2429–2436.
Gautam, G., Kumar, S., & Kumar, K. (2021). Processing of biomaterials for bone tissue engineering: state of the art. Materials Today: Proceedings.
Hamdy, T. M. (2018). Polymers and ceramics biomaterials in orthopedics and dentistry: A review article. Egyptian Journal of Chemistry, 61(4), 723–730.
Camilleri, J. (2017). Will bioceramics be the future root canal filling materials? Current Oral Health Reports, 4(3), 228–238.
Dorozhkin, S. V. (2018). Current state of bioceramics. Journal of Ceramic Science and Technology, 9(4), 353–370.
Brie, J., Chartier, T., Chaput, C., Delage, C., Pradeau, B., Caire, F., Boncoeur, M. P., & Moreau, J. J. (2013). A new custom made bioceramic implant for the repair of large and complex craniofacial bone defects. Journal of Cranio-Maxillofacial Surgery, 41(5), 403–407.
Vallet-Regi, M., & Salinas, A. J. (2019). Ceramics as bone repair materials. Bone Repair Biomaterials, 2, 141–178.
Piconi, C., & Sprio, S. (2021). Oxide bioceramic composites in orthopedics and dentistry. Journal of Composites Science, 5(8), 206.
Dorozhkin, S. V. (2018). Current state of bioceramics. Journal of Ceramic Science and Technology, 9(4), 353–370.
Mbarki, M., Sharrock, P., Fiallo, M., & ElFeki, H. (2017). Hydroxyapatite bioceramic with large porosity. Materials Science and Engineering: C, 76, 985–990.
Vallet-Regi, M., Salinas, A. J., & Arcos, D. (2006). From the bioactive glasses to the star gels. Journal of Materials Science: Materials in Medicine, 17(11), 1011–1017.
Chen, J., Zhang, X., Li, B., & Yang, Y. (2020). Flexible organic-inorganic hybrid bioceramic for bone tissue regeneration. Journal of Advanced Dielectrics, 10(04), 2050013.
Vallet-Regi, M., Ruiz-Gonzalez, L., Izquierdo-Barba, I., & Gonzalez-Calbet, J. M. (2006). Revisiting silica based ordered mesoporous materials: medical applications. Journal of Materials Chemistry, 16(1), 26–31.
Garcia, A., Cabanas, M. V., Pena, J., & Sanchez-Salcedo, S. (2021). Design of 3d scaffolds for hard tissue engineering: From apatites to silicon mesoporous materials. Pharmaceutics, 13(11), 1981.
Baino, F., Novajra, G., & Vitale-Brovarone, C. (2015). Bioceramics and scaffolds: a winning combination for tissue engineering. Frontiers in Bioengineering and Biotechnology, 3, 202.
Bari, A., Bloise, N., Fiorilli, S., Novajra, G., Vallet-Regi, M., Bruni, G., Torres-Pardo, A., Gonzalez-Calbet, J. M., Visai, L., & Vitale-Brovarone, C. (2017). Copper-containing mesoporous bioactive glass nanoparticles as multifunctional agent for bone regeneration. Acta Biomaterialia, 55, 493–504.
Shi, Q. H., Wang, J. F., Zhang, J. P., Fan, J., & Stucky, G. D. (2006). Rapid setting, mesoporous, bioactive glass cements that induce accelerated in vitro apatite formation. Advanced Materials, 18(8), 1038–1042.
Shekhawat, D., Singh, A., Bhardwaj, A., & Patnaik, A. (2021). A short review on polymer, metal and ceramic based implant materials. In IOP Conference Series: Materials Science and Engineering, 1017(1), 012038.
Park, J. B., & Lakes, R. S. (2007). Polymeric implant materials. Biomaterials, 2, 173–205.
Wiesli, M. G., & Ozcan, M. (2015). High-performance polymers and their potential application as medical and oral implant materials: a review. Implant Dentistry, 24(4), 448–457.
Guo, B., & Ma, P. X. (2018). Conducting polymers for tissue engineering. Biomacromolecules, 19(6), 1764–1782.
Rikhari, B., Mani, S. P., & Rajendran, N. (2020). Polypyrrole/graphene oxide composite coating on Ti implants: a promising material for biomedical applications. Journal of Materials Science, 55(12), 5211–5229.
Fonseca, A. C., Serra, A. C., & Coelho, J. F. (2015). Bioabsorbable polymers in cancer therapy: latest developments. Epma Journal, 6(1), 1–18.
Basak, S. (2021). Redesigning the modern applied medical sciences and engineering with shape memory polymers. Advanced Composites and Hybrid Materials, 4(2), 223–234.
Kazimierczak, P., & Przekora, A. (2020). Osteoconductive and osteoinductive surface modifications of biomaterials for bone regeneration: A concise review. Coatings, 10(10), 971.
Han, X., Yang, D., Yang, C., Spintzyk, S., Scheideler, L., Li, P., Li, D., Geis-Gerstorfer, J., & Rupp, F. (2019). Carbon fiber reinforced PEEK composites based on 3D-printing technology for orthopedic and dental applications. Journal of Clinical Medicine, 8(2), 240.
Amani, H., Arzaghi, H., Bayandori, M., Dezfuli, A. S., Pazok-Toroudi, H., Shafiee, A., & Moradi, L. (2019). Controlling cell behavior through the design of biomaterial surfaces: a focus on surface modification techniques. Advanced Materials Interfaces, 6(13), 1900572.
Mahajan, A., & Sidhu, S. S. (2018). Surface modification of metallic biomaterials for enhanced functionality: a review. Materials Technology, 33(2), 93–105.
Kulkarni, M., Mazare, A., Schmuki, P., Iglič, A., & Seifalian, A. (2014). Biomaterial surface modification of titanium and titanium alloys for medical applications. Nanomedicine, 111(615), 111.
Mercuri, L. G., Urban, R. M., Hall, D. J., & Mathew, M. T. (2017). Adverse local tissue responses to failed temporomandibular joint implants. Journal of Oral and Maxillofacial Surgery, 75(10), 2076–2084.
Manam, N. S., Harun, W. S. W., Shri, D. N. A., Ghani, S. A. C., Kurniawan, T., Ismail, M. H., & Ibrahim, M. H. I. (2017). Study of corrosion in biocompatible metals for implants: A review. Journal of Alloys and Compounds, 701, 698–715.
Manivasagam, G., Dhinasekaran, D., & Rajamanickam, A. (2010). Biomedical implants: corrosion and its prevention-a review. Recent Patents on Corrosion Science, 2, 1.
Chen, Q., & Thouas, G. A. (2015). Metallic implant biomaterials. Materials Science and Engineering: R: Reports, 87, 1–57.
Beltran, M. J., Collinge, C. A., & Gardner, M. J. (2016). Stress modulation of fracture fixation implants. Journal of the American Academy of Orthopaedic Surgeons, 24(10), 711–719.
Antunes, R. A., & de Oliveira, M. C. L. (2012). Corrosion fatigue of biomedical metallic alloys: mechanisms and mitigation. Acta Biomaterialia, 8(3), 937–962.
Hashemi, R. (2020). Failure Analysis of Biometals. Metals, 10(5), 662.
Wang, J. W., Yang, H., Wang, C. T., Jin, Z. M., & Dai, K. R. (2019). Wear and Diagnostic Analysis of Clinical Failures of Artificial Hip Joints. In UHMWPE Biomaterials for Joint Implants, 317–339.
Ramsden, J. J., Allen, D. M., Stephenson, D. J., Alcock, J. R., Peggs, G. N., Fuller, G., & Goch, G. (2007). The design and manufacture of biomedical surfaces. CIRP Annals, 56(2), 687–711.
Papageorgiou, I., Shadrick, V., Davis, S., Hails, L., Schins, R., Newson, R., Fisher, J., Ingham, E., & Case, C. P. (2008). Macrophages detoxify the genotoxic and cytotoxic effects of surgical cobalt chrome alloy particles but not quartz particles on human cells in vitro. Mutation Research/Fundamental and Molecular Mechanisms of Mutagenesis, 643(1–2), 11–19.
Terkawi, M. A., Hamasaki, M., Takahashi, D., Ota, M., Kadoya, K., Yutani, T., Uetsuki, K., Asano, T., Irie, T., Arai, R., & Onodera, T. (2018). Transcriptional profile of human macrophages stimulated by ultra-high molecular weight polyethylene particulate debris of orthopedic implants uncovers a common gene expression signature of rheumatoid arthritis. Acta Biomaterialia, 65, 417–425.
Bose, S., Robertson, S. F., & Bandyopadhyay, A. (2018). Surface modification of biomaterials and biomedical devices using additive manufacturing. Acta Biomaterialia, 66, 6–22.
Qiu, Z. Y., Chen, C., Wang, X. M., & Lee, I. S. (2014). Advances in the surface modification techniques of bone-related implants for last 10 years. Regenerative Biomaterials, 1(1), 67–79.
Zhang, B. G., Myers, D. E., Wallace, G. G., Brandt, M., & Choong, P. F. (2014). Bioactive coatings for orthopaedic implants-recent trends in development of implant coatings. International Journal of Molecular Sciences, 15(7), 11878–11921.
Kumar, M., Kumar, R., & Kumar, S. (2021). Coatings on orthopedic implants to overcome present problems and challenges: A focused review. Materials Today: Proceedings, 45, 5269–5276.
Bronzino, J. D. (2000). Biomedical Engineering Handbook 2. Springer Science & Business Media.
Dumitrescu, L. N., Neacsu, P., Necula, M. G., Bonciu, A., Marascu, V., Cimpean, A., Moldovan, A., Rotaru, A., Dinca, V., & Dinescu, M. (2020). Induced hydrophilicity and in vitro preliminary osteoblast response of polyvinylidene fluoride (PVDF) coatings obtained via maple deposition and subsequent thermal treatment. Molecules, 25(3), 582.
Wang, Y., Jeong, H., Chowdhury, M., Arnold, C. B., & Priestley, R. D. (2018). Exploiting physical vapor deposition for morphological control in semi-crystalline polymer films. Polymer Crystallization, 1(4), 10021.
Singh, J., Chatha, S. S., & Singh, H. (2021). Synthesis and characterization of plasma sprayed functional gradient bioceramic coating for medical implant applications. Ceramics International, 47(7), 9143–9155.
Harun, W. S. W., Asri, R. I. M., Alias, J., Zulkifli, F. H., Kadirgama, K., Ghani, S. A. C., & Shariffuddin, J. H. M. (2018). A comprehensive review of hydroxyapatite-based coatings adhesion on metallic biomaterials. Ceramics International, 44(2), 1250–1268.
Mucalo, M. R. (2015). Animal-bone derived hydroxyapatite in biomedical applications. In Hydroxyapatite (HAp) for Biomedical Applications, 307-342.
Sun, L., Berndt, C. C., & Grey, C. P. (2003). Phase, structural and microstructural investigations of plasma sprayed hydroxyapatite coatings. Materials Science and Engineering: A, 360(1–2), 70–84.
Singh, G., Singh, S., & Prakash, S. (2011). Surface characterization of plasma sprayed pure and reinforced hydroxyapatite coating on Ti6Al4V alloy. Surface and Coatings Technology, 205(20), 4814–4820.
Bulloch, J. H., & Callagy, A. G. (1999). An in situ wear-corrosion study on a series of protective coatings in large induced draft fans. Wear, 233, 284–292.
Knuuttila, J., Ahmaniemi, S., & Mäntylä, T. (1999). Wet abrasion and slurry erosion resistance of thermally sprayed oxide coatings. Wear, 232(2), 207–212.
Moore, B., Asadi, E., & Lewis, G. (2016). Deposition methods for microstructured and nanostructured coatings on metallic bone implants: a review. Advances in Materials Science and Engineering, 2, 2.
Schou, J. (2009). Physical aspects of the pulsed laser deposition technique: The stoichiometric transfer of material from target to film. Applied Surface Science, 255(10), 5191–5198.
Kurella, A., & Dahotre, N. B. (2005). Surface modification for bioimplants: the role of laser surface engineering. Journal of Biomaterials Applications, 20(1), 5–50.
Mohseni, E., Zalnezhad, E., & Bushroa, A. R. (2014). Comparative investigation on the adhesion of hydroxyapatite coating on Ti-6Al-4V implant: A review paper. International Journal of Adhesion and Adhesives, 48, 238–257.
Boidin, R., Halenkovic, T., Nazabal, V., Benes, L., & Nemec, P. (2016). Pulsed laser deposited alumina thin films. Ceramics International, 42(1), 1177–1182.
Popescu-Pelin, G., Sima, F., Sima, L. E., Mihailescu, C. N., Luculescu, C., Iordache, I., Socol, M., Socol, G., & Mihailescu, I. N. (2017). Hydroxyapatite thin films grown by pulsed laser deposition and matrix assisted pulsed laser evaporation: Comparative study. Applied Surface Science, 418, 580–588.
Kuppuswamy, H., & Ganesan, A. (2016). Structural, mechanical and in vitro studies on pulsed laser deposition of hydroxyapatite on additive manufactured polyamide substrate. International Journal of Bioprinting, 2, 2.
Nasar, A. (2019). Hydroxyapatite and its coatings in dental implants. In Applications of Nanocomposite Materials in Dentistry, 145-160.
Bao, Q., Chen, C., Wang, D., Ji, Q., & Lei, T. (2005). Pulsed laser deposition and its current research status in preparing hydroxyapatite thin films. Applied Surface Science, 252(5), 1538–1544.
Shi, J. Z., Chen, C. Z., Yu, H. J., & Zhang, S. J. (2008). Application of magnetron sputtering for producing bioactive ceramic coatings on implant materials. Bulletin of Materials Science, 31(6), 877–884.
Nelea, V., Morosanu, C., Iliescu, M., & Mihailescu, I. N. (2004). Hydroxyapatite thin films grown by pulsed laser deposition and radio-frequency magnetron sputtering: comparative study. Applied Surface Science, 228(1–4), 346–356.
Hamdi, D. A., Jiang, Z. T., No, K., Rahman, M. M., Lee, P. C., Truc, L. N. T., Kim, J., Altarawneh, M., Thair, L., Jumaa, T. A. J., & Dlugogorski, B. Z. (2019). Biocompatibility study of multi-layered hydroxyapatite coatings synthesized on Ti-6Al-4V alloys by RF magnetron sputtering for prosthetic-orthopaedic implant applications. Applied Surface Science, 463, 292–299.
Xu, S., Long, J., Sim, L., Diong, C. H., & Ostrikov, K. (2005). RF plasma sputtering deposition of hydroxyapatite bioceramics: synthesis, performance, and biocompatibility. Plasma Processes and Polymers, 2(5), 373–390.
Nathanael, A. J., Yuvakkumar, R., Hong, S. I., & Oh, T. H. (2014). Novel zirconium nitride and hydroxyapatite nanocomposite coating: detailed analysis and functional properties. ACS Applied Materials & Interfaces, 6(12), 9850–9857.
Socol, G., Macovei, A. M., Miroiu, F., Stefan, N., Duta, L., Dorcioman, G., Mihailescu, I. N., Petrescu, S. M., Stan, G. E., Marcov, D. A., & Chiriac, A. (2010). Hydroxyapatite thin films synthesized by pulsed laser deposition and magnetron sputtering on PMMA substrates for medical applications. Materials Science and Engineering: B, 169(1–3), 159–168.
Annavarapu, R. K., Kim, S., Wang, M., Hart, A. J., & Sojoudi, H. (2019). Explaining evaporation-triggered wetting transition using local force balance model and contact line-fraction. Scientific Reports, 9(1), 1–17.
Sojoudi, H., Kim, S., Zhao, H., Annavarapu, R. K., Mariappan, D., Hart, A. J., McKinley, G. H., & Gleason, K. K. (2017). Stable wettability control of nanoporous microstructures by iCVD coating of carbon nanotubes. ACS Applied Materials & Interfaces, 9(49), 43287–43299.
Tang, X., & Yan, X. (2017). Dip-coating for fibrous materials: Mechanism, methods and applications. Journal of Sol-Gel Science and Technology, 81(2), 378–404.
Grosso, D. (2011). How to exploit the full potential of the dip-coating process to better control film formation. Journal of Materials Chemistry, 21(43), 17033–17038.
Ritwik, A., Saju, K. K., Vengellur, A., & Saipriya, P. P. (2022). Development of thin-film hydroxyapatite coatings with an intermediate shellac layer produced by dip-coating process on Ti6Al4V implant materials. Journal of Coatings Technology and Research, 19(2), 597–605.
Su, H. Y., Chen, P. L., & Lin, C. S. (2016). Sol-gel coatings doped with organosilane and cerium to improve the properties of hot-dip galvanized steel. Corrosion Science, 102, 63–71.
Dario, A. F., Macia, H. B., & Petri, D. F. (2012). Nanostructures on spin-coated polymer films controlled by solvent composition and polymer molecular weight. Thin Solid Films, 524, 185–190.
Tyona, M. D. (2013). A theoritical study on spin coating technique. Advances in Materials Research, 2(4), 195.
Raphel, J., Karlsson, J., Galli, S., Wennerberg, A., Lindsay, C., Haugh, M. G., Pajarinen, J., Goodman, S. B., Jimbo, R., Andersson, M., & Heilshorn, S. C. (2016). Engineered protein coatings to improve the osseointegration of dental and orthopaedic implants. Biomaterials, 83, 269–282.
Soule, L. D., Pajares Chomorro, N., Chuong, K., Mellott, N., Hammer, N., Hankenson, K. D., & Chatzistavrou, X. (2020). Sol-gel-derived bioactive and antibacterial multi-component thin films by the spin-coating technique. ACS Biomaterials Science & Engineering, 6(10), 5549–5562.
Sichert, J. A., Tong, Y., Mutz, N., Vollmer, M., Fischer, S., Milowska, K. Z., García Cortadella, R., Nickel, B., Cardenas-Daw, C., Stolarczyk, J. K., & Urban, A. S. (2015). Quantum size effect in organometal halide perovskite nanoplatelets. Nano Letters, 15(10), 6521–6527.
Shrivastava, S., & Dash, D. (2009). Applying nanotechnology to human health: revolution in biomedical sciences. Journal of Nanotechnology, 2009.
Yarlagadda, T., Sharma, S., Yarlagadda, P. K., & Sharma, J. (2019). Recent developments in the Field of nanotechnology for development of medical implants. Procedia Manufacturing, 30, 544–551.
Gupta, S., Noumbissi, S., & Kunrath, M. F. (2020). Nano modified zirconia dental implants: Advances and the frontiers for rapid osseointegration. Medical Devices & Sensors, 3(3), 10076.
Kumar, S., Nehra, M., Kedia, D., Dilbaghi, N., Tankeshwar, K., & Kim, K. H. (2020). Nanotechnology-based biomaterials for orthopaedic applications: Recent advances and future prospects. Materials Science and Engineering: C, 106, 110154.
Arumugam, S., & Ju, Y. (2021). Carbon nanotubes reinforced with natural/synthetic polymers to mimic the extracellular matrices of bone-a review. Materials Today Chemistry, 20, 100420.
Epp, J. (2016). X-ray diffraction (XRD) techniques for materials characterization. In Materials Characterization using Nondestructive Evaluation (NDE) Methods, 81–124.
Nayak, B., & Misra, P. K. (2020). Exploration of the structural and dielectric characteristics of a potent hydroxyapatite coated gallium bioceramics for the forthcoming biomedical and orthopedic applications. Materials Chemistry and Physics, 239, 121967.
Inkson, B. J. (2016). Scanning electron microscopy (SEM) and transmission electron microscopy (TEM) for materials characterization. In Materials Characterization using Nondestructive Evaluation (NDE) methods, 17-43.
Reem, A. W., Jafer, R., Yahia, I. S., Al-Ghamdi, A. A., Al-ghamdi, M. A., & El-Naggar, A. M. (2017). Fast and easy synthesis of novel Strontium apatite nanostructured phase: Structure, spectroscopy, and dielectric analysis. Ceramics International, 43(18), 17153–17159.
Nehring, J., Schütz, M., Dietz, M., Nasr, I., Aufinger, K., Weigel, R., & Kissinger, D. (2016). Highly integrated 4–32-GHz two-port vector network analyzers for instrumentation and biomedical applications. IEEE Transactions on Microwave Theory and Techniques, 65(1), 229–244.
Kaygili, O., Dorozhkin, S. V., Ates, T., Gursoy, N. C., Keser, S., Yakuphanoglu, F., & Selcuk, A. B. (2015). Structural and dielectric properties of yttrium-substituted hydroxyapatites. Materials Science and Engineering: C, 47, 333–338.
Aal, N. A., Bououdina, M., Hajry, A., Chaudhry, A. A., Darr, J. A., Al-Ghamdi, A. A., El-Mossalamy, E. H., Al-Ghamdi, A. A., Sung, Y. K., & El-Tantawy, F. (2011). Synthesis, characterization and electrical properties of hydroxyapatite nanoparticles from utilization of biowaste eggshells. Biomaterials Research, 15(2), 52–9.
Kobayashi, T., Nakamura, S., & Yamashita, K. (2001). Enhanced osteobonding by negative surface charges of electrically polarized hydroxyapatite. Journal of Biomedical Materials Research: An Official Journal of The Society for Biomaterials, The Japanese Society for Biomaterials, and The Australian Society for Biomaterials and the Korean Society for Biomaterials, 57(4), 477–484.
Kaygili, O., Dorozhkin, S. V., & Keser, S. (2014). Synthesis and characterization of Ce-substituted hydroxyapatite by sol-gel method. Materials Science and Engineering: C, 42, 78–82.
Kato, R., Nakamura, S., Katayama, K., & Yamashita, K. (2005). Electrical polarization of plasma-spray-hydroxyapatite coatings for improvement of osteoconduction of implants. Journal of Biomedical Materials Research Part A: An Official Journal of The Society for Biomaterials, The Japanese Society for Biomaterials, and The Australian Society for Biomaterials and the Korean Society for Biomaterials, 74(4), 652–658.
Sarin, N., Singh, K. J., Singh, D., Arora, S., Singh, A. P., & Mahajan, H. (2020). Preliminary studies of strontium and selenium binary doped CaO-SiO2-P2O5-MgO bioceramics for faster growth of hydroxyapatite and bone regeneration applications. Materials Chemistry and Physics, 253, 123329.
Uribe, R., Rojas, I., Riofrio, M. C., Lascano, L., & González, G. (2022). Polarization and biomineralization of hydroxyapatite-barium titanate composites. In Journal of Physics: Conference Series, 2238(1), 012007.
Ratha, I., Datta, P., Balla, V. K., Nandi, S. K., & Kundu, B. (2021). Effect of doping in hydroxyapatite as coating material on biomedical implants by plasma spraying method: A review. Ceramics International, 47(4), 4426–4445.
Salem, R., Thurston, K. G., Carr, B. I., Goin, J. E., & Geschwind, J. F. H. (2002). Yttrium-90 microspheres: radiation therapy for unresectable liver cancer. Journal of Vascular and Interventional Radiology, 13(9), 223–229.
Geschwind, J. F. H., Salem, R., Carr, B. I., Soulen, M. C., Thurston, K. G., Goin, K. A., Van Buskirk, M., Roberts, C. A., & Goin, J. E. (2004). Yttrium-90 microspheres for the treatment of hepatocellular carcinoma. Gastroenterology, 127(5), 194–205.
Liu, Y., Zhou, R. J., Mo, A. C., Chen, Z. Q., & Wu, H. K. (2007). Synthesis and characterization of yttrium/hydroxyapatite nanoparticles. In Key Engineering Materials, 330, 295–298.
Webster, T. J., Ergun, C., Doremus, R. H., & Bizios, R. (2002). Hydroxylapatite with substituted magnesium, zinc, cadmium, and yttrium. II. Mechanisms of osteoblast adhesion. Journal of Biomedical Materials Research: An Official Journal of The Society for Biomaterials, The Japanese Society for Biomaterials, and The Australian Society for Biomaterials and the Korean Society for Biomaterials, 59(2), 312–317.
Kaygili, O., Ates, T., Keser, S., Al-Ghamdi, A. A., & Yakuphanoglu, F. (2014). Controlling of dielectrical properties of hydroxyapatite by ethylenediamine tetraacetic acid (EDTA) for bone healing applications. Spectrochimica Acta Part A: Molecular and Biomolecular Spectroscopy, 129, 268–273.
Singh, B., Dubey, A. K., Kumar, S., Saha, N., Basu, B., & Gupta, R. (2011). In vitro biocompatibility and antimicrobial activity of wet chemically prepared Ca10- xAgx (PO4) 6 (OH) 2 (0.0\(\le\) x\(\le\) 0.5) hydroxyapatites. Materials Science and Engineering: C, 31(7), 1320–1329.
Shahbazi, M. A., Faghfouri, L., Ferreira, M. P., Figueiredo, P., Maleki, H., Sefat, F., Hirvonen, J., & Santos, H. A. (2020). The versatile biomedical applications of bismuth-based nanoparticles and composites: therapeutic, diagnostic, biosensing, and regenerative properties. Chemical Society Reviews, 49(4), 1253–1321.
Al-Hazmi, F. E. (2016). Synthesis and electrical properties of Bi doped hydroxyapatite ceramics. Journal of Alloys and Compounds, 665, 119–123.
Sato, M., Sambito, M. A., Aslani, A., Kalkhoran, N. M., Slamovich, E. B., & Webster, T. J. (2006). Increased osteoblast functions on undoped and yttrium-doped nanocrystalline hydroxyapatite coatings on titanium. Biomaterials, 27(11), 2358–2369.
Dubey, A. K., Mallik, P. K., Kundu, S., & Basu, B. (2013). Dielectric and electrical conductivity properties of multi-stage spark plasma sintered HA-CaTiO3 composites and comparison with conventionally sintered materials. Journal of the European Ceramic Society, 33(15–16), 3445–3453.
Ahmed, M. K., Mansour, S. F., Al-Wafi, R., & Abdel-Fattah, E. (2021). Nanofibers scaffolds of co-doped Bi/Sr-hydroxyapatite encapsulated into polycaprolactone for biomedical applications. Journal of Materials Research and Technology, 13, 2297–2309.
Gentleman, E., Fredholm, Y. C., Jell, G., Lotfibakhshaiesh, N., O’Donnell, M. D., Hill, R. G., & Stevens, M. M. (2010). The effects of strontium-substituted bioactive glasses on osteoblasts and osteoclasts in vitro. Biomaterials, 31(14), 3949–3956.
Li, Y., Li, Q., Zhu, S., Luo, E., Li, J., Feng, G., Liao, Y., & Hu, J. (2010). The effect of strontium-substituted hydroxyapatite coating on implant fixation in ovariectomized rats. Biomaterials, 31(34), 9006–9014.
Bamzai, K. K., Suri, S., & Singh, V. (2012). Synthesis, characterization, thermal and dielectric properties of pure and cadmium doped calcium hydrogen phosphate. Materials Chemistry and Physics, 135(1), 158–167.
Tank, K. P., Jogiya, B. V., Kanchan, D. K., & Joshi, M. J. (2014). Dielectric properties of pure and strontium doped nano-hydroxyapatite. In Solid State Phenomena, 209, 151–155.
Bowen, C. R., Gittings, J., Turner, I. G., Baxter, F., & Chaudhuri, J. B. (2006). Dielectric and piezoelectric properties of hydroxyapatite-BaTiO3 composites. Applied Physics Letters, 89(13), 132906.
Mahabole, M. P., Aiyer, R. C., Ramakrishna, C. V., Sreedhar, B., & Khairnar, R. S. (2005). Synthesis, characterization and gas sensing property of hydroxyapatite ceramic. Bulletin of Materials Science, 28(6), 535–545.
Almond, D. P., & Bowen, C. R. (2004). Anomalous power law dispersions in ac conductivity and permittivity shown to be characteristics of microstructural electrical networks. Physical Review Letters, 92(15), 157601.
Dang, Z. M., Yao, S. H., & Xu, H. P. (2007). Effect of tensile strain on morphology and dielectric property in nanotube/polymer nanocomposites. Applied Physics Letters, 90(1), 012907.
Leyland-Jones, B. (2003). Treatment of cancer-related hypercalcemia: the role of gallium nitrate. In Seminars in Oncology, 30(2), 13–19.
Valappil, S. P., Ready, D., Neel, E. A. A., Pickup, D. M., Chrzanowski, W., O’Dell, L. A., Newport, R. J., Smith, M. E., Wilson, M., & Knowles, J. C. (2008). Antimicrobial gallium-doped phosphate-based glasses. Advanced Functional Materials, 18(5), 732–741.
Xie, W., Allioux, F. M., Ou, J. Z., Miyako, E., Tang, S. Y., & Kalantar-Zadeh, K. (2021). Gallium-based liquid metal particles for therapeutics. Trends in Biotechnology, 39(6), 624–640.
Kurtjak, M., Vukomanović, M., Krajnc, A., Kramer, L., Turk, B., & Suvorov, D. (2016). Designing Ga (iii)-containing hydroxyapatite with antibacterial activity. RSC Advances, 6(114), 112839–112852.
Panseri, S., Cunha, C., D’Alessandro, T., Sandri, M., Giavaresi, G., Marcacci, M., Hung, C. T., & Tampieri, A. (2012). Intrinsically superparamagnetic Fe-hydroxyapatite nanoparticles positively influence osteoblast-like cell behaviour. Journal of Nanobiotechnology, 10(1), 1–10.
Kaygili, O., Dorozhkin, S. V., Ates, T., Al-Ghamdi, A. A., & Yakuphanoglu, F. (2014). Dielectric properties of Fe doped hydroxyapatite prepared by sol-gel method. Ceramics International, 40(7), 9395–9402.
Mene, R. U., Mahabole, M. P., Mohite, K. C., & Khairnar, R. S. (2014). Improved gas sensing and dielectric properties of Fe doped hydroxyapatite thick films: Effect of molar concentrations. Materials Research Bulletin, 50, 227–234.
Kaygili, O., Tatar, C., & Yakuphanoglu, F. (2012). Structural and dielectrical properties of Mg3-Ca3 (PO4) 2 bioceramics obtained from hydroxyapatite by sol-gel method. Ceramics International, 38(7), 5713–5722.
Ibrahim, M., & Dawood, A. (2020). Influence of doping chromium ions on the electrical properties of hydroxyapatite. Egyptian Journal of Basic and Applied Sciences, 7(1), 35–46.
Hu, S., Li, Y. F., Yang, R., Yang, Z., & Wang, L. (2018). Structure and ionic conductivity of Li7La3Zr2- xGexO12 garnet-like solid electrolyte for all solid state lithium ion batteries. Ceramics International, 44(6), 6614–6618.
Zhao, H., Xia, Y. J., Dang, Z. M., Zha, J. W., & Hu, G. H. (2013). Composition dependence of dielectric properties, elastic modulus, and electroactivity in (carbon black-BaTiO3)/silicone rubber nanocomposites. Journal of Applied Polymer Science, 127(6), 4440–4445.
Katzir, S. (2006). The discovery of the piezoelectric effect. In The beginnings of piezoelectricity, 15-64.
Dineva, P., Gross, D., Müller, R., & Rangelov, T. (2014). Piezoelectric materials. In Dynamic fracture of piezoelectric materials, 7-32.
Xu, S., Hansen, B. J., & Wang, Z. L. (2010). Piezoelectric-nanowire-enabled power source for driving wireless microelectronics. Nature Communications, 1(1), 1–5.
Tandon, B., Blaker, J. J., & Cartmell, S. H. (2018). Piezoelectric materials as stimulatory biomedical materials and scaffolds for bone repair. Acta Biomaterialia, 73, 1–20.
Khare, D., Basu, B., & Dubey, A. K. (2020). Electrical stimulation and piezoelectric biomaterials for bone tissue engineering applications. Biomaterials, 258, 120280.
Kapat, K., Shubhra, Q. T., Zhou, M., & Leeuwenburgh, S. (2020). Piezoelectric nano-biomaterials for biomedicine and tissue regeneration. Advanced Functional Materials, 30(44), 1909045.
Halperin, C., Mutchnik, S., Agronin, A., Molotskii, M., Urenski, P., Salai, M., & Rosenman, G. (2004). Piezoelectric effect in human bones studied in nanometer scale. Nano Letters, 4(7), 1253–1256.
Sun, Q., Qian, B., Uto, K., Chen, J., Liu, X., & Minari, T. (2018). Functional biomaterials towards flexible electronics and sensors. Biosensors and Bioelectronics, 119, 237–251.
Dutta, P. K., Dutta, J., & Tripathi, V. S. (2004). Chitin and chitosan: chemistry, roperties and applications.
Aguilar, A., Zein, N., Harmouch, E., Hafdi, B., Bornert, F., Offner, D., Clauss, F., Fioretti, F., Huck, O., Benkirane-Jessel, N., & Hua, G. (2019). Application of chitosan in bone and dental engineering. Molecules, 24(16), 3009.
Petrov, I., Kalinkevich, O., Pogorielov, M., Kalinkevich, A., Stanislavov, A., Sklyar, A., Danilchenko, S., & Yovcheva, T. (2016). Dielectric and electric properties of new chitosan-hydroxyapatite materials for biomedical application: Dielectric spectroscopy and corona treatment. Carbohydrate Polymers, 151, 770–778.
Venkatesan, J., & Kim, S. K. (2010). Chitosan composites for bone tissue engineering-an overview. Marine Drugs, 8(8), 2252–2266.
Jiao, H., Song, S., Zhao, K., Zhang, X., & Tang, Y. (2020). Synthesis and properties of porous piezoelectric BT/PHBV composite scaffold. Journal of Biomaterials Science, Polymer Edition, 31(12), 1552–1565.
Nahanmoghadam, A., Asemani, M., Goodarzi, V., & Ebrahimi-Barough, S. (2021). In vivo investigation of PCL/PHBV/Hydroxyapatite Nanocomposite Scaffold in Regeneration of Critical-sized Bone Defects. Fibers and Polymers, 22(9), 2507–2516.
Wu, J., Xue, K., Li, H., Sun, J., & Liu, K. (2013). Improvement of PHBV scaffolds with bioglass for cartilage tissue engineering. PloS One, 8(8), 71563.
Numata, K., Abe, H., & Doi, Y. (2008). Enzymatic processes for biodegradation of poly (hydroxyalkanoate) s crystals. Canadian Journal of Chemistry, 86(6), 471–483.
Rajabi, A. H., Jaffe, M., & Arinzeh, T. L. (2015). Piezoelectric materials for tissue regeneration: A review. Acta Biomaterialia, 24, 12–23.
Fernandez-Yague, M. A., Vallejo-Giraldo, C., Aceret, G. O., Pandit, A., & Biggs, M. J. (2016). Biological activity on piezoelectric PVDF. In Electrically Active Materials for Medical Devices, 2, 167–176.
Pereira, J. D., Camargo, R. C., Jose Filho, C. S. C., Alves, N., Rodriguez-Perez, M. A., & Constantino, C. J. (2014). Biomaterials from blends of fluoropolymers and corn starch-implant and structural aspects. Materials Science and Engineering: C, 36, 226–236.
Gimenes, R., Zaghete, M. A., Bertolini, M., Varela, J. A., Coelho, L. O., & Silva Jr, N. F. (2004). Composites PVDF-TrFE/BT used as bioactive membranes for enhancing bone regeneration. In Smart Structures and Materials 2004: Electroactive Polymer Actuators and Devices (EAPAD), 5385, 539-547.
Ross, G. J., Watts, J. F., Hill, M. P., & Morrissey, P. (2000). Surface modification of poly (vinylidene fluoride) by alkaline treatment. The degradation mechanism. Polymer, 41(5), 1685–1696.
Neuss, S., Apel, C., Buttler, P., Denecke, B., Dhanasingh, A., Ding, X., Grafahrend, D., Groger, A., Hemmrich, K., Herr, A., & Jahnen-Dechent, W. (2008). Assessment of stem cell/biomaterial combinations for stem cell-based tissue engineering. Biomaterials, 29(3), 302–313.
Aoki, K., & Saito, N. (2020). Biodegradable polymers as drug delivery systems for bone regeneration. Pharmaceutics, 12(2), 95.
Chorsi, M. T., Curry, E. J., Chorsi, H. T., Das, R., Baroody, J., Purohit, P. K., Ilies, H., & Nguyen, T. D. (2019). Piezoelectric biomaterials for sensors and actuators. Advanced Materials, 31(1), 1802084.
Prabhakaran, M. P., Venugopal, J., & Ramakrishna, S. (2009). Electrospun nanostructured scaffolds for bone tissue engineering. Acta Biomaterialia, 5(8), 2884–2893.
Pawar, P. R., Tekale, U. S., Shisodia, U. S., Totre, T. J., & Domb, J. A. (2014). Biomedical applications of poly (lactic acid). Recent Patents on Regenerative Medicine, 4(1), 40–51.
Cheung, H. Y., Lau, K. T., Lu, T. P., & Hui, D. (2007). A critical review on polymer-based bio-engineered materials for scaffold development. Composites Part B: Engineering, 38(3), 291–300.
Sharma, G., Thakur, B., Naushad, M., Kumar, A., Stadler, F. J., Alfadul, S. M., & Mola, G. T. (2018). Applications of nanocomposite hydrogels for biomedical engineering and environmental protection. Environmental Chemistry Letters, 16(1), 113–146.
Bhatia, S. (2016). Natural polymers vs synthetic polymer. In Natural Polymer Drug Delivery Systems, 95–118.
Wang, X., Fang, J., Zhu, W., Zhong, C., Ye, D., Zhu, M., & Ren, F. (2021). Bioinspired highly anisotropic, ultrastrong and stiff, and osteoconductive mineralized wood hydrogel composites for bone repair. Advanced Functional Materials, 31(20), 2010068.
Li, Z., Lv, X., Chen, S., Wang, B., Feng, C., Xu, Y., & Wang, H. (2016). Improved cell infiltration and vascularization of three-dimensional bacterial cellulose nanofibrous scaffolds by template biosynthesis. RSC Advances, 6(48), 42229–42239.
Daugela, P., Pranskunas, M., Juodzbalys, G., Liesiene, J., Baniukaitiene, O., Afonso, A., & Sousa Gomes, P. (2018). Novel cellulose/hydroxyapatite scaffolds for bone tissue regeneration: In vitro and in vivo study. Journal of Tissue Engineering and Regenerative Medicine, 12(5), 1195–1208.
Eftekhari, S., El Sawi, I., Bagheri, Z. S., Turcotte, G., & Bougherara, H. (2014). Fabrication and characterization of novel biomimetic PLLA/cellulose/hydroxyapatite nanocomposite for bone repair applications. Materials Science and Engineering: C, 39, 120–125.
Liu, X., Zheng, C., Luo, X., Wang, X., & Jiang, H. (2019). Recent advances of collagen-based biomaterials: multi-hierarchical structure, modification and biomedical applications. Materials Science and Engineering: C, 99, 1509–1522.
Chen, L., Wu, Z., Zhou, Y., Li, L., Wang, Y., Wang, Z., Chen, Y., & Zhang, P. (2017). Biomimetic porous collagen/hydroxyapatite scaffold for bone tissue engineering. Journal of Applied Polymer Science, 134(37), 45271.
Yilmaz, E., Cakiroglu, B., Gokce, A., Findik, F., Gulsoy, H. O., Gulsoy, N., Mutlu, O., & Ozacar, M. (2019). Novel hydroxyapatite/graphene oxide/collagen bioactive composite coating on Ti16Nb alloys by electrodeposition. Materials Science and Engineering: C, 101, 292–305.
Chang, C., Peng, N., He, M., Teramoto, Y., Nishio, Y., & Zhang, L. (2013). Fabrication and properties of chitin/hydroxyapatite hybrid hydrogels as scaffold nano-materials. Carbohydrate Polymers, 91(1), 7–13.
Chakravarty, J., Rabbi, M. F., Chalivendra, V., Ferreira, T., & Brigham, C. J. (2020). Mechanical and biological properties of chitin/polylactide (PLA)/hydroxyapatite (HAP) composites cast using ionic liquid solutions. International Journal of Biological Macromolecules, 151, 1213–1223.
Bedian, L., Villalba-Rodríguez, A. M., Hernández-Vargas, G., Parra-Saldivar, R., & Iqbal, H. M. (2017). Bio-based materials with novel characteristics for tissue engineering applications-A review. International Journal of Biological Macromolecules, 98, 837–846.
Ciofani, G., Danti, S., D’Alessandro, D., Ricotti, L., Moscato, S., Bertoni, G., Falqui, A., Berrettini, S., Petrini, M., Mattoli, V., & Menciassi, A. (2010). Enhancement of neurite outgrowth in neuronal-like cells following boron nitride nanotube-mediated stimulation. ACS Nano, 4(10), 6267–6277.
Lahiri, D., Rouzaud, F., Richard, T., Keshri, A. K., Bakshi, S. R., Kos, L., & Agarwal, A. (2010). Boron nitride nanotube reinforced polylactide-polycaprolactone copolymer composite: Mechanical properties and cytocompatibility with osteoblasts and macrophages in vitro. Acta Biomaterialia, 6(9), 3524–3533.
Tayel, A. A., EL-TRAS, W. F., Moussa, S., EL-BAZ, A. F., Mahrous, H., Salem, M. F., & Brimer, L. (2011). Antibacterial action of zinc oxide nanoparticles against foodborne pathogens. Journal of Food Safety, 31(2), 211–218.
Ito, A., Kawamura, H., Otsuka, M., Ikeuchi, M., Ohgushi, H., Ishikawa, K., Onuma, K., Kanzaki, N., Sogo, Y., & Ichinose, N. (2002). Zinc-releasing calcium phosphate for stimulating bone formation. Materials Science and Engineering: C, 22(1), 21–25.
Moradpoor, H., Safaei, M., Mozaffari, H. R., Sharifi, R., Imani, M. M., Golshah, A., & Bashardoust, N. (2021). An overview of recent progress in dental applications of zinc oxide nanoparticles. RSC Advances, 11(34), 21189–21206.
Jarkov, V., Allan, S. J., Bowen, C., & Khanbareh, H. (2021). Piezoelectric materials and systems for tissue engineering and implantable energy harvesting devices for biomedical applications. International Materials Reviews, 2, 1–51.
Mantripragada, V. P., Lecka-Czernik, B., Ebraheim, N. A., & Jayasuriya, A. C. (2013). An overview of recent advances in designing orthopedic and craniofacial implants. Journal of Biomedical Materials Research Part A, 101(11), 3349–3364.
Ross, R. B. (2013). Metallic Materials Specification Handbook. Springer Science & Business Media.
Tishin, A. M., Nikitin, S. A., & Bodriakov, V. Y. (1995). Young’s modulus and internal friction of yttrium. Journal de Physique I, 5(4), 525–532.
Frerichs, A. E., & Russell, A. M. (2022). Tensile properties of strontium metal. Young, 10(3), 1.
Haynes, R. (1991). Effects of porosity on the tensile strengths of sintered irons. Metal Powder Report, 46(2), 49–51.
Jiansirisomboon, S., & Watcharapasorn, A. (2008). Effects of alumina nano-particulates addition on mechanical and electrical properties of barium titanate ceramics. Current Applied Physics, 8(1), 48–52.
Wang, S. F., Shen, L., Zhang, W. D., & Tong, Y. J. (2005). Preparation and mechanical properties of chitosan/carbon nanotubes composites. Biomacromolecules, 6(6), 3067–3072.
Lin, J., Shi, Y., Men, Y., Wang, X., Ye, J., & Zhang, C. (2020). Mechanical roles in formation of oriented collagen fibers. Tissue Engineering Part B: Reviews, 26(2), 116–128.
Ashoorirad, M., Saviz, M., & Fallah, A. (2020). On the electrical properties of collagen macromolecule solutions: Role of collagen-water interactions. Journal of Molecular Liquids, 300, 112344.
Prakash, P. S., Pawar, S. J., & Tewari, R. P. (2019). Synthesis, characterization, and coating of forsterite (Mg2SiO4) based material over medical implants: A review. Proceedings of the Institution of Mechanical Engineers, Part L: Journal of Materials: Design and Applications, 233(6), 1227–1240.
Cygan, R. T., & Lasaga, A. C. (1986). Dielectric and polarization behavior of forsterite at elevated temperatures. American Mineralogist, 71(5–6), 758–766.
Jin, W., & Chu, P. K. (2019). Orthopedic implants. Encyclopedia of. Biomedical Engineering, 1, 3.
Chen, L. Y. (2014). Dielectric performance of a high purity HTCC alumina at high temperatures-a comparison study with other polycrystalline alumina. Additional Papers and presentations, 271-277.
Yan, Y., & Han, Y. (2007). Structure and bioactivity of micro-arc oxidized zirconia films. Surface and Coatings Technology, 201(9–11), 5692–5695.
Kondo, R., Nomura, N., Tsutsumi, Y., Doi, H., & Hanawa, T. (2011). Microstructure and mechanical properties of as-cast Zr-Nb alloys. Acta Biomaterialia, 7(12), 4278–4284.
Babu, C. R., Reddy, N. R. M., & Reddy, K. (2015). Synthesis and characterization of high dielectric nano zirconium oxide. Ceramics International, 41(9), 10675–10679.
Dewidar, M. M., Yoon, H. C., & Lim, J. K. (2006). Mechanical properties of metals for biomedical applications using powder metallurgy process: a review. Metals and Materials International, 12(3), 193–206.
Capek, J., Machova, M., Fousova, M., Kubasek, J., Vojtech, D., Fojt, J., Jablonska, E., Lipov, J., & Ruml, T. (2016). Highly porous, low elastic modulus 316L stainless steel scaffold prepared by selective laser melting. Materials Science and Engineering: C, 69, 631–639.
Zaman, H. A., Sharif, S., Idris, M. H., & Kamarudin, A. (2015). Metallic biomaterials for medical implant applications: a review. Applied Mechanics and Materials, 735, 19–25.
Teo, A. J., Mishra, A., Park, I., Kim, Y. J., Park, W. T., & Yoon, Y. J. (2016). Polymeric biomaterials for medical implants and devices. ACS Biomaterials Science & Engineering, 2(4), 454–472.
Tamboli, M. S., Palei, P. K., Patil, S. S., Kulkarni, M. V., Maldar, N. N., & Kale, B. B. (2014). Polymethyl methacrylate (PMMA)-bismuth ferrite (BFO) nanocomposite: low loss and high dielectric constant materials with perceptible magnetic properties. Dalton Transactions, 43(35), 13232–13241.
Li, W., Song, Z., Zhong, J., Qian, J., Tan, Z., Wu, X., & Ran, X. (2019). Multilayer-structured transparent MXene/PVDF film with excellent dielectric and energy storage performance. Journal of Materials Chemistry C, 7(33), 10371–10378.
Li, S. T., Arenholz, E., Heitz, J., & Bäuerle, D. (1998). Pulsed-laser deposition of crystalline Teflon (PTFE) films. Applied Surface Science, 125(1), 17–22.
Nayak, S., & Khastgir, D. (2019). Polydimethylsiloxane-PbZr0. 52Ti0. 48O3 nanocomposites with high permittivity: Effect of poling and temperature on dielectric properties. Journal of Applied Polymer Science, 136(14), 47307.
Renouf-Glauser, A. C., Rose, J., Farrar, D. F., & Cameron, R. E. (2005). The effect of crystallinity on the deformation mechanism and bulk mechanical properties of PLLA. Biomaterials, 26(29), 5771–5782.
Rebelo, R., Fernandes, M., & Fangueiro, R. (2017). Biopolymers in medical implants: a brief review. Procedia Engineering, 200, 236–243.
Jayamani, E., Nair, G. A., & Soon, K. (2020). Investigation of the dielectric properties of natural fibre and conductive filler reinforced polymer composites. Materials Today: Proceedings, 22, 162–171.
Huang, Y., Zhang, X., Qiao, H., Hao, M., Zhang, H., Xu, Z., Zhang, X., Pang, X., & Lin, H. (2016). Corrosion resistance and cytocompatibility studies of zinc-doped fluorohydroxyapatite nanocomposite coatings on titanium implant. Ceramics International, 42(1), 1903–1915.
Zhang, S., Xianting, Z., Yongsheng, W., Kui, C., & Wenjian, W. (2006). Adhesion strength of sol-gel derived fluoridated hydroxyapatite coatings. Surface and Coatings Technology, 200(22–23), 6350–6354.
Xie, Y., Zhai, W., Chen, L., Chang, J., Zheng, X., & Ding, C. (2009). Preparation and in vitro evaluation of plasma-sprayed Mg2SiO4 coating on titanium alloy. Acta Biomaterialia, 5(6), 2331–2337.
Sebdani, M. M., & Fathi, M. H. (2011). Novel hydroxyapatite-forsterite-bioglass nanocomposite coatings with improved mechanical properties. Journal of Alloys and Compounds, 509(5), 2273–2276.
Kazakos, A., Komarneni, S., & Roy, R. (1990). Preparation and densification of forsterite (Mg2SiO4) by nanocomposite sol-gel processing. Materials Letters, 9(10), 405–409.
Seitz, J. M., Eifler, R., Bach, F. W., & Maier, H. J. (2014). Magnesium degradation products: effects on tissue and human metabolism. Journal of Biomedical Materials Research Part A, 102(10), 3744–3753.
Henstock, J. R., Canham, L. T., & Anderson, S. I. (2015). Silicon: the evolution of its use in biomaterials. Acta Biomaterialia, 11, 17–26.
Ni, S., Chou, L., & Chang, J. (2007). Preparation and characterization of forsterite (Mg2SiO4) bioceramics. Ceramics International, 33(1), 83–88.
Kichi, M. K., Torkaman, R., Mohammadi, H., Toutounchi, A., Kharaziha, M., & Alihosseini, F. (2020). Electrochemical and in vitro bioactivity behavior of poly (\(\varepsilon\)-caprolactone)(PCL)-gelatin-forsterite nano coating on titanium for biomedical application. Materials Today Communications, 24, 101326.
Bakhsheshi-Rad, H. R., Hamzah, E., Kasiri-Asgarani, M., Jabbarzare, S., Iqbal, N., & Kadir, M. A. (2016). Deposition of nanostructured fluorine-doped hydroxyapatite-polycaprolactone duplex coating to enhance the mechanical properties and corrosion resistance of Mg alloy for biomedical applications. Materials Science and Engineering: C, 60, 526–537.
Zomorodian, A., Santos, C., Carmezim, M. J., e Silva, T. M., Fernandes, J. C. S., & Montemor, M. D. F. (2015). “In-vitro’’ corrosion behaviour of the magnesium alloy with Al and Zn (AZ31) protected with a biodegradable polycaprolactone coating loaded with hydroxyapatite and cephalexin. Electrochimica Acta, 179, 431–440.
Suarasan, S., Focsan, M., Maniu, D., & Astilean, S. (2013). Gelatin-nanogold bioconjugates as effective plasmonic platforms for SERS detection and tagging. Colloids and Surfaces B: Biointerfaces, 103, 475–481.
Nieto-Suarez, M., Lopez-Quintela, M. A., & Lazzari, M. (2016). Preparation and characterization of crosslinked chitosan/gelatin scaffolds by ice segregation induced self-assembly. Carbohydrate Polymers, 141, 175–183.
Jeffrey, C. K. L., Kumanan, A., Pang, M. M., Yong, L. C., & Sivakumar, S. (2015). Sintering behavior of forsterite with manganese oxide as doping agent. Journal of Engineering Science and Technology, 1, 1–7.
Naga, S. M., Hassan, A. M., Awaad, M., Killinger, A., Gadow, R., Bernstein, A., & Sayed, M. (2020). Forsterite/nano-biogenic hydroxyapatite composites for biomedical applications. Journal of Asian Ceramic Societies, 8(2), 373–386.
Valaskova, M., Zdralkova, J., Tokarsky, J., Martynkova, G. S., Ritz, M., & Studentova, S. (2014). Structural characteristics of cordierite/steatite ceramics sintered from mixtures containing pore-forming organovermiculite. Ceramics International, 40(10), 15717–15725.
Terzic, A., Obradovic, N., Stojanovic, J., Pavlovic, V., Andric, L., Olcan, D., & Dorđevic, A. (2017). Influence of different bonding and fluxing agents on the sintering behavior and dielectric properties of steatite ceramic materials. Ceramics International, 43(16), 13264–13275.
Funding
The authors did not receive support from any organization for the submitted work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
On behalf of all the authors, the corresponding author states that there is no conflict of interest.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Pandey, A., Sahoo, S. Progress on Medical Implant: A Review and Prospects. J Bionic Eng 20, 470–494 (2023). https://doi.org/10.1007/s42235-022-00284-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s42235-022-00284-z