Abstract
Tendons and ligaments are collagenous connective tissues involved in locomotion and stabilization of joints. These tissues possess relatively low cellularity and vascularity, resulting in long and potentially incomplete healing responses following injury. For sub-failure injuries such as strains and sprains, the common treatment is an implementation of rest, ice, compression, and elevation. This procedure relies on the tissue’s natural healing ability, leaving the tissue prone to possible re-injury and failure. As a potential aid in the healing process, we investigated the effects of thermal stress on human tenocytes in vitro. This method exploits the activity of heat shock proteins, which assist in cellular proliferation and protein assembly. Heat shock at 40, 44, and 48 °C was applied to human hamstring tenocytes for 5–20 min. Studies were performed to determine metabolic activity, proliferation, protein secretion, and gene expression of the cells shortly after heating. A scratch wound healing assay was performed to monitor migration of cells as they recovered from heat shock. The data showed increased cellular activity following 15 and 20 min of thermal conditioning at 44 and 48 °C. Protein secretion and expression of collagens types I and III and TGF-β1 suggest that the heat shock response of tenocytes is similar to that of natural wound healing. The results revealed different responses for different temperatures and different durations of heat shock. The scratch assay revealed that heat might hasten recovery times following injury. Although additional studies that investigate additional heat shock proteins with different cell lines must be performed, these initial results suggest that heat shock may be a potential therapeutic tool that should be further investigated for the treatment of sub-failure tendon and ligament injuries. Heat shock presents a potential aid for the regeneration of damaged musculoskeletal tissues. In this preliminary study of human hamstring tenocytes in vitro, the application of thermal stress for a short duration caused rapid proliferation of cells after they were allowed to recover. Furthermore, parallels were observed between the in vitro heat shock response and the natural wound healing process of tendons and ligaments. This information provides potential for heat shock to assist in healing damage tendon and ligament tissue. Future works will need to explore the effects of heat shock on a wider range of tendon and ligament cells, as well as develop methods of applying thermal stress to tissue in vivo.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
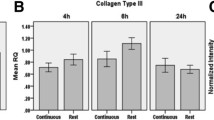
Tendons and ligaments (T/Ls) are collagenous tissues that share a similar structure composed of fibroblast cells and an extracellular matrix (ECM) made of collagen (approximately 88% type I and 12% type III), elastin, and proteoglycans [1,2,3]. Tendons function to transfer the forces generated from muscles to move bones [4]. Ligaments provide a connection between bones and play a role in joint stability [5]. T/L function is attributed to a hierarchical arrangement of collagen ranging from the molecular level to bundles of fascicles [6, 7]. Injury occurs when the biological or mechanical functionality of the T/L structure becomes impaired. T/L injuries account for approximately 45% of the 32 million annual musculoskeletal injuries that occur in the USA [8]. The natural healing response of T/Ls occurs in three phases: inflammation, proliferation, and remodeling and maturation [9]. During the proliferation phase, there is an increase in cell number and type III collagen production [10]. Collagen type I expression begins to increase during the final phase of T/L healing, while collagen type III expression and cell number decrease [11]. For mild injuries, implementation of rest, ice, compression, and elevation of the wound site, known as the RICE method, works well with the natural healing response for treatment [12]. A potential limitation to the RICE method is that the cooling effect of ice can hinder hemostasis and coagulation of blood, resulting in a prolonged recovery time for the injured tissue [13]. For severe injuries with complete tears through the tissue, surgical intervention becomes necessary.
As an alternative to the traditional methods of repair, tissue engineering offers promising methods for T/L healing. Tissue engineering combines the use of scaffolds, cells, growth factors, and small molecules to help develop functional tissue replacements. A variety of natural and synthetic polymers have been utilized to develop tissue-engineered scaffolds that attempt to mimic the mechanical and biological properties of native T/L tissue [14,15,16,17,18]. Scaffolds can be augmented with growth factors that would improve tissue regeneration and healing following implantation. Transforming growth factor-β (TGF-β) [11, 19], insulin-like growth factor-I (IGF-I) [20], vascular endothelial growth factor (VEGF) [21, 22], platelet-derived growth factor (PDGF) [21, 23], and basic fibroblast growth factor (bFGF) [24] have been demonstrated to have a role in T/L wound healing by either promoting cellular proliferation, differentiation, angiogenesis, and/or matrix protein production. Similarly, heat could be used to improve cellular proliferation and ECM deposition to aid in T/L regeneration. Thermal conditioning has been demonstrated as a potential therapeutic tool in the regeneration of muscle [25,26,27], skin [28], aortic endothelial tissue [29], teeth [30], and bone [31,32,33].
The beneficial effects of heat on tissue regeneration can be attributed to an increase in cellular heat shock protein (HSP) expression. HSPs are a family of molecular chaperones that assist in the folding of proteins, repair of denatured proteins, prevention of protein aggregation, and protein transport [34,35,36]. Basal levels of HSPs are constitutively expressed, but in response to stress from heat, ischemia, hypoxia, or oxidation, inducible HSP expression increases and makes the cell more tolerant to subsequent stress [29, 37]. The 70-kDa class of HSPs (HSP70) has been suggested to play a role in the cell cycle [38, 39] and in the rapid growth, proliferation, and inhibition of apoptosis in cancer cells [40,41,42]. The 47-kDa HSP (HSP47) binds specifically to collagen molecules, and it assists in the quality control of collagen production [43, 44]. HSP47 has been reported as a necessary molecule in the development of healthy collagen fibers and ECM formation [45]. Furthermore, there is a strong correlation between HSP47 and type I collagen expression [46].
The objective of this study was to investigate the short-term effects of heat shock on T/L cells in vitro. We hypothesized that thermal conditioning would improve cellular proliferation and ECM production compared to a non-heated control. To test this hypothesis, we investigated the effects of heat shock on cellular metabolic activity, tenocyte morphology, total protein secretion, and gene expression of matrix proteins. We also employed an in vitro scratch wound healing assay to examine cellular migration and wound healing following heat shock. We observed that heat shock at 44 and 48 °C induces rapid and immediate proliferation of tenocytes. The heat shock response also displayed similarities to natural wound healing that occurs in T/Ls. These initial findings can potentially be applied to improve T/L healing and reduce recovery times in healing tissue.
Materials and Methods
Cell Culture
Human hamstring tenocytes (hHT) were cultured as a monolayer in tissue culture flasks with growth media consisting of alpha Minimum Essential Medium (αMEM) (Life Technologies, Carlsbad, CA) supplemented with 10% fetal bovine serum (FBS) and 1% penicillin-streptomycin (P/S) in an incubator at 5% CO2 and 37 °C. Cells were obtained from a healthy 25-year-old male donor and cultured as outlined in a previous study by Ekwueme et al. [4]. The cells were isolated with approval from the Medical Ethical Research Committee at the Utrecht Medical Center and MST Twente. Permission was granted to use the cells for heat shock experiments by Rutgers Environmental Health and Safety Office. Upon reaching confluency, the cells were trypsinized, counted, and seeded at a density of 2.5 × 104 cells/cm2 into tissue culture 48-well plates with the same media conditions used for growth. Cells between passages 3 and 8 were used for the following studies.
Heat Shock
An incubator set at a constant temperature (T = 40, 44, 48 °C) and 5% CO2 was employed to provide heat shock to the experimental groups. Prior to the application of heat shock, αMEM media supplemented with 10% FBS and 1% P/S was preheated to the desired heat shock temperature. To apply heat shock, media was aspirated, wells were washed with phosphate-buffered saline (PBS), and warm media was added to the monolayer of cells. A non-heated group with cells kept at 37 °C served as a control. The cells were then incubated at the desired temperature for heating durations of 5, 10, 15, or 20 min. Subsequently, the warm media was removed, wells were washed with PBS, and fresh media at 37 °C was added to the cells. Following the heat shock protocol, the cells were incubated at 37 °C to allow for recovery from the thermal stress and examined at time points of 4 and 8 h post-heating.
Cellular Metabolic Activity
The metabolic activity of the cells (n = 4) was evaluated using a Presto Blue Mitochondrial Activity/Cell Viability assay according to the manufacturer’s instructions. Briefly, at each time point following heat shock, media was aspirated from the wells and 10% (v/v) Presto Blue (Life Technologies) solution in αMEM media supplemented with 10% FBS and 1% P/S was added. The cells were incubated with the Presto Blue solution for 1 h. The Presto Blue solution was transferred to a 96-well plate, and fluorescent values were measured from the bottom of the well at 560-nm excitation and 590-nm emission wavelengths in technical duplicate using a microplate reader (Tecan, Medford, MA). Fluorescent values from heat shock groups were normalized to a non-heated control.
Secreted Protein Quantification
Conditioned medium (n = 4) was collected from hHT at each time point following heat shock. The total protein concentration in the media was quantified using a Pierce BCA Protein Assay Kit (Thermo Scientific, Waltham, MA) according to the manufacturer’s instructions. The colorimetric assay was run in technical duplicate and the absorbance values were read at 562 nm using a microplate reader.
Immunostaining
To obtain images of cell morphology, cells were washed with PBS and fixed with 4% paraformaldehyde solution at various time points after heat shock. The fixed cells were permeabilized with 0.1% Triton X-100/PBS and blocked with 2% BSA/PBS-Tween (0.1%). Afterwards, the cells were stained with phalloidin fluorophore (1:200) to image the cytoskeleton. The cells were then washed with PBS and counterstained for DAPI to image nuclei. Images were taken using an EVOS FL Microscope (Life Technologies). The images were analyzed using ImageJ software (NIH).
Real-time Quantitative Polymerase Chain Reaction
Gene expression of collagen (types I and III), TGF-β1, HSP47, and elastin 4 h post-heating was assessed using real-time quantitative polymerase chain reaction (qPCR). Briefly, total RNA (n = 3) was extracted from each group and purified using the RNeasy Mini Kit (Qiagen, Valencia, CA). The concentration of isolated RNA in each sample was measured using a NanoDrop 2000c Spectrophotometer (Life Technologies). After the samples were normalized to the same RNA concentration, RNA was converted to cDNA using the Reverse Transcription System (Promega Corporation, Madison, WI). Following reverse transcription, the cDNA was mixed with SYBR Green PCR Master Mix (Life Technologies) and the primers for markers of interest. The forward and reverse primer sequences are presented in Table 1. The samples and reagents were subjected to qPCR using a PikoReal Real-Time PCR System (Thermo Scientific). Relative fold induction of genes was calculated using the ΔΔCT method and normalized with GAPDH, which served as an endogenous control.
Scratch Wound Healing Assay
Cellular migration of hHT was assessed using a scratch wound healing assay as previously described by Liang et al. [47]. Briefly, 5 × 104 cells/cm2 were seeded into 24-well plates and allowed to reach confluence (n = 3). A scratch to simulate a wound was applied across the cell monolayer with the use of either a 1-mL or a 200-μL pipette tip. After the scratch was induced, the culture medium was replaced with fresh medium and heat shock was applied as described above. Cells in the heat shock group were treated with 15 min of heat at 48 °C. The migration of cells as the wound closed was monitored using light microscopy after various time points. The images were analyzed using ImageJ.
Statistical Analysis
All of the quantitative data is presented as mean ± standard deviation. A two-way ANOVA with a Bonferroni’s multiple comparison post hoc analysis was utilized for comparing groups in the metabolic activity and protein secretion studies. A two-tailed Student’s t test was employed for comparing groups in the qPCR and scratch assay experiments (OriginPro Software 2016, Northampton, MA). Unless stated otherwise, differences are reported as statistically significant for p values less than 0.05.
Results
The Effect of Heat Shock on Cellular Metabolic Activity
Using the Presto Blue fluorometric assay, the metabolic activity of cells that underwent heat shock was measured 4 and 8 h post-heating (Fig. 1a, b, respectively). Following 4 h of recovery from heat shock, there were significant increases in cellular activity when cells were conditioned at 40 °C for 15 min (p < 0.5), 44 °C for 15 and 20 min (p < 0.001), and 48 °C for 15 and 20 min (p < 0.001) when compared to a non-heated control. Furthermore, metabolic activity was significantly higher for cells heated at 48 °C for 20 min (p < 0.01) than all other groups except for the cells heated for 15 min at the same temperature. Heating at 48 °C for 15 min increased metabolic activity compared to all 40 °C groups, 44 °C groups heated for durations of 10 min or less (p < 0.001), and 48 °C groups heated for durations of 10 min or less (p < 0.01). Metabolic activity was significantly lower for cells heated at 44 °C for 5 min when compared to groups heated for 10 min or more at 40 or 48 °C, as well as 15 or 20 min of heating at 44 °C (p < 0.001). Thermal conditioning of cells at 48 °C for 5 min resulted in significantly lower metabolic activity than cells heated at 44 °C for 15 min (p < 0.01) and 20 min.
At 8 h post-heating, there were significant decreases in metabolic activity for cells that were heated at 40 °C for 10 min and significant increases in activity among cells that were heated at 48 °C for 15 and 20 min compared to the non-heated control. Although insignificant, a trend showed that heating at 44 °C for less than 20 min decreased metabolic activity 8 h after heat shock (p = 0.12, 0.11, and 0.03 for 5, 10, and 15 min, respectively). A 20-min heat shock at 48 °C resulted in significantly higher metabolic activity among cells compared to all 40 and 44 °C groups (p < 0.001) and cells heated at 48 °C for durations of 10 min or less. Cellular activity was also significantly higher for cells heated at 48 °C for 15 min compared to all 40 and 44 °C groups. Heating at 48 °C for 10 min caused significantly higher metabolic activity compared to heating at 40 °C for 10 min or less and heating at 44 °C for 15 min or less. Significantly higher metabolic activity was seen among cells heated at 48 °C for 5 min compared to those heated at 44 °C for 15 min or less (p < 0.01) and 40 °C for 10 min or less (p < 0.01).
Cell-Conditioned Medium Protein Concentration Following Heat Shock
Conditioned medium was collected at 0 h (immediately after heat shock), 4 h, and 8 h post-heating and analyzed for the total protein concentration (Fig. 2(a, b, c), respectively). Immediately after heat shock, there was significantly more total protein in the groups heated at 40 °C for 5 min compared to those heated for 10 and 15 min at 40 °C (p < 0.01). There was significantly more protein in the groups heated at 40 °C for 20 min compared to those heated for 10 and 15 min at 40 °C (p < 0.05). At 4 h after heat shock, conditioned medium protein concentration was significantly higher among cells heated at 44 °C for 5 min compared to those heated at the same temperature for 10, 15, and 20 min (p < 0.05). Protein levels were significantly higher immediately after heat shock for cells heated at 48 °C for 5 min compared to the non-heated control, groups heated at 40 °C for 10 and 15 min, all groups heated at 44 °C, and the medium from cells heated at 48 °C for 10 min (p < 0.001). Furthermore, 0 h after heat shock, groups heated at 48 °C for 15 min had significantly more protein than groups heated at 40 °C for 10 and 15 min (p < 0.01), while conditioned media heated at 48 °C for 20 min possessed more protein than groups heated at 40 °C for 10 and 15 min (p < 0.01). At 8 h of recovery post-heating, the groups heated at 48 °C had significantly lower protein content in medium than the non-heated control (p < 0.05); groups heated at 40 °C for 5, 10, and 15 min (p < 0.05); and cells heated at 44 °C for 10 min (p < 0.05).
Morphological Changes Following Heat Shock
Fluorescent images were taken of the cytoskeleton (green) and nuclei (blue) of cells 4 (Fig. 3) and 8 h (Fig. 4) after heat shock. Nuclei from fluorescent images were counted from three unique fields of view (1060 × 800 μm) from four different wells (n = 4) (Fig. 5). At 4 h post-heating, the images reveal a significant increase in the number of cells based on a count of nuclei relative to the control in the groups heated at 40 °C (p < 0.05) and 48 °C (p < 0.001). In the 40 °C groups, cell count was highest when heat shock was applied for 5 and 10 min. Proliferation appeared to decrease as the heating duration increased from this point. Cells that were subject to heat shock at 44 °C did not display morphological or proliferative differences compared to the control. However, cells heated for a longer duration at this temperature were qualitatively observed to increase in size, although no size analysis was performed. In the 48 °C groups heated for 15 and 20 min, there was rapid proliferation, as seen by the abundance of nuclei in the images.
Following 8 h of recovery from heat shock, cells subjected to 44 °C did not display many differences from the control group. In the 40 °C group, wells heated for 5, 15, and 20 min contained significantly more cells than the control (p < 0.05), with the greatest number of nuclei present in the 15-min heat shock group. Although the cell count did not vary much from the control in the 44 °C group, qualitatively, the cells heated at this temperature appeared to be larger than the cells in any other group. Significantly rapid proliferation of cells occurred following recovery from a 48 °C heat shock for all durations, as seen from the large number of nuclei in the images (p < 0.01). The greatest proliferation is seen in the cells heated at 48 °C for 20 min. However, the abundance of nuclei makes it difficult to see the morphological features of tightly packed cells.
Gene Expression Following Heat Shock
The relative expression of collagen types I and III, HSP47, TGF-β1, and elastin was determined by running qPCR 4 h post-heating at 44 °C (Fig. 6a) and 48 °C (Fig. 6b). Analysis of type I collagen and elastin showed a significant decrease in expression among all groups heated at 44 °C (p < 0.05). There was a significant decrease in collagen expression in the cells heated at 48 °C for 20 min (p < 0.05). Type III collagen expression was significantly higher than the non-heated control following 5 min of heat shock at 44 °C (p < 0.01). Type III collagen and TGF-β1 expression trended to increase following 44 °C heat shock compared to the control (collagen III: p = 0.008, 0.37, 0.05, and 0.25 for 5, 10, 15, and 20 min, respectively; TGF-β1: p = 0.01, 0.16, 0.04, and 0.08 for 5, 10, 15, and 20 min, respectively). HSP47 expression was significantly overexpressed following 15 min of thermal conditioning at 48 °C (p < 0.01). No data was obtained for the expression of HSP47 in cells heated at 48 °C for 20 min.
Scratch Wound Healing Assay
A scratch was applied across a monolayer of cells to simulate a wound in vitro. The cells were then subjected to heat shock at 48 °C for 15 min. These parameters were chosen based on the increase in proliferation seen 4 and 8 h after heat shock and the gene expression of collagen and TGF-β1 4 h post-heating. Cells that were not treated with heat after the creation of the scratch served as the control. The closure of the induced wound was monitored 4, 8, 12, 16, 24, 48, and 72 h following heat shock. The wound had closed fully by the 48-h time point for all groups. The initial wound widths are provided in Table 2. The closure of the scratch is shown in Fig. 7a, and the average rate of cellular migration is displayed in Fig. 7b. Among the scratches created using a 1-mL pipette tip, heat shock produced a significant relative closure of the wound after 8 h (p < 0.05). Although insignificant, among the groups where a 200-μL pipette tip was employed to create the scratch, there was a trend which showed that heat shock caused the wound to close relatively quicker than the control between 4 and 12 h (p = 0.07 at 8 h). Heat also produced a significantly larger cell migration rate between the 0- and 4-h time points (p < 0.05).
Discussion
This preliminary study investigated the effects of thermal conditioning on the proliferation and wound healing potential of T/L cells in vitro. Although thermal conditioning and HSPs have been determined to produce beneficial effects on other cells of the musculoskeletal system, to the best of our knowledge, this is the first study to assess the effects of heat shock on human tenocytes in vitro. Mild heat shock of 42 °C has been shown to improve myogenesis and muscle development [25,26,27]. Osteoblasts and bone formation have also been seen to benefit from the application of thermal stress [31,32,33, 48]. Basic locomotion and exercise increases the temperature within core tendons and ligaments. Studies performed in horses have shown that the digital flexor tendons can reach temperatures as high as 45 °C during gallop [49]. However, the rise in temperature does not appear to last long enough to induce cell death within the tendons. In vitro studies on equine tenocytes found that exposure to heat decreases cell viability while matrix metalloproteinase (MMP) activity increases [50]. However, subsequent cooling of treated cells was able to decrease MMP activity. Based on the literature listed above, we hypothesized that heat shock could be used to improve the cellular proliferation and matrix remodeling and production of T/L fibroblasts.
T/Ls contain relatively low cellularity compared to other tissues within the body, resulting in a slow healing process following injury [51]. Improving cellular growth and proliferation is a field of interest in order to improve T/L healing from sub-failure injuries. Cellular metabolic activity and nuclei counts from fluorescent images were co-examined to determine cellular proliferation following heat shock. Metabolic activity and the number of nuclei followed similar trends in the data, although the differences among heating durations were more apparent when examining metabolic activity. Based on these two measurements, the data presented in this study shows that heat shock was able to significantly improve cellular proliferation at 4 h, particularly following the application of thermal stress at 48 °C for 15 or 20 min. There is evidence from past studies to suggest a role of HSPs in tendinopathy as proteins that inhibit apoptosis of tenocytes and assist in tissue repair following the application of stress [52]. Previous studies have shown that following heat shock, there is an accumulation of HSP70 within the nucleus [53]. Localization of HSP70 in the nucleus has also been observed during the S phase of the cell cycle [38, 39]. Thus, it can be inferred that heat shock stimulates an increase in cellular proliferation, which is consistent with the data obtained from the treated hamstring tenocytes. It is also interesting to see that there is a decrease in metabolic activity and cellular proliferation relative to the control when cells are heated at 44 °C for 5 min, but increases in metabolic activity and cell number are observed if the cells are allowed to be heated for an additional 10 or 15 min. This suggests that there may be a brief period of adaptation required in order for the cells to respond to heat shock which could be temperature and time dependent. Following 8 h after heat shock, only the cells heated at 48 °C displayed an increase in both metabolic activity and cellular proliferation compared to the control. Twenty minutes of heat shock at 48 °C significantly increased metabolic activity of cells compared to all other groups, as well as inducing a significant increase in total nuclei compared to the control. Longer durations of applied stress at 40 and 44 °C resulted in metabolic activity similar to the control, while shorter times decreased relative activity.
The effects of heat shock on protein secretion were determined by measuring the total protein concentration in conditioned medium. Immediately after heat shock, among the 40 and 48 °C heat shock groups, the media contained more protein 5 min after heat shock, followed by a dip in protein levels at 10 min. Total protein content in the conditioned media started to increase again following longer durations of heat shock. One possible reason for this observation could be that the initial application of heat could trigger the release of soluble factors that serve as stress signals and interact with nearby cells. The initial insult can also cause the death of several cells within the culture, releasing HSP70 into the extracellular milieu that would otherwise be localized within the cells [54]. Extracellular HSP70 can then interact with surviving cells, and the internalization of the protein can improve the new host’s thermotolerance [55]. The uptake of protein after the initial heat shock may occur rapidly, as seen by the drop in protein content after 10 min of thermal conditioning. Furthermore, protein levels in the 48 °C group after 8 h are lower than those in the control and other two heated groups, an inverse relationship of the cell proliferation data. As the 48 °C groups appear to have adjusted well to thermal stress, the cells may no longer require protein secretion for survival and can allocate energy to start producing and secreting matrix proteins important for the wound healing process. However, this potential explanation of the cellular response to heat shock is challenged by the data seen in the 44 °C group. The same behavior seen among the 40 and 48 °C protein data is not seen at 44 °C, but a decrease in cellularity after 5 min of heat shock at 44 °C followed by an increase after longer durations of stress is noted at 4 h.
Overall, heat shock at 40 °C did not appear to produce a beneficial cellular response compared to the non-heated control. Therefore, this group was omitted from mRNA analysis. PCR was performed on mRNA collected 4 h post-heating to determine the effect of heat shock on gene expression as the cells were recovering from the initial stress. Since the nuclei count did not display a significant difference between 4 and 8 h in the 44 and 48 °C groups, we did not perform mRNA analysis at 8 h in the present study. Heat shock at 44 °C caused a significant downregulation of type I collagen among all heating durations, but a trend in type III collagen upregulation was observed (p = 0.008, 0.370, 0.052, and 0.248 for 5, 10, 15, and 20 min, respectively). A trend showed a decrease in type I collagen expression following 48 °C heat shock as well (p = 0.216, 0.114, 0.118, and 0.033 for 5, 10, 15, and 20 min, respectively). Type III collagen appeared to be expressed more than type I collagen when cells were heated at 48 °C for 15 and 20 min. HSP47 plays a major role in the production and secretion of collagen molecules [45, 56]. Furthermore, a decrease in type I collagen production can be attributed to a downregulation of collagen-modulating genes such as HSP47 and TGF-β1 [57]. Although differences in HSP47 expression were not seen at 44 °C, a significant upregulation of the collagen-specific chaperone was seen in cells heated at 48 °C for 15 min, contrary to what literature would suggest. As mRNA upregulation occurs more rapidly than protein production, the lack of type I collagen expression suggests that HSP47 levels within the cells did not reach a threshold to induce type I collagen production. The upregulation of HSP47 can lead to an increase in collagen production and matrix deposition at later time points, and it would be worthwhile to observe how long it takes following heat shock for this phenomenon to occur in future studies. TGF-β1 expression has also been linked with collagen and ECM production in fibroblasts [58,59,60]. TGF-β1 expression was seen to increase following heat shock at 44 °C, with significant upregulation of the gene occurring after 5 and 15 min. Type III collagen appeared to be coregulated with TGF-β1 following these two heating durations. Additionally, although insignificant, a trend showed a slight increase in TGF-β1 expression 4 h after a 48 °C heat shock. These findings suggest that heat shock induces a response in tenocytes similar to that of wound healing.
Heat shock at 44 °C caused a significant decline in elastin expression after 4 h for all heating conditions. Recent studies have shown that elastin is the most prominent non-collagenous structural protein in T/L ECM, supporting up to 70% of the load when porcine medial collateral ligaments were under transverse tensile and shear deformation [61]. Furthermore, at low strains, elastin contributes to the mechanical behavior of supraspinatus tendons subjected to shear stress [62]. It has also been suggested that elastin may play a role in the T/L stress response to normal or increased loads, as seen by an increase of elastin fibers in damaged canine cruciate ligaments [63]. Although the tenocytes in the present study do not work to produce an increased number of elastin fibers, the increase in tenocyte metabolic activity, proliferation, and TGF-β1 expression may contribute to the repair and regeneration of T/L tissue without elastin production.
An increased presence of collagen III can be a sign of scar tissue development if remodeling does not take place. In natural wound healing responses, a large amount of collagen III is produced, then it is resorbed as cells lay down a more permanent matrix composed of collagen I. Wound healing in T/Ls occurs in three phases: inflammation, proliferation, and remodeling and maturation. During the proliferative phase, fibroblasts rapidly increase in number, working to produce a large concentration of matrix proteins [10, 11]. This phase is also characterized by an increase in type III collagen production and a decrease in type I collagen expression [9]. The characteristics of the proliferative phase are seen in the cellular proliferation and mRNA expression data obtained 4 h post-heating. A decrease in cell number is observed during the remodeling and maturation phase of wound healing [10, 11]. A decline in metabolic activity is seen 8 h after the 44 and 48 °C heat shock, compared to the normalized values of metabolic activity seen at 4 h. Therefore, it was hypothesized that in addition to causing a wound healing response in vitro, heat shock may also accelerate the process. To test this hypothesis, a scratch wound healing assay was performed to compare the closure of an in vitro “wound” and cellular migration after 15 min of thermal conditioning at 48 °C and a non-heated control. When comparing wound closure of scratches of similar initial width, a trend showed that heat shock induced a better healing response than the control between 4 and 12 h after thermal treatment. During later time points, the control and heated groups displayed a similar healing response. Further in vivo studies are needed to determine whether heat shock does accelerate natural T/L wound healing. If this is the case, then thermal stress could be used as a therapeutic tool for sub-failure T/L injuries. A shorter healing period can also help minimize further or repeated injury that may occur before the tissue is fully healed.
Although the results of this study do show trends between heat shock and cellular behavior, this study has several limitations. First, the experiments were performed on cells in a two-dimensional in vitro system, whereas T/L cells exist in a stressed three-dimensional matrix. However, correlations can be drawn between in vitro studies and phenomena that occur in vivo. In a recent study that examined the effects of mechanical loading on tendons, the investigators were able to see similar results in vitro and in vivo, namely in cell proliferation and gene expression [64]. The investigators had the advantage of using a previously well-established in vitro model to use for comparison with their in vivo data. With the in vitro heat shock data presented in the current study, there is not a clear indication whether the same results would occur in vivo. The scratch wound healing assay does not correlate directly to the natural wound healing response that occurs in T/L, during which several other cell types and vasculature play a role in the regeneration of the damaged tissue. Furthermore, the rapid proliferation of tenocytes following heat shock, while a potentially beneficial feature in tissue with relatively low cellularity, made it difficult to examine the morphological features of the cells. This preliminary study was also only able to look at the effects of heat shock on a single donor set. Results may vary depending on the history and health of the donor. More tests will have to be performed with additional donors before any absolute statements about cellular behavior in response to heat can be made.
Another limitation with this study is the consideration of its application in a clinical setting to heal injured T/Ls. Heat could be applied directly to the skin, but the underlying tendon or ligament may not reach the same temperature as the applicator on the skin. This could also cause unwanted irritation to the skin and other tissue types that are exposed to high levels of heat. One possible solution to apply heat would be to use ultrasounds to target T/Ls without heating other parts of the body. Low-intensity pulsed ultrasounds (LIPUS) are currently used in clinics as a safe therapeutic method for treating injuries in bone [65, 66]. By administering targeted mechanical stress, LIPUS has been demonstrated to accelerate the formation and remodeling of bone in the healing bone-tendon junction of a rabbit [65]. LIPUS have also been shown to induce human periodontal ligament cells to proliferate and undergo osteogenic differentiation for periodontal regeneration [66, 67]. At a low intensity, ultrasound waves generate a small amount of heat that is often considered negligible by investigators studying their effects in vivo. However, it may be possible to increase the intensity of the ultrasound waves to generate temperatures capable of causing heat shock.
The use of cells from one source is another limitation. In order to state that the data in this study represents the behavior of human tenocytes, the study must be repeated with cells from numerous donors. Future work will focus on repeating these studies on cells from additional donors.
Conclusions
In conclusion, we investigated the effects of thermal conditioning on human tenocytes in vitro. Heat shock proteins are known to play a role in cellular proliferation and protein production. Heat shock appeared to improve cellular proliferation after the cells were stressed at a temperature of 48 °C in this preliminary study. Cell culture medium protein concentrations and gene expression suggest that the heat shock response of tenocytes is similar to the natural healing response of T/L tissue. If thermal stress accelerates the healing response and results in the generation of healthy extracellular matrix, heat shock could be a potential tool in treating T/L injuries that would otherwise take several weeks to heal. Further investigation of heat shock on T/L fibroblasts is needed to determine if it is a viable therapeutic tool. In vivo heat shock experiments can provide more insight on the effect of heat on the wound healing capacity of living tissue. Additionally, heat shock can be used in combination with other therapies, such as exogenous growth factor delivery, to develop a hybrid technique to enhance tendon and ligament repair.
References
Freeman JW. Tissue engineering options for ligament healing. Bone Tissue Regen Insights. 2009;2:13–23.
Attia M, Huet E, Gossard C, Menashi S, Tassoni MC, Martelly I. Early events of overused supraspinatus tendons involve matrix metalloproteinases and EMMPRIN/CD147 in the absence of inflammation. Am J Sports Med. 2013;41(4):908–17. https://doi.org/10.1177/0363546512473817.
Vunjak-Novakovic G, Altman G, Horan R, Kaplan DL. Tissue engineering of ligaments. Annu Rev Biomed Eng. 2004;6:131–56. https://doi.org/10.1146/annurev.bioeng.6.040803.140037.
Ekwueme EC, Shah JV, Mohiuddin M, Ghebes CA, Crispim JF, Saris DB, et al. Cross-talk between human tenocytes and bone marrow stromal cells potentiates extracellular matrix remodeling in vitro. J Cell Biochem. 2016;117(3):684–93. https://doi.org/10.1002/jcb.25353.
Domnick C, Raschke MJ, Herbort M. Biomechanics of the anterior cruciate ligament: physiology, rupture and reconstruction techniques. World J Orthop. 2016;7(2):82–93. https://doi.org/10.5312/wjo.v7.i2.82.
Ekwueme EC, Kwansa AL, Sharif K, El-Amin SF, Freeman JW. Recent advancements in ligament replacement. Recent Pat Biomed Eng. 2011;4(3):196–204. https://doi.org/10.2174/1874764711104030196.
Hast MW, Zuskov A, Soslowsky LJ. The role of animal models in tendon research. Bone Joint Res. 2014;3(6):193–202. https://doi.org/10.1302/2046-3758.36.2000281.
Rothrauff BB, Tuan RS. Cellular therapy in bone-tendon interface regeneration. Organ. 2014;10(1):13–28. https://doi.org/10.4161/org.27404.
Kwan KH, Yeung KW, Liu X, Wong KK, Shum HC, Lam YW, et al. Silver nanoparticles alter proteoglycan expression in the promotion of tendon repair. Nanomedicine. 2014;10(7):1375–83. https://doi.org/10.1016/j.nano.2013.11.015.
Sharma P, Maffulli N. Tendon injury and tendinopathy: healing and repair. J Bone Joint Surg Am. 2005;87(1):187–202. https://doi.org/10.2106/JBJS.D.01850.
James R, Kesturu G, Balian G, Chhabra AB. Tendon: biology, biomechanics, repair, growth factors, and evolving treatment options. J Hand Surg Am. 2008;33(1):102–12. https://doi.org/10.1016/j.jhsa.2007.09.007.
Lynch SA, Renstrom PA. Treatment of acute lateral ankle ligament rupture in the athlete. Conservative versus surgical treatment Sports Med. 1999;27(1):61–71.
Forsyth AL, Zourikian N, Valentino LA, Rivard GE. The effect of cooling on coagulation and haemostasis: should “ice” be part of treatment of acute haemarthrosis in haemophilia? Haemophilia. 2012;18(6):843–50. https://doi.org/10.1111/j.1365-2516.2012.02918.x.
Kuo CK, Marturano JE, Tuan RS. Novel strategies in tendon and ligament tissue engineering: advanced biomaterials and regeneration motifs. Sports Med Arthrosc Rehabil Ther Technol. 2010;2:20. https://doi.org/10.1186/1758-2555-2-20.
Kwansa AL, Empson YM, Ekwueme EC, Walters VI, Freeman JW, Laurencin CT. Novel matrix based anterior cruciate ligament (ACL) regeneration. Soft Matter. 2010;6(20):5016. https://doi.org/10.1039/c0sm00182a.
Barber JG, Handorf AM, Allee TJ, Li WJ. Braided nanofibrous scaffold for tendon and ligament tissue engineering. Tissue Eng Part A. 2013;19(11–12):1265–74. https://doi.org/10.1089/ten.tea.2010.0538.
Cooper JA Jr, Sahota JS, Gorum WJ 2nd, Carter J, Doty SB, Laurencin CT. Biomimetic tissue-engineered anterior cruciate ligament replacement. Proc Natl Acad Sci U S A. 2007;104(9):3049–54. https://doi.org/10.1073/pnas.0608837104.
Erisken C, Zhang X, Moffat KL, Levine WN, Lu HH. Scaffold fiber diameter regulates human tendon fibroblast growth and differentiation. Tissue Eng Part A. 2013;19(3–4):519–28. https://doi.org/10.1089/ten.tea.2012.0072.
Kashiwagi K, Mochizuki Y, Yasunaga Y, Ishida O, Deie M, Ochi M. Effects of transforming growth factor-beta 1 on the early stages of healing of the Achilles tendon in a rat model. Scand J Plast Reconstr Surg Hand Surg. 2004;38(4):193–7. https://doi.org/10.1080/02844310410029110.
Dahlgren LA, Mohammed HO, Nixon AJ. Expression of insulin-like growth factor binding proteins in healing tendon lesions. J Orthop Res. 2006;24(2):183–92. https://doi.org/10.1002/jor.20000.
Molloy T, Wang Y, Murrell GAC. The roles of growth factors in tendon and ligament healing. Sports Med. 2003;33(5):381–94.
Boyer MI, Watson JT, Lou J, Manske PR, Gelberman RH, Cai SR. Quantitative variation in vascular endothelial growth factor mRNA expression during early flexor tendon healing: an investigation in a canine model. J Orthop Res. 2001;19(5):869–72. https://doi.org/10.1016/S0736-0266(01)00017-1.
Watanabe N, Woo SL, Papageorgiou C, Celechovsky C, Takai S. Fate of donor bone marrow cells in medial collateral ligament after simulated autologous transplantation. Microsc Res Tech. 2002;58(1):39–44. https://doi.org/10.1002/jemt.10115.
Chan BP, S-c F, Qin L, K-m L, Rolf CG, K-m C. Effects of basic fibroblast growth factor (bFGF) on early stages of tendon healing: a rat patellar tendon model. Acta Orthop Scand. 2000;71(5):513–8.
Shibaguchi T, Sugiura T, Fujitsu T, Nomura T, Yoshihara T, Naito H, et al. Effects of icing or heat stress on the induction of fibrosis and/or regeneration of injured rat soleus muscle. J Physiol Sci. 2016;66(4):345–57. https://doi.org/10.1007/s12576-015-0433-0.
Hatade T, Takeuchi K, Fujita N, Arakawa T, Miki A. Effect of heat stress soon after muscle injury on the expression of MyoD and myogenin during regeneration process. J Musculoskel Neuron Interact. 2014;14(3):325–33.
Riederer I, Negroni E, Bigot A, Bencze M, Di Santo J, Aamiri A, et al. Heat shock treatment increases engraftment of transplanted human myoblasts into immunodeficient mice. Transplant Proc. 2008;40(2):624–30. https://doi.org/10.1016/j.transproceed.2008.01.026.
Harder Y, Contaldo C, Klenk J, Banic A, Jakob SM, Erni D. Improved skin flap survival after local heat preconditioning in pigs. J Surg Res. 2004;119(1):100–5. https://doi.org/10.1016/j.jss.2003.11.002.
Rylander MN, Diller KR, Wang S, Aggarwal SJ. Correlation of HSP70 expression and cell viability following thermal stimulation of bovine aortic endothelial cells. J Biomech Eng. 2005;127(5):751–7. https://doi.org/10.1115/1.1993661.
Lee MW, Muramatsu T, Uekusa T, Lee JH, Shimono M. Heat stress induces alkaline phosphatase activity and heat shock protein 25 expression in cultured pulp cells. Int Endod J. 2008;41(2):158–62. https://doi.org/10.1111/j.1365-2591.2007.01331.x.
Chung E, Sampson AC, Rylander MN. Influence of heating and cyclic tension on the induction of heat shock proteins and bone-related proteins by MC3T3-E1 cells. Biomed Res Int 2014;2014:354260. doi:https://doi.org/10.1155/2014/354260, 1, 16.
Shui C, Scutt A. Mild heat shock induces proliferation, alkaline phosphatase activity, and mineralization in human bone marrow stromal cells and Mg-63 cells in vitro. J Bone Miner Res. 2001;16(4):731–41. https://doi.org/10.1359/jbmr.2001.16.4.731.
Yoshida K, Uoshima K, Oda K, Maeda T. Influence of heat stress to matrix on bone formation. Clin Oral Implants Res. 2009;20(8):782–90. https://doi.org/10.1111/j.1600-0501.2008.01654.x.
Oberringer M, Baum HP, Jung V, Welter C, Frank J, Kuhlmann M, et al. Differential expression of heat shock protein 70 in well healing and chronic human wound tissue. Biochem Biophys Res Commun. 1995;214(3):1009–14. https://doi.org/10.1006/bbrc.1995.2386.
Mosser DD, Caron AW, Bourget L, Denis-Larose C, Massie B. Role of the human heat shock protein hsp70 in protection against stress-induced apoptosis. Mol Cell Biol. 1997;17(9):5317–27.
Helmbrecht K, Zeise E, Rensing L. Chaperones in cell cycle regulation and mitogenic signal transduction: a review. Cell Prolif. 2000;33:341–65.
Sherman MY, Gabai VL. Hsp70 in cancer: back to the future. Oncogene. 2015;34(32):4153–61. https://doi.org/10.1038/onc.2014.349.
Suzuki K, Watanabe M. Modulation of cell growth and mutation induction by introduction of the expression vector of human hsp70 gene. Exp Cell Res. 1994;215(1):75–81. https://doi.org/10.1006/excr.1994.1317.
Zeise E, Kuhl N, Kunz J, Rensing L. Nuclear translocation of stress protein Hsc70 during S phase in rat C6 glioma cells. Cell Stress Chaperones. 1998;3(2):94–9.
Yoshidomi K, Murakami A, Yakabe K, Sueoka K, Nawata S, Sugino N. Heat shock protein 70 is involved in malignant behaviors and chemosensitivities to cisplatin in cervical squamous cell carcinoma cells. J Obstet Gynaecol Res. 2014;40(5):1188–96. https://doi.org/10.1111/jog.12325.
Zhe Y, Li Y, Liu D, Su DM, Liu JG, Li HY. Extracellular HSP70-peptide complexes promote the proliferation of hepatocellular carcinoma cells via TLR2/4/JNK1/2MAPK pathway. Tumour Biol. 2016;37(10):13951–9. https://doi.org/10.1007/s13277-016-5189-5.
Wu J, Liu T, Rios Z, Mei Q, Lin X, Cao S. Heat shock proteins and cancer. Trends Pharmacol Sci. 2017;38(3):226–56. https://doi.org/10.1016/j.tips.2016.11.009.
Mala JG, Rose C. Interactions of heat shock protein 47 with collagen and the stress response: an unconventional chaperone model? Life Sci. 2010;87(19–22):579–86. https://doi.org/10.1016/j.lfs.2010.09.024.
Ito S, Nagata K. Biology of Hsp47 (serpin H1), a collagen-specific molecular chaperone. Semin Cell Dev Biol. 2017;62:142–51. https://doi.org/10.1016/j.semcdb.2016.11.005.
Ishida Y, Kubota H, Yamamoto A, Kitamura A, Bachinger HP, Nagata K. Type I collagen in Hsp47-null cells is aggregated in endoplasmic reticulum and deficient in N-propeptide processing and fibrillogenesis. Mol Biol Cell. 2006;17(5):2346–55. https://doi.org/10.1091/mbc.E05-11-1065.
Satoh M, Hirayoshi K, Yokota S, Hosokawa N, Nagata K. Intracellular interaction of collagen-specific stress protein HSP47 with newly synthesized procollagen. J Cell Biol. 1996;133(2):469–83.
Liang C-C, Park AY, Guan J-L. In vitro scratch assay: a convenient and inexpensive method for analysis of cell migration in vitro. Nat Protocols. 2007;2(2):329–33.
Chung E, Rylander MN. Response of preosteoblasts to thermal stress conditioning and osteoinductive growth factors. Cell Stress Chaperones. 2012;17(2):203–14. https://doi.org/10.1007/s12192-011-0300-8.
Birch HL, Wilson AM, Goodship AE. The effect of exercise-induced localised hyperthermia on tendon cell survival. J Exp Biol. 1997;200(Pt 11):1703–8.
Hosaka Y, Ozoe S, Kirisawa R, Ueda H, Takehana K, Yamaguchi M. Effect of heat on synthesis of gelatinases and pro-inflammatory cytokines in equine tendinocytes. Biomed Res. 2006;27(5):233–41.
Hsu SL, Liang R, Woo SL. Functional tissue engineering of ligament healing. Sports Med Arthrosc Rehabil Ther Technol. 2010;2:12. https://doi.org/10.1186/1758-2555-2-12.
Millar NL, Murrell GA. Heat shock proteins in tendinopathy: novel molecular regulators. Mediat Inflamm 2012;2012:436203. doi:https://doi.org/10.1155/2012/436203, 1, 7.
Milarski KL, Welch WJ, Morimoto RI. Cell cycle-dependent association of HSP70 with specific cellular proteins. J Cell Biol. 1989;108(2):413–23.
Wang R, Kovalchin JT, Muhlenkamp P, Chandawarkar RY. Exogenous heat shock protein 70 binds macrophage lipid raft microdomain and stimulates phagocytosis, processing, and MCH-II presentation of antigens. Blood. 2006;107(4):1636–42. https://doi.org/10.1182/blood-200506-2559.
Guzhova I, Kislyakova K, Moskaliova O, Fridlanskaya I, Tytell M, Cheetham M, et al. In vitro studies show that Hsp70 can be released by glia and that exogenous Hsp70 can enhance neuronal stress tolerance. Brain Res. 2001;914:66–73.
Nagai N, Hosokawa M, Itohara S, Adachi E, Matsushita T, Hosokawa N, et al. Embryonic lethality of molecular chaperone Hsp47 knockout mice is associated with defects in collagen biosynthesis. J Cell Biol. 2000;150(6):1499–505.
Halper J, Griffin A, Hu W, Jung C, Zhang J, Pan H, et al. In vitro culture decreases the expression of TGF(beta), Hsp47 and type I procollagen and increases the expression of CTGF in avian tendon explants. J Musculoskelet Neuronal Interact. 2005;5(1):53–63.
Leask A, Abraham DJ. TGF-beta signaling and the fibrotic response. FASEB J. 2004;18(7):816–27. https://doi.org/10.1096/fj.03-1273rev.
Li L, Klim JR, Derda R, Courtney AH, Kiessling LL. Spatial control of cell fate using synthetic surfaces to potentiate TGF-beta signaling. Proc Natl Acad Sci U S A. 2011;108(29):11745–50. https://doi.org/10.1073/pnas.1101454108.
Faulknor RA, Olekson MA, Nativ NI, Ghodbane M, Gray AJ, Berthiaume F. Mesenchymal stromal cells reverse hypoxia-mediated suppression of alpha-smooth muscle actin expression in human dermal fibroblasts. Biochem Biophys Res Commun. 2015;458(1):8–13. https://doi.org/10.1016/j.bbrc.2015.01.013.
Henninger HB, Valdez WR, Scott SA, Weiss JA. Elastin governs the mechanical response of medial collateral ligament under shear and transverse tensile loading. Acta Biomater. 2015;25:304–12. https://doi.org/10.1016/j.actbio.2015.07.011.
Fang F, Lake SP. Multiscale mechanical integrity of human supraspinatus tendon in shear after elastin depletion. J Mech Behav Biomed Mater. 2016;63:443–55. https://doi.org/10.1016/j.jmbbm.2016.06.032.
Smith KD, Clegg PD, Innes JF, Comerford EJ. Elastin content is high in the canine cruciate ligament and is associated with degeneration. Vet J. 2014;199(1):169–74. https://doi.org/10.1016/j.tvjl.2013.11.002.
Zhang J, Wang JH. The effects of mechanical loading on tendons—an in vivo and in vitro model study. PLoS One. 2013;8(8):e71740. https://doi.org/10.1371/journal.pone.0071740.
Lu H, Zheng C, Wang Z, Chen C, Chen H, Hu J. Effects of low-intensity pulsed ultrasound on new trabecular bone during bone-tendon junction healing in a rabbit model: a synchrotron radiation micro-CT study. PLoS One. 2015;10(4):e0124724. https://doi.org/10.1371/journal.pone.0124724.
Hu B, Zhang Y, Zhou J, Li J, Deng F, Wang Z, et al. Low-intensity pulsed ultrasound stimulation facilitates osteogenic differentiation of human periodontal ligament cells. PLoS One. 2014;9(4):e95168. https://doi.org/10.1371/journal.pone.0095168.
Yang Z, Ren L, Deng F, Wang Z, Song J. Low-intensity pulsed ultrasound induces osteogenic differentiation of human periodontal ligament cells through activation of bone morphogenetic protein-smad signaling. J Ultrasound Med. 2014;33(5):865–73. https://doi.org/10.7863/ultra.33.5.865.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
The authors alone are responsible for the content and writing of the paper.
Conflict of Interest
The authors declare that they have no conflicts of interest.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Shah, J.V., Ekwueme, E.C. & Freeman, J.W. Investigation of the Short-term Effects of Heat Shock on Human Hamstring Tenocytes In Vitro. Regen. Eng. Transl. Med. 6, 50–61 (2020). https://doi.org/10.1007/s40883-018-0070-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40883-018-0070-2