Abstract
Purpose of Review
The majority of existing research discusses food addiction (FA) classification, which provides information for different groups and which groups may or may not be affected to differing degrees. Fewer studies report FA symptom scores, and fewer still report on individual symptoms. This paper discusses the symptoms of craving and loss of control as they are common FA symptoms that demonstrate similarities with both substance use disorders and some eating disorder pathology.
Recent Findings
Loss of control presents parallels with disordered eating, particularly binge eating disorder. Craving refers to the powerful or strong desire for something and, in contrast to lack of control, presents most overlap with substance use disorders.
Summary
While not the most common symptoms reported in published research, loss of control and craving attract attention because of parallels with substance use and eating disorder pathology, and research has increasingly focused on these symptoms in recent years.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The current state of the literature highlights that food addiction is not a homogenous condition but a multi-faceted and transdiagnostic condition arising from a complex number of individual factors [1•, 2•]. A range of terms have been used in the literature to date to describe the food addiction construct [3] including eating addiction, which is more reflective of the behavioural aspects [4], and more recently ultra-processed food addiction [5••]. The differences in nomenclature highlight the diversity of current research, with the food addiction construct being of interest to a range of researchers and clinicians from various backgrounds. This paper will use the term food addiction (FA), which most research operationalises and reports using one of the various versions the Yale Food Addiction Scale (YFAS) [3, 6]. The YFAS can be scored and reported in several ways, including a FA classification/diagnosis, level of FA severity (mild, moderate, severe), total symptom score and endorsement at the individual symptom level [3, 6]. The majority of existing research discusses FA classification, which provides information for different groups and which groups may or may not be affected to differing degrees. Fewer studies report on symptom scores, and fewer still report endorsement of individual symptoms. The aim of this narrative review is to discuss the symptoms of craving and loss of control (LOC), with a focus on research in recent (i.e. the last 5) years. Craving and LOC are common symptoms that demonstrate similarities between FA and both substance use disorders and some eating disorder pathology and, for these reasons, demonstrate considerable interest.
Food Addiction Classification
FA research is largely dominated by studies in adults, particularly females, and in these studies, FA often presents in its severe form [7••, 8••, 9, 10•]. These studies indicate that on the YFAS 2.0, individuals endorse six or more of the 11 symptoms (Table 1), in addition to the clinical impairment or distress criterion, meaning that it negatively impacts their day-to-day functioning. Clinical impairment or distress from FA has been specifically investigated as this criterion influences whether an individual is classified as FA or not. Clinical impairment or distress is more often reported among women than men and among people with obesity than those who are categorised as overweight [11, 12]. This is an interesting factor in research exploring FA prevalence and highlights why other methods of scoring, such as symptom scores with and without the endorsement of clinical distress or impairment criterion, should be considered further. For example, an individual endorsing 11 symptoms, but not clinical impairment or distress, may benefit from further assessment measures and be highlighted as ‘at risk’. Wiss and Brewerton provide suggestions for the assessment of FA and differential diagnosis [13]. Specifically, they describe a comprehensive approach for assessing FA that takes into consideration factors such as dietary restraint and comorbid psychiatric disorders. Through distinguishing FA from other forms of eating pathology, this approach may help to guide case formulation and treatment planning which is likely not a one size fits all approach for FA management.
While most FA research has been conducted in adults, recently, there has been a growing amount of literature in younger age groups. This includes children and adolescents [15•] and with more equal sex representation in these studies. Evidence from a recent systematic review including 27 studies carried out in adolescents suggests that FA in this younger population is most often reported in its mild/moderate form, indicating fewer symptoms are endorsed [15•]. This is in contrast to the adult literature and may indicate a progression in severity as someone transitions from adolescence to adulthood. In addition, publications have emerged which have considered important insights that demonstrate how FA symptoms occur cross-culturally and that there may be significant differences between sociodemographic groups [16]. Specifically, highlighting issues related to adequate lexicalisation of concepts central to FA, including craving and addiction more broadly, as well as global variations in eating culture and presentation of similar constructs (e.g. binge eating), are important considerations in future research in this area.
Food Addiction Symptomology
While many papers discuss FA classification or diagnosis, providing information in different population groups and subgroups which may or may not be affected to differing degrees, systematic reviews show that fewer studies report on individual symptoms [9]. For example, in a systematic review of 51 studies exploring FA and associations with mental health, only 20 studies reported symptom scores [9]. Similarly, in a recent review of studies that use versions of the YFAS 2.0 tool, 53 studies were included with fewer studies reporting symptom scores compared with classification/diagnosis [12].
Previous reviews report that the average symptom score differs for population subgroups, with clinical samples often endorsing more symptoms than non-clinical samples [9, 12, 17]. A 2014 systematic review of FA prevalence found that 16 of 25 included studies reported on FA symptoms, with a mean of 4.0 FA symptoms endorsed in clinical studies and 1.7 FA symptoms in non-clinical studies [17]. More recently, a 2018 review and meta-analysis of FA associations with mental health (n = 51 studies) found that the mean number of FA symptoms in those seeking treatment for weight loss (n = 9 studies) was 3.0 (upper and lower limit 2.7–3.4) and 5.2 (3.6–6.7) for those with disordered eating (n = 7 studies) [9].
Of those studies that report symptoms, the reporting is quite diverse with some reporting mean number of symptoms only, while others report on the endorsement of individual symptoms. This is an important level of detail or distinction to consider given that some symptoms may not be entirely specific to FA but relate to eating in general, for example, ‘persistent desire or repeated unsuccessful attempts to cut down foods’. Many people in the general population who have experienced or trialled some form of dieting are likely to endorse this symptom [18]. The symptoms of loss of control and craving often receive the most attention due to their perceived overlap with existing eating disorders. In the above-mentioned review of 51 studies exploring FA and associations with mental health [9], among the twenty studies which reported on symptoms, the most common were ‘repeated unsuccessful attempts to cut down’ (n = 13 studies) and ‘consumption despite significant consequences’ (n = 6 studies). In another review, the most commonly reported symptom across studies was ‘the persistent desire or unsuccessful attempts to cut down foods’ [17]. Similarly, in a sample of patients applying for bariatric surgery, ‘persistent desire or unsuccessful efforts to cut down or control consumption of certain foods’ was the most prevalent symptom reported by 93.1% of study participants [19].
In a recent review of FA in adolescents (n = 27 studies) [15•], 16 studies reported symptom scores, and 15 studies reported the frequency of symptom endorsement. Mean symptom scores ranged from 1·0 to 5·2. Similar to studies in adults, scores were found to be higher in clinical compared to non-clinical samples.
From 13 studies using the YFAS or YFAS for children (YFAS-C), the most common symptom endorsed was a ‘persistent desire or repeated unsuccessful attempts to quit’ with a mean endorsement across studies of 62·7%. Of the two studies using the YFAS 2·0, one study in a non-clinical sample reported ‘substance often taken in larger amounts or over a longer period than was intended’ (13·7% study participants) to be the most common symptom, while the other in a clinical sample reported ‘withdrawal’ (44·0% study participants) as the most common [15•].
The symptom level of detail is important, given the area of research is evolving and more recently there is the emergence and trialling of new treatments for the management [8••, 20] of addictive eating. It has been suggested that FA symptoms tend to be stable over time in adults and that the recurrent set of behaviours do not change unless acted on or intervened [21]. However, from the perspective of symptom management or determining if individual symptoms can be changed over time, some specific symptoms may be more amenable to change than others, for example, the level of craving or level of withdrawal experienced rather than other symptoms such as the persistent desire to quit. A recent systematic review of FA treatment studies identified nine intervention studies [8••]; however, only one reported at the individual symptom level [22]. This study, a weight loss focused intervention in children, used the YFAS-C to measure the endorsement of individual FA symptoms within each of the seven diagnostic criteria pre- and post-intervention [22]. Although this study reported no significant differences in symptoms pre- and post-intervention in a sample of 26 adolescents with obesity, six of the seven symptoms did improve by showing a reduction in the level of endorsement. These included ‘continued use despite problems’, ‘inability to cut down’, ‘large amount of time spent’, ‘given up activities’, ‘tolerance’ and ‘withdrawal’. Similarly, a pilot randomised controlled trial of a brief intervention for addictive overeating in adults found no significant between group differences in YFAS 2.0 total symptom scores pre- and post-intervention compared with waitlist control [23•]. However, there were significant reductions over time in the following individual symptoms: ‘substance taken in larger amounts’, ‘persistent desire’, ‘time to obtain’, ‘tolerance’, ‘withdrawal’ and ‘failure to fulfil role obligations’.
Loss of Control and Craving
While craving and LOC are not the most common symptoms of FA in reported literature, they are frequently reported by individuals with FA. This includes qualitative studies in those with lived experience [24••, 25] and in studies where FA is assessed and operationalised using tools such as the YFAS [3], the Three-Factor Eating Questionnaire [26], the Power of Food Scale [27] and the Loss of Control over Eating Scale [28], among others [29]. Craving and LOC are also symptoms common to substance use disorders and sub-types of disordered eating, namely, binge eating disorder (BED) and bulimia nervosa (BN). However, craving is not thought to be a causal mechanism of eating disorders but is considered more broadly to be an indirect contributor to overeating behaviours. For instance, dietary restraint, which is thought to elevate craving, has been identified as a causal trigger of binge eating episodes [30]. While in substance use disorders, craving is directly thought to trigger relapse and as such interventions focus on craving management [31]. Most research of FA is reported via use of the aforementioned self-report tools that align with other substance use disorders [3, 14]. It is however important to consider the behavioural aspects of addictive eating and to consider that looking at FA solely from the perspective of substance use may limit diagnosis and overlook underpinning behavioural components of FA [4].
When considering LOC and craving, it is important to consider the range of contexts in which these can be applied to FA. For some, addictive eating could be about the specific foods consumed, which are typically reported as being ultra-processed foods. That is craving for a specific food and LOC when consuming a particular food. Ultra-processed foods are a combination of mostly industrial use ingredients, such as high-fructose corn syrup, hydrogenated oils, hydrolysed proteins and flavour enhancers, which are formulated into food products by a series of industrial processes [32]. Ultra-processed foods include, for example, sugar-sweetened drinks, chocolate, savoury biscuits and reconstituted meat products. The best definition and classification system for ultra-processed foods is the NOVA system, devised by Monteiro et al. in 2009 [33], which categorises foods into four groups based on the level of processing (unprocessed or minimally processed foods, processed culinary ingredients, processed foods, ultra-processed foods). A recent systematic review exploring dietary intakes associated with addictive eating behaviours identified 15 studies, predominantly conducted in adults (n = 12) [7••]. From this review, the foods commonly associated with addictive eating were those high in fat and refined carbohydrates, while individuals that met the criteria for FA were found to have significantly higher intakes of energy, carbohydrates and fats than those without FA. When considering the broad research area of FA, 15 studies are few studies to explore this association, and of these, only one study was identified that investigated processed foods as defined by the NOVA classification system.
For other individuals, FA could be about volume eating to gain a greater intensity of fullness or satiety as a sense of reward rather than the specific food. In these cases, craving and LOC may be applied to food more generally. The volume of food consumed and sense of reward achieved from this may be an alternative driver of addictive eating behaviour for some individuals. This may be in the form of recurring binge eating episodes, with evidence demonstrating that there is some overlap between FA and BED [34]. However, the overconsumption of food may occur in the form of grazing episodes across the day or night [35], with more recent measurement tools being developed that assess grazing in terms of frequency and associated emotions, including LOC [36]. Further, grazing that is associated with FA has been shown to contribute unique variance to the YFAS symptom score [35]. These findings provide interesting insight into the association between a grazing pattern of overeating and FA and emphasise that similar to traditional addiction disorders such as alcoholism, binge consumption is not the only pattern of compulsive intake [35].
Loss of Control
The symptom of LOC in FA is operationalised through the YFAS symptom ‘substance (certain foods) taken in larger amount and for longer period than intended’. It is a subjective term and the element that is most often discussed when considering FA in parallel with disordered eating. When we consider LOC within the broader field of disordered eating, there are some attempts to separate objective from subjective binge eating [37, 38]. For example, objective binge eating is defined as LOC during eating combined with consumption of an unusually large amount of food, determined by trained clinical interviewers [37]. In contrast, subjective binge eating can be LOC without the unusually large amounts of food consumed yet considered as excessive by the individual. Interestingly, a comparison of demographic characteristics and health-related quality of life between individuals with objective versus subjective binge eating found no significant differences, providing support for a change in eating disorders diagnostic criteria to be inclusive of subjective as well as objective binge eating [38].
There have been previous reports that FA may be a sub-type of disordered eating and that the FA construct is an indicator of higher eating disorder severity [39]. Studies comparing individuals with LOC eating who do and do not have objectively large binge episodes have found that the degree of LOC is more important than binge size to psychological and behavioural outcomes [40••]. Greater LOC had a stronger independent association than binge size with higher total eating psychopathology, shape dissatisfaction, hunger, food cravings and FA symptoms [40••]. This is interesting as recent research has shown that in some individuals with FA, it may be separate from binge eating as there may not be a distinct period of bingeing or overeating but instead grazing [35] in which the quantity of food consumed may remain consistent from day to day. There is emergence of several grazing tools that may be considered alongside the assessment of FA, food intake and binge eating in future research, including the Short Inventory of Grazing (SIG) and the Grazing Questionnaire (GQ) [36, 41]. Research suggests that FA does show overlap with several disordered eating phenotypes, with the majority of existing research investigating BED and BN rather than other disordered eating categories such as anorexia nervosa (AN) [42, 43]. However, more recently, there has been emergence of FA research and overlap with AN, and while it may be a surprising finding, there have been reports that this is thought to reflect the element of control [44].
In studies that have assessed binge eating and FA, overlap has been shown but not in its entirety [34, 45]. In one study, binge eating was assessed through the Binge Eating Scale (BES) and addictive eating behaviours through the YFAS (n = 1344) [34]. The prevalence and severity of both FA and binge eating increased across weight categories. The overall correlation between the total score from the BES and FA symptoms was r = 0.76, p < 0.001; for females, it was r = 0.77, p < 0.001; and for males, it was r = 0.65, p < 0.001. Total BES score and the BES emotion factor were most often associated with FA symptoms, as was demonstrated to produce stronger correlations with FA symptoms. In contrast, the BES behaviour factor was less strongly associated to FA with the majority of correlations < 0.6. In another study, it was identified that there was overlap between FA and BED symptoms, with 92% of the individuals with BED meeting criteria for mild, moderate or severe FA assessed by the YFAS 2.0 [46]. However, the point was also made that research needs to look beyond symptoms and explore underlying mechanisms that overlap and differ between FA and BED.
The broader element of control should also be considered in the context of FA. Qualitative research provides the opportunity to explore this in greater depth [24••, 47, 48•]. Qualitative studies with individuals with lived experience of FA have identified several elements, with the most common being that the experience of FA was about difficulty and inability in gaining control [24••, 48•]. One study found that individuals felt LOC was a cause of their addictive-like eating [25], while in another more recent study, the theme of control was found to have three sub-themes including controlling actions around food, weight and relative to self-set timeframes for making change [24••]. Pre-occupation with food and eating has also been commonly reported by individuals with FA, including unrelenting cravings [24••, 48•].
Craving
Craving refers to the powerful or strong desire for something. Craving was added as a symptom to the YFAS in 2016 when revisions were made to the original YFAS tool (2009) to align with the Diagnostic and Statistical Manual of Mental Disorders (DSM-V) criteria (i.e. YFAS 2.0) [6, 49]. Craving is self-reported and therefore subjective. Many people report cravings towards particular foods, commonly cited are chocolate, chips and sweets or lollies [23•, 50]. However, this does vary from one person to the next, and for this reason, tools such as the YFAS typically use terminology such as ‘certain foods’ which individuals can interpret as whichever foods are relevant to their experience of addictive eating.
In contrast to LOC, this symptom when discussed in the context of FA presents the most overlap with substance use disorders. In addition to this, other symptoms such as tolerance and withdrawal also present similarity. In substance use disorders, the craved substance is the individuals’ substance of choice, typically a more potent form of the plant, substance or other from which it was derived, e.g. cocaine from the coca plant. Higher intakes of ultra-processed foods have been observed in association with FA [51]. This may suggest that these foods and/or individual components of them are facilitative of an addictive response and therefore craving of them, similar to the process of substance addiction. Ultra-processed foods are manufactured to be highly palatable by combining multiple processed ingredients to achieve optimised sensory properties, which may induce craving. For these reasons, there have been suggestions that evolving interventions should consider both personalised as well as societal level changes [52].
Investigation into the neurobiological mechanisms involved in compulsive behaviour driven by drugs and obesogenic diets using animal models found overlapping neuroadaptations [53]. In humans, neuroimaging studies have demonstrated that both food and drugs of abuse can stimulate dopamine-based reward pathways [54], providing support that FA may operate similarly to substance use disorders. Further, a systematic review and meta-analysis of excitatory neuromodulation interventions (n = 22) aiming to reduce craving and consumption in individuals with drug addiction (n = 18) or overeating behaviour (n = 4) found immediate and longer term reductions in craving and consumption in drug addiction and overeating interventions [31]. Links between substance use and FA in relation to craving have also drawn on research into cue reactivity [55]. Research in substance use has demonstrated that exposure to cues related to substance use, for example, the sight of drugs, induces craving among other physiological responses [56]. The combination of cue exposure and induced craving has been found to then increase the likelihood of substance use [56]. This has also been explored in relation to food, with a review and meta-analysis of such studies (n = 45) finding that both food cue reactivity and cue-induced craving had a medium effect size on eating and weight outcomes in the short and long term [55].
A recent review on FA combined perspectives from experts in addiction, nutrition, psychology and neuroscience backgrounds [57••]. Interestingly, the role of craving was discussed in two ways. Firstly, certain foods or food components may be craved as discussed above, most likely ultra-processed foods or shared components of these foods such as sugar and/or fat. Secondly, the metabolic response to consuming such foods, for example, changes in blood glucose and hormone levels, may be linked to their craving and addictive potential.
Conclusion
This paper discusses two of the symptoms associated with addictive eating and considers them in the context of both eating disorders and substance use disorders. Findings from this review demonstrate the many parallels that exist between LOC and eating disorders, particularly BED, and craving and substance use disorder. Additionally, both symptoms are often presented in the context of highly palatable or ultra-processed foods. Currently, there are a limited number of intervention studies in FA. While the review does not consider the broader range of FA symptoms or the clinical impairment or distress criterion, it provides further understanding of how LOC and craving may be targeted in future research. Specifically, it will be important to evaluate how eating disorder and substance use disorder management strategies and approaches may be incorporated into FA intervention plans. Further, clinical trials examining intervention efficacy on individual symptoms will be particularly relevant.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
De Luca A, Brunault P. Addictive-like eating: interindividual differences matter. Am J Clin Nutr. 2021;114(1):393–4. https://doi.org/10.1093/ajcn/nqab181. Letter to the editor that raises some important considerations regarding the complexity of the FA construct.
Piccinni A, Bucchi R, Fini C, Vanelli F, Mauri M, Stallone T, et al. Food addiction and psychiatric comorbidities: a review of current evidence. Eat Weight Disord. 2021;26(4):1049–56. https://doi.org/10.1007/s40519-020-01021-3. A review of FA that emphasises the parallels between FA and substance use disorders, affective disorders and eating disorders. Provides support for a transdiagnostic approach to FA.
Gearhardt AN, Corbin WR, Brownell KD. Preliminary validation of the Yale Food Addiction Scale. Appetite. 2009;52(2):430–6. https://doi.org/10.1016/j.appet.2008.12.003.
Hebebrand J, Albayrak Ö, Adan R, Antel J, Dieguez C, de Jong J, et al. “Eating addiction”, rather than “food addiction”, better captures addictive-like eating behavior. Neurosci Biobehav Rev. 2014;47:295–306. https://doi.org/10.1016/j.neubiorev.2014.08.016.
Wiss D. Clinical considerations of ultra-processed food addiction across weight classes: an eating disorder treatment and care perspective. Curr Addict Rep. 2022:1–13. https://doi.org/10.1007/s40429-022-00411-0. Review of ultra-processed FA and the associations with weight status and mental health conditions. Provides important clinical considerations for the assessment of FA.
Gearhardt AN, Corbin WR, Brownell KD. Development of the Yale Food Addiction Scale version 2.0. Psychol Addict Behav. 2016;30(1):113–21. https://doi.org/10.1037/adb0000136.
Pursey KM, Skinner J, Leary M, Burrows T. The relationship between addictive eating and dietary intake: a systematic review. Nutrients. 2022;14(1). https://doi.org/10.3390/nu14010164. Systematic review that consolidates evidence of the nutrients, foods and dietary patterns that may be associated with addictive eating.
Leary M, Pursey KM, Verdejo-Garcia A, Burrows TL. Current intervention treatments for food addiction: a systematic review. Behav Sci. 2021;11(6). https://doi.org/10.3390/bs11060080. A systematic review of intervention studies that have been trialled for the treatment and management of addictive eating. This will assist in informing future strategies to reduce FA outcomes in adults.
Burrows T, Kay-Lambkin F, Pursey K, Skinner J, Dayas C. Food addiction and associations with mental health symptoms: a systematic review with meta-analysis. J Hum Nutr Diet. 2018;31(4):544–72. https://doi.org/10.1111/jhn.12532.
Praxedes DRS, Silva-Júnior AE, Macena ML, Oliveira AD, Cardoso KS, Nunes LO, et al. Prevalence of food addiction determined by the Yale Food Addiction Scale and associated factors: a systematic review with meta-analysis. Eur Eat Disord Rev. 2022;30(2):85–95. https://doi.org/10.1002/erv.2878. A recent meta-analysis of the prevalence of FA in clinical and non-clinical samples of adults and children.
Carr MM, Lawson JL, Wiedemann AA, Barnes RD. Examining impairment and distress from food addiction across demographic and weight groups. Eat Behav. 2021;43:101574. https://doi.org/10.1016/j.eatbeh.2021.101574.
Oliveira J, Colombarolli MS, Cordás TA. Prevalence and correlates of food addiction: Systematic review of studies with the YFAS 2.0. Obes Res Clin Pract. 2021;15(3):191–204. https://doi.org/10.1016/j.orcp.2021.03.014.
Wiss D, Brewerton T. Separating the signal from the noise: how psychiatric diagnoses can help discern food addiction from dietary restraint. Nutrients. 2020;12(10):2937. https://doi.org/10.3390/nu12102937.
Schulte EM, Wadden TA, Allison KC. An evaluation of food addiction as a distinct psychiatric disorder. Int J Eat Dis. 2020;53(10):1610–22. https://doi.org/10.1002/eat.23350.
Skinner J, Jebeile H, Burrows T. Food addiction and mental health in adolescents: a systematic review. Lancet Child Adolesc Health. 2021;5(10):751–66. https://doi.org/10.1016/S2352-4642(21)00126-7. This systematic review on FA prevalence and symptomology in adolescents and children highlights the co-occurrence of FA with other mental health conditions.
Lawson JL, Wiedemann AA, Carr MM, Kerrigan SG. Considering food addiction through a cultural lens. Curr Addict Rep. 2020;7(3):387–94. https://doi.org/10.1007/s40429-020-00315-x.
Pursey K, Stanwell P, Gearhardt A, Collins C, Burrows T. The prevalence of food addiction as assessed by the Yale Food Addiction Scale: a systematic review. Nutrients. 2014;6:4552–90. https://doi.org/10.3390/nu6104552.
French SA, Jeffery RW, Murray D. Is dieting good for you?: Prevalence, duration and associated weight and behaviour changes for specific weight loss strategies over four years in US adults. Int J Obes Relat Metab Disord. 1999;23(3):320–7. https://doi.org/10.1038/sj.ijo.0800822.
Brunault P, Ducluzeau PH, Bourbao-Tournois C, Delbachian I, Couet C, Réveillère C, et al. Food addiction in bariatric surgery candidates: prevalence and risk factors. Obes Surg. 2016;26(7):1650–3. https://doi.org/10.1007/s11695-016-2189-x.
Cassin SE, Sijercic I, Montemarano V. Psychosocial interventions for food addiction: a systematic review. Curr Addict Rep. 2020;7:9–19. https://doi.org/10.1007/s40429-020-00295-y.
Pursey K, Collins C, Stanwell P, Burrows T. The stability of ‘food addiction’ as assessed by the Yale Food Addiction Scale in a non-clinical population over 18-months. Appetite. 2016;1(96):533–8. https://doi.org/10.1016/j.appet.2015.10.015.
Tompkins CL, Laurent J, Brock DW. Food addiction: a barrier for effective weight management for obese adolescents. Child Obes. 2017;13(6):462–9. https://doi.org/10.1089/chi.2017.0003.
Burrows T, Collins R, Rollo M, Leary M, Hides L, Davis C. The feasibility of a personality targeted intervention for addictive overeating: FoodFix Appetite. 2021;156(104974). https://doi.org/10.1016/j.appet.2020.104974. This study demonstrates that there is potential to reduce severity of FA with appropriate intervention strategies.
Collins R, Haracz K, Leary M, Rollo M, Burrows T. No control and overwhelming cravings: Australian adults’ perspectives on the experience of food addiction. Appetite. 2021;159:105054. https://doi.org/10.1016/j.appet.2020.105054. This study provides a unique contribution to understanding adults’ experience of FA and highlights the dominance of ‘loss of control’ and ‘craving’ in FA.
Ruddock HK, Dickson JM, Field M, Hardman CA. Eating to live or living to eat? Exploring the causal attributions of self-perceived food addiction. Appetite. 2015;95:262–8. https://doi.org/10.1016/j.appet.2015.07.018.
Stunkard AJ, Messick S. The three-factor eating questionnaire to measure dietary restraint, disinhibition and hunger. J Psychosom Res. 1985;29(1):71–83. https://doi.org/10.1016/0022-3999(85)90010-8.
Lowe MR, Butryn ML, Didie ER, Annunziato RA, Thomas JG, Crerand CE, et al. The power of food scale. A new measure of the psychological influence of the food environment. Appetite. 2009;53(1):114–8. https://doi.org/10.1016/j.appet.2009.05.016.
Latner JD, Mond JM, Kelly MC, Haynes SN, Hay PJ. The loss of control over eating scale: development and psychometric evaluation. Int J Eat Disord. 2014;47(6):647–59. https://doi.org/10.1002/eat.22296.
Vainik U, García-García I, Dagher A. Uncontrolled eating: a unifying heritable trait linked with obesity, overeating, personality and the brain. Eur J Neurosci. 2019;50(3):2430–45. https://doi.org/10.1111/ejn.14352.
Neumark-Sztainer D, Wall M, Guo J, Story M, Haines M, Eisenberg M. Obesity, disordered eating, and eating disorders in a longitudinal study of adolescents: how do dieters fare 5 years later? JADA. 2006;106(4):559–68.
Song S, Zilverstand A, Gui W, Pan X, Zhou X. Reducing craving and consumption in individuals with drug addiction, obesity or overeating through neuromodulation intervention: a systematic review and meta-analysis of its follow-up effects. Addiction. 2022;117(5):1242–55. https://doi.org/10.1111/add.15686.
Monteiro CA, Cannon G, Levy RB, Moubarac JC, Louzada ML, Rauber F, et al. Ultra-processed foods: what they are and how to identify them. Public Health Nutr. 2019;22(5):936–41. https://doi.org/10.1017/s1368980018003762.
Monteiro C, Levy R, Claro R, Castro I, Cannon G. A new classification of foods based on the extent and purpose of their processing. Cad Saude Publica. 2010;26(11):2039–49. https://doi.org/10.1590/S0102-311X2010001100005.
Burrows T, Skinner J, McKenna R, Rollo M. Food addiction, binge eating disorder, and obesity: is there a relationship? Behav Sci. 2017;7(3). https://doi.org/10.3390/bs7030054.
Bonder R, Davis C, Kuk JL, Loxton NJ. Compulsive “grazing” and addictive tendencies towards food. Eur Eat Disord Rev. 2018;26(6):569–73. https://doi.org/10.1002/erv.2642.
Heriseanu AI, Hay P, Touyz S. The short inventory of grazing (SIG): development and validation of a new brief measure of a common eating behaviour with a compulsive dimension. J Eat Disord. 2019;7:4. https://doi.org/10.1186/s40337-019-0234-6.
Brownstone LM, Mihas P, Butler RM, Maman S, Peterson CB, Bulik CM, et al. Lived experiences of subjective binge eating: an inductive thematic analysis. Int J Eat Disord. 2021;54(12):2192–205. https://doi.org/10.1002/eat.23636.
Li N, Mitchison D, Touyz S, Hay P. Cross-sectional comparison of health-related quality of life and other features in people with and without objective and subjective binge eating using a general population sample. BMJ Open. 2019;9(2):e024227. https://doi.org/10.1136/bmjopen-2018-024227.
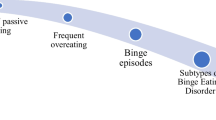
Davis C. From passive overeating to “food addiction”: a spectrum of compulsion and severity. ISRN Obes. 2013;435027:1–20.
Bruzas MB, Tronieri JS, Chao AM, Jones E, McAllister C, Gruber K, et al. Binge size and loss of control as correlates of eating behavior and psychopathology among individuals with binge eating disorder and higher weight. J Behav Med. 2022. https://doi.org/10.1007/s10865-022-00312-7. This study demonstrates the nuances of binge eating, including loss of control, and the associations with FA.
Lane B, Szabó M. Uncontrolled, repetitive eating of small amounts of food or ‘grazing’: development and evaluation of a new measure of atypical eating. Behav Change. 2013;30(2):57–73. https://doi.org/10.1017/bec.2013.6.
Schulte EM, Grilo CM, Gearhardt AN. Shared and unique mechanisms underlying binge eating disorder and addictive disorders. Clin Psychol Rev. 2016;44:125–39. https://doi.org/10.1016/j.cpr.2016.02.001.
Hilker I, Sanchez I, Steward T, Jimenez-Murcia S, Granero R, Gearhardt AN, et al. Food addiction in bulimia nervosa: clinical correlates and association with response to a brief psychoeducational intervention. Eur Eat Disord Rev. 2016;24(6):482–8. https://doi.org/10.1002/erv.2473.
Sanchez I, Lucas I, Munguía L, Camacho-Barcia L, Giménez M, Sánchez-González J, et al. Food addiction in anorexia nervosa: implications for the understanding of crossover diagnosis. Eur Eat Disord Rev. 2022;30(3):278–88. https://doi.org/10.1002/erv.2897.
Hauck C, Cook B, Ellrott T. Food addiction, eating addiction and eating disorders. Proc Nutr Soc. 2020;79(1):103–12. https://doi.org/10.1017/S0029665119001162.
Carter JC, Van Wijk M, Rowsell M. Symptoms of ‘food addiction’ in binge eating disorder using the Yale Food Addiction Scale version 2.0. Appetite. 2019;133:362–9. https://doi.org/10.1016/j.appet.2018.11.032.
Curtis C, Davis C. A qualitative study of binge eating and obesity from an addiction perspective. Eat Disord. 2014;22(1):19–32. https://doi.org/10.1080/10640266.2014.857515.
Lacroix E, von Ranson KM. Lived experience and defining addictive-like eating: a synthesis of qualitative research. Curr Addict Rep. 2020;7(4):437–45. https://doi.org/10.1007/s40429-020-00343-7. Findings from this review emphasise the central role of ‘loss of control’ in addictive-like eating and the overlap of FA with binge eating.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders: DSM-5. 5th ed. Washington, D.C.: American Psychiatric Association; 2013.
Ayaz A, Nergiz-Unal R, Dedebayraktar D, Akyol A, Pekcan AG, Besler HT, et al. How does food addiction influence dietary intake profile? PLoS ONE. 2018;13(4). https://doi.org/10.1371/journal.pone.0195541.
Schulte E, Avena N, Gearhardt A. Which foods may be addictive? The roles of processing, fat content, and glycemic load. PLoS ONE. 2015;10(2):e0117959. https://doi.org/10.1371/journal.pone.0117959.
Lustig RH. Ultraprocessed food: addictive, toxic, and ready for regulation. Nutrients. 2020;12(11). https://doi.org/10.3390/nu12113401.
Laque A, Wagner GE, Matzeu A, De Ness GL, Kerr TM, Carroll AM, et al. Linking drug and food addiction via compulsive appetite. Br J Pharmacol. 2022. https://doi.org/10.1111/bph.15797.
Fortuna JL. The obesity epidemic and food addiction: clinical similarities to drug dependence. J Psychoactive Drugs. 2012;44(1):56–63. https://doi.org/10.1080/02791072.2012.662092.
Boswell RG, Kober H. Food cue reactivity and craving predict eating and weight gain: a meta-analytic review. Obes Rev. 2016;17(2):159–77. https://doi.org/10.1111/obr.12354.
Carter BL, Tiffany ST. Meta-analysis of cue-reactivity in addiction research. Addiction. 1999;94(3):327–40.
Constant A, Moirand R, Thibault R, Val-Laillet D. Meeting of minds around food addiction: insights from addiction medicine, nutrition, psychology, and neurosciences. Nutrients. 2020;12(11). https://doi.org/10.3390/nu12113564. This review provides important and varied perspectives on FA from experts in addiction, nutrition, psychology and neuroscience.
Acknowledgement
Tracy Burrows is supported by a National Health and Medical Council (NHMRC) Emerging Leader Fellowship.
Funding
Open Access funding enabled and organized by CAUL and its Member Institutions
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
This article is part of the Topical Collection on Food Addiction
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Whatnall, M., Skinner, J.A., Leary, M. et al. Food Addiction: a Deep Dive into ‘Loss of Control’ and ‘Craving’. Curr Addict Rep 9, 318–325 (2022). https://doi.org/10.1007/s40429-022-00431-w
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s40429-022-00431-w