Abstract
Purpose
We aimed to develop and validate a simplified, novel quantification method for radioiodine whole-body scans (WBSs) as a predictor for the treatment response in differentiated thyroid carcinoma (DTC) patients with distant metastasis.
Methods
We retrospectively reviewed serial WBSs after radioiodine treatment from 2008 to 2011 in patients with metastatic DTC. For standardization of TSH simulation, only a subset of patients whose TSH level was fully enhanced (TSH > 80 mU/l) was enrolled. The radioiodine scan index (RSI) was calculated by the ratio of tumor-to-brain uptake. We compared correlations between the RSI and TSH-stimulated serum thyroglobulin (TSH_s_Tg) level and between the RSI and Tg reduction rate of consecutive radioiodine treatments.
Results
A total of 30 rounds of radioiodine treatment for 15 patients were eligible. Tumor histology was 11 papillary and 4 follicular subtypes. The TSH_s_Tg level was mean 980 ng/ml (range, 0.5–11,244). The Tg reduction rate after treatment was a mean of −7 % (range, −90 %–210 %). Mean RSI was 3.02 (range, 0.40–10.97). RSI was positively correlated with the TSH_s_Tg level (R2 = 0.3084, p = 0.001) and negatively correlated with the Tg reduction rate (R2 = 0.2993, p = 0.037). The regression equation to predict treatment response was as follows: Tg reduction rate = −14.581 × RSI + 51.183.
Conclusions
Use of the radioiodine scan index derived from conventional WBS is feasible to reflect the serum Tg level in patients with metastatic DTC, and it may be useful for predicting the biologic treatment response after radioiodine treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The incidence of thyroid cancer has increased for several decades in many countries [1–3]. Although the overall recurrence and mortality rates are lower than those of most other malignancies, distant metastasis often leads to an unfavorable prognosis with increased morbidity and mortality [4–6]. The two most frequent sites of distant metastases are the lungs and bones [4]. Radioiodine treatment has been successfully used for such metastatic DTCs for 70 years [7, 8]. The outcome of radioiodine treatment in metastatic DTC is related to the radiation dose delivered to the tumor tissue and to its sensitivity to radiation [9]. Thus, evaluation of the delivered dose to tumor tissue is essential to predict the treatment response and plan consecutive management in patients with metastatic DTC.
The radioiodine activity delivered to tumor tissue can be estimated by radioiodine dosimetry, which allows calculation of the absorbed dose to iodine-avid metastatic tissue and determination of the maximized individual dose that is safe from toxicity or serious side effects of radioiodine treatment [10]. However, the methodology, a number of imagings and samplings before or during radioiodine treatment, is cumbersome in routine clinical practice. Instead of dosimetric evaluation, there is currently no simplified, quantitative parameter derived from post-treatment whole-body scans (WBSs) to predict the treatment response in patients with metastatic thyroid carcinoma. Therefore, we aimed to develop a novel and simple quantification method for tumor radioiodine uptake on post-treatment WBS and validate its use as a predictor for the treatment response in patients with metastatic DTC.
Materials and methods
Patients
Serial WBSs after radioiodine treatment from 2008 to 2011 in patients with metastatic DTC were retrospectively reviewed. For standardization of TSH stimulation, only a subset of patients whose TSH level was fully enhanced (TSH > 80 mU/l) was enrolled. The patients who underwent other treatments such as an operation, external radiotherapy, or chemotherapy for metastatic lesions were excluded. Radioiodine treatment was performed after at least 4-week withdrawal from levothyroxine and a 2-week low-iodine diet. All patients were admitted for 3–4 days and underwent assays for TSH, TSH-stimulated serum thyroglobulin (TSH_s_Tg), and antithyroglobulin antibodies (ATA) on the day of radioiodine treatment. Repetitive treatment was performed within 6 to 12 months after initial treatment. If the patients underwent F-18 FDG PET/CT (Discovery ST System, GE Healthcare, Milwaukee, WI, USA) scans, the results were also recorded as positive or negative according to the presence of FDG uptake exceeding background activity. The local ethics committees approved the study, and all enrolled patients gave written informed consent.
Radioiodine whole-body scans
A single post-treatment WBS was performed 4–6 days after radioiodine administration. Images were acquired in the anterior and posterior projections using two variable-angle dual-head gamma cameras (Infinia, GE Healthcare, Milwaukee, WI, USA). The instrument has parallel-hole high-energy collimators, with a matrix size of 256 × 1024 and a 364-keV photopeak with 10 % windows. The table speed for whole-body imaging was 12 cm/min.
Radioiodine scan index
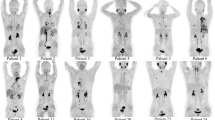
Radioiodine uptake in each region of interest (ROI) was initially estimated by the arithmetic mean of the anterior and posterior images of post-treatment WBSs (Fig. 1).
The tumor ROI, which is the fully encasing abnormal radioiodine uptake suggesting metastasis, was drawn manually, and the initial tumor uptake was obtained. A circular ROI with 1500 pixel size was drawn in the middle of the brain for background activity. None of the patients showed abnormally increased radioiodine uptake in the brain or clinical symptoms suggesting brain metastasis. Area-corrected brain uptake was calculated by the following formula:
Corrected tumor uptake was estimated by subtraction of the area-corrected brain uptake from the initial tumor uptake.
The radioiodine scan index (RSI) was calculated by the ratio of the corrected tumor uptake to the area-corrected brain uptake.
The summarized formula for RSI using initial parameter is as follows:
Analysis
The Tg reduction rate was calculated by the ratio of the TSH_s_Tg level between two sequential treatment rounds.
Data analysis using the ATA-corrected serum Tg level was also performed. The ATA-corrected serum Tg level was calculated by the following formula according to a previous report that provided a mathematical equation for estimation of the true Tg concentration under various concentrations of ATA using data from experiments using patients’ serum [11]:
Comparisons of the TSH_s_Tg level and RSI according to FDG avidity were performed using the Mann-Whitney U test. The Pearson correlation coefficient was used for assessment of correlations between the RSI and TSH_s_Tg level as well as the RSI and Tg reduction rate. The regression equation between the RSI and Tg reduction rate to predict treatment response was also derived. Medcalc software (version 11.4; MedCalc, Mariakerke, Belgium) was used for all statistical calculations, and p < 0.05 was considered statistically significant.
Results
Patients
A total of 30 rounds of radioiodine treatment in 15 patients were eligible (Table 1). Tumor histology was 11 papillary and 4 follicular subtypes. Initial T staging was 3 in 10 patients and 4 in 5 patients, and initial N staging was 0 in 3 patients, 1a in 2 patients, and 1b in 10 patients. Treatment dose of I-131 was 5.6 GBq (150 mCi) in 2, 6.7 GBq (180 mCi) in 3, and 7.4 GBq (200 mCi) in 25 rounds of treatment (Table 2). Post-treatment WBS was performed 5 days after radioiodine administration in a majority of rounds (23/30) and after 4 days in 4 rounds and 6 days in 3 rounds. The TSH_s_Tg level was mean 980 ng/ml (range, 0.5–11,244). Mean Tg reduction rate was −7 % (range, −90 %–210 %). The serum ATA level was mean 147 IU/ml (range, 12–508). The ATA-corrected Tg level was mean 1,336 ng/ml (range, 2–16,143). All patients had lung metastasis, and one patient had an additional pelvic bone metastasis (Table 3). An FDG-avid lesion was detected in five patients, whereas seven had non-FDG-avid metastasis. An F-18 FDG PET/CT scan was not performed in three patients. Mean TSH_s_Tg level and RSI between patients with FDG uptake and without FDG uptake were not statistically different [TSH_s_Tg level: 668 ± 663 ng/ml in FDG-avid patients and 1877 ± 4165 ng/ml in FDG-non-avid patients (p = 0.291), RSI: 2.47 ± 2.9 in FDG-avid patients and 0.92 ± 3.24 in FDG-non-avid patients (p = 0.213)].
Radioiodine scan index
Mean RSI was 3.02 (range, 0.40–10.97). RSI was positively correlated with the TSH_s_Tg level (R2 = 0.3084, p = 0.001) and negatively correlated with the Tg reduction rate (R2 = 0.2993, p = 0.037) (Fig. 2). In a selected cohort with high TSH_s_Tg levels (Tg >100 ng/ml), the RSI was more strongly correlated with the TSH_s_Tg level (R2 = 0.7365, p < 0.001, n = 15) and showed a weak negative correlation with the Tg reduction rate without statistical significance (R2 = 0.1594, p = 0.327, n = 8) (Fig. 3). When the TSH_s_Tg level was corrected by the serum ATA level, the RSI was also positively correlated with the ATA-corrected Tg level (R2 = 0.3116, p = 0.001). Although it did not reach statistical significance, the RSI was also negatively correlated with the ATA-corrected Tg reduction rate (R2 = 0.2386, p = 0.065) (Fig. 4). The regression equation to predict treatment response was the following: Tg reduction rate = − 14.581 × RSI + 51.183. According to the equation, the patients showing 3.5 or more RSI were suggested to have achieved Tg reduction by the radioiodine treatment.
Discussion
The extent of the metastatic tumor burden can be estimated with the serum Tg level and radioiodine WBS. Although Tg synthesis and radioiodine uptake reflect different thyroid tissue functions [12, 13], the radioiodine scan index, the ratio of background-subtracted tumor uptake to background uptake, derived from single post-treatment WBS was feasible as a simplified, quantitative parameter to estimate the metastatic tumor burden. It was well correlated with the TSH_s_Tg level and Tg reduction rate. The avidity of radioiodine is a well-known favorable prognostic factor in patients with DTC [8, 14–16]. The dose of radioiodine delivered to metastatic tissue can be calculated by a dosimetry-based regimen, but the methodology is quiet cumbersome in routine clinical practice [10, 17, 18]. Our results showed a simplified index also predicts the response, the decline of the serum Tg level, to radioiodine treatment during multiple cycles of radioiodine treatment.
Tg, which is produced only by cancerous or noncancerous thyroid follicular cells, is an excellent tumor marker for patients with DTC [19]. The sensitivity of Tg, however, depends on the serum TSH level and is much greater under TSH elevation >30 mU/l (98 %) than under TSH-suppressive thyroid hormone therapy (80 %)[19]. Because the serum Tg level is highly variable according to the serum TSH level, we enrolled only patients with a fully enhanced serum TSH level (>80 mU/l) corresponding to the upper limit of measurement in our institution.
Cervical uptake reflecting the radioiodine concentration in remnant thyroid tissue is conventionally measured using a gamma probe [20–22]. However, measurement of the whole metastatic tumor burden using a gamma probe is not easy. Instead of this, ROI-based measurement can be applied using a reference region in the brain area [23]. Brain is feasible as a background, because it only has blood pool activity, as sodium iodide cannot pass through the blood-brain barrier [24, 25]. Lim et al. [23] simply used the count ratio between the same-sized rectangular ROIs in the anterior neck and brain as the thyroid-to-background ratio in a single anterior image. We used mean counts of anterior and posterior images because metastatic organs, such as the lung, have more three-dimensional structures than the neck area. Additionally, background activity is subtracted from initial tumor activity before calculating the ratio of tumor uptake and background activity, because initial tumor uptake includes background blood pool activity. The radioiodine scan index was calculated as the ratio of ‘true’ tumor uptake to background uptake. The last step could partly correct the influence of the treatment dose and scanning time.
We acknowledge there are many limitations to this study. First, this is a retrospective analysis with a small sample size; therefore, any conclusions may be limited in their implications. Second, although the serum TSH level was well controlled, variation still remains in the serum Tg level influenced by the TSH level beyond the measurement limit (>80 mU/l). Third, circulating the ATA may cause false-negative or -positive results in the serum Tg level [11, 13, 26]. Although we observed similar results with the ATA-corrected serum Tg level compared to the measured serum Tg level, the mathematical correction cannot replace the true serum Tg level. Fourth, in WBS, the scanning time and treatment dose, which can cause variation in the radioiodine uptake, were not fully controlled. However, we tried to minimize the variation using background brain activity when determining the RSI, and the change of radioiodine activity in 4–6 days is less remarkable than that in 0–4 days [27, 28]. The last limitation is that neither the serum Tg level nor radioiodine WBS can accurately predict the ‘true’ metastatic tumor burden. Although the radioiodine WBS is the most specific imaging method to diagnose recurrence or distant metastasis of DTC, less or dedifferentiated thyroid carcinoma may lose the ability to concentrate radioiodine. The serum Tg level also depends on the capacity of the tumor to respond to TSH stimulation and the ability of the tumor to synthesize and release immunologically active Tg [29]. Hook effects arise when an excessive amount of Tg in the specimen overwhelms the antibody test reagent, also causing false-negative Tg results [13]. The dedifferentiated cancer cells that can still concentrate iodine can lose the ability to synthesize or release Tg [13]. This limitation is inherent to most other studies attempting to evaluate the radioiodine uptake and serum Tg level as an indicator reflecting tumor burden in patients with metastatic DTC.
Conclusions
Use of the radioiodine scan index derived from conventional WBS is feasible to reflect the serum Tg level in patients with metastatic DTC, and it may be useful to predict the biologic treatment response after radioiodine treatment. More controlled study in a uniform clinical setting, such as a protocol using recombinant human TSH, is needed to validate the usefulness of the simplified quantitative index in radioiodine WBS.
References
Cho BY, Choi HS, Park YJ, Lim JA, Ahn HY, Lee EK, et al. Changes in the clinicopathological characteristics and outcomes of thyroid cancer in Korea over the past four decades. Thyroid. 2013;23:797–804.
Siegel R, Naishadham D, Jemal A. Cancer statistics, 2013. CA Cancer J Clin. 2013;63:11–30.
Chen AY, Jemal A, Ward EM. Increasing incidence of differentiated thyroid cancer in the United States, 1988–2005. Cancer. 2009;115:3801–7.
Durante C, Haddy N, Baudin E, Leboulleux S, Hartl D, Travagli JP, et al. Long-term outcome of 444 patients with distant metastases from papillary and follicular thyroid carcinoma: benefits and limits of radioiodine therapy. J Clin Endocrinol Metab. 2006;91:2892–9.
Jonklaas J, Sarlis NJ, Litofsky D, Ain KB, Bigos ST, Brierley JD, et al. Outcomes of patients with differentiated thyroid carcinoma following initial therapy. Thyroid. 2006;16:1229–42.
Wada N, Nakayama H, Suganuma N, Masudo Y, Rino Y, Masuda M, et al. Prognostic value of the sixth edition AJCC/UICC TNM classification for differentiated thyroid carcinoma with extrathyroid extension. J Clin Endocrinol Metab. 2007;92:215–8.
Cooper DS, Doherty GM, Haugen BR, Kloos RT, Lee SL, Mandel SJ, et al. Revised American Thyroid Association management guidelines for patients with thyroid nodules and differentiated thyroid cancer. Thyroid. 2009;19:1167–214.
Kim DH, Jung JH, Son SH, Kim CY, Hong CM, Jeong SY, et al. Difference of clinical and radiological characteristics according to radioiodine avidity in pulmonary metastases of differentiated thyroid cancer. Nucl Med Mol Imaging. 2014;48:55–62.
Min JJ, Chung JK, Lee YJ, Jeong JM, Lee DS, Jang JJ, et al. Relationship between expression of the sodium/iodide symporter and 131I uptake in recurrent lesions of differentiated thyroid carcinoma. Eur J Nucl Med. 2001;28:639–45.
Hanscheid H, Lassmann M, Luster M, Thomas SR, Pacini F, Ceccarelli C, et al. Iodine biokinetics and dosimetry in radioiodine therapy of thyroid cancer: procedures and results of a prospective international controlled study of ablation after rhTSH or hormone withdrawal. J Nucl Med. 2006;47:648–54.
Ahn BC, Lee WK, Jeong SY, Lee SW, Lee J. Estimation of true serum thyroglobulin concentration using simultaneous measurement of serum antithyroglobulin antibody. Int J Endocrinol. 2013;2013:210639.
Johansen K, Woodhouse NJ. Comparison of thyroglobulin and radioiodine scintigraphy during follow-up of patients with differentiated thyroid carcinoma. Eur J Med. 1992;1:403–6.
Ma C, Kuang A, Xie J, Ma T. Possible explanations for patients with discordant findings of serum thyroglobulin and 131I whole-body scanning. J Nucl Med. 2005;46:1473–80.
Kim HJ, Lee JI, Kim NK, Min YK, Kim SW, Chung JH. Prognostic implications of radioiodine avidity and serum thyroglobulin in differentiated thyroid carcinoma with distant metastasis. World J Surg. 2013;37:2845–52.
Bernier MO, Leenhardt L, Hoang C, Aurengo A, Mary JY, Menegaux F, et al. Survival and therapeutic modalities in patients with bone metastases of differentiated thyroid carcinomas. J Clin Endocrinol Metab. 2001;86:1568–73.
Casara D, Rubello D, Saladini G, Masarotto G, Favero A, Girelli ME, et al. Different features of pulmonary metastases in differentiated thyroid cancer: natural history and multivariate statistical analysis of prognostic variables. J Nucl Med. 1993;34:1626–31.
Lassmann M, Hanscheid H, Verburg FA, Luster M. The use of dosimetry in the treatment of differentiated thyroid cancer. Q J Nucl Med Mol Imaging. 2011;55:107–15.
Luster M, Hanscheid H, Freudenberg LS, Verburg FA. Radioiodine therapy of metastatic lesions of differentiated thyroid cancer. J Endocrinol Invest. 2012;35:21–9.
Lind P, Kohlfurst S. Respective roles of thyroglobulin, radioiodine imaging, and positron emission tomography in the assessment of thyroid cancer. Semin Nucl Med. 2006;36:194–205.
Karam M, Gianoukakis A, Feustel PJ, Cheema A, Postal ES, Cooper JA. Influence of diagnostic and therapeutic doses on thyroid remnant ablation rates. Nucl Med Commun. 2003;24:489–95.
Salvatori M, Raffaelli M, Castaldi P, Treglia G, Rufini V, Perotti G, et al. Evaluation of the surgical completeness after total thyroidectomy for differentiated thyroid carcinoma. Eur J Surg Oncol. 2007;33:648–54.
Rosario PW, Maia FF, Cardoso LD, Barroso A, Rezende L, Padrao EL, et al. Correlation between cervical uptake and results of postsurgical radioiodine ablation in patients with thyroid carcinoma. Clin Nucl Med. 2004;29:358–61.
Im HJ, do Koo H, Paeng JC, Lee KE, Chung YS, Lim I, et al. Evaluation of surgical completeness in endoscopic thyroidectomy compared with open thyroidectomy with regard to remnant ablation. Clin Nucl Med. 2012;37:148–51.
Hurst EW, Davies OL. Studies on the blood–brain barrier. II. Attempts to influence the passage of substances into the brain. Br J Pharmacol Chemother. 1950;5:147–64.
Misaki T, Iwata M, Kasagi K, Konishi J. Brain metastasis from differentiated thyroid cancer in patients treated with radioiodine for bone and lung lesions. Ann Nucl Med. 2000;14:111–4.
Ahn BC, Seo JH, Bae JH, Jeong SY, Yoo J, Jung JH, et al. Effects of anti-thyroglobulin antibody on the measurement of thyroglobulin: differences between immunoradiometric assay kits available. Nucl Med Mol Imaging. 2005;39:252–6.
Furhang EE, Larson SM, Buranapong P, Humm JL. Thyroid cancer dosimetry using clearance fitting. J Nucl Med. 1999;40:131–6.
Tabei F, Neshandar Asli I, Azizmohammadi Z, Javadi H, Assadi M. Assessment of radioiodine clearance in patients with differentiated thyroid cancer. Radiat Prot Dosimetry. 2012;152:323–7.
Torrens JI, Burch HB. Serum thyroglobulin measurement. Utility in clinical practice. Endocrinol Metab Clin N Am. 2001;30:429–67.
Disclosure
Conflict of interest
Jong-Ryool Oh, Byeong-Cheol Ahn, Shin Young Jeong, Sang-Woo Lee and Jaetae Lee declare that they have no conflict of interest.
Informed Consent
All procedures followed were in accordance with the ethical standards of the responsible committee on human experimentation and with the Helsinki Declaration of 1975, as revised in 2000. Informed consent was obtained from all patients for being included in the study. Additional informed consent was obtained from all patients for which identifying information is included in this article.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Oh, JR., Ahn, BC., Jeong, S.Y. et al. Radioiodine Scan Index: A Simplified, Quantitative Treatment Response Parameter for Metastatic Thyroid Carcinoma. Nucl Med Mol Imaging 49, 174–181 (2015). https://doi.org/10.1007/s13139-015-0335-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s13139-015-0335-3