Abstract
The persistence of the median artery in adult life, a remnant of the early brachial artery in the embryonic stage, has been reported in many anatomical and clinical studies. Herein, we aimed to investigate the prevalence and origin of the median artery in cadavers. We examined 53 adult Japanese cadavers and carefully dissected 106 upper limbs, and the arterial systems in the forearms and hands were observed macroscopically. We found the palmar type of the median artery on 106 sides in 53 cadavers, and found that it passes through the carpal tunnel and forms the superficial palmar arch in the hand in only two cadavers. The antebrachial type, ending in the forearm before reaching the wrist joint, was detected on 63 sides in 44 cadavers. The proportions of the origins of the median artery examined in this study were as follows: originating from the common interosseous artery (CIA) on 15 sides (23%), anterior interosseous artery (AIA) on 9 sides (14%), ulnar artery (UA) on 16 sides (24%), and CIA–UA trunk on 26 sides (39%). None arose from other arteries in the upper limbs. Based on our results and the current theory on vascular development, we conclude that the term ‘persistent median artery’ must be strictly used for the one that arises from the arteries in the forearm except for the radial artery, and the presence of this ontogenetic remnant can be interpreted as paedogenesis in the human body. We also describe that the increasing trend in the incidence of the median artery since the nineteenth century, as pointed out by a few researchers, may represent ‘nearly neutral evolution’ at the phenotypic level in human populations.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Heterochrony—changes in the timing or rates of the development of morphological traits or both during ontogeny—is a significant concept in developmental and evolutionary biology, with the increased and decreased degrees of development called ‘paramorphosis’ and ‘paedomorphosis’, respectively (Reilly et al. 1997; McNamara 2012). Both the ‘paramorphic’ and ‘paedomorphic’ processes occurring during ontogeny seem to have been involved in the evolution of human traits (Bufill et al. 2011), and paedomorphic traits, defined under the term ‘neoteny’, have been detected in the human body in previous studies (Shea 1989; Godfrey and Sutherland 1996; Somel et al. 2009).
The ‘persistent median artery’, a remnant of the early brachial artery in embryonic life, has been reported to be present in the human forearm by several studies (Adachi 1928; Henneberg and George 1992a; Aragão et al. 2017). In the forearm, the brachial artery branches at the elbow joint into the ulnar artery (UA) and radial artery, which anastomose in the hand to form the superficial and deep palmar arches, and the common interosseous artery (CIA), including the anterior and posterior interosseous arteries, branches from the UA. The persistent median artery is occasionally found as an extra artery originating from one of these arteries in the forearm and running parallel to the median line of the forearm. This artery mostly disappears proximal to the carpal tunnel but rarely passes through the carpal tunnel and joins the palmar arch. A few previous researchers investigated or reviewed the anatomical characteristics of the persistent median artery, i.e. its origin, course, and prevalence, but most of their observations have been inconclusive and remain disputed (Rodríguez-Niedenführ et al. 1999; Kodama 2000; Solewski et al. 2021). Several researchers have traditionally identified this extra artery running parallel to the median line of the forearm as the persistent median artery without considering its developmental homologue and the process underlying its development (Henneberg and George 1992a; Matsunaga et al. 2001; Elhossiny et al. 2023). Therefore, in this study, we first describe the persistent median artery based on our macroscopic results, and then discuss its significance in developmental biology and human evolution.
Materials and methods
In the present study, we examined 53 adult Japanese cadavers (32 males and 21 females, aged: 50–100 years). We carefully dissected 106 upper limbs (right: 53, left: 53), and the arterial systems in the forearms and hands were observed macroscopically. Initially, the presence of the median artery was assessed and then its origin and termination were investigated. The cadavers were embalmed with an aqueous solution of 3.7% formaldehyde and 34.0% ethanol. None of the upper limbs showed evidence of previous surgical procedures or trauma to the examined region. The definitions of the two morphotypes of the median artery are as follows: the median artery passing through the carpal tunnel is a ‘palmar type’, and the one ending before reaching the wrist joint is an ‘antebrachial type’ (Rodríguez-Niedenführ et al. 1999).
Results
The prevalence of the persistent median artery in the forearm, recorded in this study, is listed in Table 1. A total of 66 median arteries (right: 31, left: 35) were found in 44 cadavers (25 males and 19 females) in their examined upper limbs (Table 2). The arteries were bilateral in 22 cadavers and unilateral in 22 cadavers (9 on the right and 13 on the left). The cadavers under examination did not exhibit co-variants in muscles, related nerves, and other arterial variants. The median arteries found in this study were located beneath the flexor digitorum superficialis and ran parallel to the median nerve (Figs. 1 and 2). These median arteries nourished the flexor digitorum superficialis (n = 38), flexor digitorum profundus (n = 7), pronator teres (n = 7), flexor pollicis longus muscle (n = 2), palmaris longus muscle (n = 2), and the median nerve (n = 16). We found no median artery penetrating the anterior interosseous or median nerve (Matsunaga et al. 2001; Buch et al. 2019).
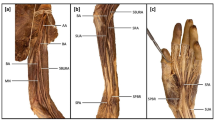
Palmar type of the persistent median artery (MA). (a) The whole image of the palmar type. (b) Image depicting the origin of the MA. (c) Image showing the superficial palmar arterial arch (SPA), continuous with the MA. Asterisks show the flexor retinaculum, which is opened and excised. Black and white arrowheads represent the paths of the MA and median nerve (MN), respectively. AIA anterior interosseous artery, AIN anterior interosseous nerve, BA brachial artery, CIA common interosseous artery, FDS flexor digitorum superficialis, FPL flexor pollicis longus, PIA posterior interosseous artery, RA radial artery, UA ulnar artery
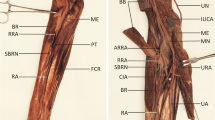
Various origins of the antebrachial type of the persistent median artery (MA). (a) Image depicting the MA originating from the anterior interosseous artery (AIA). (b) Image showing the MA originating from the common interosseous artery (CIA). (c) An image of the MA, originating from the ulnar artery (UA). Asterisks show the terminal part of the MA. Arrowheads represent the path of the MA. The arrow in (c) indicates the branching point between the AIA and posterior interosseous artery (PIA). The image of the antebrachial type originating from the CIA–UA trunk is not shown. AIN anterior interosseous nerve, BA brachial artery, FDS flexor digitorum superficialis, MN median nerve, PT pronator teres, RA radial artery
Only two cadavers revealed the presence of the palmar type of the median artery (Fig. 1 and Table 2). The median artery arose from the CIA–UA trunk (branching point between the CIA and UA) bilaterally in the male cadaver and originated from the UA only on the right side of the female cadaver. These arteries run parallel to the median nerve and pass through the carpal tunnels. Finally, these arteries merged with the UA to form the superficial palmar arterial arch in both cadavers.
The remaining 63 median arteries were of the antebrachial type (Fig. 2 and Table 2). The origins of these median arteries varied, although all arteries ran parallel to the median nerve and penetrated neither the median nor the anterior interosseous nerve. The antebrachial types identified in this study arose from the CIA (n = 15), AIA (n = 9), UA (n = 16), and CIA–UA trunk (n = 26) (Table 3). The median arteries terminate irregularly in each forearm.
Discussion
Definition of the ‘persistent median artery’ as the ontogenetic remnant
A persistent median artery has been reported by many previous researchers who have described the presence, course, size or variations of the median artery (Adachi 1928; Henneberg and George 1992a, b; Sañudo et al. 1994; Kopuz et al. 1995; George and Henneberg 1996; Mansor et al. 1999; Rodríguez-Niedenführ et al. 1999; Kodama 2000; Matsunaga et al. 2001; D’Costa et al. 2006; Tsuruo et al. 2006; Arifoğlu et al. 2008; Claassen et al. 2008; Natsis et al. 2009; Eid et al. 2011; Jelev and Georgiev 2011; Potu et al. 2011; Singla et al. 2012; Agarwal et al. 2013; Klimek-Piotrowska et al. 2013; Ariyo and Shea 2016; Patnaik and Paul 2016; Cheruiyot et al. 2017; Carry et al. 2018; Haładaj et al. 2019; Alexander et al. 2020; Elhossiny et al. 2023). However, most of these findings remain disputed, and there is little consensus regarding this anomalous artery. Plausible knowledge regarding the median artery based on the results of previous studies includes the following: (1) the median artery is the remnant of the antebrachial artery of the foetuses (Singer 1933; Rodríguez-Niedenführ et al. 2001); (2) the palmar and antebrachial morphotypes, which differ in terms of whether they pass through the carpal tunnel, have been described, and the prevalence of the former is lower than that of latter (Huelin et al. 1979; Srivastava and Pande 1990; Rodríguez-Niedenführ et al. 1999; Solewski et al. 2021); and (3) the prevalence of the median artery in foetuses or neonates is higher than that in adults (Kopuz et al. 1997; Aragão et al. 2017; Solewski et al. 2021). Most previous researchers have sporadically reported an extra artery running parallel to the median nerve in the forearm as the ‘persistent median artery’; therefore, we had no way to confirm the developmental homologue of this anomaly artery, which is one of the reasons why we faced some difficulties in elucidating the process underlying the persistence of the median artery.
The prevalence of the palmar type is significantly lower than that of the antebrachial type (Table 1). The origins of the median artery are varied (Table 2), including from the CIA (22.7%), AIA (13.6%), UA (24.2%), and CIA–UA trunk (39.3%); however, we found no cadaver with the median artery arising from the radial or brachial artery, which was reported by previous studies (Nakane and Igawa 1955; Henneberg and George 1992a; Wood et al. 1997; Rodríguez-Niedenführ et al. 1999; Elhossiny et al. 2023). The prevalence rate of the median artery arising from the radial artery is much lower than that of those with other origins (Table 3), and this type of median artery has rarely been reported hitherto (Matsunaga et al. 2001; Tsuruo et al. 2006; Natsis et al. 2009; Patnaik and Paul 2016; Aragão et al. 2017). Our results reveal that most median arteries originate from the interosseous or ulnar artery and end proximal to the wrist joint. In contrast, the palmar type of the median artery and the median artery originating from the radial artery are extremely rare. Hence, we can consider the two morphotypes of the median artery to represent the degree of regression of the artery during ontogeny, because the median artery is usually fused with the interosseous or ulnar artery at an early embryonic stage. Therefore, we propose that the ‘persistent median artery’ is the remnant of the early brachial artery (Fig. 3), and the ‘persistent median artery’ reported in some previous studies should be excluded because it is not the remnant of the median artery in the early embryonic stage. The current theory, widely accepted in textbooks, attributes the vascular development of the upper limb to sprouting angiogenesis (Singer 1933; DeSesso 2017). First, vascular development begins at stage 12 (embryonic day 26) and the capillary plexus appears in the limb bud. Then, the AIA (with a branch forming the posterior interosseous artery) exists as the main axial artery in the limb, terminating in the capillary plexus (Hubmer et al. 2004). In later stages, the median artery branched from the main brachial artery and became the main artery of the forearm (Fig. 3a). In the subsequent stages, the UA arises via sprouting angiogenesis (Fig. 3b), and the radial artery begins to arise from the brachial artery (Fig. 3c). Finally, the ulnar and radial arteries become dominant, forming the superficial and deep palmar arches in the hand region, whereas, the median artery undergoes partial or complete regression (Fig. 3d). We can describe the ‘persistent median artery’ as a remnant of partial regression, branched from the various antebrachial origins, i.e. the AIA (Fig. 3a-1, b-1, c-1, d-1), CIA (Fig. 3a-2, b-2, c-2, d-2), CIA–UA trunk (Fig. 3a-2, b-3, c-3, d-3), and UA (Fig. 3a-2, b-4, c-4, d-4). Herein, we propose that the median artery branching from the radial artery is not a remnant of regression because it is unfeasible for the median artery to originate from the radial artery during normal vascular development (Fig. 4). If the persistent median artery branches from the radial artery, at least three mutations must have occurred during ontogeny (Fig. 4a-1, a-2, a-3, a-4). However, if the medial branch of the radial artery has been misidentified as a persistent median artery, only one mutation is required (Fig. 4b-1, b-2, b-3, b-4). Another theory regarding the vascular development of the upper limb proposed by Rodríguez-Niedenführ et al. (2001) claims that the arterial pattern of the upper limb develops from an initial capillary plexus via the enlargement and differentiation of selected parts. The theory further states that the median artery is one of the early main vessels in the limb bud, and the radial artery is the main artery formed later, implying that regardless of the validity of these theories, our explanation is reasonable. Additionally, the persistent median artery originating from the radial artery, as reported in previous studies (Henneberg and George 1992a; Wood et al. 1997; Rodríguez-Niedenführ et al. 1999; Elhossiny et al. 2023), has the following common features: (1) its prevalence rate is much lower than that of those having other origins; (2) it runs in the superficial muscle layer of the forearm (superficial to the flexor digitorum superficialis); and (3) it joins the palmar arch, and its antebrachial type has never been found. These findings support our hypothesis that the persistent median artery branching from the radial artery is not the true ‘persistent median artery’. Therefore, we must use the term ‘persistent median artery’, implying the remnant of the early main artery in the upper limb, for the median arteries originating from the arteries of the forearm except for the radial artery, as the medial branch of the radial artery is likely to have been misidentified as the median artery.
Ontogenetic development of the persistent median artery (MA) with different origins. Drawings of the forearm (MA drawn in red), modified from DeSesso (2017). (a) Drawings depicting the initiation of the MA formation. (b) Drawings showing the MA, continuous with the coalescence of capillaries in the limb bud, and then the ulnar artery (UA) emerges. (c) Drawings of the UA merging with the coalescence of capillaries and the MA, while the radial artery (RA) begins to be formed. (d) As the development proceeds, the MA and anterior interosseous artery (AIA) regress. On the contrary, the RA and UA merge with the capillary plexus in the hand and form the palmar arterial arch. CIA common interosseous artery, PIA posterior interosseous artery
Drawings of presumed model regarding the ontogenetic process of the persistent median artery (MA; drawn in red) originating from the radial artery (RA), reported by the previous studies. (a) Drawings depicting the case of the persistent MA originating from the RA. (b) Drawings showing the case of branched RA. AIA anterior interosseous artery, CIA common interosseous artery, PIA posterior interosseous artery, UA ulnar artery
Evolutionary trend regarding the persistent median artery
Many previous studies have traditionally considered that the median artery in adults is formed by the regression of the median artery present in the early stage of ontogeny (Henneberg and George 1992a; Rodríguez-Niedenführ et al. 1999). Several studies have provided the following evidence to support this idea: (1) the median artery is the transitory vessel representing the arterial axis of the human forearm during the early embryonic stage (Singer 1933; Rodríguez-Niedenführ et al. 2001), (2) the prevalence of this artery in foetuses is higher than that in adults (Kopuz et al. 1997; Aragão et al. 2017; Solewski et al. 2021), and (3) the median artery may continue to regress progressively even after birth because of the probability of its regression by 4.4% every 1-year (Carry et al. 2018). The two morphotypes (the palmar and antebrachial types) of the median artery have been reported previously (Rodríguez-Niedenführ et al. 1999; Kodama 2000; Matsunaga et al. 2001; Solewski et al. 2021). In this study, we found both morphotypes (Figs. 1 and 2) and that the morphology of the antebrachial type is irregular (Fig. 2). The different morphologies of the antebrachial type, which terminated around the wrist joint, midpoint of the forearm, or elbow joint, are thought to represent the degree of regression of the median artery during ontogeny, indicating that the persistent median artery is not a simple vestigial organ in the human body. Therefore, the ‘persistent median artery’ is undoubtedly a remnant of the median artery in embryonic life, with its two morphotypes, including the antebrachial type with unstable length, indicating that the morphological differences in this artery are caused by the degree of its regression during ontogeny. Additionally, the prevalence of the persistent median artery, including the palmar and antebrachial types, maintains a certain percentage within human populations (Table 3). These findings indicate that the persistence of the median artery can be interpreted as paedogenesis, an intraspecific heterochrony generated owing to the truncated development (Reilly et al. 1997) of the arterial system in the forearm (Fig. 5).
Paedogenesis of the arterial system in the human forearm. The morphotypes of the persistent median artery (MA; drawn in red) are formed owing to the differences in the degree of the regression of the median artery, and their formation is interpreted as the paedogenesis of arterial systems in the forearm. AIA anterior interosseous artery, CIA common interosseous artery, PIA posterior interosseous artery, RA radial artery, UA ulnar artery
Several researchers have indicated that the prevalence of this phenomenon has been increasing in human populations since the nineteenth century. Henneberg and George (1995) reported a twofold increase in the presence of a median artery in Southern Africa from 1900 to 1990. Lucas et al. (2020) reviewed previous studies on the median artery and statistically analysed its prevalence since the nineteenth century. They concluded that the prevalence of the persistent median artery increased over time, from approximately 10% in people born at the end of the nineteenth century to approximately 30% by the end of the twentieth century. They further concluded that this morphological trend represents a microevolutionary change in the internal anatomy of the human body caused by damage to a specific gene that regulates the regression of the persistent median artery. If their hypothesis is correct, the paedogenesis of the persistent median artery contributes to the morphological evolution of the antebrachial artery system in the human body. They assumed the causes of the prevalence of the persistent median artery to be either of the following: (1) an environmental insult around the foetus caused by the healthcare for the mother or (2) mutations damaging the genes regulating the regression of the median artery. They favoured the former and attributed the increase in the prevalence of the persistent median artery to the improvement in healthcare provided to pregnant women globally over the last 125 years. If this explanation is valid, the increasing trend of the prevalence of the persistent median artery is not ‘biological evolution’ but must be categorised as ‘environmental variation’ or ‘hereditary disease (if the germ cells are also damaged)’. The latter explanation is that mutation/natural selection pressures may cause this trend regarding the persistent median artery; however, they did not explain the pressures concretely. We believe it is impossible to describe this evolutionary trend to be based on natural selection because the persistent median artery renders almost no benefit toward increasing the ‘fitness’ of individuals but carries a small risk of causing carpal tunnel syndrome (Maxwell et al. 1973; Lisanti et al. 1995; Kele et al. 2002; Bilgin et al. 2004; Osiak et al. 2021; Townsend et al. 2022). However, these findings imply that the persistent median artery is a mildly detrimental mutation for humans; therefore, this evolutionary trend of the median artery may be interpreted as an example of the ‘nearly neutral evolution’ at the phenotypic level. In this case, the prevalence of the persistent median artery must have been increased by genetic drift, although there is no evidence that genetic drift is working in the examined populations. However, previous studies have provided little information.
Townsend et al. (2022) reported a high prevalence rate of persistent median arteries in patients with carpal tunnel release, concluding that their results coincide with the microevolutionary change reported by Lucas et al. (2020) compared with the results of similar previous studies in living patients. However, they mentioned that their cohort comprised patients from a limited region; therefore, the possibility that the prevalence of the persistent median artery could vary between different races or populations remains. Solewski et al. (2021) investigated the prevalence and anatomical characteristics of the median artery by reviewing the literature, detecting a higher prevalence of the palmar type in a few regions, such as South Africa, Brazil and South America, than in others. Other studies have reported that the palmar type is also highly prevalent (> 10%) in Kenya, Great Britain, Israel, Malaysia, and India (Pecket et al. 1973; Mansor et al. 1999; Rodríguez-Niedenführ et al. 1999; Nayak et al. 2010; Cheruiyot et al. 2017). These results indicate a high prevalence of the persistent median artery worldwide and suggest that the frequency of this mutation increases within a local population. Generally, as the size of the population decreases, genetic drift affects the gene pool in the population relatively more strongly; therefore, we presume that the persistent median artery is spreading in the local population in specific regions. Alternatively, the increasing trend of the prevalence of the persistent median artery since the end of the nineteenth century may be attributed to the advances in our anatomical knowledge and techniques. To negate this possibility, we need to conduct further research, continued for a long time in a specific region, regarding the prevalence of the persistent median artery in a particular racial group.
Other important factors affecting the prevalence of the persistent median artery could be the differences among human races or living environments (Townsend et al. 2022), as these are closely associated with the characteristics of local populations. Henneberg and George (1992a, b) reported no differences in the prevalence of this artery between white and black people living in southern Africa; however, Carry et al. (2018) concluded that the prevalence of this artery is significantly different between African American and non-African American racial groups. These findings remain disputed; therefore, a comprehensive study with substantial results is needed.
Conclusions
The persistent median artery is the remnant of the main brachial artery in embryonic life and usually originates from the CIA, AIA, UA, and CIA–UA trunk. The presence of this artery results from the paedogenesis of the antebrachial arterial system. The increasing trend of the prevalence of the persistent median artery in human populations, as reported in previous studies, may be interpreted as ‘nearly neutral evolution’ at the phenotypic level.
Data availability
The data that support the findings of this study are available from the corresponding author, S.Y., upon reasonable request.
References
Adachi B (1928) Das Arteriensystem der Japaner, vol 1. Maruzen, Kyoto, pp 285–356
Agarwal KK, Saxena A, Soni S, Das AR (2013) Persistent median artery: a sign of primitive arterial pattern. OA Case Rep 15:128
Alexander JG, Leal MC, Baptista JS (2020) Persistent median artery inside the carpal tunnel: description and surgical implications. Autopsy Case Rep 10:e2020209
Aragão JA, da Silva AC, Anunciação CB, Reis FP (2017) Median artery of the forearm in human fetuses in northeastern Brazil: anatomical study and review of the literature. Anat Sci Int 92:107–111
Arifoğlu Y, Sevinç Ö, Barut Ç, İş M, Dıramalı M (2008) Persistent median artery: case report and review of the literature. J Nerv Syst Surg 1:195–199
Ariyo O, Shea J (2016) Bilateral triad of persistent median artery, a bifid median nerve and high origin of its palmar cutaneous branch. A case report and clinical implications. Int J Morphol 34:997–1001
Bilgin SS, Olcay SE, Derincek A, Adiyaman S, Demirtas AM (2004) Can simple release relieve symptoms of carpal tunnel syndrome caused by a persistent median artery? Arch Orthop Trauma Surg 124:154–156
Buch C, Devora CM, Johnson LY, Rahimi OB, Kar R (2019) Incomplete superficial palmar arch and bilateral persistent median artery. Int J Surg Case Rep 58:205–207
Bufill E, Agustí J, Blesa R (2011) Human neoteny revisited: the case of synaptic plasticity. Am J Hum Biol 23:729–739
Carry PM, Nguyen AK, Merritt GR, Ciarallo C, Chatterjee D, Park J, Miller NH, Scott FA (2018) Prevalence of persistent median arteries in the pediatric population on ultrasonography. J Ultrasound Med 37:2235–2242
Cheruiyot I, Bundi B, Munguti J, Olabu B, Ngure B, Ogeng’o J (2017) Prevalence and anatomical patterns of the median artery among adult black Kenyans. Anat J Afr 6:1015–1023
Claassen H, Schmitt O, Wree A (2008) Large patent median arteries and their relation to the superficial palmer arch with respect to history, size consideration and clinic consequences. Surg Radiol Anat 30:57–63
D’Costa S, Narayana K, Narayan P, Nayak SR, Madhan SJ (2006) Occurrence and fate of palmar type of median artery. ANZ J Surg 76:484–487
DeSesso JM (2017) Vascular ontogeny within selected thoracoabdominal organs and the limbs. Reprod Toxicol 70:3–20
Eid N, Ito Y, Shibata MA, Otsuki Y (2011) Persistent median artery cadaveric study and review of the literature. Clin Anat 24:627–633
Elhossiny AH, Bakir M, Dawalibi A, Behiery A (2023) Persistent median artery, bifid median nerve, and reversed palmaris longus encountered during cadaveric dissection: the first reported Case. Cureus 15:e40324
George BJ, Henneberg M (1996) High frequency of the median artery of the forearm in South African newborns and infants. S Afr Med J 86:175–176
Godfrey LR, Sutherland MR (1996) Paradox of peramorphic paedomorphosis: heterochrony and human evolution. Am J Phys Anthropol 99:17–42
Haładaj R, Wysiadecki G, Dudkiewwicz Z, Polguj M, Topol M (2019) Persistent median artery as an unusual finding in the carpal tunnel: its contribution to the blood supply of the hand and clinical significance. Med Sci Monit 25:32–39
Henneberg M, George BJ (1992a) High incidence of the median artery of the forearm in a sample of recent south African Cadavers. J Anat 180:185–188
Henneberg M, George BJ (1992b) A further study of the high incidence of the median artery of the forearm in S Afr. J Anat 181:151–154
Henneberg M, George BJ (1995) Possible secular trend in the incidence of an anatomical variant: median artery of the forearm. Am J Phys Anthropol 96:329–334
Hubmer MG, Fasching T, Haas F, Koch H, Schwarzl F, Weiglein A, Scharnagl E (2004) The posterior interosseous artery in the distal part of the forearm. Is the term ‘recurrent branch of the anterior interosseous artery’ justified? Br Assoc Plastic Surg 57:638–644
Huelin JG, Barreiro FJ, Barcia EC (1979) Etude radio-anatomique de l’artère médiane. Acta Anat 105:250–255
Jelev L, Georgiev GP (2011) A rare case of superficial median artery of high brachial origin: anatomical and clinical considerations of the superficial brachiomedian artery. Anatomy 5:39–43
Kele H, Verheggen R, Reimers CD (2002) Carpal tunnel syndrome caused by thrombosis of the median artery: the importance of high-resolution ultrasonography for diagnosis. J Neurosurg 97:471–473
Klimek-Piotrowska W, Pacholczak R, Walocha J (2013) Multiple variations of the arterial pattern in upper extremities: a case report and embryological pathogenesis. Clin Anat 26:1031–1035
Kodama K (2000) Arteries of the upper limb. In: Sato T, Akita K (eds) University of Tokyo Press, Tokyo, pp 220–237
Kopuz C, Gulman B, Baris S (1995) Persistent median artery: an anatomical study in neonatal and adult cadavers. Acta Anat Nippon 70:577–580
Kopuz C, Baris S, Gulman B (1997) A further morphological study of the persistent median artery in neonatal cadavers. Surg Radiol Anat 19:403–406
Lisanti M, Rosati M, Pardi A (1995) Persistent median artery in carpal tunnel syndrome. Acta Orthop Belg 61:315–318
Lucas T, Kumaratilake J, Henneberg M (2020) Recently increased prevalence of the human median artery of the forearm: a microevolutionary change. J Anat 237:623–631
Mansor O, Kassim Z, Henneberg M (1999) The incidence of the median artery in the forearms of Malaysians. Perspect Hum Biol 4:223–228
Matsunaga K, Matsuzaki A, Myauchi R (2001) Relationship of median artery to median nerve and anterior interosseous nerve. Orthop Traumatol 50:743–749 (in Japanese)
Maxwell JA, Kepes JJ, Ketcheum LD (1973) Acute carpal tunnel syndrome secondary to thrombosis of a persistent median artery: case report. J Neurosurg 38:774–777
McNamara KJ (2012) Heterochrony: the evolution and development. Evol Educ Outreach 5:203–218
Nakane F, Igawa K-I (1955) A rare case of anomalous superficial artery in the upper limb. Sapporo Med J 7:174–176
Natsis K, Iordache G, Gigis I, Kyriazidou A, Lazaridis N, Noussios G, Paraskevas G (2009) Persistent median artery in the carpal tunnel: anatomy, embryology, clinical significance, and review of the literature. Folia Morphol 68:193–200
Nayak SR, Krishnamurthy A, Kumar SM, Prabhu LV, Potu BK, D’Costa S, Ranade AV (2010) Palmar type of median artery as a source of superficial palmar arch: a cadaveric study with its clinical significance. Hand (New York, N.y.) 5:31–36
Osiak K, Elnazir P, Mazurek A, Pasternak A (2021) Prevalence of the persistent median artery in patients undergoing surgical open carpal tunnel release: a case series. Transl Res Anat 23:100113
Patnaik M, Paul S (2016) Persistent median artery of the forearm and palm: a cadaver study into its origin, course, fate and clinical significance. Ital J Anat Embryol 121:88–95
Pecket P, Gloobe H, Nathan H (1973) Variations in the arteries of the median nerve with special consideration on the ischemic factor in the carpal tunnel syndrome (CTS). Clin Orthop Relat Res 97:144–147
Potu BK, Ray B, Pai SR, Bhat KM, Pulakunta T, Sarda R, Mishra S (2011) A preliminary survey of the median artery in human cadavers of South Indian Origin. Bratisl Med J 112:292–295
Reilly SM, Wiley EO, Meinhardt DJ (1997) An integrative approach to heterochrony: the distinction between interspecific and intraspecific phenomena. Biol J Linn Soc 60:119–143
Rodríguez-Niedenführ M, Sañudo JR, Vázquez T, Nearn L, Logan B, Parkin I (1999) Median artery revisited. J Anat 195:57–63
Rodríguez-Niedenführ M, Burton GJ, Sañudo JR (2001) Development of the arterial pattern in the upper limb of staged human embryos: normal development and anatomic variations. J Anat 199:407–417
Sañudo JR, Chikwe J, Evans SE (1994) Anomalous median nerve associated with persistent median artery. J Anat 185:447–451
Shea BT (1989) Heterochrony in human evolution: the case for neoteny reconsidered. Yearb Phys Anthropol 32:69–101
Singer E (1933) Embryological pattern persisting in the arteries of the arm. Anat Rec 55:403–409
Singla RK, Kaur N, Dhiraj GS (2012) Prevalence of the persistent median artery. J Clin Diagn Res 6:1454–1457
Solewski B, Lis M, Pękala JR, Brzegowy K, Lauritzen SS, Hołda MK, Walocha JA, Tomaszewski KA, Pękala PA, Koziej M (2021) The persistent median artery and its vascular patterns: a meta-analysis of 10,394 subjects. Clin Anat 34:1173–1185
Somel M, Franz H, Yan Z, Lorenc A, Guo S, Giger T, Kelso J, Nickel B, Dannemann M, Bahn S, Webster MJ, Weickert CS, Lachmann M, Pääbo S, Khaitovich P (2009) Transcriptional neoteny in the human brain. Proc Natl Acad Sci 106:5743–5748
Srivastava SK, Pande BS (1990) Anomalous pattern of median artery in the forearm of Indians. Acta Anat 138:193–194
Townsend CB, Seigerman D, Aita D, Fletcher D, Gallant G, Jones C, Kwok M, Takei R, Wang M, Beredjiklian P (2022) A prospective evaluation of the prevalence of persistent median artery in patients with carpal tunnel syndrome. Arch Bone Jt Surg 10:756–759
Tsuruo Y, Ueyama T, Ito T, Nanjo S, Gyoubu H, Satoh K, Iida Y, Nakai S (2006) Persistent median artery in the hand: a report with a brief review of the literature. Anat Sci Int 81:242–252
Wood SJ, Abrahams PH, Sañudo JR, Ferreira BJ (1997) Bilateral superficial radial artery at the wrist associated with a radial origin of a unilateral median artery. J Anat 189:691–693
Acknowledgements
The authors would like to express their deep gratitude to the people who donated their bodies for this scientific research. We greatly thank the donors’ families for their cooperation and Ms. Momoko Arai for her excellent office work on the IUHW body donation program. We also thank the two anonymous reviewers for their helpful comments on this manuscript.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Author information
Authors and Affiliations
Contributions
S.Y. carried out the collection and analyzation of the data, writing and editing the original draft. K.K. also collected the data and wrote the original draft. T.I., H.M., H.Y., Y.Ma. and Y.Mo. collected the data. J.K. wrote and edited the original draft. Project administration has been done by K.K. and J.K.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Ethical approval and consent of participation
This study was approved by the Research Ethics Review Committee of the International University of Health and Welfare (IUHW) (23-Im-043). All the donors agreed to donate their bodies to the International University of Health and Welfare for medical education and research in their living will.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Yamada, S., Kawagishi, K., Ishii, T. et al. Persistent median artery: paedogenesis of the antebrachial arterial system in the human body. Anat Sci Int (2024). https://doi.org/10.1007/s12565-024-00799-x
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s12565-024-00799-x