Abstract
Neurotrauma is among the main causes of human disability and mortality. Nerve injury impairs not only neurons but also causes death of satellite glial cells remote from the injury site. We studied the dynamics of expression of different proapoptotic proteins (E2F1, p53, caspase 3) in the dorsal root ganglia (DRG) of a rat after sciatic nerve transection. TUNEL staining and immunoblotting were used for analysis of cell apoptosis and axotomy-induced biochemical changes. Apoptosis of glial cells was observed at 24 h after sciatic nerve transection and increased on day 7, when apoptosis of some neurons only started. The earliest proapoptotic event in the injured DRG was overexpression of transcription factor E2F1 at 4 h after sciatic nerve transection. This preceded the induction of p53 and cleavage of caspase 3 at 24-h post-axotomy. The nerve injury marker amyloid precursor protein and the nerve regeneration marker GAP-43 were overexpressed in DRG on day 7 after sciatic nerve transection. We also developed a novel fluorescence method for differential visualization of the rat DRG and nerves by means of double staining with propidium iodide and Hoechst 33342 that impart red and blue-green fluorescence, respectively. The present experiments showed that glial cells remote from the nerve transection site were more vulnerable to axotomy than DRG neurons. E2F1 and p53 may be considered promising molecular targets for development of potential neuroprotective agents.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neurotrauma is among the main causes of human disability and mortality, especially for young and middle age men. Peripheral nerve injury accounts about 10% cases of neurotrauma. Unfortunately, clinically effective neuroprotectors that can rescue the damaged neurons are absent yet (Hill 2016; Laskowitz and Grant 2016; Witiw and Fehlings 2015). In the central nervous system, the injured neurons do not regenerate and die. However, in the peripheral nervous system, a significant fraction of motor and sensory neurons (about 30%) survive axotomy, regenerate, and restore nerve connections (Dubový et al. 2018; Hill 2016; Patodia and Raivich 2012; Rishal and Fainzilber 2014). Severe nerve injury such as complete nerve transection, i.e., axotomy leads to either necrosis or apoptosis. The previous studies showed that dozens of cellular proteins are up- or downregulated in the axotomized neurons of invertebrate and vertebrate animals (Casas et al. 2015; Demyanenko et al. 2019; Melle et al. 2009; Mulder et al. 2007; Perlson et al. 2004). Nevertheless, the signaling pathways and most reactive target proteins that mediate cell survival or death are not well known.
The sciatic nerve transection (SNT) in rodents is a popular experimental model of neurotrauma. Its advantages include good nerve accessibility for surgical dissection and moderate animal stress (Savastano et al. 2014). The sciatic nerve contains neurites of sensory, somatic, and motor neurons. The bodies of motor neurons are located inside the vertebrae in the spinal cord, whereas the bodies of sensory neurons form the dorsal root ganglia (DRG) outside the spine. The sensory nerve fibers transmit the information on animal position and movements, on mechanical and thermal damage, and on pain to the central nervous system.
The life and functioning of neurons depends on surrounding glial cells. Satellite glial cells support the neuronal metabolism and protect neurons from the damaging and pathogenic influences (Faulkner et al. 2004; Liu et al. 2017; Verkhratsky et al. 2019). On the other hand, neurons maintain survival of surrounding glial cells (Kolosov and Uzdensky 2006). It was shown recently that axotomy induces death not only neurons and glial cells located in the vicinity of the transection site but also glial cells remote from the damaged region (Berezhnaya et al. 2017; Khaitin et al. 2015, 2018; Uzdensky 2018).
In the present work, we studied apoptosis of the sensory neurons and satellite glial cells in the rat DRG after transection of the sciatic nerve. Importantly, apoptosis was observed in the glial cells located distantly from the site of sciatic nerve transection and much earlier than in the neurons. We investigated the post-SNT dynamics of the expression of proapoptotic transcription factors p53 and E2F1, caspase 3 and its active form, neuron degeneration marker APP (amyloid precursor protein), and a marker of the post-traumatic nerve regeneration GAP-43 (growth-associated protein-43) in the DRG of a rat. We also developed the novel method of differential visualization of the rat ganglia and nerve fibers using double labelling with propidium iodide and Hoechst 33342, which imparts red and green fluorescence, respectively.
Materials and Methods
Animals and Ethical Approvement
The experiments were carried out on adult Wistar male rats (200–250 g) that were kept in standard cages in groups of 4–5 animals with free access to food and water. The animal holding room was maintained in standard conditions: 12 light/12 dark cycle, 22–25 °C, and an air exchange rate of 18 changes per hour. All applicable international, national, and/or institutional guidelines for the care and use of animals were followed. The experimental procedures were carried out in accordance with the European Union guidelines 86/609/ЕЕС for the use of experimental animals and local legislation for ethics of experiments on animals. The animal protocols were evaluated and approved by the Animal Care and Use Committee of the Southern Federal University (Approval No 08/2016). No special randomization was performed to allocate subjects in the study.
Sciatic Nerve Transection
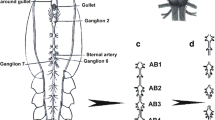
The rat dorsal root ganglia (Fig. 1) contain bodies of sensory neurons. Their neurites are included into the sciatic nerve that innervates the hind limb. General anesthesia of animals was carried out using the intramuscular injection of 0.75 ml of the 2:1 mixture of Xyla (2% xylazine hydrochloride solution; produced by Interchemie Werken “de Adelaar” BV, the Netherlands) and Telazol (a mixture of tiletamine hydrochloride and zolazepam hydrochloride; produced by Zoetis, USA). The sciatic nerve transection was performed according to the protocol described by Savastano et al. (2014). Decapitation of anesthetized rats was performed using a guillotine at 1, 4, and 24 h or 7 days after the unilateral transection of the right sciatic nerve. The undamaged contralateral (left) DRG was used as a control.
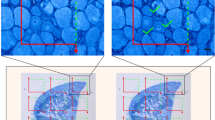
An isolated rat dorsal root ganglion labeled with propidium iodide and Hoechst 33342, which visualize the neuronal bodies (n, red fluorescence) and nerves (N, blue-green fluorescence), respectively. The nuclei of numerous satellite glial cells that surround neurons fluoresce in blue. a Objective lens 10×. b Objective lens 40×. Small arrowhead, neuronal nucleolus; big arrowhead, neuronal nucleus. Scale bar 1 mm on a, 30 μm on b, and 15 μm in the inset
DRG Visualization
The right DRGs of the 4th and 5th lumbar nerves were isolated at different time intervals after sciatic nerve transection and decapitation of the anesthetized rat, as described by Savastano et al. (2014). Isolated ganglia were fixed for 6 h by 4% paraformaldehyde dissolved in phosphate buffer (PBS; pH 7.2). They were triple washed by PBS and placed in a 30% sucrose solution. The fixed ganglia were then immersed in 7% agarose gel (low-melting agarose, Sigma-Aldrich) and sectioned on the vibratome Leica VT 1000 S (Leica Biosystems, Germany). The thickness of the sections was about 30 μm.
To visualize the DRG cells (Fig. 1), the fixed 30-μm sections were incubated 2 min with propidium iodide (20 μM) and Hoechst 33342 (20 μM) and triple washed in PBS at room temperature. The sections were then immersed in glycerol under cover glass and examined on the fluorescence microscope AxioLab A1 (Carl Zeiss, Germany).
Cell Death Visualization
Apoptosis was determined using the “In Situ Cell Death Detection Kit, TMR red” (Sigma-Aldrich), in which single-strand DNA breaks are marked by the TUNEL method (Transferase-mediated dUTP Nick-End Labeling). The reagent mixture was prepared ex tempore and kept on ice. The fixed sections were transferred onto a glass slide and, after triple washing in PBS, were permeabilized by 2-min incubation with 0.1% sodium citrate supplemented by 0.1% Triton X-100 at 4 °C. After following double washing in PBS and drying, 50 μl of the TUNEL mixture was added to each sample and incubated 60 min in the dark in a humid chamber at 37 °C. Then the samples were triple washed in PBS, dried, and mounted in glycerol. Positive control: 10-min incubation of the permeabilized sections with nuclease benzonase, which makes numerous DNA breaks that are detected by the TUNEL staining (1500 U/ml in 50 mM Tris-HCl buffer, pH 7.5) (Fig. 2a). The sections were counterstained with Hoechst 33342 that imparts blue fluorescence to the nuclear chromatin and reveals all cell nuclei (Whiteside and Munglani 1998). The preparations were studied using a fluorescent microscope Olympus BX51WI (Japan) equipped with a digital camera ORCA-Flash4.0 V3 (Hamamatsu, Japan). The fluorescence excitation range was 570–620 nm. The TUNEL-positive cells were counted in 3 sections of the 5th right (injured) and left (control) DRG obtained from 3 animals at 24 h or 7 days after sciatic nerve transection.
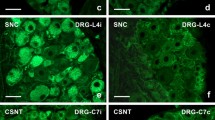
TUNEL visualization of the nuclei of apoptotic cells with DNA breaks in the rat dorsal root ganglion (DRG). Left column: TUNEL staining of cells with DNA breaks. Middle column: Hoechst 33342 staining that visualizes the nuclei of all neurons and glial cells. Right column Merged images. a Control undamaged DRG. Only rare nuclei of apoptotic cells are observed. b Positive control: numerous red nuclei of apoptotic neurons and glial cells stained by TUNEL in the DRG that was incubated with the nuclease benzonase, which induces DNA breaks. c Many nuclei of apoptotic glial cells are observed in the injured DRG at 24 h after sciatic nerve transection. d The numerous nuclei of apoptotic glial cells are observed in the injured DRG 7 days after sciatic nerve transection. e The single apoptotic neuron (arrow) in the injured DRG at 7 days after transection of sciatic nerve. Stroked arrowheads: the nuclei of DRG neurons. Empty arrowheads: the nuclei of apoptotic neurons. Scale bar 100 μm
Immunoblotting
To obtain a sufficient material amount for immunoblotting, DRGs from 4th and 5th lumbar nerves from 3 rats were combined at each post-SNT interval: 1, 4, or 24 h. The experimental and control samples were homogenized on ice by an ultrasonic homogenizer Vibra-Cell VCX 130 (Sonics, USA) in the Extraction/Labeling lysis buffer (E0655, Sigma-Aldrich) supplemented with nuclease benzonase (E1014, Sigma-Aldrich) and protease and phosphatase inhibitor cocktail (PPC1010, Sigma-Aldrich). Then, the samples were centrifuged 10 min at 10000g at 4 °C. The samples containing 10–20 μg of the protein in 15 μl were electrophoretically separated in a polyacrylamide gel in the presence of sodium dodecyl sulfate using Mini-PROTEAN Tetracell (Bio-Rad). To quantify the tested proteins, the protein standard Color Burst Electrophoresis Marker (C1992, Sigma) was used. Then the proteins were electrotransferred to the Immuno-Blot PVDF Membrane (polyvinyl difluoride membrane 162-0177, Bio-Rad) using the Trans-Blot® Turbo™ Transfer System (Bio-Rad, USA). After washing in PBS, the membrane was incubated 1 h in the 1% casein blocking buffer (TBS: 161-0782, Bio-Rad), repeatedly washed, and incubated overnight at 4 °C with the primary antibodies. We used the following antibodies (all from Sigma-Aldrich) against caspase 3 (C9598, 1:500), caspase 3 active (cleaved) form (AB3623, 1:500), p53 (P5813, 1:400), E2F1 (SAB2103144, 1:1000), amyloid precursor protein, C-terminal (A8717; 1:500), growth-associated protein Gap-43 (SAB4300525, 1:500), and β-actin (A5441, 1:5000). After incubation, the membranes were washed in Tris buffer supplemented with 0.1% Tween-20 (TTVS, 10 mM; pH 8) and incubated 1 h at room temperature with the secondary antibody anti-rabbit IgG-PEROXIDASE (A6154, Sigma-Aldrich, 1:1000). Protein detection was carried out on Сlarity Western ECL Substrate (Bio-Rad). The chemiluminescence was analyzed using the gel-documentation system Fusion SL (Vilber Lourmat, France). The resulting images were processed using the software package “ImageJ.”
Statistical Analysis
Statistical analysis was performed using one way analysis of variance (ANOVA) with Dunnett’s post hoc test. Differences were considered significant at p < 0.05 and n = 5. Mean ± SEM are shown.
Results
Differential Fluorescence Visualization of DRG and the Sciatic Nerve
Using two fluorochromes propidium iodide and Hoechst 33342, it was possible to differentially visualize the ganglia and nerves in the isolated rat DRG (red and blue-green fluorescence, respectively; Fig. 1). The neuronal cytoplasm and the nucleoli fluoresced in red (Fig. 1b, inset). The perikaryon cytoplasm consisted of large red granules (Fig. 1b, inset), presumably Nissl bodies. In contrast, Hoechst 33342 imparted the blue-green fluorescence to the nerve. The small nuclei of numerous satellite glial cells that surround the axons and neuronal bodies fluoresced in blue (Fig. 1a, b).
Cell Death in the DRG after Transection of the Sciatic Nerve
Numerous bright nuclei of glial cells that surround the bodies of the DRG neurons fluoresced in blue in the DRG sections labeled with Hoechst 33342. The nuclei of the Hoechst-stained DRG neurons were larger and fluoresced weaker (Fig. 2, middle images). Their fluorescence, size, and location allowed us to easily distinct the neuronal nuclei from the glial ones. In the control DRG treated by nuclease benzonase, which induces multiple DNA breaks (positive control), numerous TUNEL-labeled cell nuclei were observed (Fig. 2b). Their number was of the same order as the total number of the nuclei labeled by Hoechst 33342.
At 24 h after SNT, in the undamaged contralateral DRG (control) the percent of TUNEL-positive apoptotic glial cells was as low as 6.4 ± 1.2% (Fig. 2a, Table 1). However, in the axotomized right DRG the percent of apoptotic glial cells was significantly higher: 18 ± 2% (Fig. 2c, Table 1), and no apoptotic neurons were observed (Fig. 2c, Table 1). On day 7, the percent of TUNEL-positive apoptotic glial cells in the injured ganglion increased to 37 ± 6% compared with that of the control DRG (11 ± 3%) (Fig. 2d, Table 1). Only single apoptotic neurons (3 from 45 neurons were observed in 9 sections) appeared on day 7 (Fig. 2e, filled arrowhead; Table 1). Thus, glial cells were much more vulnerable to sciatic nerve transection than the DRG neurons. It should be noted that these glial cells were 2–3 cm distant from the nerve transection site and could not be damaged directly.
Protein Expression in the Rat DRG After Transection of Sciatic Nerve
Using western blotting, we studied the changes in expression of proteins that control apoptosis and different cell functions: proapoptotic proteins caspase 3 and its active cleaved form, transcription factors p53 and E2F1, amyloid precursor protein (APP), and growth associated protein 43 (Gap43) in the rat DRG at different time intervals after sciatic nerve transection. The untreated left DRG of the same animal served as control.
Caspase 3
The caspase 3 level did not change in both, the axotomized right and control left DRGs at 4 h after sciatic nerve transection, but increased similarly in both DRGs at 24 h (Fig. 3a). Possibly, this was the result of the nonspecific rat organism response to the neurotrauma. The level of activated (cleaved) caspase 3 in the axotomized right DRG was, however, higher than in the contralateral ganglion, and increased compared with its level in the injured DRG 4 h after SNT (Fig. 3b) (Fig. 3b). This could be due to the development of glial apoptosis at this time.
The effect of transection of the right sciatic nerve on the level of caspase 3 a and activated (cleaved) caspase 3 b in the ipsilateral right DRG (ipsi) and in the undamaged contralateral (left) DRG (contra) at different time intervals after injury. One way AVOVA; M ± SEM; n = 5. *р < 0.05 relative to control; # p < 0.05 relative to the indicated bars in the ipsilateral or contralateral ganglia
p53
The levels of the proapoptotic protein p53 in the nuclear and cytoplasmic fractions of the injured right DRG changed differently relative to the undamaged contralateral DRG. It did not change in the DRG nuclear fraction during the first 4 h after sciatic nerve transection, but decreased twofold at 24 h after SNT (p < 0.01, Fig. 4a). However, its level in the cytoplasmic fraction increased significantly at 24 h after sciatic nerve transection (p < 0.05, Fig. 4b). This corresponded to the enhancement of apoptosis by this time. Such redistribution of p53 between the nucleus and the cytoplasm could reduce its transcriptional activity, and enhance the proapoptotic interactions of p53 with the mitochondria.
The effect of transection of the right sciatic nerve on expression of p53 in the ipsilateral right DRG (ipsi) and in the undamaged contralateral (left) DRG (contra) at different time intervals after injury. a nuclear fraction; b cytoplasmic fraction. One way AVOVA; M ± SEM; n = 5. * p < 0.05 and ** p < 0.01 relative to control. # p < 0.05 relative to 4 h value in the ipsilateral ganglion
E2F1
The expression of p53, caspase 3, and other proapoptotic proteins (caspases 7, 8, 9, SMAC/DIABLO, Apaf-1, et al.) is controlled by the transcription factor E2F1 (Engelmann and Pützer 2010; Meng and Ghosh 2014). The level of E2F1 in both, axotomized and control DRG, increased significantly at 4 and 24 h relative to the level determined at 1 h after SNT (p < 0.05; Fig. 5). At 4 h after SNT, the level of E2F1 in the injured DRG was higher than in the control but returned to the control values by 24 h after transection (p < 0.05; Fig. 5). Thus, the overexpression of E2F1 preceded the activation of caspase 3 and the changes in the p53 level in the axotomized rat DRG.
The effect of transection of the right sciatic nerve on expression of E2F1 in the ipsilateral right DRG (ipsi) and in the undamaged contralateral (left) DRG (contra) at different time intervals after injury. One way AVOVA; M ± SEM; n = 5. * p < 0.05 relative to control; # p < 0.05 relative to E2F1 level in the right DRG at 1 h after right sciatic nerve transection; $ p < 0.05 relative to the E2F1 level in the left DRG (control) at 1 h after the right sciatic nerve transection
APP and GAP-43
The level of amyloid precursor protein (APP), a marker of traumatic nerve injury and disruption of fast axonal transport (Maxwell et al. 1999; Wang et al. 2011), did not change in the axotomized rat DRG on day 1 after sciatic nerve transection. However, APP was upregulated relative to the control contralateral ganglia at day 7 (Fig. 6a). Possibly, the interruption of APP transport along the cut axon caused its accumulation in the neuron bodies and proximal axon parts.
The effect of transection of the right sciatic nerve on expression of APP a and GAP-43 b in the ipsilateral right DRG (ipsi) and in the undamaged contralateral (left) DRG (contra) at different time intervals after injury. One way AVOVA; M ± SEM; n = 5. * p < 0.05 and ** p < 0.01 relative to control; # p < 0.05 relative to the GAP-43 level in the axotomized DRG at 24 h after sciatic nerve transection
Like APP, growth-associated protein-43 (GAP-43) was significantly overexpressed in the axotomized DRG at the seventh, but not the first day after SNT (Fig. 6b). This indicated the delayed neuron regeneration in the axotomized dorsal root ganglia.
Discussion
In the present work, we developed a novel method of differential fluorescent visualization of the dorsal root ganglion and sciatic nerve in a rat. We also showed that transection of the rat sciatic nerve induced apoptosis of DRG glial cells remote from the axotomy site at 24 h after axotomy, whereas apoptosis of DRG neurons started in 7 days. Apoptotic cell death was associated with the overexpression of transcription factors E2F1 and p53 at 4 and 24-h post-injury, respectively. Both, the nerve injury marker APP and the nerve regeneration marker GAP-43 were overexpressed in the rat DRG at 7 days after axotomy.
In the dorsal root ganglia, the pseudo-unipolar sensory neurons contain T-shaped neurites that are the components of sciatic nerve. Their long distal branches receive signals from the receptor endings in skin and muscles of the hind limb, whereas the shorter proximal branches transfer the sensory information to the spinal cord (Julius and Basbaum 2001). Each neuron was surrounded by numerous glial cells (Fig. 1) like described by Lawson (1979).
The double labelling of the isolated rat DRG with propidium iodide and Hoechst 33342 distinctly visualized the ganglia (red fluorescence), and nerves (blue-green fluorescence) (Fig. 1). Propidium iodide imparts usually red fluorescence to the nuclei of necrotic cells with the compromised plasma membranes. However, in the rat DRG, it imparts selectively red fluorescence to the neuronal cytoplasm. Large red bodies of the sensory neurons fill almost all ganglion area (Fig. 1). The similar propidium iodide staining of the neuronal bodies in the rat DRG has been observed earlier by Niu et al. (2015). Such red fluorescence belonged possibly to propidium iodide bound to the cytoplasmic RNA. Neuronal nucleoli, the ribosome factories, which are rich in RNA, had red fluorescence as well. The propidium iodide-stained red granules in the cytoplasm of DRG neurons (Fig. 1b, inset) were apparently the Nissl granules abundant with ribosomes and mRNA (Fedorenko and Uzdensky 2009; Niu et al. 2015). Hoechst 33342 bound to DNA imparts the blue-green fluorescence to the nuclear chromatin. The small nuclei of numerous satellite glial cells that surround neurons had bright blue fluorescence (Fig. 1b, Fig. 2) due to the significant chromatin condensation (Fedorenko and Uzdensky 2009). This distinguished them from the larger neuronal nuclei that fluoresced much weaker due to chromatin decondensation (Fig. 1b; Fig. 2). The similar fluorescence of Hoechst 33342-stained numerous glial cells surrounding the DRG neurons was observed by Atlasi et al. (2009).The clear difference in the nuclear size, brightness, and location of the Hoechst 33342-stained cells allows to distinct certainly DRG neurons from glial cells (Figs. 1 and 2). This was confirmed by the simultaneous application of the fluorescing neuronal and glial markers that enable to undoubtedly distinct these cells (Whiteside et al. 1998). The blue-green fluorescence of Hoechst 33342 in the sciatic nerve was apparently emitted by the numerous nuclei of glial and connective tissue cells that surround the nerve fibers. This method provides clear differential visualization of the dorsal root ganglia and nerves.
In the axotomized DRG, the glial cells were more vulnerable to injury than the sensory neurons. Rare TUNEL-positive apoptotic neurons appeared only on day 7 after SNT, whereas many apoptotic glial cells were observed as early as 24-h post-injury (Table 1). Liu et al. (1997) also showed that apoptosis of glial cells in the injured spinal cord was maximal at 24 h and, repeatedly, at 7 days after injury. The compression injury of the rat spinal cord was shown to cause apoptosis of oligodendrocytes, the progressive downregulation of the oligodendrocyte marker MBP (myelin basic protein) from 3 h to 21-day post-injury, as well as swelling and breakdown of the myelin sheaths. These events were associated with the overexpression of p53, E2F1, cytochrome C, caspase-12, and active caspase-3 (Ma et al. 2017). This was consistent with our data. The delayed death of some neurons in the first week after SNT was also reported by other authors (Atlasi et al. 2009; Schaeffer et al. 2010). However, unlike our data on relative resistance of DRG neurons to axotomy-induced apoptosis, Liu et al. (1997) observed apoptosis of some neurons at 4–24 h after injury (maximum at 8 h). About one-third of neurons and many glial cells died later, during the following weeks (Atlasi et al. 2009; Barron 2004; McKay Hart et al. 2002; Savastano et al. 2014).
It was of interest that sciatic nerve transection caused apoptosis of DRG glial cells remote for 2–3 cm from the nerve transection site. Li et al. (1999) and Ma et al. (2017) also observed apoptosis of oligodendrocytes remote for a long distance from the site of the spinal cord compression. The axotomy-induced death of remote glial cells implies the transfer of some apoptosis-inducing signals from the injured axon end to the remote glia. The proapoptotic signaling pathways from the nerve transection site to remote glial cells are unclear. As recently shown, in the isolated crayfish mechanoreceptor, apoptosis of satellite glial cells remote from the axon transection site was mediated by Ca2+, whereas MEK1/2, p38, Akt/GSK-3β, and mTOR signaling pathways played, oppositely, the protective role (Berezhnaya et al. 2017; Khaitin et al. 2018).
The first proapoptotic event observed in the present study was the upregulation of E2F1 in 4 h after SNT. The overexpression of p53 and the cleavage/activation of caspase 3 were observed later, 24-h post-injury when glial apoptosis became evident. E2F1 is known to regulate DNA synthesis and repair, cell proliferation, and apoptosis (Pelengaris et al. 2002; Raimundo et al. 2012). As a transcription factor, it controls the expression of a variety of proapoptotic proteins such as p53; p73; caspases 3, 7, 8, and 9; SMAC/DIABLO; and Apaf-1 (Engelmann and Pützer 2010; Meng and Ghosh 2014). One can suggest that E2F1 overexpression is a key event in the initiation of apoptosis of remote glial cells in the axotomized DRG. The overexpression of E2F1 and p53 was also shown in the axotomized crayfish ganglia (Demyanenko et al. 2019). A different time course of proapoptotic events was observed after compression spinal cord injury in a rat; the overexpression of p53 at 1-h post-injury was followed by the upregulation of E2F1, caspase 12, the activation of caspase 3 at 3 h, and the cytochrome C release at 12 h (Ma et al. 2017).
It is known that p53 can initiate apoptosis either by transcription-dependent or by transcription-independent way. As a transcription factor, p53 stimulates the expression of various proapoptotic proteins such as PUMA, Noxa, and caspase 6. The delayed induction of the apoptosis-related genes p53, c-Jun, and Bax was reported in the degenerating neurons after ischemia or axotomy (Hughes et al. 1999). The axotomy-induced death of motor neurons in adult mice was associated with the overexpression of the p53-controlled proapoptotic protein Noxa (Kiryu-Seo et al. 2005). The hyperactivation of the proapoptotic pathway p53/PUMA was observed in the axotomized retinal ganglion cells in mice (Lebrun-Julien and Suter 2015). These examples indicate the involvement of the transcription-dependent proapoptotic activity of p53 in the axotomy-induced neuronal apoptosis. However, our experiments showed the twofold downregulation of p53 in the nuclear fraction of DRG, and its overexpression in the cytoplasmic fraction at 24 h after SNT (Fig. 4). Therefore, the transcription-dependent activity of p53 did not participate in SNT-induced apoptosis of DRG cells. Apparently, the transcription-independent cytoplasmic activity of p53 was rather involved in apoptosis of glial cells but not neurons at 24 h after SNT. The transcription-independent proapoptotic action of p53 is known to be associated with its translocation to mitochondria, impairment of bioenergetic processes, release of cytochrome c and AIF, which induce activation of caspase 3, a key proapoptotic proteinase (Yakovlev and Faden 2001). This finally leads to apoptosis (Aubrey et al. 2018; Wan et al. 2014; Wang et al. 2014). The general level of caspase 3 did not change in the injured rat DRG at 1–24 h after sciatic nerve transection. Probably, its existing level in DRG cells was sufficient for the execution of glial apoptosis. However, its active cleaved form was upregulated at 24 h after SNT that coincided with the development of apoptosis of glial cells.
Apoptosis of DRG neurons occurred later. The delayed caspase-mediated apoptosis of the injured rat DRG neurons was also demonstrated by Momeni et al. (2013). We observed the accumulation of amyloid precursor protein in the axotomized DRG on seventh but not the first day after sciatic nerve transection. APP is a known marker of traumatic nerve injury and disruption of the fast axonal transport. Therefore, its accumulation indicated degeneration of DRG neurons. Ischemic or traumatic damage of the nervous system in the invertebrate or vertebrate animals was shown to induce axonal accumulation of APP (Maxwell et al. 1999; Muresan and Ladescu Muresan 2015; Wang et al. 2011). One can suggest that the delayed apoptosis of DRG neurons was associated with the neuroprotective role of APP. Actually, APP and its soluble fragment sAPPα have been reported to play a protective role in the injured neurons. Moreover, the neuroprotective role of APP was shown to be associated with the binding of its short sequence, APP96–110, to heparan sulfate proteoglycan, a component of the extracellular matrix (Corrigan et al. 2014; Plummer et al. 2016). In the injured neurons, APP is intensely produced and transported along the axon in order to restore the damaged intercellular contacts. However, axotomy interrupts the axonal transport that causes APP accumulation.
Simultaneously, the neuron regeneration processes developed in the axotomized DRG. This was evidenced by the upregulation of growth-associated protein-43 on day 7, but not day 1 after transection of the sciatic nerve. GAP-43 is known to be intensely expressed in the axon growth cones during early development, or regeneration of the nervous system. It binds to the plasma membrane and the cytoskeleton. Being activated by protein kinase C, GAP-43 regulates the actin cytoskeleton in neurons. GAP-43 is often considered as a marker of regeneration in the injured neurons (Bornstein and Poon 2012).
Thus, sciatic nerve transection induced apoptosis of satellite glial cells and some sensory neurons in the dorsal root ganglion during the first week after the injury. It is of importance that the glial cells remote for a long distance of several centimeters from the transection site died from apoptosis after axotomy. These glial cells were more vulnerable to axotomy than DRG neurons. In fact, glial apoptosis was observed at 24 h after SNT and increased further on day 7, whereas apoptosis of some DRG neurons started only at 7th day. We showed that the earliest proapoptotic event in the injured rat DRG was the overexpression of transcription factor E2F1 observed at 4-h post-SNT. This preceded the induction of p53 and activation of caspase 3 that occurred 24 h after sciatic nerve transection. The nerve injury marker APP and the marker of nerve regeneration GAP-43 were overexpressed in the axotomized DRG on day 7 after sciatic nerve transection. Possibly, the delayed death of DRG neurons was associated with the neuroprotective activity of APP. Thus, E2F1 and p53 may be considered potential targets for the therapy of nerve injury. Their inhibitors should be studied as promising neuroprotective drugs.
References
Atlasi MA, Mehdizadeh M, Bahadori MH, Joghataei MT (2009) Morphological identification of cell death in dorsal root ganglion neurons following peripheral nerve injury and repair in adult rat. Iran Biomed J 13:65–72
Aubrey BJ, Kelly GL, Janic A, Herold MJ, Strasser A (2018) How does p53 induce apoptosis and how does this relate to p53-mediated tumour suppression? Cell Death Differ 25:104–113. https://doi.org/10.1038/cdd.2017.169
Barron KD (2004) The axotomy response. J Neurol Sci 220:119–121. https://doi.org/10.1016/j.jns.2004.03.009
Berezhnaya EV, Bibov MY, Komandirov MA, Neginskaya MA, Rudkovskii MV, Uzdensky AB (2017) Involvement of MAPK, Akt/GSK-3β and AMPK/mTOR signaling pathways in protection of remote glial cells from axotomy-induced necrosis and apoptosis in the isolated crayfish stretch receptor. Mol Cell Neurosci 83:1–5. https://doi.org/10.1016/j.mcn.2017.06.003
Bornstein N, Poon WS (2012) Accelerated recovery from acute brain injuries: clinical efficacy of neurotrophic treatment in stroke and traumatic brain injuries. Drugs Today 48(Suppl A):43–61. https://doi.org/10.1358/dot.2012.48(Suppl.A).1739723
Casas C, Isus L, Herrando-Grabulosa M, Mancuso FM, Borrás E, Sabidó E, Forés J, Aloy P (2015) Network-based proteomic approaches reveal the neurodegenerative, neuroprotective and pain-related mechanisms involved after retrograde axonal damage. Sci Rep 5:9185. https://doi.org/10.1038/srep09185
Corrigan F, Thornton E, Roisman LC, Leonard AV, Vink R, Blumbergs PC, van den Heuvel C, Cappai R (2014) The neuroprotective activity of the amyloid precursor protein against traumatic brain injury is mediated via the heparin binding site in residues 96-110. J Neurochem 128:196–204. https://doi.org/10.1111/jnc.12391
Demyanenko S, Dzreyan V, Uzdensky A (2019) Axotomy-induced changes of the protein profile in the crayfish ventral cord ganglia. J Mol Neurosci 68:667–678. https://doi.org/10.1007/s12031-019-01329-5
Dubový P, Klusáková I, Hradilová-Svíženská I, Joukal M (2018) Expression of regeneration-associated proteins in primary sensory neurons and regenerating axons after nerve injury-an overview. Anat Rec (Hoboken) 301:1618–1627. https://doi.org/10.1002/ar.23843
Engelmann D, Pützer BM (2010) Translating DNA damage into cancer cell death-A roadmap for E2F1 apoptotic signalling and opportunities for new drug combinations to overcome chemoresistance. Drug Resist Updates 13:119–131. https://doi.org/10.1016/j.drup.2010.06.001
Faulkner JR, Herrmann JE, Woo MJ, Tansey KE, Doan NB, Sofroniew MV (2004) Reactive astrocytes protect tissue and preserve function after spinal cord injury. J Neurosci 24:2143–2155. https://doi.org/10.1523/JNEUROSCI.3547-03.2004
Fedorenko GM, Uzdensky AB (2009) Cellular structures involved in the transport processes and neuroglial interactions in the crayfish stretch receptor. J Integr Neurosci 8:433–440
Hill CS (2016) Traumatic axon injury: mechanisms and translational opportunities. Trends Neurosci 39:311–324. https://doi.org/10.1016/j.tins.2016.03.002
Hughes PE, Alexi T, Walton M, Williams CE, Dragunow M, Clark RG, Gluckman PD (1999) Activity and injury-dependent expression of inducible transcription factors, growth factors and apoptosis-related genes within the central nervous system. Prog Neurobiol 57:421–450. https://doi.org/10.1016/s0301-0082(98)00057-4
Julius D, Basbaum AI (2001) Molecular mechanisms of nociception. Nature 413:203–210. https://doi.org/10.1038/35093019
Khaitin AM, Rudkovskii MV, Uzdensky AB (2015) The method of isolation of the crayfish abdominal stretch receptor maintaining a connection of the sensory neuron to the ventral nerve cord ganglion. Invertebr Neurosci 15:1–10. https://doi.org/10.1007/s10158-014-0176-2
Khaitin A, Rudkovskii M, Uzdensky A (2018) Ca2+ mediates axotomy-induced necrosis and apoptosis of satellite glial cells remote from the transection site in the isolated crayfish mechanoreceptor. Mol Cell Neurosci 88:7–15. https://doi.org/10.1016/j.mcn.2017.12.004
Kiryu-Seo S, Hirayama T, Kato R, Kiyama H (2005) Noxa is a critical mediator of p53-dependent motor neuron death after nerve injury in adult mouse. J Neurosci 25:1442–1447. https://doi.org/10.1523/JNEUROSCI.4041-04.2005
Kolosov M, Uzdensky A (2006) Crayfish mechanoreceptor neuron prevents photoinduced apoptosis of satellite glial cells. Brain Res Bull 69:495–500. https://doi.org/10.1016/j.brainresbull.2006.02.018
Laskowitz D, Grant G (eds) (2016) Translational Research in Traumatic Brain Injury. CRC Press/Taylor and Francis Group, Boca Raton (FL)
Lawson SN (1979) The postnatal development of large light and small dark neurons in mouse dorsal root ganglia: a statistical analysis of cell numbers and size. J Neurocytol 8:275–294. https://doi.org/10.1007/BF01236123
Lebrun-Julien F, Suter U (2015) Combined HDAC1 and HDAC2 depletion promotes retinal ganglion cell survival after injury through reduction of p53 target gene expression. ASN Neuro 7(3):175909141559306. https://doi.org/10.1177/1759091415593066
Li GL, Farooque M, Holtz A, Olsson Y (1999) Apoptosis of oligodendrocytes occurs for long distances away from the primary injury after compression trauma to rat spinal cord. Acta Neuropathol 98:473–480. https://doi.org/10.1007/s004010051112
Liu B, Teschemacher AG, Kasparov S (2017) Neuroprotective potential of astroglia. J Neurosci Res 95:2126–2139. https://doi.org/10.1002/jnr.24140
Liu XZ, Xu XM, Hu R, Du C, Zhang SX, McDonald JW, Dong HX, Wu YJ, Fan GS, Jacquin MF, Hsu CY, Choi DW (1997) Neuronal and glial apoptosis after traumatic spinal cord injury. J Neurosci 17:5395–5406. https://doi.org/10.1523/JNEUROSCI.17-14-05395.1997
Ma L, Yu HJ, Gan SW, Gong R, Mou KJ, Xue J, Sun SQ (2017) p53-Mediated oligodendrocyte apoptosis initiates demyelination after compressed spinal cord injury by enhancing ER-mitochondria interaction and E2F1 expression. Neurosci Lett 644:55–61. https://doi.org/10.1016/j.neulet.2017.02.038
Maxwell WL, Donnelly S, Sun X, Fenton T, Puri N, Graham DI (1999) Axonal cytoskeletal responses to nondisruptive axonal injury and the short-term effects of posttraumatic hypothermia. J Neurotrauma1 6:1225–1234. https://doi.org/10.1089/neu.1999.16.1225
McKay Hart A, Brannstrom T, Wiberg M, Terenghi G (2002) Primary sensory neurons and satellite cells after peripheral axotomy in the adult rat. Time course of cell death and elimination. Exp Brain Res 142:308–318. https://doi.org/10.1007/s00221-001-0929-0
Melle C, Ernst G, Grosheva M, Angelov DN, Irintchev A, Guntinas-Lichius O, von Eggeling F (2009) Proteomic analysis of microdissected facial nuclei of the rat following facial nerve injury. J Neurosci Methods 185:23–28. https://doi.org/10.1016/j.jneumeth.2009.09.003
Meng P, Ghosh R (2014) Transcription addiction: can we garner the Yin and Yang functions of E2F1 for cancer therapy? Cell Death Disease 5:e1360. https://doi.org/10.1038/cddis.2014.326
Momeni HR, Soleimani Mehranjani M, Shariatzadeh MA, Haddadi M (2013) Caspase-mediated apoptosis in sensory neurons of cultured dorsal root ganglia in adult mouse. Cell J 15:212–217
Mulder J, Wernérus H, Shi TJ, Pontén F, Hober S, Uhlén M, Hökfelt T (2007) Systematically generated antibodies against human gene products: high throughput screening on sections from the rat nervous system. Neuroscience 146:1689–1703. https://doi.org/10.1016/j.neuroscience.2007.02.054
Muresan V, Ladescu Muresan Z (2015) Amyloid-β precursor protein: Multiple fragments, numerous transport routes and mechanisms. Exp Cell Res 334:45–53. https://doi.org/10.1016/j.yexcr.2014.12.014
Niu J, Li C, Wu H, Feng X, Su Q, Li S, Zhang L, Yew DTW, Cho EYP, Sha O (2015) Propidium iodide (PI) stains Nissl bodies and may serve as a quick marker for total neuronal cell count. Acta Histochem 117:182–187. https://doi.org/10.1016/j.acthis.2014.12.001
Patodia S, Raivich G (2012) Role of transcription factors in peripheral nerve regeneration. Front Mol Neurosci 5:8. https://doi.org/10.3389/fnmol.2012.00008
Pelengaris S, Khan M, Evan G (2002) c-MYC: more than just a matter of life and death. Nature Rev Cancer 2:764–776. https://doi.org/10.1038/nrc904
Perlson E, Hanz S, Medzihradszky KF, Burlingame AL, Fainzilber MJ (2004) From snails to sciatic nerve: retrograde injury signaling from axon to soma in lesioned neurons. Neurobiol 58:287–294. https://doi.org/10.1002/neu.10316
Plummer S, Van den Heuvel C, Thornton E, Corrigan F, Cappai R (2016) The Neuroprotective properties of the amyloid precursor protein following traumatic brain injury. Aging Dis 7:163–179. https://doi.org/10.14336/AD.2015.0907
Raimundo N, Song L, Shutt TE, McKay SE, Cotney J, Guan MX, Gilliland TC, Hohuan D, Santos-Sacchi J, Shade GS (2012) Mitochondrial stress engages E2F1 apoptotic signaling to cause deafness. Cell 148:716–726. https://doi.org/10.1016/j.cell.2011.12.027
Rishal I, Fainzilber M (2014) Axon-soma communication in neuronal injury. Nature Rev Neurosci 15:32–42. https://doi.org/10.1038/nrn3609
Savastano LE, Laurito SR, Fitt MR, Rasmussen JA, Gonzalez Polo V, Patterson S (2014) Sciatic nerve injury: a simple and subtle model for investigating many aspects of nervous system damage and recovery. J Neurosci Meth 227:166–180. https://doi.org/10.1016/j.jneumeth.2014.01.020
Schaeffer V, Meyer L, Patte-Mensah C, Eckert A, Mensah-Nyagan AG (2010) Sciatic nerve injury induces apoptosis of dorsal root ganglion satellite glial cells and selectively modifies neurosteroidogenesis in sensory neurons. Glia 58:169–180. https://doi.org/10.1002/glia.20910
Uzdensky AB (2018) Axotomy induces damage to glial cells remote from the transection site in the peripheral nervous system. Neural Reg Res 13:639–640. https://doi.org/10.4103/1673-5374.230285
Verkhratsky A, Ho MS, Zorec R, Parpura V (Editors) (2019) Neuroglia in neurodegenerative diseases (advances in experimental medicine and biology book (1175) Kindle Edition. Springer
Wan C, Ma X, Shi S, Zhao J, Nie X, Han J, Xiao J, Wang X, Jiang S, Jiang J (2014) Pivotal roles of p53 transcription-dependent and -independent pathways in manganese-induced mitochondrial dysfunction and neuronal apoptosis. Toxicol Appl Pharmacol 281:294–302. https://doi.org/10.1016/j.taap.2014.10.013
Wang J, Hamm RJ, Povlishock JT (2011) Traumatic axonal injury in the optic nerve: evidence for axonal swelling, disconnection, dieback, and reorganization. J Neurotrauma 28:1185–1198. https://doi.org/10.1089/neu.2011.1756
Wang DB, Kinoshita C, Kinoshita Y, Morrison RS (2014) p53 and mitochondrial function in neurons. Biochim Biophys Acta 1842:1186–1197. https://doi.org/10.1016/j.bbadis.2013.12.015
Whiteside G, Munglani R (1998) TUNEL, Hoechst and immunohistochemistry triple-labelling: an improved method for detection of apoptosis in tissue sections--an update. Brain Res Brain Res Protoc 3:52–53. https://doi.org/10.1016/s1385-299x(97)00032-9
Whiteside G, Doyle CA, Hunt SP, Munglani R (1998) Differential time course of neuronal and glial apoptosis in neonatal rat dorsal root ganglia after sciatic nerve axotomy. Eur J Neurosci 10:3400–3408. https://doi.org/10.1046/j.1460-9568.1998.00346.x
Witiw CD, Fehlings MG (2015) Acute spinal cord injury. J Spinal Disorder Techn 28:202–210. https://doi.org/10.1097/BSD.0000000000000287
Yakovlev AG, Faden AI (2001) Caspase-dependent apoptotic pathways in CNS injury. Mol Neurobiol 24:131–144. https://doi.org/10.1385/MN:24:1-3:131
Funding
The work was supported by the Ministry of Science and Higher Education of Russian Federation; grant #0852–2020-0028.
Author information
Authors and Affiliations
Contributions
Dzreyan V.A.: data generation and analysis (western blotting); Rodkin S.V.: data generation (DRG visualization, apoptosis study); Nikul V.V.: data generation (DRG visualization); Pitinova M.A.: design and data generation (fluorescence microscopy); Uzdensky A.B.: Supervision; Conceptualization; data analysis and interpretation, manuscript writing.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest. All authors agree to publish this paper.
Ethics Approval
The submitted work is original. It has not been published elsewhere and is not considered for publication and in any form or language (partially or in full).
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Dzreyan, V., Rodkin, S., Nikul, V. et al. The Expression of E2F1, p53, and Caspase 3 in the Rat Dorsal Root Ganglia After Sciatic Nerve Transection. J Mol Neurosci 71, 826–835 (2021). https://doi.org/10.1007/s12031-020-01705-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s12031-020-01705-6