Abstract
Purpose of Review
Our goal is to examine the processes—both central and peripheral—that underlie the development of peripherally-induced neuropathic pain (pNP) and to highlight recent evidence for mechanisms contributing to its maintenance. While many pNP conditions are initiated by damage to the peripheral nervous system (PNS), their persistence appears to rely on maladaptive processes within the central nervous system (CNS). The potential existence of an autonomous pain-generating mechanism in the CNS creates significant implications for the development of new neuropathic pain treatments; thus, work towards its resolution is crucial. Here, we seek to identify evidence for PNS and CNS independently generating neuropathic pain signals.
Recent Findings
Recent preclinical studies in pNP support and provide key details concerning the role of multiple mechanisms leading to fiber hyperexcitability and sustained electrical discharge to the CNS. In studies regarding central mechanisms, new preclinical evidence includes the mapping of novel inhibitory circuitry and identification of the molecular basis of microglia-neuron crosstalk. Recent clinical evidence demonstrates the essential role of peripheral mechanisms, mostly via studies that block the initially damaged peripheral circuitry. Clinical central mechanism studies use imaging to identify potentially self-sustaining infra-slow CNS oscillatory activity that may be unique to pNP patients.
Summary
While new preclinical evidence supports and expands upon the key role of central mechanisms in neuropathic pain, clinical evidence for an autonomous central mechanism remains relatively limited. Recent findings from both preclinical and clinical studies recapitulate the critical contribution of peripheral input to maintenance of neuropathic pain. Further clinical investigations on the possibility of standalone central contributions to pNP may be assisted by a reconsideration of the agreed terms or criteria for diagnosing the presence of central sensitization in humans.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Neuropathic pain is defined by the International Association for the Study of Pain (IASP) as “pain caused by a lesion or disease of the somatosensory nervous system” [1•]. This definition is broad, covering over 100 conditions [2], and it involves injuries which span the entire pain neuro-axis. These injuries are often initially painful, in which case the pain serves to protect the damaged region until it can heal. However, in chronic neuropathic pain, the nervous system responds inappropriately to the damage through multiple mechanisms involving both the nervous system and its modulators. The unfortunate result is an unbalanced sensory system that misreads sensory inputs and can spontaneously generate painful sensations. Approximately 20 million people in the USA suffer from chronic neuropathic pain, with sometimes devastating losses of quality of life [2]. Treatments for neuropathic pain are non-specific and often insufficiently effective [3]. These treatments are not innocuous, and, for patients treated with opioids, can generate life-threatening side effects, highlighting the critical societal need for improved and customized strategies.
Therapeutic strategies for treatment of chronic neuropathic pain are limited by an incomplete understanding of how the nervous system maintains spontaneous pain following resolution of the initial injury. Before clinicians can provide precise treatment strategies for neuropathic pain patients, essential targets in the pathway must be identified. To achieve this goal, it is necessary to determine if maladaptive signaling in the central parts of the somatosensory system are sufficient to generate spontaneous pain. In this review, we focus on this key issue, by first presenting a brief review of both peripheral and central mechanisms in neuropathic pain and then presenting the preclinical and clinical evidence for each potential framework.
Common Neuropathic Pain Syndromes and Overview of Mechanisms
Neuropathic pain syndromes can be divided into two general categories: those that are consequences of a peripheral lesion or disease and those that are consequences of a central lesion or disease. This review focuses on conditions that are considered consequences of a peripheral insult. Central neuropathic pain conditions, such as central post-stroke pain (CPSP), are likely to possess different underlying mechanisms and warrant separate consideration.
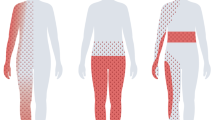
Table 1 summarizes by general etiology some of the more common (and typically irreversible) neuropathic pain syndromes that originate from damage to the peripheral nervous system (PNS). As these conditions demonstrate, there are multiple routes to peripheral nerve damage, including mechanical, chemical, and infectious. These conditions share some general features, including spontaneous pain that is shooting, lancinating, or burning [4, 5]. Allodynia—i.e., a painful response to non-painful stimuli—as well as hyperalgesia, are also common features. The overlapping features of these syndromes can lend themselves to common treatment strategies and underscore the likelihood of shared pathophysiologic mechanisms.
Peripheral Mechanisms in Neuropathic Pain
Peripheral nerve damage can result in chronic neuropathic pain through multiple routes [6••]. While the insult may be localized, the responses that lead to chronic pain are not. Peripheral terminals of pain-processing unmyelinated C fibers and thinly-myelinated Aδ fibers can spur the development of neuropathic pain after being affected by metabolic damage, toxins, medications, cytokines, and other inflammatory mediators [7], resulting in fiber density changes and neuronal hyperexcitability [8, 9, 10, 11, 12••]. Along the axon, injuries such as trauma, compression, hypoxia, inflammation, overstimulation, and chemical damage can induce fiber degeneration and alterations in channel expression and composition [13], in turn resulting in ectopic firing and faulty signal transmission [14]. In response to axonal damage and its sequelae, satellite glia and autonomic neurons can incur pain-promoting states though alterations in their overall numbers, distribution, sprouting patterns, and channel expression [15,16,17].
In the DRG and trigeminal ganglia, primary afferent cell bodies can be exposed to chemical, mechanical, and excitotoxic damage, and in neuropathic pain states demonstrate maladaptive changes in their membrane composition, synapse properties, and synapse location(s) [18,19,20]. The probability of peripheral nerve damage or its progression to neuropathic pain can also be increased by genetic predispositions and/or hereditary conditions [21, 22]. The ultimate result of the maladaptive mechanisms following peripheral nerve damage is a state of inappropriate signaling from the peripheral neuron to its second-order targets, with multi-factorial errors in both transduction and transmission [4, 23, 24] (Fig. 1).
Central Mechanisms in Neuropathic Pain
With repeated or sufficiently intense stimulation, spinal and supraspinal nociceptive pathways can become sensitized to subsequent stimuli. With persistent nociceptive input [25•], like that seen in peripheral neuropathy, this central sensitization [26] becomes maladaptive. IASP defines central sensitization as “increased responsiveness of nociceptive neurons in the central nervous system to their normal or subthreshold afferent input” [27]. At the synapse of second-order neurons, this increased responsiveness can involve changes in calcium permeability, receptor overexpression, and synapse location [18, 28]. Also promoting a chronic pain state are microglia, whose hyperactivation triggers the release of pain-promoting mediators [29]. In supraspinal regions, the resulting misbalance between descending facilitation and inhibition is another major contributor to ongoing pain [30,31,32]. Maladaptive subcortical and cortical plasticity also contributes to painful interpretation of incoming signals [31, 32], with the ultimate result promoting a chronic pain state (Fig. 1).
Evidence for Peripheral Mechanisms: Preclinical
Injury and/or damage to the nociceptive afferents predominantly accounts for the onset of neuropathic pain. Peripheral mechanisms that initiate and maintain sustained excitation of afferent nerve fibers in neuropathic pain have been extensively studied utilizing multiple rodent models, such as spared nerve injury (SNI), chronic constriction injury (CCI), and spinal nerve ligation (SNL) [33]. In addition, specific disease-related neuropathies and the associated peripheral sensitization mechanisms have also been studied in rodent models of diabetes, chemotherapy, herpes zoster, and HIV-induced peripheral neuropathy [33]. In rodent spinal/sciatic nerve injury or constriction models, increased ectopic electrical discharge in myelinated axons (A fibers) begins generally within several hours of the induction of injury, and subsequently appears in unmyelinated axons (C fibers) within several days to weeks [12••, 34]. A wide variation in the fiber specificity, frequency, type, timeline of increased and/or sustained ectopic discharge, and cross-sensitization among A and C fibers at both peripheral and DRG cell body levels have been reported, which could be linked to the type of target nerve, injury, and the species/strain of animals studied. Multiple sources have subsequently shown that these changes in nerve fiber discharge lead to the development of various reflexive alterations in rodents that are referred to as neuropathic pain behaviors [12••]. Looking from a cellular/molecular aspect, distinct classes of receptors and ion channels in specific sensory neuron subtypes have been implicated for increased/sustained ectopic discharge. Due to the hyperexcitable nature of these neuronal injuries, voltage-gated Na+ (NaV) channels account for the primary molecular entity implicated in peripheral neuropathic pain conditions. Increased expression, trafficking, and peripheral targeting of several NaV channel isoforms, such as NaV1.3 and NaV1.6 (on myelinated axons) and NaV 1.7 and NaV 1.8 (on unmyelinated axons), have been shown in multiple rodent neuropathic models [35,36,37]. In addition, modifications in channel function, which lead to fast channel activation and increased current density, account for hyperexcitation of peripheral nerve fibers in response to neuropathy [32]. Several studies utilizing mouse genetics and pharmacological interventions targeting NaV channels have confirmed their involvement in peripheral nerve fiber excitation and neuropathic pain-related behaviors in rodent models [35,36,37].
Transient receptor potential (TRP) channels account for the major class of sensory detection/transduction channels, which upon activation by multiple pain-producing physico-chemical stimuli, provide the generator potential that is often needed to activate the NaV channels to elicit action potential firing (or electrical discharge) on nerve fibers (reviewed in [38]). Under patho-/physiological conditions, TRPA1 and TRPV4 could be activated in part by mechanical stimuli, TRPA1 and TRPM8 are activated by cold temperatures, and TRPV1 is activated by hot temperatures, as well as by acidic pH. Upon nerve injury/neuropathic conditions, TRPA1 has been shown to be directly activated by cell damage-related mediators, such as reactive oxygen/nitrogen species (ROS/RNS), leading to increased nerve fiber excitation and manifestation of mechanical and cold hypersensitivity behaviors in rodents (reviewed in [38]). Similarly, administration of paclitaxel-based chemotherapeutic drugs that cause peripheral neuropathy in rodents has been suggested to induce mechanical activation/transduction through TRPV4 [39]. Nerve injury, including neuroma formation, involves an inflammatory component, both at the site of injury and at the level of cell body in DRG, with local enrichment of (pro-)inflammatory mediators that provide the spices for nerve fiber sensitization. Modulation of TRPV1 channel function accounts for a major proportion of such sensitization via inflammatory mediators. Specifically, modulated TRPV1 gets activated by minimally acidic pH and at body temperatures, leading to sustained generator potentials and electrical discharge (reviewed in [38]). Both nerve damage/injury and the increased inflammatory microenvironment have been shown to upregulate the expression of these predominant sensory TRP channels, which in addition to functional changes lead to increases in the magnitude and duration of hyperexcitability of nerve fibers [reviewed in [38]. A large number of studies utilizing genetically modified mice lacking specific functional TRP channels and with the use pharmacological blockers of individual TRP channels have shown their critical involvement in peripheral nerve fiber excitation and neuropathic pain-related behaviors in rodent models (reviewed in [38, 40]).
Contrary to NaV and TRP channels, voltage-gated K+ (Kv), leak/two-pore domain K+ (K2P), and Ca2+/voltage-activated K+ (KCa) account for the vast majority of repolarizing or regulatory channels on sensory neurons/afferents (reviewed in [41]). Activation of these channels lead to membrane repolarization, thereby resulting in the suppression of electrical discharge/firing. Decreases in the protein expression of Kv1.1, Kv1.2, K1.4, Kv2.1, Kv2.2, Kv4.3, Kv7.2, Kv7.3, and Kv9.1, as well as of a number of K2P, KCa, and Kir/KATP have been shown in multiple rodent neuropathic pain models, which lead to a decrease in K+ currents and a resultant hyperexcitation of sensory nerves (reviewed in [41]). Except for Kv7 channels, extensive validation of the role of altered expression and/or function of most K+ channels utilizing pharmacological and mouse genetic approaches remains to be explored in nerve injury/neuropathic conditions.
In addition to neuronal channels and receptors, accumulation of infiltrating immune cells such as neutrophils, macrophages, and mast cells at the site of nerve injury constitute yet another peripheral cellular mechanism for nerve fiber hyperexcitation and sustained electrical discharge in majority of neuropathic conditions [42]. Continued supply of (pro-)inflammatory mediators by these immune cells account for both nerve fiber sensitization and neuronal damage, thereby exacerbating the neuropathy. In summary, numerous preclinical studies collectively suggest that (1) multiple mechanisms of peripheral nerve fiber excitation and sensitization operate in nerve injury/neuropathy conditions; (2) these mechanisms lead to sustained electrical discharge that feeds to the CNS and (3) which presumably accounts for continued excitatory ascending pain signal propagation to the brain. Pharmacological interventions aimed at reduction and/or blockage of peripheral nerve fiber excitation in rodent neuropathic pain models by targeting several abovementioned nociceptive ion channels/receptors have shown significant blockade of neuropathic pain-related behaviors [43]. Therefore, it is reasonable to argue that hyperexcitation and sustained electric discharge of peripheral nerve fibers constitute a predominant mechanism for peripheral neuropathic pain conditions.
Evidence for Peripheral Mechanisms: Clinical
In patients with phantom limb pain, single-fiber recordings of sensory fibers projecting into the neuroma demonstrate direct evidence of spontaneous ectopic activity and excessive action potential firing in [44]. Altered firing patterns in afferent neurons are also present in patients with primary erythromelalgia, for whom a mutation in the Nav1.7 channel can cause shifts in nociceptor activation thresholds [45]. As summarized in Table 2, in multiple types of chronic neuropathic pain, studies that block peripheral activity with a local anesthetic have resulted in significant alleviation or complete reduction of pain. Peripheral nerve stimulation, which disrupts incoming sensory signaling, has also been shown to provide significant pain relief in patients with neuropathic pain from post-herpetic neuralgia (PHN), complex regional pain syndrome (CRPS) type II, and traumatic and surgical nerve damage [53,54,55,56,57]. Collectively, these results suggest that peripheral input is an essential and necessary component for spontaneous neuropathic pain.
Studies have also utilized DRG blockade techniques to demonstrate its key role in spontaneous pain generation. In amputees with phantom limb pain, Vaso et al. demonstrated that dilute lidocaine applied directly to the DRG in concentrations sufficient to suppress DRG ectopic firing, but not transmission of other sensory information, was capable of abolishing phantom limb pain in topographically appropriate regions [58•]. There is also growing evidence for the effectiveness of targeted DRG stimulation in the effective alleviation of chronic neuropathic pain [59, 60], and this evidence may expand as novel interfacing technologies continue to advance [61].
Evidence for Central Mechanisms: Preclinical
Changes in the Spinal Cord
Neuropathy-induced increases in spinal neuronal activity can be partly attributed to increased synaptic efficacy in the spinal cord dorsal horn. Activation of several protein kinases, including PKA, PKC, p38 MAPK, Src, ERK, and CaMKII, is observed in animal models of nerve injury. In painful neuropathy, ionotropic and metabotropic glutamate receptors exhibit phosphorylation and changes in trafficking that increase excitatory post-synaptic potential (EPSP) frequency and amplitude [62,63,64]. Increased post-synaptic activity is also achieved by alterations in glutamate homeostasis, resulting from increased expression of the vesicular glutamate transporters Vglut2 and Vglut3 in the superficial and deep dorsal horn, respectively [65]. This glutamate accumulation in synaptic vesicles is thought to increase EPSP amplitudes [66].
Spinal cord neurons also alter ion channel expression levels to acutely modify their properties following neuropathy. Examples include the voltage-gated calcium channel subunit α2δ-1 in the dorsal horn following induction of CIPN [67]. The ionotropic serotonin receptor 5-HT3 in the dorsal horn is the target of descending serotonergic facilitation of pain from the rostral ventromedial medulla (RVM). Activation of spinal 5-HT3 receptors is also associated with pro-inflammatory cytokine release and glial cell activation, changes that appear to be crucial for the maintenance of central sensitization [68]. Enhanced excitability is also brought about by a reduction in inhibitory tone. BDNF, in addition to its effects on microglia [69] and GluN2B phosphorylation, also inhibits presynaptic GABAA receptors, reducing presynaptic inhibition and causing spontaneous activity in lamina I output neurons, along with increased responsiveness to nociceptive input and the relaying of innocuous mechanical input [70, 71, 72•, 73]. Similar disinhibitory effects have been noted with radial neurons (morphologically distinct excitatory interneurons located in lamina II of the dorsal horn that show diminished inhibitory post-synaptic currents following injury [74]) and presynaptic reductions in GIRK potassium channel expression [75].
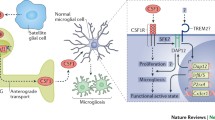
The production of inflammatory mediators by injured neurons and activated glial cells drives many of the physiological CNS changes associated with neuropathic pain. For example, dorsal horn neurons exhibit elevated expression of the chemokine SDF-1α/CXCL12 in a CIPN model [76,77,78], CXCL13 in a rat SNL model [79], and CCL3 and its receptor CCR5 in CCI in rats [80•, 81, 82]. Proinflammatory cytokines such as interferon-γ activate spinal microglia, a process that underlies many of the neuropathy-induced changes in spinal neuron behavior, most notably the hyperresponsiveness of wide dynamic range (WDR) neurons following CCI [83], and the activation of convergent nociceptive inputs following injury [84, 85]. Astrocyte activation is also crucial to the manifestation of neuropathic pain [86]. Resident astrocytes, as well as CD4+ T cells infiltrating the dorsal horn, secrete IL-17 following SNL. The resultant expression of IL-1β and IL-6 is, along with TNF-α, important in the maintenance of neuropathic pain [87,88,89]. ATP is released by injured dorsal horn neurons [90], whereupon microglial purinergic receptors are activated, leading to microglial proliferation and neuropathic pain [91,92,93,94, 95•]. The apparent reduction in the importance of microglial activity in the later stages of neuropathic pain models has led to the suggestion that microgliosis and inflammatory mediator production may be most important in the initiation of hypersensitivity and promoting the transition to chronic pain [96].
Changes in Brain Regions
In the ventral posterior thalamus (the major site of projection from the spinothalamic tract), wide dynamic range and nociceptor-specific neurons have shown hyperexcitability in neuropathy models [97]. As in the spinal cord, the vesicular glutamate transporter Vglut2 is increased in the thalamus, periaqueductal gray (PAG), and amygdala following SNI [98•]. The anterior cingulate cortex (ACC) shows increased expression of the astrocyte marker glial fibrillary acidic protein (GFAP) following CIPN—whether this is related to neuropathy-induced changes in glutamate and voltage-gated sodium channel expression in the same region remains to be investigated [99, 100]. Expression of the voltage-gated calcium channel Cav3.2 is upregulated in the ACC of rats after chronic constriction injury (CCI)—a finding that corresponds with enhanced T-type calcium currents in ACC neurons. In addition, the microinjection of a T-type calcium channel inhibitor partially relieves mechanical and thermal hypersensitivity post-CCI [101].
Microglial activation occurs in the mouse brain following CCI in regions associated with pain transmission and affect: the thalamus, sensory cortex, and amygdala [102]. Descending facilitation of neuropathic pain from the PAG is promoted by such glial cell activation in a CCI model [103]. The hippocampus has been reported to exhibit impaired long-term potentiation in SNI mice, an effect that was recently suggested to originate from the effects of tumor necrosis factor-alpha and microglial activation in this brain region [104]. This glia-driven change in synaptic plasticity and resultant mechanical hypersensitivity has also been reported in the primary somatosensory cortex in a mouse SNL model [105•].
Electrical stimulation of the thalamus causes spinal serotonin (5-HT) release that relieves neuropathic pain [106], consistent with the observation that intrathecal injection of serotonin can reverse allodynia [107]. The somatosensory cortex is also involved in descending anti-nociception through reducing “on” cell discharge in the rostral ventromedial medulla (RVM) in a 5-HT1A receptor-dependent fashion [108]. Interestingly, the administration of lidocaine to the RVM of SNL rats relieved allodynia in animals exhibiting pain, but precipitated allodynia in rats that had also undergone surgery, but did not exhibit pain-related behaviors [109], consistent with the bi-directional influence of the RVM in descending modulation. Projections from noradrenergic brainstem nuclei such as the locus coeruleus (LC), and other brain regions which project to the LC, are also regarded as mediators of descending pain inhibition [110, 111]. SNL in rats is associated with increased glutamate concentration in the LC and spinal norepinephrine release. These changes are proposed to underlie the impairment of endogenous analgesia following nerve injury [112] and can provide the rationale for the use of serotonin-norepinephrine reuptake inhibitors (SNRIs) in neuropathic pain. These combined data demonstrate a wide range of structural and functional changes occurring within the CNS following peripheral nerve injury. Spontaneous neuronal activity following neuronal disinhibition has been demonstrated in spinal cord and brainstem neurons, although whether this activity may occur in the absence of afferent (even trivial) input still requires further investigation.
Evidence for Central Mechanisms: Clinical
In human studies, features of central sensitization have been evaluated through multiple approaches [113]. Two testable parameters related to dorsal horn-level central sensitization are wind-up (exaggerated response to a train of stimuli) and secondary hyperalgesia (an increase in pain sensitivity to regions surrounding, but not including, the area of injury). In studies of humans with painful neuropathy, including CRPS type II, phantom limb, CIPN, and PHN, both wind-up and secondary hyperalgesia responses are significantly increased. Altered descending inhibition can be interrogated via conditioned pain modulation (CPM) studies, which test the endogenous ability of the CNS to inhibit painful stimuli. Studies comparing healthy volunteers with patients with peripheral polyneuropathy have demonstrated significantly impaired CPM values in painful neuropathy [114].
In patients with peripheral neuropathies, neuroimaging studies have shown multiple changes in activity and functional connectivity in CNS regions involved in pain processing and pain modulation [115, 116]. Neuroimaging of the cortical and subcortical regions in patients with painful neuropathies have identified alterations in activity and functional connectivity that correlate with the subjects’ neuropathic pain characteristics and treatment, including in patients with low back pain [32], PHN [117], diabetic polyneuropathy [118], neuroma pain [119], phantom limb [120], and CRPS [121, 122]. Additionally, structures in the mesencephalic reticular formation (including possibly the PAG and nucleus cuneiformis) that, in preclinical studies, have been shown to be essential to mechanical allodynia after peripheral nerve injury, demonstrate increased neuronal activity on functional neuroimaging in a human capsaicin-evoked secondary hyperalgesia model [123]. Cerebrospinal fluid cytokine levels in neuropathic pain patients have demonstrated increased levels of pain-promoting mediators including TNF-α, IL-6, IL-8, and IL-1β, as well as low levels of pain-decreasing IL-10 [124,125,126], providing further evidence that multiple central processes are responsible for creating a neuropathic pain state.
Recently, Alshelh et al. used resting-state fMRI in orofacial neuropathic pain patients to identify increased infra-slow oscillatory activity in the ascending pain pathway, including the spinal trigeminal nucleus, somatosensory thalamus, thalamic reticular nucleus, and primary somatosensory cortex; this increased oscillatory activity was not seen in control patients without orofacial pain [127]. This rhythm showed increased regional homogeneity in the spinal trigeminal nucleus region, consistent with a local spread of neural activity by astrocytes, and was suggestive of a self-sustaining thalamocortical dysrhythmia. While a variety of imaging studies provide evidence that critical pain pathway CNS components can generate autonomous signals, they provide neither evidence of causality between these oscillations and pain nor evidence that this activity is sustainable without afferent input.
Discussion
In contrast to the growing clinical evidence of peripheral contributions to neuropathic pain maintenance, studies demonstrating the ability of central sensitization mechanisms to independently generate neuropathic pain remain elusive. One key challenge in generating such potential evidence is the absence of agreed terms or criteria for diagnosing the presence of central sensitization in humans. Despite the existing definition (increased responsiveness of nociceptive neurons in the CNS to their normal or subthreshold afferent input), IASP taxonomy also notes that conclusions about the presence of central sensitization can only be made from indirect findings such as hyperalgesia and allodynia. Additional aspects of central sensitization, such as wind-up, long-term potentiation, and increased receptive fields—as well as potential testable criteria such as nociceptive flexion reflex or central sensitization inventory [128]—are not accounted for in the current IASP taxonomy.
Due to the above challenges, the presence of autonomic CNS pain-generating mechanisms could be tested by confirmation of the following hypothesis: “There are cases in which pain that was initiated by a peripheral nerve damage is independently maintained by central mechanisms.” To confirm this hypothesis, the following supporting data would be needed: (1) Evidence of spontaneous activity/firing of CNS neurons which does not occur under normal (non-injured) conditions, (2) causative relationship between this spontaneous/ectopic CNS firing and human pain, and (3) evidence that this spontaneous firing and pain persist despite the removal of afferent input. As of now, we are not aware of evidence confirming these three criteria. Indeed, there is evidence of spontaneous firing in the CNS neurons. The caveat is that some spontaneous activity can occur under non-painful conditions as well. Therefore, the relationship between the spontaneous activity and pain remains associative, and criterion (2) has not been met. Criterion (3) has been refuted in studies blocking peripheral input for a growing number of peripheral neuropathic pain states. Interestingly, this last criterion may also be unmet for central neuropathic pain states; it is yet to be shown whether blocking the peripheral input from areas of perceived spontaneous pain in central neuropathic pain states affect the experience of spontaneous pain.
Conclusions
Peripheral nerve damage provides opportunity for maladaptation at every point along the pain pathway. It is clear that profound CNS changes occur following peripheral nerve injury, and these changes contribute to the central sensitization. There is also evidence of spontaneous activity in CNS neurons after peripheral nerve damage, although this activity does not necessarily persist without afferent input. In peripheral neuropathic pain, effective blockade of afferent input seems to abolish spontaneous pain, even in the presence of signs suggesting central sensitization.
The nature of clinical studies—and the potential need for more definitive, agreed-upon criteria for confirming the clinical presence of central sensitization—has made it challenging to demonstrate the presence of an independent generator of neuropathic pain in the CNS. As a result, the relationship between spontaneous burst activity in the CNS and pain experience still remains associative rather than causative. In comparison, evidence continues to accumulate for the essential role that peripheral signaling plays in generation of neuropathic pain.
All these points together suggest that although many in the scientific community support the autonomous central pain-generating hypothesis, direct clinical evidence supporting this notion is yet to be generated. Therefore, our conclusion at this point in time is that central sensitization acts rather as an amplifier of peripheral signals, and not an independent pain generator in peripheral neuropathic pain conditions.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
• Jensen TS, et al. A new definition of neuropathic pain. Pain. 2011;152(10):2204–5. This paper describes the updated definition of neropathic pain and the rationale for the updated taxonomy
Sheet PNF. National Institute of Neurological Disorders and Stroke (NINDS). 2005.
Finnerup NB, et al. Pharmacotherapy for neuropathic pain in adults: a systematic review and meta-analysis. Lancet Neurol. 2015;14(2):162–73.
Woolf CJ, Mannion RJ. Neuropathic pain: aetiology, symptoms, mechanisms, and management. Lancet. 1999;353(9168):1959–64.
Bouhassira D, et al. Comparison of pain syndromes associated with nervous or somatic lesions and development of a new neuropathic pain diagnostic questionnaire (DN4). Pain. 2005;114(1–2):29–36.
•• Kuner R, Flor H. Structural plasticity and reorganisation in chronic pain. Nat Rev Neurosci. 2016;18(1):20–30. A key review article focusing on maladaptive structural plasticity in neural circuits of pain across animal models and human patients
White FA, Jung H, Miller RJ. Chemokines and the pathophysiology of neuropathic pain. Proc Natl Acad Sci U S A. 2007;104(51):20151–8.
Rowbotham MC, et al. Cutaneous innervation density in the allodynic form of postherpetic neuralgia. Neurobiol Dis. 1996;3(3):205–14.
• Ochoa JL, et al. Hyperexcitable polymodal and insensitive nociceptors in painful human neuropathy. Muscle Nerve. 2005;32(4):459–72. One of the early uses of microneurography to demonstrate spontaneous activity and hyperexcitability in C fibers in patients with painful neuropathy
Reichling DB, Levine JD. Critical role of nociceptor plasticity in chronic pain. Trends Neurosci. 2009;32(12):611–8.
Ratte S, Prescott SA. Afferent hyperexcitability in neuropathic pain and the inconvenient truth about its degeneracy. Curr Opin Neurobiol. 2016;36:31–7.
•• Latremoliere A, Woolf CJ. Central sensitization: A generator of pain hypersensitivity by central neural plasticity. J Pain. 2009;10(9):895–926. A comprehensive review on mechanisms contributing to central sensitization
Novakovic SD, et al. Distribution of the tetrodotoxin-resistant sodium channel PN3 in rat sensory neurons in normal and neuropathic conditions. J Neurosci. 1998;18(6):2174–87.
Bridges D, Thompson SW, Rice AS. Mechanisms of neuropathic pain. Br J Anaesth. 2001;87(1):12–26.
Gaudet AD, Popovich PG, Ramer MS. Wallerian degeneration: gaining perspective on inflammatory events after peripheral nerve injury. J Neuroinflammation. 2011;8:110.
Huang LY, Gu Y, Chen Y. Communication between neuronal somata and satellite glial cells in sensory ganglia. Glia. 2013;61(10):1571–81.
McLachlan EM, et al. Peripheral nerve injury triggers noradrenergic sprouting within dorsal root ganglia. Nature. 1993;363(6429):543–6.
Woolf CJ, Shortland P, Coggeshall RE. Peripheral nerve injury triggers central sprouting of myelinated afferents. Nature. 1992;355(6355):75–8.
Bennett DL, et al. The glial cell line-derived neurotrophic factor family receptor components are differentially regulated within sensory neurons after nerve injury. J Neurosci. 2000;20(1):427–37.
Liu X, Chung K, Chung JM. Ectopic discharges and adrenergic sensitivity of sensory neurons after spinal nerve injury. Brain Res. 1999;849(1–2):244–7.
Cummins TR, Sheets PL, Waxman SG. The roles of sodium channels in nociception: Implications for mechanisms of pain. Pain. 2007;131(3):243–57.
Carter GT, et al. Neuropathic pain in Charcot-Marie-Tooth disease. Arch Phys Med Rehabil. 1998;79(12):1560–4.
Sandkuhler J. Models and mechanisms of hyperalgesia and allodynia. Physiol Rev. 2009;89(2):707–58.
Study RE, Kral MG. Spontaneous action potential activity in isolated dorsal root ganglion neurons from rats with a painful neuropathy. Pain. 1996;65(2–3):235–42.
• Gracely RH, Lynch SA, Bennett GJ. Painful neuropathy: altered central processing maintained dynamically by peripheral input. Pain. 1992;51(2):175–94. A classic read. One of the first clinical reports demonstrating the the blockade of afferent input, even in patients with profound signs of central sensitization, temporarily abolishes neuropathic pain
Woolf CJ. Evidence for a central component of post-injury pain hypersensitivity. Nature. 1983;306(5944):686–8.
Loeser JD, Treede RD. The Kyoto protocol of IASP Basic Pain Terminology. Pain. 2008;137(3):473–7.
Fields HL, Rowbotham M, Baron R. Postherpetic neuralgia: irritable nociceptors and deafferentation. Neurobiol Dis. 1998;5(4):209–27.
Ji RR, Berta T, Nedergaard M. Glia and pain: is chronic pain a gliopathy? Pain. 2013;154(Suppl 1):S10–28.
Sugimoto T, Bennett GJ, Kajander KC. Transsynaptic degeneration in the superficial dorsal horn after sciatic nerve injury: effects of a chronic constriction injury, transection, and strychnine. Pain. 1990;42(2):205–13.
Flor H, et al. Phantom-limb pain as a perceptual correlate of cortical reorganization following arm amputation. Nature. 1995;375(6531):482–4.
Apkarian AV, et al. Chronic back pain is associated with decreased prefrontal and thalamic gray matter density. J Neurosci. 2004;24(46):10410–5.
Colleoni M, Sacerdote P. Murine models of human neuropathic pain. Biochim Biophys Acta. 2010;1802(10):924–33.
Devor M. Ectopic discharge in Abeta afferents as a source of neuropathic pain. Exp Brain Res. 2009;196(1):115–28.
Liu M, Wood JN. The roles of sodium channels in nociception: implications for mechanisms of neuropathic pain. Pain Med. 2011;12(Suppl 3):S93–9.
Devor M. Sodium channels and mechanisms of neuropathic pain. J Pain. 2006;7(1 Suppl 1):S3–S12.
Eijkelkamp N, et al. Neurological perspectives on voltage-gated sodium channels. Brain. 2012;135(Pt 9):2585–612.
Mickle AD, Shepherd AJ, Mohapatra DP. Sensory TRP channels: the key transducers of nociception and pain. Prog Mol Biol Transl Sci. 2015;131:73–118.
Alessandri-Haber N, et al. Transient receptor potential vanilloid 4 is essential in chemotherapy-induced neuropathic pain in the rat. J Neurosci. 2004;24(18):4444–52.
Mickle, A.D., A.J. Shepherd, and D.P. Mohapatra. Nociceptive TRP channels: sensory detectors and transducers in multiple pain pathologies. Pharmaceuticals (Basel). 2016; 9(4).
Tsantoulas C, McMahon SB. Opening paths to novel analgesics: the role of potassium channels in chronic pain. Trends Neurosci. 2014;37(3):146–58.
Ren K, Dubner R. Interactions between the immune and nervous systems in pain. Nat Med. 2010;16(11):1267–76.
Dray A. Neuropathic pain: emerging treatments. Br J Anaesth. 2008;101(1):48–58.
Nystrom B, Hagbarth KE. Microelectrode recordings from transected nerves in amputees with phantom limb pain. Neurosci Lett. 1981;27(2):211–6.
Dib-Hajj SD, et al. Gain-of-function mutation in Nav1.7 in familial erythromelalgia induces bursting of sensory neurons. Brain. 2005;128(Pt 8):1847–54.
Khaliq W, Alam S, Puri N. Topical lidocaine for the treatment of postherpetic neuralgia. Cochrane Database Syst Rev. 2007;2:CD004846.
Galer BS, et al. Topical lidocaine patch relieves postherpetic neuralgia more effectively than a vehicle topical patch: results of an enriched enrollment study. Pain. 1999;80(3):533–8.
• Haroutounian S, et al. Primary afferent input critical for maintaining spontaneous pain in peripheral neuropathy. Pain. 2014;155(7):1272–9. A systematic assessment of the effect of afferent input blockade (with a local anesthetic) in two populations of peripheral neuropathic pain patients
Finnerup NB, et al. The sodium-channel blocker lidocaine in subanesthetic concentrations reduces spontaneous and evoked pain in human painful neuroma. Scandanavian Journal of Pain. 2015;8:45–6.
Miclescu A, et al. Differential analgesic effects of subanesthetic concentrations of lidocaine on spontaneous and evoked pain in human painful neuroma: A randomized, double blind study. Scandanavian Journal of Pain. 2015;8:37–44.
Wijayasinghe N, et al. Ultrasound guided Intercostobrachial nerve blockade in patients with persistent pain after breast cancer surgery: a pilot study. Pain Physician. 2016;19(2):E309–18.
Wijayasinghe N, et al. The role of peripheral afferents in persistent inguinal postherniorrhaphy pain: a randomized, double-blind, placebo-controlled, crossover trial of ultrasound-guided tender point blockade. Br J Anaesth. 2016;116(6):829–37.
Slavin KV. Peripheral nerve stimulation for neuropathic pain. Neurotherapeutics. 2008;5(1):100–6.
Wall PD, Sweet WH. Temporary abolition of pain in man. Science. 1967;155(3758):108–9.
Waisbrod H, et al. Direct nerve stimulation for painful peripheral neuropathies. J Bone Joint Surg Br. 1985;67(3):470–2.
Eisenberg E, Waisbrod H, Gerbershagen HU. Long-term peripheral nerve stimulation for painful nerve injuries. Clin J Pain. 2004;20(3):143–6.
Yakovlev AE, Peterson AT. Peripheral nerve stimulation in treatment of intractable postherpetic neuralgia. Neuromodulation. 2007;10(4):373–5.
• Vaso A, et al. Peripheral nervous system origin of phantom limb pain. Pain. 2014;155(7):1384–91. Clinical demonstration of phantom pain alleviation by DRG blockade with local anesthetics, even in dilute concentrations. An important paper on the role of the dorsal root ganglion as a generator of post-amputation phantom and stump pain
Liem L, et al. One-year outcomes of spinal cord stimulation of the dorsal root ganglion in the treatment of chronic neuropathic pain. Neuromodulation. 2015;18(1):41–8. discussion 48-9
Eldabe S, et al. Dorsal root ganglion (DRG) stimulation in the treatment of phantom limb pain (PLP). Neuromodulation. 2015;18(7):610–6. discussion 616-7
Liem L, et al. The dorsal root ganglion as a therapeutic target for chronic pain. Reg Anesth Pain Med. 2016;41(4):511–9.
Choi SR, et al. Spinal D-serine increases PKC-dependent GluN1 phosphorylation contributing to the sigma-1 receptor-induced development of mechanical allodynia in a mouse model of neuropathic pain. J Pain, 2016.
Hildebrand ME, et al. Potentiation of synaptic GluN2B NMDAR currents by Fyn kinase is gated through BDNF-mediated disinhibition in spinal pain processing. Cell Rep. 2016;17(10):2753–65.
Kiyoyuki Y, et al. Leukotriene enhances NMDA-induced inward currents in dorsal horn neurons of the rat spinal cord after peripheral nerve injury. Mol Pain. 2015;11:53.
Peirs C, et al. Dorsal horn circuits for persistent mechanical pain. Neuron. 2015;87(4):797–812.
Wang HS, et al. Changes in VGLUT1 and VGLUT2 expression in rat dorsal root ganglia and spinal cord following spared nerve injury. Neurochem Int. 2016;99:9–15.
Yamamoto K, et al. Oxaliplatin administration increases expression of the voltage-dependent calcium channel alpha2delta-1 subunit in the rat spinal cord. J Pharmacol Sci. 2016;130(2):117–22.
Guo W, et al. Spinal 5-HT3 receptors mediate descending facilitation and contribute to behavioral hypersensitivity via a reciprocal neuron-glial signaling cascade. Mol Pain. 2014;10:35.
Zhou LJ, et al. Brain-derived neurotrophic factor contributes to spinal long-term potentiation and mechanical hypersensitivity by activation of spinal microglia in rat. Brain Behav Immun. 2011;25(2):322–34.
Chen JT, et al. Presynaptic GABAergic inhibition regulated by BDNF contributes to neuropathic pain induction. Nat Commun. 2014;5:5331.
Ferrini F, et al. Morphine hyperalgesia gated through microglia-mediated disruption of neuronal Cl(-) homeostasis. Nat Neurosci. 2013;16(2):183–92.
• Keller AF, et al. Transformation of the output of spinal lamina I neurons after nerve injury and microglia stimulation underlying neuropathic pain. Mol Pain. 2007;3:27. An elegant demonstration of spontaneous activity of dorsal horn neurons (projecting to the parabrachial nucleus) in rodents with peripheral nerve injury and the role of microglia in spinal cord sensitization
Coull JA, et al. BDNF from microglia causes the shift in neuronal anion gradient underlying neuropathic pain. Nature. 2005;438(7070):1017–21.
Imlach WL, et al. Glycinergic dysfunction in a subpopulation of dorsal horn interneurons in a rat model of neuropathic pain. Sci Rep. 2016;6:37104.
Lyu C, et al. G protein-gated inwardly rectifying potassium channel subunits 1 and 2 are down-regulated in rat dorsal root ganglion neurons and spinal cord after peripheral axotomy. Mol Pain. 2015;11:44.
Xu T, et al. Epigenetic upregulation of CXCL12 expression mediates anti-tubulin chemotherapeutics-induced neuropathic pain. Pain, 2017.
Xie F, et al. Early repeated administration of CXCR4 antagonist AMD3100 dose-dependently improves neuropathic pain in rats after L5 spinal nerve ligation. Neurochem Res. 2016;41(9):2289–99.
Luo X, et al. Crosstalk between astrocytic CXCL12 and microglial CXCR4 contributes to the development of neuropathic pain. Mol Pain. 2016;12
Jiang BC, et al. CXCL13 drives spinal astrocyte activation and neuropathic pain via CXCR5. J Clin Invest. 2016;126(2):745–61.
• Sun S, et al. Role of interleukin-4, the chemokine CCL3 and its receptor CCR5 in neuropathic pain. Mol Immunol. 2016;77:184–92. This paper illustrates a neuronal/astrocytic interaction in the spinal cord following peripheral nerve injury wherein neuron-derived CXCL13 acts on astrocytes via CXCR5 to facilitate neuropathic pain
Kwiatkowski K, et al. Beneficial properties of maraviroc on neuropathic pain development and opioid effectiveness in rats. Prog Neuro-Psychopharmacol Biol Psychiatry. 2016;64:68–78.
Piotrowska A, et al. Maraviroc reduces neuropathic pain through polarization of microglia and astroglia—evidence from in vivo and in vitro studies. Neuropharmacology. 2016;108:207–19.
Nazemi S, et al. Inhibition of microglial activity alters spinal wide dynamic range neuron discharge and reduces microglial Toll-like receptor 4 expression in neuropathic rats. Clin Exp Pharmacol Physiol. 2015;42(7):772–9.
Yamamoto Y, et al. Activated microglia contribute to convergent nociceptive inputs to spinal dorsal horn neurons and the development of neuropathic pain. Neurochem Res. 2015;40(5):1000–12.
Terayama R, et al. Peripheral nerve injury activates convergent nociceptive input to dorsal horn neurons from neighboring intact nerve. Exp Brain Res. 2015;233(4):1201–12.
Obata H, et al. Activation of astrocytes in the spinal cord contributes to the development of bilateral allodynia after peripheral nerve injury in rats. Brain Res. 2010;1363:72–80.
Sun C, et al. IL-17 contributed to the neuropathic pain following peripheral nerve injury by promoting astrocyte proliferation and secretion of proinflammatory cytokines. Mol Med Rep. 2017;15(1):89–96.
Yao CY, et al. Interleukin-17A acts to maintain neuropathic pain through activation of CaMKII/CREB signaling in spinal neurons. Mol Neurobiol. 2016;53(6):3914–26.
Choi BM, et al. The time-course and RNA interference of TNF-alpha, IL-6, and IL-1beta expression on neuropathic pain induced by L5 spinal nerve transection in rats. Korean J Anesthesiol. 2015;68(2):159–69.
Masuda, T., et al., Dorsal horn neurons release extracellular ATP in a VNUT-dependent manner that underlies neuropathic pain. 2016. 7: p. 12529.
McGaraughty S, et al. P2X7-related modulation of pathological nociception in rats. Neuroscience. 2007;146(4):1817–28.
Koyanagi S, et al. Glucocorticoid regulation of ATP release from spinal astrocytes underlies diurnal exacerbation of neuropathic mechanical allodynia. Nat Commun. 2016;7:13102.
Cirillo G, et al. Purinergic modulation of spinal neuroglial maladaptive plasticity following peripheral nerve injury. Mol Neurobiol. 2015;52(3):1440–57.
• Okubo M, et al. Macrophage-colony stimulating factor derived from injured primary afferent induces proliferation of spinal microglia and neuropathic pain in rats. PLoS One. 2016;11(4):e0153375. This study demonstrates that enhanced expression of M-CSF in spinal microglia and sensory afferents following nerve injury is sufficient to induce microgliosis and mechanical allodynia
• Gu N, et al. Spinal microgliosis due to resident microglial proliferation is required for pain hypersensitivity after peripheral nerve injury. Cell Rep. 2016;16(3):605–14. The authors use transgenic reporter mice in a spinal nerve transection model to show that injury-induced microgliosis in the spine results exclusively from local microglial proliferation, rather than infiltrating monocytes
Peng J, et al. Microglia and monocytes synergistically promote the transition from acute to chronic pain after nerve injury. Nat Commun. 2016;7:12029.
Patel R, Dickenson AH. Neuronal hyperexcitability in the ventral posterior thalamus of neuropathic rats: modality selective effects of pregabalin. J Neurophysiol. 2016;116(1):159–70.
• Wang ZT, et al. Changes in VGLUT2 expression and function in pain-related supraspinal regions correlate with the pathogenesis of neuropathic pain in a mouse spared nerve injury model. Brain Res. 2015;1624:515–24. An increase in evoked responses to mechanical and cooling stimuli in ventral posterior thalamic neurons was reported in a rat spinal nerve ligation model, along with an increase in the rate of spontaneous firing, a modification proposed to contribute to ongoing pain
Masocha W. Astrocyte activation in the anterior cingulate cortex and altered glutamatergic gene expression during paclitaxel-induced neuropathic pain in mice. PeerJ. 2015;3:e1350.
Masocha W. Gene expression profile of sodium channel subunits in the anterior cingulate cortex during experimental paclitaxel-induced neuropathic pain in mice. PeerJ. 2016;4:e2702.
Shen FY, et al. Alleviation of neuropathic pain by regulating T-type calcium channels in rat anterior cingulate cortex. Mol Pain. 2015;11:7.
Taylor AM, et al. Topography of microglial activation in sensory- and affect-related brain regions in chronic pain. J Neurosci Res, 2016.
Ni HD, et al. Glial activation in the periaqueductal gray promotes descending facilitation of neuropathic pain through the p38 MAPK signaling pathway. J Neurosci Res. 2016;94(1):50–61.
Liu, Y., et al. TNF-alpha differentially regulates synaptic plasticity in the hippocampus and spinal cord by microglia-dependent mechanisms after peripheral nerve injury. J Neurosci. 2016.
• Kim SK, et al. Cortical astrocytes rewire somatosensory cortical circuits for peripheral neuropathic pain. J Clin Invest. 2016;126(5):1983–97. Following sciatic nerve ligation, the authors detect a re-emergence of ‘immature’ mGluR5 signaling in astrocytes in the somatosensory cortex, a change thought to contribute to changes in synaptic plasticity and mechanical allodynia
Sorkin LS, McAdoo DJ, Willis WD. Stimulation in the ventral posterior lateral nucleus of the primate thalamus leads to release of serotonin in the lumbar spinal cord. Brain Res. 1992;581(2):307–10.
Avila-Rojas SH, et al. Role of spinal 5-HT5A, and 5-HT1A/1B/1D, receptors in neuropathic pain induced by spinal nerve ligation in rats. Brain Res. 2015;1622:377–85.
Sagalajev, B., et al., Descending antinociception induced by secondary somatosensory cortex stimulation in experimental neuropathy: role of the medullospinal serotonergic pathway. J Neurophysiol. 2017; p. jn.00836.2016.
De Felice M, et al. Engagement of descending inhibition from the rostral ventromedial medulla protects against chronic neuropathic pain. Pain. 2011;152(12):2701–9.
Viisanen H, Pertovaara A. Antinociception by motor cortex stimulation in the neuropathic rat: does the locus coeruleus play a role? Exp Brain Res. 2010;201(2):283–96.
Wei H, et al. Histamine in the locus coeruleus promotes descending noradrenergic inhibition of neuropathic hypersensitivity. Pharmacol Res. 2014;90:58–66.
Kimura M, et al. Impaired pain-evoked analgesia after nerve injury in rats reflects altered glutamate regulation in the locus coeruleus. Anesthesiology. 2015;123(4):899–908.
Woolf CJ. Central sensitization: implications for the diagnosis and treatment of pain. Pain. 2011;152(3 Suppl):S2–15.
Tuveson B, Leffler AS, Hansson P. Heterotopic noxious conditioning stimulation (HNCS) reduced the intensity of spontaneous pain, but not of allodynia in painful peripheral neuropathy. Eur J Pain. 2007;11(4):452–62.
Moisset X, Bouhassira D. Brain imaging of neuropathic pain. NeuroImage. 2007;37(Suppl 1):S80–8.
Seifert F, Maihofner C. Central mechanisms of experimental and chronic neuropathic pain: findings from functional imaging studies. Cell Mol Life Sci. 2009;66(3):375–90.
Geha PY, et al. Brain activity for spontaneous pain of postherpetic neuralgia and its modulation by lidocaine patch therapy. Pain. 2007;128(1–2):88–100.
Casseb RF, et al. Spinal cord diffusion tensor imaging in patients with sensory neuronopathy. Neuroradiology. 2016;58(11):1103–8.
Casey KL, Lorenz J, Minoshima S. Insights into the pathophysiology of neuropathic pain through functional brain imaging. Exp Neurol. 2003;184(Suppl 1):S80–8.
Karl A, et al. Reorganization of motor and somatosensory cortex in upper extremity amputees with phantom limb pain. J Neurosci. 2001;21(10):3609–18.
Simons LE, et al. The responsive amygdala: treatment-induced alterations in functional connectivity in pediatric complex regional pain syndrome. Pain. 2014;155(9):1727–42.
Apkarian AV, et al. Prefrontal cortical hyperactivity in patients with sympathetically mediated chronic pain. Neurosci Lett. 2001;311(3):193–7.
Zambreanu L, et al. A role for the brainstem in central sensitisation in humans. Evidence from functional magnetic resonance imaging. Pain. 2005;114(3):397–407.
Alexander GM, et al. Changes in cerebrospinal fluid levels of pro-inflammatory cytokines in CRPS. Pain. 2005;116(3):213–9.
Kotani N, et al. Cerebrospinal fluid interleukin 8 concentrations and the subsequent development of postherpetic neuralgia. Am J Med. 2004;116(5):318–24.
Backonja MM, et al. Altered cytokine levels in the blood and cerebrospinal fluid of chronic pain patients. J Neuroimmunol. 2008;195(1–2):157–63.
Alshelh Z, et al. Chronic neuropathic pain: it’s about the rhythm. J Neurosci. 2016;36(3):1008–18.
Neblett R, et al. The central sensitization inventory (CSI): establishing clinically significant values for identifying central sensitivity syndromes in an outpatient chronic pain sample. J Pain. 2013;14(5):438–45.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Kathleen Meacham declares training grant funding that provides part of her salary and involves research on painful neuropathies, but is otherwise unrelated to this manuscript, from the NIH - NIDDK T32 DK108742 01 IMAGING, MODELING AND ENGINEERING OF DIABETIC TISSUES.
Andrew Shepherd declares employment with and travel and accommodation expenses covered by Washington University School of Medicine.
Durga P. Mohapatra declares grant funding to conduct basic research in pain neurobiology from the National Institutes of Health (NIH), USA. Research grant no. NS069898.
Simon Haroutounian declares the ASPIRE neuropathic pain grant funding to his institution from Pfizer Inc. and travel reimbursement for NeuPSIG committee meeting from IASP.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Neuropathic Pain
Rights and permissions
About this article
Cite this article
Meacham, K., Shepherd, A., Mohapatra, D.P. et al. Neuropathic Pain: Central vs. Peripheral Mechanisms. Curr Pain Headache Rep 21, 28 (2017). https://doi.org/10.1007/s11916-017-0629-5
Published:
DOI: https://doi.org/10.1007/s11916-017-0629-5