Abstract
Purpose of review
The goal of this review is to gain a better understanding of marrow adipocyte development, its regulation of energy, and its characterization responsible for bone homeostasis.
Recent findings
Despite major advances in uncovering the complex association of bone-fat in the marrow, the underlying basic biological process of adipose tissue development, as well as its interaction with bone homeostasis in pathophysiological conditions, is still not well understood.
Summary
This review identifies many pro- and anti-osteogenic factors secreted by adipocytes to play a role in the manipulating the fate of mesenchymal stem cells as well as the osteoblastic activity during bone remodeling. It also addresses the function of adipose tissue capable of negative regulation of the hematopoietic microenvironment to influence the bone quantity and the nature of bone homeostasis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adipocytes are a significant component of the bone marrow, and in recent years, the understanding of their complex physiological role is emerging. There is growing evidence that adipocytes in the bone marrow are not only functioning as energy storage but also as paracrine and endocrine cells capable of modifying bone homeostasis. The bone marrow adipose tissue is functionally distinct adipose depot, located within the skeleton, with the potential to contribute to both local and systemic metabolism and makes up to 5% of total fat mass in adults [1]. Most adipose tissue in adult humans is white adipose tissue, approximately 85% of total adipose tissue, consisting of subcutaneous depots in the abdominal body parts; and brown adipose tissue, visceral fat depots approximately 10%. While classical unilocular white adipocytes are thought to serve mainly as an energy reservoir and can store vast amounts of lipid, multilocular (rich in mitochondria) brown adipocytes are able to dissipate nutrients through the uncoupling protein-1 in order to produce heat in response to cold stress and their high glucose uptake and oxidative capacities make them key players in the energy balance [2]. Bone has been revealed as a target and a regulator of characteristics consistent neither with white nor brown fat, and the marrow adipocytes are likely to be heterogeneous.
The aim of this review an understanding of marrow adipocyte development, its regulation of energy and its characterization responsible for bone homeostasis, to identify many pro- and anti-osteogenic factors secreted by adipocytes that play a role in the manipulating the generation of osteoblasts, bone-forming cells, as well as the osteoblastic activity during bone remodeling. It also addresses the function of adipose tissue capable of modifying immune response to influence bone quantity and the nature of bone homeostasis.
Anatomy and of Bone Marrow Adipose Tissue
The distribution of marrow, volume ratio, as well as appearance of marrow adipocytes vary between species. In human, adipocytes represent up to 45% of the cellular components in hematopoietic or red marrow and up to 90% of adipocyte-rich yellow marrow [3••]. Human marrow adipocytes accumulate continuously within the long bone from diaphysis to metaphysis and in direction from appendicular to axial skeleton during growth and aging [4]. While, in mice fed high-fat diet adiposity increases in the proximal tibiae [5] but not in distal tibia [6].
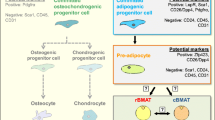
Marrow adipocytes may be unique in their surface markers and have a distinctive phenotype, beige phenotype, representing a combination of several cell types such as white and brown fat cells. All the adipocytes in the marrow express peroxisome proliferator-activated receptor (PPARγ), and they secret various signaling molecules including adipokines, FOXC2, Wnt, insulin-like growth factors, BMP, MCP-1, uncoupling protein-1, preadipocyte factor 1, and inflammatory factors [3••, 7]. It has also been demonstrated that higher beige adipocyte number (based on the expression of the marker genes) is associated with higher trabecular bone mass and is attenuated with aging and in diabetes, suggesting this phenotype of marrow adipocytes may have a positive effect on bone metabolism via endocrine, paracrine, and autocrine signals. This effect on bone will be determined by the heterogeneity of marrow adipocytes in their metabolic phenotype diversity and distribution [3••].
Developmental Origin of Marrow Adipocytes
Mesenchymal stromal cells in bone marrow have the potential to differentiate into different types of cells including osteoblasts and adipocytes. Steering the different destination is not only determined by the availability of this common progenitor population but also the regulatory signals to activate one terminally differentiated cell type lineage but suppress another phenotype. Inhibition of PPARγ gene expression, a key regulator of adipocyte differentiation, in mice reduced marrow adiposity together with increased bone formation and osteoblastogenesis from bone marrow progenitor cells [8]. Meanwhile, overexpression of PPARγ in the bone marrow progenitor cells of transgenic mice results in increased adipogenesis [9]. These studies indicate there exists a PPARγ-dependent regulation of bone metabolism in vivo. The Cbfβ gene, a non-DNA-binding partner of Runt-related transcription factors, was deleted from osteoblasts at different lineage stages in transgenic mice; these mice exhibited severe osteopenia with abundant accumulation of marrow adipocytes, which can be rescued by Cbfβ overexpression. It suggests that osteoblast differentiation from marrow mesenchymal stem cells is non-autonomously controlled by Cbfβ via enhancing β-catenin signaling to maintain osteoblast lineage commitment and suppress adipogenesis gene expression. Mesenchymal stem cells and osteoblasts in bone marrow can be programed and reprogramed, respectively, into adipocytes under Cbfβ-deficient conditions [10••]. Nevertheless, the conception of skew differentiation of osteoblastogenesis at the expense of adipogenesis is contrary to a study investigated by Post et al. [11]. Their findings suggest that clonal subpopulations of progenitor cells committed to either osteoblast or adipocyte lineage persist in bone marrow and undergo their respective cell development and differentiation during aging and in metabolic bone disease. Most adipocytes in the body can develop from adipose tissue-resident progenitors, and a report demonstrated that engrafted marrow-derived cells also generate new adipocytes within white adipose tissue, suggesting that the bone marrow likely consists of a heterogeneous population of adipocyte precursors at various stages of commitment to white or brown-adipocyte lineages [12]. A myogenic lineage marker, myogenic factor 5 (Myf5), gives rise to developmentally programmed brown but not white adipocyte differentiation and PRDM16, a positive transcriptional regulator PR-domain zinc-finger protein, has the ability to control a brown-adipocyte cell fate in Myf5-expressing progenitors in a cell-autonomous manner [13].
Bone Marrow Adipocytes as an Endocrine/Paracrine Organ in Regulation of Bone Homeostasis
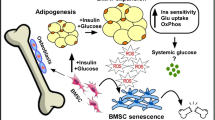
Osteoblasts and adipocytes share a common mesenchymal precursor, as described above. The activation of PPARγ in bone marrow stem cells stimulates adipogenesis while inhibiting osteoblastogenesis [8]. Interestingly, it has been recently uncovered that adipocytes can also influence osteoclasts, bone-resorbing cells, derived from the hematopoietic precursor lineage. The activation of PPARγ and its ligands can promote osteoclast differentiation and bone resorption functions through their direct regulation of c-fos expression, an essential mediator of osteoclastogenesis [14]. The coexistence of adipocytes, osteoblasts, and osteocytes in the bone marrow provide the possibility that adipocytes regulate bone homeostasis through paracrine and endocrine mechanisms, such as leptin and adiponectin, as well as adipose-derived estrogen within bone marrow microenvironment, which influence osteogenic cells function. The high expression of leptin by marrow adipocytes and leptin receptor isoform in human and animal osteoblasts suggest the direct effect of leptin on bone metabolism [15, 16]. Leptin when administered peripherally [17] and in genetically modified animals [18] demonstrates that leptin increases bone formation and decreases bone resorption. But in human epidemiological studies, the correlation of circulating leptin levels with bone mass and fracture risk are not conclusive [19, 20]. Some in vitro studies indicate leptin enhances osteoblastic proliferation and differentiation while inhibiting adipogenic differentiation from marrow mesenchymal stromal cells [21]. When peripherally acting on bone, leptin acts as a positive regulator of osteogenesis by increasing bone mineral density and bone formation rate while decreasing marrow adipogenesis in the number and the size [22]. On the contrary, when leptin is injected directly into the central nervous system or given in very high doses (300 times) peripherally, there is a substantial reduction in body weight, and the number and the size of marrow adipocytes increase, as a result of leptin effects on appetite in the hypothalamus, and then reduced bone formation results [23] (Fig. 1).
Interactions between adipocytes and bone cells as well as immune cells in the regulation of bone metabolism in the bone marrow cavity. Multiple mechanisms potentially underlie adipokines’ activity in bone via specific receptors: local direct effects of adipokines secreted from bone marrow adipocytes and the peripheral circulation and indirect effects through modulation of the sympathetic tone and the regulation of insulin sensitivity and energy homeostasis. Bone marrow adipocytes reduce osteogenic differentiation potential of mesenchymal stem cells while stimulating adipogenic differentiation from these cells. Furthermore, bone marrow adipocytes negatively affect B lymphopoiesis and induce an imbalance toward excessive osteolytic activity due to the lack of RANKL inhibition by OPG. Pro-inflammatory factors from bone marrow adipocytes are closely involved in innate immune activation and impose a negative impact on bone metabolism. Adipokines from bone marrow adipocytes also recruit pro-inflammatory adipose tissue macrophages (ATMs) which are involved in obesity-associated adipose tissue inflammation and favor osteoclast differentiation and bone resorption, while meantime, inhibiting osteogenic differentiation and the synthesis of bone matrix
Adiponectin secreted by adipocytes acts as an important regulator of metabolic homeostasis. Adiponectin and its receptors have been determined to be expressed by bone cells including osteoblast and osteoclasts [24, 25]. According to the data from a Health, Aging, and Body Composition study, adiponectin levels, but not leptin, were found in association with fracture risk among 3075 men and women, aged 70–79, suggesting elevated adiponectin may be an increased risk for fracture independent of bone mineral density and body composition [26]. The clinical condition of anorexia where there is an accumulation of marrow adipocytes also results in an increased circulating adiponectin level [27]. In addition, ectopic adiposity and levels of free fatty acids are increased with aging and obesity [28, 29]. Bone marrow adipocytes exert detrimental effect on osteoblasts by releasing fatty acids as well as adipokines [30]. Altered adiponectin secretion with increased pro-inflammatory cytokines was associated with increased hip bone loss in obese and overweight women [26]. Nevertheless, local intermittent administration of adiponectin to the mandibular osteodistraction site resulted in significant increase in intramembranous bone formation and the overall rate of bone regeneration [31]. Meanwhile, adiponectin signals in neurons of the locus coeruleus, also through FoxO1, to decrease the sympathetic tone in osteoblasts thereby increasing bone mass and preventing age-related bone loss [32]. The average number of bone marrow adipocytes in distal femur of adiponectin knockout male mice at 37 weeks of age was significantly higher than wild type mice, but no difference was found in the total adipocyte area of the two groups at all ages. These APN-KO mice had reduced cortical area fraction and average cortical thickness in all the age groups [33]. Observational studies in clinics only describe the associations between bone and adiponectin levels, but it is hard to draw conclusions about causal connections. In addition, multiple mechanisms potentially influence the role of adiponectin in bone: local direct paracrine effects of adiponectin secreted from bone marrow adipocytes on bone cells (Fig. 1), indirect endocrine effects of circulating adiponectin secreted from white adipose tissue through the modulation of the sympathetic tone and insulin sensitivity as well as energy homeostasis [34].
Bone Marrow Adipocytes Effects on Bone Homeostasis Via Negative Regulation of the Hematopoietic Microenvironment
Bone marrow cavity mainly contains a high volumetric proportion of adipocytes and the majority of the hematopoietic stem cells which produce the three classes of blood cells: red blood cells (erythrocytes), platelets (thrombocytes), and white blood cells (leukocytes). In the bone marrow cavity, adipocytes, leukocytes, mesenchymal cells, osteoblasts, and endothelial cells are assembled in an organized network to maintain the homeostatic microenvironment of bone marrow and support hematopoiesis. The expansion of hematopoietic cells is reduced as a consequence of co-culture with bone marrow-derived adipocytes in transwells, and the inhibition of bone marrow adipocyte formation in vivo promote hematopoietic reconstitution and higher leukocyte formation, indicating that adipocytes release diffusible inhibitors of hematopoiesis and leukocytogenesis. Interestingly, only simultaneous ablation of both the adipocytic and hematopoietic compartments is accompanied by marked osteogenesis. These data suggest that bone marrow adipocytes regulate bone metabolism through the hematopoietic inductive microenvironment [35]. The association of activation of the immune system and local bone loss has been recognized, and the understanding of interaction between adipocyte inflammation and bone homeostasis can lead to the understanding of functional changes of marrow fat occurring with pathological conditions and treatment of bone loss [36].
Numerous white blood cells including macrophages, leukocytes (B cells, T cells, and NK cells), and neutrophils have been identified in adipose tissue. B and T leukocytes express leptin receptor and leptin signaling deficiency impairs humoral and cellular immune responses, which suggest that leptin modulate T and B cell-mediated immune responses [37]. B cells differentiate from hematopoietic stem cells in bone marrow which is also involved in the maturation and residence of B cells. Adipocytes from bone marrow can reduce significantly the self-renewal capacity of hematopoietic stem cells compared with other types of stromal cells in an in vitro cell co-culture system. High-fat diet in vivo also disrupts the hematopoietic supportive capacity and rapidly suppresses B lymphopoiesis [38••]. Paracrine factors secreted by bone marrow adipocyte inhibit B lymphopoiesis in vitro by compromising the proliferation and maturation of lymphoid committed progenitors [39]. Normal bone mass acquisition depends on bone cell homeostasis maintained by the balanced functions of the receptor activator of nuclear factor–κB ligand (RANKL)/osteoprotegerin (OPG) signaling. OPG produced and secreted by mature-activated B cells and T cells, through CD40 ligand (CD40L) to CD40 co-stimulation, coordinates the process of osteoclast-mediated bone resorption and osteoblast-mediated bone formation. The lack of OPG production from B cells can lead to the imbalance of this system resulting in excessive osteolytic activity and consequent skeletal disease [40]. It indicates that leukocytes are critical for the preservation of bone homeostasis and bone marrow adipocytes exert a negative effect on B cells and bone metabolism (Fig. 1).
The majority of T cells presents in the bone marrow display memory and activation status and serve as a reservoir for memory T cells. T cell subsets have been shown to involve in the process of osteoclastogenesis and alter bone metabolism. Tumor necrosis factor alpha produced by the increased bone marrow CD4 (+) T cells mainly account for osteoclastic bone resorption in vivo induced by estrogen deficiency [41]. The adipose tissues from obese populations are infiltrated with CD4 and CD8 T cells. T cell profiles in two pro-inflammatory T-helper cells, Th1 and Th2, are highly involved in “cell-mediated” immunity and insulin resistance [42]. Leptin has an intrathymic role in promoting the production of thymocytes, which later become T cells [43]. Obese ob−/ob− (leptin deficient) mice have T cell deficiency and show atrophy of lymphoid organs [44]. Lipids released from adipocytes can modulate CD4 (+) T cell function and lead to an accumulation of these cells in adipose tissue [45]. Pro-inflammatory cytokines such as interleukin-1β (IL-1β), interleukin 6 (IL-6), tumor necrosis factor alpha (TNF-α), and nuclear factor-κβ (NF-κB) released by these T cell subsets initiates a pro-inflammatory cascade and subsequently contributes to osteoclastic bone resorption [46, 47]. Thus, these results suggest the excessive secretion of leptin in obesity from marrow adipocytes might enhance T cell response and impose a negative impact on bone metabolism. Marrow adipocytes were found to express their own higher levels of inflammatory response genes than visceral adipocytes, such as TNF-alpha, transforming growth factor beta 1 and IL-6, thus adipose-derived signaling can directly influence bone homeostasis [48]. Leptin signaling in bone marrow also give rise to pro-inflammatory recruited adipose tissue macrophages (ATMs) which are involved in obesity-associated adipose tissue inflammation [49]. ATMs are of the M1, or classically activated, phenotype and are responsible for the majority of adipose tissue-derived TNF-α and IL-6 expression as well as nitric oxide synthase [50]. M1 macrophages have been associated with the inhabitation of osteogenic differentiation, mineralization, and the synthesis of skeletal matrix protein [51, 52] (Fig. 1).
Conclusions
Growing evidence demonstrates that adipocytes in the bone marrow are functioning as energy storage as well as paracrine and endocrine cells capable of modifying bone homeostasis. Marrow adipocytes, bone cells, as well as immune cells act synergistically to maintain bone metabolism in the bone marrow cavity. Adipokines from marrow adipocytes play a role in the manipulating the fate of mesenchymal stem cells as well as the osteoblastic activity during bone remodeling via direct and indirect effects. Marrow adipocytes also impose negative regulation of the hematopoietic microenvironment to influence the bone quantity and the nature of bone homeostasis. Despite major advances in uncovering the complex association of bone-fat in the marrow, the underlying basic biological process of adipose tissue development, as well as its interaction with bone homeostasis in pathophysiological conditions, is still not well understood. Further understanding of the complex role of marrow adipocytes in bone metabolism may help to improve the efficacy of abnormal skeletal status during aging and in certain bone metabolic disorders, and open new therapeutic targets for bone regenerative medicine.
References
Papers of particular interest, published recently, have been highlighted as: •• Of major importance
Ghali O, Al RN, Hardouin P, Chauveau C. Increased bone marrow adiposity in a context of energy deficit: the tip of the iceberg? Front Endocrinol (Lausanne). 2016;7:125. https://doi.org/10.3389/fendo.2016.00125.
Hardouin P, Rharass T, Lucas S. Bone marrow adipose tissue: to be or not to be a typical adipose tissue? Front Endocrinol. 2016;7:85. https://doi.org/10.3389/fendo.2016.00085.
•• Lecka-Czernik B, Stechschulte LA, Czernik PJ, Sherman SB, Huang S, Krings A. Marrow adipose tissue: skeletal location, sexual dimorphism, and response to sex steroid deficiency. Front Endocrinol. 2017;8:188. https://doi.org/10.3389/fendo.2017.00188. The paper reveals the close relationship exists between bone marrow beige adipocytes and bone mass in limbs and sex steroid deficiency also impacts this positive correlation.
Baum T, Cordes C, Dieckmeyer M, Ruschke S, Franz D, Hauner H, et al. MR-based assessment of body fat distribution and characteristics. Eur J Radiol. 2016;85(8):1512–8. https://doi.org/10.1016/j.ejrad.2016.02.013.
Bartelt A, Beil FT, Schinke T, Roeser K, Ruether W, Heeren J, et al. Apolipoprotein E-dependent inverse regulation of vertebral bone and adipose tissue mass in C57Bl/6 mice: modulation by diet-induced obesity. Bone. 2010;47(4):736–45. https://doi.org/10.1016/j.bone.2010.07.002.
Scheller EL, Cawthorn WP, Burr AA, Horowitz MC, MacDougald OA. Marrow adipose tissue: trimming the fat. Trends Endocrinol Metab. 2016;27(6):392–403. https://doi.org/10.1016/j.tem.2016.03.016.
Krings A, Rahman S, Huang S, Lu Y, Czernik PJ, Lecka-Czernik B. Bone marrow fat has brown adipose tissue characteristics, which are attenuated with aging and diabetes. Bone. 2012;50(2):546–52. https://doi.org/10.1016/j.bone.2011.06.016.
Akune T, Ohba S, Kamekura S, Yamaguchi M, Chung UI, Kubota N, et al. PPARgamma insufficiency enhances osteogenesis through osteoblast formation from bone marrow progenitors. J Clin Invest. 2004;113(6):846–55. https://doi.org/10.1172/JCI19900.
Tontonoz P, Hu E, Spiegelman BM. Stimulation of adipogenesis in fibroblasts by PPAR gamma 2, a lipid-activated transcription factor. Cell. 1994;79(7):1147–56.
•• Wu M, Wang Y, Shao J, Wang J, Chen W, Li Y. Cbfβ governs osteoblast−adipocyte lineage commitment through enhancing β-catenin signaling and suppressing adipogenesis gene expression. Proc Natl Acad Sci. 2017;114(38):10119–24. https://doi.org/10.1073/pnas.1619294114. This research suggests that the osteoblast lineage commitment is regulated by core-binding factor subunit beta (Cbfβ) through enhancing β-catenin signaling in mesenchymal stem cells.
Post S, Abdallah BM, Bentzon JF, Kassem M. Demonstration of the presence of independent pre-osteoblastic and pre-adipocytic cell populations in bone marrow-derived mesenchymal stem cells. Bone. 2008;43(1):32–9. https://doi.org/10.1016/j.bone.2008.03.011.
Crossno JJ, Majka SM, Grazia T, Gill RG, Klemm DJ. Rosiglitazone promotes development of a novel adipocyte population from bone marrow-derived circulating progenitor cells. J Clin Invest. 2006;116(12):3220–8. https://doi.org/10.1172/JCI28510.
Seale P, Bjork B, Yang W, Kajimura S, Chin S, Kuang S, et al. PRDM16 controls a brown fat/skeletal muscle switch. Nature. 2008;454(7207):961–7. https://doi.org/10.1038/nature07182.
Wan Y, Chong LW, Evans RM. PPAR-gamma regulates osteoclastogenesis in mice. Nat Med. 2007;13(12):1496–503. https://doi.org/10.1038/nm1672.
Iwamoto I, Fujino T, Douchi T. The leptin receptor in human osteoblasts and the direct effect of leptin on bone metabolism. Gynecol Endocrinol. 2004;19(2):97–104.
Kapur S, Amoui M, Kesavan C, Wang X, Mohan S, Baylink DJ, et al. Leptin receptor (Lepr) is a negative modulator of bone mechanosensitivity and genetic variations in Lepr may contribute to the differential osteogenic response to mechanical stimulation in the C57BL/6J and C3H/HeJ pair of mouse strains. J Biol Chem. 2010;285(48):37607–18. https://doi.org/10.1074/jbc.M110.169714.
Cornish J, Callon KE, Bava U, Lin C, Naot D, Hill BL, et al. Leptin directly regulates bone cell function in vitro and reduces bone fragility in vivo. J Endocrinol. 2002;175(2):405–15.
Turner RT, Kalra SP, Wong CP, Philbrick KA, Lindenmaier LB, Boghossian S, et al. Peripheral leptin regulates bone formation. J Bone Miner Res. 2013;28(1):22–34. https://doi.org/10.1002/jbmr.1734.
Jurimae J, Jurimae T, Leppik A, Kums T. The influence of ghrelin, adiponectin, and leptin on bone mineral density in healthy postmenopausal women. J Bone Miner Metab. 2008;26(6):618–23. https://doi.org/10.1007/s00774-008-0861-5.
Barbour KE, Zmuda JM, Boudreau R, Strotmeyer ES, Horwitz MJ, Evans RW, et al. Adipokines and the risk of fracture in older adults. J Bone Miner Res. 2011;26(7):1568–76. https://doi.org/10.1002/jbmr.361.
Motyl KJ, Rosen CJ. Understanding leptin-dependent regulation of skeletal homeostasis. Biochimie. 2012;94(10):2089–96. https://doi.org/10.1016/j.biochi.2012.04.015.
Lecka-Czernik B. Marrow fat metabolism is linked to the systemic energy metabolism. Bone. 2012;50(2):534–9. https://doi.org/10.1016/j.bone.2011.06.032.
Philbrick KA, Wong CP, Branscum AJ, Turner RT, Iwaniec UT. Leptin stimulates bone formation in ob/ob mice at doses having minimal impact on energy metabolism. J Endocrinol. 2017;232(3):461–74. https://doi.org/10.1530/JOE-16-0484.
Berner HS, Lyngstadaas SP, Spahr A, Monjo M, Thommesen L, Drevon CA, et al. Adiponectin and its receptors are expressed in bone-forming cells. Bone. 2004;35(4):842–9. https://doi.org/10.1016/j.bone.2004.06.008.
Pacheco-Pantoja EL, Waring VJ, Wilson PJ, Fraser WD, Gallagher JA. Adiponectin receptors are present in RANK-L-induced multinucleated osteoclast-like cells. J Recept Signal Transduct Res. 2013;33(5):291–7. https://doi.org/10.3109/10799893.2013.828070.
Barbour KE, Zmuda JM, Boudreau R, Strotmeyer ES, Horwitz MJ, Evans RW, et al. The effects of adiponectin and leptin on changes in bone mineral density. Osteoporos Int. 2012;23(6):1699–710. https://doi.org/10.1007/s00198-011-1768-x.
Cawthorn WP, Scheller EL, Learman BS, Parlee SD, Simon BR, Mori H, et al. Bone marrow adipose tissue is an endocrine organ that contributes to increased circulating adiponectin during caloric restriction. Cell Metab. 2014;20(2):368–75. https://doi.org/10.1016/j.cmet.2014.06.003.
Pararasa C, Bailey CJ, Griffiths HR. Ageing, adipose tissue, fatty acids and inflammation. Biogerontology. 2015;16(2):235–48. https://doi.org/10.1007/s10522-014-9536-x.
During A, Penel G, Hardouin P. Understanding the local actions of lipids in bone physiology. Prog Lipid Res. 2015;59:126–46. https://doi.org/10.1016/j.plipres.2015.06.002.
Elbaz A, Wu X, Rivas D, Gimble JM, Duque G. Inhibition of fatty acid biosynthesis prevents adipocyte lipotoxicity on human osteoblasts in vitro. J Cell Mol Med. 2010;14(4):982–91. https://doi.org/10.1111/j.1582-4934.2009.00751.x.
Jiang X, Song D, Ye B, Wang X, Song G, Yang S, et al. Effect of intermittent administration of adiponectin on bone regeneration following mandibular osteodistraction in rabbits. J Orthop Res. 2011;29(7):1081–5. https://doi.org/10.1002/jor.21355.
Kajimura D, Lee HW, Riley KJ, Arteaga-Solis E, Ferron M, Zhou B, et al. Adiponectin regulates bone mass via opposite central and peripheral mechanisms through FoxO1. Cell Metab. 2013;17(6):901–15. https://doi.org/10.1016/j.cmet.2013.04.009.
Naot D, Watson M, Callon KE, Tuari D, Musson DS, Choi AJ, et al. Reduced bone density and cortical bone indices in female adiponectin-knockout mice. Endocrinology. 2016;157(9):3550–61. https://doi.org/10.1210/en.2016-1059.
Naot D, Musson DS, Cornish J. The activity of adiponectin in bone. Calcif Tissue Int. 2017;100(5):486–99. https://doi.org/10.1007/s00223-016-0216-5.
Naveiras O, Nardi V, Wenzel PL, Hauschka PV, Fahey F, Daley GQ. Bone-marrow adipocytes as negative regulators of the haematopoietic microenvironment. Nature. 2009;460(7252):259–63. https://doi.org/10.1038/nature08099.
Zhao E, Xu H, Wang L, Kryczek I, Wu K, Hu Y, et al. Bone marrow and the control of immunity. Cell Mol Immunol. 2012;9(1):11–9. https://doi.org/10.1038/cmi.2011.47.
Busso N, So A, Chobaz-Peclat V, Morard C, Martinez-Soria E, Talabot-Ayer D, et al. Leptin signaling deficiency impairs humoral and cellular immune responses and attenuates experimental arthritis. J Immunol. 2002;168(2):875–82.
•• Adler BJ, Green DE, Pagnotti GM, Chan ME, Rubin CT. High fat diet rapidly suppresses B lymphopoiesis by disrupting the supportive capacity of the bone marrow niche. PLOS ONE. 2014;9(3):e90639. https://doi.org/10.1371/journal.pone.0090639. The results of this study indicate that obesity is a high risk factor for the defective leukogenesis of B cells by suppressing the expression of Il-7.
Bonomo A, Monteiro AC, Goncalves-Silva T, Cordeiro-Spinetti E, Galvani RG, Balduino A. A T Cell View Of the bone marrow. Front Immunol. 2016;7:184. https://doi.org/10.3389/fimmu.2016.00184.
Li Y, Toraldo G, Li A, Yang X, Zhang H, Qian WP, et al. B cells and T cells are critical for the preservation of bone homeostasis and attainment of peak bone mass in vivo. Blood. 2007;109(9):3839–48. https://doi.org/10.1182/blood-2006-07-037994.
Roggia C, Gao Y, Cenci S, Weitzmann MN, Toraldo G, Isaia G, et al. Up-regulation of TNF-producing T cells in the bone marrow: a key mechanism by which estrogen deficiency induces bone loss in vivo. Proc Natl Acad Sci U S A. 2001;98(24):13960–5. https://doi.org/10.1073/pnas.251534698.
McLaughlin T, Liu LF, Lamendola C, Shen L, Morton J, Rivas H, et al. T-cell profile in adipose tissue is associated with insulin resistance and systemic inflammation in humans. Arterioscler Thromb Vasc Biol. 2014;34(12):2637–43. https://doi.org/10.1161/ATVBAHA.114.304636.
Gruver AL, Ventevogel MS, Sempowski GD. Leptin receptor is expressed in thymus medulla and leptin protects against thymic remodeling during endotoxemia-induced thymus involution. J Endocrinol. 2009;203(1):75–85. https://doi.org/10.1677/JOE-09-0179.
Matarese G. Leptin and the immune system: how nutritional status influences the immune response. Eur Cytokine Netw. 2000;11(1):7–14.
Ioan-Facsinay A, Kwekkeboom JC, Westhoff S, Giera M, Rombouts Y, van Harmelen V, et al. Adipocyte-derived lipids modulate CD4+ T-cell function. Eur J Immunol. 2013;43(6):1578–87. https://doi.org/10.1002/eji.201243096.
Vandanmagsar B, Youm YH, Ravussin A, Galgani JE, Stadler K, Mynatt RL, et al. The NLRP3 inflammasome instigates obesity-induced inflammation and insulin resistance. Nat Med. 2011;17(2):179–88. https://doi.org/10.1038/nm.2279.
D'Amico L, Roato I. Cross-talk between T cells and osteoclasts in bone resorption. Bonekey Rep. 2012;1:82. https://doi.org/10.1038/bonekey.2012.82.
Liu LF, Shen WJ, Ueno M, Patel S, Kraemer FB. Characterization of age-related gene expression profiling in bone marrow and epididymal adipocytes. BMC Genomics. 2011;12:212. https://doi.org/10.1186/1471-2164-12-212.
Dib LH, Ortega MT, Fleming SD, Chapes SK, Melgarejo T. Bone marrow leptin signaling mediates obesity-associated adipose tissue inflammation in male mice. Endocrinology. 2014;155(1):40–6. https://doi.org/10.1210/en.2013-1607.
Weisberg SP, McCann D, Desai M, Rosenbaum M, Leibel RL, Ferrante AJ. Obesity is associated with macrophage accumulation in adipose tissue. J Clin Invest. 2003;112(12):1796–808. https://doi.org/10.1172/JCI19246.
Lee BC, Kim MS, Pae M, Yamamoto Y, Eberle D, Shimada T, et al. Adipose natural killer cells regulate adipose tissue macrophages to promote insulin resistance in obesity. Cell Metab. 2016;23(4):685–98. https://doi.org/10.1016/j.cmet.2016.03.002.
Gong L, Zhao Y, Zhang Y, Ruan Z. The macrophage polarization regulates MSC osteoblast differentiation in vitro. Ann Clin Lab Sci. 2016;46(1):65–71.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Jillian Cornish, Tao Wang, and Jian-Ming Lin declare no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Bone Marrow and Adipose Tissue
Rights and permissions
About this article
Cite this article
Cornish, J., Wang, T. & Lin, Jm. Role of Marrow Adipocytes in Regulation of Energy Metabolism and Bone Homeostasis. Curr Osteoporos Rep 16, 116–122 (2018). https://doi.org/10.1007/s11914-018-0425-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11914-018-0425-0