Abstract
Purpose of Review
Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS) is a recently described treatable, inflammatory, brainstem predominant encephalomyelitis. The diagnosis of CLIPPERS is challenging without a specific biomarker, and thus it is important to consider if both the clinical and radiographic features are consistent with the diagnosis, or rather a disease mimicker.
Recent Findings
Many patients with CLIPPERS-like lesions have been described in the literature with follow-up revealing a range of alternative diagnoses, such as malignancies, vasculitis, and other specific inflammatory diseases. As a result, some have proposed that CLIPPERS might represent a pre-malignancy state or simply an initial clinical syndrome of a variety of possible etiologies.
Summary
We describe the typical clinical, radiographic, and pathological features of CLIPPERS and emphasize consideration for alternative diagnoses when findings are not classic. A recommended diagnostic evaluation and initial treatment plan is provided.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS) is a brainstem predominant encephalomyelitis with punctate curvilinear post-gadolinium contrast enhancement centered in the pons and cerebellum on brain MRI, with biopsy findings consisting of prominent perivascular CD3+ T cell predominant lymphocytic inflammation, and an exquisite clinical and radiographic response to corticosteroids [1]. Since the original description of the syndrome, several other groups have reported similar cases [2, 3], supporting the existence of the syndrome. The absence of a definitive diagnostic biomarker has led to some confusion in the field, with primary central nervous system (CNS) malignancy [4, 5•, 6,7,8], systemic T cell lymphoma [9], Hodgkin’s lymphoma [10], chronic hepatitis B infection [11], myelin oligodendrocyte glycoprotein (MOG) antibodies [12], CNS lymphomatoid granulomatosis [13], and multiple sclerosis (MS) [14, 15] all being described in association with neuroimaging features similar to CLIPPERS. The purpose of this review is to summarize the clinical, radiological, and pathological features of CLIPPERS and to describe a suggested evaluation and treatment plan when faced with a patient with suspected CLIPPERS.
Clinical Findings
CLIPPERS is a brainstem predominant encephalomyelitis, with clinical and radiographic features predominating in the pons and cerebellum. Given this predilection, it is not surprising that the most common clinical features include gait ataxia, diplopia, dysarthria, and altered facial sensation accompanied by additional brainstem, myelopathy, and cognitive findings [2, 3, 16••]. Additional features include pseudobulbar affect [2, 17], tinnitus [2], tremor [16••, 17], nystagmus [2, 3, 16••], long-tract signs [16••, 17,18,19], paraparesis [1, 3, 16••], dizziness, nausea, and dysgeusia. Symptoms typically evolve over weeks or months. A rapid onset of symptoms progressing to severe deficits within days is atypical for CLIPPERS. The usual age of onset is in midlife, but a wide range has been reported (median 45.5 years; range 16–86 years) [1]. There is no clear gender predilection. None of the clinical characteristics commonly seen in CLIPPERS are pathognomonic; however, a predominance of clinical features that are not commonly seen in CLIPPERS at presentation or relapse, such as optic neuritis, seizures or systemic symptoms, should prompt a reevaluation of the diagnosis.
Laboratory Findings
There are no specific serum laboratory markers available to make the diagnosis of CLIPPERS. Patients with CLIPPERS have not been found to have aquaporin-4 (AQP4)-IgG, Glial fibrillary acidic protein (GFAP)-IgG, or other neural-specific autoantibodies. Laboratory testing is useful to exclude alternative diagnoses, such as HIV, vasculitis, and autoimmune glial fibrillary acidic protein (GFAP) astrocytopathy [20].
There is also no specific cerebrospinal fluid abnormality in CLIPPERS. The most common finding is a mild elevation in protein [1, 3]. Oligoclonal bands and IgG index are elevated in some cases. A highly inflammatory cerebrospinal fluid with a marked pleocytosis (>150 total nucleated cells/mcL), marked elevation in protein, and/or hypoglycorhacia should prompt consideration of an alternative diagnosis.
Neuroimaging
Brain MRI in CLIPPERS is characterized by punctate, curvilinear post-gadolinium enhancement centered in the pons and cerebellum [1, 3, 16••, 21, 22]. Most lesions are less than 3 mm in diameter, and larger asymmetric lesions should prompt evaluation for alternate diagnoses. Lesions become less numerous further away from the pons, but can extend into the cerebral hemispheres and spinal cord. The area of T2-hyperintensity tends to be similar to the area of post-gadolinium enhancement, as shown in Fig. 1. Despite significant clinical disability, T2 and T2-FLAIR images may be relatively unrevealing, with lesions readily apparent on post-gadolinium T1-weighted images [3]. Published cases of CLIPPERS-like MRI features which have ultimately had an alternate diagnosis have included patients with pial enhancement and both clinical and radiological worsening on corticosteroid treatment [23]; asymmetric contrast-enhancing lesions with a larger area of T2 hyperintensity than post-gadolinium enhancement [5•, 6]; and larger, asymmetric areas of contrast enhancement than previously described [4], underscoring the necessity of only considering “typical” MRI features as being compatible with CLIPPERS.
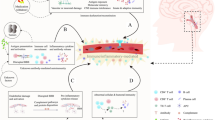
Imaging examples differentiating CLIPPERS from alternative diagnoses. Typical MRI examples of CLIPPERS (A–C), and examples of imaging that is not consistent with CLIPPERS (D–F). Each T2-FLAIR image (A1–F1) is accompanied by T1-weighted post-gadolinium image (A2–F2). CLIPPERS demonstrated by symmetric punctate and curvilinear gadolinium enhancement centered in the pons and cerebellum with a relative paucity of T2-FLAIR signal that does not extended far beyond the enhancement (A–C). Imaging findings of significant asymmetry (D), gadolinium enhancement that is confluent and not punctate (E), and T2-FLAIR signal that extends far beyond the associated area of contrast enhancement (F) are not typical of CLIPPERS and warrant strong consideration of an alternative diagnosis
Lesion distribution outside of the pons and adjacent brainstem with extension through the basal ganglia and spinal cord (cervical and thoracic) can be seen [1], and the lesion burden tends to be lower further away from the pons and cerebellum. More extensive areas of involvement have been described, including bilateral posterior limbs of the internal capsule [19], thalamus [3], diffuse gadolinium peppering throughout the white matter of the entire brain (including the cortico-subocortical region) [24, 25], and extensive cervical [18] and thoracic spinal cord involvement [19, 26].
Responsiveness to corticosteroids constitutes a key element of the diagnosis of CLIPPERS. In the majority of cases, the enhancing lesions tend to resolve completely within weeks following treatment with corticosteroids, although lesions may recur if corticosteroids are withdrawn. If rapid resolution of enhancement is not seen after corticosteroids, the working diagnosis of CLIPPERS should be reconsidered [4]. Worsening of enhancement during corticosteroid treatment, a lack of robust radiological response, a change in the predominant imaging pattern, or a significantly different area of involvement on follow-up imaging should prompt consideration of alternative etiologies [6].
Cerebellar atrophy and generalized cerebral atrophy have been observed, despite resolution of contrast-enhancing lesions with treatment, and more pronounced atrophy has been associated with persistent cognitive impairment [17]. Brainstem and spinal cord atrophy have also been seen in CLIPPERS [2].
The role of advanced imaging techniques in the diagnosis of CLIPPERS is uncertain. MR spectroscopy (MRS) [6] and cerebral angiography [3] may be helpful in identifying patients with alternate diagnoses such as lymphoma or vasculitis.
Neuropathology
No pathological hallmark has been identified for the diagnosis of CLIPPERS. As such, the primary reason to perform a brain biopsy is to exclude findings concerning for an alternative diagnosis. Specifically, findings consistent with vasculitis, granulomatous disease, infection, malignancy, or other neuroimflammatory disease should not be seen. The eloquent nature of areas typically involved in CLIPPERS has led to reticence to recommend biopsy in all patients with CLIPPERS [27]. However, in carefully selected patients at centers that perform a high volume of posterior fossa biopsies, the operative risk is similar to hemispheric biopsies [28•].
Pathological findings in CLIPPERS are defined by perivascular inflammation with CD3 reactive T lymphocytes (predominantly CD4 positive), activated microglia, CD68 positive histiocytes, and a lesser degree of accompanying CD20 positive B lymphocytes [1]. The lack of granulomas and lymphocyte clonality on biopsy in patients with CLIPPERS is felt to reasonably exclude lymphomatoid granulomatosis (LYG) at the initial diagnosis [3]. However, perivascular T cell infiltrates can also be seen in primary CNS lymphoma sentinel lesions and grade I LYG, indicating that the typical pathological findings in CLIPPERS as reported to date are non-specific and require complete clinical assessment and follow-up to secure the diagnosis of CLIPPERS [29]. An important consideration is that corticosteroid treatment before biopsy and sampling error may alter the diagnostic accuracy and lead to non-specific inflammatory findings on brain pathology for some diseases, such as CNS lymphoma [30, 31].
Response to Treatment
A robust clinical and radiological response to corticosteroid treatment is a classic feature of CLIPPERS. This finding is not specific though, as other inflammatory and neoplastic disorders often respond to corticosteroids. Recrudescence of symptoms with post-gadolinium enhancement on brain MRI is the norm in the absence of prolonged treatment and with low doses of corticosteroids (≤ 20 mg prednisone daily) [2]. Symptoms of relapse related to CLIPPERS are similar to those of the initial presentation. Depending on the degree of deficits and duration of untreated disease, not all patients have complete clinical recovery. Most patients should have absence of gadolinium-enhancing lesions on brain MRI within weeks of commencing corticosteroids.
Red Flags for Alternate Conditions
Perhaps more important than recognizing the typical features of CLIPPERS, a clinician should be aware of findings that raise concern for an alternative diagnosis. Some of the most commonly encountered clinical red flags when considering CLIPPERS include lack of significant response to corticosteroids, lack of typical brainstem predominant findings, progression to severe deficits within days, fever or marked B symptoms, early-onset of seizures, depressed level of consciousness, and any other findings localizing outside the CNS. Although atypical cases of CLIPPERS have been reported with suspected peripheral nerve [19], cutaneous [32•], pulmonary [9], salivary gland [17], and ocular involvement [17], diagnosis of atypical CLIPPERS may lead to overdiagnosis in the absence of a specific diagnostic biomarker. Brain MRI lesions with significant edema or mass effect, normal neuroimaging while symptomatic, and ring-enhancing brain lesions are all inconsistent with CLIPPERS [2]. Although in some cases an asymmetric lesion distribution can occur, significant asymmetry is suggestive of an alternate process [5•]. Cortical, leptomeningeal, dural, and hypothalamic-pituitary lesion locations on MRI are not currently recognized as features of CLIPPERS [33••].
Pathogenesis
The underlying pathogenesis of CLIPPERS is unclear. A neoplastic or paraneoplastic etiology has been proposed, following association of some reported cases of CLIPPERS with malignancy [9, 22, 34]. The majority of cases do not have a malignancy, however, either at presentation or follow-up. A neural autoantibody marker has not been found in CLIPPERS. Vasculitis has similarly been proposed as the etiology; however, this is not supported by pathological evidence in the majority of cases. A temporal relation to vaccination [35] and herpes zoster reactivation [36] in two separate cases is supportive of an inflammatory etiology. The predominance of CD4 positive T cells and the response to immunotherapy is also supportive of an inflammatory cause [37]. In the absence of a definitive biomarker, CLIPPERS as currently understood may represent more of a syndrome rather than a unique disease [38].
Diagnostic Evaluation
A suggested initial evaluation of patients with suspected CLIPPERS is outlined in Table 1. The differential diagnosis depends on the clinical and imaging findings for a given case. Specific diagnoses to be considered include vasculitis, CNS lymphoma, intravascular lymphoma, lymphomatoid granulomatosis, neurosarcoidosis, CNS demyelinating disease, hemophagocytic lymphohistiocytosis, Behçet’s disease, chronic perivascular infections (tuberculosis, neurosyphilis, Whipple’s disease), autoimmune GFAP astrocytopathy [20], Erdheim-Chester disease, and Langerhans cell histiocytosis [33••]. With no definitive biomarker for CLIPPERS, consideration should be given to brain biopsy prior to initial treatment. This serves primarily to exclude CNS malignancies and vasculitis which may require a different treatment approach.
Suggested Treatment Strategy
Once the diagnosis of CLIPPERS is confirmed, treatment is recommended with high-dose corticosteroids. Typical initial treatment is IV methylprednisolone 1 g daily for 5 days. Treatment thereafter should be continued with 1 mg/kg of oral prednisone daily with appropriate precautions regarding infection prevention including PCP prophylaxis, osteoporosis prevention, and weight management. Once the expected clinical and radiological improvement with corticosteroids has been achieved, the authors typically treat with a steroid-sparing agent, such as methotrexate (target dose of 22.5 mg weekly), azathioprine (2.5 mg/kg per day), or mycophenolate mofetil (2 g per day in divided doses). Patients should remain on oral prednisone at doses ≥20 mg per day until the steroid-sparing therapy is therapeutic. Intravenous immunoglobulin does not appear effective for CLIPPERS [24]. The total duration of appropriate immunotherapy in CLIPPERS is unclear, but patients should remain on therapy at least until the disappearance of enhancing lesions. The authors typically treat for a minimum of 12 months prior to withdrawing immunotherapy. Careful monitoring with brain MRI should be performed following treatment cessation.
Future Directions
The CLIPPERS syndrome is well characterized. A consensus on diagnostic criteria is necessary to facilitate research on the etiology and treatment of the condition. Identification of a reliable biomarker is crucial to better understand the spectrum of CLIPPERS, increase diagnostic specificity, and ultimately lead to improved treatment and clinical outcomes.
Conclusion
CLIPPERS is a recently described inflammatory disorder of the CNS with characteristic clinical, radiological, and pathological findings. Diagnosis requires exclusion of other mimicking diseases, and brain biopsy should be considered. Clinical and radiographic responsiveness to corticosteroids is necessary for the diagnosis, although clinical response may be incomplete. Patients typically require prolonged immunotherapy for best outcomes.
References
Papers of particular interest, published recently, have been highlighted as: • Of importance •• Of major importance
Pittock SJ, Debruyne J, Krecke KN, Giannini C, van den Ameele J, De Herdt V, et al. Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS). Brain : a journal of neurology. 2010;133(9):2626–34.
Taieb G, Duflos C, Renard D, Audoin B, Kaphan E, Pelletier J, et al. Long-term outcomes of CLIPPERS (chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids) in a consecutive series of 12 patients. Arch Neurol. 2012;69(7):847–55.
Kastrup O, van de Nes J, Gasser T, Keyvani K. Three cases of CLIPPERS: a serial clinical, laboratory and MRI follow-up study. J Neurol. 2011;258(12):2140–6.
Jones JL, Dean AF, Antoun N, Scoffings DJ, Burnet NG, Coles AJ. ‘Radiologically compatible CLIPPERS’ may conceal a number of pathologies. Brain : a journal of neurology. 2011;134(Pt 8):e187.
• De Graaff HJ, Wattjes MP, Rozemuller-Kwakkel AJ, Petzold A, Killestein J. Fatal B-cell lymphoma following chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids. JAMA neurology. 2013;70(7):915–8. This case is one of several demonstrating that inflammatory brainstem lesions on MRI are not unique to CLIPPERS, and can be seen in several alternative etiologies including lymphoma, and thus a patient should be assessed for all of the typical neuroimaging and clinical findings of CLIPPERS before establishing the diagnosis.
Limousin N, Praline J, Motica O, Cottier JP, Rousselot-Denis C, Mokhtari K, et al. Brain biopsy is required in steroid-resistant patients with chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS). J Neuro-Oncol. 2012;107(1):223–4.
Lin AW, Das S, Fraser JA, Ang LC, Florendo-Cumbermack A, Jenkins ME, et al. Emergence of primary CNS lymphoma in a patient with findings of CLIPPERS. The Canadian journal of neurological sciences Le journal canadien des sciences neurologiques. 2014;41(4):528–9.
Taieb G, Uro-Coste E, Clanet M, Lassmann H, Benouaich-Amiel A, Laurent C, et al. A central nervous system B-cell lymphoma arising two years after initial diagnosis of CLIPPERS. J Neurol Sci. 2014;344(1–2):224–6.
Nakamura R, Ueno Y, Ando J, Matsuda H, Masuda A, Iiduka K, et al. Clinical and radiological CLIPPERS features after complete remission of peripheral T-cell lymphoma, not otherwise specified. J Neurol Sci. 2016;364:6–8.
Mashima K, Suzuki S, Mori T, Shimizu T, Yamada S, Hirose S, et al. Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS) after treatment for Hodgkin’s lymphoma. Int J Hematol. 2015;102(6):709–12.
Weng CF, Chan DC, Chen YF, Liu FC, Liou HH. Chronic hepatitis B infection presenting with chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS): a case report. J Med Case Rep. 2015;9:266.
Symmonds M, Waters PJ, Kuker W, Leite MI, Schulz UG. Anti-MOG antibodies with longitudinally extensive transverse myelitis preceded by CLIPPERS. Neurology. 2015;84(11):1177–9.
Wang X, Huang D, Huang X, Zhang J, Ran Y, Lou X, et al. Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS): a lymphocytic reactive response of the central nervous system? A case report. J Neuroimmunol. 2017;305:68–71.
Ferreira RM, Machado G, Souza AS, Lin K, Correa-Neto Y. CLIPPERS-like MRI findings in a patient with multiple sclerosis. J Neurol Sci. 2013;327(1–2):61–2.
Ortega MR, Usmani N, Parra-Herran C, Adams DJ, Steingo B, Rammohan KW. CLIPPERS complicating multiple sclerosis causing concerns of CNS lymphoma. Neurology. 2012;79(7):715–6.
•• Blaabjerg M, Ruprecht K, Sinnecker T, Kondziella D, Niendorf T, Kerrn-Jespersen BM, et al. Widespread inflammation in CLIPPERS syndrome indicated by autopsy and ultra-high-field 7T MRI. Neurology(R) neuroimmunology & neuroinflammation. 2016;3(3):e226. This paper demonstrates the presence of inflammatory pathology outside of the originally described areas centered in the pons and cerebellum in CLIPPERS.
Simon NG, Parratt JD, Barnett MH, Buckland ME, Gupta R, Hayes MW, et al. Expanding the clinical, radiological and neuropathological phenotype of chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS). J Neurol Neurosurg Psychiatry. 2012;83(1):15–22.
Biotti D, Deschamps R, Shotar E, Maillart E, Obadia M, Mari I, et al. CLIPPERS: chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids. Pract Neurol. 2011;11(6):349–51.
Tohge R, Nagao M, Yagishita A, Matsubara S. A case of chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids (CLIPPERS) in East Asia. Internal medicine (Tokyo, Japan). 2012;51(9):1115–9.
Fang B, McKeon A, Hinson SR, Kryzer TJ, Pittock SJ, Aksamit AJ, et al. Autoimmune glial fibrillary acidic protein astrocytopathy: a novel meningoencephalomyelitis. JAMA neurology. 2016;73(11):1297–307.
Kleinschmidt-DeMasters BK, West M. CLIPPERS with chronic small vessel damage: more overlap with small vessel vasculitis? J Neuropathol Exp Neurol. 2014;73(3):262–7.
Tan BL, Agzarian M, Schultz DW. CLIPPERS: induction and maintenance of remission using hydroxychloroquine. Neurology(R) neuroimmunology & neuroinflammation. 2015;2(1):e56.
Alsherbini K, Beinlich B, Salamat MS. Diffusely infiltrating central nervous system lymphoma involving the brainstem in an immune-competent patient. JAMA neurology. 2014;71(1):110–1.
Gabilondo I, Saiz A, Graus F, Villoslada P. Response to immunotherapy in CLIPPERS syndrome. J Neurol. 2011;258(11):2090–2.
Gul M, Chaudhry AA, Chaudhry AA, Sheikh MA, Carsons S. Atypical presentation of CLIPPERS syndrome: a new entity in the differential diagnosis of central nervous system rheumatologic diseases. Journal of clinical rheumatology : practical reports on rheumatic & musculoskeletal diseases. 2015;21(3):144–8.
Zhang YX, Hu HT, Ding XY, Chen LH, Du Y, Shen CH, et al. CLIPPERS with diffuse white matter and longitudinally extensive spinal cord involvement. Neurology. 2016;86(1):103–5.
Keegan BM, Pittock SJ. Cutting-edge questions about CLIPPERS (chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids). Arch Neurol. 2012;69(7):819–20.
• Tobin WO, Meyer FB, Keegan BM. Diagnostic yield and safety of cerebellar and brainstem parenchymal biopsy. World neurosurgery. 2015;84(6):1973–6. This paper provides the safety and yield of posterior fossa biopsy in patients with presumed non-malignant brain disease, as is typical in patients with CLIPPERS.
Taieb G, Renard D, Labauge P. Should CLIPPERS be considered a prelymphoma state or a new inflammatory disease? JAMA neurology. 2013;70(9):1200–1.
Binnahil M, Au K, Lu JQ, Wheatley BM, Sankar T. The influence of corticosteroids on diagnostic accuracy of biopsy for primary central nervous system lymphoma. The Canadian journal of neurological sciences Le journal canadien des sciences neurologiques. 2016;43(5):721–5.
Porter AB, Giannini C, Kaufmann T, Lucchinetti CF, Wu W, Decker PA, et al. Primary central nervous system lymphoma can be histologically diagnosed after previous corticosteroid use: a pilot study to determine whether corticosteroids prevent the diagnosis of primary central nervous system lymphoma. Ann Neurol. 2008;63(5):662–7.
• Smith A, Matthews Y, Kossard S, Turner J, Buckland ME, Parratt J. Neurotropic T-cell lymphocytosis: a cutaneous expression of CLIPPERS. J Cutan Pathol. 2014;41(8):657–62. This case raises the important awareness of the non-specific pathological findings of perivascular lymphocytic predominant inflammation in CLIPPERS, which can also be seen in systemic inflammatory and neoplastic diseases.
•• Taieb G, Duran-Pena A, de Chamfleur NM, Moulignier A, Thouvenot E, Allou T, et al. Punctate and curvilinear gadolinium enhancing lesions in the brain: a practical approach. Neuroradiology. 2016;58(3):221–35. The authors review the important concept that punctate and curvilinear gadolinium enhancement is not unique to CLIPPERS, but rather there is a broad differential for these neuroimaging findings which depends heavily on the clinical context.
Taieb G, Renard D, Joujoux JM, Labauge P. Cutaneous lesions in a CLIPPERS patient: further confusion between CLIPPERS and grade I lymphomatoid granulomatosis. J Cutan Pathol. 2014;41(9):759–60.
Hillesheim PB, Parker JR, Parker JC Jr, Escott E, Berger JR. Chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids following influenza vaccination. Archives of pathology & laboratory medicine. 2012;136(6):681–5.
Wang L, Holthaus EA, Jimenez XF, Tavee J, Li Y. MRI evolution of CLIPPERS syndrome following herpes zoster infection. J Neurol Sci. 2015;348(1–2):277–8.
Dudesek A, Rimmele F, Tesar S, Kolbaske S, Rommer PS, Benecke R, et al. CLIPPERS: chronic lymphocytic inflammation with pontine perivascular enhancement responsive to steroids. Review of an increasingly recognized entity within the spectrum of inflammatory central nervous system disorders. Clin Exp Immunol. 2014;175(3):385–96.
Kira J. The expanding phenotype of CLIPPERS: is it a disease or a syndrome? J Neurol Neurosurg Psychiatry. 2012;83(1):2–3.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Nicholas L. Zalewski and W. Oliver Tobin declare that they have no conflict of interest.
Human and Animal Rights and Informed Consent
This article does not contain any studies with human or animal subjects performed by any of the authors.
Additional information
This article is part of the Topical Collection on Demyelinating Disorders
Rights and permissions
About this article
Cite this article
Zalewski, N.L., Tobin, W.O. CLIPPERS. Curr Neurol Neurosci Rep 17, 65 (2017). https://doi.org/10.1007/s11910-017-0773-7
Published:
DOI: https://doi.org/10.1007/s11910-017-0773-7